Bone and Joint EXAM 3
1/255
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
256 Terms
stem
marrow
osteoblasts
Key points about osteoprogenitor cells
- From ____ cells
- Reside in the _____
- Give rise to the _____
Produce and mineralize bone
what is the function of osteoblasts
osteoblast; lacuna
mechanical
Osteocyte
- An ______ that is completely embedded in the bone matrix in a _____
- Is responsible for detecting and responding to ______ forces
resorption
mineralized
Osteoclasts
- Bone _____
- Only reabsorb _____ bone
macrophages
what type of cell are osteoclasts similar to
- epiphysis
- metaphysis
- diaphysis
what are the 3 compartments of long bone
Epiphysis
- From subarticular bone plate to the growth plate
- Source of red marrow, site of erythropoiesis
- Location of articulation at the tip of long bone
Metaphysis
- From the growth plate to the area where the bone develops its fluted shape
- Responsible for linear growth
- After ossification important for mechanical load
Diaphysis
- Shaft or "body" of the bone between the 2 metaphyses
- hollow; contains the bone medulla, which houses yellow marrow
periosteum and endosteum
what are the two layers of bone
periosteum of bone
- Fibrous capsule covering the bone
- Provides innervation, circulation and nutrition (esp. to outer 1/3)
endosteum of bone
- Inner surface of bone
- Typically in contact with bone marrow
osteoprogenitor cells
what can be found in both the periosteum and endosteum
Involved in fracture healing and bone growth
what is role of osteoprogenitor cells found the in periosteum and endosteum
- compact bone
- cancellous bone (spongy bone)
what are the 2 Structural Types of Bone
compact bone
- Dense (AKA "cortical"); the outer shell that defines the shape of the bone
- 80% of the adult skeleton
- Shafts and around cancellous bone at the end of joints
cancellous bone
- "trabecular," "spongy" bone
- At ends of long bones within the medullary canal, in vertebrae, and in flat bones
- MANY more bone cells than compact bone
cancellous bone
- Reduces impact of strong external forces
- Leaves space for hematopoeisis
the trabecula
what is the basic unit of cancellous bone
Femoral head and condyles
what are examples of trabecula
lamellar bone
- Parallel alternating arrangement of Type I collagen fibers that are highly organized to provide strength to bone
- Normal adult skeleton will ONLY have this
- Cortical and trabecular bone have this pattern
- Manufactured slowly
woven bone
- Irregular arrangement of Type I collagen
- Numerous osteocytes in the matrix
- Haphazardly arranged collagen causing low tensile strength
- acts as a scaffolding
- Rapidly produced
- Found in the fetus, areas surrounding tumors and infections and healing fractures
- Always "pathologic" in the adult skeleton
osteon
functional unit of compact (cortical) bone
osteons
- Run parallel to the bone shaft
- Made up of the Haversian canal and the osseous lamellar bone around it
- Cylinder composed of 4 to 20 concentric lamellae arranged around a central opening
- Haversian canals
- Volkmann's canals
- Lacunae
- Canaliculi
what are the components of an osteon
Haversian canals
- Central canal of osteon containing blood vessels, lymphatics, nerves
- Run parallel to the long axis in the cortex
Volkmann's canals
- Carry blood vessels for nutrient exchange between osteons
- Connect the Haversian canals to one another and to the periosteum
- Run perpendicular to the long axis
Lacunae
small, microscopic cavities, pits, or spaces that house osteocytes
canaliculi
microscopic canals or tunnels that facilitate nutrient transport and communication between osteocytes
- Nutrient arteries
- Perforating arteries
what are the 2 types of arteries that supply blood to bone
nutrient arteries
Supply the marrow and internal 1/3 - 2/3 of the cortex
perforating arteries
- From the periosteal arteries
- They anastomose in the cortex with branches from the nutrient arteries
- Organic matrix
- Inorganic matrix
what is the Bone matrix comprised of:
organic matrix of bone
_____ matrix of bone: type I collagen secreted by osteoblasts and non-collagenous proteins
inorganic matrix of bone
______ matrix of bone
- composed primarily of a form of calcium phosphate called hydroxyapatite
- Mineral component that provides bone with its strength
hyaline
epiphyseal plate
chondrocytes
osteoblasts
Bone Growth for Length
- Main cartilage mass at end of bone is typical _____ cartilage which gets replaces with bony tissue
- The cartilage in the region of the ________ next to the epiphysis continues to grow by mitosis. The ________, in the region next to the diaphysis, age and degenerate. ________ move in and ossify the matrix to form bone.
- Cartilage proliferation
- Calcification of cartilage and then degeneration
- Bone formation on the cartilage remnants
- Resorption of bony trabecular tips
what is the order of events for the growth of bone in terms of length
periosteal; osteogenic
Bone growth for width
- Bone laid down in regular fashion at _____ surface of diaphysis by _____ cells
- Appositional growth
- Concurrent resorption of bone on inner, endosteal surface
fracture
Any deficit in the continuity of bone
fractures
what is the most common type of bone lesion
stress fractures
Fracture in normal bone that is unable to withstand repeated abnormal stress
insufficiency fracture
A Fracture as a result of normal stress applied to bone with deficient elastic resistance or has been weakened by decreased mineralization is classified as what type of fracture
pathologic fracture
A Fracture in diseased, weakened bone due to focal pathology is classified as what type of fracture
incomplete
full
Key points about stress fractures
- Stress reaction in small fracture usually _____
- Stress fracture is ___ thickness
open fracture
- AKA: Compound
- Communicate with "outside world"- dirt!
- If it breaks through the skin
closed fracture
Skin remains intact, fracture remains enclosed
open fracture
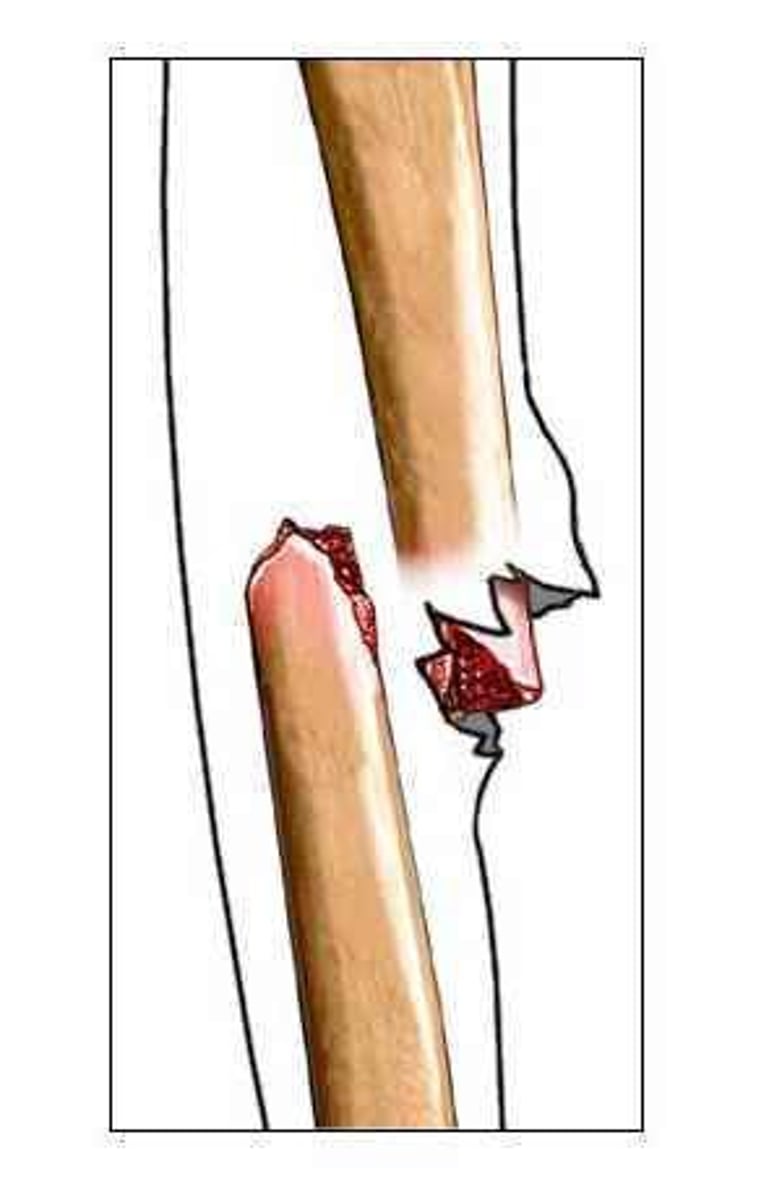
closed fracture
simple fracture
One fracture line
simple fracture

segmented fracture
Two fracture lines, resulting in "floating" piece of bone
segmented fracture
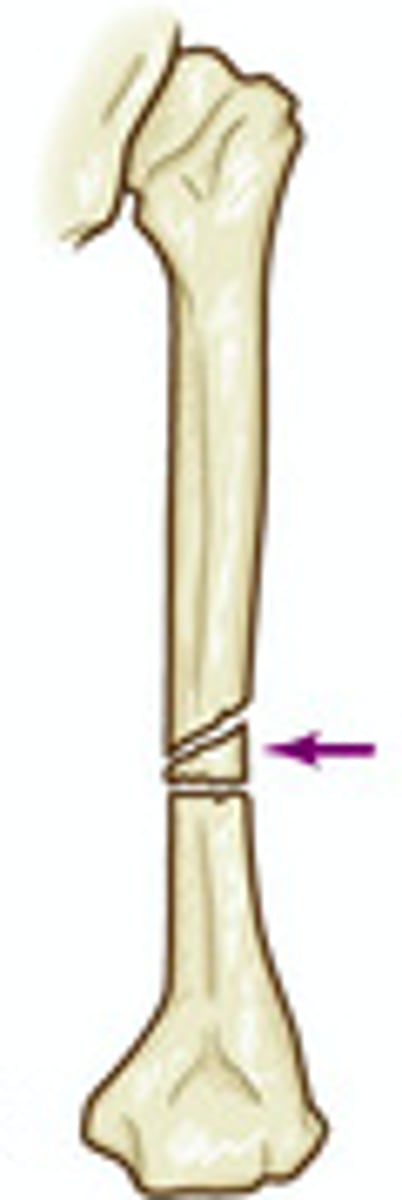
comminuted fracture
Multiple fragments at fracture site, associated with multiple fracture lines
Comminuted fracture
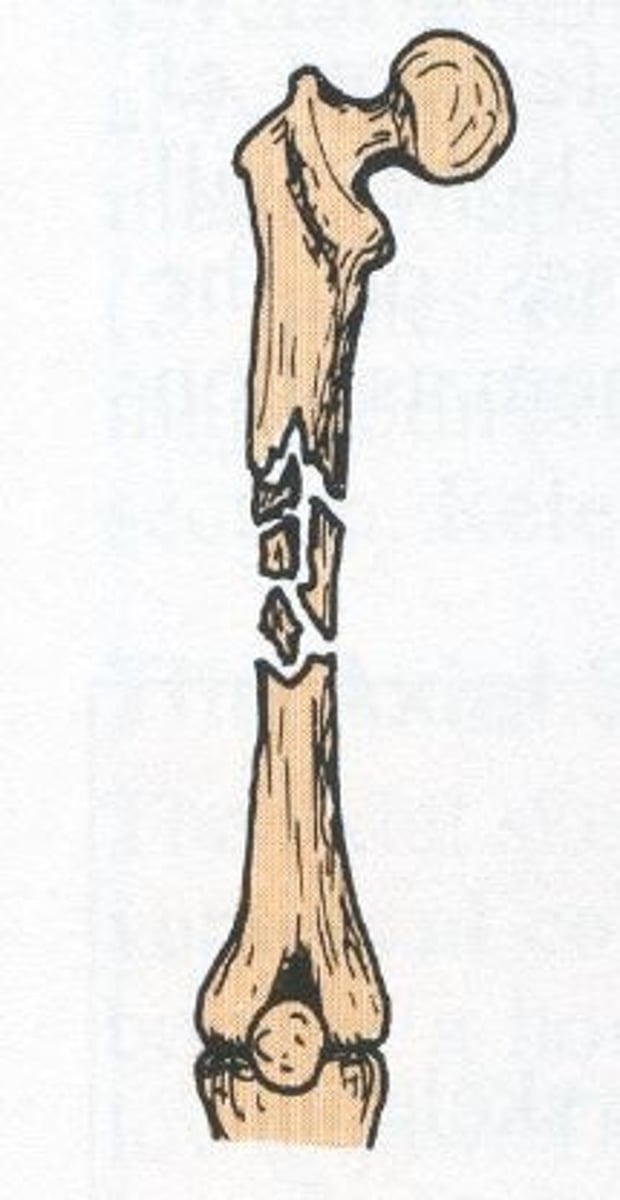
displaced fracture
Fracture associated with fragments moving out of alignment, necessitating medical realignment (reduction)
angulation fracture
distal segment tilts away from normal axis
by the position of the distal segment in relation to the proximal
how are displaced fractures named
medial displaced fracted

lateral displaced fracture
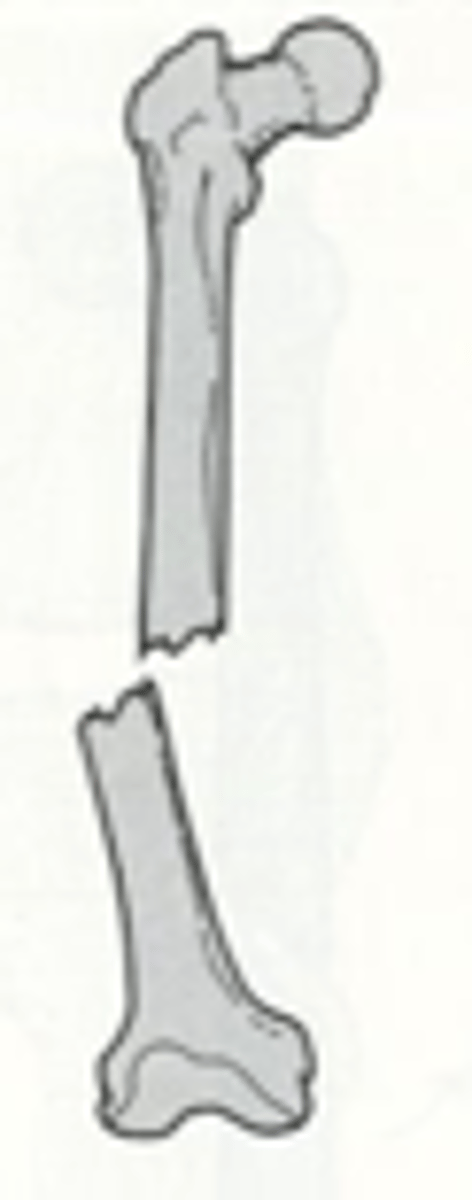
distracted displaced fracture
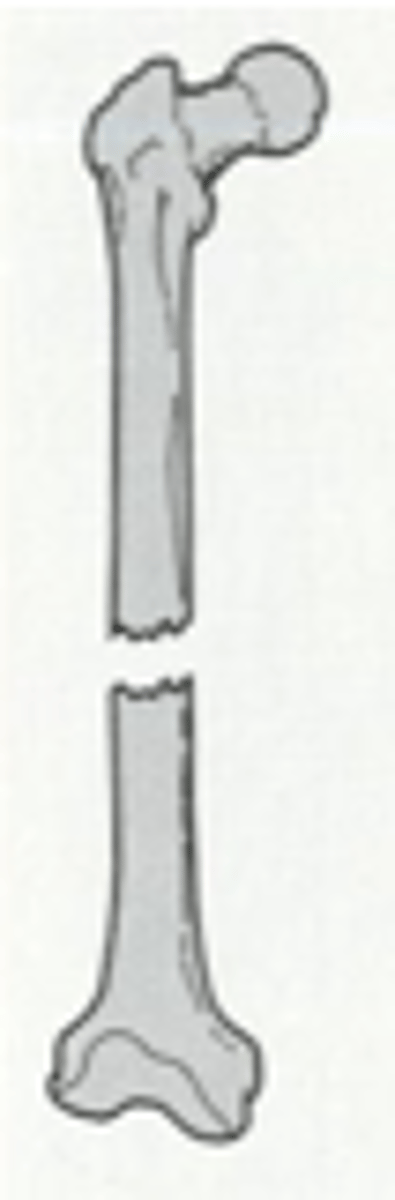
overriding with posterior and superior displacement fracture
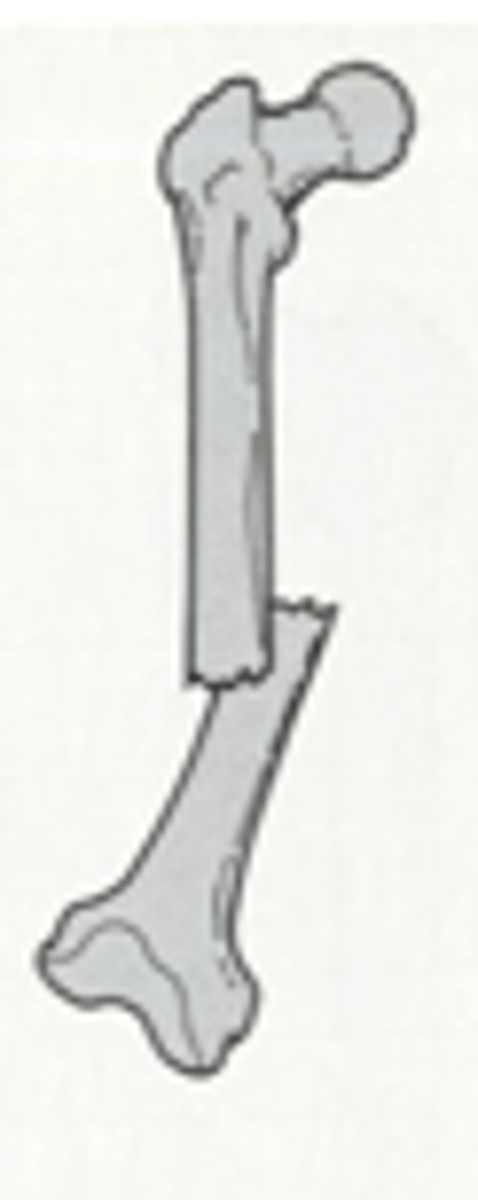
distracted and rotated laterally displacement fracture
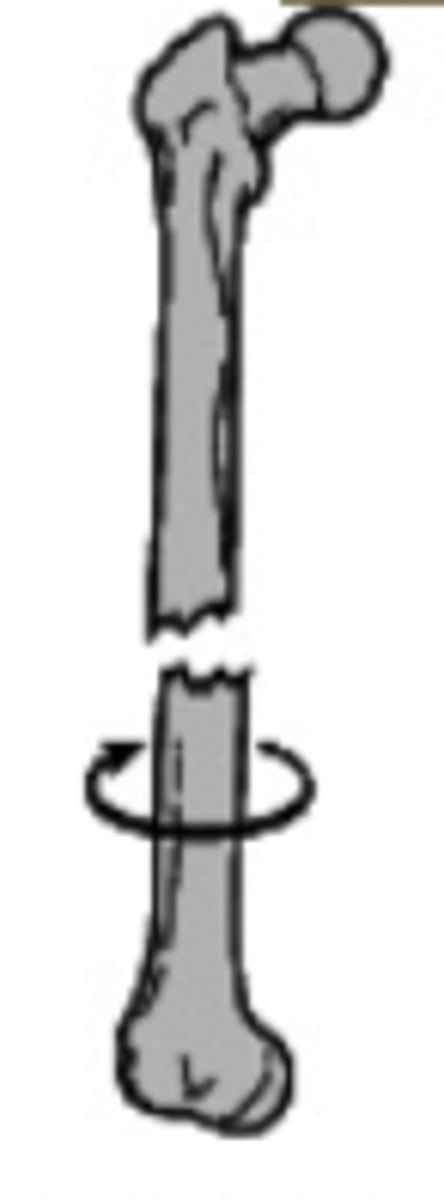
transverse fracture line
fracture is perpendicular to bone axis
transverse fracture line
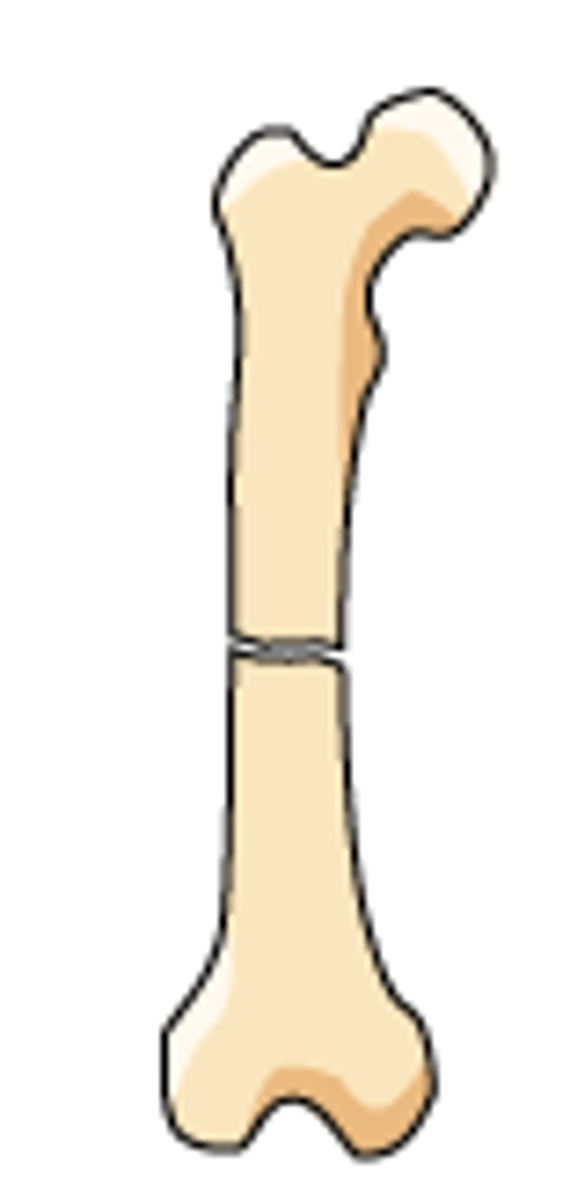
oblique fracture line
fracture occurs diagonal across bone axis
oblique fracture line
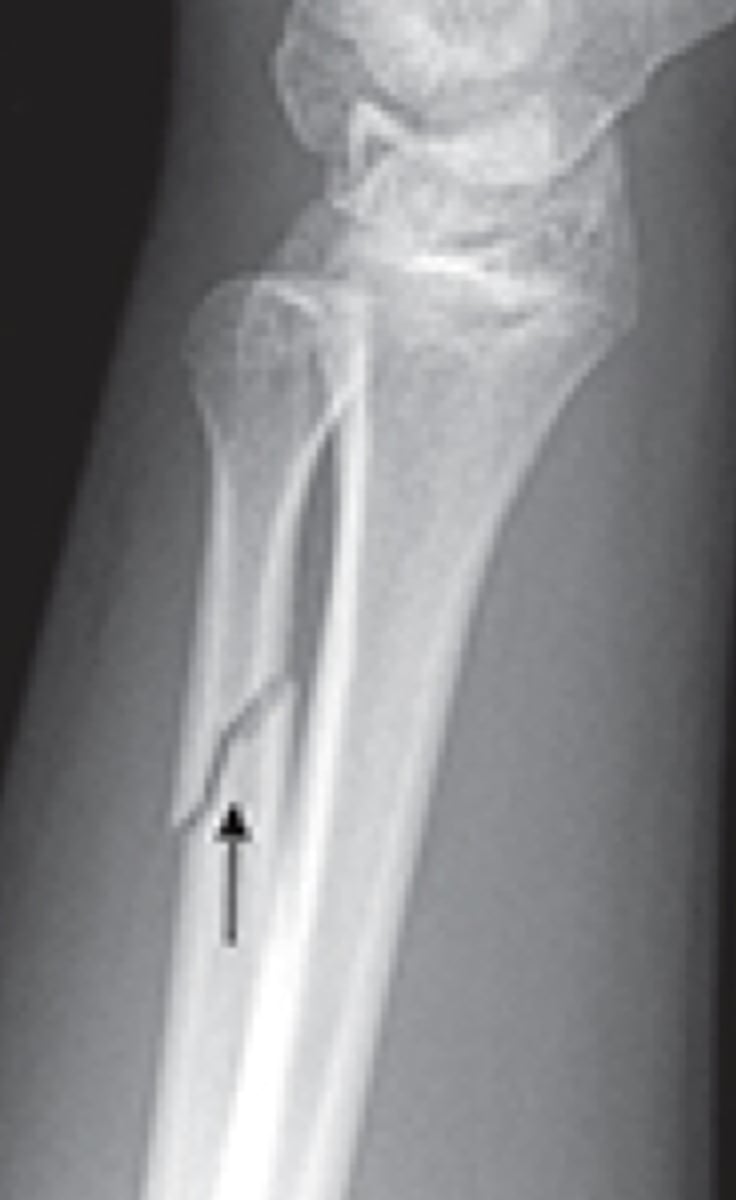
spiral fracture line
torsional fracture that spirals around bone, often due to twisting
spiral fracture line
linear/longitudinal fracture line
fracture is parallel with axis of bone
linear/longitudinal fracture line
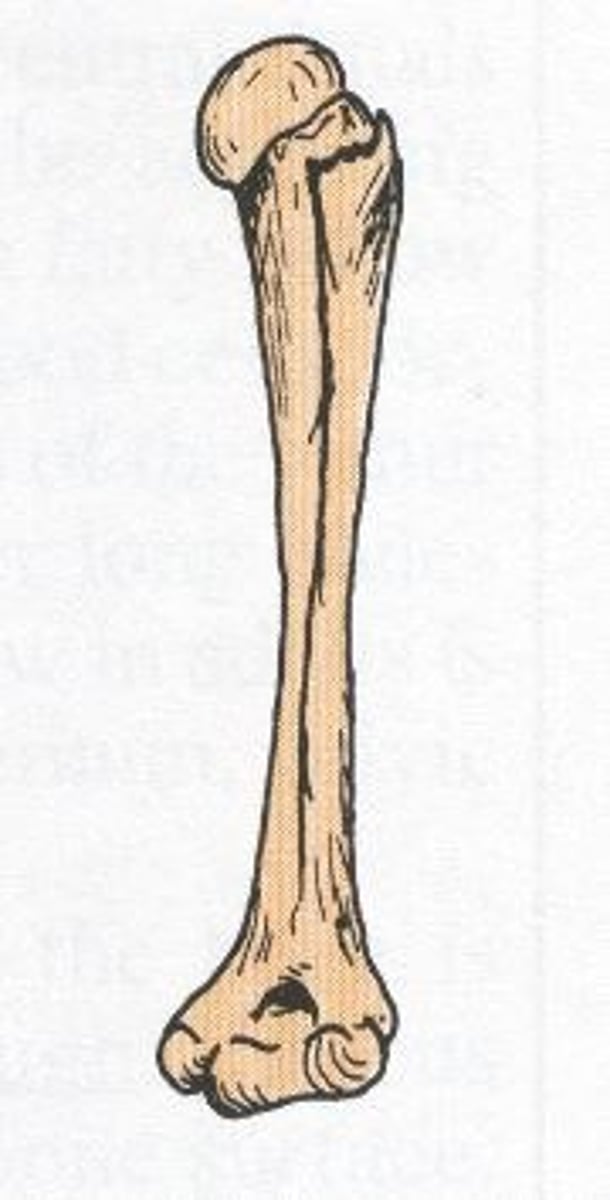
greenstick fracture
Incomplete break, causing bending of bone
greenstick fracture
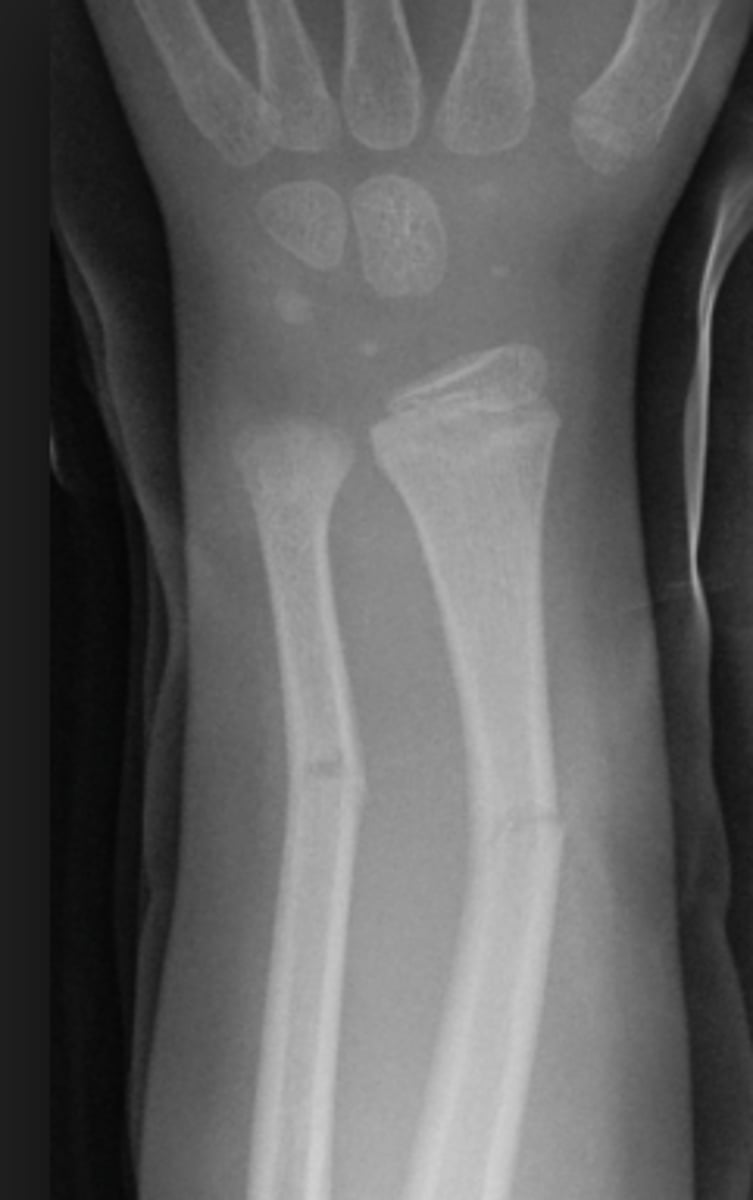
torus fracture
- AKA: impacted, buckle
- Broken bone ends driven into one another
torus fracture
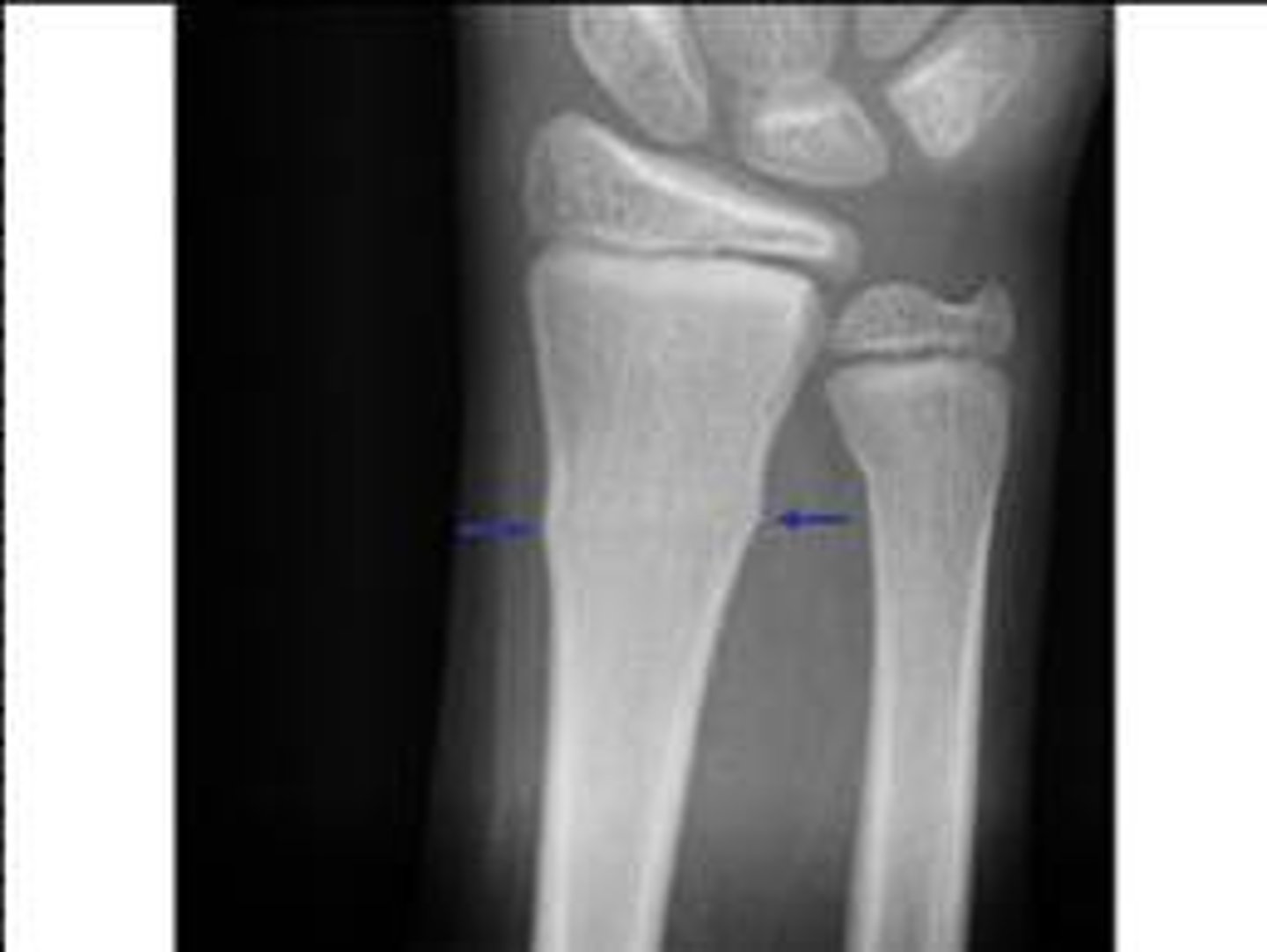
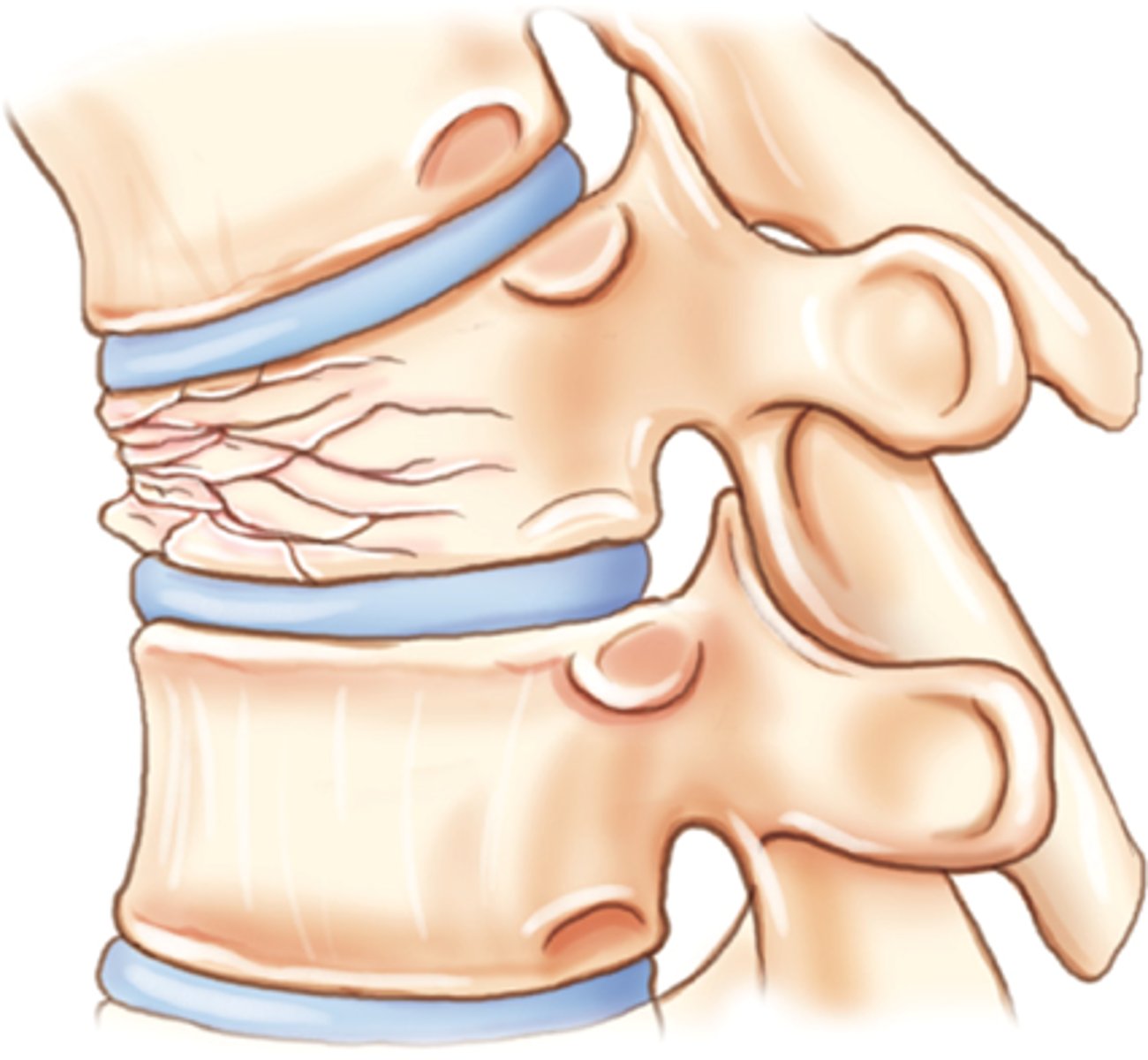
compression fracture
Crushed bone, causing wider/flatter appearance
vertebral fractures
where are compression fractures commonly seen
compression fracture
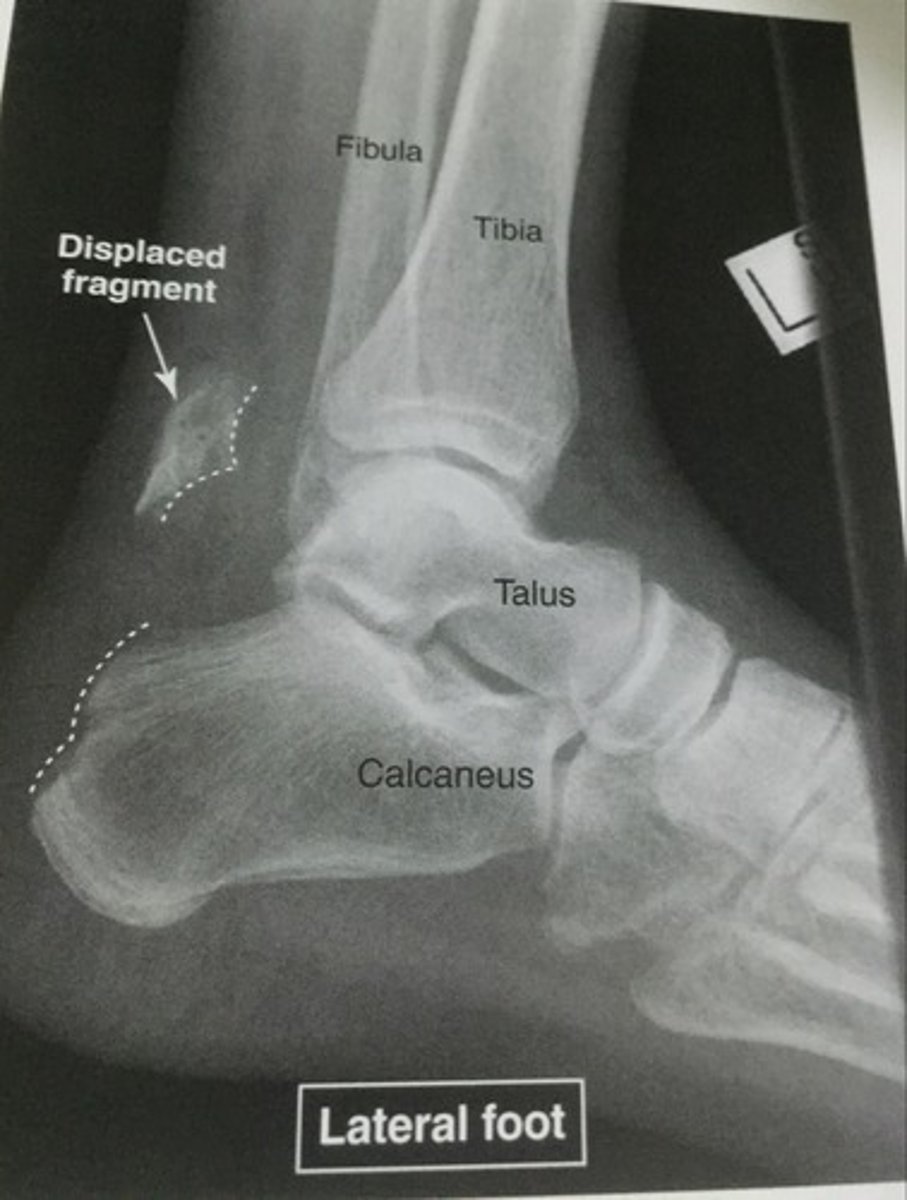
avulsion fracture
Fracture due to tendon/ligament pulling off small piece of bone
avulsion fracture
- Greenstick Fracture
- Epiphyseal (growth plate) fractures
- Plastic deformation
what types of fractures are more likely to be seen in children (3 types)
- Can cause growth to be arrested or altered
- Immediate intervention required
what are the clinical implications of Epiphyseal (growth plate) fractures
plastic deformation of bone
No fracture but the bone permanently bends
Salter Harris grading scale
a system used to grade pediatric fractures that involve the growth plate (physis), categorized into Types I–V based on the injury's impact on the growth plate, metaphysis, and epiphysis
Salter Harris grade 1 growth plate fracture
Salter Harris grade?
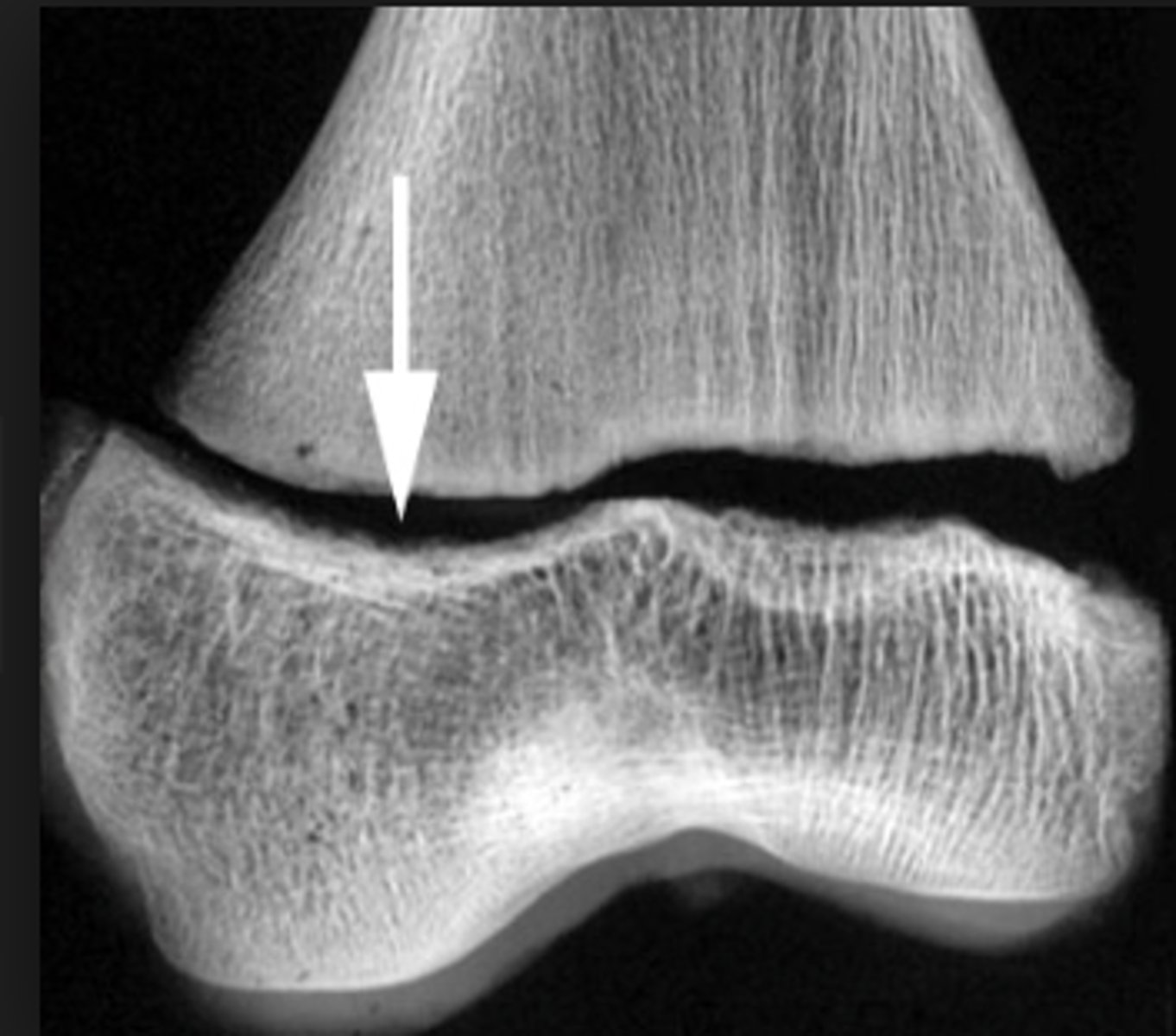
Salter Harris grade 2 growth plate fracture
Salter Harris grade?
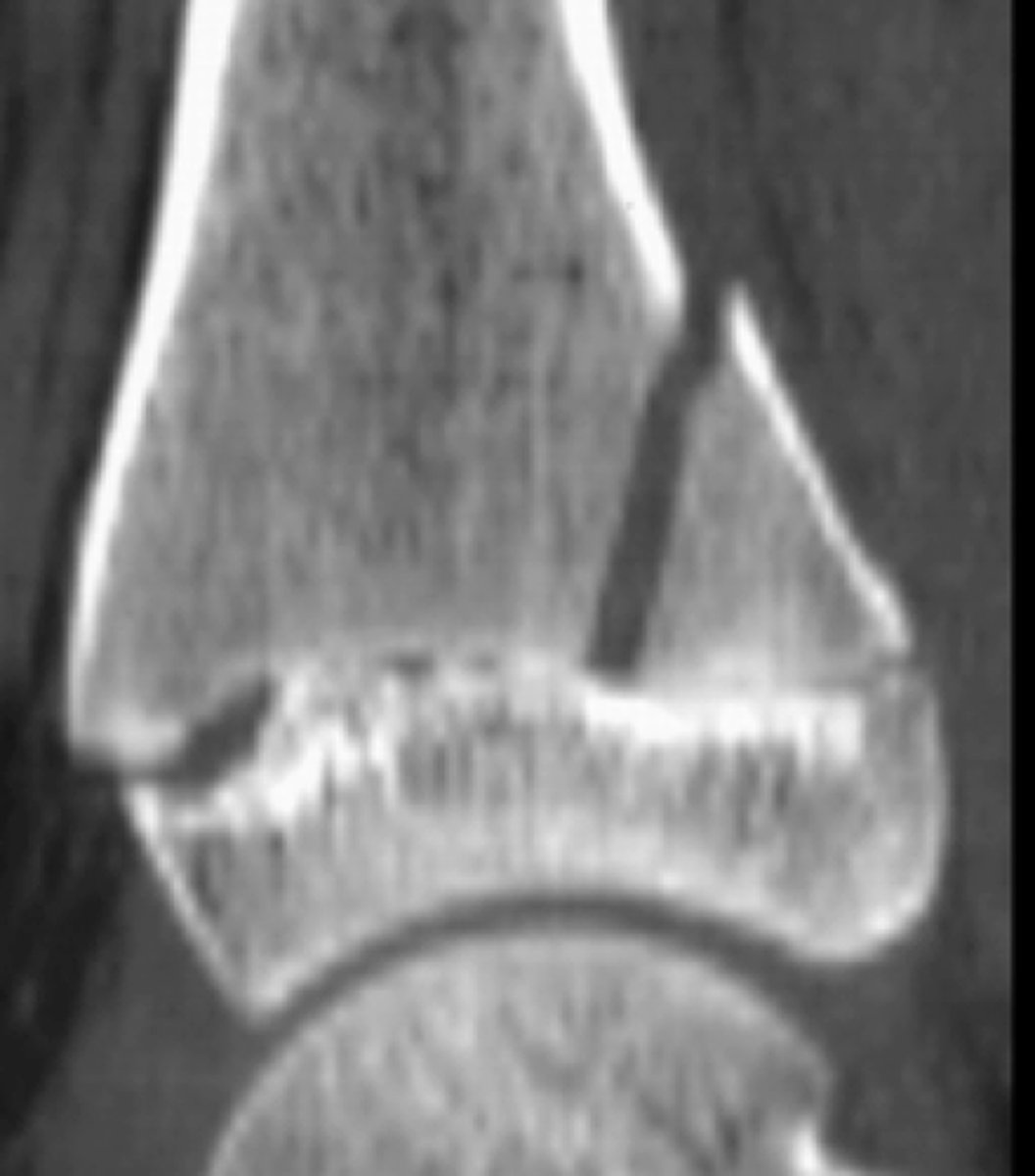
Salter Harris grade 3 growth plate fracture
Salter Harris grade?
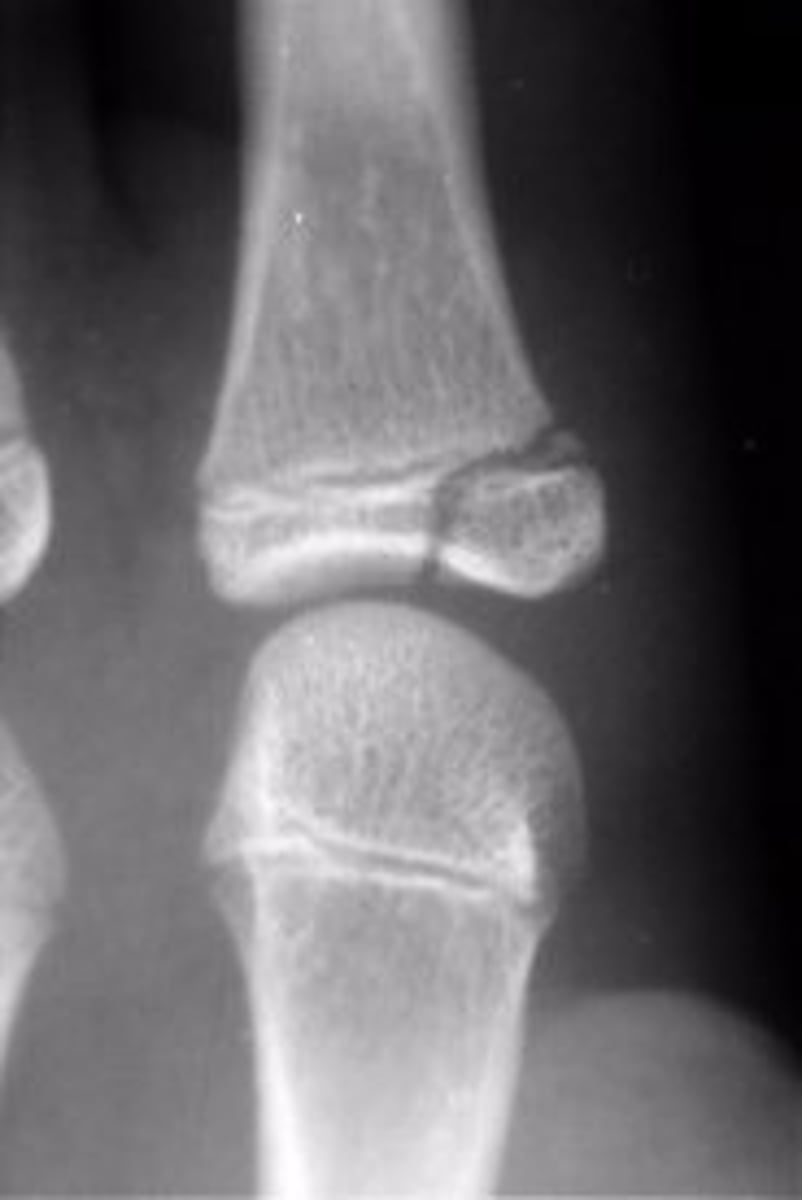
Salter Harris grade 4 growth plate fracture
Salter Harris grade?
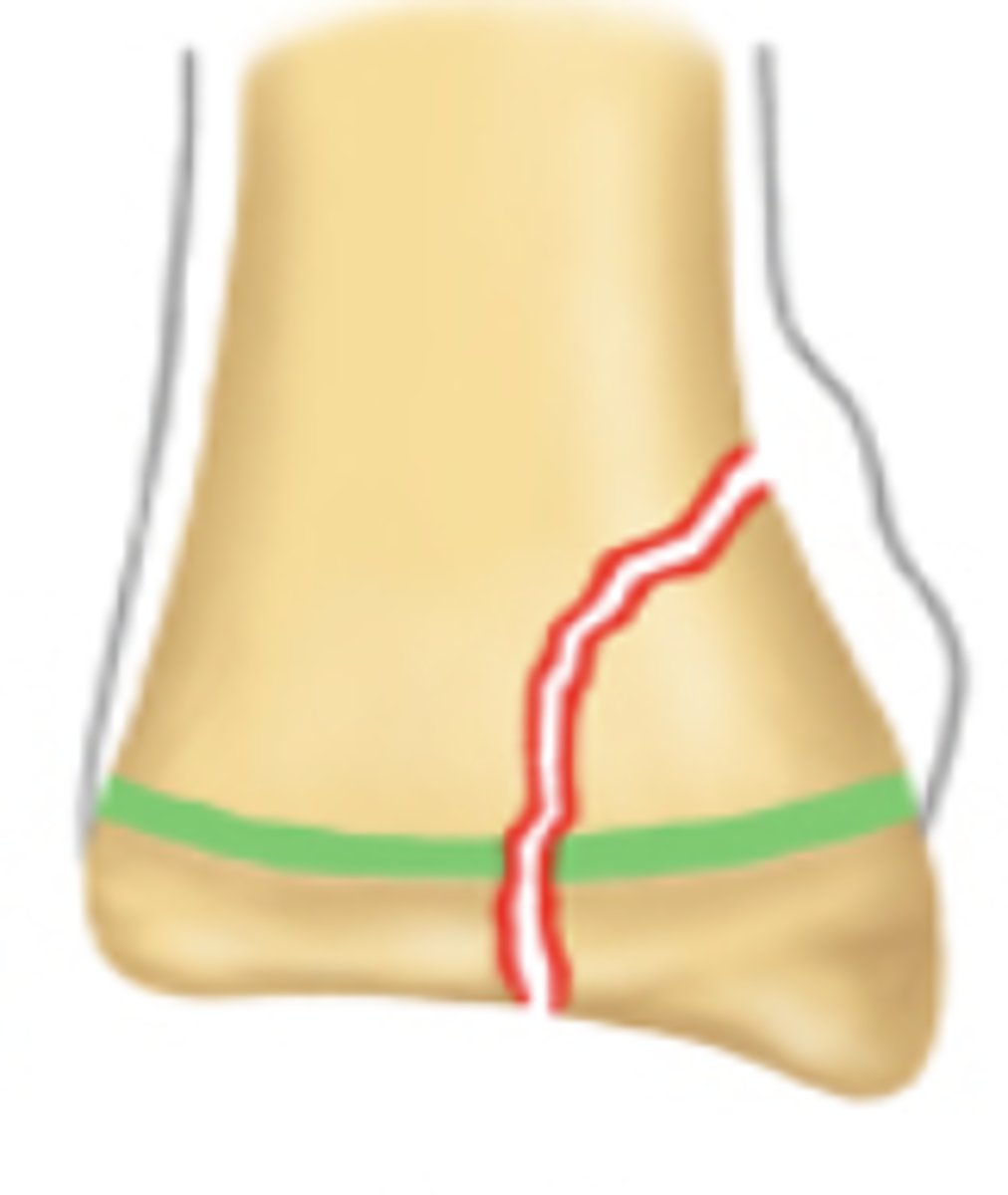
Salter Harris grade 5 growth plate fracture
Salter Harris grade?

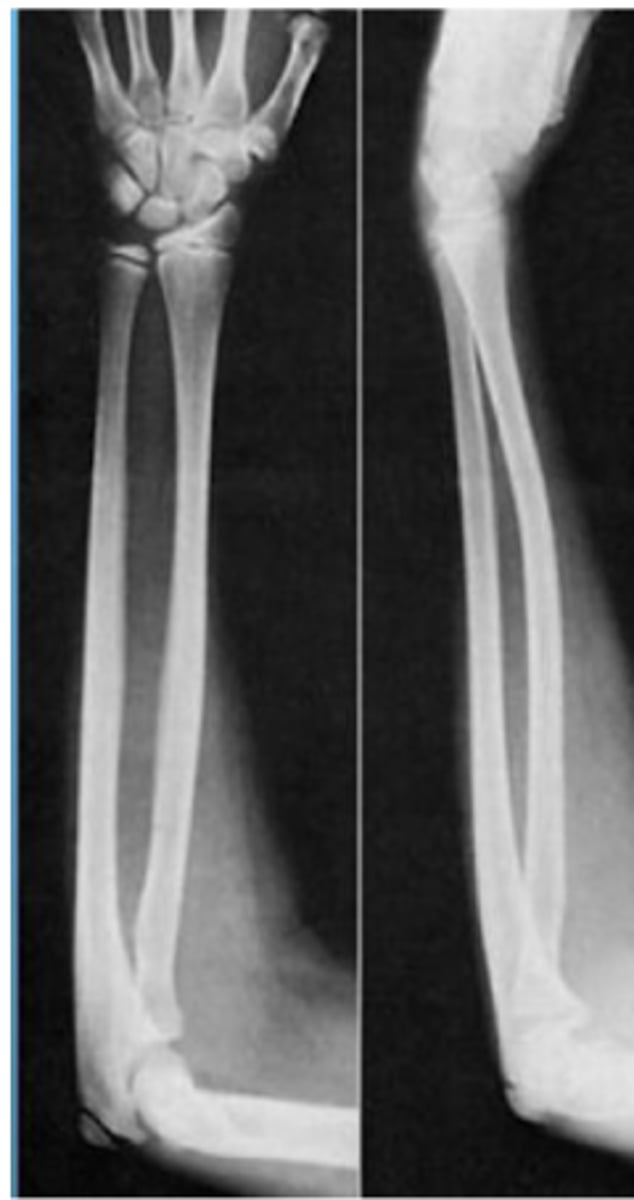
Plastic deformation of bone
when reach 30 y/o
when does bone mass reach its peak
- Women experience loss beginning in late 30s, accelerated during and after menopause
- Men experience bone loss in mid-late 60s
what happens once Bone mass reaches it peak at 30 y/o
- Low bone mineral density (BMD)
- Age
what are the 2 most important risk factors for fractures
- hematoma formation
- cellular proliferation
- callus formation and ossification
- consolidation and remodeling
what are the phases of healing for fractures (4 steps)
clotting
fibrin
leukocytes, macrophages
Neo
Hematoma formation phase of bone healing
- Within 48-72 hours _____ factors initiate the formation of hematoma
- Creates ____ meshwork
- Extensive necrosis requiring _____ and ____ to clean up debris
- ___-vascularization
the hematoma formation phase
what phase of bone healing is characterized by the creation of a fibrin meshwork, the presence of leukocytes and macrophages, as well as neovascularization
48-72 hours
how long does it take for Clotting factors initiate the formation of hematoma during bone healing from a fracture
Fibroblasts and osteoblasts
Cellular proliferation phase of bone healing
______ and ______ proliferate and form fibrocartilage collar around fracture site
cellular proliferation phase of bone healing
what stage of bone healing is characterized by Fibroblasts and osteoblasts proliferate and form fibrocartilage collar around fracture site
fracture
osteoblasts
woven
Callus formation and Ossification phase of bone healing
- Callus bridges gap between ends of _____
- Cartilage collar is replaced by bone by _____
- Early _____ bone formed within 7 days
Callus formation and Ossification phase of bone healing
what phase of bone healing is characterized by the formation of Callus bridges that gap between ends of fracture and osteoblasts replacing cartilage with bone