3: disorders of the orbit and systemic associations
1/36
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
37 Terms

ptosis
drooping of the upper eyelid. occasional visual compromise often gets wose with reading at night
both congenital ( got from birth) or acquired
in babies if obstructive can impair visual development and lead to amblyopia or anisometriopia
causes of ptosis
myogenic
aponeurotic
neurogenic
mechanican
traumatic
pseudoptosis
neurogenic causes of pstosis
nerve issue due to paresis or disease eg horners syndrome
tosis, miosis and anhydrosis
myogenic causes of pstosis
nearly always congentical .
present at birth and is caused by restriction of levator palpebrae superiorisis. including from conditions such as myathenia gravis - automimmune condition that causes muscle weakness and difficulty controlling eyelids and eye movements
children have neuroplastic cortex - brain more easy to adapt
aponeurotic causes of ptsosis
defect of the levator muscle, or effect of aging, repetitive eye rubbing , use of rigid contact enses, tauma or prvious intraocular surgery
mechanical causes of pstosis
effect of a mass, prior trauma or scar tissue
forieign body or retained contact lens in upper fornix or forniceal inflammation
what are the following tests done for pstosis
levator function assessment
pupil assessment
ocular motility
assessment for jaw winking syndrome- nerve related to opening jaw relates to nerve opeing the eye
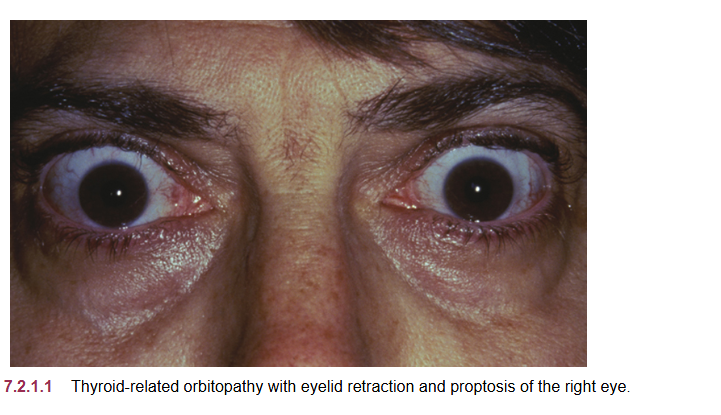
thyroid eye disease
retraction of the upper eyelids with lateral flare and eyelid lag on downward gaze, lagopthalmos.
thyroid issue scan occur at any ages but usually more in women and those over 40. leads to a visible goitre
thyroid gland
used to regulate some of the bodys hormones and metabolism, located in the neck, it is an endocrine gland eaning it releases hrmones into the blood stream
what is thyroid gland used to regulate for
regulates metabolism
regulating heart rate
food digestion
breathing
fertility
helps process bodily calcium
endocrine gland: releases hormones into the bloodstream
exocrine gland: releases into a duct
what systemic issues occur when you have n over reactive or under reactive thyroid
temperature tolerance
weight changes
heart rate changes
mental staus and hormonal changes
hypothyroidism
causes a reduction in the metabolic effects
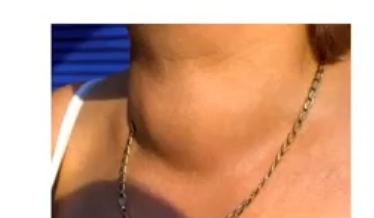
hyperthyroidism
causes an increase in the metabolic effects
rapid pulse hot and dry skin
enlarged thyroid gland (goiter)
weight loss ]
ocular synptoms of thyroid eye disease
foreign body sensation, redness, tearing, photophobia
upper eyelid retraction tends to develop
lateral flare
prominent eyes
eyelid swelling
treamtents of thyroid eye disease
px take levothyroxine to supplement the lack of this either by the condition of hypothyroidism or the treatment of hyperthyroidism which is surgical removal or radiation to reduce its inital functino and then supplement this
thyroid eye disease common causes
via autoimmune condition known as graves disease and this can cause hyperthyroidism and associated conditions which can affect the eye
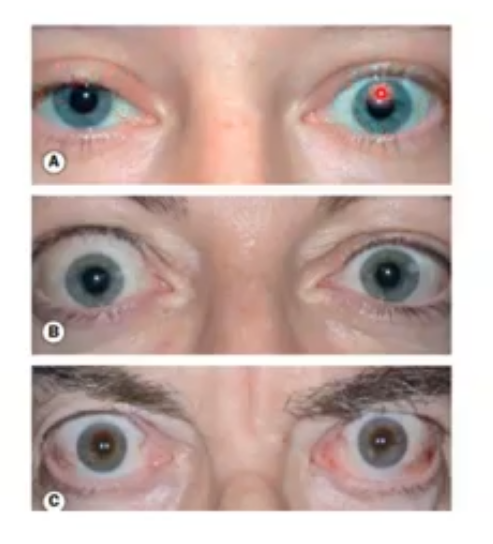
TED signs
can appear asymptomatic or red and painful
px can get double vision
can get upper lid retraction and proptosis ; bulding forward of eyes
px can lose their sight and visual fields through optic nerve difficulties
dryness
impaied vision
more signs of TED
lid retraction occurs in 50% of those with graves
due to sympathetic overstimulation of the lid muscles.
px may complain about appearance, or dry eyes and exposure to cornea, raised lid on downgace another warning sign - if px looks down and lid still looks retracted then likely TED
proptosis is an extensino of this where eyes begin to bulge, unilateral, bilateral or aymmetric- due to metabolic activity increases, over production of the fat tissue of orbit behind eye. due to this it compresses the eye muscles and optic nerve causing vision loss
progress to restrictive myopathy, and optic neuropathy
referral to HES urgently if any of thsi is suspected
orbital infections
preseptal cellulitis and orbital cellulitis
mostly seen in children
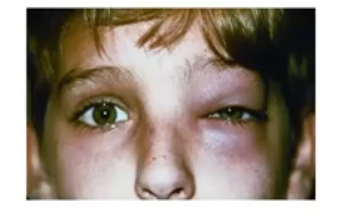
preseptal cellulitis
infection of the subcutaneous tissue of the eyelid and skin around the eye
more anterior
less serios than orbital cellulitis , but moderate risk of progressing to orbital so urgent referral needed
bacterial infection usually the case, and usually staphylococcus or streptococcus, and usually spreads from infection/skin trauma , some bite, or conjunctivitis, acute hordeolum
signs of preseptal cellulitis
eyelid appears swollen firm and tender, ad in moderate pain
red eye swelling can appear very severe and they may have a fever
assume it isnt preseptal until you confirm that there is no proptosis, VA unaffectedm pupil reactions are equal and ocular motility isnt impaired
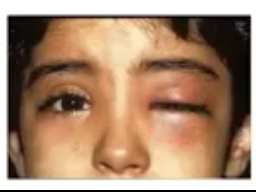
orbital cellulitis
an infection of the soft tissues behind the orbital septum which are sight and life threatening if not treated quickly
usually starts as a sinus infection which then spreads
px has fever and lot of pain
VA reduction and colour vision between eyes, any pupil RAPD is diagnositic
much chemosis and redness and swellnig of conjunctival haemorrhage, proptois presen but may be hidded due to lid swelling
px hospitalised with IV antibiotics and any abcess will be drained with surgery
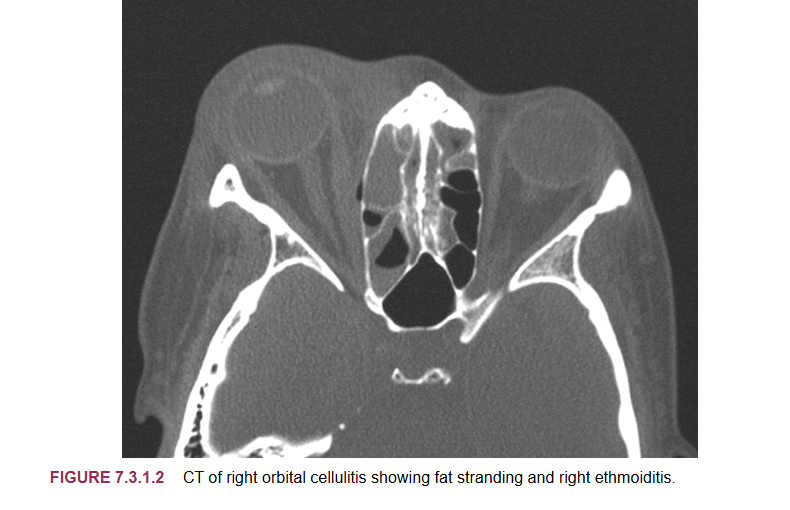
what exam is done with those with orbital cellulitis
exam will occur with a CT and MRI to assess situation
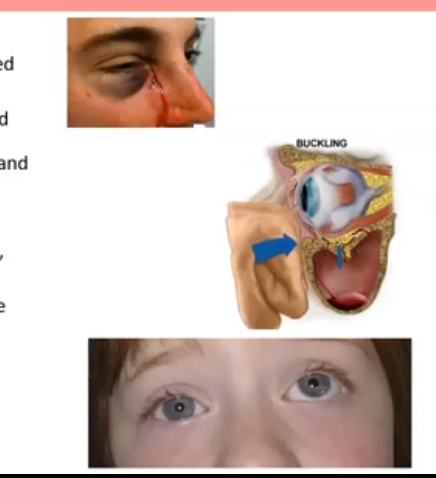
trauma
lid laceration and black eyes
any subvonjunctival haemorrhage or bleed needs to be assessed to identify extent of bleeding
any open wound on lid needs urgent treatment
diinfection and closure is important to prevent risk of orbitla cellulitis
observe foreign bodies
effects of blunt trauma
blow out fracture with associated enopthalmos, motility issues, and potential diplopia ; inferior rectus muscle gets stuck so eye is restricted from looking up
some may give corneal abrasions , tears in corneal layers, visible with fluorescein
look out for hyphaema or impact on iris such as a displaced pigment iridiodialysis
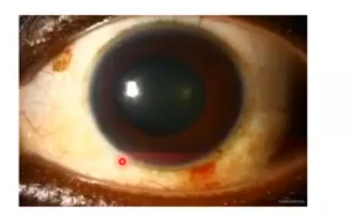
hyphaema
blood collected in the anterior chamber and due to gravity it deposits at the bottom
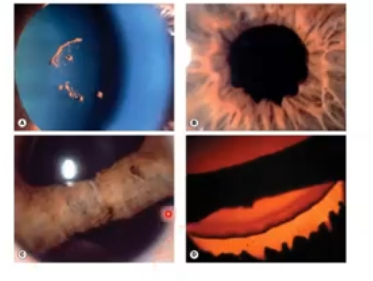
sticky iris due to trauma
in severe trauma cases the iris might disappear
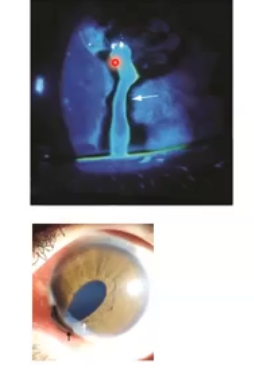
seidels sign
penetrating injury of the cornea due to trauma
symptoms vary from nothing/mild visual reduction to severe pain and light sensitivity
may appear normal or may have circulinear injection with a reduced IOP
use fluorescein to show a waterfall like effect. requires same day referral
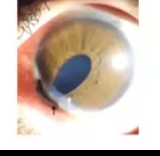
iris prolapses
can occur after surgery or a perforated cornea , or in the case of trauma or infection
px will have a foreign body sensation, pain and epiohora
needs emergency same day referral. not to take eye drops ad will need surgery to correct
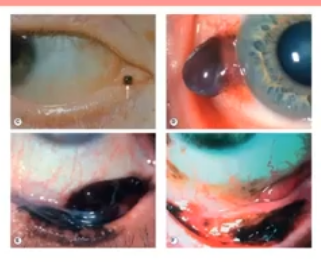
tumours
look for irregular shapes, raised areas, growth and invasive approach to other tissues for soething malignant
refer within 4-6 weeks
treatment incolves excisino, blood assessment and body assessment for metastasic possibilities. ocular tumors can be primary or secondary sites for malignancy
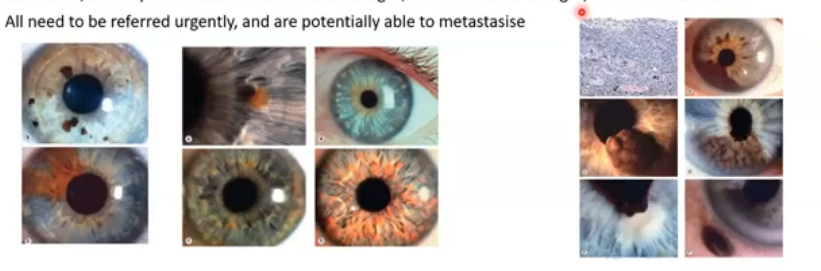
iris tumours
can also have naevi here
can be flat or raised, and there can be several or few
greater risk of malignancy so need to monitor and observe lifelong change
present at a younger age, inferior iris location, light skin and iris colour, melanosis elsewhere and any odd features such as diffuse edges or blood vessel/bleeds on naevus
refferred urgently and are potentially able to metastasise
diabetes
endocrine condition where body either doesnt produce enough insulin ( type 1) or becomes resistant to insulin (type 2)
type 1 diabetes
immune system attacks and destroys the cells in the islet of langerhans in the pancreas, and thus you do not have insulin and this can cause issues with sugar control
type 2 diabetes
the body either doesnt produce enough insulin or the cells dont react to the insulin and thus you get the same issues with sugar control
cause from diabetes
both of these cause issues to the blood vessels in the bdy but also the nerves, because sugar is toxic
also bevause your blood becomes sticky, as the amount of glucose attached to it is too high and raises inflammatory markers
loss of efficent circulation and innervation means you are at greater risk of inflammation, infection and damage to small capillaries and smaller cells of the body
diabetes damage to the anterior eye
cataracts
corneal sensation lossneuropathy
dry eye
iris neovascukarisation
slow healing of tissues - higher risk of infections
less regulated lid control
greater risk of infarcts and bleeds
risk factors of diabetes thus affecting the eye
poor control of blood sugar
length of time with diabetes
greater BMI and/other systemic conditions such as hypertensino
asian/black ethnicity
older age