D3.1 Reproduction SL
1/53
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
54 Terms
asexual reproduction
1 parent
all genes passed on to offspring
no gametes formed, offspring genetically identical to parent and siblings if no mutations
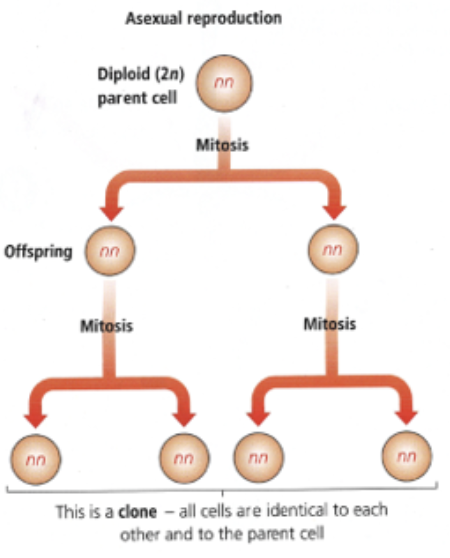
examples of asexual reproduction
regeneration in flatworms (planaria)
fragmentation and regeneration in sea stars
budding in hydra
budding in yeaast
binary fission in bacteria
propagation in some plants
examples of plant asexual reproduction
formation of plantlets in spider plants
formation of plantlets in kalanchoe
vegetaative propagation in potatoes or tubers
negative propagation in strawberries by runners
advantages of asexual reproduction
efficient (e.g, bacteria every 20 minutes)
no STDs
mating partner unnecessary - less energy used
more offspring produced
not season dependent
disadvantages of asexual production
no genetic variation, less adaptable to environmental changes
selective pressures cause more competition
only locally disperseed
sexual reproduction
2 parents
haploid gametes formed, sexual intercourse and fertilization form diploid zygote; offspring receives half genetic material from each parent
offspring has unique combination of genetical and phenotypical characteristics inherited from each parent
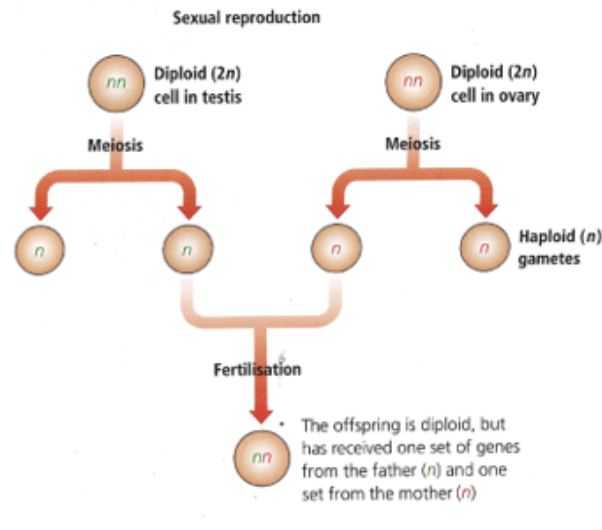
examples of sexual reproduction
mammals, fish, reptiles, flowering plants, conifers
advantages of sexual reproduction
genetic recombinations allow more potential to adapt to selective pressures
offspring is widely dispersed, allowing for more resource availability
safeguard against erroneous alleles
disadvantages of sexual reproduction
needs mating partner - requires time and energy
often season-dependent
risk of failed continuity due to small number of offspring produced
anisogamy
trend of different male and female gametes in eukaryotes
features of male sex cells
motile, often move by own means (e.g. tail, wind, pollinators)
smaller size (human sperm ~30 μm)
limited food reserves, enough to support movement but not development
large number (millions) produced
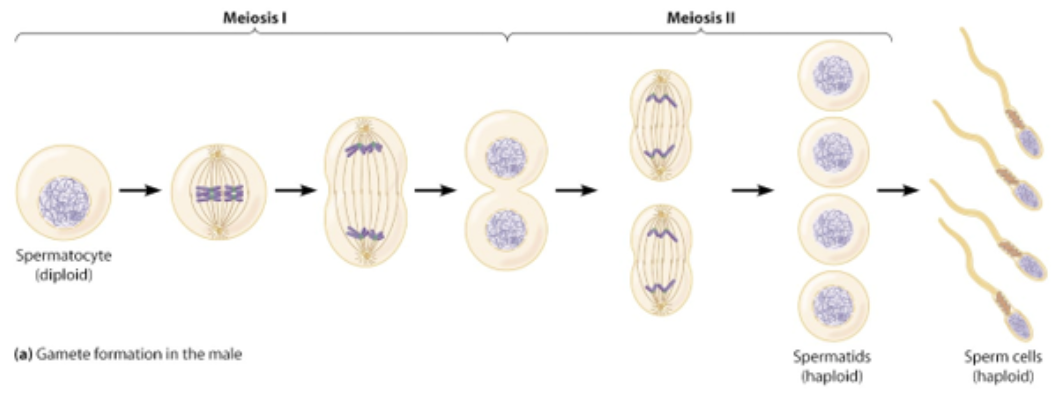
reproductive strategies of male sex cells
large number of gametes and production throughout lifetime means only few succeed
more competition to fertilize the limited number of female gametes
fuels evolution of mating competition
features of female sex cells
sessile, move within very limited parameters
relatively large size (human egg cell ~120 μm)
large food reserves for development of embryo over an extended period of time
fewer produced, often only 1-2 egg cells during time from where fertilization can occur
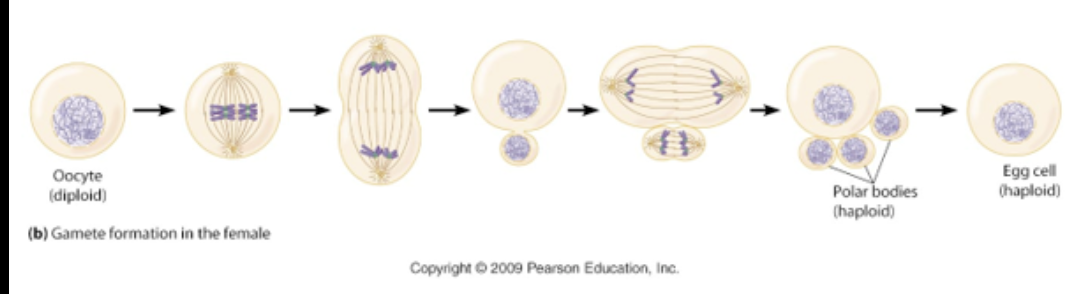
reproductive strategies of female sex cells
small number and large gametes only produced once peer moth and until menopause indicates better provision of food sources and reproductive success due to more investment
enhances female choice and drives selective pressure for males
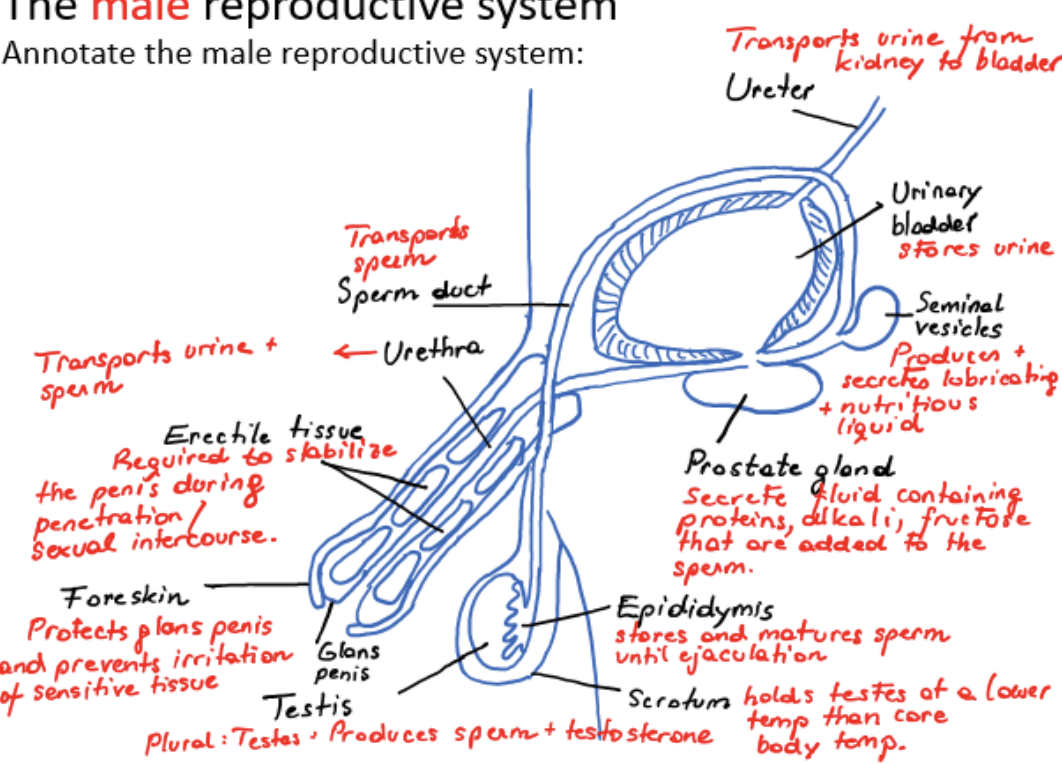
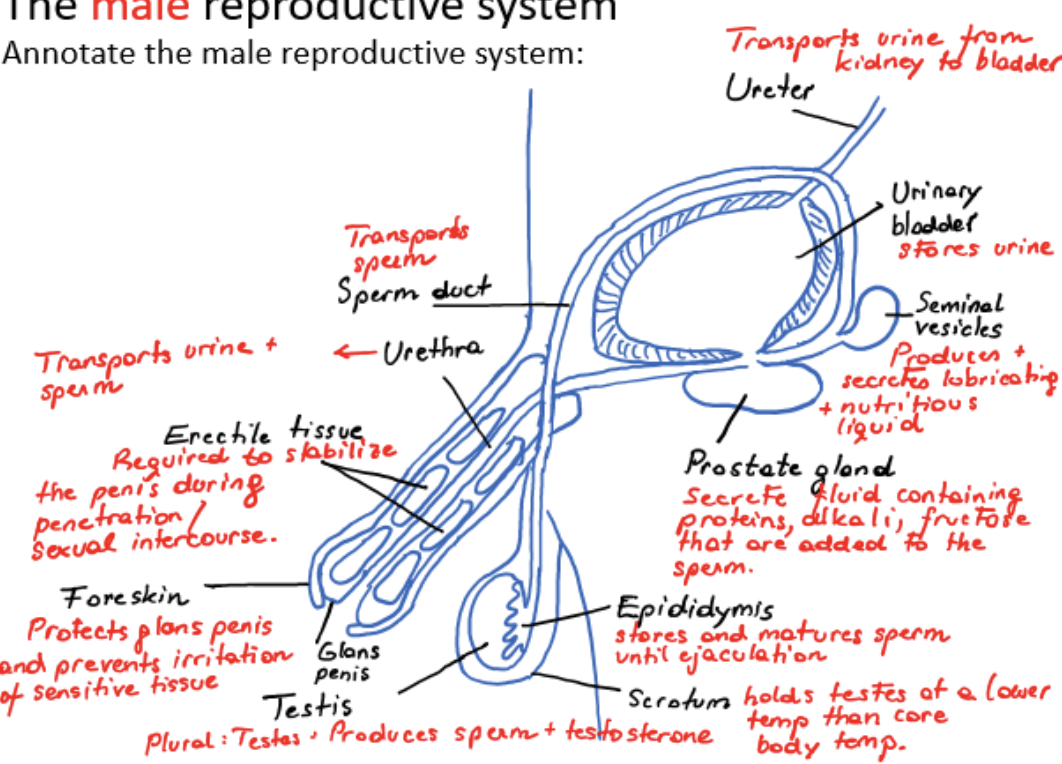
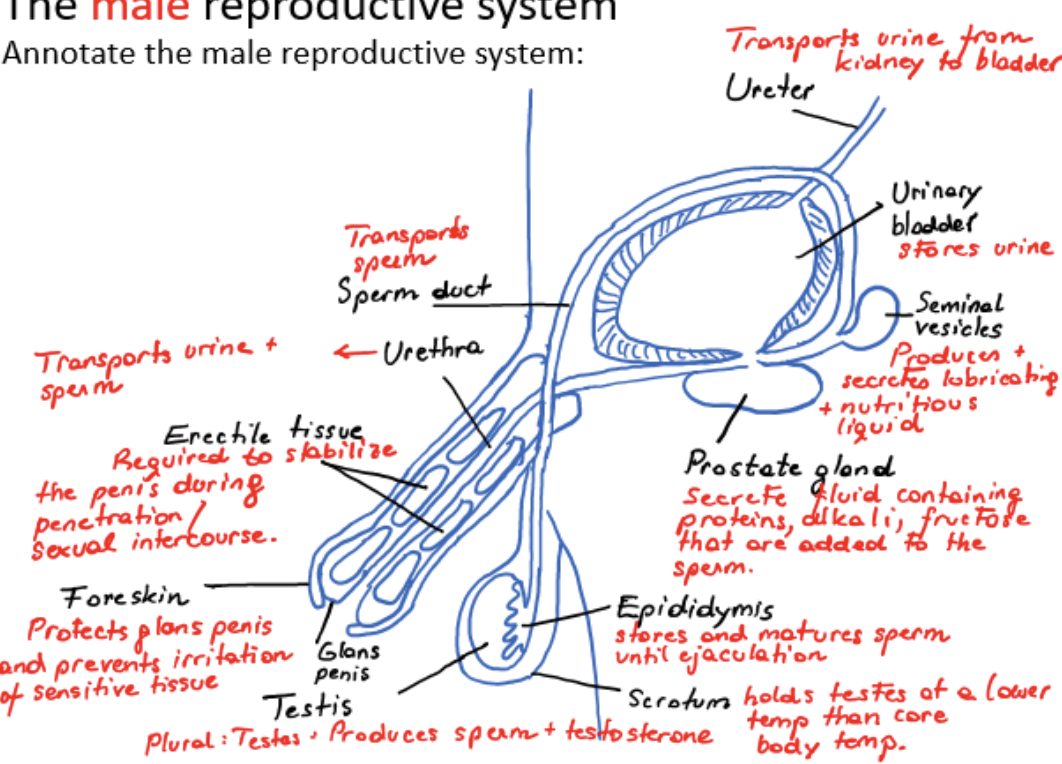
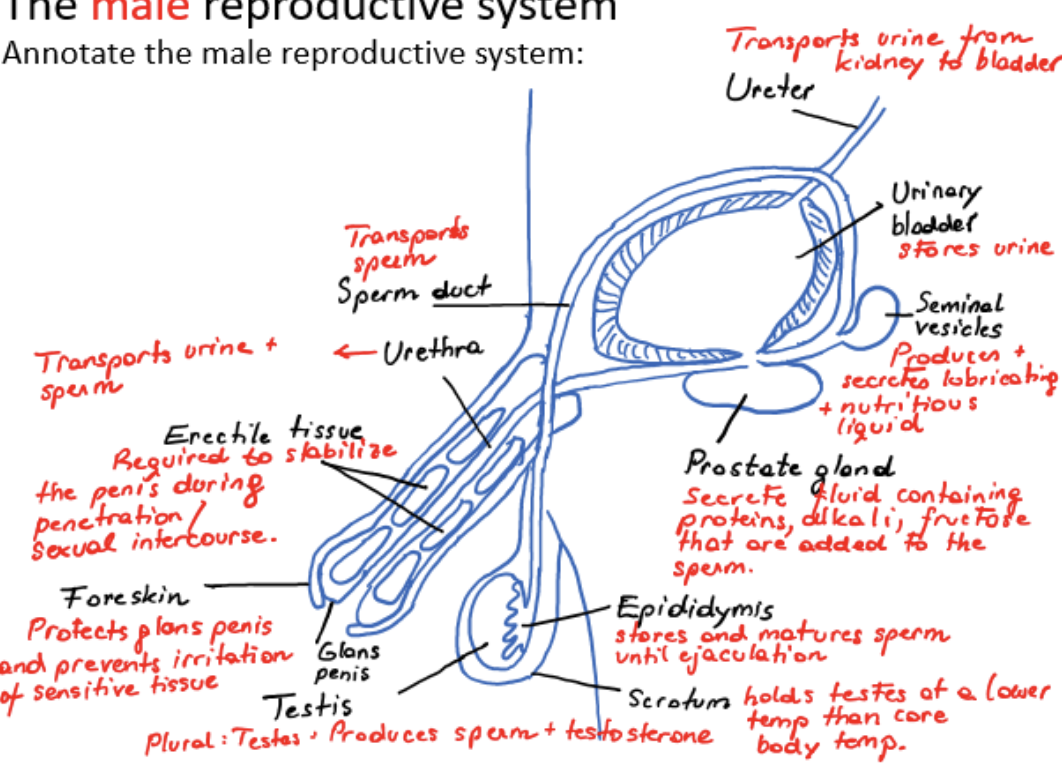
male reproductive system
ureter
urinary bladder
scrotum
testis (plural testes)
epididymis
sperm duct
seminal vesicles
prostate gland
urethra
erectile tissue
foreskin
glans penis
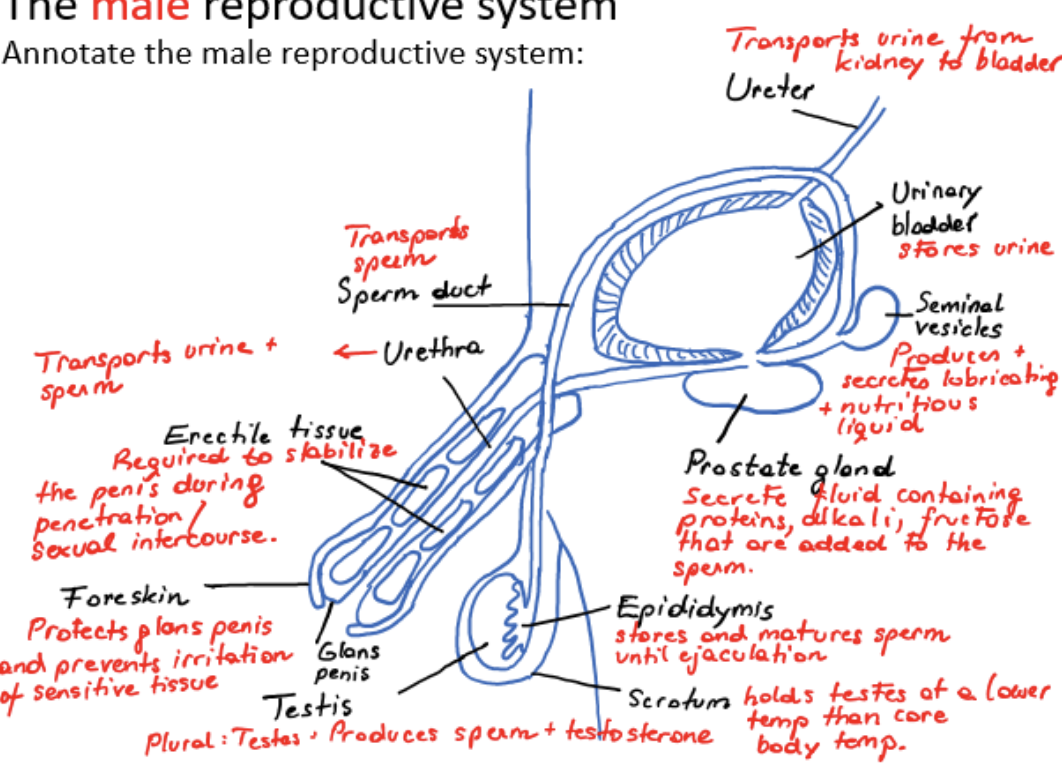
ureter
transports urine from kidney to bladder
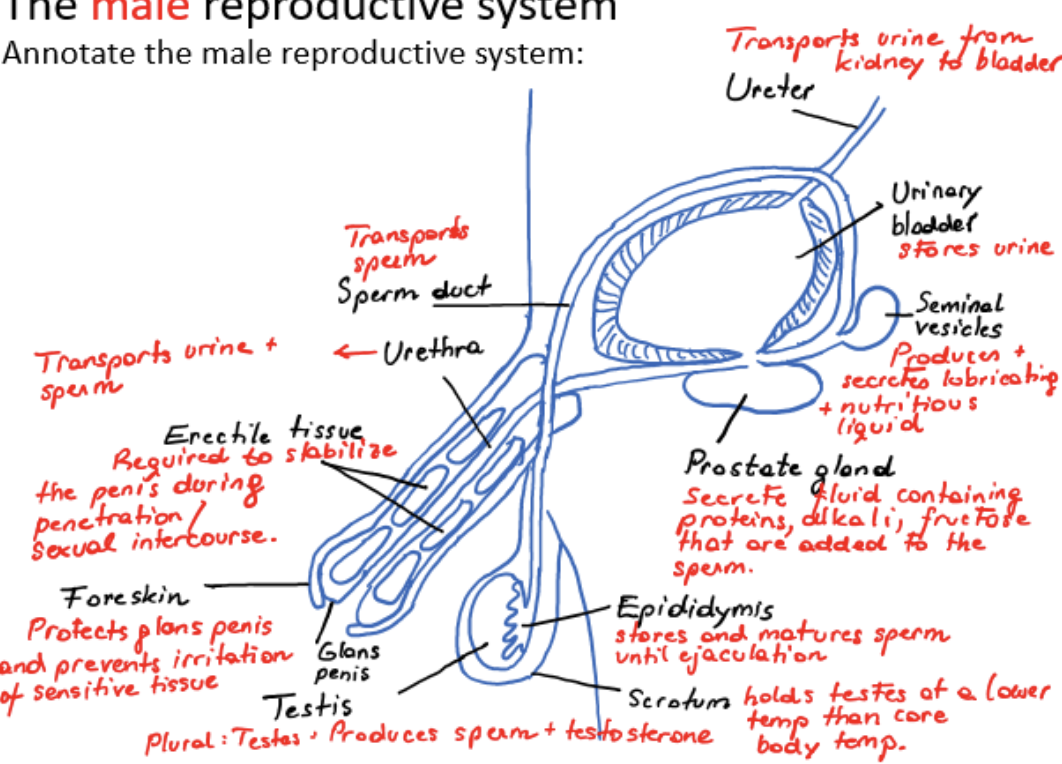
urinary bladder
stores urine
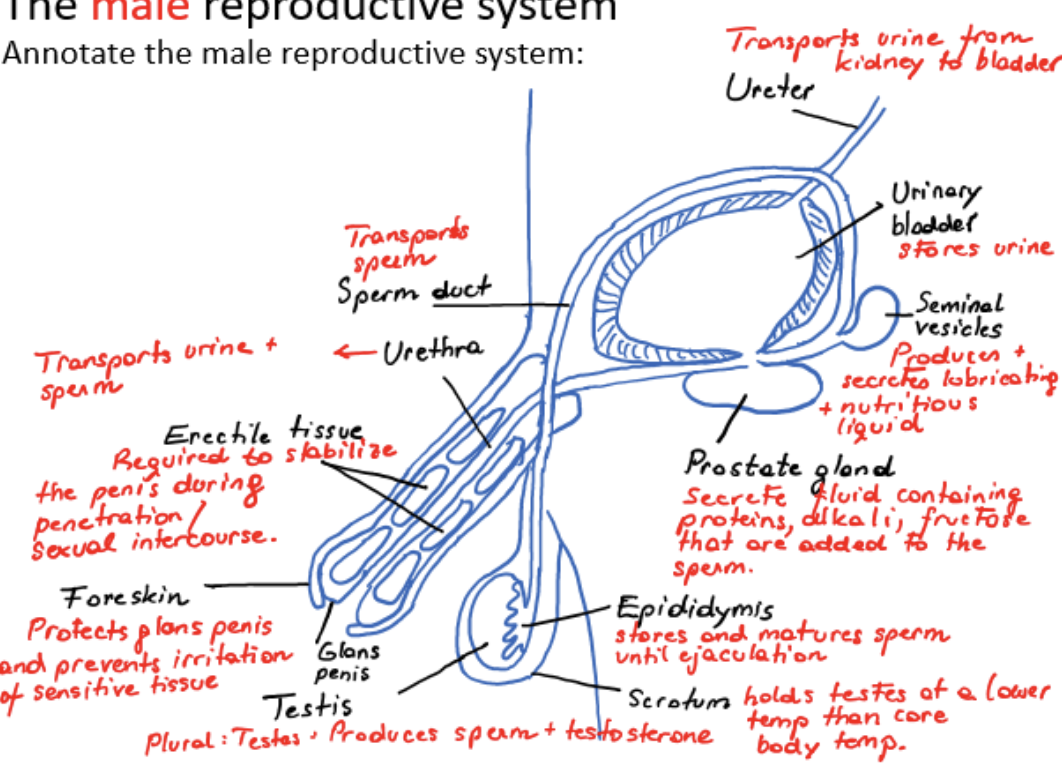
scrotum
holds testes at a lower temperature than core body temperature
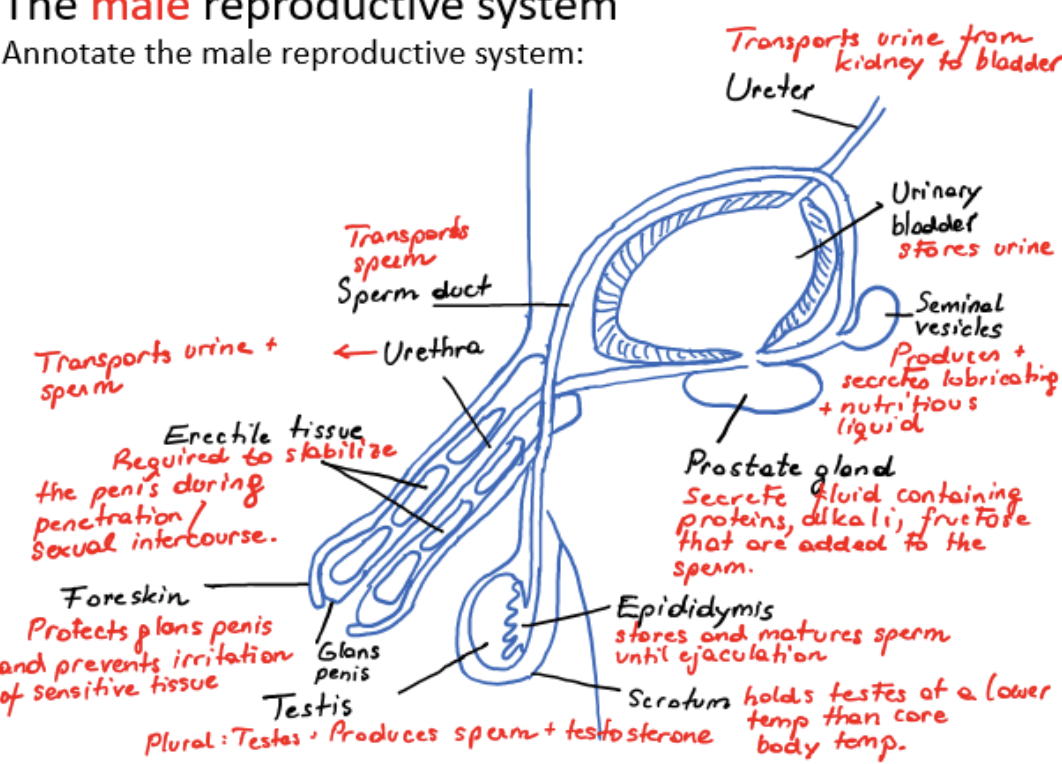
testis
produces sperm and testosterone
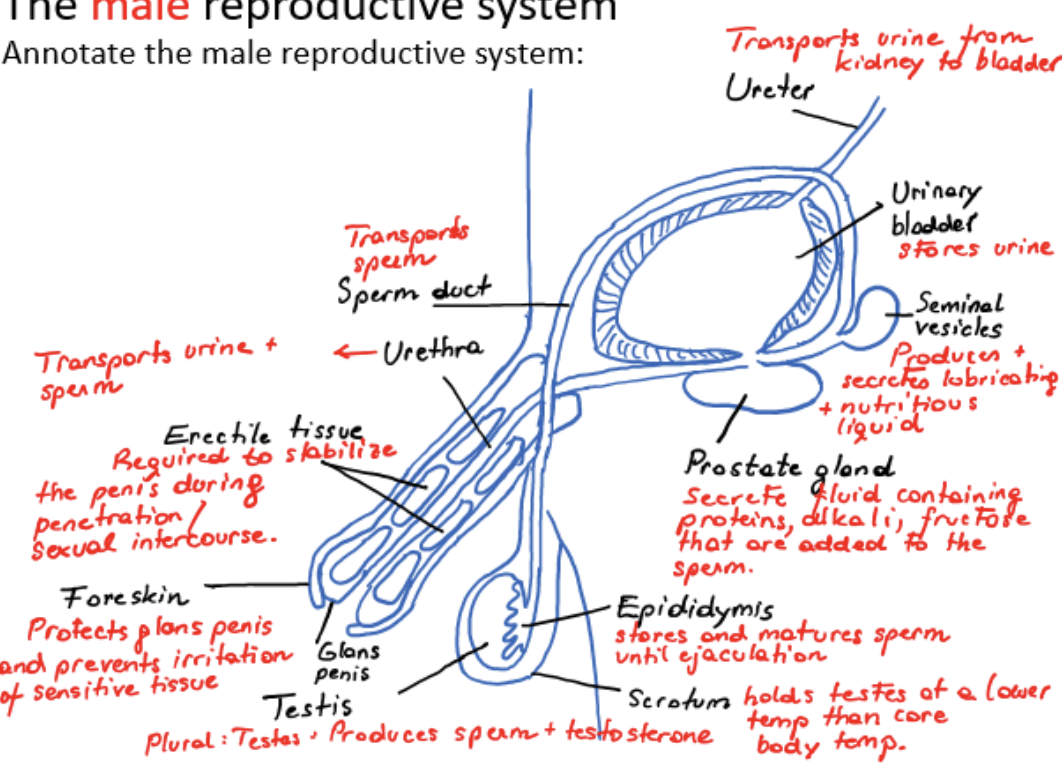
epididymis
stores and matures sperm until ejaculation
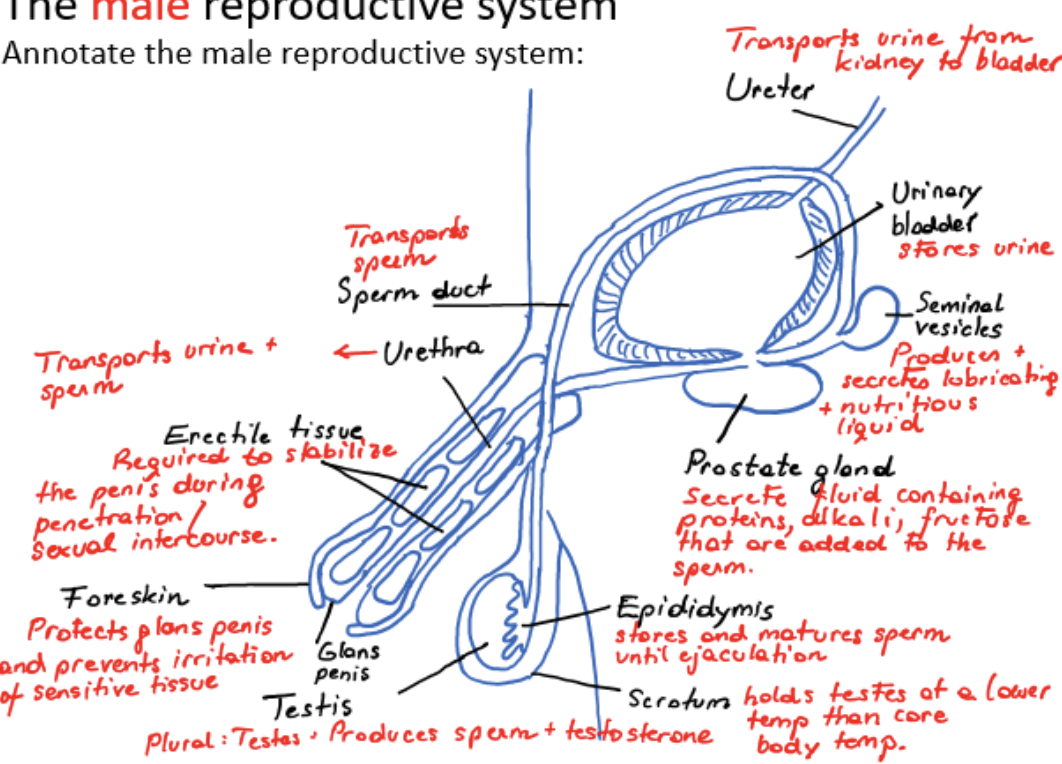
sperm duct
transports sperm from testis
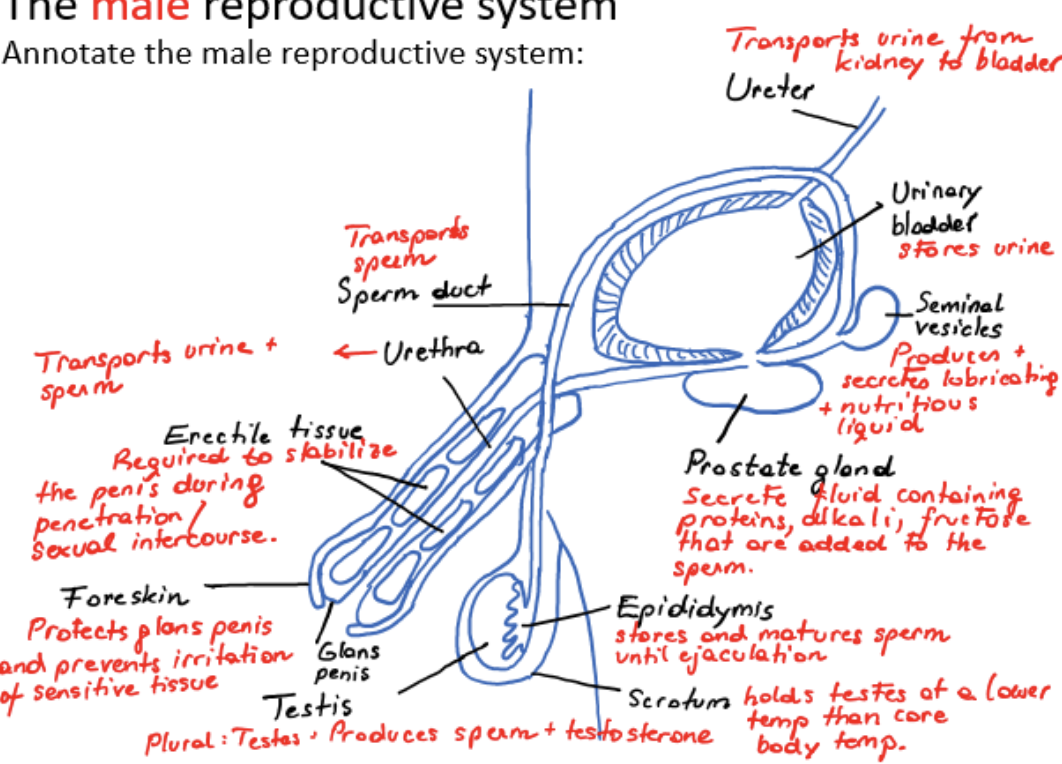
seminal vesicles
produces and secretes lubricating and nutritious liquid
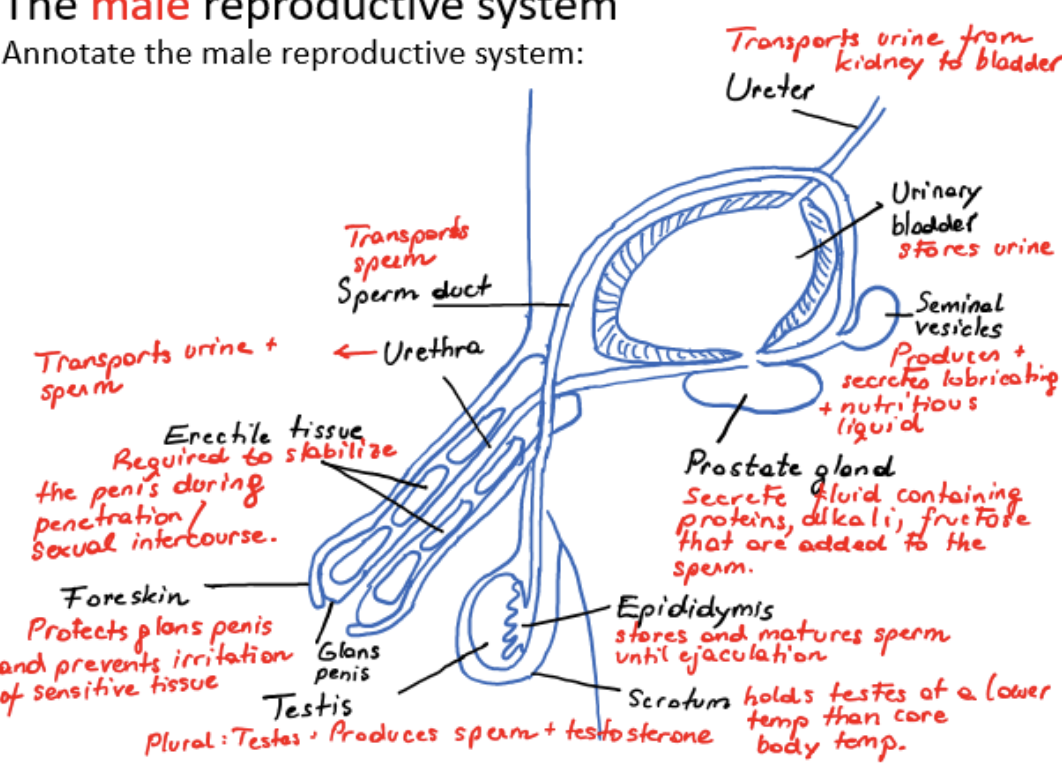
prostate gland
secretes fluid containing proteins, alkali, fructose that are added to the sperm
urethra
transports urine and sperm
erectile tissue
required to stabilize the penis during penetration/sexual intercourse
foreskin
protects glans penis and prevents irritation of sensitive tissue
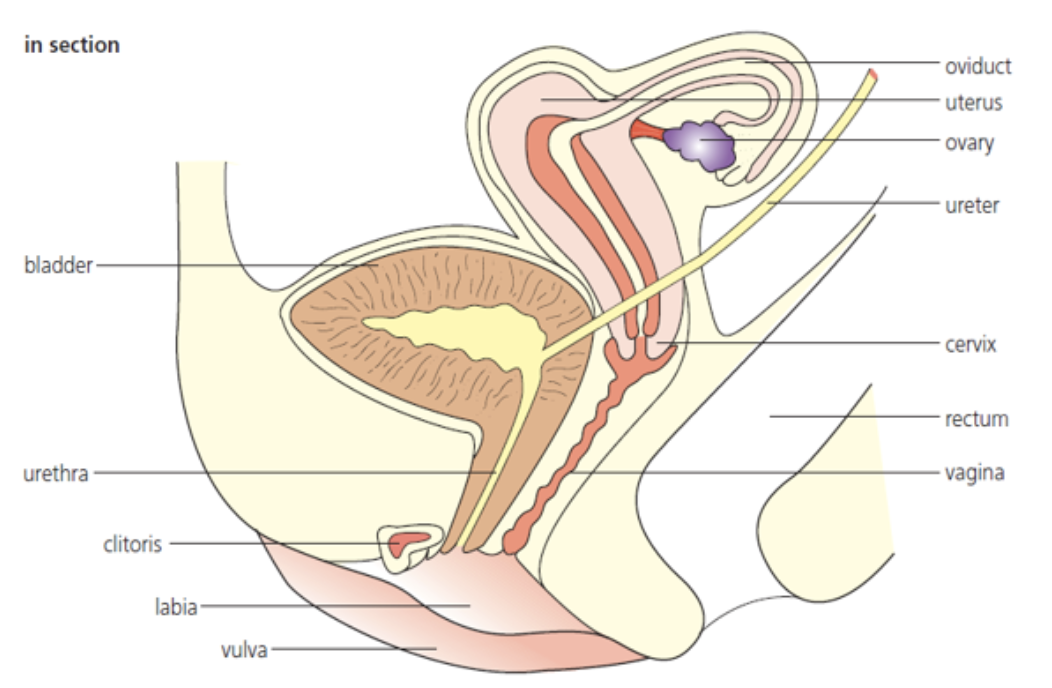
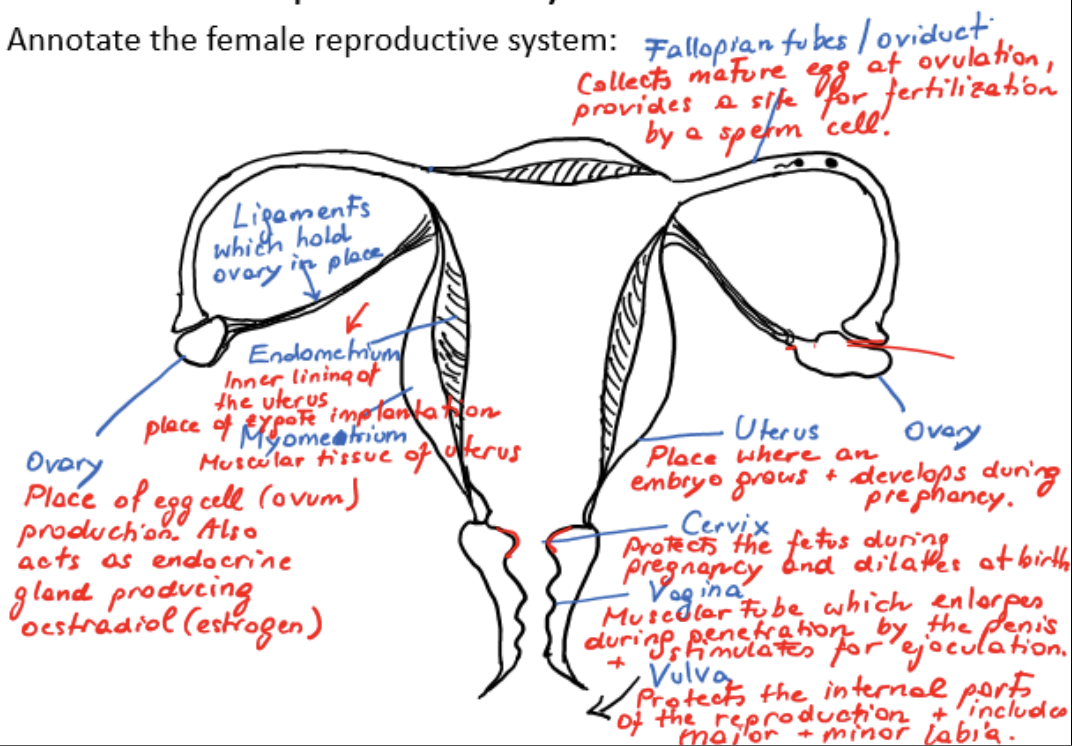
female reproductive system
ovaries
ligaments
fallopian tubes/oviducts
myometrium
endometrium
uterus
cervix
vagina
vulva
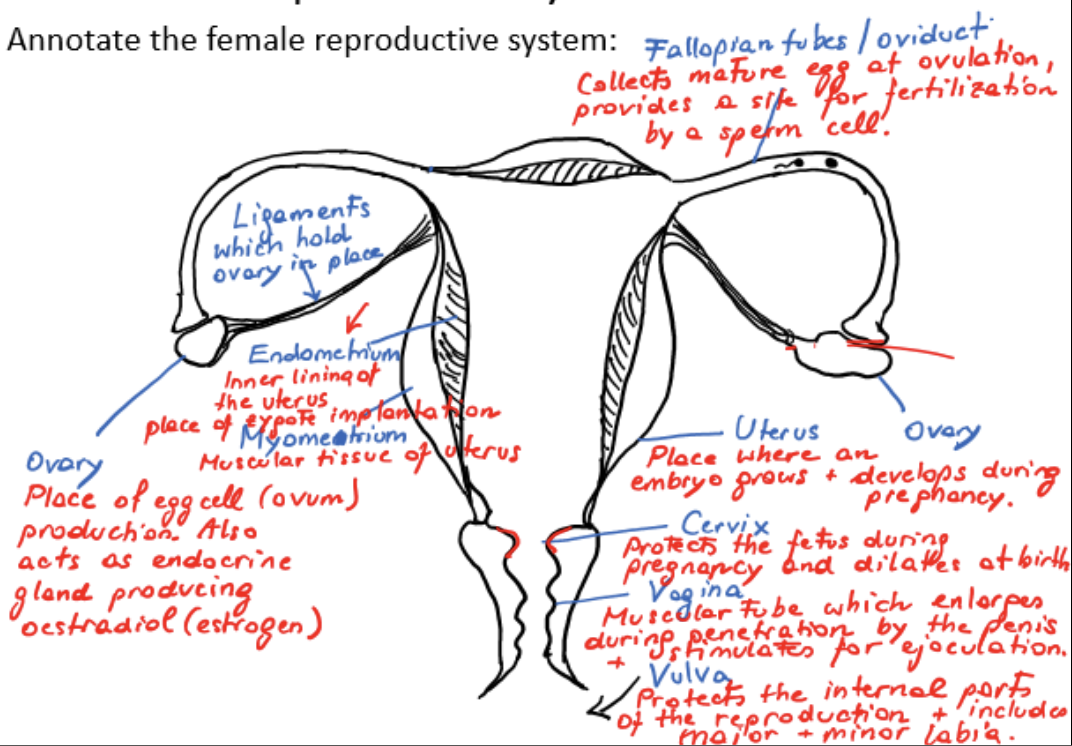
ovary
place of egg cell/ovum production
acts as endocrine gland, producing estradiol/estrogen
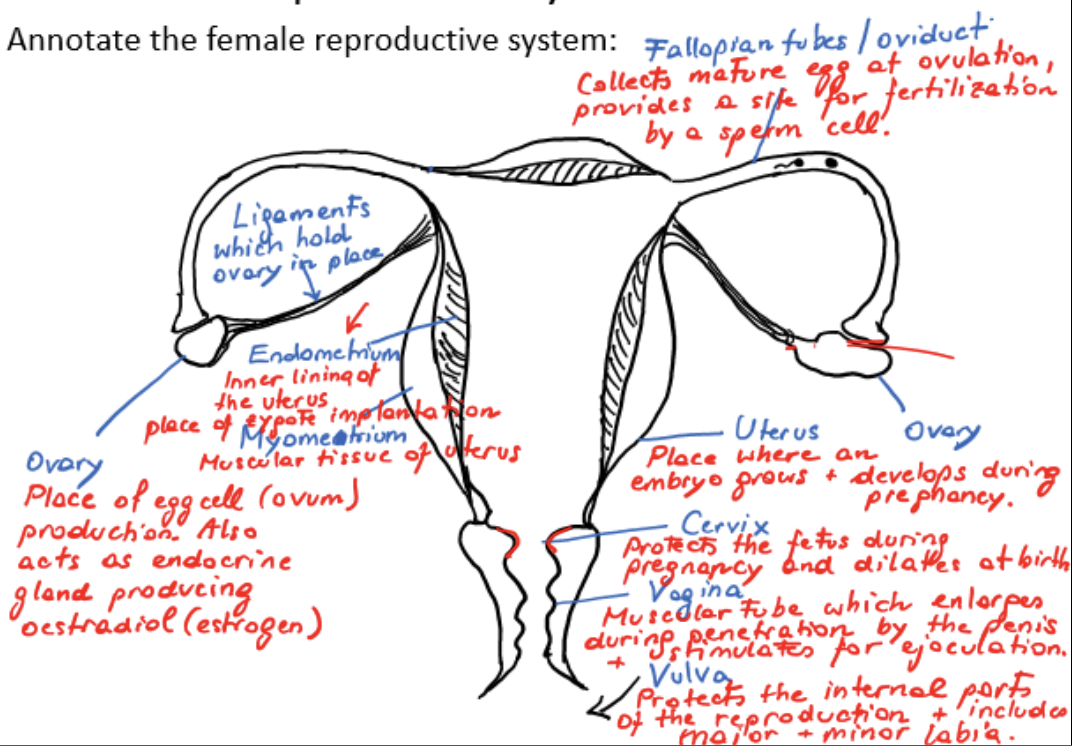
ligament
holds ovary in place
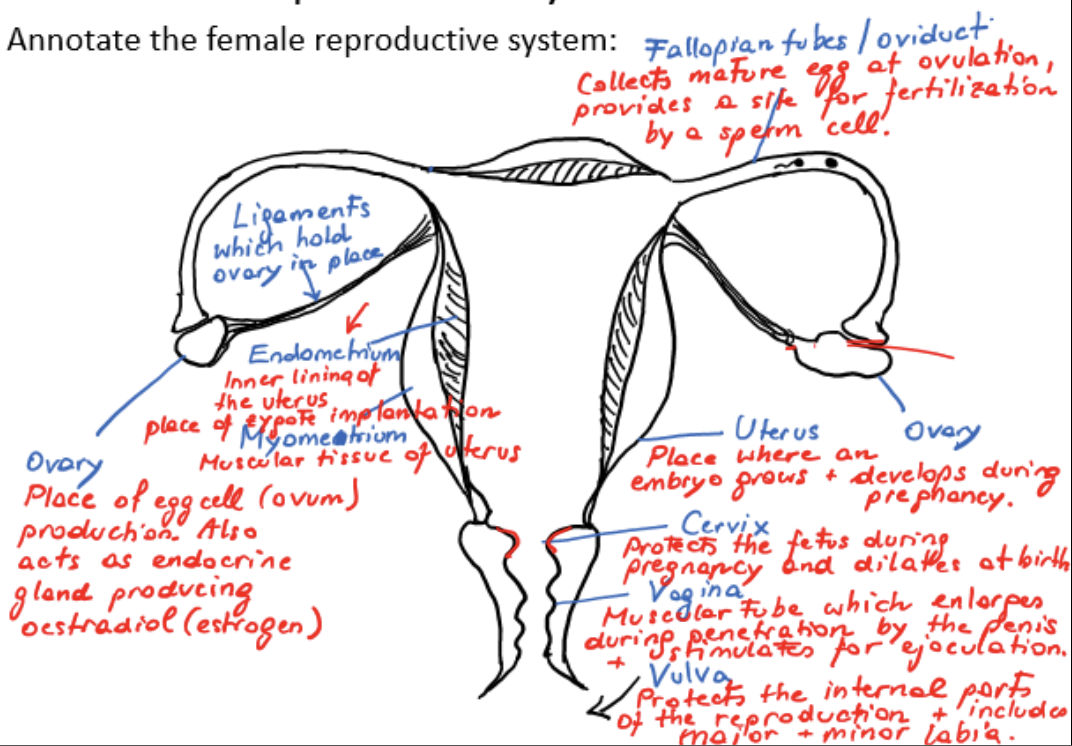
fallopian tube/oviduct
collects mature egg at ovulation, provides a site for fertilization by a sperm cell
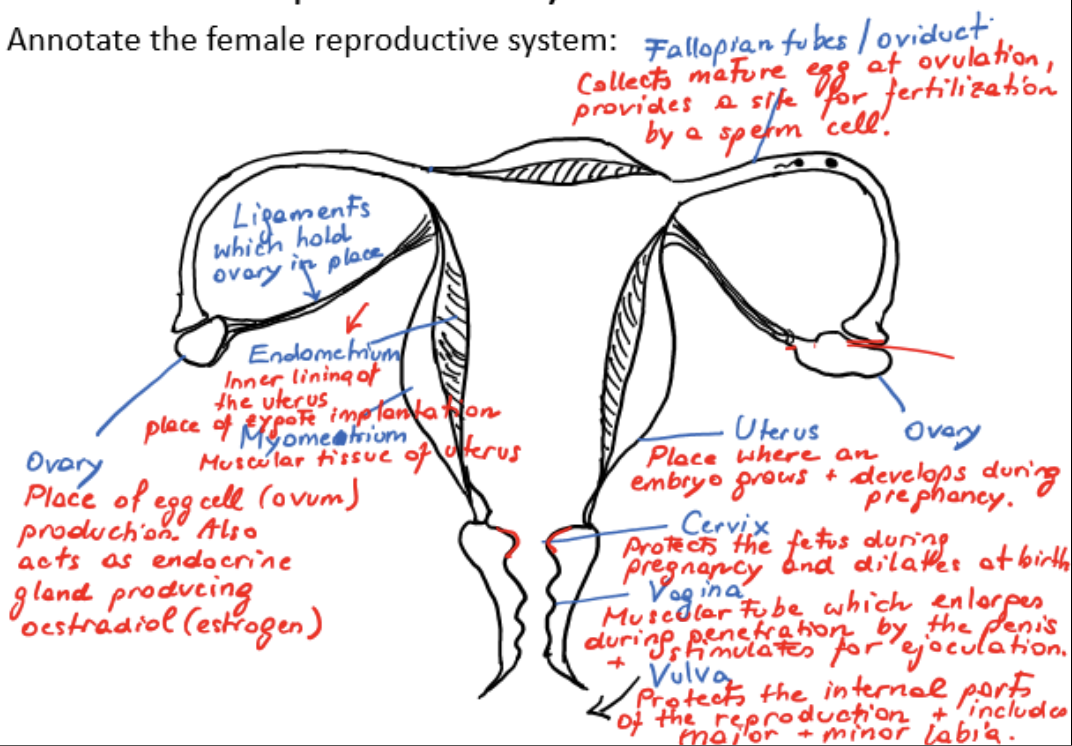
myometrium
muscular tissue of uterus
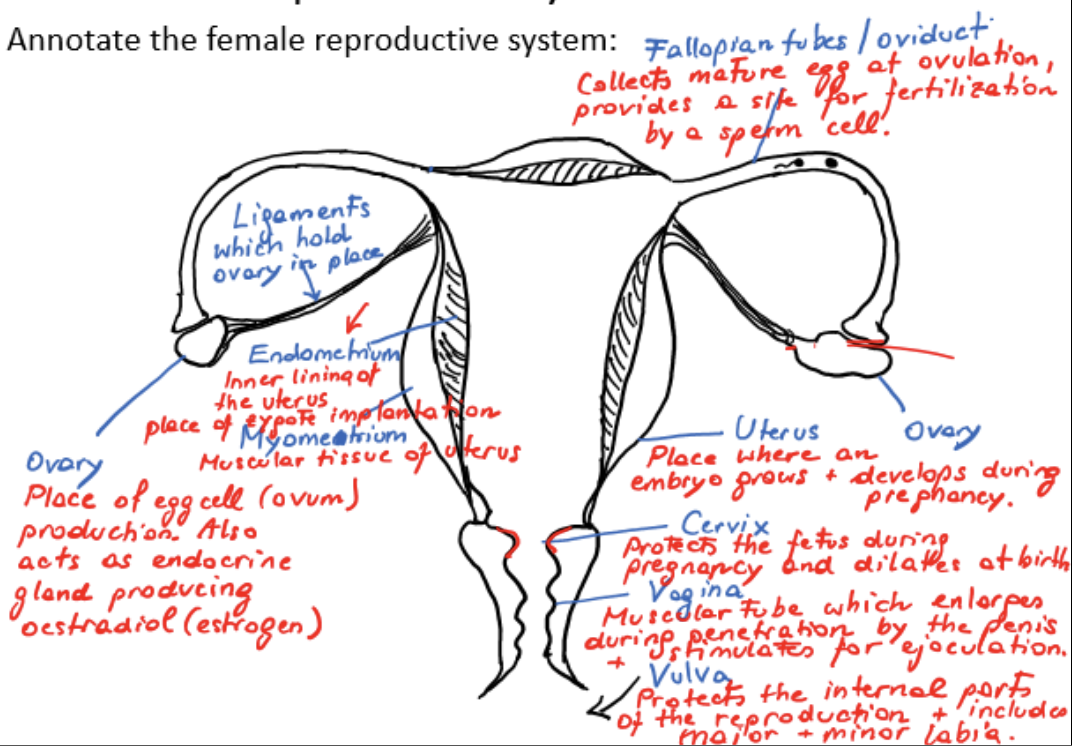
endometrium
inner lining of uterus, place of zygote implantation
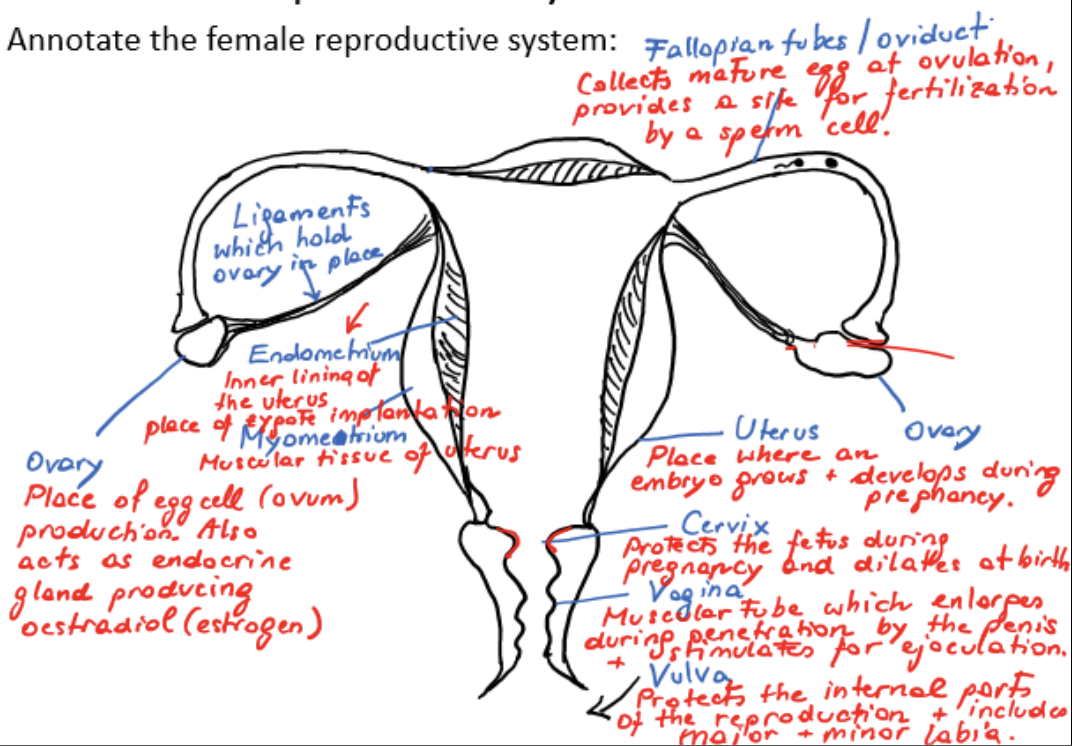
uterus
site where embryo grows and develops during pregnancy
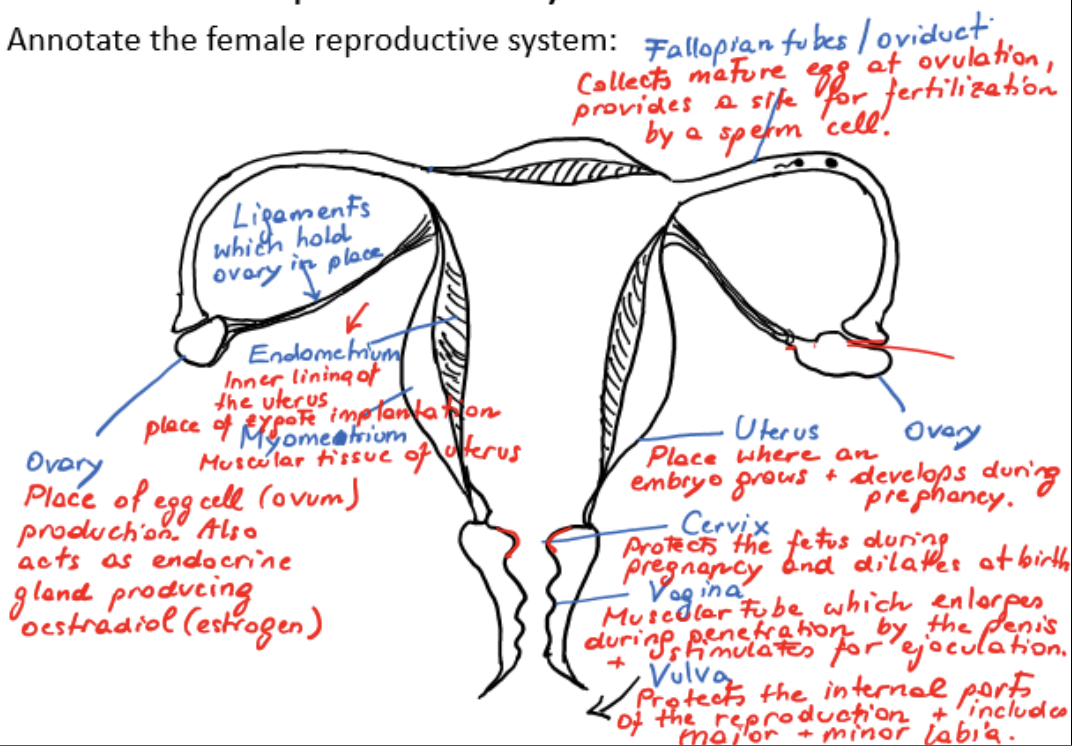
cervix
protects fetus during pregnancy, dilates at birth
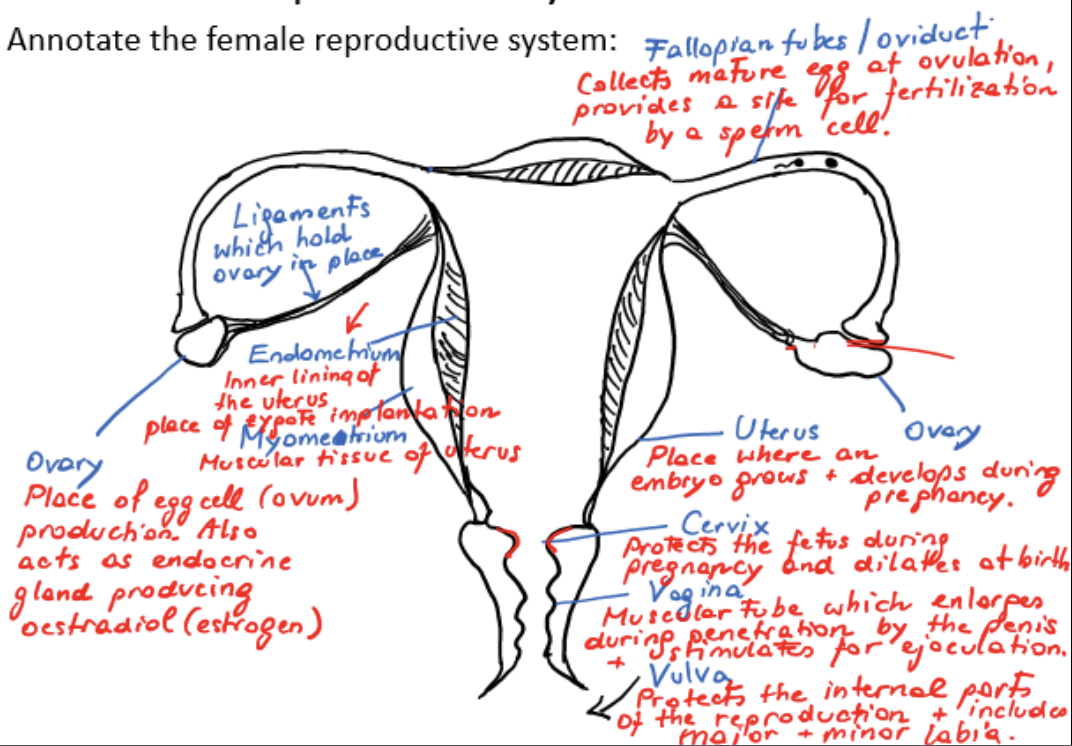
vagina
muscular tube which enlarges during penetration by the penis and stimulates ejaculation
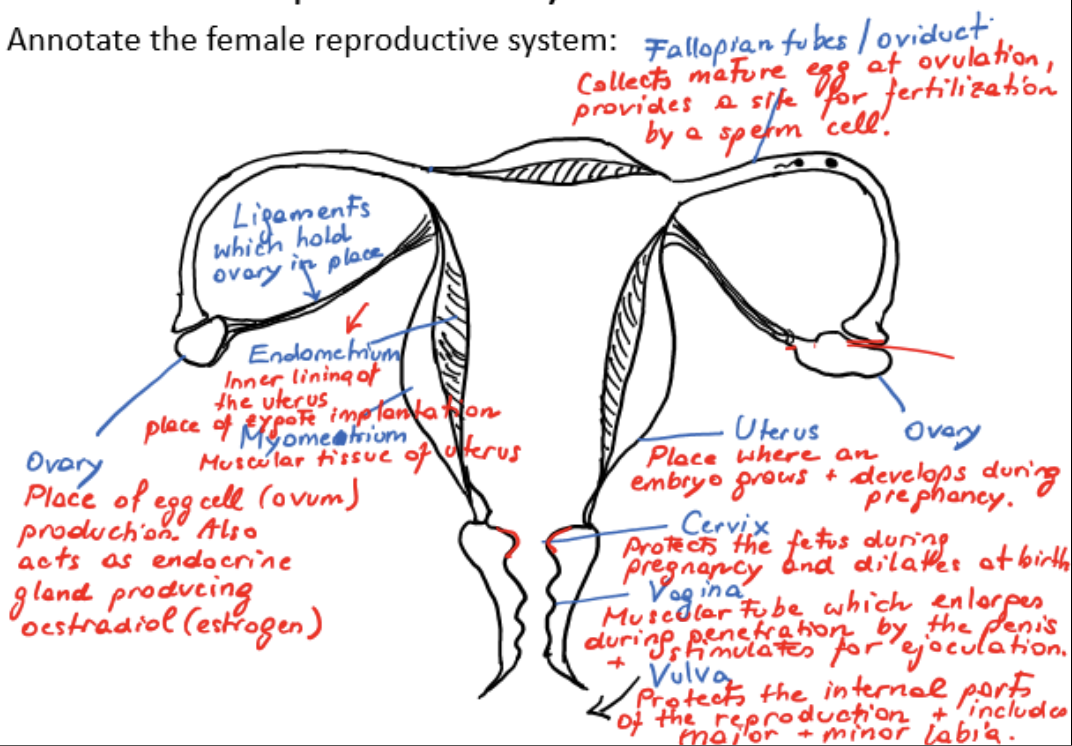
vulva
protects internal parts of reproduction and includes major and minor labia
zygote
formed when male and female nuclei fuse during fertilization
embryo
formed when cells begin to take up positions they will occupy in the young animal
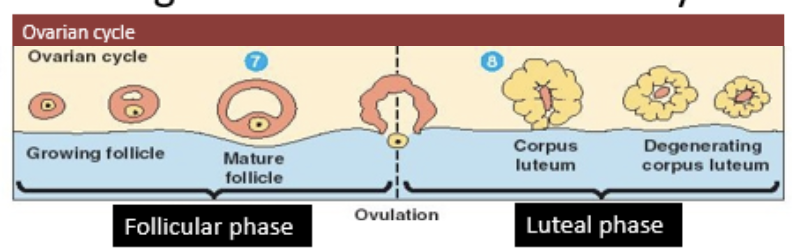
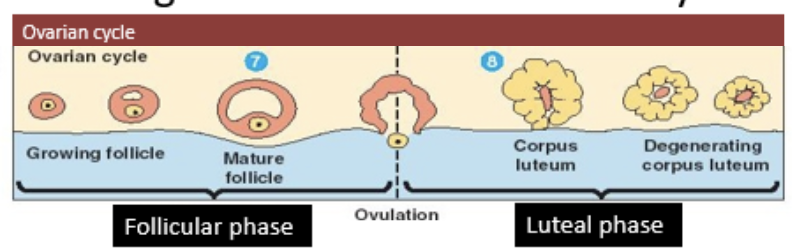
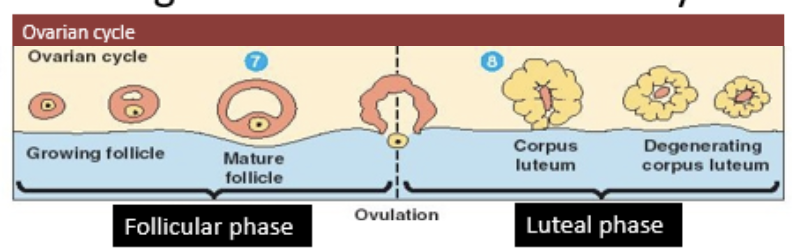
phases of the menstrual cycle
follicular phase and luteal phase
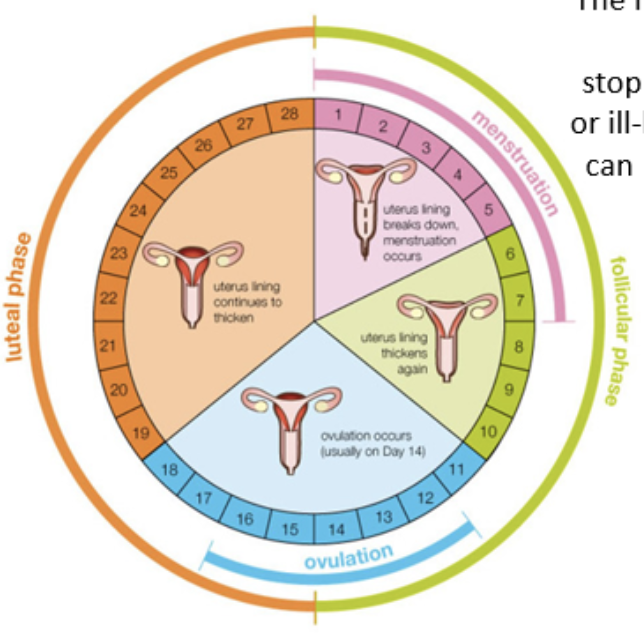
follicular phase
follicles develop inside the ovary and the female egg cell matures
follicles
nourishing cells surrounding the egg cell
ovum
female gamete, egg cell
ovulation
ovum is released into the oviduct from one of the ovaries
ovum moves down oviduct by peristalsis and cilia
peristalsis
rhythmic contractions of muscles in wall of oviduct
luteal phase
cells which released egg cell turn into corpus luteum
if no fertilization takes place, corpus luteum degenerates and new cycle begins
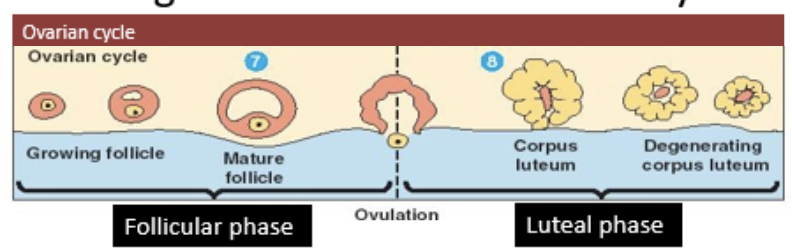
cycles of the menstrual cycle
ovarian cycle and uterine cycle
uterine cycle
uterine membrane breaks down during menstruation
uterine membrane is rebuilt slowly with blood vessels and tissue growth
endometrium becomes thicker and more richly supplied with blood vessels in preparation for egg cell implantation
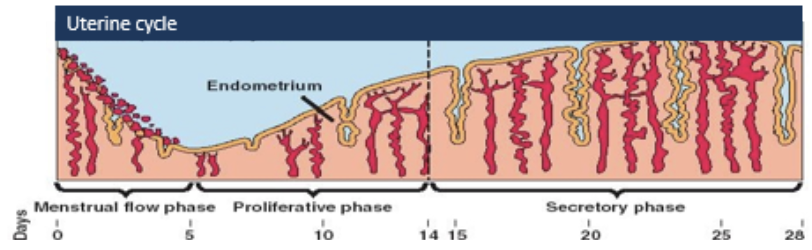
follicle stimultaing hormone (FSH)
secreted by pituitary gland
stimulates development of follicles, each containing an oocyte
stimulates follicles to secrete estradiol
determines ovarian cycle
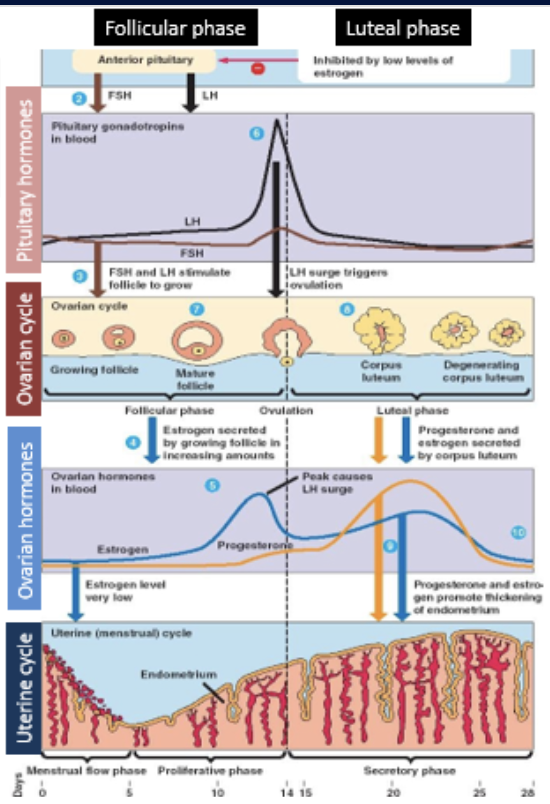
estradiol/estrogen
hormone responsible for repair and thickening of the endometrium in the uterus after menstruation, prepares for a potential implantation of a fertilized egg cell
ovarian hormone produced by developing egg inside ovary
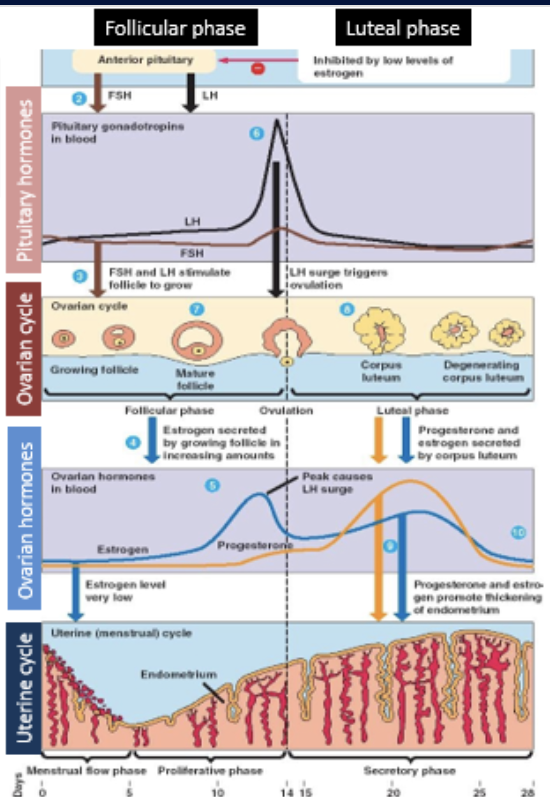
estradiol in low concentration
stimulates increase in FSH receptors
makes follicles more receptive to FSH
estradiol secretion increases
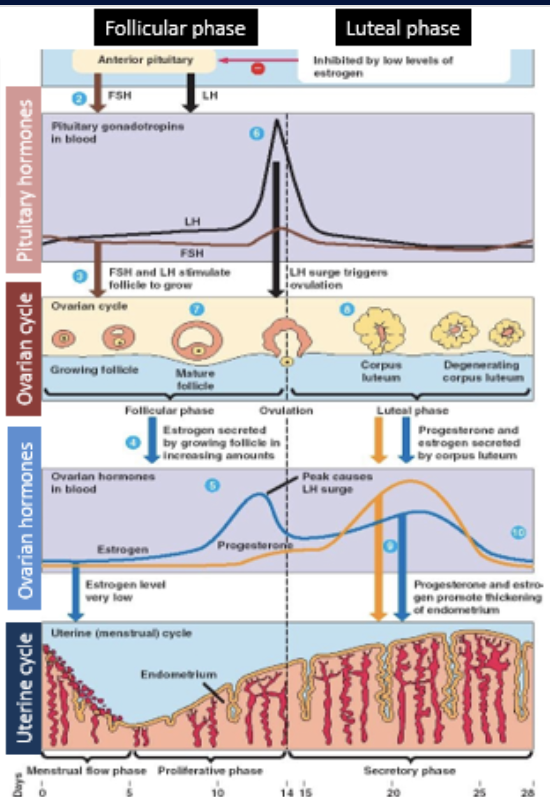
estradiol in high concentration
inhibits FSH release
stimulates secretion of LH by pituitary gland
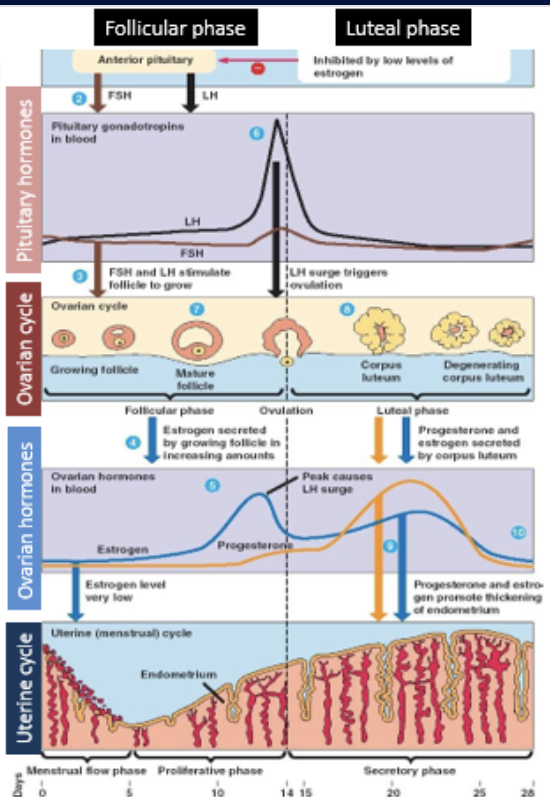
luteinizing hormone (LH)
peaks at the end of follicular phase in response to high estradiol concentration
stimulates completion of meiosis in the oocyte, causes ovulation
promotes conversion of follicle wall into temporary corpus luteum gland
stimulates corpus luteum to secrete estradiol and progesterone
hormone released from pituitary gland deetermining the ovarian cycle
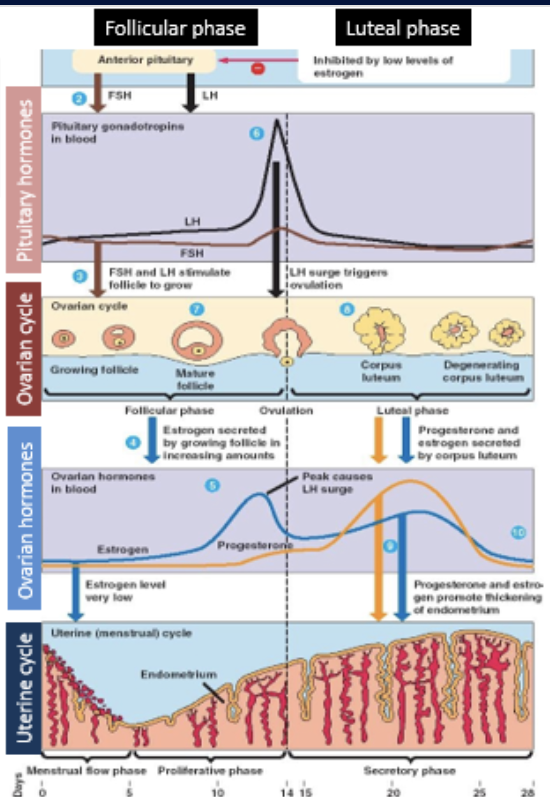
progesterone
secreted by corpus luteum
reaches peak by end of luteal phase
promotes thickening of endometrium
inhibits FSH and LH through negative feedback loop
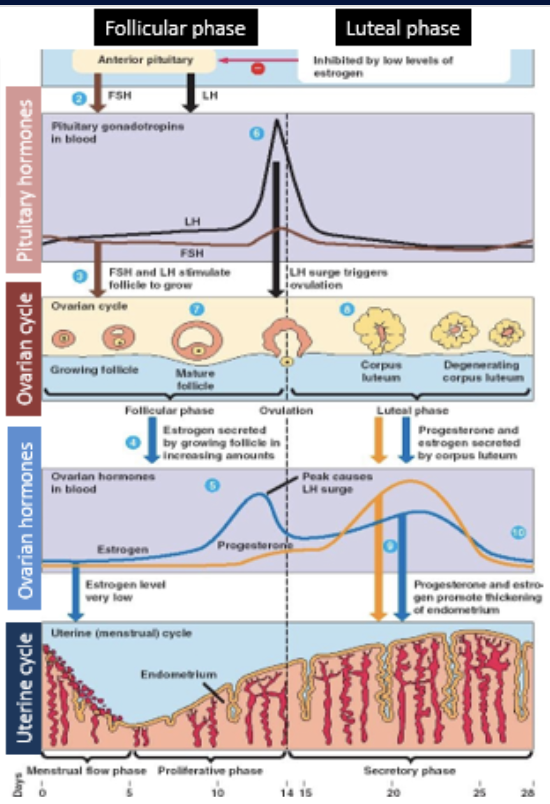
biological processes at the end of the luteal phase
levels of FSH and LH in bloodstream decrease due to high progesterone levels
low levels of FSH and LH cause the corpus luteum to degenerate