Pregnancy, Lactation, and Birth - 24 Months
1/58
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
59 Terms
How do we determine the nutrient/energy needs for those who are pregnant?
make used of a factorial model
have a basal baseline (for non-pregnant, non-lactating woman)
add other factors onto the baseline (amount deposited in fetus and related tissues, increased need for other tissues that expand during pregnancy such as blood volume, and different activity levels)
Are a woman’s needs the same through each trimester?
no
first trimester: little change compared to non-pregnant and non-lactating women
second trimester: needs increase
third trimester: highest caloric needs
What are the different weeks associated with the first, second, and third trimesters?
first: 1 - 13 weeks
second: 14 - 27 weeks
third: 28 - 40 weeks
How do we determine the energy needs during the different trimesters of pregnancy mathematically?
EER Equations made for each trimester (make sure age is in years, height in cm, and weight in kg, gestation in weeks, and takes into consideration physical activity levels)
for those in the first trimester, you can use the non-pregnant EER prediction equations
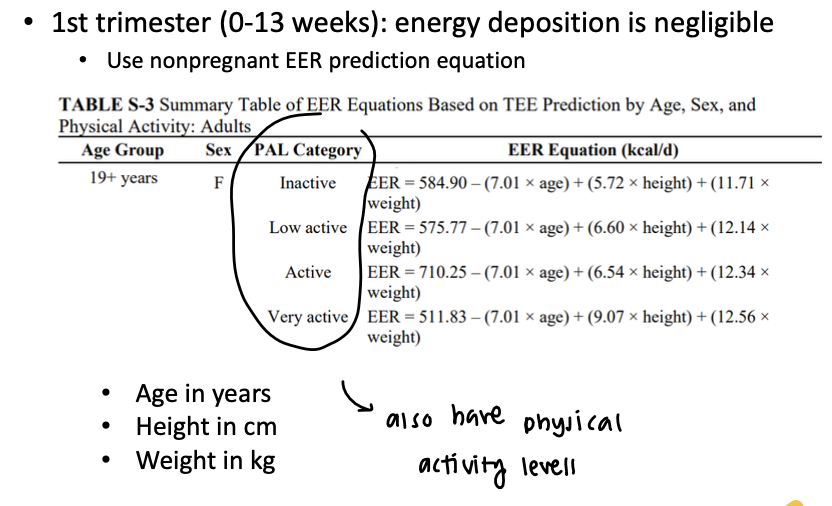
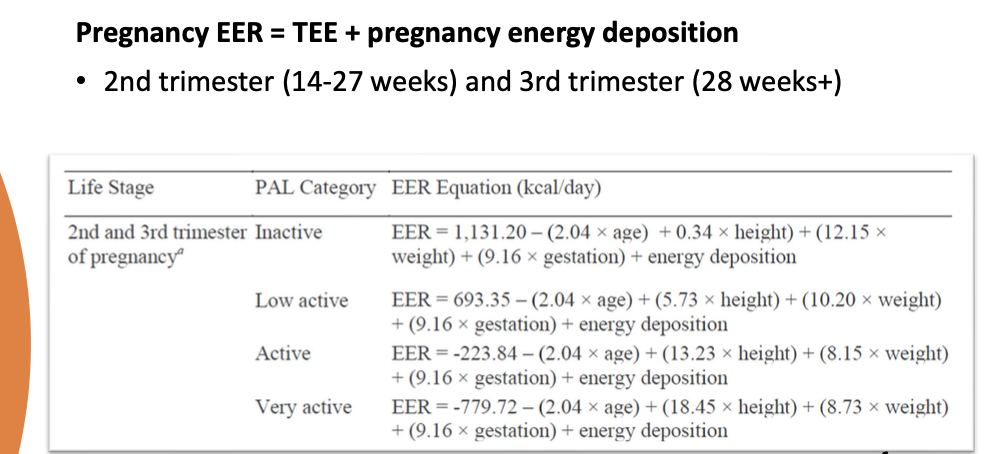
What is energy deposition? Why is it only taken into consideration when talking about the EER for the 2nd and 3rd trimester but not the first?
the extra calories needed for fetal growth and maternal tissue accumulation
different levels based on pre-pregnancy BMI
energy deposition in the first trimester is so little that it is negligible
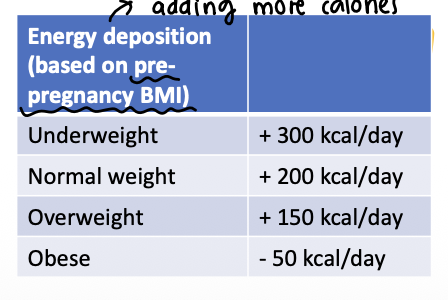
What is the healthy range of total weight gain for those who are pregnant (take into consideration their pre-pregnancy weight category)?
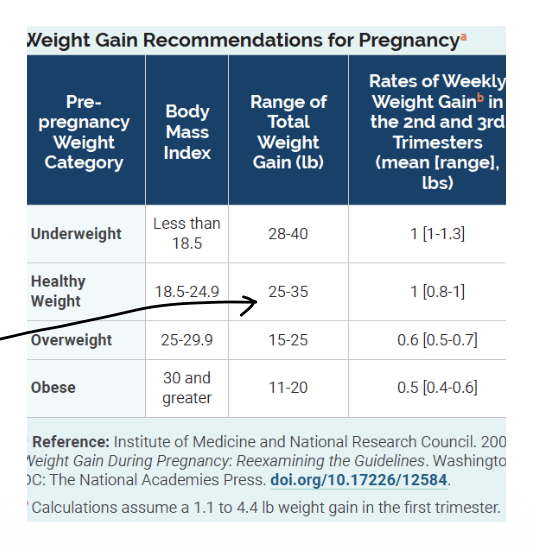
What are three Institute of Medicine (IOM) recommendations for pregnant women/those expecting to get pregnant ?
encourage women to reach normal body weight before pregnancy
promote prenatal weight gain within recommended ranges
women to return to normal weight by one year after delivery
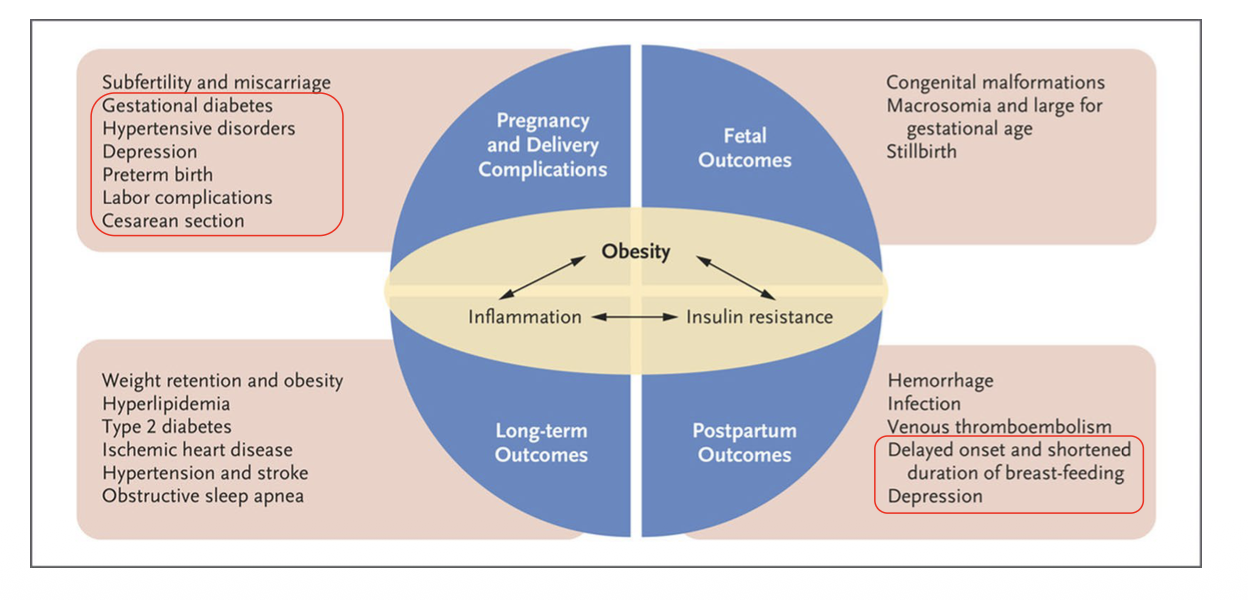
What is the issue with being overweight while pregnant?
being overweight/obese can impact the child and maternal health adversely
we see that the rates of those who are overweight and obese increasing in terms of those giving birth
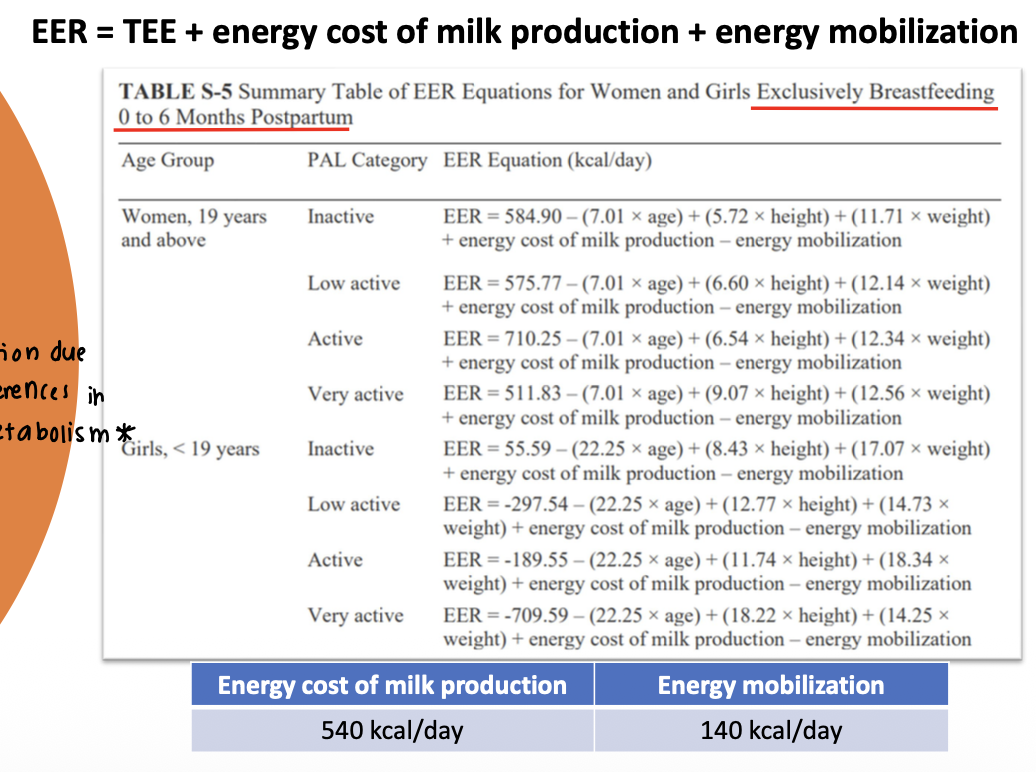
How do we determine the energy needs during lactation?
factorial model
basal needs for non-pregnant non lactating women
add onto the amount secreted in milk (assuming that milk output is 0.7 L/d at 0-6 months and 0.6 L/d at 7-12 months)
needs vary by stage of lactation
adjustments for amount available from other body tissues
girls < 19 separated from 19+ bc they have different metabolic needs, those < 19 are still growing themselves

What is the relationship between inches and cm? lbs and kg?
1 inch = 2.54 cm
1 kg = 2.2 lbs
What months are exclusively breastfeeding? What does this entail? What is partial breastfeeding?
exclusive = 0 - 6 months
breastfeeding every three hours
partial = 7 -12 months
What takes more metabolic energy, being pregnant or producing milk?
producing milk
What are the calorie changes that need to happen during lactation?

EER for first 6 months was calculated by adding 500 cal/day to pre-pregnancy needs - 170 cal/day to account for weight loss in the first 6 months postpartum
In general, why do women who are pregnant/lactating have a higher HEI score?
more conscious about being healthy
still lowkey low ~ 60, but still better than the average ~50
What are the 8 nutrients of concern for pregnant and lactating women? Which one apply to the general public? Which ones are specific for pregnancy and lactation?
general public too
calcium
vitamin D
potassium
dietary fiber
iron
specific for pregnancy and lactation
iron
folate/folic acid
iodine
choline
What changes occur for iron needs for those who are pregnant vs pre-pregnancy?
increases
pregnant: 27 mg
pre-pregnancy: 19 mg
How do iron requirements change during lactation before menstruation returns?
decreases
pre-pregnancy: 19 mg
lactation: 9 - 10 mg
How many women who are pregnant are affected by iron deficiency?
1/10
Wha are good sources of iron?
red meat and fortified cereals
How many women who are pregnant in their third trimester are affected by iron deficiency?
¼
more prevalent bc this is when most blood volume is developed within the baby
What is the RDA for folate during pregnancy and lactation?
pregnancy: 600 mcg DFE
lactation: 500 mcg DFE
typical: 400 mcg DFE
Why is folate important during pregnancy?
to prevent neural tube defects
1 month prior to conception
food sources and supplementation are both recommended
2-3 months of pregnancy
What are good sources of folate?
mushroom
dark leafy greens
legumes
Why is iodine important during pregnancy and lactation?
important for neurocognitive development of the fetus
many prenatal supplements do no contain iodine
What foods have iodine (4)?
dairy products
eggs
seafood
iodized table salt
What is the AI of iodine during pregnancy and lactation?
pregnancy: 220 mcg
lactation: 290 mcg
Why is choline important during pregnancy and lactation?
supports growth and development of child’s brain and spinal cord
many prenatal supplements do not contain choline
What is the AI of choline during pregnancy and lactation?
pregnancy: 450 mg
lactation: 550 mg
What foods have choline?
many dairy and protein foods
eggs
meats
some seafood
beans
peas
lentils
What is the recommended alcohol consumption for those who are pregnant/lactating?
pregnant: none
lactation: 1 drink/day is not known to be harmful to the infant
What is the recommended caffeine consumption for those who are pregnant/lactating?
pregnancy: low < 200 mg/day
lactation: ~ 300 mg/day OR 2-3 cups
What amount of exercise is recommended for women during pregnancy/lactation/postpartum?
at least 150 minutes/week of moderate intensity aerobic activity
helps to reduce risk of excessive weight gain and gestational diabetes
According to the 2025 DGAs, what are the top three nutrient priorities during pregnancy?
iron
folate
iodine
According to the 2025 DGAs, what should breastfeeding women consume?
a wide variety of nutrient-dense foods, including vitamin B12 rich protein sources (meats, poultry, eggs, and dairy), omega-3-rich seafood, folate rich legumes, and vitamin A rich vegetables
What are the age ranges for infants? toddlers?
infant: 0 - 1 year
toddler: 1 - 3 years
According to the 2025 DGA, what supplement should be provided to infants soon after birth?
vitamin D
What is recommended the first 6 months of life? What if no human milk is available?
0 - 6 months: exclusive breastfeeding with human milk
contains immunoglobulins that are beneficials for babies
if no human milk = switch to iron fortified infant formula
continue as long as mutually desired
Why is it recommended that the first 6 months of life are exclusively breastfeeding (5)?
promotes bonding between baby and parent
protective against gastrointestinal infections
prolongs duration of lactational amenorrhea (temporary infertility)
accelerates maternal weight loss
may enhance motor, cognitive, and social-emotional development of child
What percent of infants were ever fed human milk?
84%
What percent of infants were exclusively fed human milk through 6 months?
35%
What percent of kids continue to be fed any human milk at 12 months?
35%
What has contributed to low breastfeeding of kids?
no federally mandated paid maternal leave
When should infants be introduced to nutrient dense complimentary foods, and potentially allergenic foods?
at about 6 months
need to be nutrient dense bc its a time of rapid growth and they have small stomachs
should still complement human milk or infant formula
not recommended to introduce before 4 months
What nutrients should be fed to infants? Especially for those who are fed human milk?
iron and zinc
What is the main source of nutrition for infants up to 12 months of age?
breast milk/formula
According the DGA how should parents encourage healthy eating?
offering new foods multiple times (8 - 10 exposures) and modeling healthy eating behaviors
What food groups do 12- 23 month year olds have trouble meeting the requirement for?
vegetables
fruits
grains
dairy
protein foods
vegetables
What are the four benefits of introducing complementary foods?
adequate nutrition
exposure to flavors, textures, and different types of foods
age and developmentally appropriate foods to prevent choking
introduction of potentially allergenic foods
Which of the following is not a nutrient of concern for breastfed infants?
folic acid
iron
vitamin D
zinc
folic acid
the rest are low in breastmilk
folic acid primarily an issue during pregnancy
What is the role of iron for infants and toddlers?
supports neurologic development and immune function
Why do breastfed babies need iron?
human milk contains low iron
born with body stores of iron adequate for first 6 months
77% of infants fed human milk have inadequate iron intake
What is the role of zinc for infants and toddlers?
supports growth and immune function
What are food sources of zinc (3)?
meats
beans
zinc fortified iron cereals
Why do breastfed babies need zinc?
zinc content in human milk declines after 6 months
54% of infants fed human milk have inadequate zinc intake
What are the top allergenic foods (8)?
peanuts
egg
cow milk products
tree nuts
wheat
crustacean shellfish
fish
soy
What are some foods to avoid for infants and toddlers (4)?
sugar
sodium
honey (has botulism)
unpasteurized foods and beverages
What are five signs that a child is ready to begin eating solid foods?
can control head and neck
sitting up alone or without support
bringing objects to the mouth
trying to grasp small objects (toys or foods)
swallowing food rather than pushing it back out
What are some signs that a child is hungry or full?

What are some benefits of baby led weaning?
they themselves can become familiar with different textures and flavors
learns self regulation, grows independence, and improves their manual dexterity