NAPLEX Pharmacy Foundations 1: Chapter 2 Basic Science Concepts
1/101
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
102 Terms
Define substrate (or ligand)
A substance that creates a signal or produces an effect by binding to a receptor, enzyme, or transporter
Define endogenous
A substance produced by the body (such as a naturally produced substrate)
Define exogenous
Substances produced outside of the body (e.g. drugs and chemicals)
Define agonist
A substance that combines with a receptor to initiate a reaction
Can be endogenous or exogenous (i.e. mimicking an endogenous substrate)
Define antagonist
A substance that combines with a receptor and blocks or reduces a reaction by preventing the agonist from binding to the receptor
Can be endogenous or exogenous
Define induction
When a substance increases the activity of an enzyme
induction = increase
Define inhibition
When a substance decreases or blocks the activity of an enzyme
What makes up the central nervous system (CNS)?
brain and spinal cord
What does the CNS control? How?
Controls bodily functions by sending signals to the peripheral nervous system (PNS)
What are the two systems of the PNS?
somatic nervous system and autonomic nervous system
What does the somatic nervous system control?
skeletal muscles (i.e. voluntary movements)
What does the autonomic nervous system control?
Digestion, cardiac muscle, BP (i.e. involuntary actions)
How is signal transmission between the CNS and PNS accomplished?
Via Neurotransmitters (NTs)
What are neurotransmitters? Where are they released?
chemical messengers released by presynaptic neurons
What are common neurotransmitters?
Acetylcholine (ACh)
Epinephrine (Epi)
Norepinephrine (NE)
Dopamine (DA)
Serotonin (5-HT)
What is the primary NT involved in the somatic nervous system?
ACh
What receptors in the skeletal muscles do ACh bind to affect muscle movement?
nicotinic receptors (Nn)
What are the two divisions of the autonomic nervous system?
Parasympathetic nervous system (PSNS) and sympathetic nervous system (SNS)
What is the PSNS responsible for?
rest and digest
How does the PSNS work?
Releases ACh, which binds to muscarinic receptors throughout the body (e.g. GI tract, bladder, eyes)
What is the physiologic response to activation of the PSNS?
increased SLUDD
What does SLUDD stand for?
Salivation
Lacrimation
Urination
Defecation (peristalsis)
Digestion (peristalsis)
What is SNS known as?
fight or flight
How does the SNS work?
Releases Epi and NE, which act on adrenergic receptors (alpha-1, beta-1, and beta-2) in the cardiovascular and respiratory systems
What is the physiologic response on SNS activation?
increased BP, HR, and bronchodilation
Describe the process and effects of a substrate binding to a receptor
A substrate (ligand) binds to a receptor. The receptor-substrate complex causes a signal cascade into the cell which causes a biologic effect/response
Describe competitive inhibition
Occurs when an antagonist binds to the same active site of a receptor as the endogenous substrate, thus preventing it from binding
Describe non-competitive inhibition
Occurs when an antagonist binds to the receptor at a site other than the active site (i.e. allosteric site), which changes the shape of the active site and prevents the endogenous substrate from binding
True or False: Some medications affect multiple receptors.
True
What are a couple examples of drugs that affect multiple receptors?
1) Isoproterenol: mixed beta-1 and beta-2 agonist
2) Carvedilol: alpha-1, beta-1, and beta-2 antagonist
3) Vasopressors: stimulate alpha-1 and beta-1 receptors
How does clonidine affect the amount of NT released and available to the PNS?
Clonidine acts centrally as an agonist of the alpha-2 adrenergic receptors. Stimulation reduces release of Epi and NE and decreases sympathetic output
For Muscarinic Receptors:
Endogenous Substrate?
Agonist Action?
Drug agonists?
Antagonist Action?
Drug antagonists?
Endogenous Substrate: ACh
Agonist action: ↑ SLUDD
Drug agonists: pilocarpine, bethanechol
Antagonist action: ↓ SLUDD
Drug antagonists: atropine, oxybutynin
For Nicotinic Receptors:
Endogenous Substrate?
Agonist Action?
Drug agonists?
Antagonist Action?
Drug antagonists?
Endogenous Substrate: ACh
Agonist Action: ↑ HR, BP
Drug agonists: Nicotine
Antagonist Action: Neuromuscular blockade
Drug antagonists: Neuromuscular blockers (e.g. rocuronium)
For Alpha-1 Receptors (mostly peripheral):
Endogenous Substrate?
Agonist Action?
Drug agonists?
Antagonist Action?
Drug antagonists?
Endogenous Substrate: Epi, NE
Agonist Action: Smooth muscle vasoconstriction, ↑ BP
Drug agonists: Phenylephrine, dopamine (dose-dependent)
Antagonist Action: smooth muscle vasodilation, ↓BP
Drug antagonists: Alpha-1 blockers (e.g. doxazosin, carvedilol, phentolamine)
For Alpha-2 Receptors (mainly brain; central):
Endogenous Substrate?
Agonist Action?
Drug agonists?
Antagonist Action?
Drug antagonists?
Endogenous Substrate: Epi, NE
Agonist Action: ↓ release of Epi and NE, ↓BP, HR
Drug agonists: Clonidine, brimonidine (ophthalmic for glaucoma)
Antagonist Action: ↑ BP, HR
Drug antagonists: Ergot alkaloids, yohimbine
For Beta-1 Receptors (mainly heart):
Endogenous Substrate?
Agonist Action?
Drug agonists?
Antagonist Action?
Drug antagonists?
Endogenous Substrate: Epi, NE
Agonist Action: ↑ myocardial contractility, CO, HR
Drug agonists: dobutamine, isoproterenol, dopamine (dose-dependent)
Antagonist Action: ↓ CO, HR
Drug antagonists: Beta-1 selective blockers (metoprolol) and non-selective beta blockers (carvedilol, propranolol)
For Beta-2 Receptors (mainly lungs):
Endogenous Substrate?
Agonist Action?
Drug agonists?
Antagonist Action?
Drug antagonists?
Endogenous Substrate: Epi
Agonist Action: bronchodilation
Drug agonists: albuterol, terbutaline, isoproterenol
Antagonist Action: bronchoconstriction
Drug antagonists: Non-selective beta blockers (carvedilol, propranolol
For Dopamine Receptors:
Endogenous Substrate?
Agonist Action?
Drug agonists?
Antagonist Action?
Drug antagonists?
Endogenous Substrate: Dopamine
Agonist Action: Many, including renal, cardiac, and CNS effects
Drug agonists: Levodopa, pramipexole
Antagonist Action: Many, including renal, cardiac, and CNS effects
Drug antagonists: 1st Gen antipsychotics, (e.g. haloperidol), metoclopramide
For Serotonin Receptors:
Endogenous Substrate?
Agonist Action?
Drug agonists?
Antagonist Action?
Drug antagonists?
Endogenous Substrate: 5-HT
Agonist Action: Many, including platelet, GI, and psychiatric effects
Drug agonists: Triptans (e.g. sumatriptan)
Antagonist Action: Many, including platelet, GI, and psychiatric effects
Drug antagonists: Ondansetron, 2nd Gen/Atypical antipsychotics (e.g. quetiapine)
What is an enzyme?
Compounds that speed up (catalyze) a reaction
How do substrates interact with enzymes?
Can be agonistic or antagonistic and competitive or non-competitive
What NTs is MAO (monoamine oxidase) enzyme responsible for breaking down?
Catecholamines:
Dopamine
Epi
NE
5-HT
What occurs when multiple drugs work similarly at the same receptor or enzyme?
Additive effects, which can be detrimental
What AEs can occur due to additive effects with MAO inhibitors? Why?
Hypertensive crisis
Serotonin syndrome
Occurs due to excess catecholamine accumulation
Examples of drug classes that can cause additive effects with MAO inhibitors?
SSRIs
SNRIs
TCAs
Etc.
For the Acetylcholinesterase enzyme:
Endogenous effects?
Drug Inhibitors?
Drug Action?
Endogenous effects: breaks down ACh
Drug Inhibitors: donepezil, rivastigmine, galantamine
Drug Action: Inhibits acetylcholinesterase, resulting in ↑ ACh
For the Angiotensin-Converting Enzyme (ACE):
Endogenous effects?
Drug Inhibitors?
Drug Action?
Endogenous effect: converts angiotensin I to angiotensin II
Drug Inhibitors: ACE-inhibitors (e.g. ramipril, lisinopril)
Drug Action: inhibits conversion of angiotensin I to angiotensin II, resulting in ↓ vasoconstriction and ↓ aldosterone secretion
For the Catechol-O-methyltransferase (COMT) enzyme:
Endogenous effects?
Drug Inhibitors?
Drug Action?
Endogenous effects: Breaks down levodopa
Drug Inhibitors: COMT-inhibitor (entacapone)
Drug Action: Inhibits the COMT enzyme to prevent peripheral break down of levodopa, resulting in ↑ duration of action of levodopa
For the Cyclooxygenase (COX) enzyme:
Endogenous effects?
Drug Inhibitors?
Drug Action?
Endogenous effects: converts arachidonic acid to prostaglandins (cause inflammation) and thromboxane A2 (causes platelet aggregation)
Drug Inhibitors: NSAIDs (e.g. aspirin, ibuprofen)
Drug Action: Block COX enzymes to ↓ prostaglandins and thromboxane A2
For the Monoamine oxidase (MAO) enzyme:
Endogenous effects?
Drug Inhibitors?
Drug Action?
Endogenous effects: Breaks down catecholamines
Drug Inhibitors: MAO inhibitors (MAOIs): phenelzine, isocarboxazid, tranylcypromine, selegiline, rasagiline
Drug Action: Inhibits MAO which ↑ catecholamine levels
For the Phosphodiesterase (PDE) enzyme:
Endogenous effects?
Drug Inhibitors?
Drug Action?
Endogenous effects: Breaks down cGMP, a smooth muscle relaxant
Drug Inhibitors: PDE-5 inhibitors (e.g. sildenafil, tadalafil)
Drug Action: Competitively binds to the same active site as cGMP on the PDE-5 enzyme, preventing the breakdown of cGMP and prolonging smooth muscle relaxation
For the Vitamin K epoxide reductase (VKOR) enzyme:
Endogenous effects?
Drug Inhibitors?
Drug Action?
Endogenous effects: converts vit. K to the active form required for production of clotting factors
Drug Inhibitors: Warfarin
Drug Action: Inhibits VKOR enzyme which ↓ production of clotting factors II, IV, IX, and X
For the Xanthine Oxidase enzyme:
Endogenous effects?
Drug Inhibitors?
Drug Action?
Endogenous effects: Breaks down hypoxanthine into xanthine and then xanthine into uric acid
Drug Inhibitors: Xanthine oxidase inhibitor: allopurinol
Drug Action: Blocks xanthine oxidase enzyme which decreases uric acid production
What is structure-activity relationship?
the relationship between the molecular structure of a drug and its activity
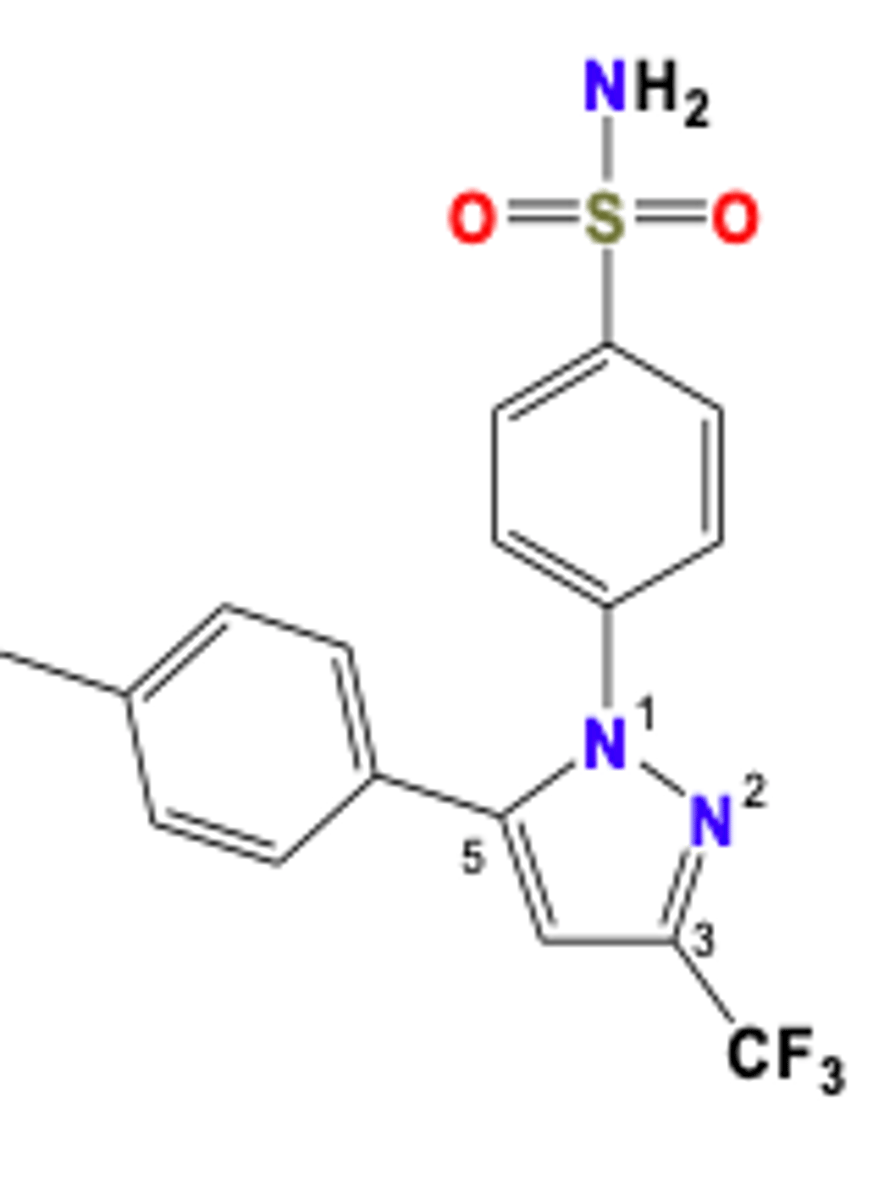
Celecoxib structure
Has a sulfa group
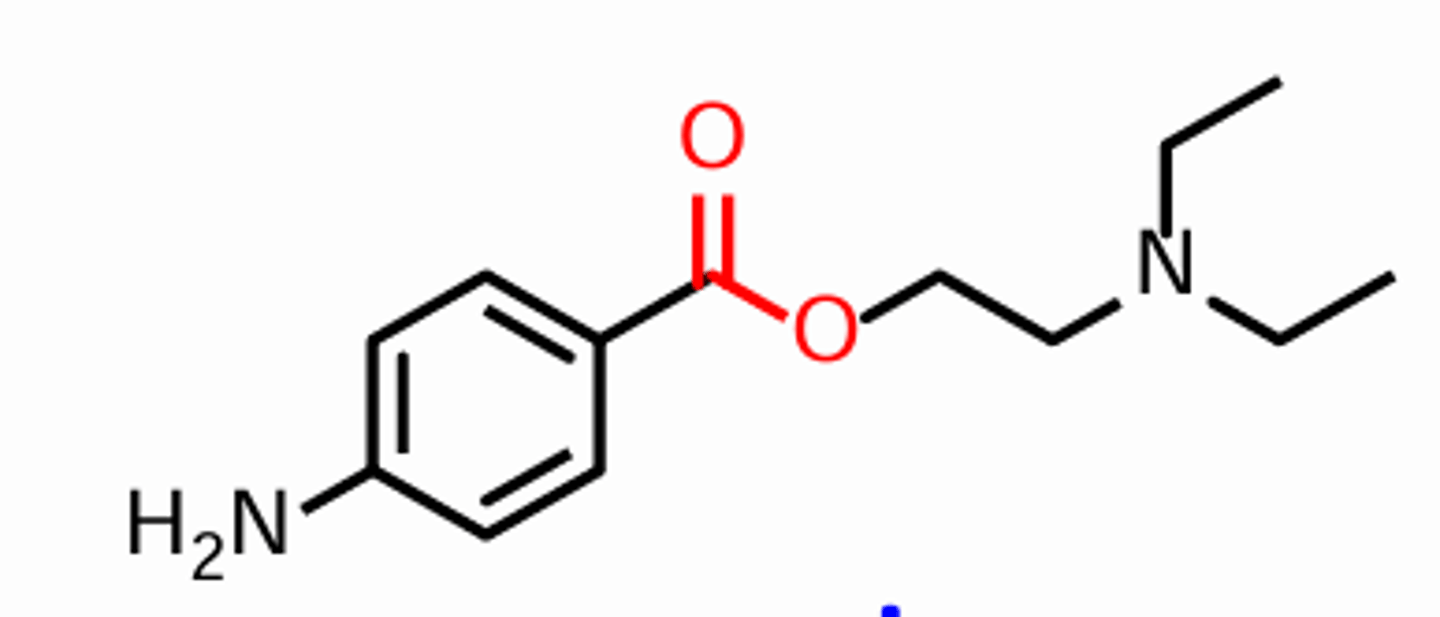
Procaine structure
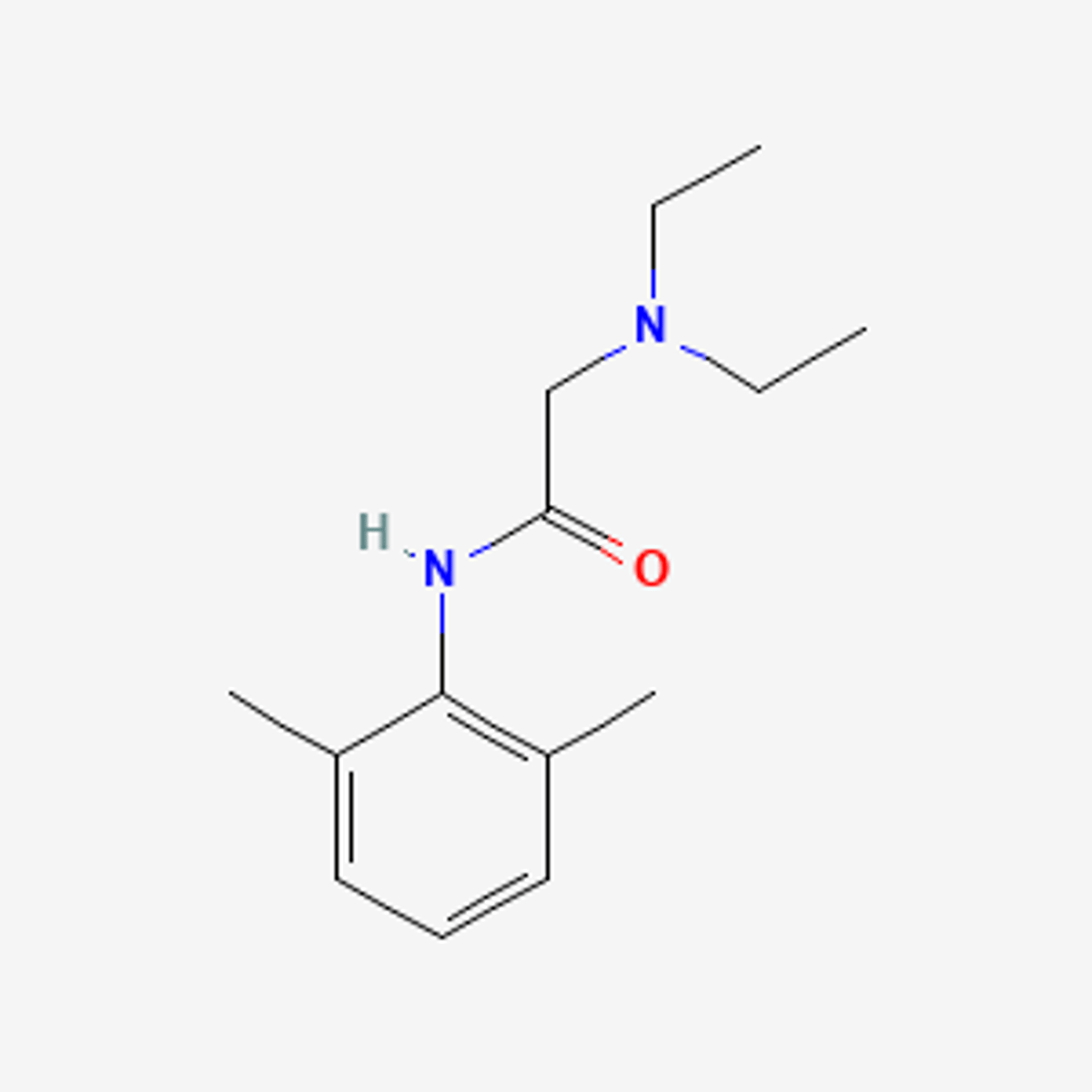
Lidocaine structure
What are the neutral functional groups?
Hydroxyl or alcohol (primary)
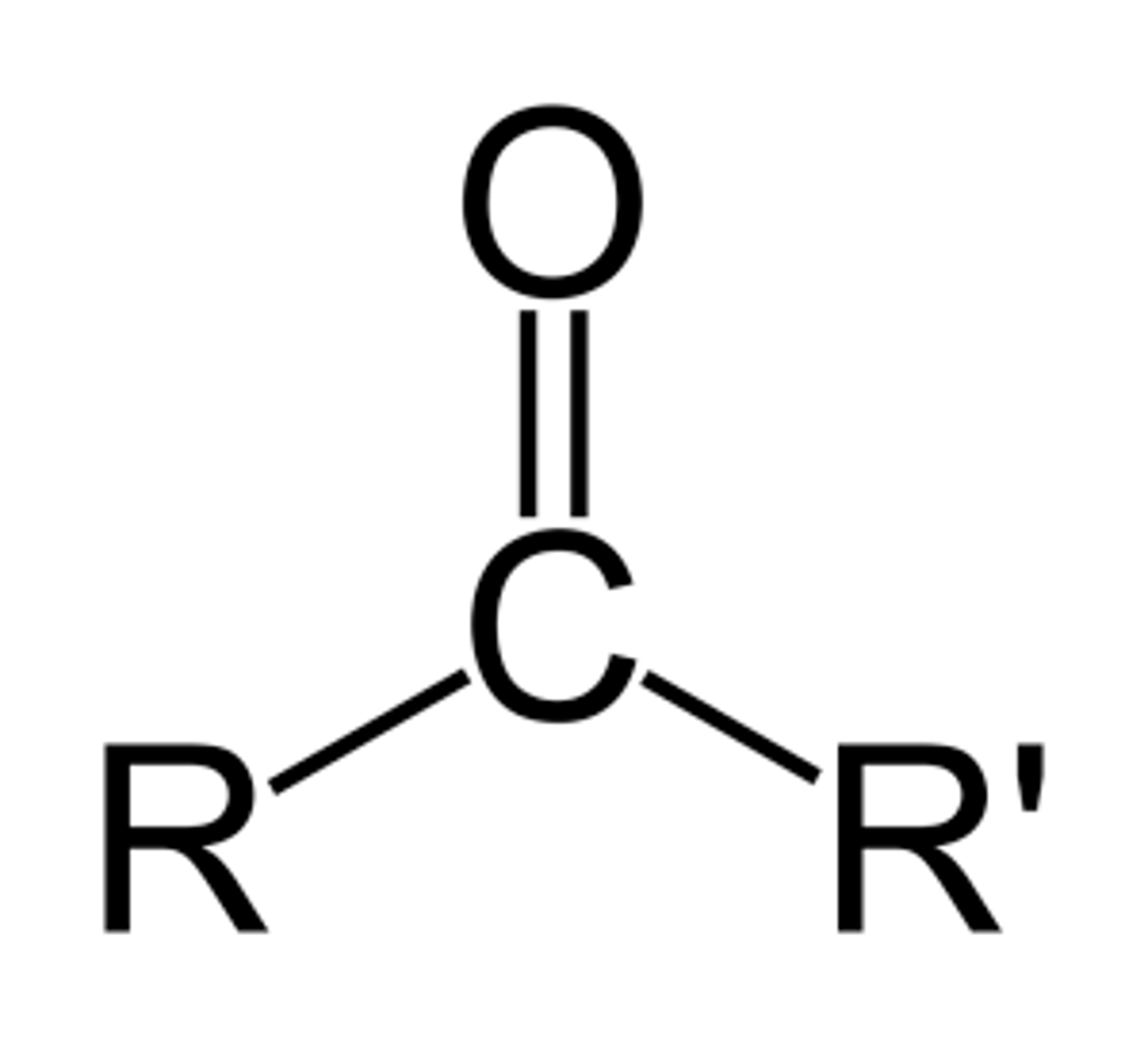
Ketone
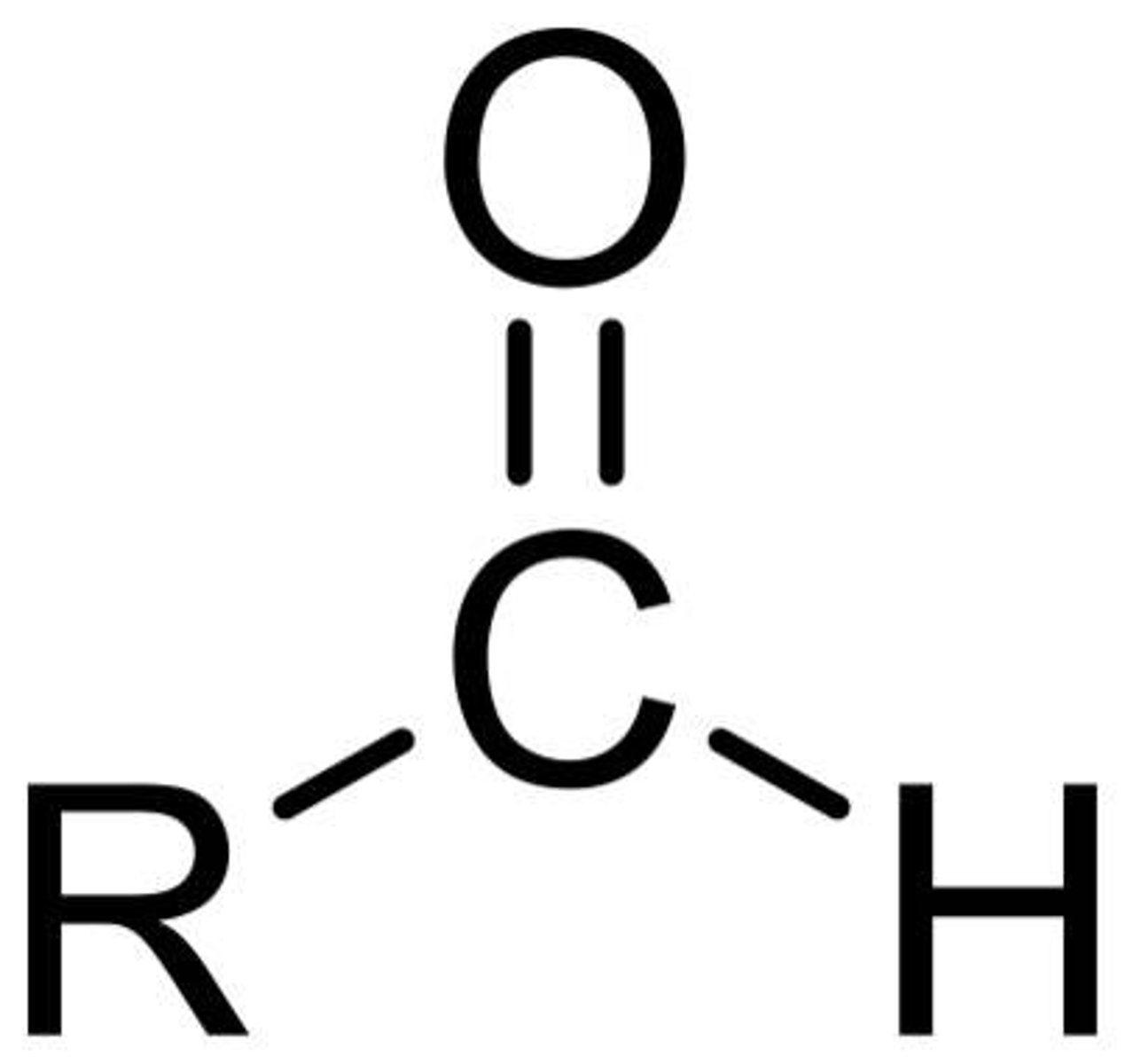
Aldehyde
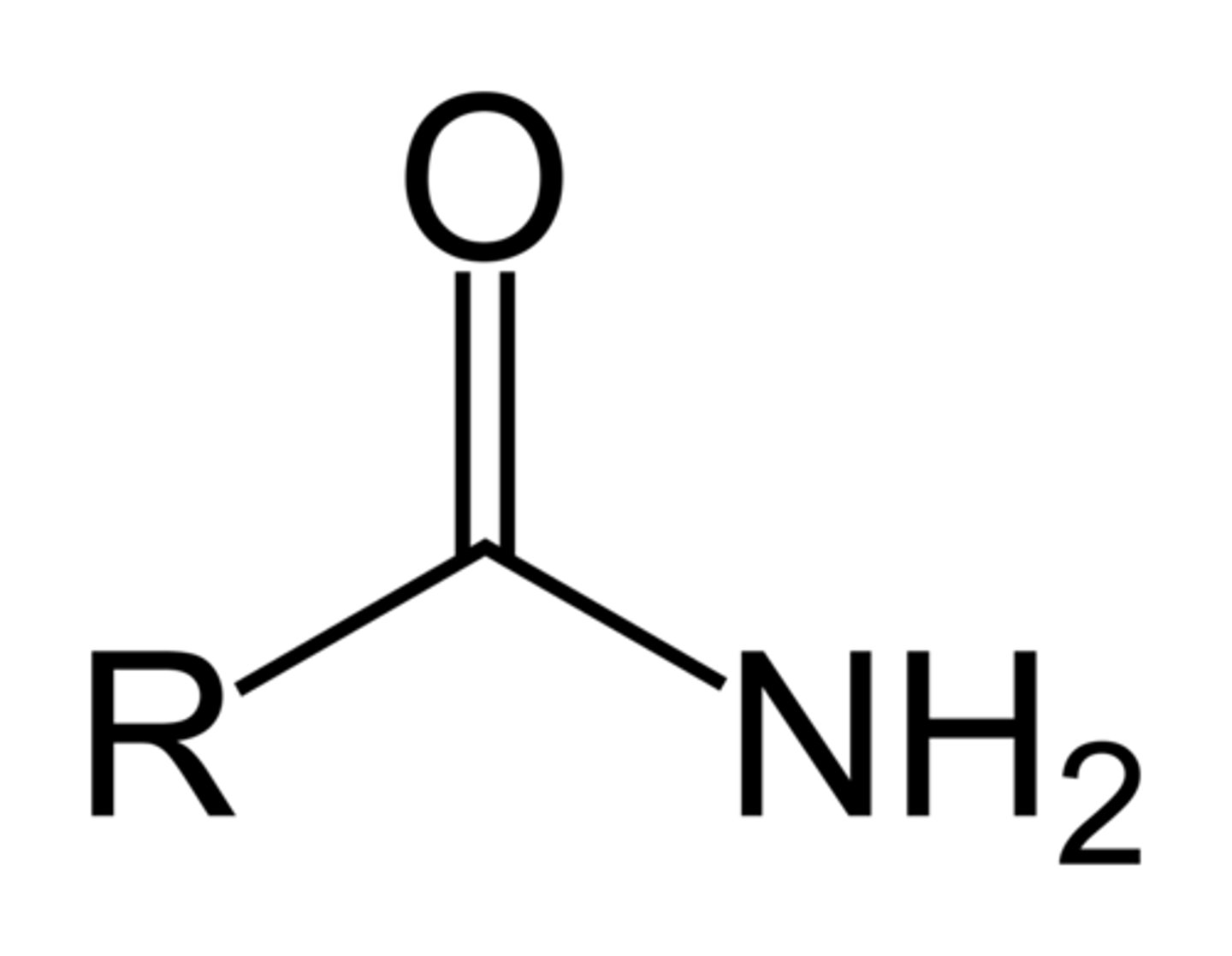
Amide
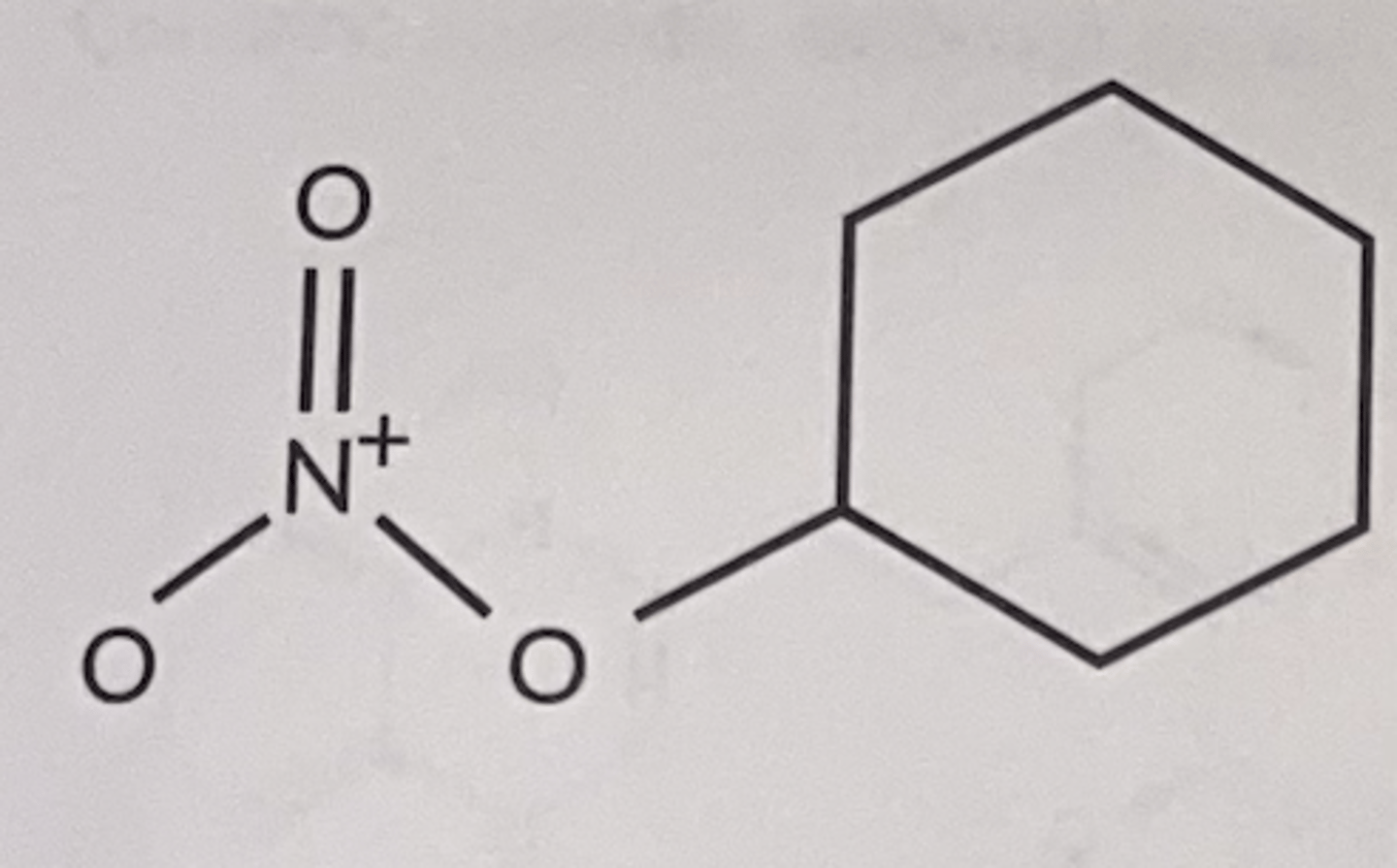
Nitrate
Nitro
Aromatic (Benzo) ring
Urea
Carbonate
Carbamate
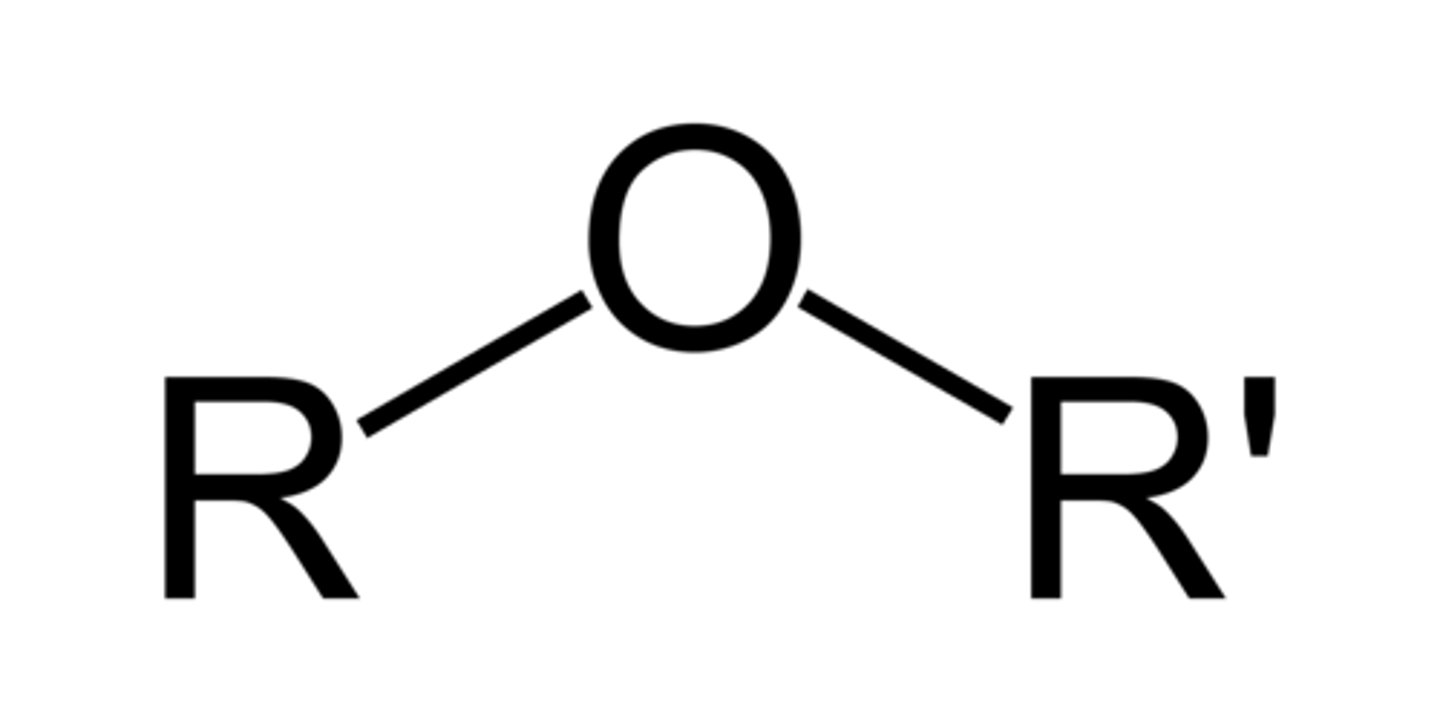
Ether
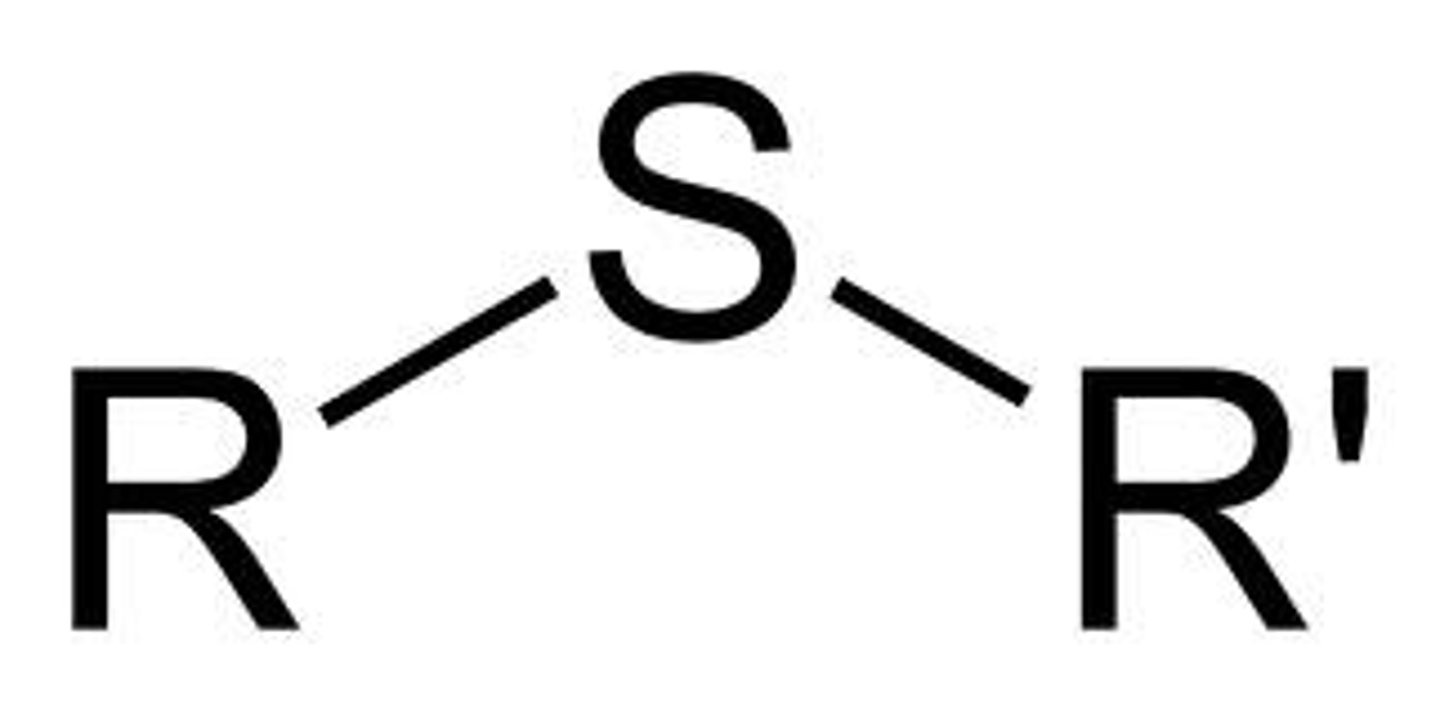
Thioether
Hydroxyl functional group
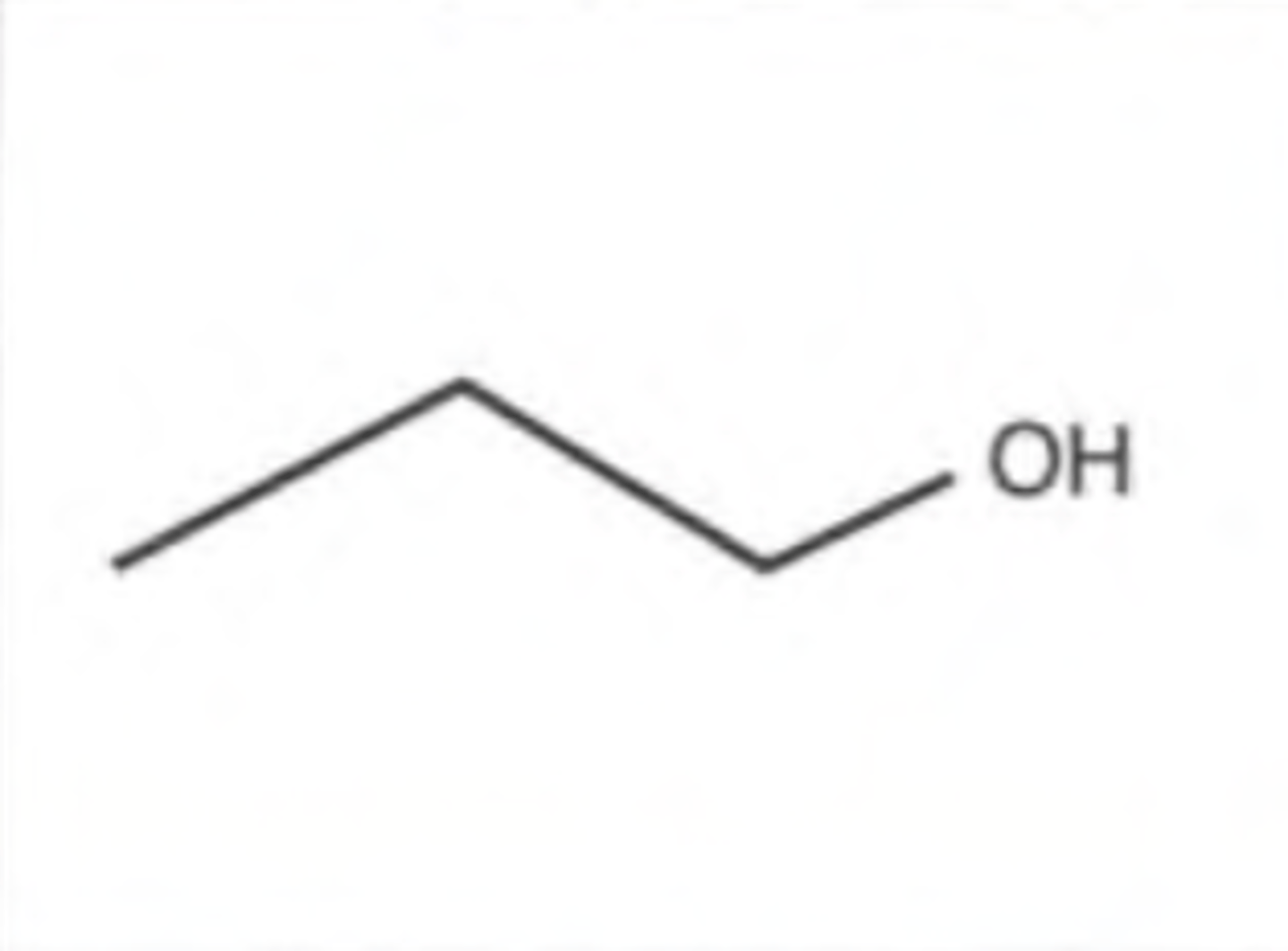
Ketone functional group
Aldehyde functional group
Amide functional group
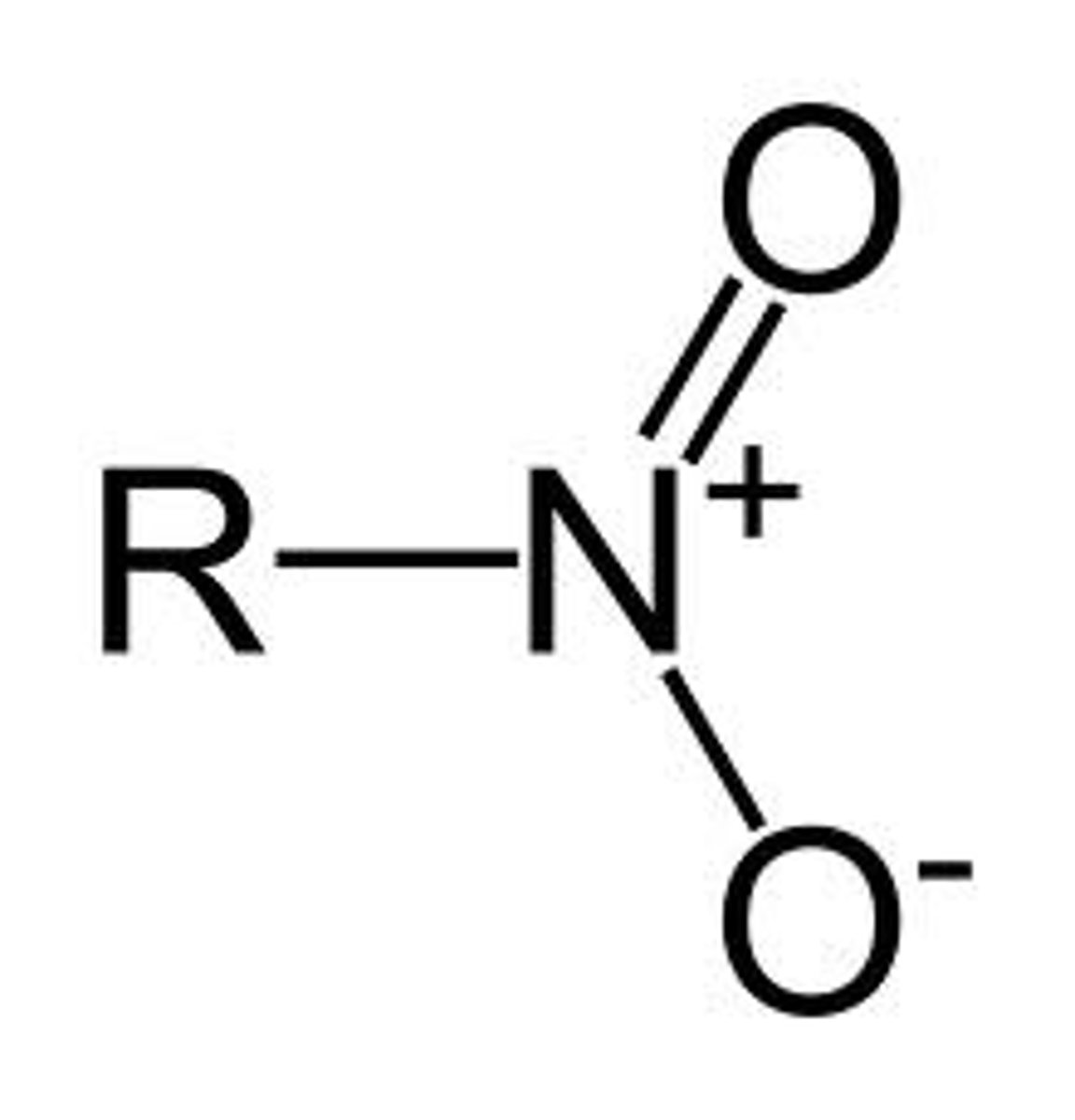
Nitrate functional group
Nitro functional group
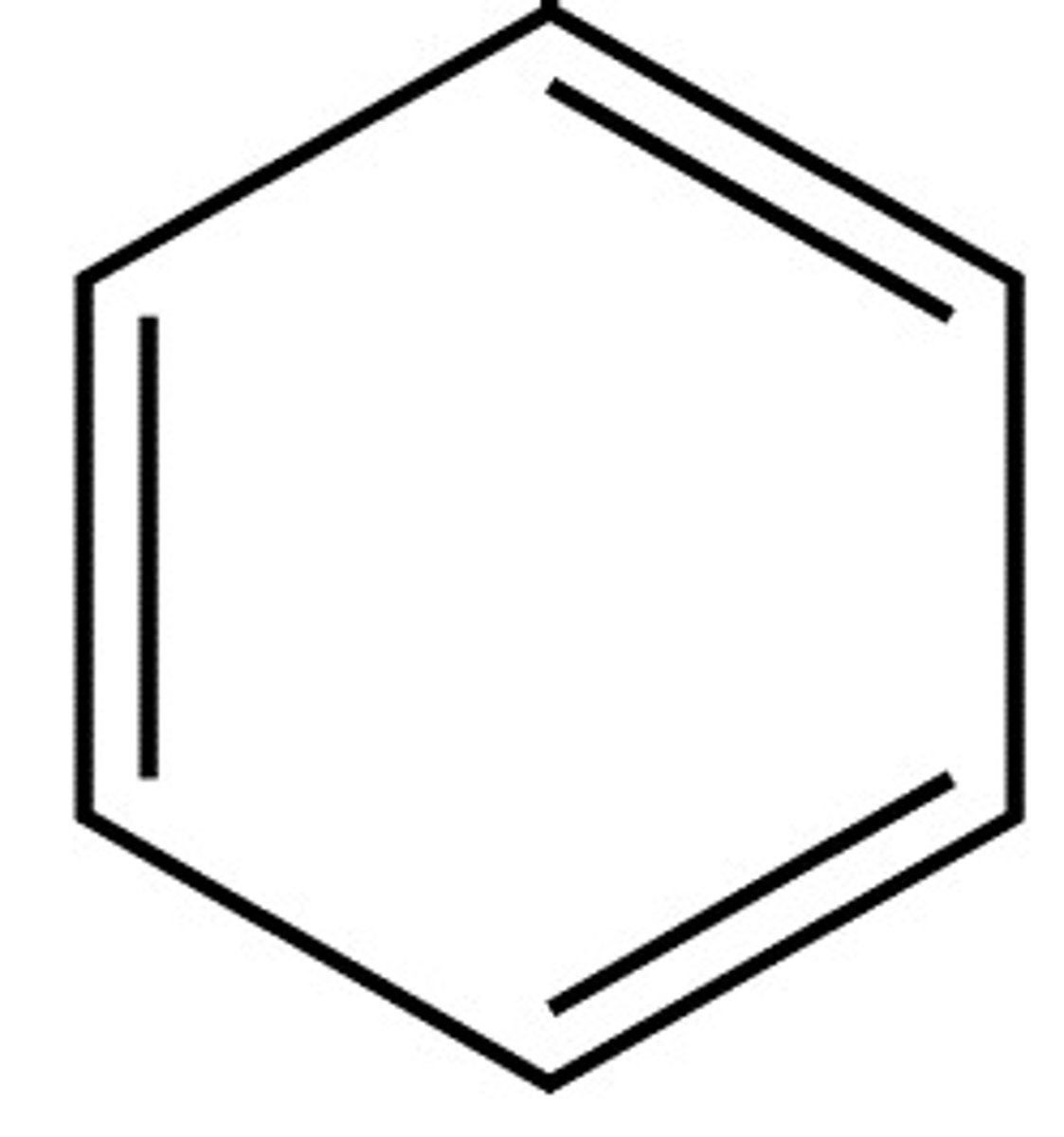
Benzene ring
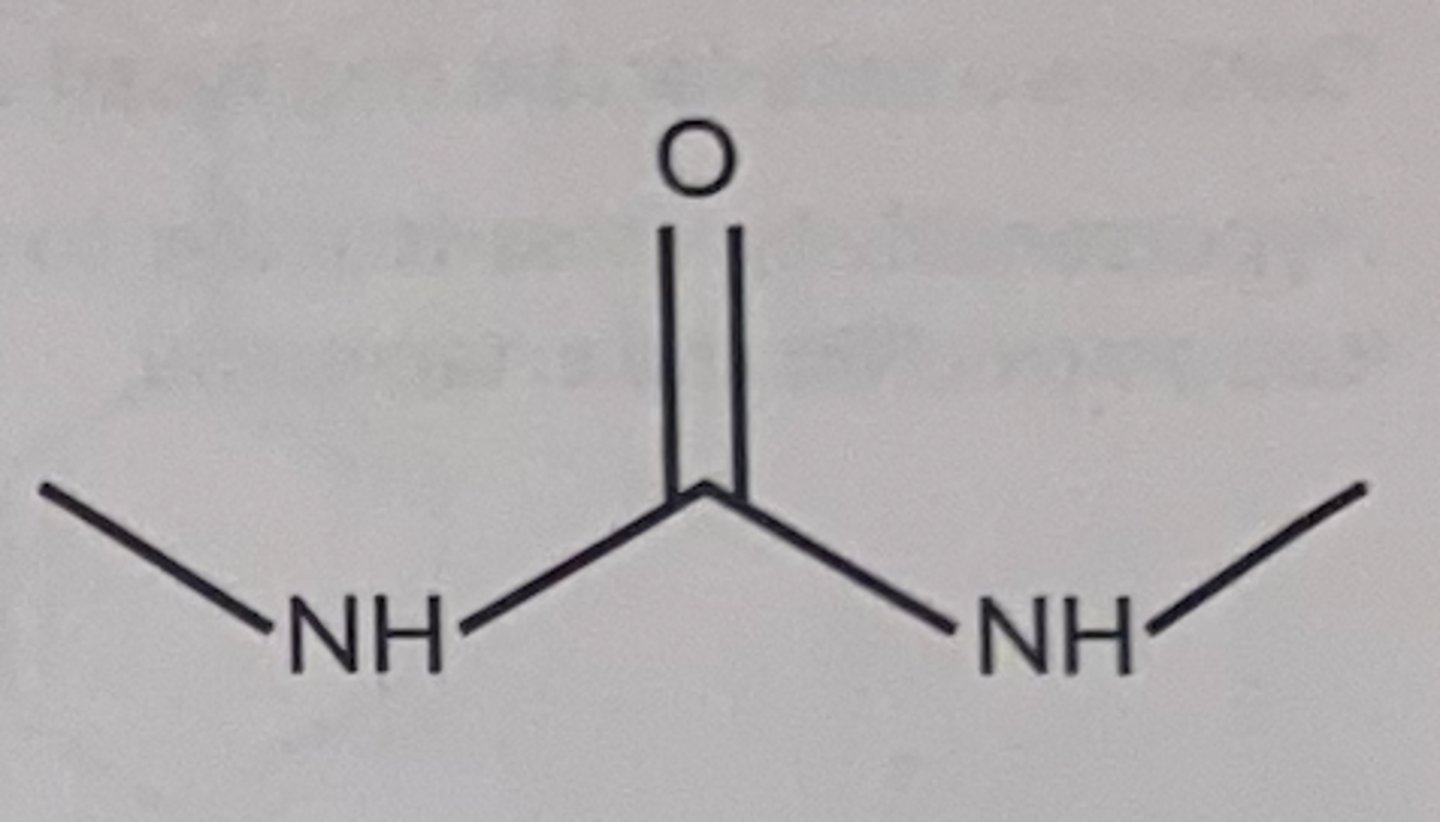
Urea functional group
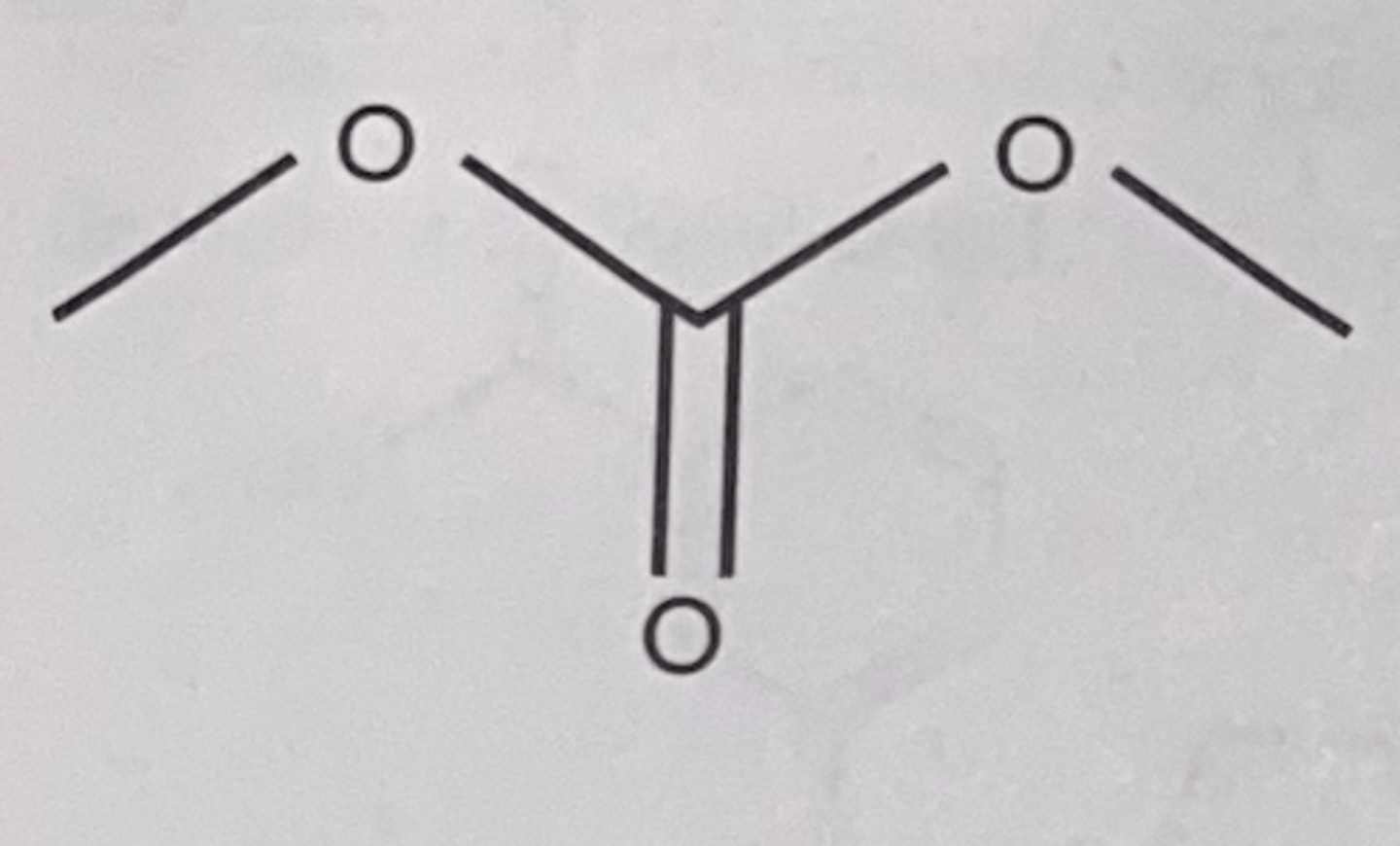
Carbonate functional group
Carbamate functional group
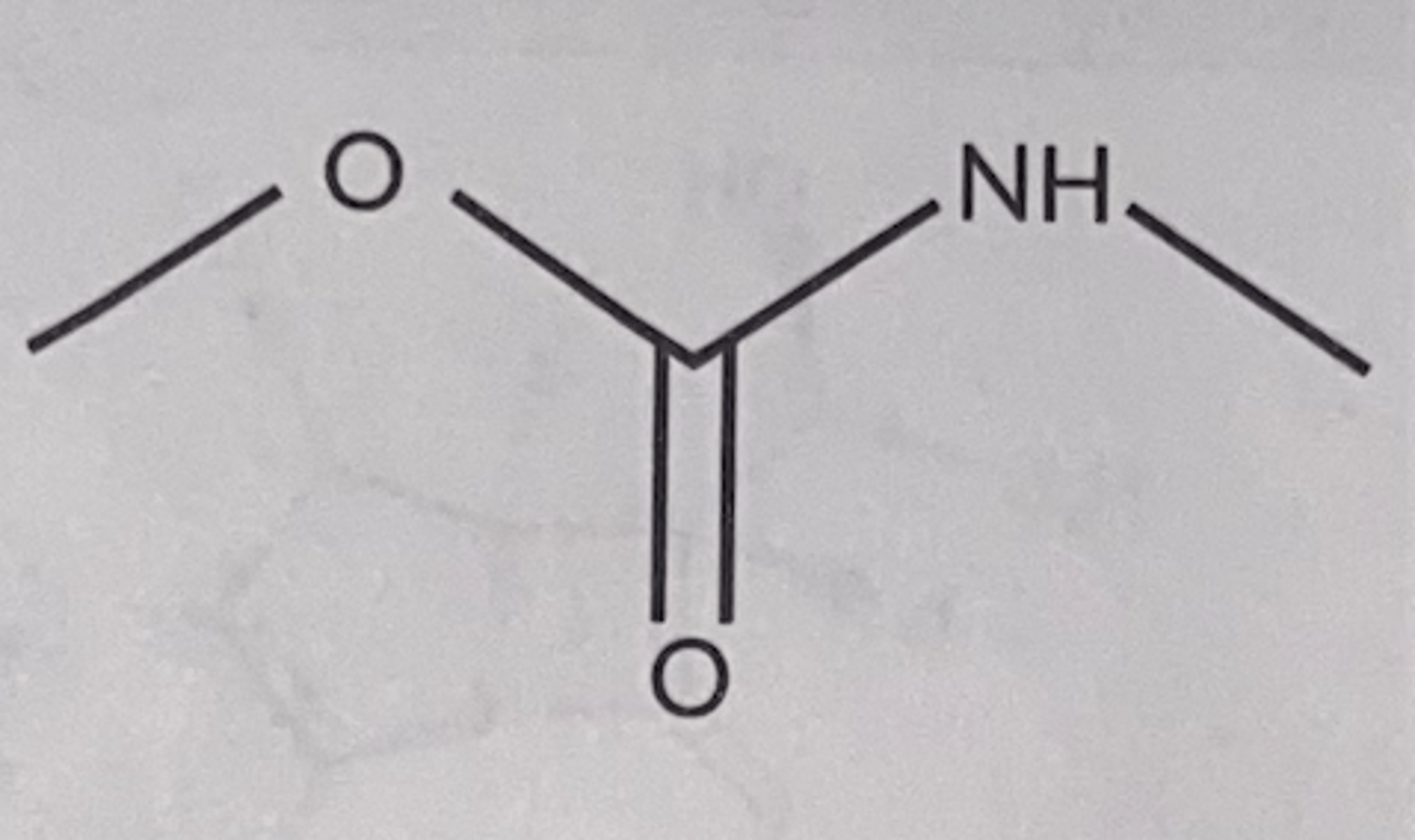
Ether functional group
Thioether functional group
What are the acidic functional groups?
Carboxyl
Phenol
Imide
Sulfonamide
Carboxyl functional group
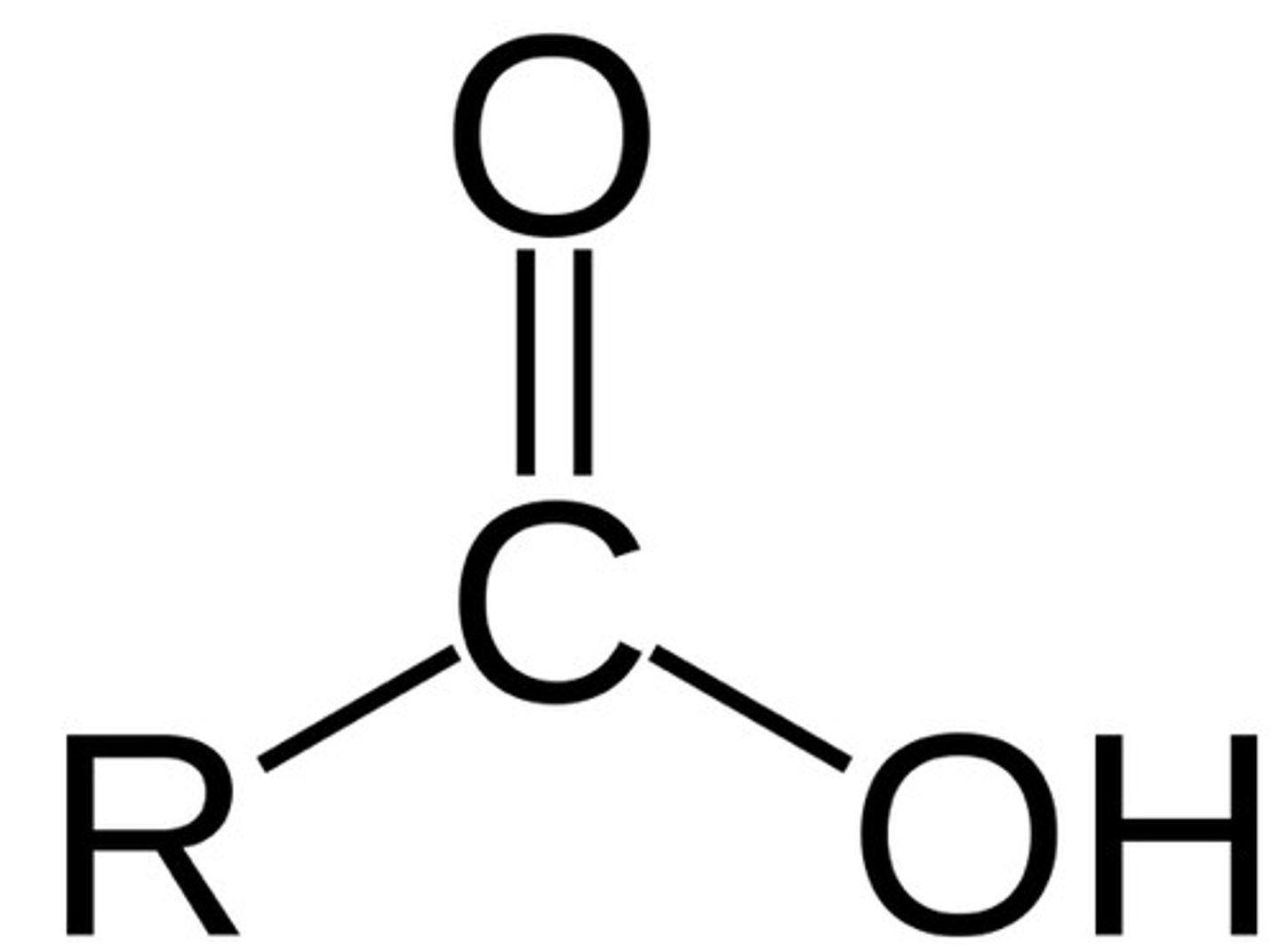
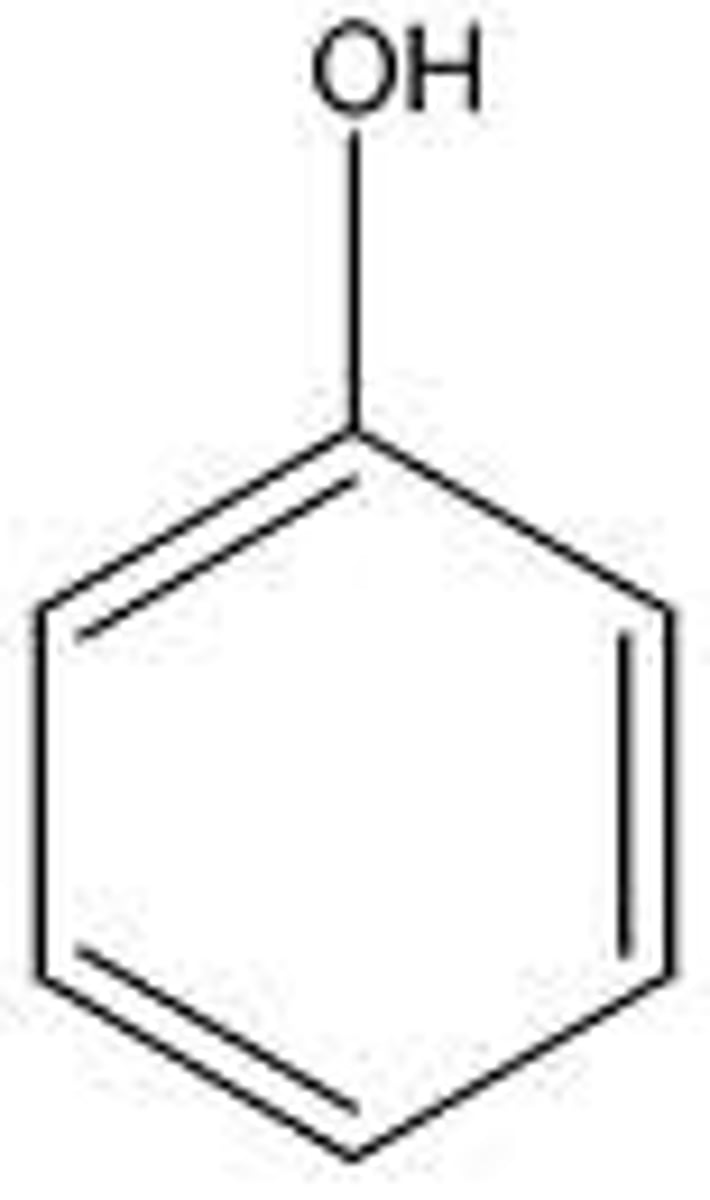
Phenol functional group
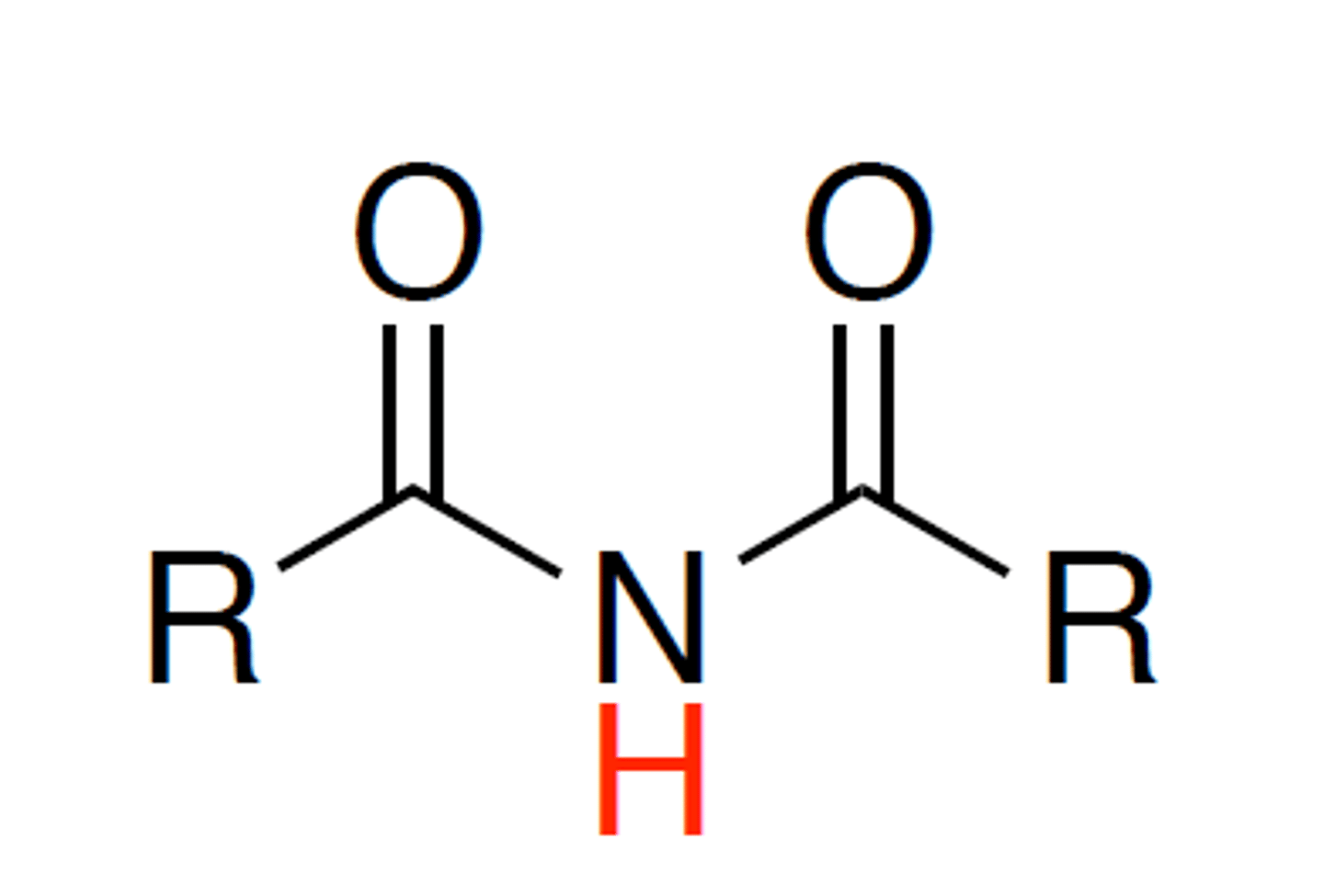
Imide functional group
Sulfonamide functional group
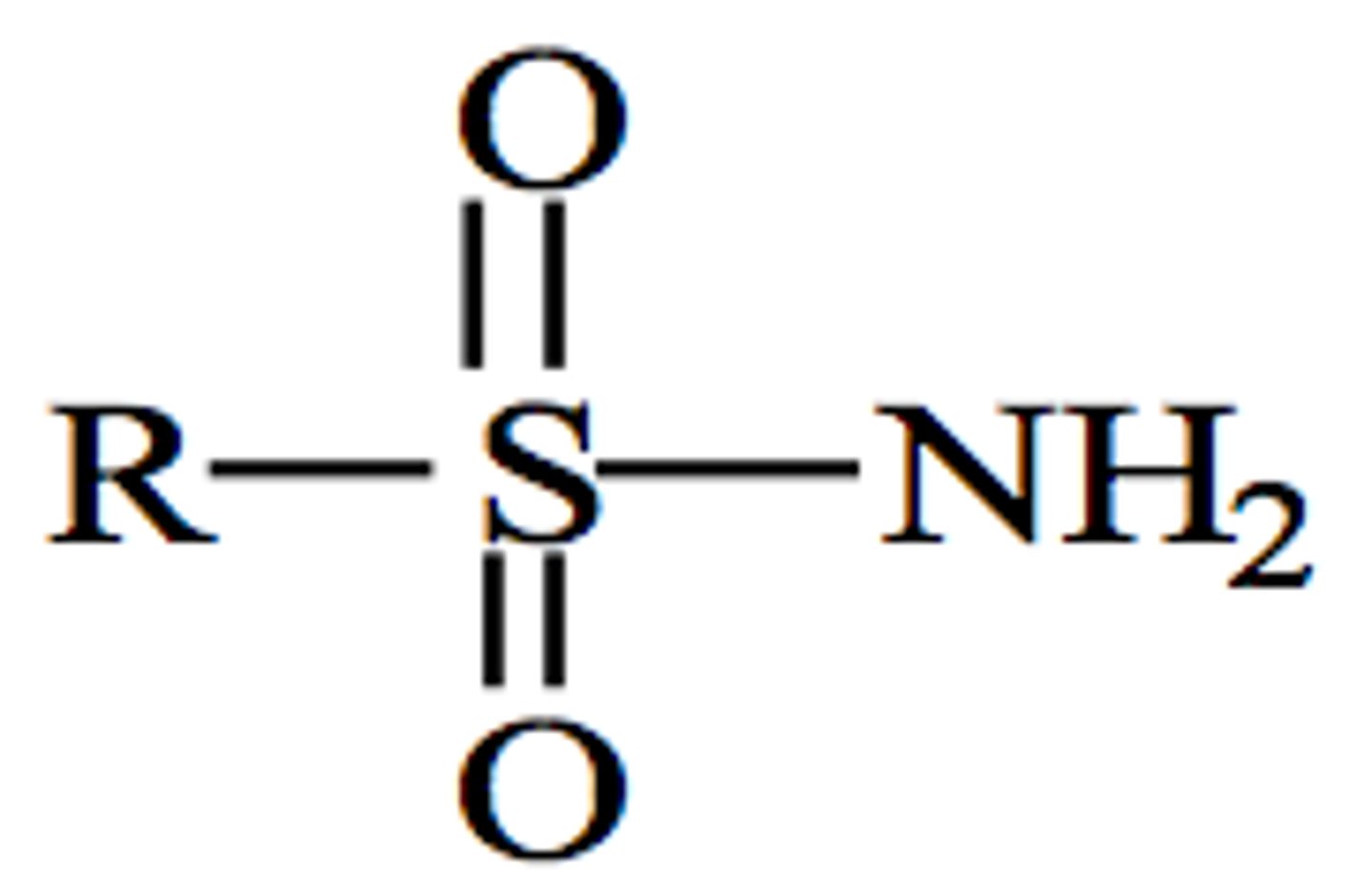
What are the basic functional groups?
Amine (primary and tertiary)
Imine
Amidine
Primary Amine functional group
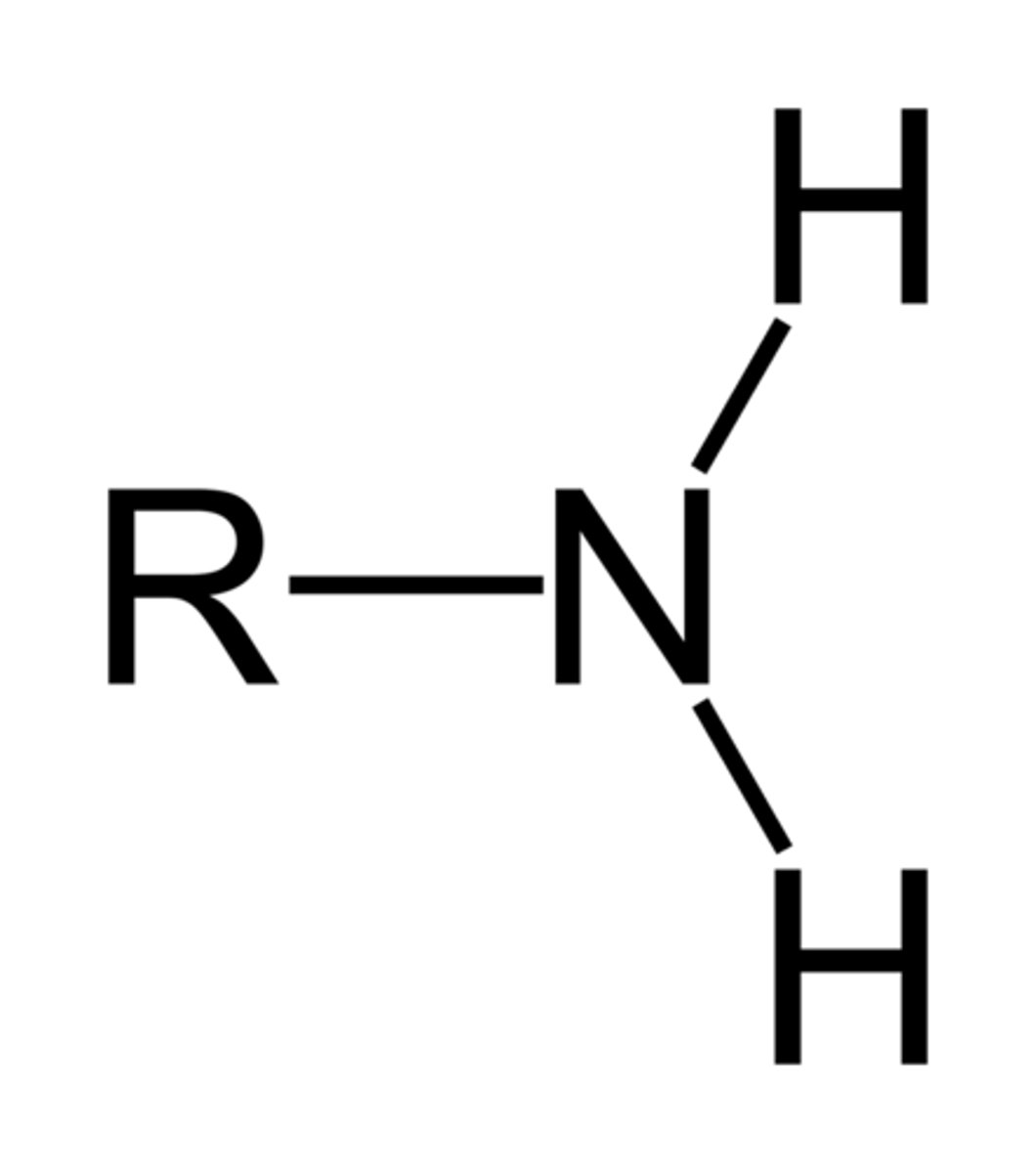
Tertiary amine functional group
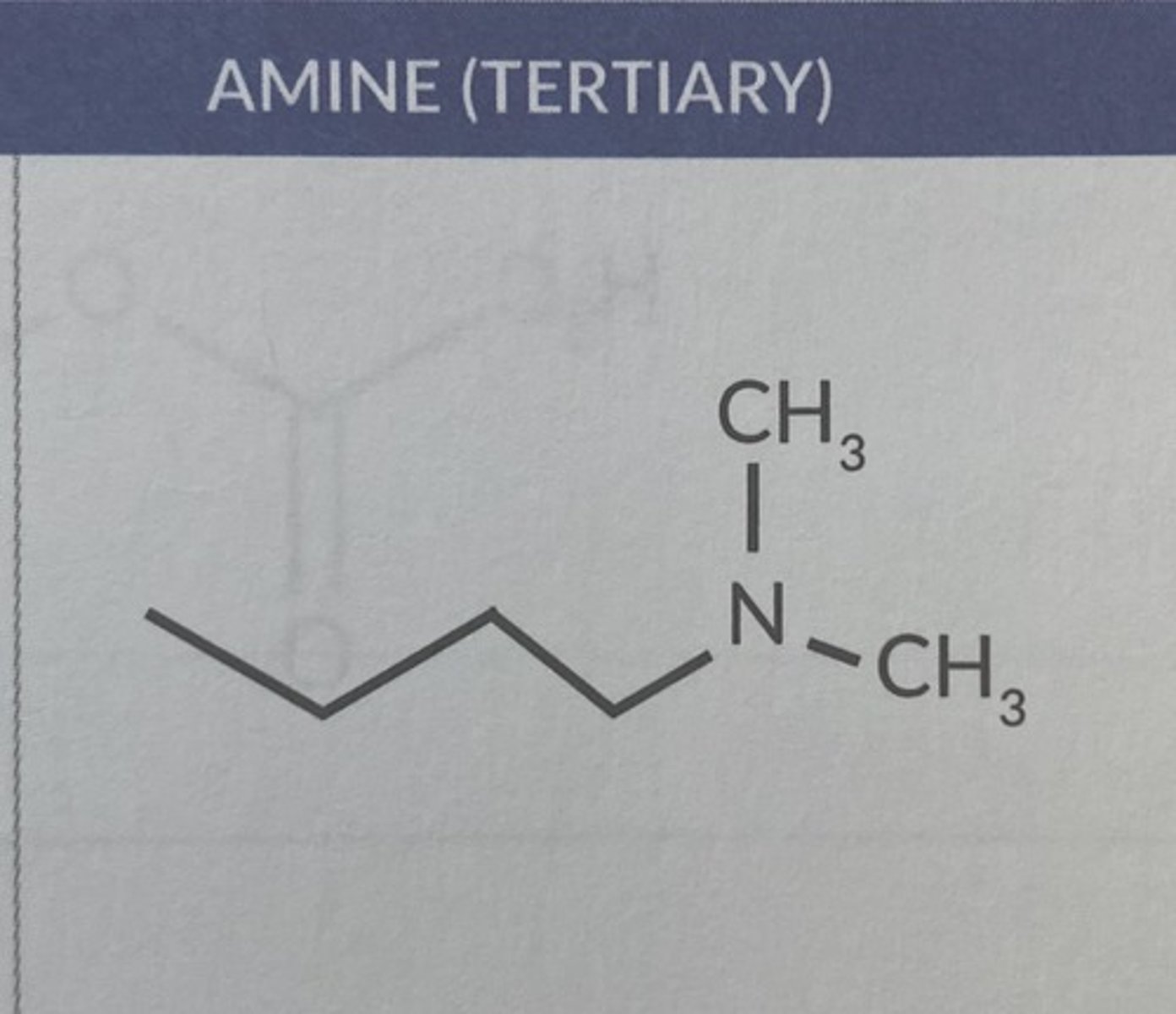
Imine functional group
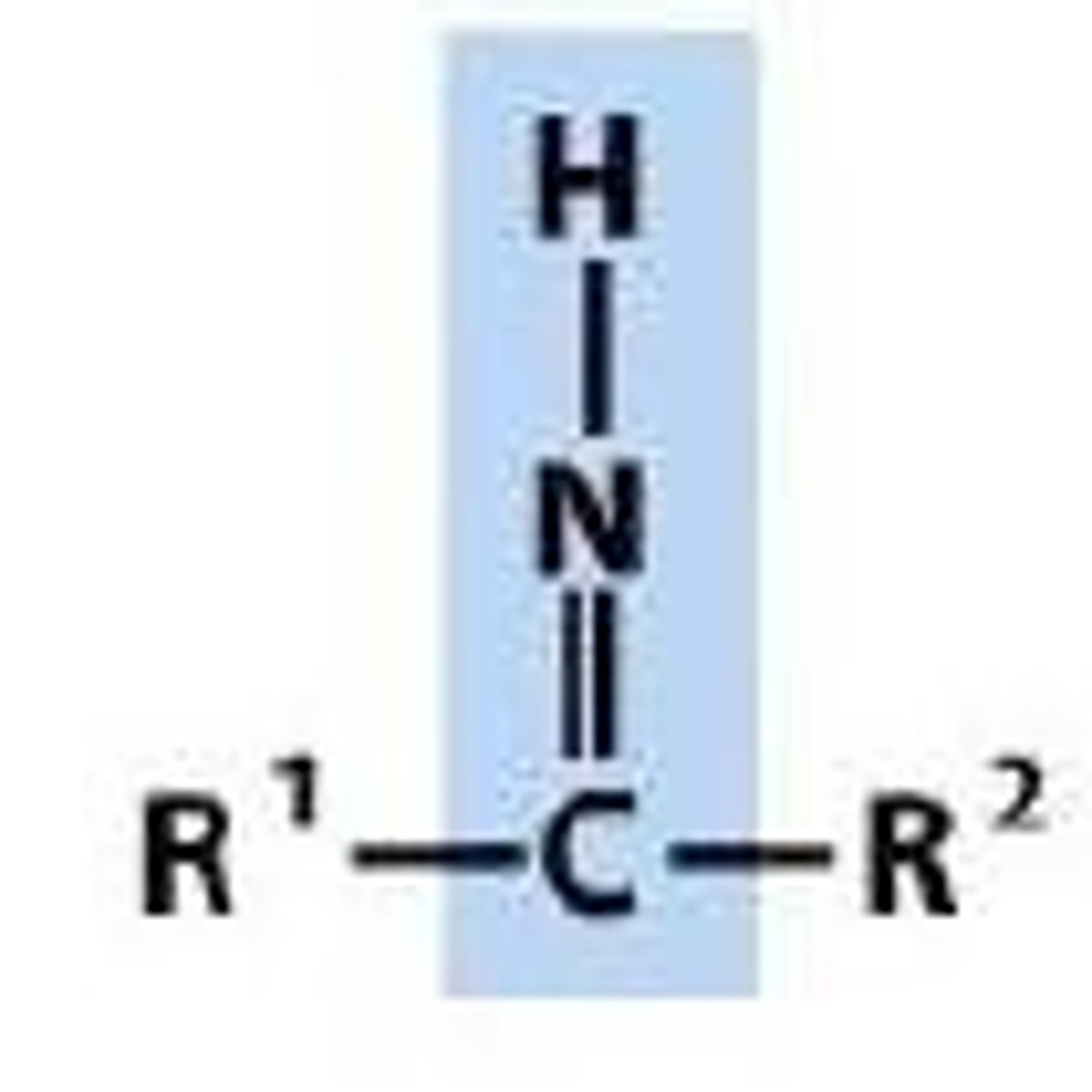
Amidine functional group
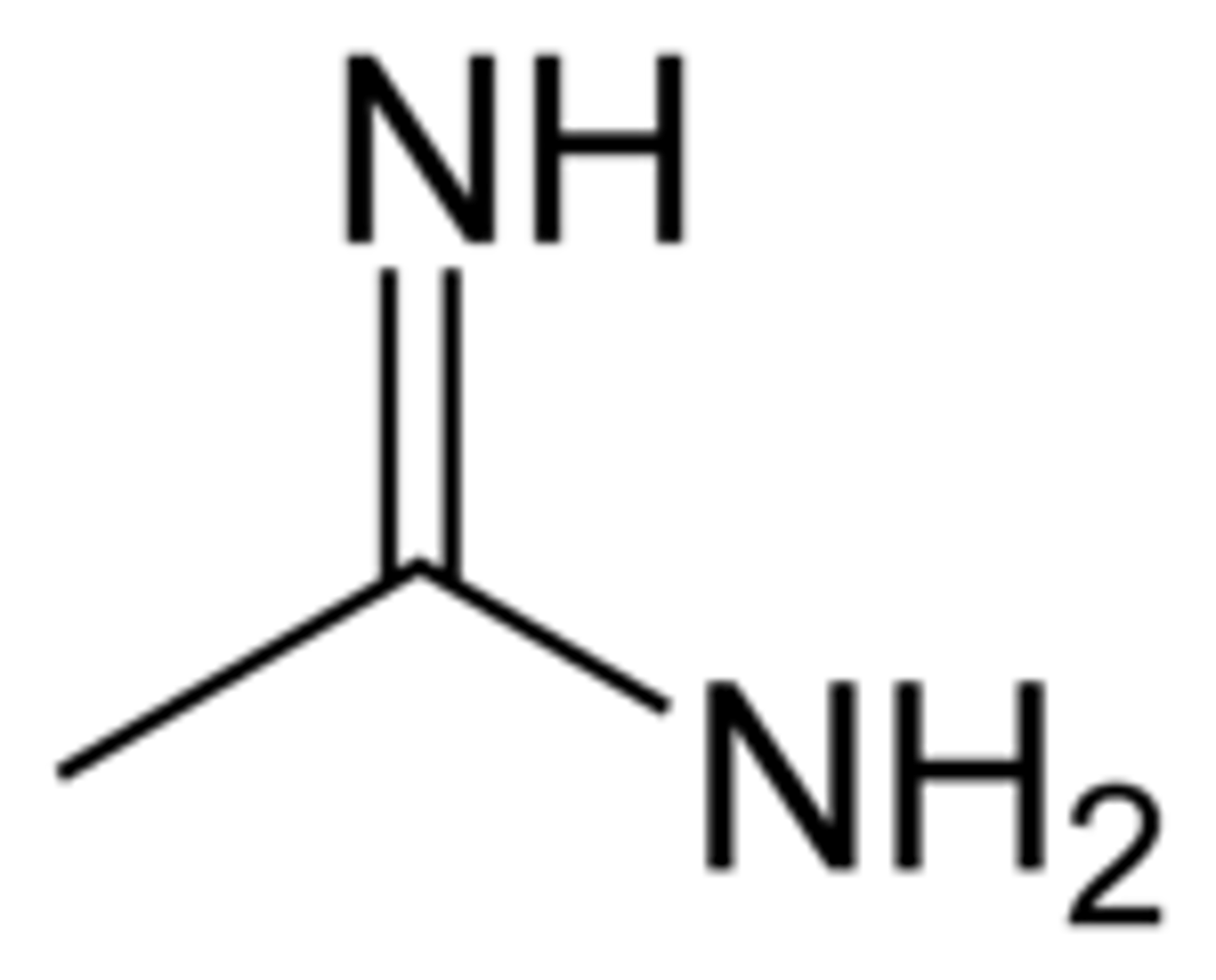
Beta-lactam Ring
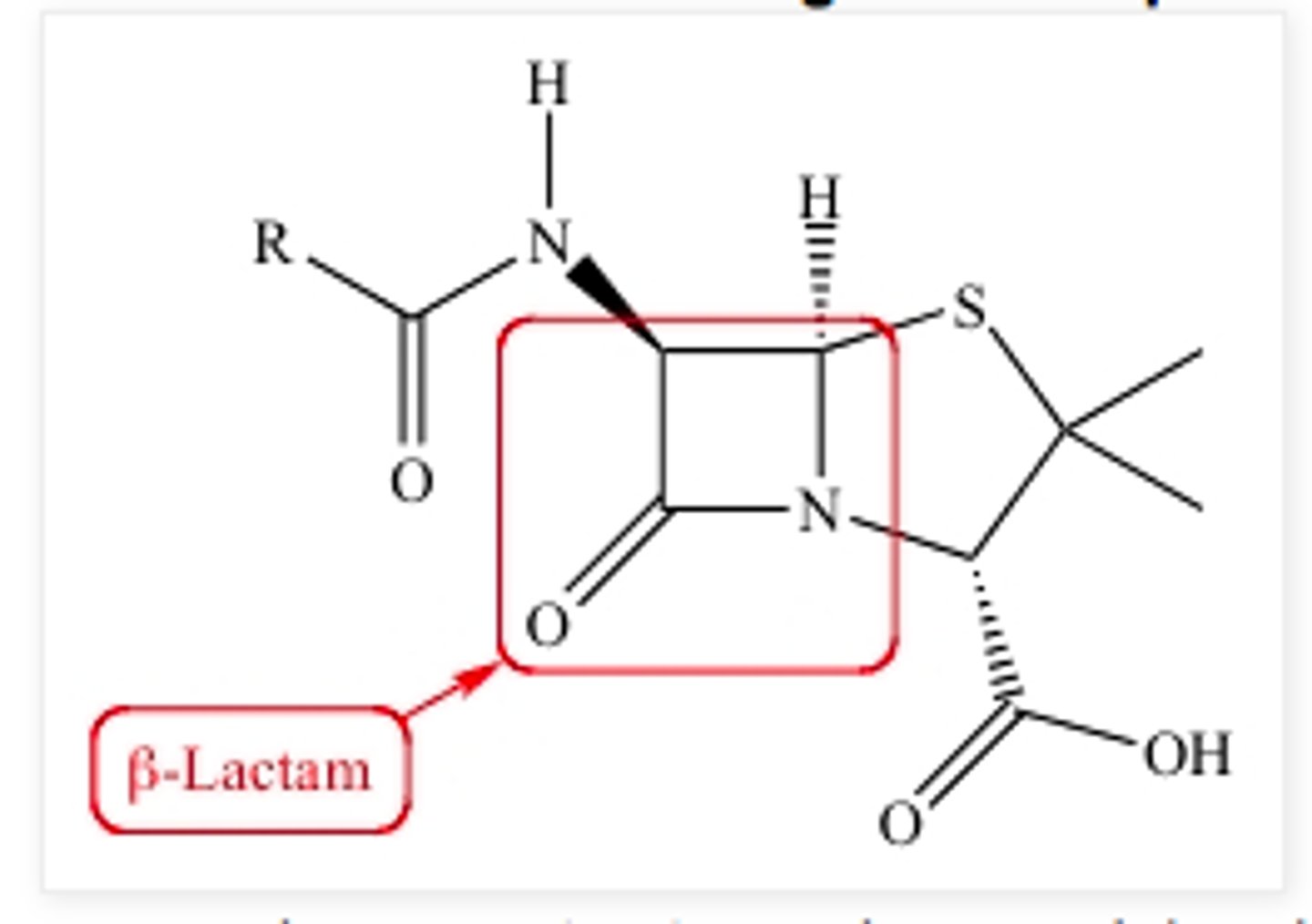
Define stability of a drug
the extent to which a product retains, within specified limits, and throughout its period of storage and use (i.e. the shelf-life), the same properties and characteristics it possessed at the time it was made
TL:DR the extent to which a drug retains is properties and characteristics compared to when it was made
What factors indicate compromised drug stability?
Changes in texture, color, smell, or development of precipitates
In terms of functional groups, what common causes may lead to drug degradation?
Reactions involving functional groups can lead to degradation and make a drug ineffective, unpalatable, and/or toxic
What are the 3 types of chemical reactions that cause most drug to become unstable or degrade?
1) Oxidation-reduction
2) Hydrolysis
3) Photolysis
What is oxidation?
loss of electrons
What is reduction?
gain of electrons
What is meant by "re-dox reaction"?
Oxidation and reduction reactions occur together, when one compound is oxidized the other is reduced
What is a common sign of oxidation for some drugs?
Color change
What color does Epi become when oxidized?
Amber-colored (yellow/orangish)
What is another common color drugs turn when oxidized?
pink/reddish
What functional group is highly oxidizable? What are drug examples?
Hydroxyl group directly bonded to an aromatic ring
Examples: Catecholamines
What does oxidation produce?
Free radicals
What catalyzes oxidation?
Heat
Light
Metal ions
What are methods to prevent oxidation of drugs?
Light protection: Amber glass/plastic
Temp. Control
Antioxidants (free radical scavengers): ascorbic acid (Vit. C), tocopherols (Vit. E)
Chelating Agents: chelate metal ions. Start with "ED-", EDTA
pH control: use of buffers
Define hydrolysis
Occurs when water causes cleavage of a bond in a molecule
What functional groups are most susceptible to hydrolysis? What component of these functional groups is the usual target of hydrolysis?
Ester, amides, and lactams (beta-lactam ring)
The carbonyl (C=O) component is most likely target of hydrolysis
What are methods to prevent/reduce hydrolysis?
Protect drug from moisture:
Desiccants (absorbents): absorb moisture that enter the container
Lyophilized powders (freeze-dried)
Manufactured as a less hygroscopic salt
Storage: avoid storing meds in bathrooms or humid places and close container lid tightly
Oxidation prevention can also reduce hydrolysis
What is photolysis?
Breakage of covalent bonds and drug degradation due to UV light exposure
Is photosensitivity common for drugs?
Yes