CNM - GU System (DUGAN)
1/192
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
193 Terms
reddish-brown semilunar shaped positioned on either side of the vertebral column from T12-L3 vertebrae
Describe kidneys
11cm in length, 3cm thick, 6cm wide
What is the average length, thick, and width of kidneys?
left
Which kidney is larger?
right
Which kidney is lower?
metabolic waste is drained from them by ureters which empty into the bladded and are excreted from the body
What is the main function of the kidneys?
24-30cm in length and 0.9cm diameter
Ureters are tubular structures that average _____ length and ____ diameter
retroperitoneal
The kidneys are considered _____ organs
between the muscles of the back and peritoneal cavity; allows kidneys to be exposed surgically without opening the peritoneal cavity
Where are the kidneys located? Why is it good?
1. filter blood
2. excrete waste
3. control fluid volume and ion composition
4. regulate blood pressure
4. influence RBC production
5. regulate pH of blood and body fluids
List the 5 functions of the kidneys
1. nephrons
2. cortex
3. medulla
4. hilum
What are the 4 main components of the kidneys?
microscopic functional unit of the kidney (more than 1 million nephrons in each kidney)
Nephron
1. filtration
2. reabsorption
3. secretion functions
What is the nephron responsible for?
1. glomerulus
2. renal tubule
What are the two parts the nephron consists of?
nephron
This is an image of a
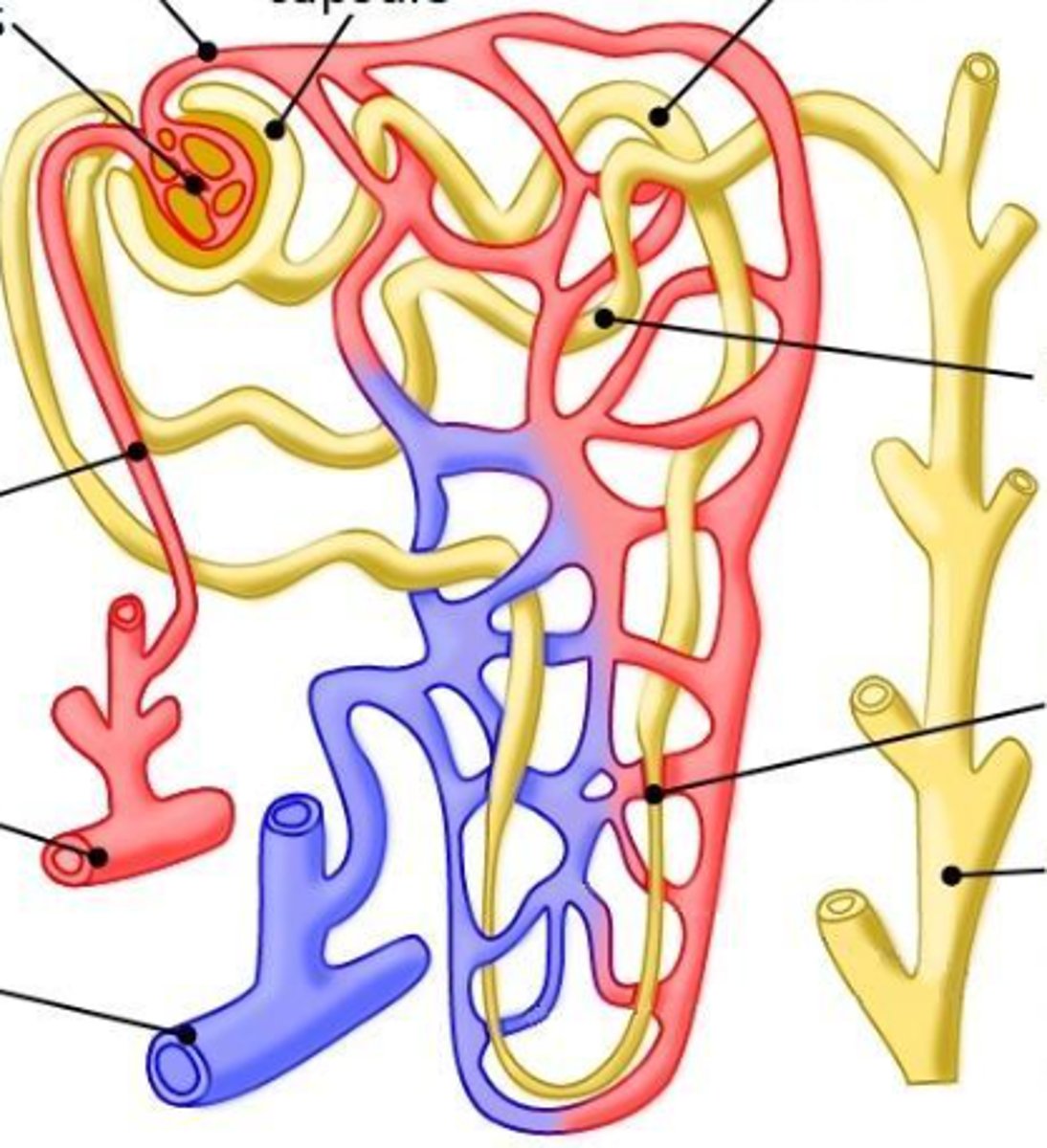
afferent arteriole
What is the arrow pointing at?
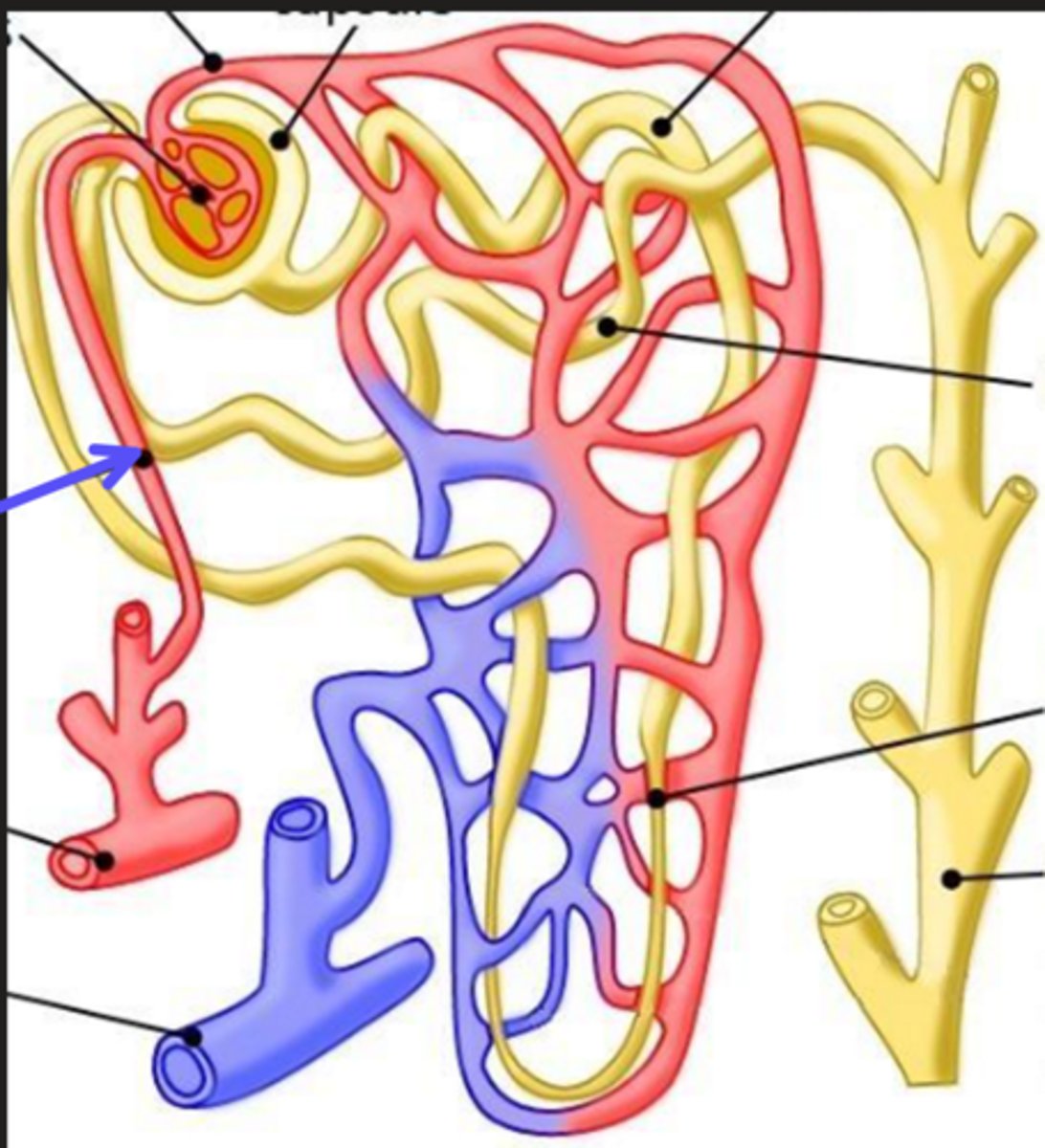
arcuate artery
What is the arrow pointing at?
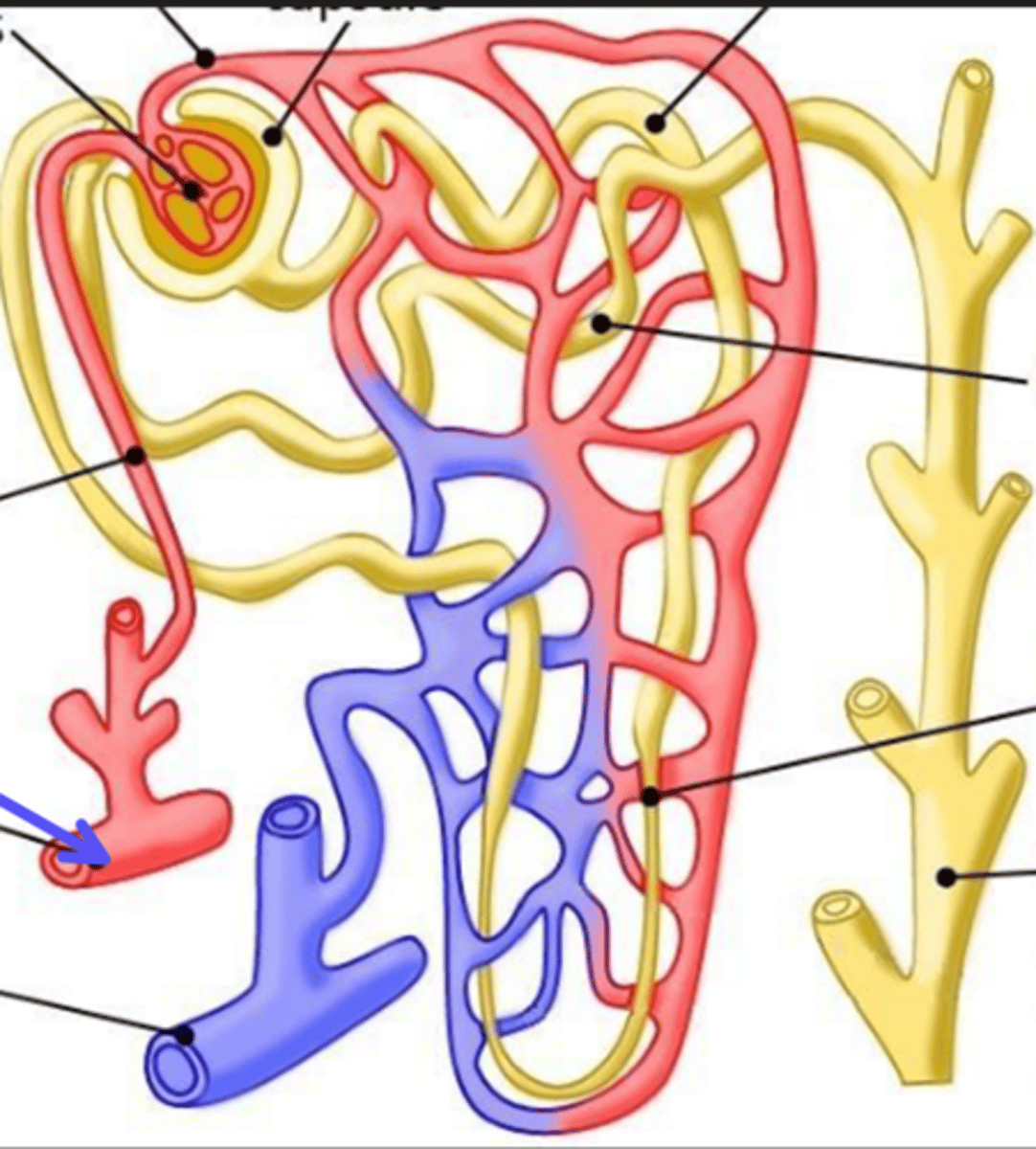
arcuate vein
What is the arrow pointing at?
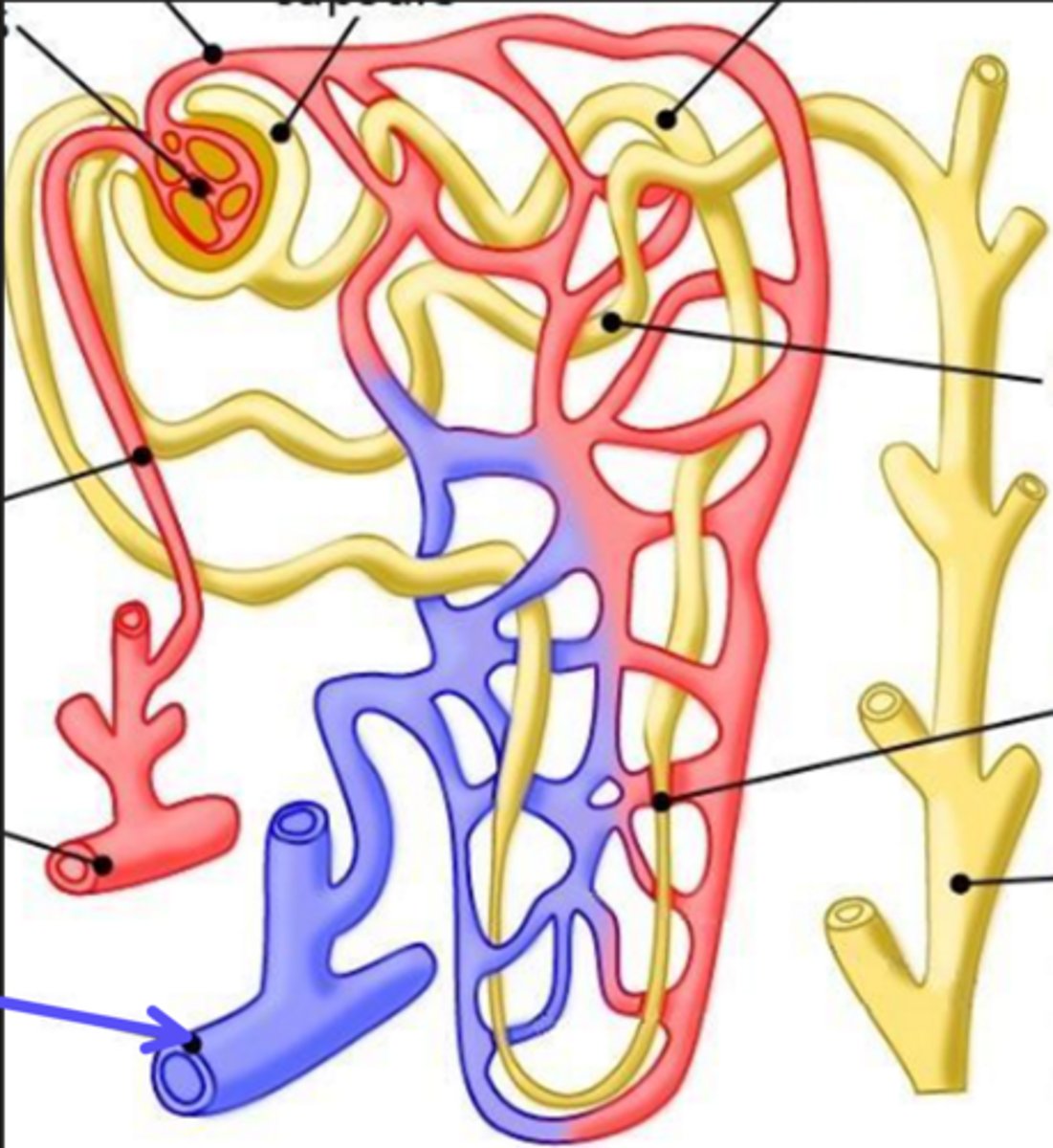
ascending limb
What is the arrow pointing at?
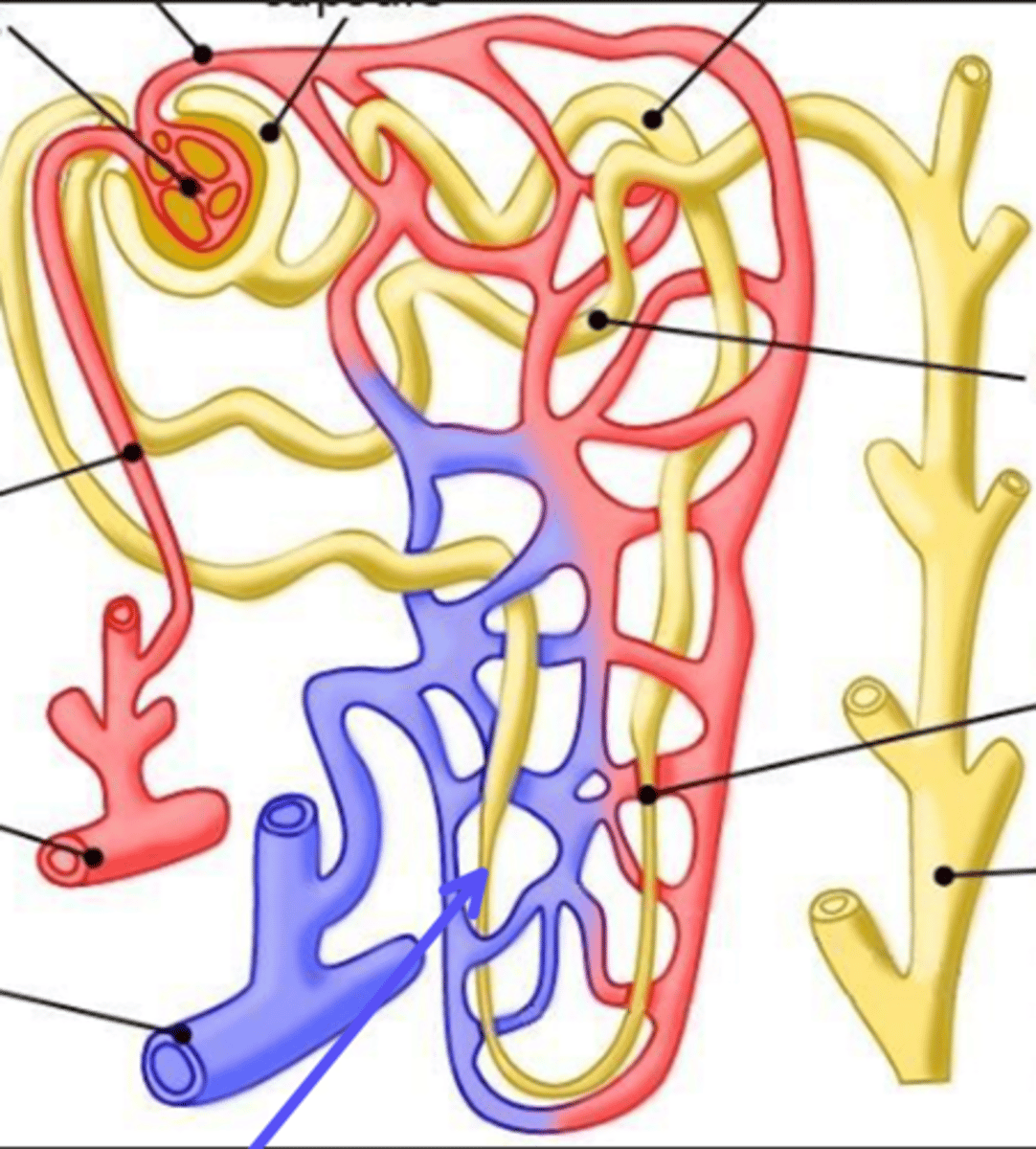
collecting duct
What is the arrow pointing at?
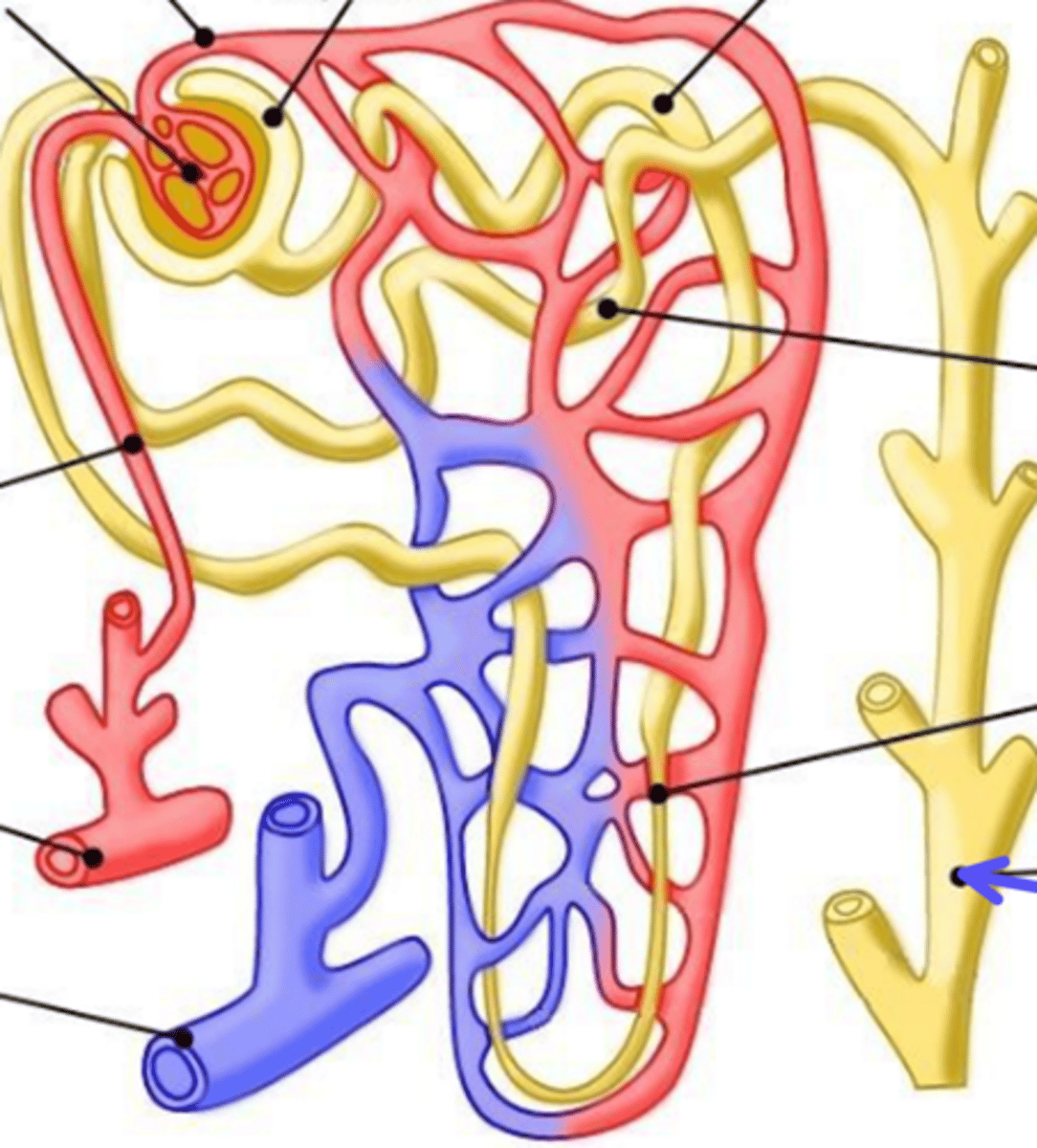
bowmans capsule
What is the arrow pointing at?
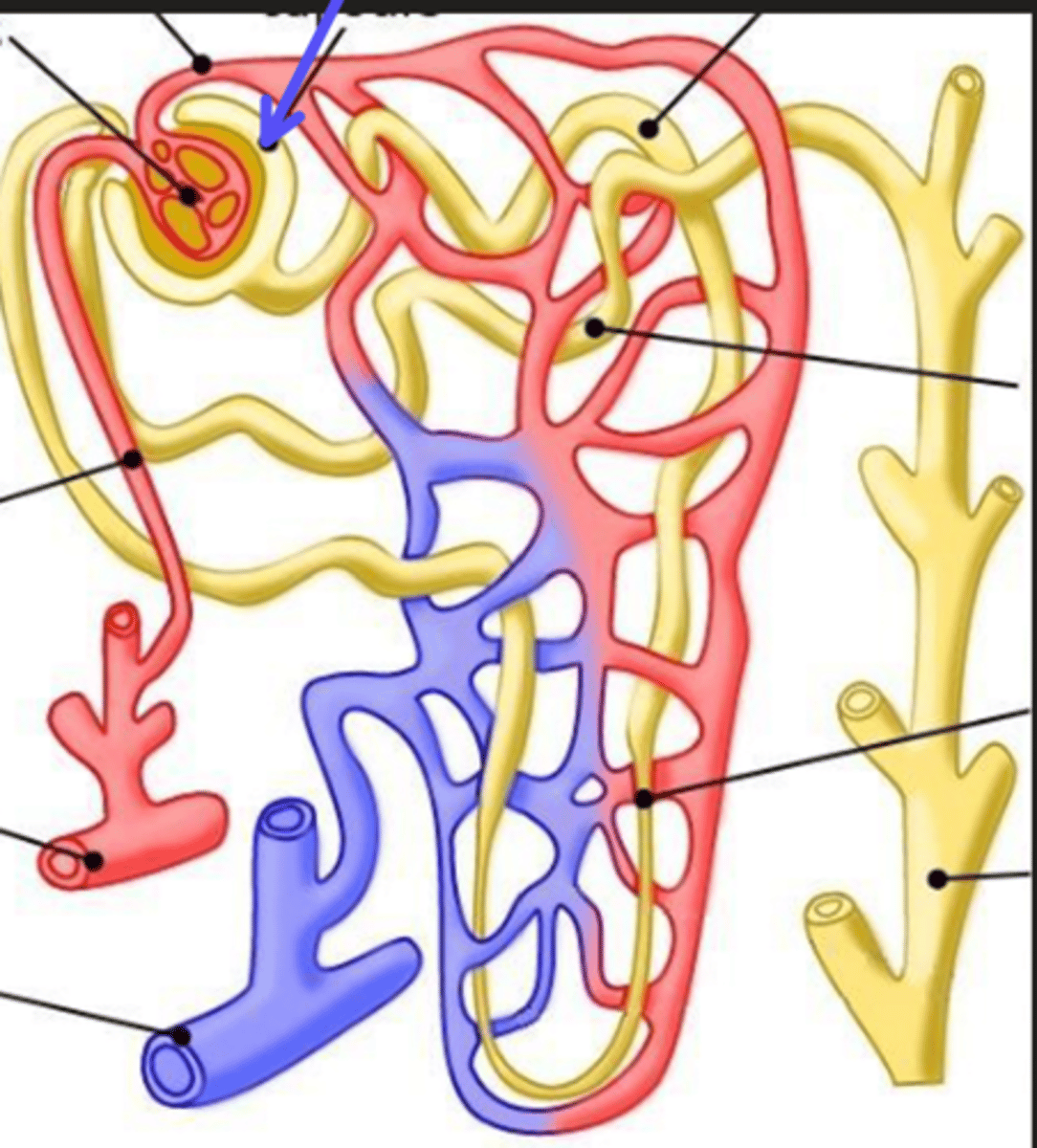
descending limb
What is the arrow pointing at?
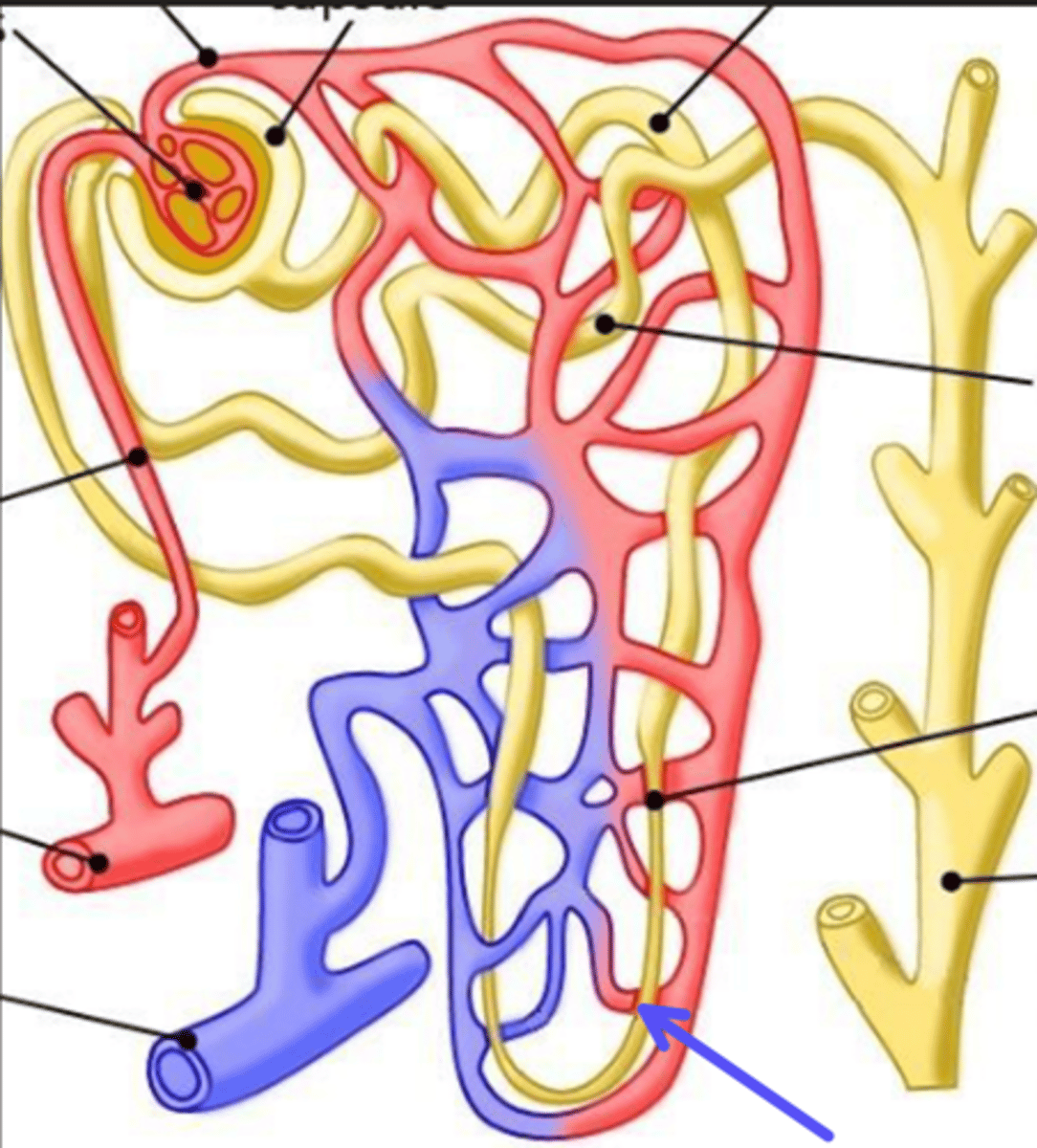
distal convoluted tubule
What is the arrow pointing at?
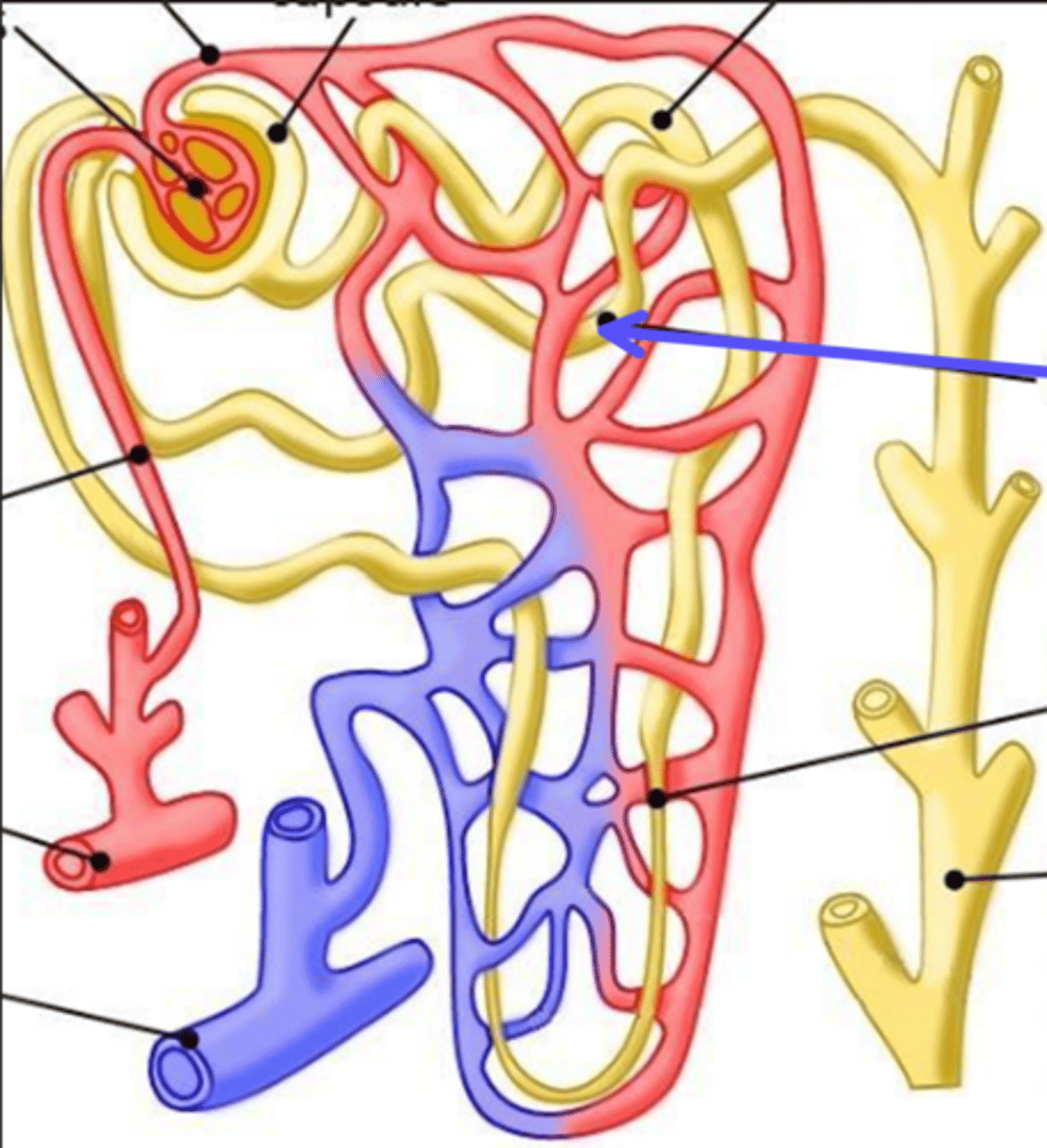
efferent arteriole
What is the arrow pointing at?
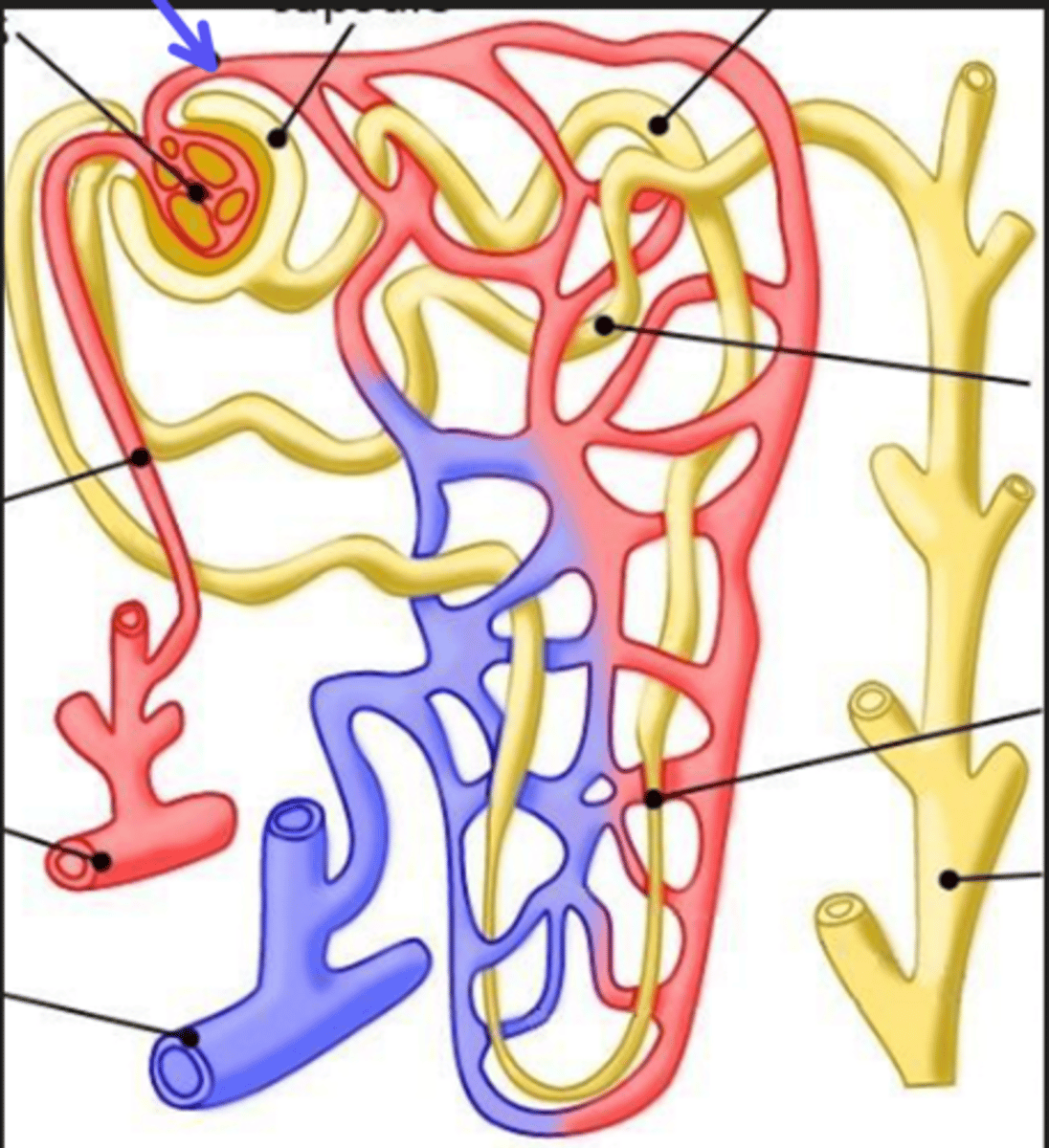
glomerulus
What is the arrow pointing at?
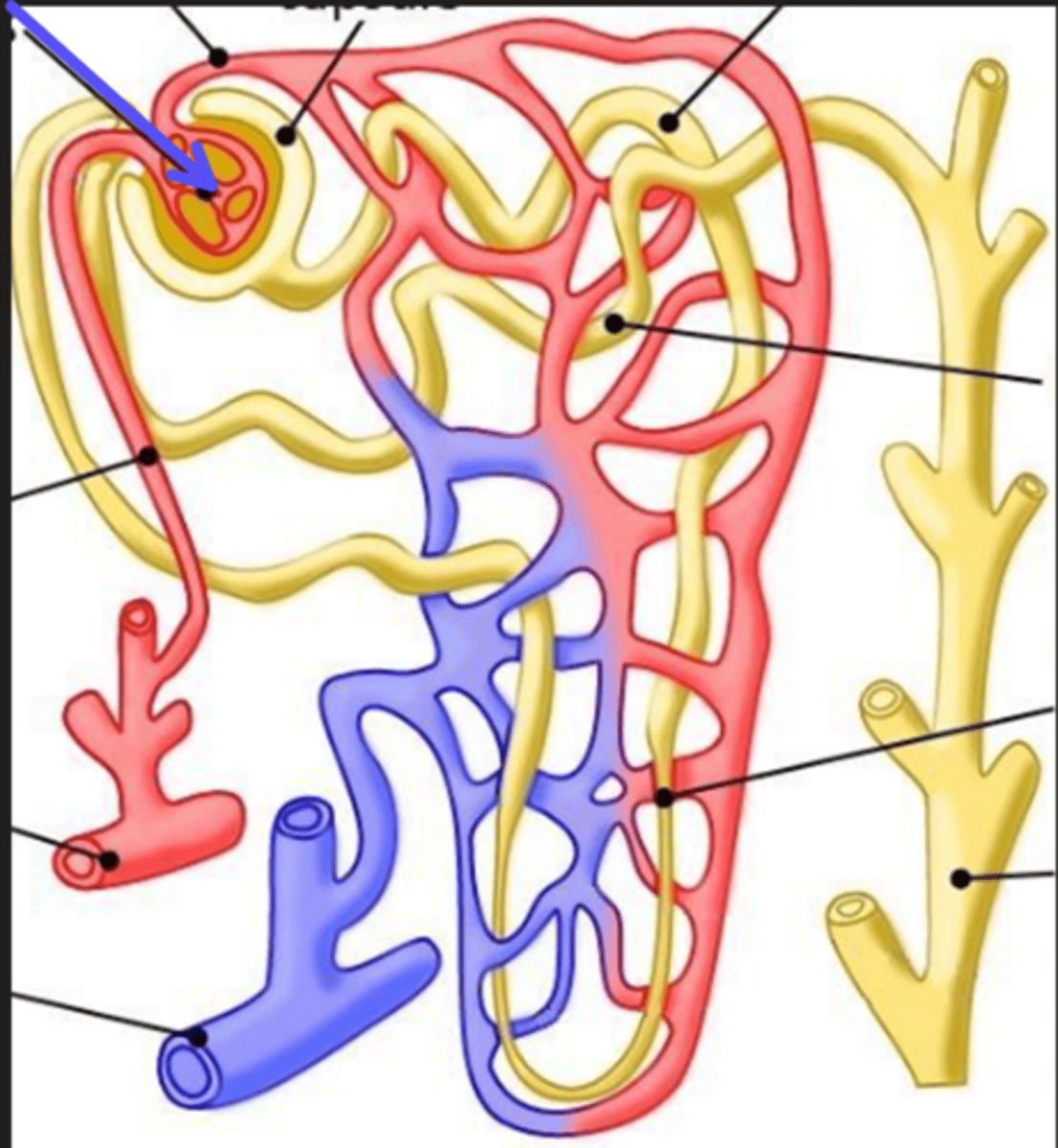
interlobar artery
What is the arrow pointing at?
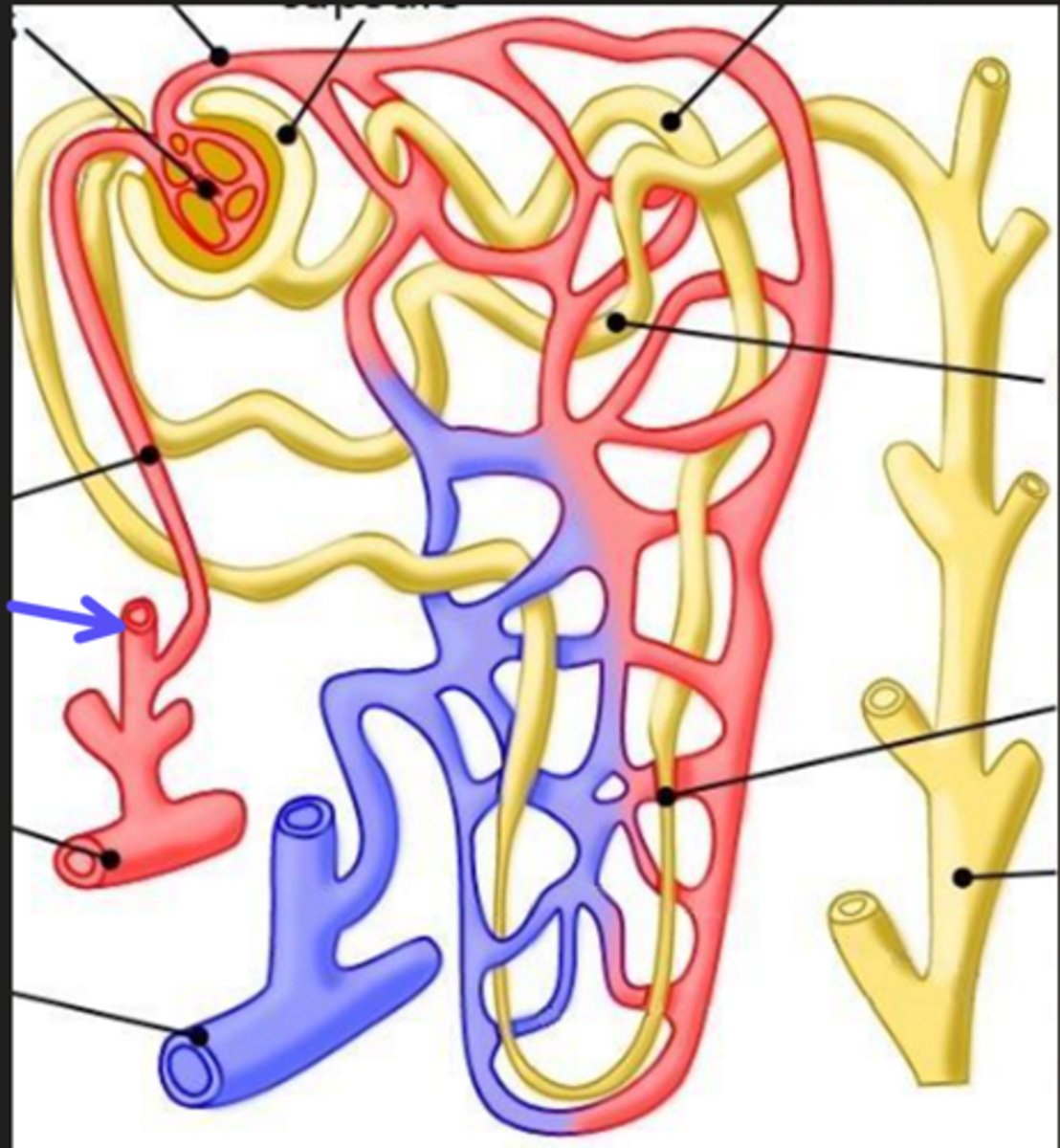
interlobar vein
What is the arrow pointing at?
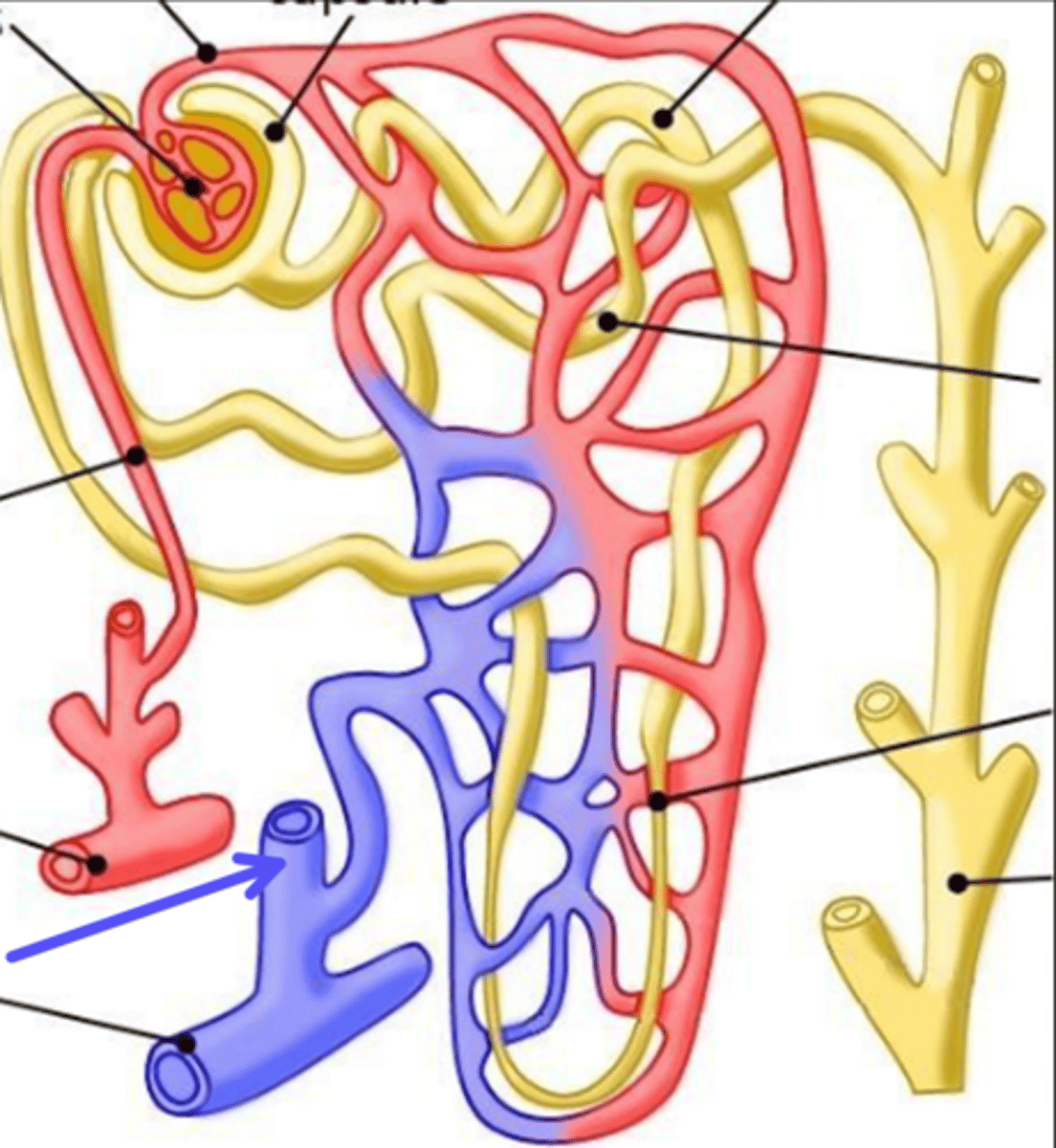
nephron loop (loop of henle)
What is the arrow pointing at?
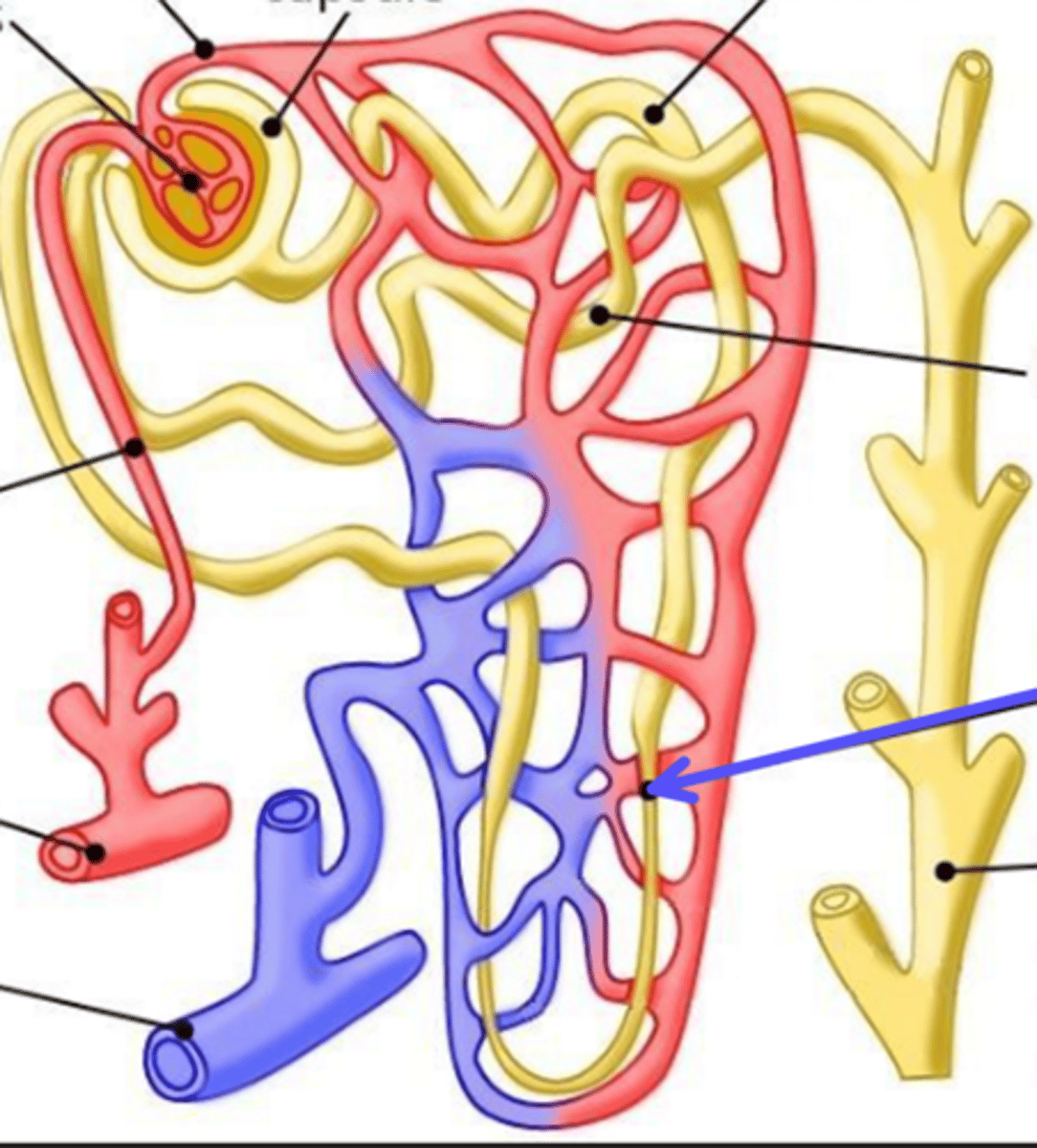
peritibular capillary
What is the arrow pointing at?
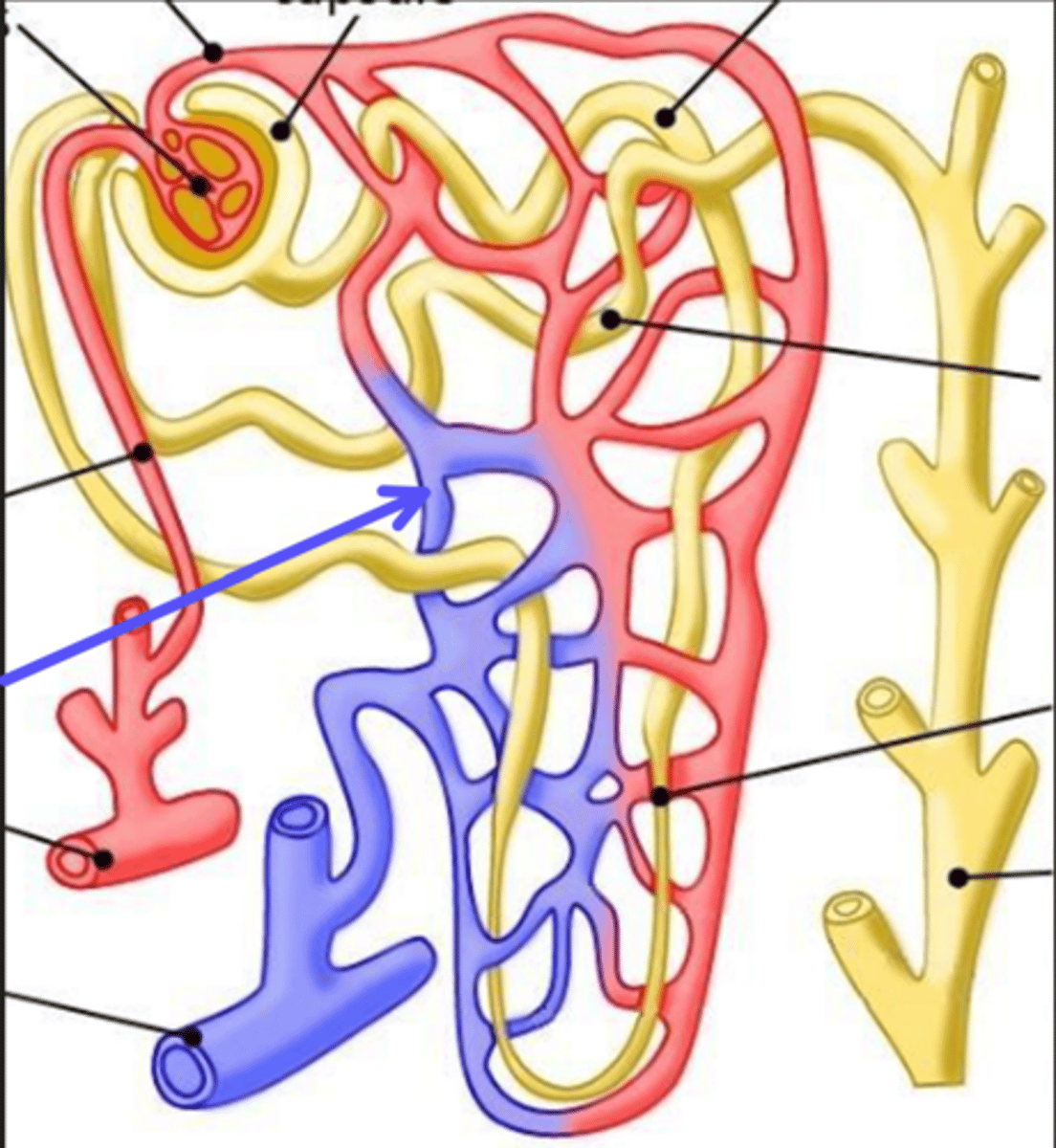
proximal convoluted tubule
What is the arrow pointing at?
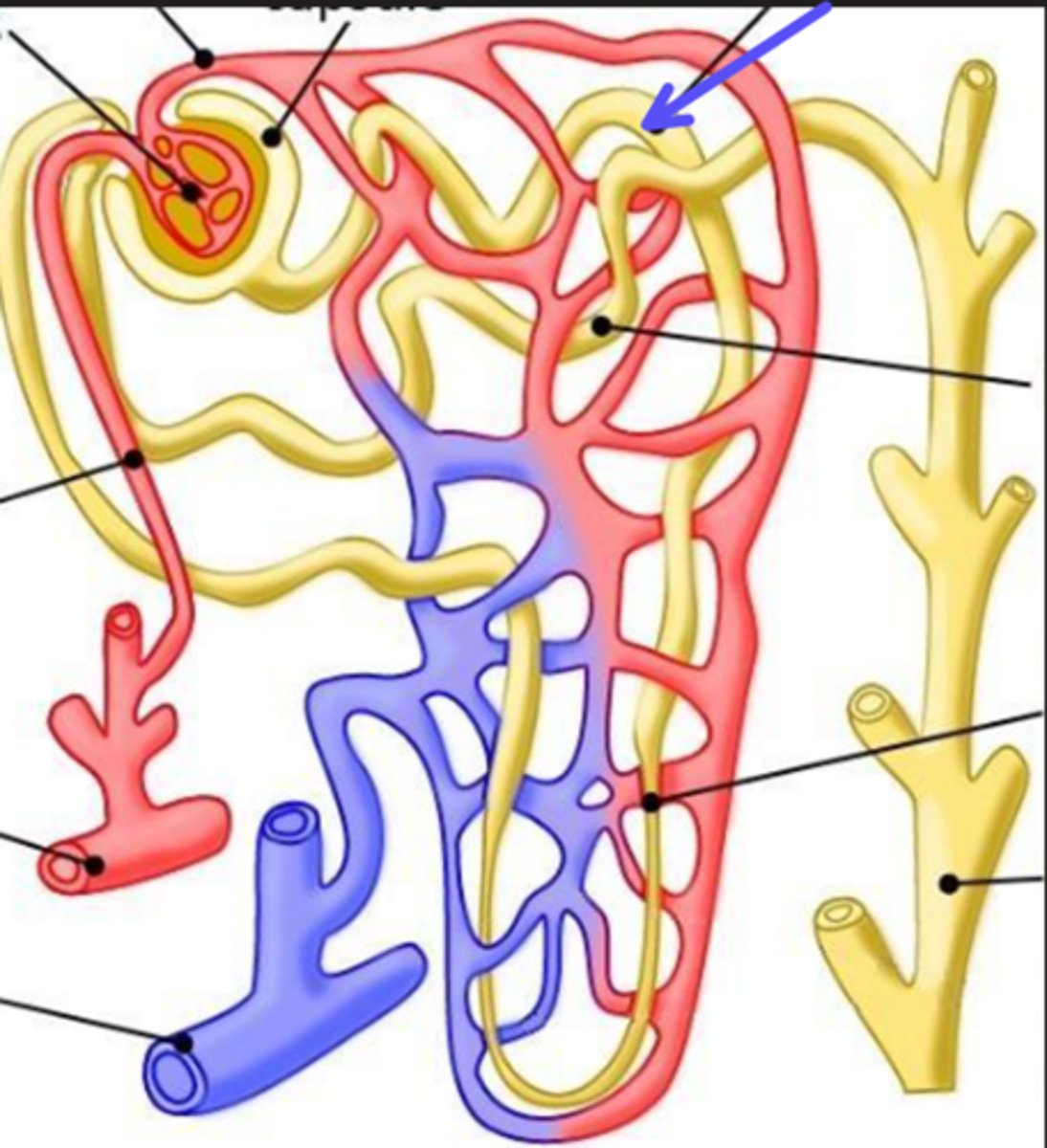
cortical and juxtamedullary
What are the two types of nephrons?
80% and have a shorter loop of henle
What percentage of all nephrons is cortical? What's it's difference?
20% and have longer loop of henle that extends further in medulla
What percentage of all nephrons are juxtamedullary? What's it's difference?
1. blood enters glomerulus through afferent arteriole
2. it's filtered in glomerulus
3. then passes into bowman's capsule
4. then drains into proximal convoluted tubule
5. it travels through nephron loop into the distal convoluted tubule
6. then exits through the collecting duct into renal calyces and pelvis forming urine
Explain the step by step passageway of blood through a nephron.
protein free plasma
What is glomerulus filtrate?
proximal convoluting tubule
The bowmans capsule is an expanded portion of what?
false, composition changes as the tubules reabsorb liquid and have secretions added
T/F The filtrate in the tubules is the same composition as it is when it's in the glomerulus.
1. nephron
2. glomerulus
3. PCT and DCT where most kidney function occurs (1-2cm thick)
What does the cortex consist of?
1. tubules
2. nephron loop
3. renal pyramids
4. renal columns
What does the medulla consist of?
major and minor calyxes, connects to hilum
What does the pelvis consist of?
entry and exist site for the structures servicing the kidney
What is the function of the hilum?
medulla
What is the arrow pointing at?
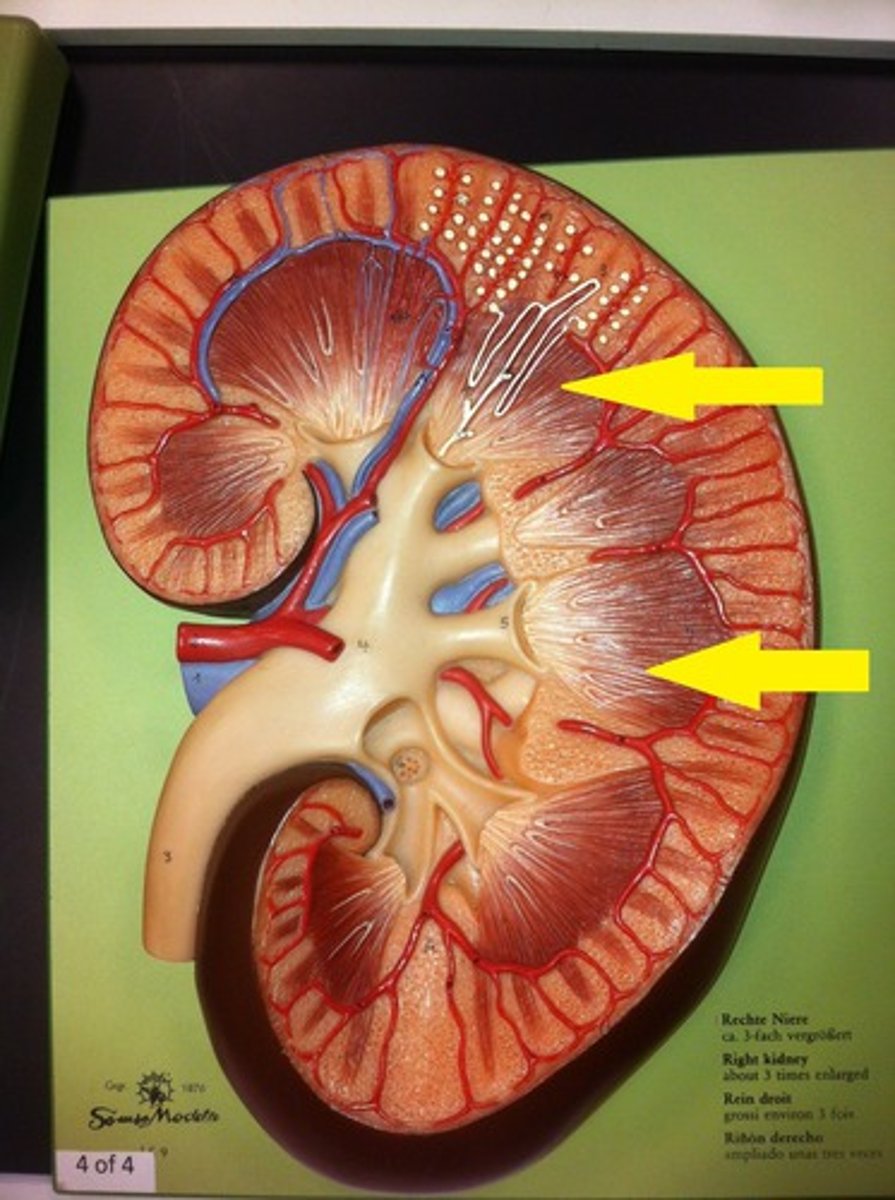
cortex
What is the arrow pointing at?
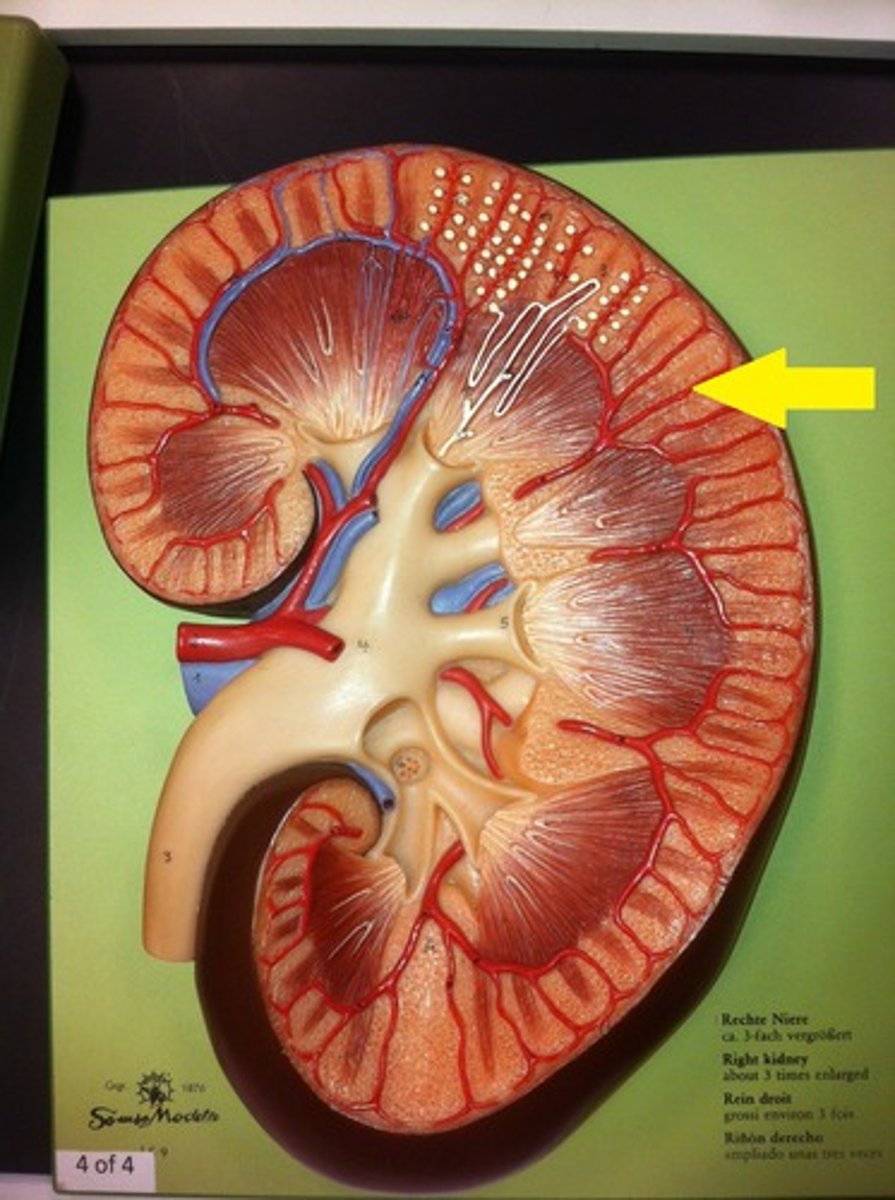
renal artery
What is the arrow pointing at?
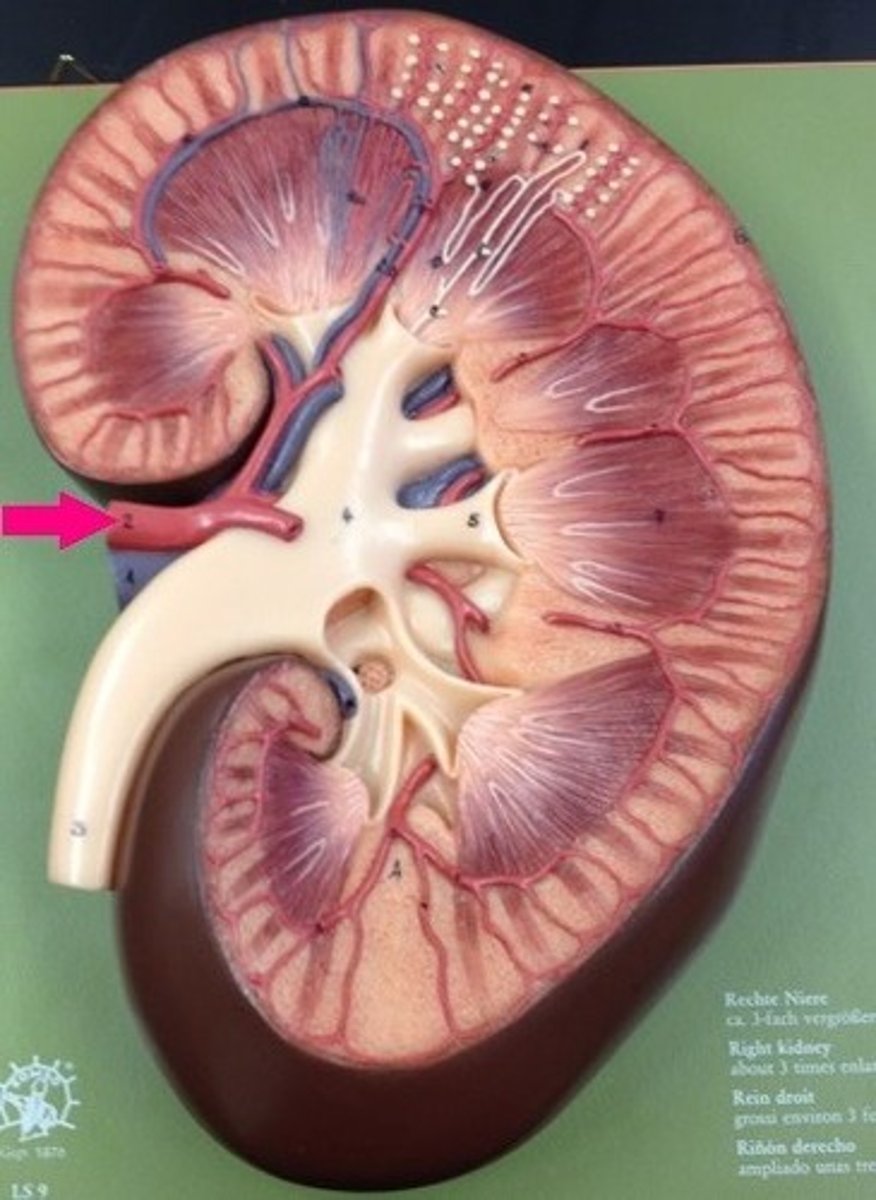
renal vein
What is the arrow pointing at?
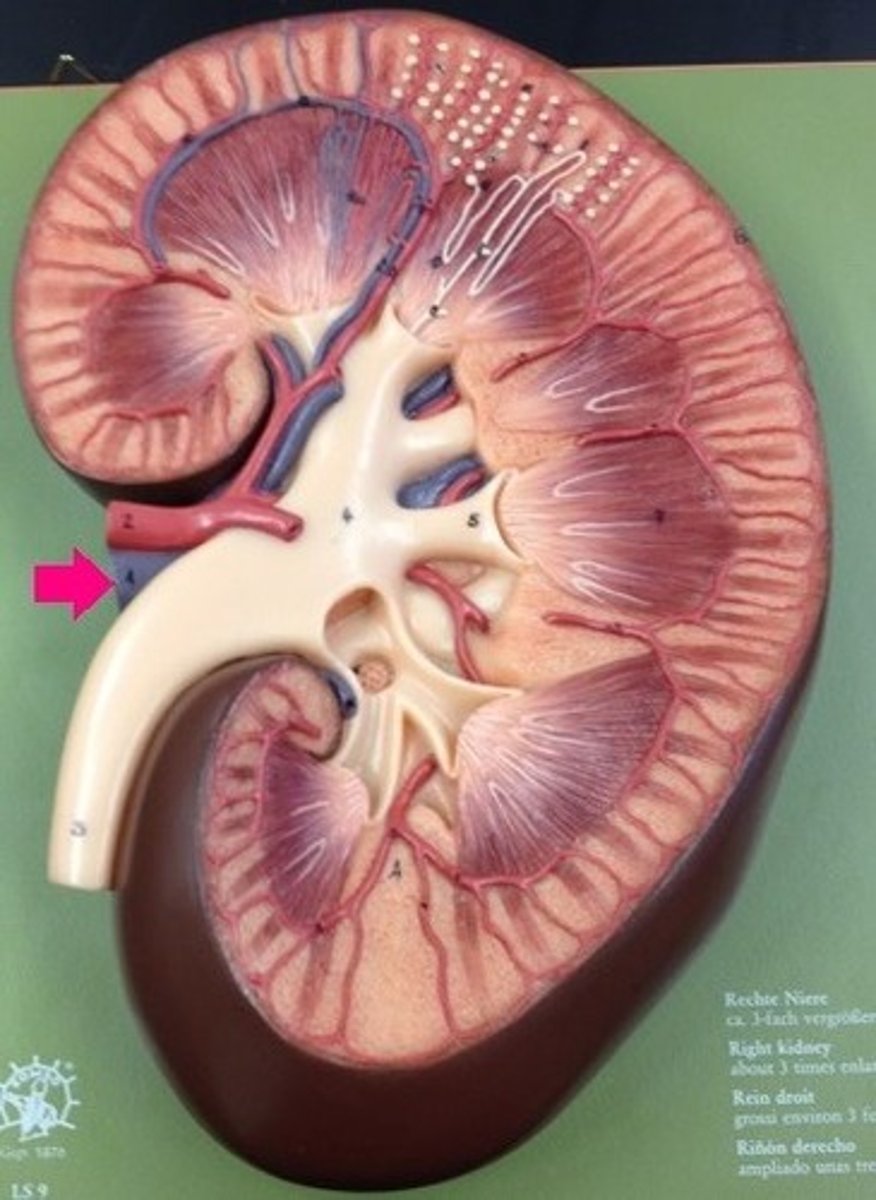
renal pelvis
What is the arrow pointing at?
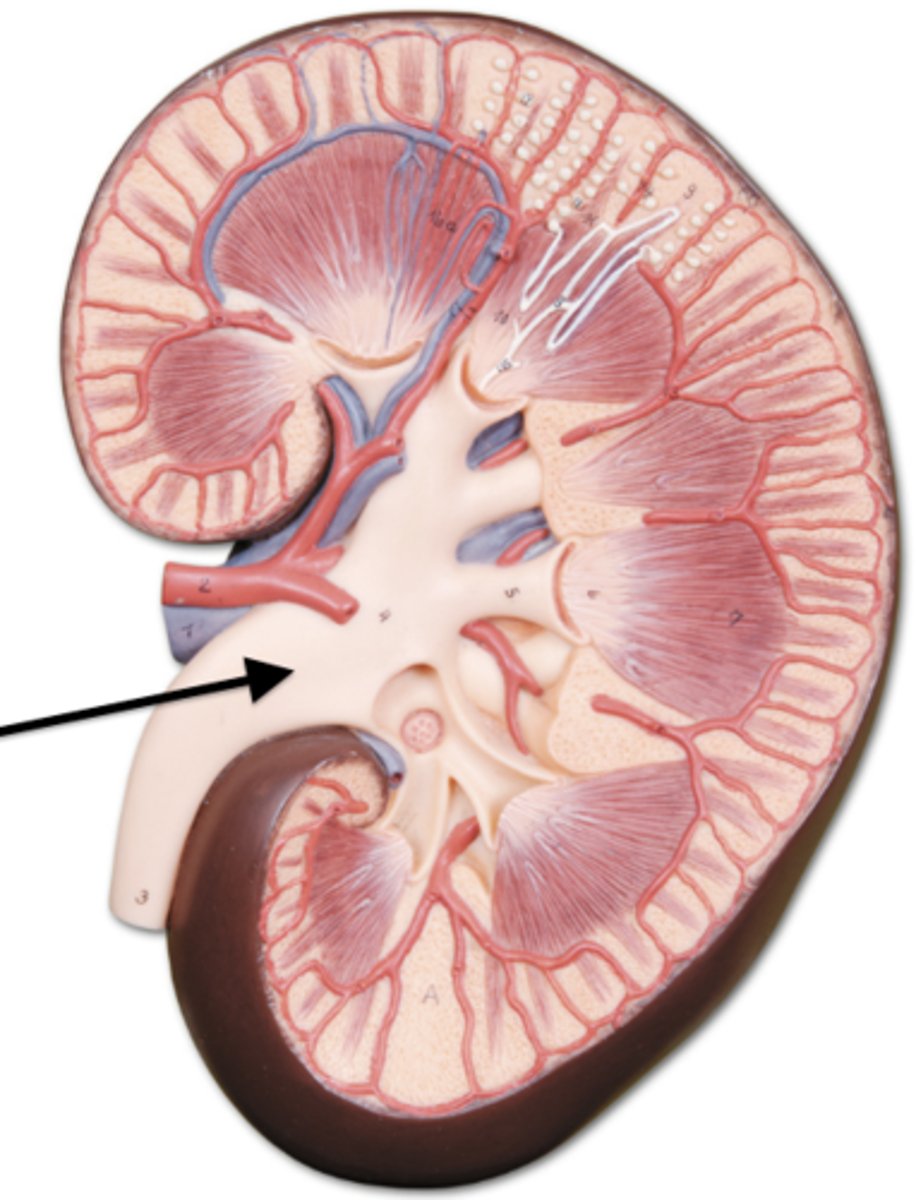
renal capsule
What is the arrow pointing at?
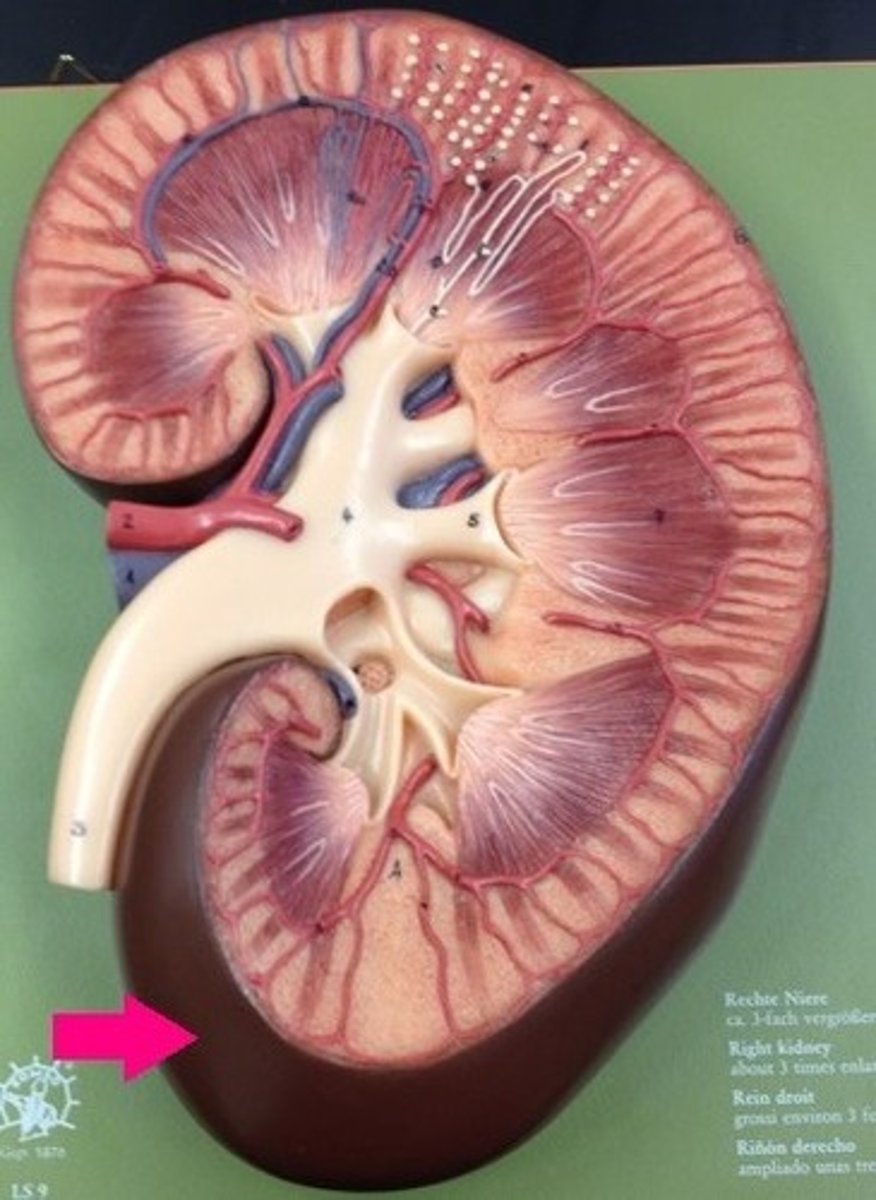
ureter
What is the arrow pointing at?
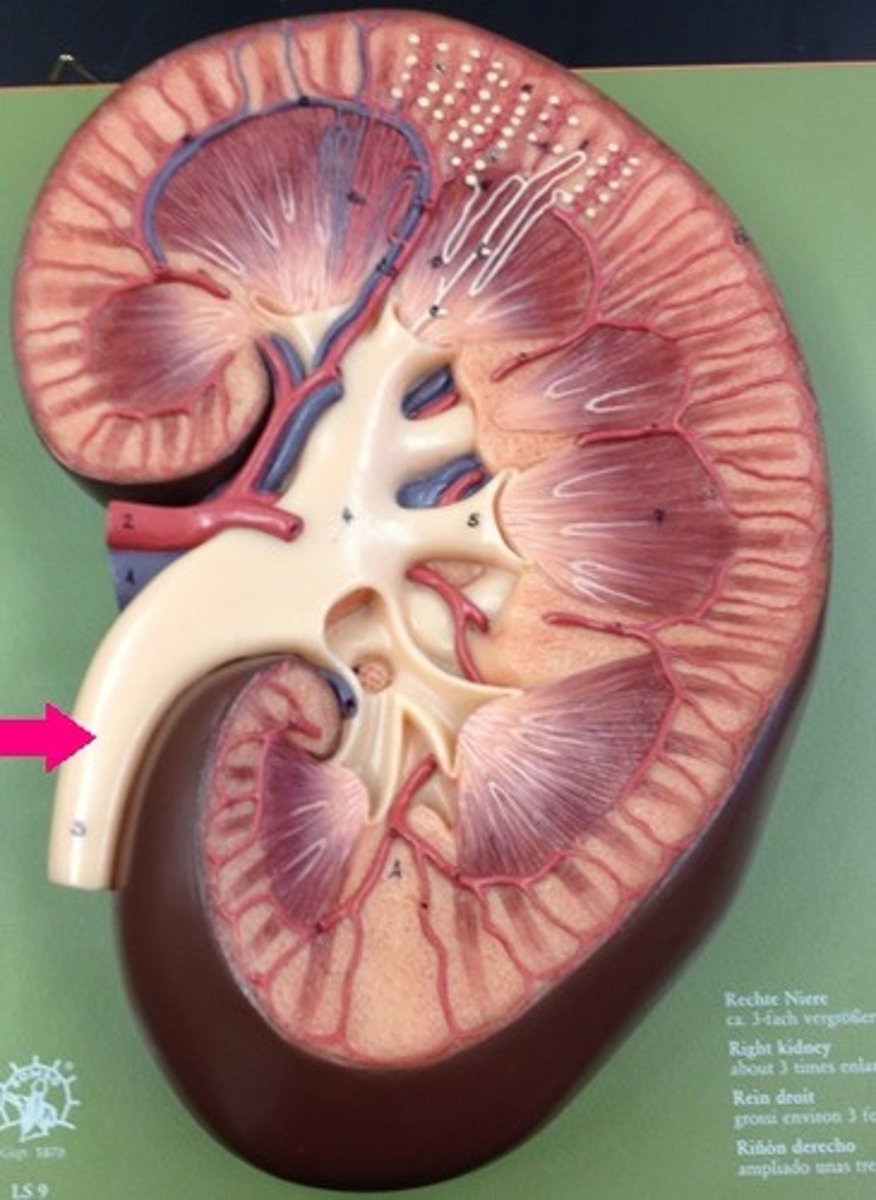
hilum
What is the arrow pointing at?
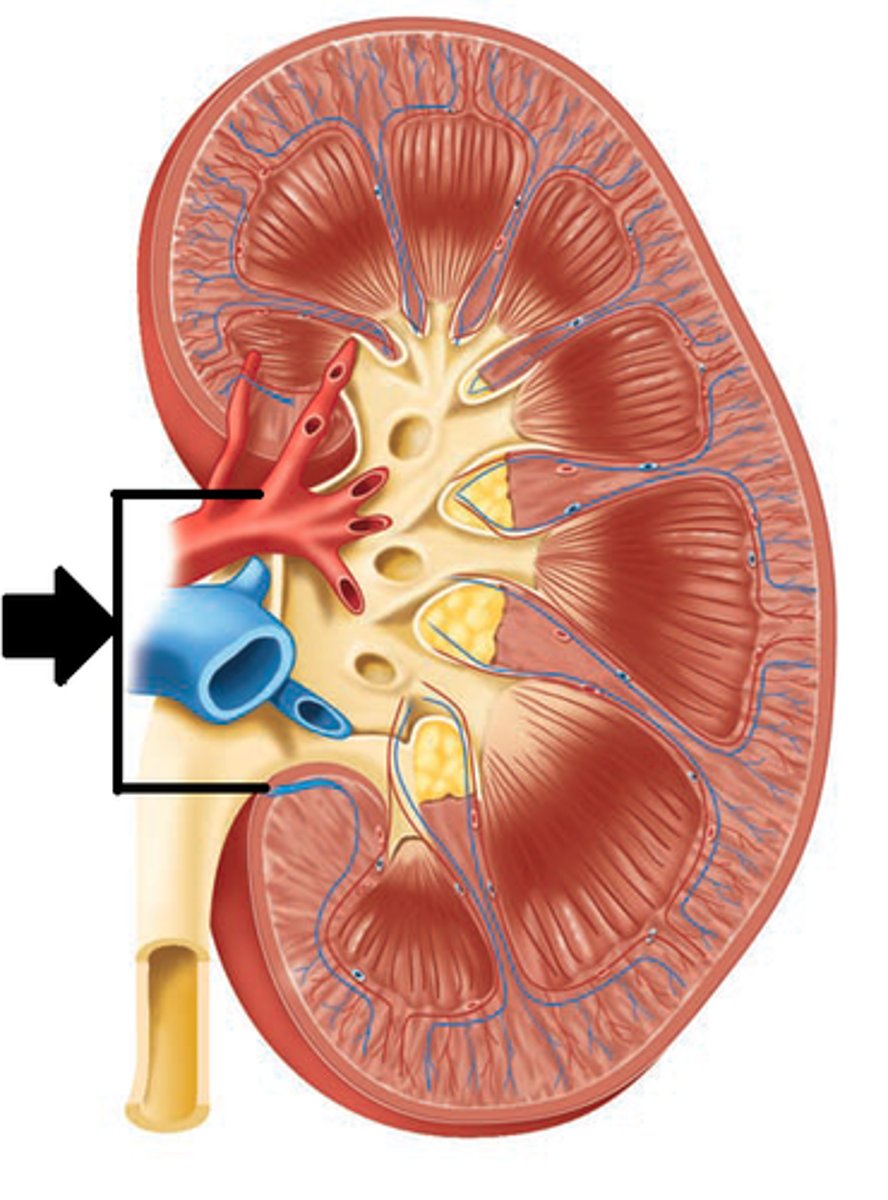
1. blood vessels
2. lymphatic vessels
3. ureter
What structures converge at the hilum?
renal pelvis, which is the upper expanded end of the ureter and where major calyces are joined
What renal structure does the hilum contain?
1. renal artery
2. afferent arterioles
3. glomeruli
4. efferent arterioles
5. renal vein
List the renal structures that blood flows through in the kidney starting with the renal artery
blood flow
All renal function is dependent upon adequate
exocrine and endocrine
Kidneys are responsible for what two main functions?
regulates volume and composition of plasma and fluid through filtration, tubular secretion, and tubular reabsorption and elimination of metabolic waste products primarily urea into urine
What are the functions of exocrine system?
renal control of sodium chloride excretion
What is the main determinant of extracellular fluid volume?
1. acid base balance
2. phosphate
3. potassium
4. calcium
List what the exocrine regulates in regards to plasma concentrations?
1. regulates blood pressure(vasodiliation)
2. RBC production
3. calcium homeostasis
4. prostaglandin synthesis
What are the endocrine functions?
afferent arteriole is larger in diameter than efferent arteriole
What greats a pressure gradient across the capillary walls?
very thin walls that are more permeable than tissue capillaries
What is unique about glomerulus capillaires?
some is filtered through the capillary membranes into bowmans capsule, and travels through renal tubules and the rest leaves through the efferent arteriole
When there is proper pressure gradient what happens with the plasma?
double-walled cup shaped structure surrounding the glomerulus of each nephron of the kidney
Describe bowmans capsule
filters to remove organic wastes, excess inorganic salts and water
What is the bowmans capsule function?
occurs in tubules and reabsorbs substances to return them into the circulation via peritubular capillaries
How does tubular reabsorption work?
occurs in tubules and allows movement of certain substances out of the blood in the peritubular capillaries and into the distal tubules then to collecting ducts
How does tubular secretion/excretion work?
regulates renal blood flow and glomerular filtration
What is the function of renin?
lower blood pressure by blocking angiotensin 1 from converting to angiotensin 2
What is the purpose of ACE inhibitors such as captopril? How?
is also reduced, resulting in a lower GFR
If afferent arteriole pressure is reduced, then the pressure in the glomerulus
releasing renin which is secreted by the juxtaglomerular apparatus
How do the kidneys respond to a lower GFR occuring?
angiotensinogen into angiotensin 1
What does renin convert?
peptide produced by the liver
What is angiotensinogen?
angiotensin converting enzyme (ACE)
What converts angiotensin I to angiotensin II?
vasoconstricts efferent arteriole increasing the pressure gradient causing higher blood pressure and an increased GFR
What does angiotensin 2 do?
decreased renal perfusion pressure, which decreases afferent arterioles pressure, decreasing filtration pressure and GFR
Renal artery stenosis (RAS) results when?
between afferent and efferent arterioles
Where is the juxtaglomerular apparatus located?
renin production and secretion controlling renal blood pressure
What is the juxtaglomerular apparatus function?
proximal, nephron loop, distal convoluted
What are the three primary renal tubules?
reabsorbs 2/3 of water and salts, all amino acids, glucose, and regulate pH filtrate
What is the function of the proximal convoluted tubule?
nephron removes water and solutes from the tubular fluid and returns them to the circulating blood
Reabsorption Definition
concentrates urine by reabsorbing water in descending loop, and salt ions in ascending loop
What is the function of the loop of henle (nephron loop)?
regulates potassium, sodium, calcium, and pH (only 1% of water in original filtrate is still present after passing through it)
What is the function of the distal convoluted tubule?
receives fluid from the DCT and the duct then empties into the renal calyces, renal pelvis, ureter, and then bladder
What is the function of the collection ducts?
95% water, nitrogenous wastes, hormones, blood or glucose (last two not normal)
Urine consists of?
1200-1600mL/day
How much urine is produced in a day?
kidney function impairment, RAS, obstructive, non-obstructive dilatation of renal pelvis, prevoid and postvoid, renal viability, uretal reflux, basically any renal issue
Indications for a renal scan?
horseshoe kidney (0.2%)
What is a anomaly with the kidneys?
anterior pelvic region
Where is a kidney transplant located?
neobladder, urostomy, nephrostomy
What are bladder change disorders?
thick kidneys with salt retention and edema
Glomerulonephritis
bacterial injection of the urinary tract
UTI (urinary tract infection)
infected urethra
Urethritis
bladder infection
Cystitis
infection from bacteria causes renal scarring
Pyelonephritis(kidney)
trauma, ingestion of a nephrotoxin, compromised blood flow to kidneys, urinary flow obstrction
Acute Renal Failure
causes necrosis of epithelium of tubules from things like mercury, lead, carbon tetrachloride
What does ingesting a nephrotoxin cause? What causes it?
kidney blood supply is cut off and tissue becomes necrotic
Explain renal infarct
simply kidney cysts (1:5 chance if over 50yrs) or polycystic disease
What are the types of kidney cysts?
inherited and cysts enlarge kidney and lose function over time
Explain polycystic disease
most common where there's a blockage where the ureter meets the kidney
Urinary Pelvic Junction (UPJ) Obstruction
blockage where the ureter meets the bladder
Ureterovesical Junction (UVJ) Obstruction
ureter is dilated, but with diuretic urine can clear
Dilated Non-obstructed kidney