Visual Perceptual Deficits
1/32
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
33 Terms
visual impairment
change in quality and amount of visual input to the brain; impacts how the brain processes and uses visual input; results from disease, trauma, aging
neurological- TBI, concussion, PD, MS, AD
limits occupational engagement, social isolation, risk for depression
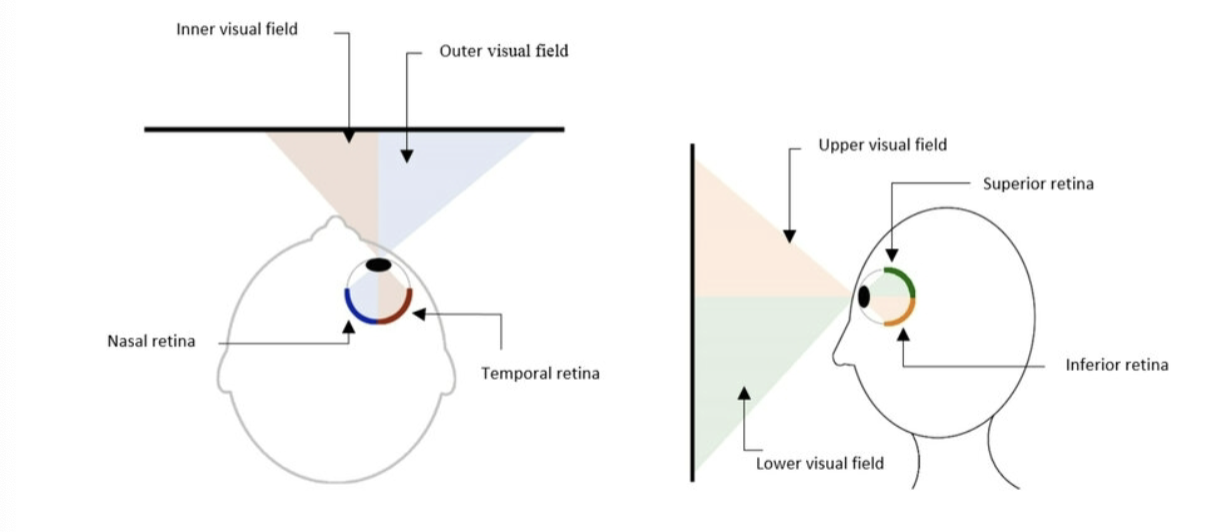
visual field
fixated eye can detect visual stimulation in a specific part of the environment; photoreceptors and visual pathway take info into retina from a point of fixation
factors: distance from eye, apparent size, stimulus duration, background lighting, intensity of stimulus, contrast, color, patient factors, adapting to light/dark
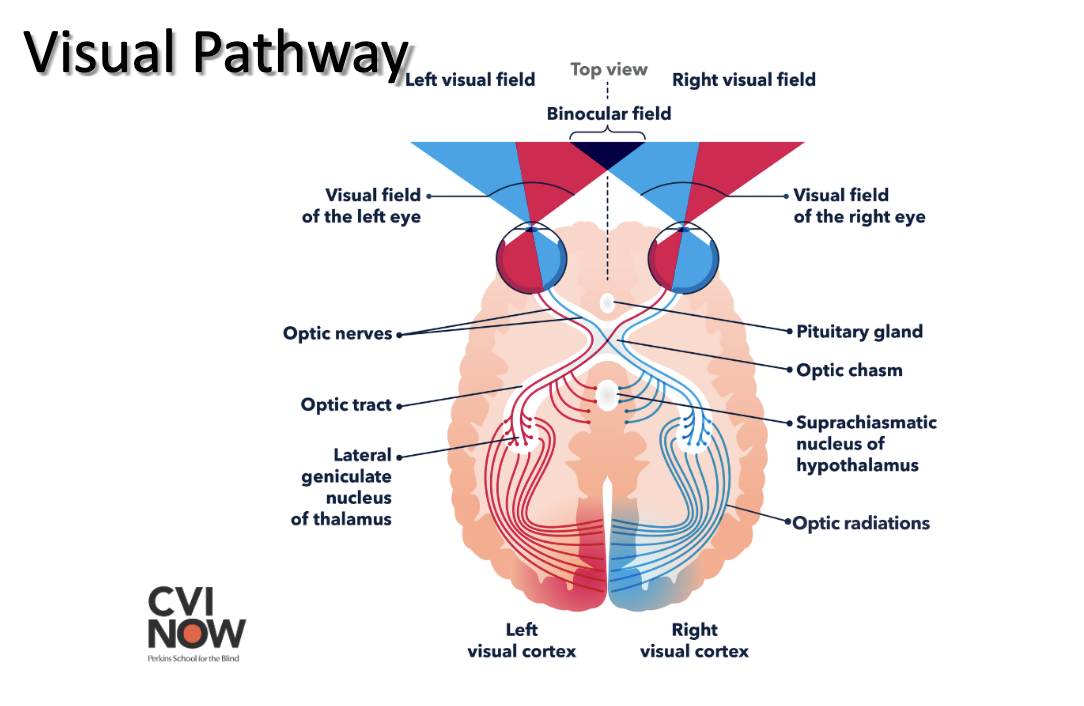
Visual pathway
Visual Streams
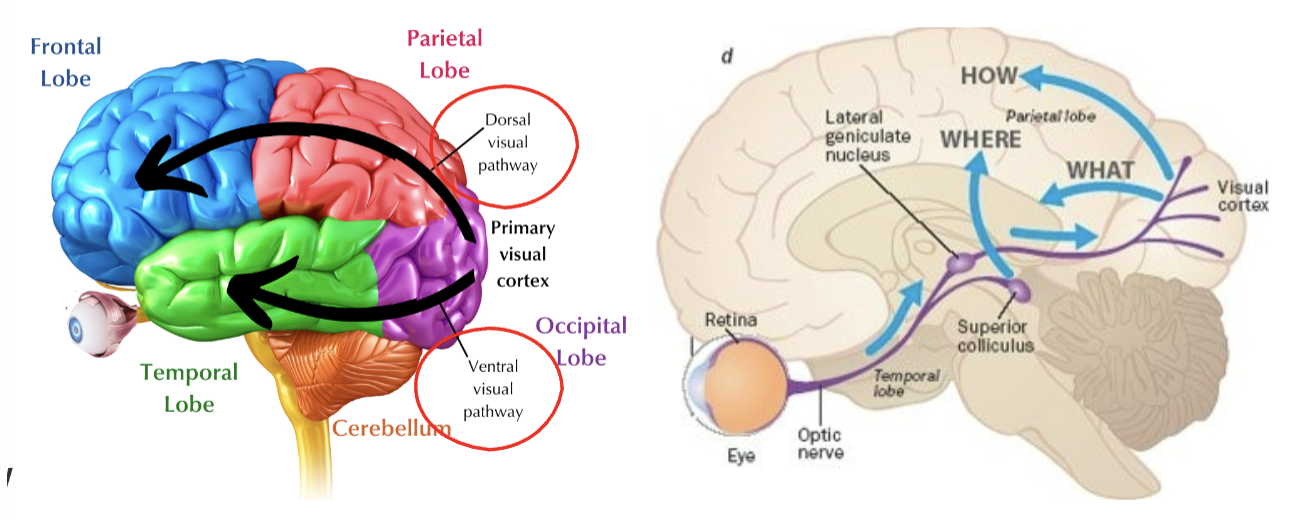
Vision and Lobes of the Brain
occipital: primary visual cortex, visual association cortex (analyzing orientation, position, movement, initiation of smooth pursuits, visual field loss)
temporal lobe- combines sensory info associated with the recognition and identification of objects (people, place things)
frontal lobe- saccades, attention
parietal lobe- locating objects, eye movement, drawing/constructing objects, neglect, movement through space
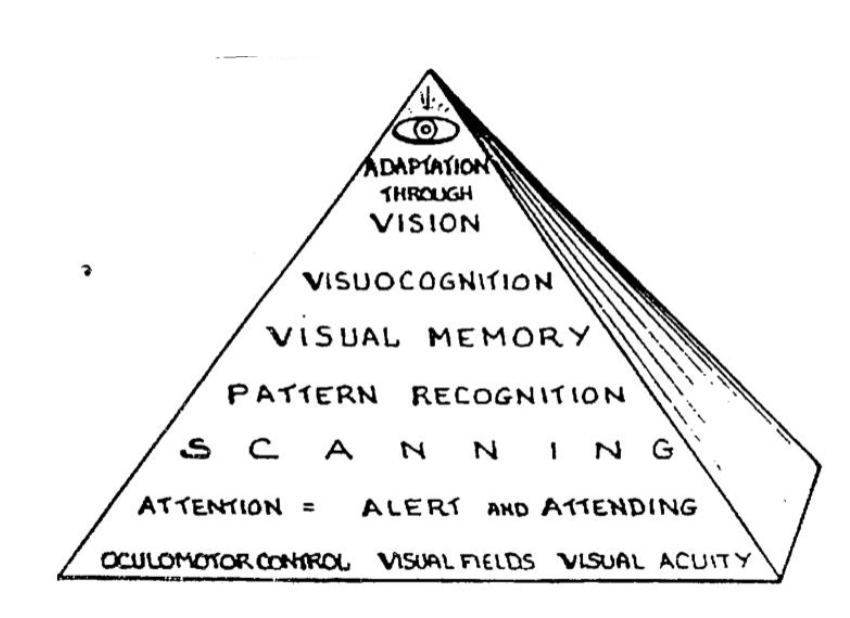
Warren’s visual perceptual hierarchy
oculomotor control- allow eyes to move smoothly, coordinated through pursuits, saccades, ability to accommodate and fixate, focus of target on fovea of retina (head movement, gaze shift, fixation); binocular vision
impairments: diplopia, reduced depth perception, difficulty tracking, reduced fixating/localizing, strabismus, convergence insufficiency
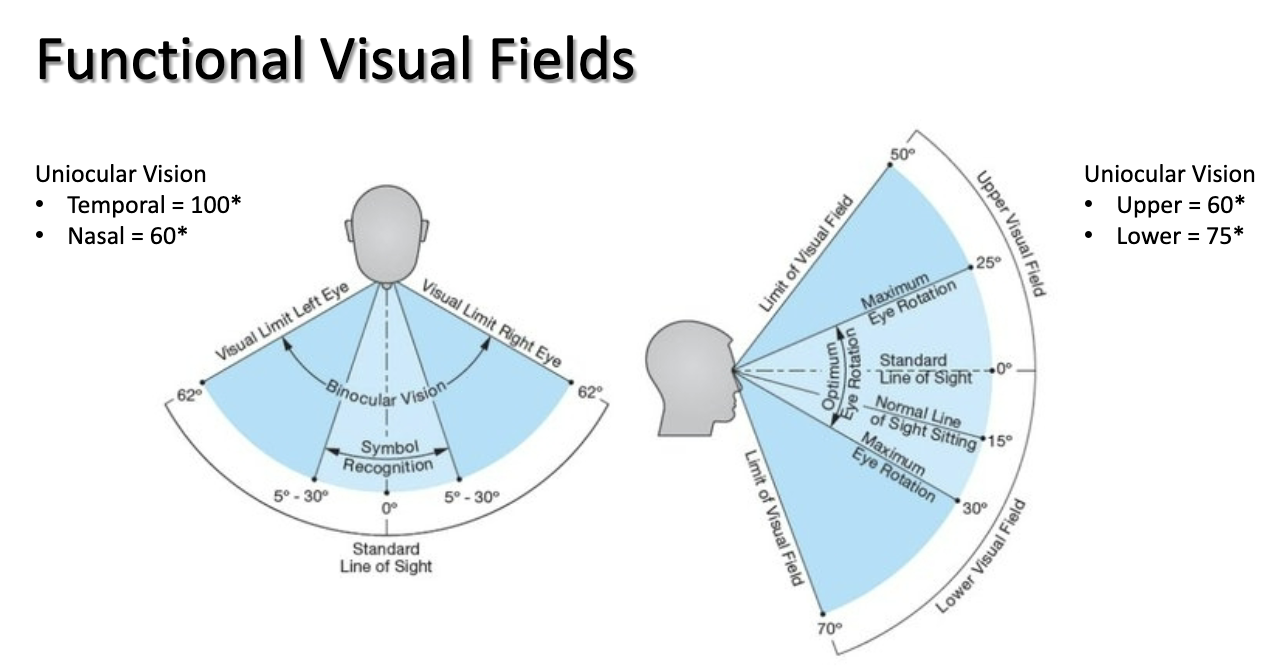
visual field- amount of visual surroundings that can be seen when a person looks straight ahead; monocular peripheral vision and binocular cen
impairments: hemianopia, quadrantopia, depends on lesion location where visual field deficit is
visual acuity- ability to see clear and precise images for small visual details
impairments: difficulty focusing, damage to the retina, optic nerve, posterior cortical processing
Visual Attention and Scanning
focal/selective- distinguish visual details; used for object recognition and identification
ambient/peripheral- big picture, location of objects in the environment and proximity
impairments: hemi-inattention (impaired vs lost, reactive vs processing, inattention to different sensory input contralateral from lesion), spatial bias, nonlateralized attention deficit, mental representation of space
Pattern Recognition
perceptual process of matching incoming visual stimuli with stored visual memories
visual memory
take in stimuli, retain details, store it for later retrieval
visual cognition
ability to use visual info to solve problems, make decisions, and complete planning and organizational tasks through mental manipulation
Form constancy
form, shape, and object is recognizable even when it changes in size, position, or is in a different environment
clinical presentation: difficulty recognizing people wearing different clothing, difficulty following directions with pictures
figure ground perception
ability to distinguish foreground from background or differentiate an object from background
clinical presentation: unable to sort/match socks while folding laundry, locating items in drawers, missing road signs or other obstacles when driving, locate toy in toybox
visual closure
ability to accuratly identify objects that are partially covered or missing
clinical presentation: can’t identify traffic sign partially hidden behind a tree, difficulty locating objects in fridge that are partially hidden
visual organization
ability to group objects based on their identifying properties
clinical presentation: poor spacing in handwriting, difficulty locating objects in the store
spatial orientation
ability to recognize that position of oneself or objects in relation to opposing positions, directions, movement, and environmental locations
clinical presentation: letter/number reversal, spacing out writing
topographical orientation- ability to orient oneself within the environment and navigate
clinical presentation: lost/wandering behavior
depth perception
visual ability to perceive relative distance
clinical presentation: missing a step, missing the counter when setting things down, unable to catch a ball
visual discrimination
ability to identify unique characteristics of objects, shapes, colors, and people for comparison
difficulty sorting
agnosias
visual agnosia: condition in which a person can’t interpret visual info
see common objects and don’t know what it is, but can identify it with other senses like touch or smell
color agnosia: inability to recognize colors despite intact color perception, semantic memory for color, and color naming
selective loss of associations between objects and color (can’t answer what color is a banana, name things that are red)
prospagnosia- inability to identify familar faces
simultanagnosia- inability to see more than one object or part of an object at the same time
metamorphopsia
objects or straight lines appear warped, distorted, or bent
OTs Role
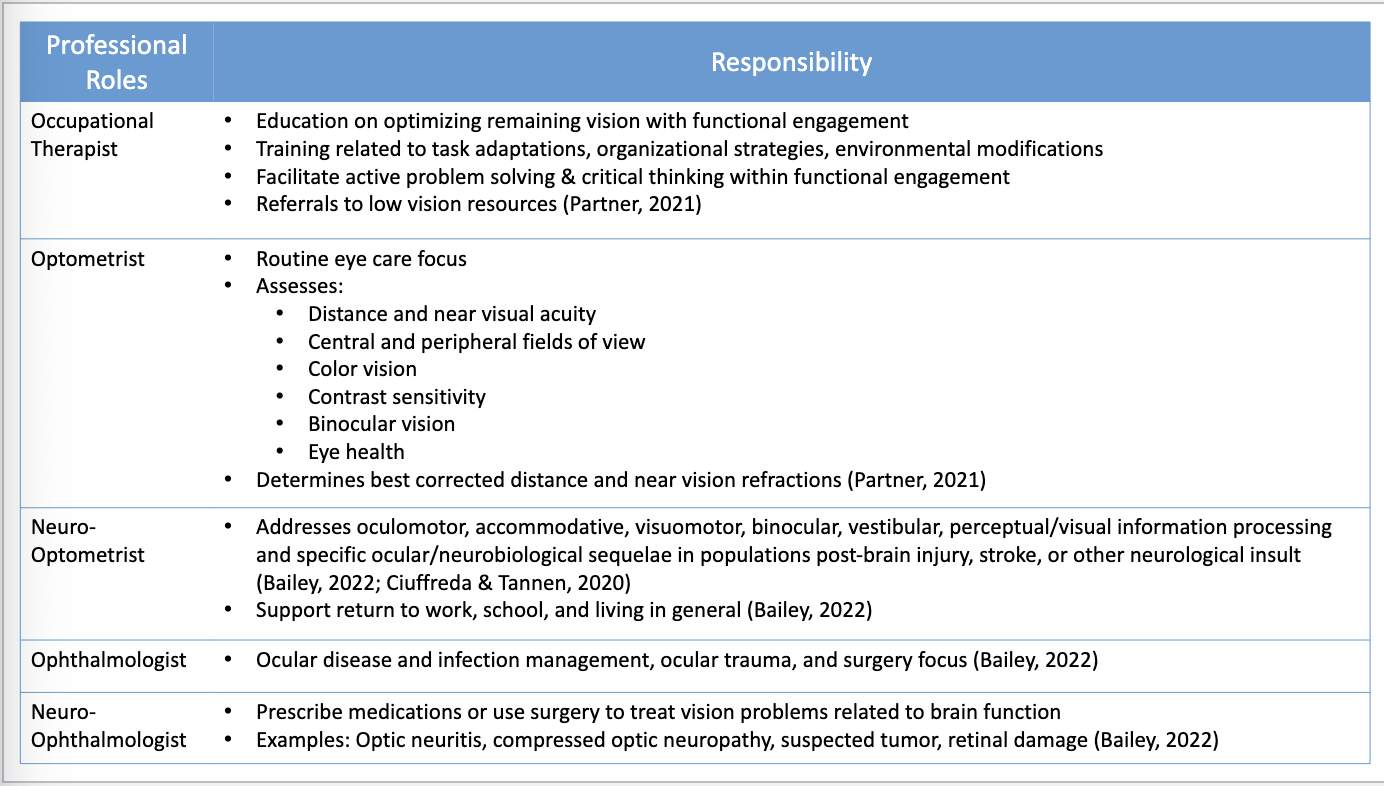
Vision Screen
visual acuity- snellen eye chart for distance and near
accommodation- automatic adjustment of they eye for seeing at different distances; use near acuity chart and move until blurry
diplopia- double vision; note what quadrants are affected
pursuit- ocular motor skills of following a moving taret with head still; note lack of smooth moment, sluggish, overshooting/undershooting, double vision, pain

Vision Screen Assessments
Depth perception- stereo fly test
suppression- ability to disregard info from one eye through natural adaptation to make sense of info received
frequently following prolonged double vision. red/green activities
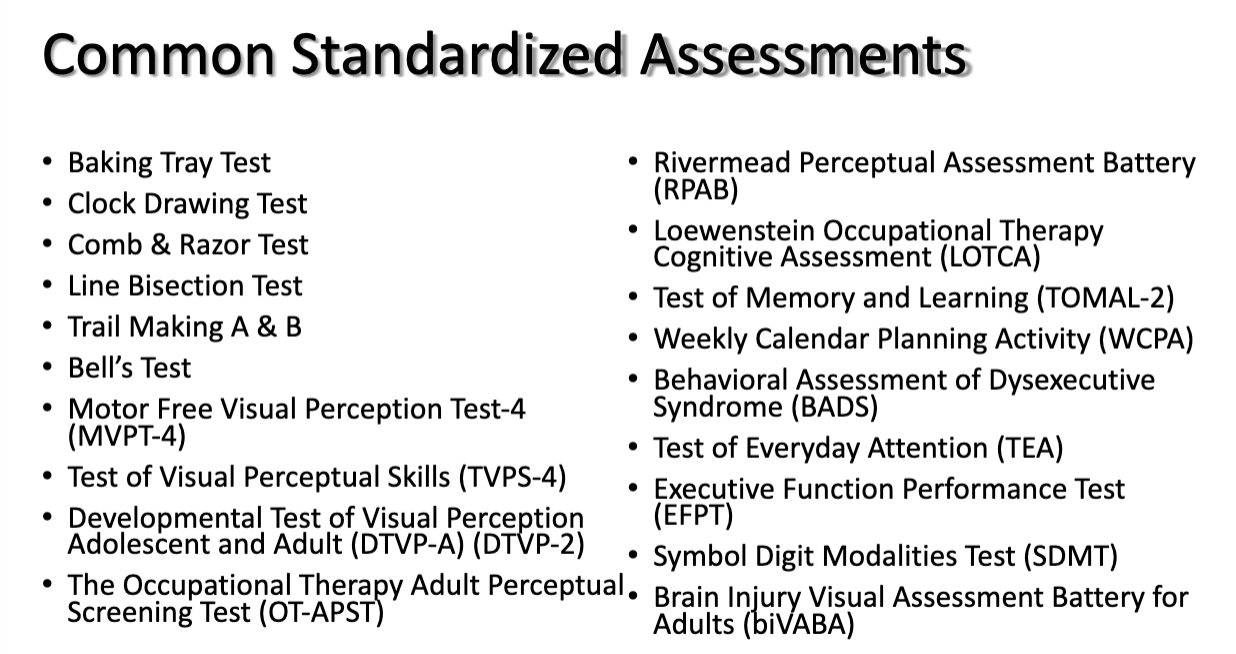

Treatment approaches
remediation- preferred as first measure when they show potential for improvement, awareness of limitations, ability to receive feedback
scanning/tracking to increase strength of eye muscles, increase in complexity, repeated practice, building confidence
not affective for decreased acuity
compensation- internal/external strategies to improve performance; maximize function and safety
adaptation- change the environment or task demands to increase safety and function
adjusting placement/intensity of lighting, increased contrast, adjust print size
compensation + adaptation- when remediation is not effective; introduce in VFD, use first when safety is at risk
visual acuity eval and intervention
observe function, especially reading
screen high and low contrast acuity
use best corrected vision for refractive errors
measure person’s ability to identify progressively smaller letters/numbers/symbols
intervention: clean and prescribed glasses→referral to optometrist/ophthalmologist
increase contrast, reduce patterns, good lighting, enlarge items, structured/predictable environment

Oculomotor eval and intervention
obtain visual history, listen to complaints, observe eye movements (pupil asymmetries, eyelid function, eye position)
track moving target vertically, horizontally, diagonally
track convergence with moving target towards nose
diplopia- access each eye covered/uncovered for deviation
intervention- education on visual stress, identify triggers, environmental mod (contrast, increase size, reduce pattern, lighting), habits/routines
under the supervision of eye physician: occlusion, prisms and lenses, eye exercises, surgery
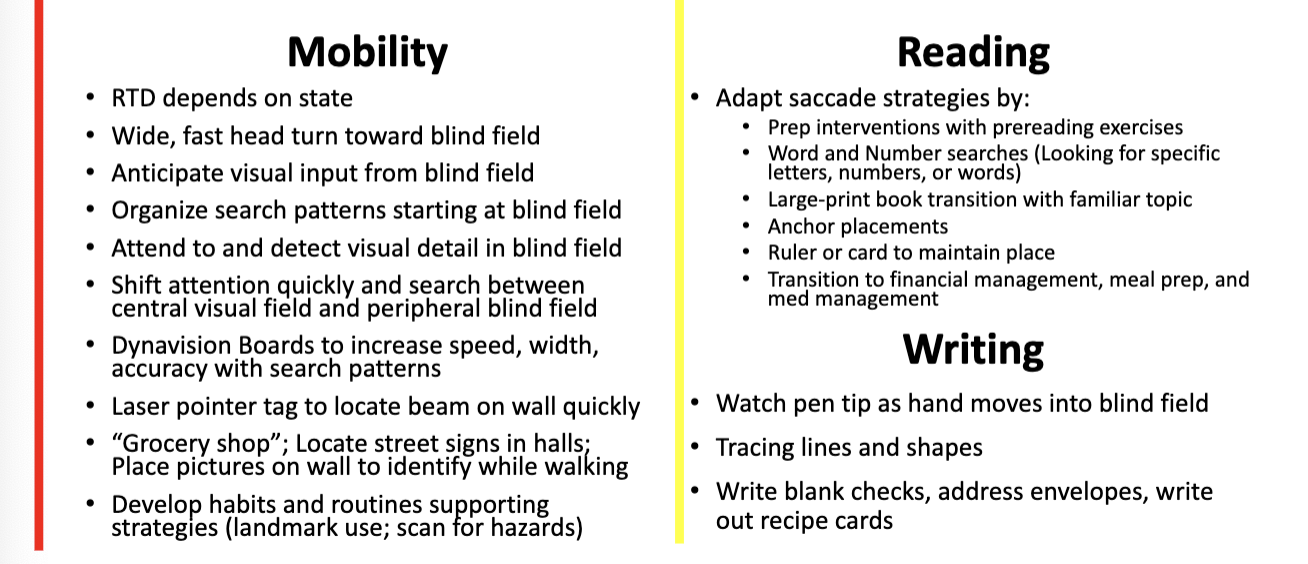
Visual field eval and intervention

visual attention/scanning eval
first eval for aphasia, motor impairment, visual acuity, oculomotor, visual fields
observe visual search task while monitoring for organized search strategies (L to R, top to bottom, symmetrical search of both sides), sustained visual search or drifting off, locate targets accurately
cancellation tests: lines, rows, numbers, symbols; record time to complete and accuracy
intervention: modification (focus on environmental and task mod; minimize patterns, increase environment structure); compensation (visual scanning strategy, interact physically with target, conscious attention to detail, lighthouse)

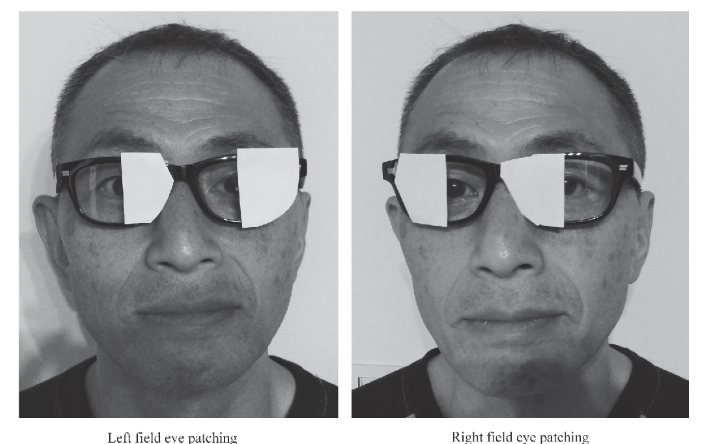
Patching
quick, effective, inexpensive tool to decrease unilateral inattention; occluding one ye facilitates attention and visual saccades to contralateral side
caution: studies found that once removed, did not translate into function
hemi field patching demonstrated greater improvements in functional independence
Pattern recognition intervention
skills required in form constancy + figure ground perception + visual closure + visual organization + spatial orientation
reduce visual stimulation and overlapping objects; change spatial arrangements, slow down processing times, proper scanning strategies, multi sensory techniques
laundry sorting: form piles of clothes by type, sort by color, search for specific clothes using a L-R top-bottom scanning strategy

visual perceptual screening

unilateral inattention screening

depth perception screening

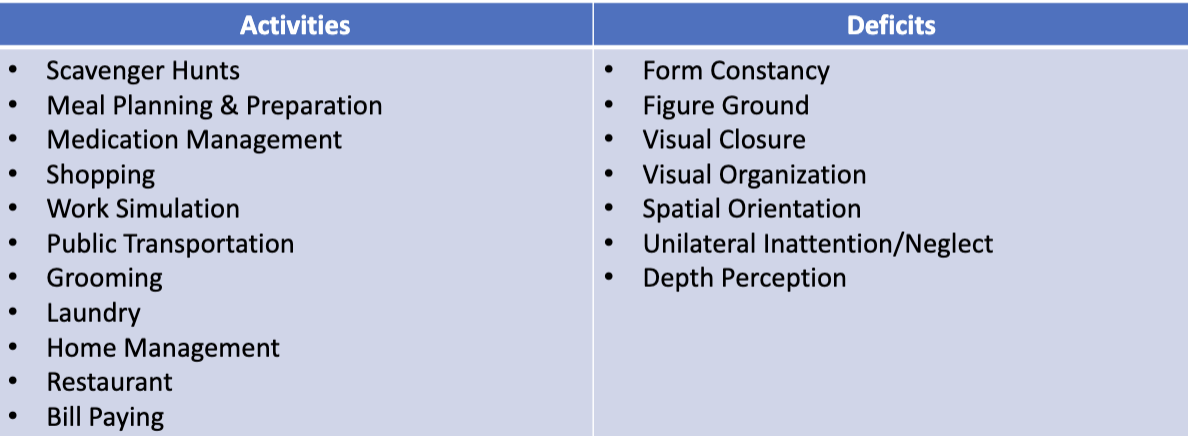
Functional Therapy Activities for Perceptual Deficits