A&P Exam 4
1/169
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
170 Terms
Major Structures of Urinary System
Kidneys
Ureters
Urinary bladder
Urethra
Kidney functions
Excretion of wastes
Regulation of blood ionic composition
Regulation of blood pH
Regulation of blood volume (and blood pressure)
Maintenance of blood osmolarity
Production of hormones
Regulation of blood glucose level
Excretion of wastes
Most wastes result from metabolic reactions
Include: Urea, ammonia, creatinine, uric acid, and urobilin (nitrogenous wastes)
Regulation of blood ionic composition
Kidneys can adjust the amount of ions that are excreted into the urine
Regulation of blood pH
Kidneys can adjust the amount of acids or bases that are excreted into the urine
Regulation of blood volume (and blood pressure)
Kidneys can adjust the amount of water that is excreted into the urine
Increased water in blood = increased blood volume = increased blood pressure
Decreases blood volume = decreased blood pressure
Maintenance of blood osmolarity
Adjusting the amount of water and solutes that are excreted into the urine
Production of hormones
Calcitrol
Eyrthropoetin
Calcitrol
Active form of Vitamin D
Helps regulate calcium homeostasis
Eyrthropoetin
Stimulates the production of blood cells
Regulation of blood glucose level
Kidneys can use the amino acid glutamine to synthesize new glucose molecules (gluconeogenesis) to help maintain a normal blood glucose level
Ureter function
Urine passes through this
Urinary bladder function
Where urine is stored
Urethra function
Urine leaves through this
External gross anatomical features of the kidney
Renal hilum
Layers of tissue surrounding each kidney (superficial to deep)
Renal hilum
Indentation on the medial border
Passage of blood vessels, nerves, lymphatic vessels, and the ureter
Layers of tissue surrounding each kidney (superficial to deep)
Renal fascia
Adipose capsule
Renal capsule
Renal fascia
Thin layer of dense irregular connective tissue that anchors the kidney to the surrounding structures and to the abdominal wall
Adipose capsule
Mass of fatty tissue that protects the kidneys and holds it in place within the abdominal cavity
Renal capsule
Smooth, transparent sheet of dense irregular connective tissue that protects and helps maintain the shape of the kidney
This layer is continuous with the outer coat of the ureter
Internal gross anatomical features of the kidney
Regions
Regions
Renal cortex
Renal medulla
Renal cortex
Outer
Contains nephrons (functional units)
Renal medulla
Inner
Made up of renal pyramids and columns
Minor calyx
Major calyx
Renal pelvis
Columns
Portions of cortex that extend between each pyramid
Renal papilla
Apex of each pyramid
Minor calyx
Where renal papilla empties urine
Major calyx
Minor calyx widens to form this
Renal pelvis
Major calyces merge to form this
Funnel-shaped expansion at the proximal end of the ureter
Nephron Parts
Renal corpuscle
Renal tubule
Renal corpuscle parts
Glomerulus
Glomerular (Bowman’s capsule)
Glomerulus
Tangled, ball-shaped network of capillaries formed by branches of the renal artery
Glomerular (Bowman’s capsule)
Double-walled epithelial cup that surrounds the glomerular capillaries (visceral and parietal layers)
Blood plasma is filtered out of the glomerular capillaries and collected by this
Renal tubule
Filtered liquid (filtrate) passes into this
Tubules modify filtrate to produce urine
Collecting duct
Papillary ducts
Renal tubule sections
Proximal convoluted tubule (PCT)
Nephron loop (loop of Henle)
Distal convoluted tubule
Collecting duct
Distal convoluted tubules of several nephrons empty into a single one of these
Papillary ducts
Drain into the minor calyces
Several collecting ducts merge to form this
Functions performed by nephrons and collecting ducts
Glomerular filtration
Tubular reabsorption
Tubular secretion
Glomerular filtration
Movement of water and solutes from plasma into the glomerular capsule -> then into the renal tubule
In the glomerulus
Tubular reabsorption
Movement of water and solutes out of the various segments of the tubule and into the peritubular capillaries
All along the renal tubules and collecting duct
Tubular secretion
Movement of water and solutes out of the peritubular capillaries into the tubule for excretion
Removes a substance from the blood
All along the renal tubule and collecting duct
Filtration membrane
Leaky barrier
Substances from the blood cross three barriers
Substances from the blood cross three barriers
Glomerular endothelium
Basement membrane
Filtration slits
Glomerular endothelium
Prevents filtration of blood cells but allows all components of blood plasma to pass through
Basement membrane
Prevents filtration of larger proteins
Filtration slits
Prevents filtration of medium-sized proteins
Leaky barrier
Formed by
Glomerular capillaries
Podocytes
Podocytes
Cells that form the visceral layer of the glomerular capsule
Foot-like processes that wrap around the capillaries but do not fully encapsulate them
Form the filtration slits
Glomerular filtration depends on 3 main pressures
Glomerular blood hydrostatic pressure (GBHP)
Capsular hydrostatic pressure (CHP)
Blood colloid osmotic pressure (BCOP)
Glomerular blood hydrostatic pressure (GBHP)
Blood pressure in the glomerular capillaries
Created by the imbalance of the afferent and efferent arterioles
Afferent arteriole
Larger diameter
Allows more blood to flow into the glomerulus
Efferent arterioles
Small diameter
Prevents blood from leaving
Created by the imbalance of the afferent and efferent arterioles
Creates a small "back up” of blood - forcing water and solutes through the vessels and into the capsule
Promotes filtration by forcing water and solutes through the filtration membrane
Capsular hydrostatic pressure (CHP)
Pressure exerted against the glomerulus by the fluid already in the capsular space
Opposes filtration
Blood colloid osmotic pressure (BCOP)
Due to presence of proteins in the blood plasma
Opposes filtration
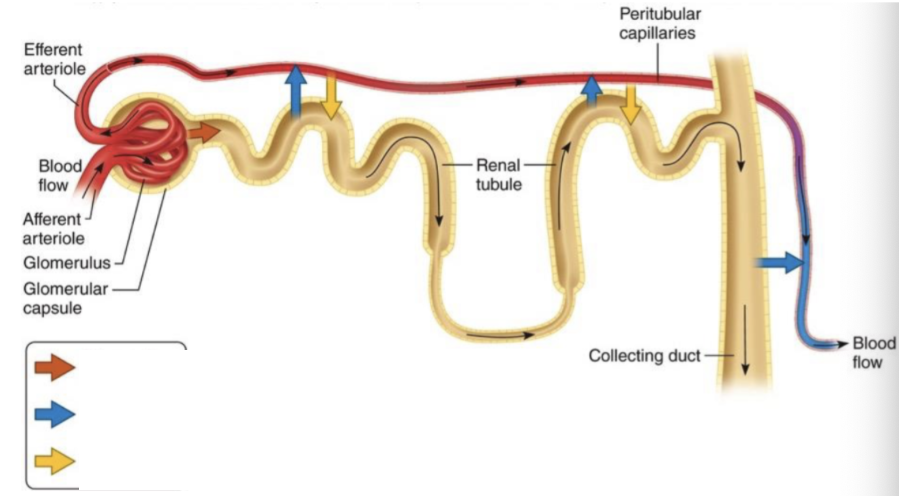
Orange Arrow
Glomerular filtration
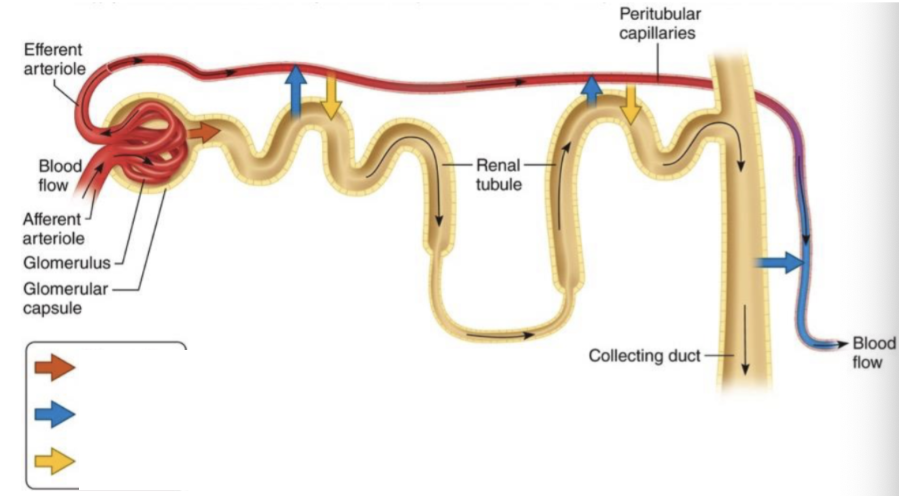
Blue Arrow
Tubular reabsorption
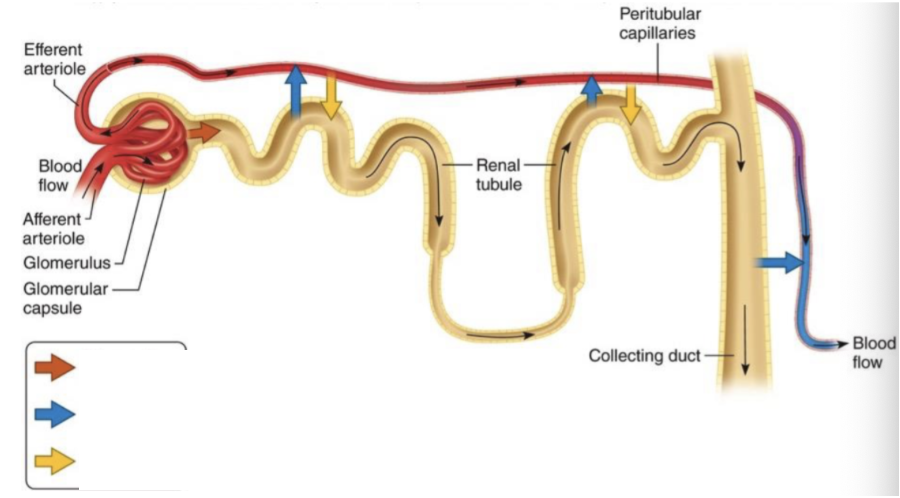
Yellow Arrow
Tubular Secretion
Proximal Convoluted Tubule Reabsorption
Largest amount of solute and water absorption takes place here
65% of the filtered water, Na+, K+, and Ca2+
100% of most filtered organic solutes (glucose and amino acids)
50% of the filtered Cl-
80% of the filtered HCO3-
50% of the filtered urea
Variable amount of Mg2+ and HPo42- (phosphate)
Nephron Loop Reabsorption
15% of the filtered water (descending limb)
25% of the filtered Na+, K+, Ca2+
35% of the filtered Cl-
10% of the filtered HCO3-
Variable amount of Mg2+
DCT Reabsorption
5% of the filtered Na+ and Cl-
Variable amounts of Ca2+
Proximal Convoluted Tubule Secretion
Variable amounts of
H+
NH4+ (ammonium ions)
Urea
DCT Secretion
Excess K+ can be secreted into the tubular fluid from the bloodstream based on need
Urinalysis
An analysis of the volume and physical, chemical, and microscopic properties of urine
Urinalysis Importance
Reveals much about the state of the body
Fluid intake
Blood pressure
Blood osmolarity
Diet
Body temperature
Diuretics
Mental state
General health influence urine volume
Ureter Physiology
Carry urine from the kidneys to the urinary bladder through peristaltic contractions, hydrostatic pressure, and gravity
Urinary Bladder Anatomy
Hollow, muscular
Urinary Bladder Layers
Inner
Intermediate
Superficial
Inner
Mucosa
Mucous membrane made up of traditional epithelium
Intermediate
Muscular layer, also called the detrusor muscle
Consists of 3 layers of smooth muscle
Internal urethra sphincter
External urethral sphincter
Internal urethra sphincter
Formed by circular muscle fibers around the opening to the urethra
External urethral sphincter
Skeletal muscle
Inferior to internal urethral sphincter
Superficial
Posterior and inferior surfaces = adventitia
Superior surface = serosa
Adventitia
Layer of areolar connective tissue
Serosa
Layer of peritoneum
Urinary bladder physiology
Where urine is stored
Urethra anatomy
Small tube leading from the internal urethral orifice of the urinary bladder to the exterior of the body
Urethra in males
It passes through the prostate, then through the deep perineal muscles, and finally through the penis
Prostatic urethra
Membranous urethra
Spongy urethra
Urethra physiology
Conveys urine to the outside
Primary functions of the reproductive systems
Produce gametes
Transport gametes
Enable fertilization
Support development (female)
Secrete hormones
Gametes
Sex cells
Male Gametes
Sperm
Small
Motile
Female Gametes
Oocyle (egg)
Large
Non-motile
Role of hormones in regulating reproduction
Regulate reproductive processes
Control gamete production
Maintain secondary sex characteristics
Scrotum structure
External pouch
Dartos muscle
Cremaster muscle
Dartos muscle function
Wrinkles skin (heat conservation)
Cremaster muscle function
Raises/lower testes
Scrotum functions
Houses testes
Keeps testes 2-3 degrees C below body temperature
Essential for normal sperm production
Testes Structure
Male gonads located in scrotum
Seminiferous tubules
Sertoli (sustentacular) cells
Leydig (interstitial) cells
Seminiferous tubules
Site of spermatogenesis
Sertoli (sustentacular) cells
Support developing sperm
From blood-testis barrier
Produces inhibin
Leydig (interstitial) cells
Produce testosterone
Testes Function
Produce
Sperm
Testosterone
Pathway of sperm from production to exit
Seminiferous tubules
Epididymus
Ductus (vas) deferens
Ejaculatory duct
Urethra
Epididymus function
Site of
Sperm maturation
Storage
Ductus (vas) deferens function
Carries sperm from epididymis
Urethra function
Shared exit pathway
Accessory glands
Forms semen
Seminal vesicles
Prostate gland
Bulbourethral glands
Seminal vesicles
Add fructose-rich fluid (~60%)
Prostate gland
Adds enzymes (~25%)