myelogram, lumbar puncture, epidural injection, arthrogram, steroid injection, joint aspiration
1/100
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
101 Terms
clean asepsis is aka what
medical asepsis
what is the definition of clean asepsis
the reduction in microorganisms using water, soap, friction, and chemical disinfectants
clean asepsis would be used prior to what?
administering medications
enemas
tube feedings
interactions with patients
daily hygiene
what are two examples of clean asepsis
hand washing with soap and water
using an alcohol-based hand rub
surgical asepsis is aka
sterilization
what is the definition of surgical asepsis
the complete removal of microorganisms and their spores by using a heat or chemical process
what does surgical asepsis eliminate
eliminates all pathogens
where is the sterilized equipment that is used during invasive procedures in radiology obtained from?
obtained from the central supply department
what is the definition of disinfection
used when articles or surfaces cannot be sterilized (like countertops)
what are 2 examples of disinfection
sani wipes
bleach
lysol wipes
what is the definition of antiseptic
used to cleanse the skin
what are two examples of antiseptic
hand sanitizer
hydrogen peroxide
iodine
rubbing alcohol
when does the CDC require a mask to be worn
when a catheter is being placed or material injected into the spinal canal or subdural space
what two anatomic features must a mask fully cover
mouth
nose
how should a mask be removed
remove by handling the ties only
what is a sterile field
the area that has been prepared for the use of sterile equipment and supplies and a microorganism free area
items are considered sterile when they are:
clean
dry
unopened/not punctured
the expiration date has not passed
the sterility indicators have changed to the predetermined color that indicates the package is sterile
what are 4 things you should not do over a sterile field
sneeze
cough
laugh
talk over
once a sterile field is prepared, should it be left unattended
no
what type of contamination is just as serious as a break in the sterile technique
airborne contamination
what are the steps for opening a sterile package
wash your hands
remove tape and open the corner away from you
open next 2 corners to the left and right
pull last corner towards your body
if you need to add any items to the sterile field, how would you do so
while holding the edges of the wrapper, drop the item onto the sterile field
why must a small amount of solution be poured out prior to it being placed on the sterile field
to “wash” the containers lip and avoid the possibility of contaminating the tray
describe how you would add a sterile solution to a sterile field
discard a small amount of solution
place container at the edge of the sterile field
pour from a distance to prevent contamination pour away from the label
pour away from the label
what are the two types of gloving techniques used
open gloving
closed gloving
describe how you would put gloves on utilizing the open gloving technique
glove dominant hand first
pick up right glove with left hand at folded cuff
slide the right hand into the glove, do not unfold the cuff
pick up left glove with the gloved right hand under the fold
pull glove on over the hand and cuff of gown, then place fingers of gloved left hand under the cuff of the right glove, pull it over the cuff of the gown, then adjust
describe how you would put gloves on utilizing the closed gloving technique
glove package needs to be opened before the scrub procedure
cover both hands with sterile gown sleeves
pick up right glove with the left hand
place fingers of glove towards elbow
grasp cuff of glove through the gown
pull glove over the fingers and cuff of gown
with gloved hand pick up left glove
place fingers pointing towards the elbow
grasp cuff and pull second glove into place
which of the two techniques described would you utilize when setting up a sterile field in radiology
open gloving
the sterile field ends at what level
at the level of the tabletop or the waist of the sterile persons gown on the front side only
what abbreviation does CNS stand for
central nervous system
what two parts of the central nervous system divided into
the brain that occupies the cranial cavity
the spinal cord that is suspended within the vertebral column
where does the spinal cord begin and end
beings at the brain and ends at L1-L2
what is the name for the terminal end of the spinal cord
cauda equina
what is the function of the meninges
cover and protect the brain and spinal cord
what are the 3 layers of the meninges
dura mater (outer layer)
arachnoid mater (middle layer)
pia mater (inner layer)
what color is the cerebral spinal fluid
clear and colorless
at a given time, how much CSF is present in the body
150 mL
what is a cistern
expanded areas of the subarachnoid space
what is the most common site for lumbar punctures to be performed
lumbar cistern
what is the purpose of preparing the skin prior to beginning a procedure
to remove as many microorganisms as possible from the skin to reduce the risk of infection
what are the 2 ways to prepare the skin prior to a procedure
mechanical
chemical
when should hair be removed for a procedure
if it interferes with the procedure
describe the procedure when shaving a patient
hold the skin tight (taut)
shave in the direction of hair growth
dont nick or cut the skin
shave with short, firm strokes
wet sterile sponge with alcohol, removing all of the hair
when is chemical skip prep performed
after mechanical preparation
describe the steps for performing a chemical skip prep
get out gloves and a prep set
always ask if the patient is allergic to iodine before starting to cleanse the area
put on sterile gloves using the open gloving technique
prep 6-12” around the operation site
rub antiseptic solution in a circular motion (inside to outside)
repeat with a new sponge and watch for signs of irritation
allow skin to dry
what action is needed to remove microorganisms
friction
how would you know the proper amount of dry time is used using iodine to prepare the skin
the manufacturer has a stated amount of time
what does the informed consent discuss
risks and benefits of the procedure
alternative treatment options
who must sign the informed consent
patient
provider performing the procedure
when is the pre-procedure time out performed
done prior to the exam beginning
what is confirmed with the pre-procedure time out
the correct patient
the correct procedure
the correct site (lumbar, extremity)
who must agree to the time out before the procedure can begin
everyone in the room
where is the specific time the time out was performed documented?
documented on the computer with a specific time
what is a myelogram
a radiographic study of the CNS structures situated within the vertebral column
performed by introducing a non-ionic, water-soluble contrast medium into the subarachnoid space by spinal puncture
what are examples of why a myelogram would be performed
identifying CSF leaks
surgical planning
spinal tumors
cord swelling
herniated disks
narrowing of the canal due to spinal stenosis
what are the contraindication for a myelogram
blood in the CSF
arachnoiditis
increases intracranial pressure
recent lumbar puncture
what contrast is used for lumbar myelograms
isovue M 200
what contrast is used for cervical myelograms
isovue M 300
how many times must contrast be checked before it is able to be administered
3
how many people must check the contrast before it is able to be administered
2
what are radiographers expected to know about contrast
safe dosage
safe route (location) of administration
limitations of the drug
side effects
potential adverse and toxic reactions
indications
dont forget contrast media is considered a drug/medication
how should the radiographer prepare the examination room prior to a myelogram
using aseptic technique on table and equipment
place the padded shoulder supports and footboard on the table
why is the table tilted during a myelogram
facilitate positioning so the contrast medium will go to the desired region
what is the proper patient dress for a myelogram
in a gown with the back fully exposed
what are the procedure steps for a myelogram
get all necessary pre-procedure paperwork done and have pt in a comfortable prone position
the radiologist or PA will first fluoro to determine which level to access and mark the skin in that area
the radiologist or PA will perform chemical skin prep
a local anesthetic agent (lidocaine) is used to numb the skin prior to inserting spinal needle
radiographer (or student) will need to move the fluoro tube as the needle is advanced into the subarachnoid space
the correct location in the subarachnoid space is confirmed by the presence of CSF backflowing unobstructed into the spinal needle
contrast is hand injected through the spinal canal
after the injection is completed, the spinal needle is fully removed from the pt
the radiologist will tilt the table and instruct the patient to rotate in various positions as needed
be prepared to assist the pt in anyway they need and remind them about the table tilting prior
the radiologist will save spot images as the contrast reaches the desired location as well as when the patient is in the correct position
once the radiologist is finished, a band aid will be placed over the puncture site
the patient is then log-rolled onto a cart and taken to CT for post myelogram images
when completing the contrast screening tool, what must be documented regarding contrast
the time that contrast was administered
the type of contrast administered
the location where the contrast was administered
what procedure could be needed if a patient develops a severe headache following a myelogram
a blood patch procedure
where does the blood needed for a blood patch procedure come from
the patients own blood
what is the purpose of having an epidural blood patch procedure
used to patch a dural tear that is leaking CSF after the initial myelogram
what is a lumbar puncture
a diagnostic and therapeutic procedure performed to collect a sample of CSF for laboratory testing
what unit of measurement are opening pressures record in
mmH2O
what could higher than normal levels of CSF be an indicator for
meningitis
idiopathic intracranial hypertension
what type of contrast is used for a lumbar puncture
there is no contrast used
what type of infections could a lumbar puncture help diagnose
bacterial infections
viral infections
fungal meningitis
what type of neurological conditions could a lumbar puncture help dianose
multiple sclerosis
Guillain-Barre syndrome
how many tubes are typically collected during a lumbar puncture
4
what must be present on each tube collected
patients name and DOB
time and date of collection
tubing sequence (1,2,3,4)
initials of the person who received the tube and specimen from the performing provider
what is an arthrogram
a minimally invasive radiographic examination of the joint following the injection of a contrast medium into the joint space
what does an arthrogram aid in detecting
damage in soft tissues like ligaments, cartilage, and tendons that arent visible with regular x-ray
what are the steps for performing an arthrogram
place the patient in a supine position on fluoro table
radiologist/PA will prep the area with a cleaning agent
radiologist/PA will fluoro to determine area to access
radiologist/PA will numb the area with lidocaine
radiologist/PA will place needle (20-22g) into joint
radiologist/PA will have tech/student fluoro for needle placement
once the needle is placed, a small amount of omnipaque 300 (or whichever radiopaque contrast is used) will be injected to verify correct placement
once contrast placement is confirmed, the MRI specific contrast will be injected into the joint space
after the injection is complete, the needle will be removed and a bandaid will be placed over the puncture site
the rad tech/student will then assist the pt in dressing, so that they do not move their joint space more than necessary before they are taken to MRI or CT
what is a joint aspiration
a procedure to remove fluid from the space around a joint using a needle and syringe
why is a joint aspiration performed
to relieve swelling
obtain fluid for analysis to diagnose a joint disorder or problem
where does fluid obtained from a joint aspiration go
sent to the lab for analysis
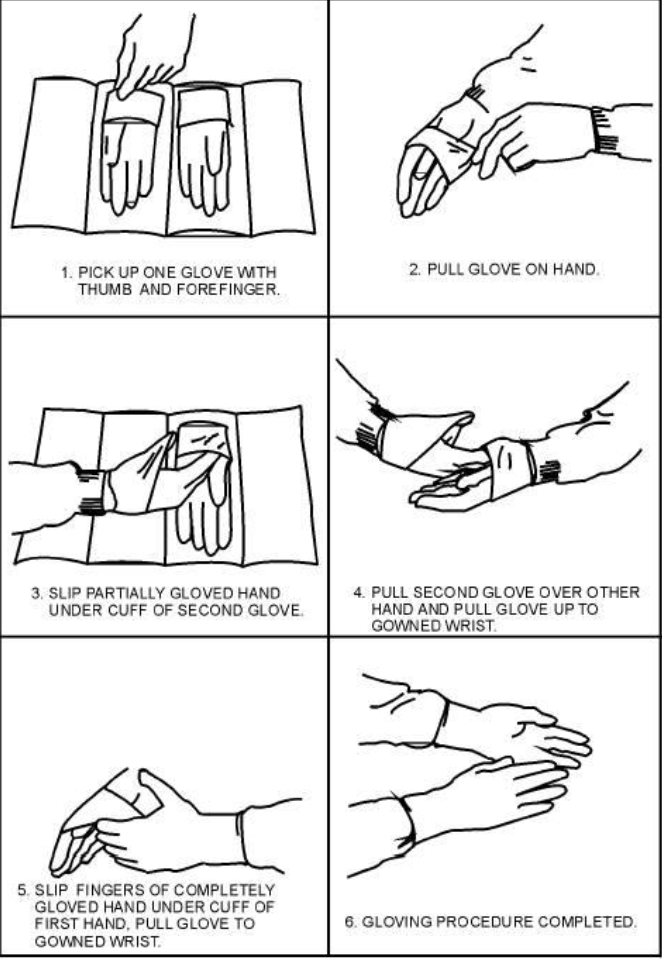
what gloving technique is demonstrated
open gloving technique
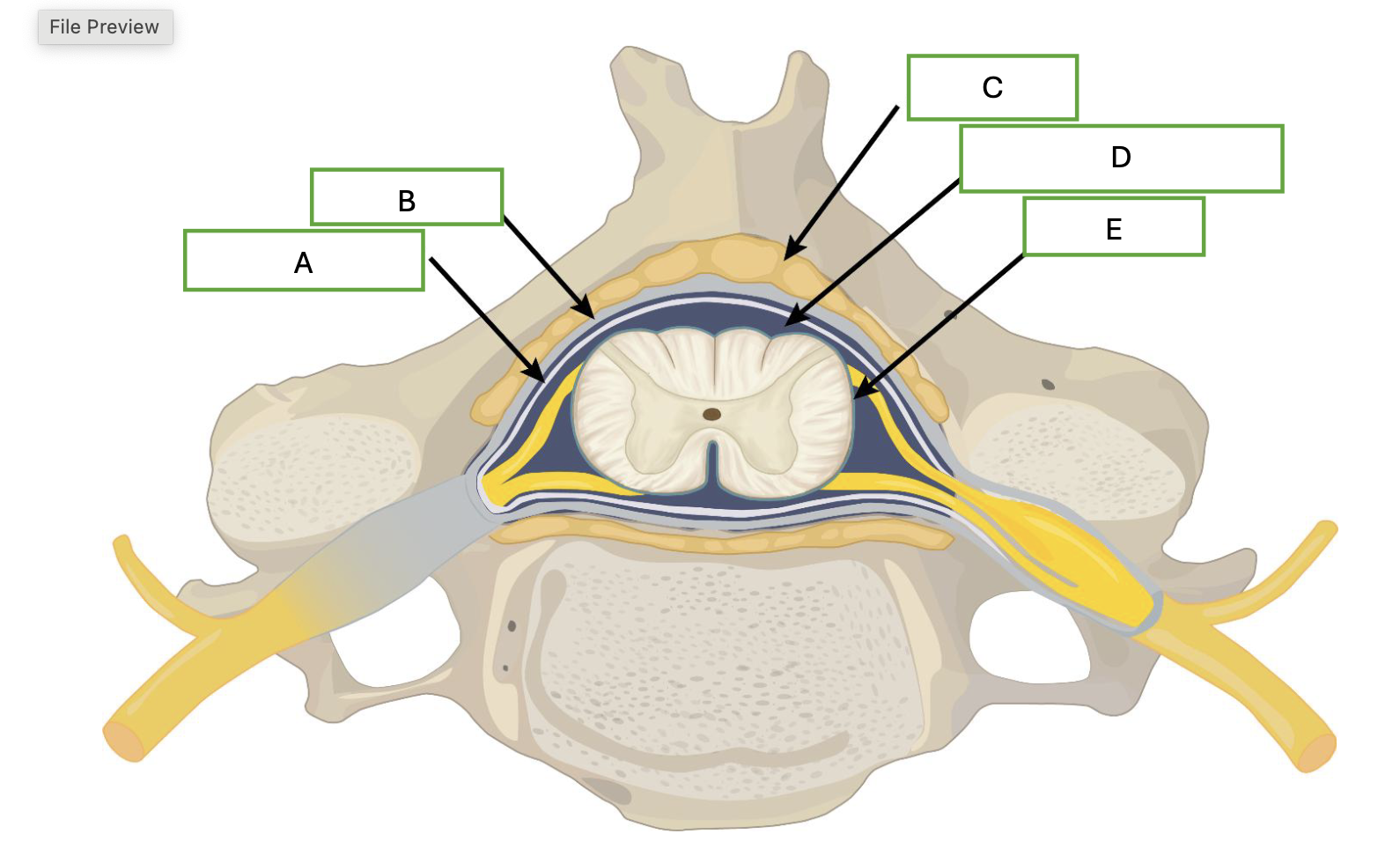
what is labeled by A
arachnoid mater
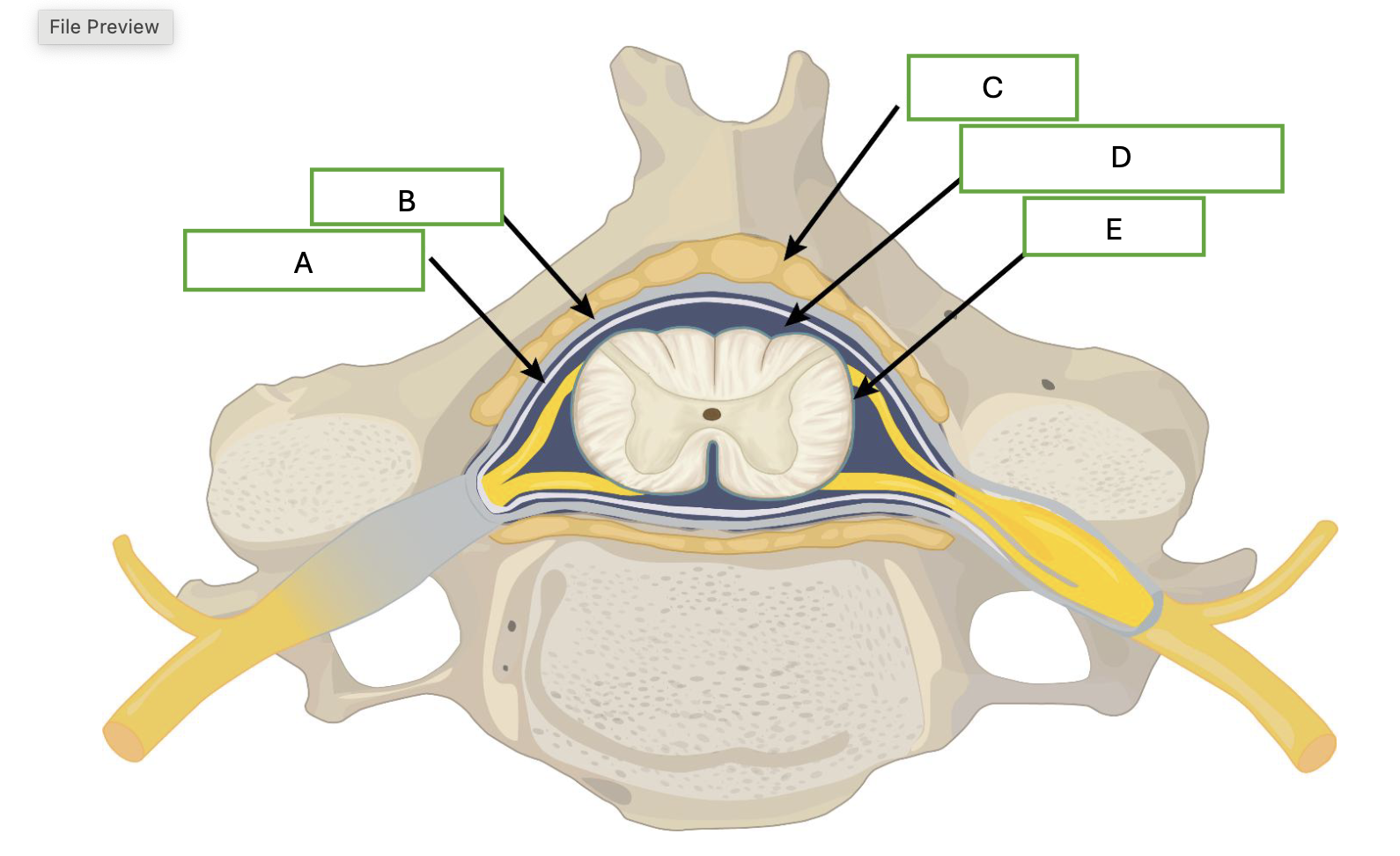
what is demonstrated by B
dura mater
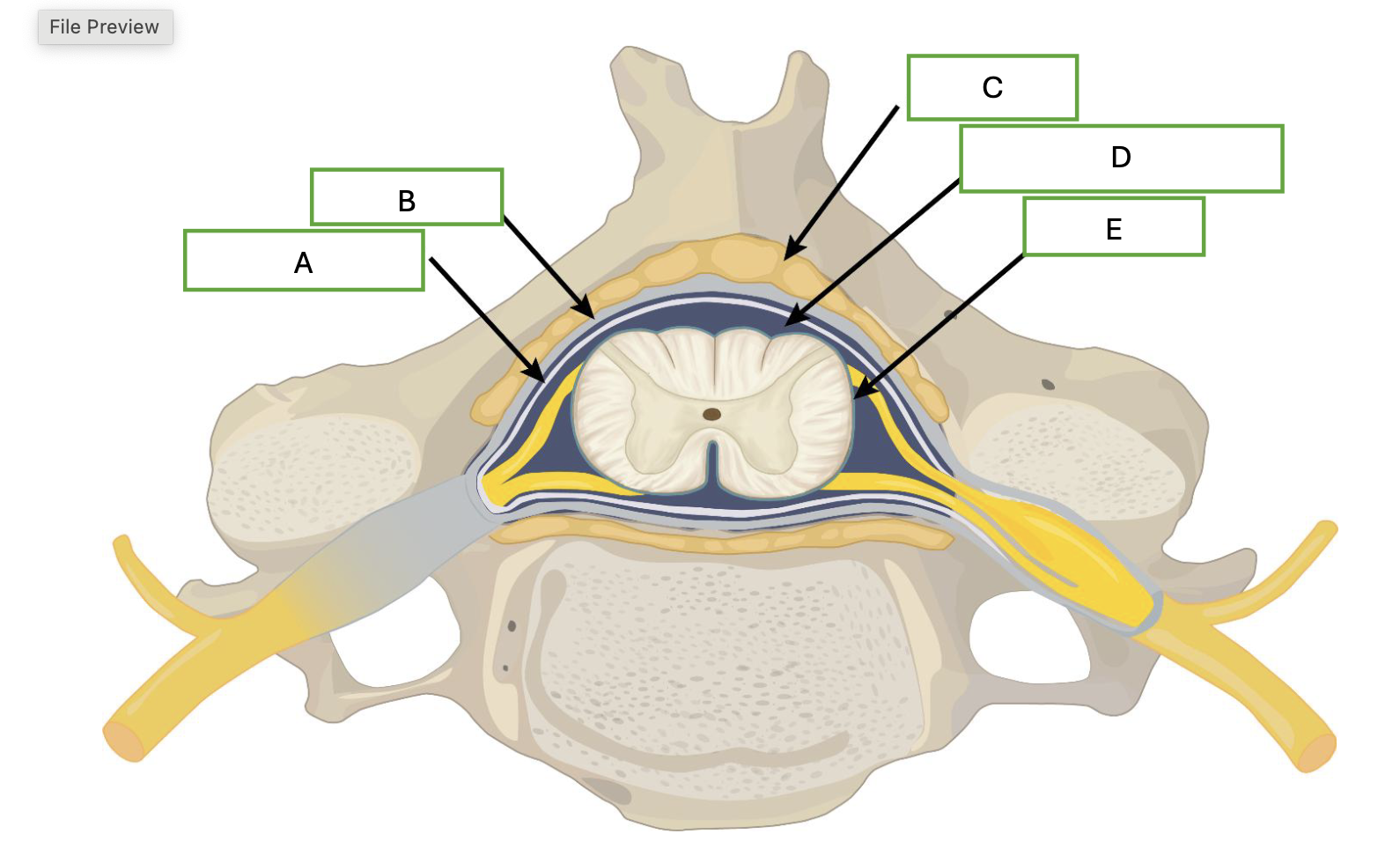
what is demonstrated by letter C
adipose
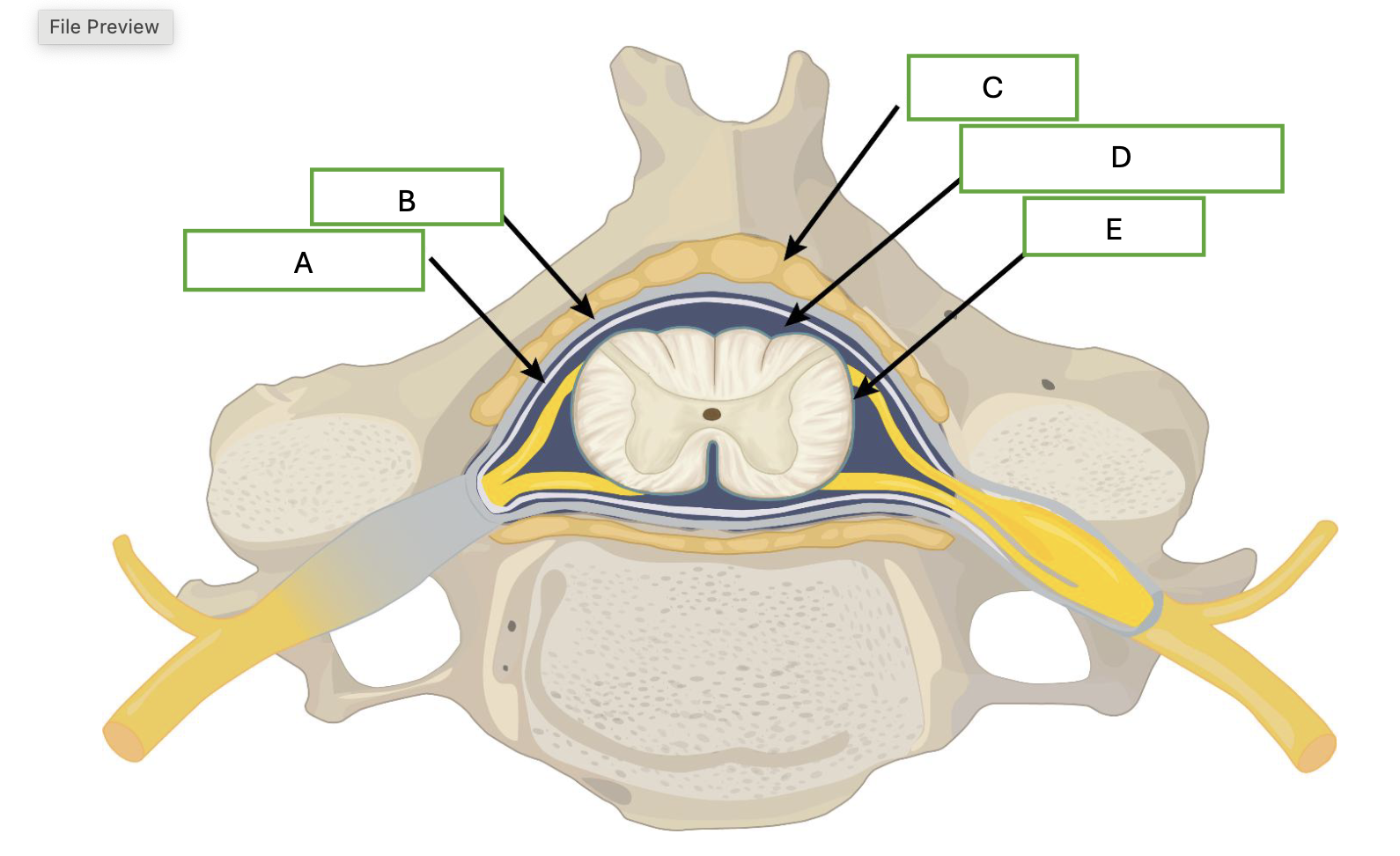
what is demonstrated by letter D
cerebral spinal fluid
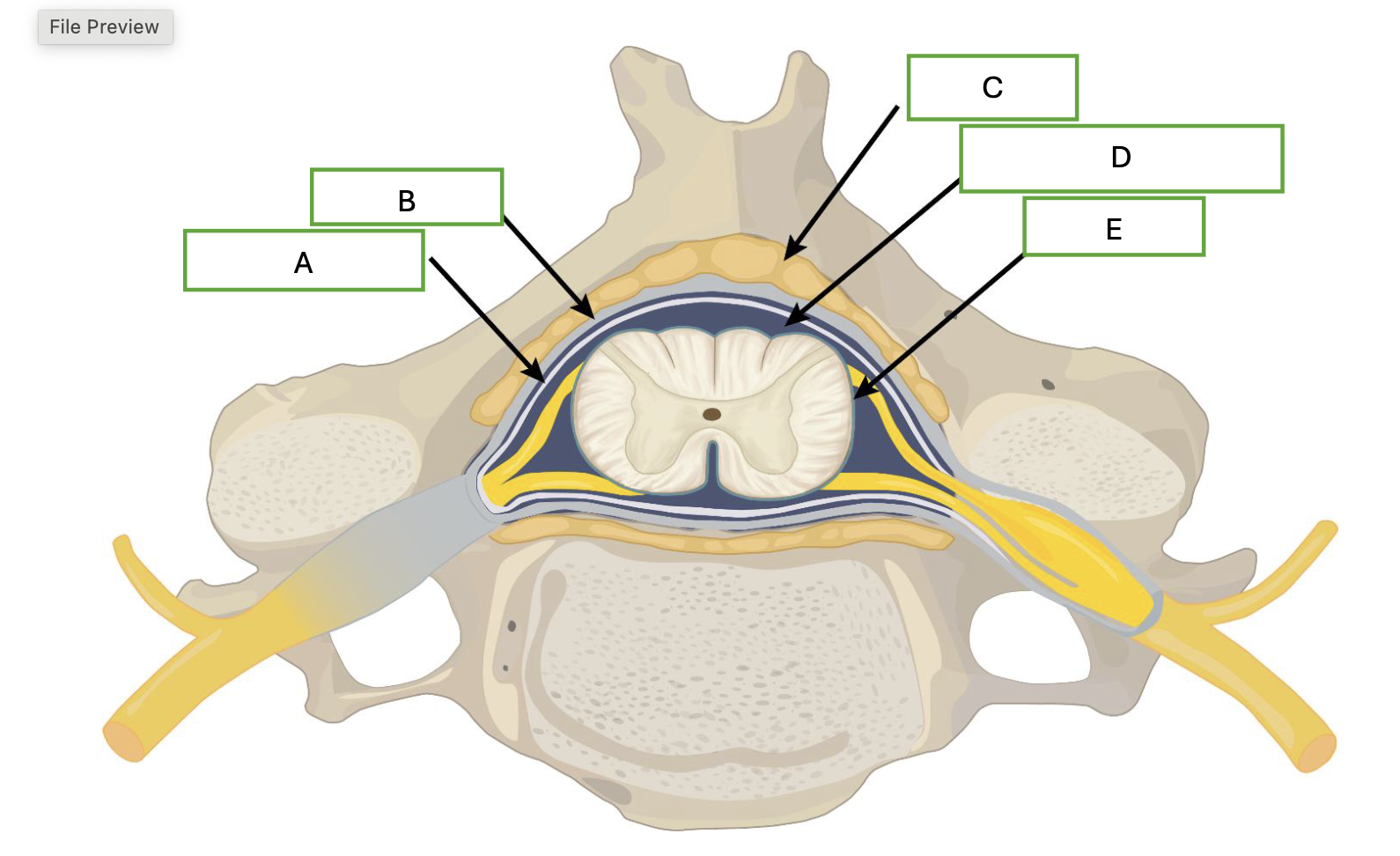
what is demonstrated by letter E
pia mater
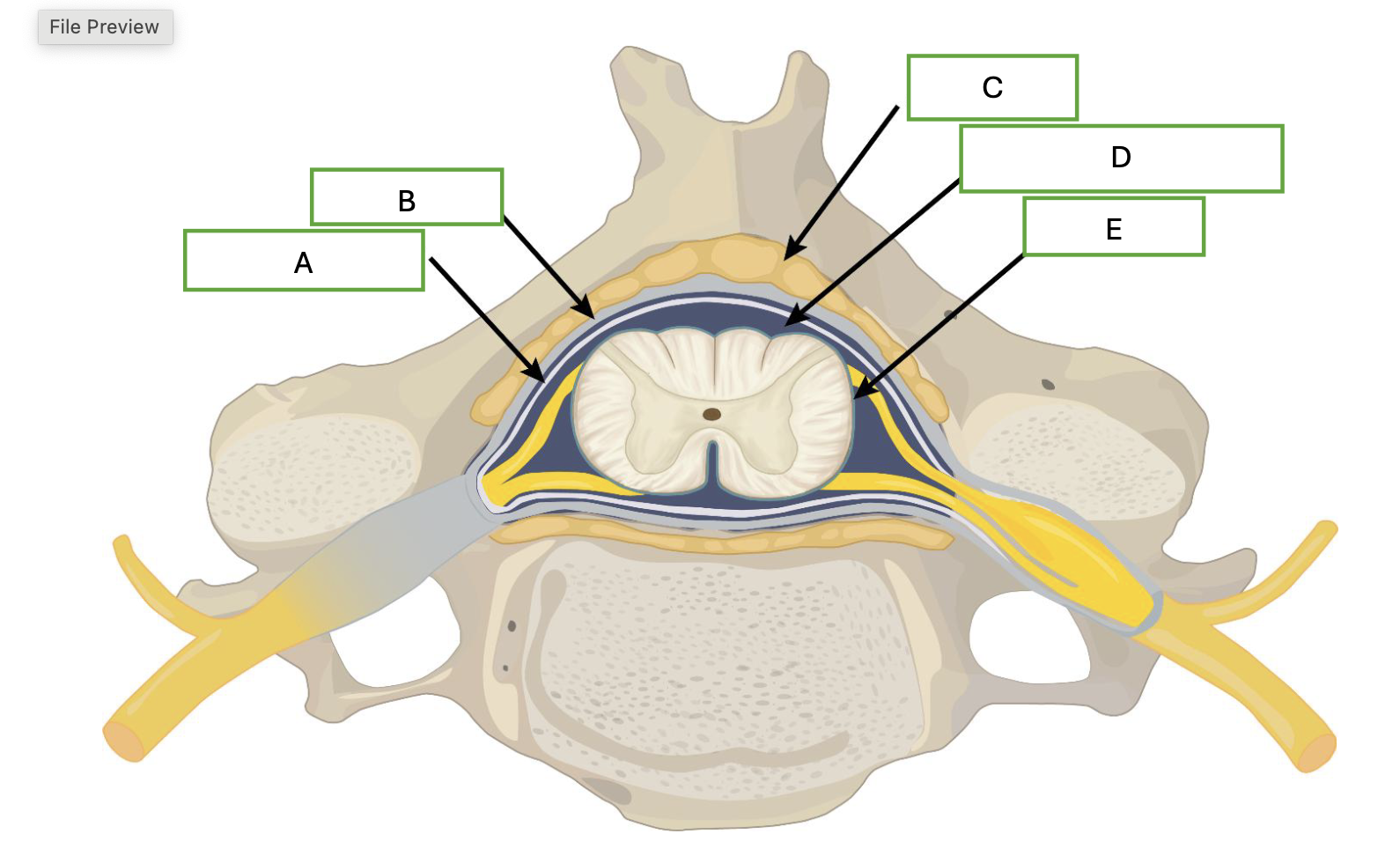
which letter represents the middle layer of the meninges
A
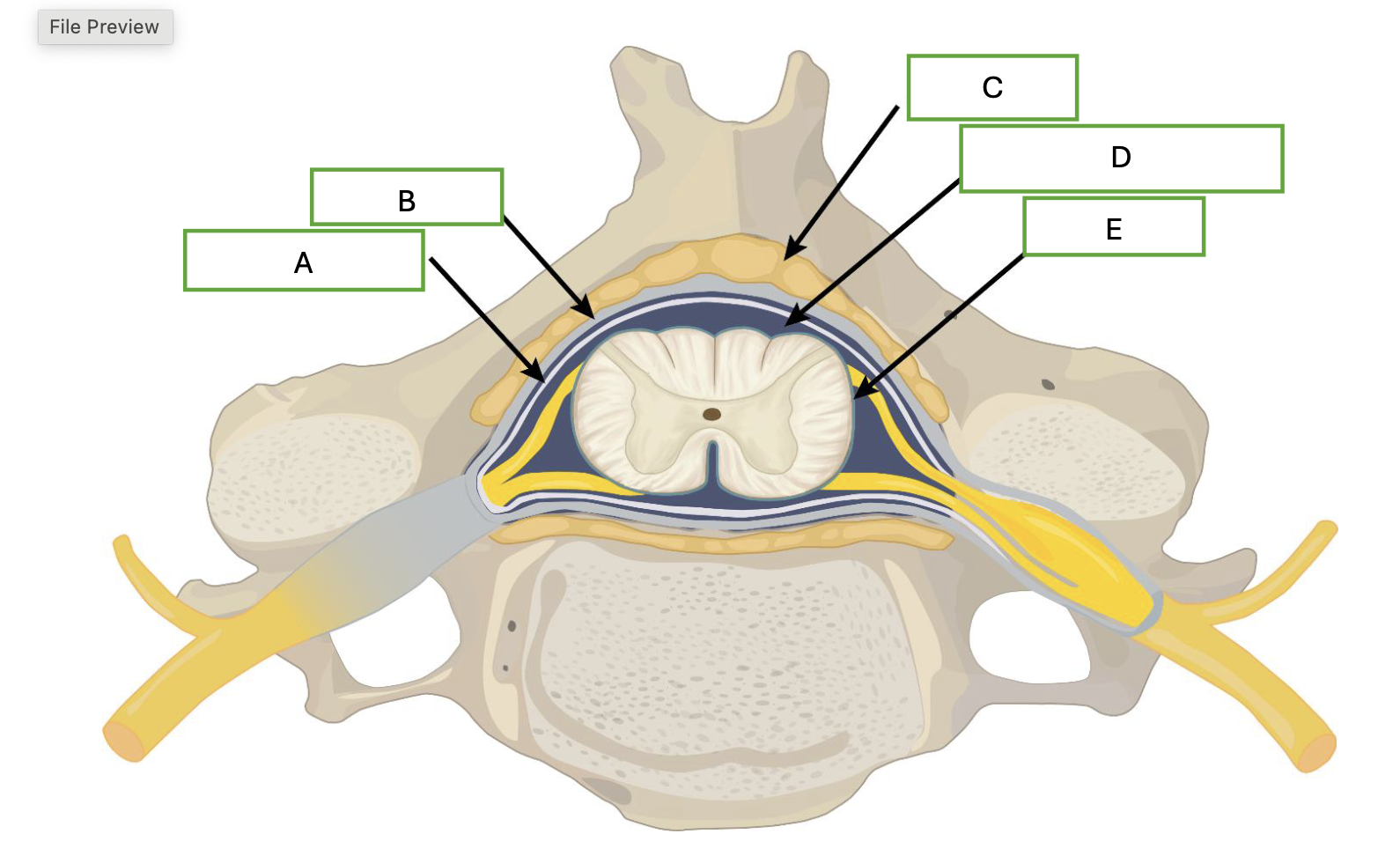
which letter represents the outer layer of the meninge
B
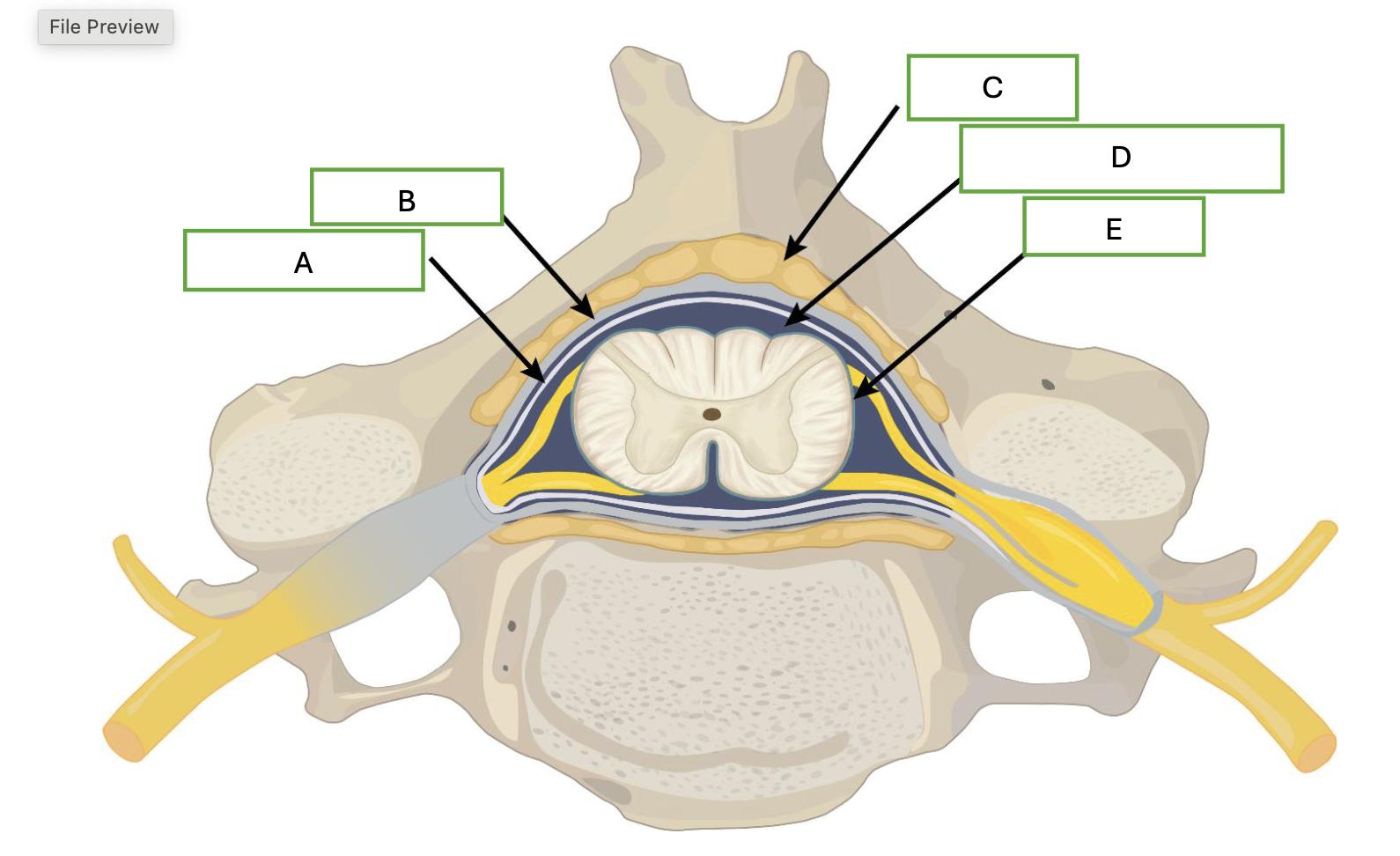
which letter represents where contrast would be injected for a myelogram
D
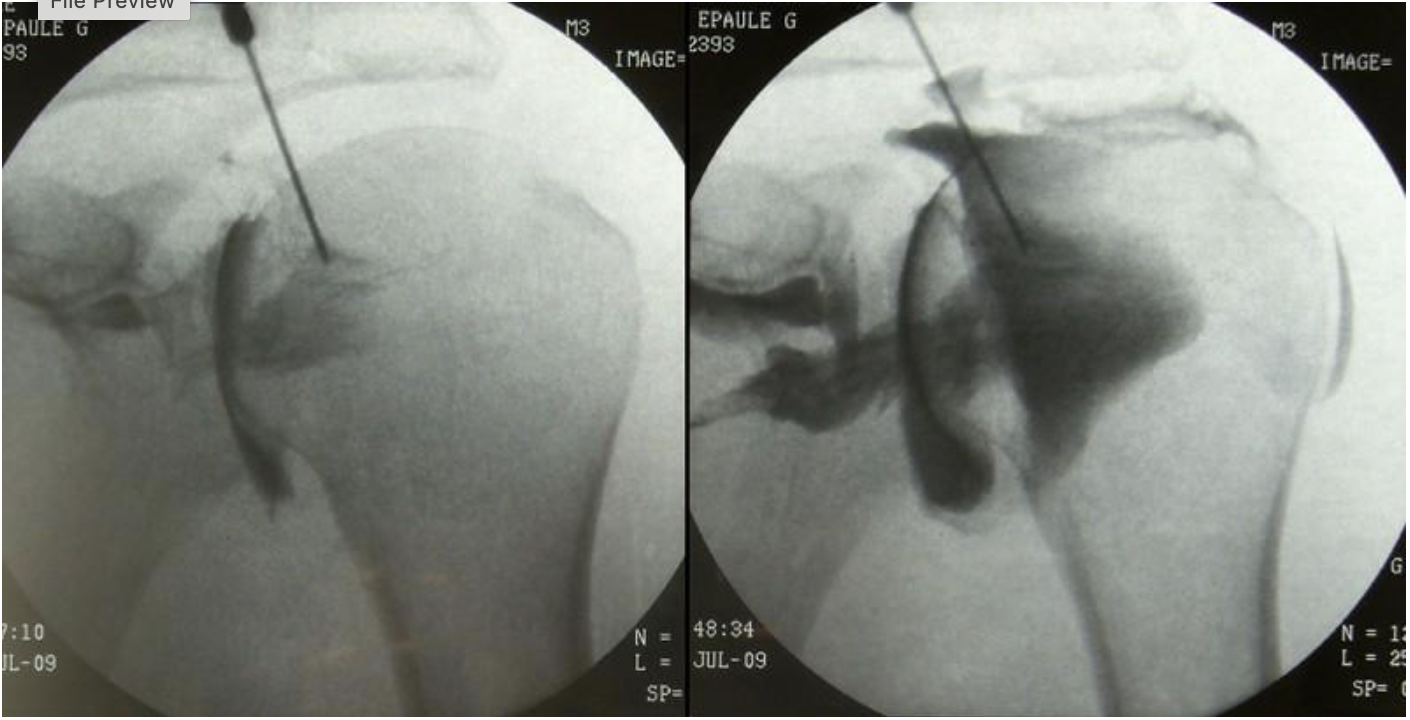
what procedure is being performed
arthrogram of shoulder
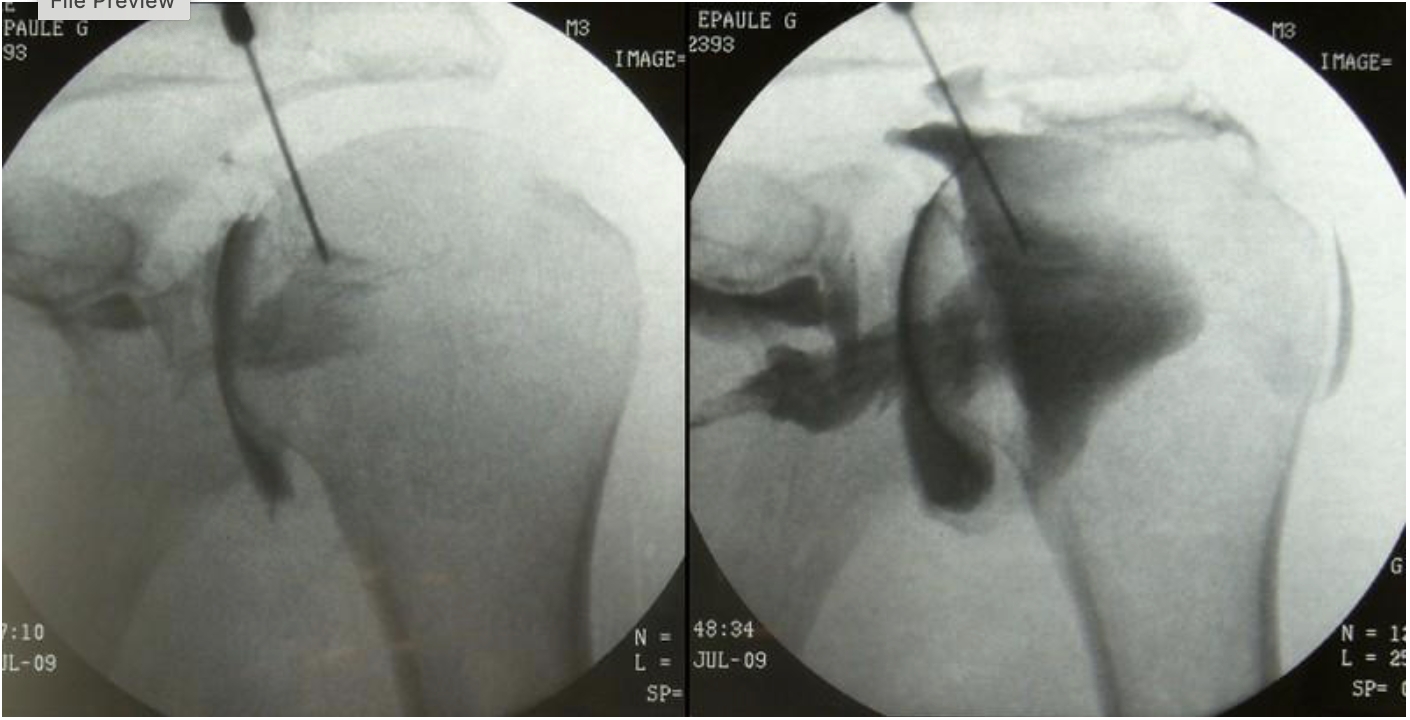
what substance is shown as black on this image
radiopaque contrast (omnipaque 300)
what modality will a patient typically go to after having this procedure performed
MRI or CT
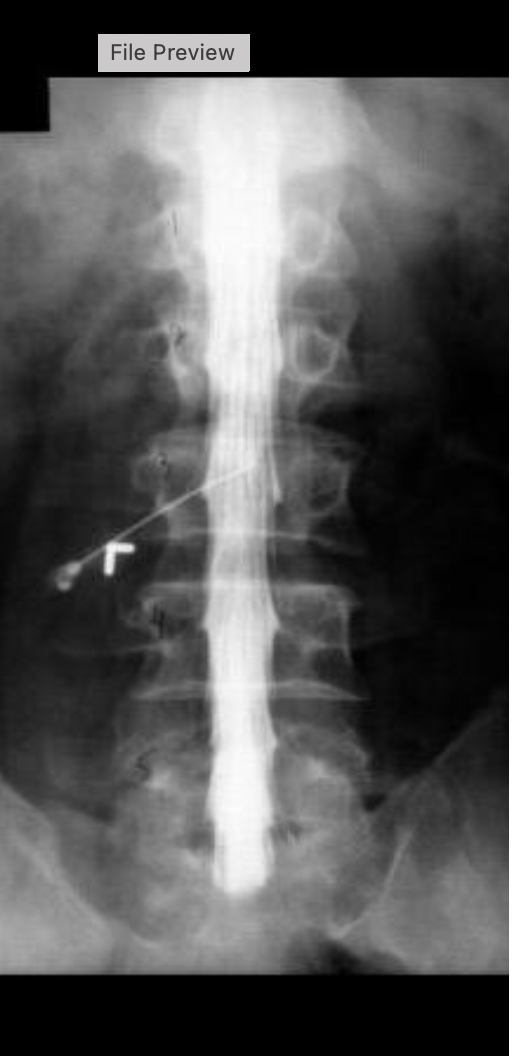
what procedure is being performed on this image
lumbar myelogram
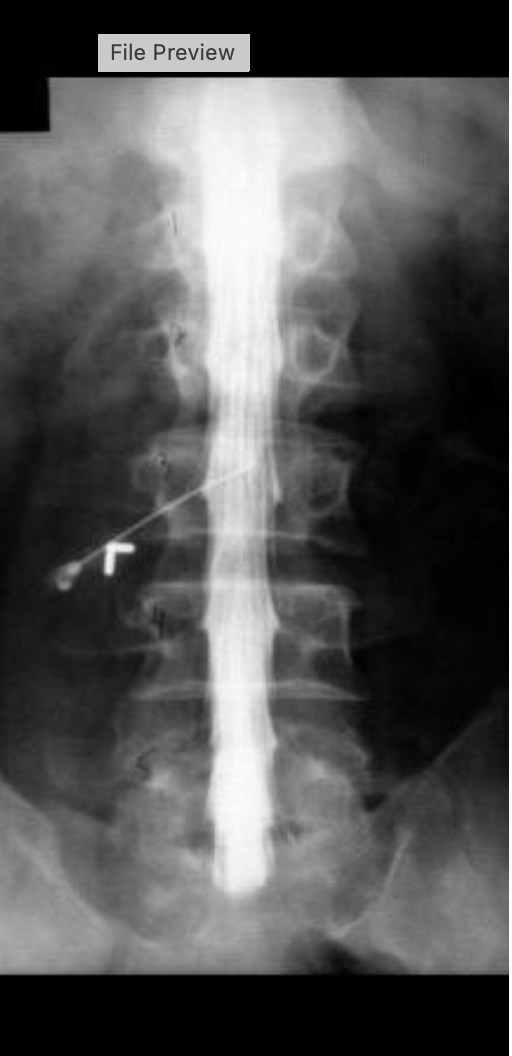
what level is the needle placed at for this procedure
L2/L3
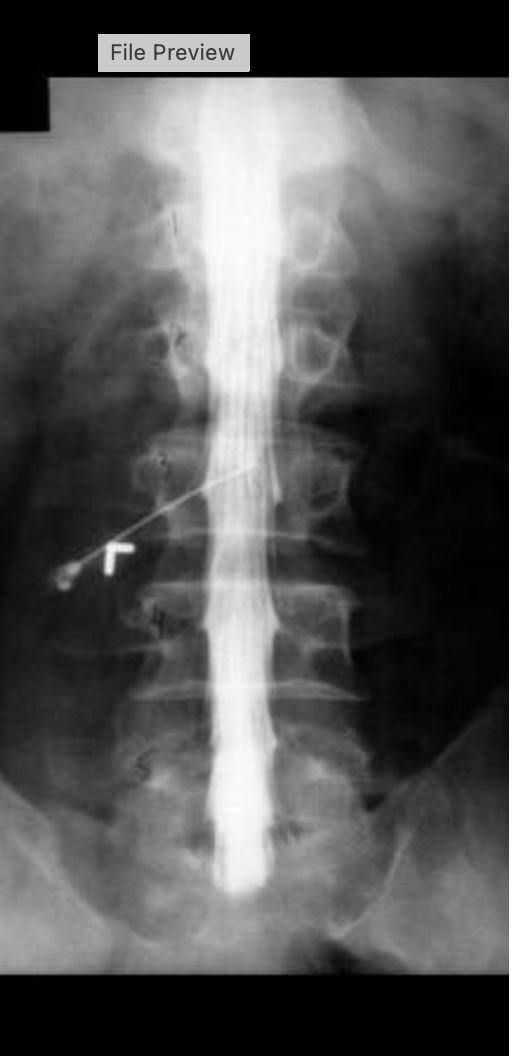
what contrast was used for this procedure
isovue M 200
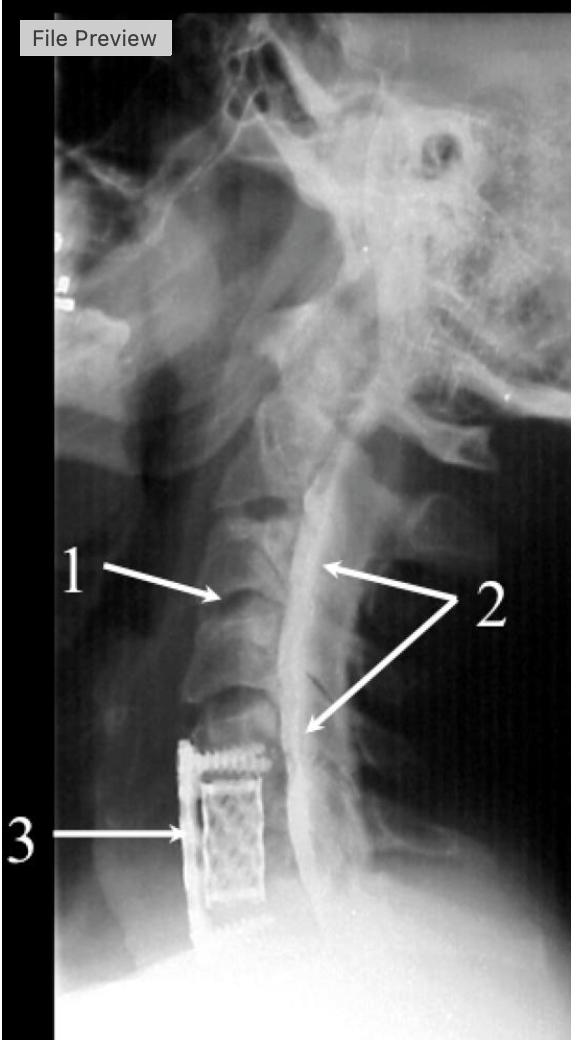
what procedure is being performed
cervical myelogram
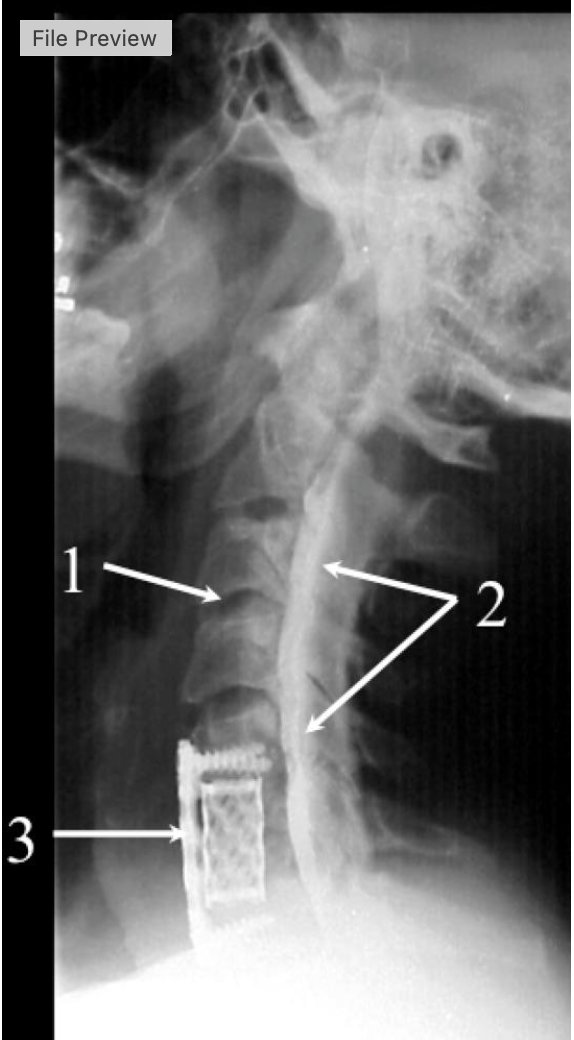
what intervertebrak disk space is at #1
C3-C4