image quality, radiologic interpretation, radiographic safety
1/70
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
71 Terms
define image quality
"It is that characteristic of an X-ray that describes as well as the shadows identified in the film reveal the anatomy and / or the pathology under investigation"
(how well the shadows of the xray reveal the anatomy/pathology)
the quality of the xray depends on what 4 factors?
-positioning
-exposure factors (mAs and kV)
-use of the Bucky/grid when necessary
-number of projections
a radiograph is possible because of the ability of __________
xrays to penetrate matter
what produces the blackening of a radiograph?
when the xrays pass through the patient unchanged (are not absorbed)
when xrays pass through the patient unchanged (are not absorbed), this appears what color on the radiograph?
black
some xrays are absorbed by the patient and some pass through unchanged, producing...
film blackening
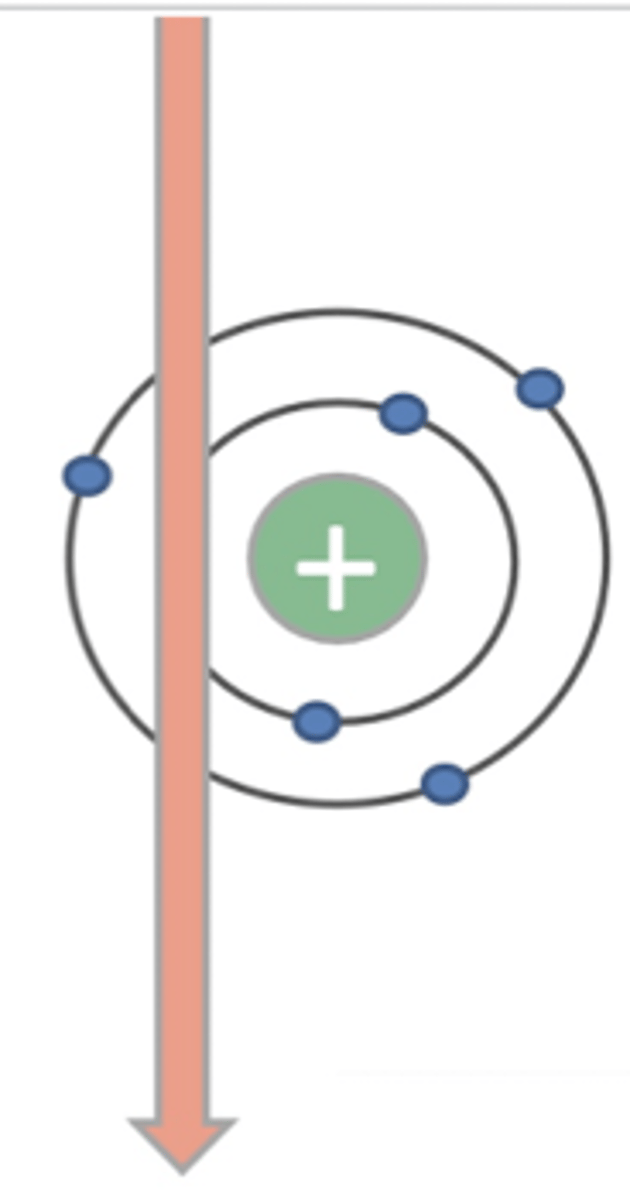
why do the lungs appear black on a radiograph?
because the lungs are mostly air, so there is not much matter for the xrays to interact with
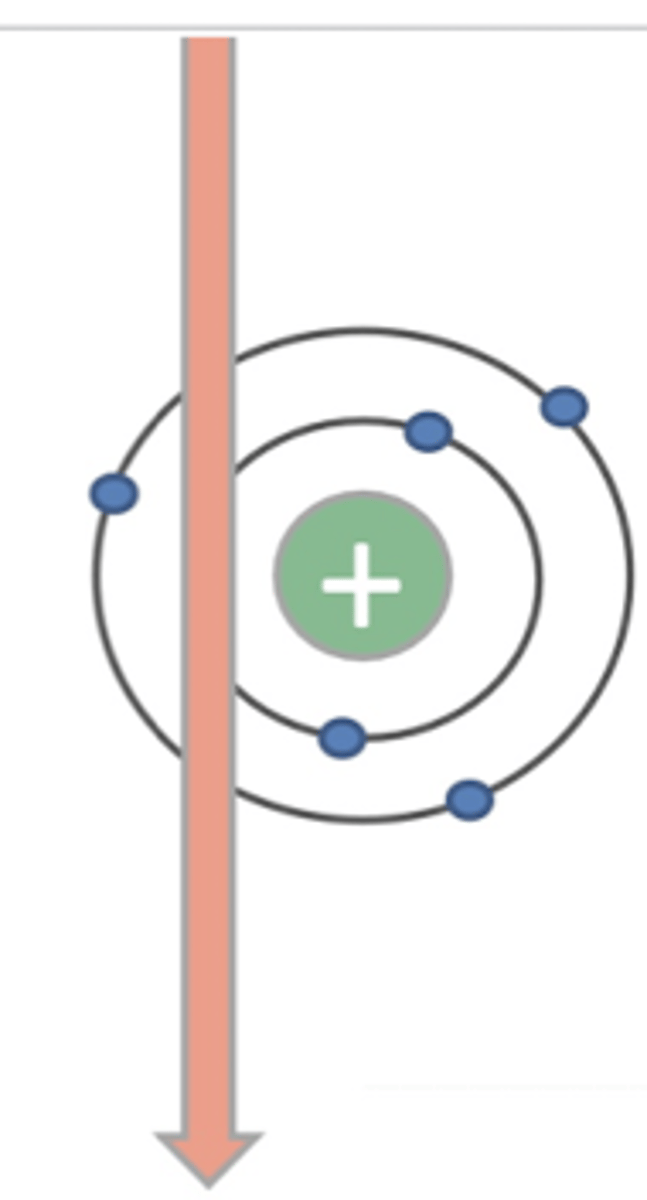
what is the photoelectric effect?
when the xray interacts with an electron, the electron gets ejected out of the atom so there is no energy left. this produces a white image.
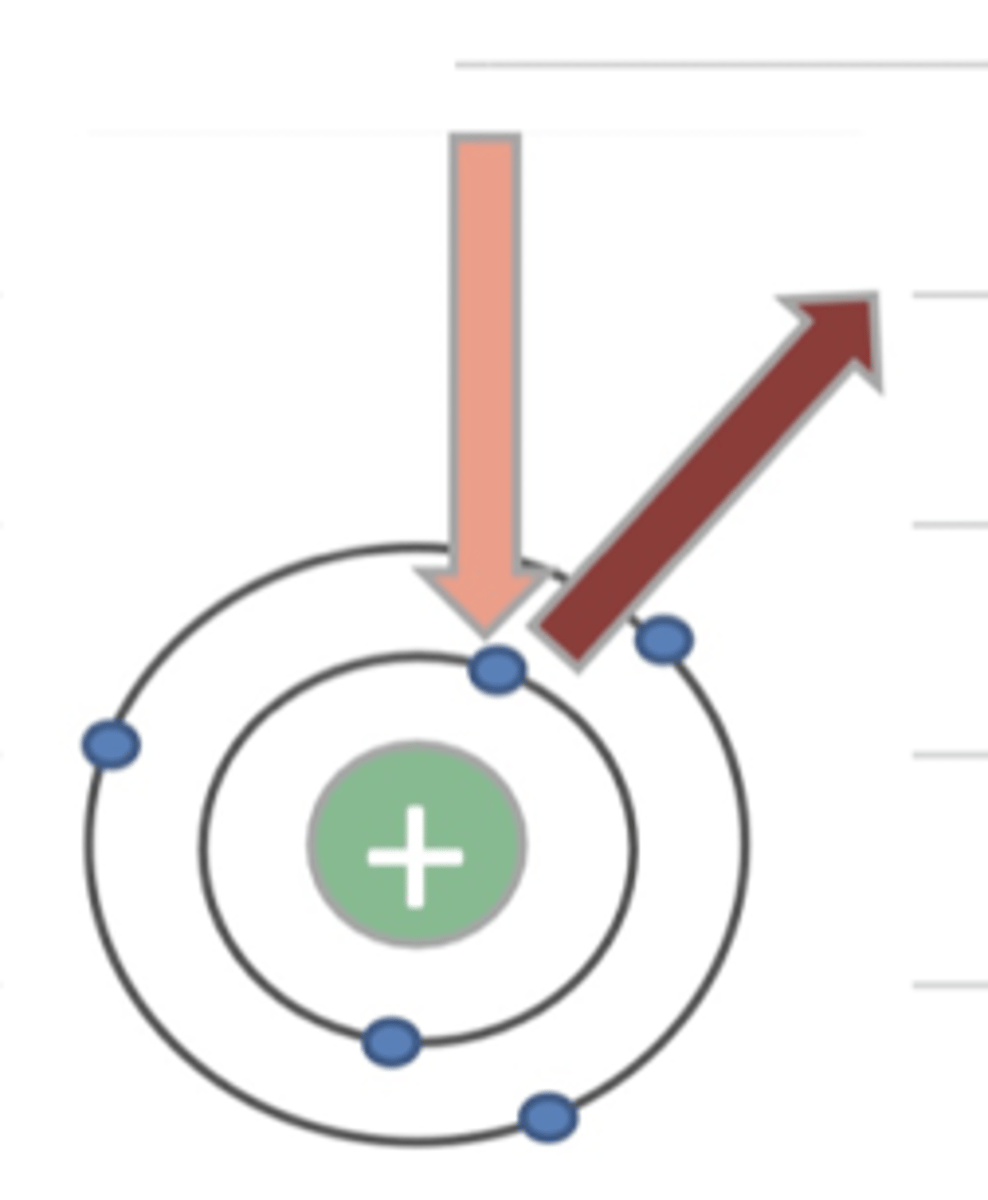
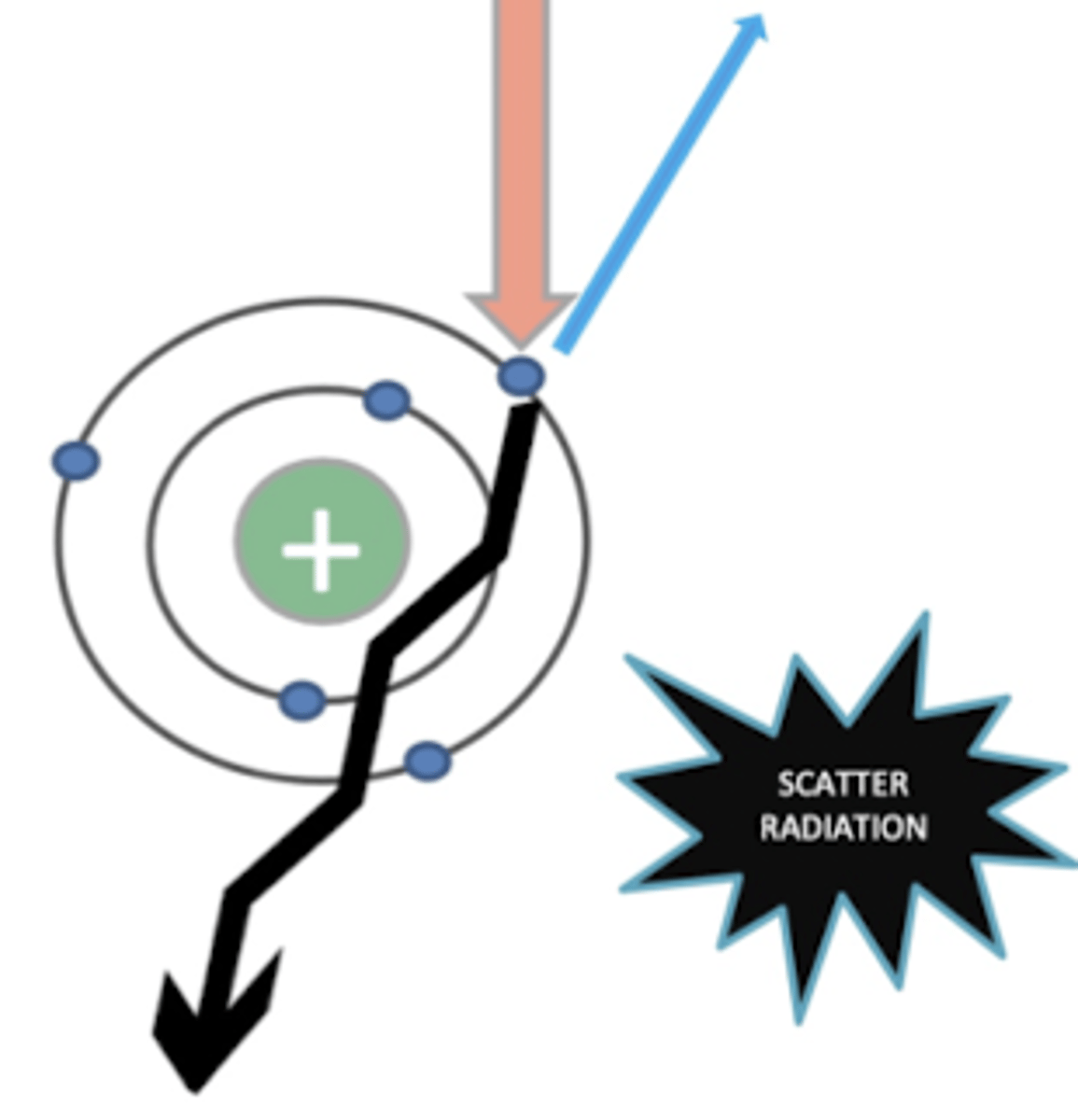
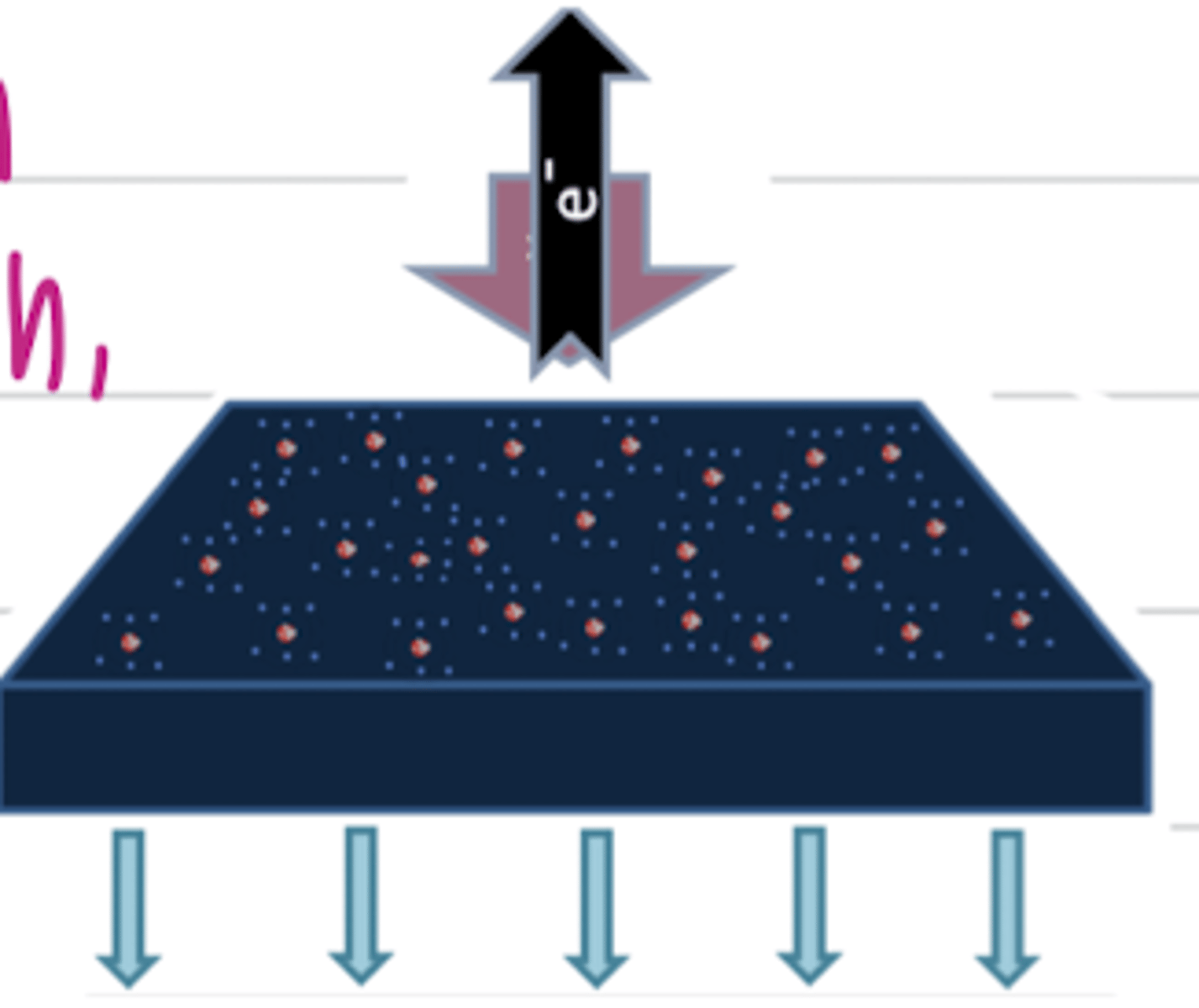
what is "compton scattering"?
it is an interaction between the xray and an outer layer electron of an atom, making the xray to not go straight. this produces a blurry image.
WE DO NOT WANT THIS
what does "radiopaque" mean?
the tissue is dense, so the xrays are absorbed more by the atoms. the image appears white.
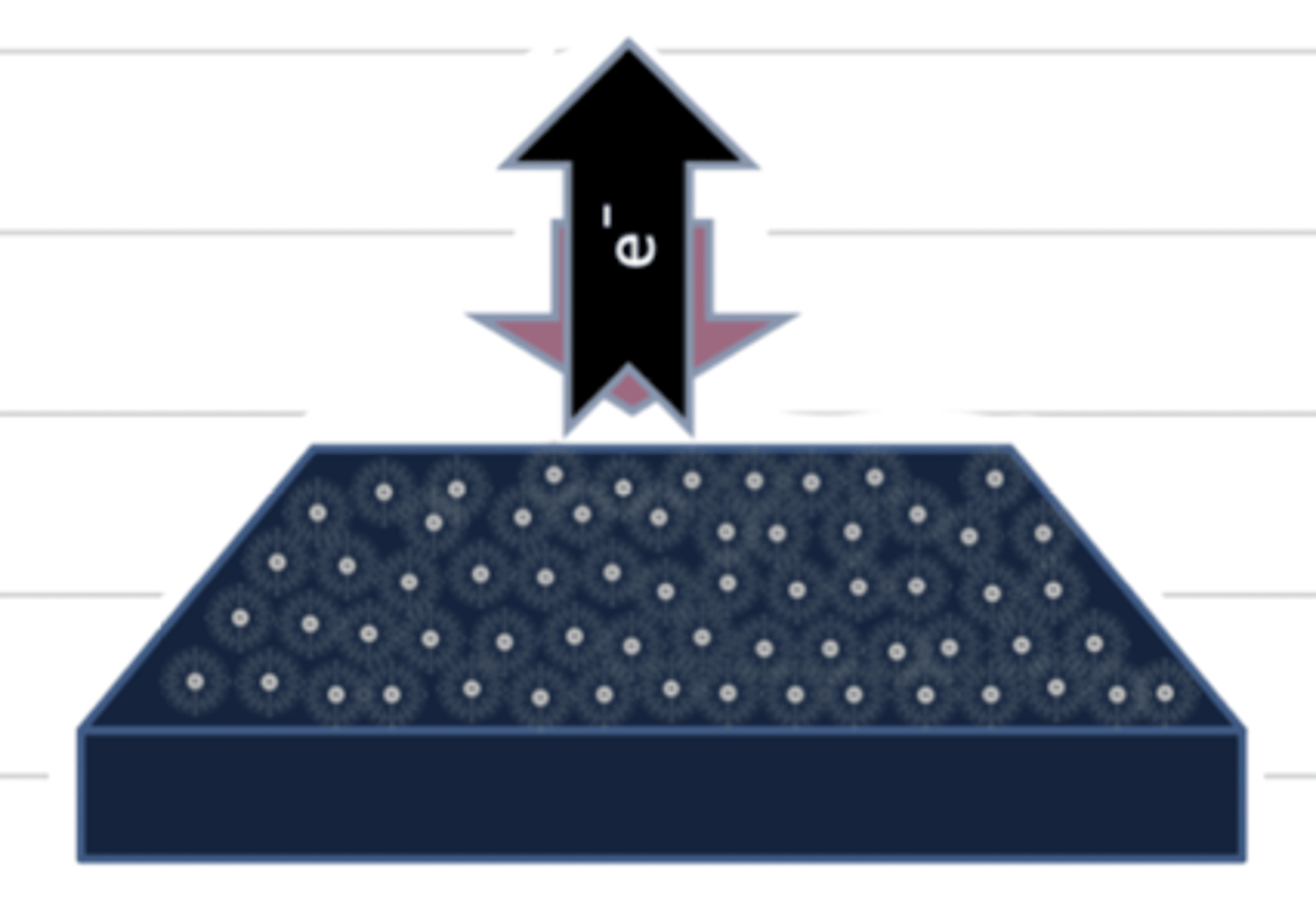
a tissue that is radioopaque appears what color?
white
the word for a low density tissue is...
radioluscent
what does radioluscent mean?
the tissue is low density, so the xrays pass through. these tissues appear black
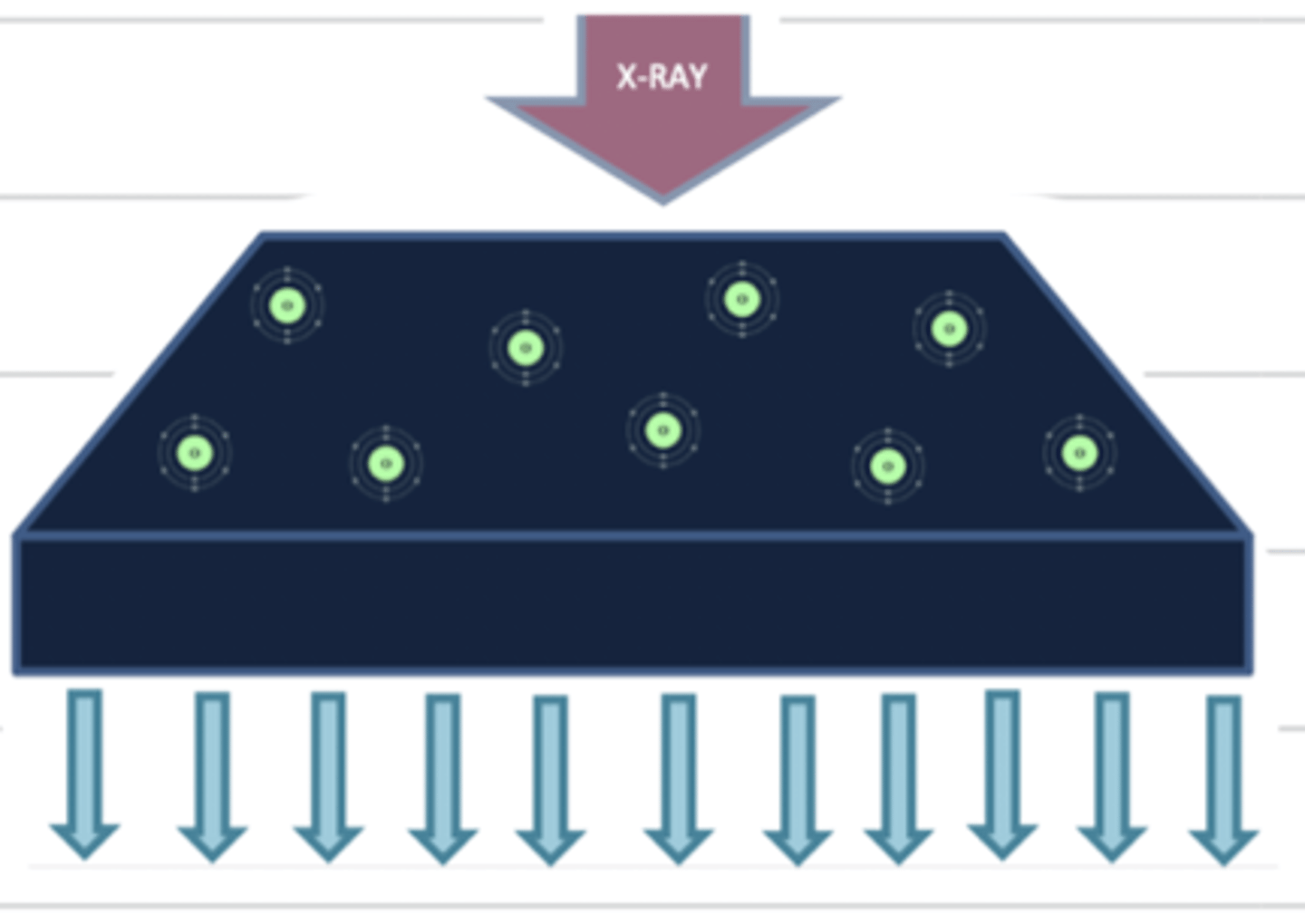
when there is a medium amount of atoms in a tissue, the xray in this area will appear what color? why?
grey, because some xrays will pass through, and some will interact with atoms.
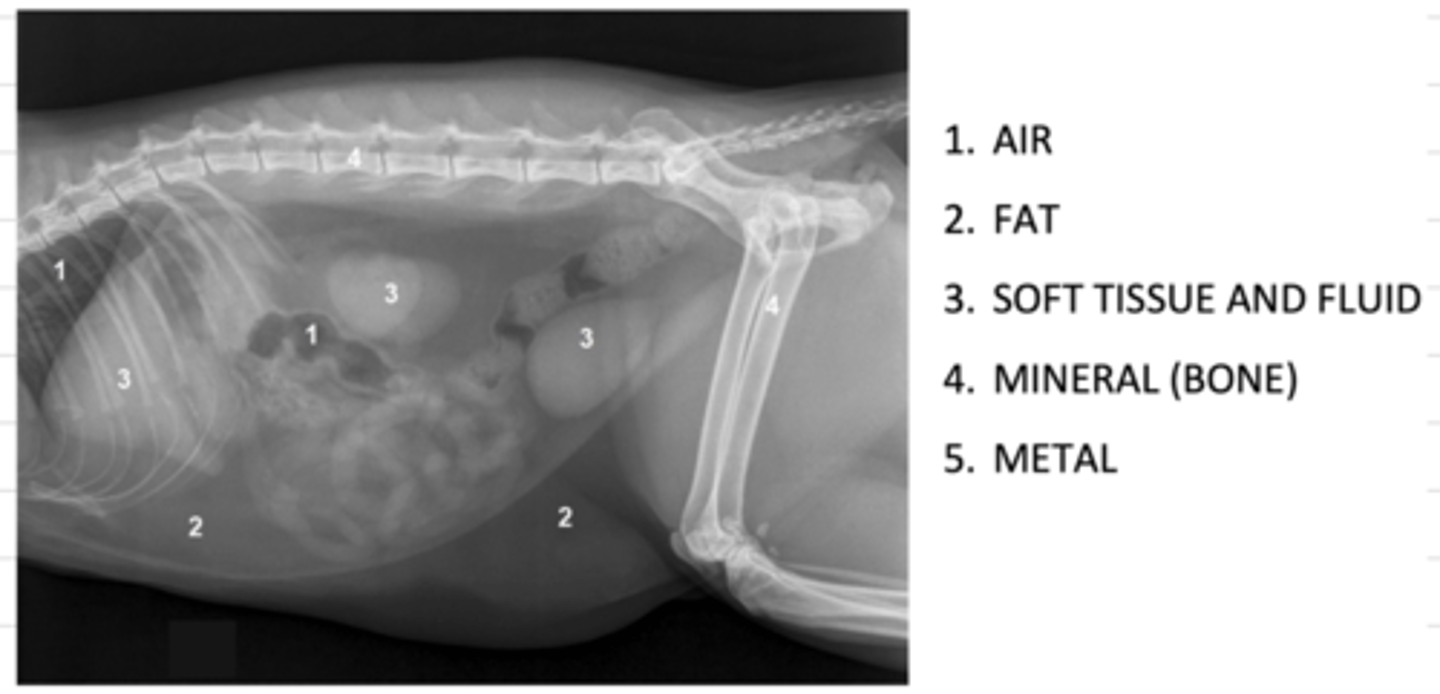
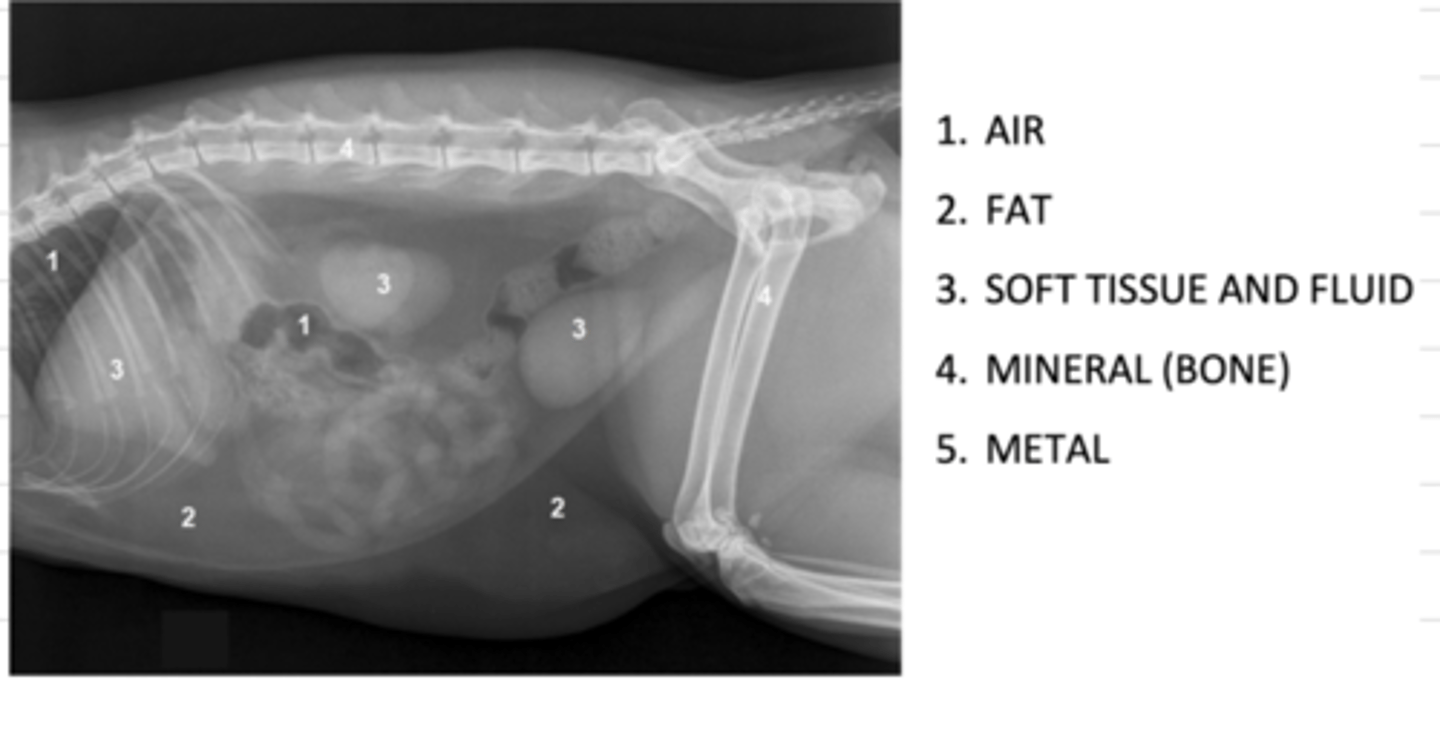
what are the 5 opacities of a radiograph, from most radioluscent to most radiopaque?
1. air
2. fat
3. soft tissue and fluid
4. mineral (bone)
5. metal
radiographic contrast is....
the difference in the film between 2 opacities.
this depends on the patient, the kV, and the scatter radiation.
in a very skinny patient, to achieve a good radiographic contrast, must we use a high or low voltage (kV)?
we should use a low kV, because there is not much tissue for the xrays to pass through.
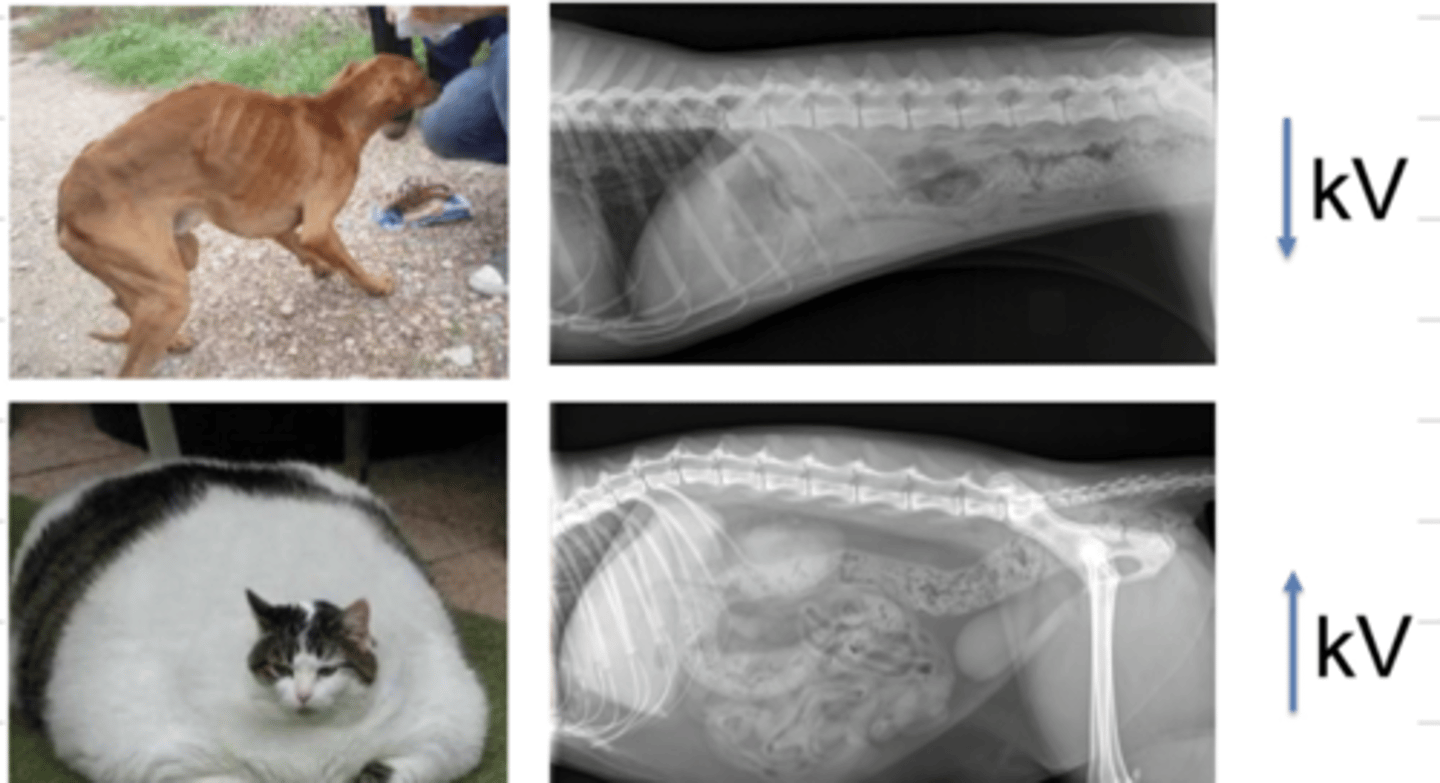
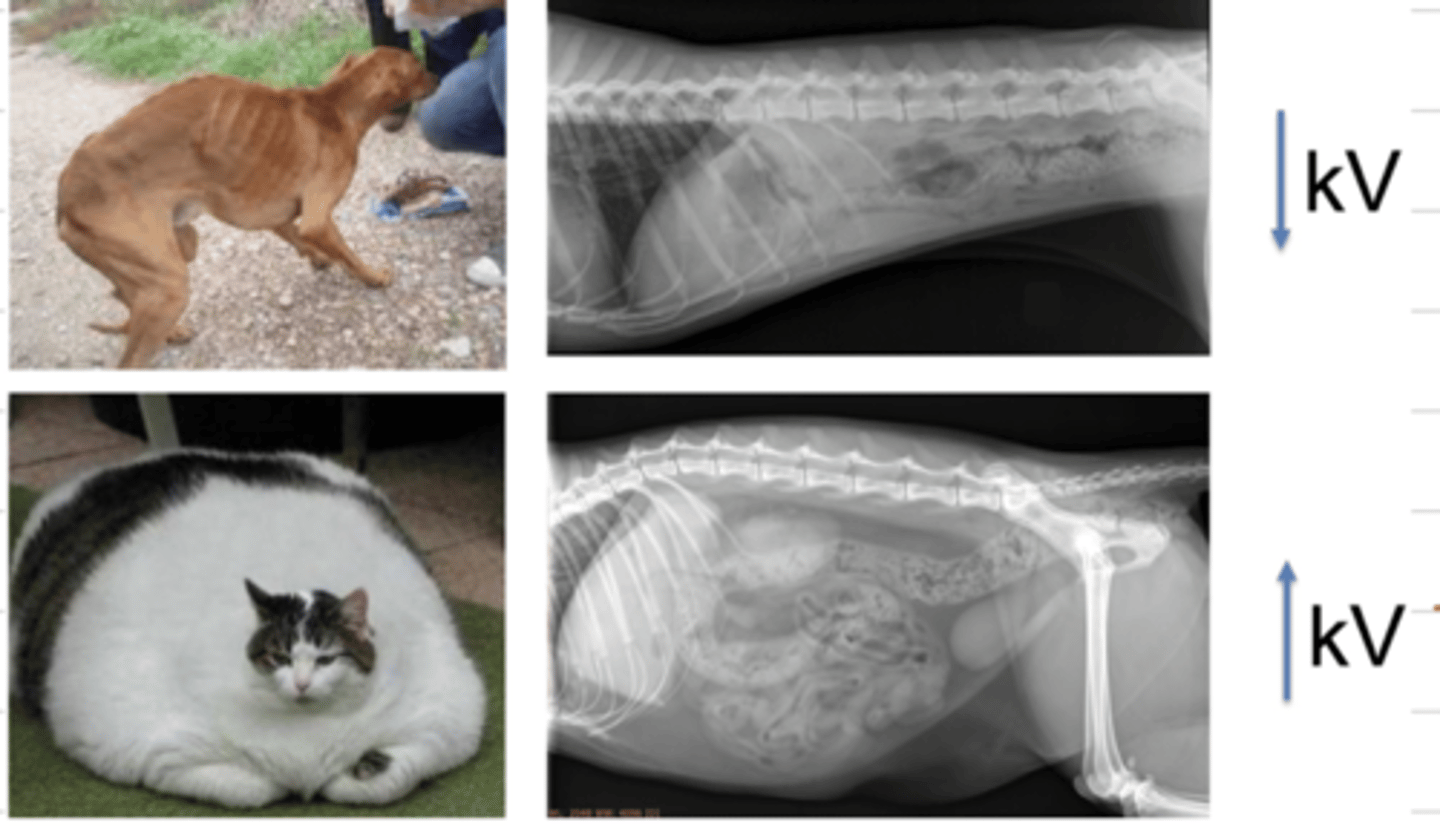
in an overweight patient, to achieve a good radiographic contrast, must we use a high or low voltage (kV)?
we should use a high kV, because there is more tissue that the xrays need to pass through
what is mAs?
# of xrays
what is kV?
voltage (energy)
what is the kilovoltage peak?
the maximum voltage that is applied across an xray tube to produce the xrays
if we use a kV that is too high, we produce what type of film?
a dark film, because of overexposure. when we increase the kV, the xrays have so much energy that even when interacting with atoms, they will still pass through/
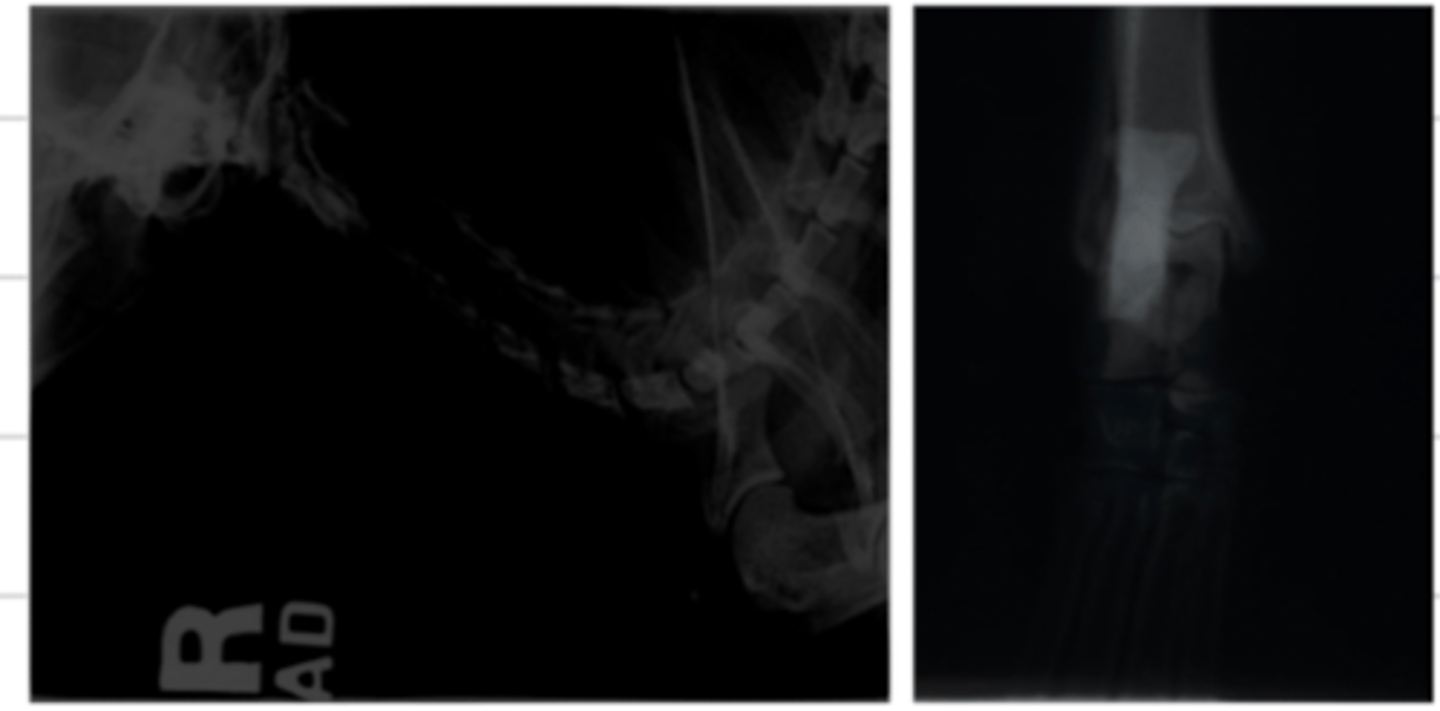
what does "underexposure" mean?
when we use a kV that is too low, it will cause a bright film.
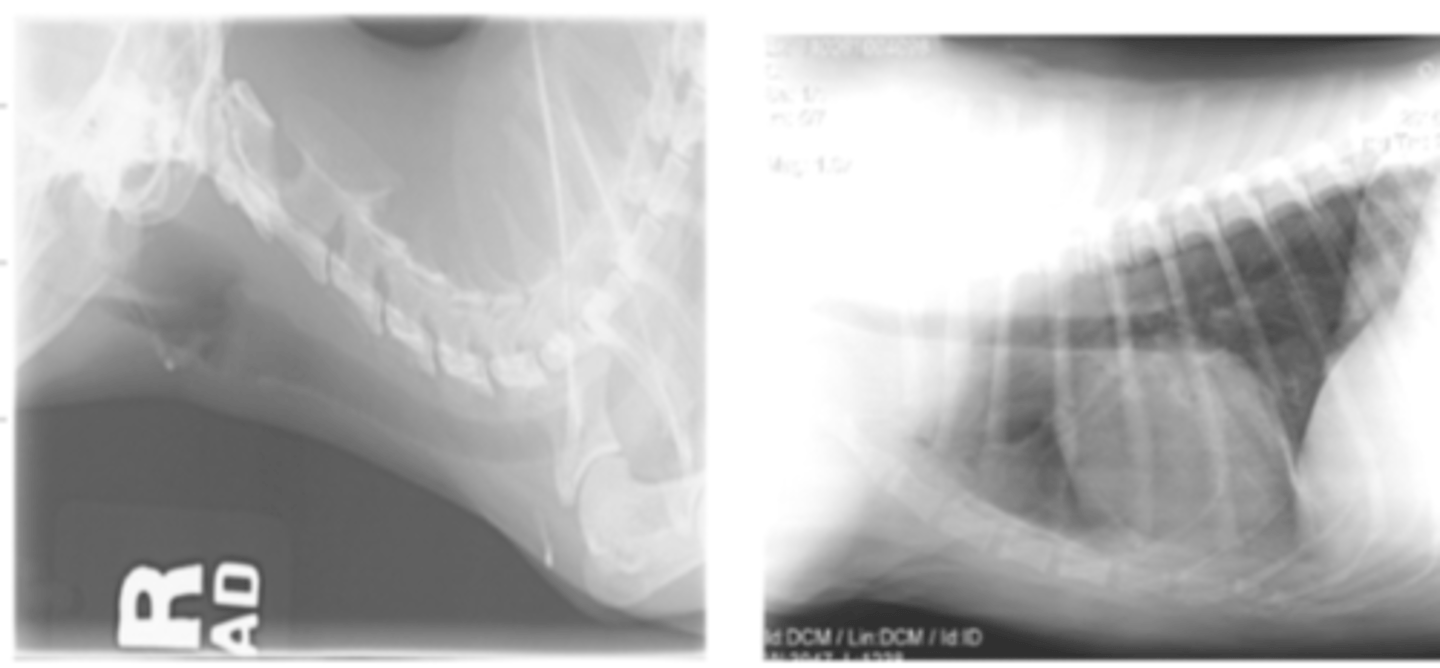
if we use a kV that is too low, what is the result?
a bright film, because of underexposure. when we decrease the kV, the xrays are not energetic enough to pass through tissues
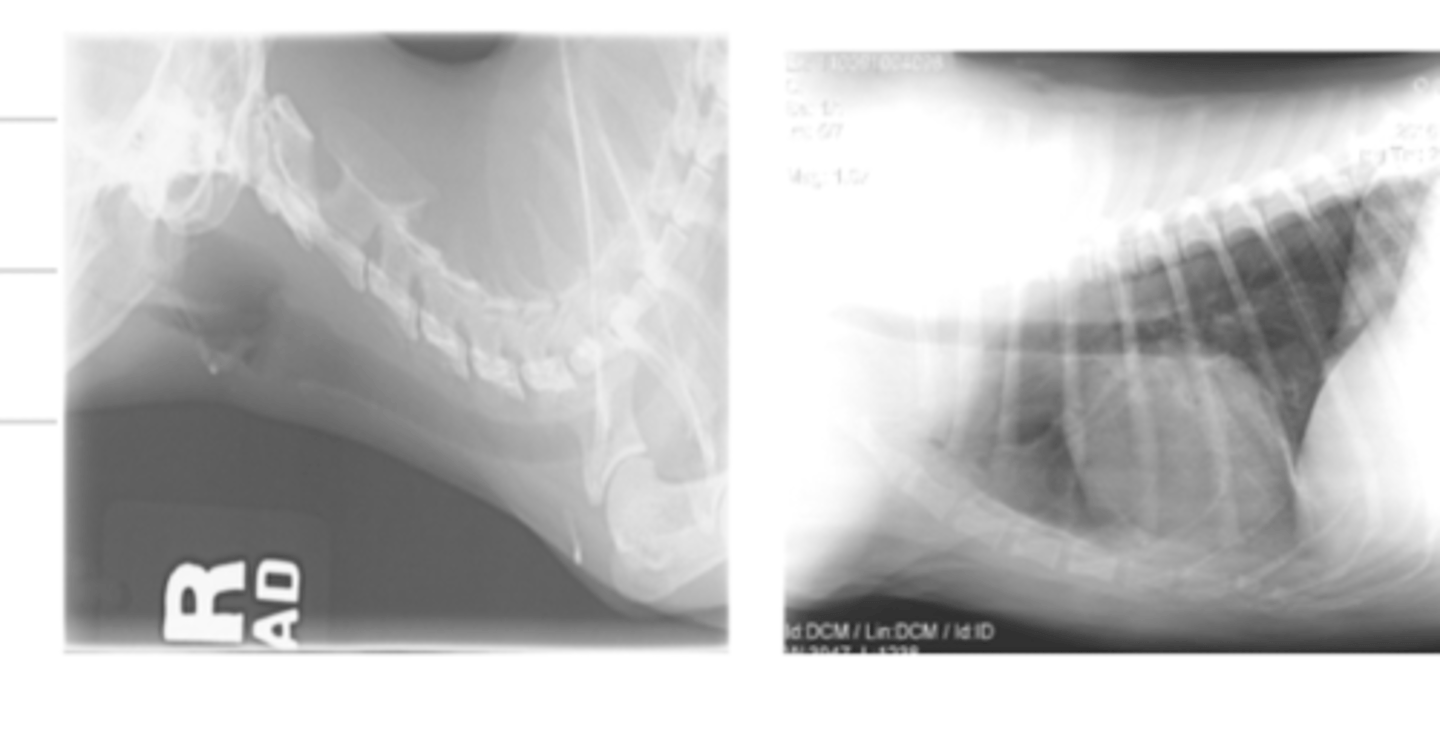
in what circumstances (to view what structures) do we prefer to have a high contrast?
bones
to visualize bones, do we want a high or low contrast?
high
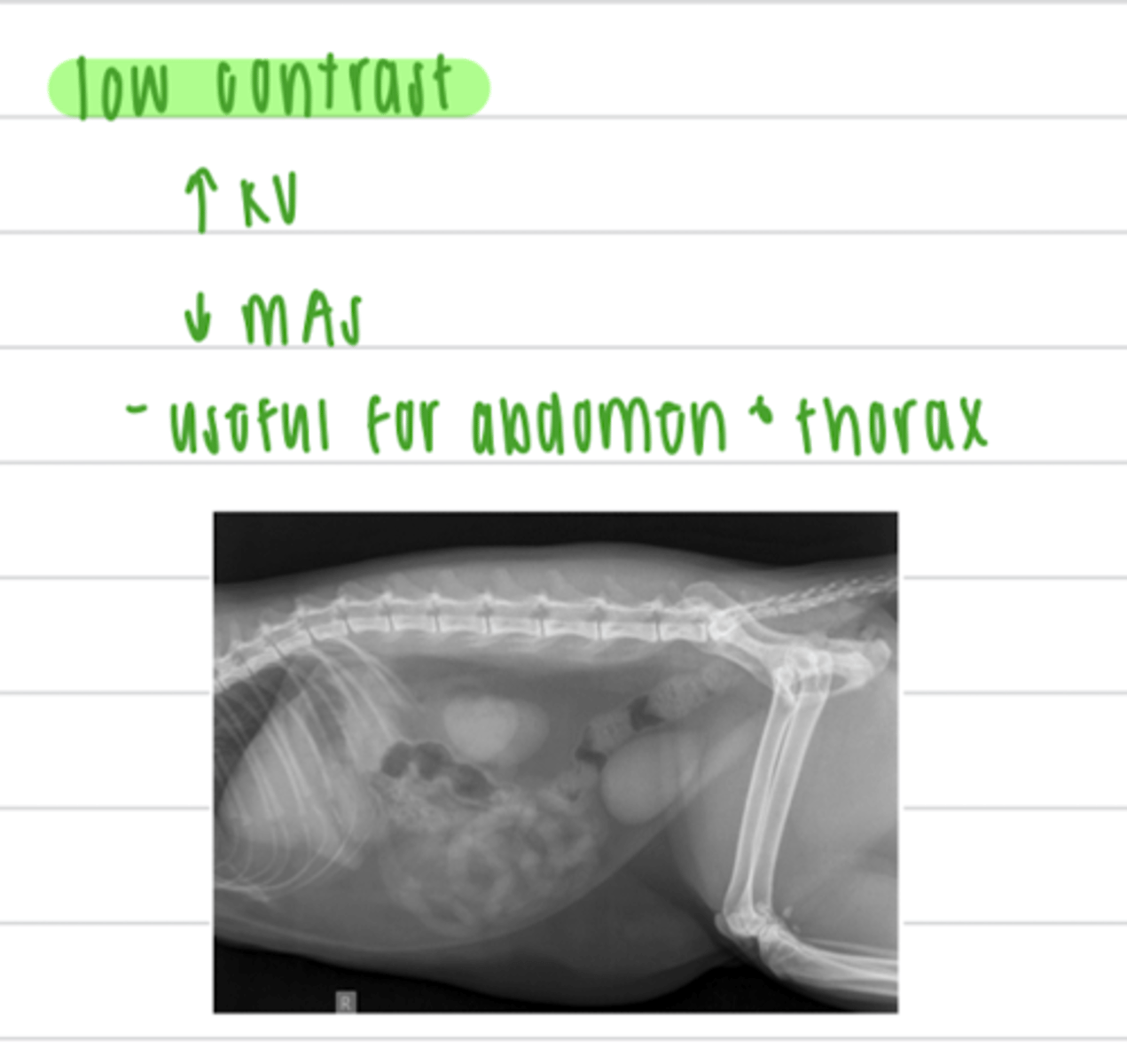
to visualize the abdomen or thorax, do we want a high or low contrast?
low
using a low contrast is useful to visualize what anatomical structures?
the abdomen and thorax
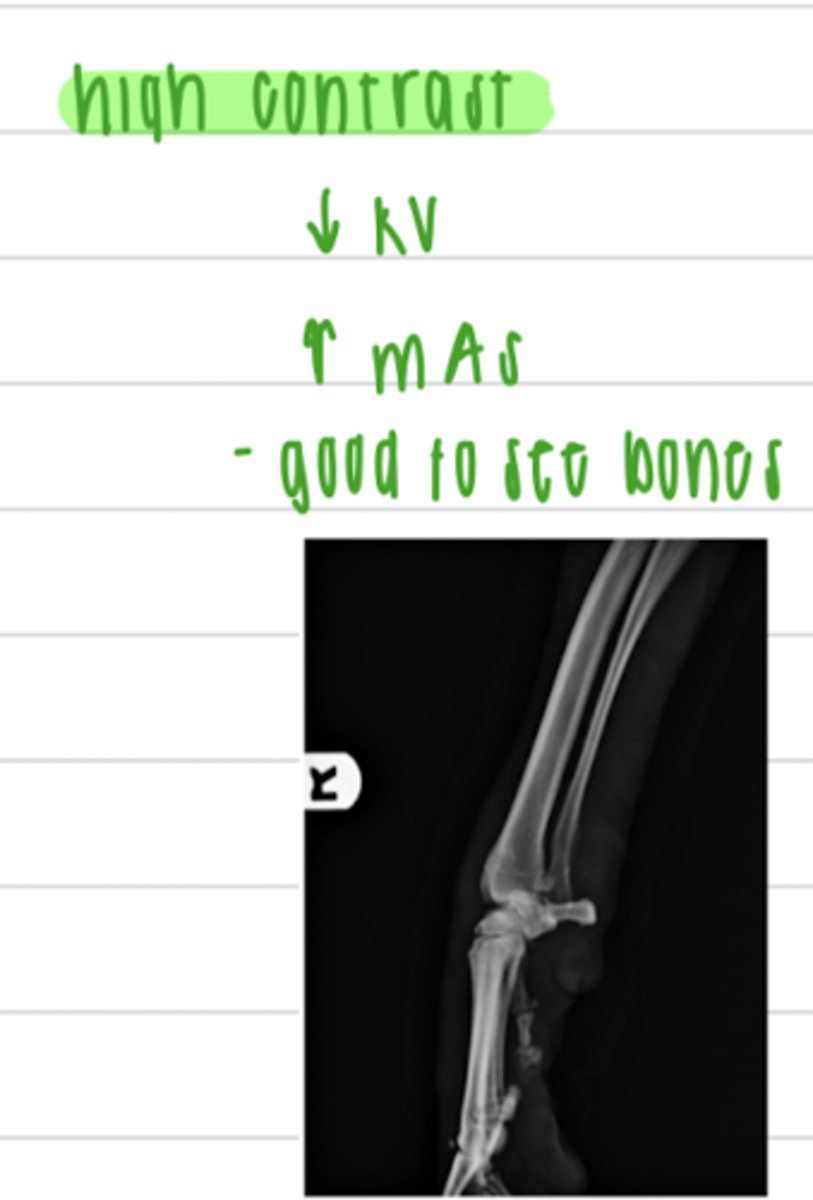
to achieve a high contrast, we want to use a __________ (high or low) kV and a __________ (high or low) mAs.
low; high
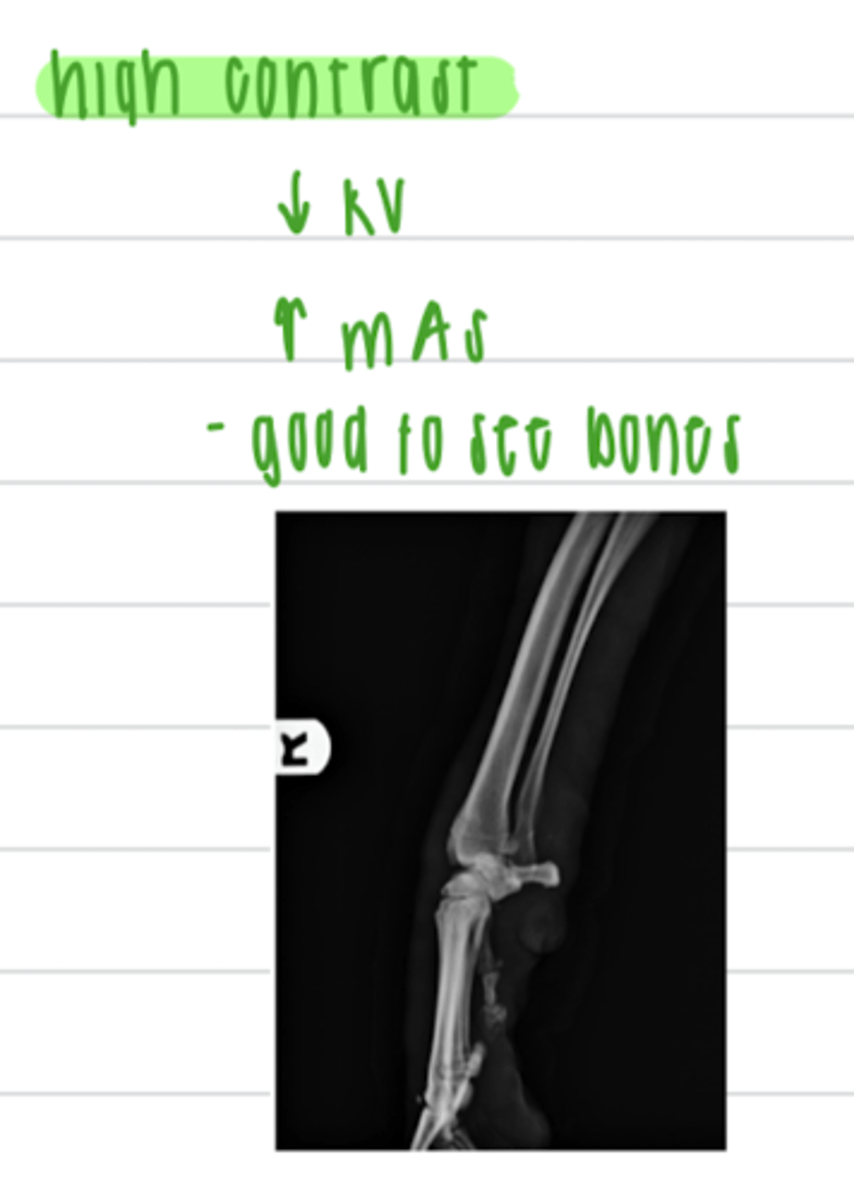
to achieve a low contrast, we want to use a __________ (high or low) kV and a __________ (high or low) mAs.
high; low
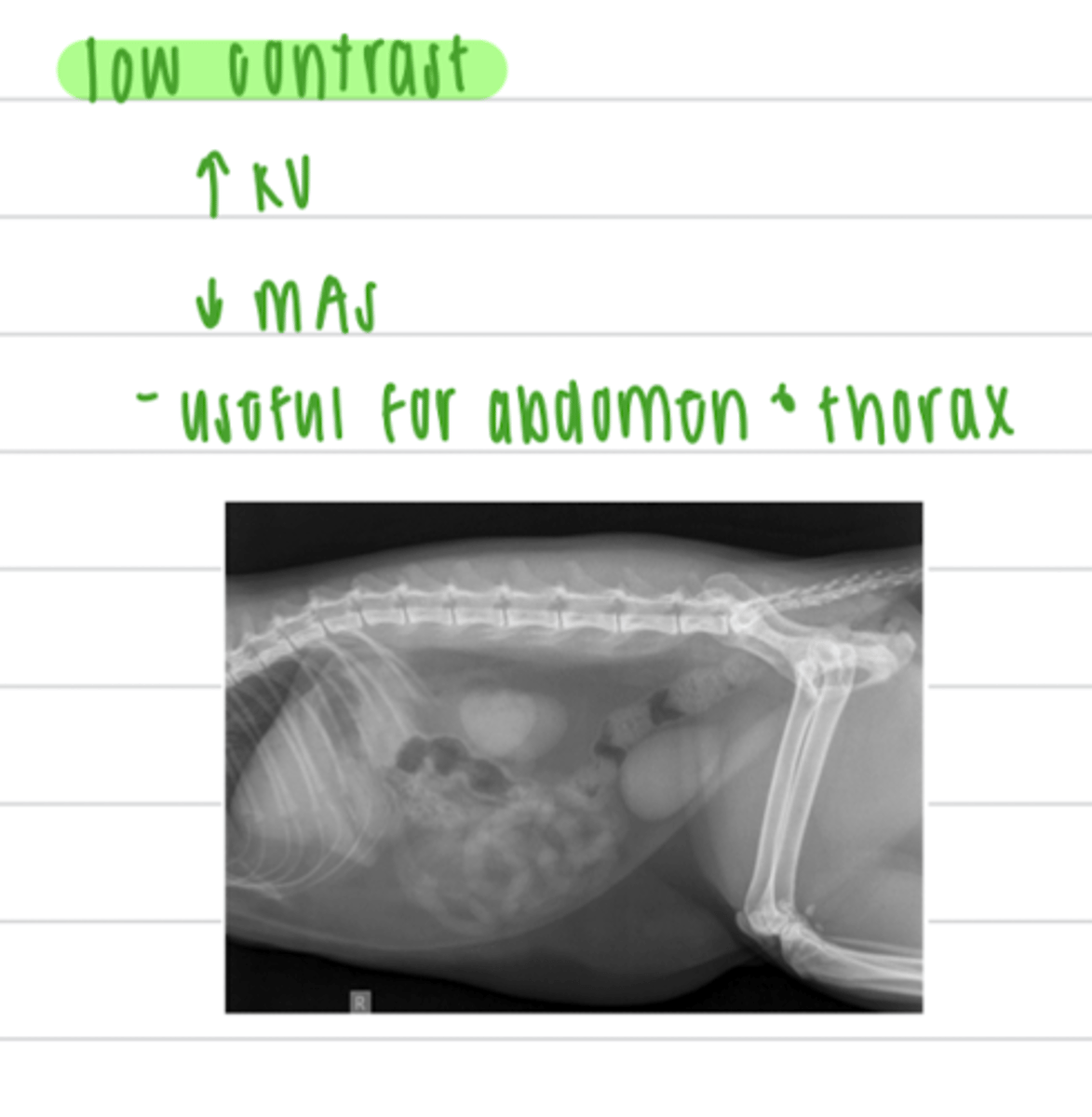
a low kV and high mAs will produce an image with _________(high or low) contrast.
high
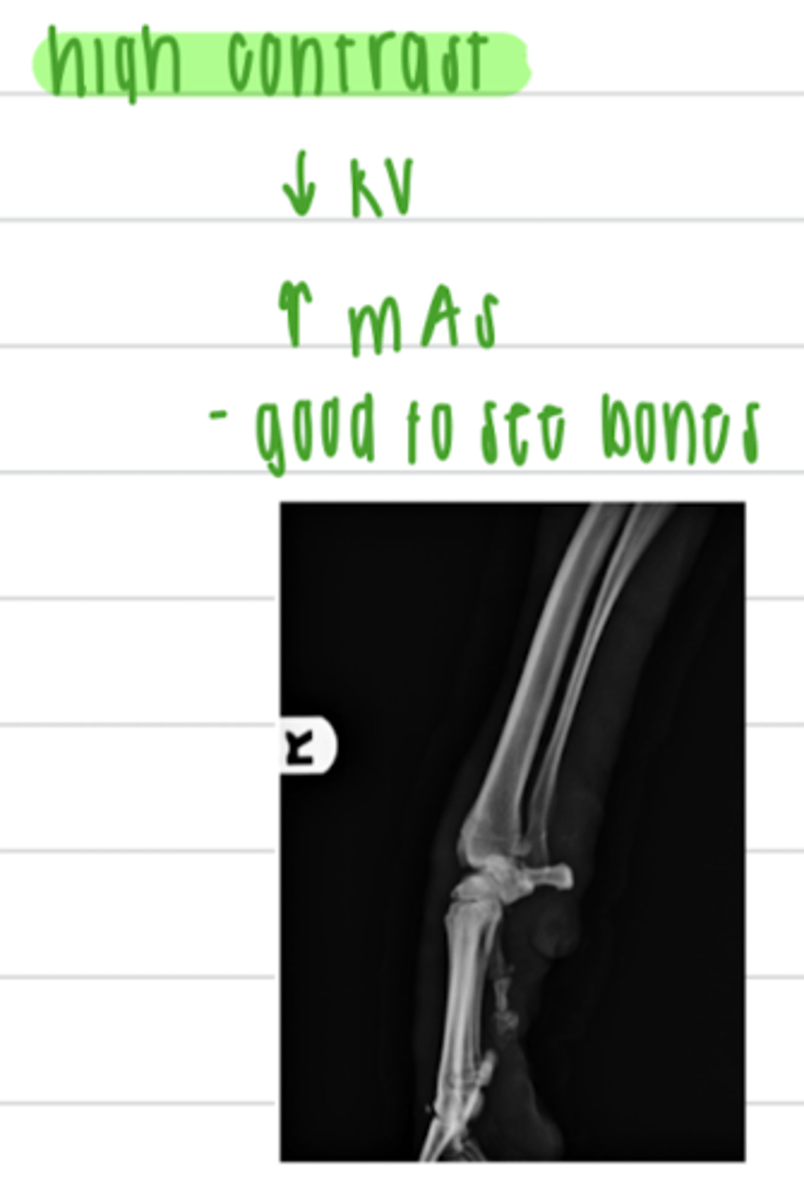
a high kV and low mAs will produce an image with _________(high or low) contrast.
low
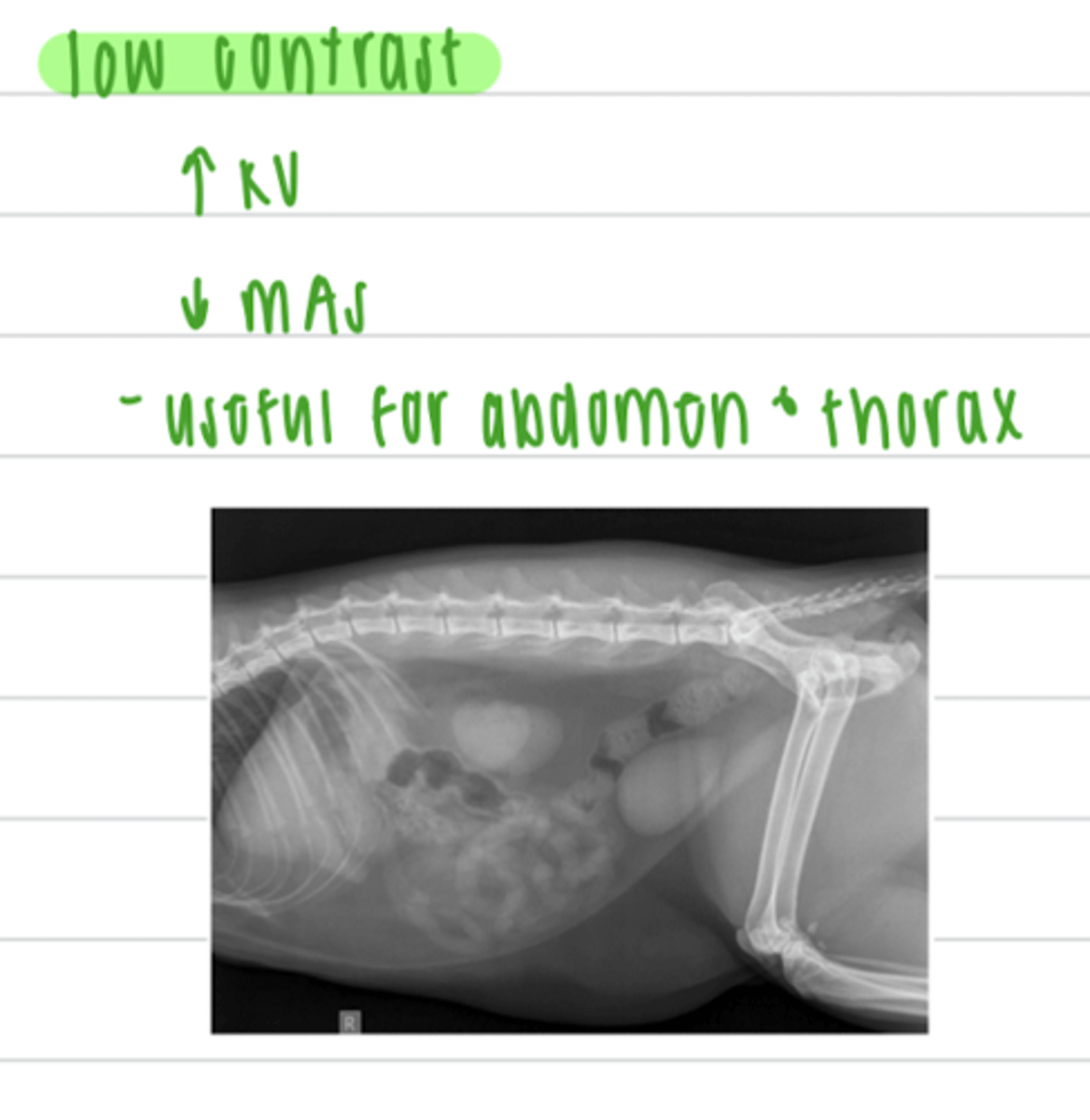
scattered radiation is produced due to the __________ effect
compton
how does the presence of the compton effect impact the contrast of a radiograph?
the compton effect produces scattered radiation, which decreases the radiographic contrast.
how can we avoid the compton effect (scattered radiation)?
using good collimation and a grid/Bucky
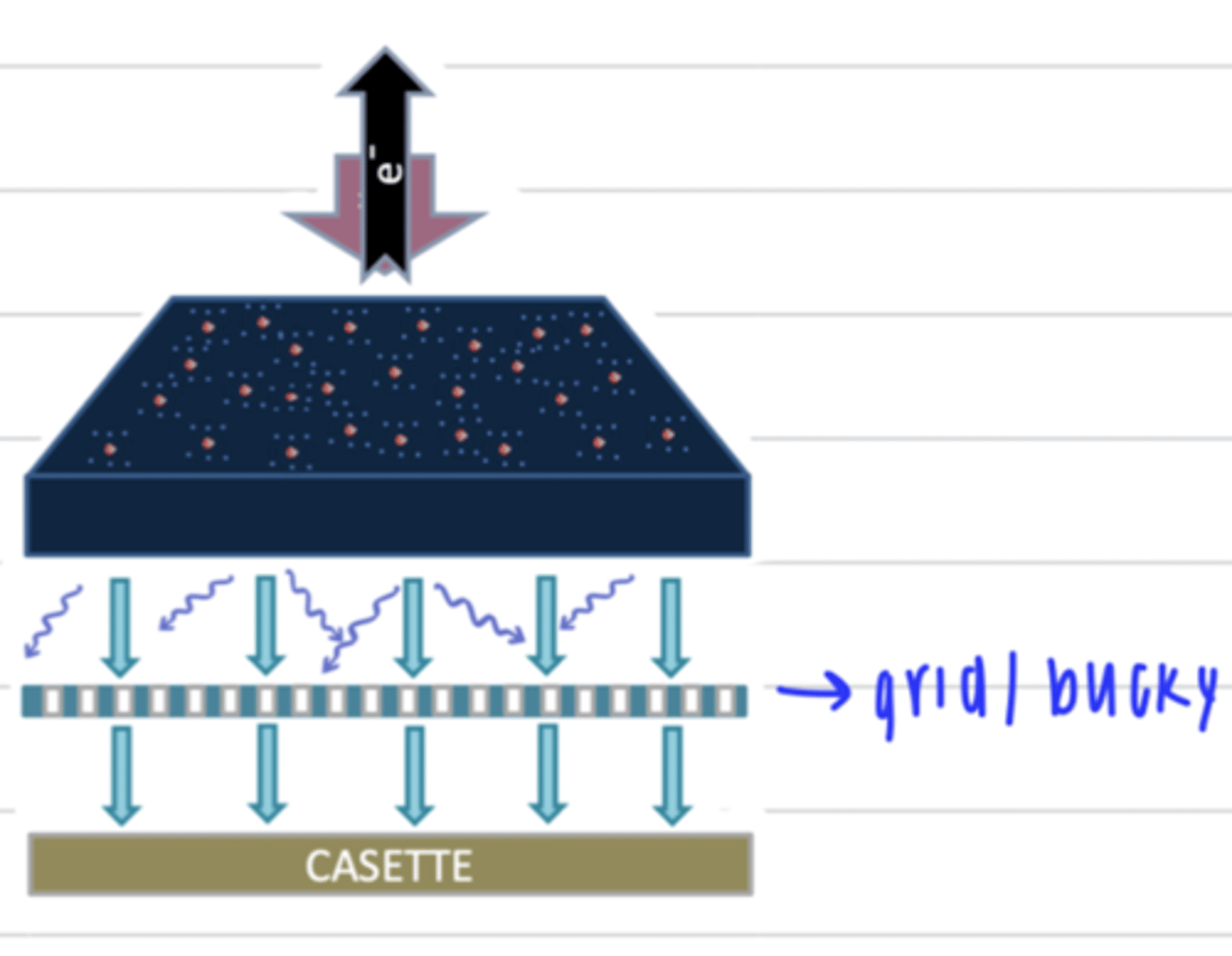
what is the purpose of the grid/Bucky?
to prevent the compton effect/scattered radiation
what is image detail (radiation)?
the degree of definition with which the margins of different structures located very close to each other are appreciated in radiography. this depends on the patient movement, image geometry, and film/screen system.
what 3 factors impact the image detail (resolution)?
1. patient movement
2. image geometry
3. film/screen system
how does patient movement impact the image detail?
when the patient moves, the xray will have less detail/resolution.
in order to prevent this, we use a fast exposure time and sedate the animal
how do we avoid patient movement from decreasing the image detail?
we can use a fast exposure time and sedate the animal
why is image geometry important in radiology?
because we are capturing a 2D image of a 3D object, so it is easy to mess up
what is focus film distance (FFD)?
the distance between the X-ray tube (the source of X-rays) and the cassette
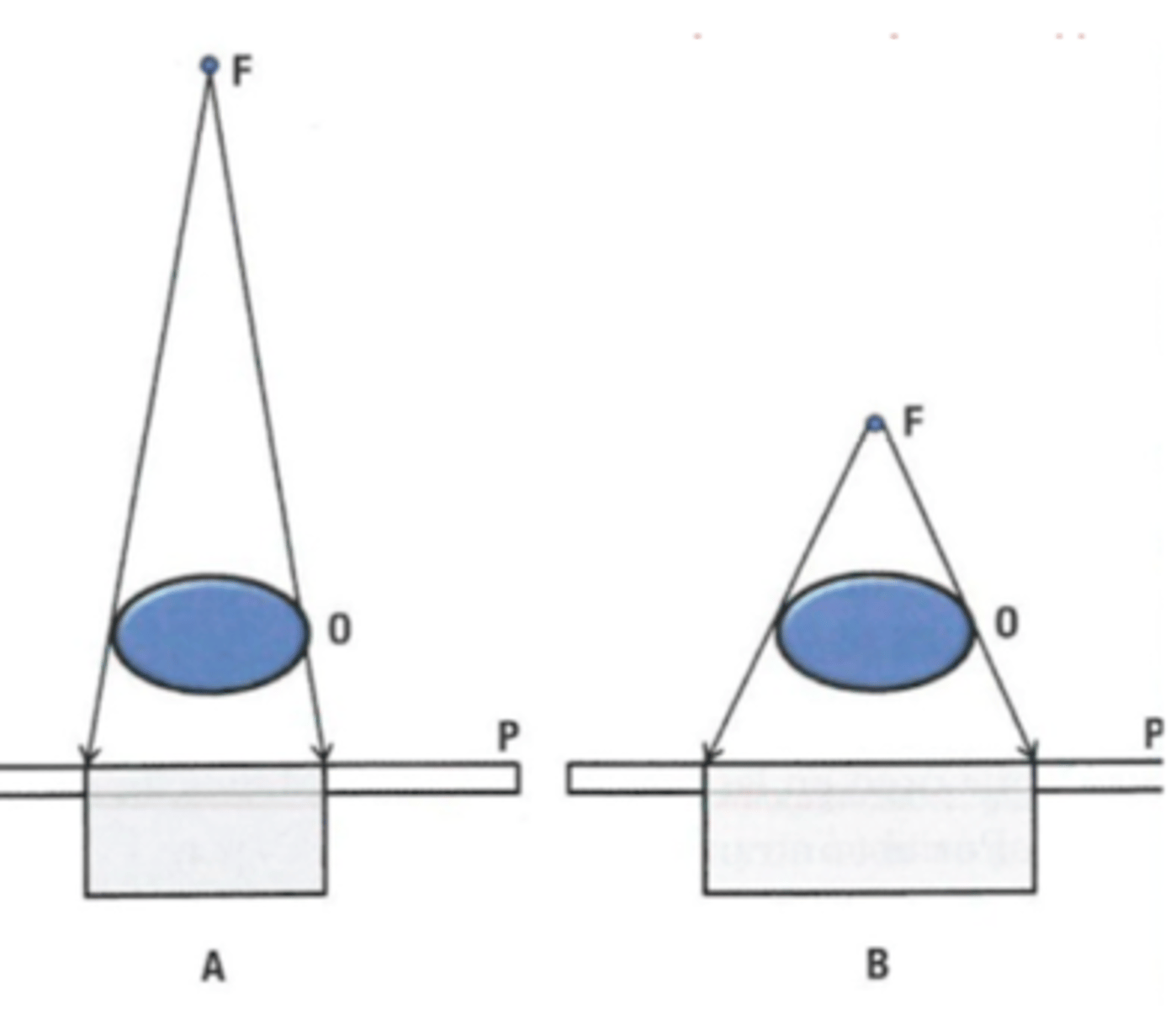
if there is a low focus film distance (FFD), is there high or low magnification?
high magnification
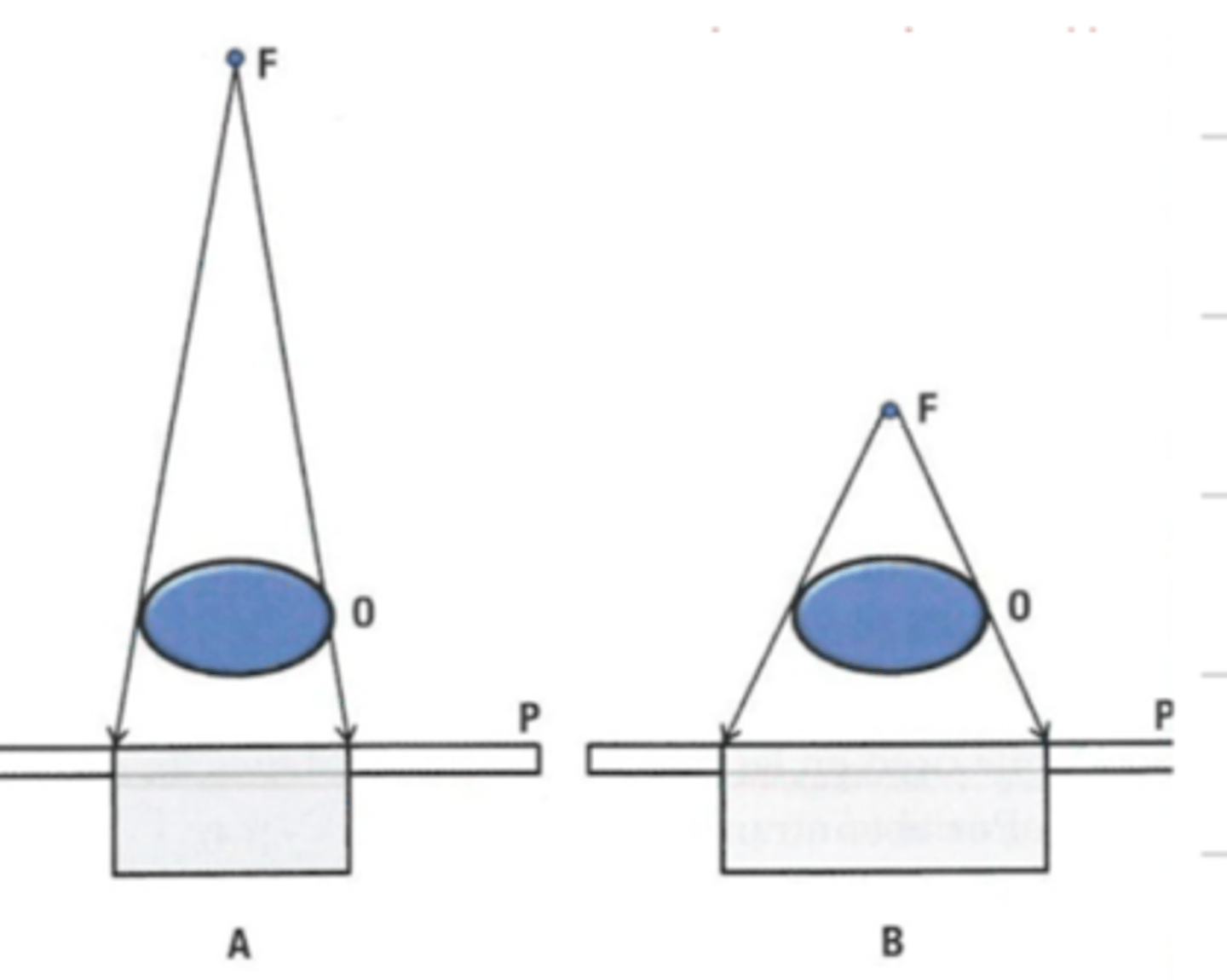
if there is a high focus film distance (FFD), is there high or low magnification?
low magnification
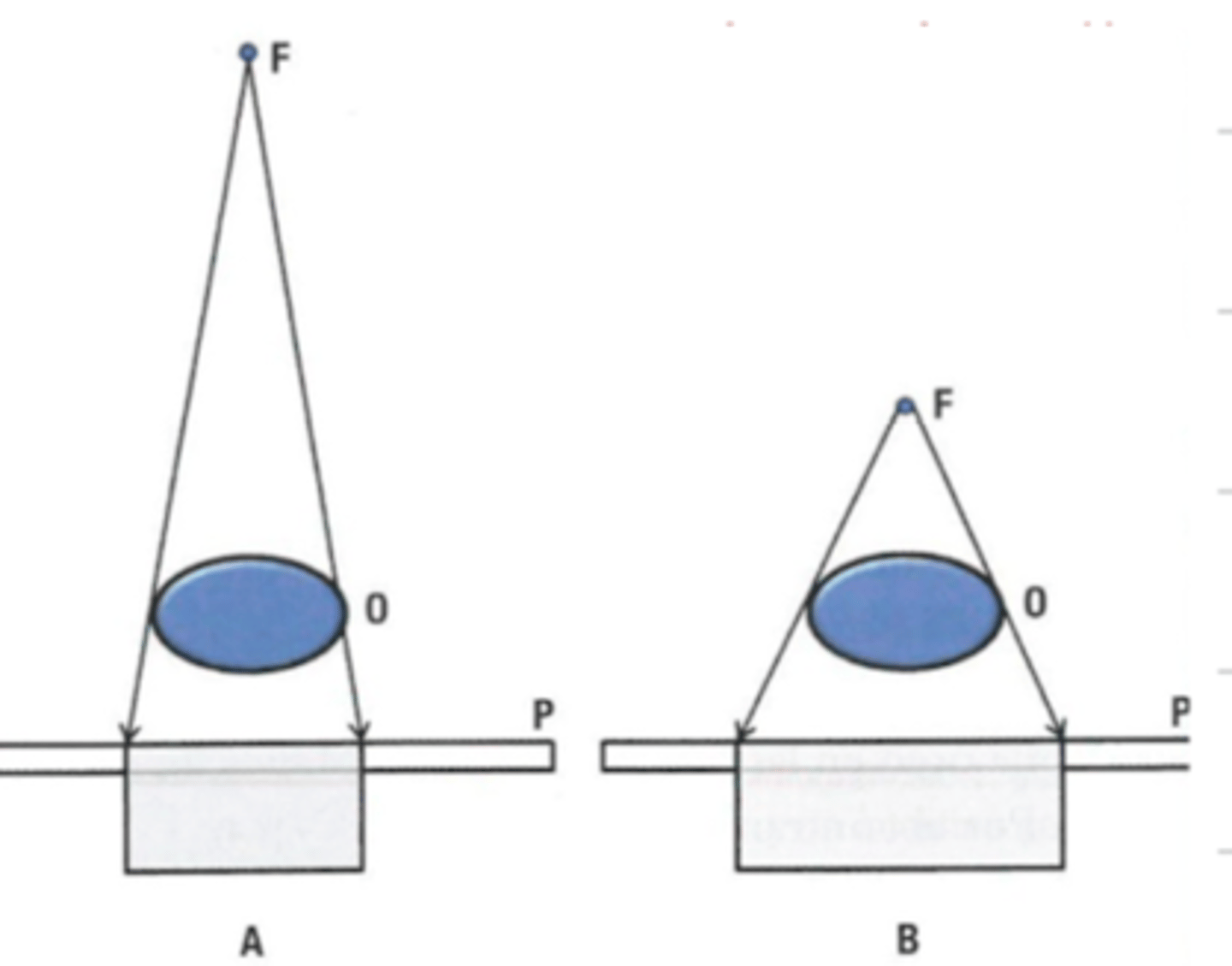
what is object film distance?
the distance between the object being imaged and the film cassette
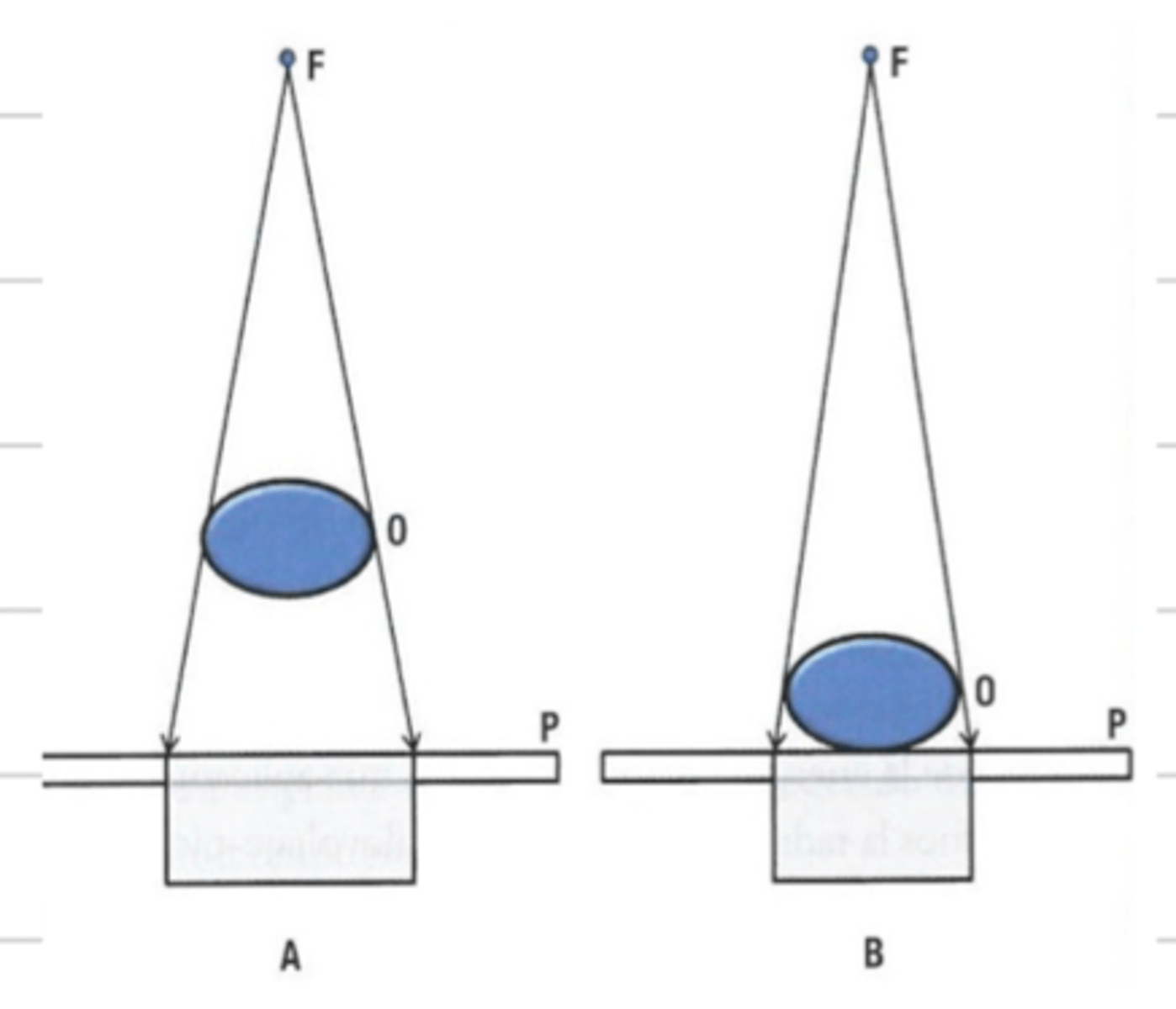
if there is an increased object film distance, is there higher or lower magnification?
high
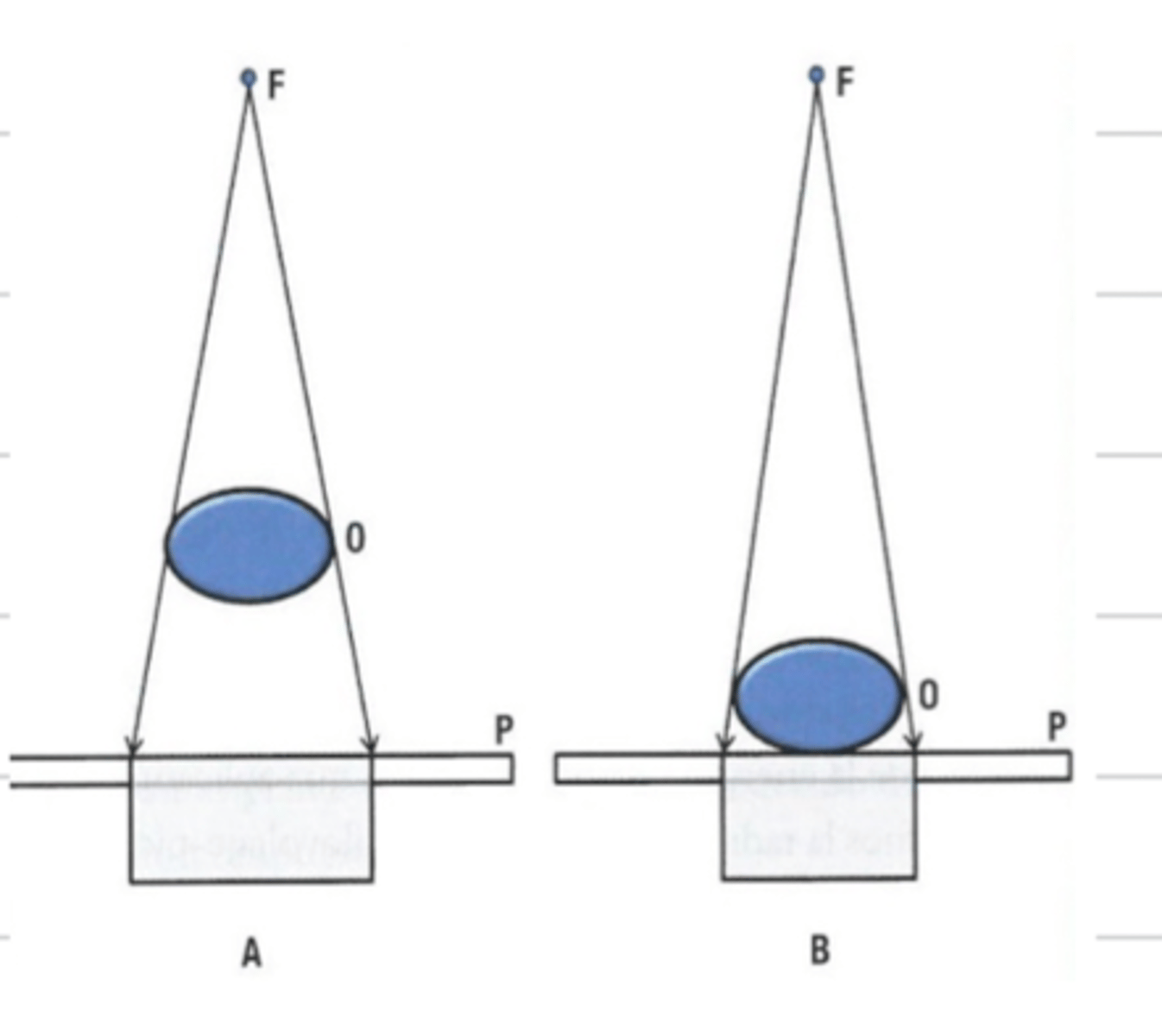
if there is a low object film distance, if there higher or lower magnification?
low
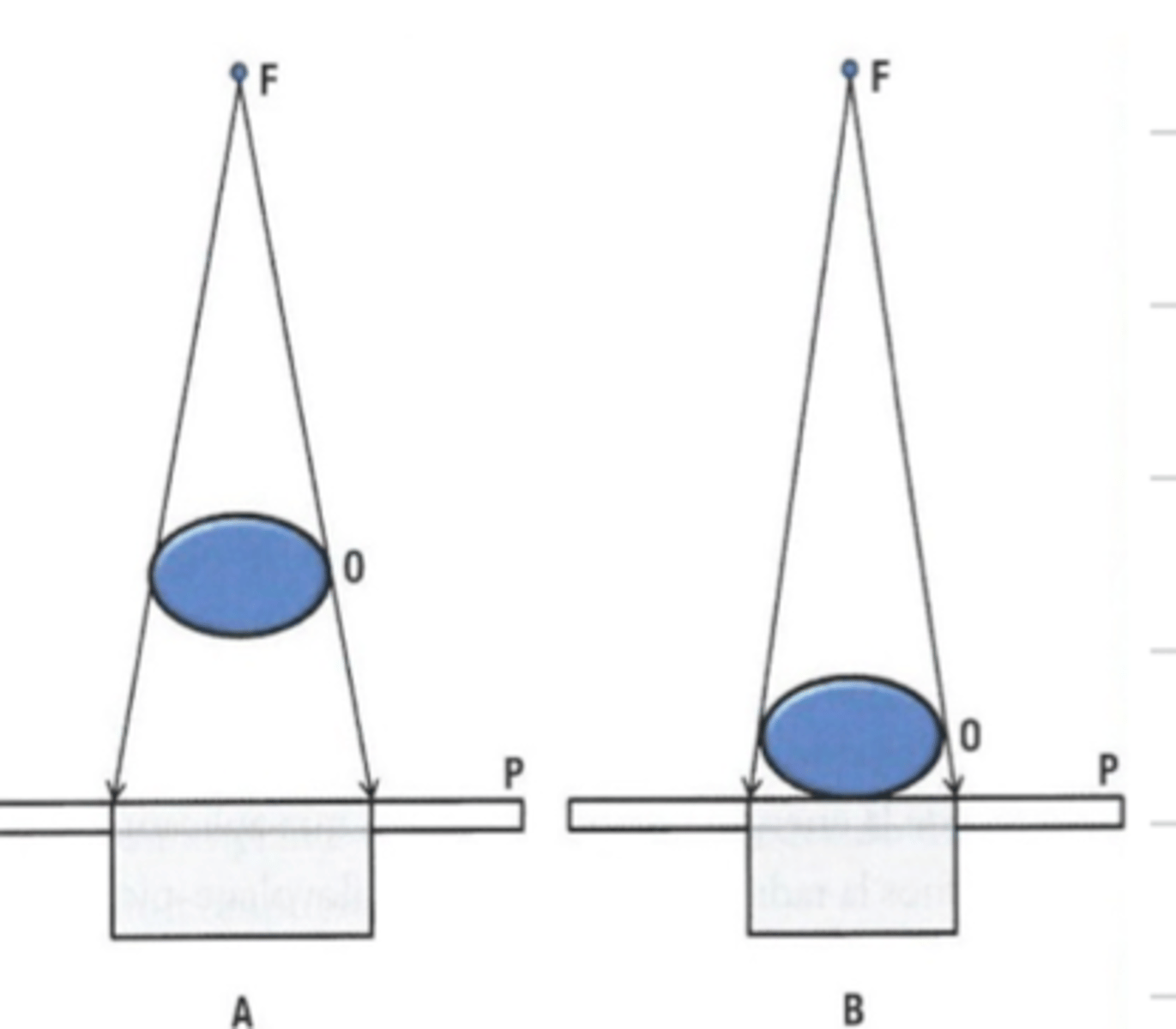
what is distortion in radiology?
when the object (patient) is not parallel to the film, it distorts the image
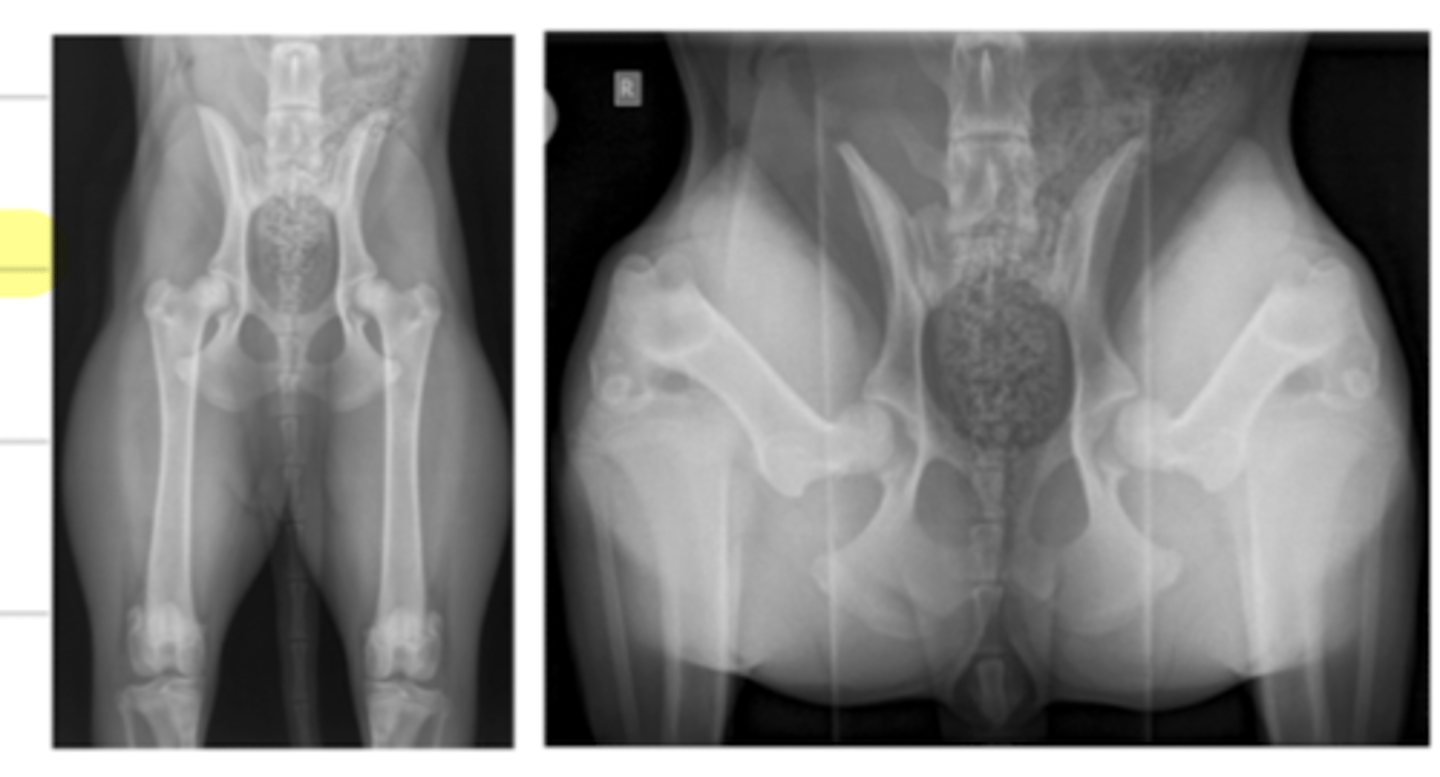
what factors affect the image geometry?
-magnification
-distortion
-loss of depth perception
-silhouette sign
-summation sign
why do we need orthogonal projections?
because we cannot see the depth in radiographs since they are 2D images.
what is "silhouette sign" in radiography?
when 2 structures of the same opacity are in contact, so we cannot distinguish their margin in the image.
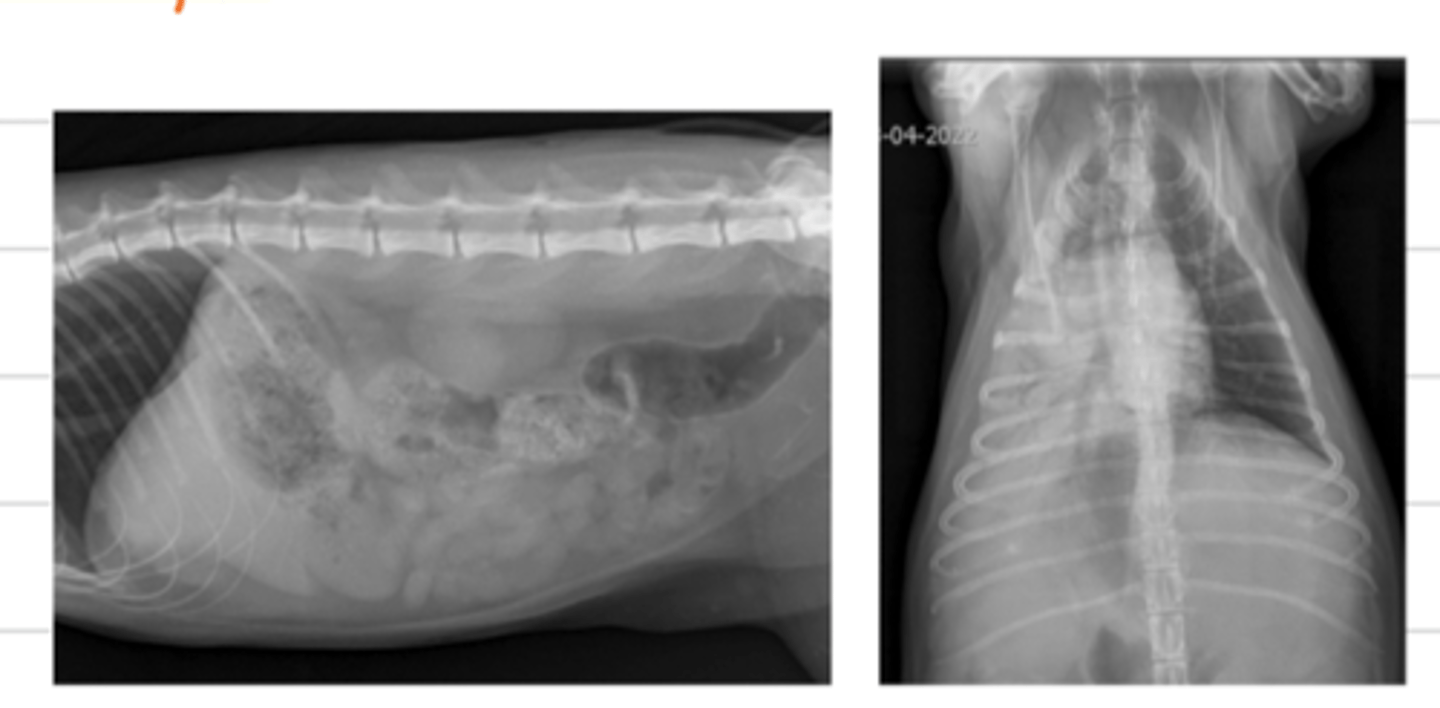
when 2 structures of the same opacity are touching, we cannot distinguish where one begins and the other ends (their margins). what is this called?
silhouette sign
when 2 structures of the same opacity are overlapping, but not in the same plane, the opacity of these structures add up. this is called...
summation sign
what is "summation sign" in radiology?
when 2 structures of the same opacity are overlapping, but not in the same plane, the opacity of these structures add up
when taking radiographs of a patient, we must fill a report containing what information?
-patient ID (age, breed sex BCS)
-projections (RL, LL, VD, DV)
-assessment of radiographic technique (positioning, collimation, exposure factors)
-findings (abnormalities)
-radiographic diagnostics
-differential diagnosis
-recommendations (other diagnostic methods and tests)
the 5 radiographic signs are:
1. size
2. shape/margins
3. position
4. number
5. opacity
when 2 structures of the same opacity are touching, we cannot distinguish where one begins and the other ends (their margins). what is this called?
silhouette sign
what are the 5 opacities of a radiograph?
1. air
2. fat
3. soft tissue and fluid
4. mineral (bone)
5. metal
what is radiobiology?
the science that studies the biological effects of ionization radiation in living tissues
how do we classify the type of radiobiology?
1. depending on the type of cell affected
-somatic or hereditary/genetic
2. according to its characteristics
-deterministic or stochastic/ deterministic
how is radiobiology classified according to the type of cell affected?
somatic- affects the individual either immediately or later
hereditary/genetic- affects the individual's offspring
how is radiobiology classified according to the characteristics?
deterministic- a higher dose means a more severe injury, and it is only affecting somatic cells
stochastic/probabilistic- the dose is not related to the severity- it is always serious. can affect somatic or hereditary cells
what are stochastic/probabalistic biological effects?
the biological effects caused by xrays that occur by chance and have a probability of occurring, rather than being directly proportional to the dose of radiation received.
Unlike deterministic effects, which have a threshold dose below which they do not occur and increase in severity with higher doses, stochastic effects do not have a threshold. Instead, as the dose of radiation increases, the probability of stochastic effects occurring also increases, but there is no guarantee that any individual will experience these effects.
what are deterministic biological effects in radiology?
biological effects caused by xrays that exhibit a clear dose-response relationship. Unlike stochastic effects, deterministic effects have a threshold dose below which they do not occur, and their severity increases with increasing radiation dose.
Examples of deterministic effects include skin erythema (redness), radiation burns, and cataract formation. These effects typically manifest above a certain threshold dose of radiation exposure, and their severity is directly related to the radiation dose received. Below the threshold dose, deterministic effects do not occur, but as the dose increases beyond the threshold, the severity of the effects becomes more pronounced.
why do we need to use radiologic protection?
to prevent the occurrence of deterministic biological effects and limit the probability of stochastic effects.
in radiology, we use a dose limitation system that is based on 3 requirements. what are the requirements?
1. justification- why do we need to take an xray
2. optimization- ALARA (use the kV as low as reasonably achievable)
3. dose limitation
what is "ALARA"?
"As Low As Reasonably Achievable."
It is a principle used in radiography to minimize radiation exposure to patients and doctors while still obtaining the necessary diagnostic information or achieving the desired outcome.
the "equivalent dose" is...
the average dose absorbed in a tissue/organ
what is the "effective dose"?
the sum of the weighted equivalent doses in all the tissues and organs
what factors can we manipulate in order to reduce the exposure to radiation?
1. distance between the patient and the tube (more distance= less exposure)
2. the time (less time= less exposure)
3. shielding (protective gear, walls, windows, etc)
what is a dosimeter?
a device that measures the safety of the xrays.
there are area dosimeters for the room and personal dosimeters that the workers wear.