Cartilage and Bone
1/37
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
38 Terms
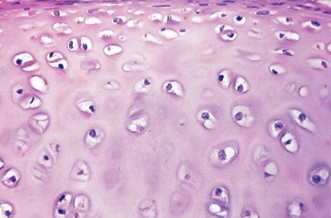
Cartilage
Avascular connective tissue
Chondrocytes
Abundant solid extracellular matrix
3 types:
Hyaline cartilage
Elastic cartilage
Fibro cartilage
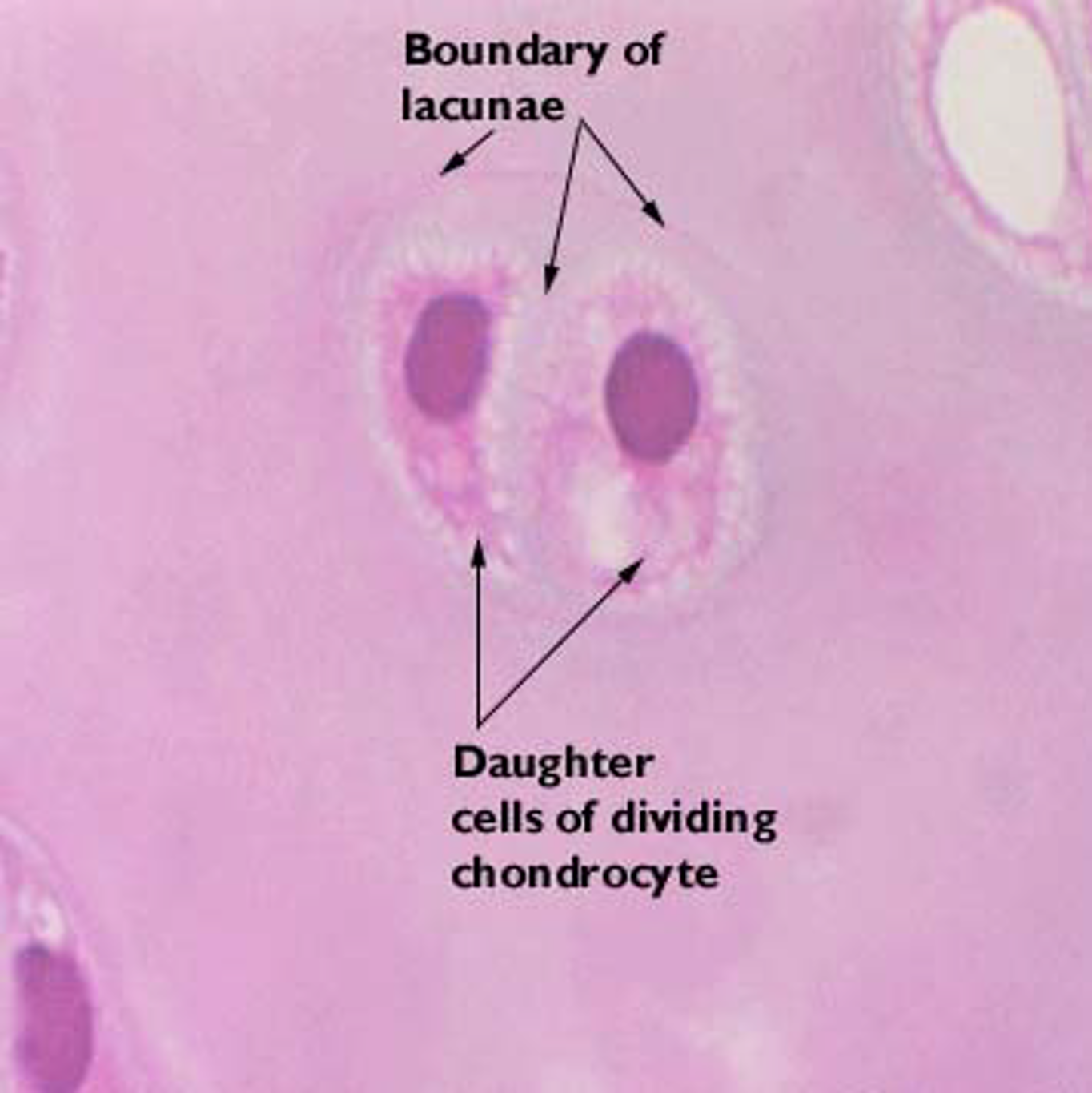
Chondrocytes
Basic cell type
Enclosed in lacunae, clustered in isogenous groups (recent division)
Division / matrix formation determines spacing
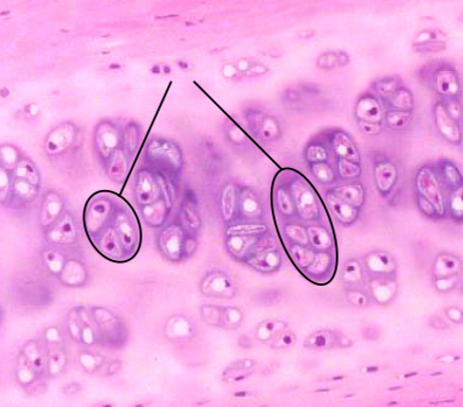
Chondrocytes Isogenous Groups
Cell groups are farther, if matrix growth is more than cell division
Cell groups are closer, if matrix growth is less than cell division
Chondrocytes Lacunae
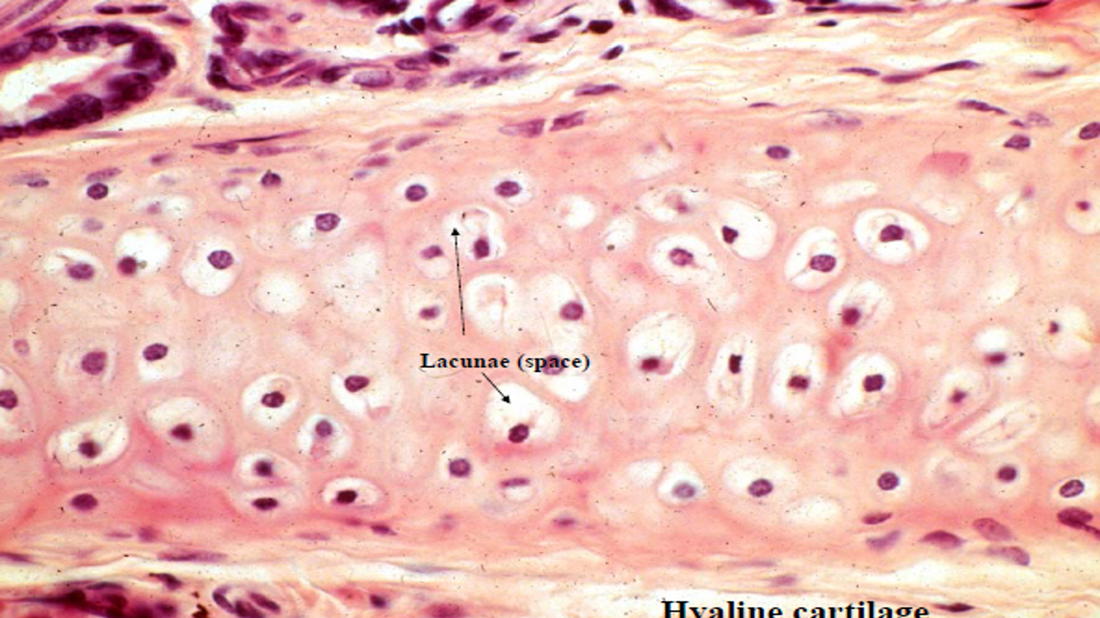
Chondrocytes
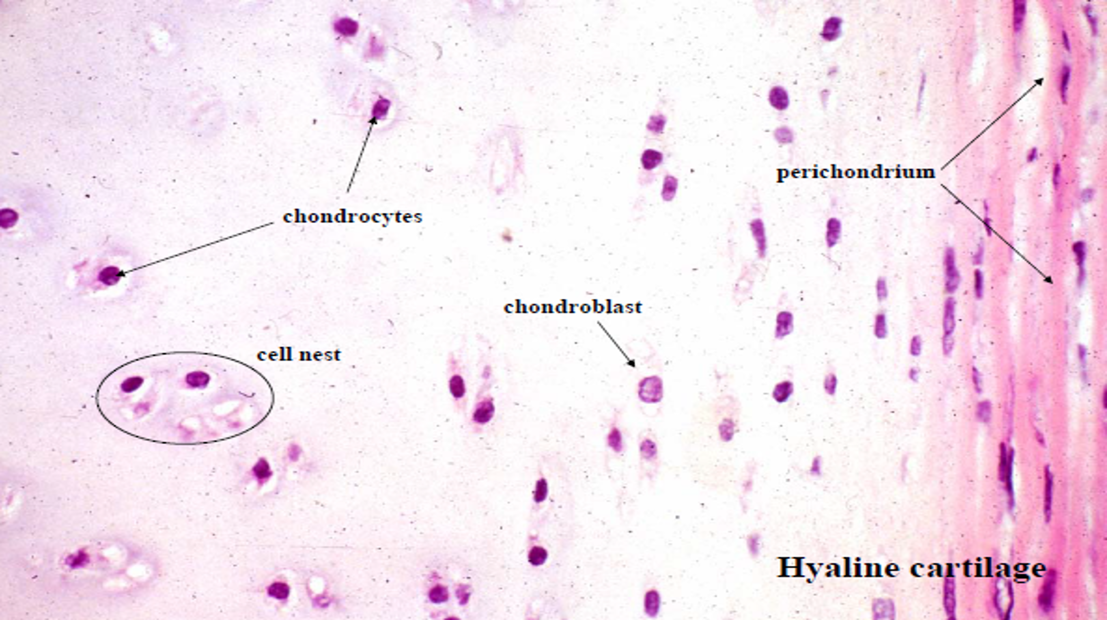
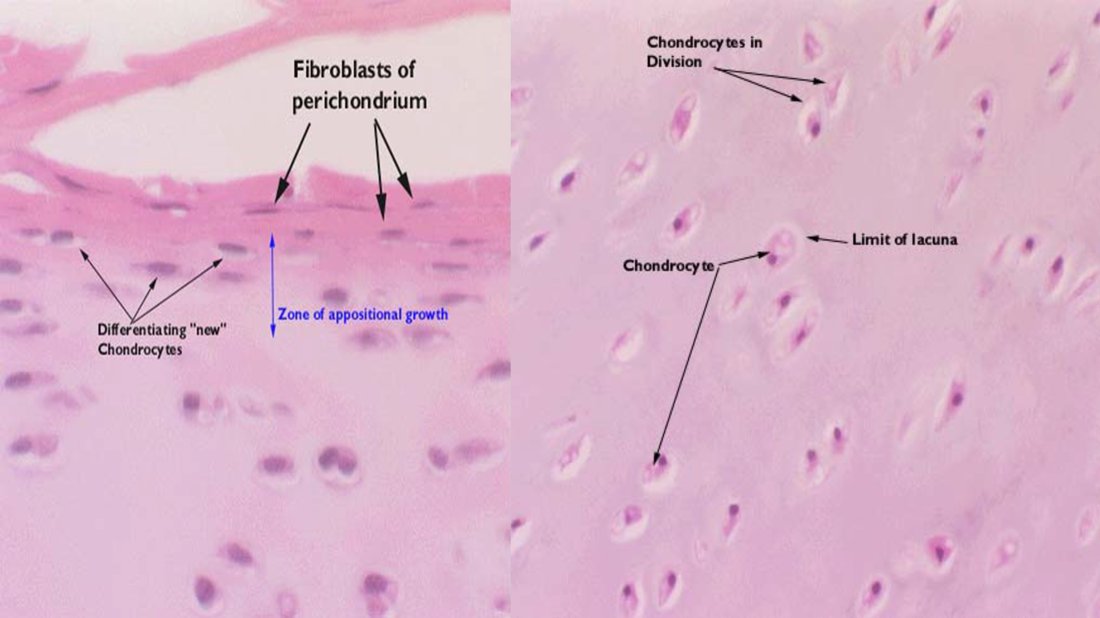
Cartilaginous Growth
Two processes:
Appositional growth: forms new cartilage at the surface of an existing cartilage
Interstitial growth: forms new cartilage within an existing cartilage mass.
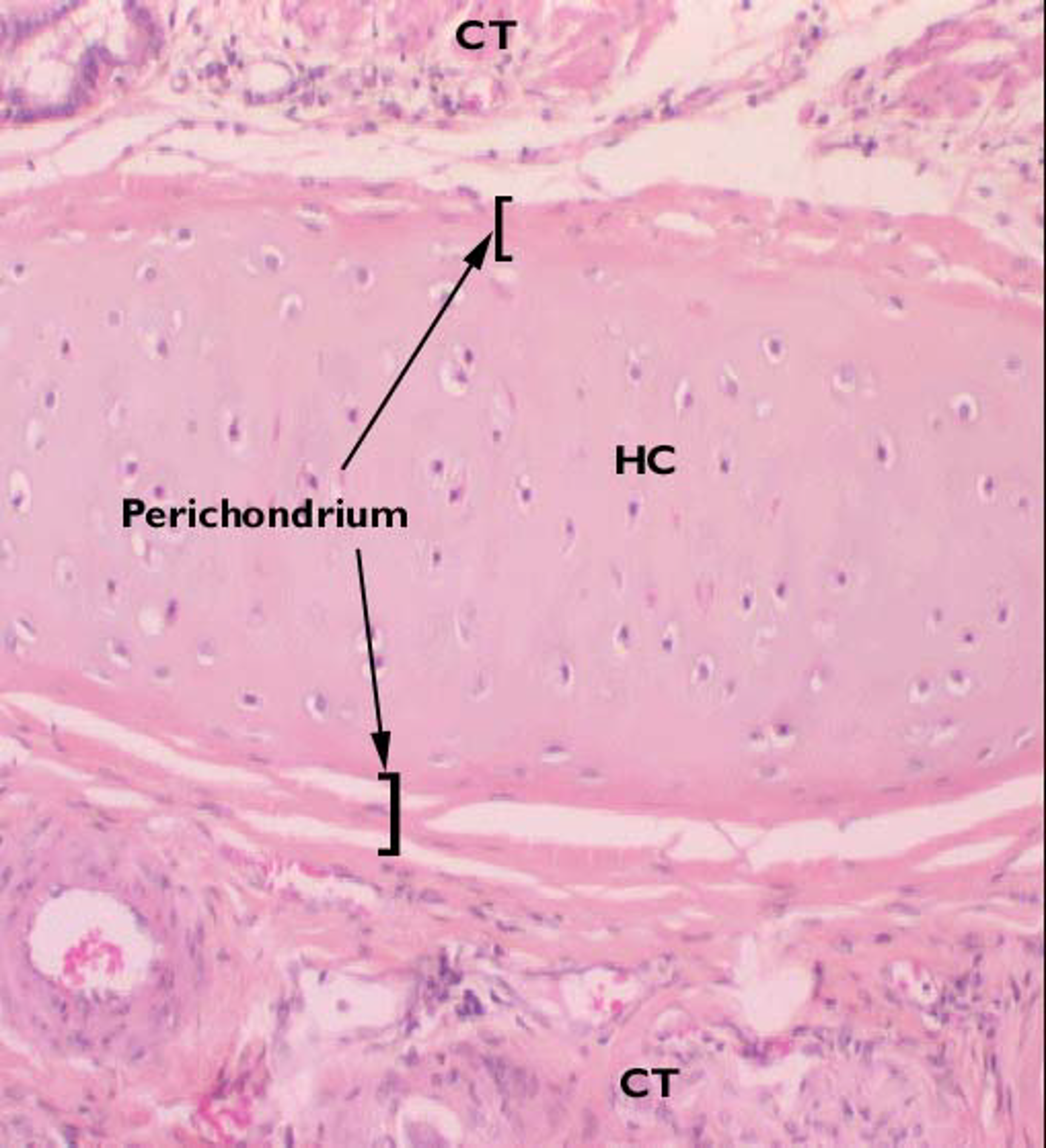
Perichondrium
Dense irregular connective tissue
Composed of Chondrogenic cells, appear like fibroblasts
Surrounds almost all forms of cartilage
Perichondrium
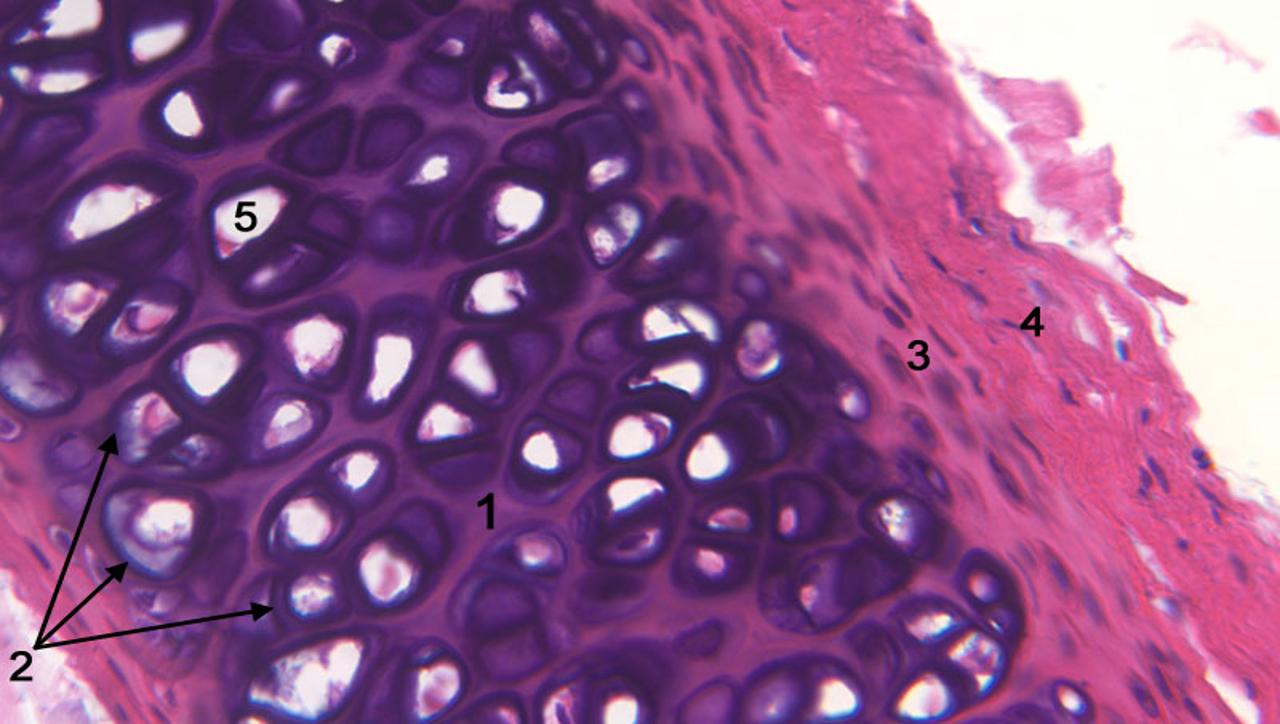
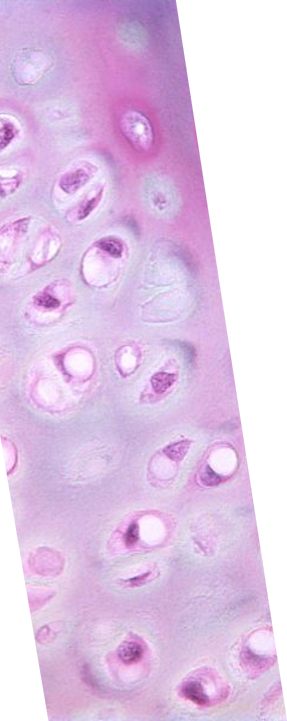
Hyaline Cartilage
Most common type of cartilage
Collagen type II fiber
Proteoglycans (creates ground substance)
Glycoproteins (multi-adhesive)
Appears glassy
Function:
Provides cushioning, low friction surface for joints
Provides structural support in respiratory system
Foundation for fetal skeleton development and endochondral bone formation
Fetal skeletal tissue, epiphyseal, synovial joints, costal, nasal cavity, larynx, trachea, bronchi
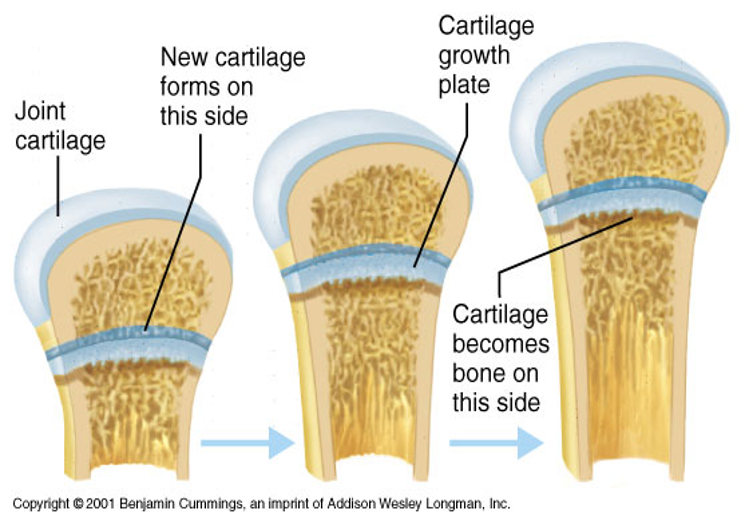
Endochondral ossification
During fetal development hyaline cartilage is the precursor for bone
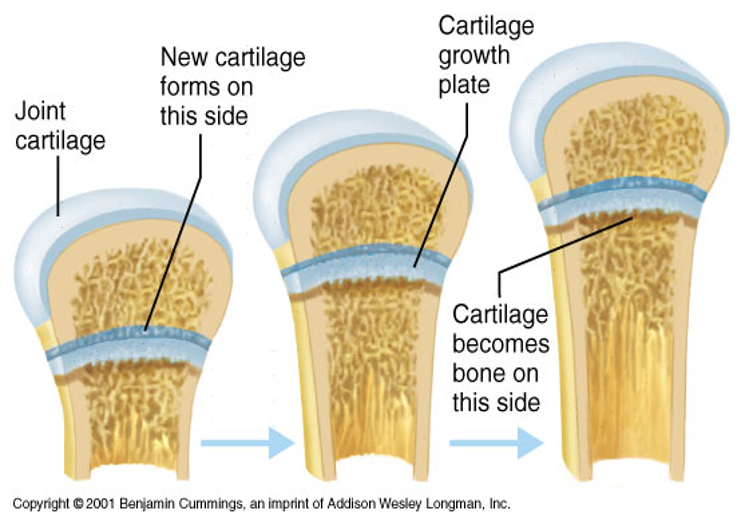
Epiphyseal growth plates
Made of hyaline cartilage and is replaced by bone as the bone continues to grow length wise.
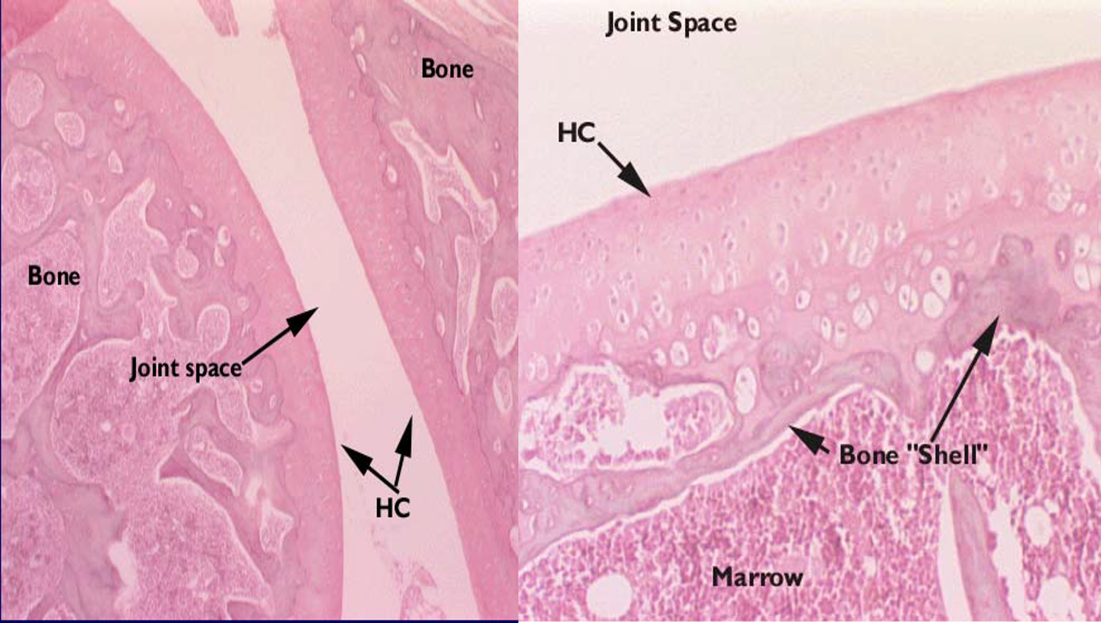
Articular cartilage
Hyaline cartilage that covers the articular surfaces of moveable joints
Do not have perichondrium
A remnant of the hyaline cartilage from the developing bone that persists throughout life
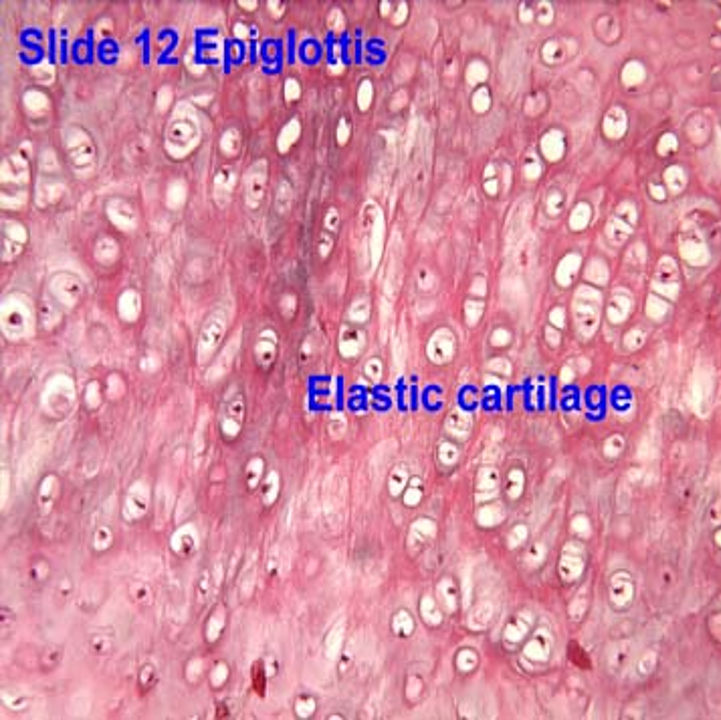
Elastic cartilage
Contains components of hyaline cartilage matrix, but also elastic fibers
Surrounded by perichondrium
Mostly elastic fibers, less collagen fibers
Large Chondrocytes, Close isogenous groups
Function
Provides flexible support for soft tissues
Pinna of external ear, external acoustic meatus, auditory tube, epiglottis
Elastic cartilage
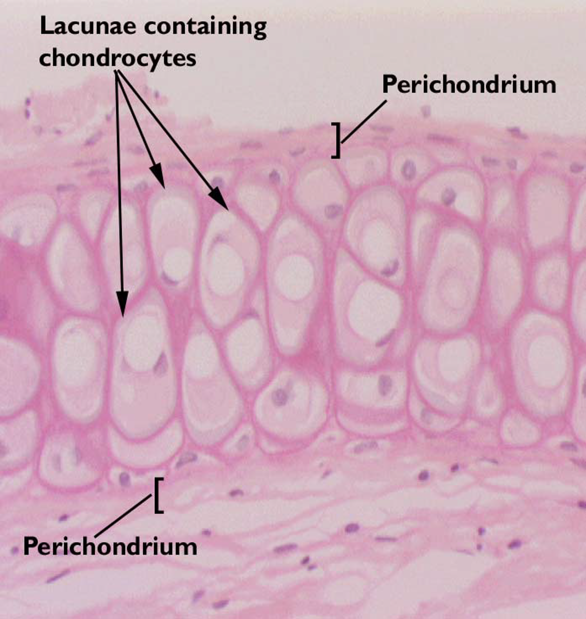
Elastic cartilage
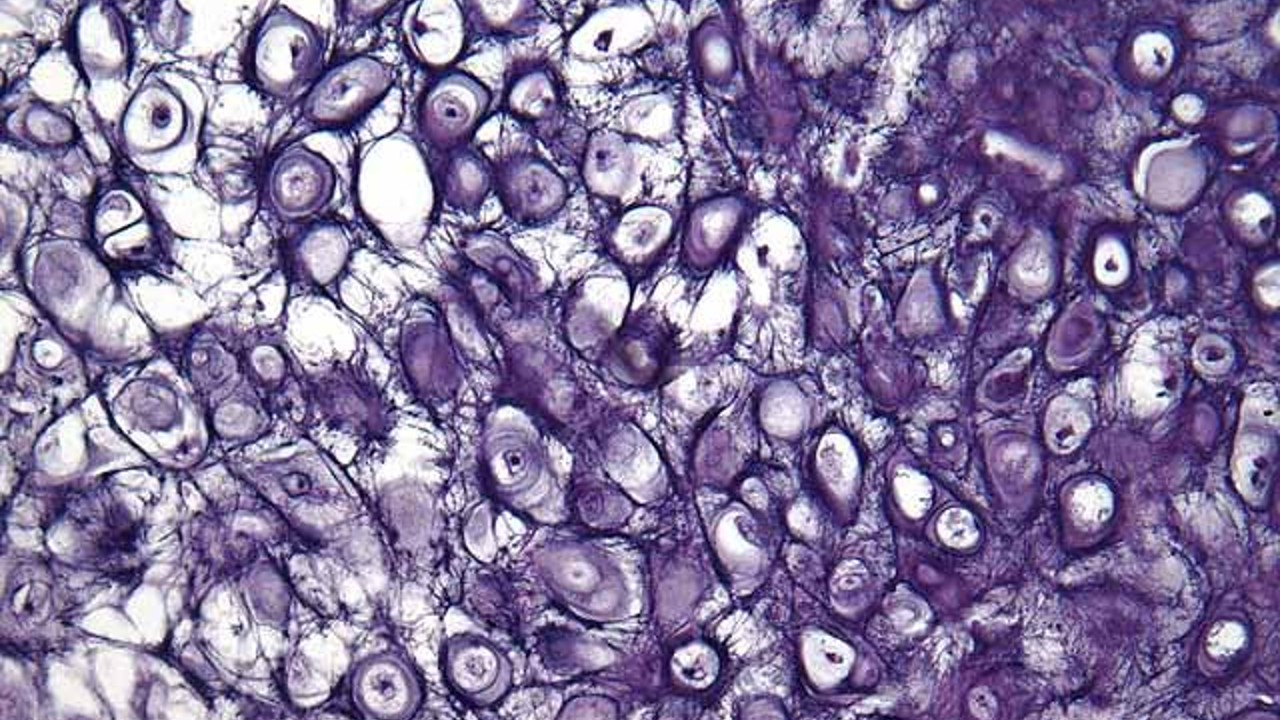
Elastic cartilage
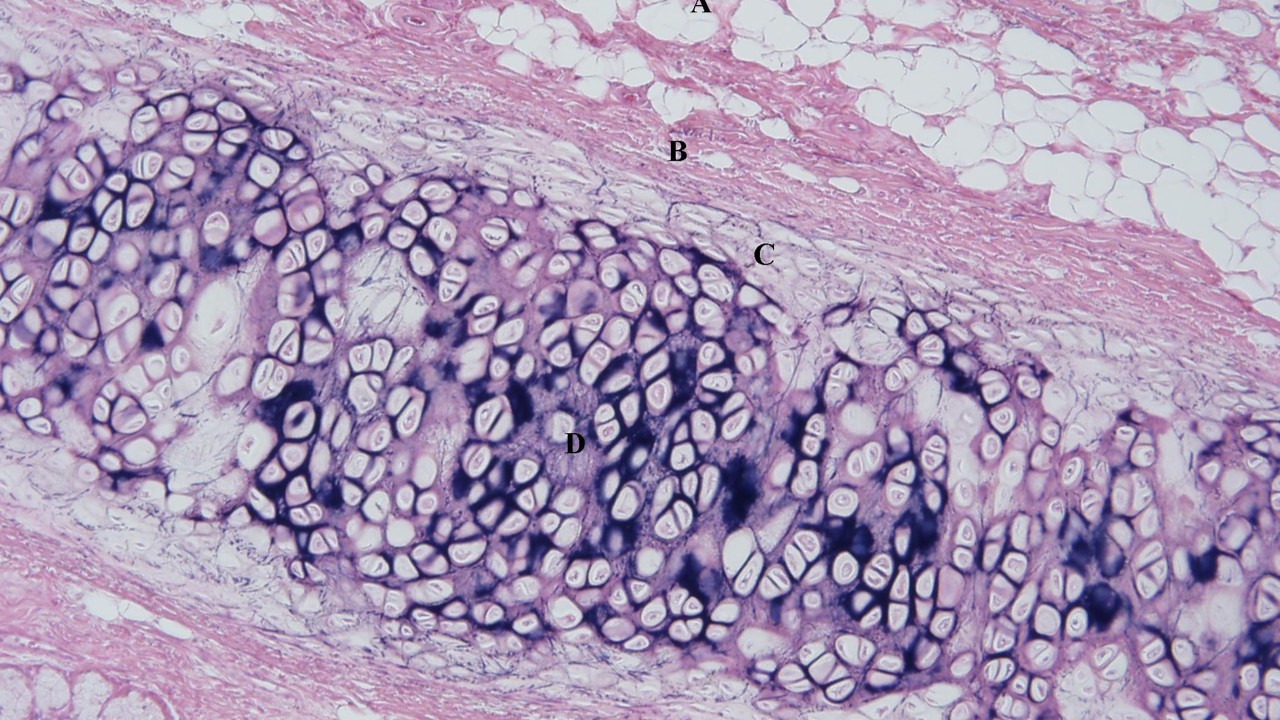
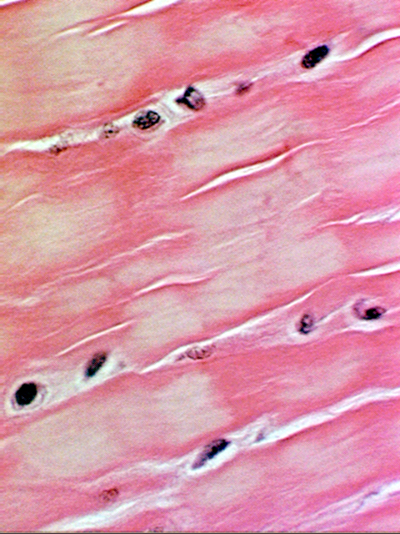
Fibrocartilage
Combination of dense regular connective tissue and hyaline cartilage
Mostly type I and II collagen
Less cartilaginous matrix
No surrounding perichondrium
Function
Resists deformation under stress, shock absorber
Intervertebral discs, pubic symphysis, articular discs
Fibrocartilage
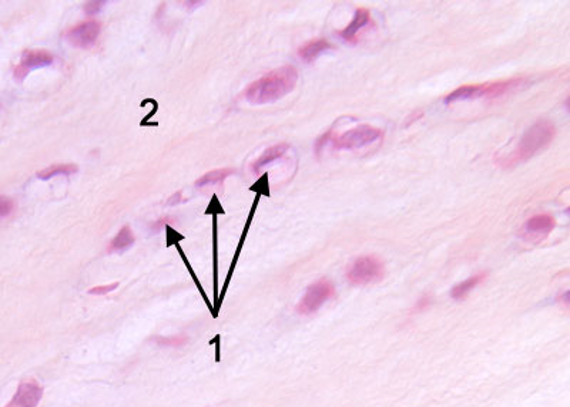
Fibrocartilage
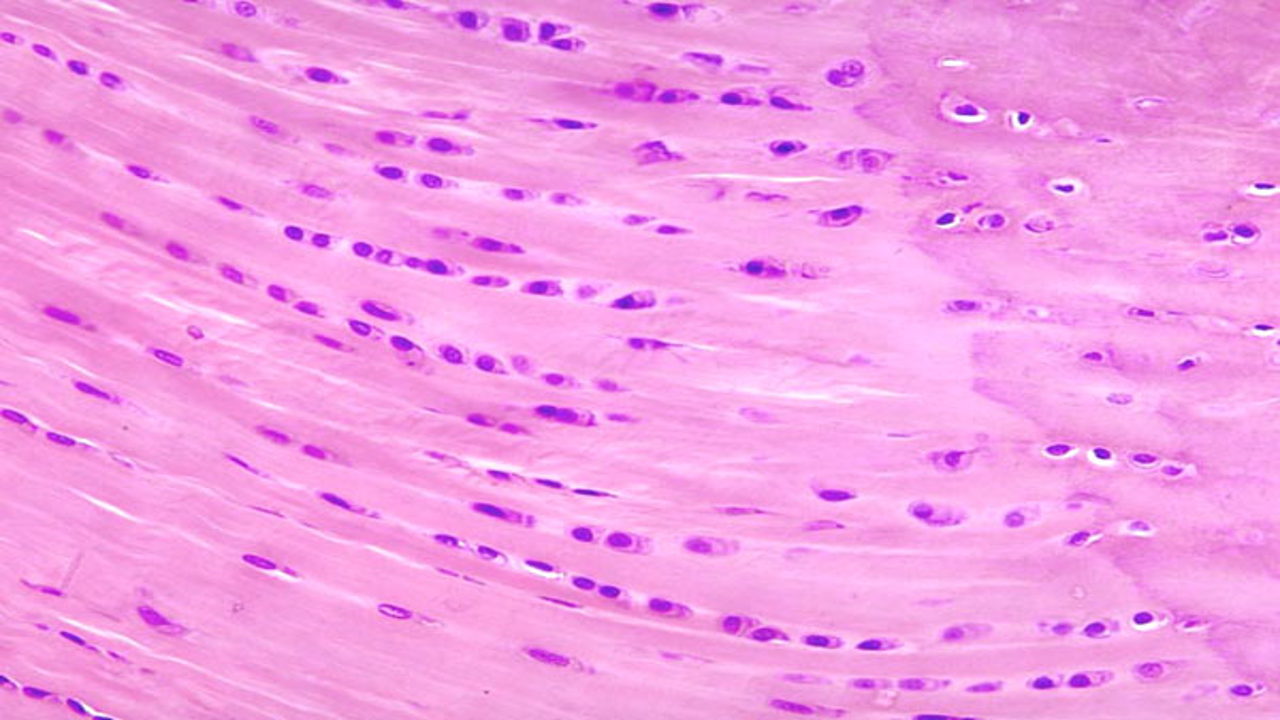
Fibrocartilage
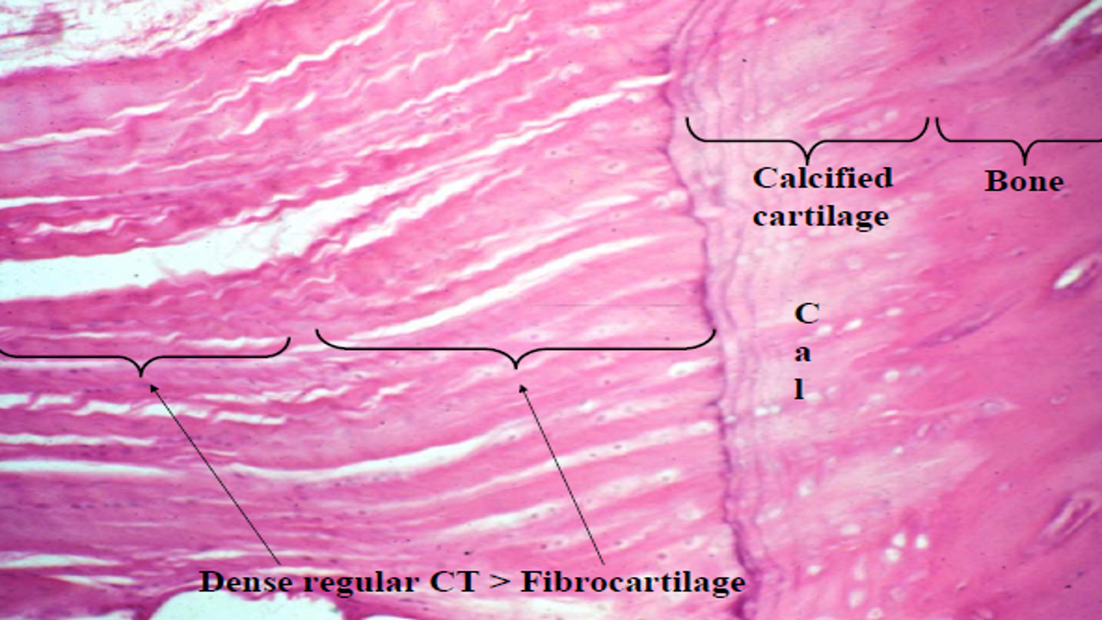
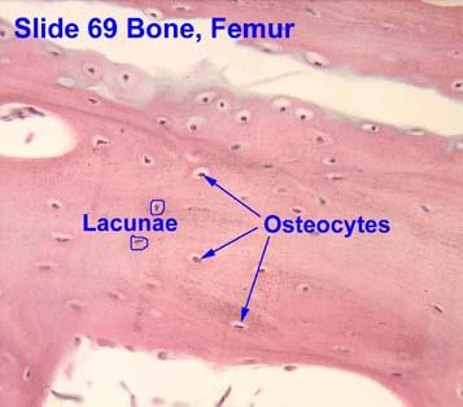
Bone
Specialized hard connective tissue w/ mineralized extracellular matrix
Cells (contained in lacunae)
Osteoblasts, Osteoclasts, Osteocytes (have processes called canaliculi)
Extracellular matrix is mineralized
Type I collagen, proteoglycans, glycoproteins, and Calcium
Function
Support, protection, homeostatic regulation of blood calcium, blood cell formation and muscle attachment.
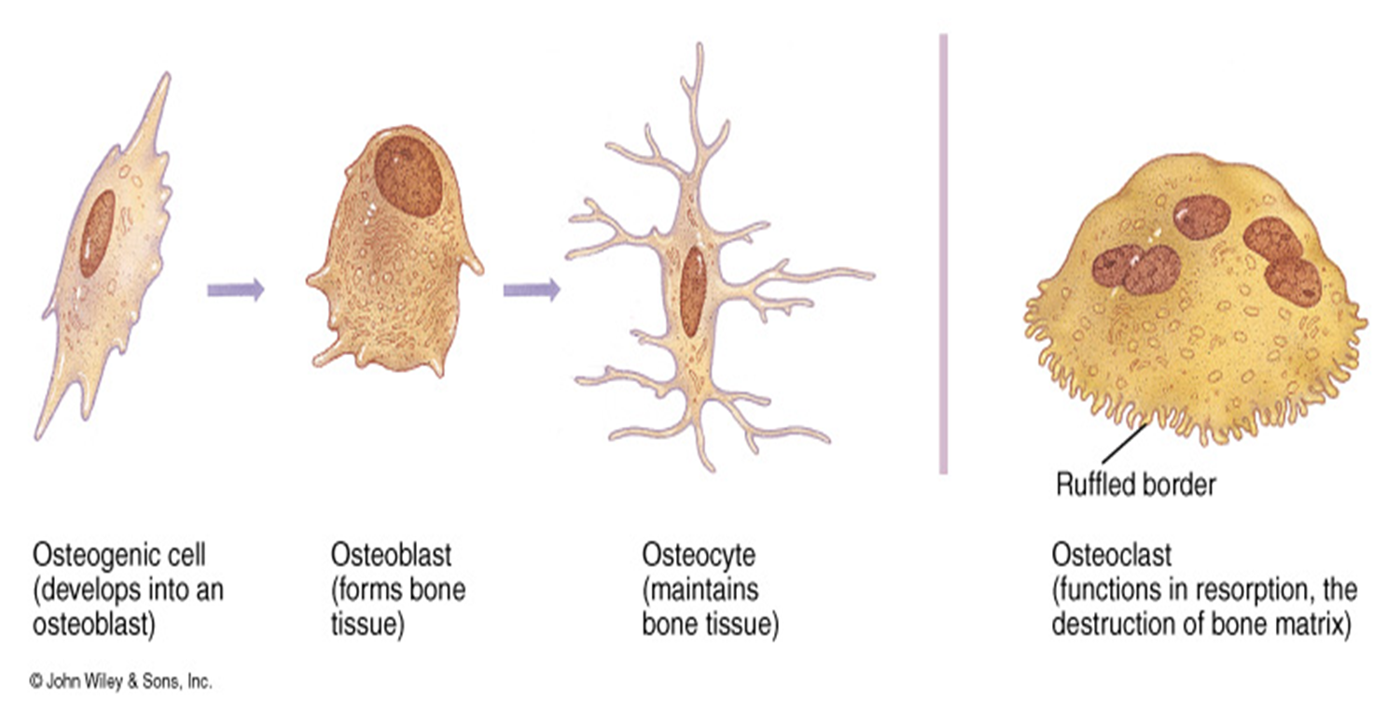
Bone tissue cells
Composed of 4 different cells:
Osteoprogenitor
Osteoblasts
Osteocytes
Osteoclasts
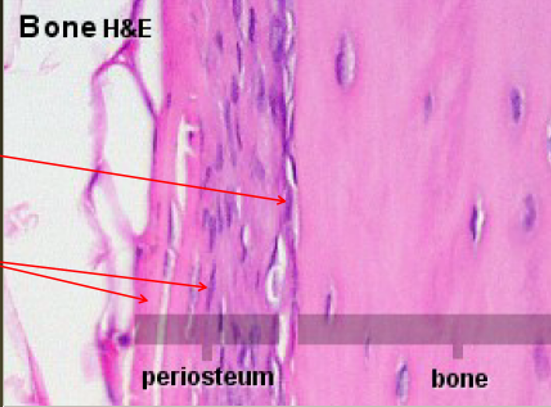
Osteoprogenitor Cells
Mesenchymal stem cells
Flatened, elongated oval nuclei
Found in periosteum, endosteum
Undergo mitosis, develop into many cell types (ex. osteoblasts)
Secrete bone matrix and has a vital role in growth and repair
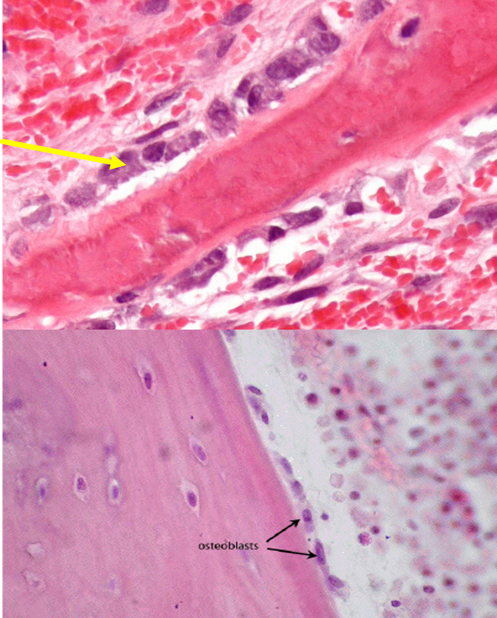
Osteoblast
Found on bone surface
Type 1 collage, proteoglycans and glycoproteins
Do not mitotically divide
May change to an osteocyte after matrix is secreted
Function:
Bone calcification
Form and maintain matrix
Osteoblast
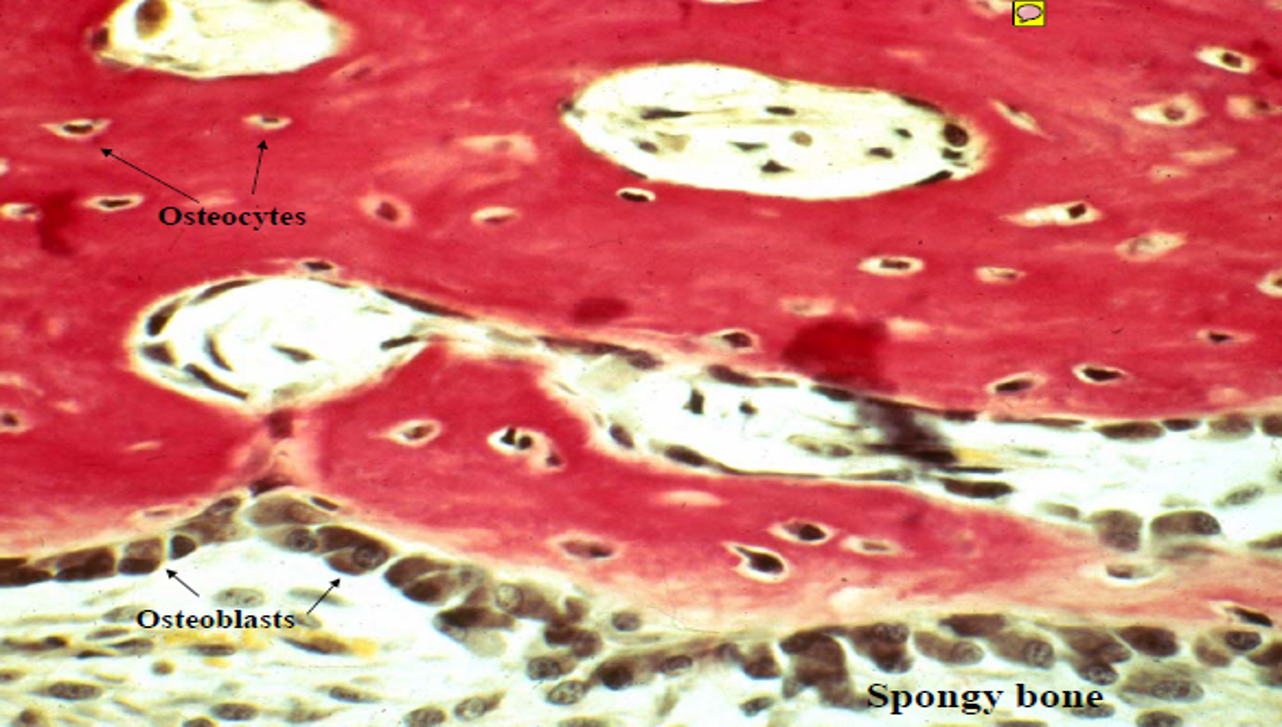
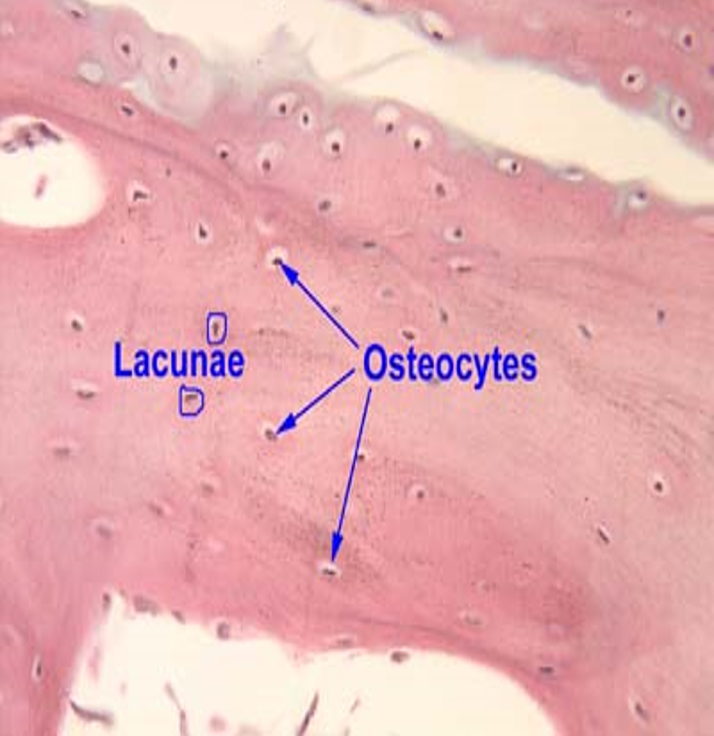
Osteocytes
Located in lacunae
Do not secrete matrix material
Function:
Extend cytoplasmic processes through canaliculi for nutrition
Exchange of nutrients and waste with blood supply
Death of osteocytes will lead to bone resorption
Communicate by gap junctions
Osteocytes
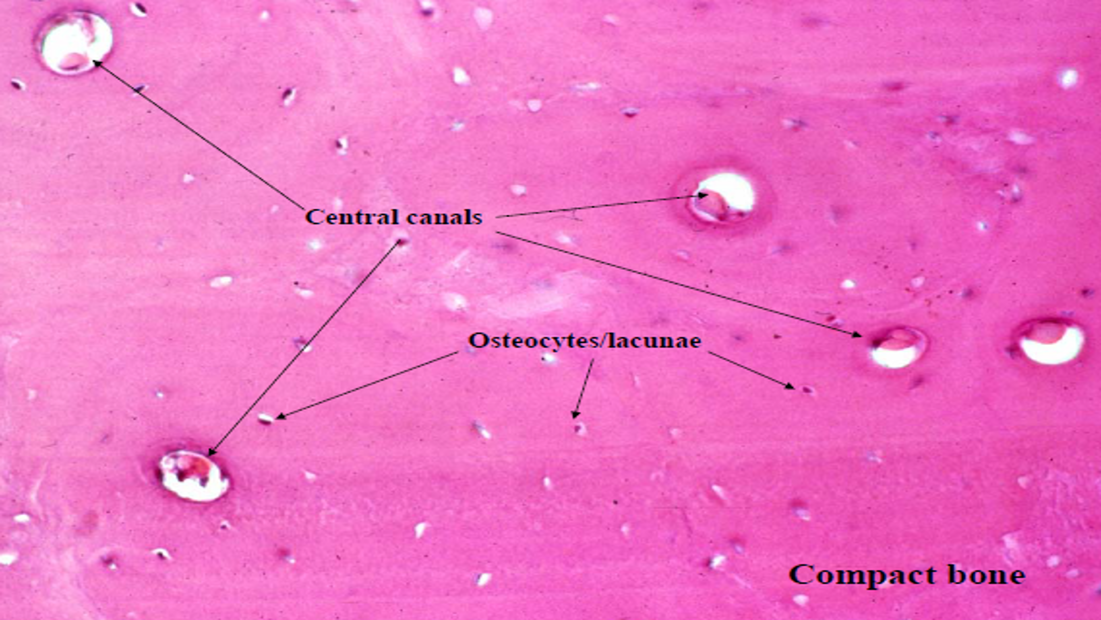
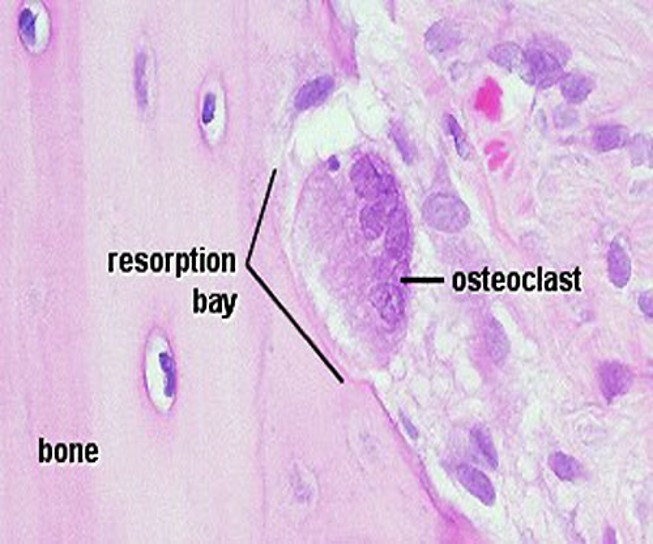
Osteoclasts
Found on bone surface
Large, multinucleated, branched, motile cells
The surfacing matrix have projections > ruffled border
Contain many lysosomes, many mitochondria
Found in Howship’s lacunae
Phagocytic
Function:
Involved with bone growth, maintenance, and bone repair
Release lysosomes into extracellular space, phagocytic, remodeling
Osteoclasts
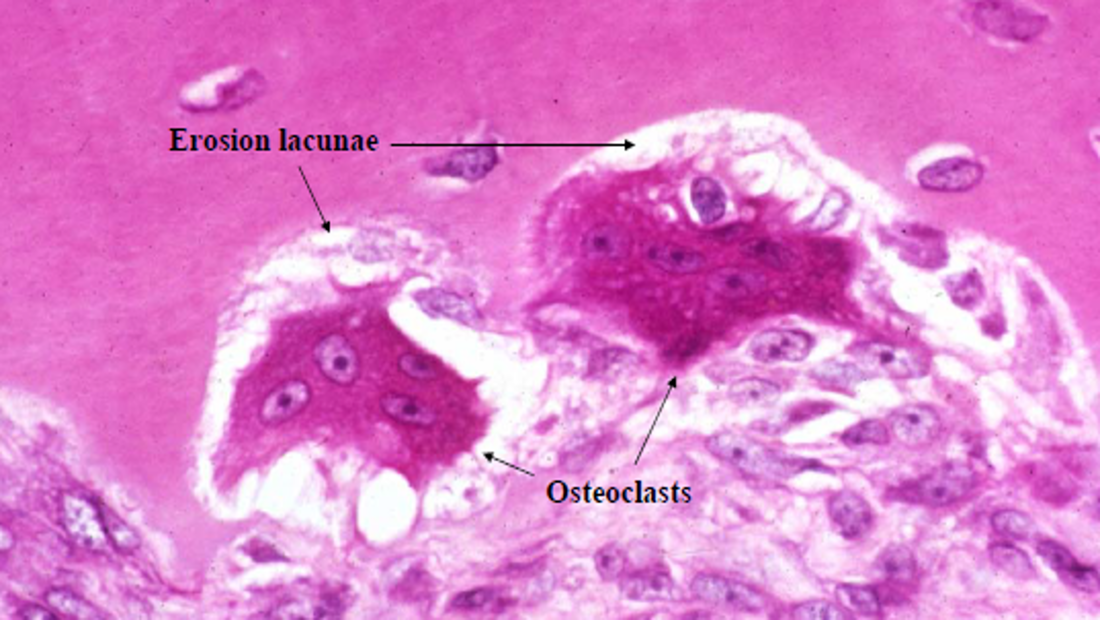
Osteoclasts
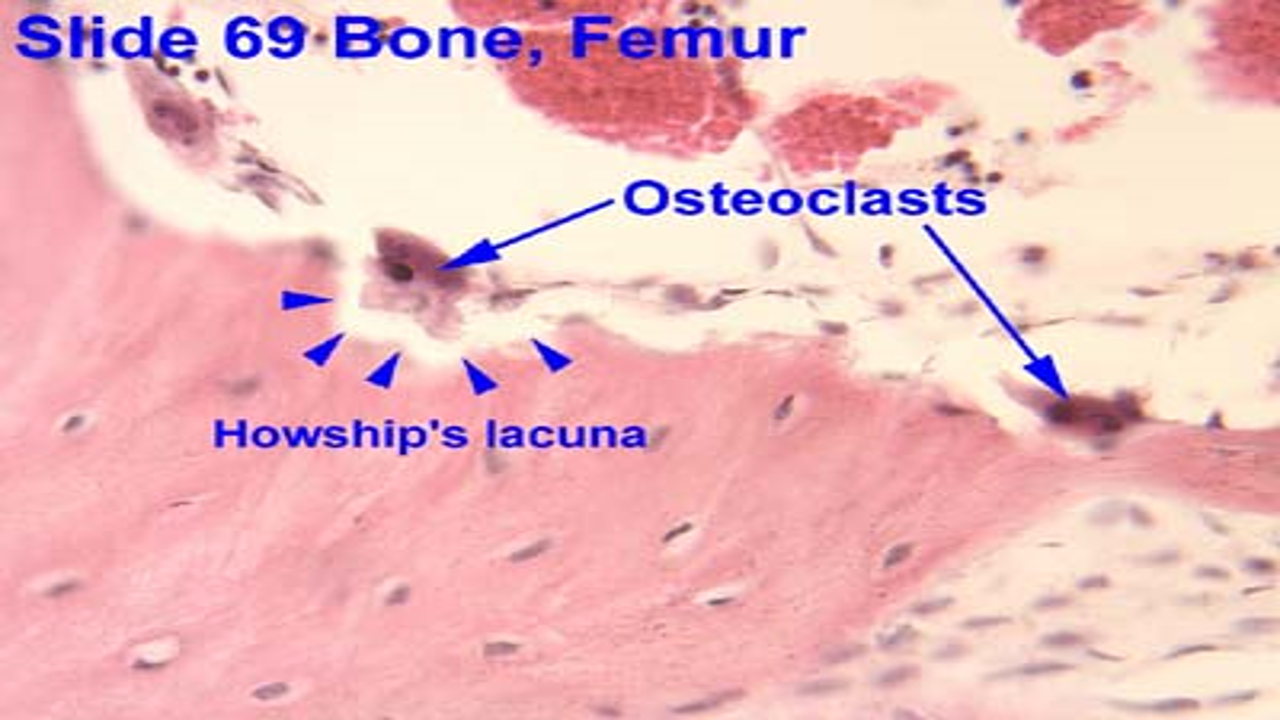
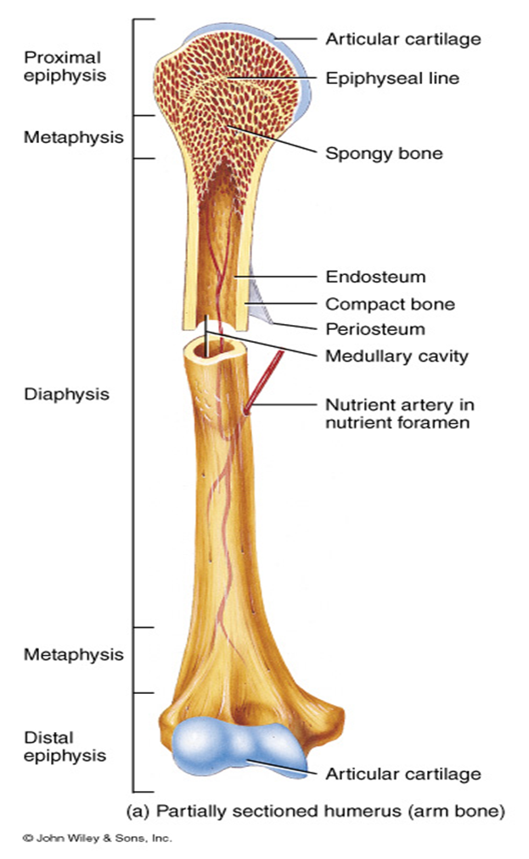
Bone Anatomy
Diaphysis : shaft of bone
Epiphysis: ends of bone
Epiphyseal Plate: Growth plate
Metaphysis: between epiphysis and diaphysis
Medullary cavity
Periosteum
Endosteum
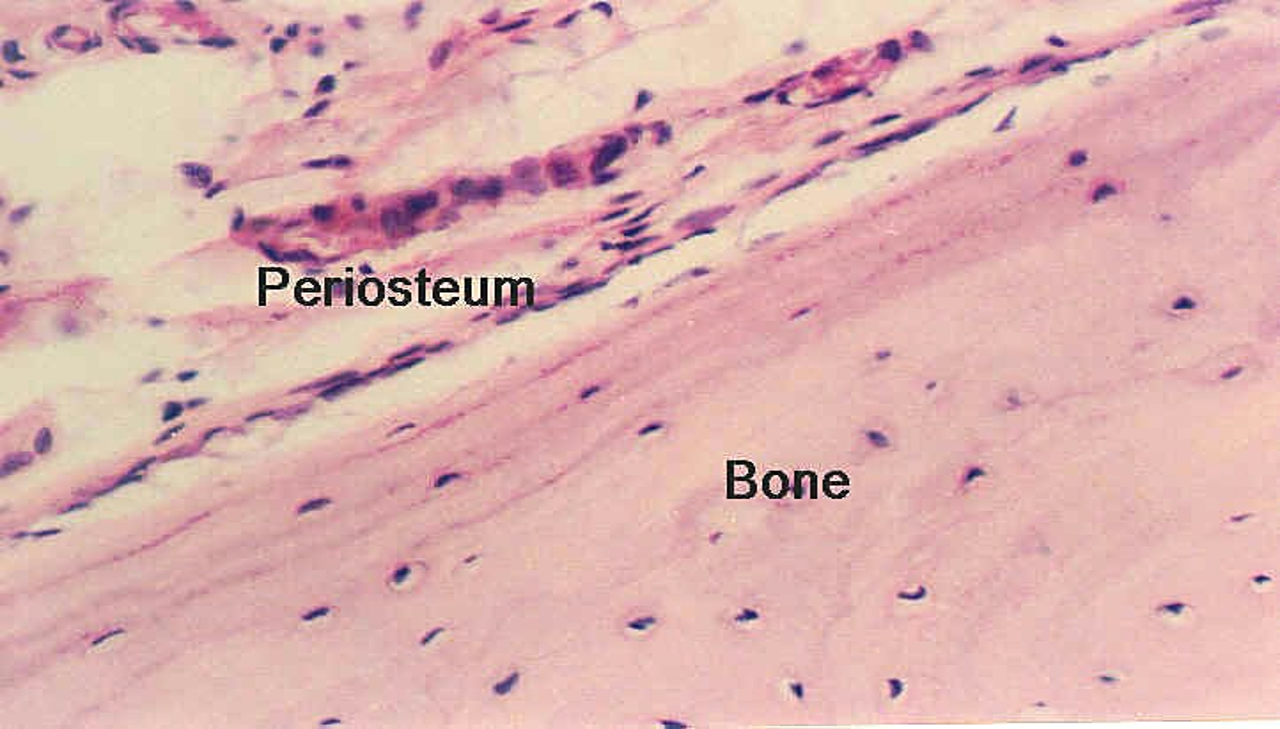
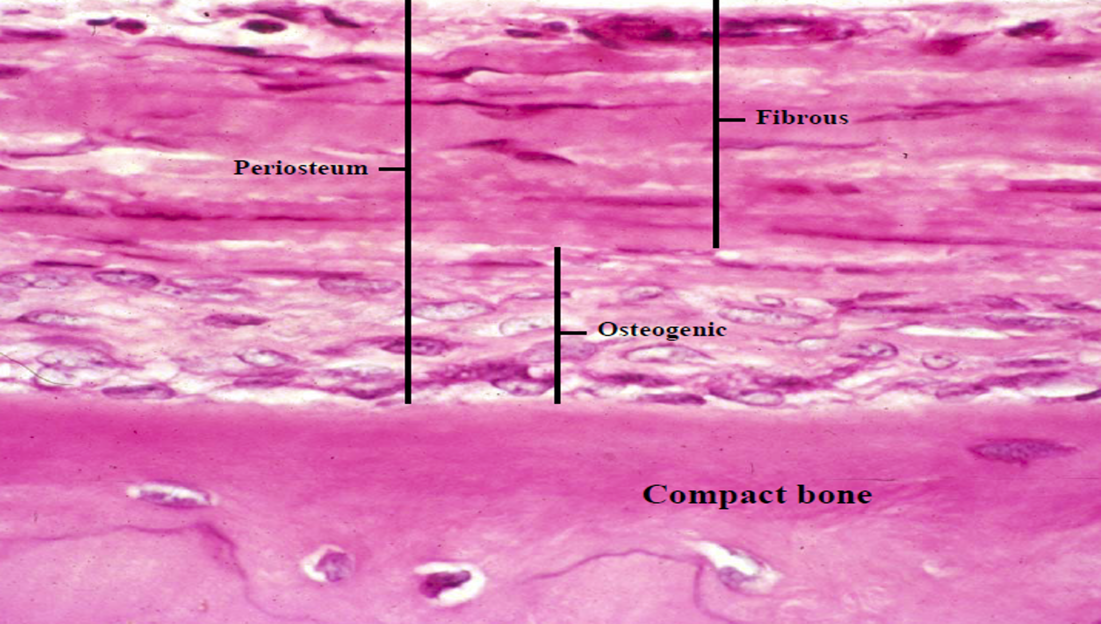
Periosteum
Dense connective tissue covering bone
Outer fibrous layer
Inner cellular layer (osteoprogenitor cells)
Collagen fibers extend directly into the bone
Nutrient foramina
Periosteum
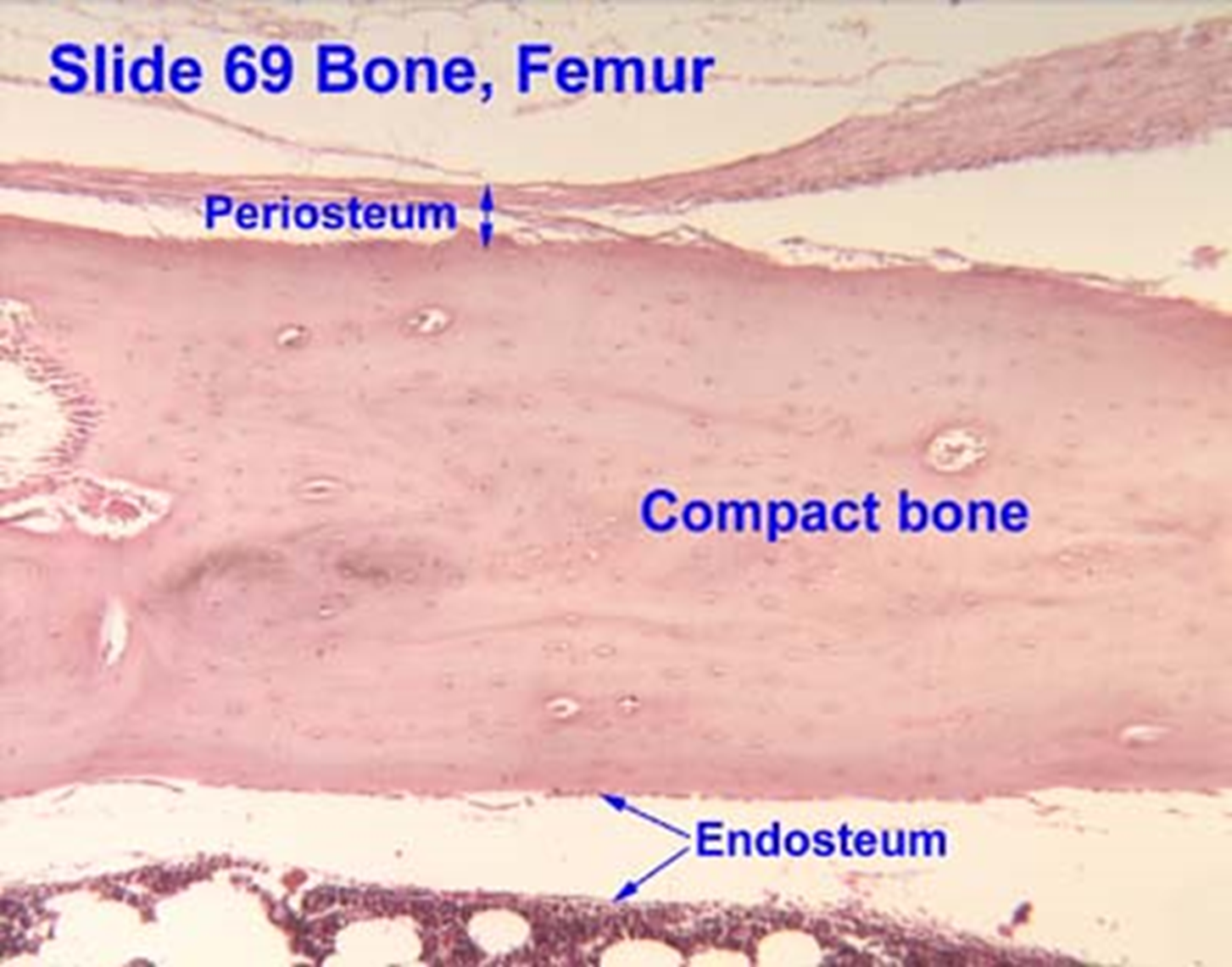
Endosteum
Inner lining of compact and spongy bone facing medullary cavity.
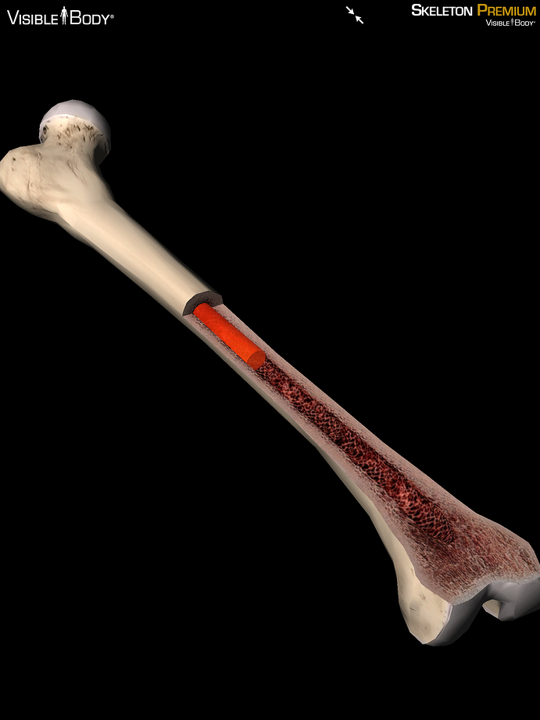
Medullary Cavity
Hollow chamber in bone
Contains
Red marrow produces blood cells – high activity
Yellow marrow of adipose – low activity
Osteon
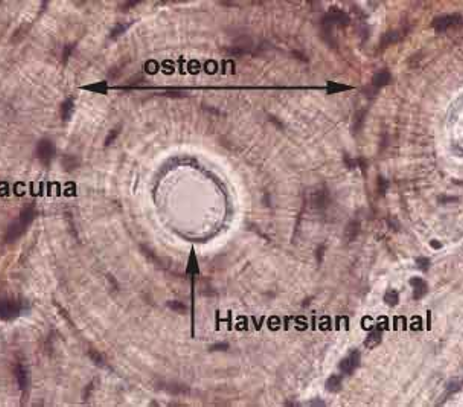
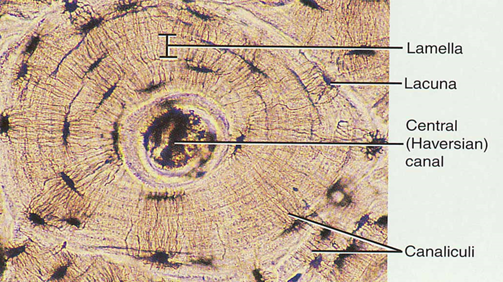
Compact Bone
Lacunae are connected to one another by canaliculi
Osteon contains:
Central Canal (Haversian canal)
Surrounding lamellae
Lacunae
Osteocytes
Canaliculi
Volkmann’s Canal: horizontal canal that connects the central canals
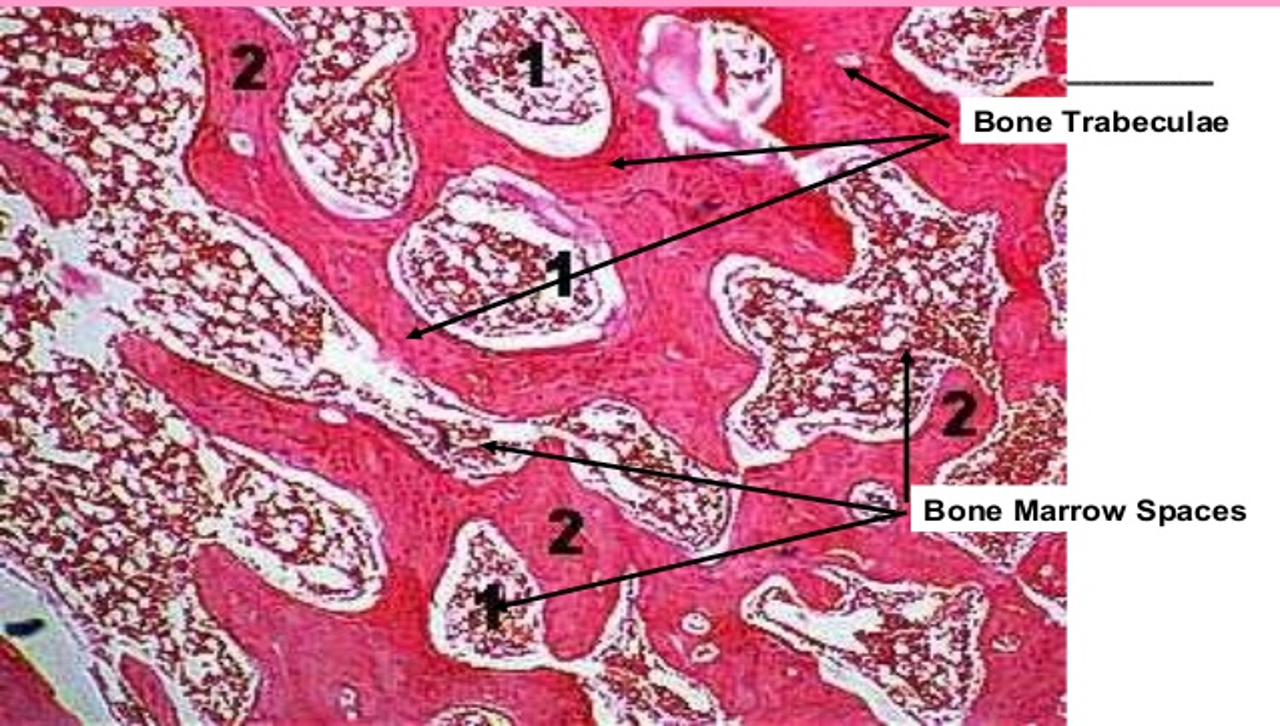
Spongy Bone
Internal layer of bone, marrow cavity
Trabecular bone tissue forming a meshwork
Filled with red and yellow bone marrow
Osteocytes get nutrients directly from circulating blood