human pathology exam 3 content
1/149
Earn XP
Description and Tags
vascular and pulmonary
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
150 Terms
hypertension (definition + level)
high blood pressure, 130/80 mm Hg and higher signifies high blood pressure
hypertension shorthand
htn
how many cases of primary hypertension are idiopathic?
95%
what are the causes of primary hypertension?
obesity
stress
lack of activity
high sodium diet
age
race
what is secondary hypertension caused by?
renal artery stenosis (renovascular hypertension) (stenosis = narrowing). stenosis decreases blood to the kidney, stimulating the renin-angiotensin system, further increasing B.
fibromuscular dysplasia of blood vessels is a defect in the blood vessel wall, causing arteries to thicken (renal and carotid artery), “string of pearls sign”
atherosclerosis in the elderly
what is the string of pearls sign caused by?
fibromuscular dysplasia of blood vessels that causes arteries to thicken
arteriosclerosis
hardening of arteries
what are the three forms of arterioscleoris?
atherosclerosis
arteriolosclerosis
Monckeberg’s medial calcific sclerosis
atherosclerosis definition/process
fatty plaque develops in the intimal layer of large and medium arteries
excess lipids leak into intimal layer
lipids are oxidized and are attacked by macrophages causing an inflammatory response
fatty plaque structure
fatty plaque has a necrotic lipid core made of cholesterol surrounded by a calcified fibrous capsule
what arteries are most commonly affected by atherosclerosis?
abdominal aorta, coronary arteries, internal carotid artery, and popliteal
causes of atherosclerosis
elevated LDL (hypercholesterolemia), low HDL, smoking, and diabetes
complications of plaque formation lead to (regarding atherosclerosis)
stenosis of blood vessel and ischemia
plaque will rupture with thrombosis (myocardial infarction)
plaque ruptures with embolization (atherosclerotic emboli)
weakens vessel wall causing aneurysm
atherosclerotic emboli
plaque ruptures with embolization
arteriolosclerosis (the subtype)
narrowing of small arteries
two types: hyaline and hyperplastic
hyaline arteriosclerosis
formed when proteins leak into vessel wall causing thickening of vessel wall
hyperplastic arteriosclerosis definition
it is hyperplasia (increase # of cells) of the tunica media of the blood vessel, “onion skin” appearance.
what can hyperplastic arteriosclerosis cause?
malignant hypertension
end organ ischemia
kidney necrosis with hemorrhage
Monckeberg’s medial calcified necrosis
calcification of the tunic media; not clinically significant as it’s an incidental finding on a plain film xray.
thoracic aortic aneurysm (TAA)
the aortic wall weakens and balloons out.
can cause aortic root dilation and aortic valve insufficiency, can push on other mediastinal structures
seen in tertiary syphilis, aortic trauma, Marfan’s syndrome, and age
abdominal aortic aneurysm (AAA) definition
fatty plaque buildup and blood clotting will cause pressure against the vessel wall, weakening it and causing its dilation.
dilation of of the abdominal aorta inferior to renal arteries, but superior aortic bifurcation (into common iliacs).
risk for rupturing (>5cm) increases overtime.
what is primary cause of abdominal aortic aneurysm?
atherosclerosis typically seen in hypertensive males over the age of 60; smokers.
is abdominal aortic aneurysm primary asymptomatic or symptomatic?
asymptomatic
how does abdominal aortic aneurysm present?
presents as pulsating abdominal mass when aorta is palpated. pulsation will come up to meet your fingers from deep to superficial.
how to palpate abdominal aorta
go 1 inch up and 1 inch to the left of the umbilicus and push down on that spot.
what is width once abdominal aorta ruptures and what does it immediately cause?
>5cm
hypotension, pulsating mass, flank pain
fusiform aneurysm
spindle-shaped aneurysm
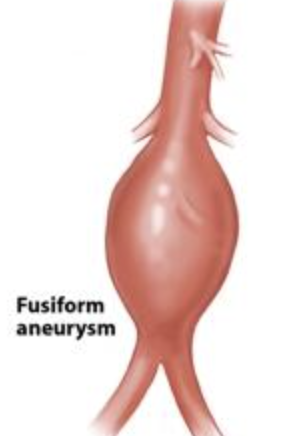
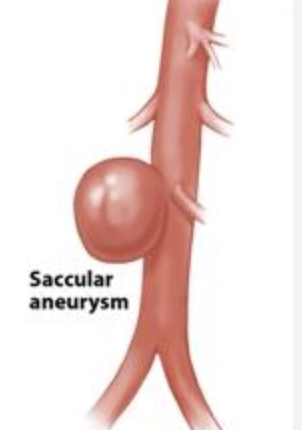
saccular aneurysm
looks like sac
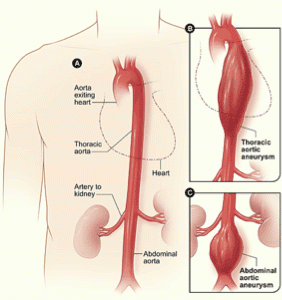
remember this picture for thoracic vs abdominal aortic aneurysm
aortic dissection definition
tear located in the tunic initima with blood surging between the intimal and medial layers.
occurs in the proximal 10cm of the aorta (highest stress point).
pain presents with searing, tearing chest pain that radiates to the back
complications of rupture are death
causes of aortic dissection
in older patients: hypertension
in younger patients: defect in connective tissue (Marfan’s Syndrome)
what are the upper respiratory tract disorders?
rhinitis
nasal polyps
singer’s nodule
croup
laryngeal carcinoma
rhinitis
caused by inflammation of the nasal mucosa typically seen by an adenovirus.
seen with common cold and allergies. seen in patients with asthma and eczema.
symptoms: rhinorrhea (nose discharge), sneezing, and congestion
nasal polyps
inflamed and edematous nasal mucosa (swelling of inner nose lining).
seen in patients with cystic fibrosis, aspirin-intolerant asthma, and aspirin induced bronchospasms and nasal polyps.
nasal polyps are seen in 10% of asthmatic adults
Singer’s nodule
arises on the true vocal cords and are non-neoplastic. occurs bilateral (on both sides) and is an overuse injury.
presents with hoarseness of the voice, 50% of cases require surgery
anatomical space where Singer’s nodules arise
Reinke’s space
the tighter the vocal cords the _____ the pitch
higher
croup (laryngotracheobronchitis)
caused by parainfluenza virus.
patient presents with a barking cough, hoarse voice, and inspiratory stridor (high-pitched sound made upon inspiration)
worse at night
stridor is primarily _____?
inspiratory
if stridor is heard both during inspiration and expiration, it is called ____?
biphasic
laryngeal carcinoma
squamous cell carcinoma that arises from the epithelial lining of the vocal cords.
can be caused by alcohol and tobacco use
presents with hoarseness, stridor, and cough
use the bell of the stethoscope to hear what?
blood flow through artieries
low frequencies
use the diaphragm of stethoscope to hear?
breathing sounds
high pitch
where is the apex of the lung?
supraclavicular fossa
what are the auscultation points for lungs?
apices, superior lobes, middle lobes, inferior lobes
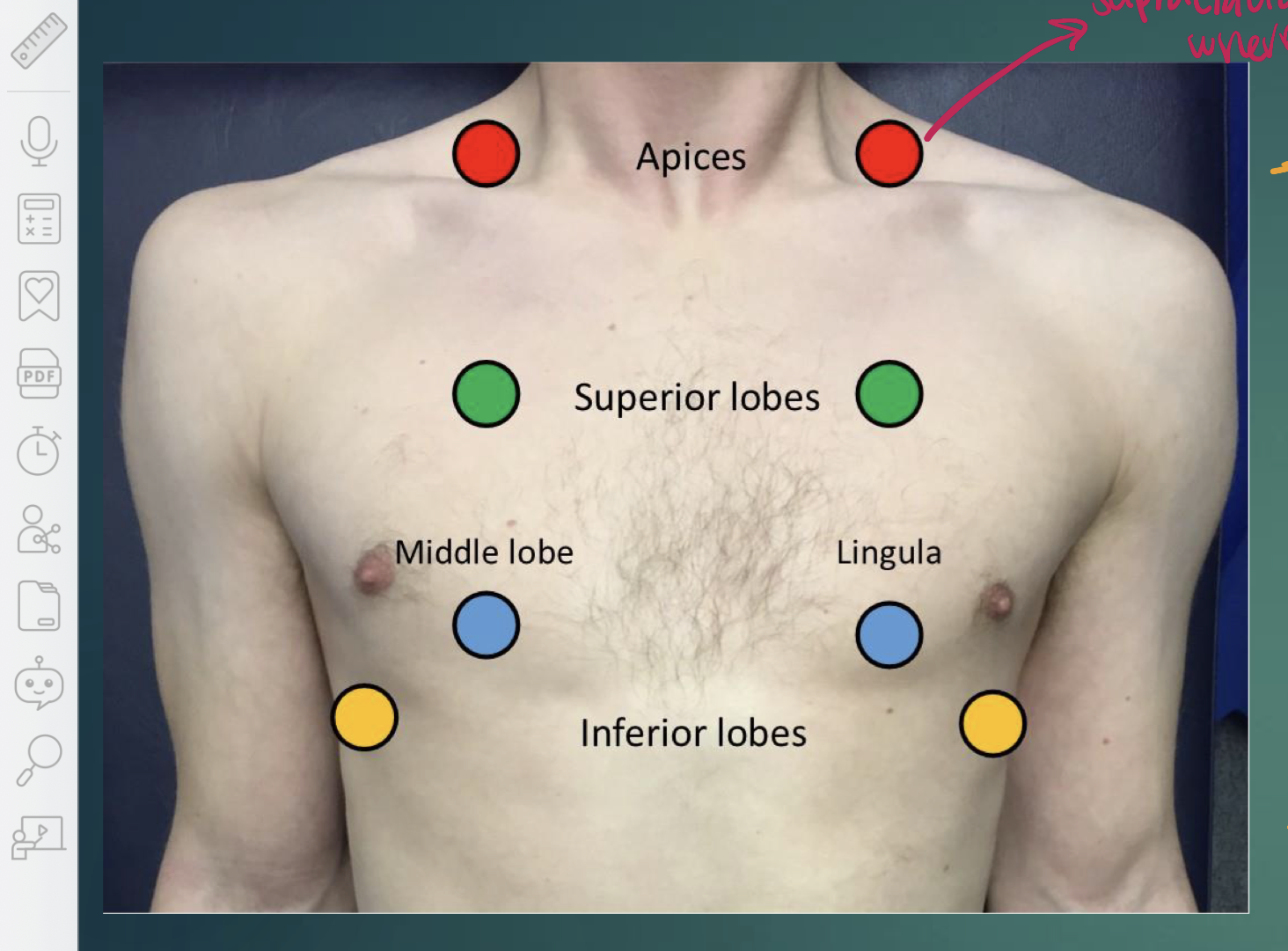
triangle of auscultation on back borders
superior border: trapezius
inferior border: latissimus dorsi
lateral border: scapula/medial border
which bronchi is larger?
right primary bronchi
abnormal lung sounds are:
rhonci
rales (crackles)
wheezes
stridor
rhonci definition
low-pitched rattling noises, like snoring
caused by inflammatory secretions or obstructions in the large airways (trachea + bronchus). occurs when air leves trachea and hits secretion or mucus.
in what disorders is rhonci seen in?
pneumonia and COPD
fine rales (crackles)
higher-pitched popping noise heard upon inspiration like crackling cellophane.
these sounds are discontinuous, individual sounds
caused by fluid in smaller airways like bronchioles or alveoli
course rales (crackles)
lower-pitched popping noise heard upon inspiration. located in large airways like bronchi
occurs when patients try to breathe but large airways are partially blocked by mucus
sounds like gurgling.
conditions where fine rales are heard
CHF, atelectasis, pneumonia
conditions where course rales are heard
heart failure due to pulmonary edema, pneumonia, bronchiectasis, infections that result in mucus secretions.
wheezes
high-pitched whistling sounds resulting in narrowing of the bronchial tree as seen in asthma.
mainly heard on expiration, located throughout respiratory system. sound occurs because of narrow airways
conditions where wheezes can be heard
asthma, COPD, lung infections that can narrow airways
stridor
high-pitched wheeze dependent on if it occurs during inspiration or expiration. occurs in upper respiratory tract. occurs due to narrowing of larynx and trachea bc of swelling or blockage
conditions where stridor occurs
epiglottis, croup, anaphylaxis, obstruction
pleural friction rub
low pitch, found in pleura layers. harsh grating sound + pain during breathing or cough.
occurs when pleura layers get inflamed and rub up on each other (usually there’s a space between pleura)
in what conditions can pleural friction rub be found in?
pleurisy, pneumonia, tuberculosis
bronchophony
patient told to say 99 when stethoscope touches them.
it’ll sound muffled NORMALLY. If there’s an area of consolidation (like pneumonia), the 99 will sound clearer
egophony
patient told to say “E".” Normally you’ll hear eeeee. If there’s areas of consolidation (abnormal), it’ll sound like ahhhh or ehhhh
whispered pectorilaquy
tell patient to whisper 99. areas of consolidation will make the whisper louder
tactile fremitus
use your hand, put palm to patient, have them say 99. touch their back to feel vibrations, should be equal or symmetrical. different vibration is abnormal
lower respiratory disorders
pneumonia
tuberculosis
mesothelioma
emphysema
pneumonia (definition)
infection found in the lung parenchyma, occurs when normal pulmonary defenses are weakened.
pneumonia symptoms
fever, chills, cough producing thick yellow/green (pus) sputum, rusty colored sputum indicates blood (hemoptysis), fast breathing rate (tachypnea), chest pain, SOB, elevated WBC, dullness to percuss and decreased breath sounds
hemoptysis
coughing off blood, associated with pneumonia
tachypnea
fast breathing rate, occurs in pneumonia because body is trying to get more oxygen in
how to diagnose pneumonia?
chest x-ray, sputum culture with gram stain, and blood culture
three forms of pneumonia (found by x-ray)
lobar pneumonia
bronchopneumonia (bacterial)
interstitial pneumonia (viral)
lobar pneumonia
consolidation (fills with fluid or dense stuff) of an entire lobe of lung.
occurs in the intra-alveolar space.
caused by two main bacteria: Streptococcus pneumoniae (95%) and Klebsiella pneumoniae)
gross changes/phases of lobar pneumonia
congestions due to edema and inflammation in the first 24 hrs
red hepatization: alveolar air space fills with neutrophils, bloody exudate, and fibrin. red cells extravasate intra-alveolar space
gray hepatization: red cells hemolyze (RBCs rupture) within exudate
resolution
what does grey hepatization look like?
lung tissue becomes firm, airless, and liver-like. caused by alveoli filling with fluid and cells. starts “red” early and then “grey” later.
S. pneumoniae (hint: s for senior citizen)
community-acquired pneumonia, seen in middle age and elderly population
K. pneumoniae
individuals who are malnourished and debilitated (elder care homes), caused by alcoholism and diabetes. presents with “currant jelly” sputum
bronchopneumonia
characterized by scattered and patchy consolidations around the bronchioles. multifocal and bilateral, this pneumonia can cross multiple lobes
bacteria that can cause bronchopneumonia
Staphylococcus aureus - typically superimposed on a viral upper respiratory tract infection
Haemophilus influenza - COPD
Pseudomonas aeruginosa - cystic fibrosis
pulmonic exams for pneumonia
1. Tactile Fremitus
2. Bronchophony/Egophony
3. Whispered Pectroliquy
interstitial (atypical) pneumonia definition
Scarring in tissues around alveoli
interstitial (atypical) pneumonia causes
etiological agents:
influenza virus: high risk for immunocompromised elderly
mycoplasma pneumoniae: most common type of atypical pneumonia, found in college students (from dorms); “walking pneumonia”
respiratory syncytial virus (RSV) - most common atypical pneumonia in infants
MRSA - methicillin resistant staphylocuccus aulcus definition
can decrease macrophage ability in air sacs. virus suppresses immune system by suppressing macrophages
to get full chest x-ray, which way does it go?
posterior to anterior
what are the forms of tuberculosis and what causes tb?
two forms: primary and secondary
caused by the inhalation of aerosolized mycobacterium tuberculosis
primary tb process
M. tuberculosis is inhaled deep into lungs. immune response initiated and alveolar macrophages begin to engulf the bacteria
M. tuberculosis secretes a protein SapM that prevents the lysosome in the macrophage from fusing with the phagosome containing the bacteria. the bacteria begin to multiply and produce a mild infection.
at this point, patient is asymptomatic or exhibits mild flu-like symptoms.
3 weeks post-infection, cell-mediated immunity will wall off the infection producing a granuloma (tuberculoma), which will hide the bacteria from the immune system. the center of the granuloma dies and appears as caseous necrosis (Ghon’s focus)
bacteria get transported to nearby lymph nodes. these lymph nodes undergo fibrosis and calcification. the lung granulomas (Ghon’s focus) and fibrotic lymph nodes combines are called a Ghon’s complex.
The Ghon’s complex produces calcified scar tissue that can be seen on plain-film xray. this scar tissue is called Ranke’s complex
immune system can destroy tb or it can become dormant
granuloma
a small, localized cluster of immune cells (macrophages) that forms to wall off foreign substances, infections (ex: TB)
Ghon’s focus
when the center of the granuloma (tuberculoma) dies and appears as caseous necrosis
process to Ranke complex (simplified)
granuloma (tubercolumo) → Ghon’s focus → Ghon’s complex → Ranke complex
Ranke complex
when Ghon’s complex becomes calcified scar tissue that can be seen on xray and becomes this new complex
Ghon’s complex
when the lung granuloma (Ghon’s focus) and fibrotic lymph nodes combine.
how many tb cases are primary?
90%
how long can tb be dormant for?
2 years
how many tb cases are secondary tb?
5-10%
secondary tb process
if immunocompromised (AIDS, organ transplant, IVDU - IV drug use, or aging), the tb reactivates and travels to upper lobes of the lung where there os greater oxygenation bc bacteria wants the oxygen
memory T-Cells release cytokines causing more infectious caseous necrosis.
tissue cavitates (bubbles form) and bacteria spread through lymphatic drainage and airways causing bronchopneumonia. the patient is infectious as they cough.
tb can enter the vascular system and become system (systemic miliary TB)
systemic miliary tb
when TB enters the vascular system and becomes systemic
structures affected by systemic miliary tb
kidneys - sterile pyuria (pus) with high WBC count
cervical lymph nodes - lymphadenitis (inflamed lymph nodes - scrofula)
adrenal glands: Addison’s disease (adrenal hypofunction)
lumbar vertebrae - Pott’s disease
meninges - meningitis
liver - hepatitis
scrofula
inflamed lymph nodes
signs and symptoms of tb
hemoptysis
coughing that lasts three or more weeks
chest pain or pain w/ breathing or coughing
SOB
fatigue
night sweats
unintentional weight loss
fever
chills
scrofula
Pott’s disease
causes severe back pain + vertebral deformity
how to test for TB?
PPD (purified protein derivative) - Mantoux test. inject stuff into the skin, if it becomes firm, it’s a positive result. results interpreted based on firmness
tine test
IGRA - blood test that detects TB protein, very efficient, does not give false positive even if patient has the BCG vaccine to prevent tb. patient doesn’t need to return to get results