chapter 11,12,14
1/82
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
83 Terms
Explain mucociliary clearance as defense in the respiratory system.
Mucociliary clearance is a vital defense mechanism in the respiratory system that protects the lungs by trapping and removing inhaled particles, pathogens, and debris. (with mucus and cilia)
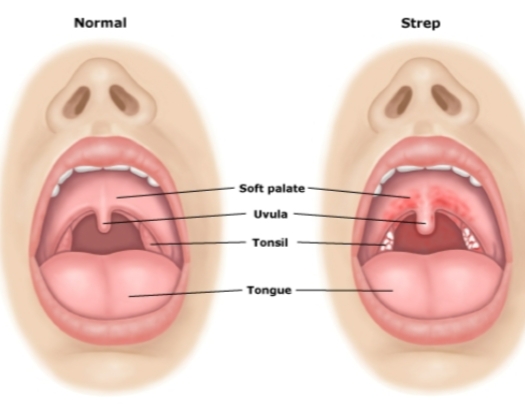
Streptococcal pharyngitis a. Causative agent: b. Transmission: c. Symptoms: d. What is its hemolytic reaction? e. Lancefield classification: f. Significance of pili and capsule g. M protein: h. Scarlet fever: i. Erythrogenic toxins: j. What is rheumatic fever and rheumatic heart disease?
Caused by Streptococcus pyogenes
Group A (Lancefield classification)
Beta-hemolytic
spreads through respiratory droplets
Virulence factors
Capsule
Pili
Symptoms include high fever, inflamed pharynx, coughing, swollen lymph nodes in neck, and swollen tonsils.
The organism secretes toxin that damages pharyngeal cells.
Recovery is hastened by antibiotics.
Scarlet fever is strep throat with a rash.
Rash caused by erythrogenic toxins.
Toxins cause bleeding in the skin.
Rheumatic fever is a serious complication.
Fever and pain
Heart tissue inflammation
Heart valve damage
A hemolytic reaction especially beta is a complete break down of red blood cells.
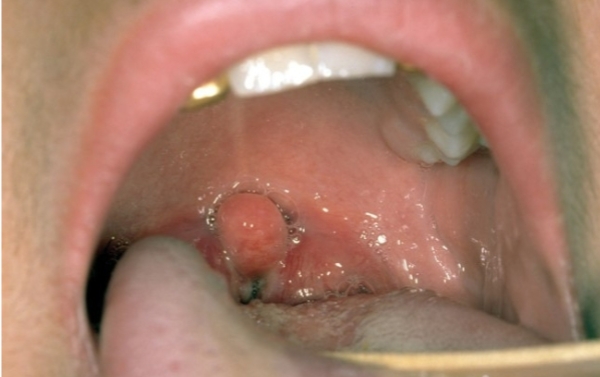
Diphtheria a. Causative agent: b. Transmission: c. What is the action of the exotoxin? d. Symptoms: e. What is the pseudomembrane? f. Treatment: g. Prevention:
Caused by Corynebacterium diphtheriae
Symptoms due to exotoxin
Exotoxin inhibits protein synthesis in epithelial cells by inactivating 80 S ribosomes.
Combination of dead tissue, WBCs, and scar tissue form pseudomembrane
Pseudomembrane can cause airway blockages.
Air passageway may swell shut.
Treated with antibiotics and antitoxin
Prevented by DTaP vaccine
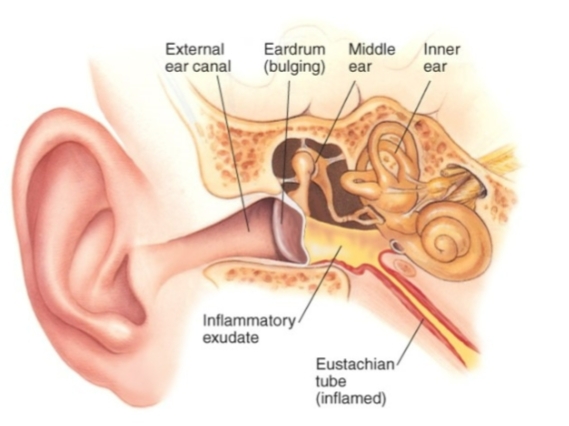
How do bacteria of the URT reach the middle ear to cause otitis media?
Acute otitis media—middle ear infection
Bacteria from URT can gain entry to middle ear by Eustachian
(auditory) tube.
Bacteria from the upper respiratory tract reach the middle ear by traveling through the Eustachian tube, which connects the nasopharynx to the middle ear. When this tube becomes blocked or inflamed, pathogens can move upward and cause otitis media.
Common cold: a. Causative agent: b. Transmission: c. Symptoms:
Rhinoviruses cause the commoncold.
Virus transmitted by respiratory droplets or fomites
Symptoms:
Sneezing
Sore throat
Runny or stuffy nose
Mild aches and pains
Hacking cough
Illness lasts between 7 to 10 days.
Virus transmitted by respiratory
droplets or fomites.
More common in fall and spring
Whooping cough a. Causative agent: b. Transmission: c. What is the physiological action of the major exotoxin? i. Stages of disease 1. Catarrhal stage 2. Paroxysmal stage 3. Convalescent stage ii. Treatment: iii. Prevention:
Caused by Bordetella pertussis
Whooping cough (pertussis) is transmitted through respiratory droplets.
Most important exotoxin immobilizes cilia
More severe in small children
Catarrhal stage:
Buildup of excessive discharge in respiratory tract
Most contagious stage
Paroxysmal stage:
Dead cells and mucus accumulation over 2–4-week period
Labored breathing
Spasmodic coughing due to paralyzed cilia; can’t eliminate mucus
Rapid-firing coughs in one exhalation followed by high-pitched whoop.
This is due to forced inhalation over a partially closed glottis.
Convalescent stage:
Persistent coughing decreases
Treated with antibiotics
Prevented by DTaP
Increasing due to:
Not getting vaccinated
Immunity declines of time
Evolution of resistant strains
Influenza a. Causative agent: b. Transmission: c. Symptoms: d. Role of hemagglutinin (H) spike: e. Role of neuraminidase (N) spike: g. How does integrated pig-duck farming contribute to pandemic strains. h. What are the characteristics of influenza A virus? i. What causes most of the deaths due to influenza? Who is the most vulnerable?: k. Prevention: l. Treatment:
Influenza is caused by the influenza viruses, primarily Influenza A and Influenza B, which are responsible for seasonal flu epidemics.
Influenza is transmitted mainly through respiratory droplets
Two spike proteins are found in envelope:
Hemagglutinin: for attachment & penetration
Neuraminidase: for release from host cell Virus attacks epithelial cells of nasopharynx and tracheo-bronchial tree.
Most pandemic strains arise in southern Asia due to integrated pig-duck farming. Pigs are a reassortment vessel since they can be infected with avian, human and swine strains.
Influenza virus characteristics:
Orthomyxoviridae
ssRNA, helical, enveloped
Each strand is surrounded by a nucleocapsid protein.
Matrix protein surrounds core RNA segments
Symptoms of influenza:
Incubation period 1-4 days
Chills
Fatigue
Headache
Fever can rise to 40 degrees C
Pain most pronounced in chest, back, and legs
Sore throat
Nasal congestion
Sneezing
Tight chest
* Most flu deaths are caused by spread to the lungs or secondary bacterial pneumonia.
*Most susceptible groups include infants, small children, elderly, and immunocompromised.
Influenza is prevented with vaccines (People that are allergic to chickens or eggs are not recommended to take this vaccine)
Treatment:
Several antiviral agents can lessen the course of infection:
Zanamivir (Relenza)
Oseltamivir (Tamiflu)
Both drugs target N spikes and block viral release.
Covid-19 a. Causative agent: b. Transmission: c. Symptoms: d. Complications: e. Prevention: f. treatment
Caused by SARS-CoV-2 virus
Spread by respiratory route or fomites.
Symptoms:
Temporary loss of taste and smell
included fever, dry cough, and difficulty breathing
Virus multiplies in the pneumocytes of the alveoli
Alveolar infection triggers cytokine release, causing fluid buildup
Complications:
can cause complications affecting nearly every organ system, including the lungs, heart, brain, kidneys, blood vessels, and long‑term post‑viral syndromes such as Long COVID.
Prevention:
Three vaccines are used in the United States
Treatment:
Treatment includes remdesivir, dexamethasone, and antibody treatments
Tuberculosis a. Causative agent: b. Acid fast c. Transmission: d. Symptoms: e. Distinguish between latent tuberculosis and active tuberculosis. f. How is the tubercle formed? g. What is miliary tuberculosis? h. What is the Mantoux or tuberculin test? What is induration? What does a positive tuberculin test indicate? What is the next step after a positive tuberculin test? i. What has made tuberculosis treatment precarious? j. Why are simultaneous infections of tuberculosis and HIV dangerous? k. What is BCG?
Caused by Mycobacterium
tuberculosis
Acid-fast bacillus
Waxy cell wall resistant to drying and
disinfectants
18 hour generation time
Tuberculosis was formerly known as
consumption.
Disease is a worldwide threat.
Factors that facilitate spread
Poor ventilation
Overcrowding
Malnutrition
AIDS
Infection is arrested in 90% who
become infected. This is called
latent tuberculosis.
This is due to the action of the immune
system and host defenses.
Infection progresses in remaining
10% of people.
This is called primary active
tuberculosis.
Secondary active tuberculosis occurs
when someone with latent TB has a
change in immune status.
85% of infections are respiratory.
Respiratory symptoms:
Fatigue
Chronic cough
Difficulty breathing
Chest pain
Spitting up bloody sputum
Fever
Night sweats
Weight loss
Miliary tuberculosis occurs when
infection spreads from the primary site
into secondary sites
What are common causes of nosocomial pneumonia?
Pneumococcal pneumonia a. Causative agent: b. Transmission: c. Symptoms: d. What is a typical pneumonia? e. Who is at risk? f. Treatment: g. Prevention:
Caused by Streptococcus
pneumoniae
Gram-positive
Diplococci
Encapsulated
Over 90 capsular serotypes
Causes 80% of serious pneumonia
Organism resides in upper respiratory
tract
May invade lower respiratory tract
Risk groups include infants, elderly,
alcoholics, malnourished, &
immunologically compromised
Typical pneumonia
Symptoms include high fever, sharp
chest pains, difficulty breathing, and
rusty sputum
Pneumonia involves the alveoli of the
lungs. The infection can impair
respiratory gas exchange.
Damage to respiratory membrane can
allow fluids to leak in alveoli, displacing
space for air or causing collapse.
Treated with antibiotics
Vaccines are available
Mycoplasma pneumonia a. Causative agent: b. Transmission: c. Symptoms: d. What is atypical pneumonia? e. What is unique about Mycoplasma? f. Why isn’t penicillin effective? g. Treatment:
Caused by Mycoplasma
pneumoniae
No Gram reaction
No cell wall
No sensitivity to penicillin
Tiny bacterium about 0.2 micrometers
Pleomorphic cells
Fried egg-like colonies
Atypical pneumonia
Symptoms include chronic cough,
low-grade fever, fatigue, and
headache
Common in institutional settings
Very contagious disease
Patients recover spontaneously
Recovery can be hastened by
antibiotics
Legionaire’s disease a. Causative agent: b. Transmission: c. Symptoms: d. What are the common sources of the organism? e. Treatment:
Caused by Legionella pneumophila
Gram-negative rod
Silver stain is best because of weak Gram-
reaction
Aquatic bacterium
Multiplies in amoebae
Biofilm-former
Name was given after outbreak at
American Legion convention in
Philadelphia in 1976. 221 affected, 34
died.
8000-12,000 hospitalizations each year
2-10 day incubation period
Person-to-person transmission does
not occur.
Common sources of bacteria: air
conditioning cooling towers, air
conditioners, humidifiers, hot-tubs,
and showers
Bacteria resistant to heat and
chlorine
Symptoms include coughing, fever,
chills, breathing difficulties
Necrotic pneumonia with
inflammation
Infects alveolar macrophages
Treated with antibiotics
Respiratory syncytial virus a. Causative agent: b. Transmission: c. Symptoms: d. Age class at risk: e. Cytopathic effect seen in infected cells: f. Treatment:
Causative agent is Respiratory
Syncytial Virus (RSV).
Paramyxoviridae, SS RNA, helical,
enveloped.
Common serious LRT infection of
infants and toddlers.
Virus causes pneumonia.
Infection is localized in bronchioles
and alveoli.
Virally-infected cells fuse to form a
giant multinucleate cell called a
syncytium.
95% of children under five have
been exposed to the virus.
Disease causes 75,000-125,000
hospitalizations each year.
4500 die
Treated with ribavirin
Fungal respiratory diseases, causative agent, symptoms, treatment a. Histoplasmosis b. Pneumocystis pneumonia c. Aspergillosis
HISTOPLASMOSIS
Causative agent is
Histoplasma capsulatum
Ascomycota
Common in Ohio River valley
80-90 % of people in this area react
positively to the histoplasmin
hypersensitivity test.
Thermal dimorphic fungus
Is a mold in the soil
Becomes a yeast in the body
PNEUMOCYSTIS PNEUMONIA
Causative agent is Pneumocystis
jiroveci
Formerly thought to be a protozoan
Has complex life cycle in the alveoli
of lungs
Transmitted by person-to-person
transmission by respiratory droplets
Commonly found in the alveoli of
humans and animals
Causative agents are Aspergillus
species, particularly A. fumigatus.
Mitosporic
Ascocomycota
Common mold in environment
May cause highly invasive
pulmonary and systemic infections in
immunocompromised individuals
Invades blood vessels
Causes endocarditis
Aspergillus fumigatus
ASPERGILLOSIS, CONT.
Another risk factor for aspergillosis
is inhaling an overwhelming number
of spores.
Aspergilloma is a round mass of
mycelium growing in the lungs.
Has to be surgically removed.
Aspergillosis is treated with
voriconazole.
Aspergilloma in lung
What are the differences among the following? a. Synthetic b. Antibiotic c. Semisynthetic
Synthetics are antimicrobial agents synthesized by chemists.
• Antibiotics are antimicrobial agents synthesized by microorganisms.
Most “antibiotics” are really semisynthetics. Base molecules,
synthesized by microorganisms, are modified by chemists.
• To increase effectiveness
• To target certain bacteria
What is selective toxicity? What is the toxic dose, therapeutic dose, and therapeutic window?
Selective toxicity states that the antimicrobial drug harms the pathogen, but not the patient.
• Therapeutic dose refers to the concentration of the antimicrobial drug that effectively destroys the pathogen.
• Toxic dose refers to the concentration of the antimicrobial drug that harms the patient.
• Therapeutic window is the concentration range of the antimicrobial drug that is tolerated by the patient but will eliminate the pathogen
What is the difference between a narrow-spectrum drug and a broad-spectrum drug?
Broad-spectrum drugs affect a large range of bacteria.
Narrow-spectrum drugs affect a small range of bacteria.
What are the common sources of antibiotics?
Bacteria
• Streptomyces and closely-related Actinobacteria
• Bacillus
Fungi
• Penicillium chrysogenum
• Cephalosporium acremonium
List the roles of antibiotics in microbial communities?
Functions of antibiotic production is
multidimensional, beyond microbial
weapons.
• Other functions include:
• Chemical cues
• Synergistic signals to induce
cooperation
• Competitive manipulators to allow
some species to flee to avoid
competition
What is an antimetabolite? What is the mode of action of sulfa drugs? What kind of enzyme inhibitor are sulfa drugs?
Antimetabolites are synthetic drugs that
Sulfonamide drugs act as competitive inhibitors of a bacterial enzyme involved in folic acid synthesis.
• target key microbial enzymes.
What is the mode of action of quinolone drugs? Name some examples.
Quinolone drugs are synthetic.
They interfere with DNA gyrase that is needed to unravel the double helix during replication.
• Examples are levofloxacin and ciprofloxaci
What is the primary physiological target of penicillin and cephalosporin drugs? What are the advantages of cephalosporin drugs over penicillin drugs?
Penicillins target cell wall synthesis.
Cephalosporin drugs target cell wall synthesis.
Drugs are largely beta-lactamase resistant.
• They can target Gram-negatives because
they penetrate the outer membranes via
porin proteins.
What is beta-lactamase?
BETA-LACTAMASE DEGRADES PENICILLIN BY BREAKING BETA-
Beta-lactamase is a bacterial enzyme that breaks down penicillins.
What are carbapenems? What is the mode of action? What are they used for? What is CRE?
Common Gram-negative organisms with this new enzyme are called carbapenem-resistant Enterobacteraceae or CRE.
Carbapenems are very effective β‑lactam antibiotics used to treat severe or multidrug‑resistant bacterial infections
Carbapenems kill bacteria by binding to penicillin‑binding proteins (PBPs) and blocking cell‑wall synthesis, leading to bacterial death.
What is vancomycin? What is the mode of action? What is vancomycin used for?
Vancomycin is a glycopeptide antibiotic
Targets cell wall synthesis
• Used to treat MRSA
What are the cyclic polypeptide drugs? What is the mode of action of bacitracin? What is the mode of action of polymyxin? What is bacitracin and polymyxin used for?
Bacitracin, a topical antibiotic, affects peptidoglycan synthesis.
Cyclic polypeptide antibiotics are toxic for internal use.
Polymyxin B, a topical antibiotic, targets the outer membrane of Gram-negative organisms.
What is the primary physiological target of tetracyclines on bacteria? What are tetracyclines used for?
Tetracyclines targets translation.
• Tetracyclines are antibiotics and semi-
synthetics.
• From Streptomyces species
• Tetracyclines block the attachment of
tRNAs to the small subunit.
Name some aminoglycosides? What is the mode of action? What are they used for?
Aminoglycosides include streptomycin,
gentamycin, tobramycin, and neomycin.
• Streptomycin was first drug to treat TB.
• From various Actinobacteria
What is chloramphenicol? What is the mode of action? What is it used for?
Chloramphenicol is drug of choice for
epidemic typhus.
• Can cause chemically-induced aplastic
anemia
• One of the few antibiotics that can be
autoclaved for microbiological media
• From Streptomyces venezuelae
What is the mode of action of macrolides, such as erythromycin? What is the use of erythromycin?
Macrolides are bacteriostatic in action;
from Actinobacteria
• Erythromycin is example:
• Treat Gram-positive infections in
people with penicillin allergies
• Eye drops to prevent Neisseria
gonorrhoeae and Chlamydia
trachomatis conjunctivitis in neonates
• Produces by Saccharopolyspora
erythraea
What is the mode of action of rifampin on bacteria? What is it used for?
Rifampin targets transcription.
• Rifampin is a semisynthetic.
• Rifampin inhibits the bacterial form of
RNA polymerase.
• Used to treat TB
How do these antibiotic sensitivity tests work?
a. Tube dilution method, minimum inhibitory concentration b. Etest c. Kirby-Bauer test, disc diffusion method
Tube dilution method determines the lowest concentration of drug that will prevent bacterial growth—minimum inhibitory concentration (MIC).
• Method is used to determine therapeutic window.
ETEST uses a strip, impregnated with antibiotic.
• Strip is placed on an agar plate, inoculated with a lawn of bacteria.
Kirby-Bauer test uses small paper disks, impregnated with antibiotics.
What is an antibiogram?
An antibiogram is a report that summarizes how well different antibiotics work against bacteria isolated in a specific hospital, clinic, or region.
What are antiviral agents? How do they work? What are base analogs?
Antiviral agents interfere with specific steps of the viral replication cycle.
Antiviral agents are drugs that block different steps of the viral life cycle, and base analogs are a major class that mimic natural nucleotides to disrupt viral genome replication.
Why are many antifungal drugs toxic to the human body? What are the modes of action of polyenes (nystatin and amphotericin B), azoles, echinocandins, and flucytosines? What is each used for?
Antifungal drugs are often more toxic because they target aspects of eukaryotic metabolism.
Polyenes
• Alter membrane permeability
• Nystatin treats yeast infections.
• Amphotericin B treats severe systemic fungal infections.
• Azoles
• Target sterol synthesis
• Treat dermatophyte pathogens and yeast infections
Echinocandins
• Target cell wall synthesis
• For Candida and Aspergillus infections
Flucytosine
• Inhibits nucleic acid synthesis
• Used for severe systemic fungal infections
• Often combined with amphotericin B
What antimalarial substance comes from the chinchona tree? Name some common anti-malarial drugs used today.
Native South Americans recognized that the bark of the cinchona tree could treat malaria.
• Bark contained quinine.
• Most antimalarial drugs are aminoquinolines.
• Chloroquine
• Mefloquine
• Primaquine
• Another antimalarial drug is artemisinin from sweet wormwood.
Name some anti-protozoal drugs?
Sulfamethoxazole and trimethoprim
are used to treat some protozoal
infections.
• Inhibits folic acid synthesis
• Metronidazole is a common
antiprotozoal drug.
• Inhibits DNA synthesis
What are antihelminthic drugs? Name some examples.
These drugs treat infestations of
parasitic worms.
• Praziquantel
• Mebendazole
• Ivermectin
Differentiate among multidrug-resistant strains, extensively drug resistant strains, and totally drug resistant strains.
Multidrug-resistant strains (MDR) are
resistant to several drugs.
Extensively drug-resistant strains
(XDR) are resistant to all but one or two
classes of drugs.
Totally drug-resistant strains (TDR)
are resistant to all drugs.
What does ESKAPE stand for? Why is Clostridioides difficile a concern?
MAJOR CULPRITS OF DRUG
RESISTANCE
Remember the acronym ESKAPE:
• E
• Enterococcus faecium
• S
• Staphylococcus aureus
• K
• Klebsiella pneumoniae
• A
• Acinetobacter baumanii
• P
• Pseudomonas aeruginosa
• E
• Enterobacter species
Additionally, Clostridioides difficile, is
another important bacterium that has
become largely resistant.
What are the two genetic causes of antibiotic resistance? What are the three types of horizontal transfer?
Mutation is a permanent change in the
DNA.
• Spontaneous mutations occur
• Can lead to antibiotic resistance
Horizontal transfer is passing DNA
among members of the same
generation of organisms.
• Conjugation
• Transformation
• Transduction
• Conjugation is the most common
mechanism of antibiotic resistance.
What is the role of persister cells in antibiotic tolerance? How do antibiotics act as a selective agent on populations of bacteria?
Persister cells are often responsible
for antibiotic tolerance.
• Remember that persister cells are non-
dividing cells with low metabolic rates.
Antibiotics act as a selective agent by killing or inhibiting susceptible bacteria while allowing naturally resistant bacteria to survive and multiply, leading to a population dominated by resistant strains.
What are the various mechanisms that cause antimicrobial drug resistance?
Bacteria become resistant to antimicrobial drugs through several well‑defined molecular mechanisms, all of which reduce the drug’s ability to reach its target, bind its target, or exert its effect.
What are the causes of the global rise of antimicrobial drug resistance?
Prescription abuse
• Prescribing the wrong antimicrobial drug without culturing the pathogen.
• Often the pathogen does not respond to the given antimicrobial drug.
• Prescription misuse by individuals
• Patient stops taking antimicrobial drug when feeling better.
• Patient takes leftover antimicrobial drugs when sick.
• Prescription misuse by health organizations
• Overuse of antimicrobial drugs
• Giving broad spectrum antimicrobial drugs
• Superbugs often develop in healthcare settings.
• Antibiotic abuse in livestock
• Animal feed mixed with low levels of antimicrobial drugs to prevent disease or to promote growth.
• 79% of antibiotic use is for this purpose!
• Animal feedlots are often environments that superbugs develop.
How does antibiotic misuse select for resistant strains?
Antibiotic misuse intensifies natural selection, giving resistant bacteria a survival advantage and allowing them to dominate the population. The key idea is simple: whenever antibiotics are used incorrectly, they kill the susceptible bacteria and leave behind the ones that can withstand the drug. Those survivors then multiply.
What is the difference between sterilization and sanitation?
Sanitation reduces the number of pathogenic microbes to safe levels, so they are not harmful to public health.
Sterilization involves destroying all microbes, spores, and viruses.
Autoclaving
What is the difference -cidal and -static?
“-cidal” means killing, while “-static” means inhibiting (reducing) growth without killing.
Differentiate between dry heat and moist heat techniques. How does each kill microorganisms? What are the advantages and disadvantages of each?
Dry heat methods are characterized by high temperatures and low humidity. Materials to be sterilized is placed in hot air oven at high heat and low humidity.
Moist heat methods are characterized by low temperatures and high humidity. Require lower temperatures to sterilize and shorter exposure times. Good method for disinfecting water
Bacterial endospores may survive boiling.
Most water-borne pathogens do not form endospores. Good for emergencies, infrastructure incapacitation, camping, etc.
How long does it take to kill endospores in the dry air oven at 160 degrees C?
Bacterial endospores are killed at 160 degrees C for two hours.
Does boiling sterilize? What is the use of boiling for microbial control?
Good method for disinfecting water
Bacterial endospores may survive boiling.
Good for emergencies, infrastructure incapacitation, camping, etc.
What is autoclaving? What is it used for? What is the standard autoclaving pressure, temperature, and time to kill endospores?
Autoclaving uses steam under pressure to sterilize materials.
Bacterial endospores are killed at 15 psi, 121.5 degrees C for 30 minutes.
What is Pasteurization? What does it want to accomplish? What is the batchmethod?
Pasteurization is heating a beverage to a high temperature to accomplish the following:
Kill all pathogens
Reduce most spoilage microorganisms
Not damage the product
Milk is pasteurized at 63 degrees C for 30 minutes in holding or batch method.
What are the two toughest milk-borne pathogens to kill by Pasteurization?
Toughest milk-borne pathogens are Mycobacterium tuberculosis and Coxiella burnetii
How does refrigeration and freezing control microorganisms?
Cold temperature—inhibits growth
How does salting, desiccation, and canning preserve food?
Canning—sterilized food in sealed container
High osmotic pressure—removes water
What is lyophilization?
Freezing drying (lyophilization)—food is immersed in liquid nitrogen and vacuum removes water in the form of vapor
What are membrane filters? What are they used for?
Membrane filters are used to purify heat- sensitive liquids such as beverages, some microbiological media, pharmaceuticals, etc.
Microbes are removed by a filter in filtration
What are HEPA filters? What are they used for? What are biological safety cabinets?
High-efficiency particulate air filters (HEPA) remove microbes, particulate pollutants, and spores from air; these filters are made of fibrous materials.
Biological safety cabinets are used to safely handle higher level pathogens.
Distinguish between nonionizing radiation and ionizing radiation?
Nonionizing radiation is electromagnetic energy that is not powerful enough to eject electrons. (UV light or germicidal lamp)
Ionizing radiation is electromagnetic energy that is powerful enough to eject electrons, forming ions of various molecules in the cell. (x-rays and gamma rays)
How does ultraviolet light damage DNA? What is the use of this type of control?
Ultraviolet radiation causes disruptive pyrimidine dimers in the DNA, kinking the double helix and disrupting DNA replication. Commonly used in surgical rooms.
What is gamma irradiation? What is the use of this type of control?
Pasteurizing dose uses gamma irradiation to preserve, extend shelf life, and kill pathogens.
Gamma irradiation is a form of ionizing radiation
What is the difference between disinfectant and antiseptic?
Disinfectant is a chemical substance that
reduces the number of microbes except
endospores. Disinfectants are used on
inanimate objects.
Antiseptic is a chemical substance that
reduces the number of microbes on living
tissue like the skin or mucous membrane.
What factors affect the activity of an antimicrobial chemical substance?
The activity of an antimicrobial chemical substance is shaped by three major categories of factors: microbial characteristics, properties of the chemical agent, and environmental/host conditions.
What is the phenol coefficient?
Phenol coefficient is used to
measure the effectiveness of a
disinfectant or antiseptic.
What is the disc diffusion test?
Disk diffusion test
Paper discs are impregnated with chemical
agent.
Paper disc placed on plate, swabbed for a
lawn of bacteria.
Plates incubated for 24 to 48 hours.
Look for zones of inhibition.
What are these halogens used for? How do they kill microorganisms? a. Chlorine i. Gaseous ii. Sodium hypochlorite iii. Chloramines b. Iodine i. Tincture of iodine ii. Iodophores
Halogens include fluorine, chlorine, bromine, and iodine.
Halogen means “salt generating” when reacting with metals.
Chlorine and iodine are the most important halogens for microbial control.
Halogens are effective because they are oxidizing agents.
Kill broad variety of microbes
Chlorine occurs in many forms:
Gaseous
Inorganic forms
Organic forms
Chlorine oxidizes and denatures proteins.
Chlorine is used to treat drinking water to make it safe
Sodium hypochlorite in laundry bleach is used as a disinfectant.
Chloramines are organic chlorine- containing compounds used as microbicides and for making drinking water safe.
Iodine is larger and more reactive than chlorine.
Tincture of iodine is an antiseptic that is composed of 2% iodine in ethanol.
Iodophors are organic compounds that bear iodine, and release iodine slowly.
What is phenol? Who used it first as an antiseptic? How does it kill microorganisms? What are the disadvantages?
Phenol was first used by Joseph Lister in his antiseptic surgery.
Hydroxylated aromatic ring
Denature proteins
Very toxic
Caustic to skin in high concentrations
Used more as a disinfectant today rather than antiseptic
Phenol denatures proteins and disrupts membranes.
What is chlorhexidine?
Chlorhexidine is used as surgical hand scrub, antiseptic, and mouth rinse for gum disease.
What is merbromin (mercurochrome) and thimersol (merthiolate)? What are they used for? How do they kill microorganism? Why were they banned?
Found in topical antiseptics like merbromin (Mercurochrome) and thimerosal (Merthiolate). These are
organic molecules that bear mercury.
Thimerosal was used as a vaccine preservative.
Both were banned because of mercury content.
What is copper sulfate used for?
Copper sulfate used as algicide.
What was silver nitrate used for?
1% silver nitrate was used in the past to prevent acute hyperconjunctivitis caused by Neisseria gonorrhoeae
What are the two alcohols used as antiseptics? How do they kill microorganisms? Which is more effective in killing microorganisms, 70% or 95% alcohol?
Includes ethanol (ethyl alcohol) and isopropanol (isopropyl alcohol)
Used as antiseptics
Popular in hand sanitizers
70% alcohol is more effective than 95% alcohol in killing microbes.
Alcohols coagulate proteins, disrupt membranes, and dehydrate cells.
What are soaps and how do they work?
Soaps are surfactants made from saponified lipids.
Since soaps have pH of 8.0, alkaline pH damages microbes.
What are surfactants?
Surfactants are substances that degerm by solubilizing particles clinging to surfaces by reducing surface tension
What are quaternary ammonium compounds? What are they used for? How do they kill microorganisms?
Quaternary ammonium compounds or quats contain nitrogen bound to four organic groups.
Examples include benzakonium chloride in Zephiran and cetylpyridinium chloride in Cepacol.
Used as antiseptics and disinfectant
What is hydrogen peroxide used for? What is benzoyl peroxide used for? How do they kill microorganisms?
Hydrogen peroxide (H2O2) is commonly used as an antiseptic and mouth rinse.
Benzoyl peroxide is found in over-the-counter acne medications.
What is formaldehyde used for? How does it kill microorganisms?
Formalin is aqueous formaldehyde solution. It is the most common aldehyde used.
Disinfectant.
Embalming fluid
Inactivates viruses for vaccines
Denatures microbial toxins to make toxoid vaccines
What is ethylene oxide used for? How does it kill microorganisms?
Ethylene oxide is a gas that denatures proteins and inactivates nucleic acids.
Will kill vegetative cells and spores
Toxic, carcinogenic, and explosive
Mixed with Freon or carbon dioxide to make less explosive
Used in “gas autoclaves”
Sterilizes plastics that would melt in an autoclave, catheters, artificial heart valves, heart-lung machine components, and optical equipment
What is chlorine dioxide used for? How does it kill microorganisms?
What is the difference between genetic shift and a genetic drift.
Genetic drift involves small point mutations in the viral genome due to replication errors.
Genetic shift involves major changes in the influenza A virus due to genetic recombination.
What are the two rare complications you can get from influenza?
Two rare complications are associated with influenza infections:
Guillain-Barre syndrome causes damage to PNS, leading to muscle weakness and paralysis.
Reye syndrome is correlated with viral infection and aspirin use. Symptoms include nausea, vomiting, and progressive mental changes, leading to delirium. Syndrome affects brain and liver.