NREMT Medical
1/69
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
70 Terms
Aldosterone
is a naturally occurring steroid hormone produced by the adrenal glands, regulating sodium and potassium levels in the body.
Antidiuretic Hormone (ADH)
is produced by the posterior pituitary gland and regulates water balance by accelerating water reabsorption, though it is not directly involved in sodium and potassium regulation.
Aldosterone
Its primary function is to regulate sodium and potassium levels, helping control blood pressure and fluid balance.
Thiamine
Is known as vitamin B. Chronic alcoholism interfere with the intake, absorption, and utilization of this vitamin. Serious, neurological disease may result due to the bodies inability to use it.
Upper GI bleed
Characterized by melena (dark tarry stool) and/or bright red vomit (hematemesis)
Lower GI bleed
Characterized by hematochezia (bright red stool) and/or dark coffee ground hematemesis .
Esophageal varices
Blood cannot flow properly through a damaged liver and backs up in the portal veins. Increasing pressure in these veins is known as portal hypertension which can cause them to rupture. Signs & symptoms: Sudden onset dysphagia, vomiting bright red blood.
Peptic Ulcer Disease
Excessive stomach acid erodes away the mucous lining. Stomach acid secretion can increase in response to chronic alcohol and nicotine use, extreme stress states, and infection.
Signs & symptoms: “Burning, gnawing,” epigastric pain relieved with eating, hematemesis, melena. Pain can progress to diffuse abdominal pain with rebound tenderness when ulcer perforates
Mallory-Weiss Syndrome
Increases in stomach pressure during frequent vomiting can cause structural tearing of the esophagus.
Signs & symptoms: Vomiting bright red blood, epigastric abdominal pain.
Treatments: Determine the extent of blood loss. Fluid resuscitation. Airway management may include suctioning. Shock management and upgrading the airway may be required.
GERD
Affected Anatomy: Lower esophageal sphincter (LES), AKA “cardiac sphincter”
Pathophysiological Summary: Smoking, obesity, pregnancy, or consuming fatty/fried foods, alcohol, and citrus fruits can cause the LES to open and allow stomach acid to move upwards. Over time, this can damage the esophagus and cause bleeding.
Signs & symptoms: Heartburn.
Gastritis
Excessive stomach acid causes inflammation of the stomach, but is not eroded.
Signs & symptoms: “Burning, gnawing,” epigastric pain relieved with eating.
Small Bowel Obstruction
Affected Anatomy: Small Intestine -
Pathophysiological Summary: Cancer, Crohn disease, hernias, scar tissue post-operation, and volvulus can decrease the diameter and/or the small intestine’s ability to stretch.
Signs & symptoms: Eventual constipation and abdominal distention. Hyperactive bowel sounds in early stages, hypoactive bowel sounds in late stages. Feculent emesis.
Treatments: Assess for sepsis. Maintain hemodynamic stability. NG tube for gastric decompression. Antiemetics and analgesics.
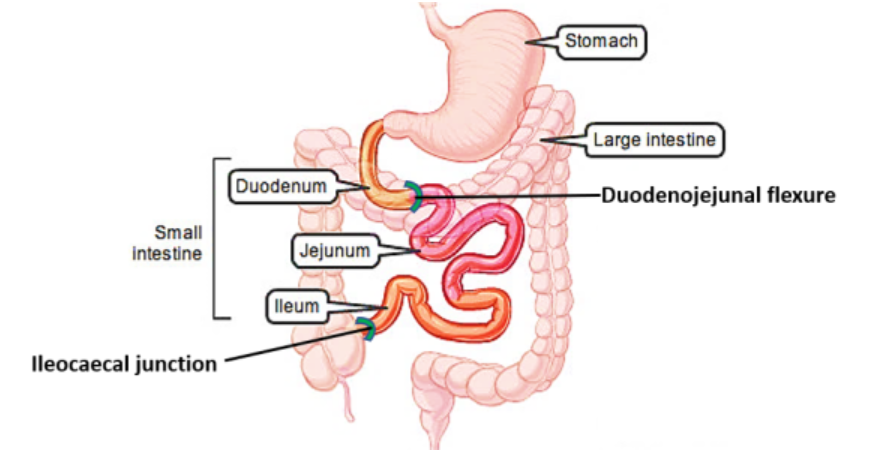
duodenum, jejunum, and ileum
are the three components of the small intestine, working together to digest food, absorb nutrients, and transport waste to the large intestine.
ascending, transverse, and descending colon
three main segments of the large intestine, crucial for water absorption and waste formation.
Hyperresonance
an abnormally loud, low-pitched, booming sound heard during physical chest percussion, indicating excessive air trapping or abnormal air accumulation in the chest
Cirrhosis
Pathophysiological Summary: Early liver failure presenting with portal hypertension, coagulation deficiency, and diminished detoxification.
Signs & symptoms:
1st phase - urticaria, easy bruising, and pruritus( itchy skin) .
2nd phase - alcoholic stools(white, gray, or light tan (clay-colored) feces indicating a severe lack of bile), jaundice, dark urine, icteric conjunctiva, ascites(fluid in the abdomen), and RUQ pain.
Treatments: Special attention to fluid shifts. Avoid lactated ringers. Use the lower end of dose ranges for medications. Caution with opiates.
Hepatic Encephalopathy
Pathophysiological Summary: As cirrhosis progresses, ammonia levels rise, metabolism diminishes, and the blood-brain barrier can allow passage of neurotoxins, affecting the brain and altering mental status.
Signs & symptoms: Mental status changes resulting from loss of memory to coma. Bradykinesia(slow movement), shuffling gait, Parkinson disease. CT and MRI inconclusive. Opiates, benzos, and psychotropics can worsen presentation.
Treatments: Ensure altered LOC is not being caused by something else. Care is supportive.
Pancreatitis
The pancreatic duct is blocked, and enzymes that usually digest food are trapped inside the pancreas so they instead begin breaking the pancreas itself down in a process called autodigestion which leads to inflammation. This is mainly caused by alcohol consumption and gallstones.
Signs & symptoms: Epigastric and LUQ pain, radiating to the back. Extremity muscle spasms. Cullen sign(bruising (ecchymosis) around the umbilicus), Grey Turner sign.
Treatments: Fluid resuscitation, maintaining hemodynamic stability. Analgesics
Grey turner’s sign
bruising or bluish-purple discoloration of the flanks It indicates severe retroperitoneal hemorrhage, which is bleeding behind the lining of the abdominal cavity.
Cullen’s sign
superficial edema and bruising (ecchymosis) in the fatty tissue around the umbilicus (belly button). It is a serious clinical indicator of intra-abdominal or retroperitoneal hemorrhage
cholecystitis
is defined as the acute or chronic inflammation of the gallbladder, typically caused by an obstruction of the cystic duct by gallstones———>Acalculous is WITHOUT gallstones——-calculous is with gallstones
Signs & symptoms: Five F’s: Fair, Fat, Female, Fertile, Forty-Fifty years old. RUQ pain that radiates to the right shoulder, pain after a fatty meal, positive Murphy sign.
Murphy’s Sign
is a specialized physical examination technique used to identify acute cholecystitis (gallbladder inflammation), it is characterized by the sudden arrest of inspiration due to sharp pain during deep palpation of the Right Upper Quadrant (RUQ)
How to Perform Murphy’s Sign
Positioning: Have the patient lie supine (on their back).
Palpation: Locate the Right Upper Quadrant (RUQ), specifically at the midclavicular line just below the right costal margin (rib cage).
Pressure: Apply firm, upward and inward pressure with your fingers.
Inhalation: Ask the patient to take a deep breath in.
Observation: As the patient inhales, the diaphragm descends, pushing the liver and gallbladder down onto your fingers.
Cholestasis
A condition where bile flow from the liver is reduced or blocked. This can occur due to liver diseases, bile duct obstructions, or genetic conditions. Reduced bile flow leads to the accumulation of bile acids in the liver and bloodstream, causing liver damage and jaundice.
Signs & symptoms: Jaundice, itching (pruritus), dark urine, pale stools,
fatigue, and abdominal pain.
cholelithiasi
the presence or formation of gallstones (calculi) within the gallbladder. While it is the most common cause of cholecystitis (inflammation)
Signs & symptoms: Biliary colic (intense, intermittent pain in the right upper quadrant
Peritonitis
The rupture of an internal organ or movement of bacteria out of the intestines irritates the peritoneum. It can result from injury of HOLLOW organs - stomach, intestines, gallbladder, urinary bladder, uterus, and ureters.
Signs & symptoms: Diffuse abdominal pain, stiff/rigid abdomen, aversion to lying supine. Treatments: Treat shock, analgesics, and antiemetics
Appendicitis
Fecal matter or other material accumulates in the appendix, and the increase in pressure decreases lymph and blood flow, decreasing the appendix’s ability to fight infection. The increased pressure can lead to rupture.
Signs & symptoms: “Early” - periumbilical pain, “ripe” - RLQ pain, McBurney point, “rupture” - diffuse abdominal pain and rebound tenderness.
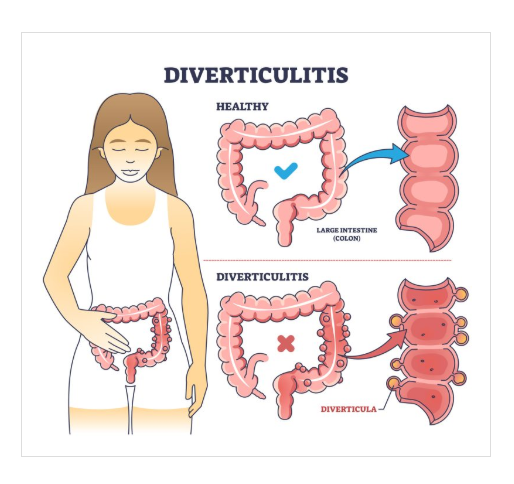
Diverticulitis
Weak areas of the colon form pouches called diverticula that become inflamed by trapped bacteria.
Signs & symptoms: LLQ pain, bleeding is rare. Treatments: Maintain patient comfort. Analgesics and antiemetics.
Ulcerative Colitis
Genetics, stress, or autoimmunity can cause inflammation of the colon which thins the walls of the intestine and results in a dilated rectum. The damaged colon is susceptible to infections and bleeding.
Signs & symptoms: Hematochezia, LLQ pain, and tenesmus (the urge to have a bowel movement).
Treatments: Assess and treat shock.
Chron’s Disease
The activity of WBC’s during series of attacks on the GI tract by the immune system damages all layers of the portion involved, resulting in scarred, narrowed, weakened portions of the intestines. (Autoimmune)
Irritable Bowel Sydrome
Commonly observed hypersensitivity of bowel pain receptors, hyperresponsiveness of smooth muscles in the bowel, psychiatric disorder connection.
Sign & symptoms: Defined as abdominal pain at least 1 day a week for 3 months, associated with changes in stool consistency or frequency. Diffuse, non-radiating abdominal pain relieved by bowel movement.
Acute Gastroenteritis
Most commonly viruses such as norovirus, but also conditions like allergies, lactose intolerance, toxins, and immune disorders cause inflammation that can lead to hemorrhage and erosion of the GI tract and can alter the way water and nutrients are absorbed.
Signs & symptoms: Abrupt and violent onset of vomiting and diarrhea.
Oral Candidiasis ( Thrush )
A condition in which the fungus Candida albicans accumulates on the lining of the mouth.
Signs & symptoms: Creamy white lesions on inner lining of mouth. “Cottony” feeling in mouth. Commonly seen in infants and patients who have compromised immune systems, wear dentures, or use inhaled corticosteroids frequently.
Epiglottitis
Inflammation of the epiglottis often resulting from Haemophilus influenzae type B virus.
Signs & symptoms: Common in children, or adults who don’t have Hib vaccine. Tripod or “sniffing” position, fever, sore throat, dysphagia and drooling.
Treatments: Minimize on-scene time. Assume position of comfort, supplemental O2 if tolerated (blow-by). Do NOT look in mouth
Ludwig Angina
Bacteria from an infected tooth root or mouth injury causes cellulitis in the mouth.
Type 1 Diabetes
a chronic autoimmune condition where the immune system destroys insulin-producing beta cells in the pancreas, resulting in little to no insulin production
Type 2 diabetes
Characterized by insulin resistance and relative insulin deficiency. It is often associated with obesity, sedentary lifestyle, and genetic factors.
Hyperglycemia
Characterized by elevated blood glucose levels (typically above 200 mg/dl), often due to insufficient insulin or insulin resistance. It can lead to complications like diabetic ketoacidosis or hyperosmolar hyperglycemic state. “Hot and Dry, they might be high”
Signs & Symptoms: 3 Ps - Polyuria (frequent urination), Polydipsia (increased thirst), and Polyphagia (increased hunger), N/V, LOC, and fatigue.
Treatment: IV fluids and will ultimately need insulin.
Hypoglycemia
Occurs when blood glucose levels drop below normal, often due to excessive insulin, insufficient food intake, or excessive physical activity. It can impair brain function due to inadequate glucose supply. “Cool and clammy, need some candy.”
Signs & Symptoms: Sweating, AMS, tremors, seizures, and anxiety.
Treatment: Oral glucose, IV dextrose if unconscious or unable to swallow, Glucagon injection if IV access is not available.
Hyperglycemic Hyperosmolar State (HHS)
A severe hyperglycemic state without significant ketosis, often seen in type 2 diabetes. It results from high blood glucose leading to extreme dehydration and hyperosmolarity.
Signs & Symptoms: 3 Ps, tachycardia, dehydration, seizures, AMS, and LOC. ETCO2 35-45 mmHg. (often >600 mg/dL)
Treatment: Aggressive IV fluid replacement, electrolyte replacement, and will ultimately need insulin.
Diabetes Ketoacidosis
is a serious complication of diabetes, characterized by hyperglycemia, ketosis, and acidosis. It occurs when the body starts breaking down fats for energy due to a lack of insulin, leading to the production of ketones.
Signs & Symptoms: 3 Ps, N/V, fruity smelling breath (or acetone), Kussmaul respirations (deep, labored breathing), AMS, and LOC. ETCO2 <35 mmHg.
Treatment: IV fluids and will ultimately need insulin.
Primary adrenal insufficiency
Also known as “Addison's Disease” is a condition where the adrenal glands do not produce enough cortisol and aldosterone, often due to autoimmune destruction.
Signs & Symptoms: Fatigue, weight loss, hyperpigmentation, hypotension, salt craving, and N/V.
Treatment: Glucocorticoid replacement (Hydrocortisone), electrolyte management, and treat the symptoms.
Secondary adrenal insufficiency
Secondary adrenal insufficiency is a condition where the pituitary gland fails to produce sufficient adrenocorticotropic hormone (ACTH), causing the adrenal glands to produce too little cortisol.
Common causes include long-term steroid use, pituitary tumors, or radiation. Symptoms include extreme fatigue, weight loss, and low blood pressure
Treatment: Glucocorticoid replacement (Hydrocortisone), electrolyte management, and treat the symptoms.
Cushing’s Syydrome
A condition caused by prolonged exposure to high levels of cortisol, often due to corticosteroid medication or adrenal/pituitary tumors.
Signs & Symptoms: Weight gain (central obesity), moon face, buffalo hump, purple striae (stretch marks), acanthosis (neck, armpits, & groin), hypertension, and hyperglycemia. Treatment: Supportive care
Hypothyroidism
A condition characterized by insufficient production of thyroid hormones by the thyroid gland. This leads to a slowed metabolism and can be caused by autoimmune diseases, iodine deficiency, or thyroid surgery.
Signs & symptoms: Fatigue, weight gain, cold intolerance, constipation, dry skin, hair loss, bradycardia, depression, and myxedema (severe cases).
Hyperthyroidism
is a condition where the thyroid gland produces excessive thyroid hormones, leading to an increased metabolic rate. Common causes include Graves' disease, toxic multinodular goiter, and thyroiditis.
Signs & symptoms: Weight loss, heat intolerance, increased appetite, tachycardia, palpitations, tremors, anxiety, irritability, and exophthalmos (in Graves' disease).
Grave’s Disease
is an autoimmune disorder that leads to hyperthyroidism. The immune system produces antibodies that stimulate the thyroid gland to produce excessive hormones. ( overactive thyroid)
Signs & symptoms: Diffuse goiter, exophthalmos, and pretibial myxedema (thickening of the skin on the shins).
Thyrotoxicosis
A clinical syndrome resulting from excess thyroid hormones in the bloodstream, which can be due to hyperthyroidism or other causes like thyroiditis or excess thyroid hormone intake. Thyroid storm is a life-threatening condition with severe manifestations of thyrotoxicosis. It can develop from untreated hyperthyroidism.
Signs & symptoms: Similar to hyperthyroidism, including weight loss, heat intolerance, tachycardia, palpitations, tremors, anxiety, and irritability. Thyroid storm: Fever, delirium and AMS.
Hashimoto’s Disease
is an autoimmune disorder where the immune system attacks the thyroid gland, leading to hypothyroidism over time. It is the most common cause of hypothyroidism.
Signs & symptoms: Symptoms of hypothyroidism, Fatigue, weight gain, cold intolerance, constipation, dry skin, hair loss, bradycardia, and depression.
Myxedema Coma
A severe, life-threatening form of hypothyroidism that can occur due to untreated or poorly managed hypothyroidism, often triggered by infection, cold exposure, or sedative use.
Signs & symptoms: Altered mental status, hypothermia, bradycardia, hypotension, hypoglycemia, and respiratory depression.
Hyperparathyroidism
Characterized by excessive secretion of parathyroid hormone (PTH), leading to hypercalcemia. It can be primary (due to parathyroid adenoma) or secondary (due to chronic kidney disease).
Dialysis disequilibrium syndrome
is a rare but serious complication of dialysis characterized by neurological symptoms due to rapid changes in fluid and electrolyte balance during hemodialysis.
Signs & symptoms: Headache, nausea, vomiting, altered mental status, seizures, and, in severe cases, coma
Urinary retention
The inability to empty the bladder completely, which can be due to obstruction, nerve problems, or muscle weakness.
Signs & symptoms: Difficulty starting urination, weak urine stream, frequent urination in small amounts, and a feeling of incomplete bladder emptying.
Urine incontinence
The involuntary leakage of urine, which can be due to stress, urge, overflow, or functional causes.
Signs & symptoms: Uncontrolled urine leakage, frequent urination, and urgency.
Acute Kidney Injury
A sudden decline in kidney function, leading to the accumulation of waste products in the blood. Causes include dehydration, infection, and nephrotoxic medications.
Signs & symptoms: Oliguria( decrease in urine output), edema, fatigue, and confusion.
Renal Calculi
Kidney stones, are hard deposits of minerals and salts that form in the kidneys and can cause pain and urinary obstruction. Signs & symptoms: Severe flank pain, hematuria(blood in the urine), nausea, vomiting, and urinary frequency or urgency.
Hyperkalemia from missing dialysis
is an elevated level of potassium in the blood, which can be life-threatening if not treated promptly. In patients with end-stage renal disease (ESRD) who miss dialysis sessions, the kidneys are unable to excrete potassium adequately, leading to dangerous accumulations. Dialysis is critical for these patients to maintain electrolyte balance.
Signs & symptoms: Muscle weakness, fatigue, paresthesia, palpitations, and, in severe cases, arrhythmias such as ventricular fibrillation or cardiac arrest. ECG changes include peaked T waves, widened QRS complexes, and prolonged PR intervals.
Treatments: Immediate interventions include administering calcium gluconate to stabilize cardiac membranes, sodium bicarbonate if acidosis is present, and beta-agonists like albuterol, insulin with glucose to shift potassium into cells. Emergency dialysis is often required to rapidly decrease potassium levels.
Orchitis
Inflammation of one or both testicles, which can be caused by bacterial or viral infections, including mumps.
Epididymitis
Inflammation of the epididymis, often caused by bacterial infection, including sexually transmitted infections like chlamydia and gonorrhea.
Benign Prostatic Hyperplasia (BPH)
is a non-cancerous enlargement of the prostate gland, which can obstruct urine flow.
Signs & symptoms: Urinary frequency, urgency, nocturia( wake up in the night to urinate), weak urine stream, and difficulty starting urination.
Cystitis
Inflammation of the bladder, usually caused by bacterial infection.
Signs & symptoms: Dysuria, urinary frequency, urgency, hematuria, and suprapubic pain.
Pyelonephritis
A bacterial infection of the kidneys, which can be acute or chronic.
Signs & symptoms: Flank pain, fever, chills, nausea, vomiting, and urinary symptoms such as dysuria and frequency.
Thrombocytosis
Characterized by an abnormally high platelet count, which can lead to increased risk of thrombosis or, paradoxically, bleeding if the platelets are dysfunctional.
Signs & symptoms: Thrombosis (e.g., deep vein thrombosis, pulmonary embolism), bleeding (e.g., gastrointestinal bleeding, easy bruising), headache, dizziness, and visual disturbances.
Von Willebrand disease
A hereditary bleeding disorder caused by a deficiency or dysfunction of von Willebrand factor, which is essential for platelet adhesion and aggregation.
Signs & symptoms: Easy bruising, frequent nosebleeds, prolonged bleeding from cuts, heavy menstrual bleeding, and excessive bleeding after surgery or dental work.
Hemophilia A
A genetic disorder caused by a deficiency of factor VIII, leading to impaired blood clotting and prolonged bleeding.
Signs & symptoms: Prolonged bleeding, spontaneous bleeding into joints (hemarthrosis), muscle hematomas, and excessive bleeding after injuries or surgeries.
Hemophilia B
A genetic disorder caused by a deficiency of factor IX, leading to impaired blood clotting and prolonged bleeding.
Signs & symptoms: Prolonged bleeding, spontaneous bleeding into joints, muscle hematomas, and excessive bleeding after injuries or surgeries.
Thrombocytopenia
Characterized by a low platelet count, which increases the risk of bleeding and bruising.
Signs & symptoms: Easy bruising, petechiae, prolonged bleeding from cuts, spontaneous bleeding from gums or nose, and heavy menstrual bleeding.
Disseminated Intravascular Coagulation (DIC)
is a complex condition where widespread clotting occurs in small blood vessels, leading to organ damage, and is followed by excessive bleeding due to the consumption of clotting factors and platelets.
Signs & symptoms: Bleeding from multiple sites, bruising, thrombosis, organ dysfunction, and hypotension.
Thalassemia
is a genetic blood disorder characterized by reduced production of hemoglobin, leading to anemia and increased destruction of red blood cells.
Signs & symptoms: Fatigue, pallor, jaundice, bone deformities, and growth retardation in severe cases.
Polycythemia
is characterized by an increased red blood cell mass, which can lead to increased blood viscosity(thickness of blood) and risk of thrombosis.
Signs & symptoms: Headache, dizziness, hypertension, pruritus(itchy skin), and erythromelalgia (burning pain in hands and feet)