Exam 3: Degenerative Diseases (I & II)
1/99
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
100 Terms
degenerative diseases of the CNS are typically caused by.....
structural or neurochemical changes in the CNS
onset of degenerative diseases typically occur....
post-childhood/adolescence
degenerative diseases. progressive or not progressive?
progressive!!!!!
t or f: All degenerative diseases share a common trait of decreased self-efficacy.
true
All degenerative diseases share a common trait of decreased self-efficacy. Why?
-b/c of adult onset, roles, habits, and routines are already established and then stripped away post-dx
-becoming more dependent on caregivers bc of decrease in independence as disease progresses
decreased self-efficacy leads to decreased.....
-locus of control
-self-worth/self-esteem
general OT intervention for degenerative diseases
-support client's ability to fully participate in their roles, ADL/IADLs
-consider the progression of the disease! is it slow? rapid?
-consider any limitations in : physical, cognitive, social, emotional
amyotrophic lateral sclerosis (ALS)
-condition of progressive deterioration of motor nerve cells resulting in total loss of voluntary muscle control
-symptoms advance from muscle weakness in the arms and legs, to the muscles of speech, swallowing, and breathing, to total paralysis and death
-also known as Lou Gehrig's disease
"prisoner in own body" bc cognition intact
cause of ALS
no known cause
3 types of ALS
1) progressive bulbar palsy (PBP)
2) progressive spinal musculature atrophy (PSMA)
3) primary lateral sclerosis (PLS)
progressive bulbar palsy (PBP)
oral motor dysfunction most prevalent
-dysarthria, dysphagia, etc.
progressive spinal musculature atrophy (PSMA)
muscle wasting in limbs most prevalent
primary lateral sclerosis (PLS)
spastic paraparesis affecting both UE and LE
t or f: ALS leads to involvement of both upper- and lower-motor neurons.
true
t or f: ALS is a fatal disease
true
ALS life expectancy
50% live 3+ years
20% live 5+ years
10% live 10+ years
ALS has a __________ decline in function
rapid, steady
does ALS have periods of remission?
NO
4 stages of ALS
1) early stage
2) early-middle stage
3) late-middle stage
4) end stage
early stage (ALS)
-slight limitations in performance of ADL/IADL
-some pain may be present
-decreased endurance
OT intervention for decreased endurance in the early stages of ALS includes
work simplification
energy conservation
early-middle stage (ALS)
-muscle imbalance/weakness
-increased fatigue (inc. energy req. for ADL/IADL - use AE)
-weight loss
-spasticity
-muscle cramping
-fasciculation
late-middle stage (ALS)
-progressive weakness of trunk muscles
-greater loss of mobility and endurance (use a power WC)
-assistance needed for many/most ADL/IADL
what stage is a power WC recommended for ALS?
late-middle
end stage (ALS)
-total dependence for ADL/IADL
-tube feeding
-ventilator
what remains intact with ALS?
-cognition!!!
-eye function
-bowel/bladder function
-sensory function
medical management of ALS includes....
-noninvasive/invasive ventilator support system
-dysphagia and feeding tube
-mgmt of saliva
-pain mgmt
-depression
-hospice services (at end stage)
OT intervention for ADLs/self-care (ALS)
-adaptive devices
-automated self feeder
-changes in food consistency (chopped, pureed)
-communication aids (AAC, etc.)
-environment-adapted aids for remote operation (Alexa, Siri - lights, tv/sound system, climate controls)
OT intervention for sensorimotor (ALS)
-hand splints (maintain fxnl hand position)
-neck supports (provide stabilization)
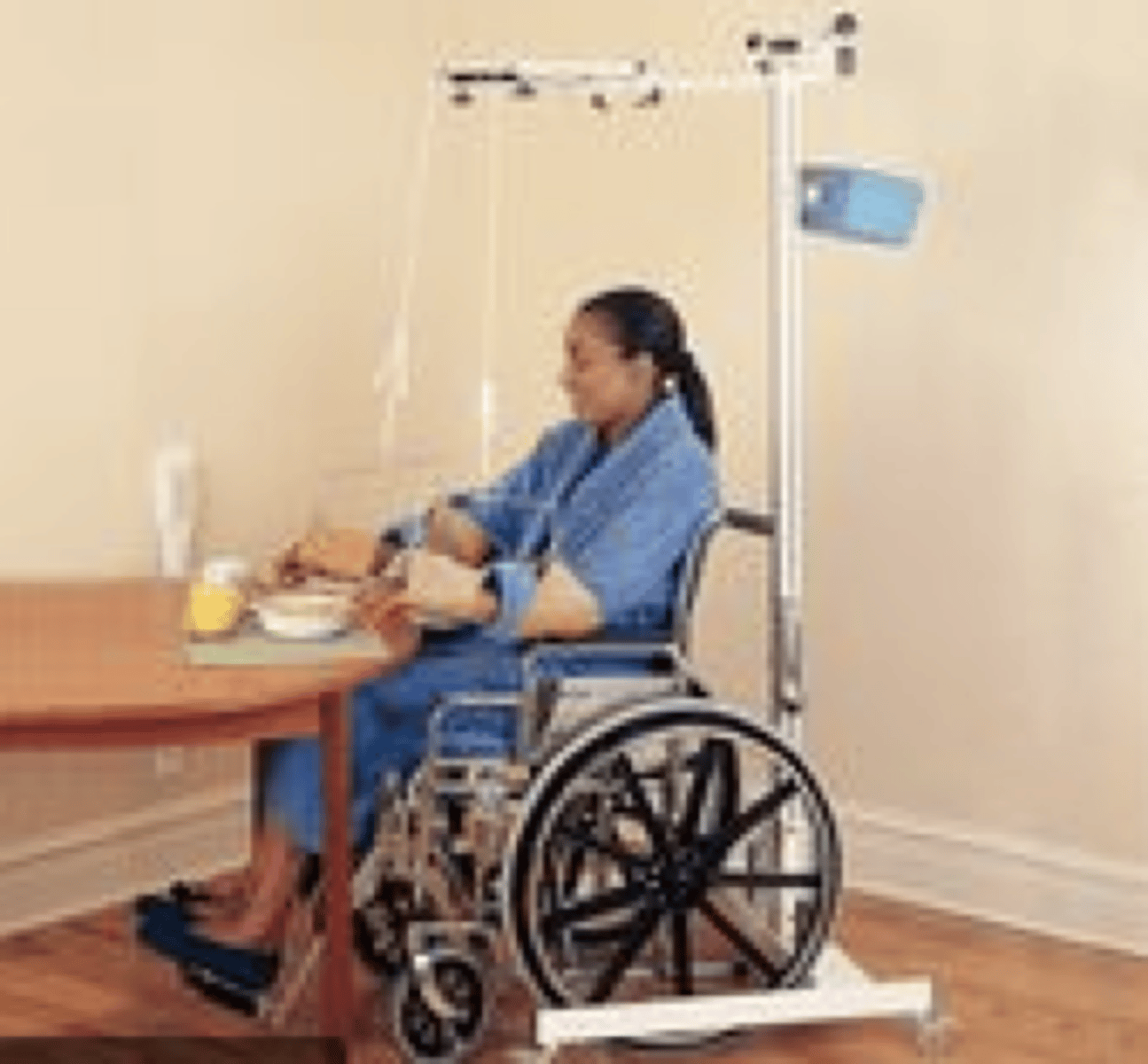
-overhead slings (support weakened muscles)
-mobile arm supports (provides AAROM)
adaptive devices for ALS
1) elongated handle (dec. ROM)
2) built up handles (dec. ROM)
3) zipper pulls (dec. fine motor)
4) button hooks (dec. fine motor)
5) universal cuff (dec. strength & grip)
6) Velcro closure/magnetic buttons (dec. fine motor)
7) cups w/ 2 handles (dec. strength & grip)
8) plate guards (hemitechnique - 1 hand)
why are cup with 2 handles great for ALS patients?
-no grip needed
-no squeeze and hold, just thread hands through handles
t or f: we should create strengthening goals for ALS patients.
FALSE
their muscles are weak and will not get stronger
***only strengthen with functional tasks (cans in cabinet)
OT intervention for mild exercise (ALS)
-brief duration over several days (avoid fatigue)
-aquatic programs may be beneficial (dec. fall risk)
-strengthening with functional tasks only
-teach positions and techniques to decrease spasticity
-passive stretching/ROM to prevent contractures during late stage (caregiver training)
OT intervention for productivity (ALS)
-modification of work/home environment
-alternative keyboard or input devices for computer use
-energy conservation/work simplification
-exploration : alternative jobs, volunteering
wheelchair recommendations for ALS should include
-reclining back
-headrest
-elevating padded leg rest
-padded arm rest
-safety belt
-positioning devices
-lap tray
-mobile arm supports
t or f: strengthening exercises are not recommended for ALS patients.
true!!!
-it will not alter the course of the disease
-may cause cramping and fatigue
ALS precautions
-strengthening not recc.
-watch for reactive depression
-watch for dec. respiratory function
-protect from respiratory infection
-swallowing difficulties and choking
-avoid fatigue
-pressure sores
A client with ALS reports increased muscle cramping, fasciculations, and noticeable fatigue during dressing tasks. Which stage of ALS is this presentation most consistent with?
a) Early stage
b) Early-middle stage
c) Late-middle stage
d) End stage
b) Early-middle stage
An OT is working with a client in the late-middle stage of ALS who is showing progressive trunk weakness and difficulty with safe mobility. What is the most appropriate recommendation?
a) Begin strengthening exercises to build trunk stability
b) Train the client in using a manual wheelchair
c) Recommend a power wheelchair with appropriate positioning features
d) Initiate feeding tube training
c) Recommend a power wheelchair with appropriate positioning features
Which of the following remains intact throughout the progression of ALS?
a) Fine motor coordination
b) Cognitive function
c) Respiratory muscle strength
d) Swallowing ability
b) Cognitive function
A client with ALS in the end stage is now totally dependent for all ADLs. Which of the following interventions is most appropriate for the OT to prioritize?
a) Teach strengthening exercises for upper extremities
b) Implement a spasticity reduction program
c) Train caregivers in positioning and passive ROM
d) Recommend hand splints for improving grip strength
c) Train caregivers in positioning and passive ROM
Which adaptive aid would be most appropriate for a client with ALS experiencing decreased grip strength during mealtime?
a) Button hook
b) Plate guard
c) Universal cuff
d) Reacher
c) Universal cuff
An OT is working with a client in the early stage of ALS who experiences mild muscle soreness. What strategy would best support occupational performance?
a) Introduce dynamic splinting
b) Recommend brief, functional tasks spread over several days
c) Prescribe progressive resistance training
d) Initiate passive ROM twice daily
b) Recommend brief, functional tasks spread over several days
A client with ALS in the early-middle stage experiences spasticity and muscle cramping. Which OT intervention is most appropriate?
a) Increase activity to reduce stiffness
b) Teach relaxation and positioning techniques
c) Begin progressive resistance exercises
d) Focus on aerobic conditioning
b) Teach relaxation and positioning techniques
A client in the late-middle stage of ALS is struggling with mobility due to trunk weakness. Which feature is most important in a wheelchair recommendation?a) Tilt-in-space only
b) Manual propulsion capacity
c) Reclining back with headrest and padded supports
d) Lightweight transport frame
c) Reclining back with headrest and padded supports
Which of the following precautions is MOST important to follow when working with a client who has ALS?
a) Encourage high-intensity strength training
b) Ensure activities require maximal effort
c) Avoid fatigue and monitor for respiratory distress
d) Increase stretching frequency to improve strength
c) Avoid fatigue and monitor for respiratory distress
Multiple Sclerosis (MS)
-myelin sheath destruction (brain and spinal cord affected)
-disruptions in nerve impulse conduction
"leaky hose" - they have the mvmt, but it is very slow and weakened
what is myelin?
fatty protein that surrounds nerves and aids in transmission of nerve impulses
MS has a __________ decline in function
slow
does MS have periods of exacerbation and remission?
yes!!!!
what is the most common progressive, inflammatory neurologic disease in young adults
MS
3 types of MS
1) Relapsing-remitting
2) Secondary progressive
3) Primary progressive
relapsing-remitting MS
most common type of MS (70-80%)
episodes of exacerbation and remission
-full recovery or
-partial recovery with residual deficits
no progression between relapses
step-wise decline
what type of MS has a step-wise decline?
relapsing-remitting MS
type of MS that has periods of exacerbation and remission
relapsing-remitting MS
secondary progressive MS
-begins with periods of exacerbation and remission
-develops into primary progressive (no remission)
type of MS that begins with periods of exacerbation and remission that develops into primary progressive MS.
secondary progressive
primary progressive MS
-affects 10-15%
-progressive disease from onset
-no distinct relapse
-may have occasional plateaus or minor improvements
type of MS that is progressive from onset and has no distinct relapse stage
primary progressive MS
what causes MS?
specific cause unknown
theories of
-allergies
-slow-acting virus
-autoimmune disorder
-genetic susceptibility
MS is more common in
a) men
b) women
b) women
t or f: MS more common in caucasians of European descent.
true
onset of MS
approx. 15-50 yrs of age
functional limitations associated with MS
-exacerbations of muscle weakness
-increased fatigue
-visual impairment
-loss of sensation (touch, pain, and/or temp.)
-loss of position in space
-dysphagia
-cognitive deficits
visual impairment is associated with which degenerative disease?
MS
loss of sensation (touch, pain, and/or temp.) is associated with which degenerative disease?
MS
what cognitive deficits are prevalent with MS?
-inattention, distractibility
-short attention span, difficulty concentrating
-short-term memory loss
-difficulty learning or forming new concepts
-poor judgment and impulsivity
-emotional lability
-dysarthria
can you teach a patient with MS new strategies on how to perform a task?
not really!
they have short-term memory loss and have difficulty learning new concepts
emotional lability is common with which degenerative disease?
MS
OT intervention for ADL/self-care (MS)
-energy conservation, pacing techniques, simplification, proper body mechanics
-AE
-instruction in safe transfer techniques
-home safety evals
OT intervention for productivity (MS)
-environmental modifications
-task performance adaptations
-alternative work/volunteer opportunities
OT intervention for sensorimotor (MS)
-maintain/increase UE strength through PRE (avoid fatigue)
-maintain/improve coordination
-maintain/increase endurance (alternating physical task demands)
-increase tactile skill to compensate for visual impairment
-teach sight inspection for skin integrity
t or f: we can strengthen with MS patients.
true!!!!
just always be sure to monitor PRE to avoid fatigue and injury! (fatigue can cause exacerbations of disease)
OT intervention for cognition (MS)
-time management strategies (energy conservation, pacing, work simplification)
-external memory aids
-cognitive strategies for coping
precautions associated with MS
-remissions do not mean complete return of PLOF
-inactivity can lead to decreased endurance and muscle atrophy
-avoid heat and stress
-monitor PRE to avoid fatigue and injury
-use of vision may not compensate for sensory loss
-increased fall risk
t or f: remissions in MS do not mean complete return of prior level of function.
true
t or f: with MS, inactivity can lead to decreased endurance and muscle atrophy
true
which degenerative disease should avoid heat and stress?
MS
t or f: fatigue can cause an exacerbation in MS.
true
t or f: with MS, use of vision may not compensate for sensory loss; therefore we should always assess vision before providing compensatory techniques.
true
A 42-year-old client with secondary-progressive MS is concerned about maintaining employment as their endurance declines. What should the OT focus on FIRST when addressing vocational needs?
a) refer to a social worker to file for disability
b) educate the employer about MS and request reduced hours without client consent
c) conduct a job analysis and suggest reasonable accommodations
d) encourage the client to resign to avoid stress
c) conduct a job analysis and suggest reasonable accommodations
During a home safety evaluation for a client with MS experiencing fluctuating mobility, what is a critical modification to recommend?
a) Use of bright lights to enhance sensory input
b) Grab bars in the bathroom and stair rails
c) Manual wheelchair for outdoor use only
d) Avoid nonslip mats in showers
b) Grab bars in the bathroom and stair rails
A client with MS wishes to continue working but is experiencing reduced tolerance and memory lapses. Which approach would the OT take first?
a) Recommend full disability leave
b) Introduce external memory aids and modify workload schedule
c) Refer for vocational retraining immediately
d) Encourage the use of memory-intensive tasks to build cognition
b) Introduce external memory aids and modify workload schedule
An OT is treating a client with MS who has mild upper extremity weakness. What strengthening recommendation is appropriate?
a) Daily weightlifting with progressive resistance
b) Functional PRE, with careful monitoring to avoid fatigue
c) Strength training to fatigue at least 3 times a week
d) Avoid all strengthening to prevent exacerbations
b) Functional PRE, with careful monitoring to avoid fatigue
Which OT strategy would best help a client with MS who has visual impairments and reports bumping into furniture?
a) Limit light to reduce overstimulation
b) Recommend alternating sensory tasks with rest
c) Incorporate tactile cues and teach scanning techniques
d) Instruct the client to rely more on vision for orientation
c) Incorporate tactile cues and teach scanning techniques
A client with MS is having difficulty remembering steps during meal preparation. What is the most appropriate OT strategy?
a) Have the client complete tasks from memory repeatedly
b) Provide verbal directions only once per session
c) Use step-by-step visual cue cards and timers
d) Focus on strength-based cognitive training only
c) Use step-by-step visual cue cards and timers
Which of the following is the most important precaution when working with a client with MS during therapy?
a) Increase activity intensity to build tolerance
b) Use heat modalities to improve joint flexibility
c) Avoid fatigue and overheating during sessions
d) Prioritize passive ROM to prevent spasticity
c) Avoid fatigue and overheating during sessions
Why should strengthening programs for MS patients be carefully monitored?a) MS clients are typically hyperactive and need calming
b) Inactivity leads to sensory loss
c) Overexertion may lead to increased fatigue and exacerbation
d) Strength training accelerates MS progression
c) Overexertion may lead to increased fatigue and exacerbation
Parkinson's disease
a progressive disease of basal ganglia that destroys brain cells and is identified by muscular tremors, slowing of movement, and partial facial paralysis
parkinson's has a __________ decline in function
slow
which two degenerative diseases have a slow decline in function?
MS and parkinsons
what is parkinson's characterized by?
-akinesia
-bradykinesia
-rigidity
-resting tremor ("pilling")
-postural instability
akinesia
loss or impairment of voluntary movement
bradykinesia
slowness of movement
rigidity
stiff movements, increased tone
disturbances in gait and postural reactions are key characteristics of which degenerative disease?
parkinon's
Parkinson's gait characteristics
-wide BOS
-shuffling
-looking down
-lack of/slowed protective reactions
t or f: patients with parkinson's typically have decreased facial expressions, also known as a masked face.
true
why do patients with parkinson's often have undiagnosed depression?
because of the typical characteristic of a masked facial appearance and low tone in voice
-symptom overlap, the impact of Parkinson's on mood, and potential misattribution of depression symptoms to the disease itself
-symptoms of depression, like fatigue, sleep disturbances, and difficulty concentrating, also occur in Parkinson's
**their depression is not only reactive to the disease!
are cognitive deficits prevalent with parkinson's? if so, what are they?
yes!!
-memory loss and dementia
-loss of spatial orientation