Module 1 - Blood
1/39
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
40 Terms
Leukocytes
White blood cells (WBCs)
Leukocyte function
Main defense inside the body → defend against invading microorganisms and defective body cells (old cells, cells with defective DNA, virus infected cells)
Characteristics of leukocytes
Less abundant than RBCs
Much larger than RBCs
Only formed elements that are complete cells
Much shorter lifespan than RBCs
Diapedesis
WBCs can leave capillaries or small blood vessels to perform defense functions in tissues
→ some WBCs leave the bloodstream to enter a tissue but remain fixed there instead of reentering the bloodstream
Chemotaxis
Process by which leukocytes are attracted o infection by nearby chemical signals
Granular leukocytes
Leukocytes that contain granules, produced in red bone marrow, have lobed nuclei
Neutrophils
Eosinophils
Basphils
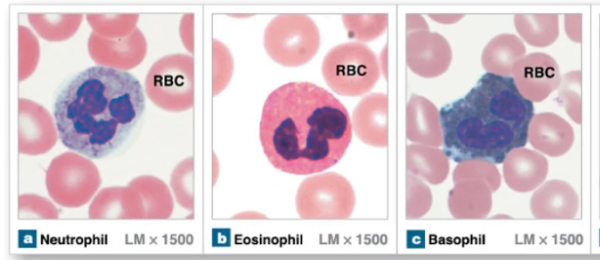
Agranular leukocytes
Leukocytes that lack granules
Monocytes
Lymphocytes
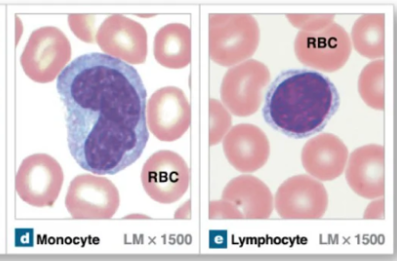
Neutrophils
Rapid responders to infections → bacterial and acute infections
Granules stain light purple and are in the nucleus
Nuclei have 2-5 lobes
Capable of phagocytosis
Most abundant leukocyte
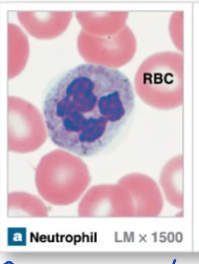
Eosinophils
Granular leukocyte that is mainly involved in allergic reaction and parasitic infections
Granules are large and stain red-orange color
Nuclei have 2 lobes
Capable of phagocytosis
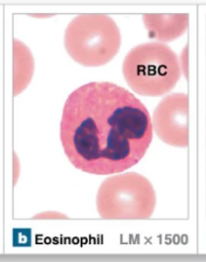
Neutrophil granules
Lysozyme → enzyme to lyse bacteria cell walls
Defensins → proteins that puncture bacterial and fungal cell walls
Eosinophil granules
Antihistamine molecules → counteract histamine to balance inflammatory response
Molecules toxic to parasitic worms
Basophils
Granular leukocytes that intensify immune response → allergic reactions and inflammation
Large granules that stain dark blue → can make it hard to see nucleus
Nuclei have 2 lobes
Release histamine and heparin
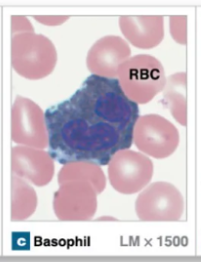
Basophils release…
Histamine → inflammatory chemical, vasodilator, attracts other WBCs
Heparin → opposes blood clotting
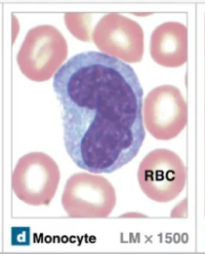
Monocytes
Agranular leukocytes that originate form myeloid stem cells that are a type of macrophage → chronic infections
Large size and have a U-shaped nucleus
Can leave circulation to enter tissues
Help activate lymphocytes and engulf pathogens
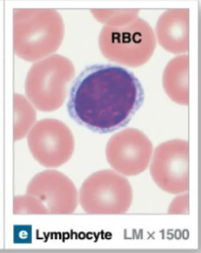
Lymphocytes
Agranular leukocyte that arises from lymphoid stem cells
There are 3 kinds: NK cells, B cells, and T cells
Have large round nucleus with very little cytoplasm
Initially form in bone marrow and mature in lymphatic tissues
Natural killer (NK) cells
Type of lymphocyte that recognizes non-self cells or abnormal surface proteins on cells and kills them locally
Generalized, non-specific immunity because they don’t need prior exposure to act
Identifies cells as cancerous or virus-infected
B lymphocytes (B cells)
Type of lymphocytes that form plasma cells that produce antibodies (Y-shaped proteins)
Antibodies circulate in bloodstream and bind to pathogens to mark them for destruction
T lymphocytes (T cells)
Type of lymphocyte that kills virus-infected cells or tumor cells by secreting local toxins to kill cells directly
Platelets (thrombocytes)
Cell fragments (not true cells) that form clots and secrete growth factors for tissue growth and repair
Cytoplasm fragments off of megakaryocytes (large bone marrow cells that produce platelets)
Megakaryocytes
Large cells with lobed nuclei in the bone marrow that produce platelets
Release 2000-3000 platelets per lifetime
Get phagocytized by macrophages after they have release all of their cytoplasm
Thromboprotein
Hormone secreted by the kidneys and liver to stimulate the growth of megakaryoblasts (cells that mature into megakaryocytes)
Hemostasis
Process where the body seals a rupture blood vessel to prevent further blood loss
Ending “-penia”
Too few of a type of blood cell
Ending “-cytosis”
Too many of a type of blood cell
Leukopenia
Too few WBCs being produced → can be caused by chemotherapy
WBCs are the body’s main defense so not having enough leaves someone vulnerable to infection
More susceptible to life-threatening complications
Leukocytosis
Too many leukocytes being produced
Having too many means they aren’t being formed properly → you have a lot of them but they aren’t fully functional or working the right way
Makes you vulnerable because WBCs aren’t killing pathogens like they should be
More susceptible to life-threatening complications
Leukemia
Form of cancer caused by an abundance of leukocytes
Leukocytes are not developed properly → a lot of them but they don’t work
Lymphoma
Form of cancer caused by cancerous B and T cells → malignant B and T cells begin to collect in the liver and the spleen, lymph nodes, and liver
B and T cells don’t function properly leaving someone vulnerable to infection
Thrombocytosis
Too many platelets in circulation → blood clots more frequently than it should so blood clots form where they aren’t needed
Thrombocytopenia
Too few platelets in circulation → results in lack of clotting which can cause excessive bleeding
Process of Hemostasis
Vascular spasm
Formation of platelet plug
Coagulation cascade
Clot retention
Hemostasis: 1) vascualr spasm
Smooth muscle in vessel wall constricts to reduce blood flow after injury
Occurs immediately after vessel wall is damaged or severed → endothelins are released by cells in vessel walls that trigger vasoconstriction
Helps minimize blood loss
Hemostasis: 2) Formation of platelet plug
Platelets form a temporary seal to buy time for the body to make a more durable clot
Platelets are activated and transition from being smooth to spiky → they clump together at the vessel opening and form a plug
Platelets release chemicals
ADP → helps more platelets stick to injury site
Serotonin → helps maintain vasoconstriction and enhances platelet aggregation
PDGF (platelet derive growth factors) → attract cells called fibroblasts
Von Willebrand factor
Bridge between platelets and collagen so that the platelets stick to that area
Hemostasis : 3) Coagulation cascade
Series of clotting reactions that form fibrous network (fibrin mesh) that lays overtop platelets → reinforce the platelet plug
Main goal is converting fibrinogen (soluble) into fibrin (insoluble) → done one of two ways
Intrinsic pathway
Extrinsic pathway
Intrinsic pathway (contact activation pathway)
Method of coagulation cascade has more steps and is more complex → gets completed in minutes
Factors in the blood activate factor XII → ex: exposed collagen in blood vessel
Clotting factors
Proteins in blood plasma circulating in the blood, ready but not active (must be activated)
Part of coagulation cascade because an activated clotting factor activates more clotting factors
Where do clotting factors come from?
They are secreted by the liver
How many clotting factors are there?
12 known clotting factors
I