Anatomy 2 Practical
1/342
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
343 Terms
pulmonary ventilation
breathing
inspiration
air taken into lungs
respiratory muscles contract: intercostal muscles (rise) and diaphragm (flattens)
size of thoracic cavity increases and expands the attached lungs
intrapulmonary volume increases, lowering air pressure within lungs
causing air to flow into the lungs
nose
description: external portion supported by bone and cartilage; internal nasal cavity divided in half by midline nasal septum and lined with respiratory mucosa
function: produces mucus; filters, warms, and moistens incoming air; resonance chamber for speech. Receptors for sense of smell
pharynx
description: passageway connecting nasal cavity to larynx and oral cavity to esophagus; three divisions: nasopharynx, oropharynx, and laryngopharynx. Houses tonsils
function: passageway for food and air. Tonsils are lymphoid tissue that responds to inhaled or ingested antigens
trachea
description: flexible tube running from larynx and dividing inferiorly into two main primary bronchi; walls contain C-shaped cartilage that are incomplete posteriorly where trachealis muscle exists
function: air passageway; filters, warms, and moistens incoming air
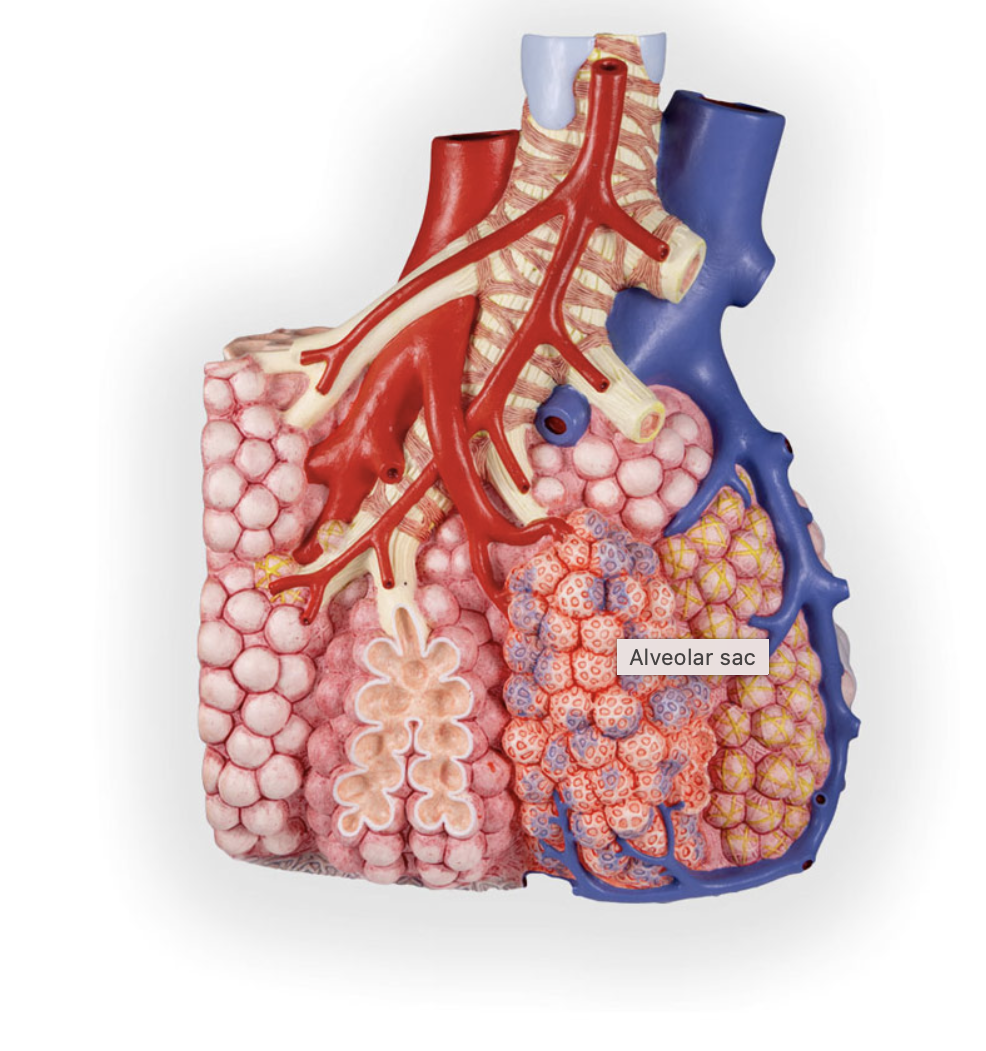
alveoli
description: microscopic chambers at ends of bronchial tree’ walls of simple squamous epithelium—type 1 alveolar cells—underlain by thin basement membrane’ external surfaces intimately associated with pulmonary capillaries. Simple cuboidal epithelium, consisting of type II alveolar cells, produces surfactant.
function: main sites for gas exchange. Surfactant reduces surface tension; help prevent lung collapse
lungs
description: paired composite organs surrounded by pleural cavities of thorax; composed primarily of alveoli and respiratory passageways; stroma is fibrous elastic connective tissue,k allowing lungs to recoil passively during expiration
function: house passageways smaller than primary bronchi
parietal pleura
description: lines thoracic cavity
function: produce lubrication fluid and compartmentalize lungs
visceral pleura
description: covers external lung surface
function: produce lubricatin fluid and compartmentalize fluid
tidal volume
volume of air exchanged with normal, quiet breathing
average male: 500 mL
average female: 500 mL
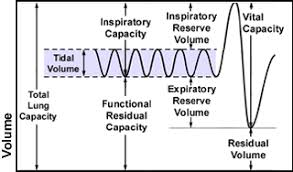
inspiratory reserve volume
maximum volume of air that can be forcibly inspired after a tidal inspiration
average male: 3100 mL
average female: 1900 mL
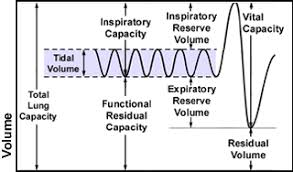
expiratory reserve volume
maximum volume of air that can be forcibly expired after a tidal expiration
average male: 1200 mL
average female: 700 mL
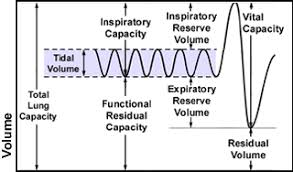
residual volume
volume of air that remains in the lungs after forced expiration
average male: 1200 mL
average female: 1100 mL
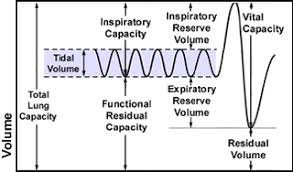
inspiratory capacity
total amount of air that can be inspired; equalt ot tidal volume plus inspiratory reserve volume
TV + IRV =
average male: 3600 mL
average female: 2400 mL
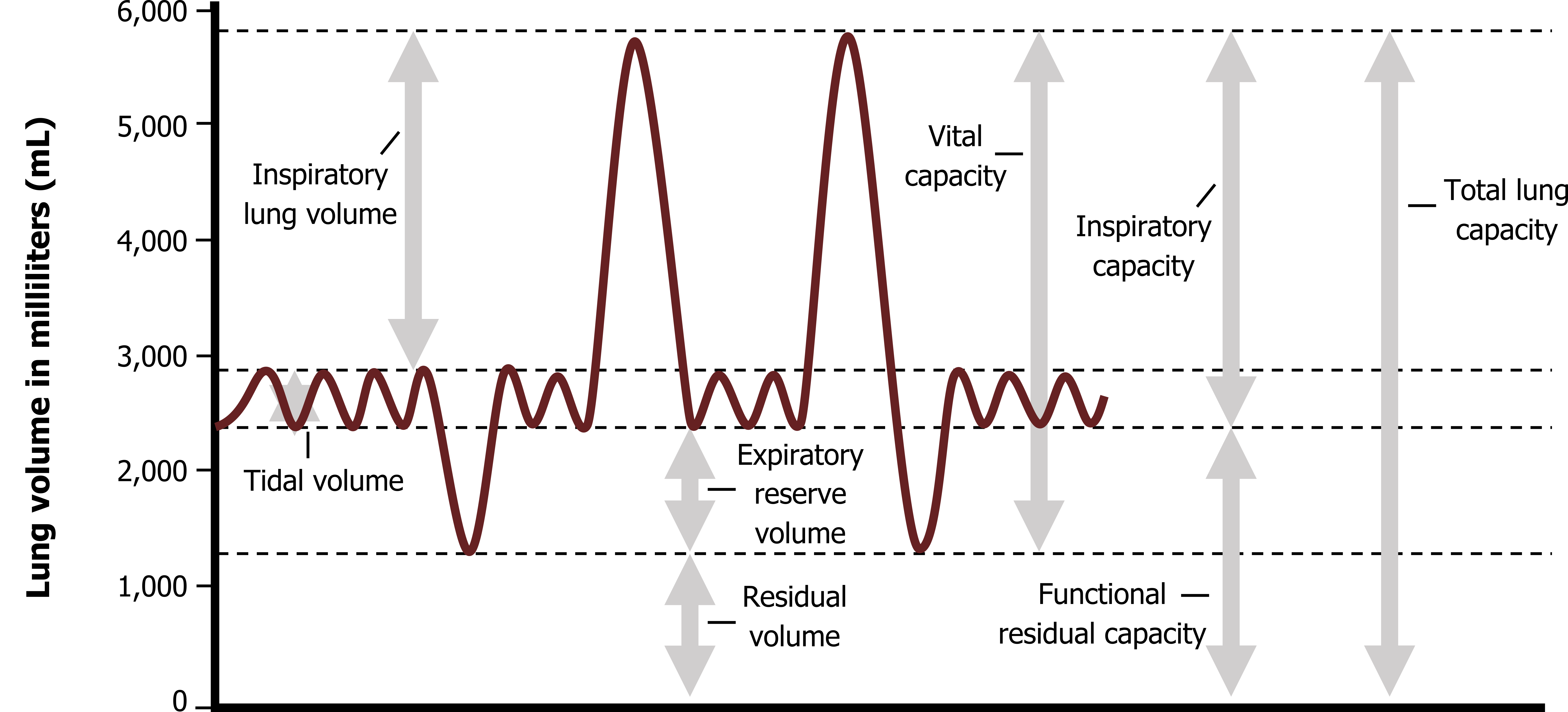
functional residual capacity
total amount of air that normally remains in the lungs after a tidal expiration; equal to the residual volume plus expiratory reserve volume
ERV + RV
average male: 2400 mL
average female: 1800 mL
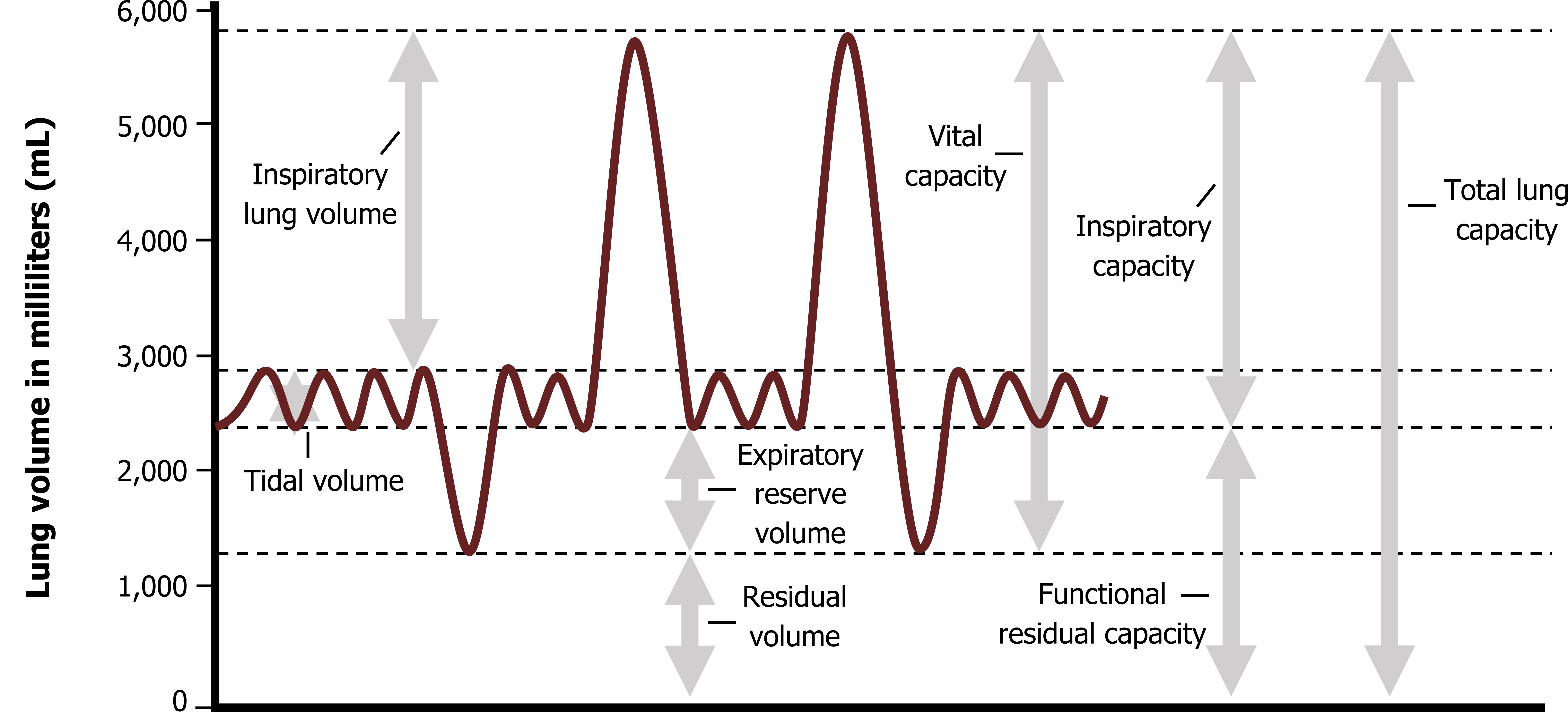
vital capacity
total amount of exchangeable air; equal to sum of the tidal volume, expiratory reserve volume, and inspiratory reserve volume
TV + IRV + ERV =
average male: 4800 mL
average female: 3100 mL
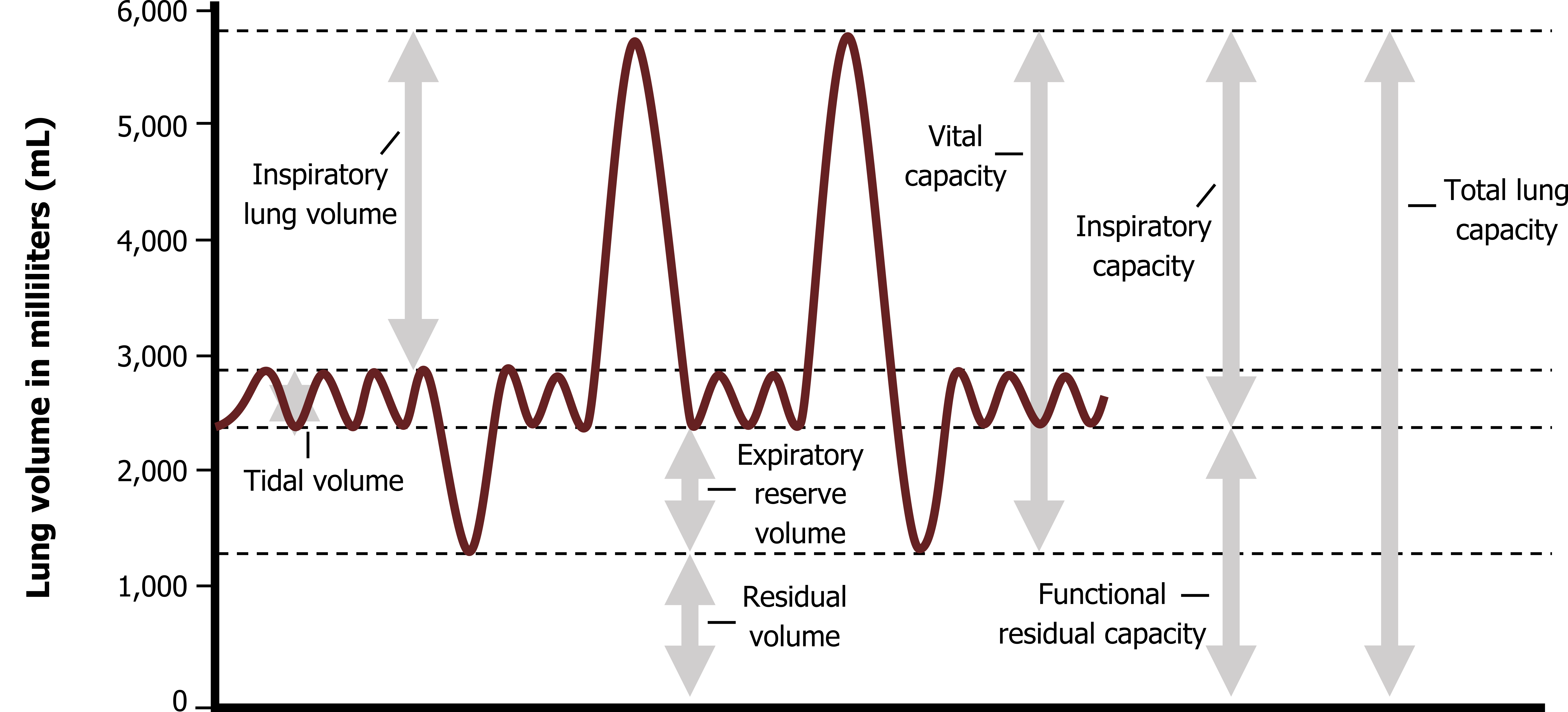
total lung capacity
total amount of exchangeable and nonexchangeable air; equal to the sum of all the pulmonary volumes
TV + IRV + ERV + RV =
average male: 6000 mL
average female: 4200 mL
thyroid cartilage
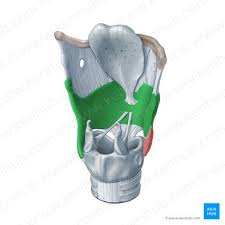
cricoid cartilage
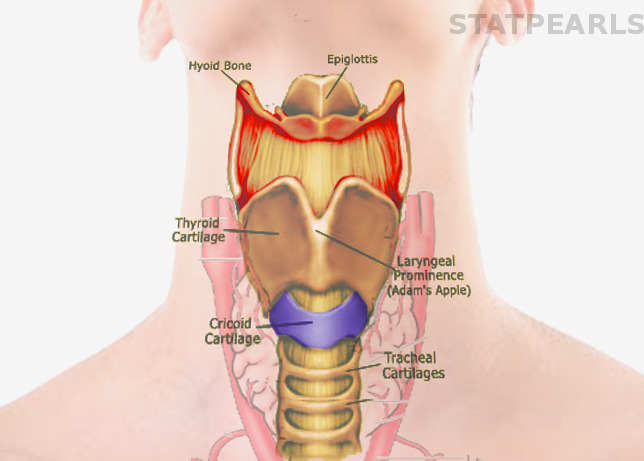
arytenoid cartilage
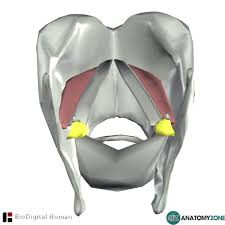
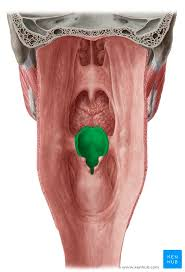
glottis
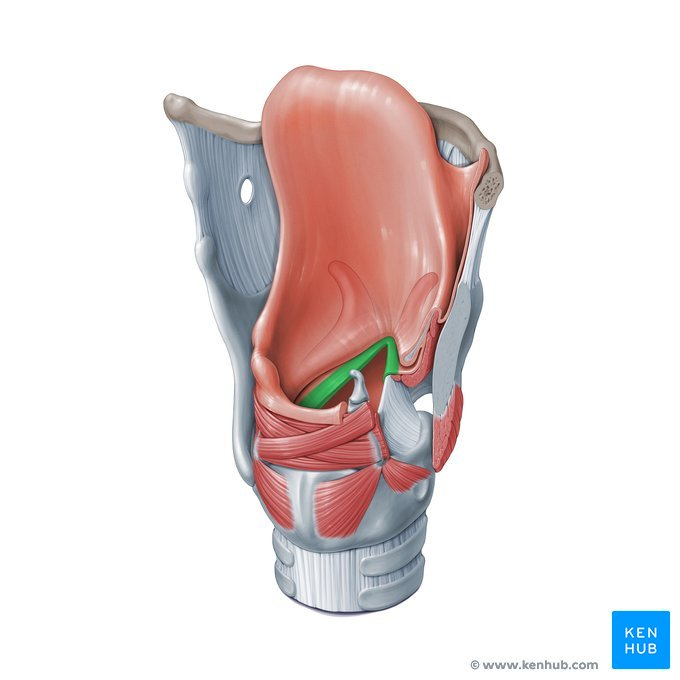
epiglottis
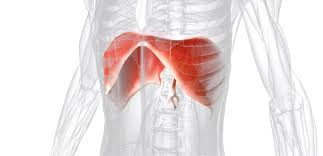
diaphragm
muscle of inspiration
contracts, moves inferiorly, and flattens, expanding the thoracic cavity and compressing the abdominal organs
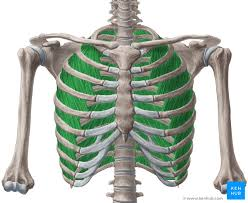
external intercostal muscle
muscle of inspiration
pull the ribs up and out to further expand the thoracic cavity
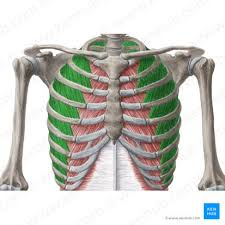
internal intercostal muscle
muscle of expiration
pull the ribs down and in, compressing the thoracic cavity during forced expiration
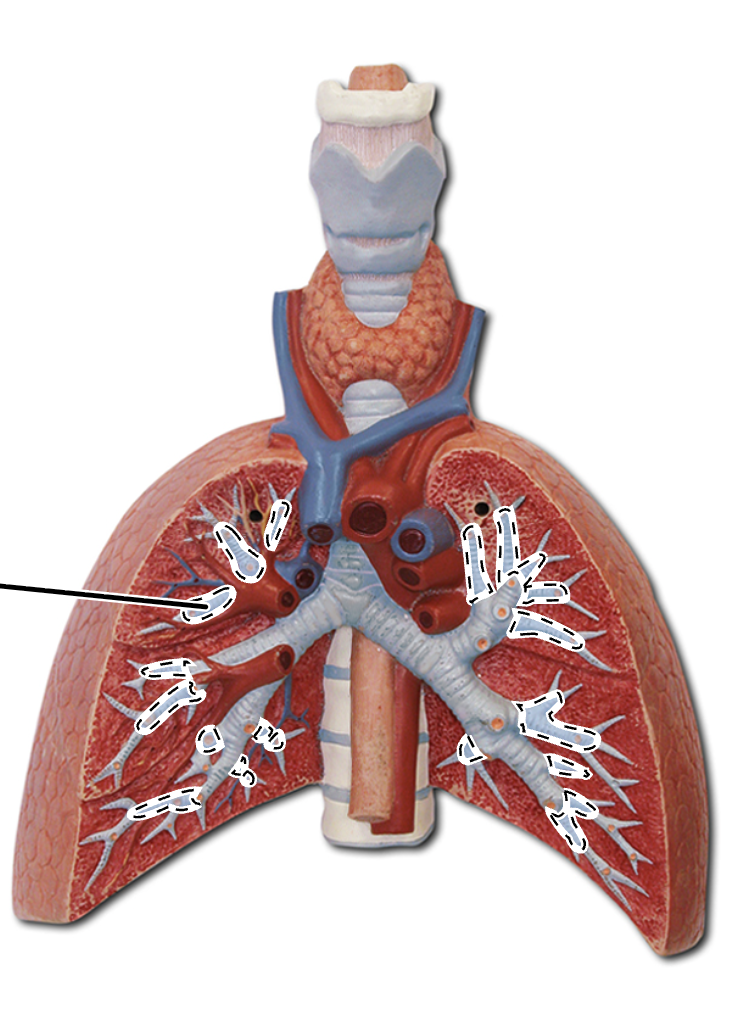
primary bronchi
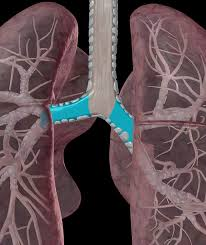
secondary bronchi
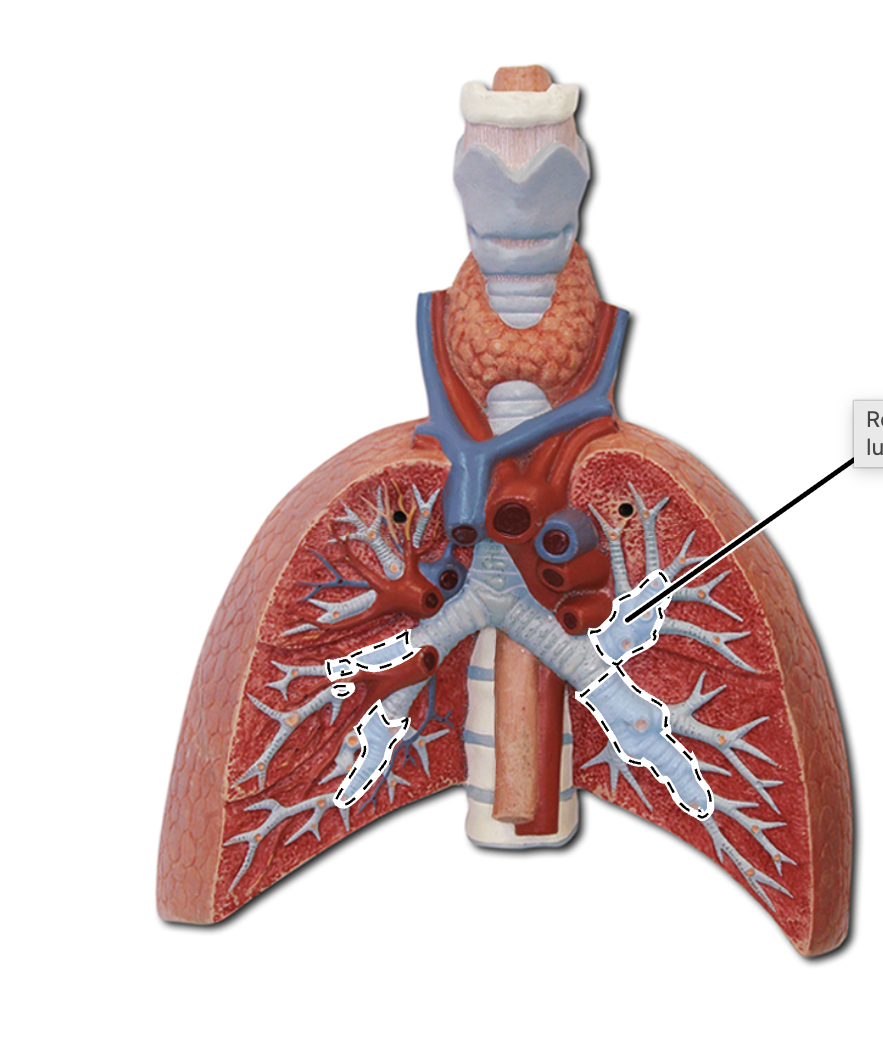
segmental bronchi
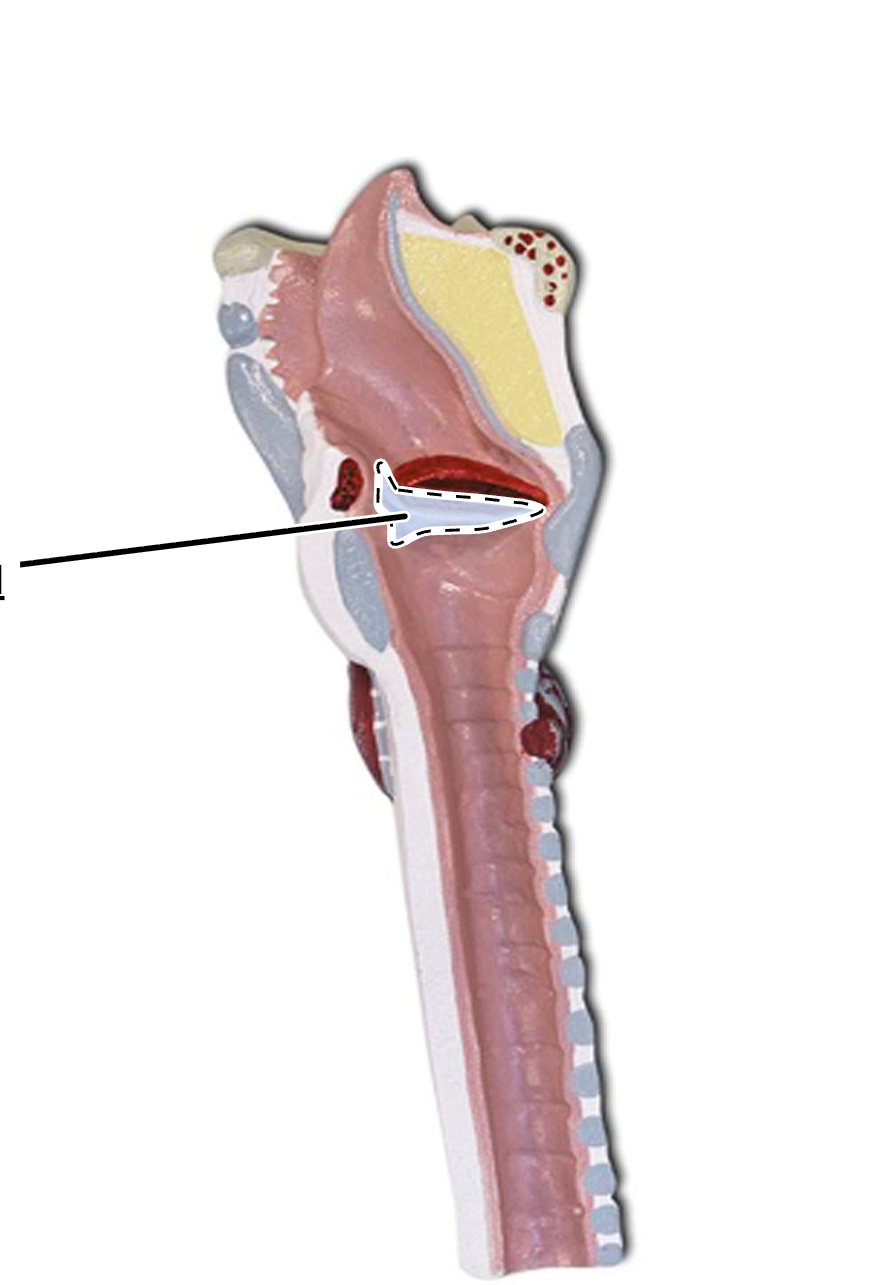
vocal folds
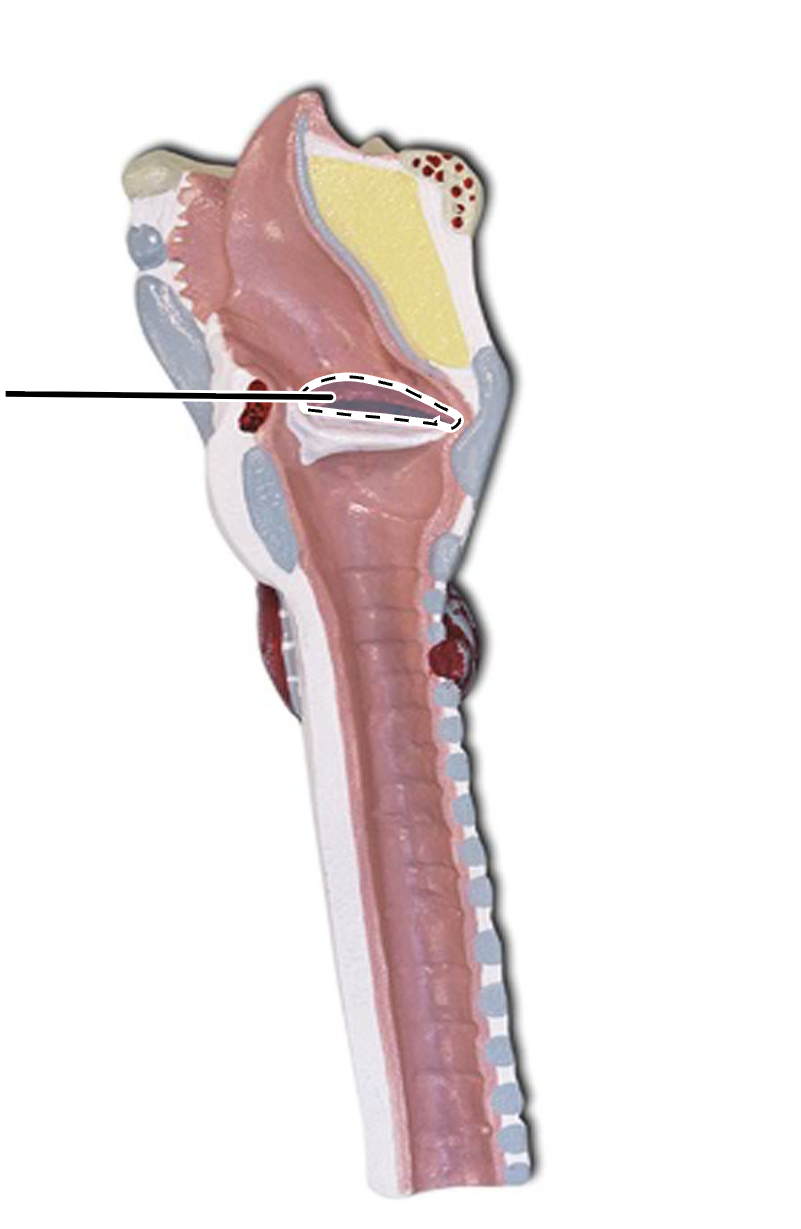
vestibular folds
right superior lung lobe
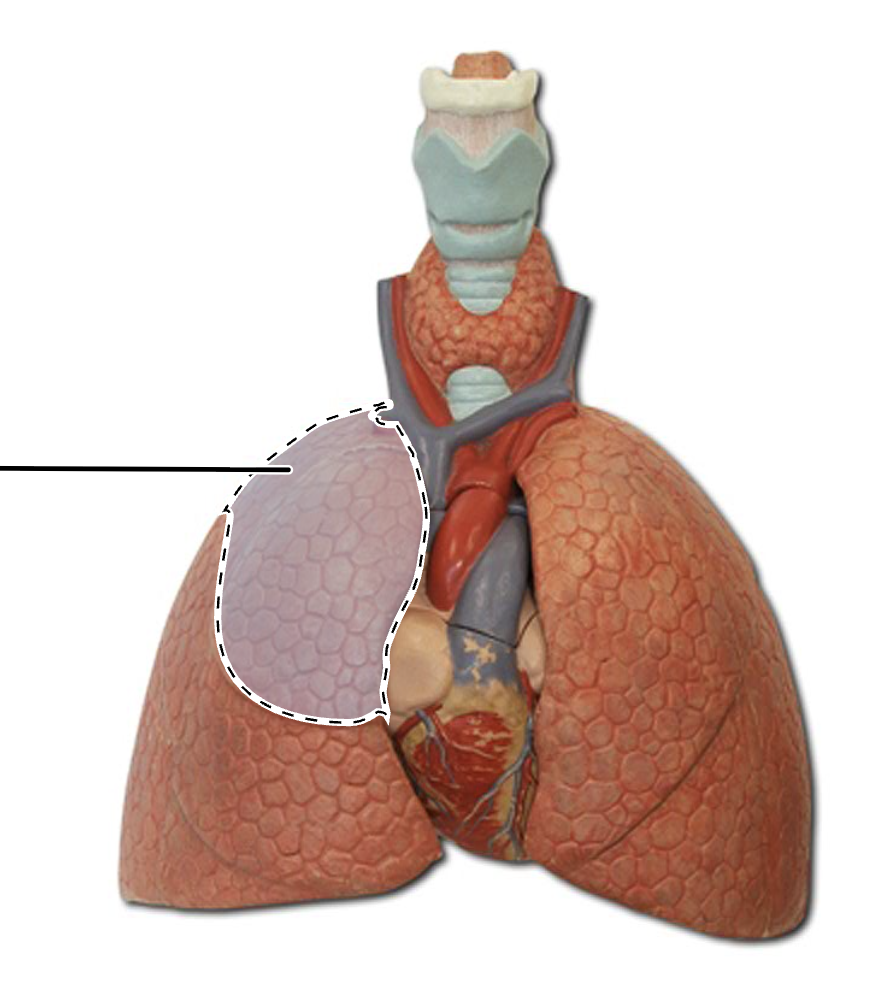
right middle lung lobe
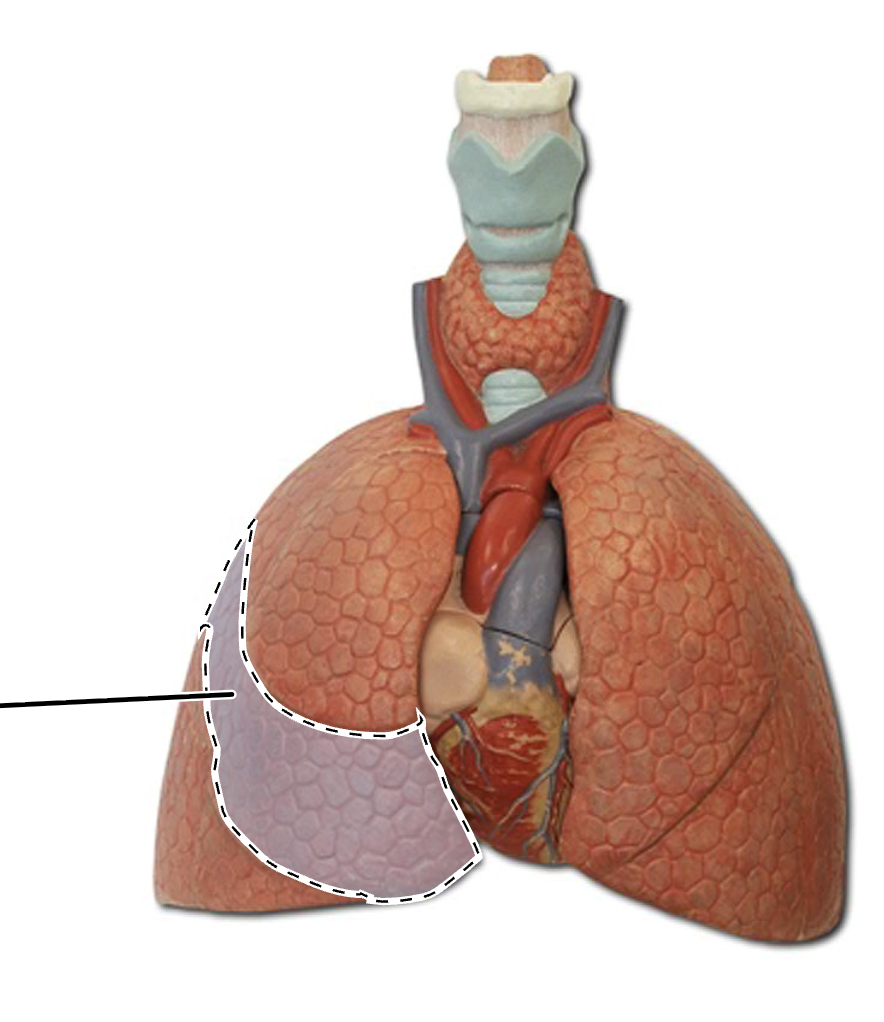
right inferior lung lobe
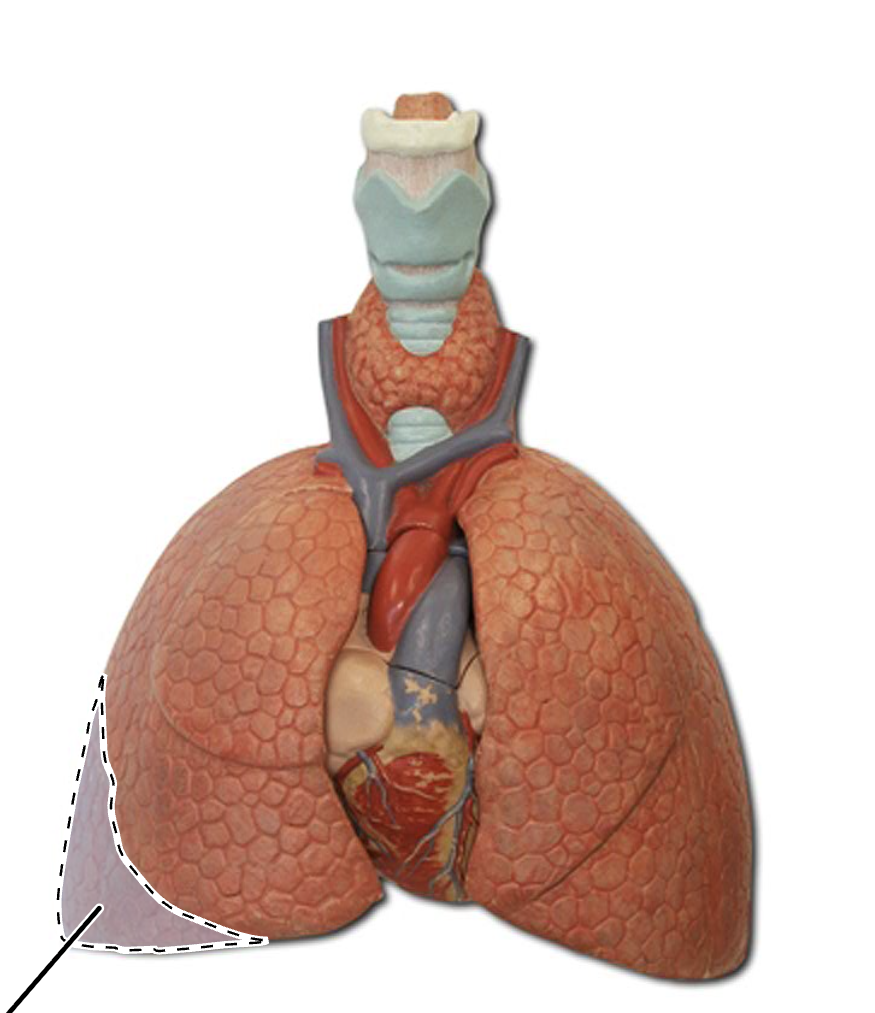
left superior lung lobe
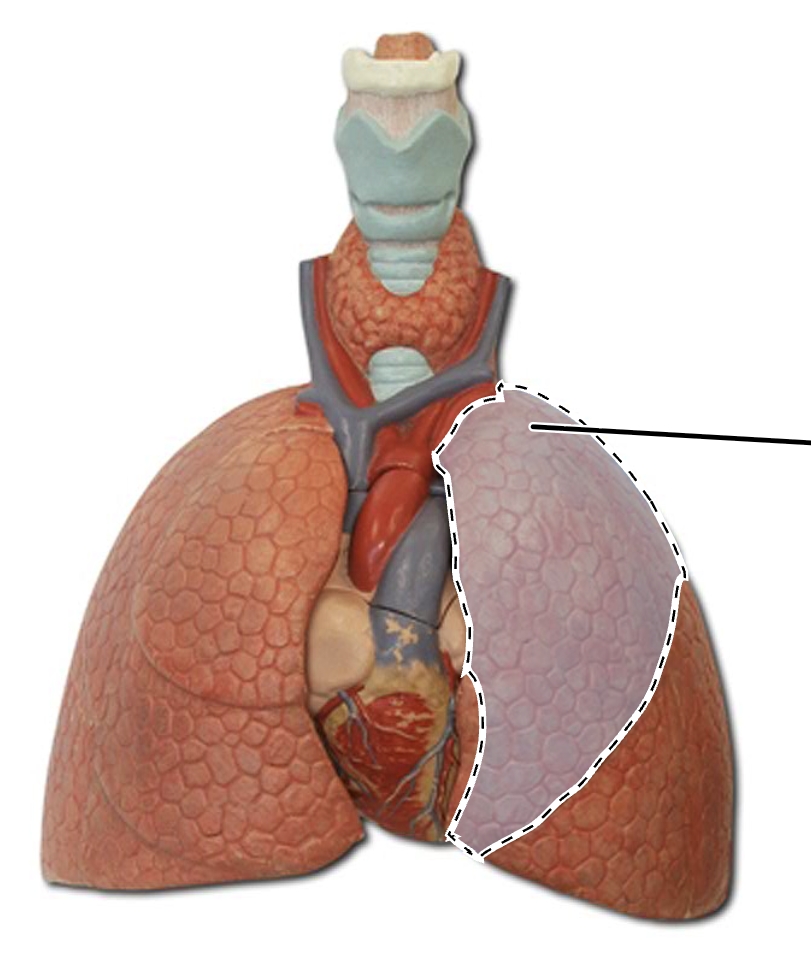
left inferior lung lobe
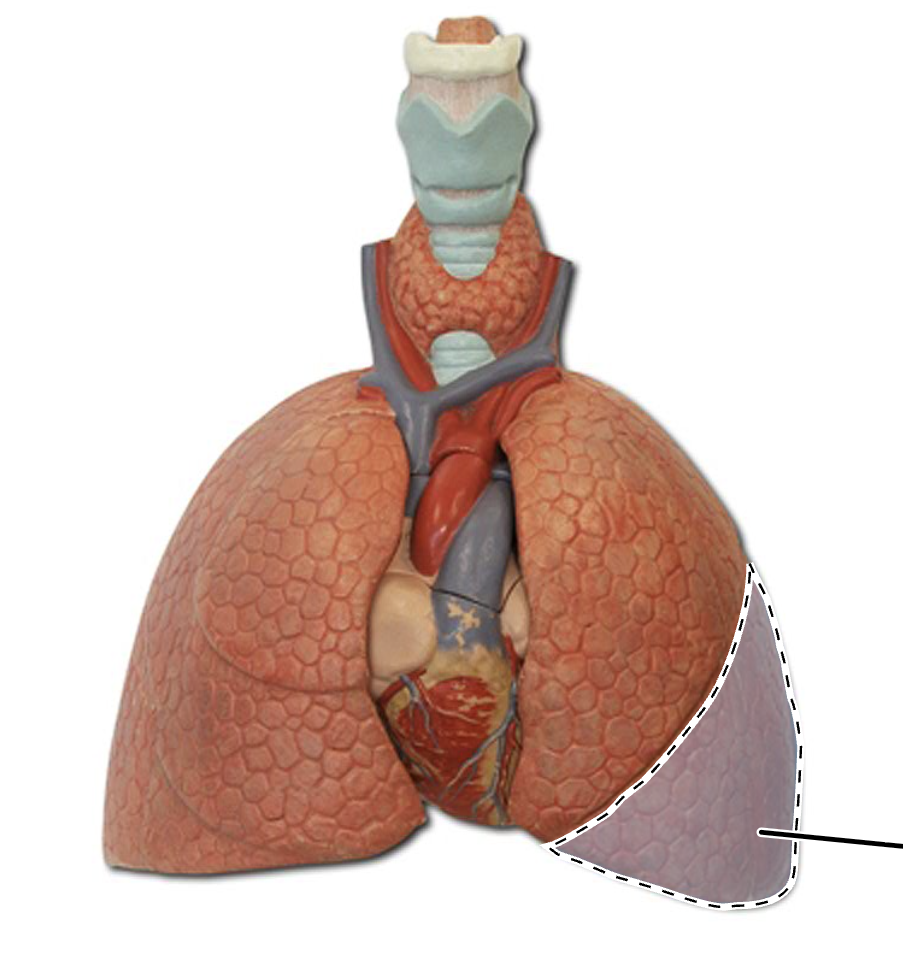
horizontal fissure
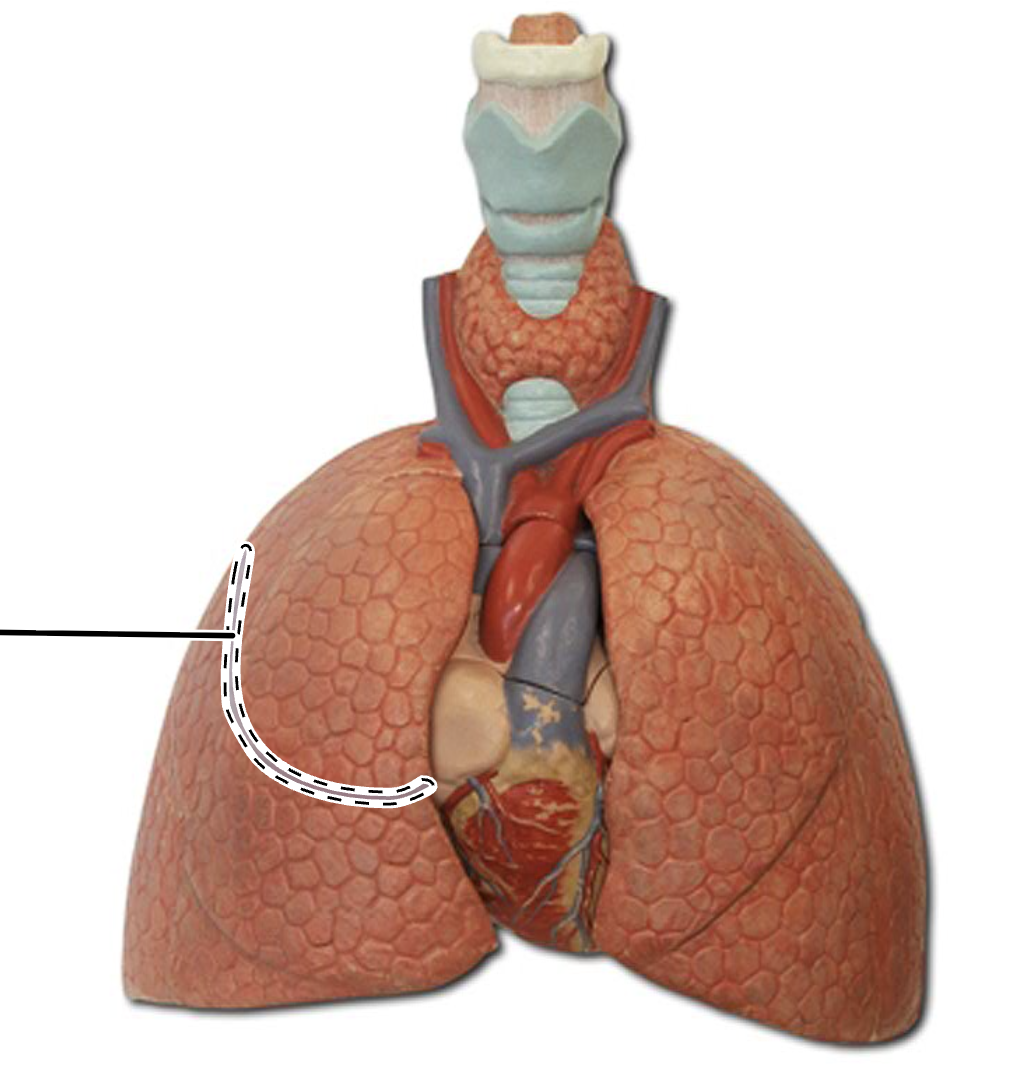
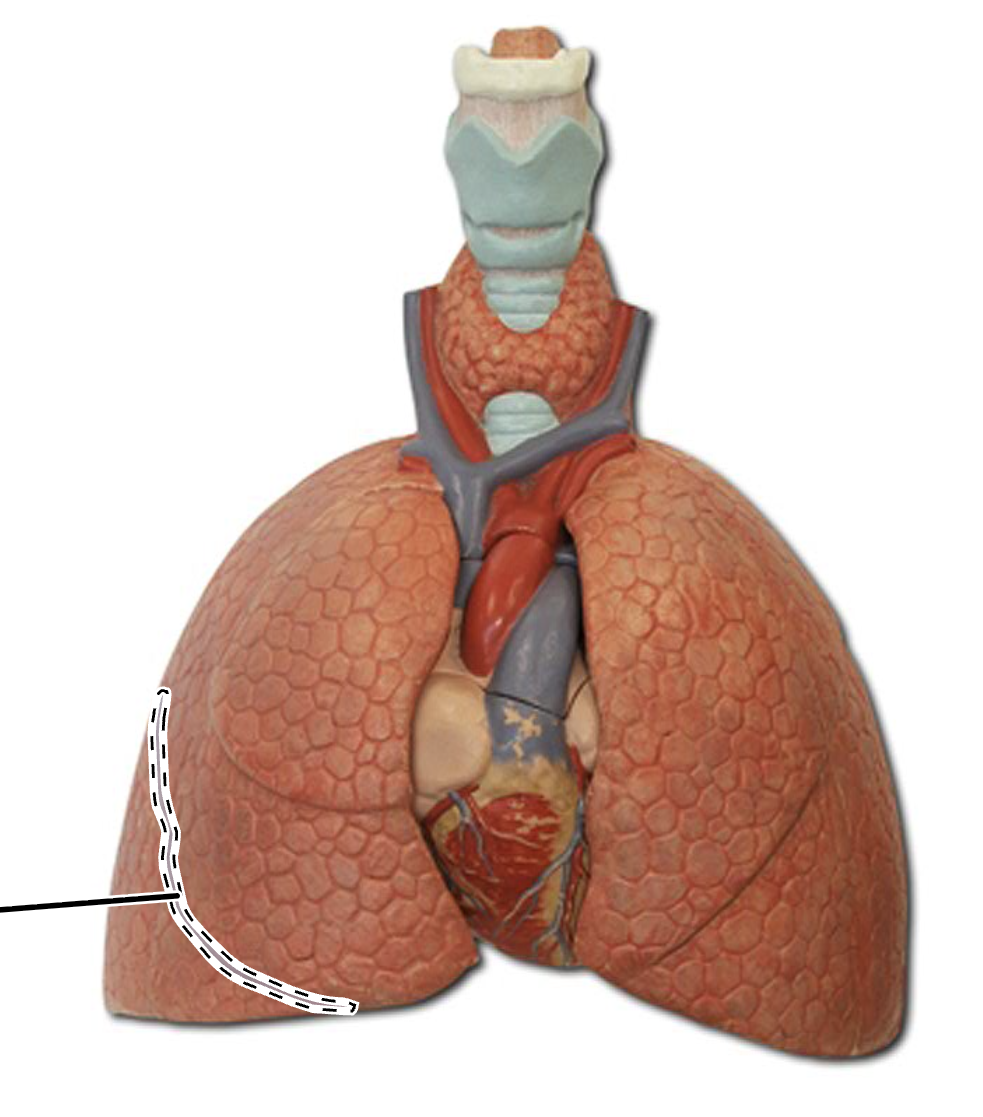
oblique fissure
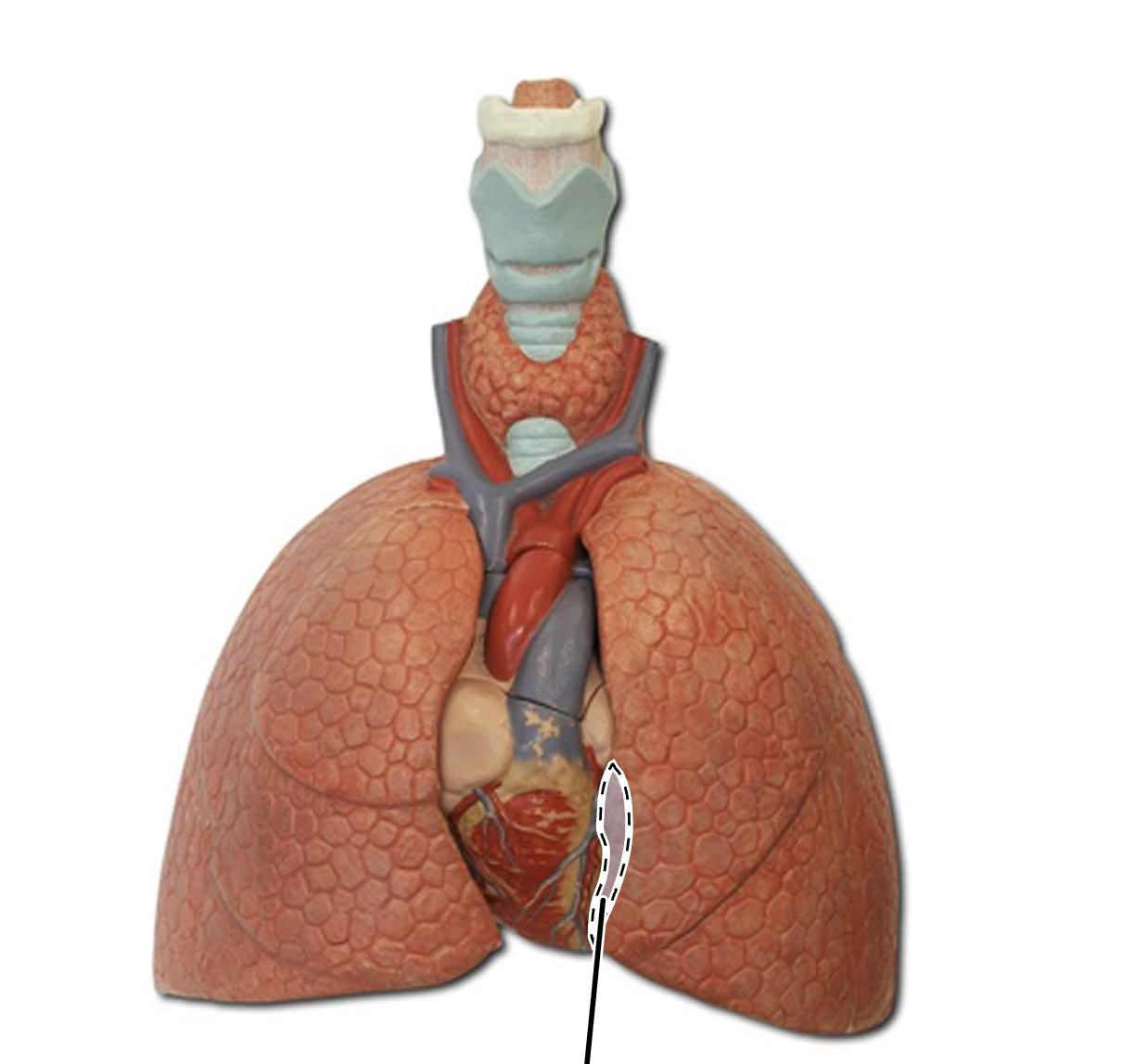
cardiac notch
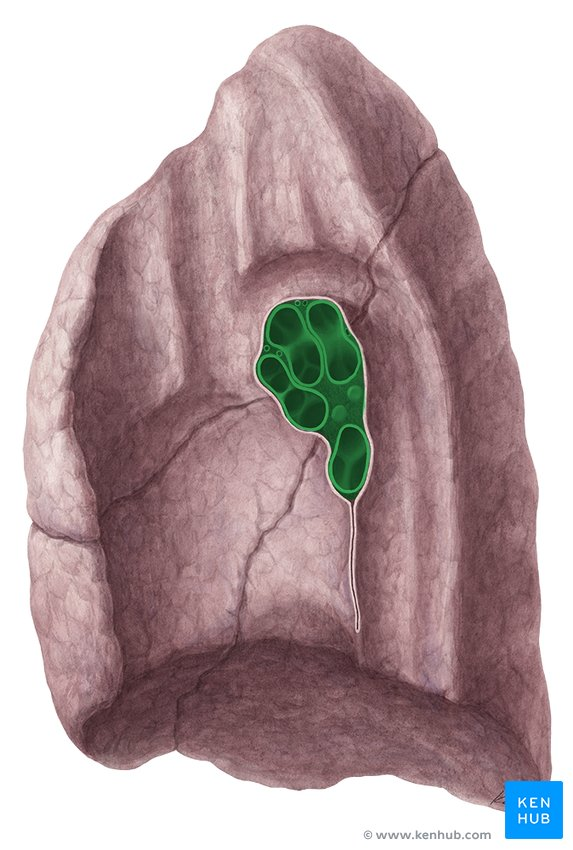
hilum (lung)
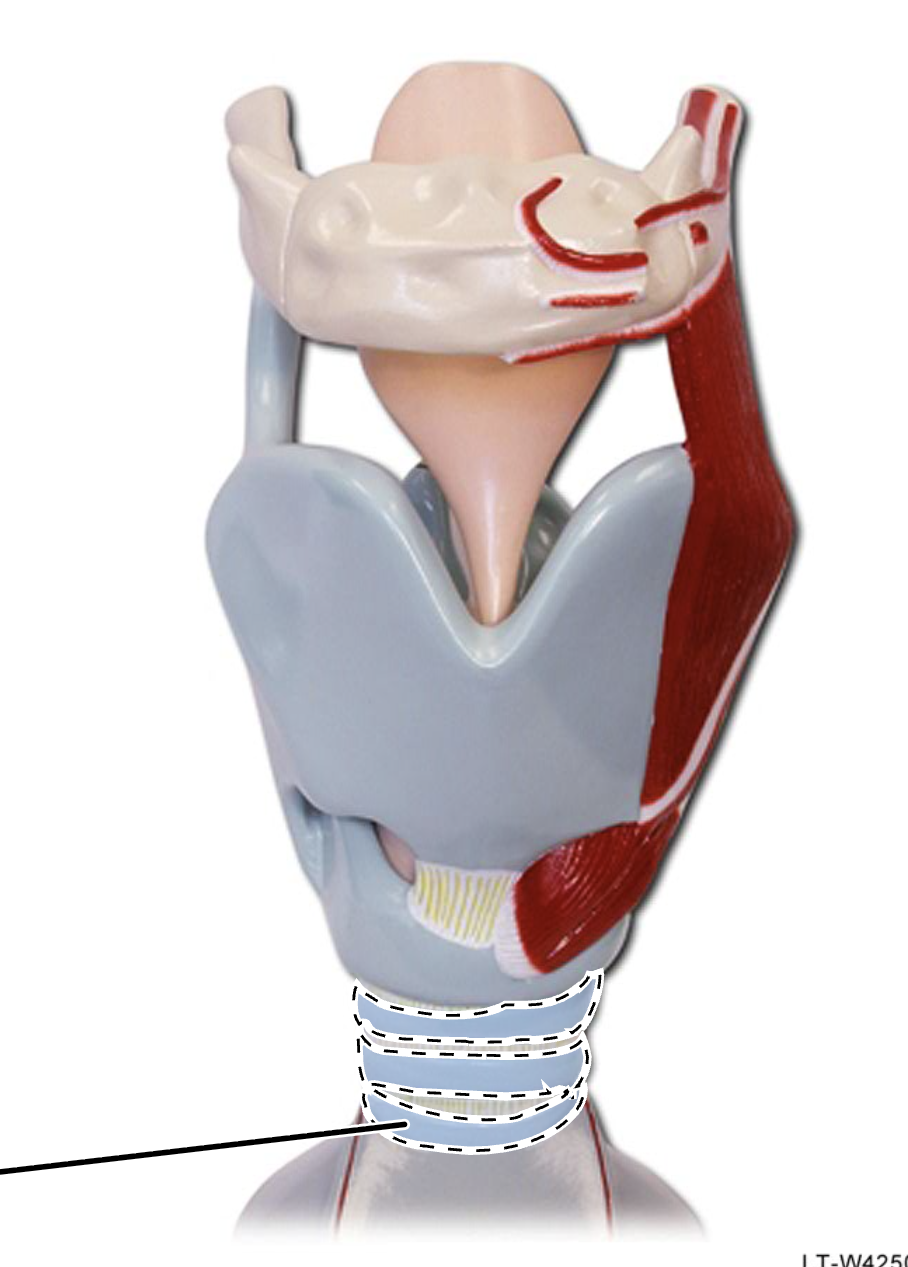
tracheal cartilage rings
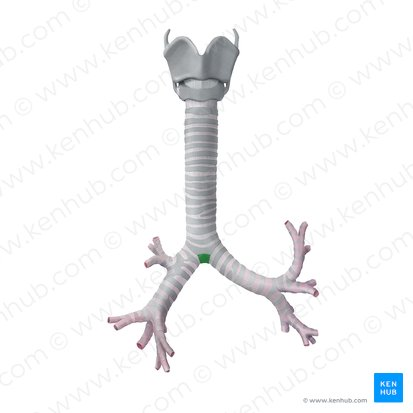
carina
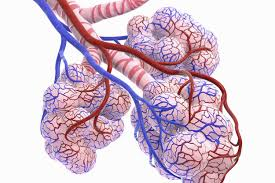
alveolar sacs
elastic baskets
*structure that has yellow lining
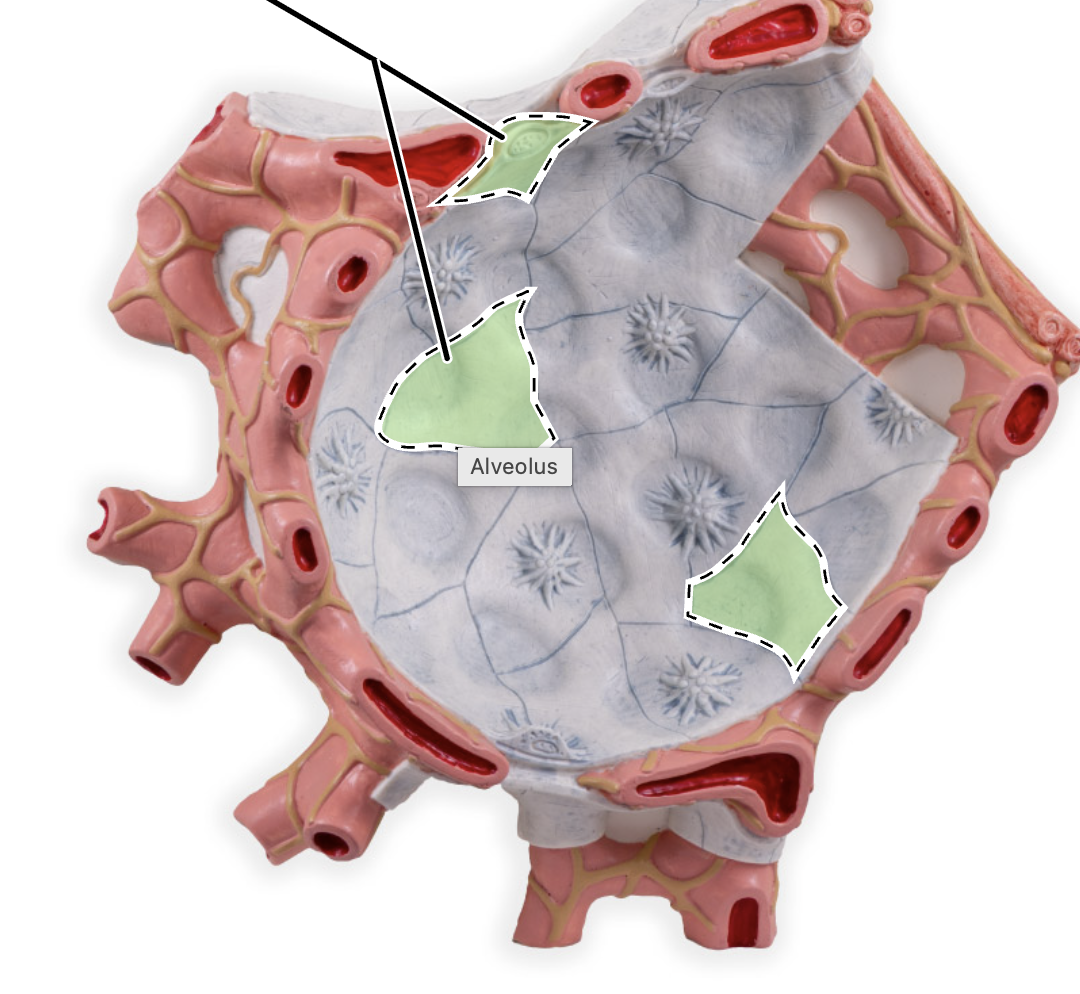
type 1 alveolar cells
conducting bronchioles
the smallest bronchi lead to this type of bronchiole
lined with simple columnar epithelium
respiratory bronchioles
conducting bronchioles lead to this type of bronchiole
lined with simple squamous epithelium
they later lead to alveolar ducts.
alveolar duct
structure that leads into alveolar sacs
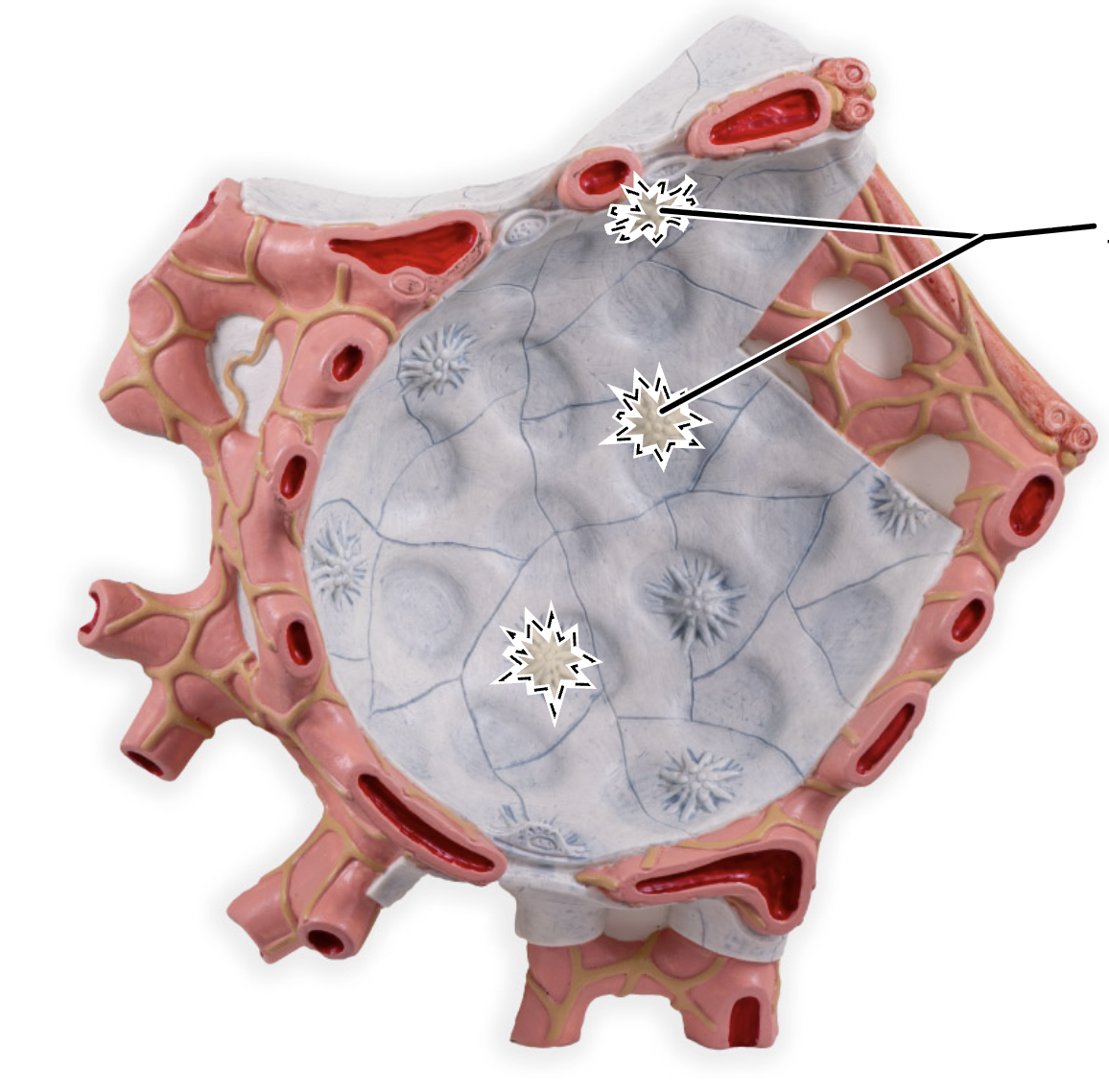
alveolar macrophage
pulmonary arteriole
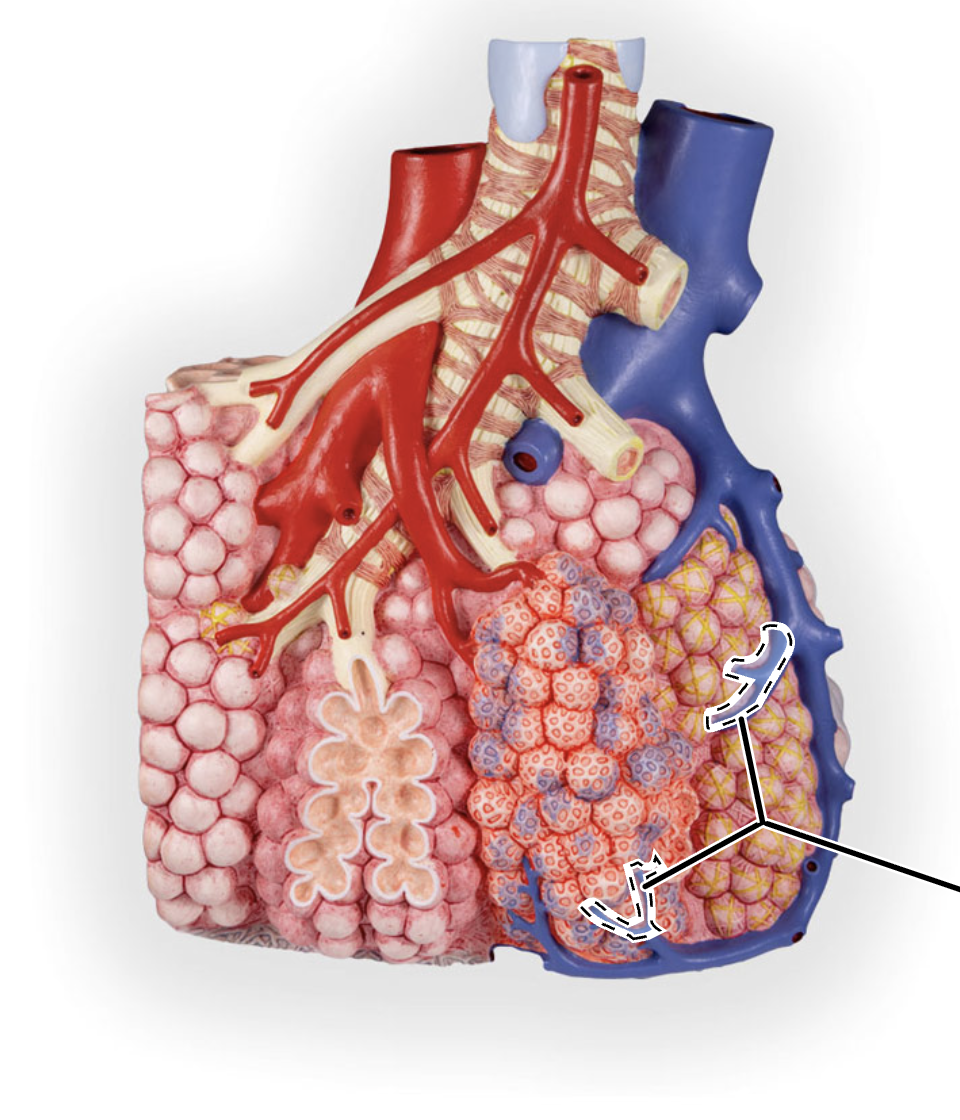
pulmonary venule
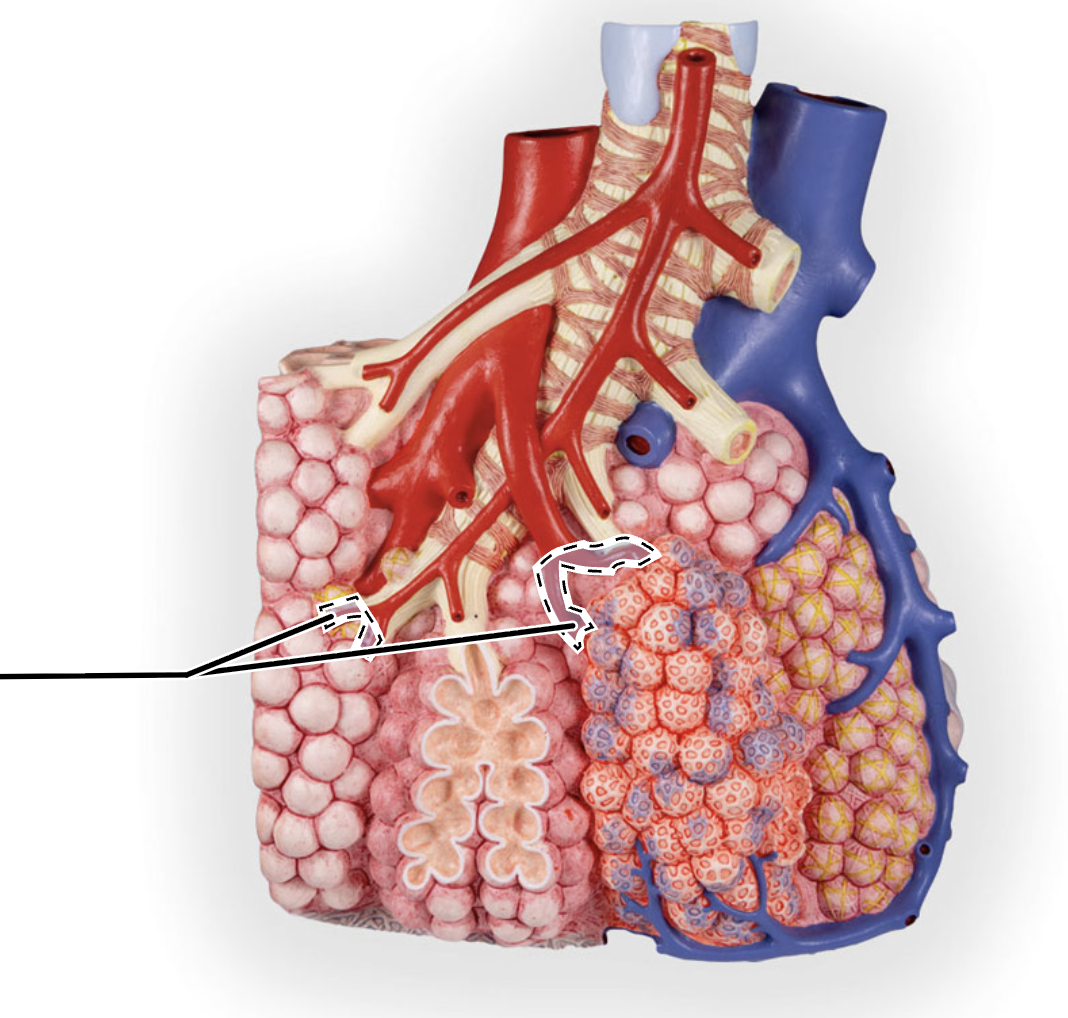
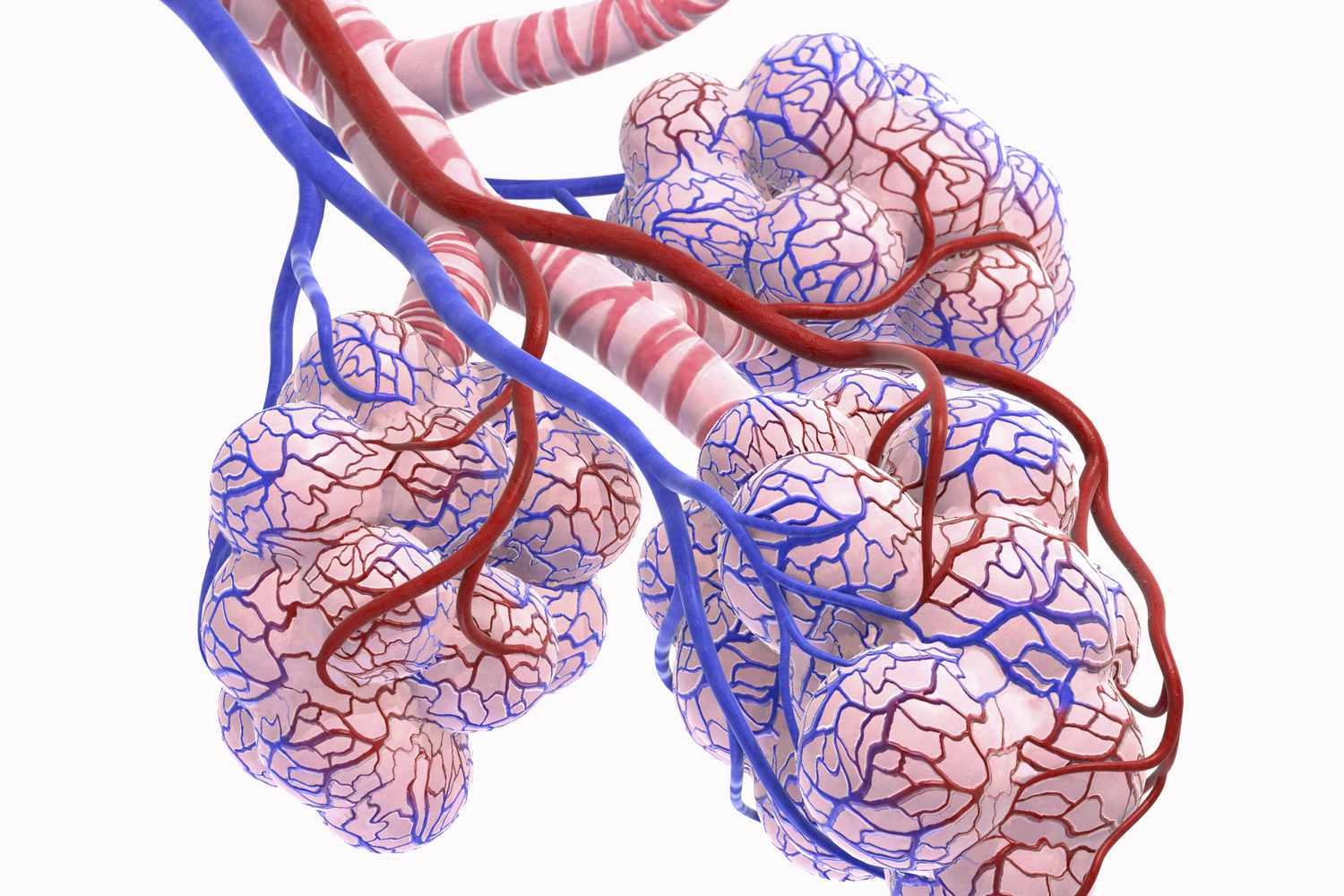
capillary network (lung)
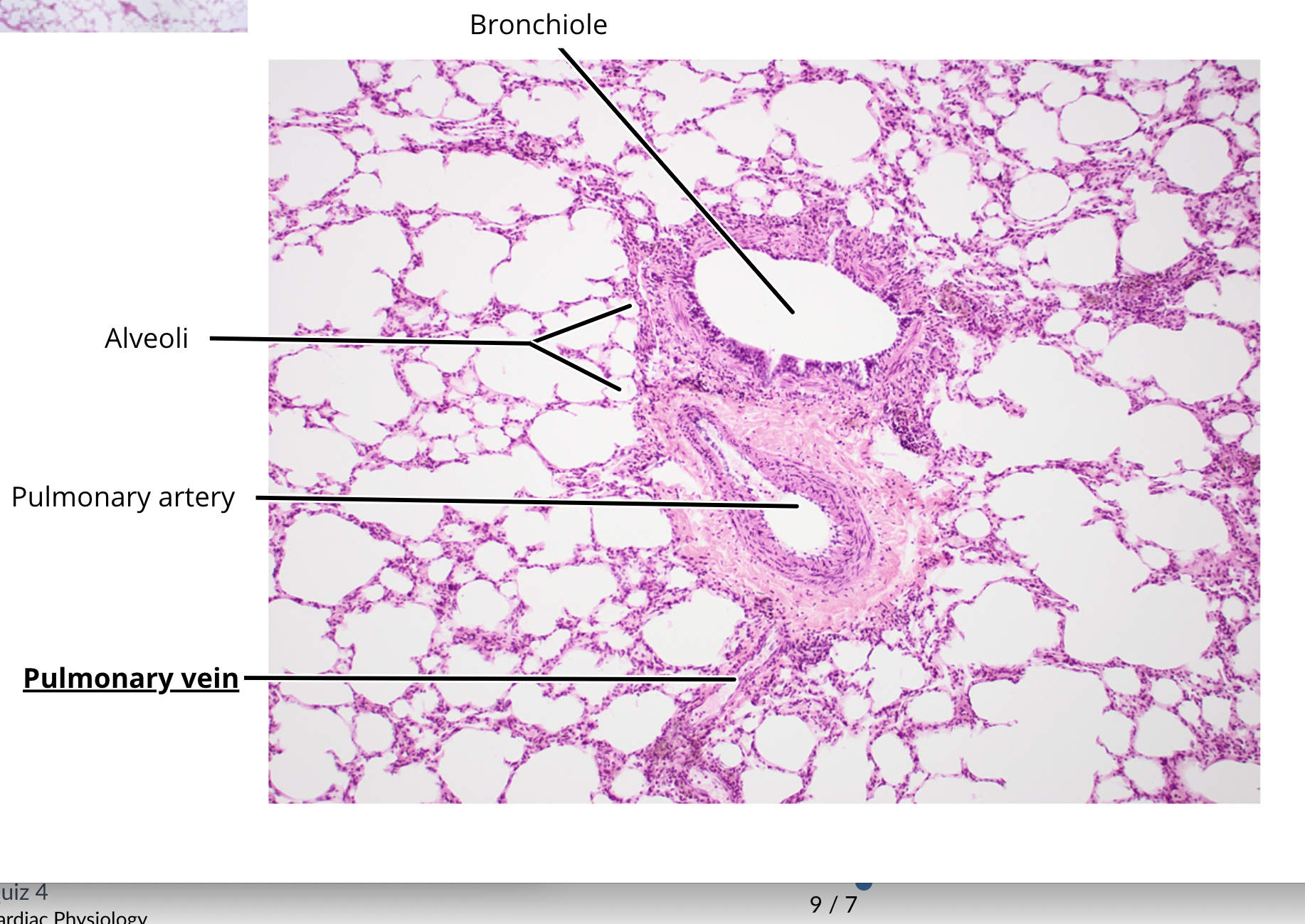
lung histology
bronchi
bronchiole
alveoli
esophagus
muscular tube extending from the pharynx to the stomach
lined with stratified squamous epithelium
muscularis of superior third is skeletal, middle third is both skeletal and smooth, and inferior third is smooth muscle
functions in propulsion with limited secretion
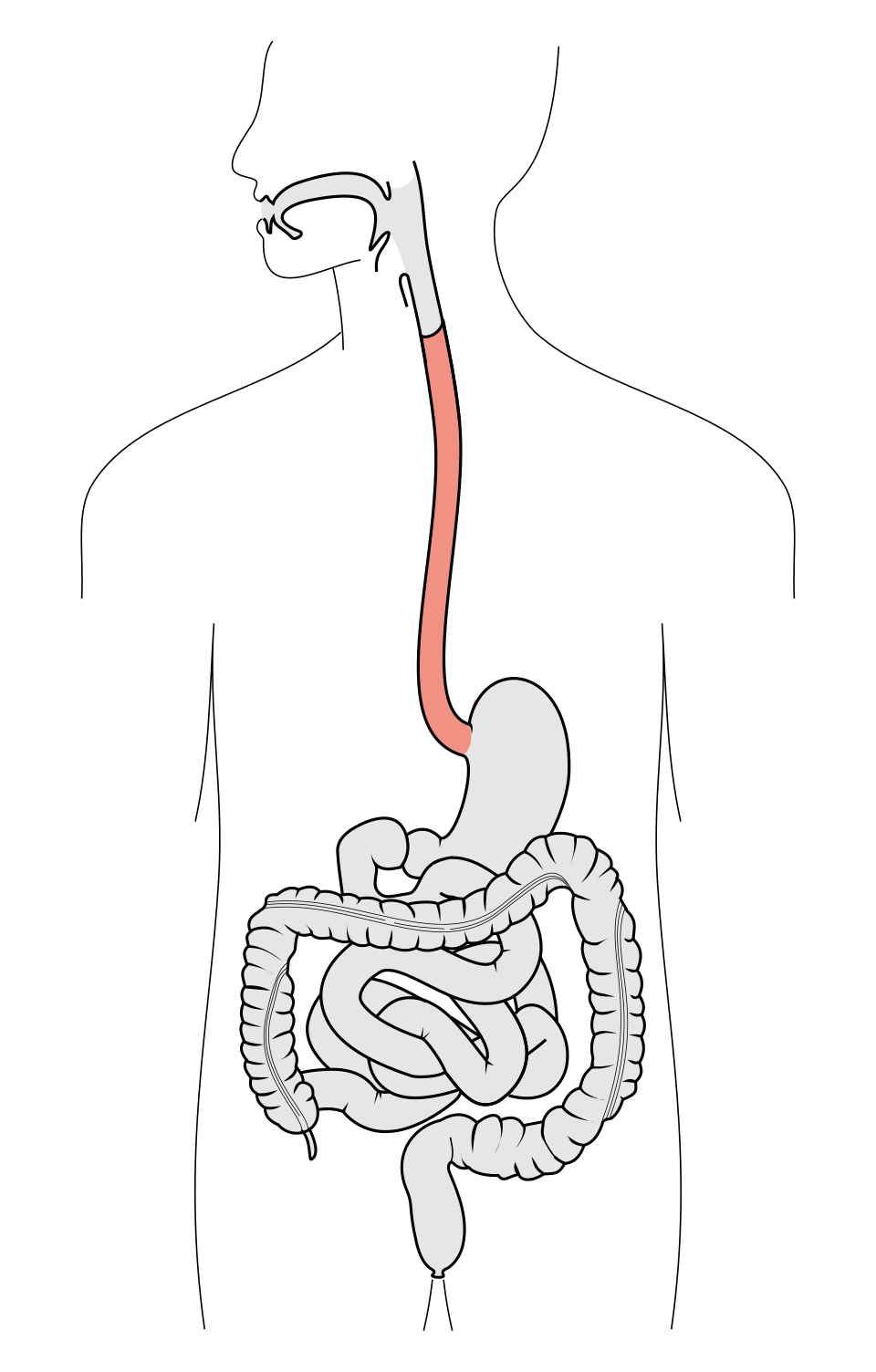
stomach
J-shaped muscular organ extending from the esophagus to the duodenum
lined with simple columnar epithelium
the mucosa is folded into rugae and contains gastric pits
muscularis contains a third layer of oblique smooth muscle
functions in propulsion, chemical digestion, mechanical digestion, and secretion with limited absorption
cardiac region stomach
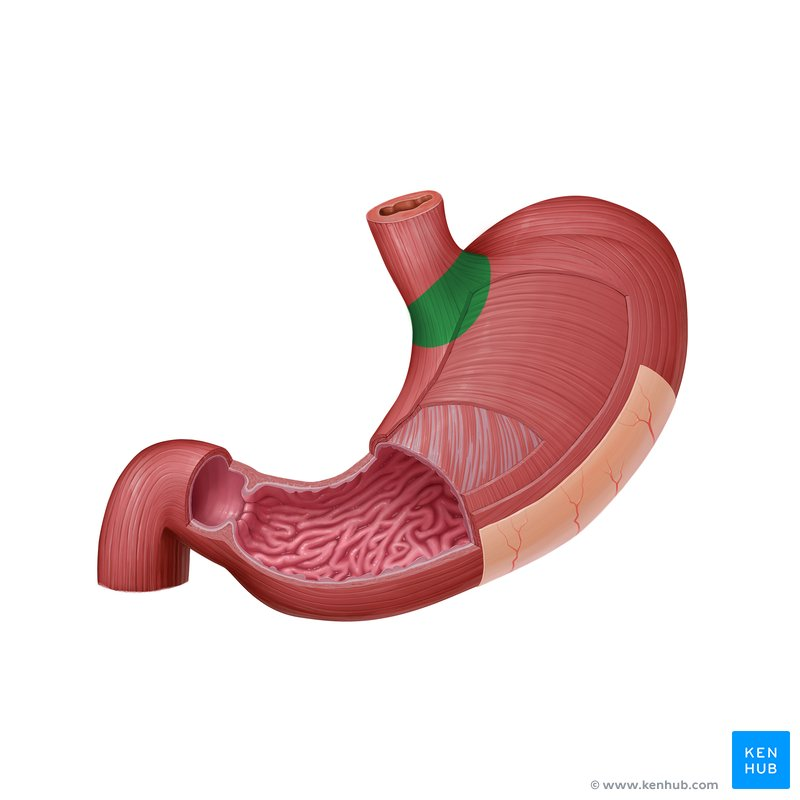
fundic region stomach
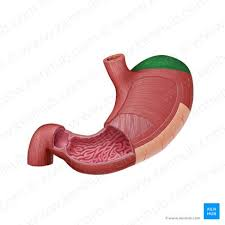
body region stomach
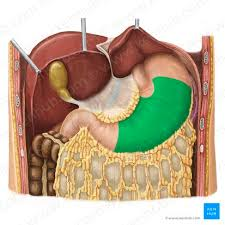
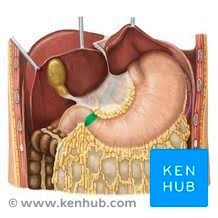
pyloric region
greater curvature stomach
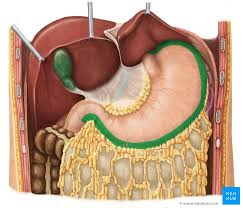
lesser curvature stomach
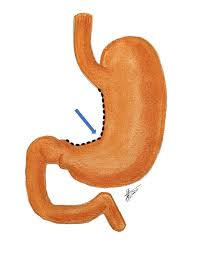
stomach rugae
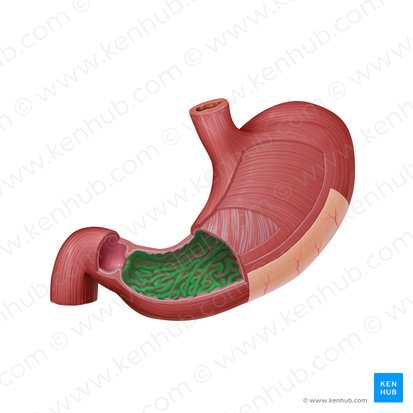
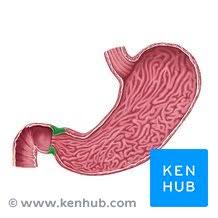
pyloric sphincter
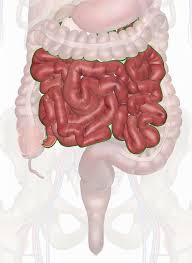
small intestine
long tube extending from the stomach to the large intestine
lined with simple columnar epithelium
wall arranged into three progressively small structures: circular folds, villi, and microvilli
functions in chemical digestion, mechanical digestion, absorption, secretion, propulsion.
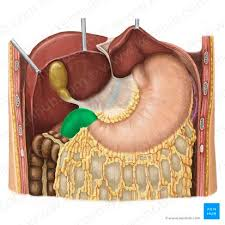
duodenal region
first region of small intestine
jejunal region
middle region of small intestine
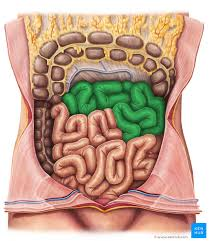
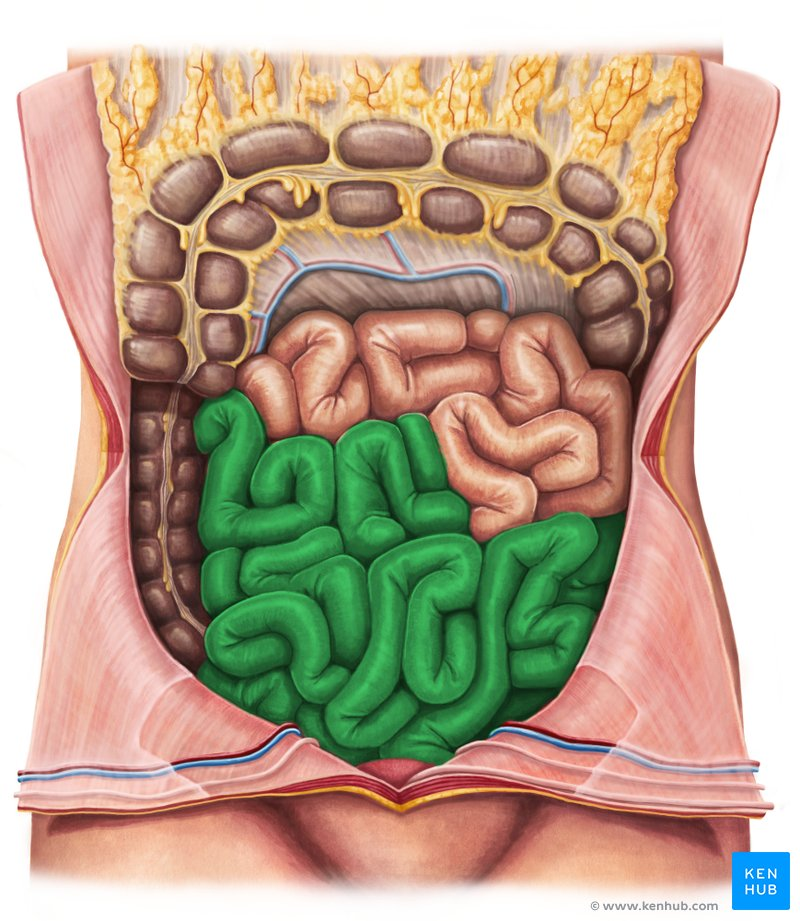
ileal region
final region of small intestine
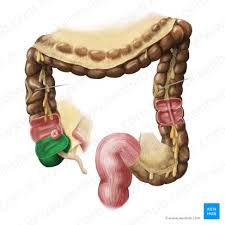
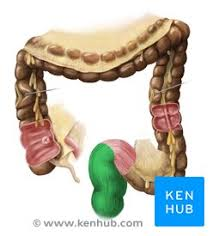
cecum
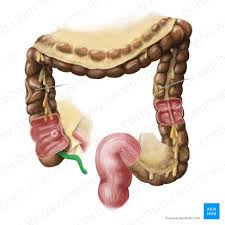
appendix
large intestine
terminal portion of the alimentary canal extending from the small intestine ot the anal canal
lined with simple columnar epithelium
muscularis arranged into ribbon-like taeniae coli
contains a large number of bacterial flora
functions in the absorption of water, electrolytes, and vitamins, propulsion, defecation, and limited secretion.
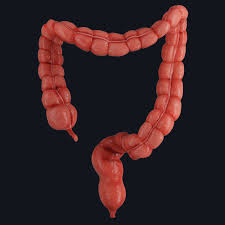
ascending colon
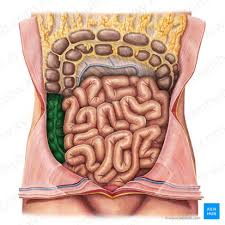
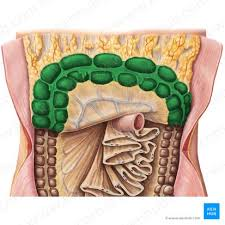
transverse colon
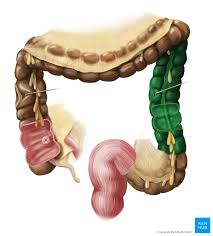
descending colon
liver
consists of hexagonal liver lobules surrounding a central vein
lobules contain plates of hepatocytes
functions in bile production and excretion (excretes waste in bile)
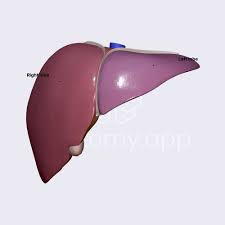
left lobe liver

right lobe liver

quadrate lobe liver

caudate lobe liver

hepatic portal vein
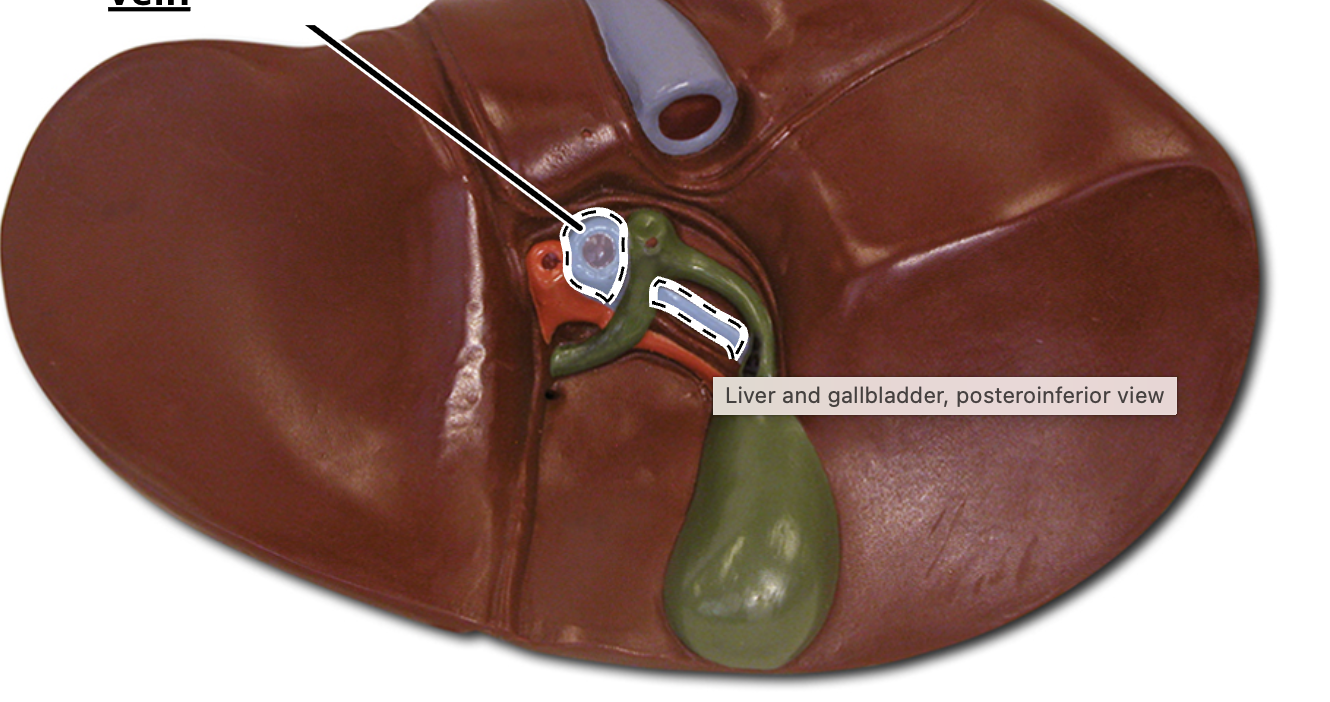
gallbladder
muscular sac on the posteriorinferior liver
stores, concentrates, and releases bile

cystic duct

bile duct
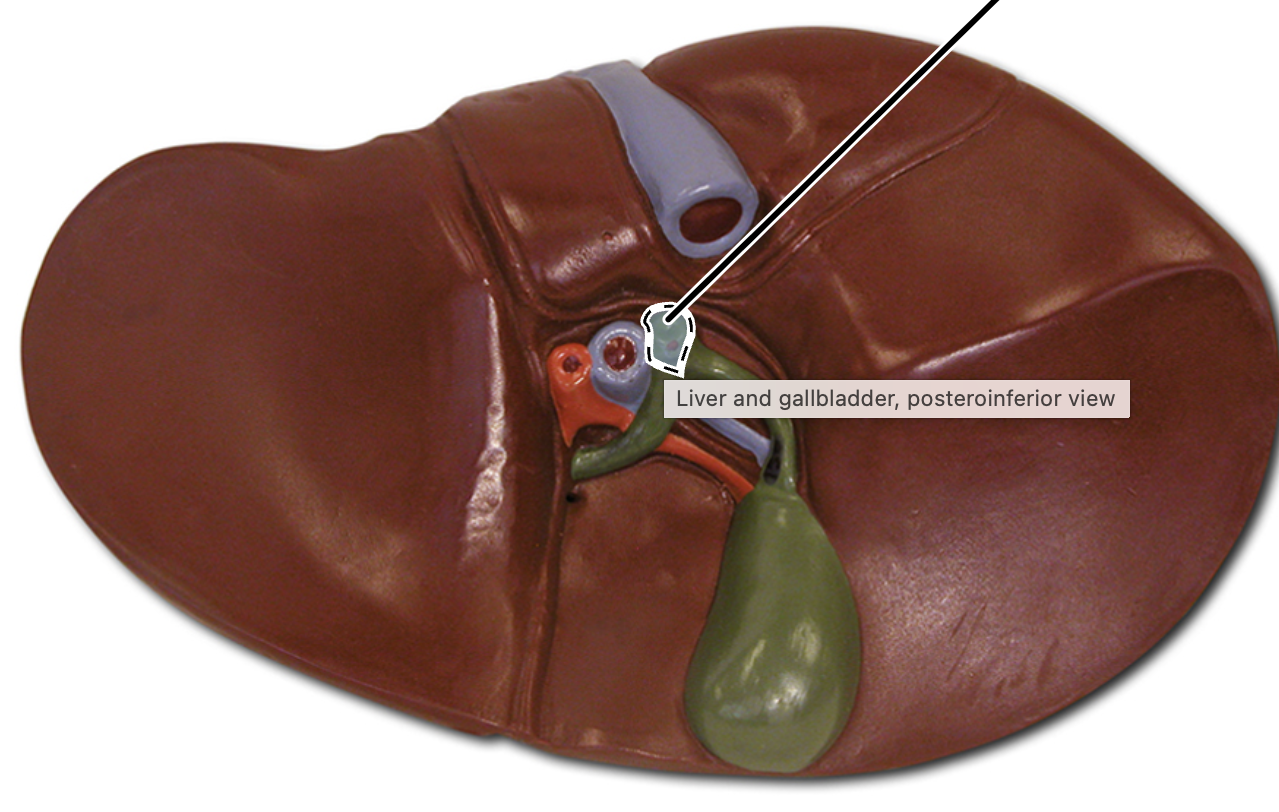
common hepatic duct
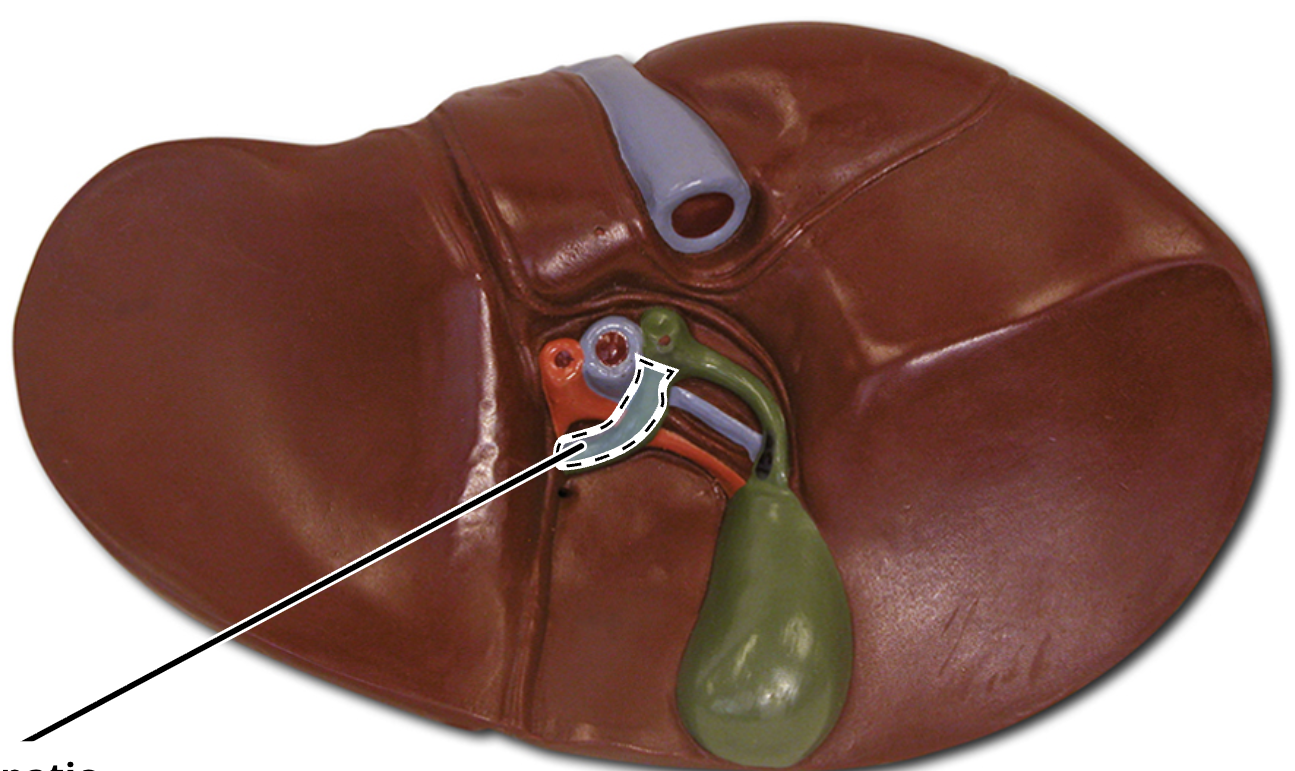
falciform ligament
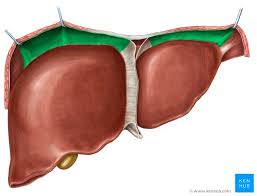
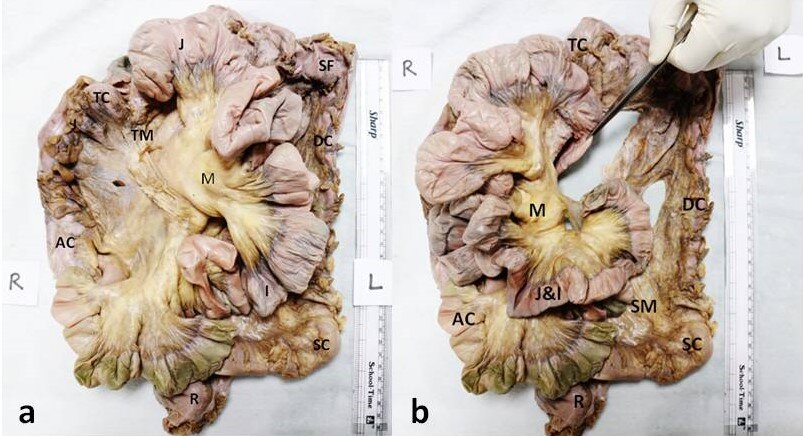
mesentery
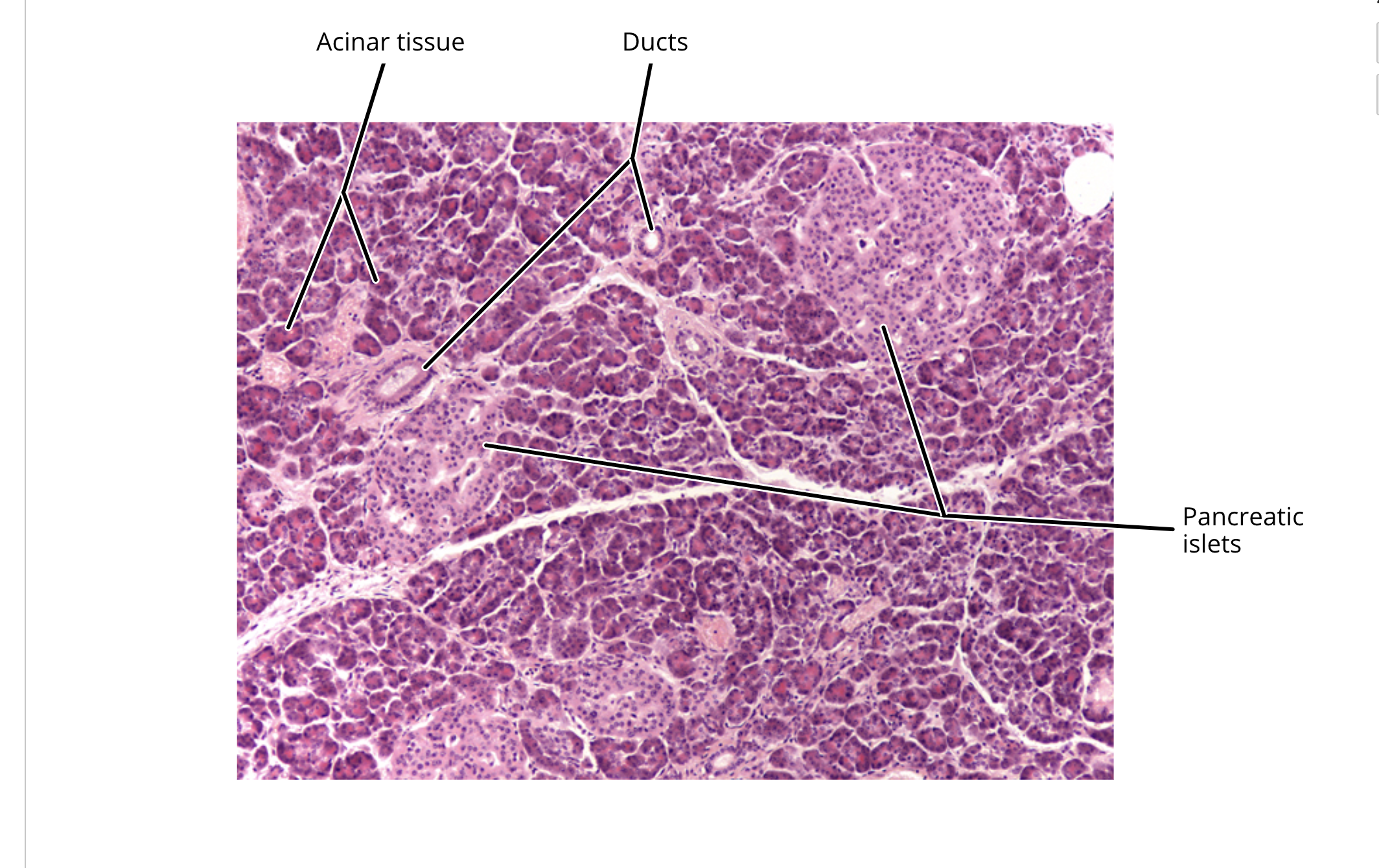
pancreas
consists of pancreatic acini, composed of acinar cells surrounding a duct
functions:
secretes enzymes that catalyze chemical digestion of lipids, carbs, proteins, and nucleic acids
secretes bicarbonate ions to neutralize acidic chyme
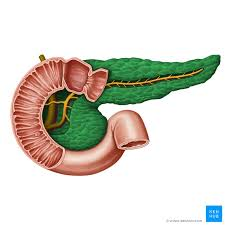
pancreatic duct
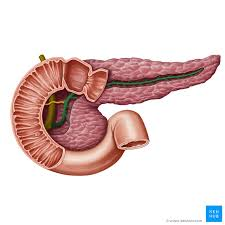
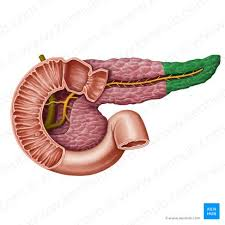
head of pancreas
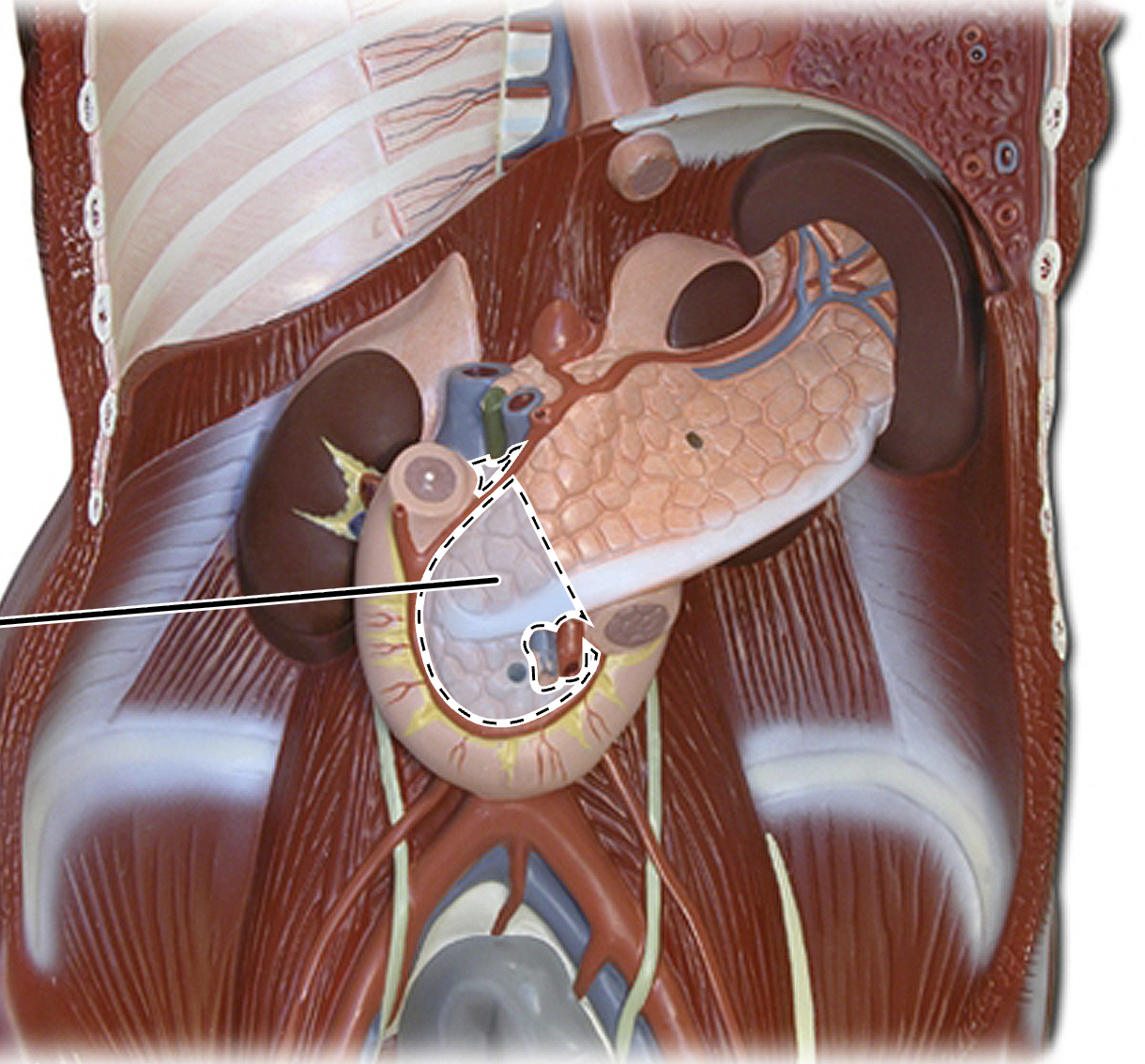
tail of pancreas
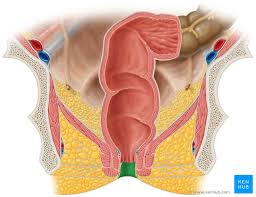
rectum
anus
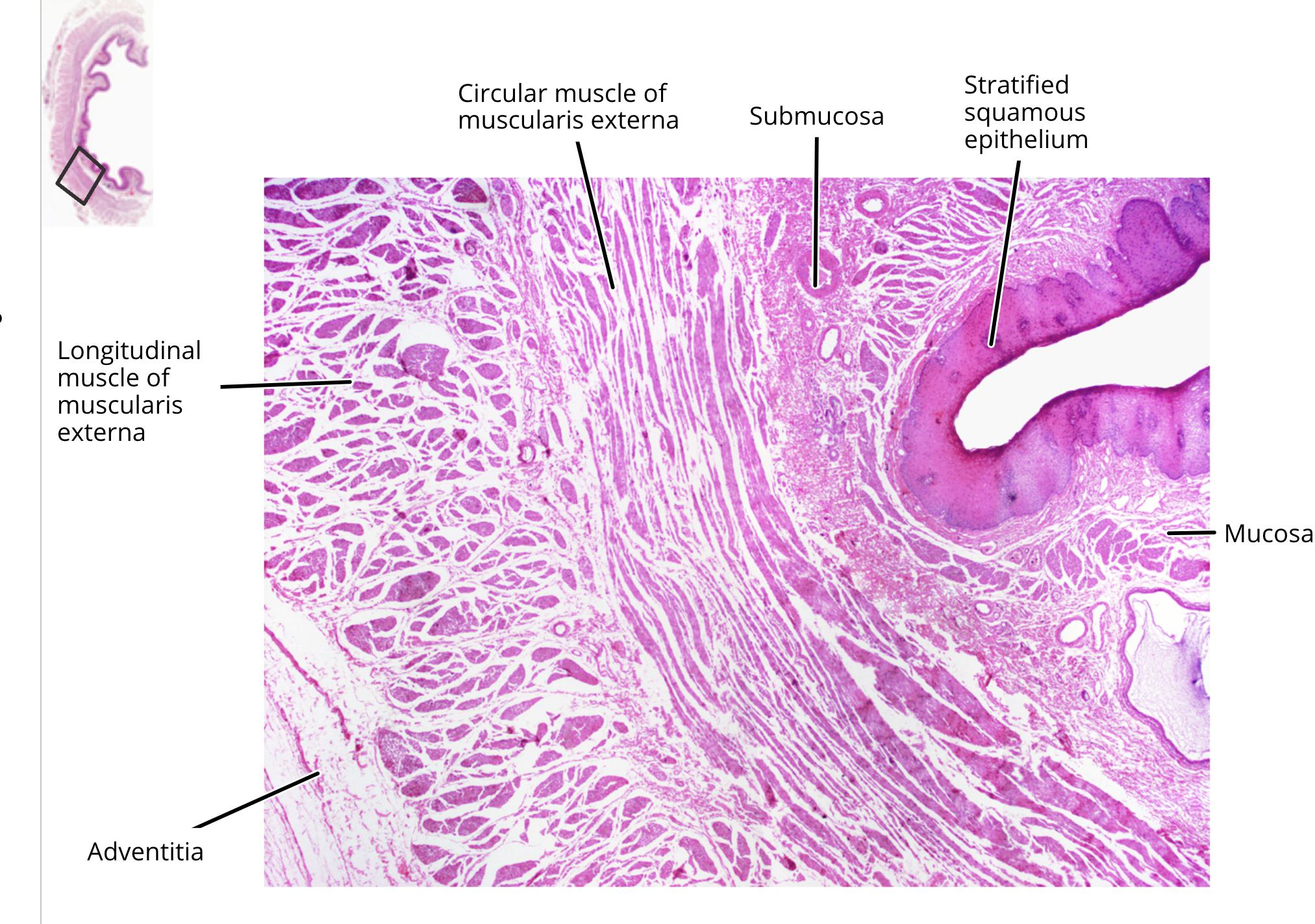
esophagus histology
mucosa
muscularis mucosae
submucosa
muscularis externa
serosa
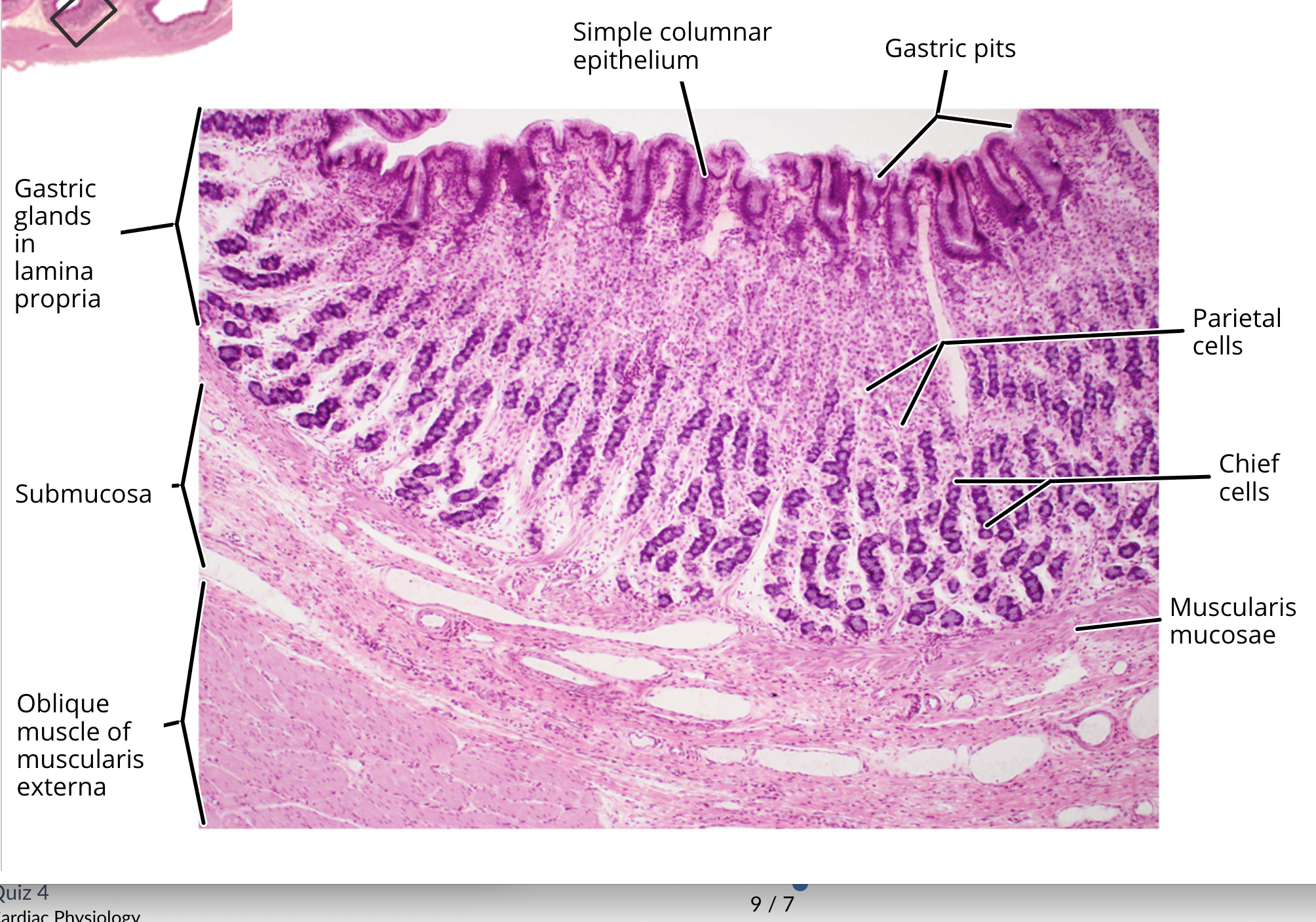
stomach histology
mucosa
muscularis mucosa
submucosa
muscularis externa
serosa
gastric pit
mucous neck cells
parietal cells
chief cells
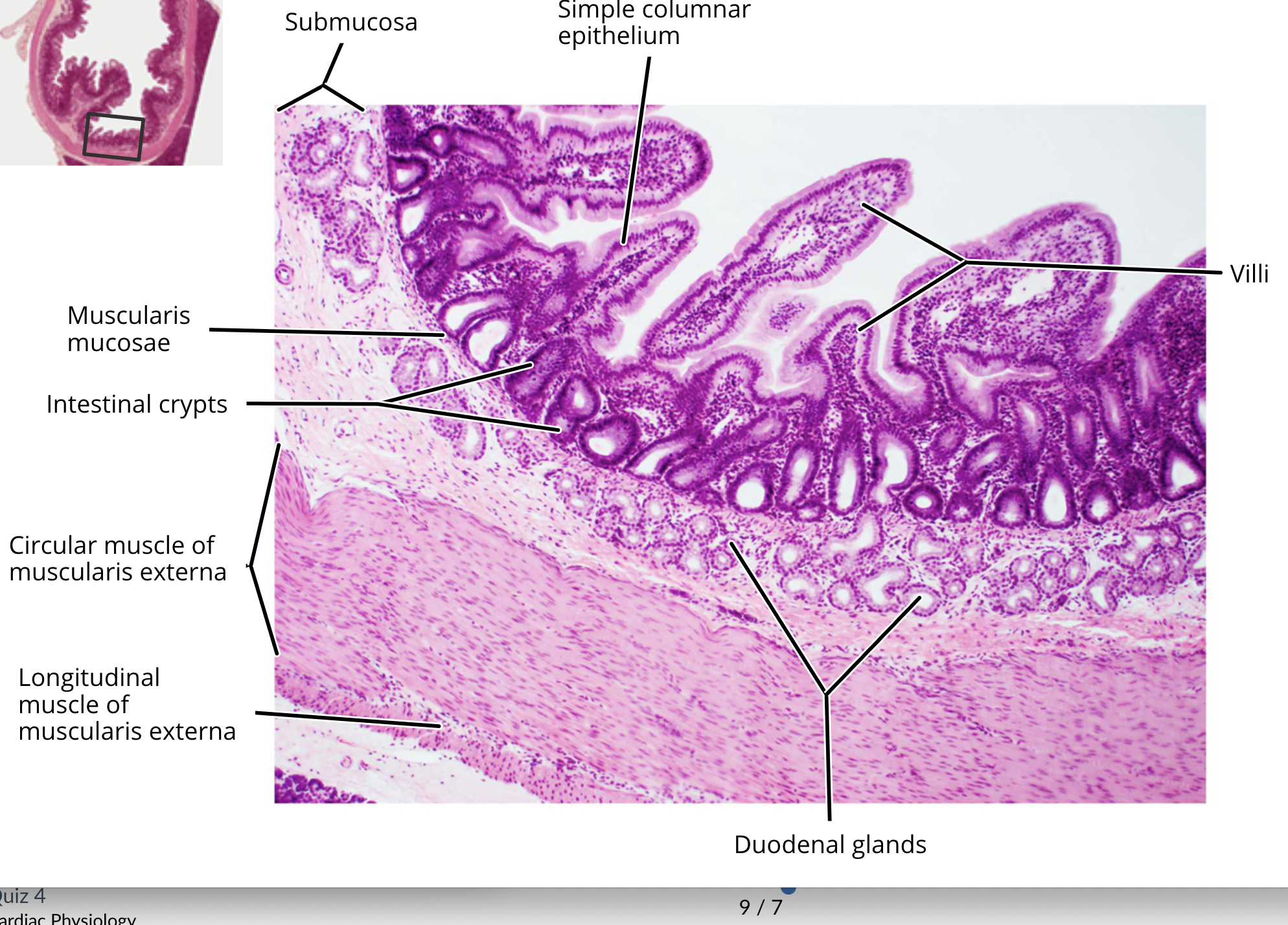
small intestine histology
mucosa
muscularis mucosa
submucosa
muscularis externa
serosa
enteroendocrine cell
enterocyte
paneth cell
goblet cells
duodenal glands
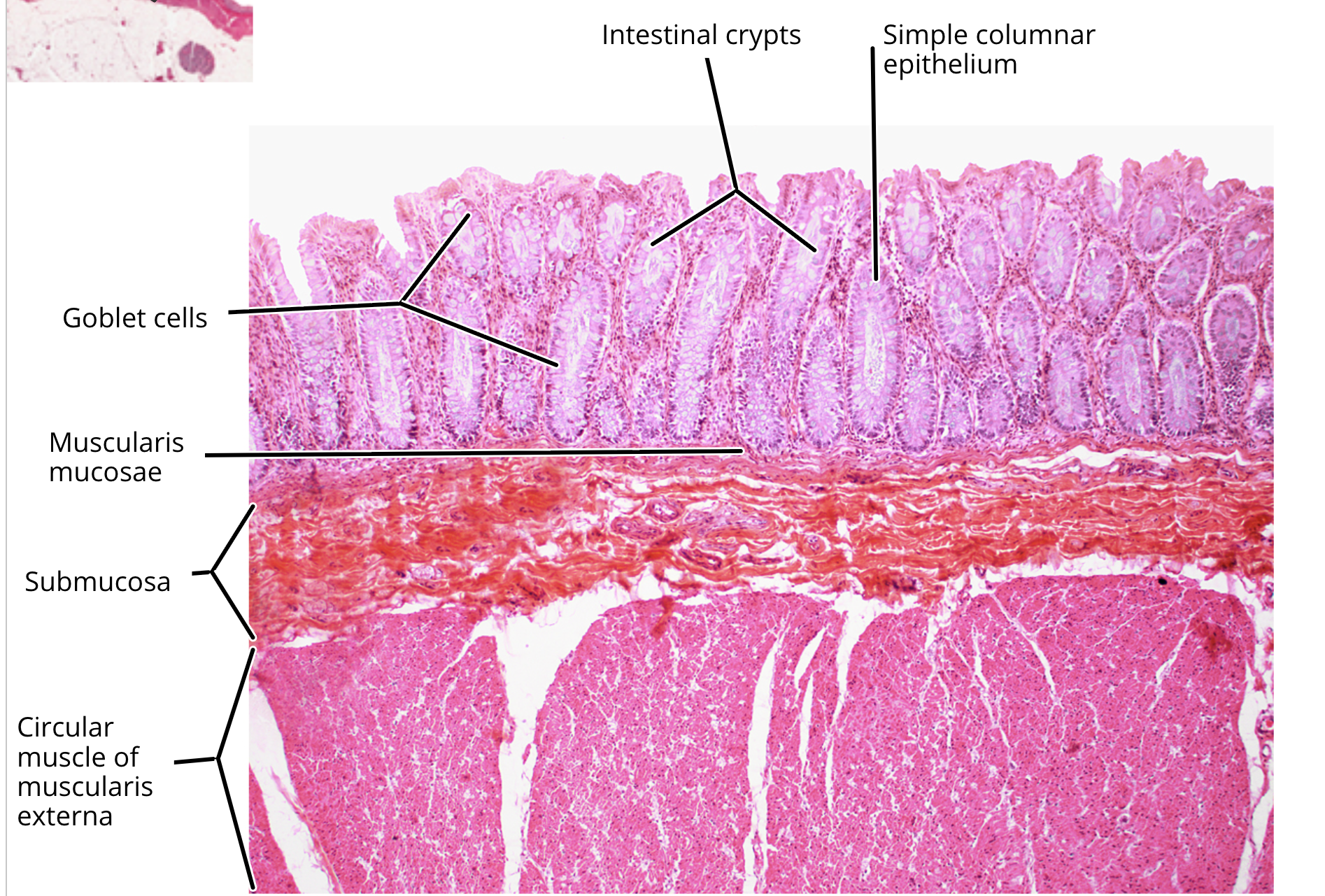
large intestine histology
mucosa
muscularis mucosa
submucosa
muscularis externa
serosa
colonocyte
goblet cell
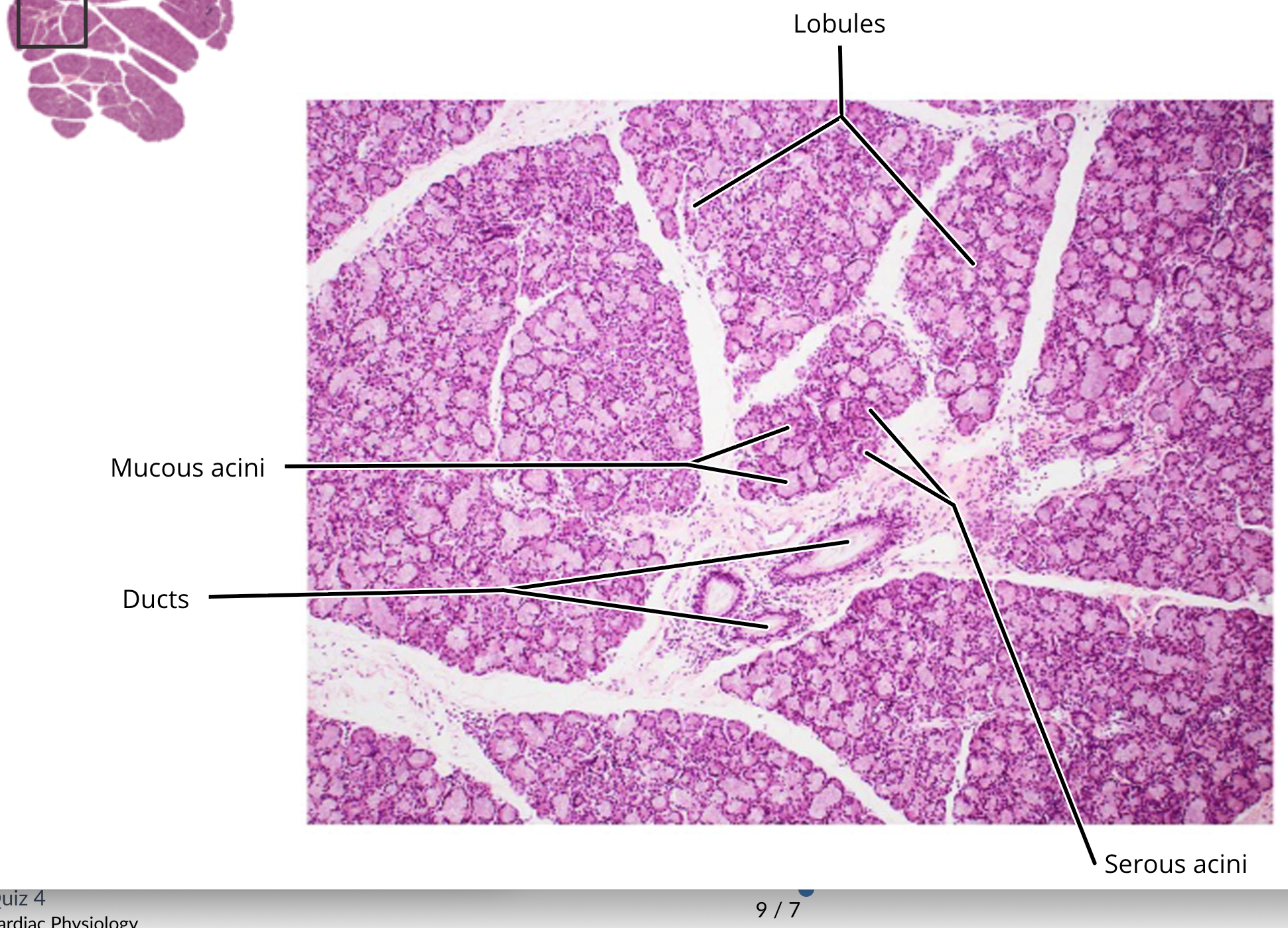
sublingual salivary gland histology
mucous cells
ducts
serous acini cells
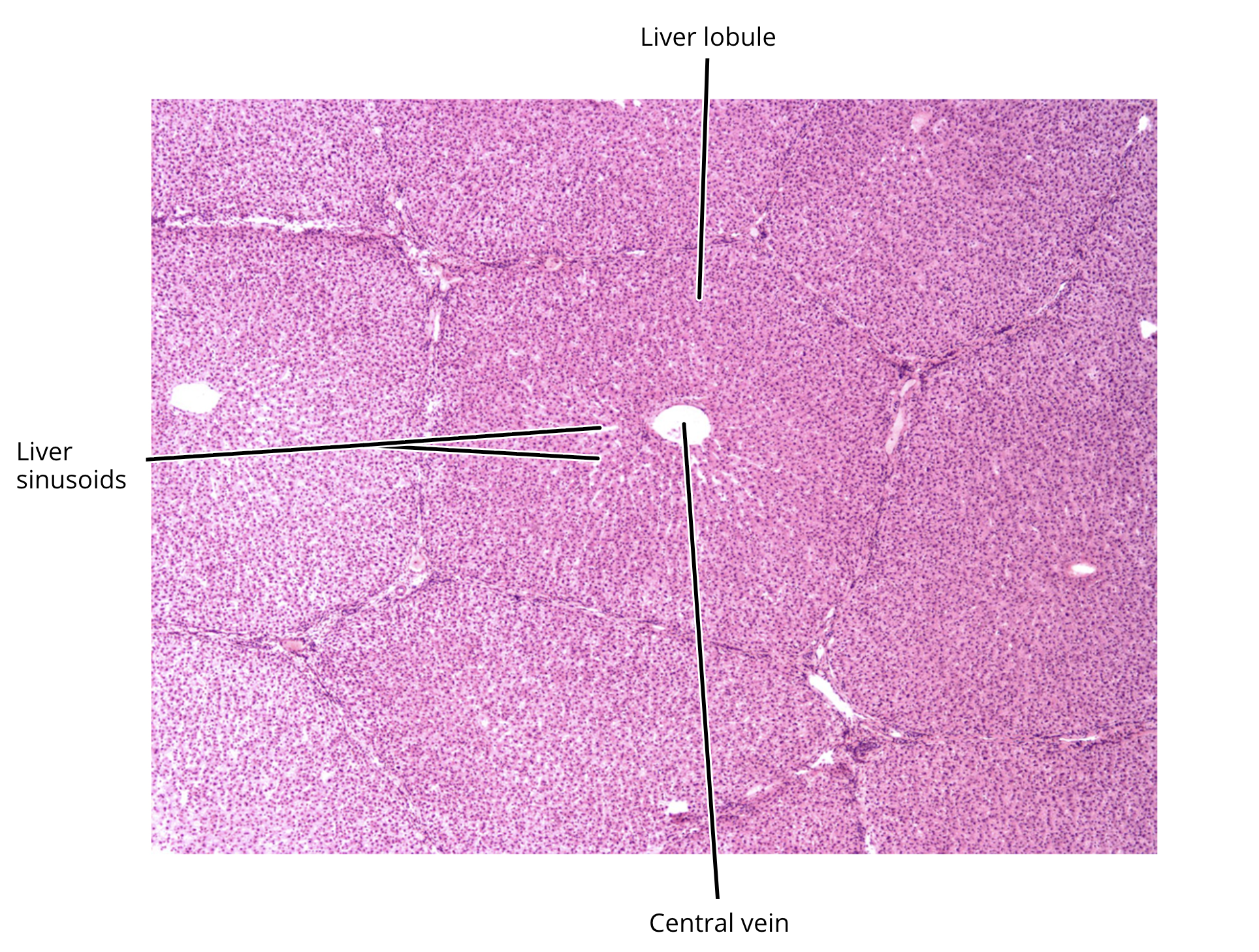
liver histology
lobule
central vein of lobule
pancreas histology
chewing
This process involves the mechanical breakdown of food by the teeth and is controlled by a specific group of muscles and joints
peristalsis
an involuntary, wave-like series of muscle contractions and relaxations that propel substances through tubular organs.
receptive relaxation
a physiological reflex in the stomach where the proximal portion (fundus and body) relaxes to accommodate incoming food without a significant increase in intragastric pressure