IPT 3 - Exam 3 In-Class Questions
1/87
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
88 Terms
Dr. Ali's NAPLEX Questions
Which pathological feature is considered an early and primary driver of neuronal dysfunction in Alzheimer’s disease?
A. Amyloid plaques
B. Neurofibrillary tangles
C. More hydrophobic Aβ42
D. Ventricular enlargement
C. More hydrophobic Aβ42
Which diagnostic modality primarily evaluates brain metabolic activity rather than anatomy in Alzheimer’s disease?
A. CT
B. MRI
C. PET
D. Standard X-ray
C. PET
Which enzyme complex is directly responsible for producing Aβ42 peptides from amyloid precursor protein (APP)?
A. α-secretase
B. β-secretase alone
C. γ-secretase
D. Monoamine oxidase
C. γ-secretase
Which genetic abnormality leads specifically to increased production of Aβ42 peptides?
A. ApoE ε4 polymorphism
B. TREM2 mutation
C. Presenilin-1 mutation
D. APP A673T mutation
C. Presenilin-1 mutation
Which drug is a selective, non-competitive AChE inhibitor with low hepatotoxicity and is used across mild to severe AD?
A. Tacrine
B. Donepezil
C. Galantamine
D. Rivastigmine
B. Donepezil
Which Alzheimer’s drug is described as a pseudo-irreversible AChE inhibitor with a duration of action of ~10 hours?
A. Donepezil
B. Tacrine
C. Galantamine
D. Rivastigmine
D. Rivastigmine
Which drug improves symptoms in moderate-to-severe Alzheimer’s disease by blocking NMDA receptor-mediated excitotoxicity?
A. Donepezil
B. Galantamine
C. Memantine
D. Tacrine
C. Memantine
A 76-year-old patient with moderate Alzheimer’s disease continues to decline cognitively despite AChEI therapy. A medication is added that blocks glutamate induced calcium influx. Which medication was added?
A. Rivastigmine
B. Galantamine
C. Memantine
D. Donepezil
C. Memantine
A patient undergoes CSF analysis during evaluation for early Alzheimer’s disease. Which biomarker pattern is most consistent with AD?
A. ↑ Aβ42, ↓ tau
B. ↓ Aβ42, ↑ phospho-tau
C. ↑ dopamine, ↓ acetylcholine
D. Normal Aβ42, ↑ serotonin
B. ↓ Aβ42, ↑ phospho-tau
Explanation: AD is associated with reduced CSF Aβ42 (due to plaque deposition) and elevated tau/phospho-tau
A patient presents with resting tremor, bradykinesia, and rigidity. Pathology would most likely reveal:
A. Amyloid plaques
B. Neurofibrillary tangles
C. Lewy bodies
D. Prion aggregates
C. Lewy bodies
Why is carbidopa routinely given with levodopa in Parkinson’s therapy?
A. It increases dopamine receptor sensitivity
B. It crosses the BBB to activate dopamine receptors
C. It inhibits peripheral DOPA decarboxylase
D. It blocks MAO-B centrally
C. It inhibits peripheral DOPA decarboxylase
What distinguishes prion diseases from all other infectious diseases?
A. Bacterial origin
B. Requirement for RNA
C. Absence of nucleic acids
D. Immune-mediated toxicity
C. Absence of nucleic acids
Which γ-secretase inhibitor failed in Phase III trials due to worse outcomes than placebo?
A. Gantenerumab
B. Solanezumab
C. Semagacestat
D. Memantine
C. Semagacestat
Which feature allows galantamine to cross the BBB?
A. Quaternary amine
B. Tertiary amine
C. High polarity
D. Large molecular weight
B. Tertiary amine
Parkinson’s disease symptoms primarily result from:
A. Excess dopamine
B. Loss of dopaminergic neurons in substantia nigra
C. Increased acetylcholine activity only
D. Increased serotonin
B. Loss of dopaminergic neurons in substantia nigra
Why is dopamine NOT used directly to treat Parkinson’s disease?
A. Rapid metabolism.
B. Cannot cross BBB.
C. Causes hepatotoxicity.
D. Poor receptor affinity
B. Cannot cross BBB.
Which drug inhibits COMT to increase L DOPA levels?
A. Selegiline
B. Entacapone
C. Bromocriptine
D. Amantadine
B. Entacapone
NOTES:
* Selegiline (MAO-B inhibitor)
* Bromocriptine (Dopamine agonist)
* Amantadine (NMDA antagonist)
Which drug reduces Parkinson’s symptoms by decreasing ACh activity?
A. Benztropine
B. Levodopa
C. Selegiline
D. Amantadine
A. Benztropine
Which prion species is most toxic?
A. Insoluble fibrils
B. Soluble oligomers
C. Monomers
D. Amyloid plaques
B. Soluble oligomers
What was the goal of modifying aminothiazole compounds for prion disease?
A. Increase polarity
B. Reduce molecular weight
C. Improve brain penetration
D. Increase protein binding
C. Improve brain penetration
A patient with moderate Alzheimer’s is not responding adequately to donepezil. Next step?
A. Add memantine
B. Add levodopa
C. Switch to atropine
D. Add benztropine
A. Add memantine
Dr. Thangavel's Kahoot March 31st
Which of the following best described the MOA of donepezil?
a. GABA enhancer
b. NMDA receptor antagonist
c. Dopamine agonist
d. Acetylcholinesterase inhibitor
d. Acetylcholinesterase inhibitor
Alzheimer's diseases is associated with decreased levels of:
a. dopamine
b. serotonin
c. glutamate
d. acetylcholine
d. acetylcholine
Which combination is appropriate for advanced Alzheimer's disease?
a. Levodopa + Carbidopa
b. Donepezil + Memantine
c. Haloperidol + Diazepam
d. Fluoxetine + Lithium
b. Donepezil + Memantine
Which gene mutation is most strongly associated with early-onset familial Alzheimer's disease?
a. APP
b. BRCA1
c. APOE4
c. HTT
a. APP
The APP gene is located on which chromosome?
a. Chromosome 14
b. Chromosome 21
c. Chromosome 1
d. Chromosome 19
b. Chromosome 21
Mutation in PSEN1 is found on which chromosome?
a. Chromosome 14
b. Chromosome 21
c. Chromosome 1
d. Chromosome 19
a. Chromosome 14
Which allele increases the risk of late-onset Alzheimer's disease?
a. APOE3
b. APOE2
c. APOE4
d. APOE1
c. APOE4
Which of the following is a hallmark pathological feature of Alzheimer's disease?
a. Lewy bodies
b. Beta-amyloid plaques
c. demyelination
d. neutrophil infiltration
b. Beta-amyloid plaques
Neurofibrillary tangles in Alzheimer's disease are primarily composed of:
a. Actin filaments
b. Tau protein
c. Alpha-synuclein
d. Collagen
b. Tau protein
Which of the following is a characteristic of Pick's disease?
a. beta-amyloid plaques
b. demyelination
c. Lewy bodies
d. misfolded prion protein
d. misfolded prion protein
Which protein is characteristically aggregated in Pick's disease?
a. beta-amyloid
b. TDP-43
c. Tau protein
d. Alpha-synuclein
c. Tau protein
Which brain regions are primarily affected in Pick's disease, in contrast to Alzheimer's disease?
a. Substantia nigra
b. Occipital lobes
c. Hippocampus and parietal lobes
d. Frontal and temporal lobes
d. Frontal and temporal lobes
Parkinson's disease primarily results from degeneration of:
a. Substantia nigra pars compacta dopaminergic neurons
b. Cortical pyramidal neurons
c. Caudate nucleus
d. Globus pallidus internus
a. Substantia nigra pars compacta dopaminergic neurons
Which of the following is a classic triad of Parkinson's disease?
a. memory loss, tremor, rigidity
b. bradykinesia, tremor, dementia
c. tremor, rigidity, bradykinesia
d. chorea, rigidity, bradykinesia
c. tremor, rigidity, bradykinesia
Which histopatholgoic finding is classic for Parkinson's disease?
a. neurofibrillary tangles (tau)
b. Lewy bodies (α-synuclein)
c. beta-amyloid plaques
d. Pick bodies
b. Lewy bodies (α-synuclein)
Which neurotransmitter is primarily deficient in Parkinson's Disease?
a. Acetylcholine
b. Serotonin
c. GABA
d. Dopamine
d. Dopamine
The most effective treatment to improve motor symptoms in Parkinson's disease is:
a. Levodopa/carbidopa
b. Haloperidol
c. Tetrabenazine
d. Donepezil
a. Levodopa/carbidopa
Loss of dopaminergic neurons in Parkinson's Disease leads to:
a. Enhanced thalamic stimulation -> tremor
b. Overactivation of the indirect pathway -> hypokinesia
c. Overactivation of the direct pathway -> hyperkinesia
d. Loss of indirect pathway -> chorea
b. Overactivation of the indirect pathway -> hypokinesia
In idiopathic Parkinson's disease, the primary pathology involves:
a. Degeneration of substantia nigra with Lewy bodies
b. Pick bodies in frontal/temporal lobes
c. Beta-amyloid plaques in cortex
d. Corticospinal tract demyelination
a. Degeneration of substantia nigra with Lewy bodies
A patient develops Parkinsonian symptoms after starting an antipsychotic. This is classified as:
a. idiopathic Parkson's disease
b. progressive supranuclear palsy
c. Secondary Parkinsonism (drug-induced)
d. Huntington's disease
c. Secondary Parkinsonism (drug-induced)
Which trinucleotide repeat expansion is responsible for Huntington's disease?
a. GAG
b. GAA
c. CGG
d. CAG
d. CAG
CAG repeat expansion results in accumulation of which amino acid?
a. Glutamine
b. Alanine
c. Glycine
d. Glutamic acid
a. Glutamine
What is the primary role of HAP1?
a. DNA replication
b. Intracellular transport and neuronal survival
c. Neurotransmitter synthesis
d. Ion channel regulation
b. Intracellular transport and neuronal survival
Which of the following drugs is commonly used to treat chorea in Huntington's disease?
a. Levodopa
b. Haloperidol
c. Tetrabenazine
d. Donepezil
c. Tetrabenazine
Which neurons are primarily lost first in Huntington's disease?
a. Direct pathway (D1) striatal neurons
b. Dopaminergic neurons in substantia nigra
c. Cortical pyramidal neurons
d. Indirect pathway (D2) striatal neurons
d. Indirect pathway (D2) striatal neurons
What type of protein accumulates in neurons due to CAG repeat expansion in the HTT gene?
a. Tau protein
b. Beta amyloid
c. Polyglutamine (polyQ) huntingtin protein
d. Alpha-synuclein
c. Polyglutamine (polyQ) huntingtin protein
The earliest histopathologic change in the basal ganglia of a patient with Huntington's disease is:
a. Amyloid plaques in cortex
b. Demyelination of corticospinal tracts
c. Neuronal loss in the striatum (caudate/putamen)
d. Lewy body formation in substantia nigra
c. Neuronal loss in the striatum (caudate/putamen)
Which neurotransmitter is decreased early in Huntington's disease due to striatal degeneration?
a. Acetylcholine
b. GABA
c. Dopamine
d. Glutamate
b. GABA
Which basal ganglia pathway is disrupted first in Huntington's disease, leading to chorea?
a. Nigrostriatal pathway
b. Corticospinal pathway
c. Direct (D1) pathway
d. Indirect (D2) pathway
d. Indirect (D2) pathway
Dr. Thangavel's Kahoot April 1st
Mutations in the SOD1 gene primarily cause which form of ALS?
a. familial ALS
b. bulbar ALS
c. sporadic ALS
d. secondary ALS
a. familial ALS
ALS primarily affects which type of neurons?
a. Lower motor neurons only
b. Both upper and lower motor neurons
c. Upper motor neurons only
d. Sensory neurons
b. Both upper and lower motor neurons
Which drug is FDA approved to slow disease progression in ALS?
a. tetrabenazine
b. riluzole
c. donepezil
d. levodopa
b. riluzole
which neurotransmitter is primarily responsible for excitotoxic motor neuron death in ALS?
a. acetylcholine
b. GABA
c. dopamine
d. glutamate
d. glutamate
which strategy targets SOD1 toxicity and mitochondrial iron-induced oxidative stress?
a. beta blockers
b. iron chelators and antioxidant therapy
c. cholinesterase inhibitors
d. dopamine agonists
b. iron chelators and antioxidant therapy
how do mutant SOD1 proteins contribute to neuronal damage?
a. increase acetylcholine synthesis
b. reduce glutamate release
c. promote myelination
d. cause oxidative stress and mitochondrial dysfunction
d. cause oxidative stress and mitochondrial dysfunction
Excess mitochondrial iron in motor neurons leads to:
a. increased ATP production
b. generation of reactive oxygen species (ROS)
c. enhanced axonal transport
d. reduced excitotoxicity
b. generation of reactive oxygen species (ROS)
What statement best describes the connection between mutant SOD1 and mitochondrial iron in ALS?
a. mutant SOD1 reduces mitochondrial iron levels
b. no relationship exists
c. mutant SOD1 enhances mitochondrial iron export
d. mutant SOD1 aggregates in mitochondria
d. mutant SOD1 aggregates in mitochondria
Which statement correctly differentiates PLS from PMA?
a. PLS affects upper motor neurons only
b. PLS is sensory, PMA is motor
c. PLS affects lower motor neurons only
d. Both affect upper and lower motor neurons
a. PLS affects upper motor neurons only
Which gene is mutated in Friedreich Ataxia?
a. FXN
b. APP
c. HTT
d. SOD1
a. FXN (frataxin)
What is the function of the frataxin protein?
a. dopamine synthesis
b. mitochondrial iron-sulfur cluster assembly
c. cytoskeletal support
d. myelin formation
b. mitochondrial iron-sulfur cluster assembly
Which of the following best describes the pathophysiologic consequence of frataxin deficiency?
a. increased acetylcholine at NM3
b. mitochondrial iron accumulation
c. excess dopamine in basal ganglia
d. beta-amyloid deposition
b. mitochondrial iron accumulation
Which of the following is a therapeutic approach in Friedreich Ataxia?
a. Idebenone and supportive therapy
b. Levodopa
c. Tetrabenazine
c. Riluzole
a. Idebenone and supportive therapy
Friedreich Ataxia is caused by GAA trinucleotide repeat expansion number in the FXN gene consider the positive of Ataxia?
a. 5-20 repeats
b. 2000-5000 repeats
c. 30-70 repeats
d. 66-1700 repeats
d. 66-1700 repeats
Which protein is deficient in DMD?
a. Frataxin
b. Lamin A/C
c. Utrophin
d. Dystrophin
d. Dystrophin
Deficiency of dystrophin in DMD leads to:
a. Demyelination
b. Mitochondrial iron accumulation
c. Excitotoxic neuronal death
d. Sarcolemma instability
d. Sarcolemma instability
At what age to most boys with DMD lose ambulation?
a. 18-20 years
b. 2-3 years
c. 10-12 years
d. 5-7 years
c. 10-12 years
Which treatment is used to slow disease progression in DMD?
a. Levodopa
b. Corticosteroids
c. Riluzole
d. Idebenone
b. Corticosteroids
Most BMD patients remain ambulatory until:
a. 10-12 years
b. 30s-40s
c. 15-20 years
d. 5-7 years
b. 30s-40s
Which complication is common in BMD?
a. pulmonary fibrosis
b. arrhythmogenic right ventricular cardiomyopathy
c. aortic stenosis
d. dilated cardiomyopathy
d. dilated cardiomyopathy
Which gene is mutated in Alexander disease?
a. DMD
b. GFAP
c. LMNA
d. FXN
b. GFAP (glial fibrillary acidic protein)
Alexander disease is caused by:
a. astrocyte dysfunction
b. demyelination of motor neurons
c. neuronal iron accumulation
d. amyloid deposition
a. astrocyte dysfunction
Which is a hallmark feature of infantile Alexander disease?
a. Cardiac failure
b. Macrocephaly
c. Ataxia only
d. Hypertonia only
b. Macrocephaly
Dr. Pho's Poll EVs
All are important non-drug measures to keep the brain healthy EXCEPT:
a. discontinue drugs that can worsen dementia if possible
b. exercise
c. eat a healthy diet
d. control blood glucose, blood pressure, and cholesterol
e. engage in activities that stimulates the brain
f. be ambitious and sleep less to get more done
f. be ambitious and sleep less to get more done
All of the following can worsen dementia EXCEPT:
a. phenobarbital
b. clonazepam
c. diphenhydramine
d. oxybutynin
e. metformin
e. metformin
All of the following medications INCREASE acetylcholine and is used to treat Alzheimer EXCEPT?
a. donepezil
b. aricept
c. adlarity
d. rivastigmine
e. memantine
e. memantine
BN is a 68 year-old female with Alzheimer dementia. She is taking Aricept 10 mg tabs daily. Her MMSE score last year was 10 and today it is 8 and currently reside with the nursing home medical care team you're rounding with around the clock care.
What will be your best recommendation for BN?
a. increase Aricept to 23 mg daily
b. switch to Adlarity patch
c. switch to Exelon patch
d. add rivastigmine
e. add memantine
e. add memantine
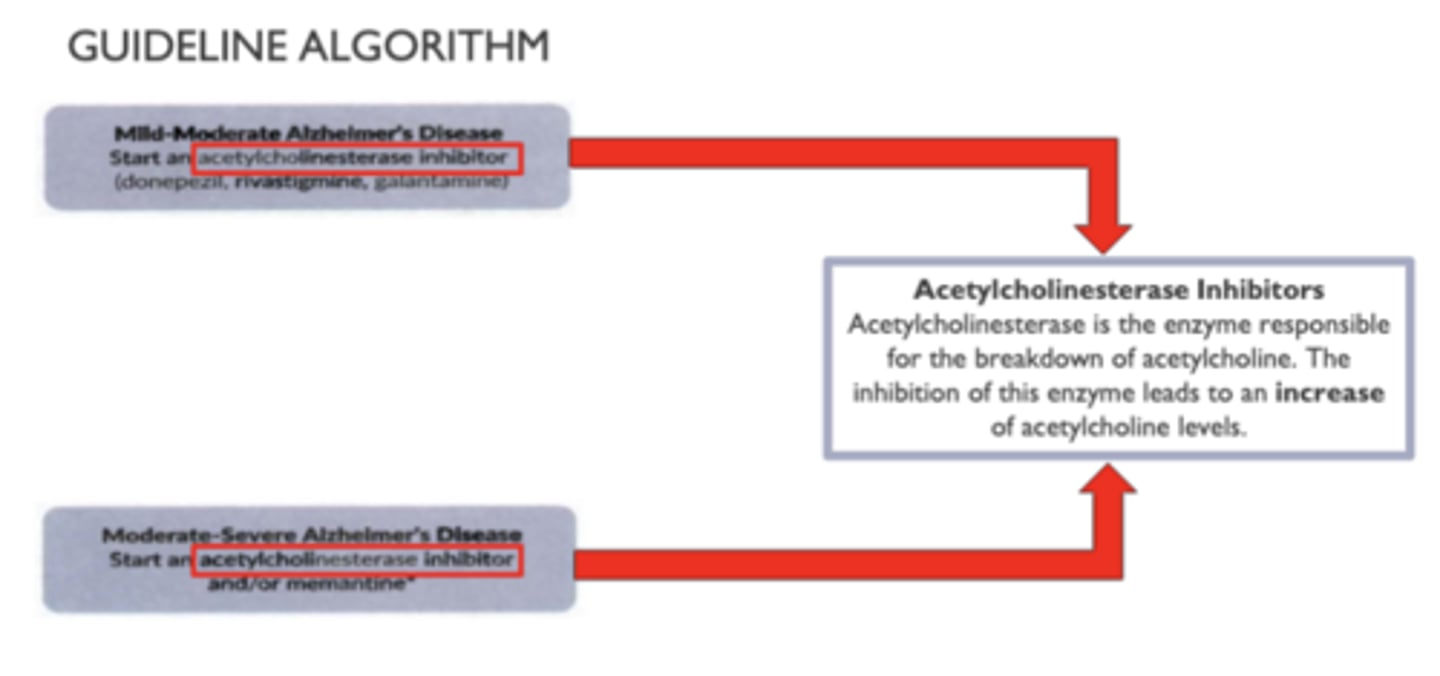
BN is a 68 year-old female with Alzheimer dementia. She is taking Aricept 10 mg tabs daily. Her MMSE score last year was 10 and today it is 8 and currently reside with the nursing home medical care team you're rounding with around the clock care.
What will be your recommended starting dose for BN new med with the IR formulation?
a. 5 mg daily
b. 10 mg daily
c. 7 mg daily
d. 20 mg daily
e. 28 mg daily
a. 5 mg daily
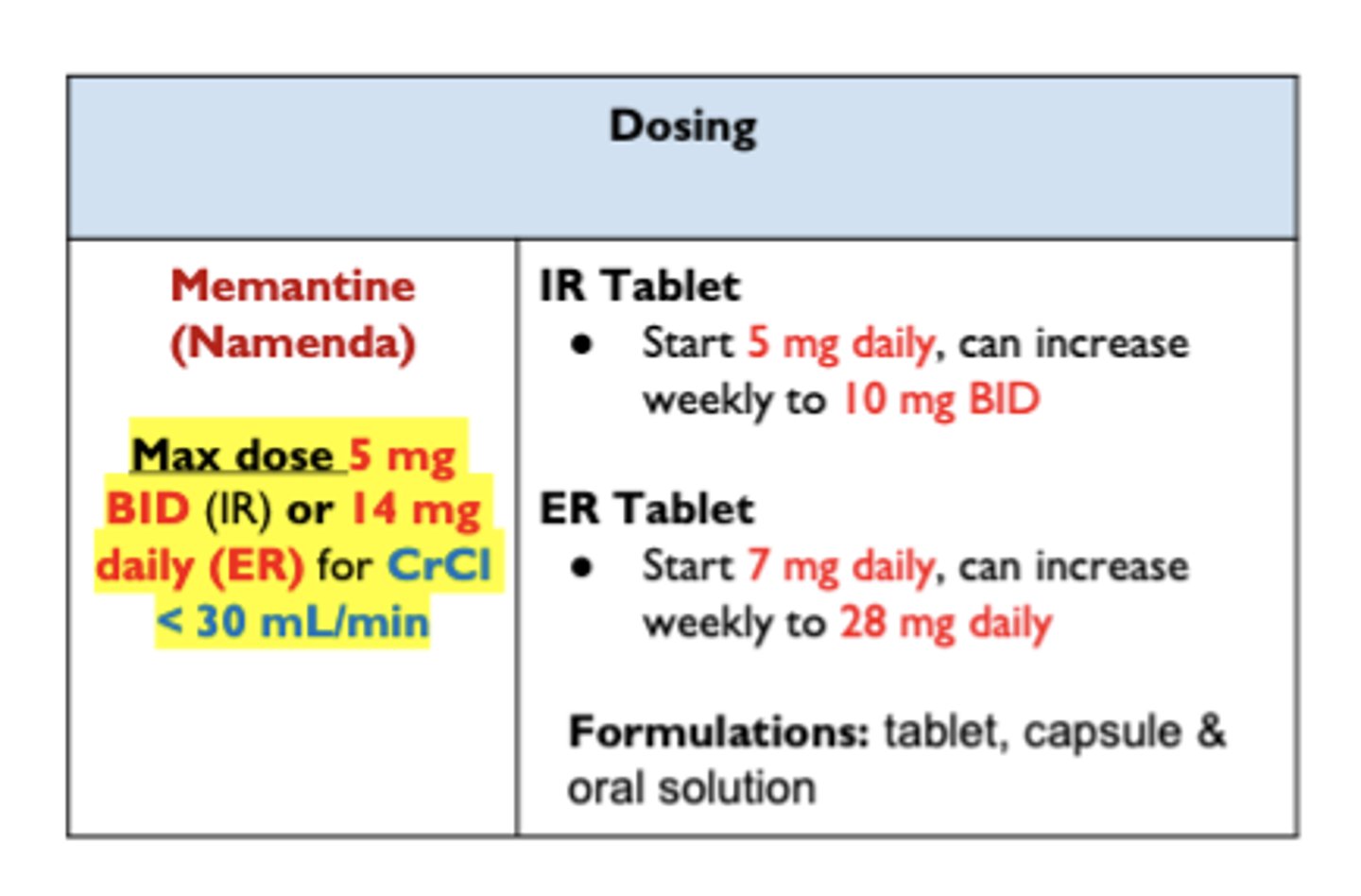
Your patient complained that she can't sleep ever since she started the donepezil. What will be your best recommendation?
a. Increase the dose to 23 mg daily
b. Tell her the side effects will resolve after 3-4 weeks
c. Give patient a benadryl
d. Give patient a hypnotic
e. Switch her donepezil to AM dosing
e. Switch her donepezil to AM dosing
check recordings for any missed poll evs
JD return to the clinic and express concern that his stool and urine have turned dark brown and sometimes black ever since he started his new drug for his Parkinson. Which medication could be the cause for this side effect?
a. Sinemet
b. Comtan
c. Requip
d. Amantadine
e. Selegiline
a. Sinemet
Which of the following is not considered appropriate initial monotherapy for Parkinson's Disease?
a. Dopamine replacement
b. Dopamine receptor agonist
c. MAO-B inhibitors
d. Anticholinergics
e. Sinemet
d. Anticholinergics
Which food interactions reduces levodopa absorption?
a. Citrus fruit
b. High protein meals
c. Low fat dairy
c. Simple carbohydrate
e. Watermelon
b. High protein meals
If you need to start patient on an antipsychotic, what will be your best recommendation that will be PD-friendly?
a. Haloperidol
b. Risperidone
c. Olanzapine
d. Metoclopramide
e. Quetiapine
e. Quetiapine