Chapter 27: Male Reproductive System
1/71
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
72 Terms
What are the functions of the reproductive system (4)
store
nurish
produce
transport
gametes (reproductive cells0
Fertilization is what
the fusion of male and female gametes (sperm and ovum) to for a zygote
Gondas are what
primary sex organs (reproductive organs), testies and ovary
accessory glands and organs to reproductive system are what (3)
ducts
glands
external genitalia
what kind of chromosomes do males have
XY (Y chromosome has SRY gene that codes for it being male), can have Y chromosome present with no SRY gene and have a female presenting child
Failure to make or respond to testosterone and other male hormones during early stages of development results in what
results in development of a person anatomically becoming female (androgen insensitivity)
Failure to make or respond to testosterone after early stages of development results in formation of what
female secondary sexual characteristics like breasts, widen hips, ect.
male gonads produce what (2)
testies produce spermatozoa and male hormones (androgens): testosterone
Write out the pathway of sperm (7)
seminiferous tubules, rete testi, efferent ductiles, epididymis, ductus deferens, ej duct, urethra
what are the accessory glands that add secretions into the ejaculate (3)
seminal vesicles (largest amount)
proastate gland (30%)
buluurethral gland (pre-ejaculate)
external genitalia of male repro. (2)
penis and scrotum
Testes develop where and are attached to what and called what
inside of body near kidneys, attach to posterior wall of the peritoneum, called gubernaculum testes
testies decend throught where and when does this happen
decend through inguinal canal into scrotum during fetal development
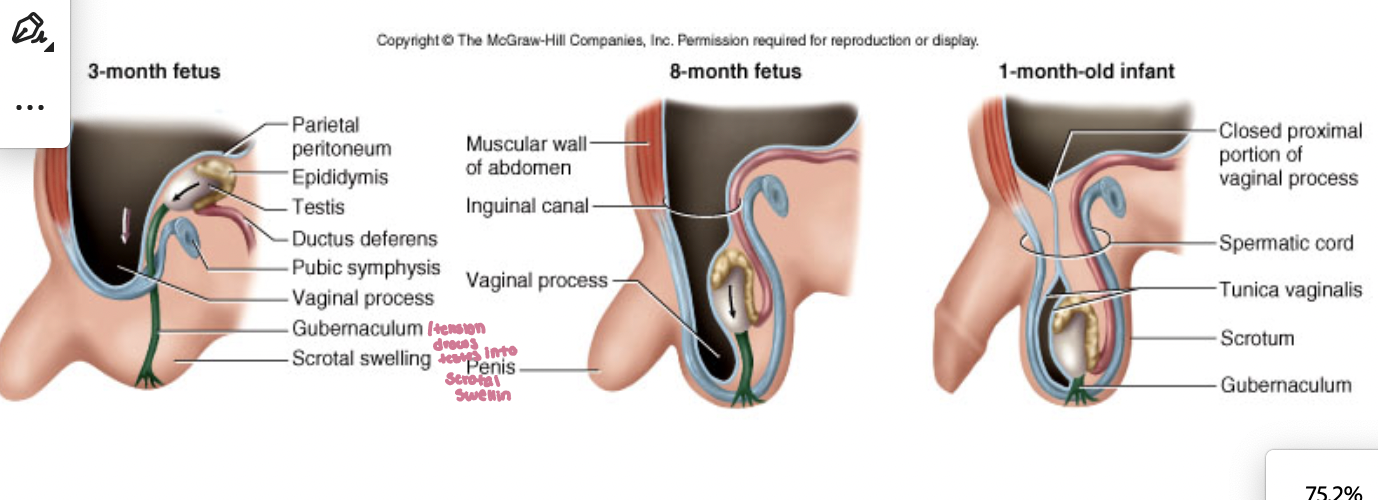
testies are connected to what that contain what (3)
spermatic cord which contains blood vessels, vas defernes, and lymphatics
what is it called when one of more testies doesn’t decend into the scrotum
cryptorchidism
Scrotum is separated into two sacs by what
raphe (dividing line)
Muscles of testies and jobs (2)
dartos muscle: smooth muscle, wrinkles sac
cremaster muscle: skeletal muscle, pulls ac close to body
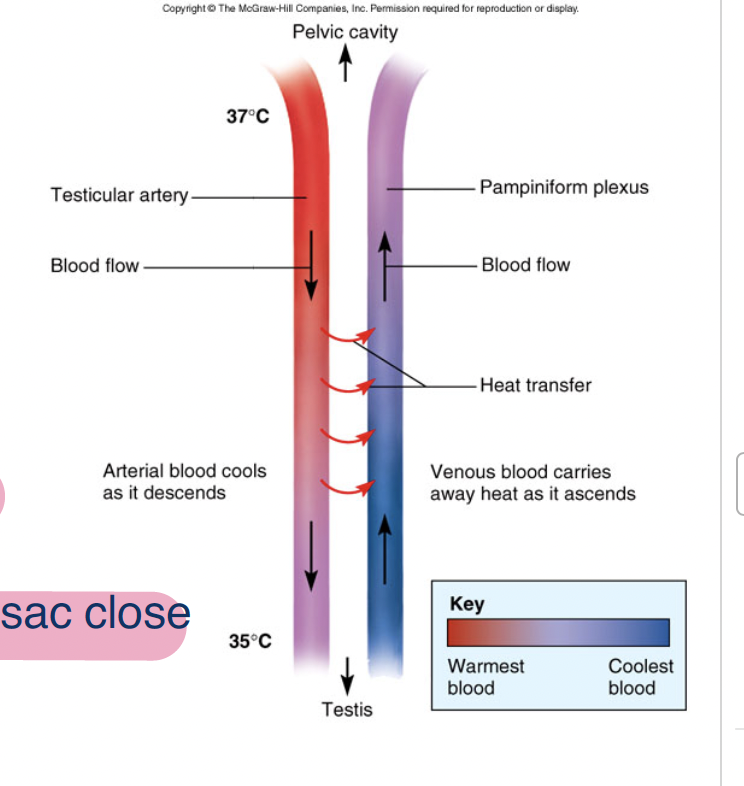
Scrotum preforms what to protect sperm
counter heat exchange: exchnages heat from oxygenated blood going to testies to venous blood returning to body to testies don’t get too hot and kill the sperm
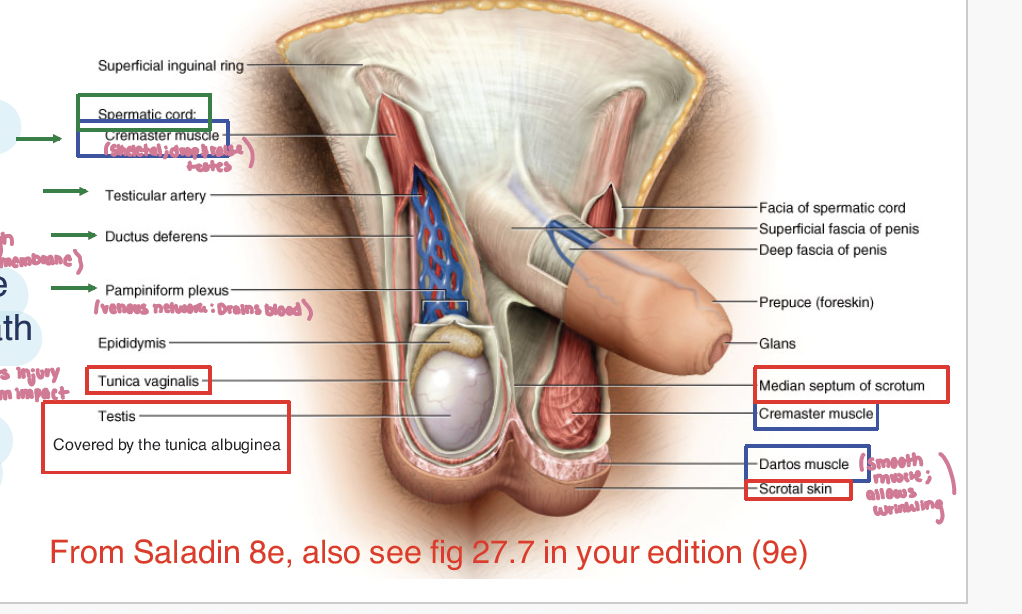
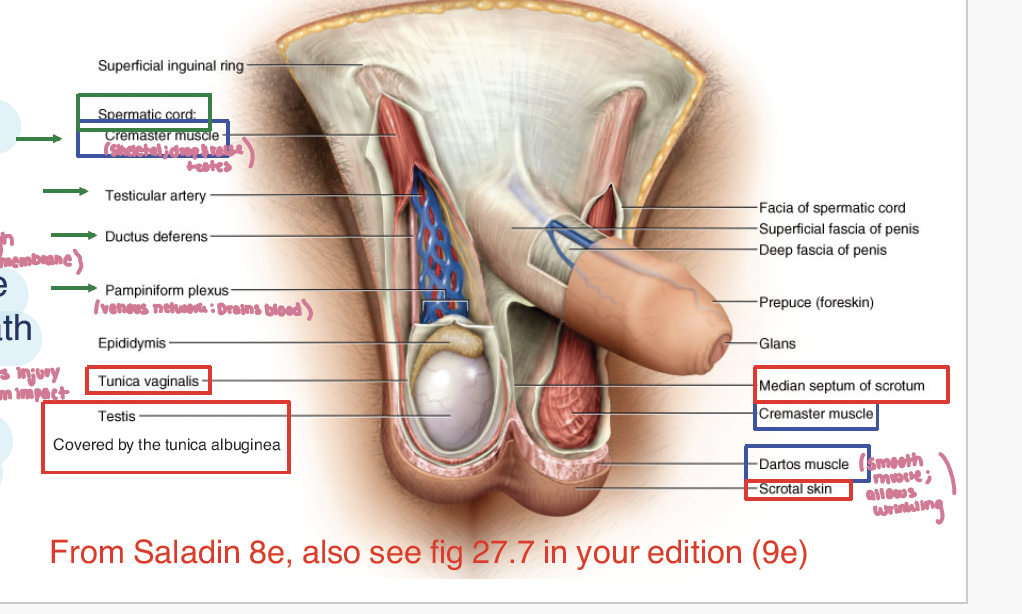
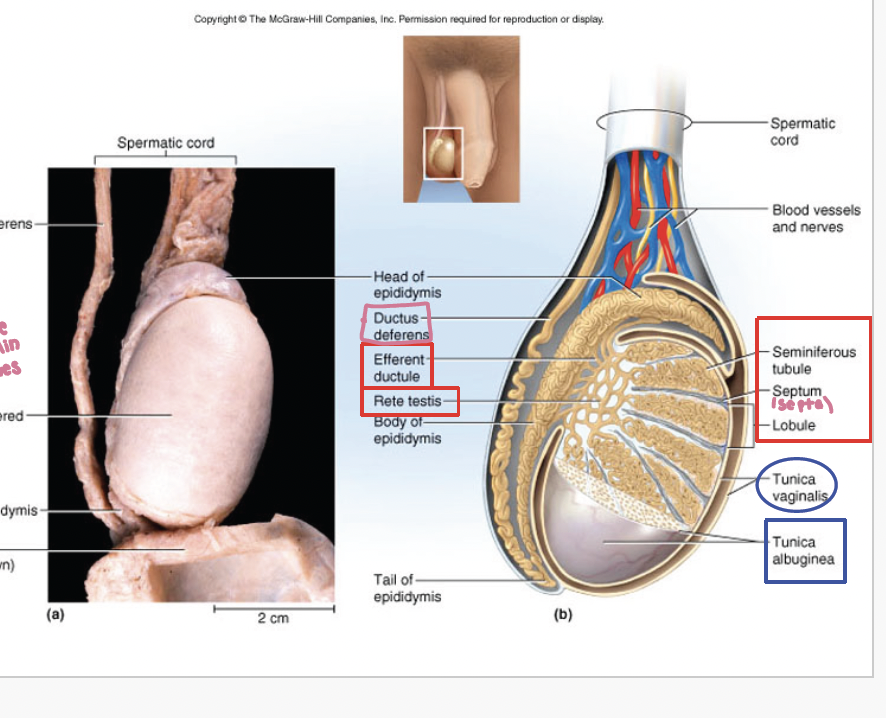
Testies are covered by what membrane layers (2)
tunica vaginalis: serous membrane (akin to peritoneum)
tunica albugenia: collagenous membrane surrouns testies, under tunica vaginalis
septa are made from what
septa are made from the tunica albugenis that make lobes from seminiferous tubules
seminiferous tubules have what, produce what, and have what special cells
have long coiled tubes, produce sperm, and interstitial (leydig) cells between tubules which secrete sex hormones (androgens): testosterone
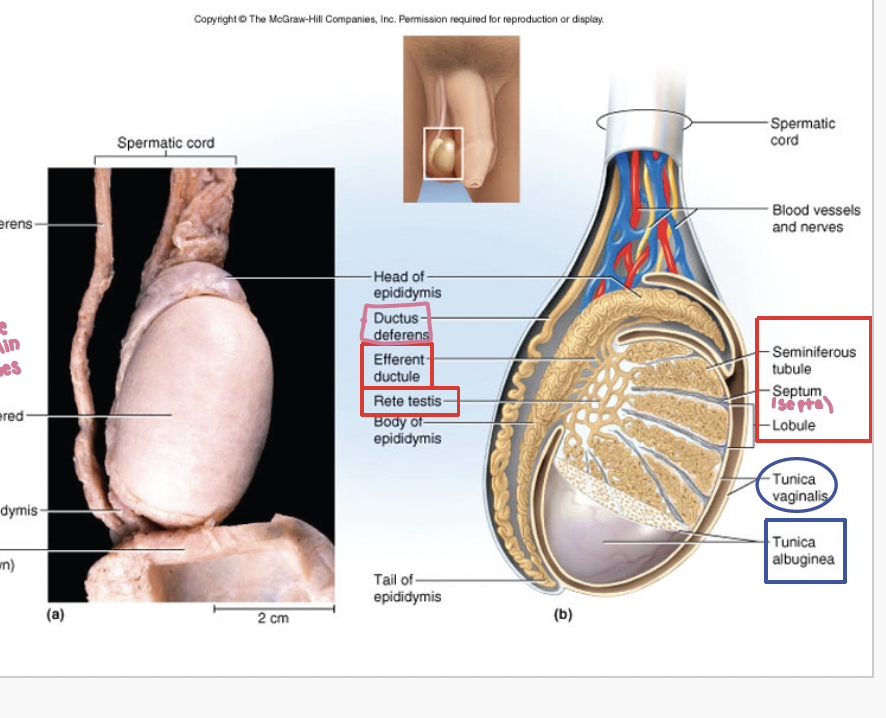
efferent ducties connect what
rete testies and epididymis
Susentacular cells (nurse cells) maintain what
blood testes barrier
Susentacular cells (nurse cells) support what (2)
mitosis and meiosis after stimualtion by GnRH and FSH, support spermatogenesis
Susentacular cells (nurse cells) secrete what (3)
inhibin: peptide hormone that acts as a negative feedback to prevent secretion of GnRH and FSH
androgen binding protein (ABP): traps androgens to raise their levels
mullerian inhibiting factor: hormone causes regression of mullerian ducts which from uterine tubes and uterus
ductus deferens starts where, goes through where, and elarges where
starts at epidiymis, goes through inguinal canal, enlarges are ampulla
ductus deferenes moves sperm how and can store sperm how long
using peristalsis, can store sperm for several months
urethras of penis in order (3)
prostatic urethra
membranous urthra
spongey urethra
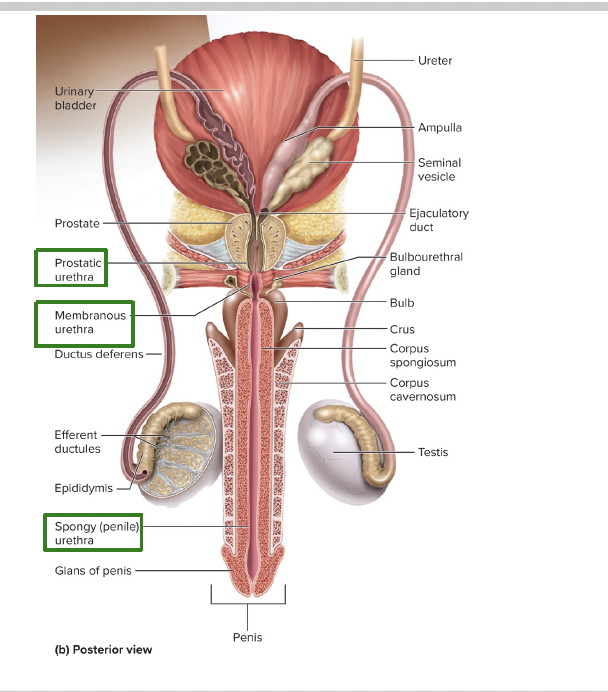
seminal vesicles contribute how much to volume of semen
65-75%
seminal vesicles secretion contain (4)
fructose
prostaglandins
fibrogen (prosemenogelin)
alkaline secretion
semeinal vesicles causes what for sperm and what is it the start of
caused motility for sperm, first step of capacitation which makes them capable of fertilization
Prostate gland makes up how much volume of seminal fluid
25-30%
prostate gland secretion contains (3)
alkaline secrteion
seminalplamin (antibiotic)
fibronlysin (serine protese) dissolves fibrin
Bulbourethral gland secretes what into seminal volume
alkaline mucus with lubrication properties into the urethra
prepuce (foreskin) produces what
smegma
penis have how many masses of erectile tissue and what are they
2 corpus cavernosa beneath fascia
1 corpus spongiosum around urethra
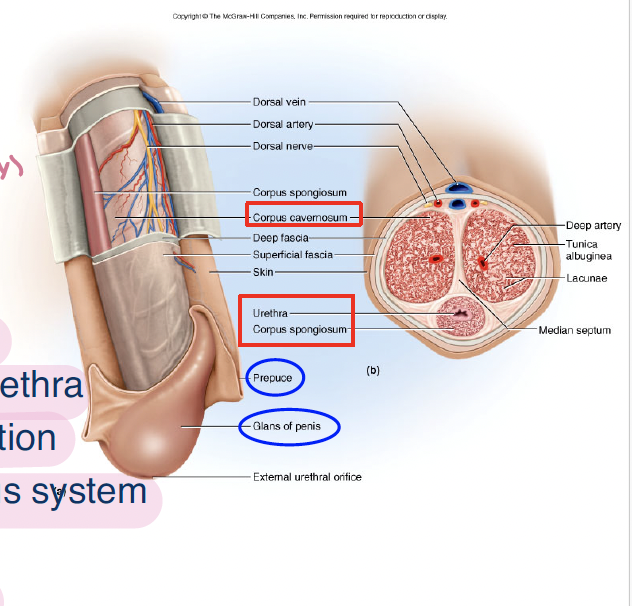
dilation of erectile tissue causes what
erection
erection is stimulated by what (4)
PNS
release of nitrix oxide (NO)
relaxation of vasuclar smooth muscle
increased blood flow
head of sperm has what (2)
nucleus and densly packed chromosomes, acrosomal cap
middle peice of sperm has what (1)
mitochondria that produce that ATP needed to move the tail (uses fructose as its main energy soruce)
tail of sperm is the only what in human body
flagellum
sperm maturation in epidiymis what happens (4)
epididymis monitor and adjusts fluid in the seminiferous tubules via absorption and secretion from pseudostratified columnar epithelium
stores and protects spermatozoa
facilitates functional maturation of spermatozoa and prevent ability to fertilize
capacitation: when sperm gain the ability to become motile and fully functional
how much fluid is a normal ejaculate
2-5 ml
how many spermatazoa per ml of ejaculate
50-120 million
how much spermatozoa in ml of ejaculate is considered functionally sterile
20-25 million
how much of ejaculate is actually sperm
2-5%
seminal fluid break down in perecents (4)
seminal vesicles: 65-75%
prostate gland:25-30%
susentacular cells and epidiymis: 5%
buluuethral gland: 1%
enzymes in semen (3) and their job
dissolve vaginal mucus
seminalplasmin: antibiotic
proastatic enzymes: that covert fibrinogen to fibrin (prosemenogelin)
fibrinolysis: (serine protease) dissolve fibrin
GnRH is what
gonadotropin releaseing hormone (causes gonads to release gonagotropins)
GnRH is released from where
hypothalamus in small bursts
GnRH releasing levels are
levels are continuous and released at even levels (does not change throughout month)
GnRH causes the release of what
FSH and LH from the pituitary gland
FSH is what and released from where
follicel stimulating horomone, released from the anterior pituitary
FSH in males targest what and causes what
targets sustentacular cells to release androgen binding proteins and promote spermatogenesis
What kind of lop between GnRH and FSH and inhibin controls spermatogenesis
negative feeback loop
LH is what and released from where
lutenizing hormone, released from anterior pituitary
LH target what cells and causes what
targets interitial cells and triggers the secretion of testosterone and other androgens
Three male androgens
testosterone (main)
dihydrotestosterone
dehydroepiandrosterone (made in adrenal gland)
Androgens (testostrone) are carried by what
albumin (1/3), and gonadal steroid binding globulin (2/3)
androgenes (testosterone) are necessary for what
spermatogenesis and sperm maturation
androgens affect the function of what
CNS (can make you angry faster)
androgens (testosterone) stimulate what (3)
metabolism, ertythopoesis, bone and muscle growth
androgens (testosterone) maintain what
secondary sex characteristics and male acessory organs (epo, vas def)
Draw feedback regulation #1
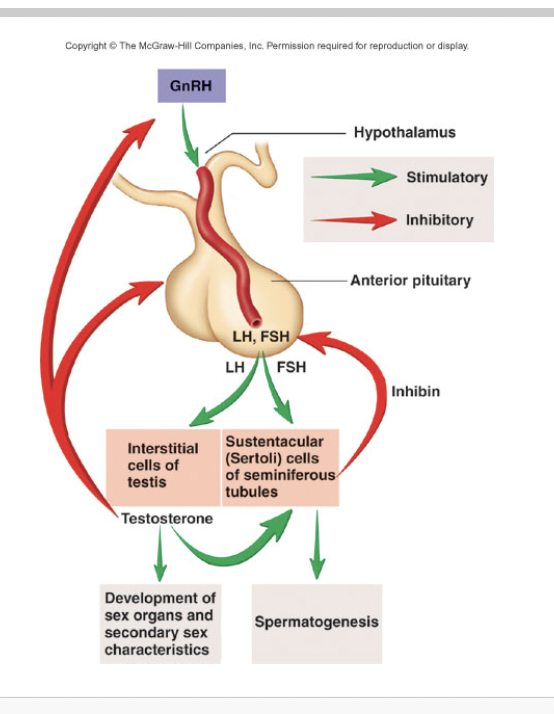
Draw Feedback Regulation #2 males
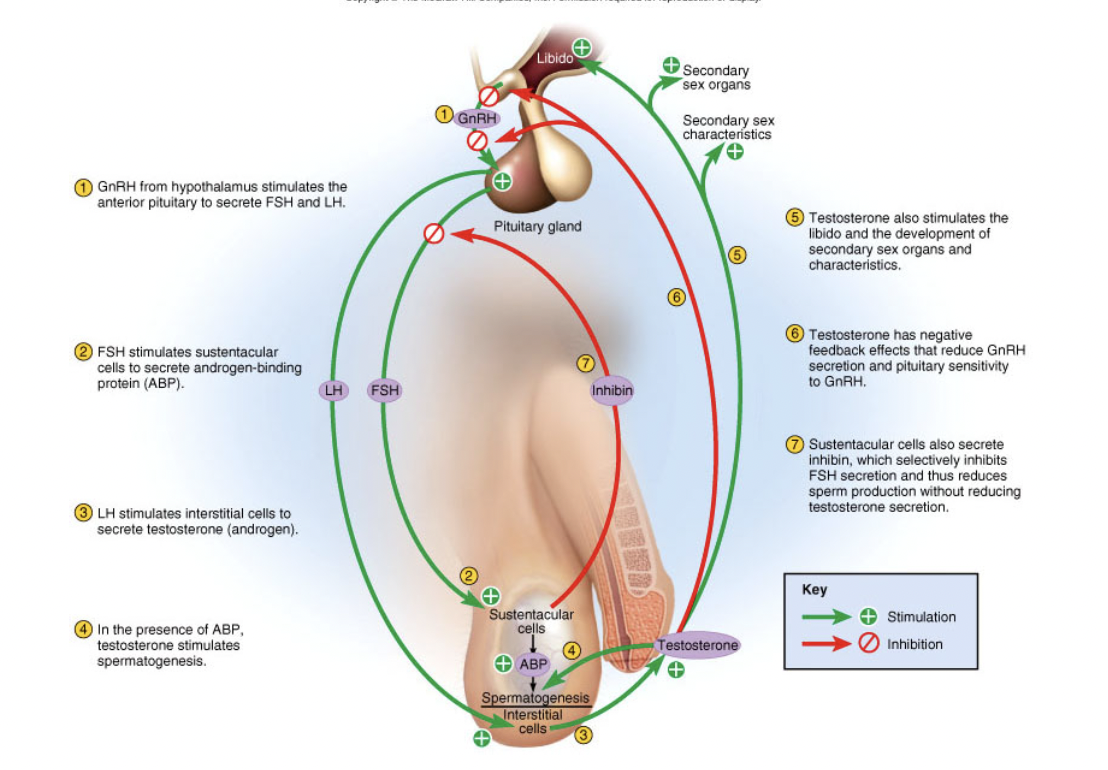
fetal testosterone begins when
about 7th week
fetal testosterone affects where and does what (3)
affects hypothalamus
sex behavior
sex drive
programs GnRH, FSH, and LH release
fetal testosterone activates susentacular cells to release what
mullerian inhibiting factors, causes degeneration of mellerian ducts that form uterine tubes and uterus
arousal leads to what and how (3)
erection of penis, parasympathtic outflow over the pelvic nerves, release Ach and NO (PDE5 inhibitors)
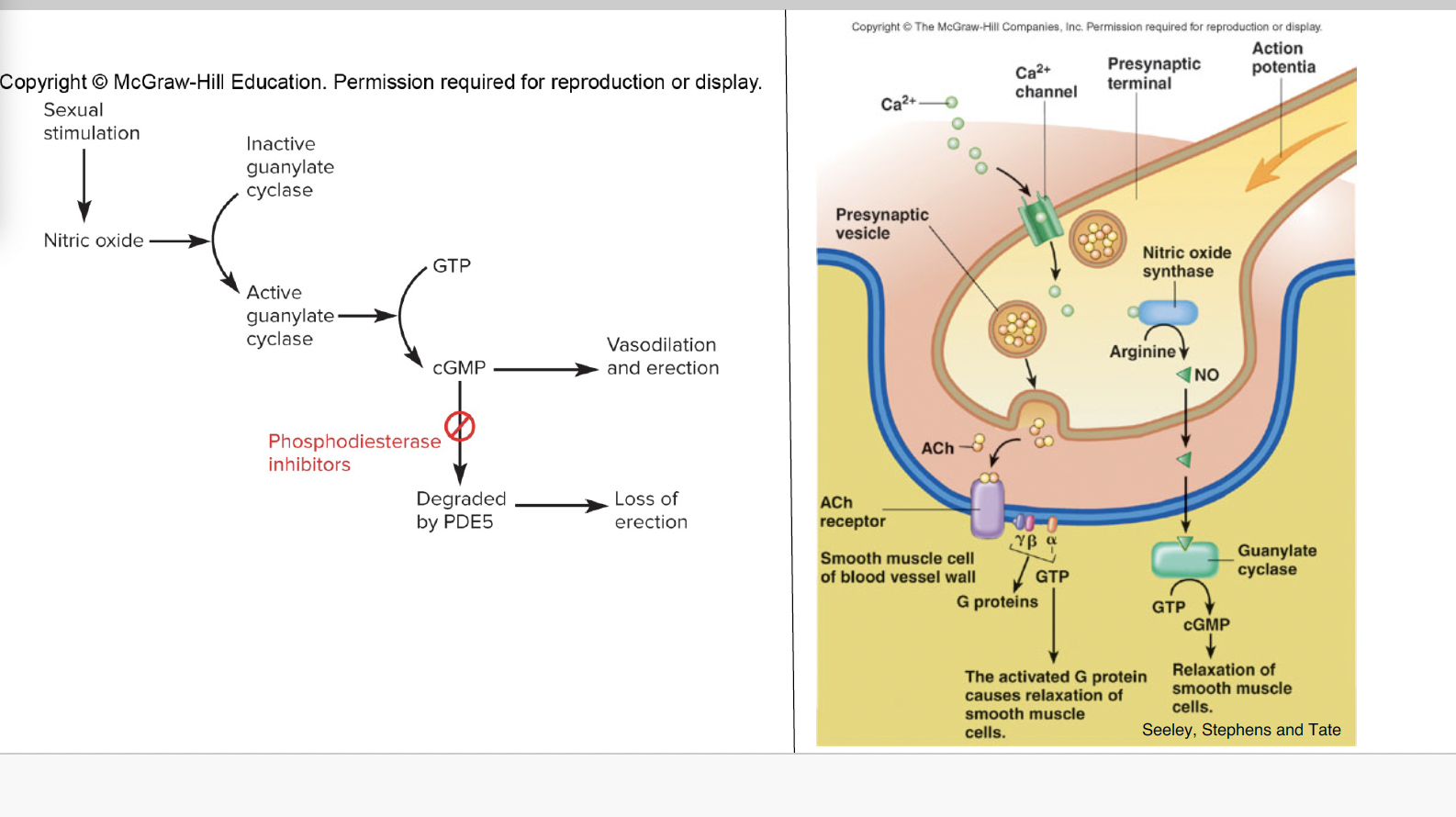
emission and expulsion occur how and why
occur under sympathetic control, bulbospongiosus muscle are under somatic control, results in semen begin pushed twoard the urthral opening
detumescence is what
subsidence of erection, mediated by sympathetic nervous system
what happens after climax
levels of testosterone decline, FSH and LH levels rise, gradula resuction in sexual activity