Lecture 1 - Periodontum
1/33
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
34 Terms
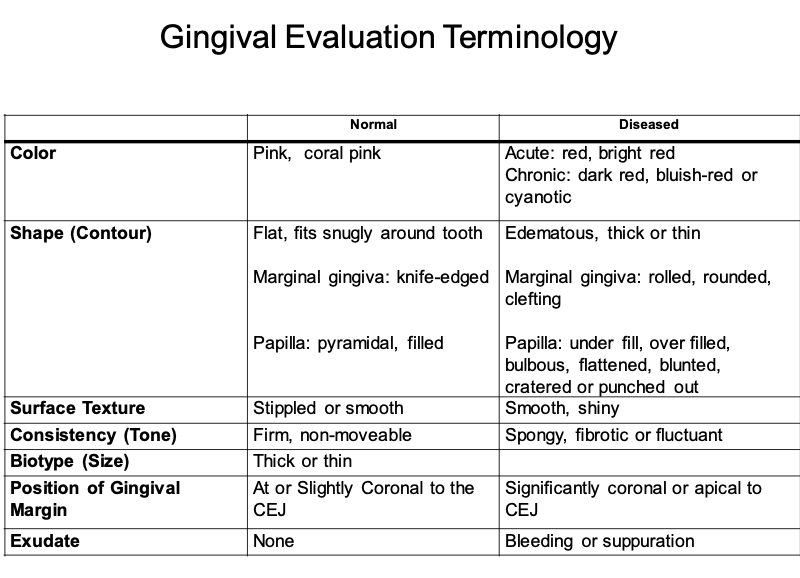
Parts of the gingiva
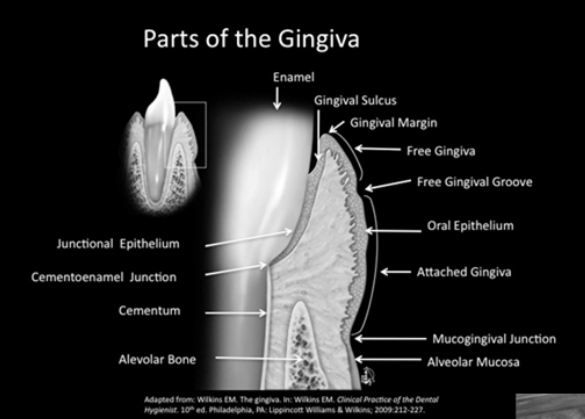
3 types of soft tissue in oral mucosa
1. Masticatory mucosa:
Is a tissue that is firmly attached to the underlying bone and covered with parakeratinized or keratinized epithelium. The gingiva and the tissue covering the hard palate are examples.
2. Lining mucosa:
Loosely attached to their underlying structures and covered with non-keratinized epithelium. Lips, cheeks, floor of the mouth are examples.
3. Specialized mucosa:
Covers the dorsal surface of the tongue
Alveolar Mucosa (Lining Mucosa)
Thin and non-keratinized
• Predominant connective tissue fibers are elastic, therefore is bound loosely to the underlying bone (permits movement)
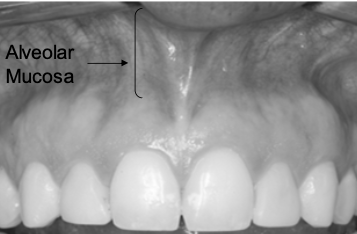
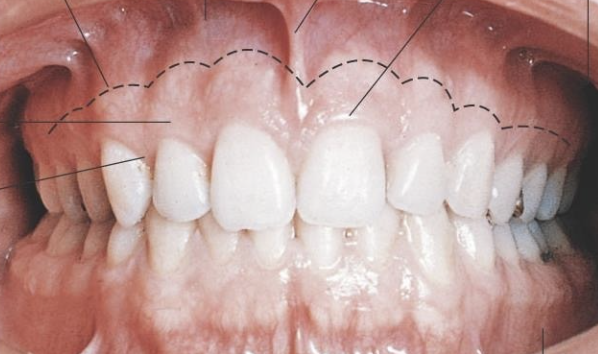
Mucogingival Junction
(MGJ) is the anatomical boundary marking the transition between the firm, keratinized attached gingiva and the loose, movable, nonkeratinized alveolar mucosa
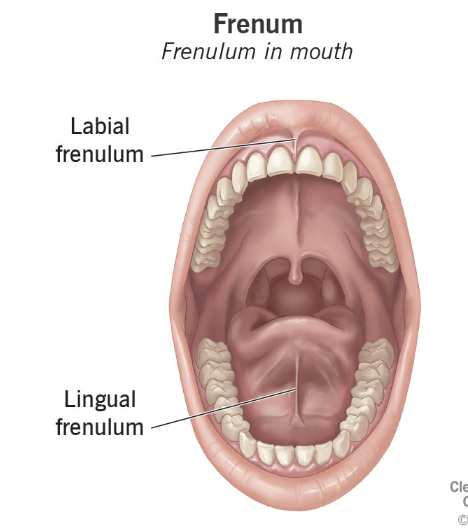
Frenum
A membranous fold of skin or mucous membrane that supports or restricts the movement of a part or organ, such as the small band of tissue connecting the tongue to the floor of the mouth.
Tori and exostoses
are nodular protuberances of mature bone
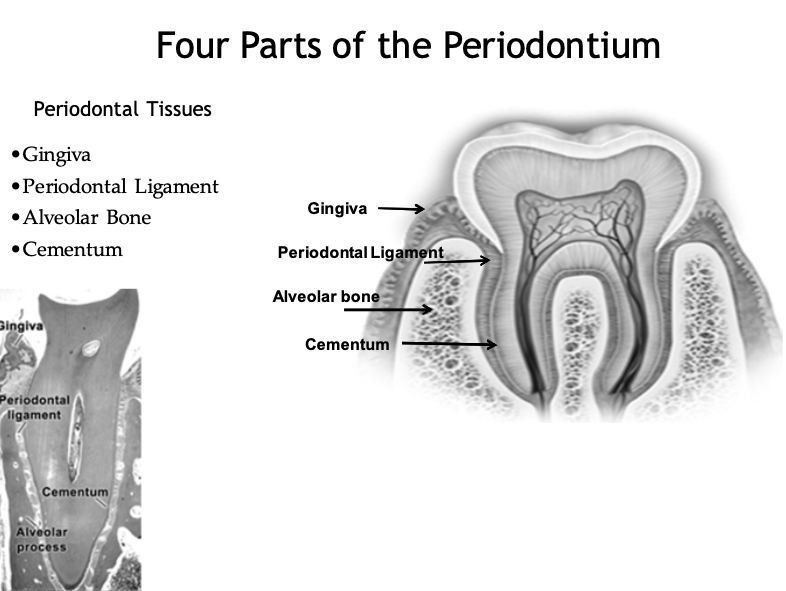
Four Parts of the Periodontium
• Gingiva
• Periodontal Ligament
• Alveolar Bone
• Cementum
Gingiva
The gingiva is that part of the masticatory mucosa that covers the alveolar process and surrounds the cervical portion of the teeth
two types attached and unattached (marginal or free gingiva)
Attached Gingiva
• Continuous with the marginal gingiva
• Extends from the external surface of the base of the sulcus to the mucogingival junction
• Firm, resilient and tightly bound down to the underlying bone
• Width varies in different areas of the mouth
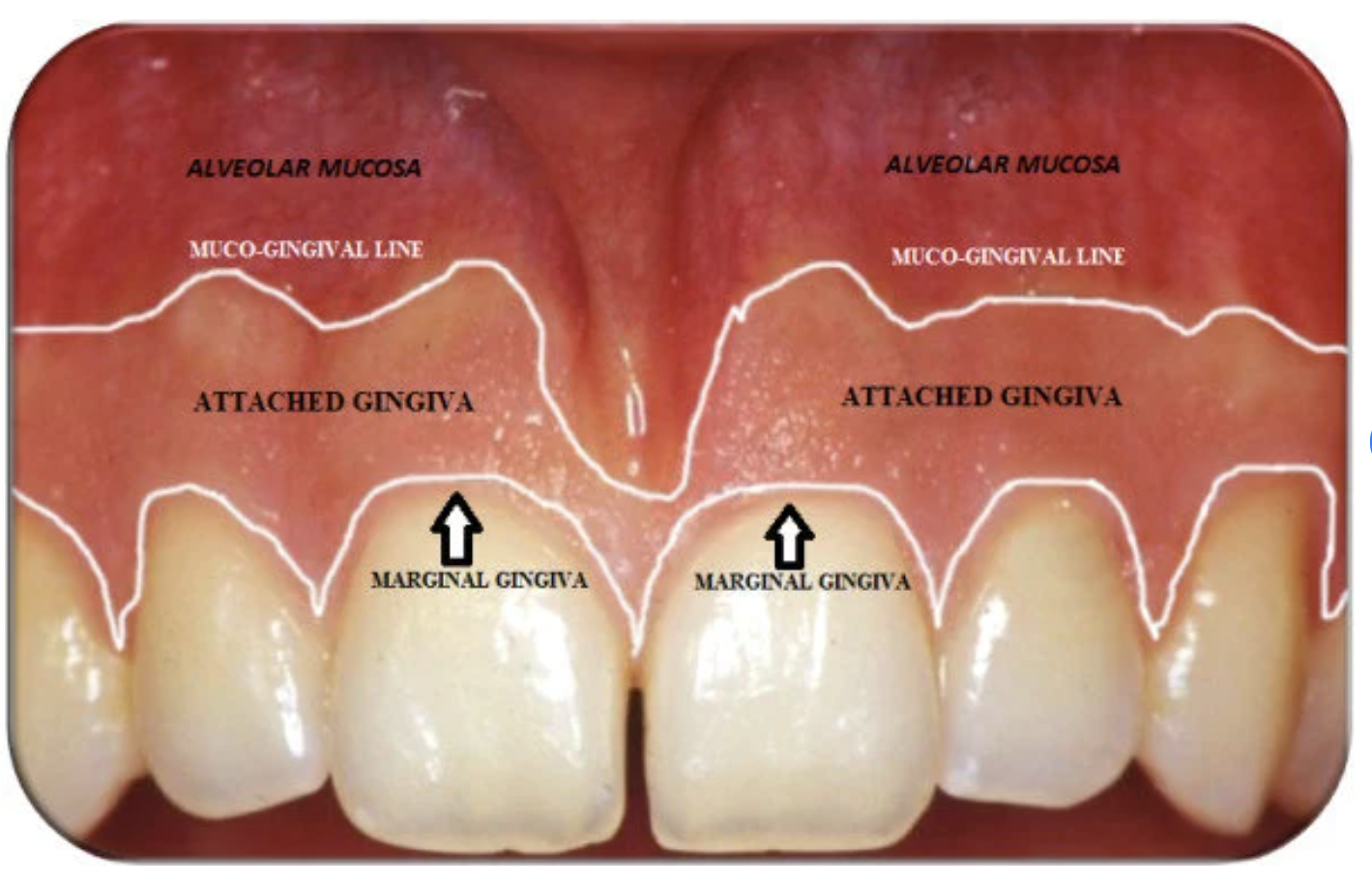
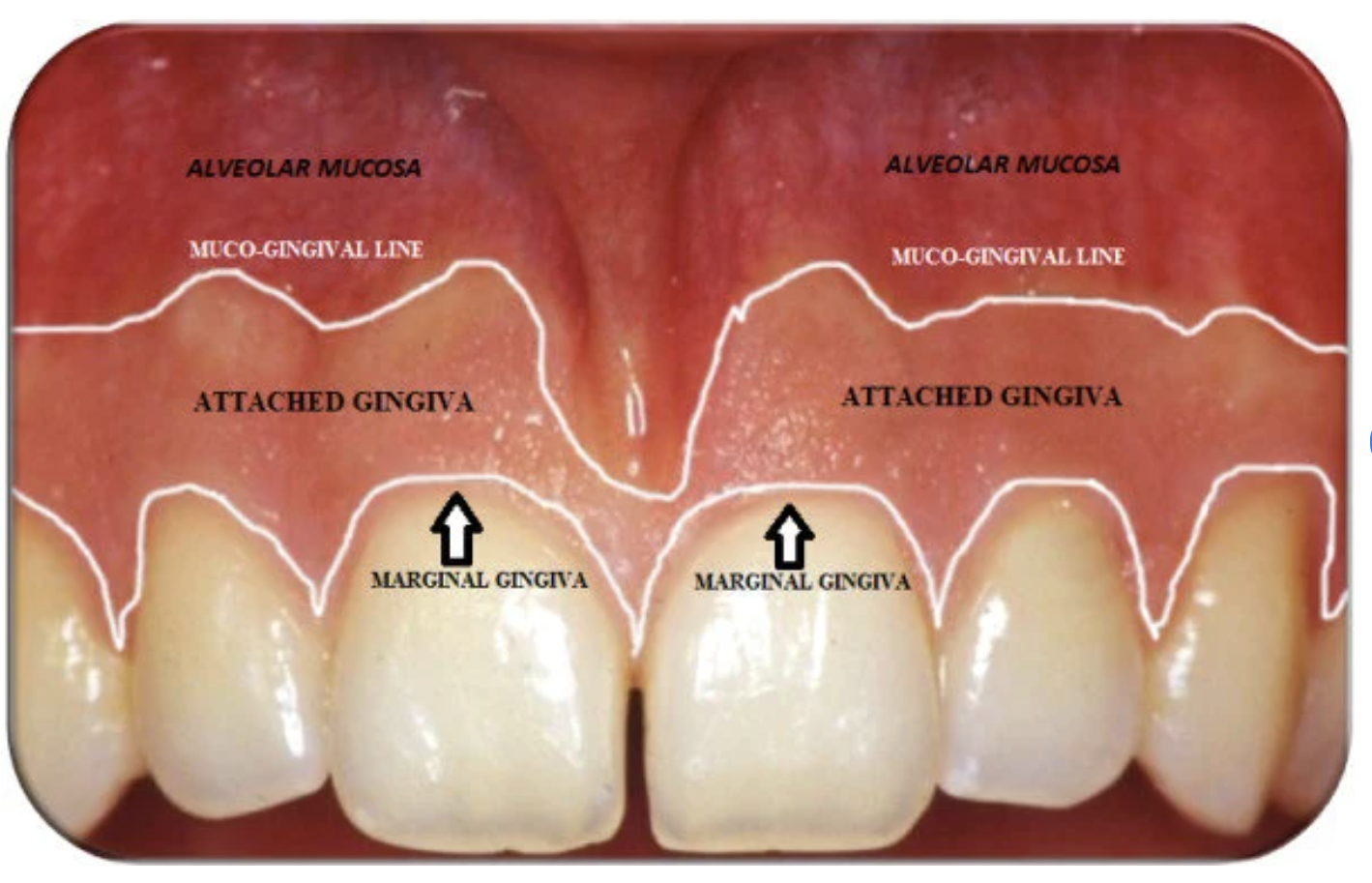
Marginal Gingiva (Unattached Gingiva)
• Terminal edge or border of the gingiva that surrounds tooth in a collar like fashion
• It is not attached to the tooth, and it creates the soft tissue wall of the gingival sulcus. (external surface of sulcus)
• Is the most coronally positioned portion of the gingiva.
• In health, is knife-edged in contour, firm in consistency, and smooth in texture.
Oral Epithelium (attached + unattached gingiva)
• Oral keratinized epithelium: stratified squamous epithelium with primary cell the keratinocyte.
• Function is to protect the deep structures.
• The stratum corneum can be orthokeratinized or parakeratinized (retain nuclei).
• Keratin layer gives “coral pink” color to the attached gingiva
Cyanotic
Marked by bluish/purplish discoloration of the skin/gingiva due to a lack of oxygen in the blood
Surface Characteristics of Gingiva Shape (contour)
healthy:
Flat, fits snugly around tooth
Marginal gingiva: The gingival contour should slope coronally to end in a thin (knife) edge.
Mesiodistally the gingival margin should be scalloped in form. (Following CEJ)
Scallop flattens out from anterior to posterior teeth
Cleft
a space or opening made by or as if by splitting : fissure or a V-shaped indented formation
usually caused by aggressive flossing
Surface Characteristics of Gingiva (Texture)
healthy: Stippled or smooth
diseased: Smooth and shiny
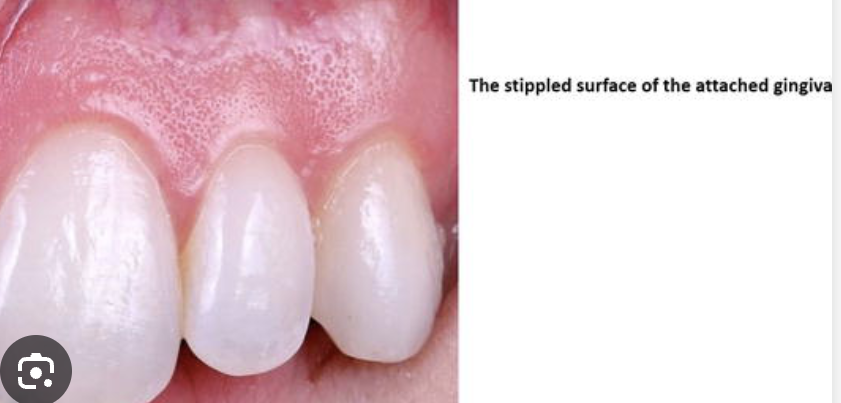
Surface Characteristics of Gingiva (Consistency)
healthy: Firm, non-moveable
diseased: Spongy, fibrotic or fluctuant
Interdental Gingiva
• Occupies Gingival Embrasure
• Pyramidal or “Col” Shaped
• The shape of the interdental tissue depends on the contact point of the adjacent teeth and the presence or absence of recession
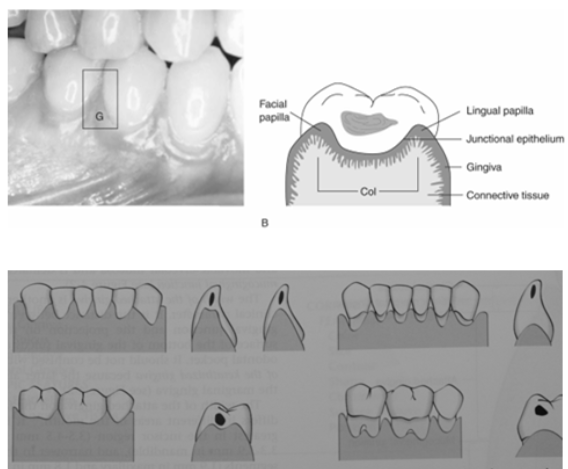
Surface Characteristics of Gingiva (Papilla- triangular space between adjacent teeth)
healthy Papilla: pyramidal, Fills interproximal space (with age a more blunted more than pointed contour may be considered normal)
diseased: Papilla: under fill, over fill, bulbous, flattened, blunted, cratered or punched out
Phenotype of Periodontium
The phenotype indicates a dimension that may change through time depending upon environmental factors and clinical intervention and can be site-specific (phenotype can be modified, not the genotype).
Periodontal phenotype is determined by gingival phenotype (gingival thickness, keratinized tissue width), and bone morphotype (thickness of the buccal bone plate).
1) Probe visible: thin (≤1 mm).
2) Probe not visible: thick (> 1 mm).
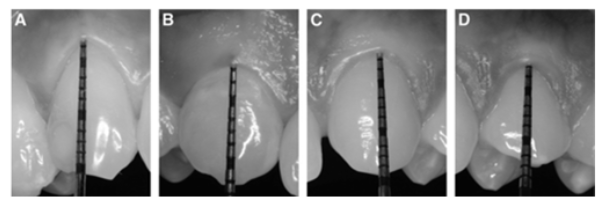
In the clinical examination of the gingiva, the observations noted should be described using the following:
• Location: Generalized or localized
• Distribution: Diffuse, marginal or papillary
• Severity: Slight, moderate or severe
GINGIVAL EVALUATION GUIDELINES summary:
• Color
• Shape
• Surface texture
• Consistency
• Size: “Phenotype”
Thick vs Thin Periodontium
• Position of Gingival Margin: Above, at or below CEJ (recession)
• Bleeding/exudates
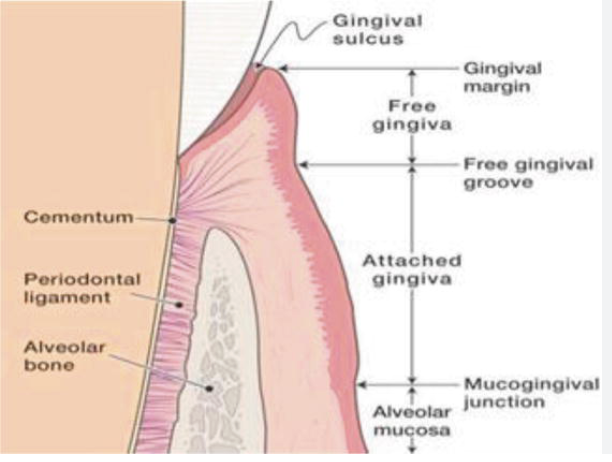
Sulcus
Is the shallow crevice or space around the tooth bounded by the surface of the tooth on one side and the epithelium lining the free margin of the gingiva on the other side.
t is V shaped, and it permits the entrance of a periodontal probe
The clinical determination of the depth of the gingival sulcus is an important diagnostic parameter.
The histologic depth of a sulcus will not be equal to the depth of penetration of the probe.
The so-called probing depth of a clinically normal gingival sulcus in humans is less than 3 mm
Gingival Crevicular Fluid
Cleanse material from the sulcus
Contain plasma proteins that may improve adhesion of the epithelium to the tooth
Possess antimicrobial properties
Exert antibody activity to defend the gingiva
Gingival Attachment:
1) Epithelial Attachment
2) Connective Tissue Attachment
Epithelial Attachment
Joins junctional epithelium to tooth surface
Attached to tooth surface (enamel, cementum, or dentin) through basal lamina-hemidesmosomes (adhesion of cells)
Completely restored after instrumentation or surgery and forms around dental implants
Attachment is reinforced by gingival fibers
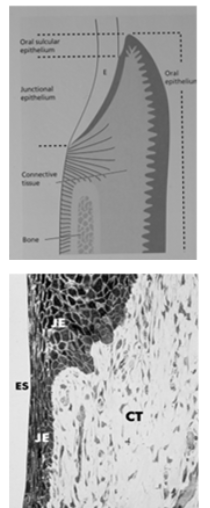
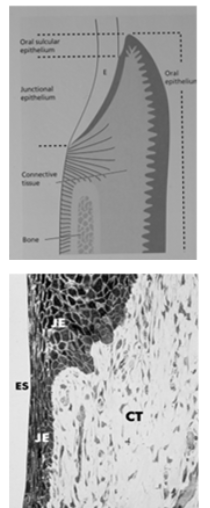
Junctional Epithelium
Nonkeratinized epithelium
More permeable than the oral or sulcular epithelium.
Junctional epithelium is firmly attached to the tooth surface, forming an epithelial barrier against plaque bacteria.
Allows access of gingival fluid, inflammatory cells, and components of the immunologic host defense to the gingival margin.
Junctional epithelial cells exhibit rapid turnover, which contributes to the host- parasite equilibrium and rapid repair of damaged tissue.
Has 2 basal laminas, one that faces the tooth (internal basal lamina) and one that faces the connective tissue (external basal lamina)
Connective Tissue Attachment
The supra-crestal fibers of the periodontal ligament
Function to:
a. brace marginal gingiva firmly against tooth
b. provide rigidity necessary to withstand the forces of mastication without being deflected away from the tooth
c. to unite the free marginal gingiva with the cementum of the root and the adjacent attached gingiva
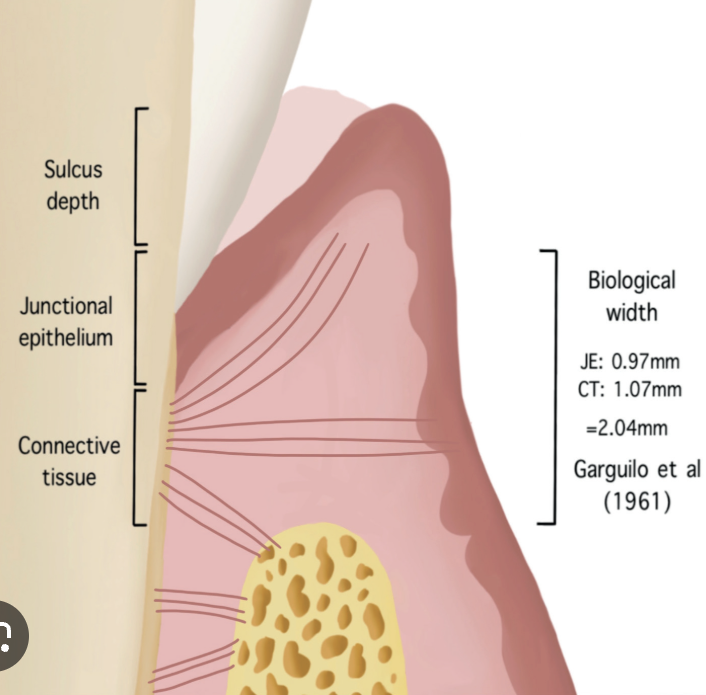
Gingival Fibers
• A. Gingival fibers (Connective Tissue)
• B. Periodontal Ligament
• C. Alveolar crest
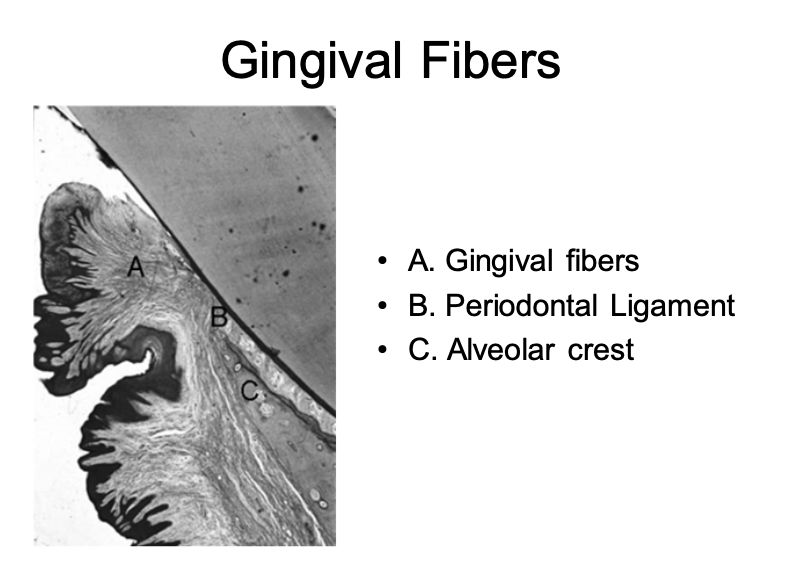
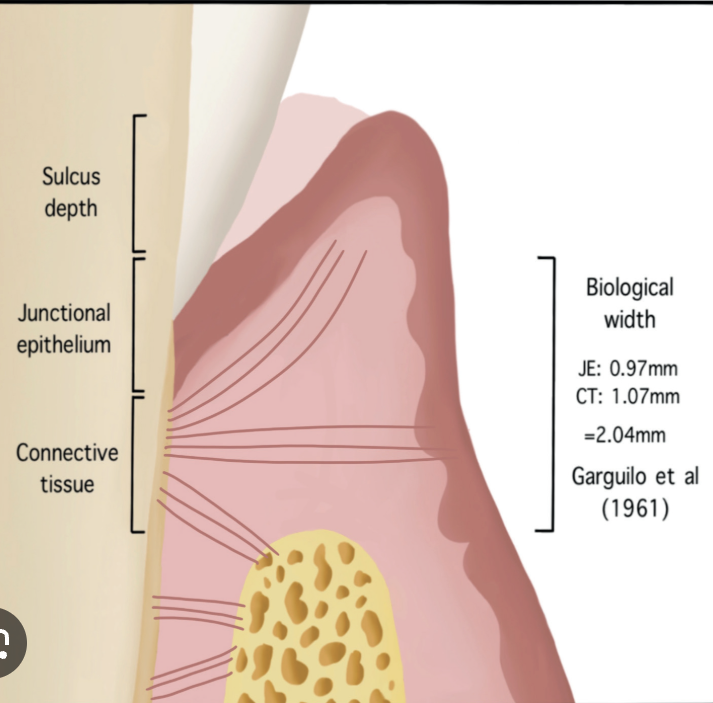
Dimensions and relations of the dentogingival junction in humans.
• Sulcus depth = 0.69mm
• Epithelial Attachment = 0.97mm
• Connective tissue = 1.07mm
basically 1mm each
Periodontal Ligament (PDL)
• PDL: The periodontal ligament is the connective tissue that surrounds the root and connects it with the bone. It is continuous with the connective tissue of the gingiva and communicates with the marrow spaces through vascular channels in the bone.
0.1 to.25 mm in width (average .2mm in width) Resorption and deposition continues throughout life
Cementum covers root surface. Fibers of PDL are attached-50 to 200 microns in thickness
Alveolar bone (process) provides housing for the roots of the teeth. Dependent on presence of teeth.
Fibers of PDL are attached.
Collagen fiber bundles that attach cementum of root to the alveolar bone
Function: anchorage and protection of the tooth
Portion of the fibers that insert into the cementum and bone are called Sharpey’s fibers
Contains vessels and nerves
Apical to cemento-enamel junction (CEJ)
High fiber turnover rate. Occlusal functional adaptation
Epithelial cell colonies found in the PDL are referred to as Epithelial Rests of Malassez
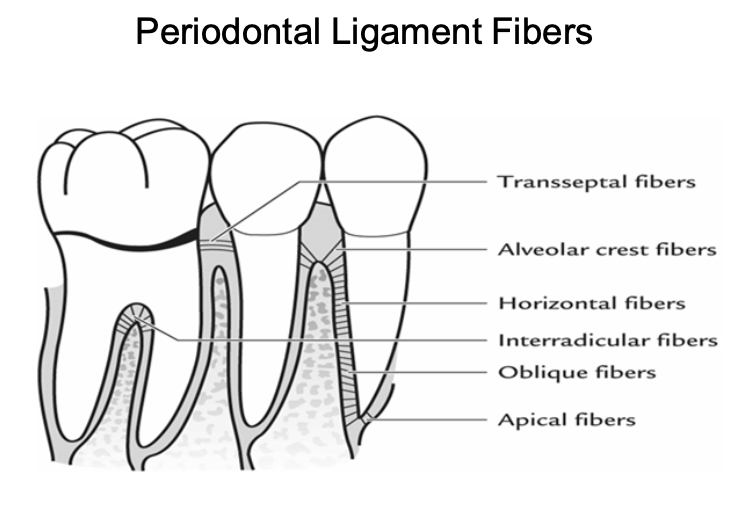
Periodontal Ligament Fibers
Alveolar crest: retain tooth, oppose lateral forces, protect deeper structures
Oblique: oppose axially directed forces
Transseptal: prevent teeth from loosing contact
Horizontal: oppose lateral forces
Interradicular: prevent tooth tipping and extrusion
Apical: prevent tipping and extrusion, protect vessel and nerve supply
Cementum
Covers entire root surface varying thickness (16-200µm)
Calcified avascular mesenchymal tissue
function: to anchor the tooth to the bone socket by means of periodontal ligament.
Ankylosis: fusion of cementum and alveolar bone
2 types:
– Acellular-cervical half, no cells
– Cellular: apical half and in furcations, cells (cementocytes)
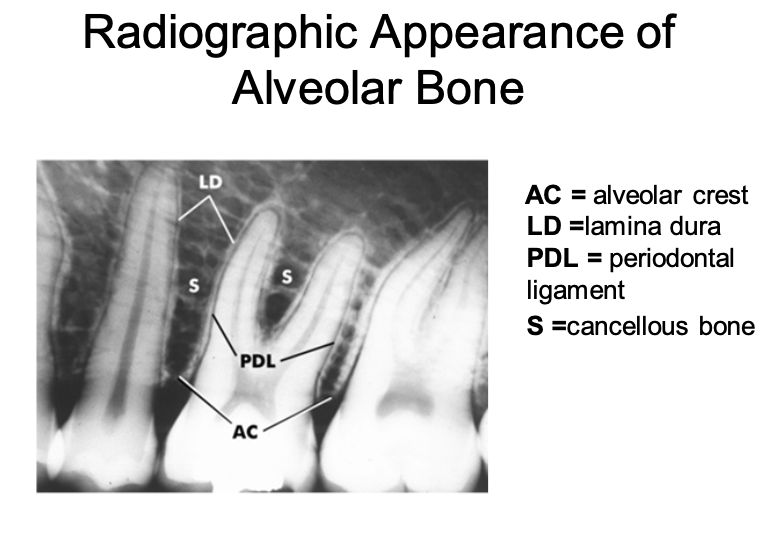
Alveolar Bone
That portion of the maxilla and mandible that forms and supports the alveolar housing (sockets of the teeth).
Constant remodeling: activity of osteoblast and osteoclast.
The least stable of the periodontal structures due to its constant state of flux
Osteoid: newly deposited, nonmineralized bone matrix
Bundle bone: bone adjacent to the PDL that contains the Sharpey’s fibers. Inner layer of alveolar bone proper (lamina dura)
Periosteum: connective tissue layer covering outer surface of the bone
The bone height is within 2 millimeters of the CEJ
Radiographic Changes seen in Periodontal Disease
• Localized erosions of the marginal bone
• Thinning of crestal lamina dura
• Loss of sharp border with the lamina dura of
the adjacent teeth
• Slight loss of bone height (<15%)
• Moderate loss of bone height (15-33%)
• Severe loss of bone height (>33%)