Neuromuscular Diseases: TBI, Concussion, and Plexus Injuries
1/82
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
83 Terms
What is Traumatic Brain Injury (TBI)?
A negative effect on brain function resulting from external physical force.
What percentage of individuals with closed head injuries die on site?
Almost half.
What are common behavioral changes seen in TBI patients?
Changes in behavior and emotional control.
What demographic is at higher risk for TBI?
Men, particularly those aged 15-24 and the elderly population.
What are some common causes of TBI?
Concussions, motor vehicle accidents (MVA), gun violence, and military conflict.
What is the primary damage in TBI?
Damage resulting from forces exerted on the brain at the time of injury.
What does secondary damage in TBI refer to?
Changes compromising brain function due to the brain's reaction to trauma, such as swelling and impaired perfusion.
What are cerebral contusions?
Bruises on the brain tissue resulting from impact.
What are the parenchymal changes associated with TBI?
Axonal injury from shear and tensile forces that disrupt transport of proteins and cause swelling.
What is hypoxia in the context of TBI?
A condition caused by blockages or decreased oxygen in the blood, affecting brain function.
What are common clinical manifestations of a concussion?
Minor head injury, short loss of consciousness, dizziness, disorientation, nausea, headache, fatigue, and personality changes.
What motor deficits may occur as a result of TBI?
Monoplegia, hemiplegia, and abnormal reflexes.
What is heterotopic ossification?
Abnormal bone growth around a joint, where bone forms in muscle tissue.
What are some medical complications associated with TBI?
Cardiovascular effects, respiratory complications, intravascular coagulation, diabetes insipidus, and iatrogenic infection.
What is the first step in diagnosing TBI?
Assessing the level of consciousness through eye opening, best motor response, and verbal response.
What imaging techniques are used in TBI diagnosis?
CT and MRI scans.
What is the goal of acute treatment for TBI?
Stabilization and prevention of secondary complications.
What does rehabilitation for TBI aim to achieve?
Return to optimal function, restoration of mobility, self-care, and recreational activities.
What is community reentry in TBI rehabilitation?
The transition from rehabilitation unit to independent living.
What factors influence the prognosis of TBI?
The severity of the injury.
What are associated injuries with TBI?
Lacerations, cerebral contusions, basal skull fractures, epidural hematomas, and subdural hematomas.
What is the significance of the article 'Ethical Issues in Using Deception to Facilitate Rehabilitation for a Patient With Severe Traumatic Brain Injury'?
It discusses ethical considerations in rehabilitation practices for severe TBI patients.
What is a concussion considered?
A mild Traumatic Brain Injury (TBI).
What are common symptoms of a concussion?
Headache, dizziness, variable amnesia, difficulty concentrating, depression, apathy, and anxiety.
How long do concussion symptoms typically last?
Symptoms typically resolve in 7-10 days.
What diagnostic methods are used for concussions?
Examinations for vestibular, balance, and vision problems; MRI and CT imaging; and blood tests like the Banyan Brain Trauma Indicator.
What is the Concussion Graded Symptom Checklist?
A tool used for assessing concussion symptoms.
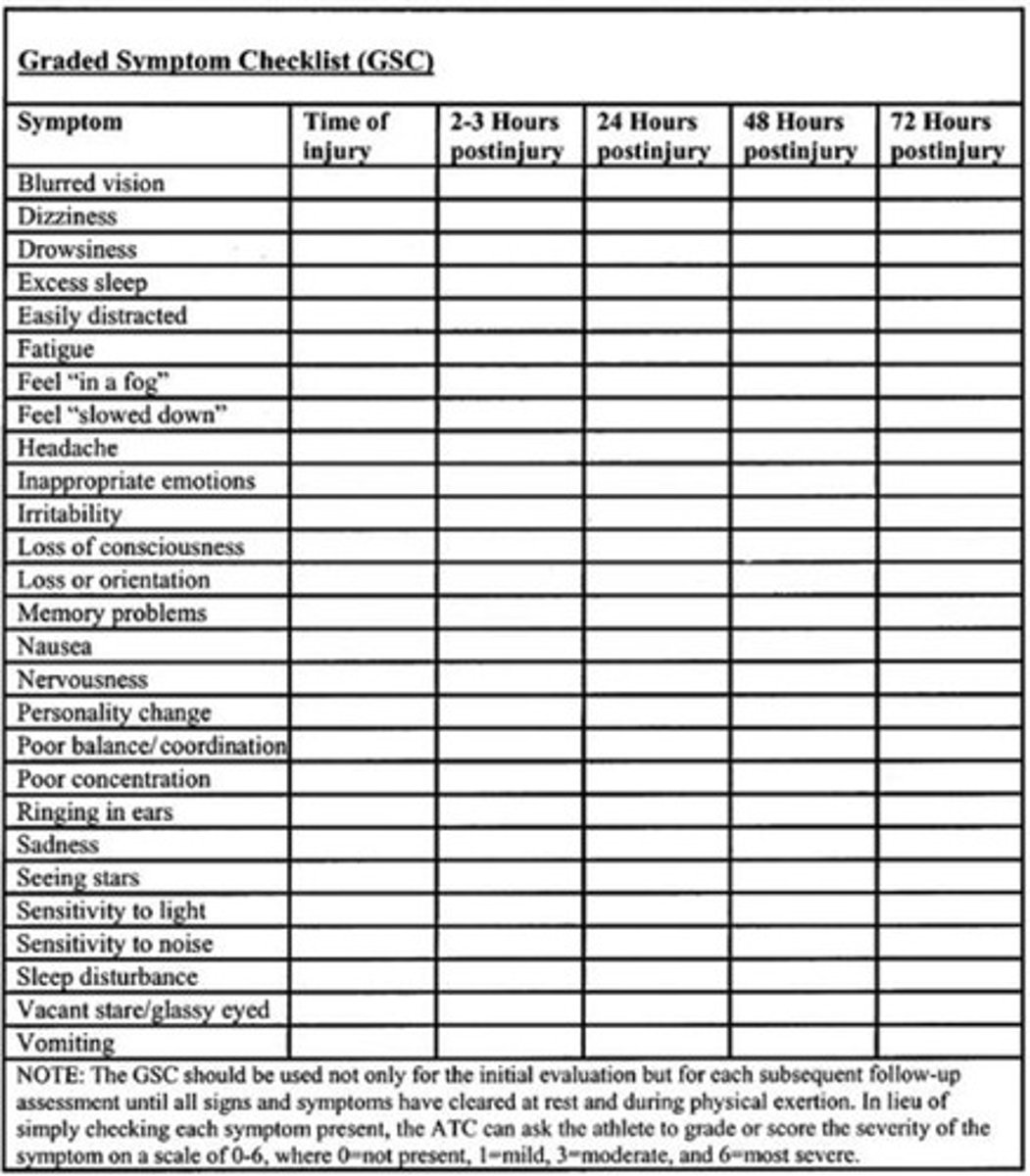
What is the protocol for returning to activities after a concussion?
Absence of symptom complaints, return to school, and return to play with clearance from a licensed health care provider.
What is Post Concussion Syndrome?
A condition that commonly follows a mild head injury, characterized by persistent symptoms like headache and dizziness.
What are the clinical manifestations of a Basal Skull Fracture?
Battle's sign, raccoon eyes, CSF rhinorrhea, CSF otorrhea, and halo sign.
What is Battle's sign?
Bruising over the mastoid process that develops within 24-48 hours after a head injury.
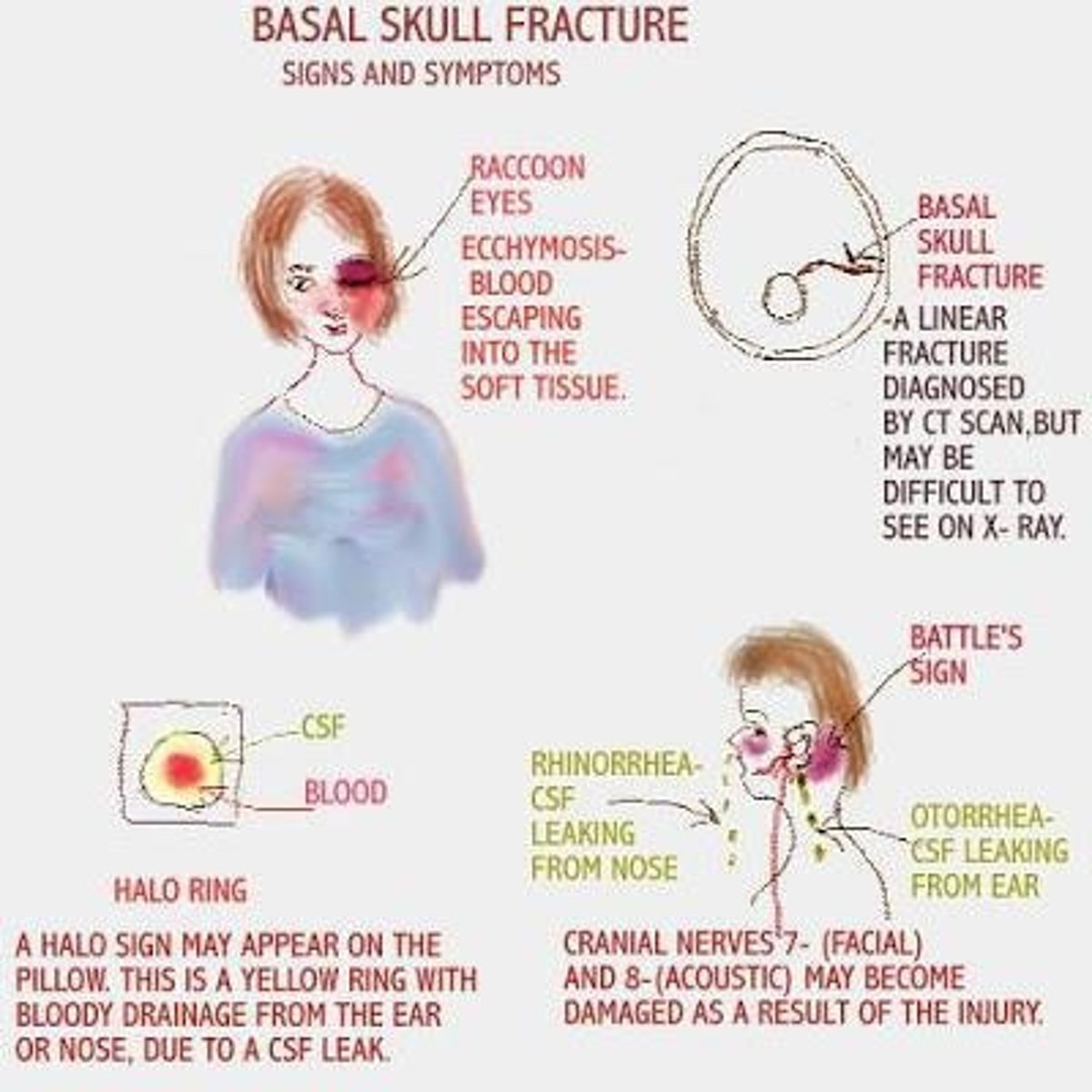
What does raccoon eyes indicate?
Bilateral bruising around the eyes resulting from a skull fracture.
What is CSF rhinorrhea?
The drainage of cerebrospinal fluid through the nose, usually unilateral.
What is the treatment for asymptomatic adults with simple linear fractures?
They do not require any intervention.
What is Erb's Palsy?
A condition resulting from a traction injury to the brachial plexus at birth, affecting C5-C6 nerves.
What are the symptoms of Klumpke's Palsy?
Claw hand due to injury of the C7-T1 nerves, often from a traction injury at birth.
What is Saturday Night Palsy?
A radial nerve injury resulting from compression or ischemia.
What is the role of physical therapy in TBI management?
Includes monitoring motor behaviors, pulmonary care, positioning, ROM exercises, and vestibular therapy.
What is the prognosis for non-displaced basal skull fractures?
They usually heal without intervention.
What should be done if a concussion is suspected in an athlete?
The athlete should be removed from athletic activity.
What are common PT interventions for plexus disorders?
Maintenance of ROM, contracture prevention, splinting, and strengthening once nerve recovery begins.
What is the significance of the Banyan Brain Trauma Indicator?
It is an FDA-approved blood test for diagnosing concussions.
What cognitive and behavioral impairments are associated with traumatic brain injury?
Problems with attention, memory (including amnesia), concentration, and executive functions.
What types of pain can occur due to traumatic brain injury?
Head and neck pain, neurogenic pain, and psychological suffering.
What are common clinical manifestations of traumatic brain injury?
Cranial nerve damage, motor deficits (monoplegia, hemiplegia, abnormal reflexes), and heterotopic ossification.
What medical complications can arise from traumatic brain injury?
Cardiovascular effects, respiratory complications, intravascular coagulation, diabetes insipidus, and iatrogenic infection.
How is traumatic brain injury diagnosed?
By assessing the level of consciousness through eye opening, best motor response, and verbal response, along with diagnostic imaging (CT, MRI) and neuropsychologic evaluation.
What is the acute treatment goal for traumatic brain injury?
Stabilization and prevention of secondary complications such as hypoxia, edema, increased intracranial pressure, or bleeding.
What is the focus of rehabilitation for traumatic brain injury?
Return to optimal function, restoration of mobility, self-care, employment, and recreational activities.
What are associated injuries with traumatic brain injury?
Lacerations to the scalp, concussions, cerebral contusions, basal skull fractures, epidural hematomas, and subdural hematomas.
What are the symptoms of a concussion?
Headache, dizziness, variable amnesia, difficulty concentrating, depression, apathy, and anxiety.
What is the typical duration for concussion symptoms to resolve?
Symptoms typically resolve in 7-10 days.
What is the concussion graded symptom checklist used for?
It is used for concussion assessment.
What is the protocol for returning an athlete to play after a concussion?
The athlete should be cleared by a licensed health care provider trained in concussion evaluation and management.
What is the role of physical therapy in managing concussion?
To provide rest and recovery, restore strength and endurance, manage dizziness and balance, and counsel on returning to normal activities.
What is a basal skull fracture?
A fracture to the base of the skull, occurring in about 4% of severe head injuries.
What are common clinical manifestations of a basal skull fracture?
Battle's sign, raccoon eyes, CSF rhinorrhea, CSF otorrhea, and the halo sign.
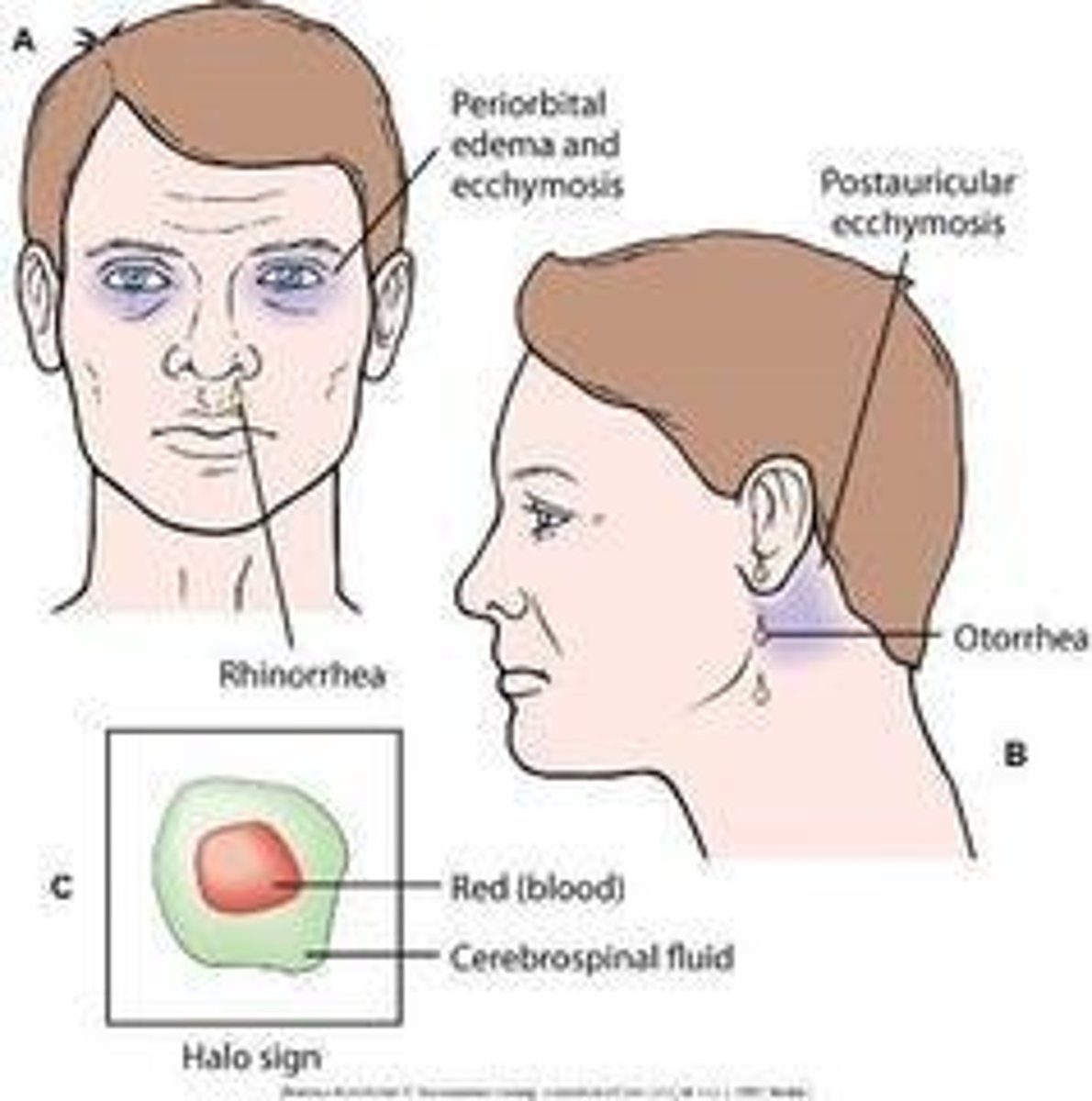
What is Battle's sign?
Bruising over the mastoid process that develops within 24-48 hours after a basal skull fracture.
What is Erb's Palsy?
A brachial plexus injury resulting from a traction injury at birth, affecting C5-C6 nerves.
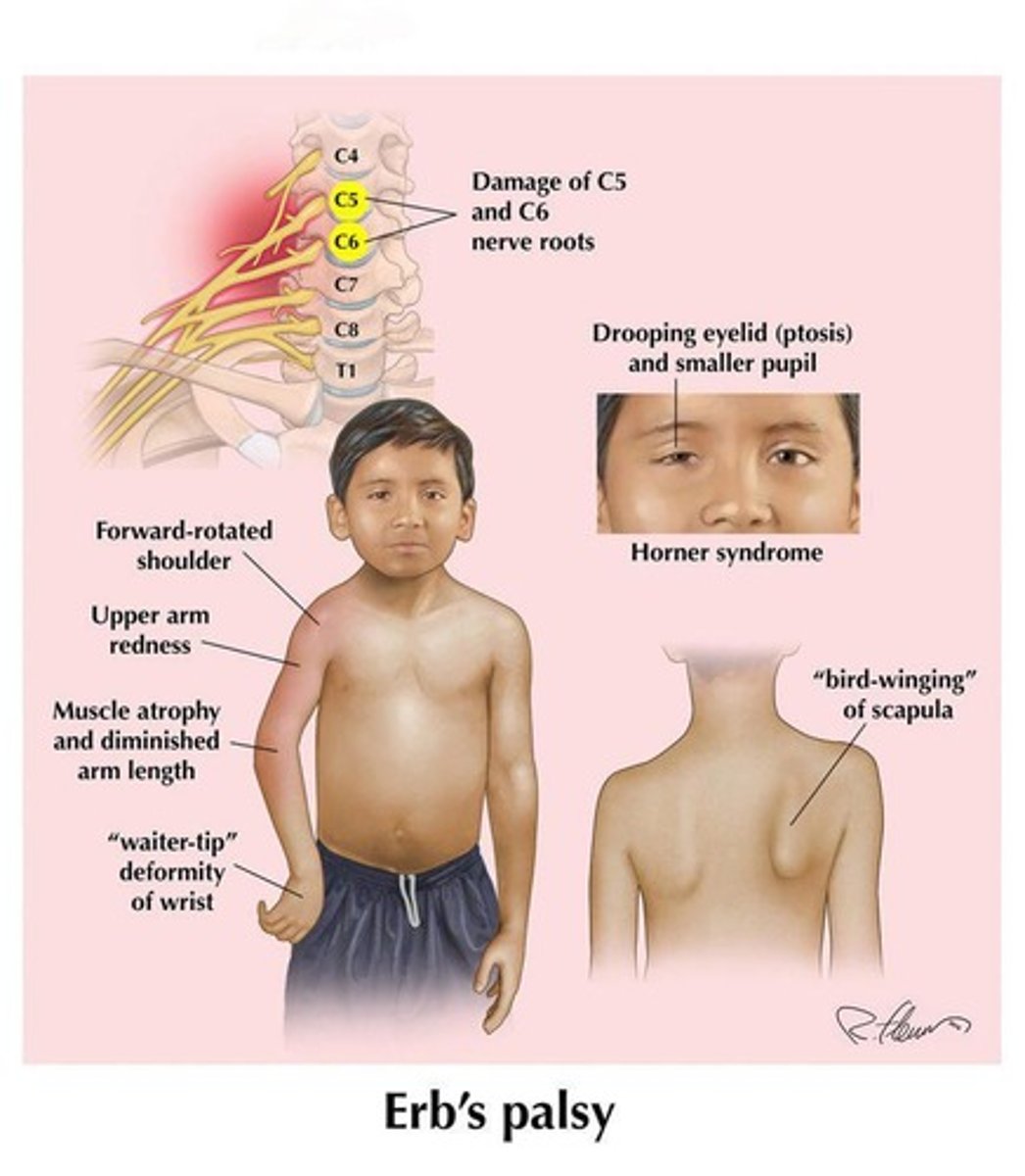
What is Klumpke's Palsy?
A brachial plexus injury affecting C7-T1 nerves, often resulting in claw hand.
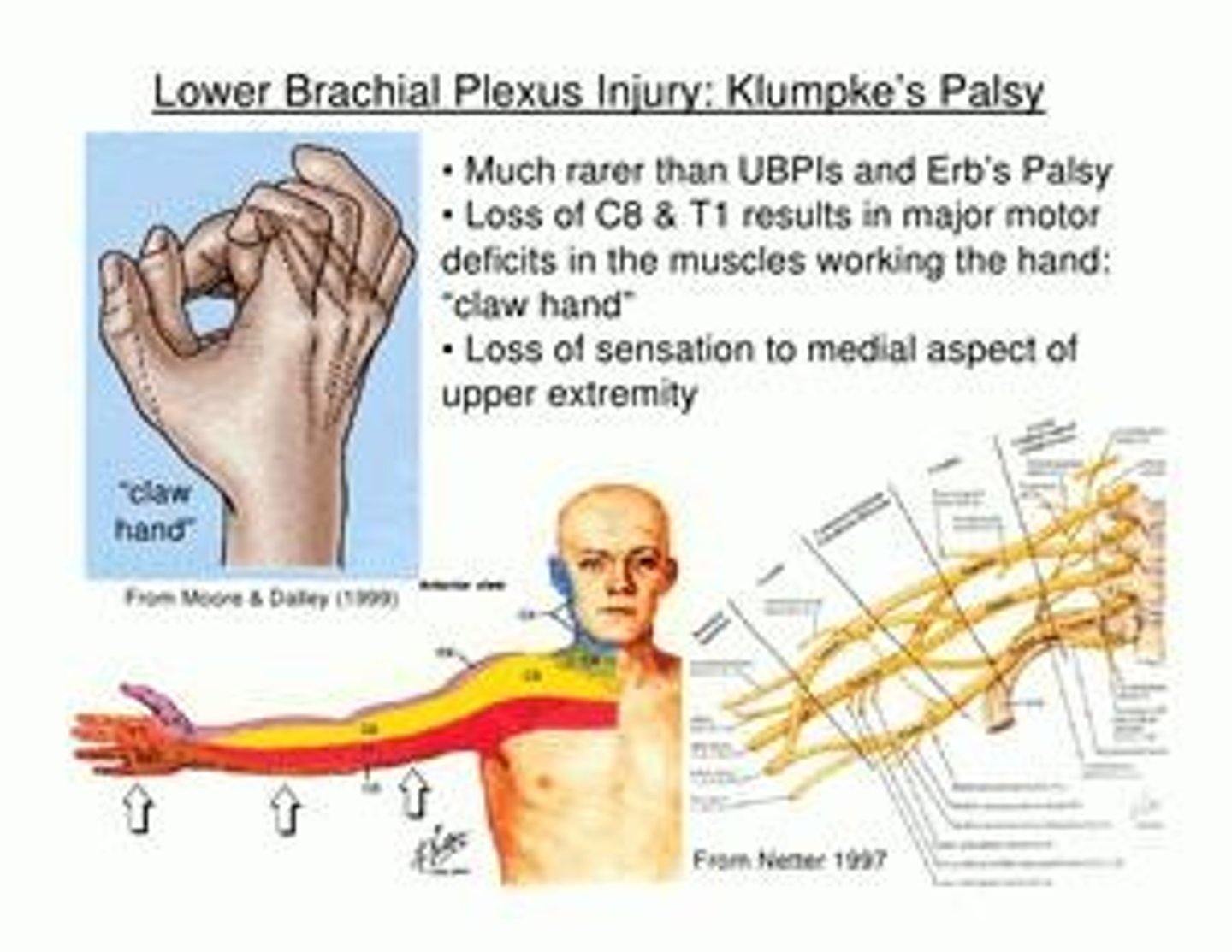
What is the treatment for brachial plexus injuries?
Includes maintenance of ROM, contracture prevention, splinting, and strengthening once nerve recovery begins.
What is the common cause of Saturday Night Palsy?
Radial nerve injury due to compression or ischemia, often from prolonged pressure on the arm.
What is the role of physical therapists in concussion management?
To provide guidance on activity levels, rehabilitation, and monitoring recovery.
What are common cognitive and behavioral impairments associated with traumatic brain injury?
Problems with attention, memory (including amnesia), concentration, and executive functions.
What types of pain are associated with traumatic brain injury?
Head and neck pain, neurogenic pain, and psychological suffering.
What are some cardiovascular complications of traumatic brain injury?
Neurogenic hypertension and cardiac dysrhythmias.
What respiratory complications can arise from traumatic brain injury?
Neurogenic pulmonary edema and aspiration pneumonia.
What is the initial step in diagnosing traumatic brain injury?
Assessing the level of consciousness by observing eye opening, best motor response, and verbal response.
What imaging techniques are used in the diagnosis of traumatic brain injury?
CT and MRI scans.
What is the primary goal of acute treatment for traumatic brain injury?
Stabilization and prevention of secondary complications such as hypoxia, edema, increased intracranial pressure, or bleeding.
What is the prognosis for traumatic brain injury dependent on?
The severity of the injury.
What is the recommended treatment protocol for athletes suspected of having a concussion?
They should be removed from activity and require clearance from a licensed health care provider trained in concussion management.
What does CSF rhinorrhea indicate?
Cerebrospinal fluid drains through the nose, usually unilateral, indicating a possible skull fracture.
What is the treatment for asymptomatic adults with simple linear skull fractures?
They do not require any intervention.
What is Klumpke's Palsy?
A condition affecting the C7-T1 nerves, often from traction injury at birth, leading to claw hand.
What is the role of physical therapy in managing traumatic brain injury?
Monitor motor behaviors, provide pulmonary care, positioning, ROM exercises, and vestibular therapy.
What is the common outcome of post-concussion syndrome?
Symptoms such as headache, dizziness, and difficulty concentrating often follow a mild head injury.
What is the purpose of the Concussion Assessment Tool?
To evaluate symptoms and guide the management of concussions.
What are the common plexus injuries associated with brachial plexus injuries?
Erb's Palsy, Klumpke's Palsy, Saturday Night Palsy, and scapular winging.
What is the typical incidence of Erb's Palsy?
Incidence ranges from 0.5 to 2 per 1000 births.
What is the recommended intervention for children with simple linear fractures of the skull?
They should be admitted for overnight observation.
What are the signs that indicate a potential need for surgical intervention in skull fractures?
Depressed fractures and the risk of meningitis in patients with basilar skull fractures.
What is the role of vestibular therapy in physical therapy for traumatic brain injury?
To address dizziness and balance issues.