PANCE - PREP PEARLS
1/1994
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
1995 Terms
systolic "ejection" crescendo-decrescendo harsh murmur at RUSB that radiates to carotids
aortic stenosis
harsh diastolic rumble murmur at apex (low) in LLD that may be preceded by OPENING SNAP and is MCC by ________
mitral Stenosis
rheumatic heart disease
what is a diastolic decrescendo blowing murmur @ LUSB and is associated with hammer rumble
aortic regurgitation
note:
wide pulse pressure
increases with handgrip
decreases with amyl nitrate
+/- austin flint murmur = mid-late diastolic rumble at apex
aortic regurgitation + head bobbing
DeMussets
aortic regurgitation + nailbed pulsations
Quincke pulses
blowing holosystolic murmur @ apex that radiates to axilla
mitral regurgitation
note:
increases with handgrip
decreases with amyl nitrate
midsystolic ejection click at apex is caused by what
mitral valve prolapse
note: reassurance and good prognosis in asymptomatic pts or with mild sx
systolic ejection crescendo-decrescendo flow murmur at PULMONIC AREA
atrial septal defect
note:
ostium secundum most common
left to right shunt (noncyanotic)
continuous machinery murmur that is loudest at pulmonic area
patent ductus arteriosus
note: left to right shunt (noncyanotic), continued PGE2 production promotes patency, IV indomethacin if preterm to close PDA
systolic murmur that radiates to the back/scapula/chest
increase BP upper > lower extermities
delayed/weak femoral pulses
coarctation of aorta
along with coarctation of aorta, 70% also have ____
bicuspid aortic valves
coarctation of aorta
CXR
rib notching
note:
"3 sign" on barium swallow
angiogram gold standard
Tx balloon angioplasty, PGE1
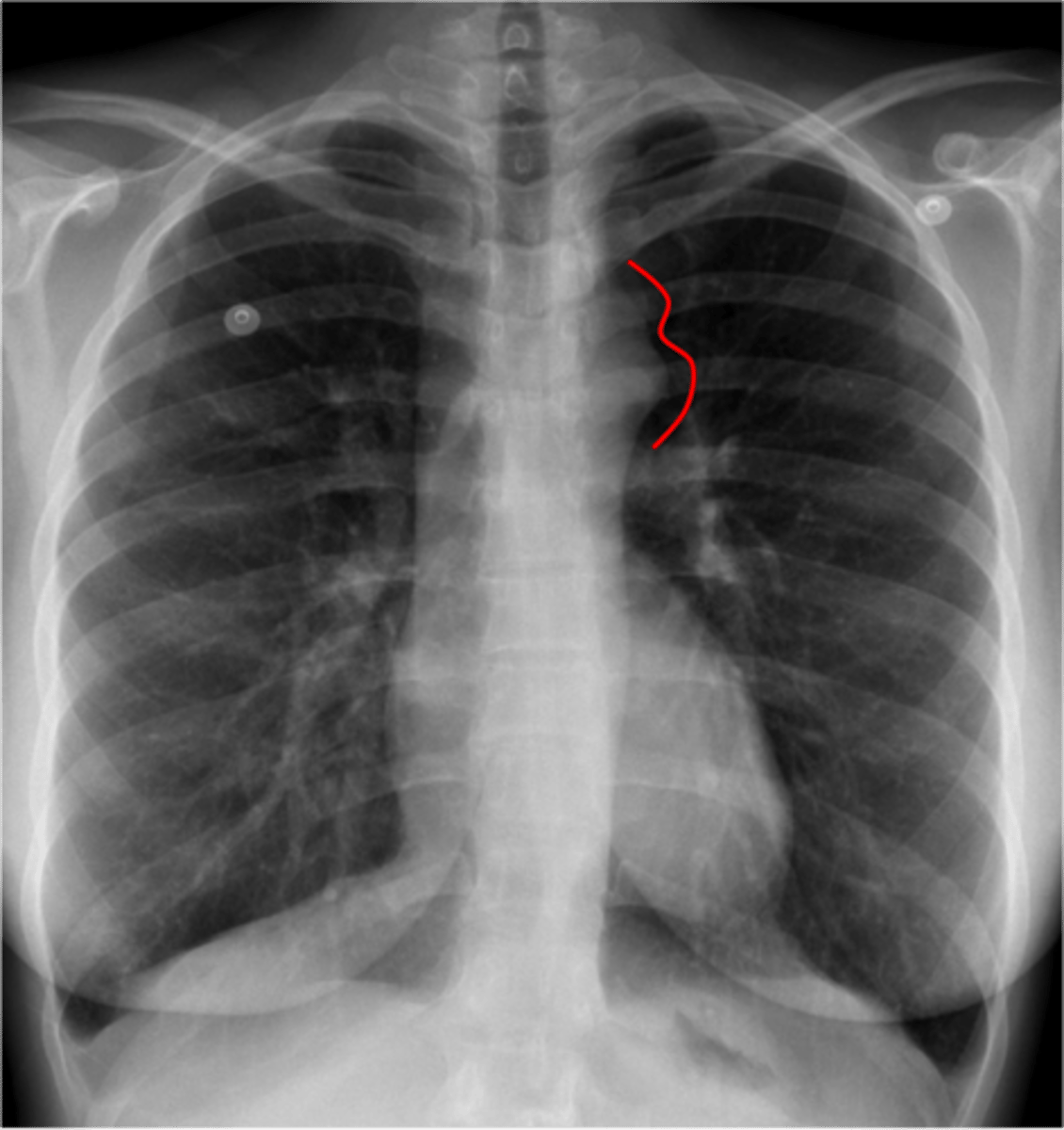
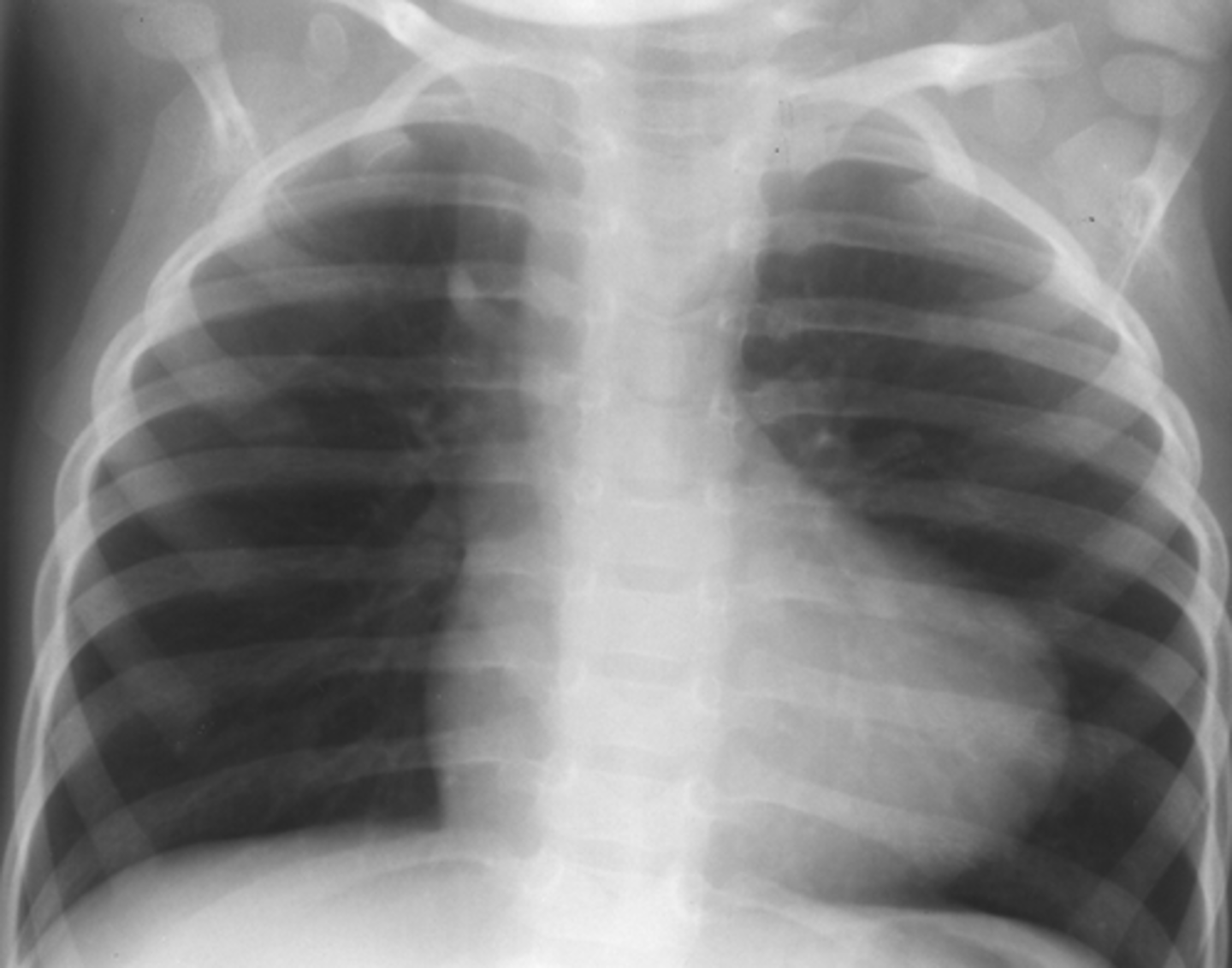
tetralogy of fallot is what type of shunt?
What are the defects
1.
2.
3.
4.
right to left
1. VSD
2. R ventricular hypertrophy
3. overriding aorta
4. pulmonic stenosis (RV outflow obstruction)
(photo: boot-shaped heart)
anti-arrhythmic classes
I
II
III
IV
V
I- Na+ channel blockers (slow conduction velocity)
Ia- procainamide, prolongs repolarization
Ib- lidocaine, shortens repolarization
II- beta blockers (propranolol, metoprolol, esmolol)
III- K+ channel blockers (K+ prevents efflux)
IV- CCB (verapamil, diltiazem)
V- others, adenosine
atropine is first line treatment in _________________
bradycardia
adenosine is used for treatment in ________
tachycardia
causes transient heart block in AV node
class V
amiodarone is used as treatment for ___________
supraventricular arrhythmias (class III)
blocks SA/AV node
EKG: how can we calculate rate
300-150-100-75-60-50
EKG: which lead to look at for atrial enlargement
lead II
left atrial enlargement- "m-shaped" P wave
right atrial enlargement- tall P
how do bundle branch blocks present on EKG
leads V1* and V6
left bundle branch block- downward deflection; deep S in V1...when you turn left, you pull the steering wheel down
right bundle branch block- upward deflection; RsR' in V1...
when you turn right, you pull the steering wheel/turn signal up
epinephrine and norepinephrine are _______ hormones that __________ HR
sympathetic, increase
acetylcholine (secreted by vagus n) is _________ hormone and causes ______ HR
parasympathetic, decereased
note: vagal maneuvers do the same; hold breath, bear down, carotid massage
what is normal sinus rate
60-100 bpm
sinus arrest w/ alterations of paroxysms of atrial tachy and bradyarrhythmias, caused by sinoatrial node disease is called ________________. how is it treated
sick sinus syndrome aka brady-tachy syndrome
permanent pacemaker
EKG: prolonged PR-interval is criteria for _______________
first degree AV block
PR interval > 0.20 sec
describe second degree AV block (mobitz I)
aka wenckebach
increased lengthnening of PR interval with dropped QRS
describe second degree AV block (mobitz II)
constant/prolonged PR interval w/ dropped beat
P waves are not related to QRS in what type of AV block? what is the treatment for this
third degree AV block
permanent pacemaker
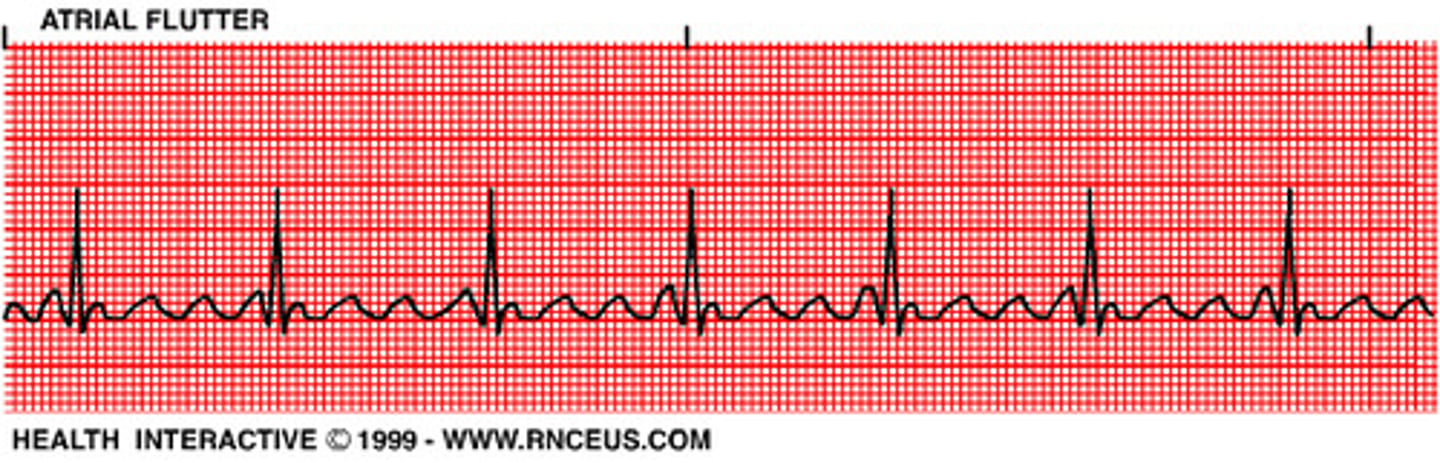
what is the atrial flutter rate and how does it look on EKG
250-350 bpm
note: sawtooth pattern
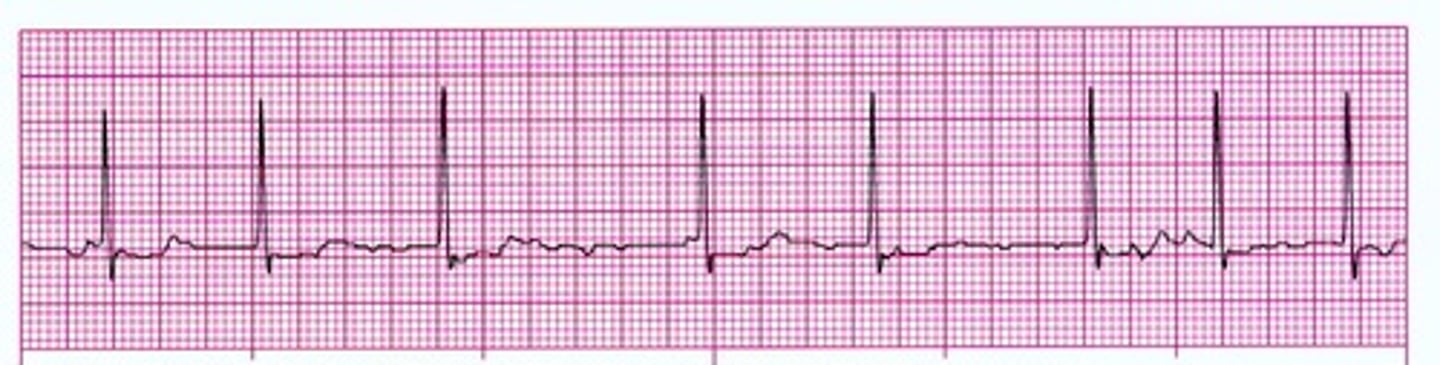
irregularly irregular rhythm defines ______________. What is the treatment
atrial fibrillation
rate vs rhythm control...
rate
-vagal
-CCB
-BB
rhythm
-DC cardioversion
-DCC may also be done after 3-4 weeks of anticoagulation or TEE showing no atrial thrombi
pts w/ atrial fibrillation are on warfarin or aspirin for prophylaxis for ____ based on ____ score
stroke
CHADS2 = CHF, HTN, age > 75 yo, DM, Stroke/TIA
note:
high risk (score > 2)-on warfarin (INR 2.0-3.0)
moderate risk (score 1) -on warfarin or aspirin
low risk (score 0)- none or aspirin
describe wandering atrial pacemaker
> 3 P wave morphologies w/ rate under 100
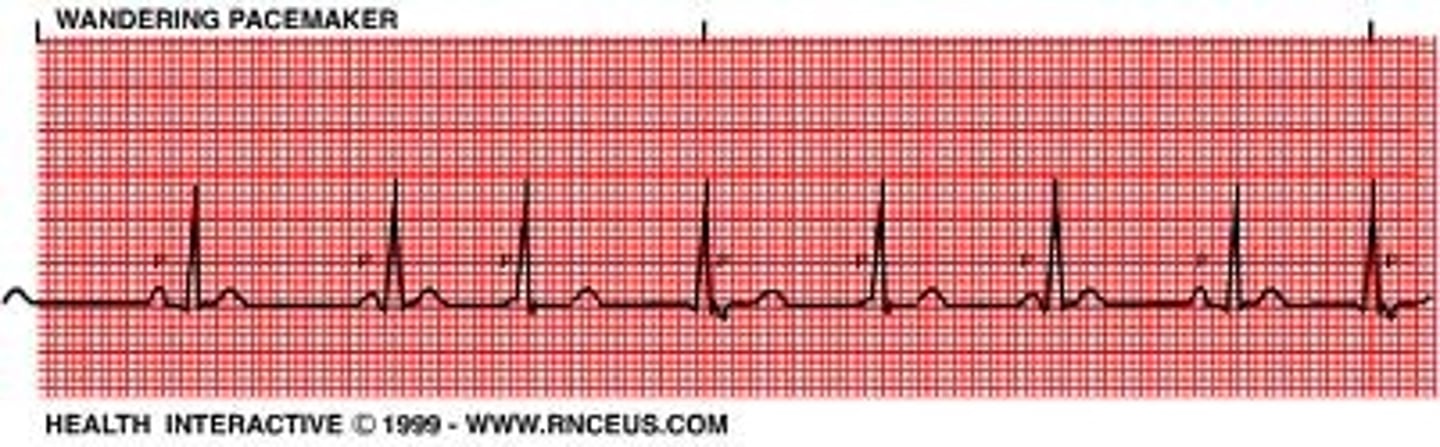
multifocal atrial tachycardia (MAT) is associated with severe ______
COPD
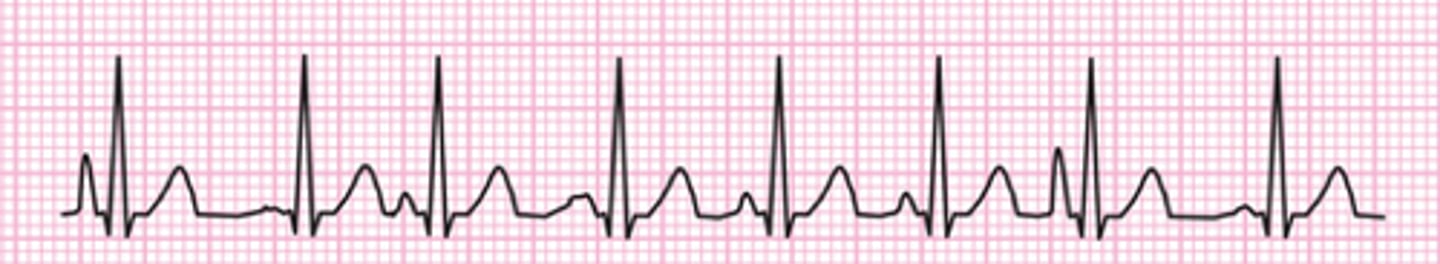
definitive tx for paroxysmal supraventricular tachycardia (PSVT) is _______________
radiofrequency catheter ablation
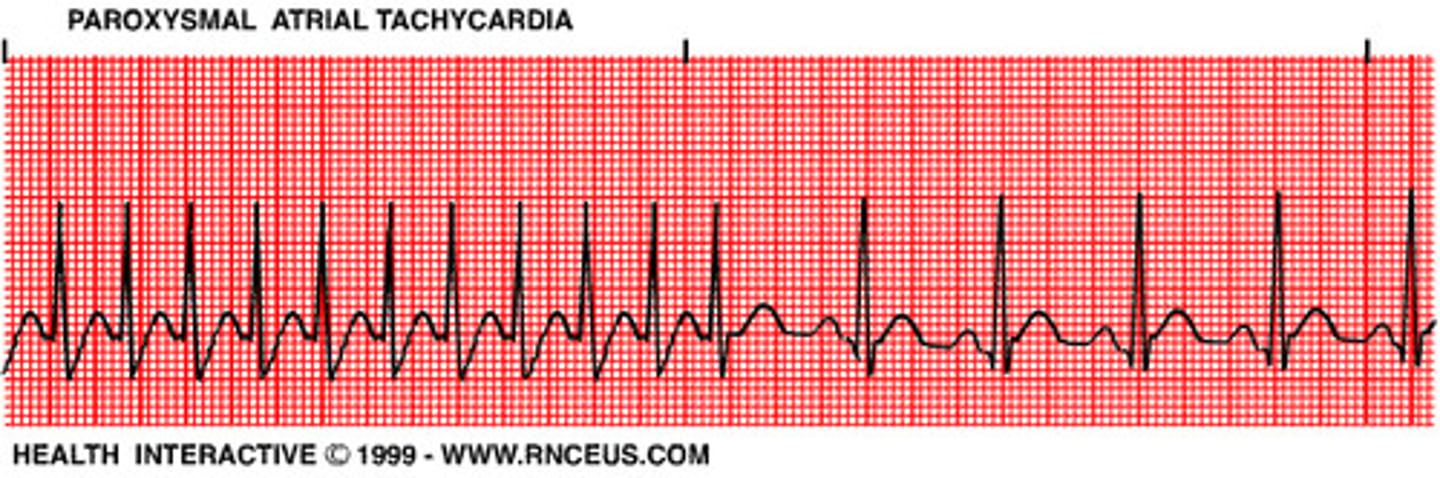
delta wave (slurred QRS upstroke) and a short PR interval is present in ______________. What is the accessory pathway called
wolff-parkinson white
kent bundle
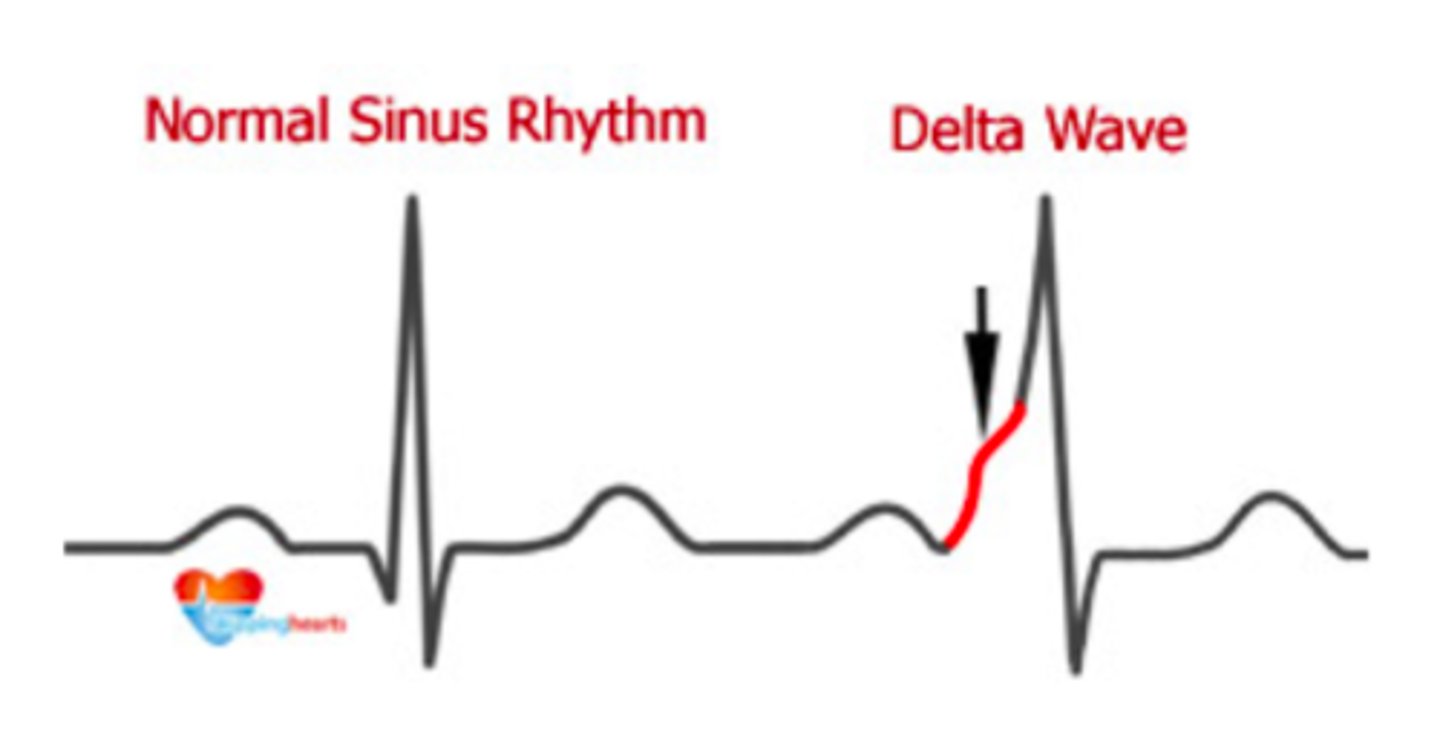
why must we avoid A-V nodal blocking agents in wolff-parkinson white? Sooo then what is the tx
may cause preferential conduction through accessory pathway
vagal maneuvers
antiarrhythmics (ex: procainamide, amiodarone)
radiofrequency ablation *definitive tx
most common rhythm seen with digitalis toxcity
AV junctional dysrhythmia
what is the junctional rhythm rate
40-60 bpm
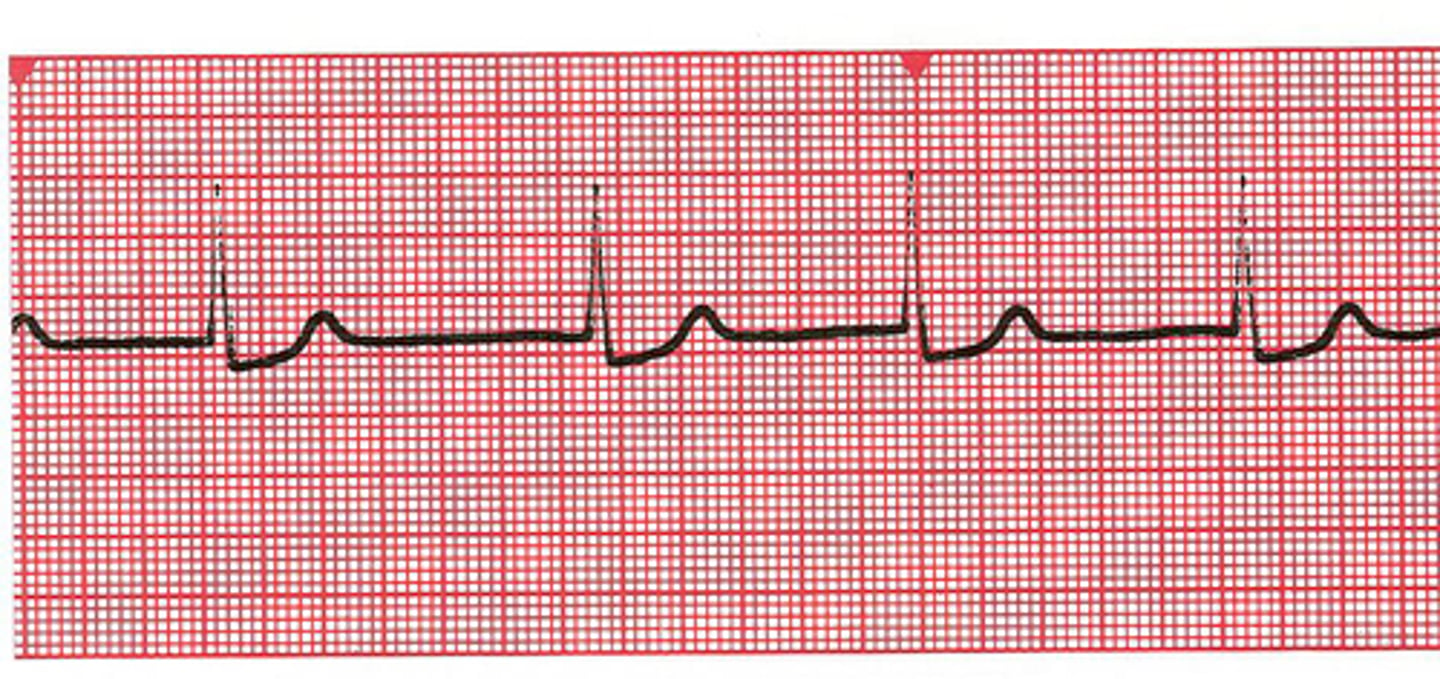
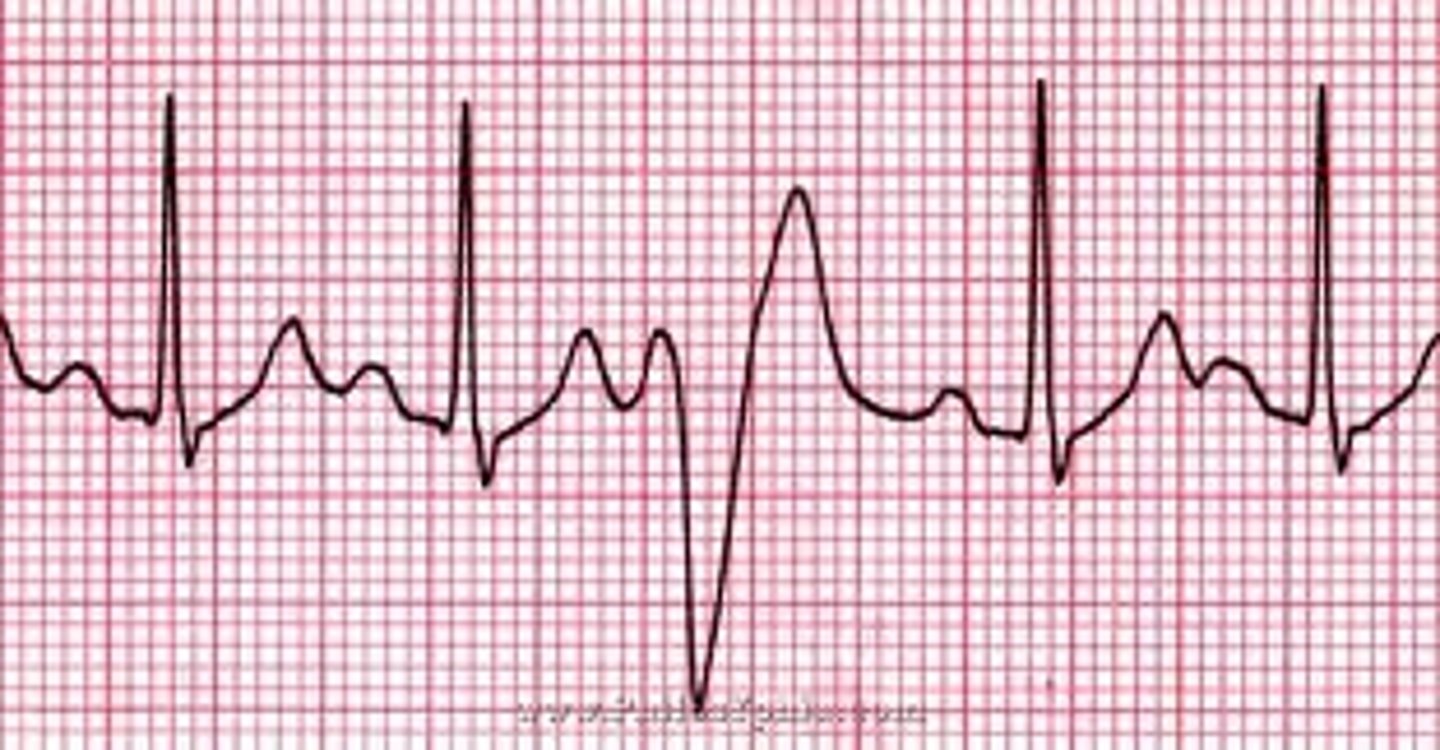
wide, bizarre QRS occurring earlier than expected, usually the T wave is in the opposite direction of the R, associated with compensatory pause. this describes what?
premature ventricular complexes
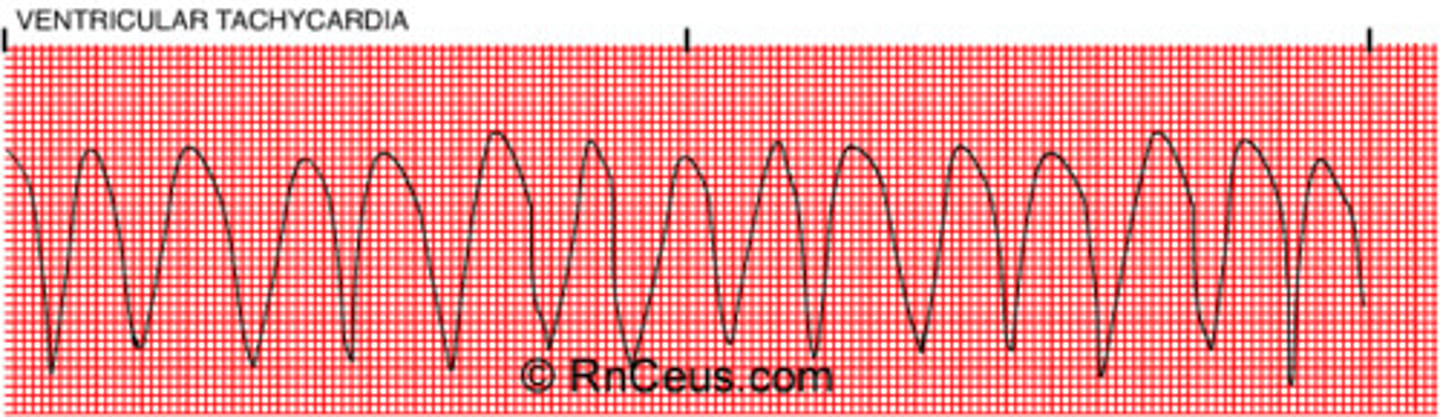
describe ventricular tachycardia
> 3 consecutive PVCs at a rate of > 100 bpm
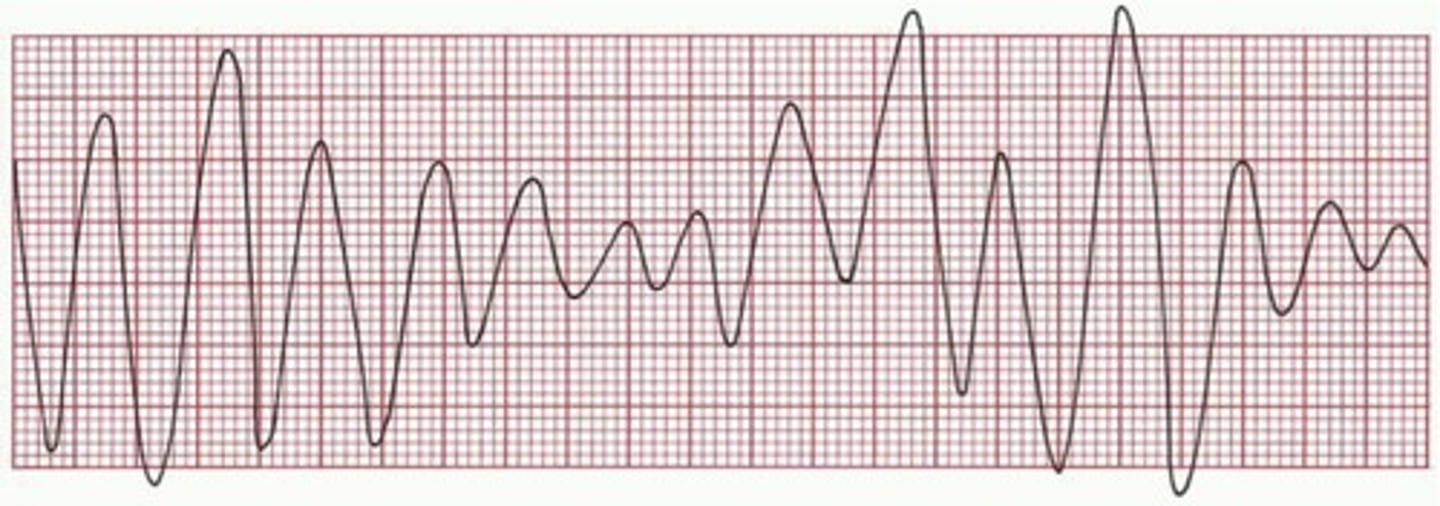
electrolyte status with torsades
hypomagnesium
hypokalemia
what is tx for stable sustained VT
anti-arrhythmics (Amiodarone*, lidocaine, procainamide)
what is treatment for unstable VT with a pulse
synchronized (direct current) cardioversion (DCC)
what is tx for VT withOUT a pulse
defibrillation/CPR (tx as ventricular fibrillation)
tx for torsades de pointes is ____________
IV magnesium
electrical activity that is not coupled with mechanical contraction is called ____________
pulseless electrical activity
note: no mechanical contraction aka no pulse
asystole rhythm (ventricular standstill) Tx
CPR
epinephrine
checks for shockable rhythm q 2 mins
______ leads and _____ (vessel)
II, III, aVF
inferior
right coronary artery
______ leads and _____ (vessel)
V1-V4
anterior
left anterior descending artery
______ leads and _____ (vessel)
I, AVL, V5, V6
lateral
circumflex artery
sokolow-lyon:
S in V1 + R in V5 = 35 mm (men)
S in V1 + R in V5 = 30 mm (women)
criteria for left ventricular hypertrophy
ST depression usually indicates ______________
ischemia
ST depression
horizontal-
upslope-
downslope-
horizontal-pathological
upslope-may be benign
downslope-pathological
ST elevation CONCAVE precordial leads
PR depression seen in the same leads with the ST elevations
no reciprocal changes
acute pericarditis
describe brugada syndrome
right bundle branch syndrome
ST elevation V1, V2, V3 (often downsloping pattern)
T wave inversion in V1, V2
+/- S wave in lateral leads
most common in Asian males
may cause syncope, ventricular fibrillation, sudden cardiac death
prevented by implantable cardiodefribrillator
equation for cardiac output
CO = HR X SV
note: normal physiologic variation....during inspiration, left sided stroke volume decreases
_____-sided murmurs are best heard at end expiration
Left
_____-sided murmurs are best heard at end inspiration
Right
don't use nitrogen and morphine in ____-sided (inferior) myocardial infarction
Right-sided
(because right-sided heart failure is preload dependent and nitrogen and morphine decrease preload via vasodilation)
3 ways renin increases BP
1. increases ACE > increase BP
2. increases ADH > increase H2O > increase BP
3. increases aldosterone > increase sodium > increase BP
note:
ACE = angiotension converting enzymes
ADH = antidiuretic hormone
what makes a positive stress test and what is it most useful for?
ST depressions
exercise-induced hypertension/hypotension
arrhythmias
Sx
abnormalities in heart rate
suspected coronary disease
what is the benefit of radionuclide myocardial perfusion imaging
localize region of ischemia
what drugs used in pharmacologic stress testing
adenosine or dipyridamole
dobutamine (2nd line)
what is gold standard diagnostic test for definitive diagnosis of coronary artery disease/angina
coronary angiography aka "cath"
what is the most useful test to dx heart failure
echocardiogram
what is the primary noninvasive test for assessing cardiac anatomy and fx
transthoracic echocardiogram
(transesophageal echocardiogram is more invasive but better at imaging)
what drugs are used in pharmacologic stress stressing, why are they used, and what are they CI in?
adenosine, dipyridamole
pts unable to exercise to localize area of ischemia
bronchospastic disease
why is a dobutamine stress echo used for
localize area of ischemia in patients that are CI for vasodilators
define coronary artery disease
inadequate tissue perfusion due to imbalance bt decreased coronary blood supply and increased demand
what is MCC of coronary artery disease
atherosclerosis
what are the major risk factors for coronary artery disease
DM, smoking, hyperlipidemia, HTN, male, increased age, FH
what are the 3 phases of formation of atherosclerotic plaque
fatty streak: lipid deposits in WBC
early plaque: LDL is oxidized attracting macrophages/smooth muscle cells to ingest harmful LDL
fibrous plaque: narrowing of arterial lumen and calcification
define myocardial ischemia
narrowing of arterial lumen reduce cardiac blood flow in conditions of increased demand
usually >70% of lumen reduction
define angina and the classes
substernal chest pain brought on by exertion that is poorly localized and relieved with rest/nitro
I: angina w/ only unusually strenuous activity
II: angina w/ more prolonged activity
III: angina w/ daily activity
IV: angina at rest
what is Levine's sign
present in angina

what are the percutaneous transluminal coronary angiography indications
1 or 2 vessels NOT involving main left coronary artery
near/normal left ventricular function
(definitive tx for angina)
coronary artery bypass graft (CABG) indications
left main coronary artery disease
symptomatic 3 vessel disease
left ventricular ejection fraction < 40%
(definitive tx for angina)
nitroglycerin MOA and contraindications
MOA: increase myocardial blood supply and decrease in demand
CI: PDE5 inhibitors, R ventricular MI, SBP<90mmHg
1st line drug for chronic management of stable angina
beta blockers (increase myocardial blood supply and decrease in demand)
note: reduces mortality
____ play a major role in preventing/terminating ischemia induce by coronary vasospasm (Prinzmetal's angina)
calcium channel blockers (increase myocardial blood supply and decrease in demand)
aspirin: MOA
prevents platelet activation/aggregation
(by inhibiting cyclooxygenase)
reduced risk of thrombosis
prevents progression of from chronic stable angina to ACS
what is classic outpatient regimen for angina
aspirin, sublingual nitro, daily B-blocker and statin
who is at risk for a silent MI
women, elderly, diabetics, obese
what defines chronic stable angina?
caused by fixed stenosis (coronary plaque)
relieved by rest/NTG
chronic stable angina Tx
aspirin
beta blocker
statin
PRN sublingual NTG
what makes it unstable angina?
fixed stenosis
negative cardiac enzymes
NOT relieved by rest/NTG
new onset angina
note: > 90% occlusion can cause anginal Sx at rest aka pian at rest indicates 90% blockage!
what defines NSTEMI?
positive cardiac enzymes
no ST elevations on EKG
what defines STEMI
ST elevations >1mm in >2 contd leads + reciprocal leads
new LBBB
most common cause of MI
atherosclerosis
most common causes of coronary artery vasospasm
cocaine
prinzmetal's variant angina
troponin vs CK/CK-MB
troponin
-most sensitive and specific for cardiac ischemia
-appears 4-6 h
-peaks 12-24 h
-returns to baseline 7-10 d
CK/CK-MB
-appears 4-6 h
-peaks 12-24 h
-returns to baseline 3-4 d
what is anti-thrombotic tx in UN/NSTEMI
1. aspirin
2. unfractionated heparin
3. enoxaparin (Lovenox)
4. clopidogrel (Plavix)
5. GP IIb/IIIa inhibitors (eptifibatide, tirofiban, abciximab)
6. Fondaparinux (factor Xa inhibitor)
what is the MOA and indiction for unfractionated heparin
binds and potentiates antithrombin III's ability to inactivate factor Xa , inactivates thrombin
ACS pts w/ EKG changes or + cardiac markers
what is enoxaparin (Lovenox), what is the MOA, and what is the SE
define: low molecular weight heparin
MOA:binds to antithrombin III to inhibit factor Xa
SE: thrombocytopenia
____ is useful in initial tx of acute coronary syndrome in pts with aspirin allergy
clopidogrel (Plavix)
what is adjunctive anti-ischemic therapy in UA or NSTEMI
B blockers: metoprolol
nitrates
morphine
Ca channel blockers
how does morphine contribute to relief of UA or NSTEMI
decreases pain
venodialation to reduce preload
what is the 3 part approach to treatment of STEMI
reperfusion therapy: PCI or thrombolytics (used if PCI unavailable)
antithrombotics
adjunctive therapy
(additional: replinish Mg and K, monitor glucose and bp, reduce risk factors, statin therapy)
(page 28***)
percutaneous coronary intervention is best w/in _____ of sx onset
3hr
describe clot formation
factor Xa converts prothrombin (II) > thrombin (factor IIa)
thrombin activates fibrinogen > fibrin clot