Lecture 3: Reproduction 1 (Meiosis, Sex Determination and Differentiation, Basic Steroidogenesis, Puberty, and Reproductive Capacity, Male Reproductive Structures, Spermatogenesis, Erection, and Ejaculation
1/38
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
39 Terms
how many autosomes and sex chromosomes in sperm?
22 autosomes + X or Y sex chromosome
how many autosomes and sex chromosomes in ovum?
22 autosomes + X sex chromosome
how many autosomes and sex chromosomes in fertilized egg
22 pairs of autosomes and 1 pair of sex chromosomes (male XY, female XX)
how many chromosomes in somatic cells
46 chromosomes (by mitosis)
how many chromosomes in germ cells
23 chromosomes
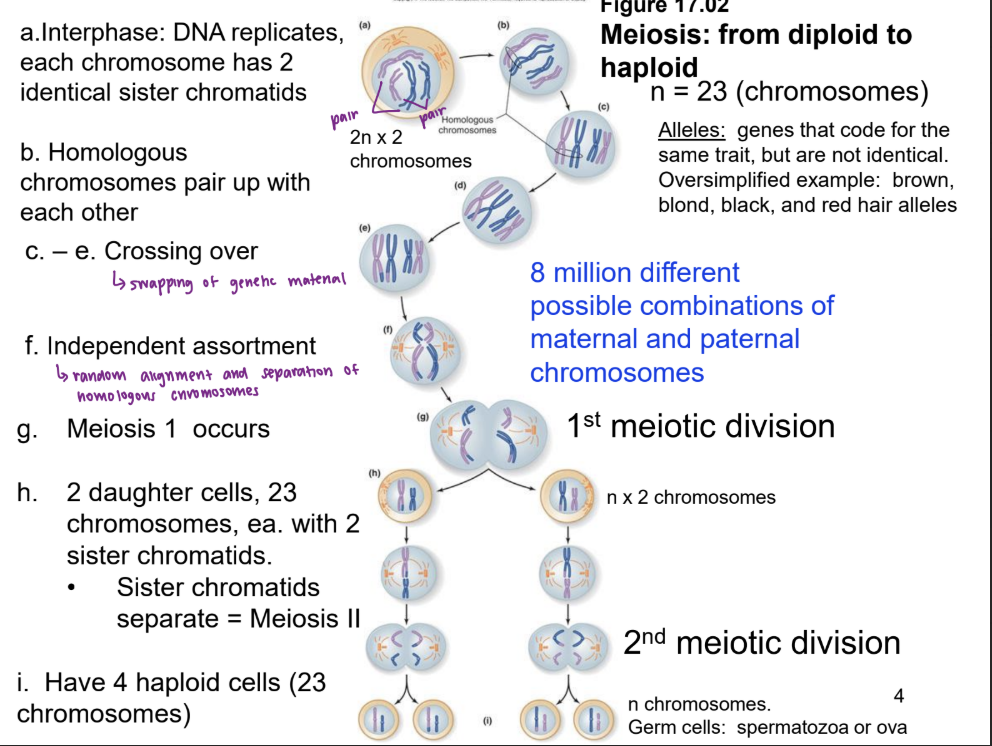
steps of meiosis
interphase: DNA replicates, each chromosome has 2 identical sister chromatids
homologous chromosomes pair up with each other
crossing over occurs (exchange of alleles)
independent assortment (random alignment and separation of homologous chromosomes)
meiosis 1 occurs
2 daughter cells with 23 chromosomes, each chromosome still containing 2 sister chromatids (nx2)
23 chromosomes line up along the equator, and the sister chromatids separate = meiosis II
have 4 haploid cells (n, or 23 chromosomes/cell nucleus)
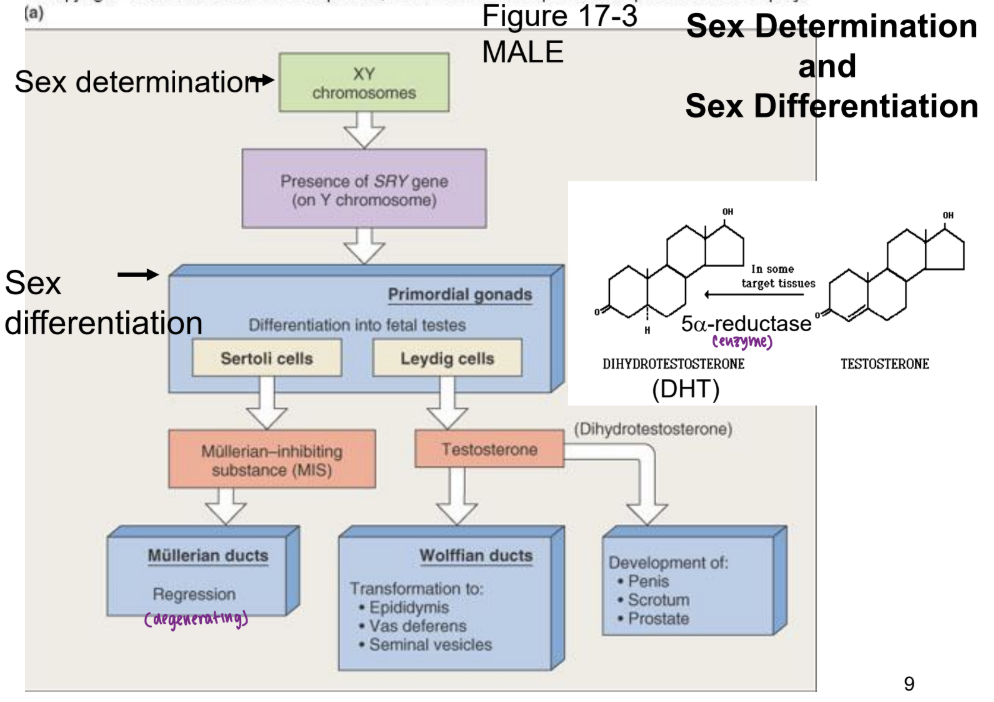
male sex determination
Y chromosome (XY) → SRY gene expression → testes develop
female sex determination
absence of Y chromosome (XX) → no SRY gene → ovary determining (OD) genes expression → ovaries develop
male sex differentiation
sertoli cells → MIS secreted → Mullerian ducts regress → no female internal structures
leydig cells → testosterone → wolffian ducts develop → development of male internal structures
testosterone → 5-alpha-reductase (enzyme) → dihydroxytestosterone (DHT) → development of external male structures
female sex differentiation
no MIS → development of female internal structures
no testosterone → wolffian ducts regress and development of female external genitalia
HPG axis
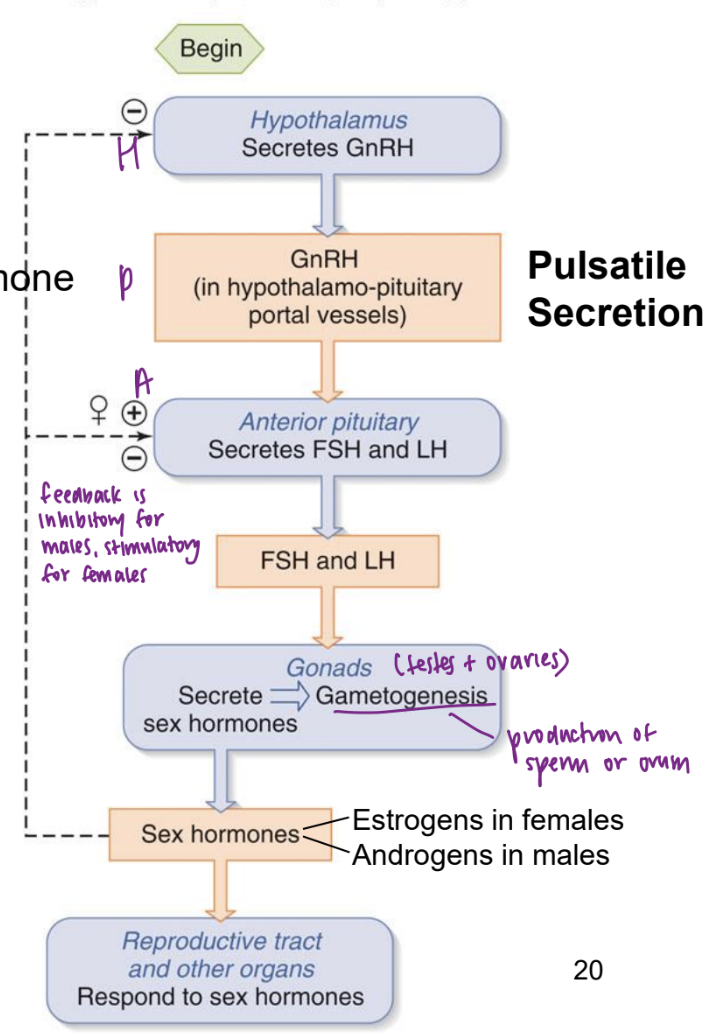
GnRH = gonadotropin releasing hormone
FSH = follicle stimulating hormone
LH = luteinizing hormone
** sex hormones are typically inhibitory at hypothalamus and anterior pituitary. however, estrogens can be stimulatory to anterior pituitary during a particular time of the menstrual cycle.
steroidogenesis
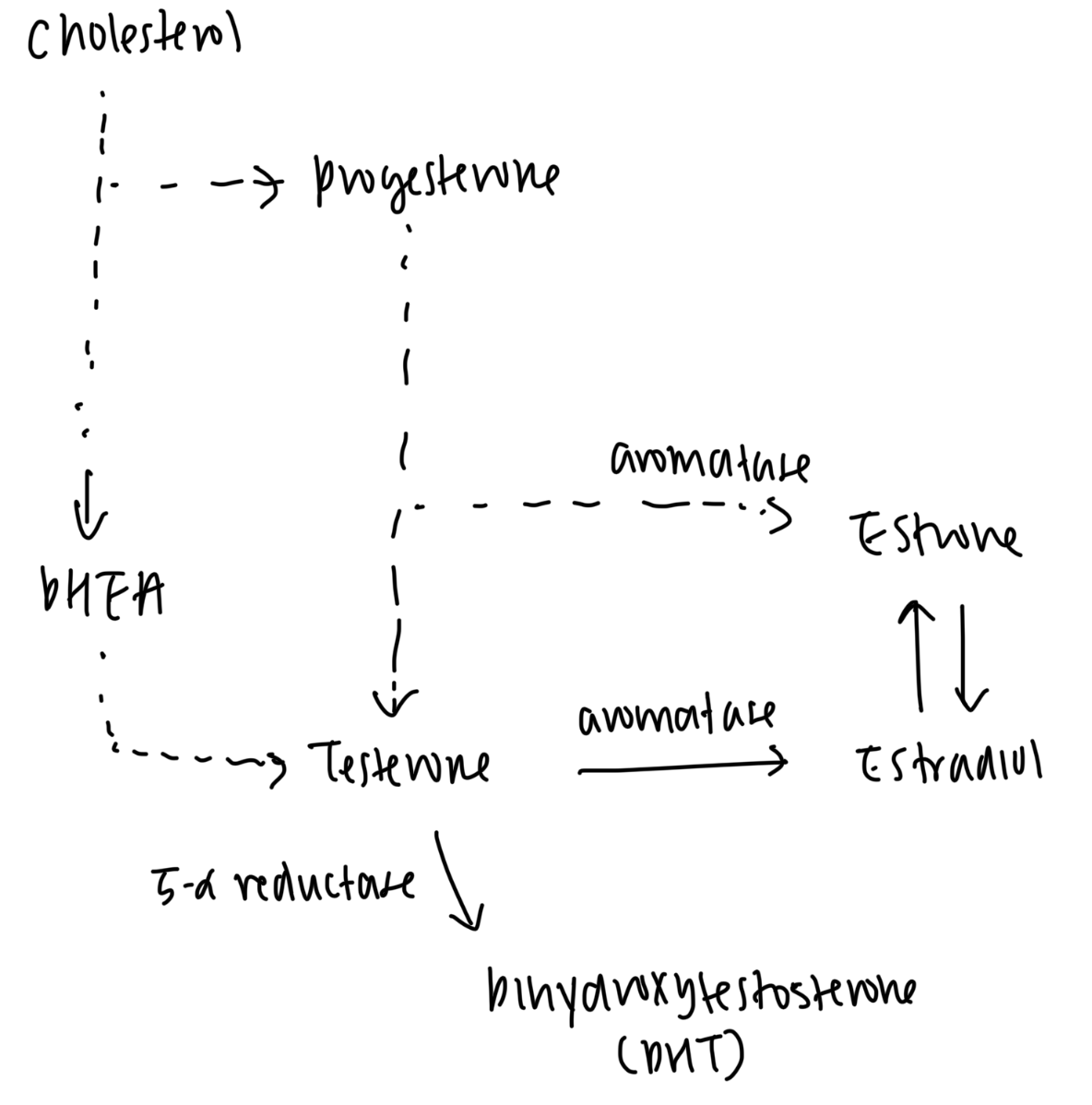
where and when is testosterone produced
males: leydig cells of testes
females: theca cells of ovary in follicular phase, large luteal cells of ovary in luteal phase, and during pregnancy by placenta
DHEA (an androgen) is produced by adrenal gland of males and females → testosterone derived
where and when is estrogen produced
females: granulosa cells of ovary in follicular phase, large luteal cells of ovary in luteal phase, and during early pregancy by large luteal cells and placenta
some male tissues (ex. breast tissue and brain) produce estrogen
DHEA → estrogen
where and when is DHT produced
requires 5alpha-reductase and testosterone
male (in utero): development of penis, scrotum, prostate
male (after puberty): in prostate, also in hair follicles (associated with male pattern baldness)
where and when is progesterone produced
female: large luteal cells in ovary during luteal phase, and placenta during pregnancy
can be converted to testosterone and then estrogens
puberty in female
GnRH secretion increases → FSH and LH secretion increases → estrogen secretion increases
puberty in males
increased GnRH secretion → increased LH and FSH → stimulates seminiferous tubules and testosterone secretion
why is pulsatile pattern in GnRH release important
continuous GnRH → LH and FSH desensitize
pulsitate GnRH → LH and FSH constant
male reproductive capacity
continuously active after puberty
reproduce at least into their 70s and 80s, possibly longer
female reproductive capacity
a single oocyte is released per 28 day cycle
after ovulation, egg remains viable for 24-48 hours
menopause occurs around age 50 and females lose reproductive capacity
testis
(located in scrotum) — where sperm is produced and stored
epididymis
where sperm matures.
vas deferens
where sperm travels during ejaculation
semniferous tubules
primary site of spermatogenesis in testes
leydig cells
secrete testosterone
role of sertoli cells in spermatogenesis
transports androgen binding protein which binds and transports testosterone from Leydig to Sertoli cells where it can be released to bathe the developing sperm
generate other secretions that nourish and guide sperm development
phagocytize defective sperm
circualting androgens can be converted to
DHT by 5alpha-reductase (particularly important in utero for metal development of male external genitalia)
beta-estradiol by aromatase in some tissues (like adipose, liver, testes, and brain)
steps of spermatogenesis
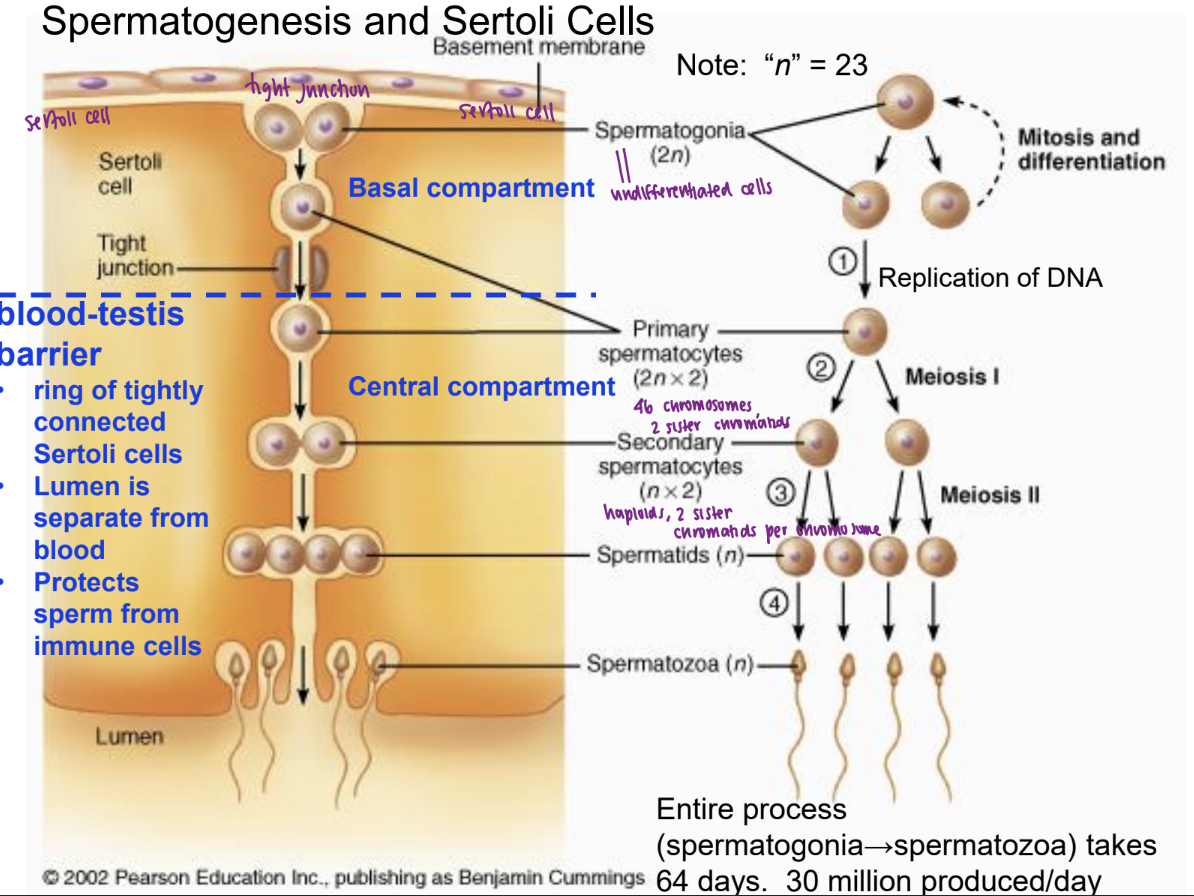
primary spermatocytes is produced by
spermatogonia during and after puberty due to FSH and LH actions
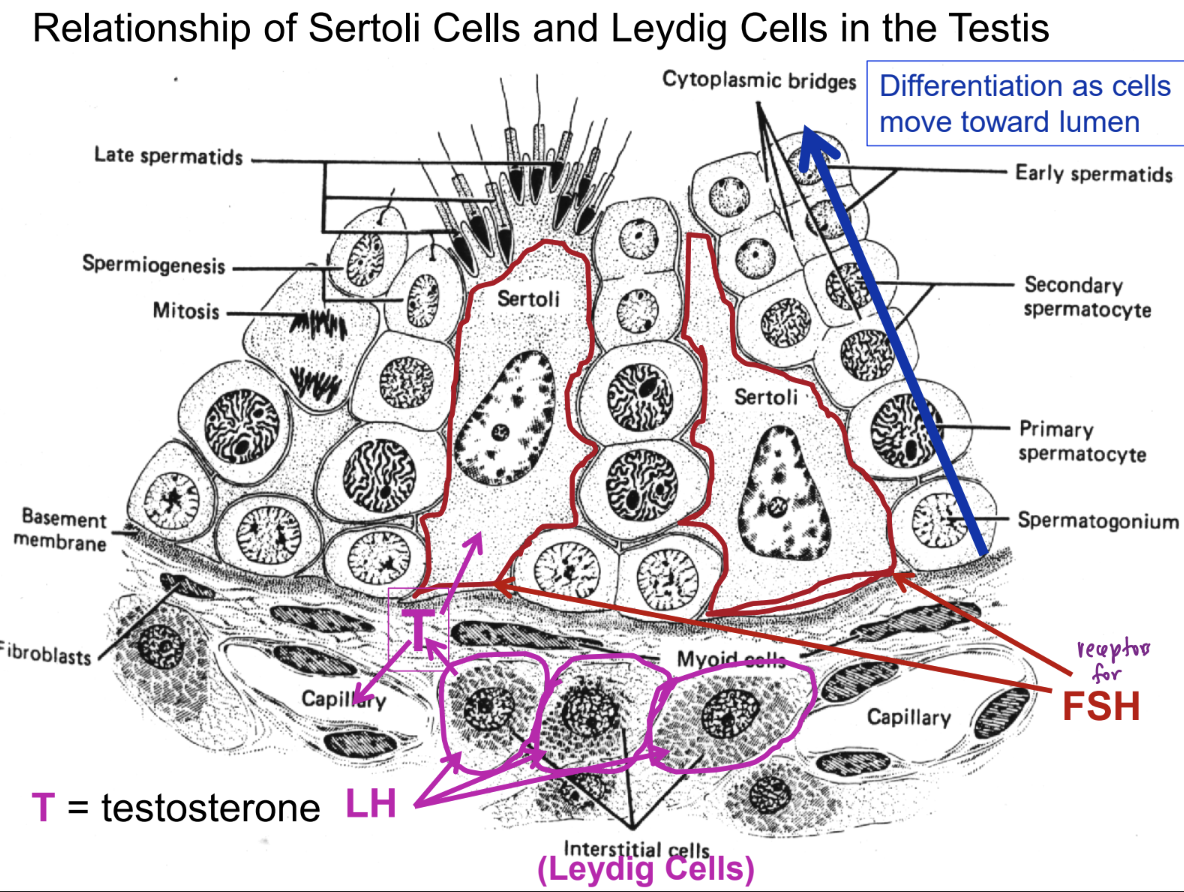
relationship of sertoli cells and leydig cells in testis
LH stimulates Leydig cells → produce testosterone
FSH stimulates sertoli cells + testosterone from leydig cells move into sertoli cells → support spermatogenesis
differentiation as cells move toward the lumen
mechanism of erection
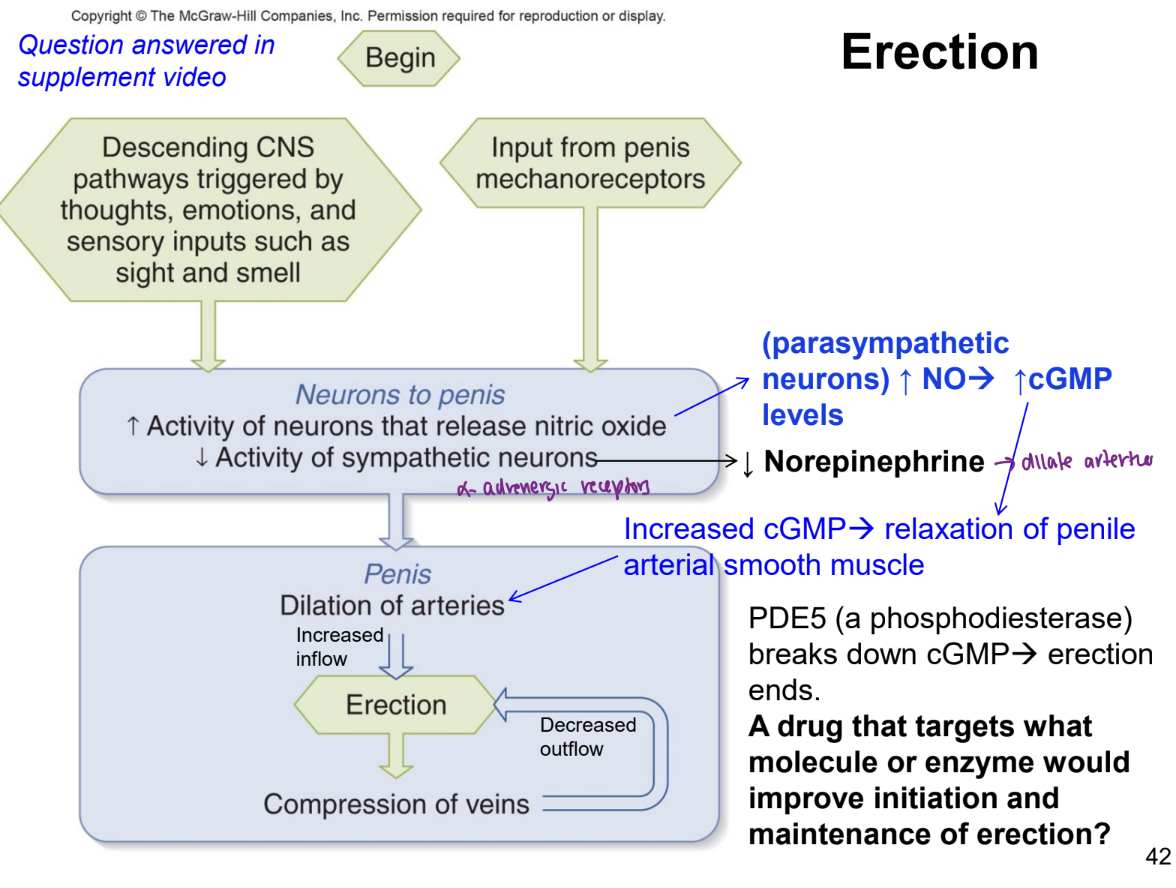
A drug that targets what molecule or enzyme would improve initiation and maintenance of erection?
PDE5 inhibitors (ex. Viagra, Levitra, Cialis) cause maintained elevation in cGMP
PDE5 (a phosphodiesterase) breaks down cGMP → erection ends.
ejaculation mechanism
increased sympathetic activity
strong contractions of epididymis, vas deferens, ejaculatory ducts, prostate, and seminal vesicles
increased secretion of fluids by seminal vesicles and prostate
emission: sperm and semen move to urethra
ejaculation: expulsion of sperm and semen via rapid contractions of urethral smooth muscle and skeletal muscle at base of penis
urethral sphincter at bladder closes so that urine doesn’t mix with semen and so that sperm doesn’t enter the bladder
Explain why there is decreased functioning of the reproductive tract (decreased fertility) with anabolic steroid use?
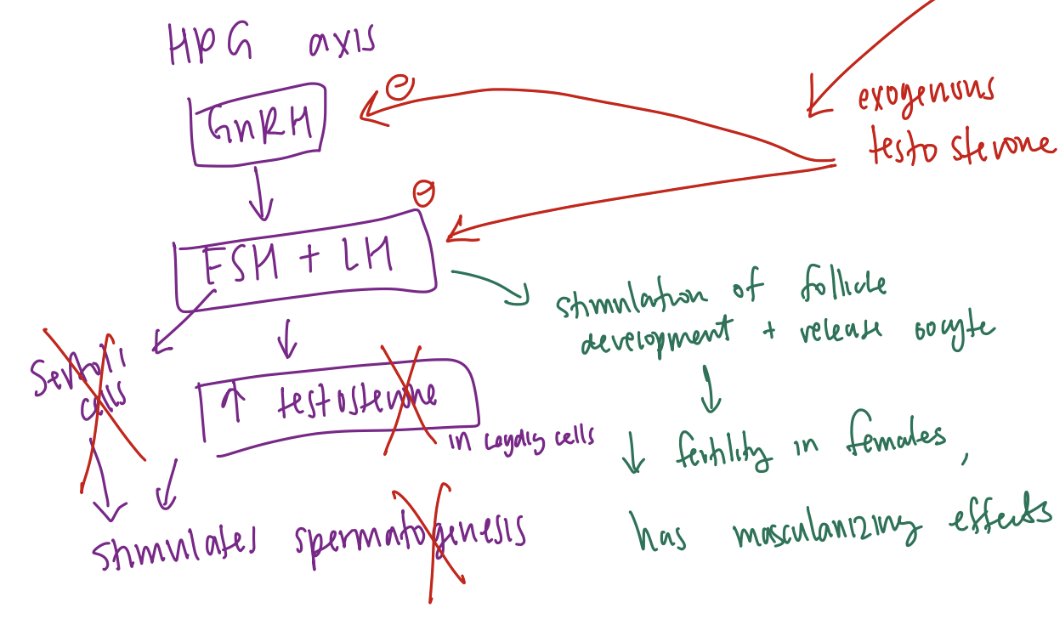
Increased plasma testosterone→
Decreases GnRH and LH directly →Decreased testosterone production by Leydig cells
Decreases FSH indirectly via decreased GnRH→ in combination with the decreased local [testosterone] in the testes →decreased Sertoli cell function→
Decreased spermatogenesis and decreased fertility
In females: decreased GnRH and LH and FSH also occurs, which decreases female fertility as well, plus high circulating testosterone has masculinizing effects.
prostate fluid secretion
30% seminal fluid
vas deferens fluid secretion
10% seminal fluid
seminal vesicles fluid secretion
60% seminal fluid
bulbourethral gland fluid secretion
lubricating mucus