Challenge Test 2
1/199
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
200 Terms
The amount of radiation deposited per unit length of tissue traversed by incoming photons is called:
a. Tissue exposure
b. Linear deposition of energy
c. Linear energy transfer
d. Effective dose limit
C. More energy is deposited by particulate forms of radiation than by waveforms of radiation.
Cataractogenesis, life span shortening, embryologic effects, and carcinogenesis are examples of:
a. Short-term somatic effects
b. Genetic effects
c. Acute radiation syndrome
d. Long-term somatic effects
D. All are examples of radiation effects on the individual being exposed.
Compton interaction:
a. Increases contrast in the radiographic image
b. Results in scattering of the incident electrons
c. Decreases recorded detail in the radiographic
image
d. Decreases contrast in the radiographic image
D. Choice A is incorrect because photoelectric interaction produces contrast.
Grayt multiplied by a radiation weighting factor equals:
a. Air kerma
b. Becquerel
c. Sievert
d. Gray(a)
C.
Effective dose limit (EfD):
a. Is the level of radiation that an organism can receive and probably sustain no appreciable effects
b. Is a safe level of radiation that can be received with no effects
c. Should be absorbed annually to maintain proper immunity to radiation
d. Is 500 mSv per year for the general public
A. Choice B is incorrect because no level of radiation is considered completely safe. Choice C is incorrect because no such immunity has been proved. Choice D is incorrect because the effective dose limit for the gen- eral public is 5 mSv per year.
Radiation with a high LET:
a. Has low ionization
b. Is highly ionizing
c. Carries a low quality factor
d. Equates with a low RBE
B. High-LET radiation is depositing a lot of energy in the tissues, causing much ionization.
Radiation protection is based on which doseresponse relationship?
a. Linear-threshold
b. Nonlinear-nonthreshold
c. Linear-nonthreshold
d. Nonlinear-threshold
C. It is assumed that for every dose of radiation, a response occurs in the atoms of the person being irradiated.
Which of the following states that the radiosensitivity of cells is directly proportional to their reproductive activity and inversely proportional to their degree of differentiation?
a. Inverse square law
b. Law of Bergonié and Tribondeau
c. Reciprocity law
d. Ohm's law
B. Cells such as epithelial, ovarian, and sperm cells.
Which of the following causes about 95% of the cellular response to radiation?
a. Direct effect
b. Law of Bergonié and Tribondeau
c. Target theory
d. Indirect effect
D. Because the cellular cytoplasm is substantially larger than the cellular nucleus, it is more likely to be struck by incoming x-ray photons. Thus, most of the cellular response to radiation is indirect. The direct effect results from x-ray photons directly striking the cellular
nucleus.
When radiation strikes DNA, which of the following occurs?
a. Direct effect
b. Law of Bergonié and Tribondeau
c. Target theory
d. Indirect effect
A. Indirect effect occurs when radiation strikes the cytoplasm of the cell. Target theory states there is a master molecule that governs cellular activities (i.e., DNA).
The amount of radiation that causes the number of genetic mutations in a population to double is called the:
a. Threshold dose
b. Doubling dose
c. Mutagenic dose
d. Genetic dose
B.
The SI units of equivalent dose, activity, air kerma, and absorbed dose are, respectively:
a. Roentgen, rad, rem, curie
b. Rad, coulomb per kilogram, curie, becquerel
c. Rem, curie, roentgen, rad
d. Sievert, becquerel, gray(a), gray(t)
D. Be sure to review the units of radiation measurement.
Medical x-rays are an example of:
a. Natural background radiation
b. Artificially produced radiation
c. Nonionizing radiation
d. Ionizing, natural background radiation
B. This is human-produced radiation.
The effective dose limit for a fetus for the entire gestational period is:
a. 5.0 mSv
b. 0.5 mSv
c. 0.05 mSv
d. 50 mSv
A.
The photoelectric effect:
a. Results in absorption of the incident photon
b. Results in absorption of the incident electron
c. Produces contrast fog on the radiographic image
d. Is the same as brems radiation
A.
The annual effective dose limit for radiographers is:
a. 10 mSv
b. 100 mSv
c. 50 mSv
d. 100 mSv
C. Be sure to get the amount and unit of measurement correct!
The average dose to active bone marrow as an indicator of somatic effects on a population is called:
a. Doubling dose
b. Bone dose
c. GSD
d. Mean marrow dose
D. This is the definition of mean marrow dose (MMD). It is not called the bone dose. The doubling dose is the amount of radiation that causes the number of mutations in a population to double. The GSD is the genetically significant dose.
An early tissue reaction that may occur during prolonged interventional procedures is:
a. Interruption of mitosis
b. Sterility
c. Erythema
d. Early cataract formation
C.
A lead apron of at least what thickness should be worn while being exposed to scatter radiation?
a. 0.25-mm Pb equivalent
b. 0.50-mm Pb equivalent
c. 0.50-mm Al equivalent
d. 0.10-mm Al equivalent
B. Shielding of lead (Pb) equivalent, not aluminum (Al) equivalent, is used to protect from scatter radiation. The requirement for a lead apron is at least 0.25-mm Pb equivalent; 0.5-mm Pb equivalent should be worn, which is what the question asks. There is a difference between "shall" and "should."
Use of a thyroid shield of at least what thickness should be used for fluoroscopy?
a. 0.10-mm Pb equivalent
b. 0.50-mm Pb equivalent
c. 0.50-mm Al equivalent
d. 0.10-mm Al equivalent
B. The requirement for a thyroid shield, if used, during fluoroscopy is 0.5-mm lead, not aluminum, equivalent.
How thick are primary protective barriers?
a. 1⁄32-inch lead equivalent
b. 1⁄16-inch aluminum equivalent
c. 1⁄32-inch concrete
d. 1⁄16-inch lead equivalent
D. Primary protective barriers consist of 1/16-inch lead equivalent, not aluminum equivalent. Secondary protective barriers consist of 1/32-inch lead equivalent.
Primary protective barriers, if in the wall, must extend to a height of at least:
a. 5 feet
b. 6 feet
c. 7 feet
d. 10 feet
C. Primary protective barriers in the wall must extend to a height of at least 7 feet because this height is taller than most people.
Secondary protective barriers must extend to a height of:
a. 5 feet
b. 6 feet
c. The ceiling
d. 10 feet
C. The secondary protective barrier extends from where the primary protective barrier ends to the ceiling with a 1⁄2-inch overlap.
The protective curtain hanging from the fluoroscopy tower must be at least:
a. 0.50-mm Pb equivalent
b. 0.25-mm Al equivalent
c. 0.10-mm Pb equivalent
d. 0.25-mm Pb equivalent
D. The protective curtain hanging from the fluoroscopy tower must be at least 0.25-mm Pb, not Al, equivalent. Be sure to remember all the shielding requirements.
The Bucky slot cover must be at least:
a. 0.50-mm Pb equivalent
b. 0.25-mm Al equivalent
c. 0.10-mm Pb equivalent
d. 0.25-mm Pb equivalent
D. Be sure to remember all the shielding requirements.
Thermoluminescent dosimeters use what type of crystals to record dose?
a. Dilithium crystals
b. Lithium fluoride
c. Flux capacitors
d. Bromide crystals
B. Lithium fluoride crystals, which release energy as visible light when heated, are used to record dose in TLDs.
TLDs are heated and release what type of energy to indicate dose?
a. Laser
b. Visible light
c. X-rays
d. Gamma rays
B. TLDs are heated and release visible light energy to indicate dose. This energy is read by a photomultiplier tube.
Optically stimulated luminescence (OSL) dosimeters provide readings as low as:
a. 1μSv
b. 10 μSv
c. 50 μSv
d. 100 μSv
B. OSL dosimeters are very sensitive. This feature, along with their wide dynamic range, greater accuracy, and long-term stability, makes them ideal for personnel monitoring.
The recording material in an OSL dosimeter is:
a. Dilithium
b. Lithium fluoride
c. Aluminum oxide
d. Silver halide
C. The recording material in an OSL dosimeter is aluminum oxide, which is then scanned by a laser beam. Film badges use film as the recording material; TLDs use lithium fluoride.
The energy stored in an OSL dosimeter is released when the dosimeter is exposed to:
a. Heat
b. White light
c. Laser
d. Ultrasound
C. The energy stored in an OSL dosimeter is released by exposure to a laser. The energy is then released as visible light. The energy stored in a TLD is released by heat.
OSL dosimeters may be worn for up to:
a. 1 month
b. 1 week
c. 3 months
d. 1 year
C. OSL dosimeters can be worn for up to a quarter, although in many cases they may be changed monthly.
OSL dosimeters may be scanned and reanalyzed:
a. Only once
b. Monthly
c. Five times
d. An unlimited number of times
D. One of the key advantages of OSL dosimeters is the capability of reanalysis for confirmation of dose, which is especially important if a dose is in question.
For optimal radiation protection, what type of exposure technique should be used?
a. Low kVp, high mAs
b. Small focal spot
c. All manual technique
d. High kVp, low mAs
D. Low mAs reduce the amount of radiation striking the patient. Choosing the optimum kVp for the part being radiographed increases the quality of the x-ray beam. Low kVp, high mAs would result in the opposite.
For optimal radiation protection of the radiographer performing mobile radiography, what should always be done? (Select 2)
a. Use the 6 foot exposure switch cord to its maximum length
b. Stand at a 25-degree angle from the patient
c. Stand at a 45-degree angle from the portable machine
d. Wear a lead apron
A, D.
The minimum source-to-skin distance for portable radiography is:
a. At least 12 inches
b. At least 15 inches
c. At least 72 inches
d. At least 40 inches
A. Be sure to review the source-to-skin distance requirements.
How often is added filtration adjusted by the radiographer?
a. After several exposures
b. Daily
c. As part of weekly quality control
d. Never
D. Added filtration is adjusted by a medical radiation physicist, not by the radiographer. Compensating filtration devices, such as wedge filters, are manipulated by the radiographer.
What report does a radiographer consult and initial to verify occupational dose received?
a. PACS
b. Dosimeter
c. Radiation
d. Annual dose report
B.
What are radiation effects that manifest themselves in the person being irradiated?
a. Genetic
b. Exposed cell
c. Somatic
d. Molecular
C. Radiation effects manifested in the next generation are called genetic effects.
What type of background radiation is radon?
a. Man-made
b. Radioactive water
c. Natural
d. Natural form of electromagnetic waves
C. Radon is present in the environment as a gas, frequently found in the basements of older homes.
The photoelectric effect is responsible for:
a. The brightness of the image
b. Producing scatter radiation
c. Differential absorption of the x-ray beam by the body
d. Spatial resolution
C. As a result of differential absorption of the beam, photoelectric effect produces contrast on the image.
The unit of measurement that is determined by measuring ions produced in air as radiation passes through it is the:
a. Becquerel
b. Gray
c. Air kerma
d. Sievert
C. Air kerma has replaced coulombs per kilogram.
One (1) is the radiation weighting factor (WR) for:
a. Neutrons
b. Gamma rays
c. Cosmic rays
d. Radon
B. WR is used to modify the absorbed dose amount to account for greater damage caused by high-LET radiations. Gamma rays have lower LET so the WR is only 1.
Atomic number is represented by the letter:
a.M
b.A
c.Z
d.Q
C.
Atomic mass is represented by the letter:
a.M
b.A
c.Z
d.Q
B.
The primary purpose of filtering the x-ray beam is to:
a. Increase contrast
b. Improve radiation protection
c. Soften the beam for proper imaging
d. Remove short-wavelength rays
B. Filters reduce the number of "soft" rays striking the patient, lowering skin dose.
Considering probability, x-ray photons will probably strike:
a. The nucleus
b. RNA
c. DNA
d. Water
D. The cytoplasm is larger than the nucleus.
X-ray photons depositing their energy in the water of the cytoplasm may cause:
a. Electrolysis
b. Radiolysis
c. Radioactivity
d. Pair production
B.
Free radicals may recombine to form:
a. DNA
b. Hydrogen peroxide
c. Sulfuric acid
d. New cytoplasm
B.
What is the thickness of a thyroid shield that may be worn during fluoroscopy?
a. 0.10-mm lead equivalent
b. 0.50-mm lead equivalent
c. 0.50-mm aluminum equivalent
d. 0.10-mm aluminum equivalent
B.
For shielding purposes, what is the x-ray control booth considered?
a. Secondary protective barrier
b. Primary protective barrier
c. Equivalent to a lead apron
d. A tertiary protective barrier
A.
An ionization chamber circuit places:
a. A photomultiplier tube between the IR and the patient
b. An ionization chamber beneath or behind the IR
c. An ionization chamber between the patient and the x-ray tube
d. An ionization chamber between the IR and the patient
D.
Full-wave rectification uses:
a. A single semiconductor
b. Four silicone-based semiconductors
c. The x-ray tube as a semiconductor
d. Four silicon-based semiconductors
D. Answer B is incorrect because of "silicone," which is not the same substance used in rectifiers.
A full-wave rectified, three-phase, 12-pulse x-ray machine produces approximately ____% more average pho- ton energy than a full-wave rectified, single-phase x-ray machine.
a. 35
b. 50
c. 41
d. 100
C.
According to the anode heel effect, the intensity of radiation is greater at the _______ side of the x-ray tube.
a. Anode
b. Central x-ray
c. Neither side; the beam is of uniform intensity
d. Cathode
D.
The amount of time needed for an AEC to terminate the exposure is called:
a. Exposure latitude
b. Minimum reaction time
c. Chamber response time
d. Electronic time
B.
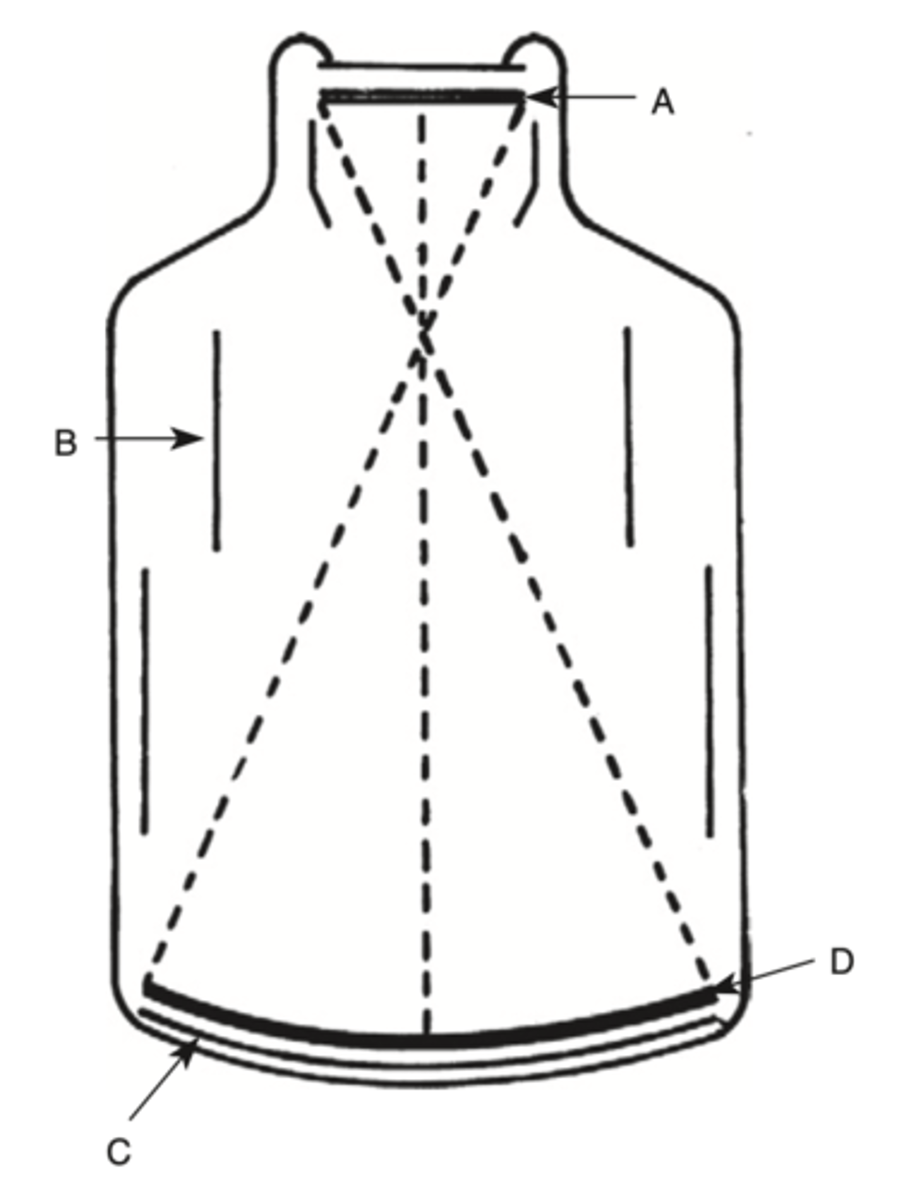
Where is the electron beam focused?
a. A
b. B
c. C
d. D
B.
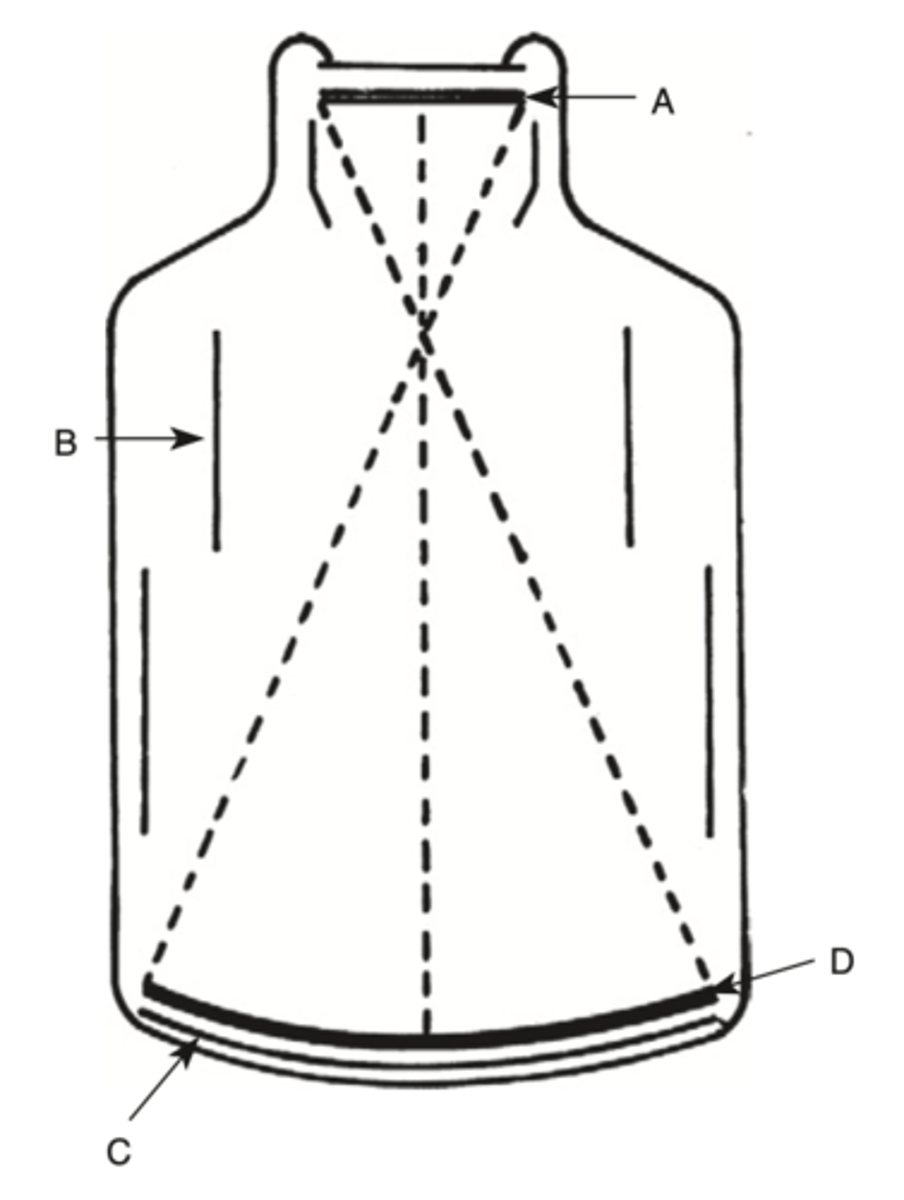
Where is light energy converted to electrons?
a. A
b. B
c. C
d. D
D.
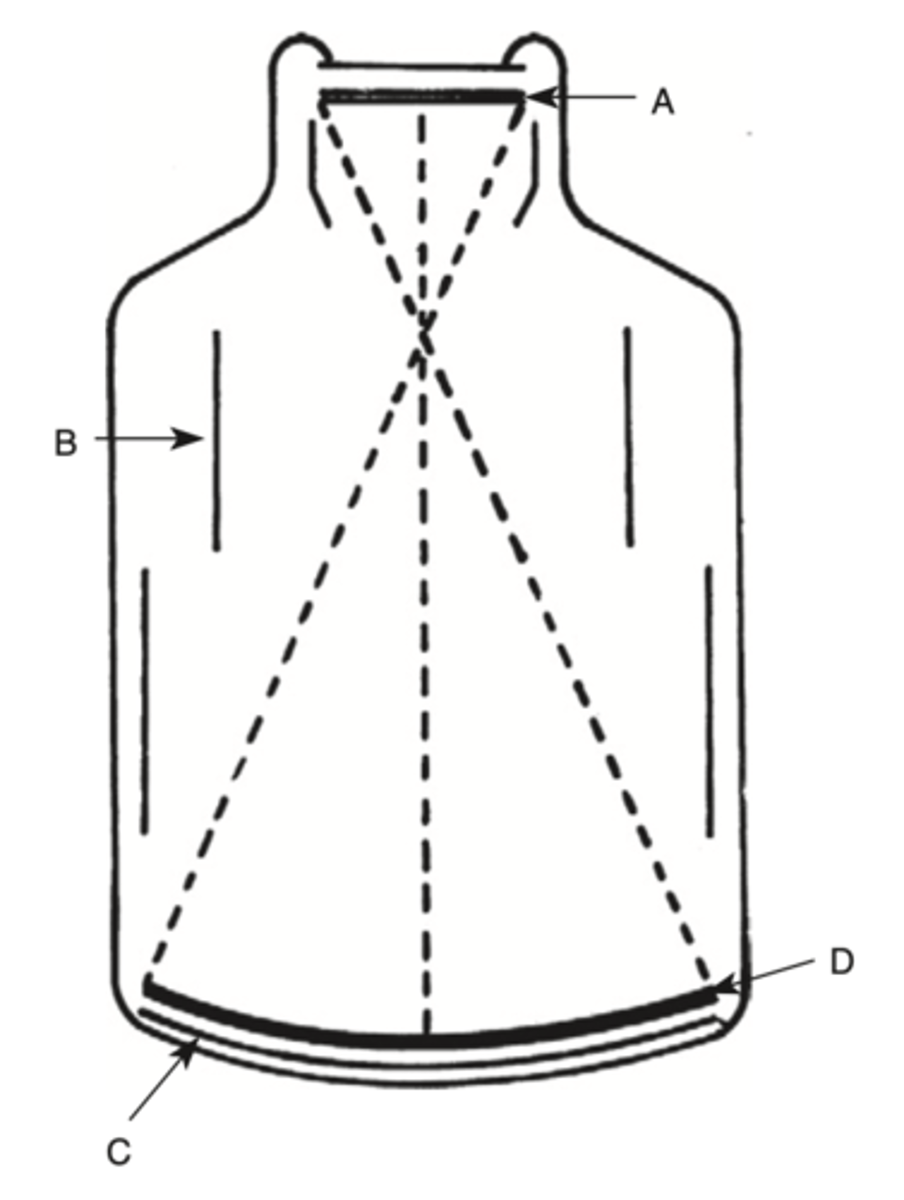
From where is the visible image distributed to viewing or recording media?
a. A
b. B
c. C
d. D
A.
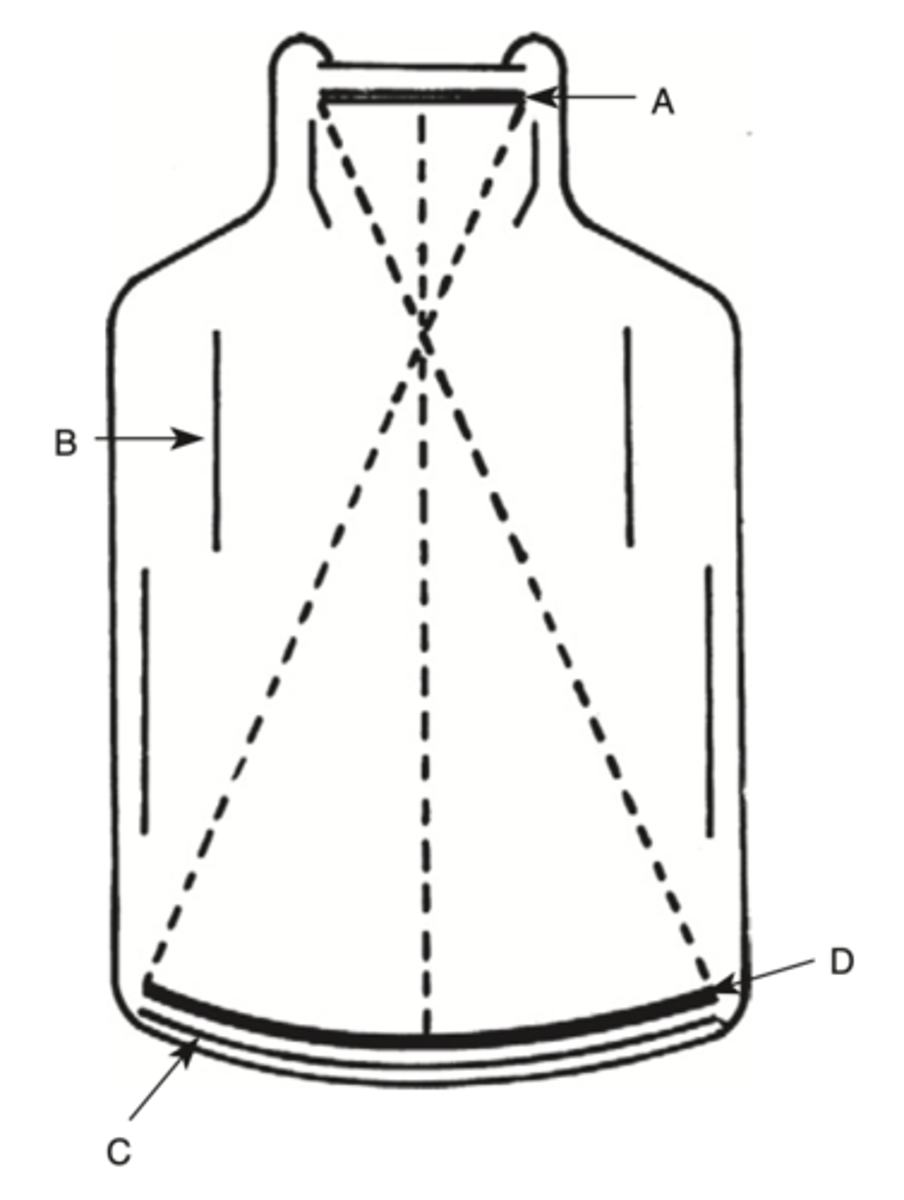
Where is x-ray energy converted to visible light?
a. A
b. B
c. C
d. D
C.
A particular x-ray room is "shooting dark." The problem arises when a change is made from 200 to 300mA using fixed kVp techniques at 0.16seconds. Which of the following would lead to an accurate diagnosis of the problem?
a. Resolution test pattern
b. Measurement of HVL
c. Use of a digital dosimeter to determine exposure reproducibility
d. Use of a digital dosimeter to determine exposure linearity
D.
An outpatient radiographic room is used primarily for tabletop radiography of the extremities. On a particularly busy afternoon, the radiographers find that similar exposure techniques on successive patients result in substantially different radiographs. Which of the following would lead to an accurate diagnosis of the problem?
a. Contrast test pattern
b. Measurement of HVL
c. Use of a digital dosimeter to determine exposure reproducibility
d. Use of a digital dosimeter to determine exposure linearity
C.
X-ray beam quality is expressed in terms of:
a. Half-value layer
b. Exposure linearity
c. Exposure reproducibility
d. mAs
A.
The accuracy of collimation at a 40-inch SID must be:
a. ± 4 inches
b. ± 8⁄10 inch
c. ± 1 inch
d. ± 1⁄10 inch
B. 2% of the SID
The accuracy of kVp at 80 kVp must be:
a. Within 5%
b. Within 10%
c. Within 15%
d. Within 20%
B. Some sources indicate it must be within 4 to 6 kVp.
The apparent size of the focal spot as viewed by the image receptor is called the:
a. Actual focal spot
b. Target angle spot
c. Anode heel effect
d. Effective focal spot
D.
Which of the following interactions is the primary source of diagnostic x-rays?
a. Photoelectric effect
b. Bremsstrahlung
c. Compton
d. Pair production
B.
Which set of exposure factors would produce the greatest receptor exposure?
a. 100 mAs, 70 kVp, 0.5-mm focal spot, 60-inch SID
b. 200 mAs, 60 kVp, 1.2-mm focal spot, 60-inch SID
c. 100 mAs, 70 kVp, 1.2-mm focal spot, 60-inch SID
d. 300 mAs, 90 kVp, 0.5-mm focal spot, 60-inch SID
D. Highest mAs and highest kVp
Which set of exposure factors would produce the lowest receptor exposure?
a. 80 mAs, 85 kVp, 40-inch SID, 1.2-mm focal spot
b. 40 mAs, 60 kVp, 40-inch SID, 0.5-mm focal spot
c. 160 mAs, 70 kVp, 40-inch SID, 1.2-mm focal spot
d. 160 mAs, 90 kVp, 40-inch SID, 0.5-mm focal spot
B. Lowest mAs and lowest kVp
The components of a grid are:
a. Pb strips and Pb interspacers
b. Al strips and Pb interspacers
c. Pb strips and Al interspacers
d. Pb strips and cardboard interspacers
C.
The components of a grid are:
a. Pb strips and Pb interspacers
b. Al strips and Pb interspacers
c. Pb strips and Al interspacers
d. Pb strips and cardboard interspacers
A.
Bit depth describes:
a. The available gray scale of an imaging system
b. Window level
c. Spatial resolution
d. Optimum exposure needed for an imaging system
A.
If it is necessary to reduce exposure by half, and it is impossible to do so by changing mAs, the radiographer may:
a. Reduce SID by half
b. Double SID
c. Decrease kVp by 15%
d. Decrease kVp by 50%
C. The 15% rule
The dynamic range for digital imaging is:
a. Wide
b. Narrow
c. Unrelated to diagnostic imaging
A.
Dynamic range is defined as:
a. The range of exposures over which a detector can acquire image data
b. Exposure latitude
c. Window width
d. Window level
A.
Modulation transfer function (MTF) is:
a. The controlling factor of contrast resolution
b. A measure of the ability of the imaging system to preserve signal contrast as a function of the spatial resolution
c. A function of exposure
d. A function of pixel density
B.
2n (where n equals the number of bits) defines:
a. Pixel density
b. Shades of gray
c. Bit depth
d. Detector element size
C.
A scintillator:
a. Absorbs x-ray energy and emits part of that energy as visible light
b. Absorbs x-ray energy and emits that energy as electrons
c. Converts visible light into electrons
d. Converts electrons into visible light
A.
The magnitude of the signal differences in the remnant beam refers to:
a. Subject contrast
b. IP contrast
c. Window level
d. Spatial resolution
A.
A term used to describe the mathematical formula used by the computer to reconstruct the image is:
a. Bit depth
b. Algorithm
c. Mathematical function
d. Exposure equation
B. It's important to choose the correct algorithm for each exam
When speed is essential in completing an imaging examination, the preferred IR is:
a. CR
b. DR
c. Wireless DR plate
C.
Pixel is an acronym meaning:
a. Detector element
b. Picture element
c. Volume element
d. Bit element
B.
Improper use of grids with a digital imaging system may cause an artifact known as:
a. Moiré pattern
b. Grid cutoff
c. Motion artifact
d. Quantum mottle
A.
An integrated system of images and information is called:
a. DICOM
b. DDR
c. CR/DDR
d. PACS
D. Picture Archiving and Communication System
Image noise may be described as:
a. Undesirable fluctuations in brightness
b. Undesirable fluctuations in contrast
c. Inadequate spatial resolution
d. A function of mAs
A.
The measurement of the luminance of a monitor is called:
a. Density
b. Contrast
c. Brightness
d. Detail visibility
C.
Grid radius is:
a. The total amount of lead in a grid
b. The range of SIDs that may be used with a focused grid
c. The objective plane
d. H/D
B.
Visibility of an object's edge may be limited by:
a. Speed class
b. Modulation transfer function
c. Contrast resolution
d. Quantum noise
D.
Detective quantum efficiency indicates:
a. Patient dose
b. Potential speed class
c. Spatial resolution
d. Contrast resolution
B.
Digital receptors have what kind of response to exposure?
a. Nonlinear
b. Linear
c. Curvilinear
d. Hyperlinear
B.
If the angle on the anode is decreased, what effect is there on spatial resolution?
a. Increases
b. Decreases
c. No appreciable effect
A. The line-focus principle in action
If mAs is increased four times, what is the effect on receptor exposure?
a. Increases
b. Decreases
c. No appreciable effect
A. This is a directly proportional relationship
If SID is increased, what is the effect on IR exposure?
a. Increases
b. Decreases
c. No appreciable effect
B. This is the inverse square law
If OID is decreased, what is the effect on spatial
resolution?
a. Increases
b. Decreases
c. No appreciable effect
A.
A photodiode converts:
a. AC to DC
b. Light into a charge
c. Electrons into light
d. MRI signal into PACS data
B.
If kVp is increased, what happens to attenuation of the beam in the patient?
a. Increase
b. Decrease
c. No appreciable effect
B. The beam is more penetrating
In a conversion from a nongrid to a 12:1 grid, what happens to image contrast?
a. Increases
b. Decreases
c. No appreciable effect
A. Scatter is absorbed by the grid
If SID is decreased from 60 inches to 30 inches, what happens to magnification?
a. Increases
b. Decreases
c. No appreciable effect
A.
If the IR is moved from tabletop to Bucky, what happens to spatial resolution?
a. Increases
b. Decreases
c. No appreciable effect
A.
If there is a decrease in source-to-object distance, what happens to spatial resolution?
a. Increases
b. Decreases
c. No appreciable effect
B. This results in magnification of the image
The amount of lead in a grid is referred to as:
a. Grid frequency
b. Grid ratio
c. Grid radius
d. Grid cleanup ability
A.