Renal System and Long-Term Blood Pressure Regulation ~ Anatomy 2 Chapter 24
1/197
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
198 Terms
Renal system
Organ system that filters blood, removes wastes, regulates fluid/electrolytes, and maintains blood pressure
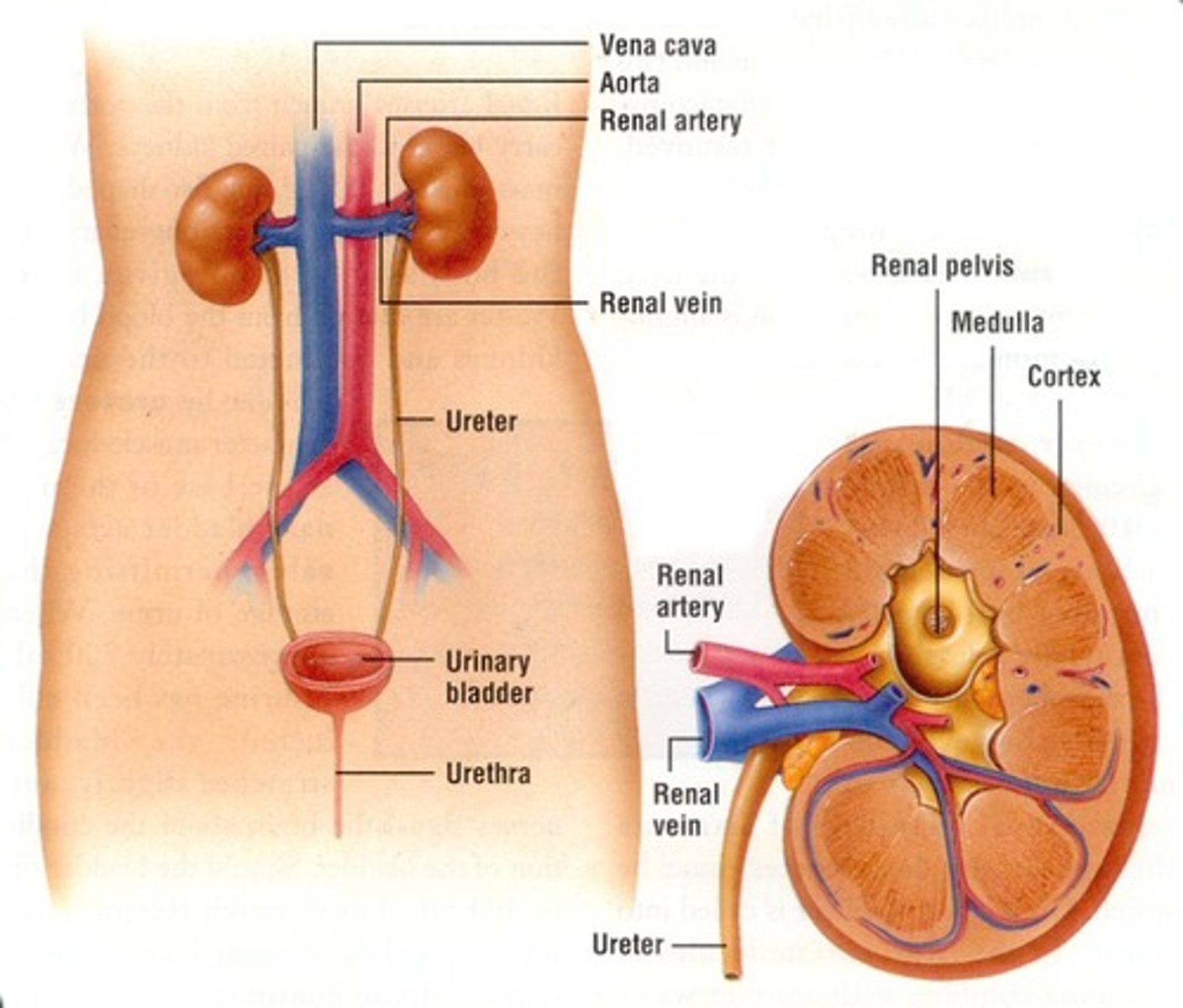
filters blood, removes wastes, regulates water content (fluid/electrolytes), and maintains blood pressure
What are the functions of the renal system?
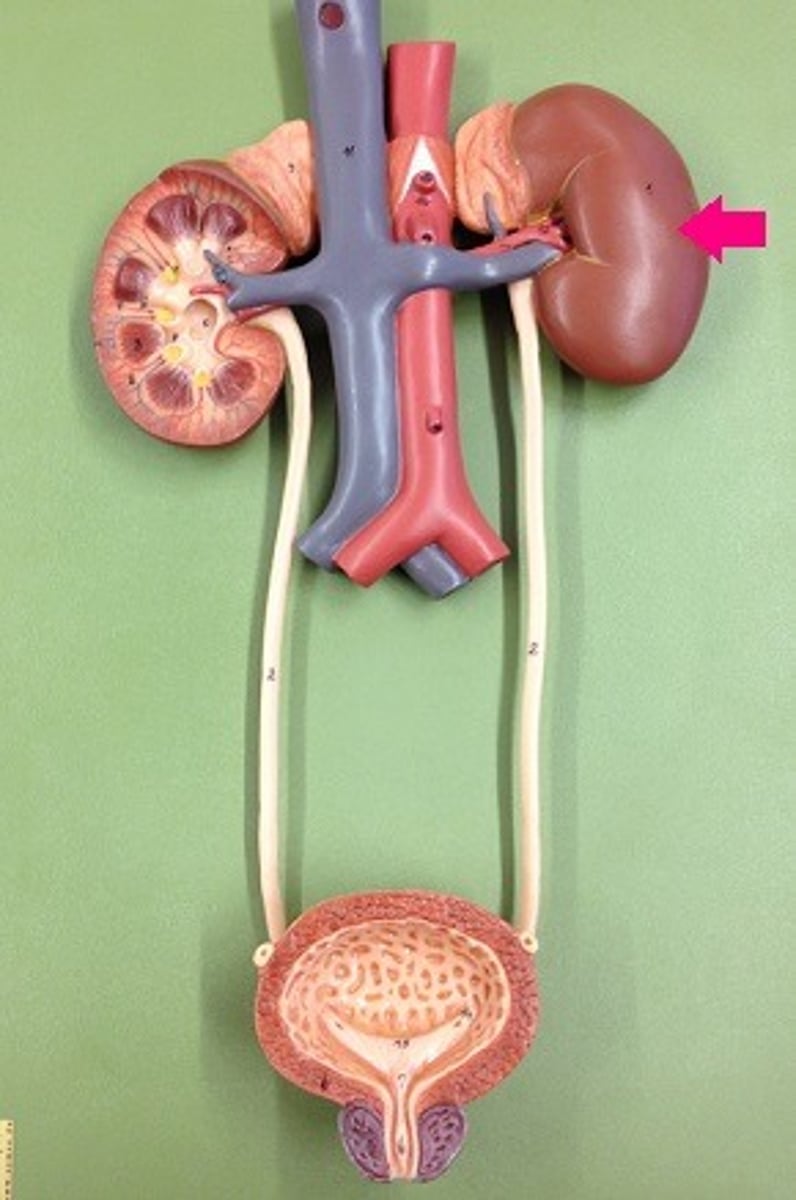
~20%, cardiac output
Kidneys receive ____% of _________
Filters blood and removes metabolic wastes (e.g., remove toxins)
The Primary kidney function is -
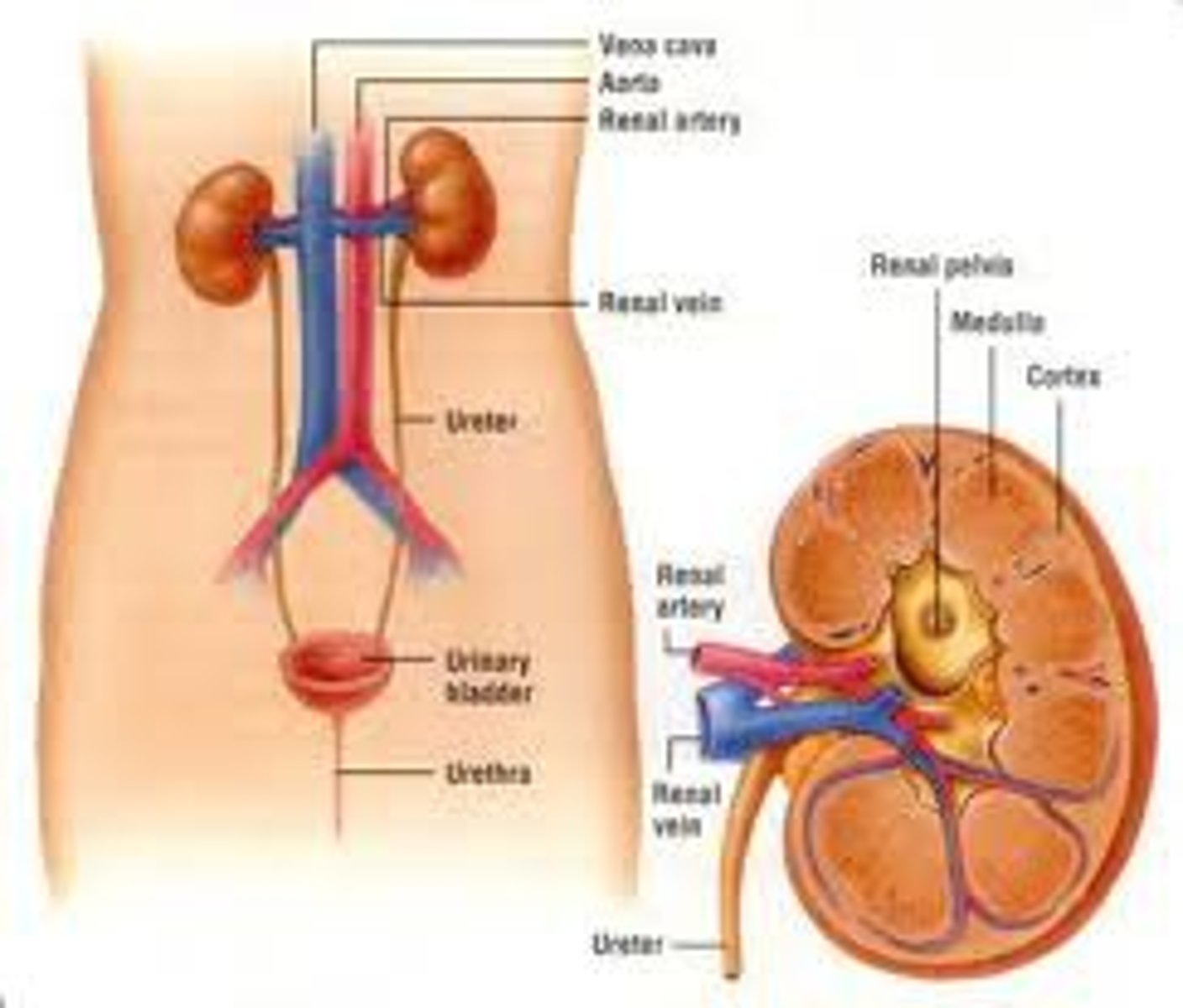
Selective reabsorption
Kidneys retain necessary substances and eliminate toxins
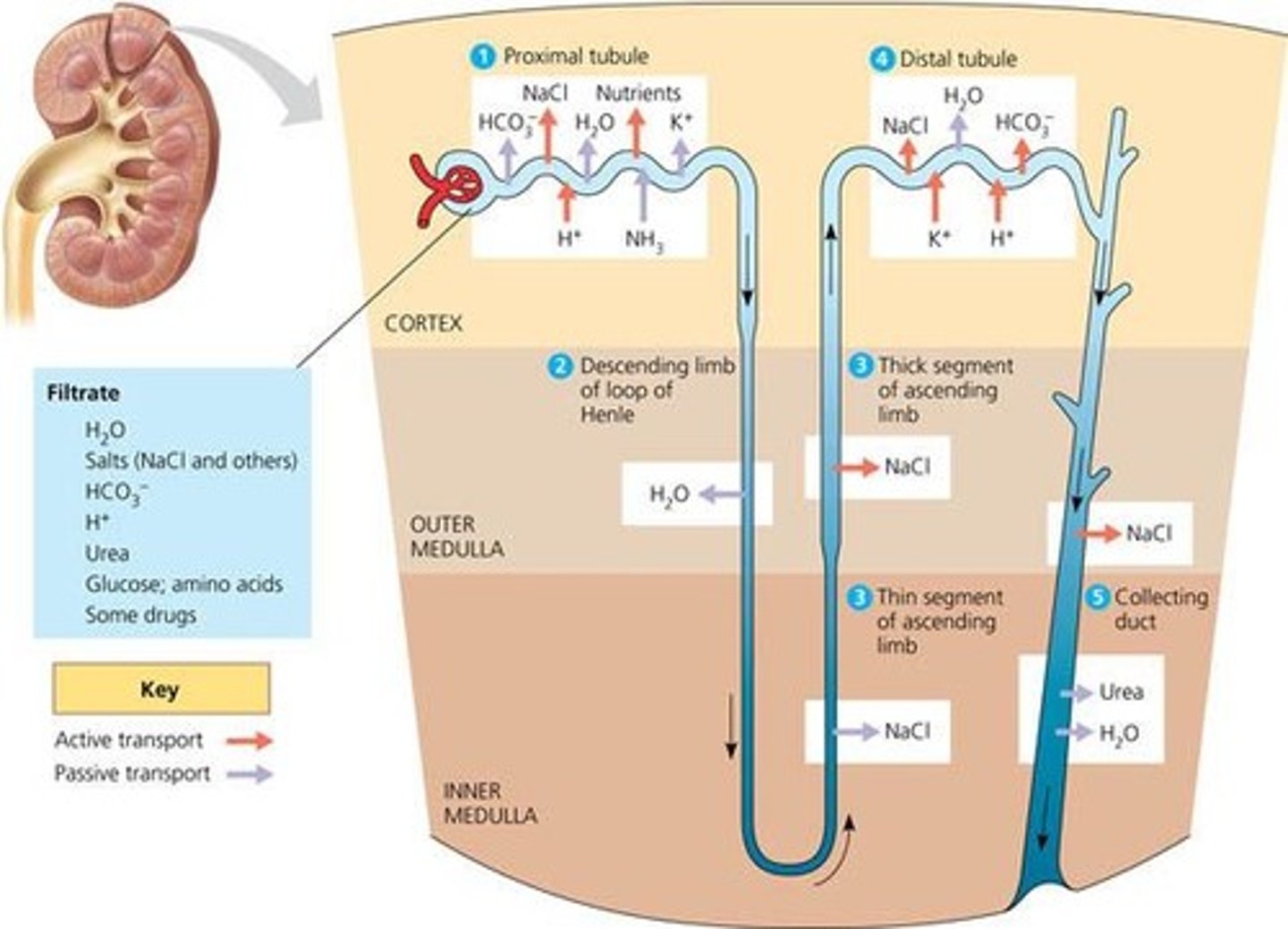
blood pressure and RBC production
Kidneys release hormones (endocrine) that regulate -
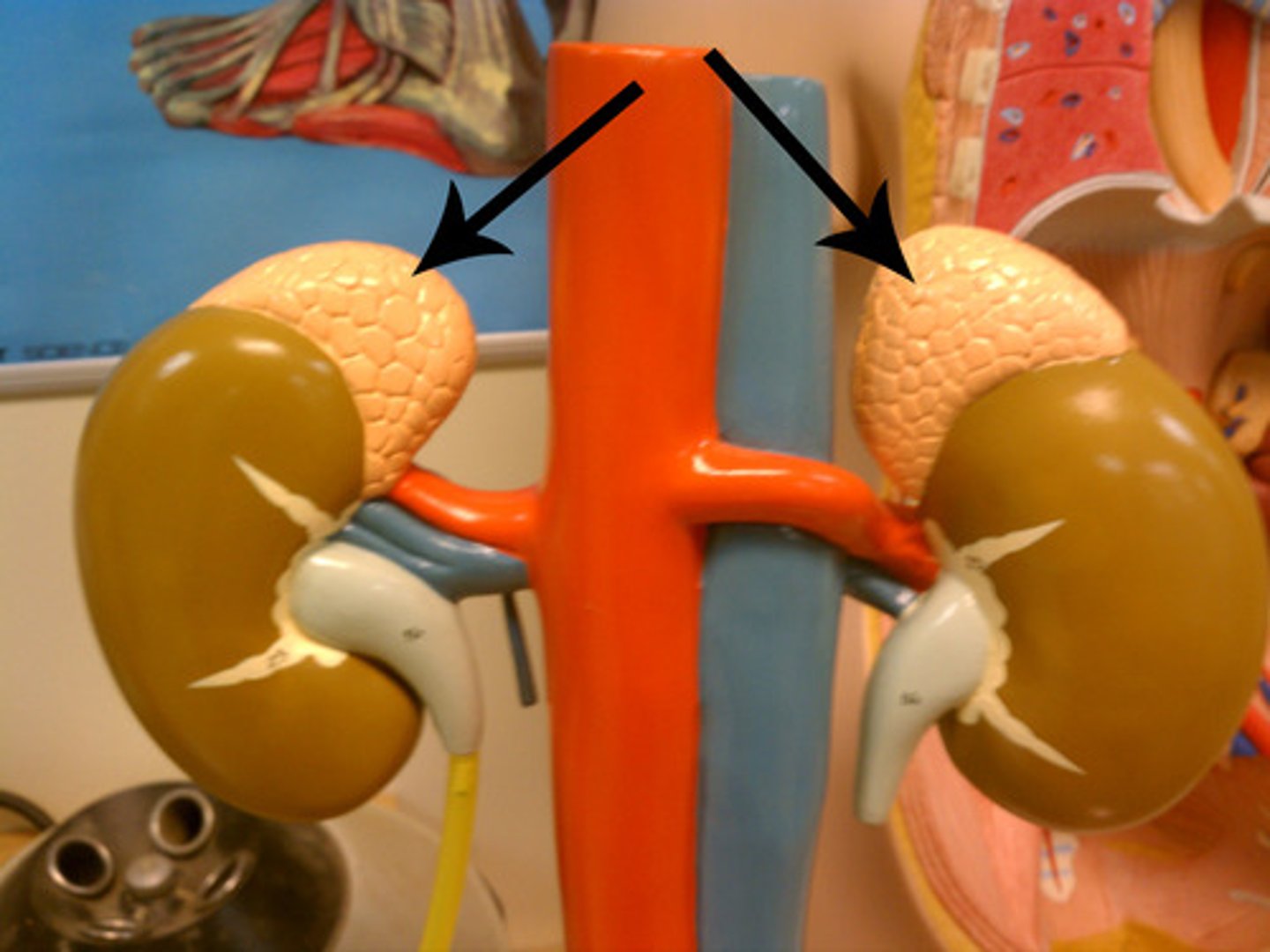
renin, erythropoietin, calcitriol
What are 3 hormones (ligands?) produced by the kidneys?
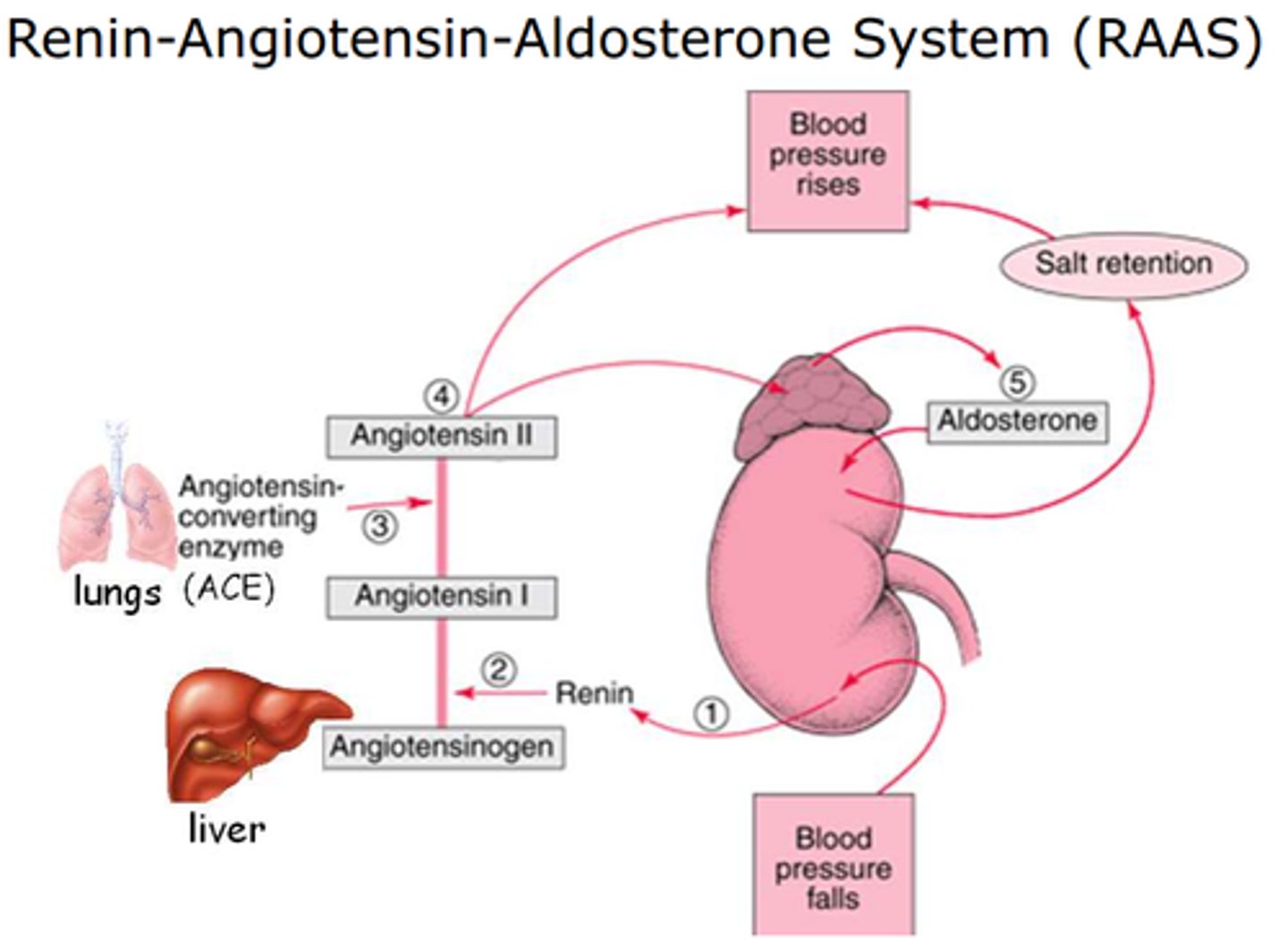
Renin
Hormone that increases blood pressure and volume via RAAS
- functions in increasing antidiuretic (ADH/vasopressin and aldosterone)
Erythropoietin (EPO)
Hormone that stimulates red blood cell production in bone marrow
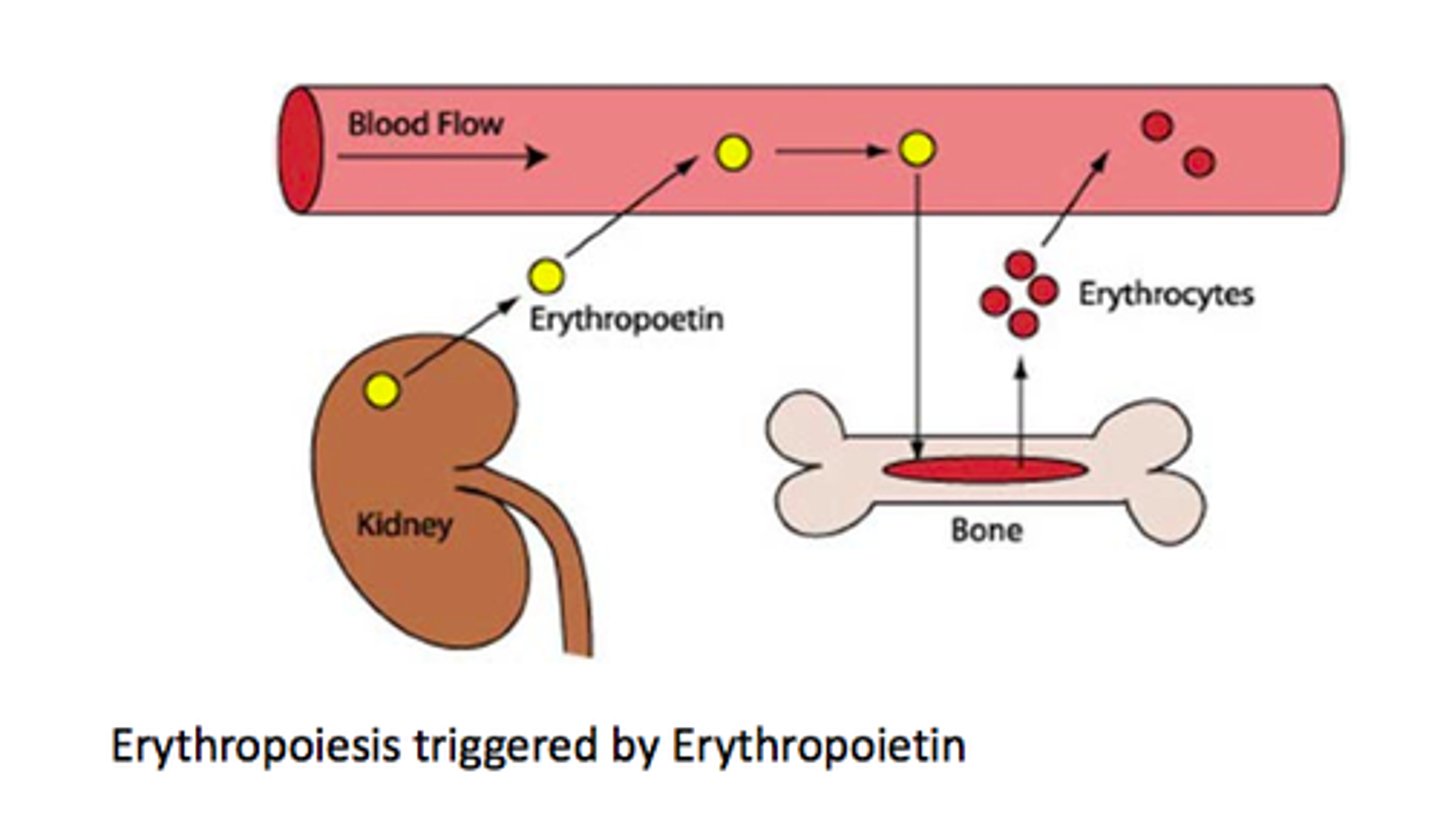
hypoxia (low oxygen)
EPO is released in response to-

Calcitriol
Active vitamin D that regulates calcium levels and gluconeogenesis
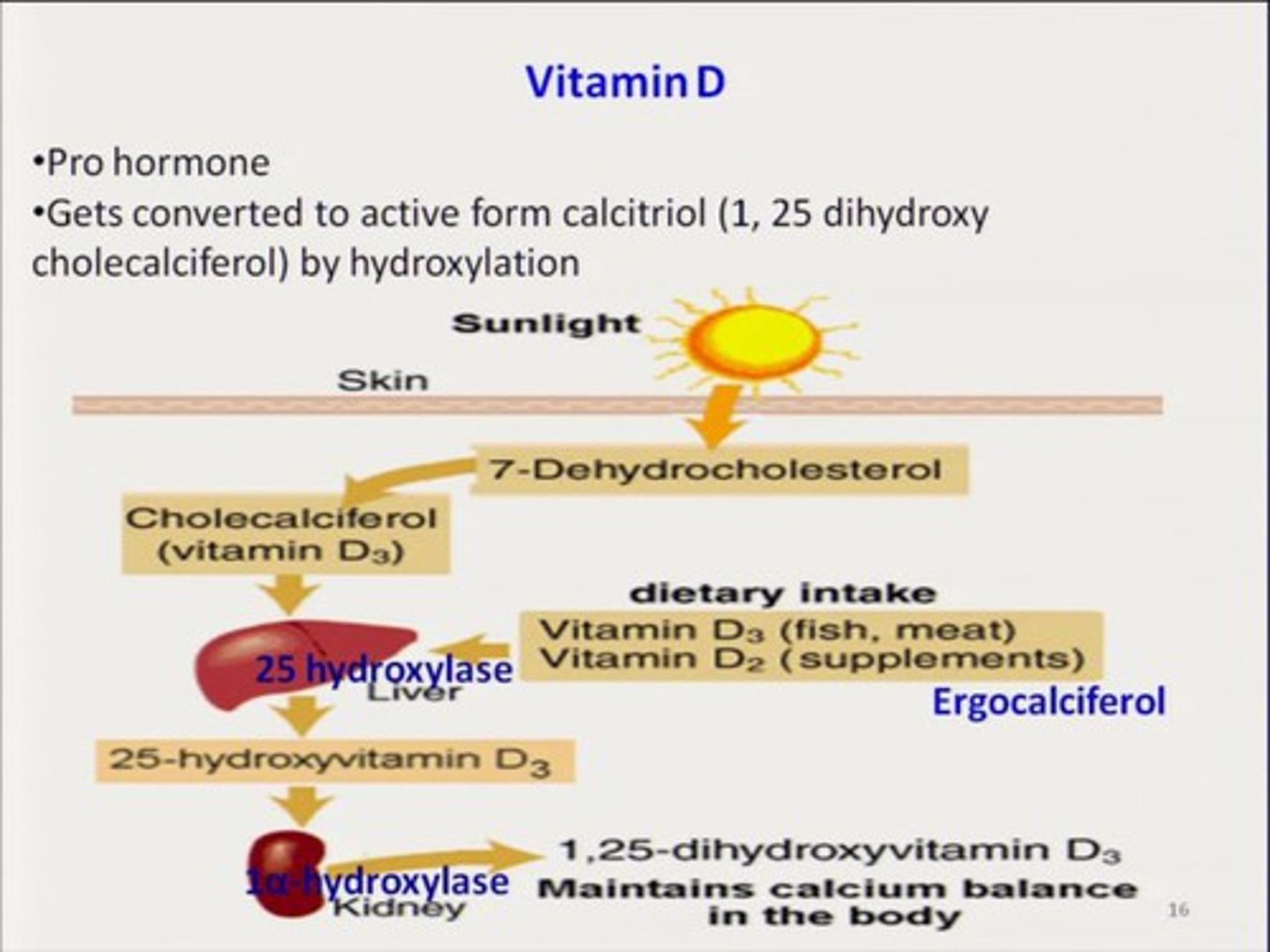
gluconeogenesis
formation of glucose from noncarbohydrate sources.
- Kidney metabolic role is to perform ___________ during fasting.
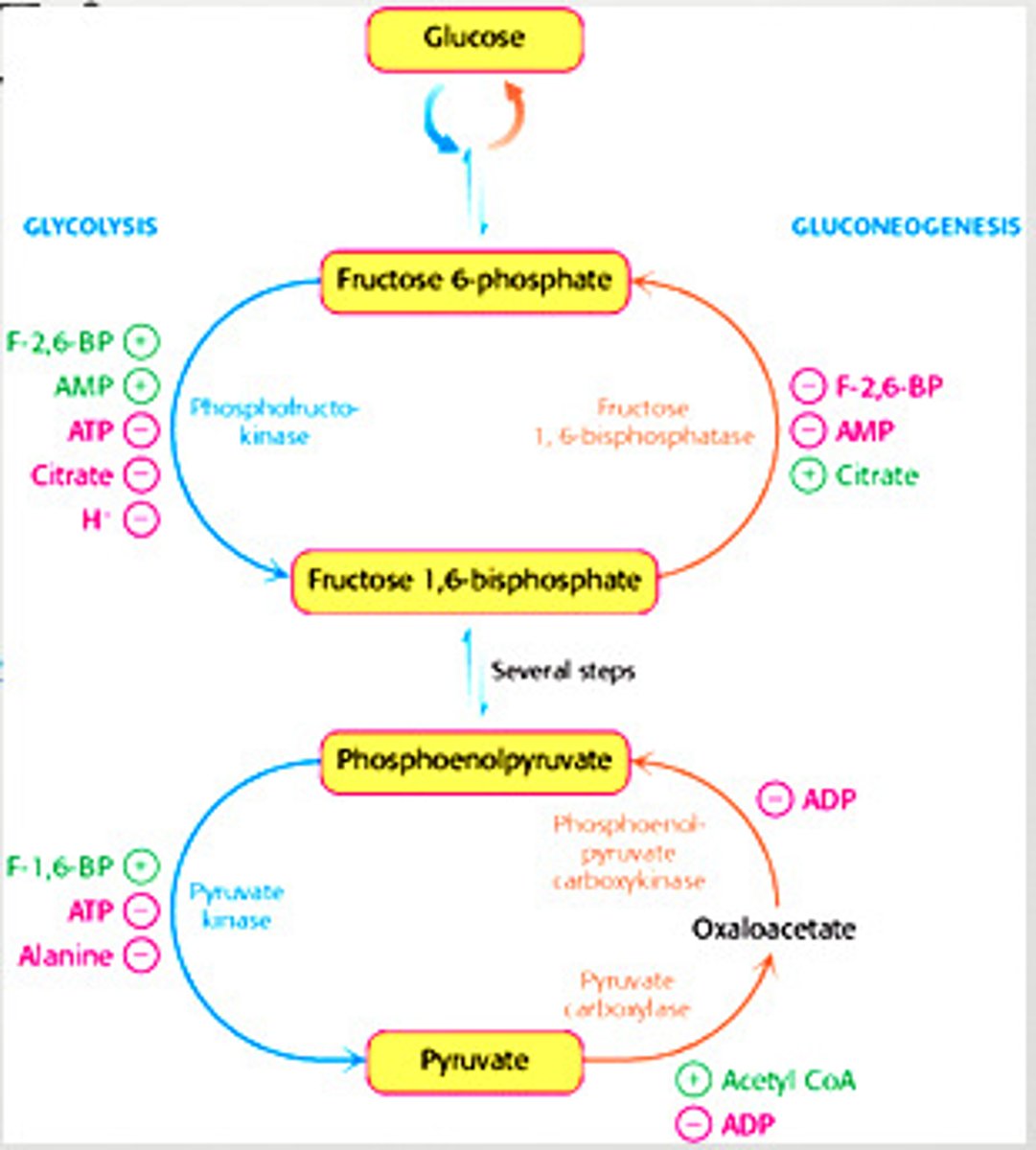
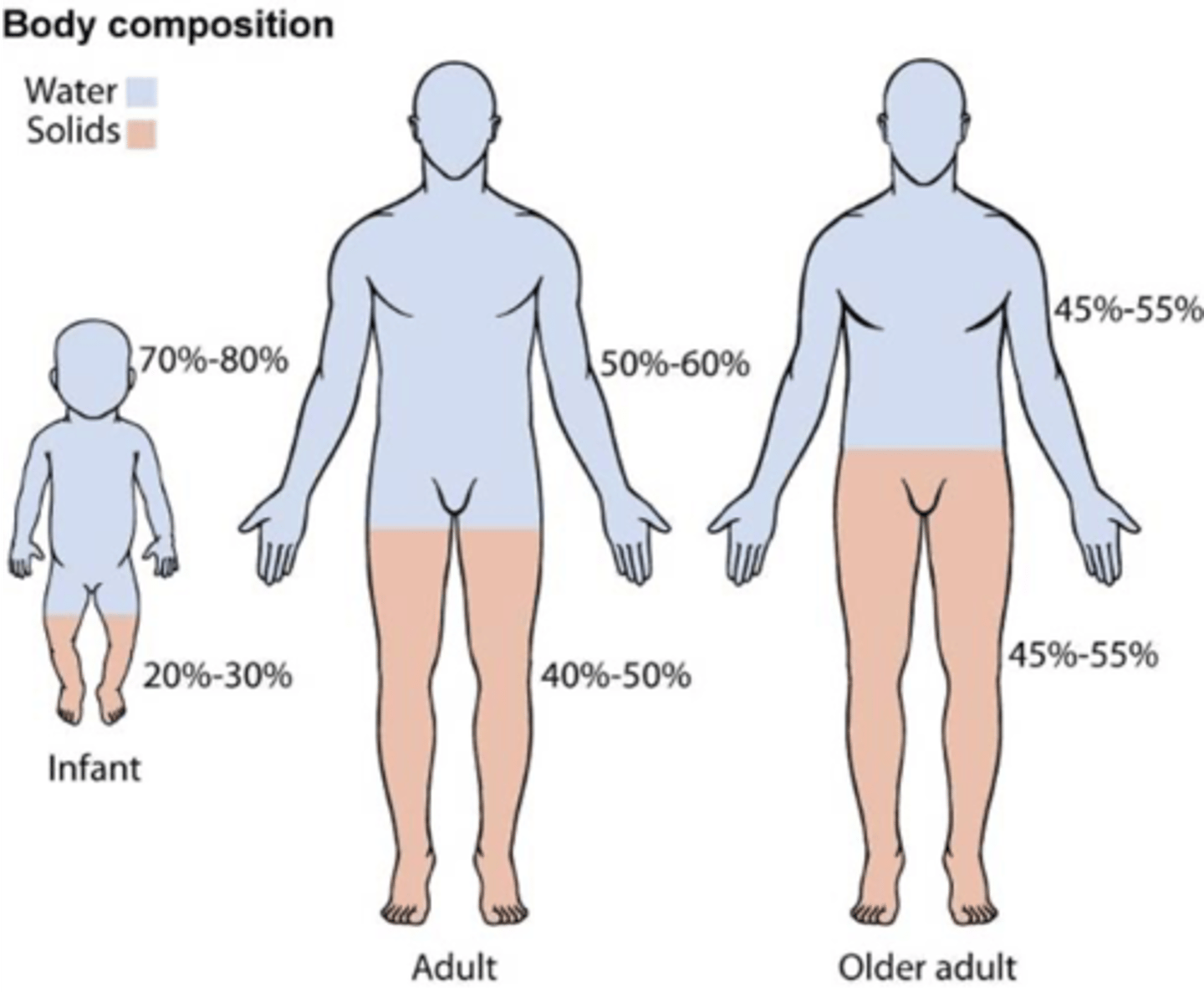
water content
Kidneys adjust total body-
Retroperitoneal (behind peritoneum)
Kidney location is-
(separated from other abd. organs 😢)
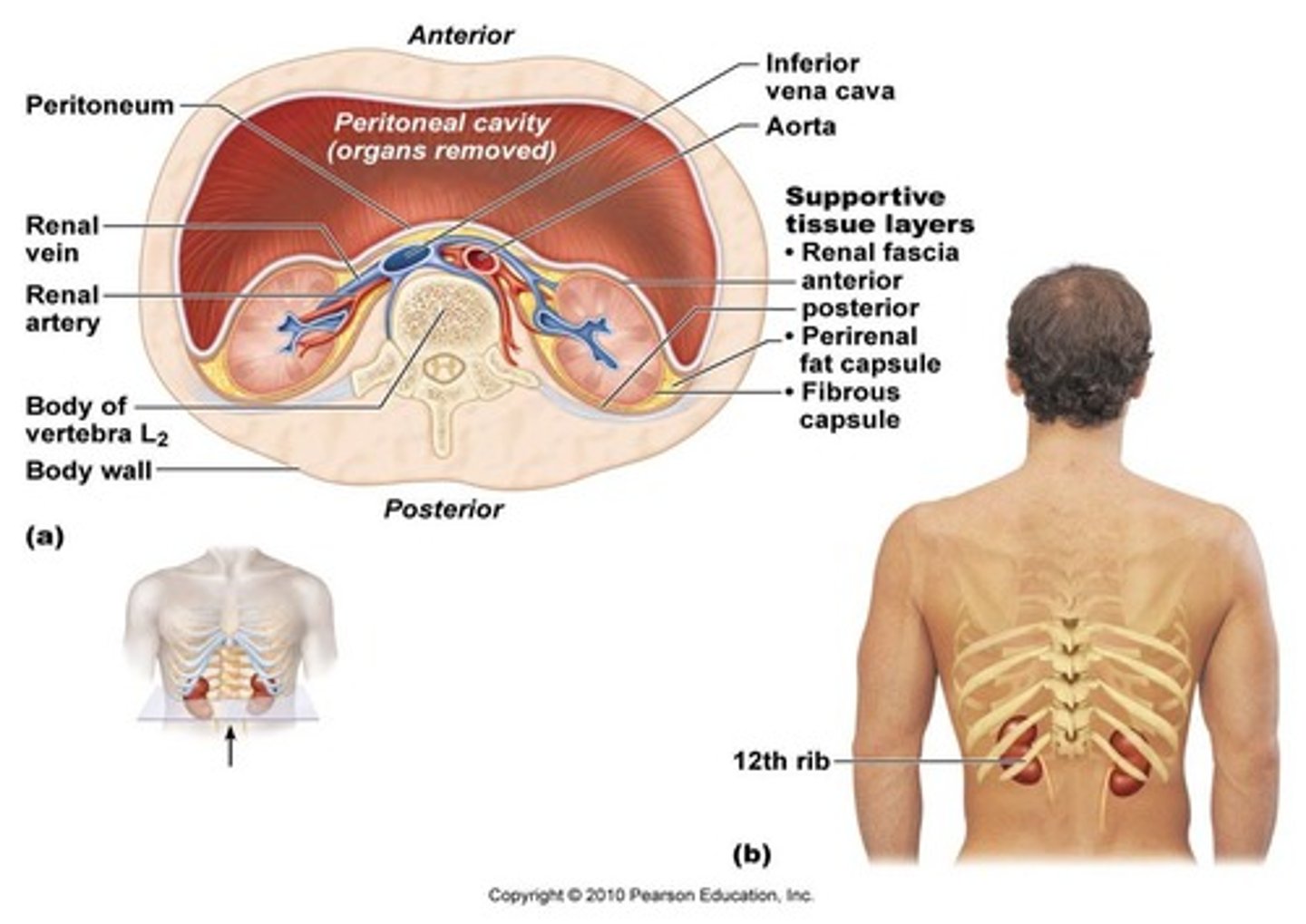
T12-L3
Vertebral level of kidneys
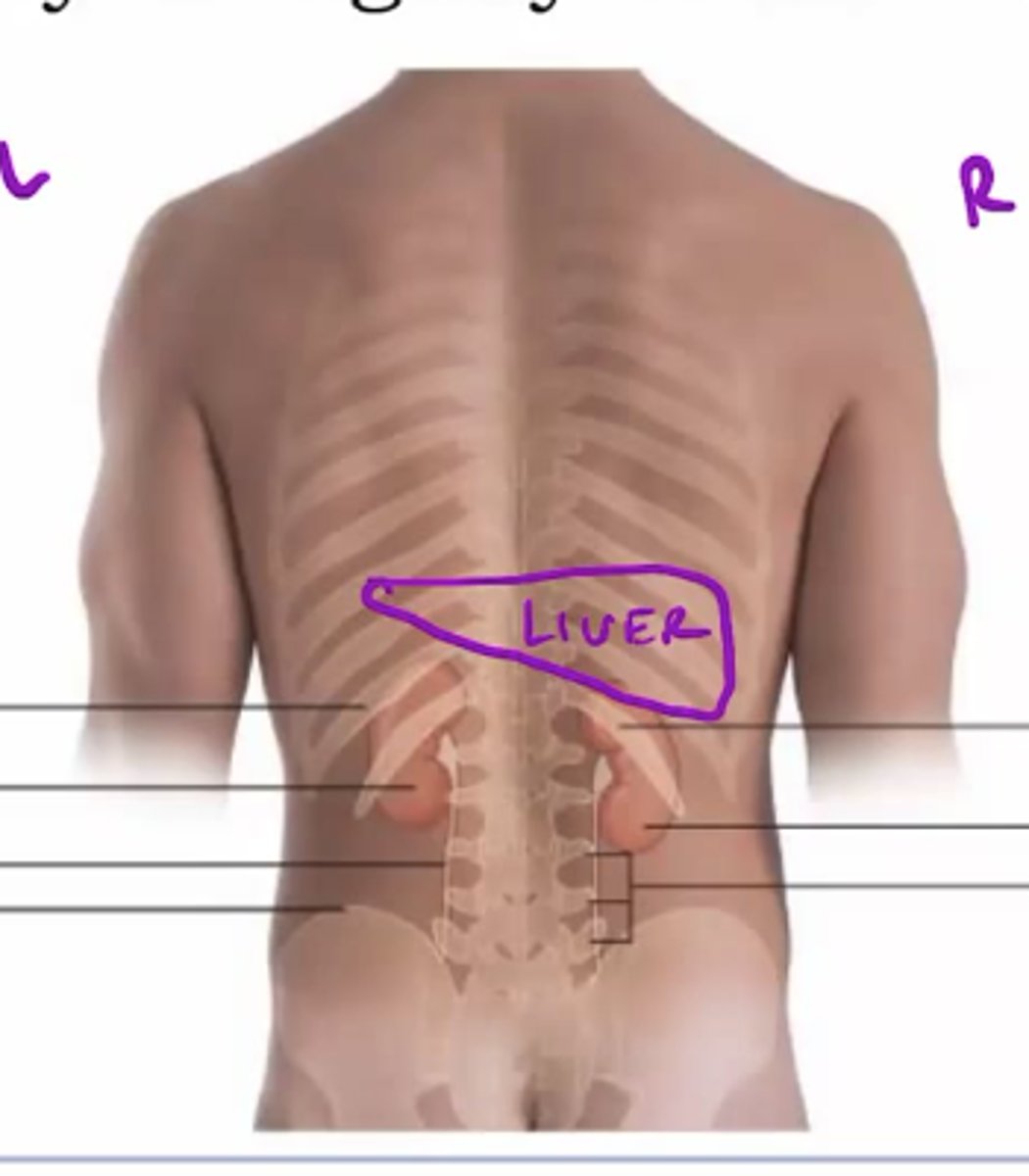
Posterior ribs (floating ribs)
Kidney are protected by-
(mostly lmao)
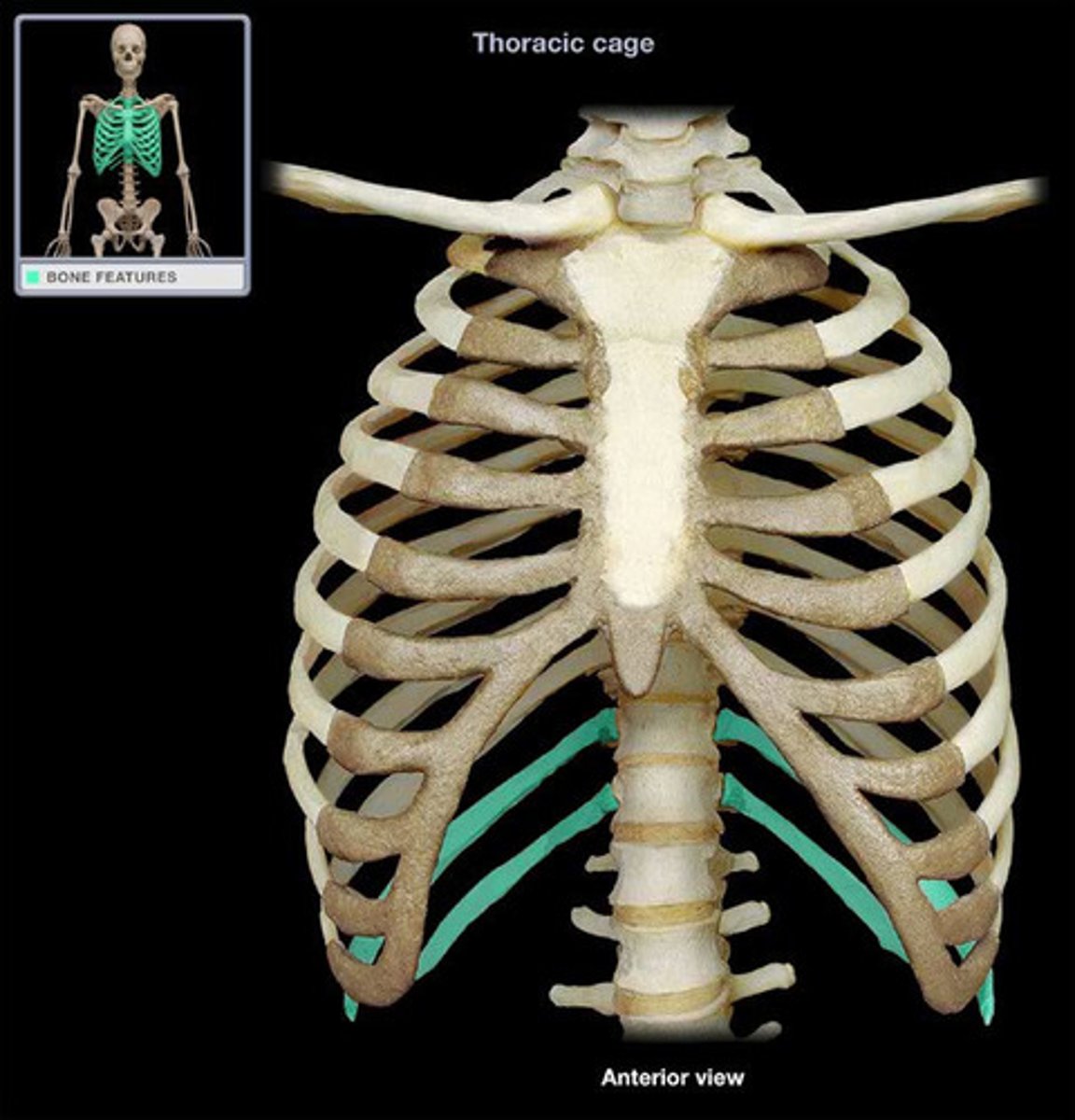
Renal fascia
Outer dense connective tissue anchoring kidneys and adrenal glands
- covers fat capsule
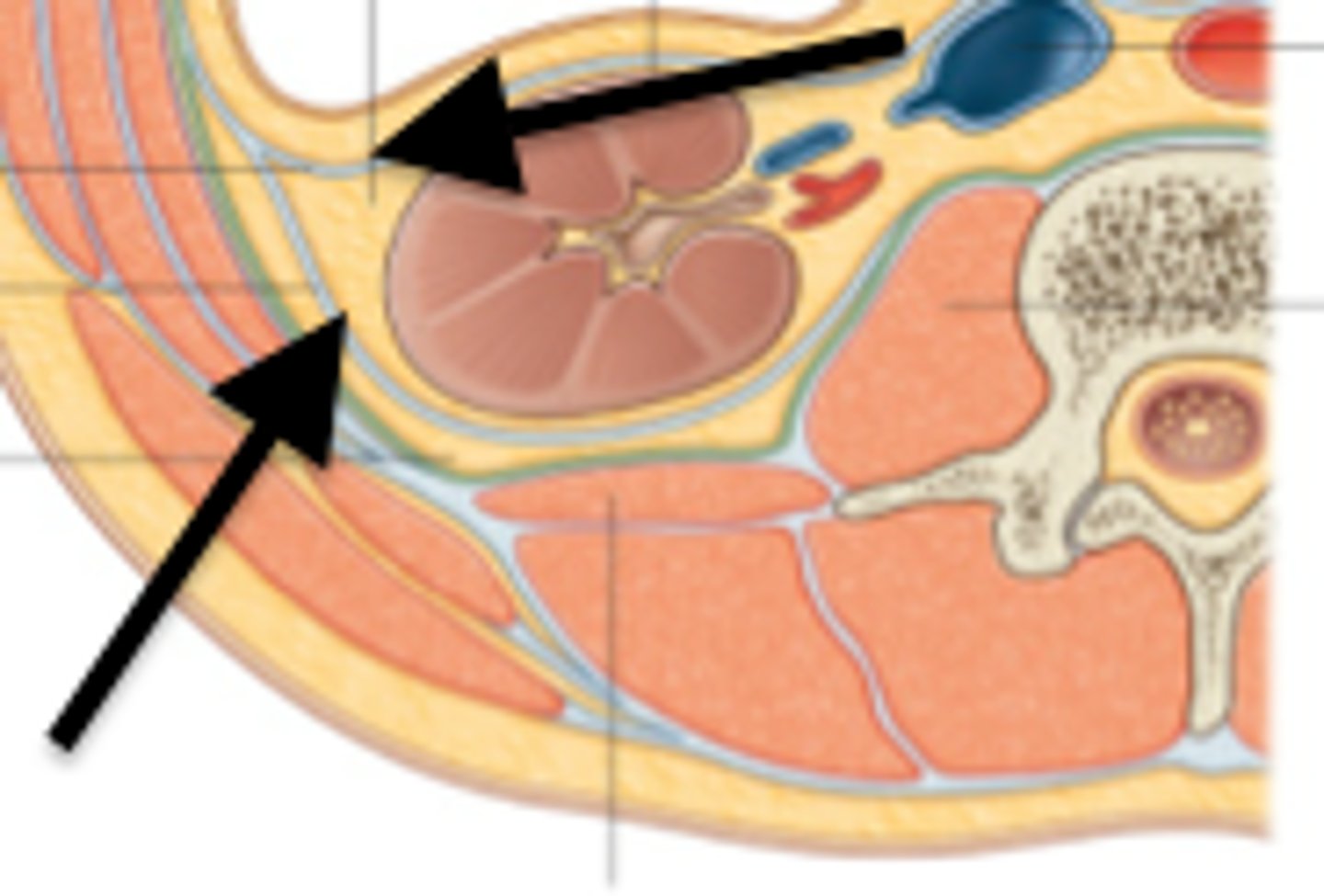
Perinephric/perirenal fat capsule
Middle adipose layer cushioning kidneys and adrenal gland
- covers renal capsule
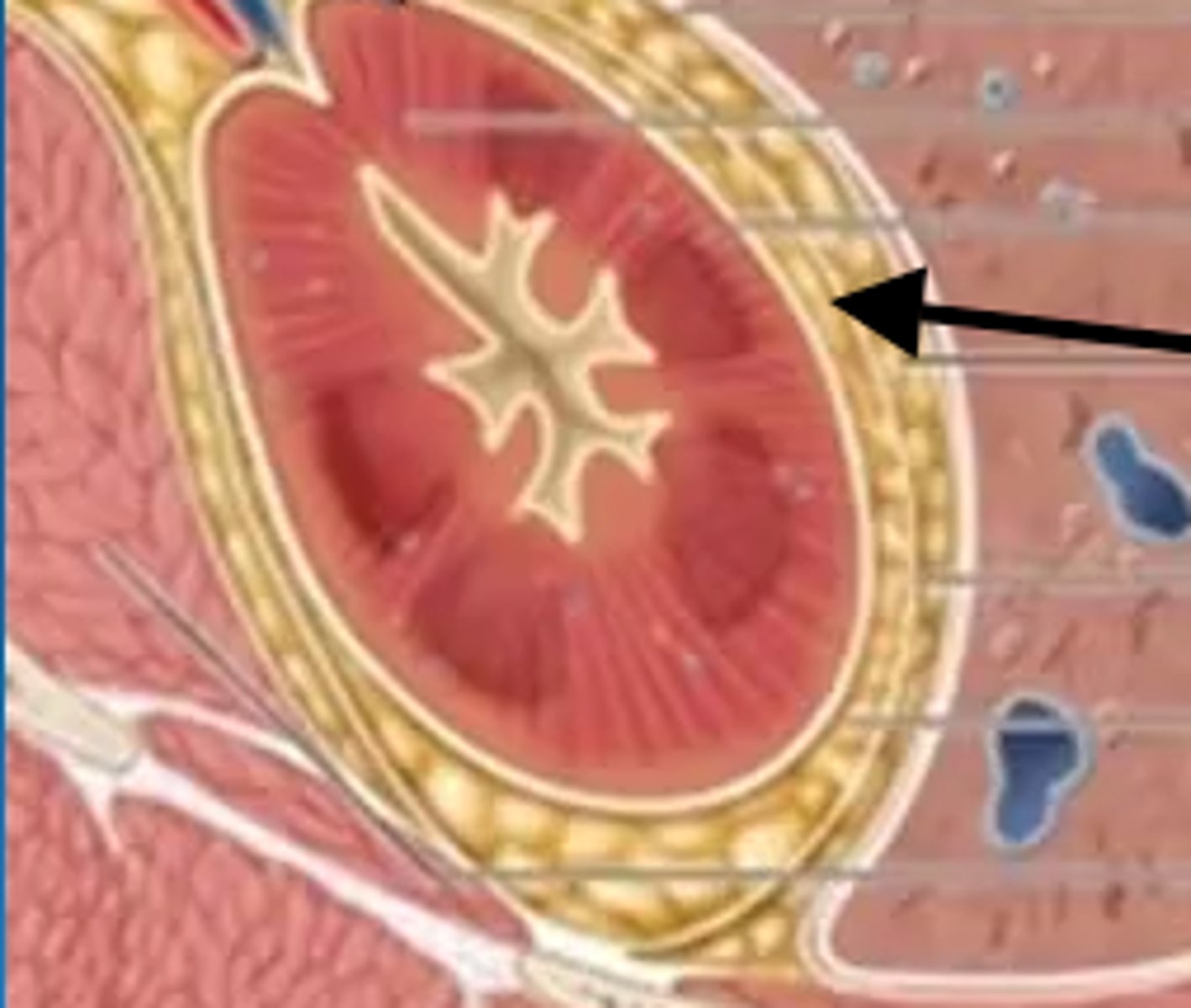
Renal capsule
Inner fibrous layer directly covering kidney
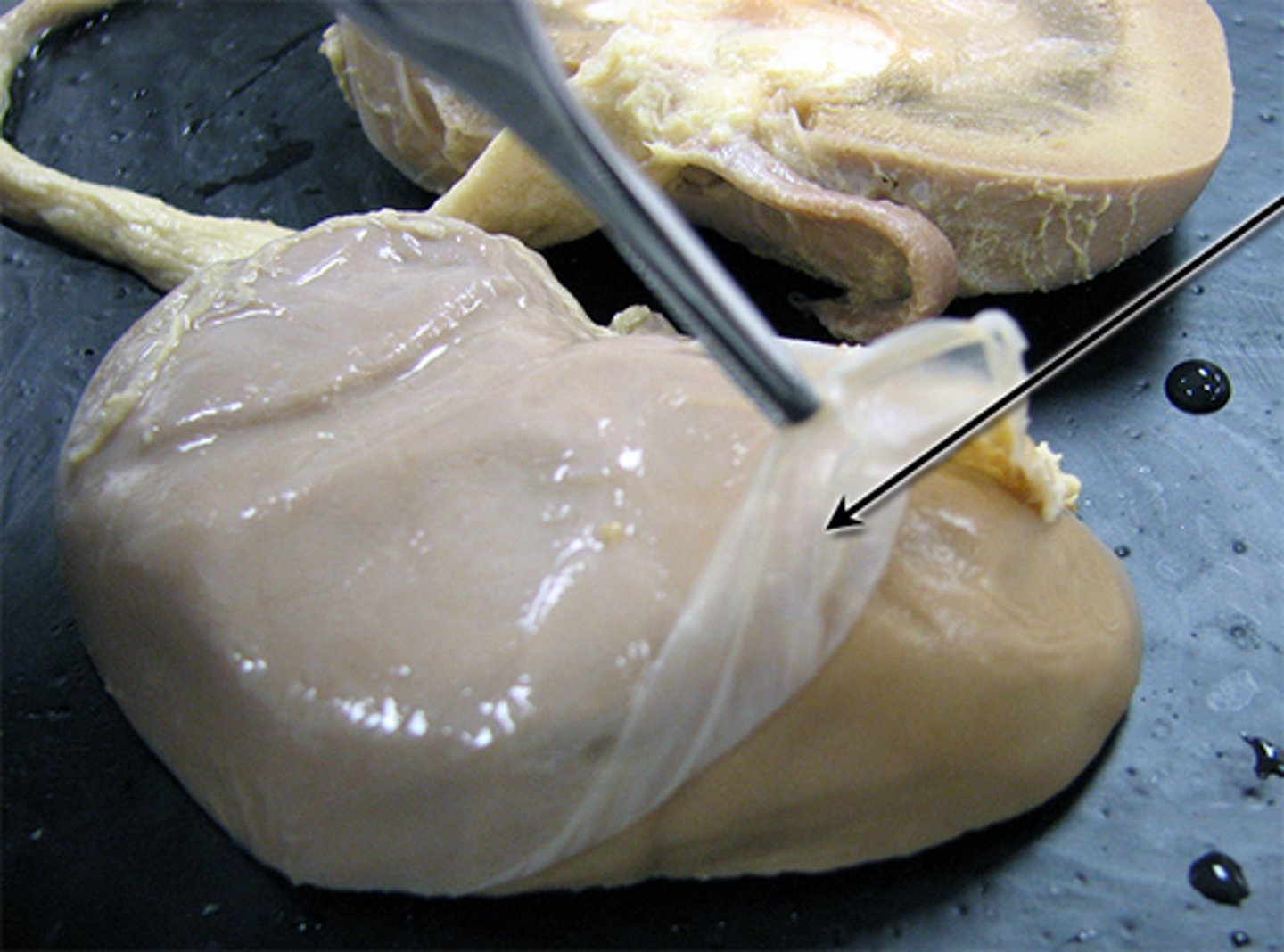
Renal fascia -> perirenal fat capsule -> renal capsule
What are the kidney connective tissue layers from superficial to deep?
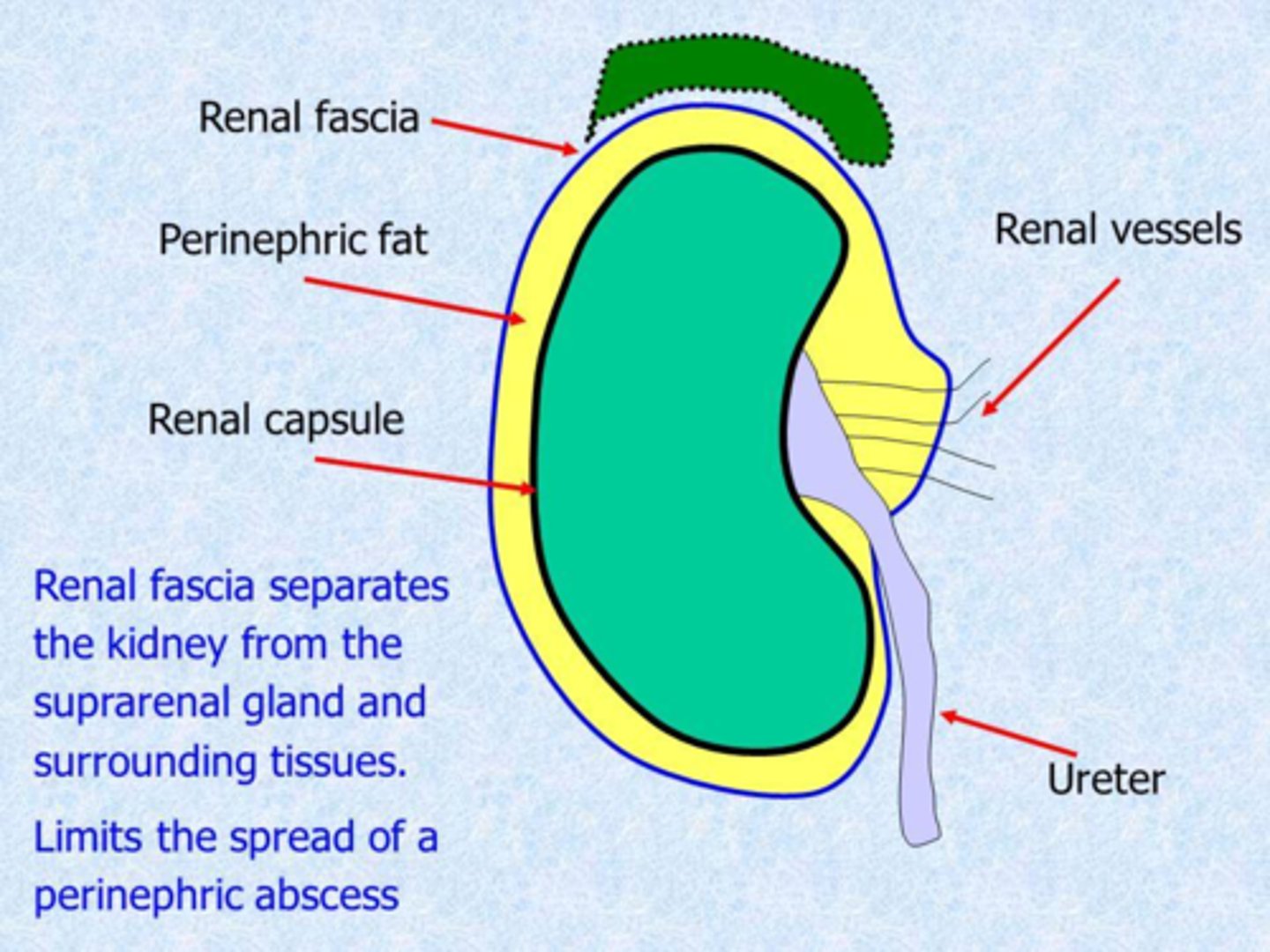
renal capsule -> perirenal fat capsule -> Renal fascia
What are the kidney connective tissue layers from deep to superficial?
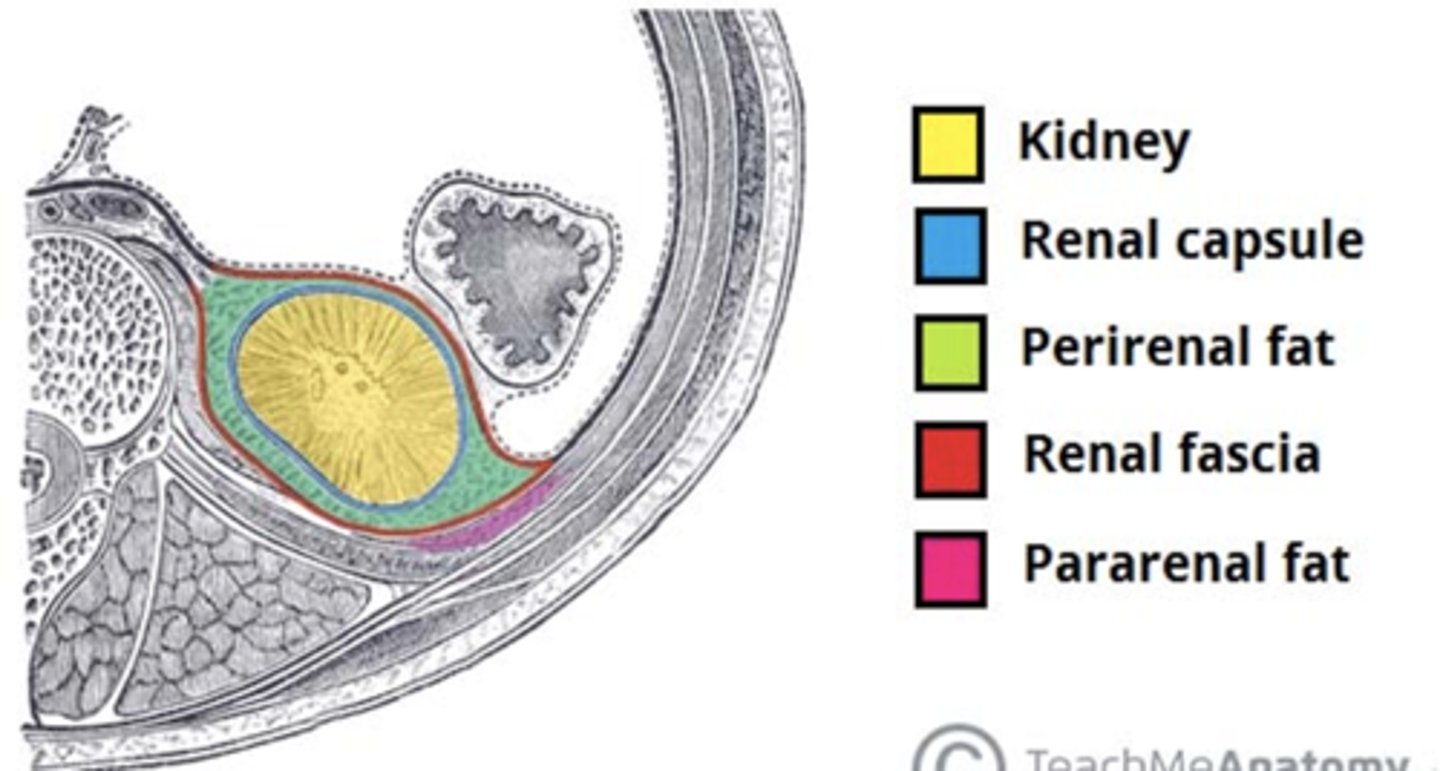
Renal cortex
Outer region; granular appearance; contains most nephrons
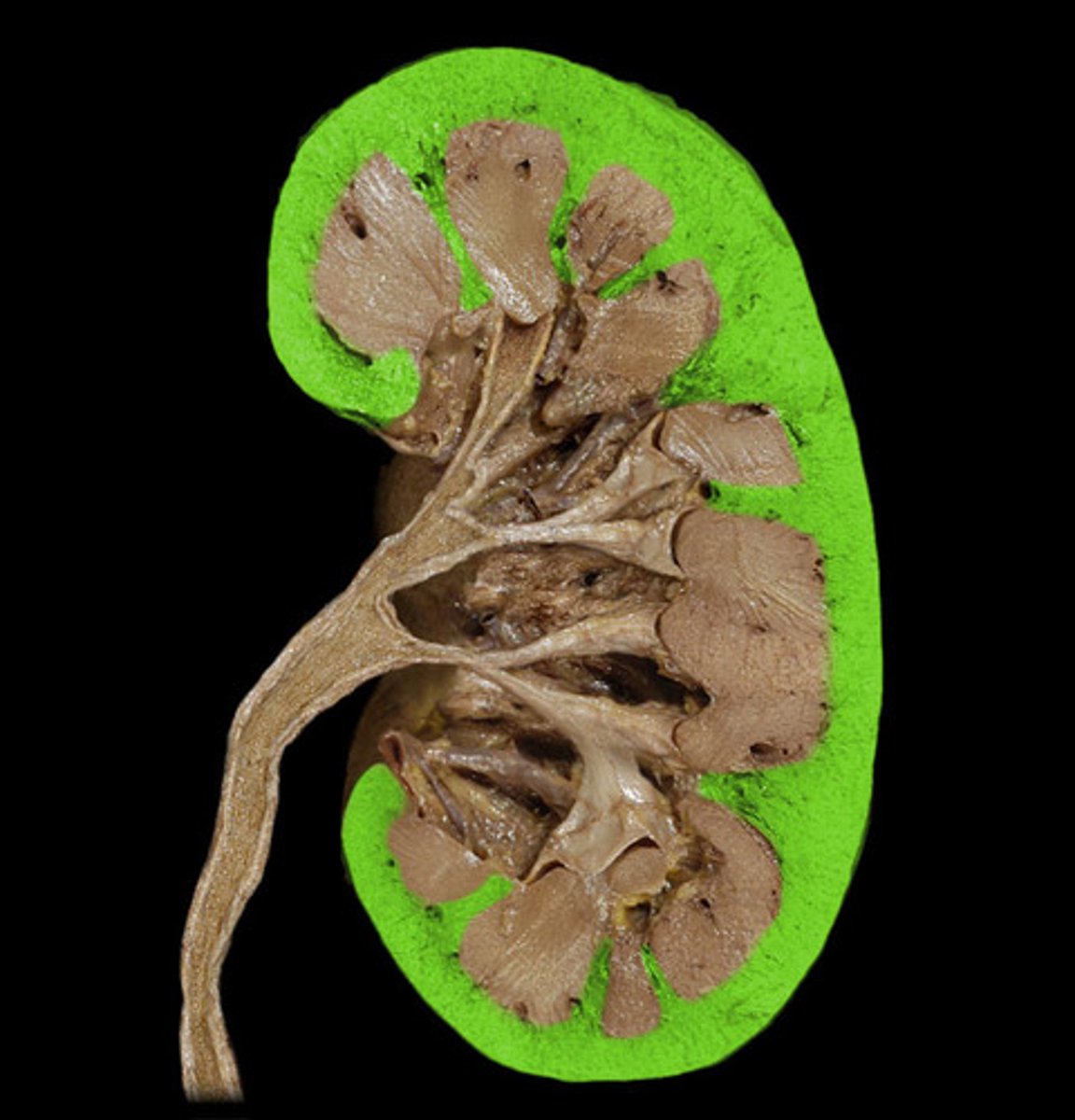
Renal medulla
Inner region composed of renal pyramids
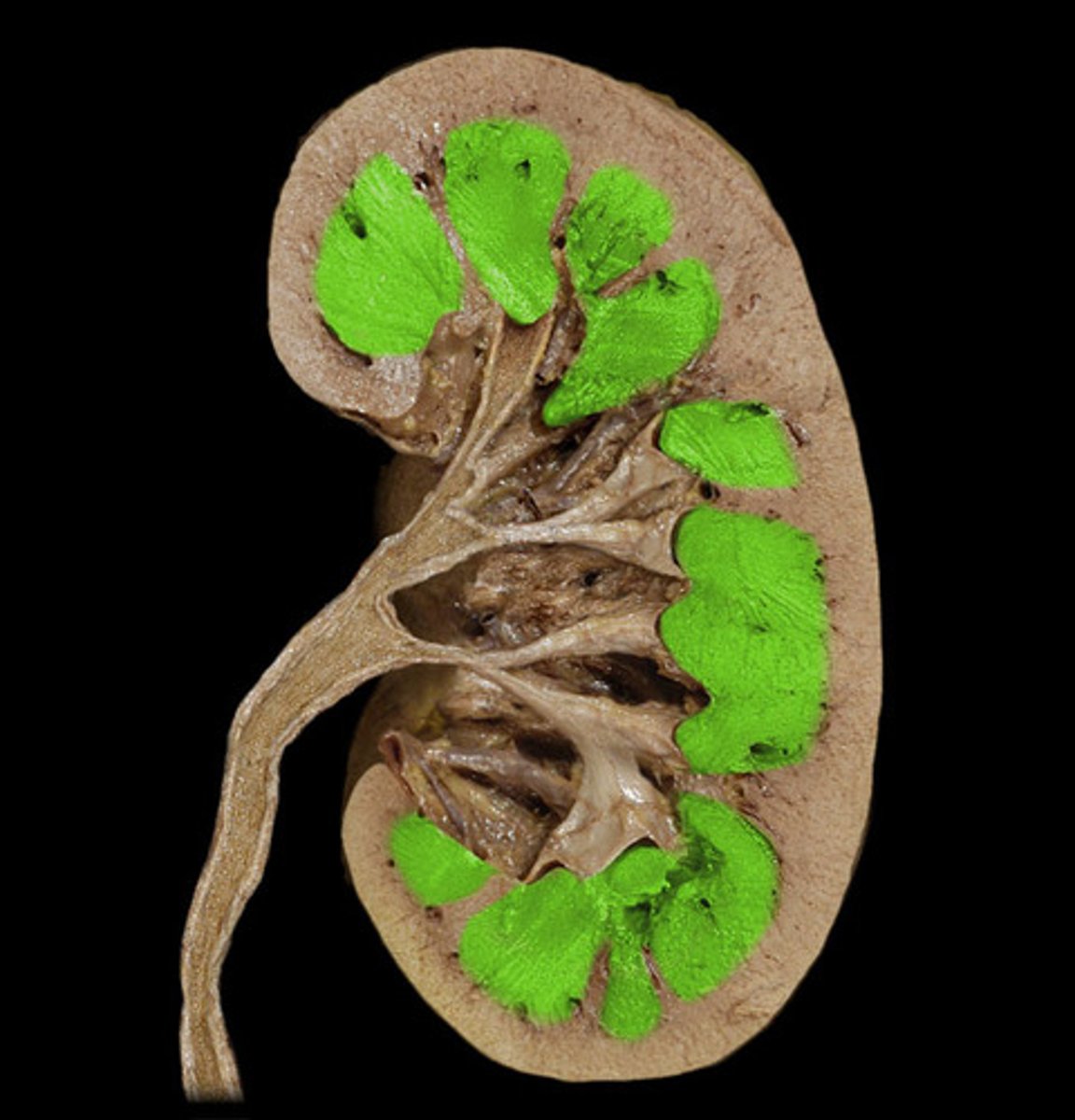
Renal pyramids
Cone-shaped structures containing tubules that make up the renal medulla
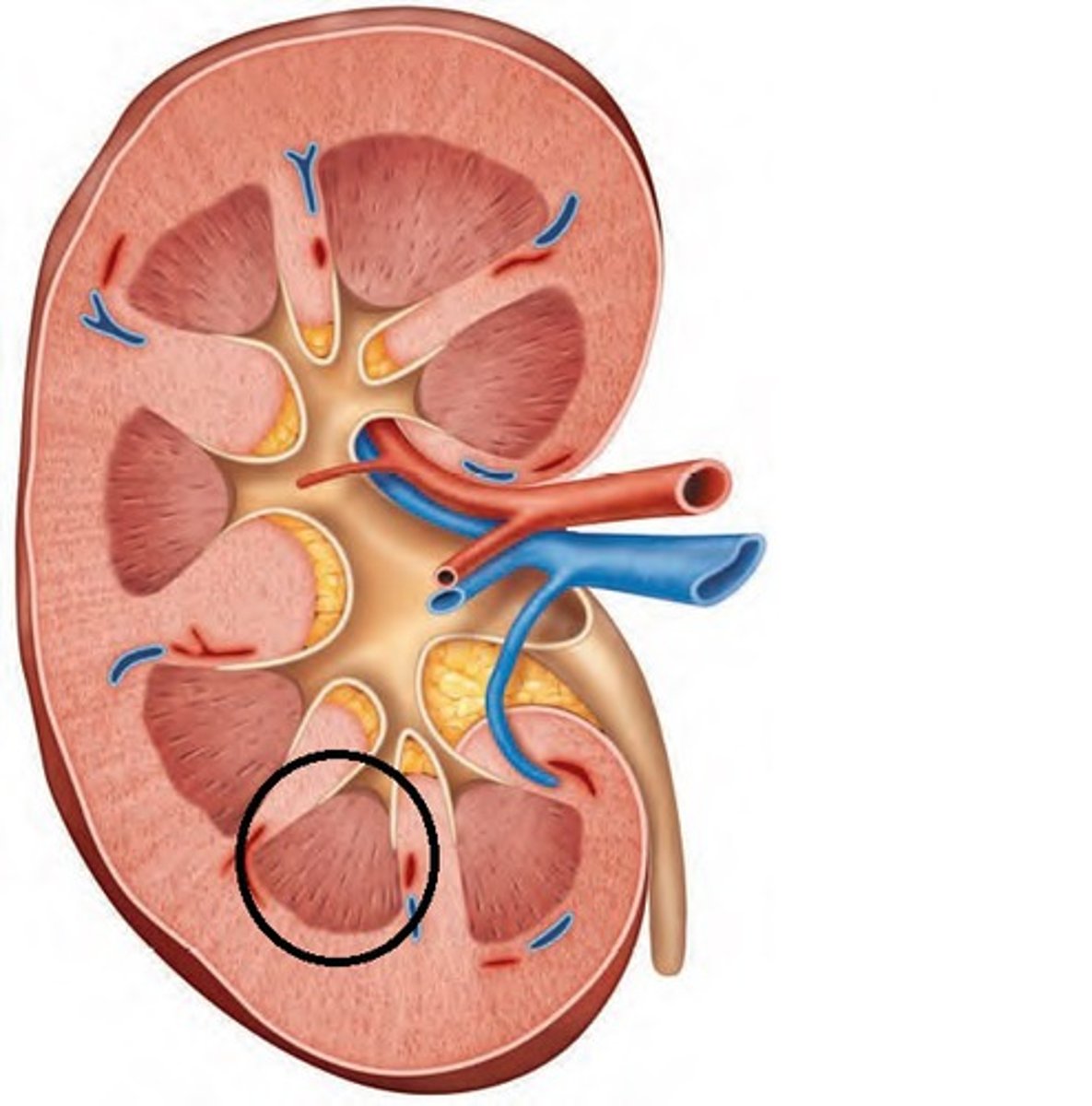
renal papilla
narrow, innermost apex end of a pyramid
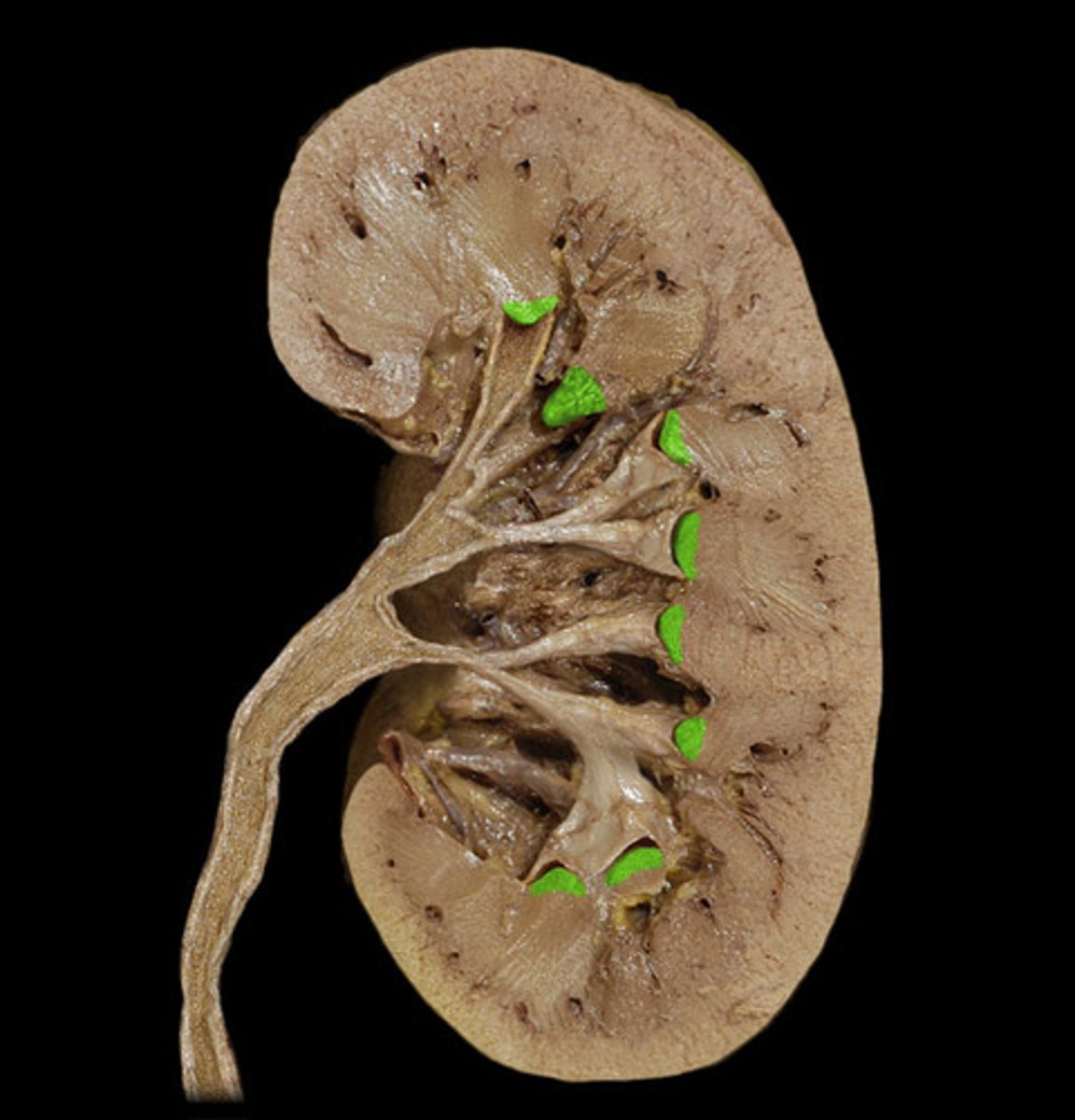
Renal columns
Tissue separating pyramids
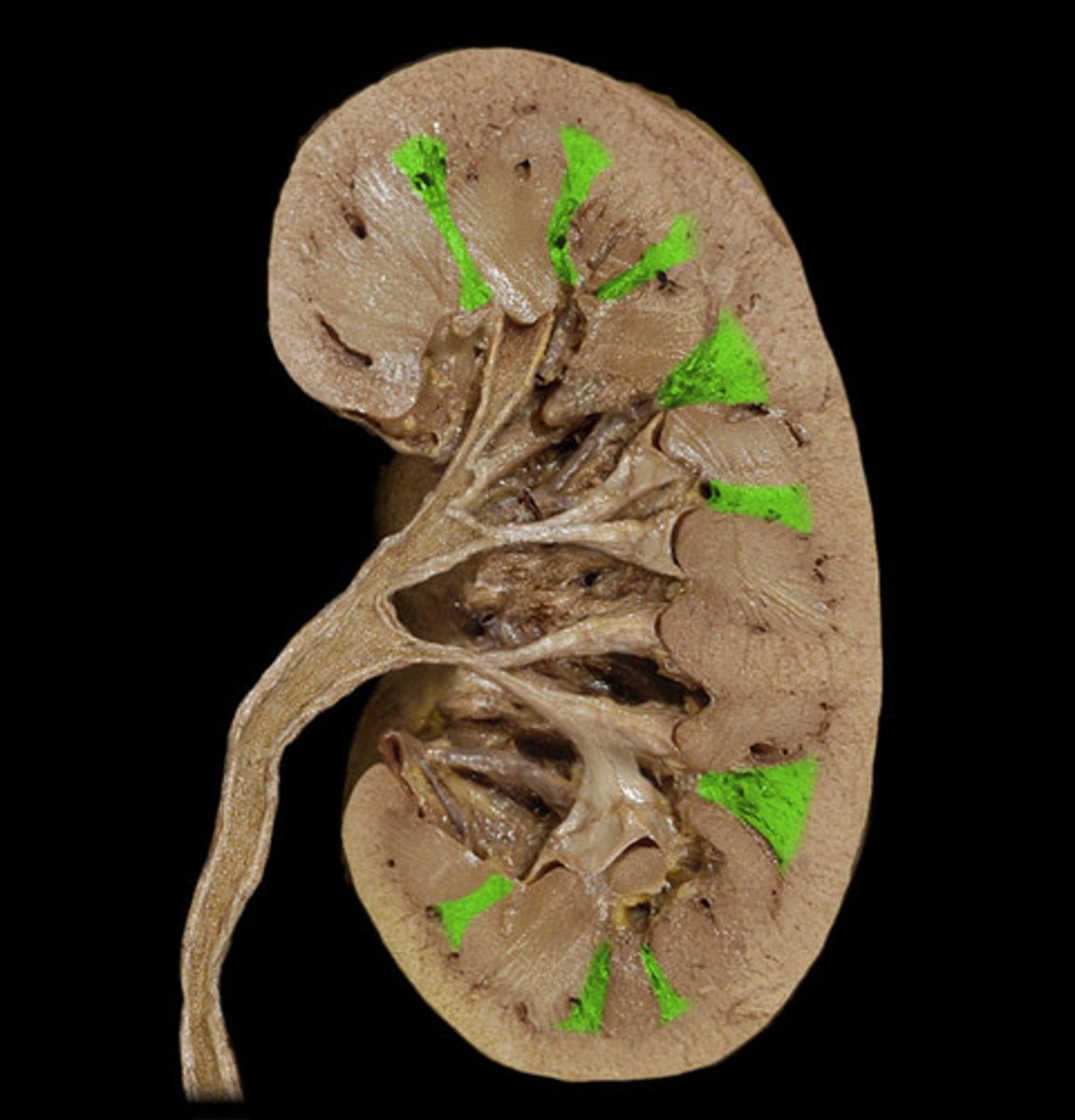
Renal lobe
Pyramid plus surrounding cortex
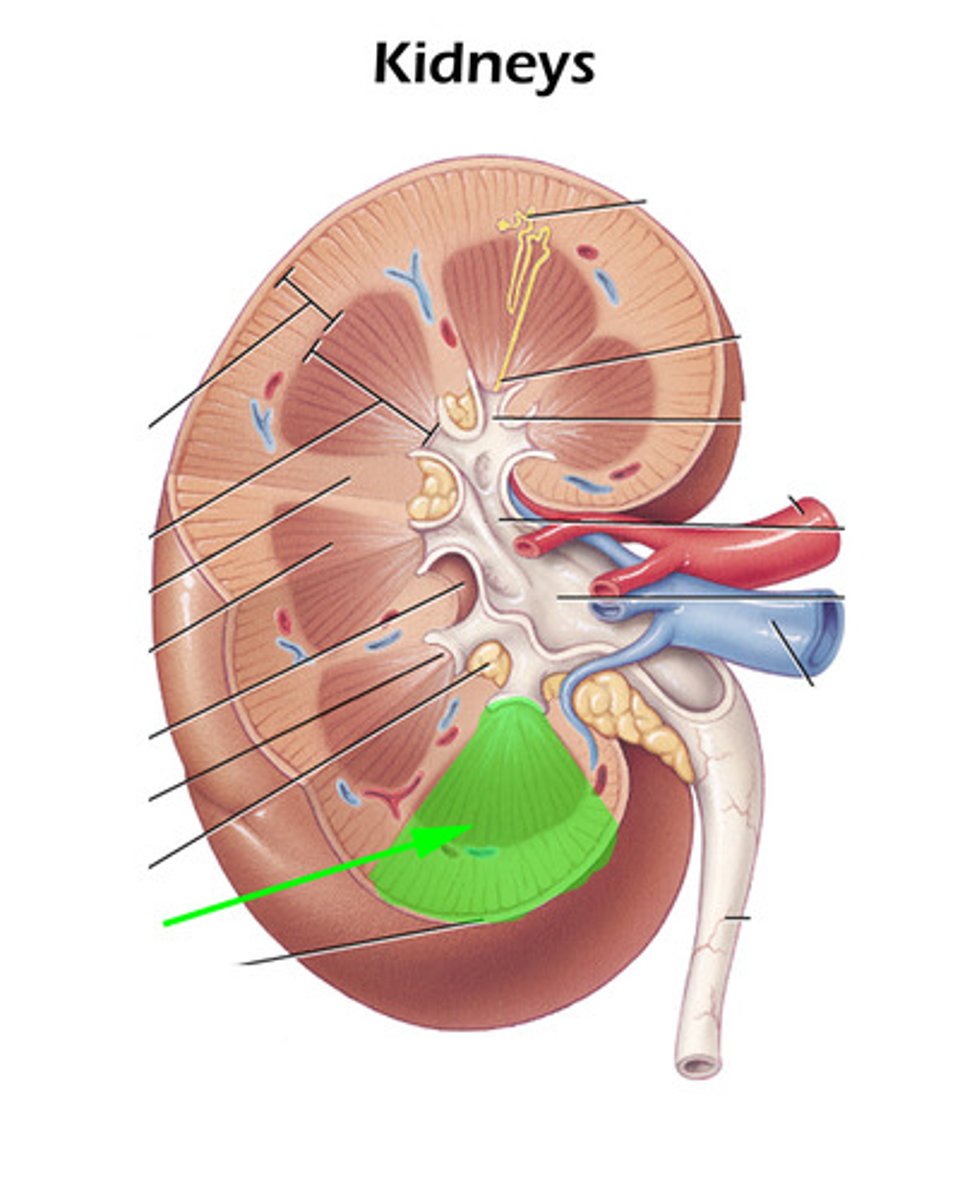
Minor calyx
Collects urine from a single renal lobe
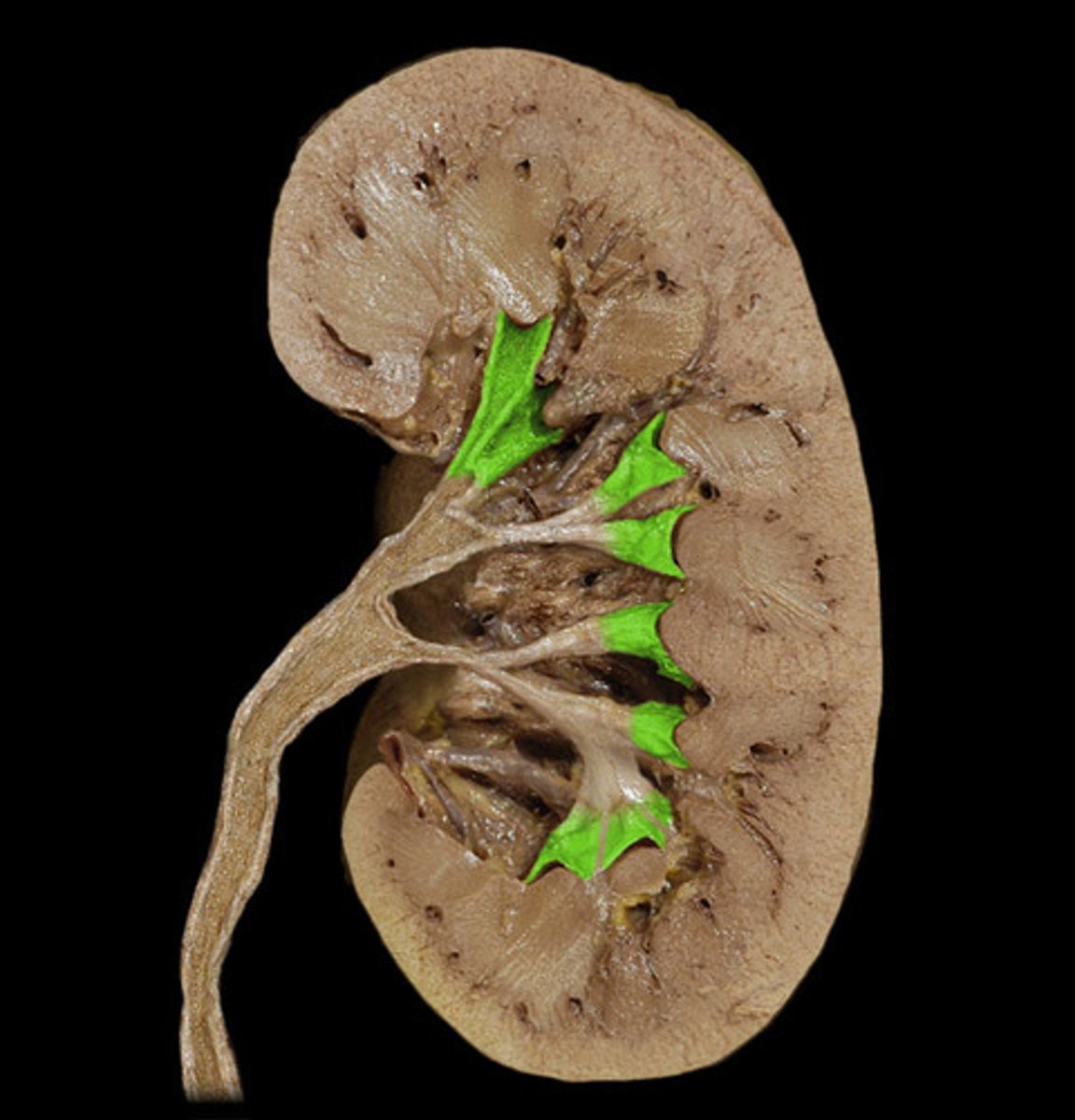
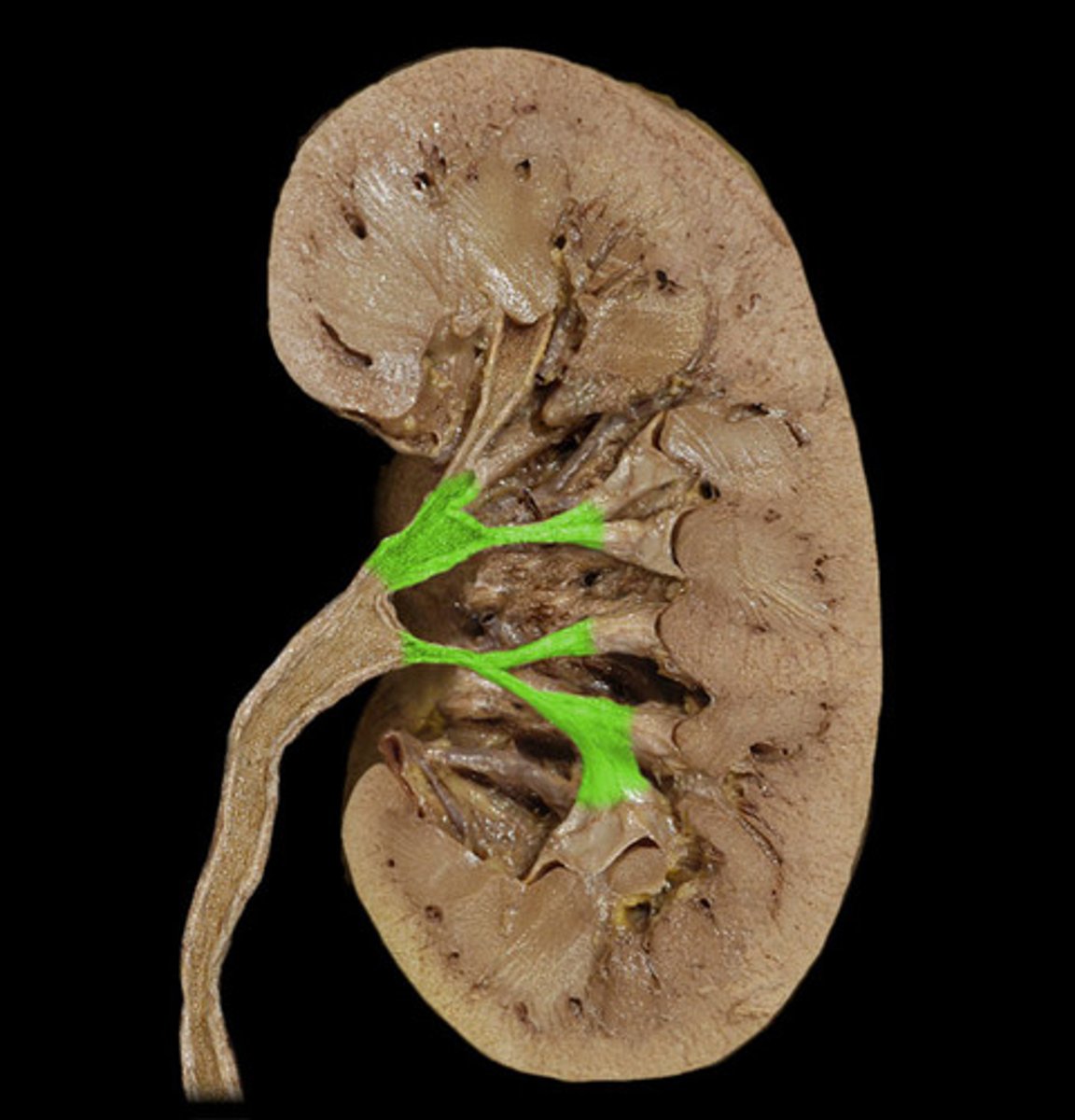
Major calyx
Receives urine from multiple minor calyces
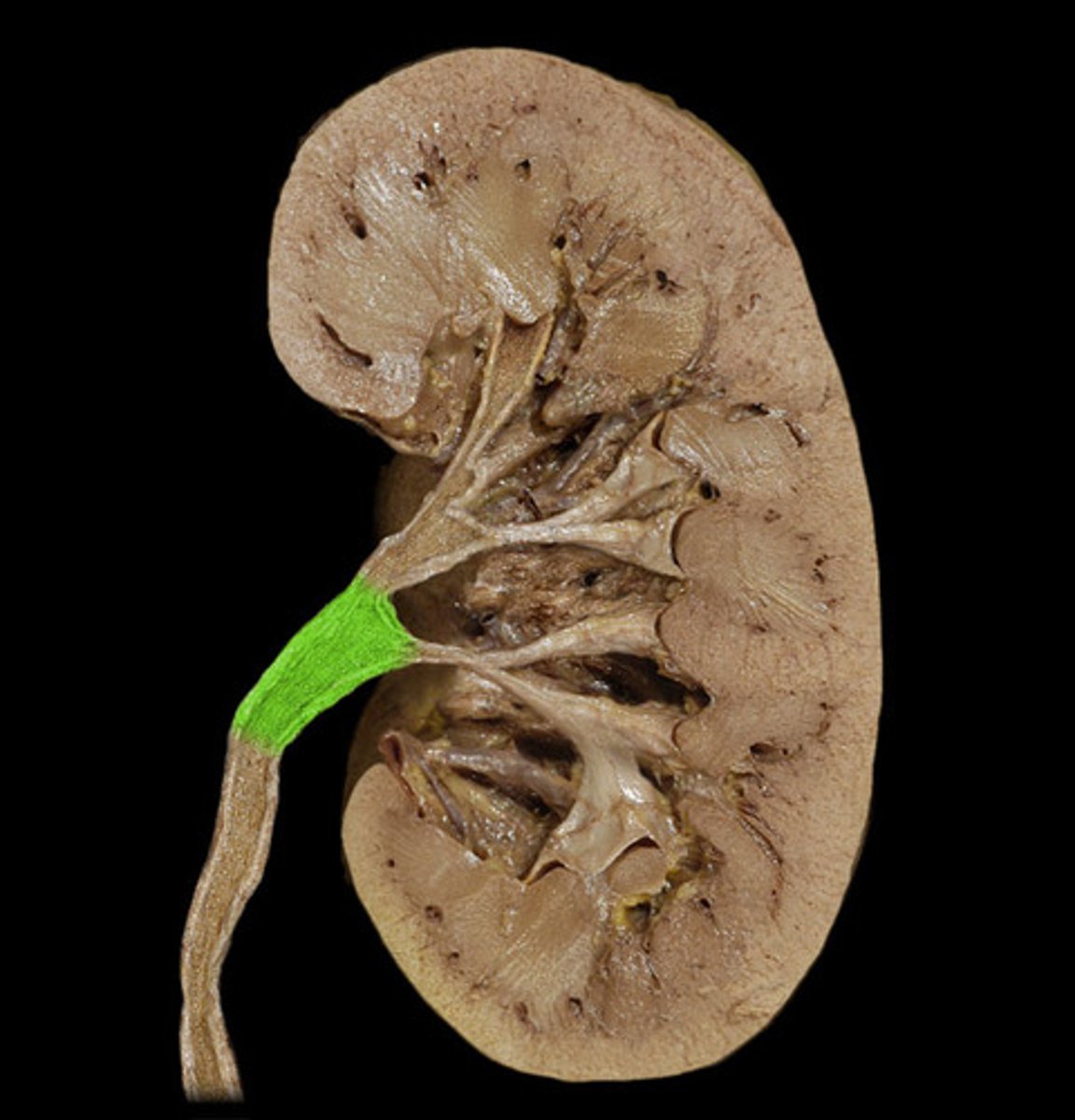
Renal pelvis
funnel-shaped reservoir that collects the urine and passes it to the ureter
renal papilla, minor calyx, major calyx, renal pelvis, ureter, urinary bladder
What is the flow of urine from a renal papilla to the urinary bladder?
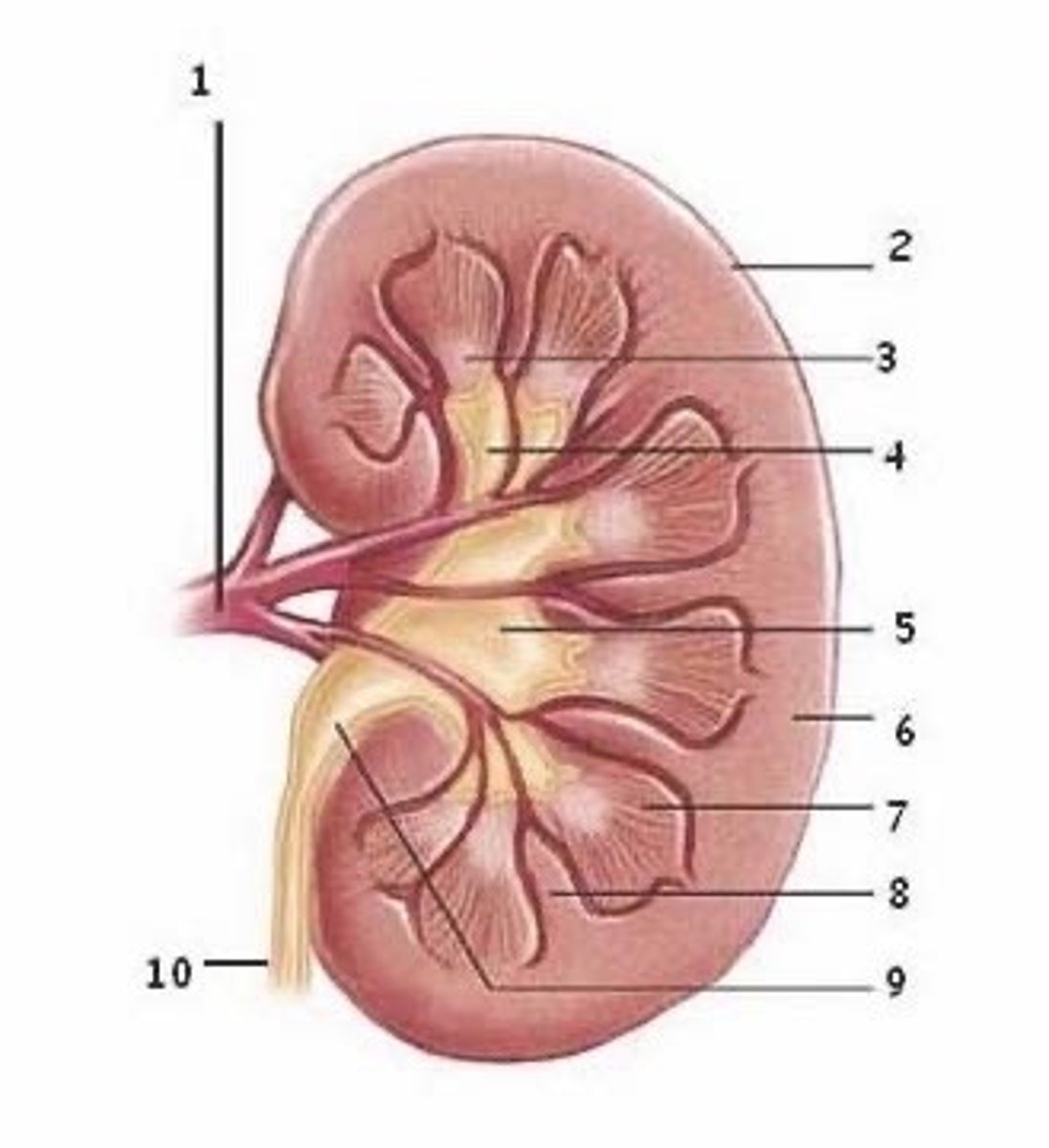
urinary bladder, ureters, renal pelvis, major calyx, minor calyx, renal papilla
What is the flow of urine BACKWARDS from a renal papilla to the urinary bladder?
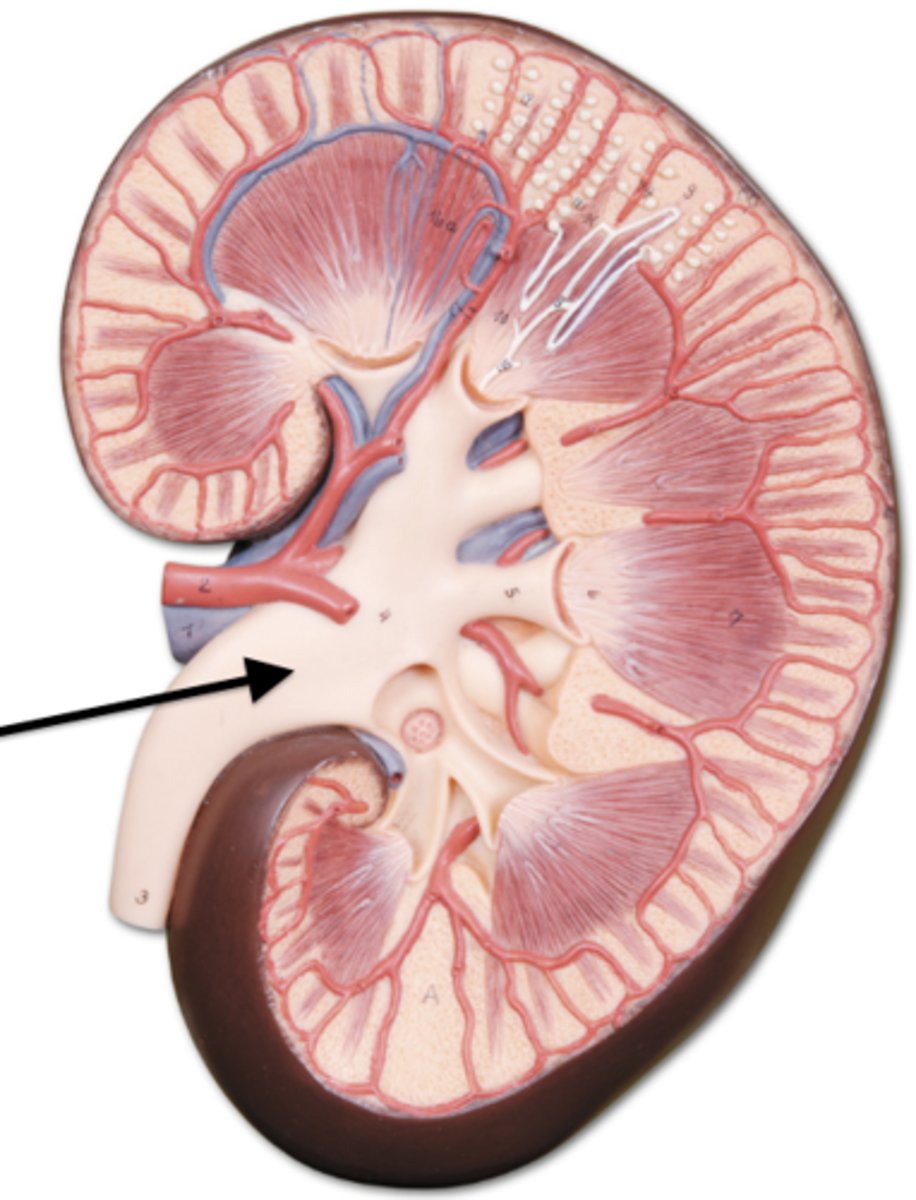
cortex, medulla, pelvis
Arrange the regions of the kidney in the order from superficial to deep.
- renal medulla
- renal pelvis
- renal cortex
Ureter
structures that transport urine from kidneys to bladder
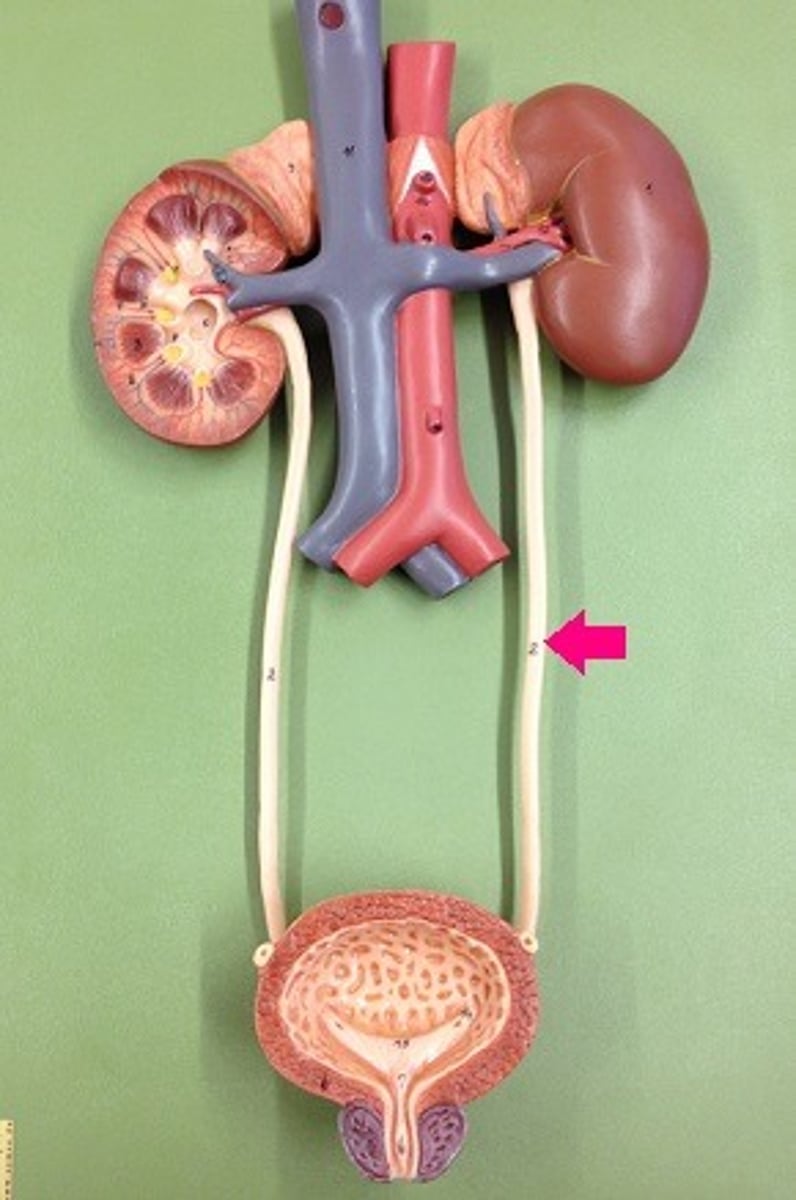
Peristalsis
Smooth muscle contractions that move urine
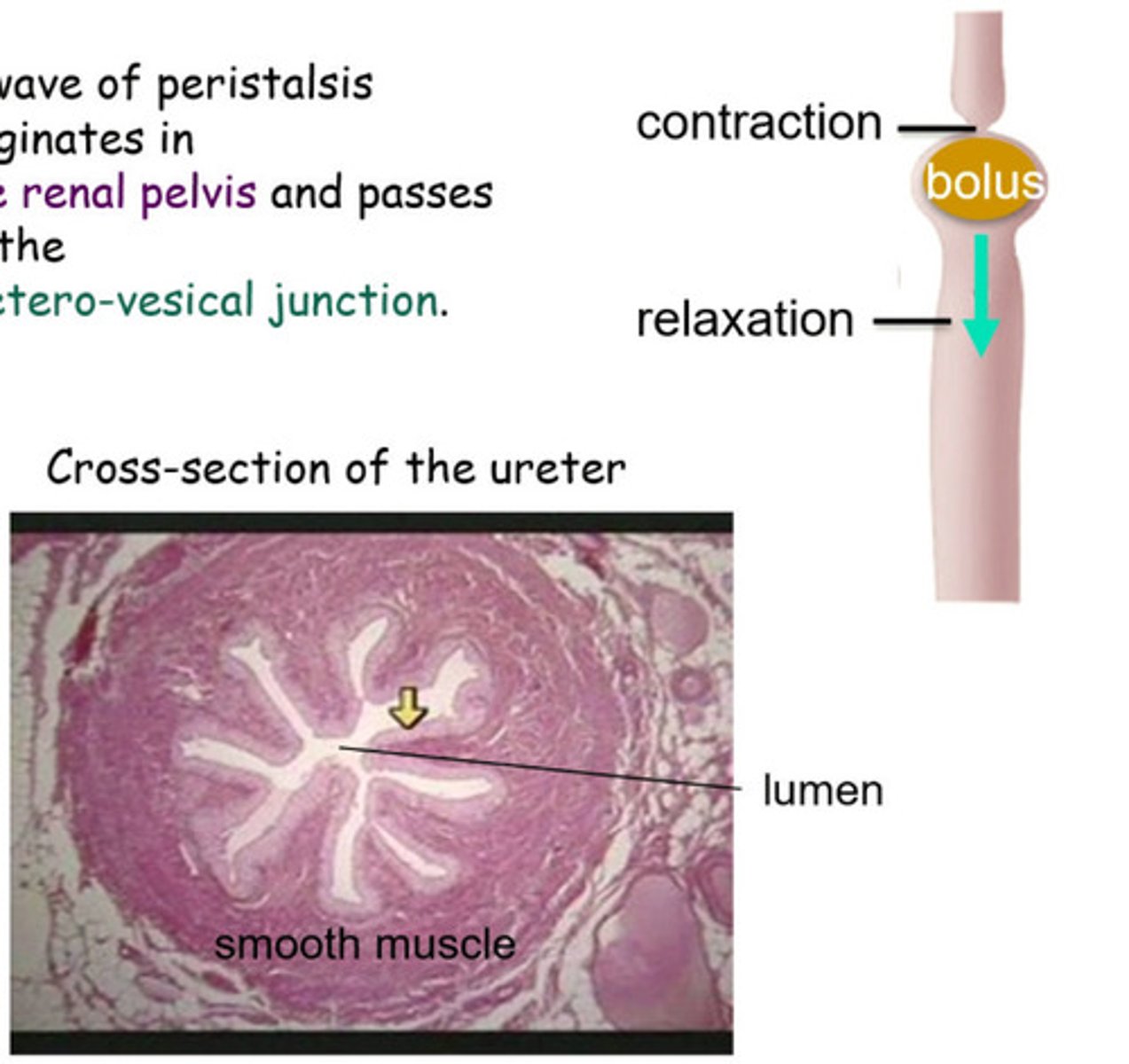
Anti-reflux design
Ureters enter bladder at an oblique/posterior angle to prevent backflow
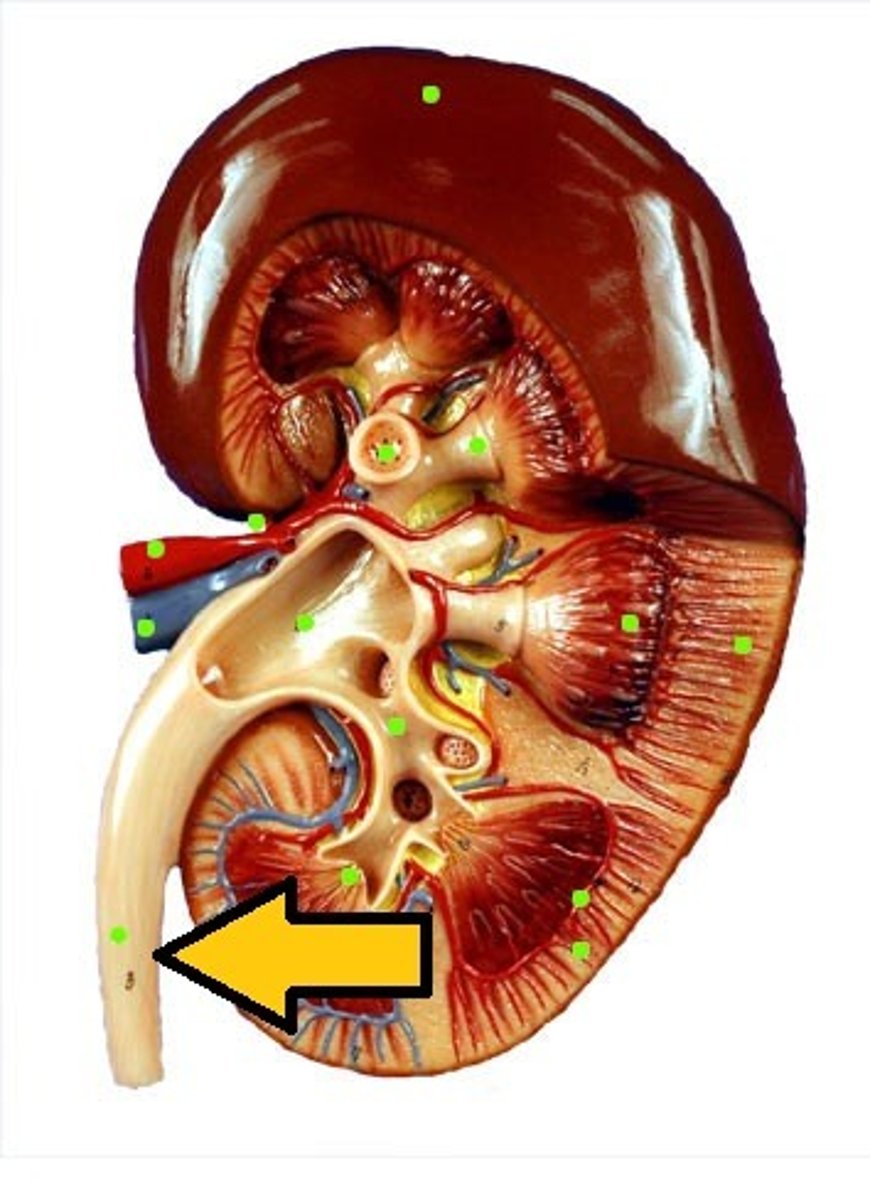
compresses distal ureters
Increased bladder volume _______ ________ to prevent reflux
Ureter mucosa
Transitional epithelium that stretches
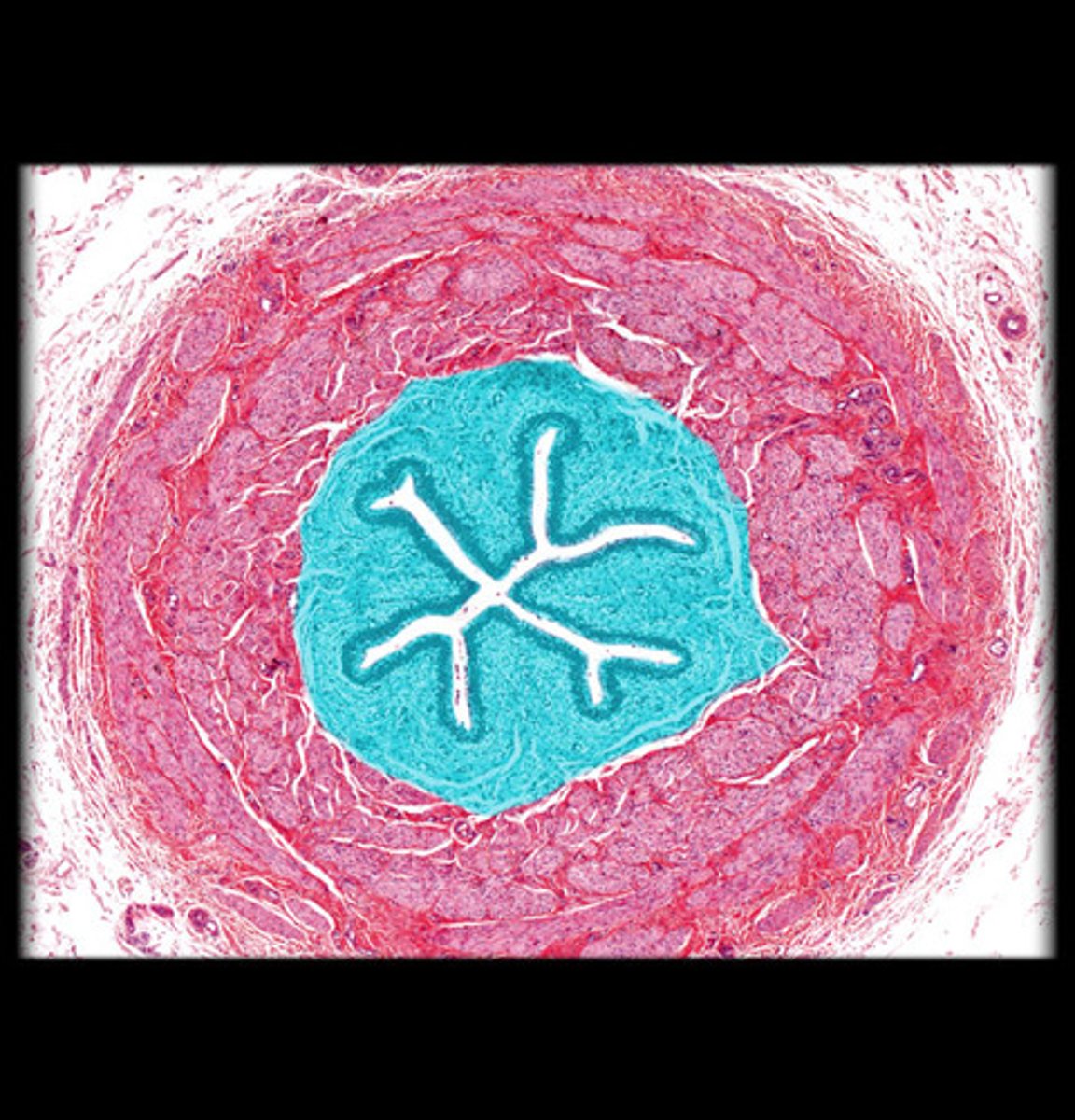
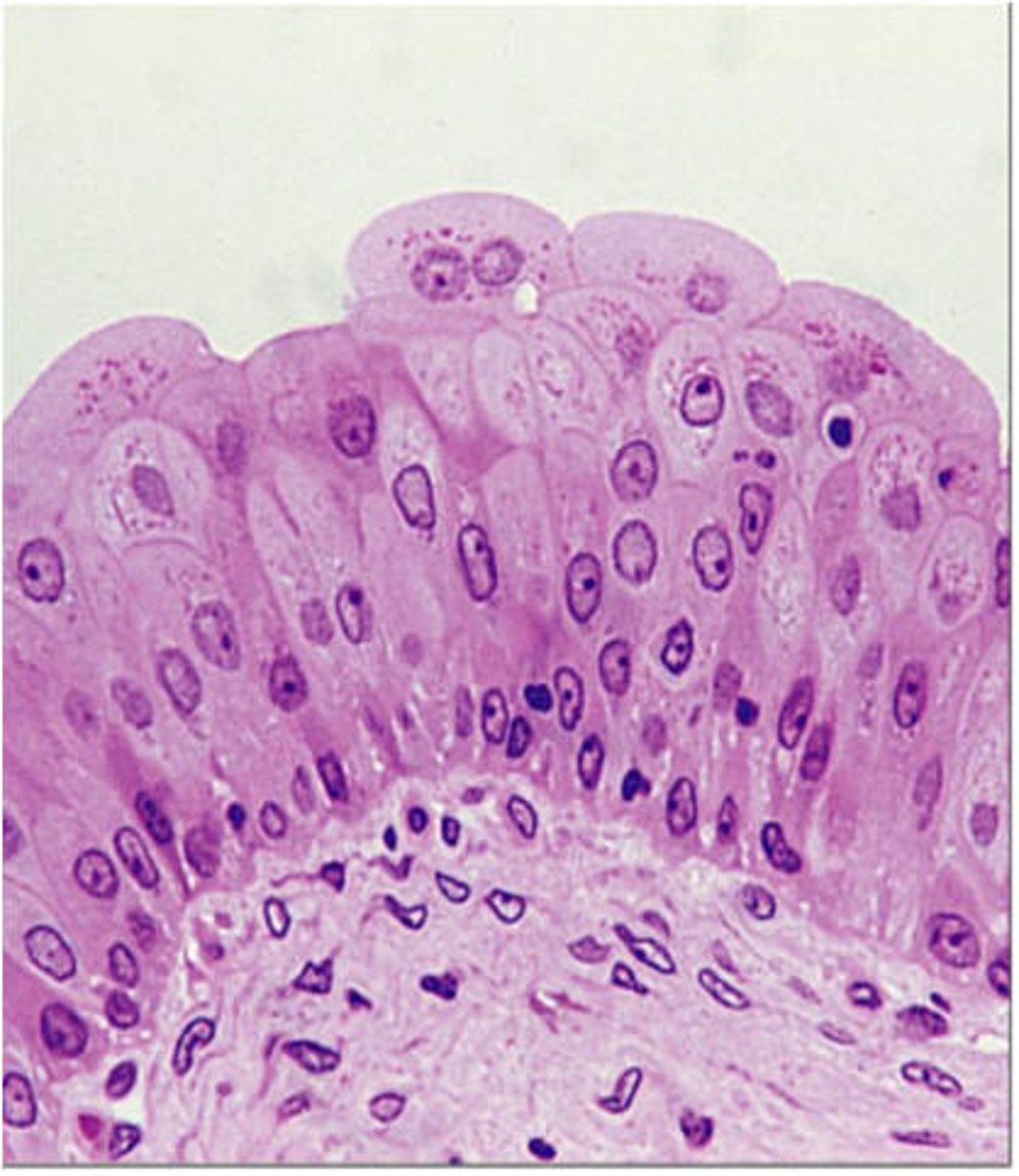
transitional epithelium
type of tissue that stretches readily and permits distension (expansion) of urinary organ by contained urine
- lines the ureters, urinary bladder, and part of the urethra
Ureter muscularis
Smooth muscle that generates peristalsis
- senses distention with urine filling and triggers reflexive peristalsis
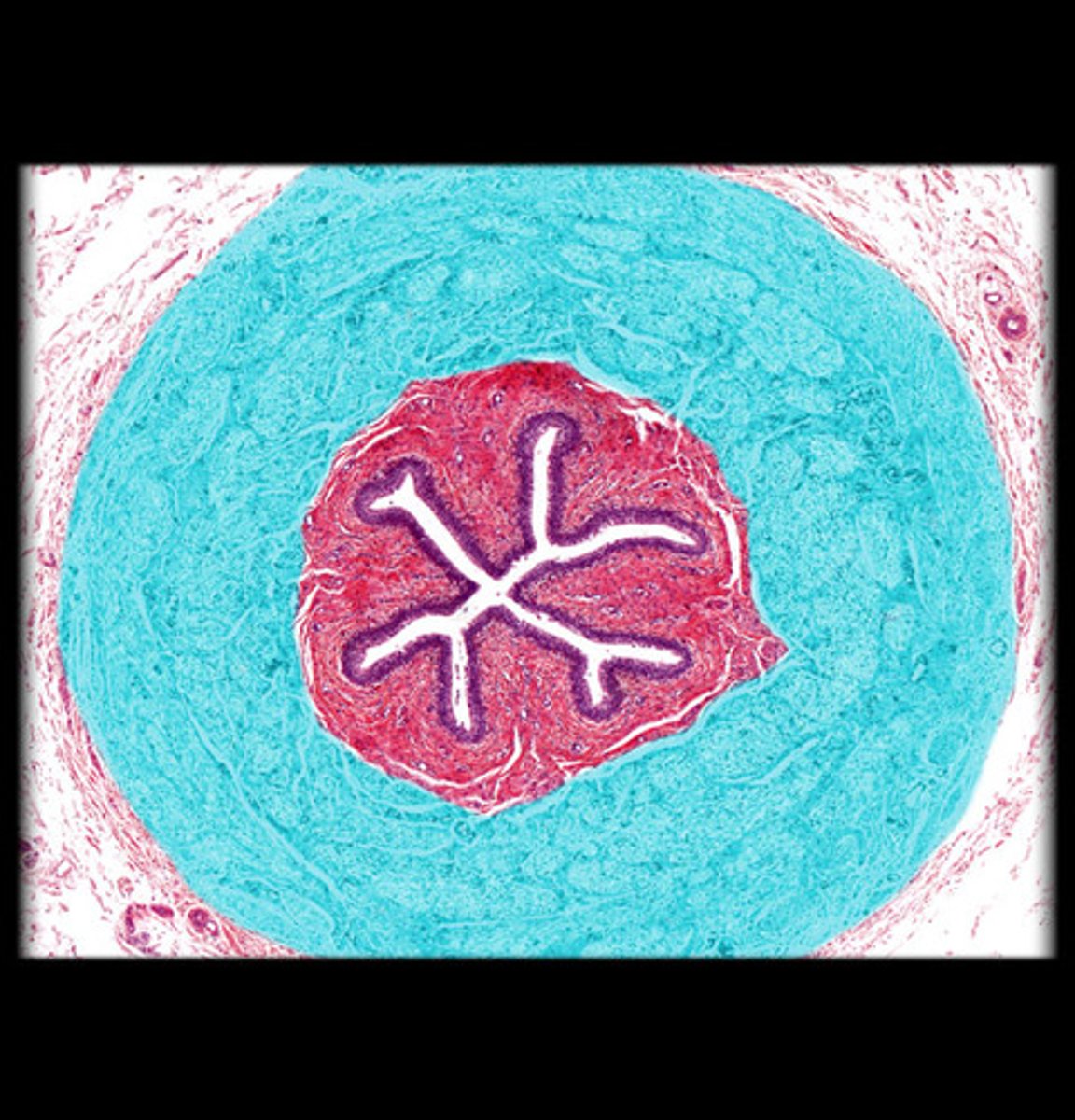
Ureter adventitia
Outer fibrous connective tissue anchoring ureter in place
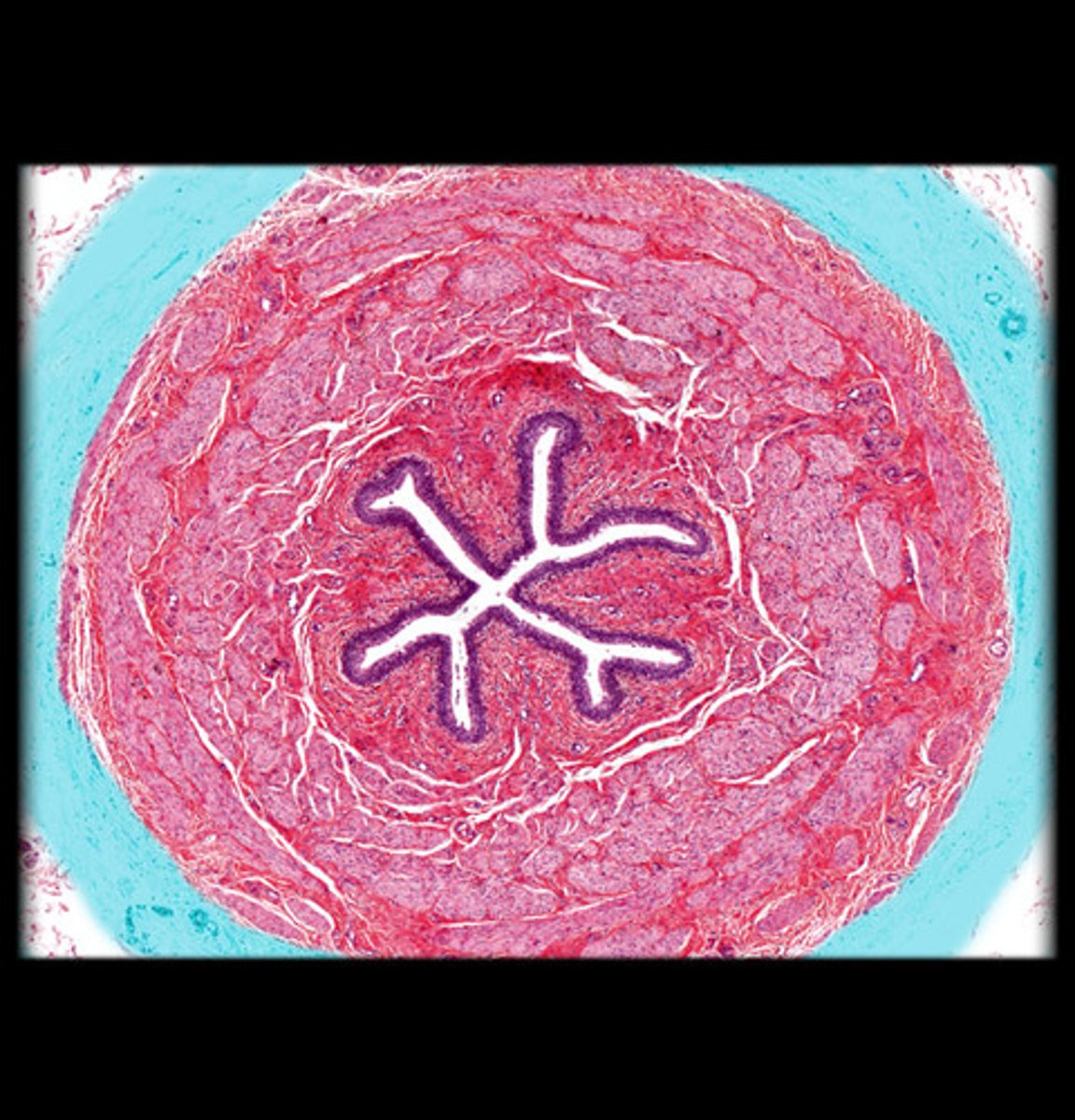
Mucosa, muscularis, adventitia
What are the 3 ureter layers from deep to superficial?
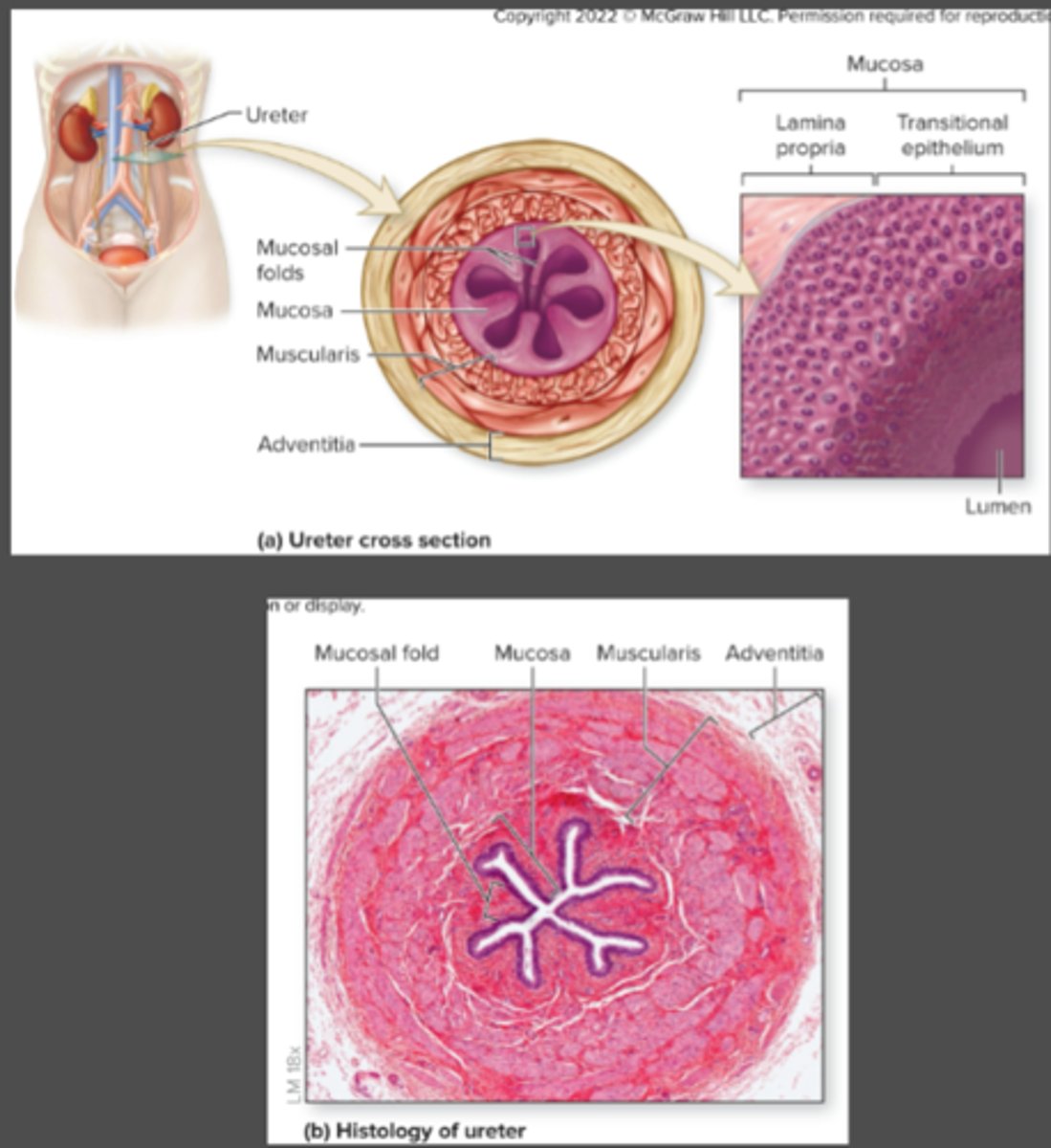
Adventitia, muscularis, mucosa
What are the 3 ureter layers from superficial to deep?
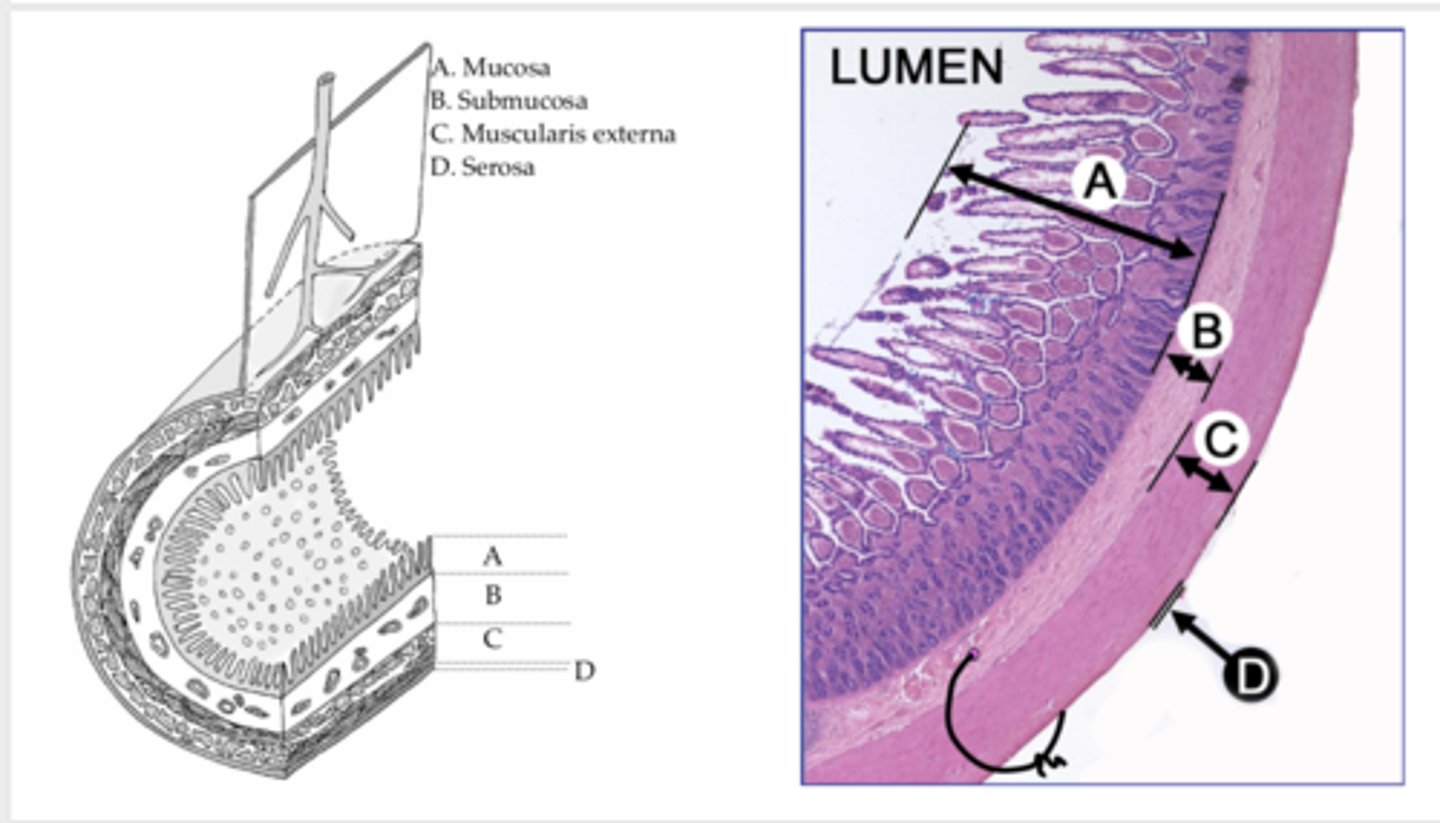
muscularis layer
The _______ layer of the ureter mucosa contracts to move urine by peristalsis.
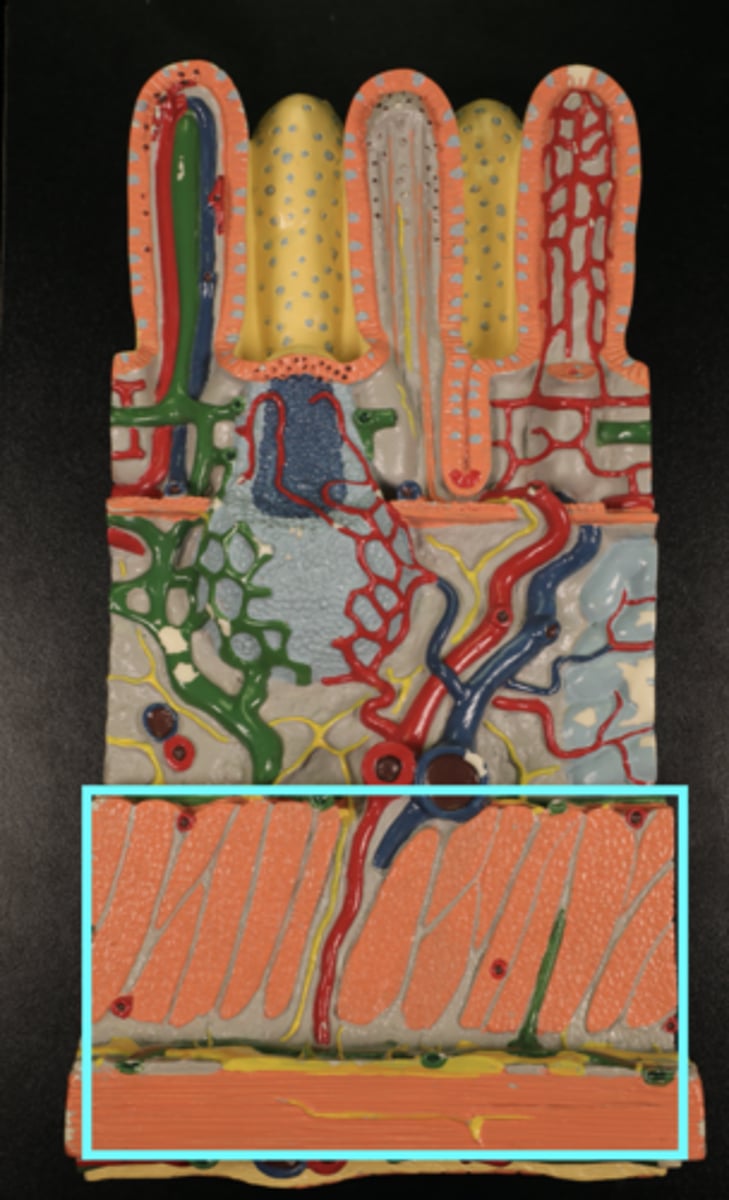
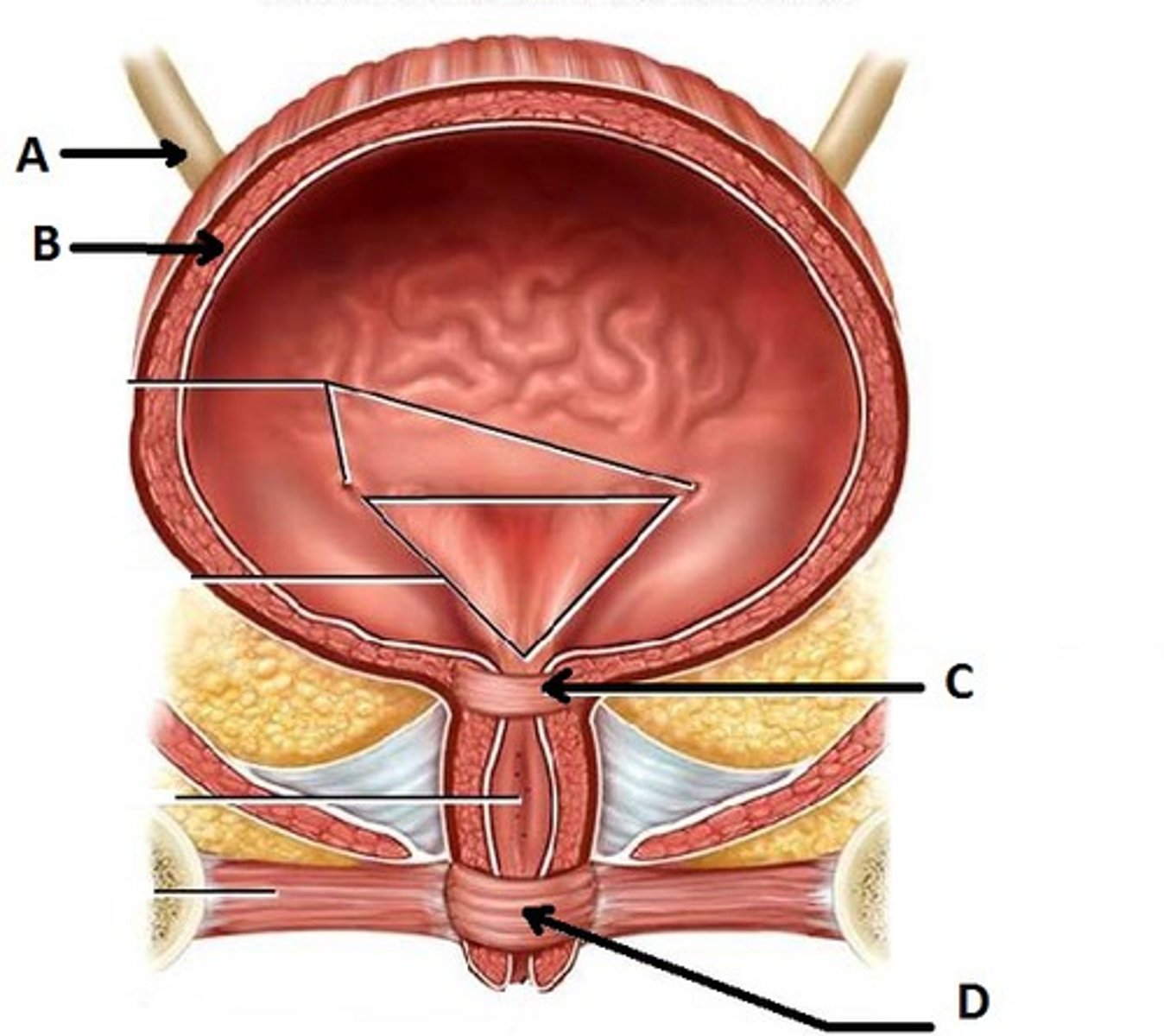
Trigone
Triangular region between ureter openings and urethra
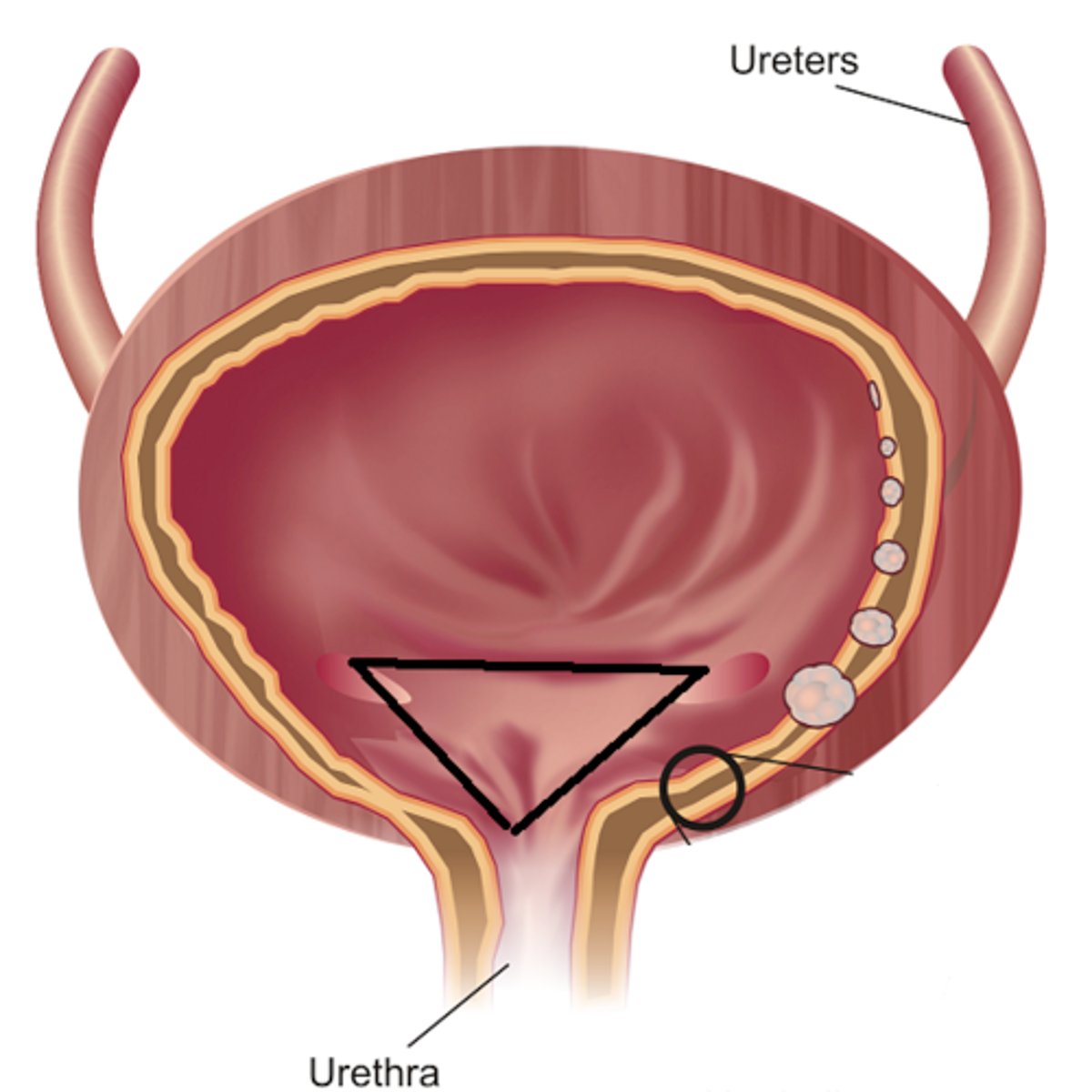
Bladder mucosa
Transitional epithelium forming rugae
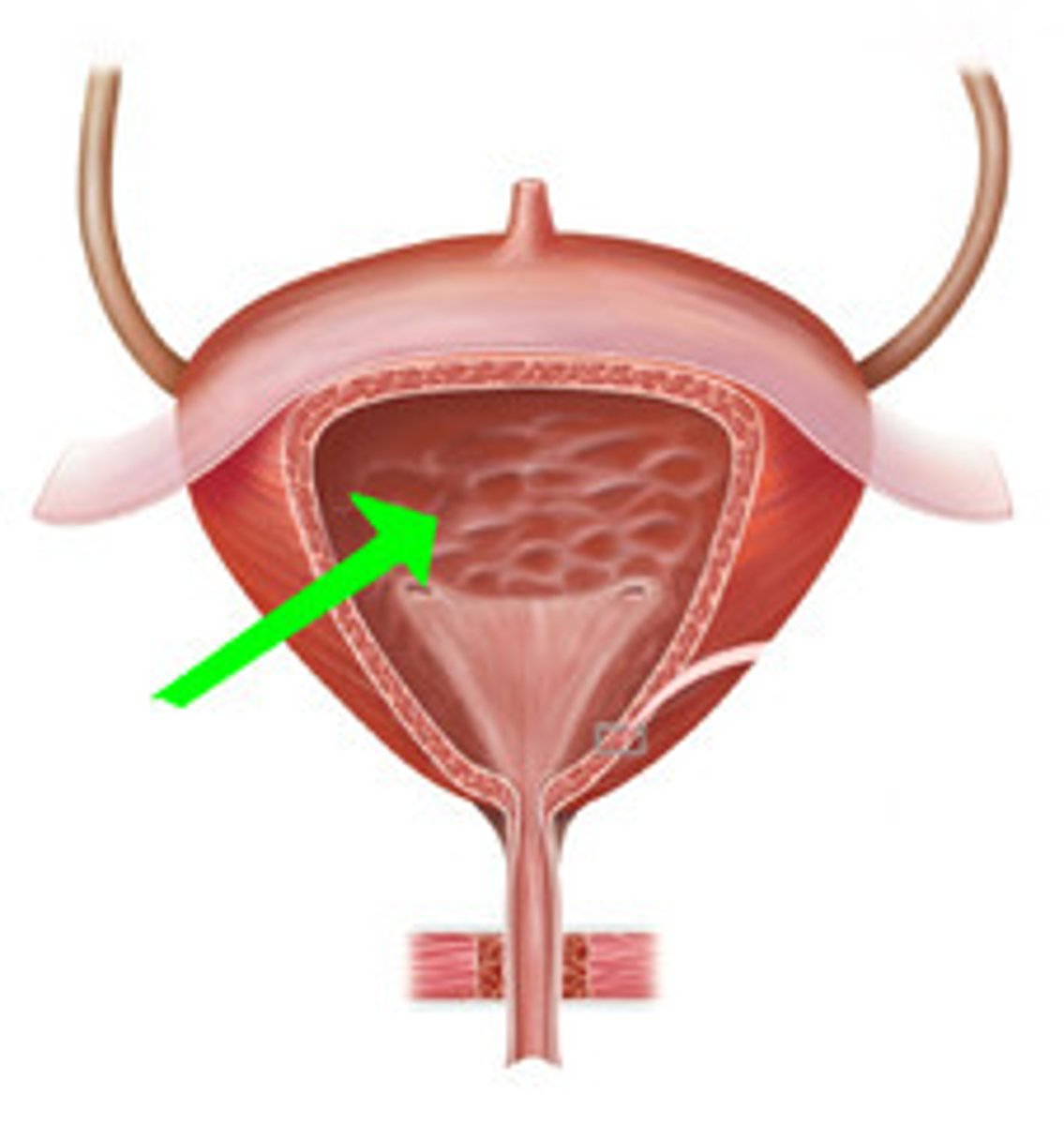
Rugae
series of folds of transitional epithelium in the mucosa lining the bladder
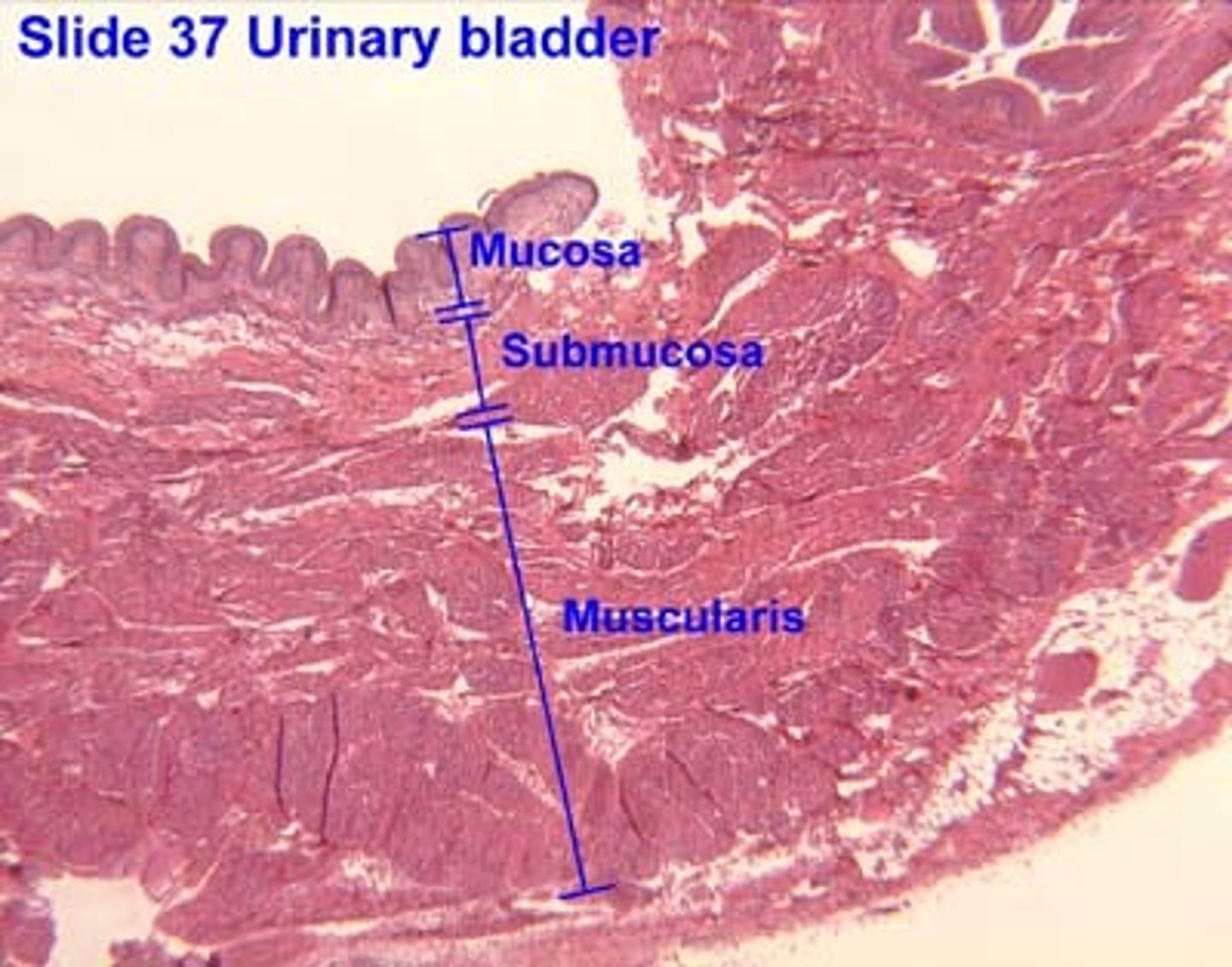
Detrusor muscle
Smooth muscle that contracts to drive urination
- is usually relaxed, but contracts to squeeze urine out of bladder
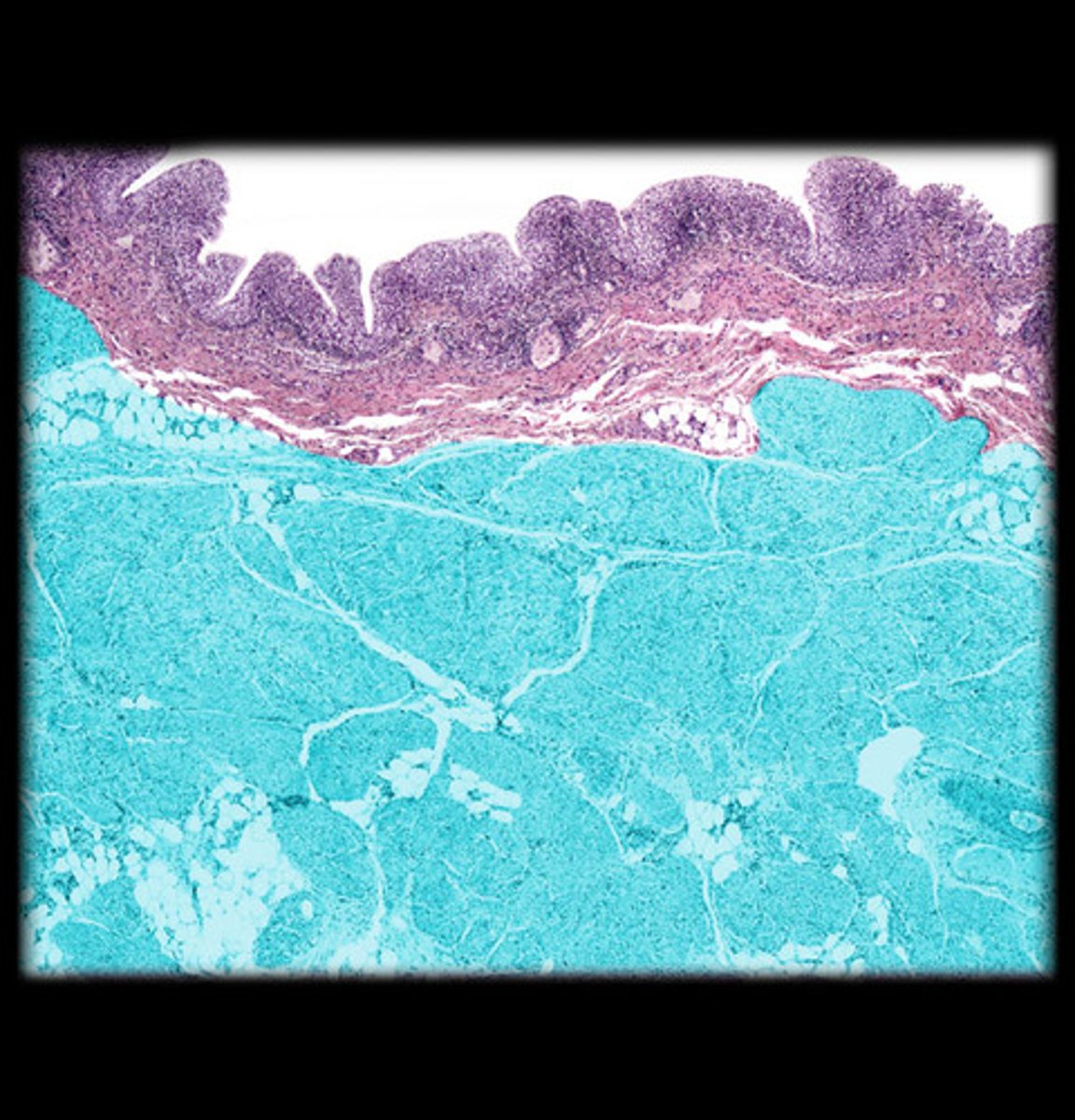
inner mucosa and detrusor
bladder layers to remember...
(just whats on slides lol)
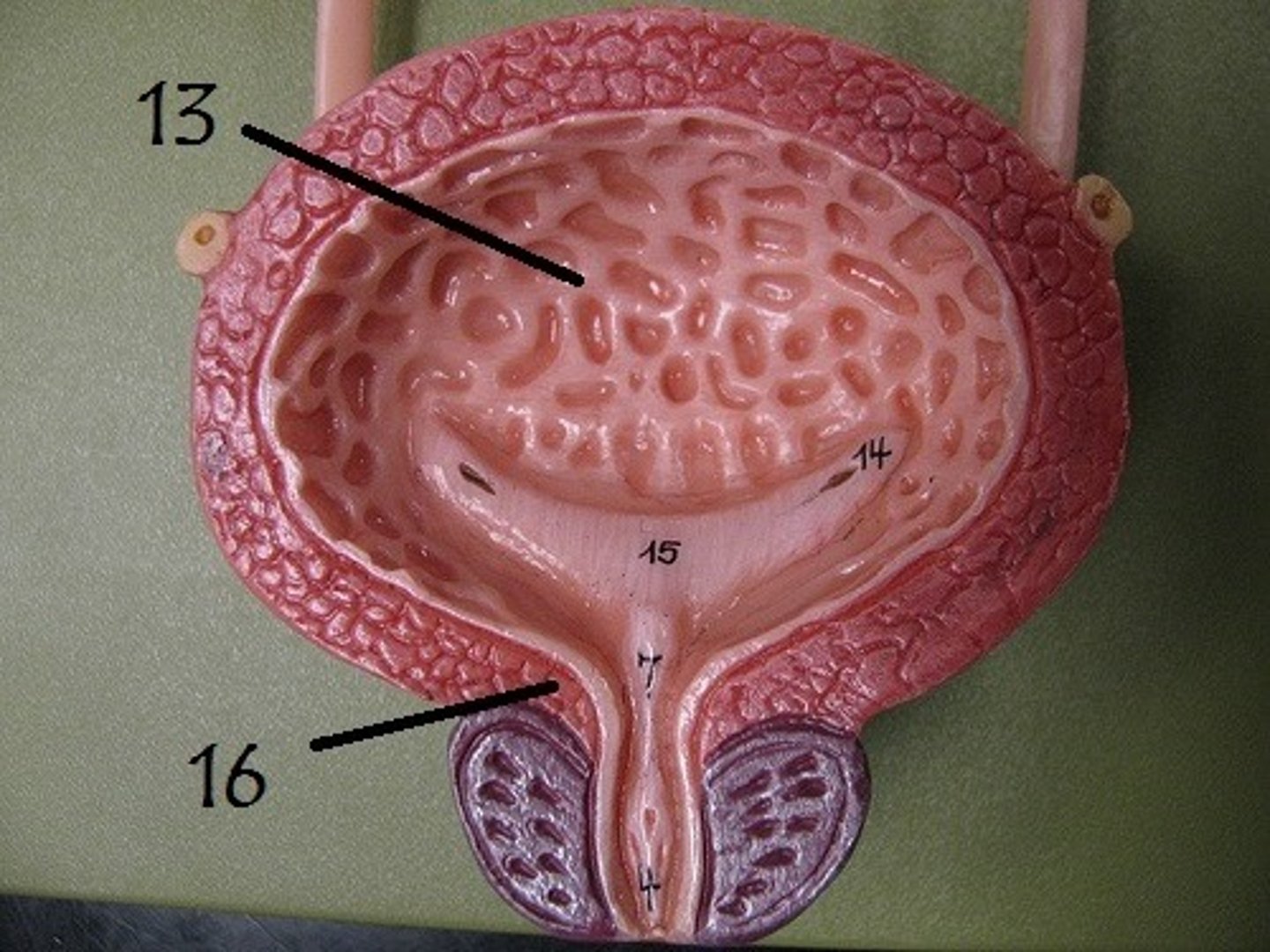
Internal urethral sphincter
thick involuntary smooth muscle at bladder-urethra junction that contracts to open
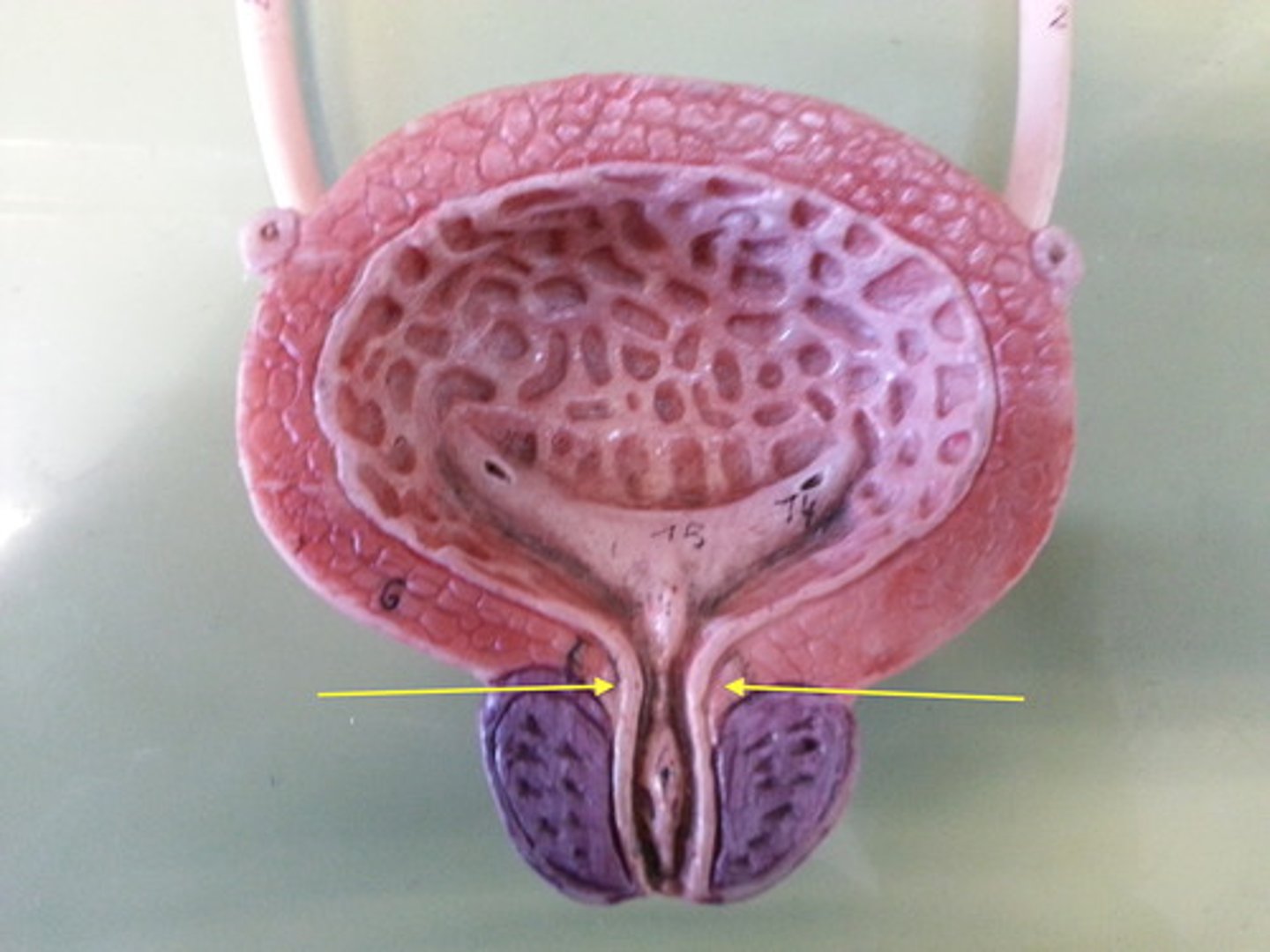
External urethral sphincter
Voluntary skeletal muscle ring surrounding the urethra as it passes through the pelvic floor, on its way out.
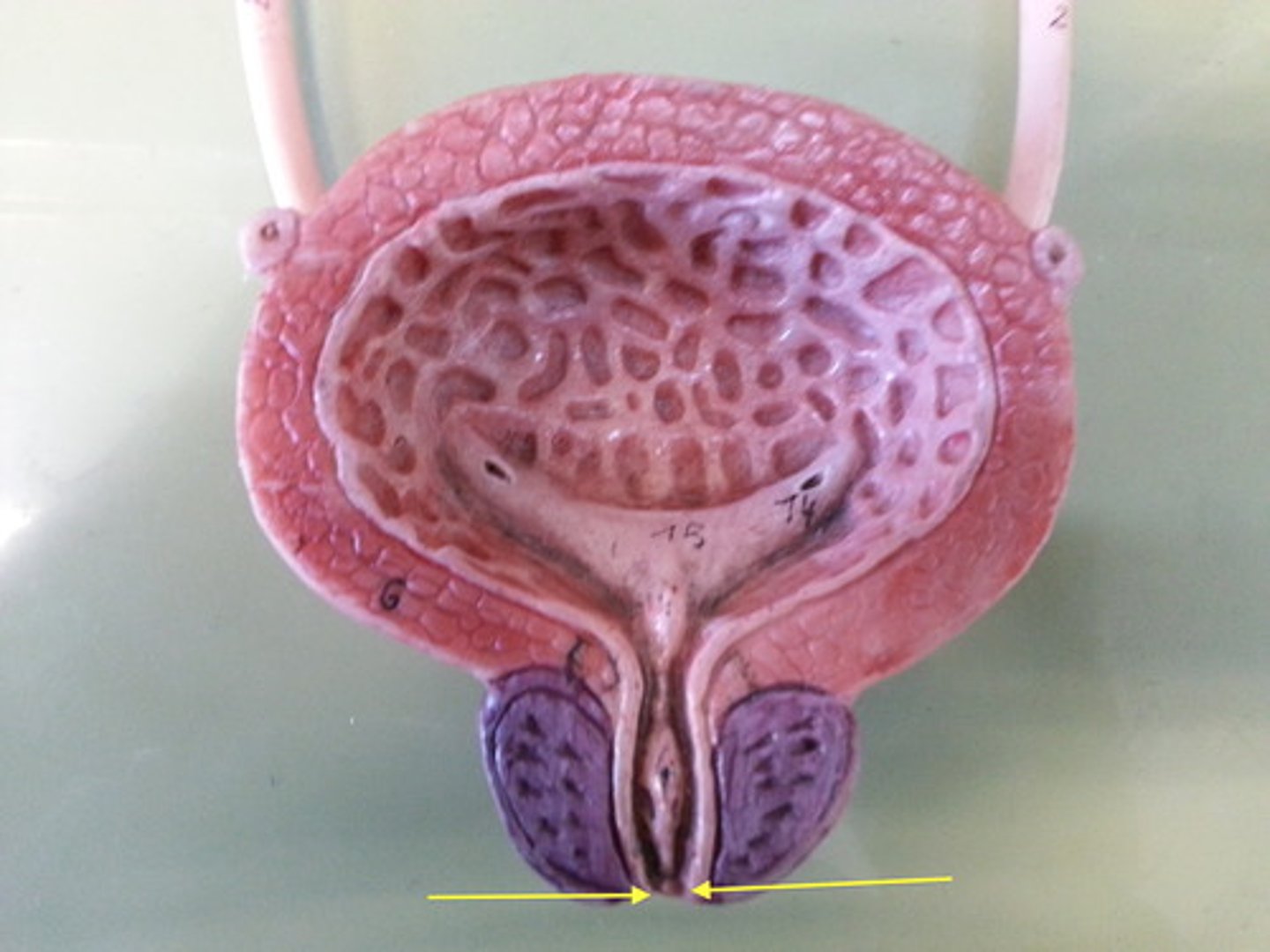
Stratified squamous for protection
Epithelium (transitions to this type of tissue) near urethra opening is made of-
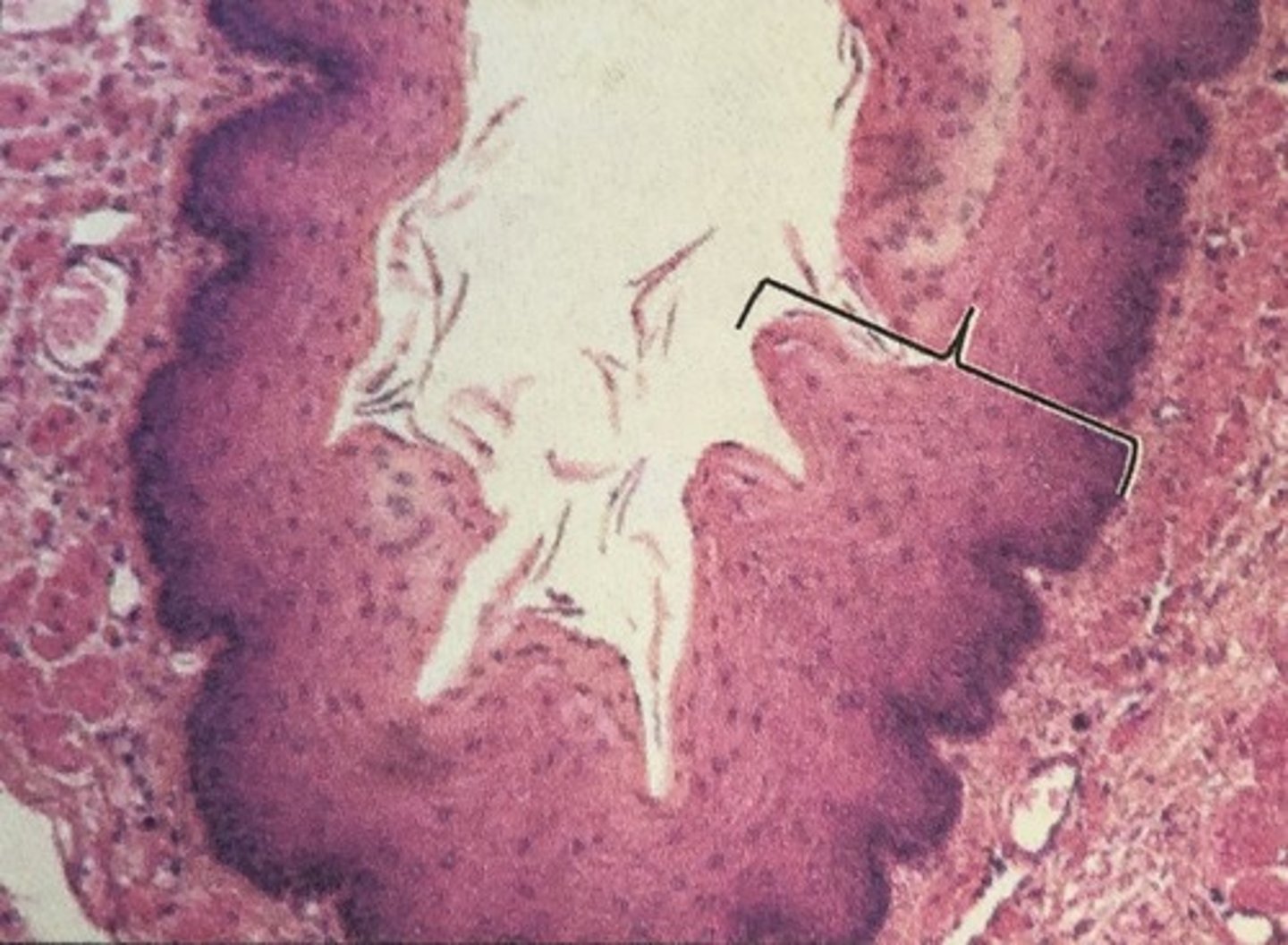
3-5 cm, only urine
The Female urethra is ____ cm long and transports ______.
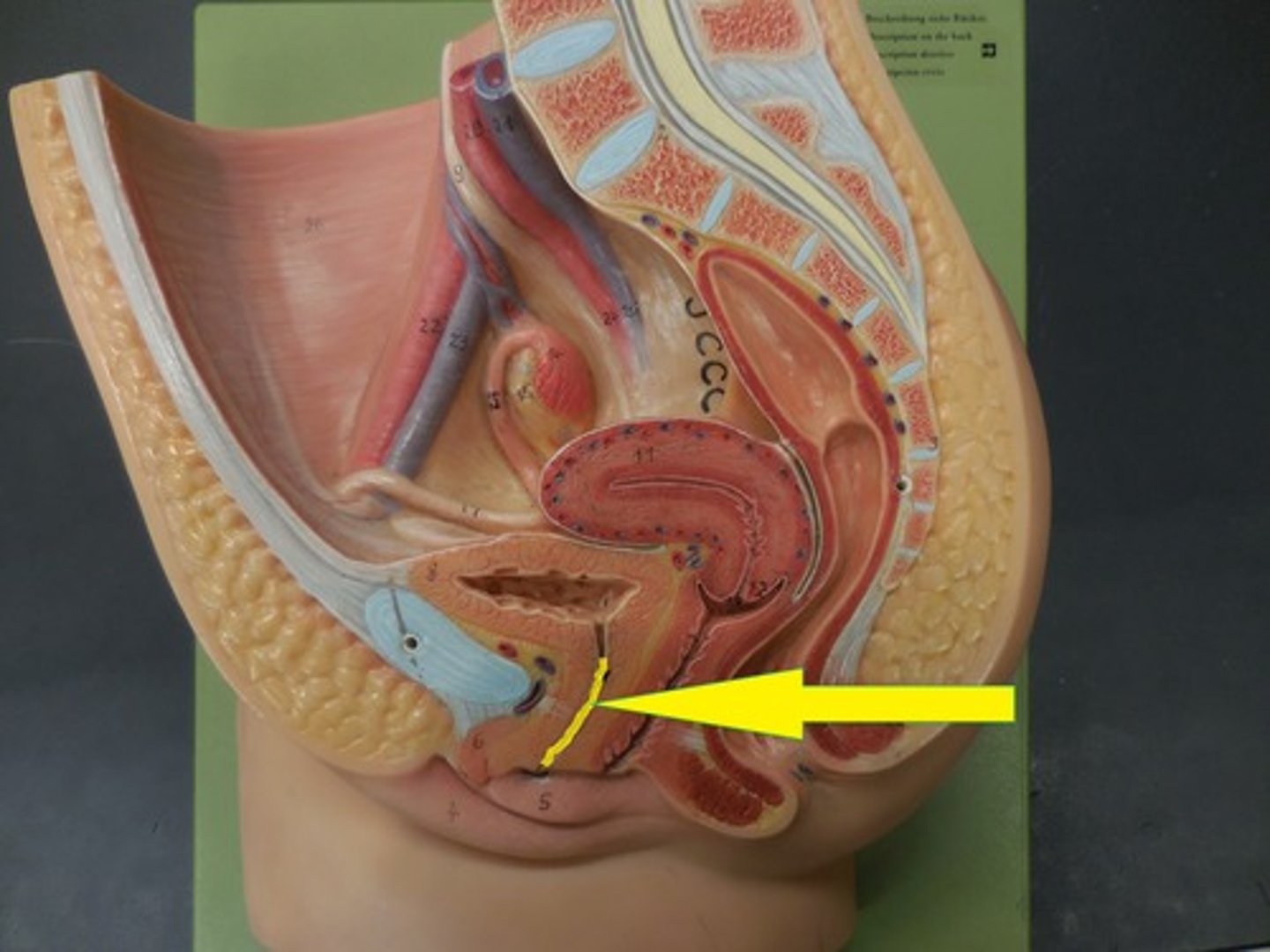
~20 cm, urine and semen
The Male urethra is ____ cm long and transports ______.
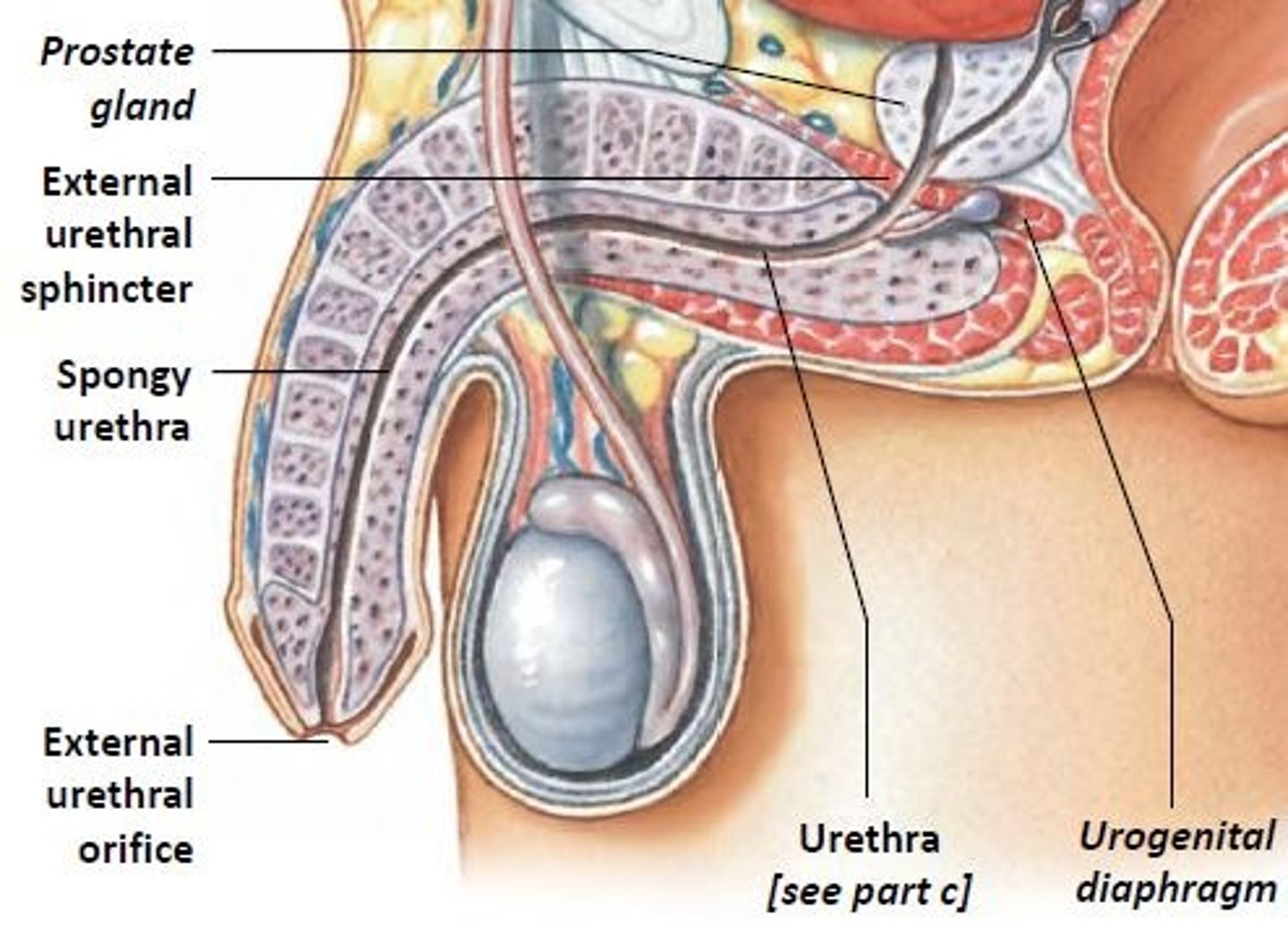
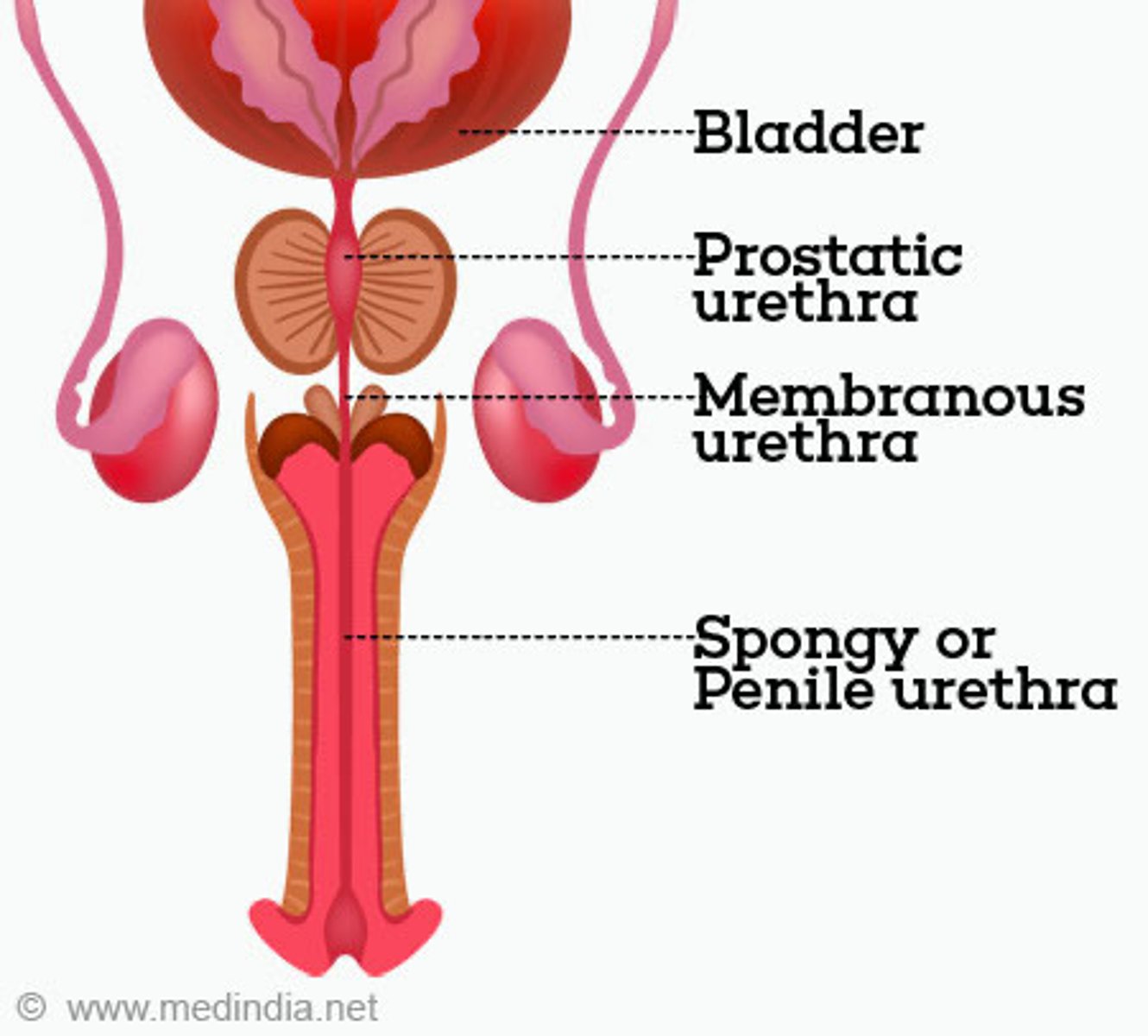
spongy urethra, membranous urethra, prostatic urethra
What are the regions of the male urethra in the order that they would be encountered by a catheter?
(external to bladder)
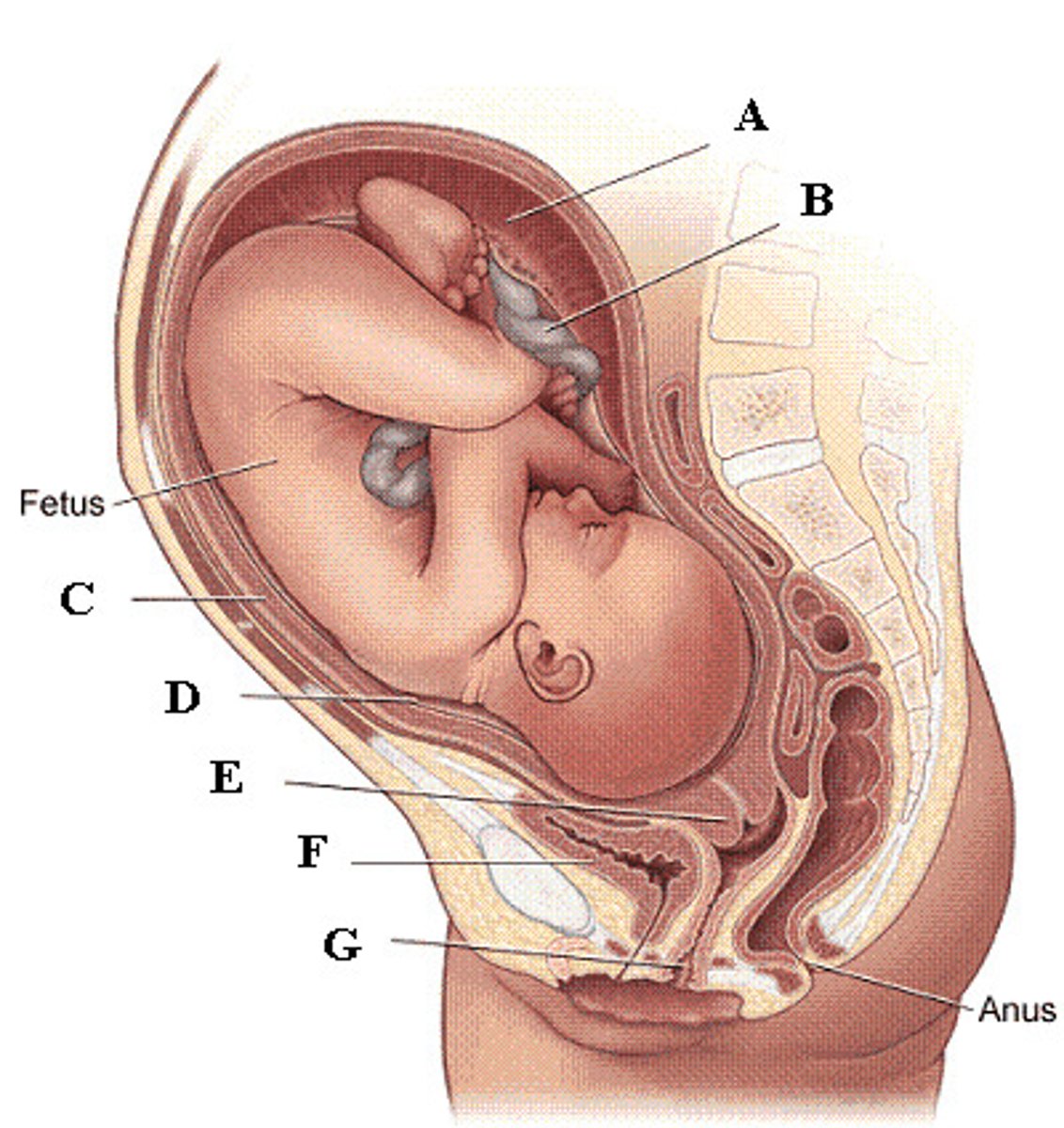
The urinary bladder in females is anterior to the uterus, vagina, and rectum. This arrangement limits its capacity during pregnancy, as it is crowded by the growing uterus.
Why do pregnant women urinate with greater frequency?
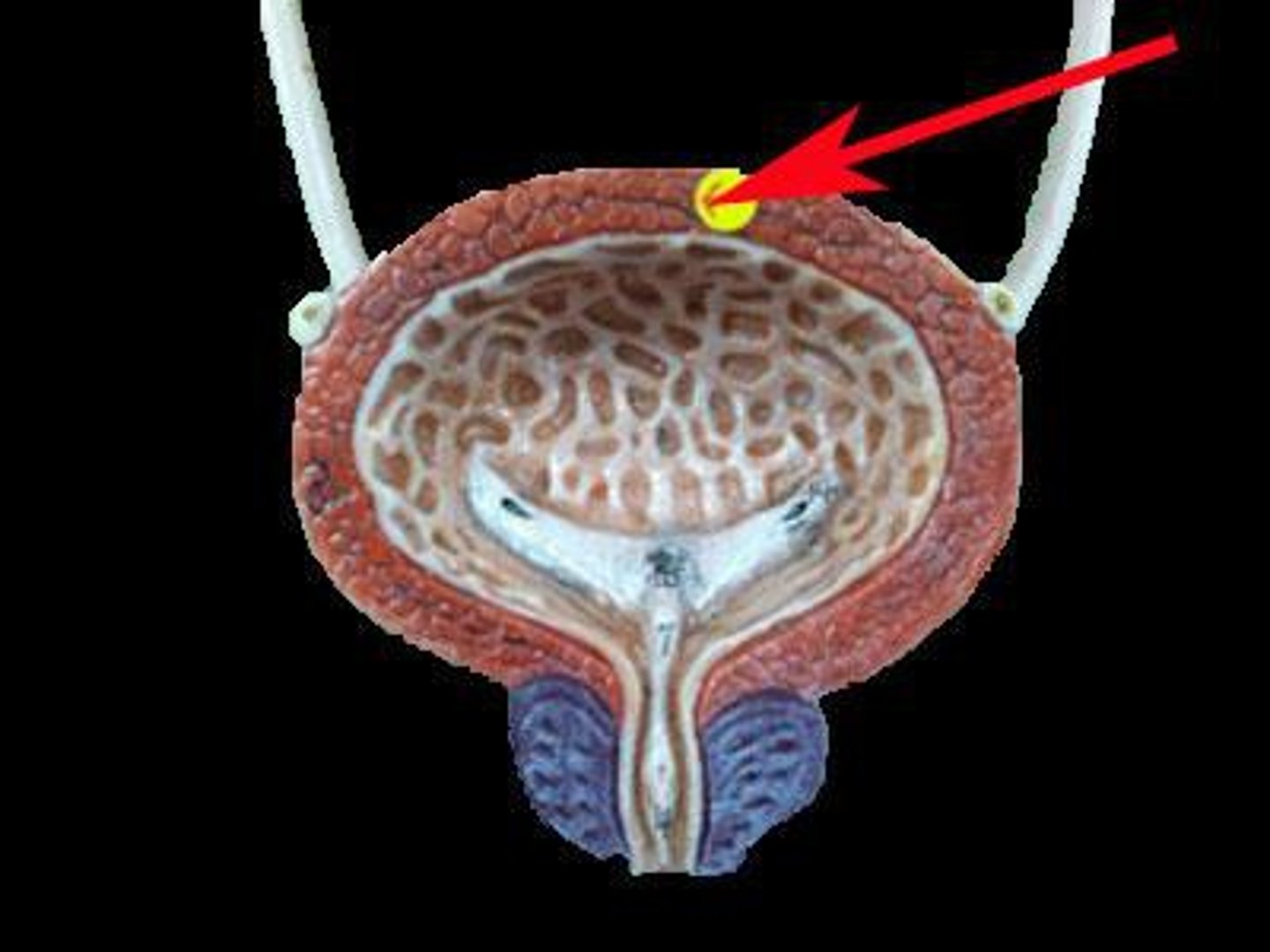
relaxed (filling), passively contracted, contracted
During sympathetic stimulation (higher CNS input), the bladder is ________.
Internal sphincter is __________, external sphincter is ________.
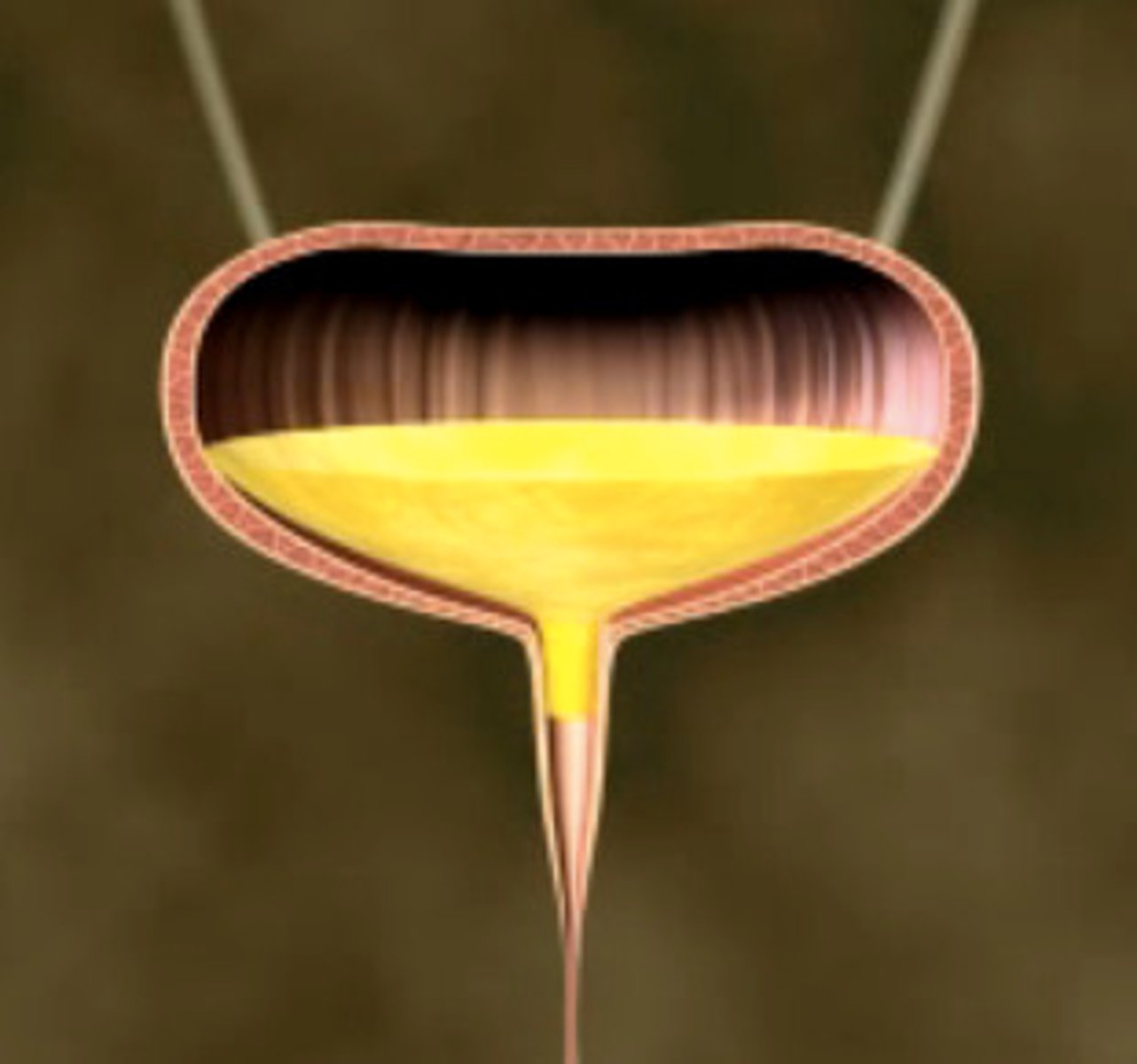
contracted (emptying), passively pulled open, relaxed
During parasympathetic stimulation (lower CNS input), the bladder is ______________.
Internal sphincter is __________, external sphincter is ________.
micturition (voiding)
another term for urination
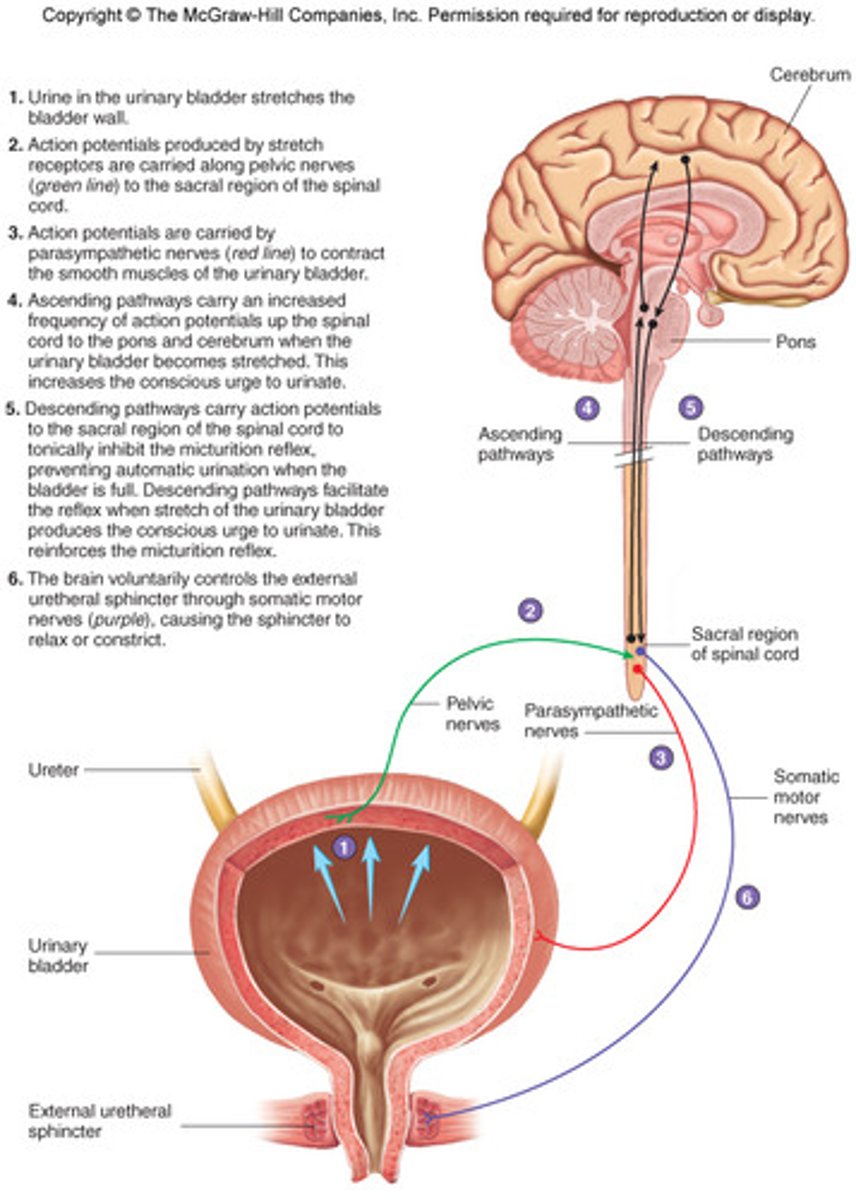
parasympathetic, inhibited, stimulated
detrusor muscle is under _________ control, is _______ during filling and _______ during micturition (emptying)
contract
parasympathetic control causes the detrusor muscle to-
sympathetic, stimulated, inhibited
internal urethral sphincter muscle is under _________ control (to open), is _______ during filling and _______ during micturition (emptying)
close
sympathetic control causes internal urethral sphincter muscle contraction to-
somatic motor, stimulated, inhibited
external urethral sphincter muscle is under _________ control (to open), is _______ during filling and _______ during micturition (emptying)
close
somatic motor control causes external urethral sphincter muscle contraction to-
stretch receptors
receptors that sense bladder muscle stretch and contraction
1. Stretch Receptors fire
2. Parasympathetic neurons fire. Motor Neurons stop firing.
3. Bladder smooth muscle contracts. Internal sphincter is passively pulled apart. External sphincter relaxes.
Steps of micturition via parasympathetic stimulation 💤
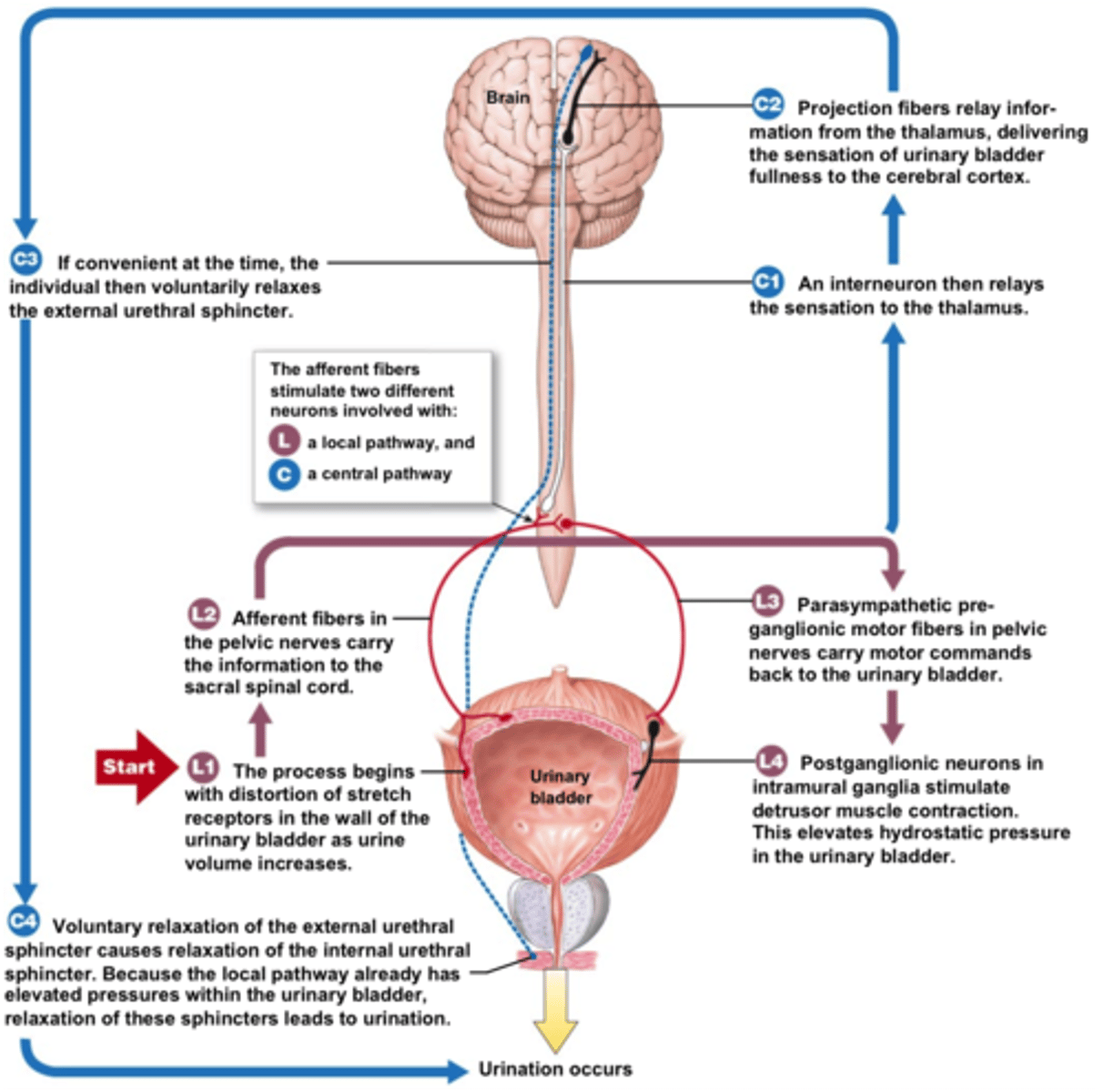
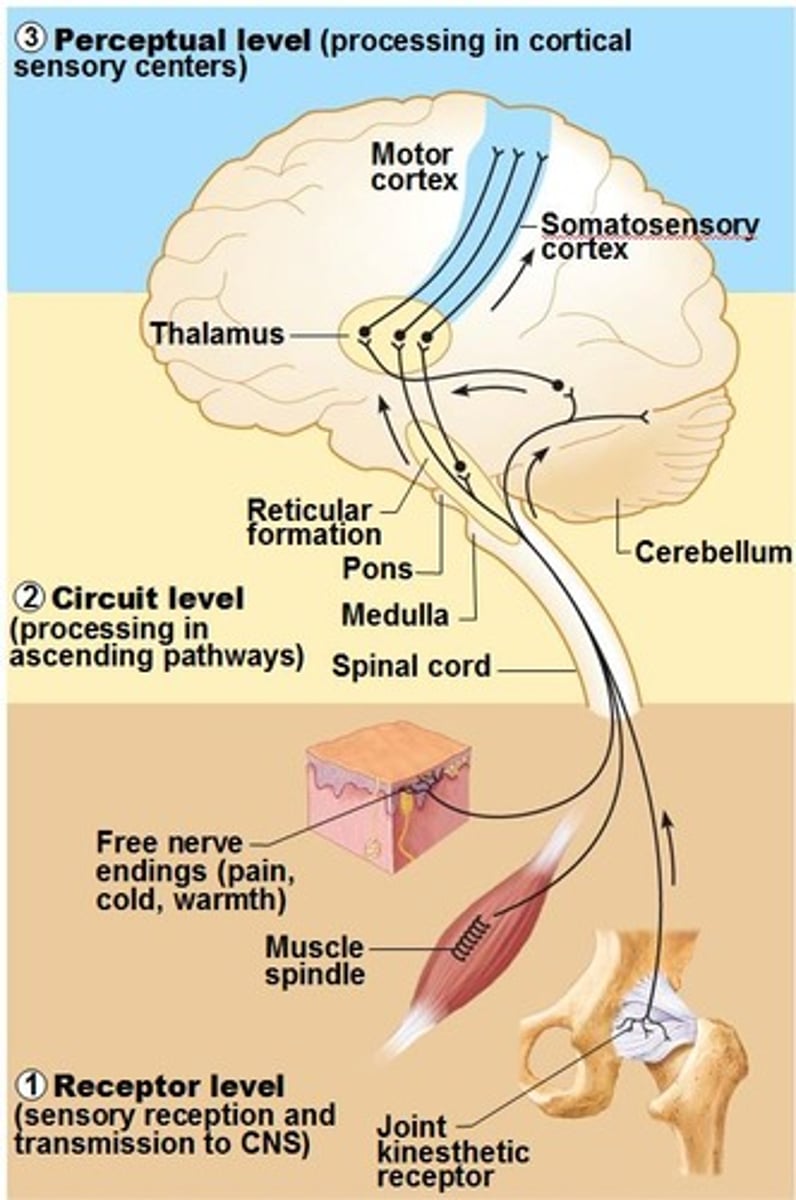
Higher CNS input
________ may facilitate or inhibit the micturition reflex in spinal arc
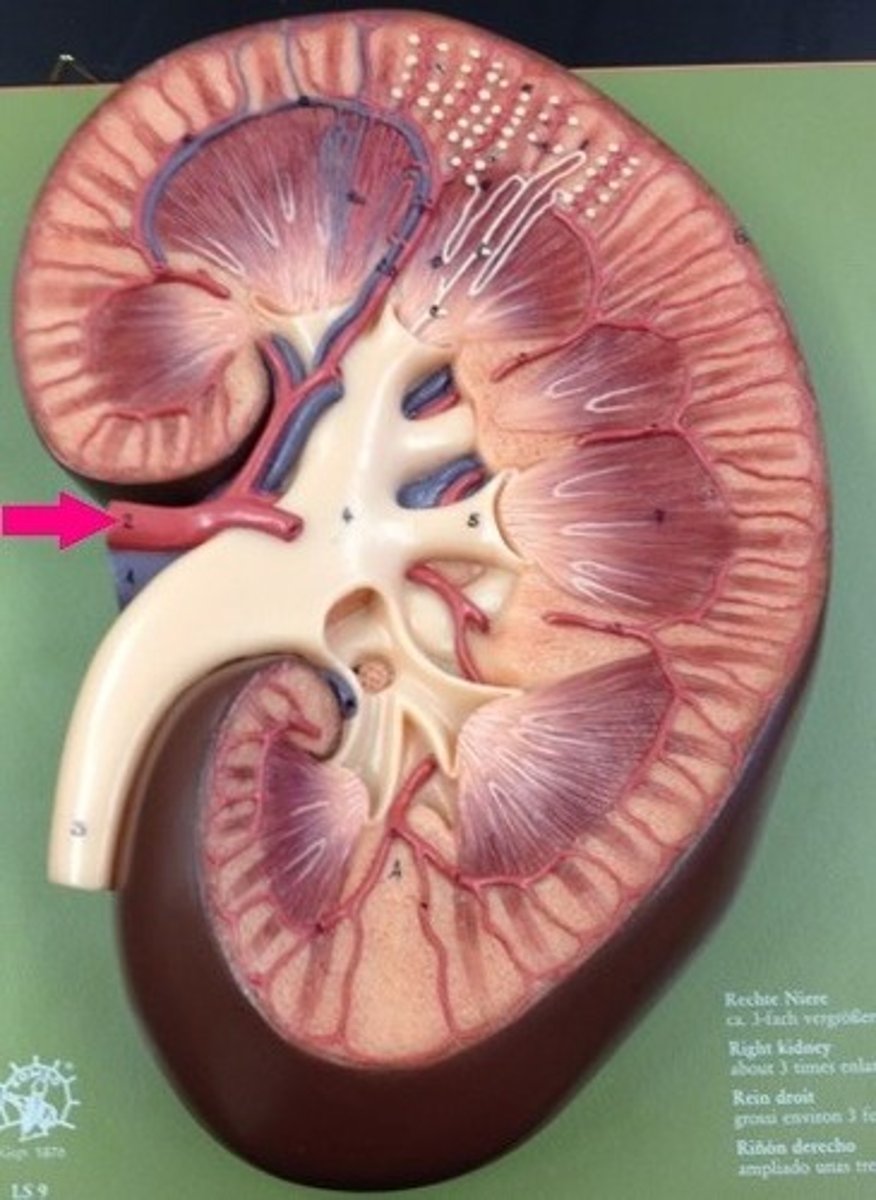
Renal artery
Supplies blood to kidney
Segmental arteries
First branches of renal artery
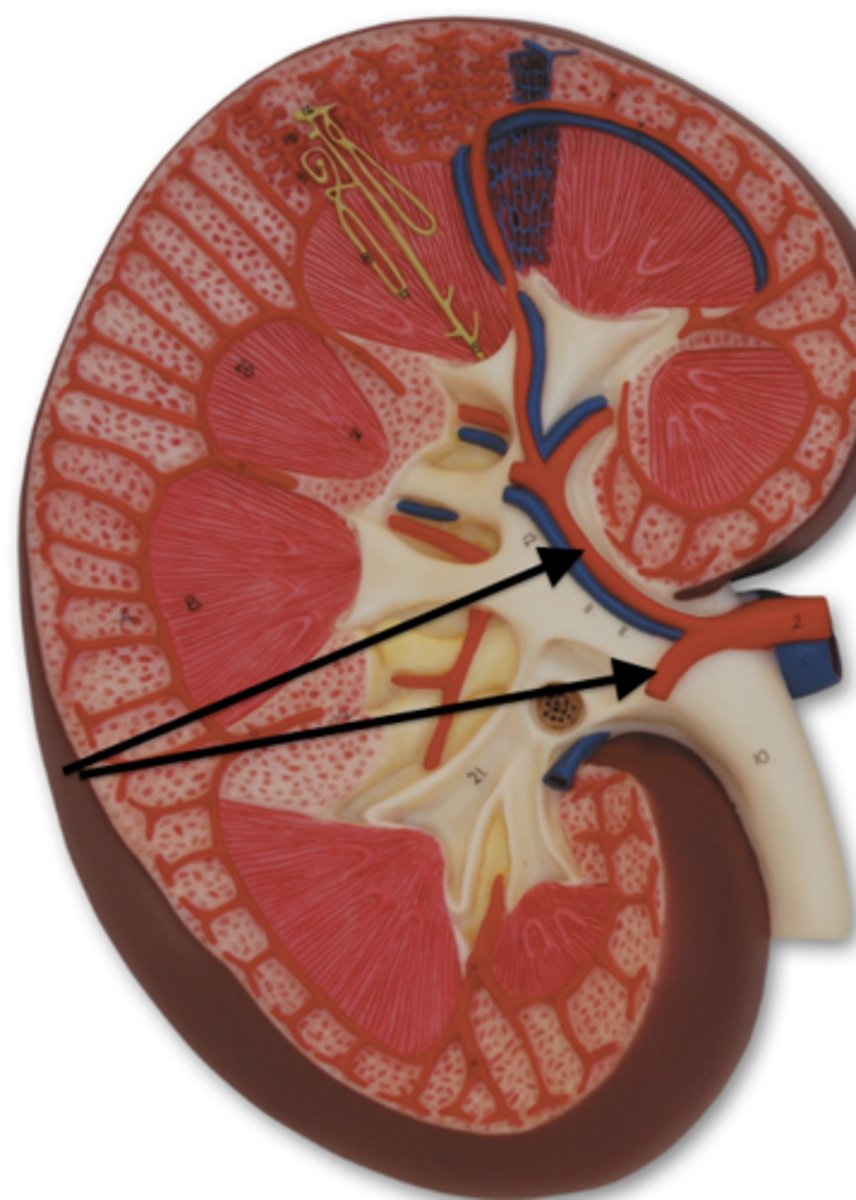
Interlobar arteries
oxygenated blood vessels that travel through renal columns
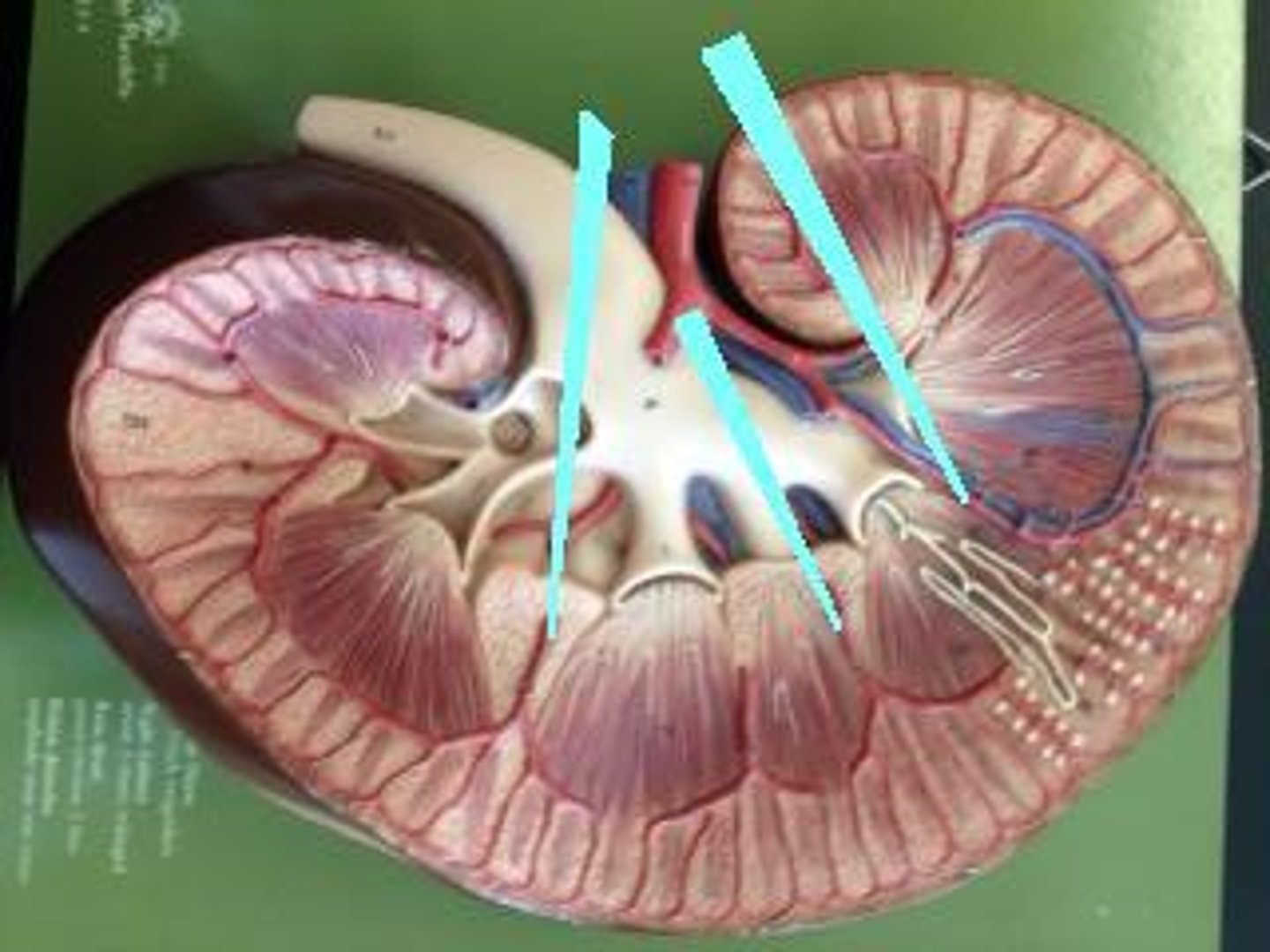
interlobar veins
deoxygenated blood vessels that travel through renal columns, ultimately carrying filtered blood back to the inferior vena cava
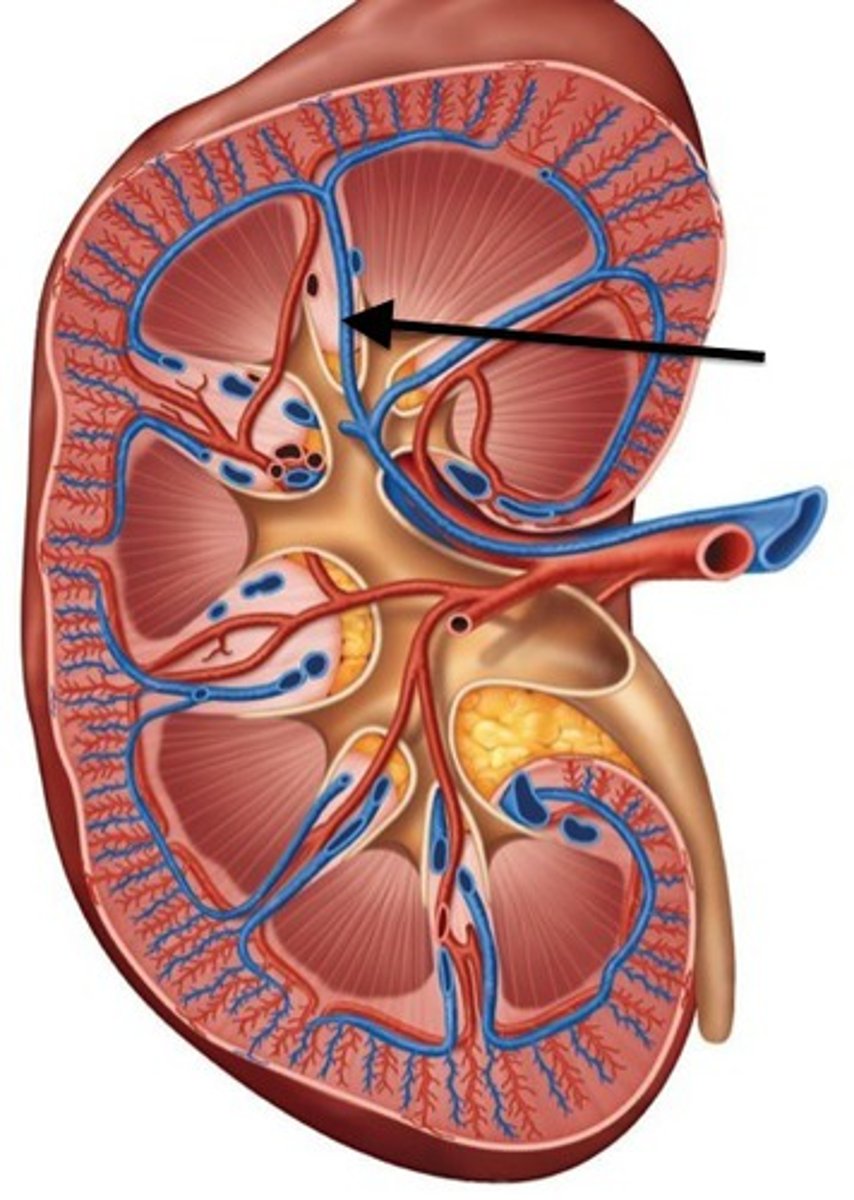
Arcuate arteries
Located at cortex-medulla boundary
- eyelash spine lol
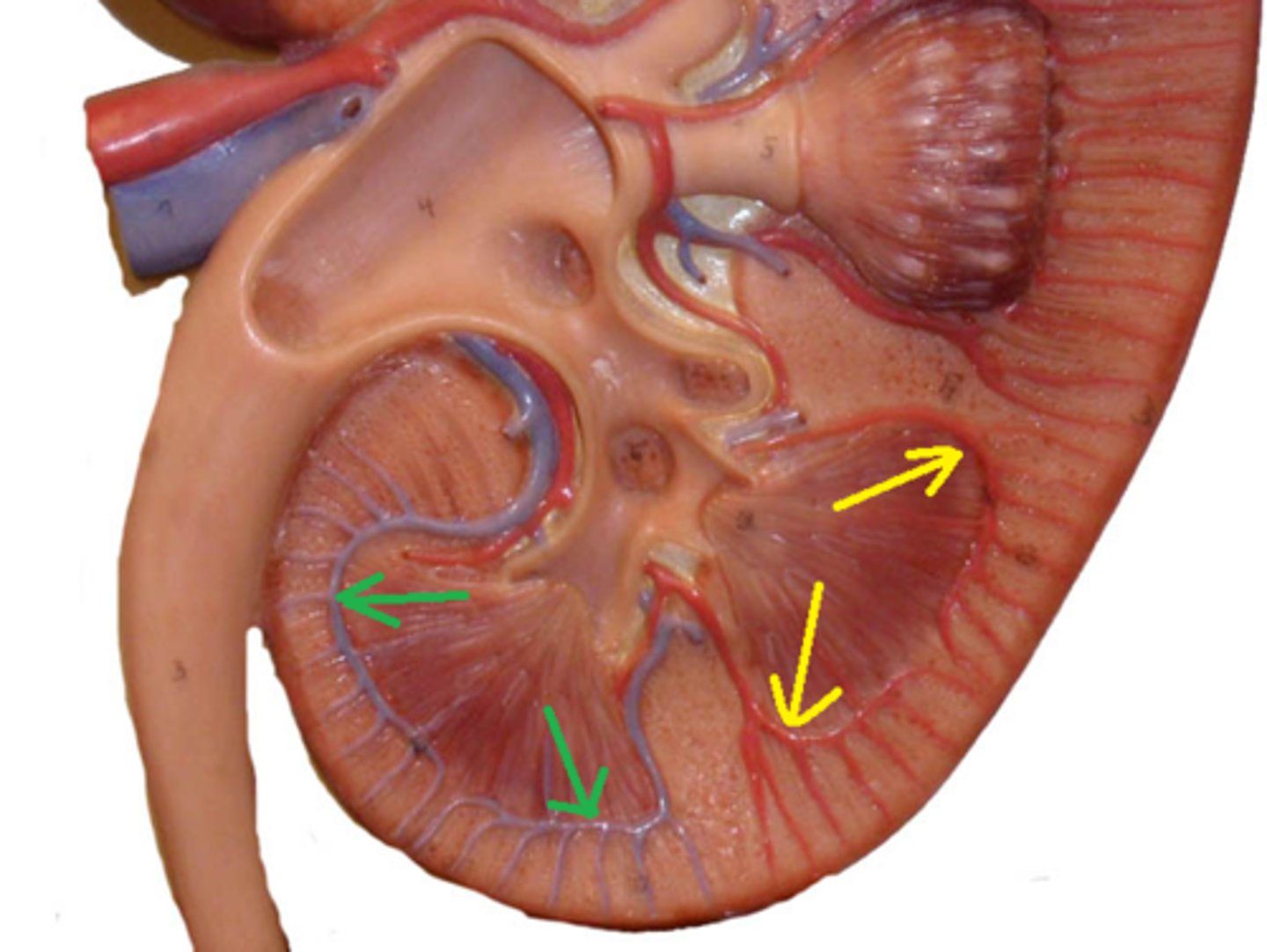
Cortical radiate arteries (Interlobular Arteries)
Extend into cortex
- eyelashes
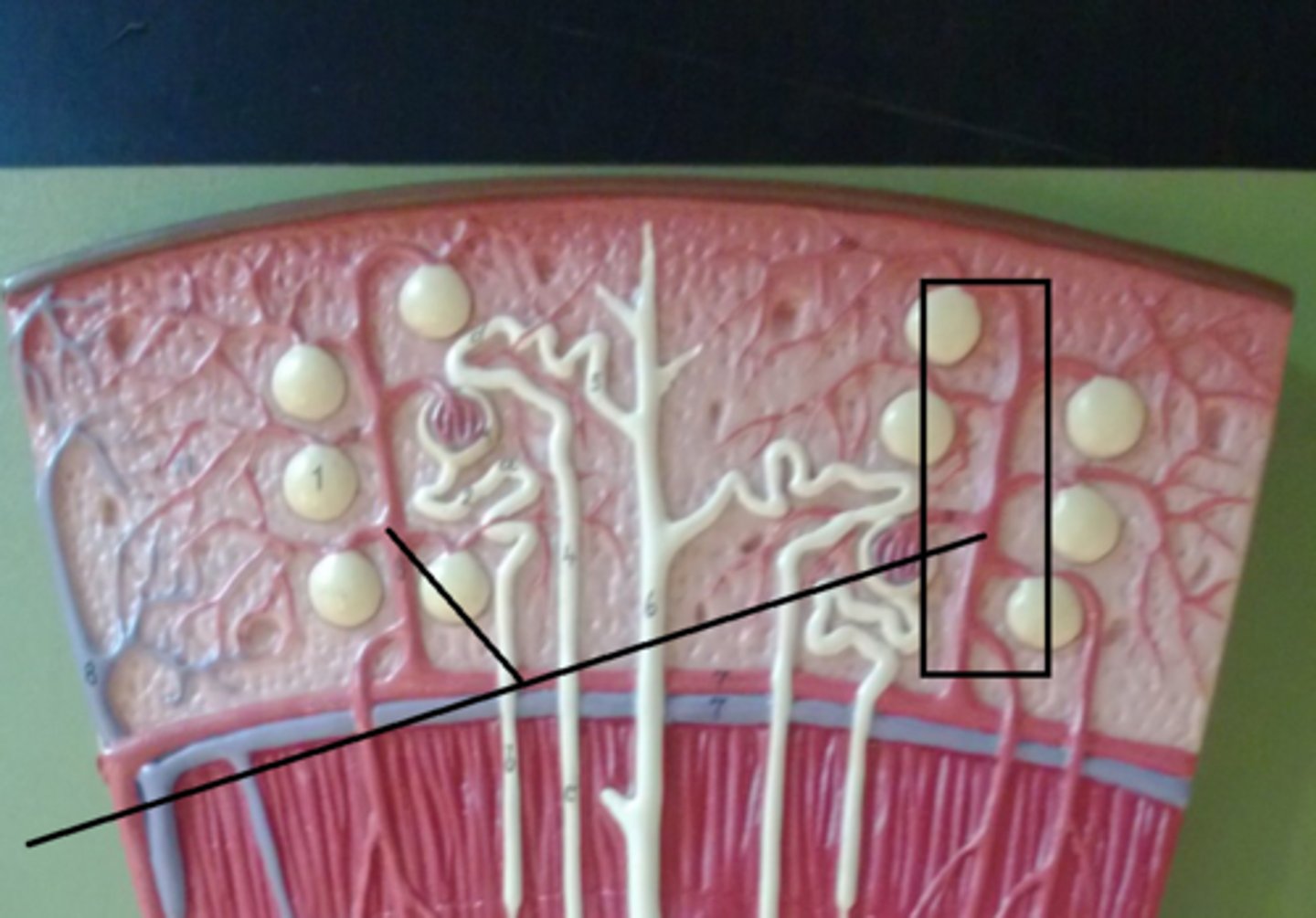
Afferent arteriole
Brings blood to glomerulus from Cortical radiate arteries
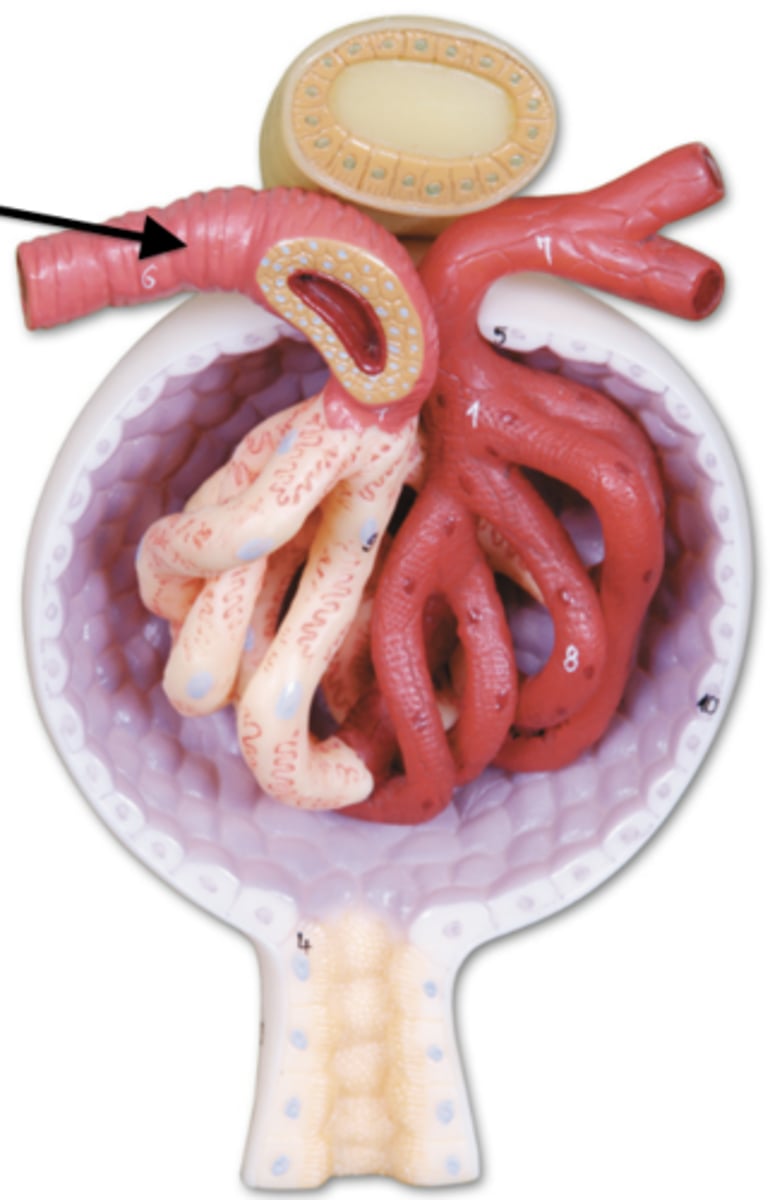
Really Smart Interns Always Carry Apples
Pneumonic for arery flow into kidneys....

Efferent arteriole
carries blood away from the glomerulus
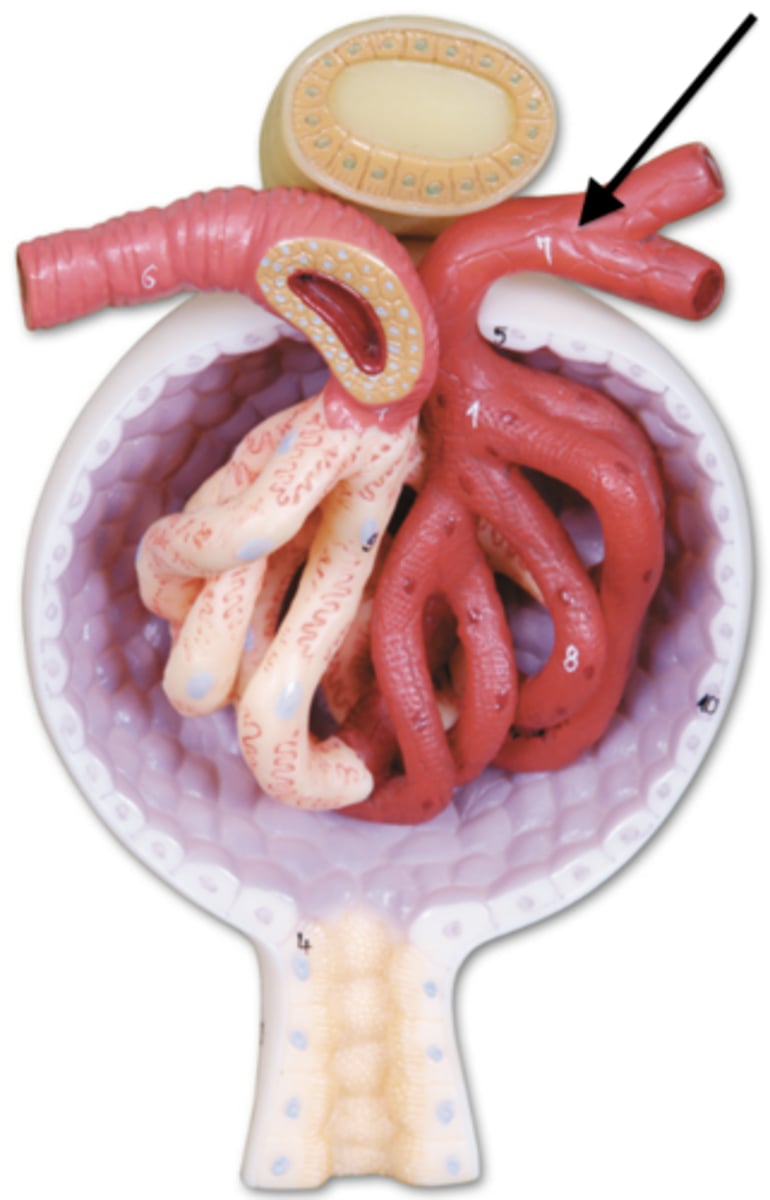
Renal artery, segmental artery, interlobar artery, arcuate artery, cortical radiate, afferent arteriole
What is the order of artery flow from the hilum to the cortex (into the kidney)?
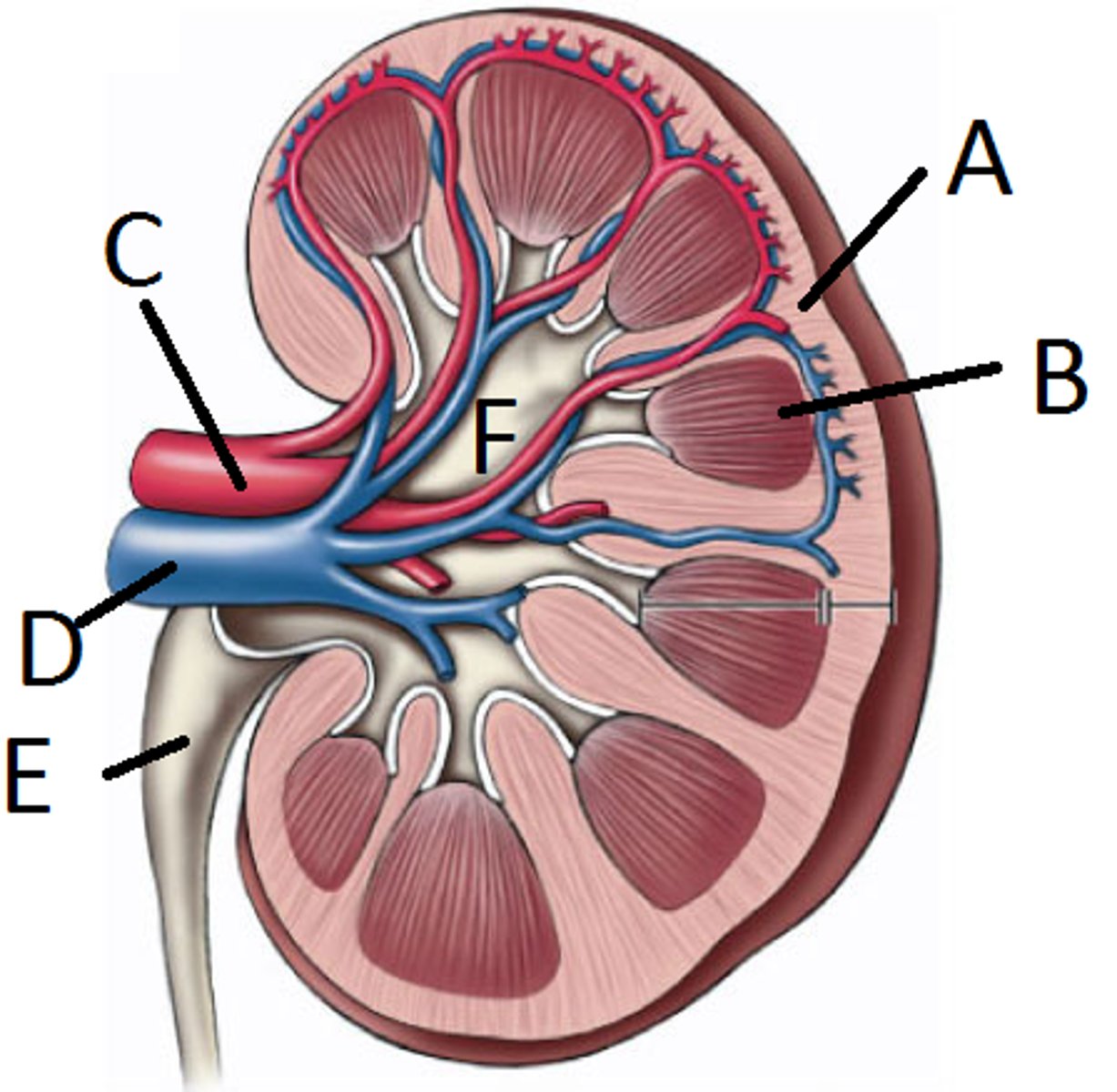
Nephron
Functional unit of kidney that forms urine
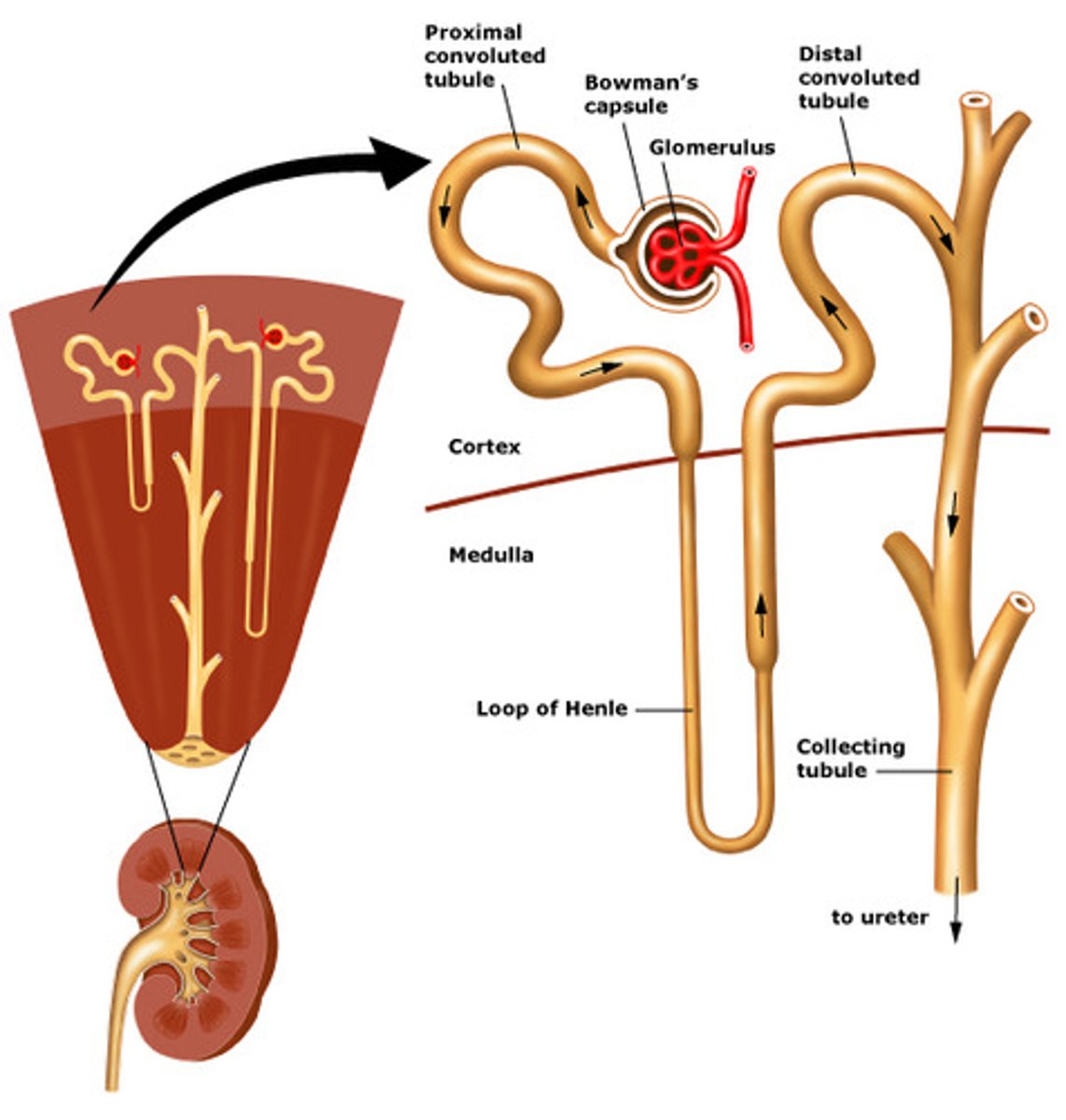
80%, 20%
___% of nephron is in cortex, while ___% in medulla
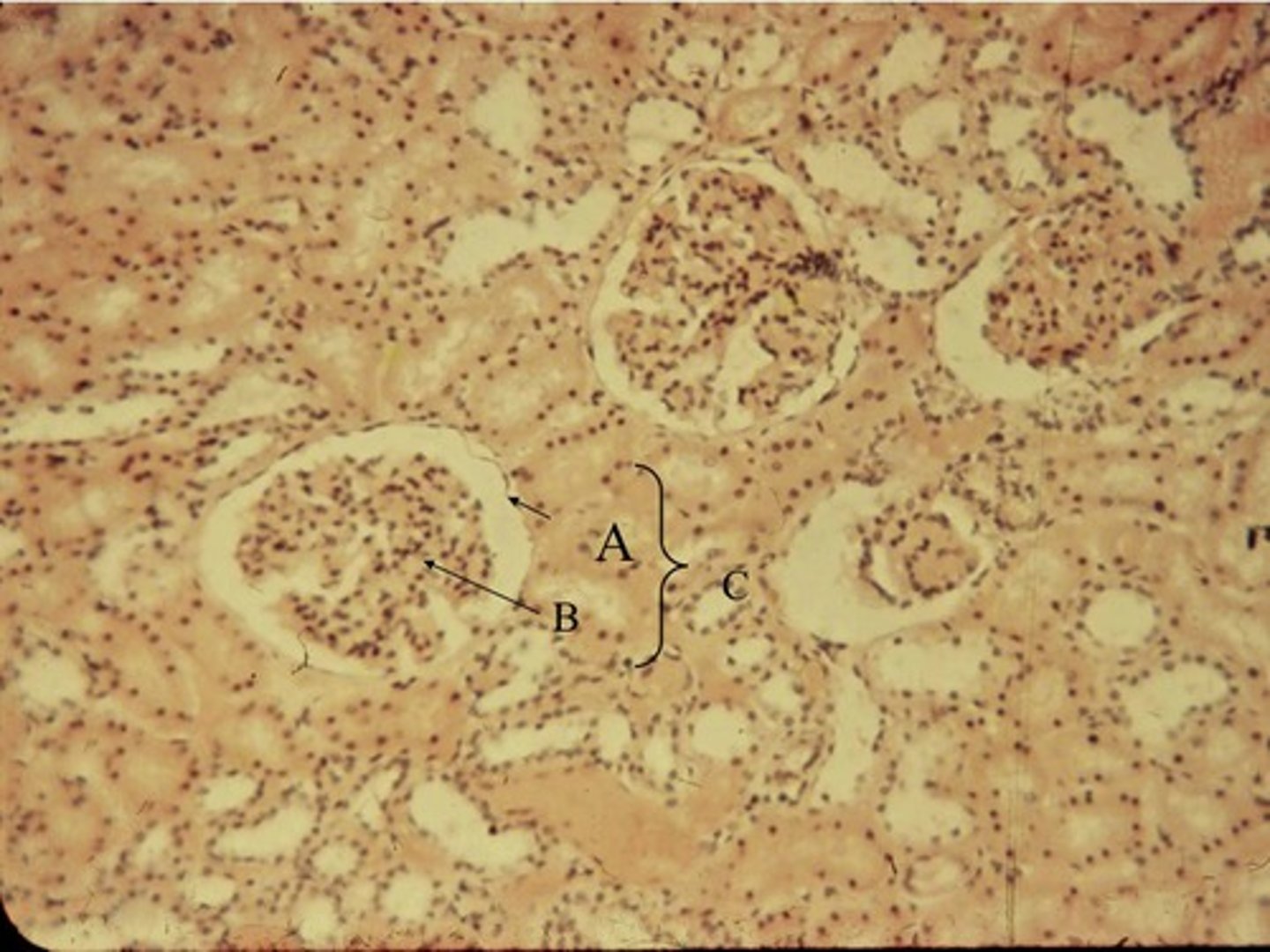
Glomerulus
Capillary network where filtration occurs
- ball-like bunch of capillaries
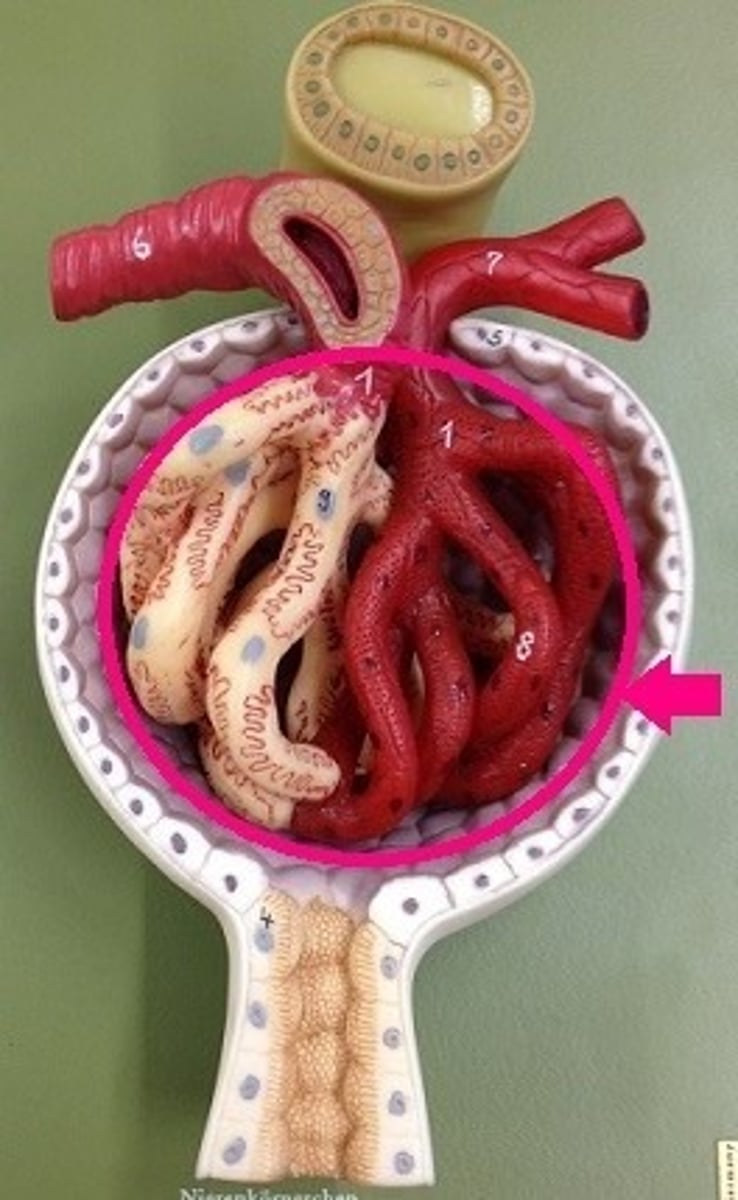
Bowman's capsule
cup-shaped structure of the nephron of a kidney which encloses the glomerulus and which filtration takes place.
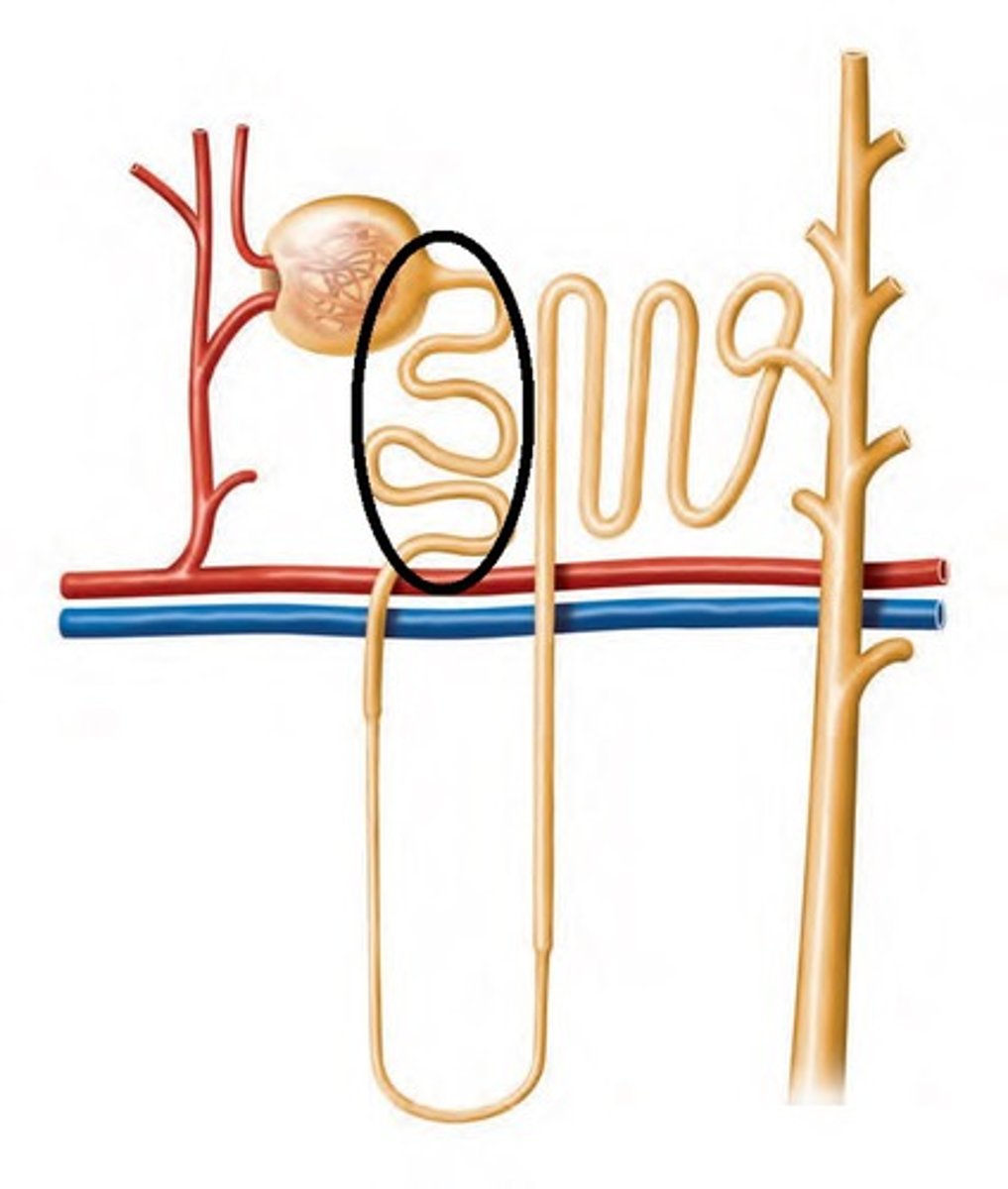
- Collects filtrate from glomerulus (B in picture)
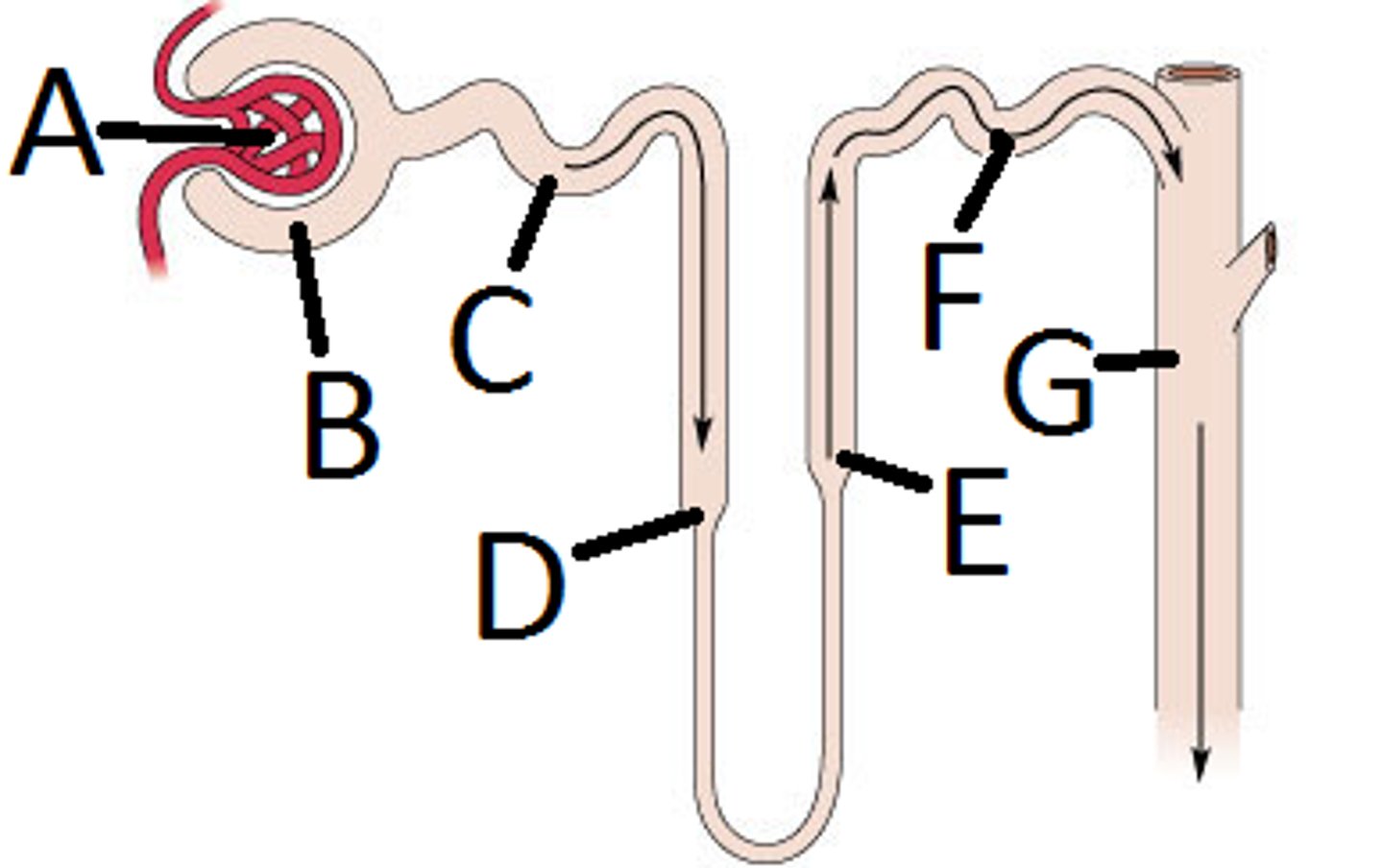
renal corpuscle
glomerulus + bowman's capsule =
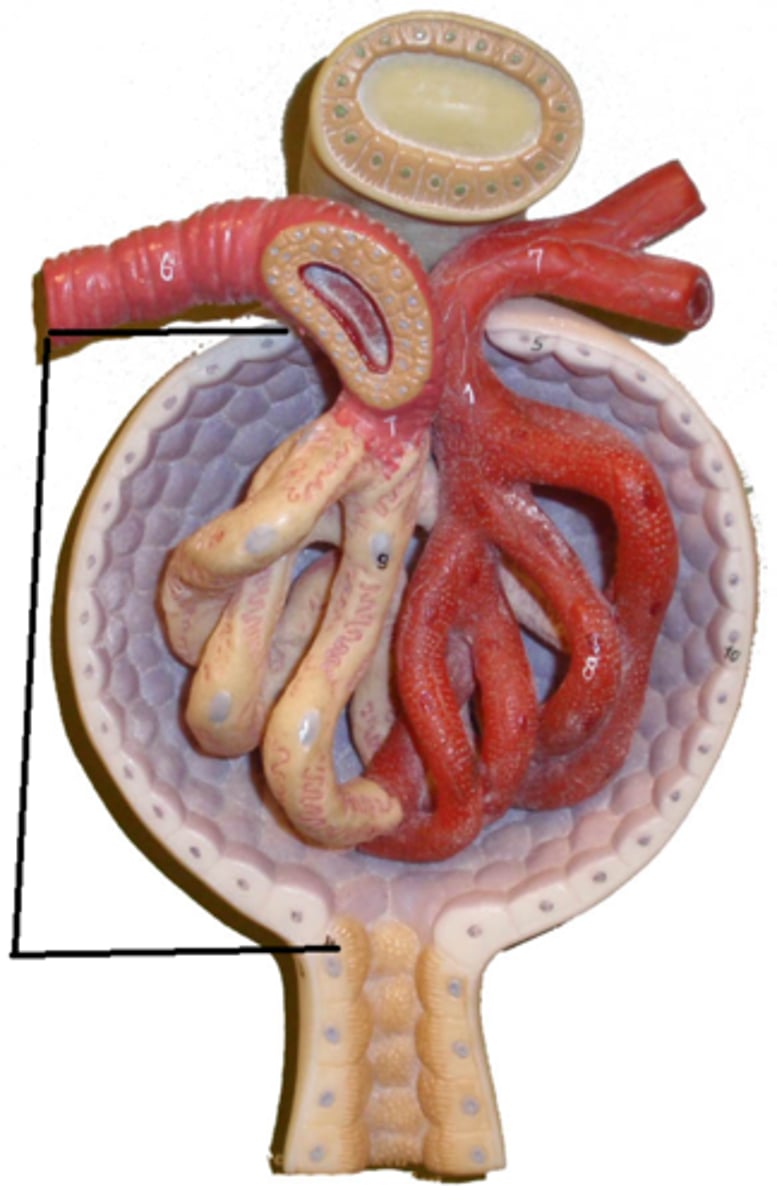
Filtration
Movement of plasma and solutes into nephron
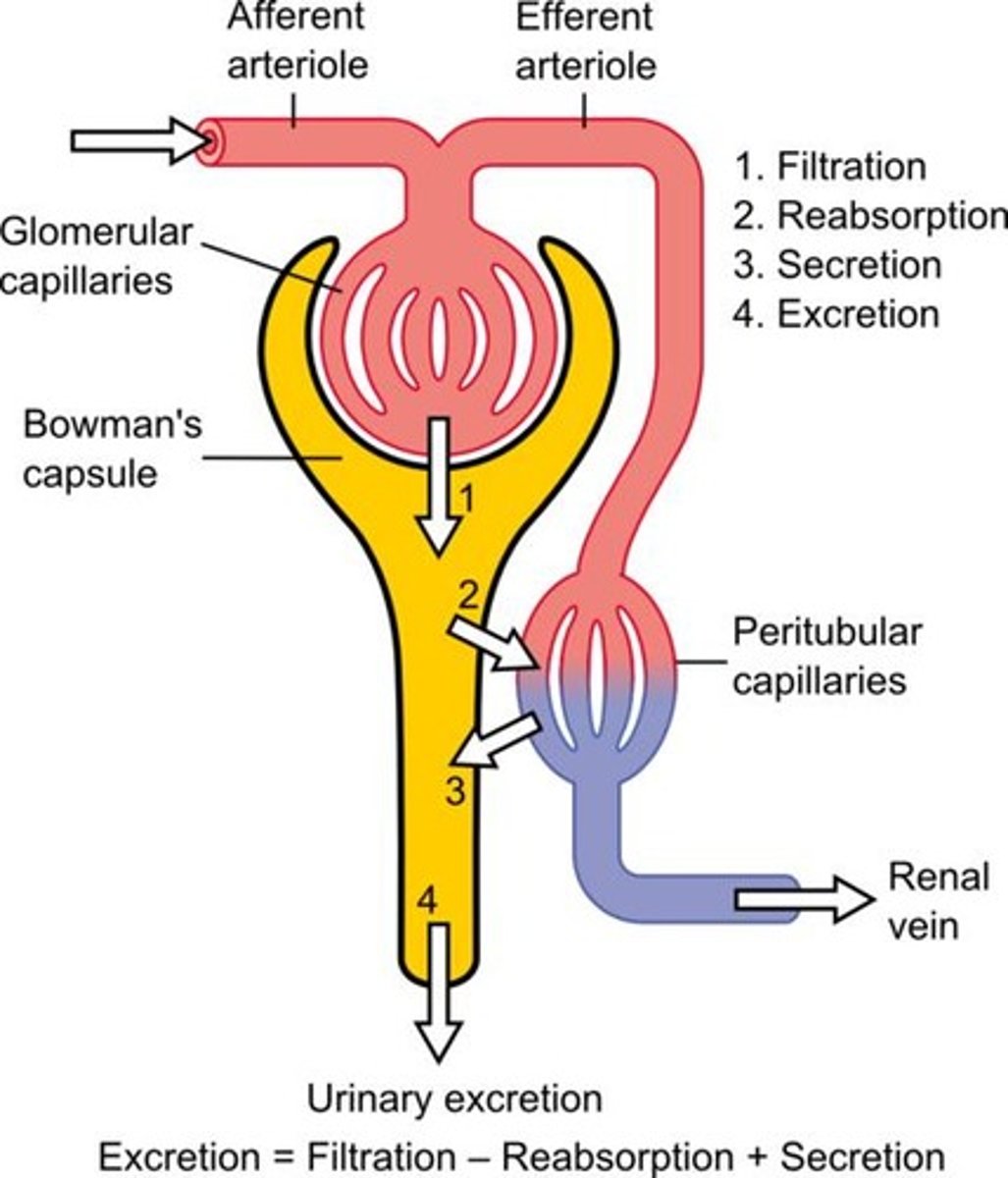
space surrounding the Bowman's capsule
Filtration occurs when fluid and solutes are forced from the blood in the glomerulus into the-
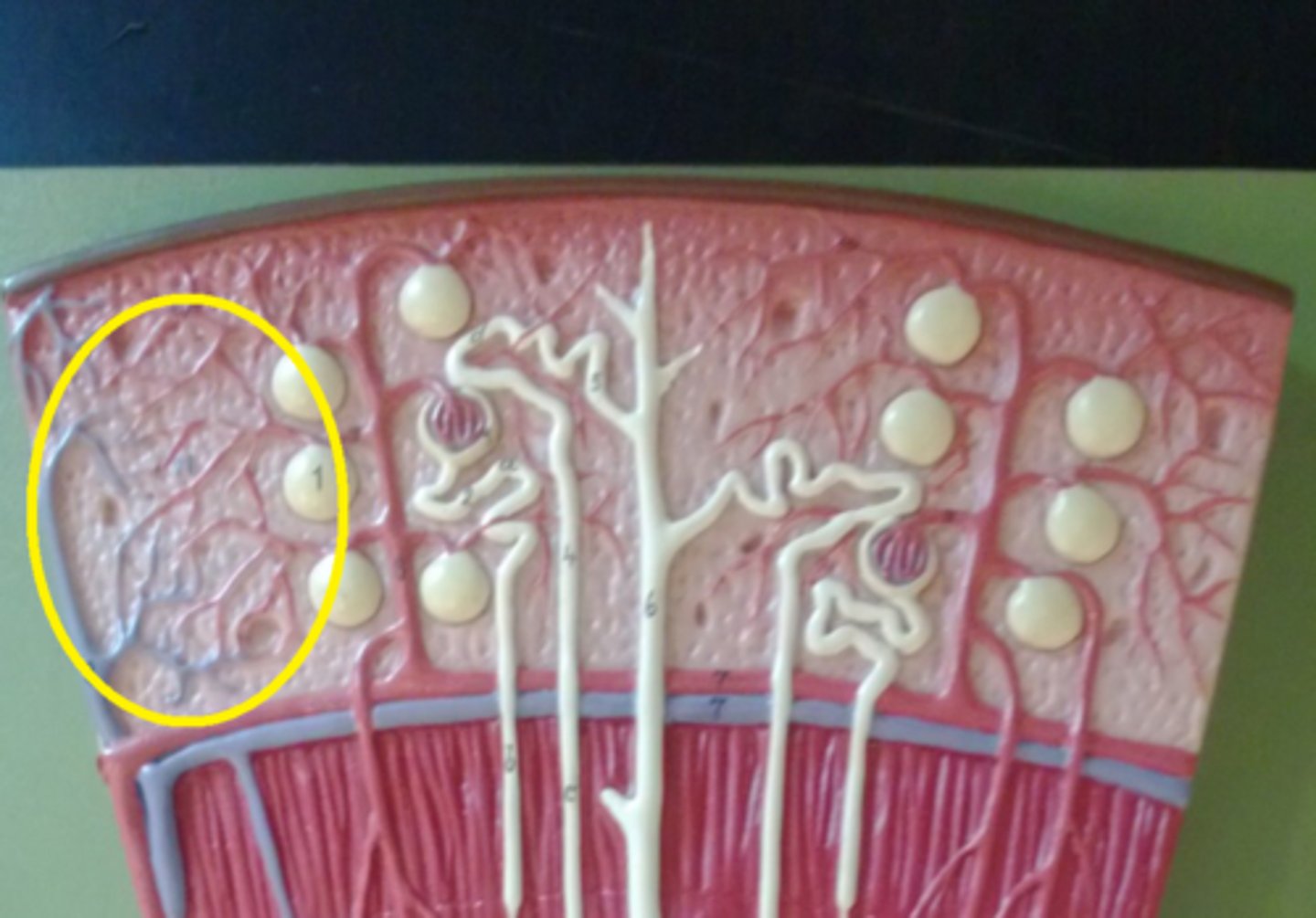
Peritubular capillaries
Blood supply that directly receives substances from the tubular cells. Site of reabsorption and secretion
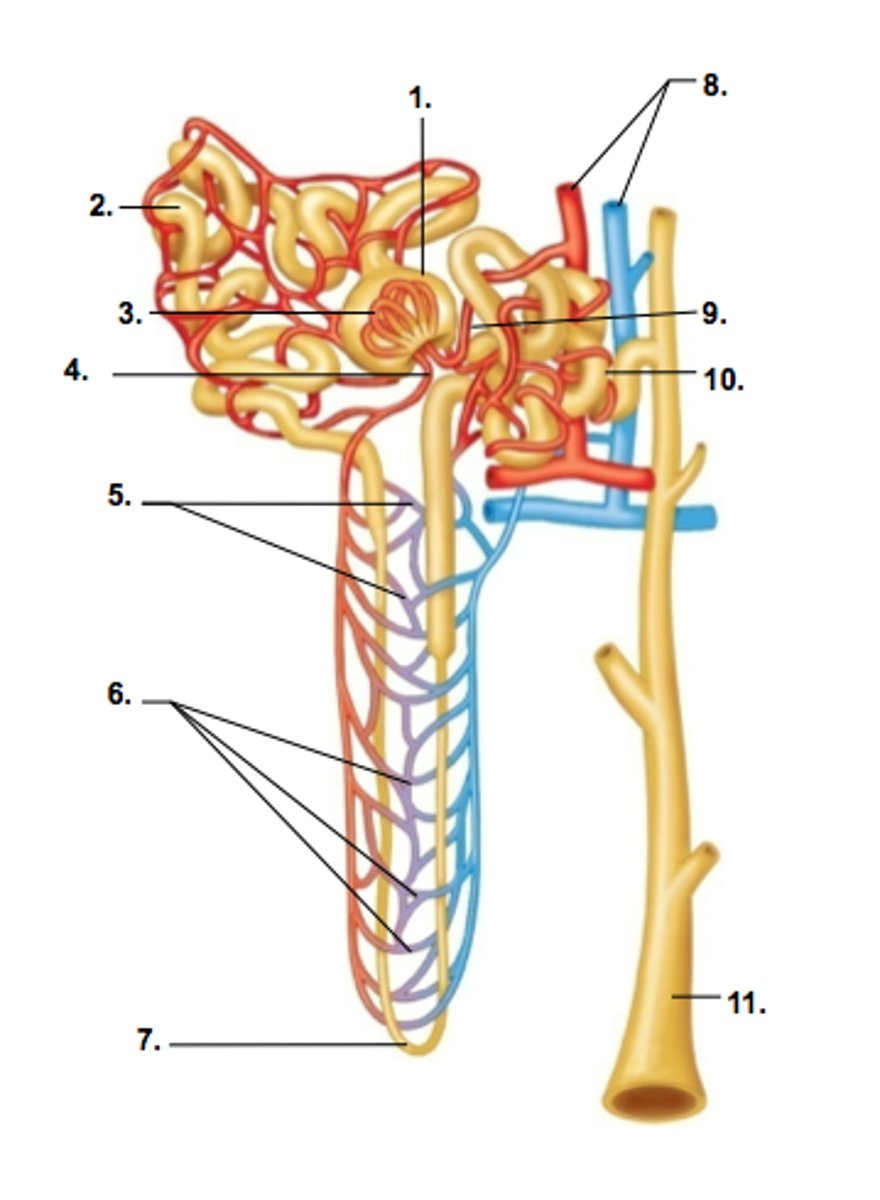
Vasa recta
Capillaries around loop of Henle maintaining gradient
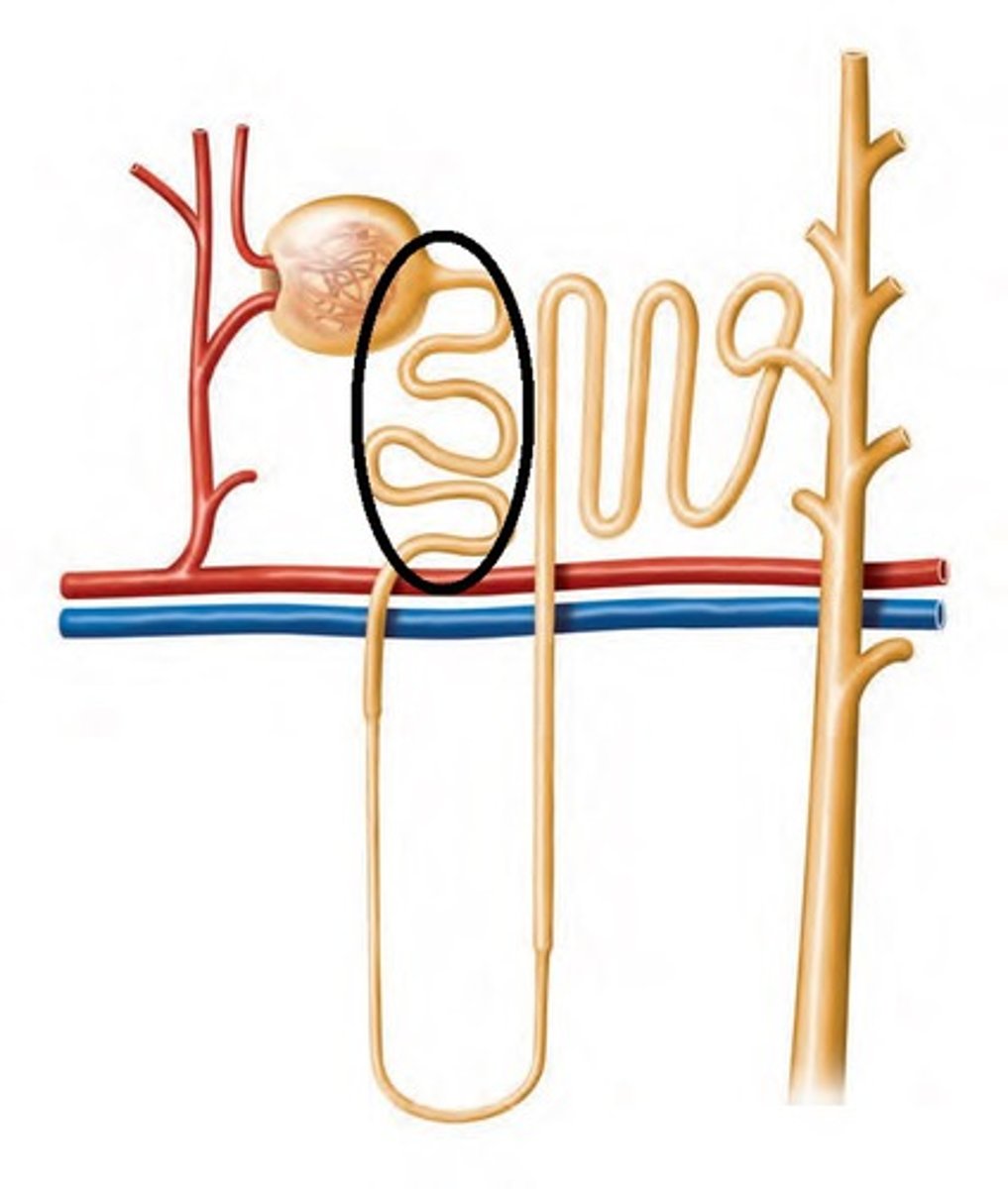
Proximal convoluted tubule (PCT)
Major site of reabsorption located entirely within the cortex
- simple cuboidal epithelium with microvilli
surface area, reabsorption, 99%
Microvilli in PCT are finger-like projections significantly increase the _________ to enhance ________ efficiency, returning, for example, ____% of filtered substances back into the bloodstream
Loop of Henle
establishes osmotic gradient for water reabsorption
- connects descending and ascending tubes, dipping into medulla
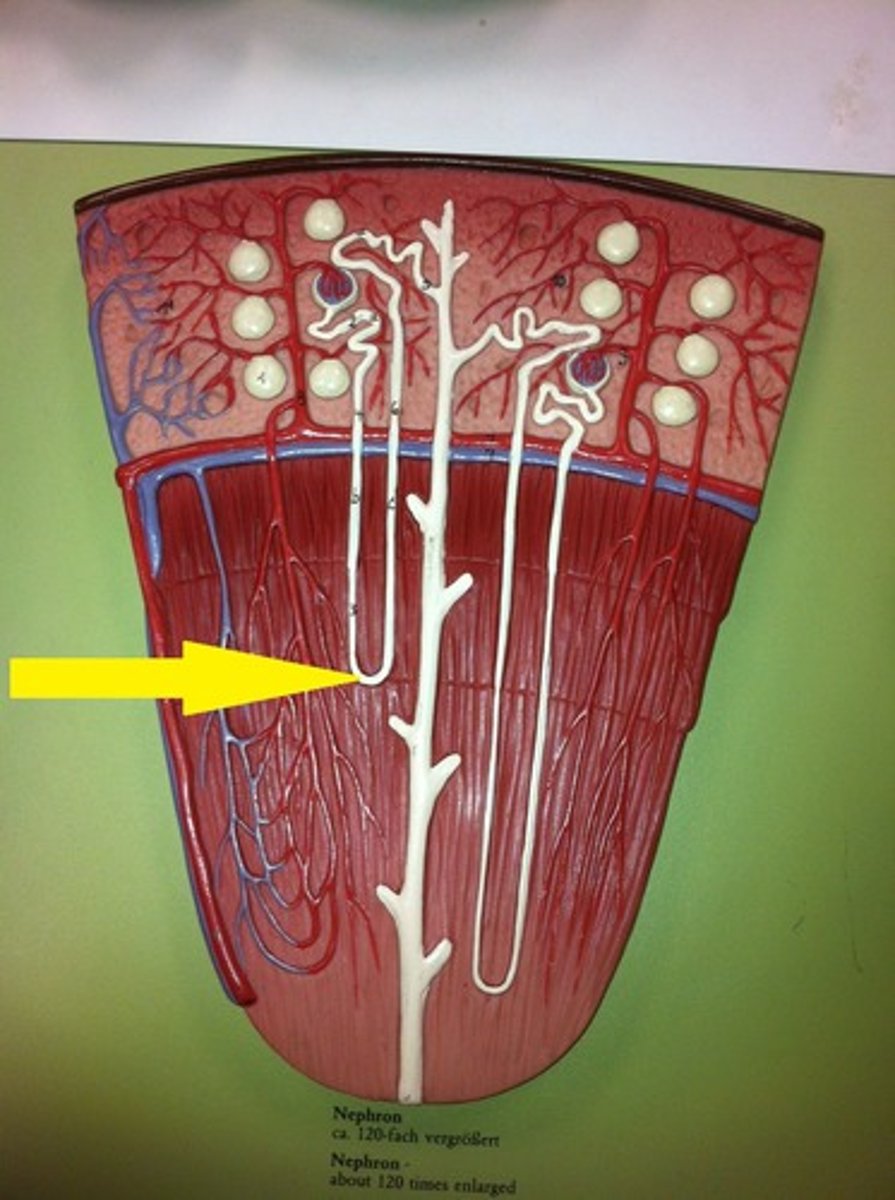
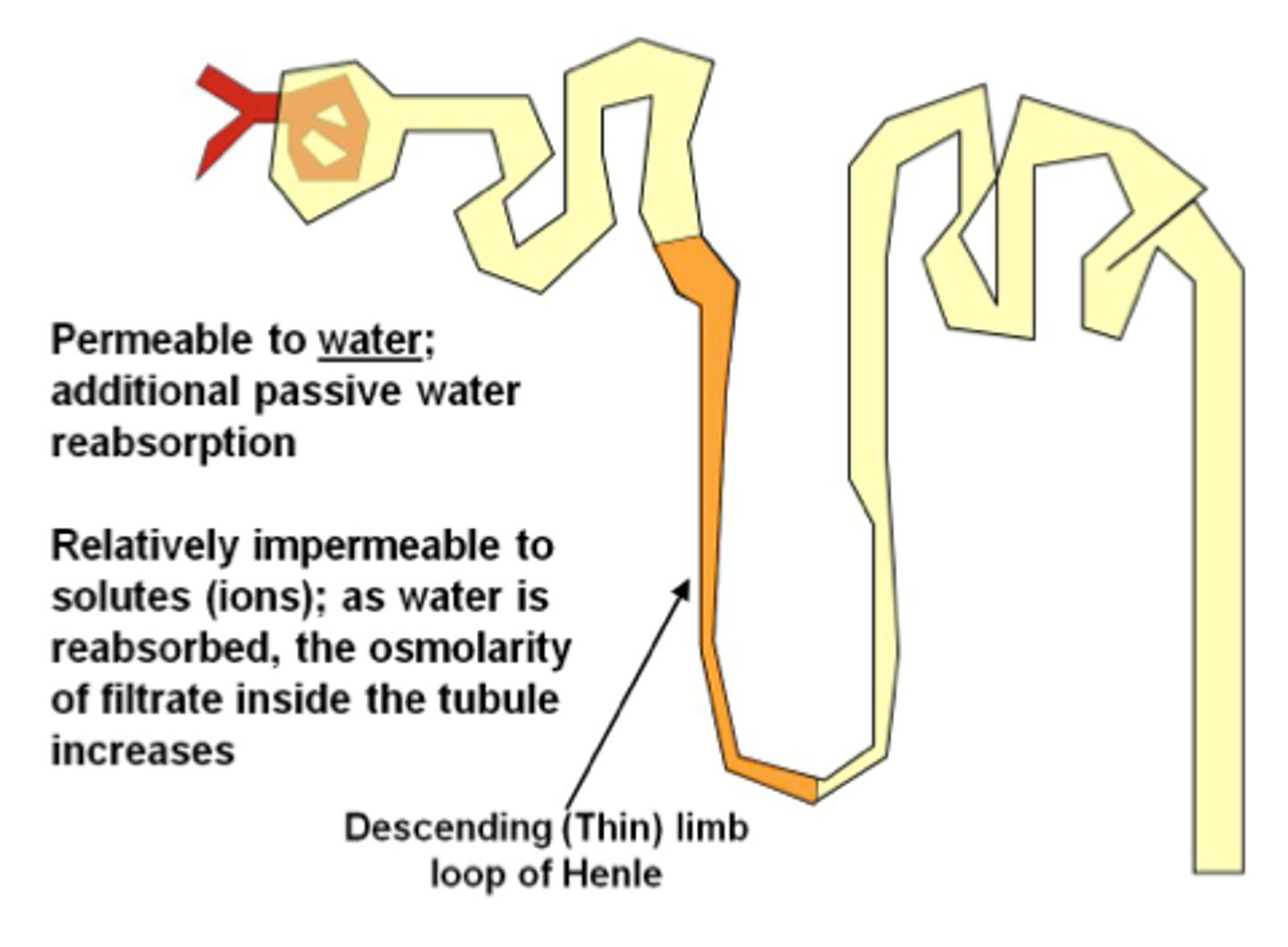
Descending tube (limb)
descends into the medulla, THIN, alternates between thick and thin segments
🌟 Permeable to water
- simple squamous epithelium
Ascending tube (limb)
ascends from medulla, THICK, alternates between thick and thin segments
🌟 Permeable to solutes, impermeable to water (water does not come out, only Na and Cl)
- simple squamous epithelium
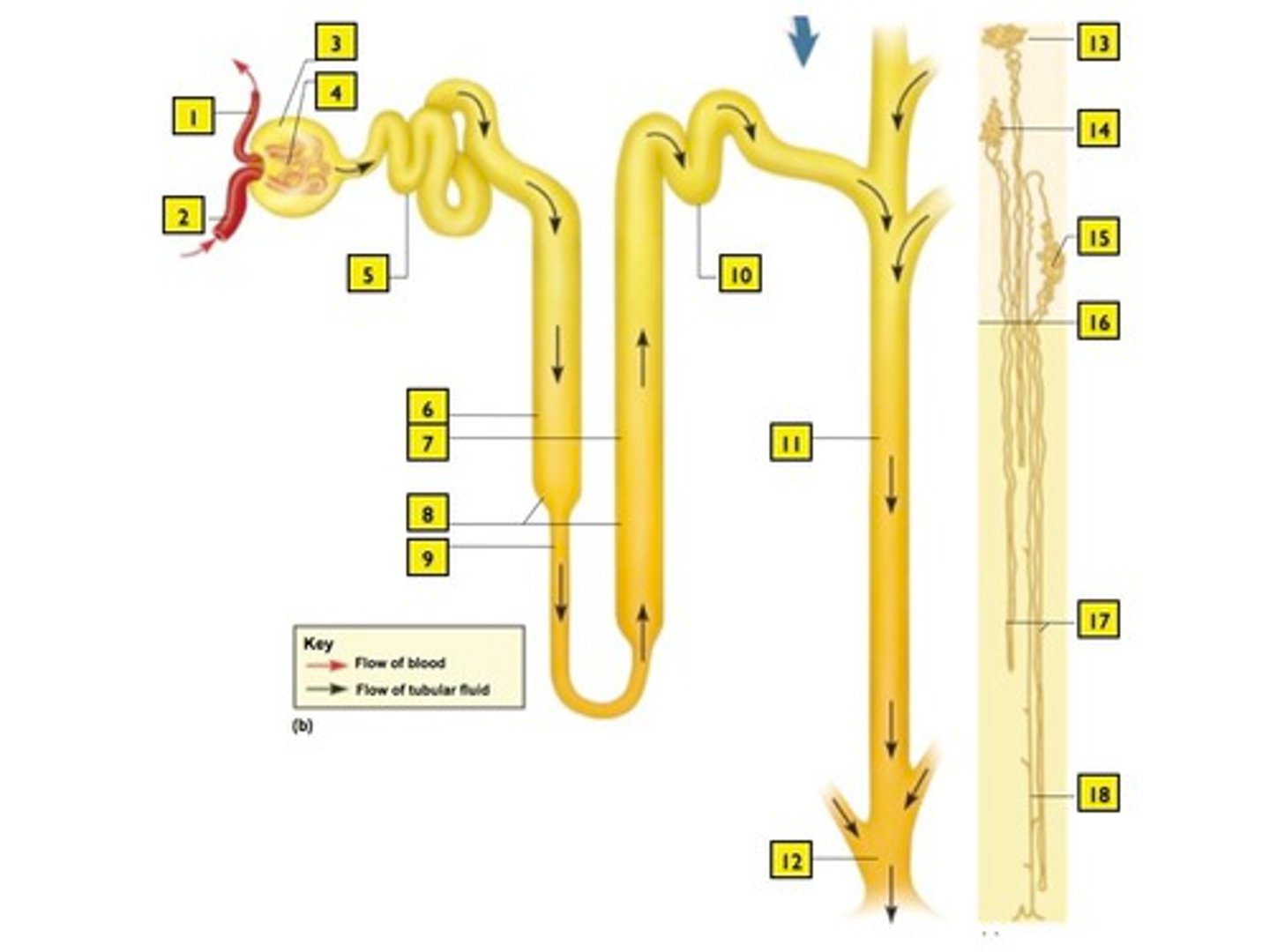
Distal convoluted tubule (DCT)
Regulates ion balance
- simple cuboidal epithelium WITHOUT microvilli
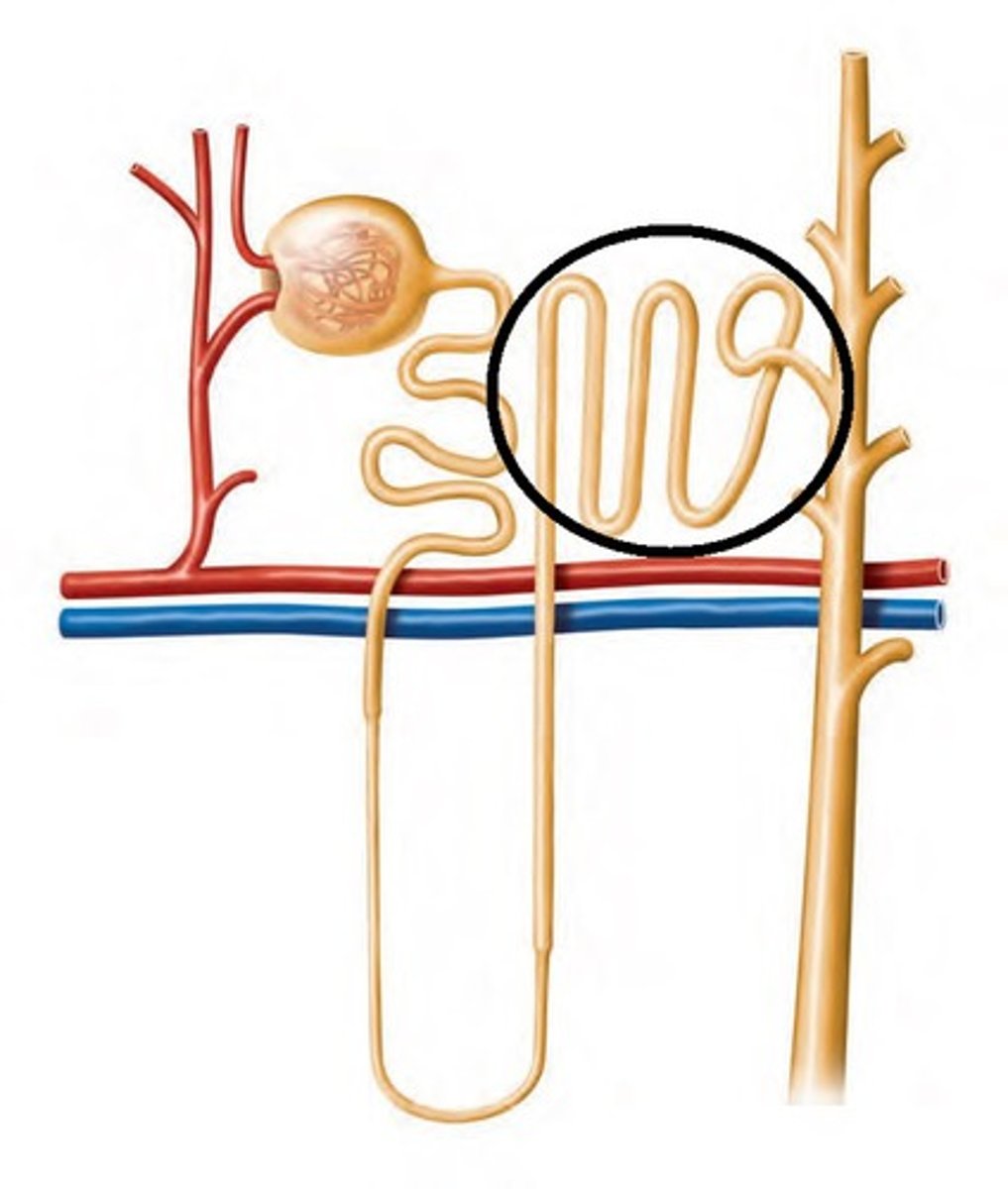
Proximal
Which tubule has microvilli?
Collecting duct
Several nephrons empty into each collecting duct; Final regulation of urine composition
- urine must pass through on its way to the ureter.
- where water reabsorption is regulated via antidiuretic hormone (ADH)???
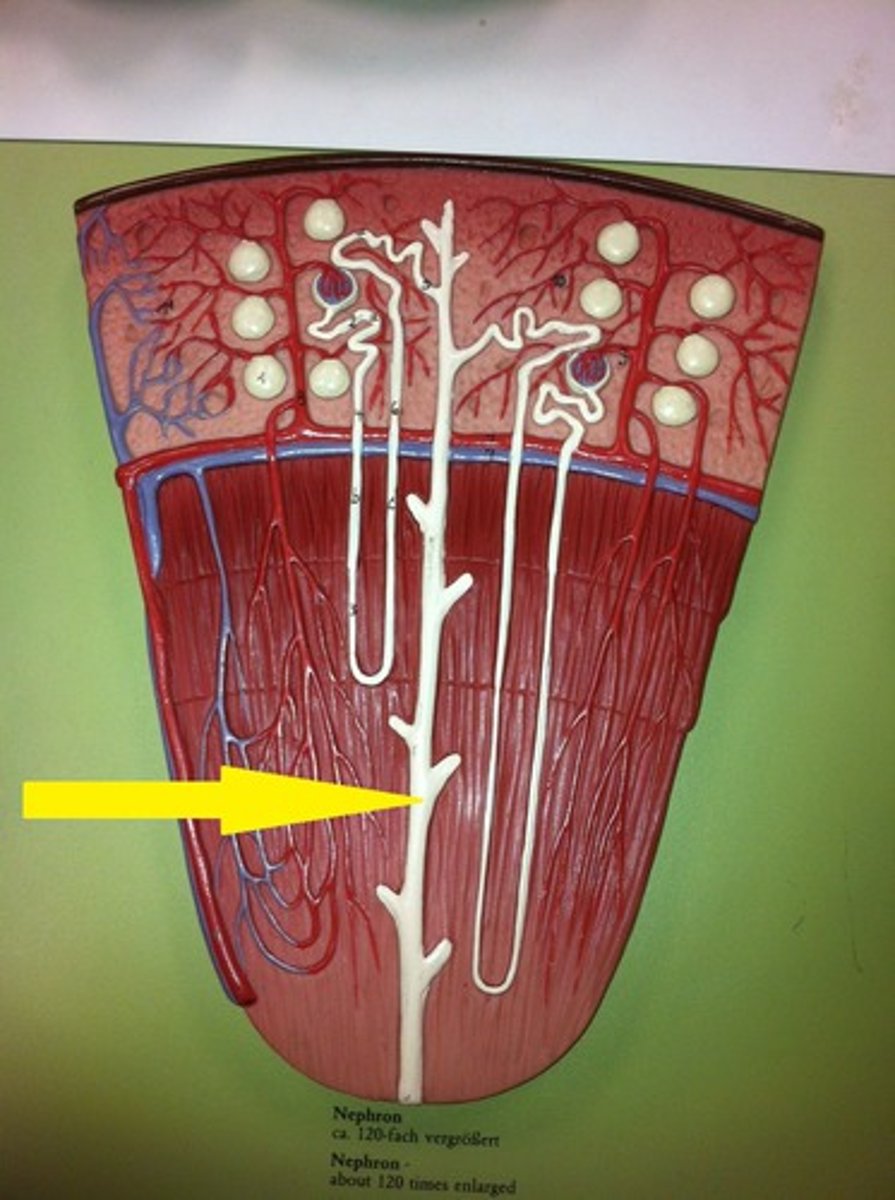
proximal convoluted tubule
Which region of the renal tubule is the most active in terms of filtrate processing?
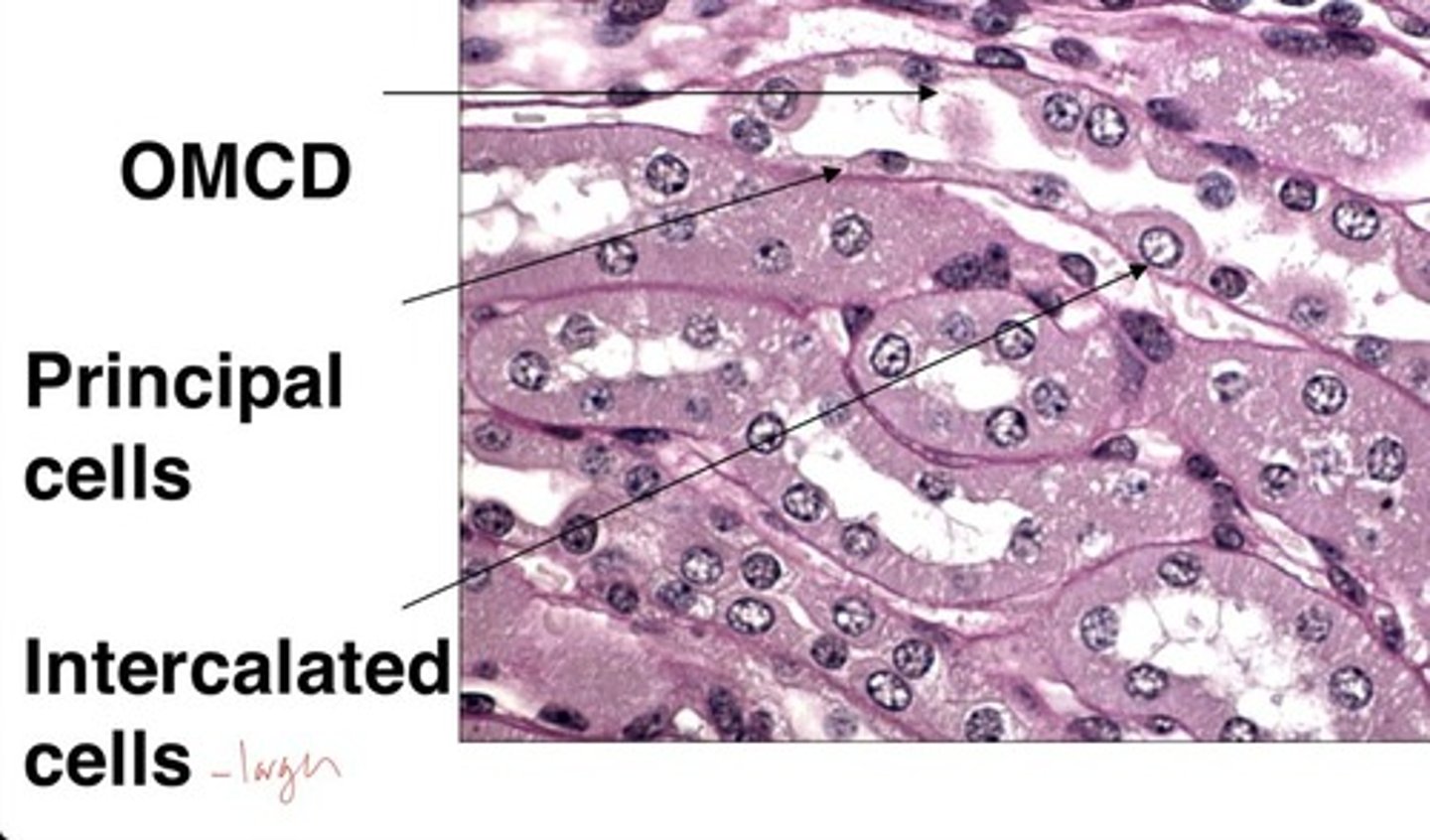
Principal cells
conducting duct cells that adjust urine to regulate body's water, Na⁺, and K⁺ balance
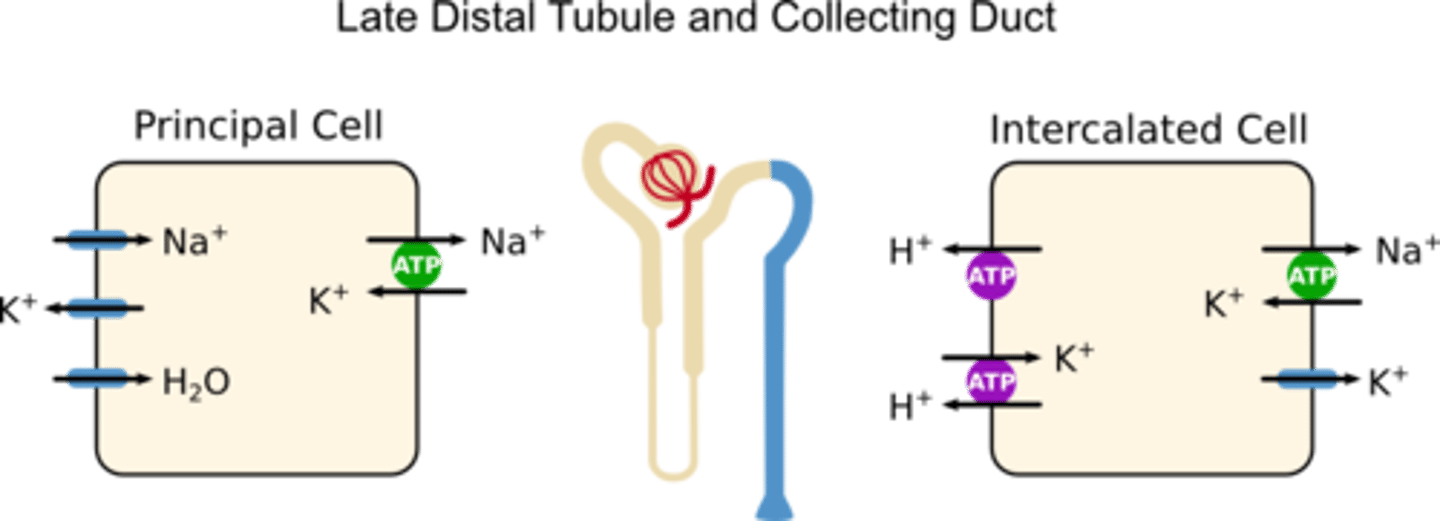
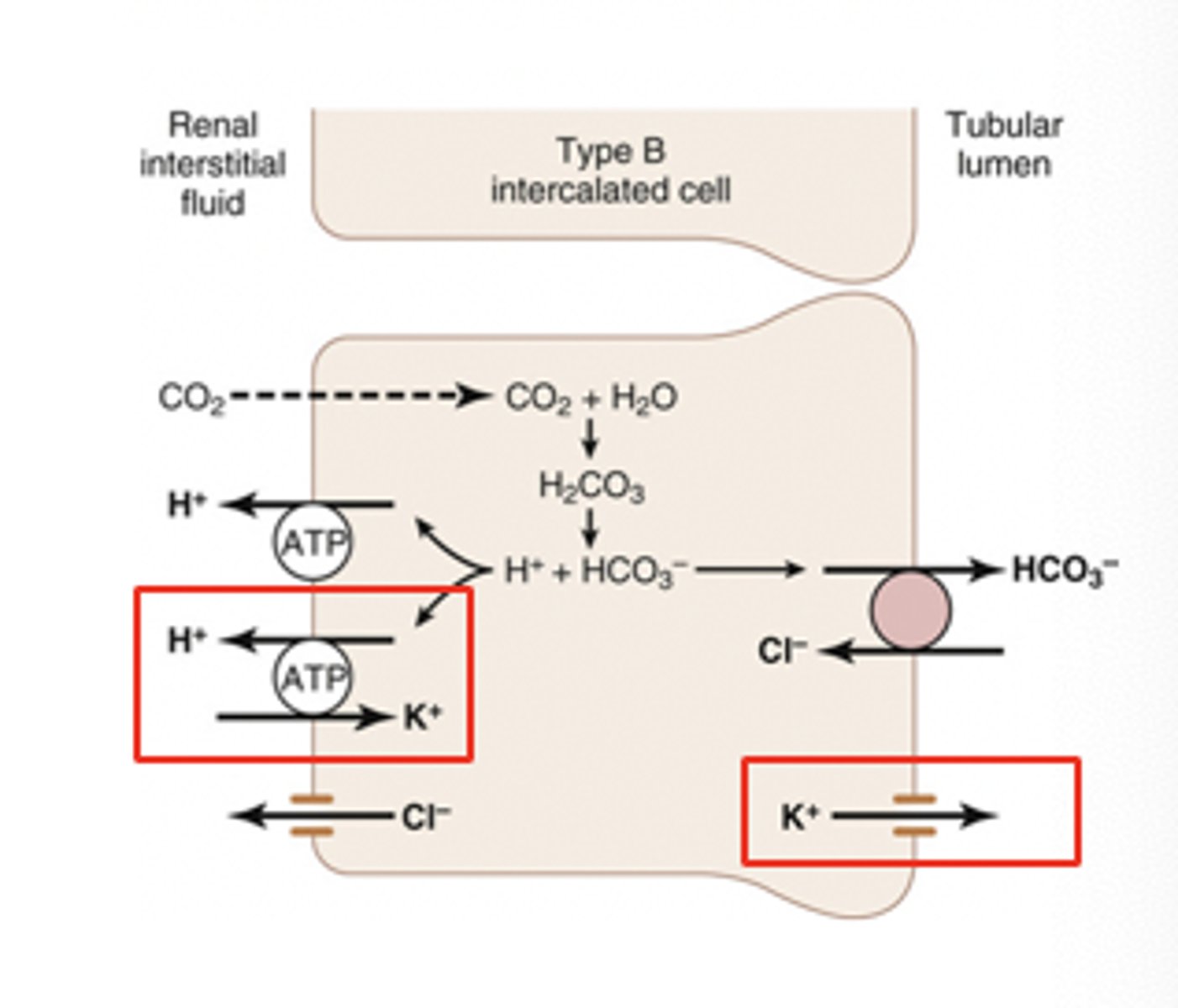
Intercalated cells
conducting duct cells that regulate acid-base (pH) balance through HCO3- and H+
principal cells and intercalated cells
collecting duct cells include
water, Na⁺, and K⁺ balance
what do principle cells regulate?