CAD/CHD, Valve, MI, Infective Endocarditis, Pericarditis
1/48
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
49 Terms
What is Coronary Heart Disease (CHD)?
CHD is insufficient delivery of oxygen to the heart muscle due to narrowing or blockage of the coronary arteries, most commonly from atherosclerosis which can l/t MI
What Causes CHD? – Atherosclerosis
Endothelial injury → inflammation
Lipid-laden macrophages form foam cells
Fatty streaks develop
Fibrous plaque forms and may calcify
Plaque protrudes into lumen → ↓ blood flow → angina/MI
Non-Modifiable Risk Factors (Cannot Change) of CHD
Increased age
Family history
Male gender
Female post-menopause
Modifiable Risk Factors (Can Change) of CHD
Dyslipidemia (↑ LDL, ↓ HDL, ↑ triglycerides)
Hypertension
Cigarette smoking
Diabetes mellitus
Obesity
Sedentary lifestyle
Why Smoking Is So Dangerous?
↑ HR & BP
↑ LDL & triglycerides
↓ HDL
↑ platelet aggregation
↑ endothelial dysfunction
↓ oxygen carrying capacity
↑ inflammatory proteins
Accelerates atherosclerosis
Diet for CHD
What Increases Risk
High saturated fats
High LDL foods
High triglyceride intake
Excess sodium
Obesity-promoting diet
Heart-Healthy Diet Recommendations
From DASH diet & cardiovascular management slides
Hypertension%2C+PVD%2C+arterial…
:
🥦 4–5 servings vegetables daily
🍎 4–5 servings fruits daily
🌾 7–8 servings whole grains
🥛 Low-fat/nonfat dairy
🐟 Lean protein (fish, poultry)
🥜 Nuts, seeds, beans
🍭 Limit sweets
🧂 Reduce sodium
❤ How Diet Protects the Heart
↓ LDL cholesterol
↑ HDL cholesterol
↓ BP
↓ inflammation
↓ workload on heart
Remember from your HF slides:
High sodium → fluid retention → ↑ preload → ↑ cardiac workload.
What is Myocardial Ischemia?
Temporary reduction in blood flow → not enough oxygen to the heart muscle.
Myocardial cells become ischemic within 10 seconds of a coronary occlusion.
Reversible if blood flow returns in time
No permanent cell death
Troponin usually normal
What is Stable Angina and Prinzmetal/variant angina?
Stable angina and Variant (Prinzmetal) angina are manifestations of myocardial ischemia.
Stable Angina
What it means:
Predictable chest pain
Occurs when oxygen demand increases
Triggered by:
Exercise
Stress
Cold weather
Heavy meals
Why?
The coronary arteries are narrowed by plaque (atherosclerosis).
When the heart works harder → it needs more oxygen → narrowed artery cannot supply enough → pain.
Key characteristics:
Predictable
Relieved by rest
Relieved by nitroglycerin
Lasts < 15 minutes
Prinzmetal Angina
Also called:
Variant or vasospastic angina
What happens?
Coronary artery spasms
Temporary severe narrowing
Occurs at rest
Unpredictable
Important:
NOT caused by exercise
Often occurs at night or early morning
Can cause serious arrhythmias
From your slide:
Rarely associated with MI, but can lead to VF
VF = Ventricular Fibrillation → life-threatening.
Key Differences between Myocardial Infarction and Ventricular Fibrlilation
Feature | MI | VF |
|---|---|---|
Problem Type | Blood flow blockage | Electrical chaos |
Cause | Coronary artery clot | Electrical instability |
Pulse | Usually present (early) | No pulse |
Conscious? | Usually awake (initially) | Unconscious |
Troponin | Elevated | Not primary issue |
Treatment | MONA, PCI, thrombolytics | CPR + Defibrillation |
What is MI? what is happening?
MI = prolonged ischemia → irreversible cell death
Oxygen supply stops
Anaerobic metabolism begins
Lactic acid builds up
↓ ATP
Cells become acidotic
Troponin released
Cell death → possible heart failure
Two types of MI
ST-Elevation Myocardial Infarction (STEMI)
What it means:
“ST-Elevation” on ECG.
What is happening?
Complete coronary artery occlusion
Full-thickness damage (transmural infarction)
Large area of myocardium affected
ECG:
⬆ ST segment elevation
Troponin:
⬆ Elevated
Treatment:
Immediate reperfusion required
PCI (angioplasty) is preferred
Thrombolytics if PCI unavailable
Non-ST-Elevation Myocardial Infarction (NSTEMI)
What it means:
No ST elevation on ECG.
What is happening?
Partial coronary artery occlusion
Partial-thickness damage (subendocardial infarction)
Smaller area of myocardium affected
ECG:
ST depression or T-wave inversion
No ST elevation
Troponin:
⬆ Elevated
Treatment:
Antiplatelets
Anticoagulants
Possible PCI
Not usually immediate thrombolytics
Early sign of MI
Diaphoresis
Nausea & vomiting
Chest pain radiating to neck/shoulder
Hypertension
Tachycardia (starts off tachy!)
Late sign of MI
↓ BP (due to ↓ cardiac output)
Bradycardia (can occur later)
Crackles
JVD
S3 or S4
Fever (inflammatory response from cell death)
Skin: ashen, clammy, cool
NCLEX clue:
Early = SNS stimulation
Late = Pump failure
What is Stable Angina in more detailed?
Temporary myocardial ischemia - angina is the symptoms
NO permanent cell death
NO troponin elevation
Heaviness or tightness
Comes on gradually
Predictable (stable angina)
Goes away with rest
Goes away with SL nitroglycerin
May radiate to arm, jaw, scapula
Associated nausea or dyspnea
Angina is NOT:
Sharp, fleeting pain
Random stabbing pain
Angina Management
Nitroglycerin
How it works:
Dilates blood vessels
↓ preload
↓ afterload
Improves coronary blood flow
teaching about nitroglycerin
Sit down before taking - d/t otho. hypo.
1 tablet, then call EMS (home setting)
Assess vitals
Apply oxygen (if needed)
Put patient on cardiac monitor
Give SL nitroglycerin
Reassess pain and BP
May repeat every 5 minutes × 3 if BP stable
You do NOT call EMS — because you are already in an acute care setting.
Store in dark bottle
Headache is common (treat with acetaminophen)
Remove transdermal patch after 10–12 hrs and have free time. Rotates sites
Nurses: Wear gloves when administering, do not apply where defibrillator pads might go—can cause burning if needed
Pt has chest pain with transdermal patch recently applied –contact HCP—do not give another patch
DO NOT take with sildenafil (Erectile dysfunction drug) (severe hypotension risk)→ s/s priapism
Chest Pain Differences from MI and Angina
Occurs in BOTH:
Radiating chest pain
Epigastric distress
MI ONLY:
Pain not relieved by NTG
Fear/impending doom
Pain relieved by opioids
Persistent >20 min
Biomarker elevation
ANGINA ONLY:
Pain relieved by NTG
Main Diagnostic measure for MI
Troponin (>0.05=MI)
Others: Increased Myoglobin, Lactate dehydrogenase, Creatin Kinase (CK)
What about if troponin comes negative? How to further assess the narrowing?

Angina vs MI — KEY DIFFERENCES
Feature | Angina | MI |
|---|---|---|
Cause | Temporary ischemia | Prolonged ischemia → cell death |
Pain Duration | <15 minutes | >20 minutes |
Relief | Rest & nitroglycerin | Not relieved by NTG |
Troponin | Normal | Elevated |
ECG | May be normal | ST changes (STEMI/NSTEMI) |
Tissue Damage | No | Yes |
Fever | No | Yes (late sign) |
Opioids needed? | No | Yes (often morphine) |
What is Acute Coronary Syndrome (ACS)
Unstable Angina + Myocardial Infarction = ACS
ACS occurs when:
Atherosclerotic plaque ruptures
Acute thrombus forms
Coronary blood flow is reduced or blocked
Myocardial ischemia occurs
May progress to infarction (irreversible damage)
It is a medical emergency.
Emergency Management of ACS
MONA-B:
Morphine
Oxygen
Nitroglycerin
Aspirin
Beta blocker
What is Sudden Cardiac Arrest?
Unexpected death within 1 hour of symptom onset.
It is usually caused by a lethal dysrhythmia, most commonly:
Ventricular Fibrillation
How Sudden Cardiac Arrest connect to MI?
A myocardial infarction can:
Damage tissue
Create electrical instability
Trigger VT → VF
Cause sudden cardiac arrest
Thrombolytic drugs: Indication, contraindications, s/e, antidote?
Suffix: ase
Examples: Streptokinase, Alteplase,
Indication: dissolve (lysis) unwanted blood clots; Used for strokes, heart attack, pulmonary embolism, DVT
Contraindications:
Recent surgery, active bleeding, uncontrolled ypertension, current anticoagulant use, NSAIDS
AE: Bleeding
Antidote: Aminocaproic Acid
What is Mitral valve stenosis?
The mitral valve opening is narrowed
Blood cannot pass easily into the LV
Blood backs up into the LA
Common caused of Mitral valve stenosis?
After untreated strep throat:
Rheumatic Fever → s/ s Joint Inflammation, Sydenham chorea, Truncal Rash ← Primarily in Children
What Happens to Blood Flow during Mitral valve stenosis?
1⃣ LA pressure increases
2⃣ LA enlarges
3⃣ Blood backs up into lungs
4⃣ Pulmonary congestion occurs
What is Mitral Valve Regurgitation?
“Permits backflow of blood from the left ventricle to the left atrium during ventricular systole.”
The valve does NOT close completely
Blood leaks backward into the left atrium
That backward flow causes the murmur.
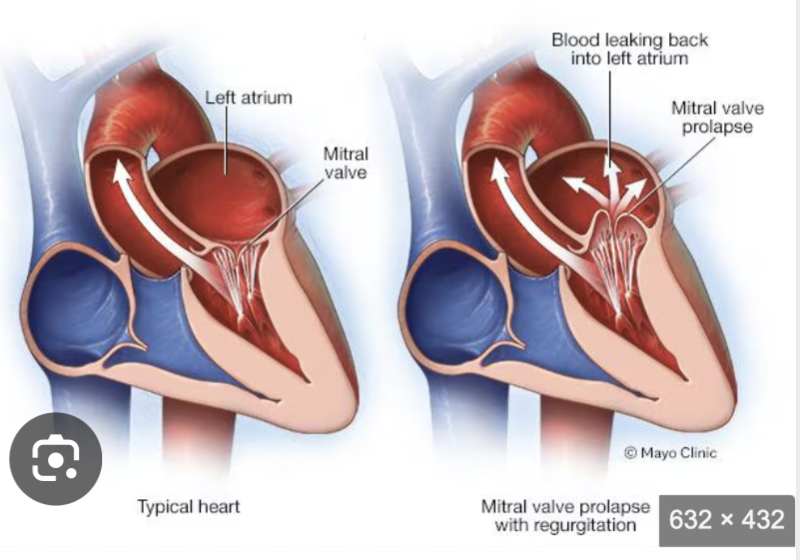
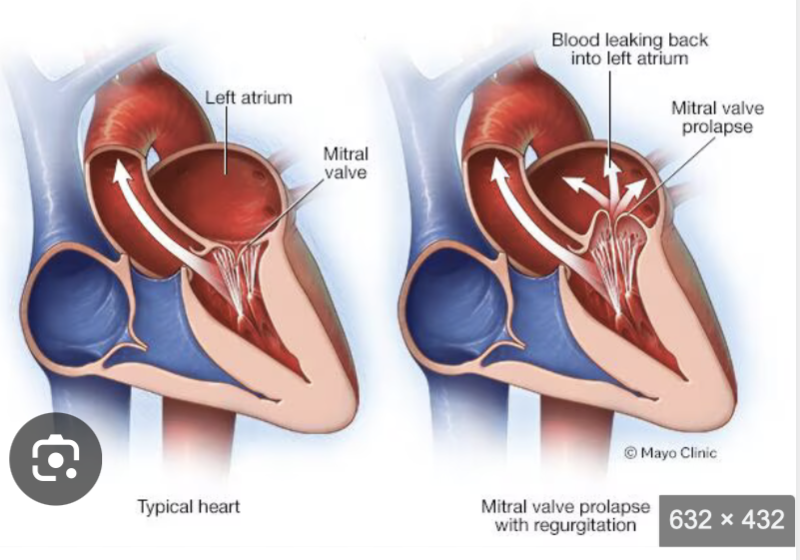
What is Mitral Valve Prolapse?
What Happens in Mitral Valve Prolapse?
Normally:
During systole (ventricular contraction)
The mitral valve closes tightly
Blood moves forward into the aorta
In MVP:
The valve cusps bulge (billow) upward into the left atrium during systole
Because they do not close tightly:
Blood may leak backward into the LA
This can cause mitral regurgitation
What is Aortic stenosis
The aortic valve opening is narrowed
Blood has difficulty leaving the LV
The LV must work much harder to pump blood out
Why Does It Happen?
Age-related calcification
Congenital bicuspid aortic valve
Accumulates Over Decades
This is a slow, progressive disease.
What Happens to the Heart?
LV pressure increases
LV muscle thickens (left ventricular hypertrophy)
Eventually → ↓ cardiac output
This is a pressure overload problem.
SAD
Syncope (especially with exertion)
Angina
Dyspnea (heart failure)
What is Aortic Regurgitation?
“The leaflets cannot close properly during diastole.”
Normally:
During diastole, the aortic valve closes
Prevents blood from flowing back into the left ventricle (LV)
In aortic regurgitation:
The valve does NOT close completely
Blood leaks backward from the aorta → left ventricle
This is called regurgitation (insufficiency).
What Is Infective Endocarditis?
An infection of the inner lining of the heart (endocardium), usually affecting the heart valves.
Most commonly caused by:
Bacteria
How Do Bacteria Get There that causes Infective Endocarditis (Valves)?
Bacteria enter the bloodstream (bacteremia) through:
IV drug use (injection of drugs)
Trauma
Dental procedures
Genitourinary procedures
Indwelling urinary catheters
GI instrumentation
Spread from respiratory infections
What Happens in the Heart that causes Infective Endocarditis (Valves)?
Bacteria attach to damaged endothelium (usually a valve)
2⃣ They multiply
3⃣ They form vegetations
Blood-borne microorganisms adhere and proliferate, infiltrate thrombi, and accelerate the clotting cascade
That means:
Infection + clot formation happen together.
Manifestations of Infective Endocarditis, complication
Fever
New or changed cardiac murmur
Petechial lesions of the skin, conjunctiva, and oral mucosa
weight loss
back pain
night sweats
Manifestations secondary to embolism in any organ
Why Is Aortic Valve Endocarditis So Dangerous?
Heart failure in up to 80% with aortic valve endocarditis
Manifestations secondary to embolism in any organ
Spleen, kidney, peripheral blood vessels
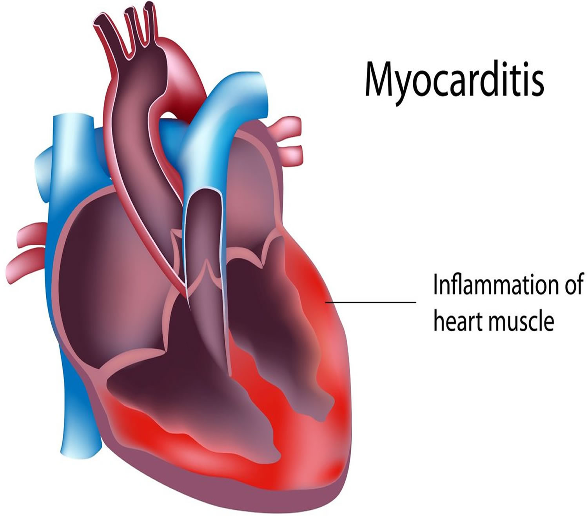
What Is Myocarditis?
inflammation of the heart muscle (myocardium).
This can reduce contractility → ↓ cardiac output.
what causes Myocarditis?
Immune –mediated disease (IBD, SLE)
Physical agents (ETOH)
Bacteria, Viruses, Fungal and Parasitic (see Box 18.3)
(i.e., HIV, Influenza, Strept, Candida)
what is Pericardial Effusion? s/s
“Fluid Around the Heart”
The heart sits inside a sac called the pericardium.
Normally:
There is a small amount of lubricating fluid (15–50 mL).
In pericardial effusion:
Excess fluid accumulates in the pericardial space.
S/S of right heart failure
an abnormal accumulation of fluid in the pericardial cavity.
what is Cardiac Tamponade
when Pericardial Effusion become severe → Fluid in the pericardium builds up and results in compression of the heart.
Onset may be rapid or more gradual.
Sign and Symptoms of Cardiac Tamponade
cardiogenic shock; shortness of breath, weakness, lightheadedness, and cough
muffled
What Is Acute Pericarditis?
inflammation of the pericardium, the sac surrounding the heart.
When inflamed:
The pericardial layers rub against each other
Causes sharp chest pain
May produce a friction rub
What causes Acute Pericarditis?
Idiopathic
Viral Cause (influenza, hepatitis, measles, mumps, varicella)
HIV* most common complication of HIV is Pericarditis
MI, Trauma, surgery, uremia, TB
Connective tissue diseases
Radiation therapy
Clinical Manifestations Acute Pericarditis?
Pain worsen when supine → Position in upright position and sl leaning forward as this decrased pain by using gravity to take pressure off heart muscle
Inflammation
Fever
Pericardial Damage
Leukocytosis
Malaise
Tachycardia
What is Chronic Pericarditis?
After repeated or severe pericarditis:
The inflamed pericardium heals with fibrosis and scarring
The sac becomes thick, rigid, and non-elastic
It may even calcify
Instead of being soft and flexible, it becomes like a tight shell around the heart.
Symptoms of Chronic Pericarditis
Activity intolerance
Weakness
Fatigue
Systemic venous congestion
Goal: improve cardiac contractility.