Mastitis and Ketosis in cattle
1/64
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
65 Terms
Managing mastitis risk
Mastitis risk varies throughout lactation
typically the risk of infection when milking decreases as the lactation progresses
Key points in lactation when the cow’s risk of infection is highest
drying off
calving
Teat and udder defences
The udder comprises 4 separate quarters
each is a separate gland
Mammary cistern- reservoir of milk ready for release
Lactiferous ducts- Interlobular ducts group together to form a network
Mammary lobes- mammary lobules (groups of mammary alveoli) surrounded by connective tissue drain into an interlobular duct
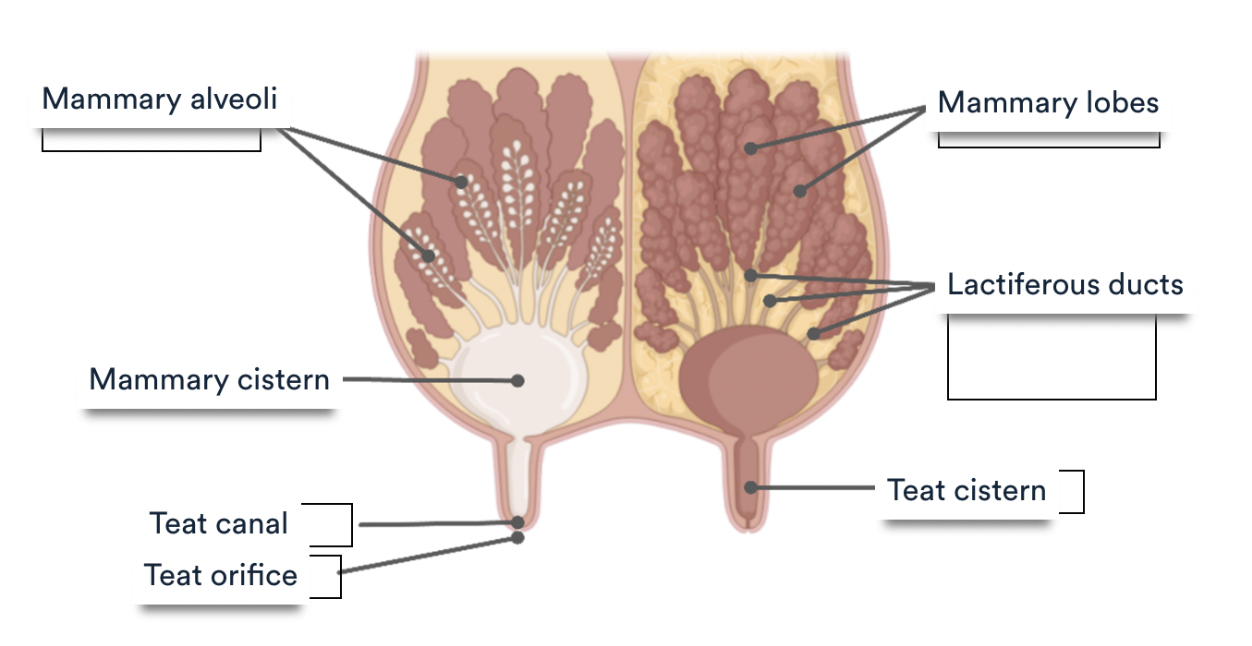
What are the main immunological cells (4) which are able to protect against invading pathogens?
macrophages
epithelial cells
small numbers of lymphocytes and neutrophils
How many cells cells does a healthy gland normally have?
<100,000 cells/ ml but it varies with lactation stage and parity
How is the teat canal built for defence?
Teat canal has its own physical defences against pathogens
It is lined with stratified squamous epithelial keratinised for protection and kept closed by a tight muscular sphincter.
The irregular inner surface and lipid layer is naturally hostile to bacteria preventing them from colonising
Sphincter closure forms a tight seal and prevents entry on contact
If any bacteria enter, its trapped here and flushed out when milked (“keratin flush”)
During dry period a keratin plug made from sloughed cells forms here creating a physical barrier
Outer teat skin creates a hostile substrate for bacterial growth through a layer of bacteriostatic fatty acid
What does lactoferin do?
It competes with pirate to remove iron (needed for bacterial growth)
Effective only during the dry period, as levels are low during lactation.
What does lactoperoxidase do?
Inhibits bacterial growth
What do complement proteins, antibodies and WBC do?
Involved in local immune responses to kill bacteria within the udder
What does the inflammatory response do?
Facilitates systemic immune response if local responses fail, is responsible for clinical signs associated with mastitis and can lead to severe systemic illness
What are the biggest risk factors that increase the risk of mastitis in cows at herd level?
Environment:
teats in contact with ground for 12-14 hours/ day
bacteria in bedding
faecal contamination of bedding
high ambient temperatures or humidity
Contagious:
transmission between cows using same machines in parlour
teat-teat contact
contamination of milking machine and its components through people or cow cleanliness
poor dry cow management
Mastitis prevention
Clinical cases of mastitis require treatment but prevention is crucial management
important for animal health and welfare, productivity, economics, food security, farm staff morale
Mastitis prevention- 5 point plan
using antibiotic dry cow treatment for infected cows at the end of lactation
early and effective treatment in lactation and recording clinical mastitis cases
culling chronic mastitis cases
post-milking teat dipping
milking- achine maintenance
*dramtic drop in contagious mastitis but not environmental mastitis
Name a big factor in managing mastitis risk from environmental causes?
Bedding substrate
Name different types of bedding substrates?
Straw
Sand
Rubber mats or mattresses
Oat husks
Sawdust or wood shavings
Straw as a bedding substrate
Staw can be used long or chopped, not suitable if there are slats, chopped straw can be spread on top of other bedding to improve comfort
Sand as a bedding substate
Sand is inorganic, inhibits bacterial growth. Sand can be difficult to dispose of and can damage machinery. Comfortable if deep enough
Rubber mats or mattresses as a bedding substrate
Can be disinfected, not always very comfortable (mats especially)
Oat husks as a bedding substrate
Comfortable if deep enough, by product of food industry. Cheaper than sand and non-abrasive so better for machinery. Added disinfectant e.g. lime recommended to inhibit bacterial growth
Sawdust or wood shavings as a bedding substrate
Cheap and comfortable if deep enough, does not dry quickly when damp and allows bacterial growth. Commonly has a disinfectant added to control bacterial growth e.g. lime. Poor quality shavings can be abrasive and uncomfortable
What bedding substrate is best to prevent mastitis?
Sand
When is the most effective time to achieve bacteriological cure?
During the dry period
Treatment of cows with a long acting intramammary antibiotic at drying off can be very effective
Utilising the dry cow period makes it more likely to achieve complete cure, lowers the risk of milk contamination with antibiotic residues, and offers some protection for pathogens of dry period origin.
True to false:
It is recommended to to dry off chronically affected cows early
True- if necessary
How to achieve bacteriological cure during dry period?
Through the use of teat sealants- used to enhance the natural keratin plug or provide an artificial plug creating a barrier to infection
What are the types of sealants that are available?
Internal and external
What type of sealant is more effective (and more common)?
Internal sealants
Recommendations for sealants
all cows are treated with a teat sealant at drying off
sealants are suitable for organic herds
NOT recommended that all cows are treated with antibiotics at drying off due to antimicrobial resistance
Hygiene
Good cleanliness and hygiene in the milking parlour and milk storage is important for control of contagious pathogens and food security and regulations set by EU
Hygiene in the milking parlour
Milking machines must be hosed down during milking and cleaned immediately after every milking- external and then internal surfaces
2 ways to do this:
Hot circulation cleaning
Acidified boiling water cleaning
Hot circulation cleaning
warm pre rinse, a hot re- circulation wash with a sanitiser solution and a final cold rinse (ideally containing 25ml hypochlorite/ 40l of water)
± milk stone remover as needed to prevent scale build up
Acidified boiling water cleaning
A once through hot wash with acid solution. Replace acid with hypochlorite once weekly to prevent biofilms
Milk tank storage rules- temperature
Milk must not be exposed to risk of contamination whilst stores. It must be cooler immediately after collection to <8DC if collected daily or 6DC if not collected daily. The interior of the rank must be cleaned every time it is empties
How to treat mastitis?
Antibiotic treatment of individual cows to kill or inhibit bacterial growth
How can mastitis treatment be administered?
Can be:
intramammary- application into the mammary gland
or systemic- injectable antibiotics
Other than antibiotics what other treatment should be given?
poin relief
fluid therapy
regular stripping of the udder
good nursing care
What do you do if cows don’t respond to treatment?
Cull
send cows to abattoir
but only cows that are not unwell- need to be fit for travel and food chain
cows with chronic high cell count (i.e. sub-clinically affected cows) or cows with recurrent mastitis during the time they are healthy.
If unwell and welfare is compromised she can be humanely euthanised on farm, only in severe cases
Other options apart from cull for a cow not responding to mastitis antibiotics
Dry off early
many cure themselves in dry period
most suitable if she is coming to end of lactation
also possible to dry off individual quarters- more suitable in early lactation when milk yield is high
How do you assess for milk cleanliness and quality?
routine testing of bulk tank milk
total bacteria count (TBC) done on individual samples
What is important when collecting samples?
aseptic collection of samples
e.g. no contamination with bacteria
important to avoid misdiagnosis
not waste money on tests that don’t get an answer
What tests are routinely used now?
Bactoscan
SCC
(TBC is an old test not used commonly anymore)
What is tested before milk leaves farm?
bulk tank sample tested for:
bactoscan
SCC
antibiotic residues
What is bactoscan?
A measure of total number of bacteria present- dead and alive
Used electronic counting method- 10 mins
Quicker and more accurate than TBC
When do penalties occur for bactoscan?
>50 = penalties
but aim for <20
What is SCC used for?
Important measure of milk quality
number of cells per ml of milk
What cells are measured in SCC?
Leucocytes
Epithelial cells
NOT bacterial cells
How often is milk tested?
Minimum monthly
What must the rolling 3 month average be for EU consumption?
<400,000 cells/ ml
What is the US threshold for SCC?
<750,000 cells/ml
What is the normal level before penalties are introduced for SCC?
Most milk buyers introduce penalties if SCC > 200,00 cells/ ml
Total bacterial count (TBC)
measures number of bacterial cultured (cfu)
Takes 72 hours at 30DC
Requires special growth media
Does not measure all types of bacteria
Milk must be tested twice monthly minimum
Must have rolling 2 month average <100,000 cfu/ ml to be considered fit for consumption
Replaced by bactoscan for routine use by most milk buyers
TBC= TVC total viable count
Identifying pathogens
Mastitis management is conducted at herd level and farm data analysis to identify trends and make decisions regarding management. Identification of individual pathogens is useful in some circumstances such as new outbreaks, suspected treatment failures.
If pathogen identification is required there are 2 key rules:
1- Sample the cows that are representative of your problem
2- Take clean samples so that the only bacteria in the milk are those causing mastitis
How to identify the species of bacteria?
Milk samples are cultured on agar plates to grow the bacteria which is present in milk
The resulting colonies are examined for their appearance, and if needed biochemical assays can then be used to identify the species present
What is the standard method for identifying Staphylococcus species?
Blood agar culturing
Conditions needed for blood agar sampling
The aseptic milk sample is streaked onto a blood agar plate and incubated at 37DC for 24hrs.
What are blood agar plated used to determine?
Bacterial enzymes which haemolyse red blood cells
Visual appearance of blood agar plate?
Distinctive glistening, smooth, raised colonies, with a golden-brown colouration, but this is not conclusive.
Visual appearance of blood agar plate?
The way the bacterial enzymes haemolyse (clear zone around colonies) the blood cells in the agar can be used for identification
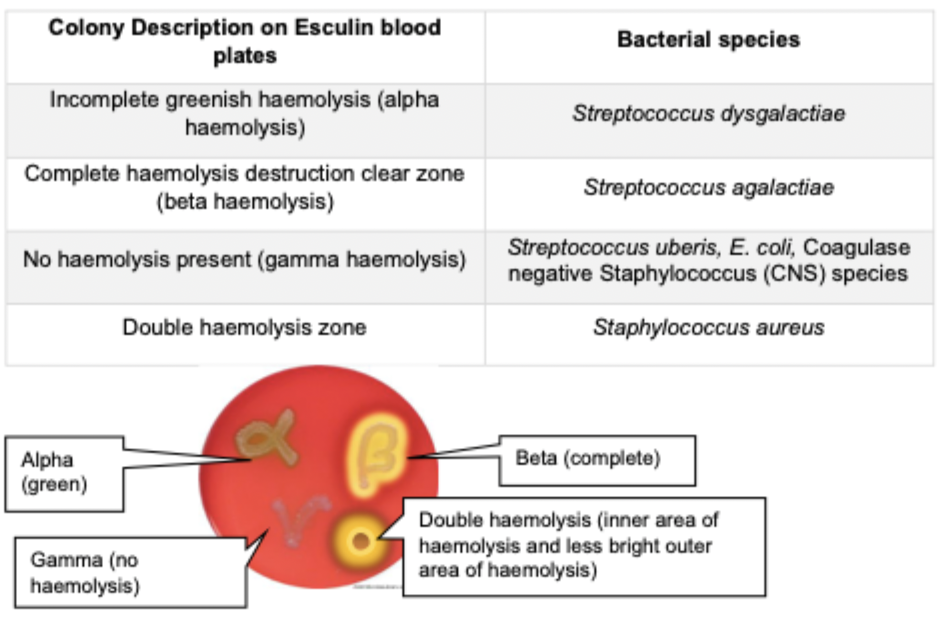
What does adding Esculin to agar do?
Allow identification of S. uberis
Fluorescence under UV light
When Esculin is cleaved by S. uberis, the medium surrounding the bacterial colony turns black
What does the CAMP test allow identification of?
To differentiate streptococcus agalactiae from other Streptococci
S. agalactiae produces a protein called the CAMP factor which reacts with the Beta haemolytic of Staphylococcus an extra zone of haemolytic can be seen where 2 factors interact.
This forms an ‘arrowhead’ when the 2 bacterial species are grown perpendicular to each other
What is the catalase test used for?
Distinguishing between Streptococcus and Staphylococcus species
Catalase is an enzyme that breaks down hydrogen peroxide into water and oxygen resulting in bubbles being seen when the reaction occurs.
Results of a catalase reaction?
positive result will bubble = staphylococci
if no bubbles = streptococci
What is the coagulase test used for?
Distinguish between coagulase positive Staphylococcus aureus and coagulase negative Staphylococcus haemolytic or epidermidis
Coagulase negative staphylococcus (CNS) are typically normal skin flora and often naturally cleared from the udder.
The test involves mixing the bacterial samples with rabbit plasma; the fibrinogen in the plasma is converted to fibrin and forms a clot or aggregate.
What is a positive coagulase test?
The test is positive if clumps form
MacConkey agar
A selective agar used to differentiate between coliforms (gram negative lactose fermenters). Pink colony growth shows the presence of lactose fermenting bacteria, E. coli grow as small non-mucoid colonies, and Klebsiella grow as large colonies with a ymucoidal appearance