Lecture 6 - Clinical Psychology
1/89
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
90 Terms
mood disorders
• Disorders, such as depressive disorders or bipolar disorders, in which there are disabling disturbances in emotion.
distinct categories of mood disorders (2)
• unipolar mood disorder
• bipolar mood disorder
Types of unipolar mood disorder (4)
• major depressive disorder
• persistent depressive disorder
• premenstrual dysphoric disorder
• disruptive mood dysregulation disorder
Types of bipolar mood disorder (3)
• Bipolar I
• Bipolar II
• Cyclothymia
episodic disorder
• A condition, such as major depressive disorder, whose symptoms dissipate but that tends to recur.
major depressive disorder (MDD)
• An episodic disorder marked by sadness or anhedonia, along with symptoms such as feelings of worthlessness and guilt; withdrawal from others; loss of sleep, appetite, or sexual desire; and either lethargy or agitation.
Criteria for diagnosis of major depressive disorder (8)
• sad mood or anhedonia
At least 5 of following symptoms:
• increase/decrease in weight or appetite
• insomnia or hypersomnia
• psychomotor retardation or agitation
• fatigue or loss of energy
• poor attention or concentration or indecisiveness
• sense of worthlessness or guilt
• recurrent thoughts of death or recurrent suicidal ideation
anhedonia
• A negative symptom in schizophrenia or a symptom in depression in which the individual experiences a loss of interest and pleasure. See also anticipatory pleasure and consummatory pleasure.
psychomotor agitation
• A symptom characterized by pacing, restlessness, or inability to sit still.
psychomotor retardation
• A symptom commonly observed in major depressive disorder in which the person moves their limbs and body slowly.
How is the clinical picture of MDD characterized?
• very complex → >10.000 unique combinations of symptoms possible if you account for all sub-symptoms
• MDD not single-entity disorder, but heterogenous condition with multiple clinical presentations
persistent depressive disorder
• A DSM-5-TR disorder defined by depressive symptoms that last at least 2 years in adults or 1 year in youths.
Criteria for bipolar depression
• all symptoms of depression + mania
→ lasting at least 1 week (for mania) / 4 days (for hypomania) and present most of days
manic symptoms (7)
• Distinctly elevated or irritable mood
• Abnormally increased activity or energy
At least 3 of following (4 if mood is only irritable):
• inflated self-esteem or grandiose ideas
• decreased need for sleep
• increased talkativeness (pressure to keep talking)
• flight of ideas or subjective experience that thoughts are racing
• increased distractibility
• increase in goal-directed activity or psychomotor agitation
• excessive involvement in pleasurable activities (that are likely to have painful consequences)
flight of ideas
• A symptom of mania that involves rapidly shifting thoughts, manifested in a conversation style in which a person shifts rapidly from one topic to another with only superficial associative connections.
hypomania
• An extremely happy or irritable mood accompanied by symptoms such as increased energy and decreased need for sleep, but without the significant functional impairment associated with mania.
key differences between mania and hypomania (3)
• mania: >/=7 days, psychotic symptoms, impaired daily functioning (social, work, family)
• hypomania: >/= 4 days, no psychotic symptoms, no impaired daily functioning
bipolar I disorder
• A diagnosis defined on the basis of at least one lifetime episode of mania. Most people with this disorder also experience episodes of major depression (but not diagnostic criterion).
bipolar II disorder
• A form of bipolar disorder diagnosed in those who have experienced at least one major depressive episode and at least one episode of hypomania.
cyclothymic disorder
• A form of bipolar disorder characterized by swings between elation and depression over at least a 2-year period, but with mood changes not so severe as manic or major depressive episodes.
epidemiology of depression
• unipolar depression: ~280 million people suffer from it, ~15-20% life time prevalence of MDD
• bipolar depression: ~37 million people suffer from it, ~3-4% life time prevalence of bipolar I and II
onset of mood disorder
• early → ~25-30 years globally
recurrence risk of mood disorders
• MDD ~50% after first episode, ~70-90% after >/= 2 episodes
• comparable for bipolar (often >80% lifetime recurrence)
episode duration of mood disorders
• 3-6 months for depressive episode
• 2-3 months for manic episode
suicide risk of mood disorders
• depression: ~2-6%
• bipolar: up to 10-15%
gender differences in mood disorders (3)
• more pronounced in depression (twice as likely in women)
• less pronounced in bipolar disorder (similar prevalence across sexes) → women more likely to experience bipolar II because of depressive symptoms
• differences emerge in adolescence
possible explanations for gender differences in depression(4)
• biological: hormonal fluctuations (puberty, postpartum, menopause)
• psychological: higher internalizing coping styles (rumination)
• social: gender roles, discrimination, unequal burden of caregiving, exposure to violence
• men may show depression differently (e.g. irritability, substance use) and are more likely to be underdiagnosed
risk factors for mood disorders (3)
• socioeconomic status (SES): higher rates with poverty, unemployment, financial
• education: lower education is associated with higher depression risk
• employment: job insecurity and work stress linked to mood disorders
cultural/ethnic differences (3)
• stigma influences reporting and help seeking
• symptom presentation varies (e.g. somatic symptoms more common in non-Western contexts)
• chronic stress and adversity (e.g. discrimination) increase risk
comorbidity of mood disorders
• high comorbidity: most individuals with mood disorders meet criteria for at least 1 additional disorder
common comorbid condition (3)
• anxiety disorder
• substance use disorders
• impulse-control disorders (especially in bipolar disorder)
Shared vulnerabilities of mood disorders and comorbidities (4)
• genetics
• neuroticism
• early life stress
• dysregulated stress response
clinical implications of comorbidities (3)
• more severe symptoms
• greater functional impairment
• more complex clinical course
physical comorbidities (3)
→ most strongly established for depression, also relevant in bipolar disorder
• cardiovascular disease (CVD): depression associated with increased risk of CVD and poorer health outcomes → possible mechanisms: inflammation, HPA dysregulation, lifestyle factors
• chronic medical conditions (e.g. diabetes): depression more common in individuals with chronic illness → can negatively affect health behaviors and treatment adherence
• other conditions: bidirectional relationships between mood disorders and physical health
burden of disease
• measures impact of living with illness and injury by financial cost, mortality, morbidity, or other indicators
global burden of disease
• summarizes global trends for wide range of illnesses and causes of injury
DALYs
• disability-adjusted life years
YLLs
• years of life lost
YLDs
• years lost through disability → depression leading cause of years lost through disability
How do you “calculate” disease burden?
• disability-adjusted life years (DALYs) = years lost through disability (YLDs) + years of life lost (YLLs)
Why are mood disorders like depression leading contributors to the disease burden?
• excess rates of mortality (e.g. suicide)
• disability - poor functioning: education, unemployment, work disability, economic consequences, intimate relationships, intimate partner violence, poor parental functioning and offspring outcomes
biomedical model
• depression is caused by chemical imbalances, brain structure changes, or genetics
• treatment: medication, brain stimulation (e.g. transcranial magnetic stimulation)
psychosocial model
• depression caused by negative life experiences, stress, or maladaptive thoughts
• treatment: psychotherapy, social support, lifestyle changes
biopsychosocial model
• combines views of biomedical model and psychosocial model
biological factors in depression (4)
• genetics: often runs in families along with SUD, anxiety disorders (40% risk for offspring of parents with depression), in most cases preceded by childhood onset disorders (e.g. ADHD)
• brain damage before birth: low birth weight, infections during pregnancy, birth complications increase risk
• medical & drug-related causes: some illnesses, medications, and substances (e.g. alcohol, drugs) trigger depression
• brain imaging studies: depressed individuals often have reduced brain volume in areas controlling emotion
striatum
• A region of the brain involved in motor action and responses to reward.
dorsolateral prefrontal cortex
• A region of the prefrontal cortex that is involved in working memory, motor planning, organization, and regulation. Atypical activation patterns are implicated in many psychopathologies.
anterior cingulate
• In the subcortical region of the brain, the anterior portion of the cingulate gyrus, stretching around the corpus callosum.
sickness behavior
• A syndrome triggered by illness and by pro-inflammatory cytokines, characterized by decreased motor activity, lower food consumption, social withdrawal, changes in sleep patterns, and reduced motivation to pursue rewards.
circadian rhythms
• Twenty-four-hour biological rhythms that guide activity, alertness, and body functions.
clock genes
• Genetic polymorphisms that influence the strength and timing of circadian (day/night) rhythms
psychological factors in depression (3)
• early psychological stress: childhood trauma makes people more vulnerable to depression later in life
• personality traits: people high in neuroticism at greater risk
• cognitive biases: depressed individuals focus more on negative thoughts and struggle to shift attention away from them
social factors in depression (2)
• life stressors: events like job loss, divorce, or death of loved one often trigger depressive episode
• social support matters: having strong relationship can protect against depression, while loneliness increases risk
expressed emotion (EE)
• Hostility, criticism, and emotional overinvolvement directed from family members toward a person with a psychological disorder.
neuroticism
• The tendency to react to events with more frequent or greater-thanaverage negative affect; a strong predictor of onset of anxiety disorders and depression.
information-processing biases
• Tendencies to perceive events in a negative manner, for example, by attending to or remembering negative information more than positive information; hypothesized to be driven by underlying negative schemas.
attribution
• The explanations a person forms for why an event occurred.
attributional style
• Trait-like tendency to make a certain type of attribution for life events.
hopelessness theory
• Cognitive theory that focuses on hopelessness as a major influence of depression—an expectation that desirable outcomes will not occur and that no available responses can change the situation.
rumination
• Repetitive thought about why a person is experiencing a negative mood or sad events.
pathogenesis of depression
• likely multiple causes occurring together that cause depression → interaction
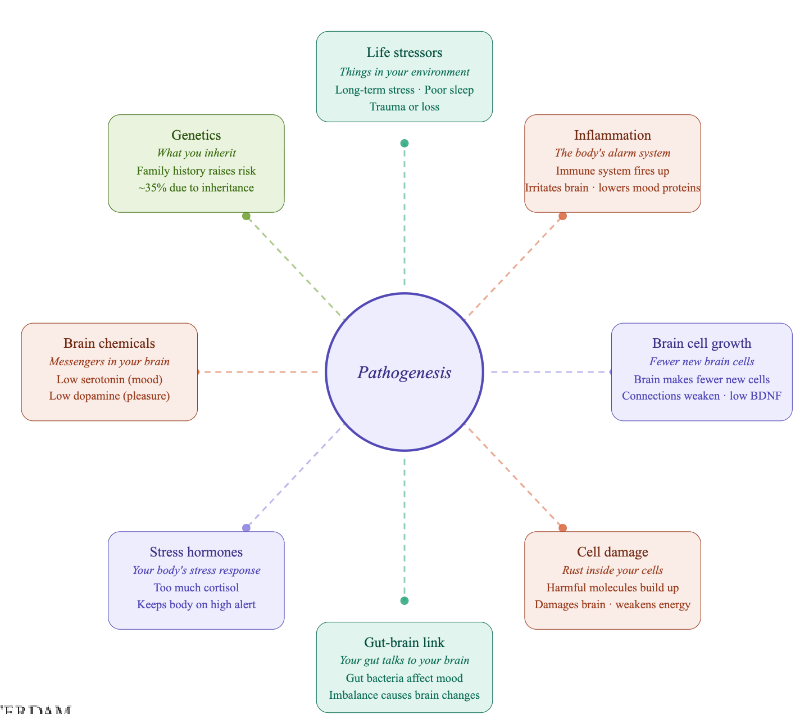
In which 3 phases does the biopsychosocial model explain depression?
• predisposing factors: genetics, childhood trauma, personality traits create foundation for risk
• precipitating factors: major stressor
• sustaining factors: negative thoughts, social withdrawal, low energy reinforce depressive state, making it harder to recover
implications of different factors for treatment of depression (3)
• biological approaches: e.g. Antidepressants (restore neurotransmitter balance), brain stimulation (e.g. TMS) (reactivate underactive brain areas)
• psychological approaches: e.g. CBT (helps change negative thought patterns)
• social approaches: e.g. building social support (connecting with family and friends), improving life circumstances (work, finances, relationships)
most important families of psychological treatments in depression (4)
• cognitive behavioral therapy
• interpersonal therapy
• behavioral activation
• problem solving therapy
effects of psychological treatments
• moderate to large
• considerably overestimated because of problems of randomized trials examining effects
• effects measured in “standardized mean differences” indicating difference between treatment and untreated control group in terms of standard deviations: 0.2 = small, 0.5 = moderate, 0.8 = large
Beck’s cognitive model (1967)
• emphasizes role of negative schemas
• core idea: depression results from maladaptive thought patterns shaped by negative schemas
• incorporates cognitive/negative triad
negative triad
• In Beck’s theory of depression, a person’s negative views of the self, the world, and the future, in a reciprocal causal relationship with pessimistic assumptions (schemas) and cognitive biases such as selective abstraction → negative beliefs reinforce each other
mindfulness-based cognitive therapy (MBCT)
• Adaptation of cognitive therapy for major depression; aims to “decenter” the person’s perspective in order to break the cycle between sadness and thinking patterns.
psychoeducation
• Especially with bipolar disorder and schizophrenia, intervention to help people learn about symptoms, expected time course, triggers for symptoms, and treatment strategies.
antidepressant
• Any drug that alleviates depression; also widely used to treat anxiety disorders.
different types of antidepressant medication (4)
• MAOIs (usually no longer used)
• SSRIs
• SNRIs
• TCAs
monoamine oxidase inhibitors (MAOIs)
• A group of antidepressant drugs that prevent the enzyme monoamine oxidase from deactivating catecholamines and indolamines.
tricyclic antidepressants
• A group of antidepressants with molecular structures characterized by three fused rings; they interfere with the reuptake of norepinephrine and serotonin.
selective serotonin reuptake inhibitors (SSRIs)
• A specific form of serotonin reuptake inhibitors (SRIs) with less effect on dopamine and norepinephrine levels; SSRIs inhibit the reuptake of serotonin into the presynaptic neuron so that serotonin levels in the cleft are sustained for a longer period.
serotonin–norepinephrine reuptake inhibitors (SNRIs)
• Any of various drugs that inhibit the presynaptic reuptake of serotonin and norepinephrine, such that both neurotransmitters will have more prolonged effects on postsynaptic neurons.
Effect of antidepressants
• strong placebo effect (38% respond after placebo, 52% after medication)
• not advised in children and adolescents (maybe increased suicide risk)
• some side effects: suicidality, agitation, irritability, sleep problems, weight gain, gastrointestinal, sexual problems
What’s better: antidepressants or psychotherapy (study results)? (3)
• combined treatment more effective than psychotherapy alone or pharmacotherapy alone
• no significant difference between psychotherapy and pharmacotherapy alone
• long-term follow-up (6-12 months): combined treatment > psychotherapy > pharmacotherapy
Clinical implications of these study results (4)
• best option: combination, especially for moderate to severe depression
• if only one treatment is offered, psychotherapy preferable due to higher acceptability
• current care often over-relies on pharmacotherapy alone, which may not be optimal
• health systems should invest more in making psychotherapy widely accessible
treatment gap
• ~80% of people don’t receive any treatment
approaches to decrease treatment gap (4)
• group psychotherapy
• telephone-based therapy
• task-sharing → delegation of care-task to non-specialists (e.g. nurses, or grandmothers)
• digital interventions
Effectiveness of these approaches
• individual, group, telephone, guided self-help: all effective vs. control & no significant differences among them
• unguided self-help: less effective than other formats, better than waiting list
Acceptability of these approaches
• individual & group CBT: more acceptable than guided self-help
• guided self-hel: less acceptable than individual, group, waiting list, care as usual
• telephone CBT: high acceptability
• unguided self-help: less acceptable than wait list
ranking of formats of psychotherapy
Group
Individual
Telephone
Guided self-help
Unguided self-help
Esketamine (Spravato)
• Esketamine (Spravato) is a nasal spray that was approved only for patients who did not obtain relief after trying two other antidepressants.
lithium
• A medication useful in treating both mania and depression in bipolar disorder.
suicide
• The intentional taking of one’s own life.
suicidal ideation
• Thoughts about intentionally taking one’s own life.
suicide attempt
• Acts intended to cause one’s own death.
nonsuicidal self-injury (NSSI)
• Behaviors that are meant to cause immediate bodily harm but are not intended to cause death.
means restriction
• An approach to suicide prevention in which access to lethal methods is reduced. Examples include keeping guns locked in cabinets, reducing the unrestricted sale of poisons, and erecting suicide barriers on bridges.