3. substance exchange
1/205
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
206 Terms
summarise the process of lipid digestion:
starts in mouth and stomach, but most takes place in duodenum and ileum
bile salts (not an enzyme!) emulsify lipids
then lipase hydrolyses ester bonds
describe the digestion of lipids:
bile salts neutralise stomach acid and emulsify large lipid globules → smaller lipid droplets
this increases SA for lipase to act on - triglycerides → fatty acids and monoglycerides
bile salts surround FA chains and monoglycerides to form micelles, making the FA chains more water soluble
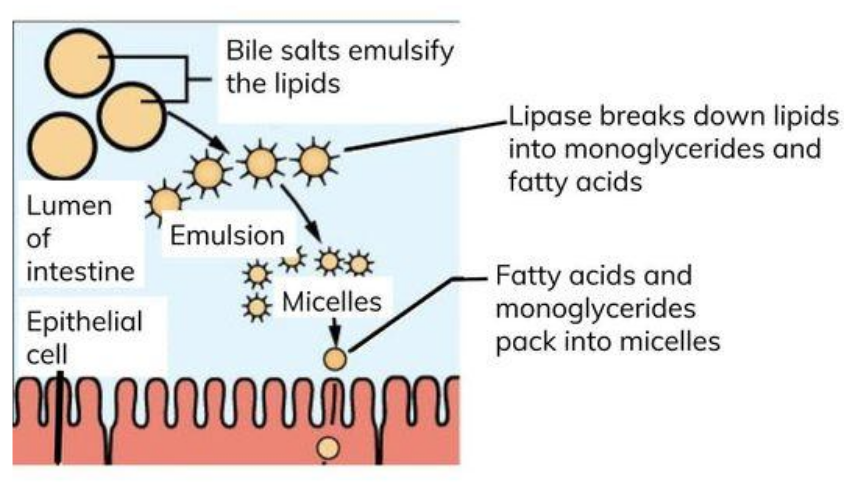
describe the process of absorption of triglycerides:
micelles contain bile salts, fatty acids and monoglycerides
micelles make fatty acids more water soluble and carry fatty acids to epithelial lining of ileum
micelles are broken down close to epithelial cells to release fatty acids and monoglycerides
micelles maintain a higher concentration of fatty acids to the lining of the ileum
fatty acids and monoglycerides diffuse into the epithelial cells that line the ileum
triglycerides reform inside the cell’s ER
triglycerides are packaged in the Golgi w/ cholesterol and proteins to form chylomicrons for transport
chylomicrons are released from the epithelial cells by exocytosis into lacteals (lymphatic vessels in the villi)
chylomicrons are transported via lymph vessels in the lymphatic system to the blood
where is lipase produced?
pancreas
where are bile salts produced and stored? how are they secreted into the duodenum and ileum?
produced in liver, stored in gall bladder
secreted into duodenum and ileum via bile duct
why can fatty acids diffuse across the epithelial lining?
non charged/non polar
explain the advantages of lipid droplet and micelle formation:
droplets increase SA for lipase action
∴ faster hydrolysis of triglycerides
micelles carry fatty acids and glycerol to intestinal epithelial cell
what is digestion?
the process in which large insoluble molecules are hydrolysed by enzymes to produce smaller molecules that can be absorbed and assimilated
give and explain 2 examples of mechanical digestion:
larger food molecules broken down into smaller pieces by teeth - allows ingestion and a large SA:V for chemical digestion
food churned by muscles in stomach wall
what does chemical digestion involve?
HCl
bile
digestive enzymes !
what is the duodenum?
first part of the SI
what is the ileum?
last part of the SI
describe the process of starch digestion:
glycosidic bonds in starch (polysaccharide) hydrolysed by amylase → maltose (disaccharide)
glycosidic bonds in maltose hydrolysed by maltase - membrane bound - → glucose (monosaccharide)

what does it mean for disaccharidases to be membrane bound?
positioned on membrane surface of epithelial cells in ileum
give 2 examples of disaccharidases (other than maltase) and where they are produced:
both produced in ileum:
sucrase
lactase
what is sucrase? what does it hydrolyse?
membrane bound disaccharidase
hydroluses sucrose → glucose + fructose
what is lactase? what does it hydrolyse?
membrane bound disaccharidase
hydrolyses lactose → glucose + galactose
where are carbohydrases produced?
salivary glands
pancreas
SI
describe the process of protein digestion:
peptide bonds hydrolysed
endopeptidases break internal peptide bonds
exopeptidases break terminal peptide bonds
membrane bound dipeptidases break dipeptides to AAs

what are endopeptidases? give 3 examples:
peptidases that act to hydrolyse internal peptide bonds, forming multiple peptide fragments
e.g. trypsin, chymotrypsin, pepsin

what are exopeptidases?
peptidases that act to hydrolyse terminal peptide bonds, removing single AAs from proteins and so forming a single peptide fragment and multiple AAs
what are dipeptidases? why are they important?
act to release the 2 AAs that make up a dipeptide by hydrolysing the peptide bond between them
membrane bound to the cell surface membrane of epithelial cells
important as amino acids can cross (cell) membrane whereas dipeptides cannot
where are peptidases produced?
(act in stomach) stomach
(act in duodenum and ileum) pancreas and epithelial cells
describe the absorption of glucose/AAs in the bloodstream:
co transport - how glucose/AAs are absorbed from epithelium into bloodstream:
Na+ ions are actively transported out of the epithelial cell into the blood
this lowers the conc of Na+ ions in the epithelial cell, creating a conc gradient of Na+ ions for Na+ to enter from gut
glucose enters by facilitated diffusion w/ Na+ - this is co-transport
there is now a higher conc of glucose inside the epithelial cell than the blood
glucose moves from cell to blood by facilitated diffusion
(there is no glucose buildup in the blood as the blood flows and carries away absorbed glucose)
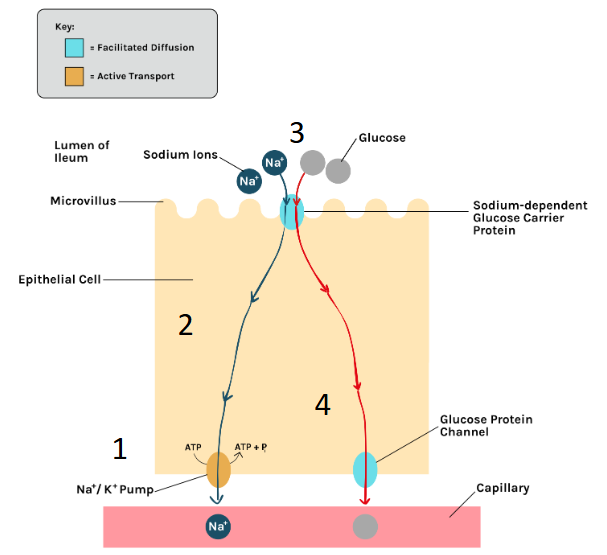
how is the surface of the ileum adapted to absorb digested substances?
villi and microvilli - increase SA for absorption
mitochondria - release ATP for active transport
carrier proteins - allow active transport/facilitated diffusion into epithelial cells
network of capillaries and peristalsis of muscles maintain diffusion gradient
what are microvilli?
highly folded cell-surface-membrane
explain the function of ATP hydrolase:
(hydrolyses ATP → ADP + Pi) release E
allows ions to be moved against a conc gradient/allows active transport of ions
describe and explain 4 structural features of capillaries that make them adapted for the exchange of substances between the blood and surrounding tissues (4):
any 4 from:
capillary wall permeable (has fenestrations) so molecules can pass through
capillary wall is 1 cell thick so reduces diffusion distance
flattened (endothelial) cells so reduces diffusion distance
small diameter/narrow so large SA:V/short diffusion distance
narrow lumen so reduces flow rate, giving more time for diffusion
why does blood flow through the lungs at a lower pressure?
prevents damage to capillaries around the alveoli
reduces speed of blood flow - more time for gas exchange
why is oxygenated blood pumped out of the blood at a higher pressure?
to ensure blood reaches all respiring cells
what is the role of the arteries?
to carry blood away from the heart
describe and explain the structure and function of arteries:
muscle withstands high pressure and control blood flow
elastic stretches and recoils to maintain blood pressure
smooth endothelium reduces friction
protein coat withstands high pressure

what is the role of the veins?
to return blood to the heart
describe and explain the structure and function of veins:
thin muscle layer - constriction and dilation cannot control blood flow
wide lumen - blood at low pressure
thin outer wall - does not need to w/stand high pressure
valves - prevent backflow
what is the function of capillaries?
link arterioles to veins - site of substance exchange
describe and explain the structure and function of capillaries:
wall 1 cell thick, flattened endothelial cells and small diameter - short diffusion distance
small diameter - larger SA:V
narrow lumen reduces flow rate - more diffusion time
fenestrations allow larger molecules to pass through
numerous and highly branched - large SA:V
what is the role of arterioles?
to reduce blood flow from arteries to capillaries
describe the structure and function of arterioles:
relatively thicker muscle layer than arteries
relatively thinner elastic layer than arteries
muscle layer contraction allows constriction of lumen - restricts blood flow into capillaries
elastic layer thickness due to lower blood pressure
compare veins and arteries:
veins have valves whereas arteries do not
veins have a wider lumen than arteries
arteries have more elastic tissue than veins
arteries have a thicker wall than veins
arteries have more muscular tissue than veins
why do all blood vessels have a smooth endothelium?
to reduce friction
what is diastole? what occurs during this process?
both atria and ventricles relaxed:
blood enters heart through vena cava and pulmonary vein
atrial pressure increases as blood is entering the atria
this causes the atrioventricular valve to open as the pressure in the atria is higher than the pressure in the ventricles
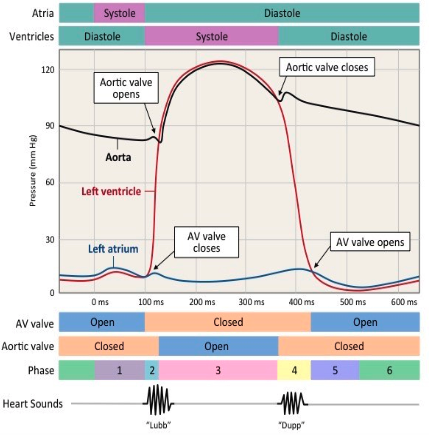
what is atrial systole? what occurs during this process?
atria contract (and ventricles relax):
contraction of atria causes atrial pressure to increase further
atrioventricular valves open
semi lunar valves still closed because pressure in arteries > pressure in ventricles
blood is being pumped from the atria to the ventricles
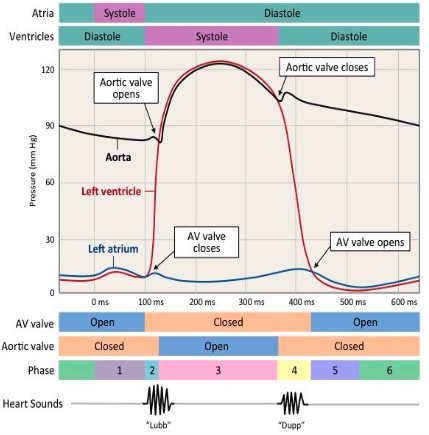
what is ventricular systole? what occurs during this process?
ventricles contract (and atria relax):
there is a short delay before the ventricles can contract because ventricles need to fill up completely before contracting
atrioventricular valves close as pressure in ventricles > pressure in atria
semi lunar valves open as pressure in ventricles > pressure in arteries
blood moves from ventricles to pulmonary artery/aorta
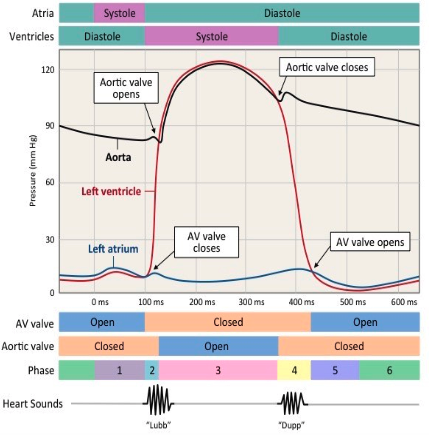
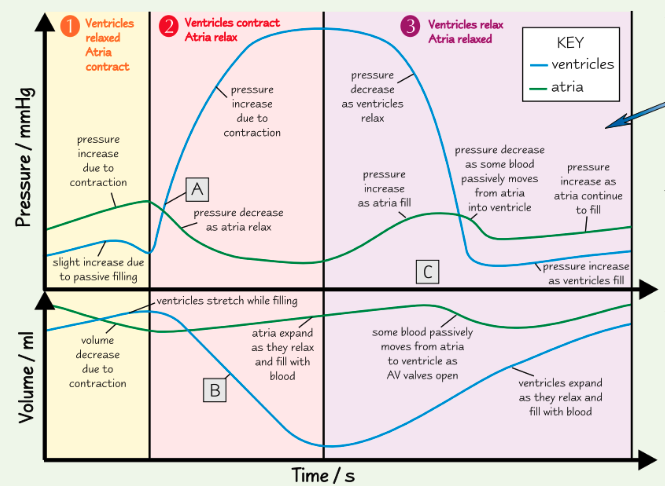
when does blood start flowing into the aorta? how do you know?
at point A, the ventricles are contracting (and AV valves are shut), forcing blood into the aorta
this can be seen by pressure increase in ventricles, meaning SL valve must open as ventricle pressure > aorta pressure
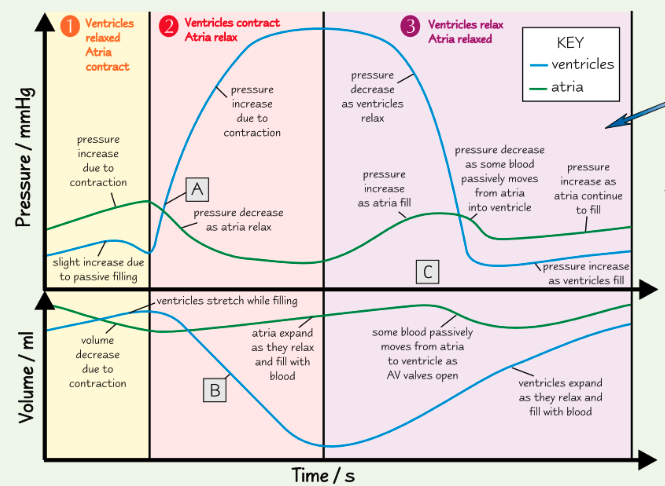
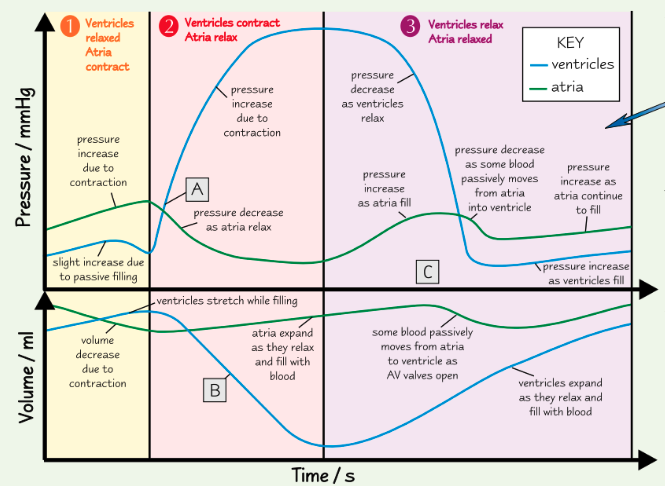
why is ventricular volume decreasing at point B? how do you know?
ventricles contract, reducing the volume of the chamber
can also be seen by pressure increase in ventricles
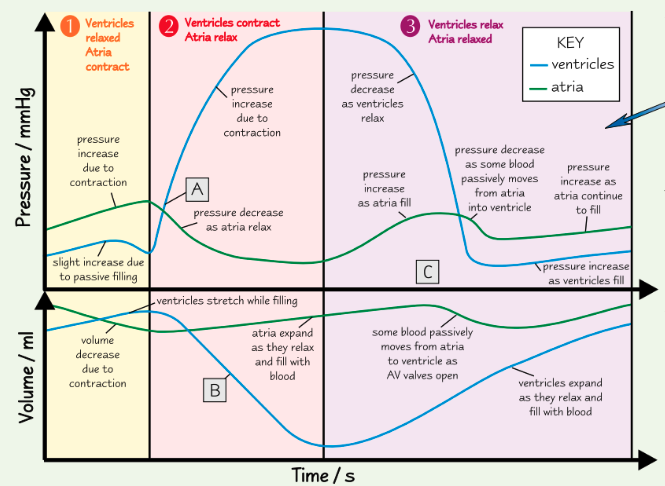
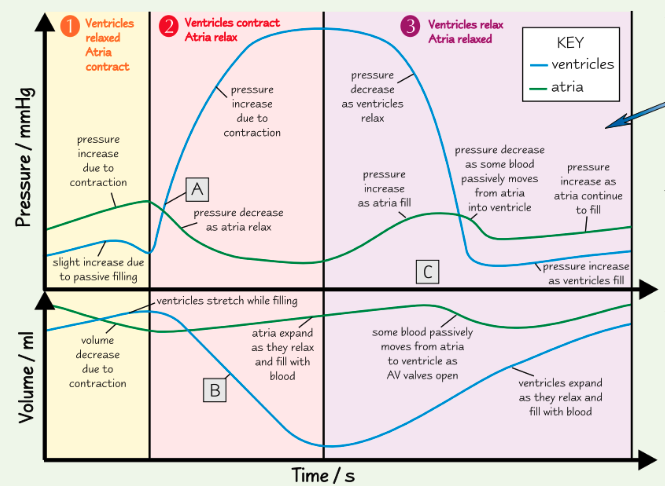
are the SL valves open or closed at point C? how do you know?
ventricles relaxed and refilling, so pulmonary artery/aorta pressure > ventricle pressure
so SL valves must be closed
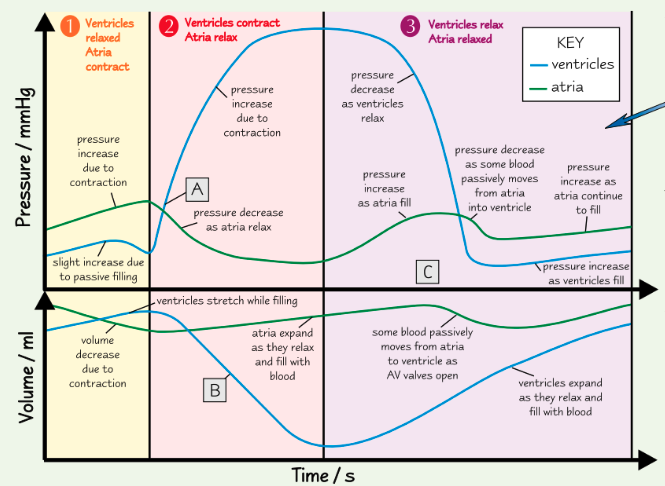
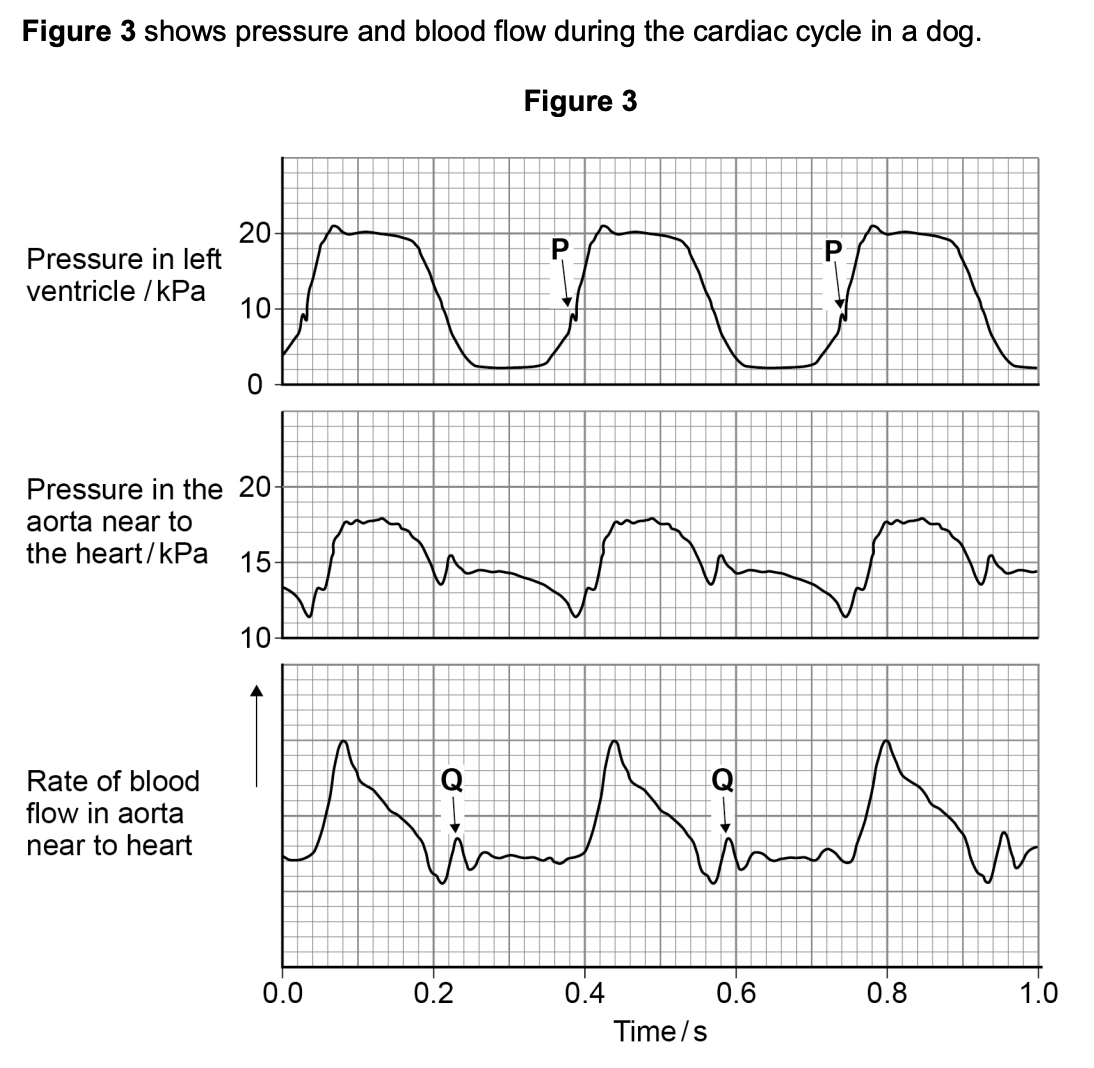
at Q in the diagram above there is a small increase in pressure and in rate of blood flow in the aorta - explain how this happens and its importance (2)

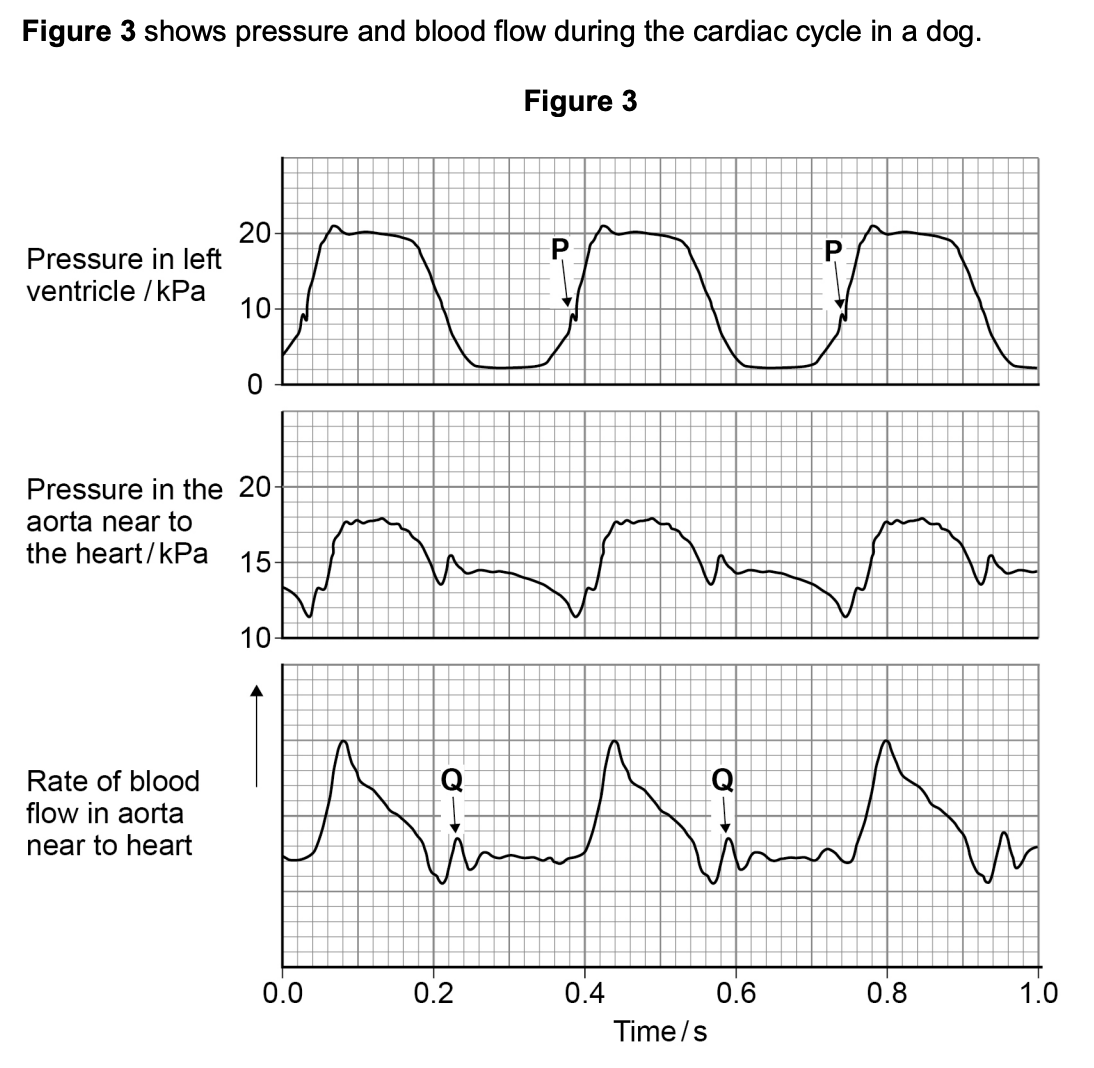
at P in the diagram above, the pressure in the left ventricle is increasing. at this time, the rate of blood flow has not yet started to increase in the aorta - use evidence from the diagram above to explain why (2)
semi-lunar valves closed
because pressure in aorta higher than pressure in the ventricle
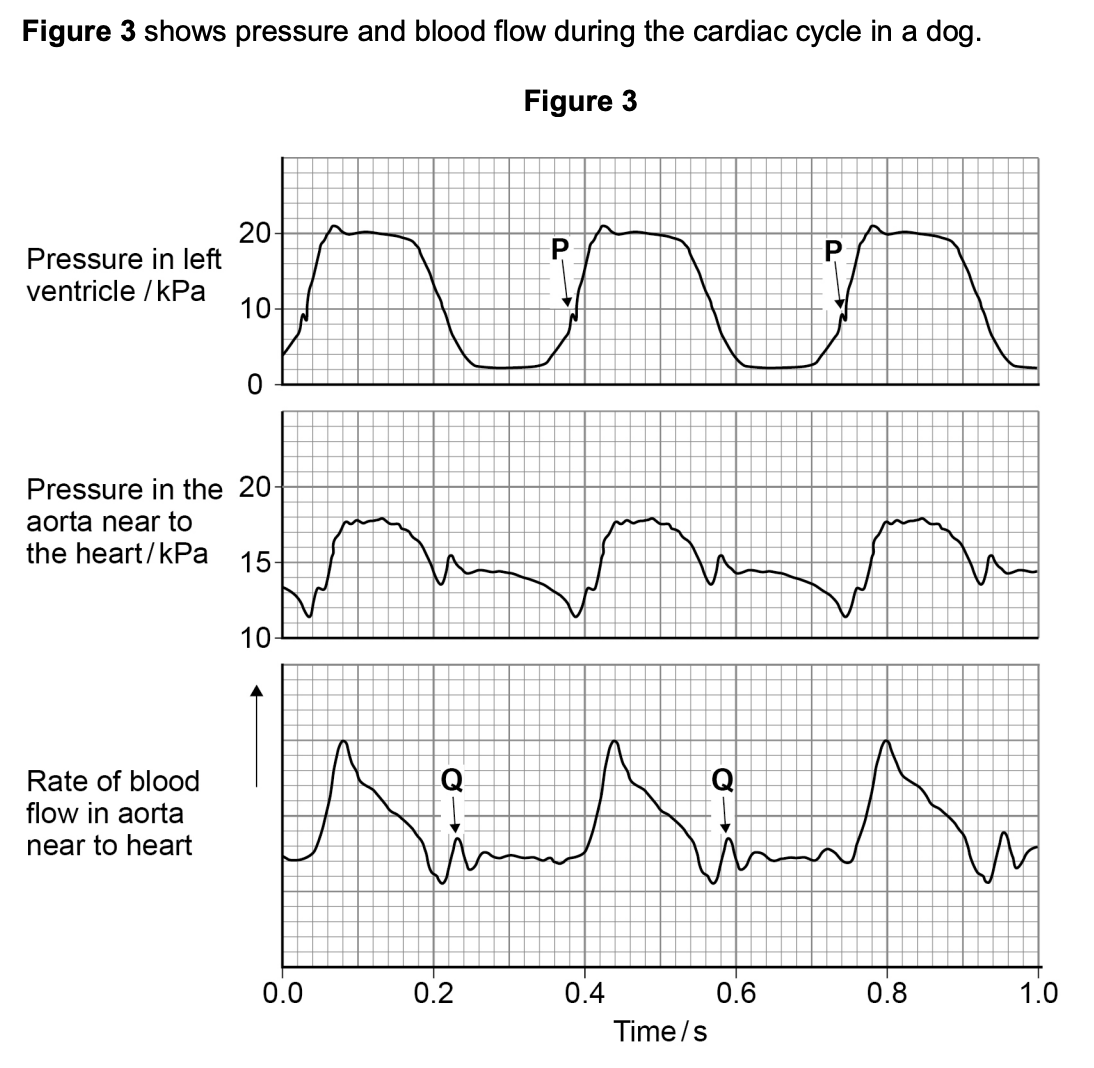
how do we calculate heart rate from a graph?
calculate length of each cardiac cycle (in this e.g. = 0.36)
divide 60 by length of cardiac cycle to find bpm (in this e.g. = 167)
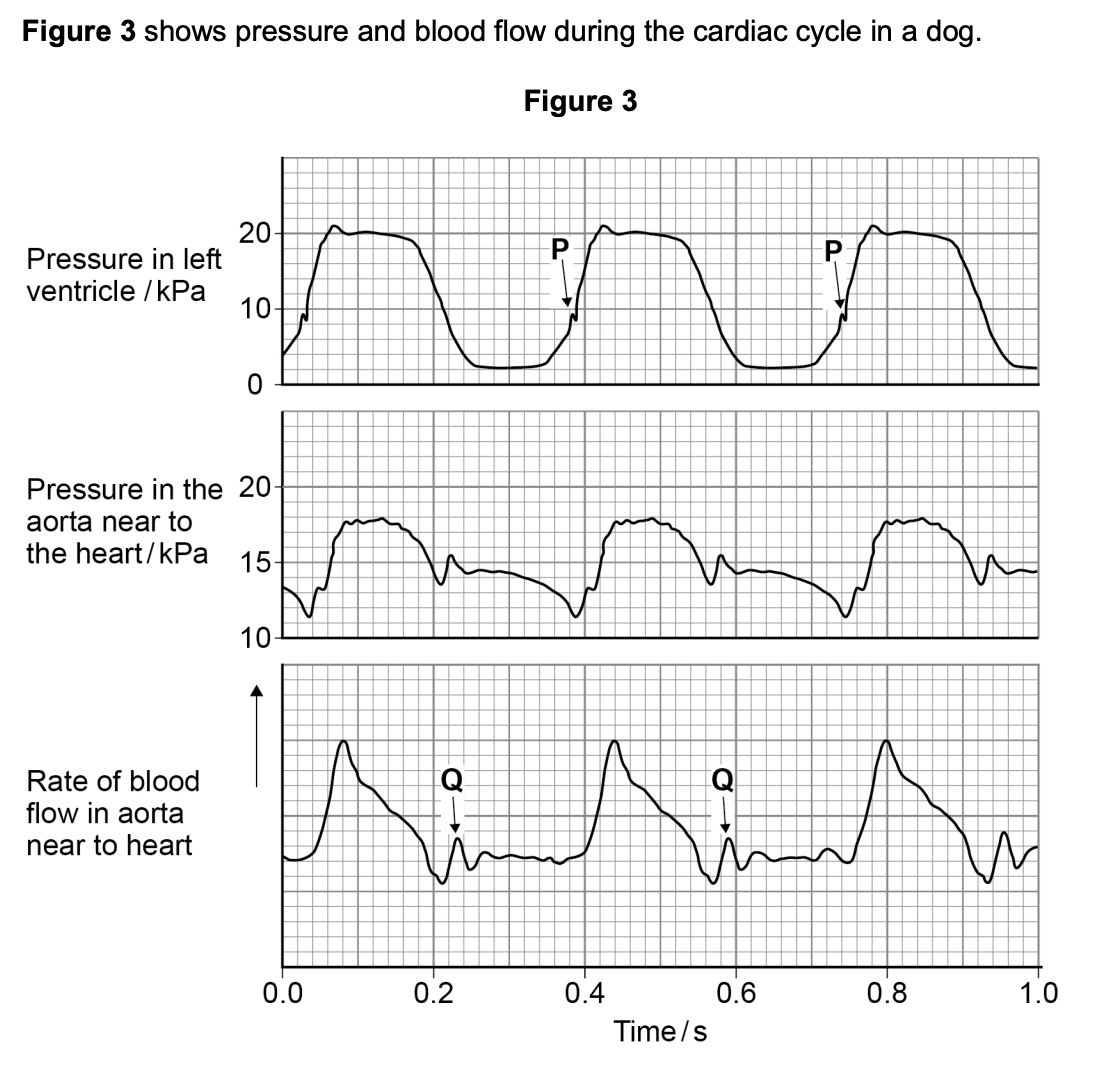
give the eqn for cardiac output:
cardiac output = stroke volume x heart rate
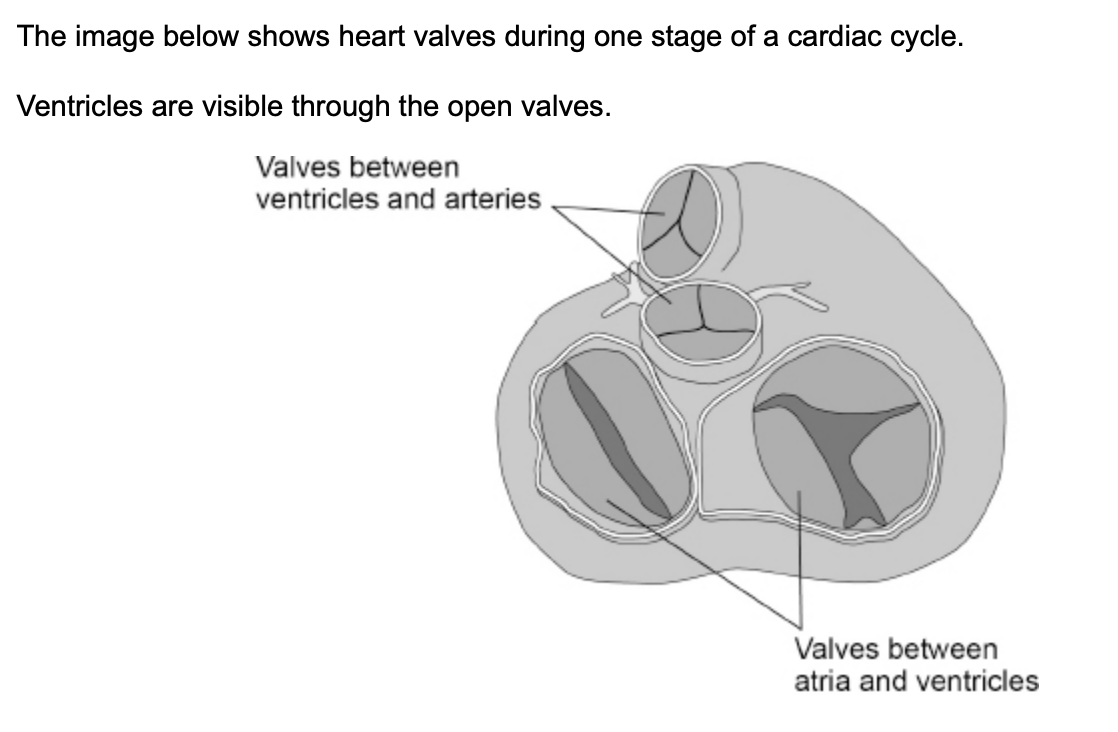
what can you conclude from the appearance of valves in the image above about heart muscle activity and movement between:
ventricles and arteries? (2)
atria and ventricles? (2)
ventricles and arteries:
ventricles relaxed
no backflow into ventricles
atria and ventricles:
atria contracted
blood movement from atria into ventricles

which blood vessel carries blood at the lowest pressure?
capillary
pulmonary vein
renal vein
vena cava
vena cava
what is haemoglobin?
globular protein found in RBCs
quaternary structure made of 4 polypeptide chains
each polypeptide has a haem group containing a Fe2+
what is loading/associating?
binding of Hb w/ O2
what is unloading/disassociating?
Hb releasing O2
draw the shape of the oxyhaemoglobin dissociation curve:
how is O2 loaded in terms of pressure?
loaded in regions w/ high partial pressure and unloaded in regions of low partial pressure
explain what happens at the first stage of the oxygen dissociation curve:
it is difficult for the first O2 molecule to bind
at low O2 concs, little O2 binds to Hb
so the gradient of the curve is shallow initially
explain the second stage of the oxygen dissociation curve:
binding of the first O2 changes the shape of Hb, making it easier for O2 to bind to the other subunits
the binding of the first O2 molecule allows more O2 to bind/greater saturation w/ O2/cooperative binding
so the gradient of the curve steepens
explain the last stage of the oxygen dissociation curve:
after binding of the third O2 molecule, the gradient of the curve decreases/flattens
it is harder to bind the fourth O2 molecule because most of the binding sites are occupied
so it is less likely that an O2 molecule will find an empty site to bind to
what is the Bohr effect?
affinity of Hb changing due to changes in CO2 conc
explain the Bohr effect in terms of the alveoli:
CO2 conc low/O2 conc high
so O2 affinity increases
O2 less readily unloaded by Hb
so dissociation curve shifts to the left
explain the Bohr effect in terms of respiring tissues:
CO2 conc high/O2 conc low
O2 affinity decreases
O2 readily unloaded/released by Hb
so dissociation curve shifts right
explain the release of O2 into respiring tissues in terms of pH:
in respiring tissues, CO2 is produced, which decreases the pH
lower pH changes the quaternary structure of Hb into one w/ a lower affinity for O2
so Hb releases its O2 more readily into the respiring tissues → more O2 for respiration
explain the loading of O2 from the alveoli in terms of pH:
in the alveoli, there is a low CO2 conc, which increases the pH
this higher pH changes the quaternary structure of Hb into one w a higher affinity for O2
Hb loads O2 from the alveoli more readily
describe and explain the Bohr effect for foetal Hb:
curve shifts to left - even at same PP, Hb has a higher affinity for O2
foetal Hb more saturated
as foetus cannot inhale/exhale
so requires higher affinity in order to load O2
describe and explain the Bohr effect for llama Hb (lives in high altitudes):
lives in high altitudes where PP of O2 is lower
so curve shifts left - llama Hb more saturated
so requires higher affinity in order to load O2
describe and explain the Bohr effect for earthworm Hb (lives in environment w/ depleted O2):
lives in environment w/ depleted O2 so PP of O2 is lower
so curve shifts left - earthworm Hb more saturated
so requires higher affinity in order to load O2
describe and explain the Bohr effect for dove Hb (has a faster metabolism):
faster metabolism so curve shifts right
Hb has a lower affinity for O2
offloads at same PP
ensures respiring tissue has an abundant supply of O2
why may some organisms have a dissociation curve which is to the right of ours?
very active so have a high O2 demand
so have Hb w/ a lower affinity for O2 than human Hb
why may some organisms have a dissociation curve which is to the left of ours?
live in areas w/ low O2 conc/very inactive
so have Hb w/ a higher affinity for O2 than human haemoglobin
explain a property of iron ions that enables these ions to carry out their role in RBCs
charged
so binds w/ oxygen
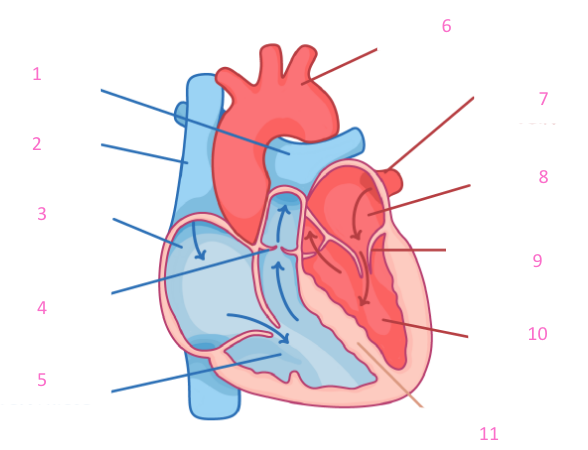
can you label this heart?
yes
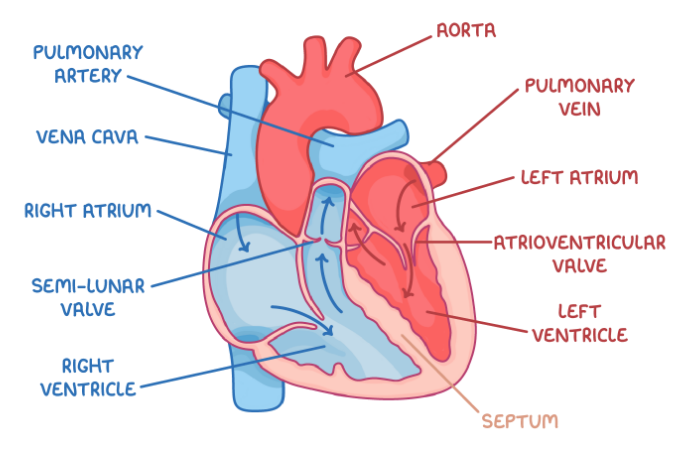
what is the significance of the double circulatory system?
blood pressure decreases in the lungs
single pump would slow blood flow to cells
2 pumps increase pressure before it circulates
prevents oxygenated and deoxygenated blood mixing
which part of the body does the term ‘pulmonary’ refer to?
lungs
which part of the body does ‘renal’ refer to?
kidneys
which part of the body does ‘hepatic’ refer to?
liver
give 3 features of the atria:
thin walled
elastic, stretch, recoil
do not need to contract as hard as ventricles
what is the thickness of the ventricle wall? why is this significant?
thicker muscular wall
contracts strongly to pump blood some distance (either lungs or rest of body)
bigger contraction = higher blood pressure
give 3 features of the cardiac muscle in general:
thick muscular walls
myogenic
never fatigues
what is the function of the left side of the heart?
pumps blood to the body
does the right hand side of the heart have a higher or lower blood pressure? why?
lower blood pressure:
to prevent damage to capillaries
slows down blood flow → allows time for gas exchange
does the left side of the heart have a higher or lower blood pressure? why?
higher blood pressure to ensure blood reaches all cells
what is the function of the right side of the heart?
pumps blood to the lungs
how do valves work?
open when pressure is higher behind the valve
close when pressure is higher in front of the valve
prevent backflow
what may cause an increase in pressure in the heart?
filling/contraction
give 2 safety precautions that should be followed when dissecting a heart (2)

give an overview of the heart dissection:
before cutting - identify coronary arteries. run water into top of heart to see valves close, squeeze to see valves open
cut down each side of heart - identify tendinous cords, examine thickness of walls, stick finger/needle through aorta/pulmonary arteries
give the ‘do’s of a biological drawing:
include a title
take proportions into account
use single, clear, joined lines
write labels horizontally
include magnification and scale (where relevant)
give the ‘don’t’s of a biological drawing:
shading
sketchy lines
arrowheads
hanging lines
aortic valves removed from donors were stored in isotonic containing an antibiotic before being used in valve replacement surgery - explain why the valves were stored in a solution containing an antibiotic (1)
kills bacteria that could cause infection/disease

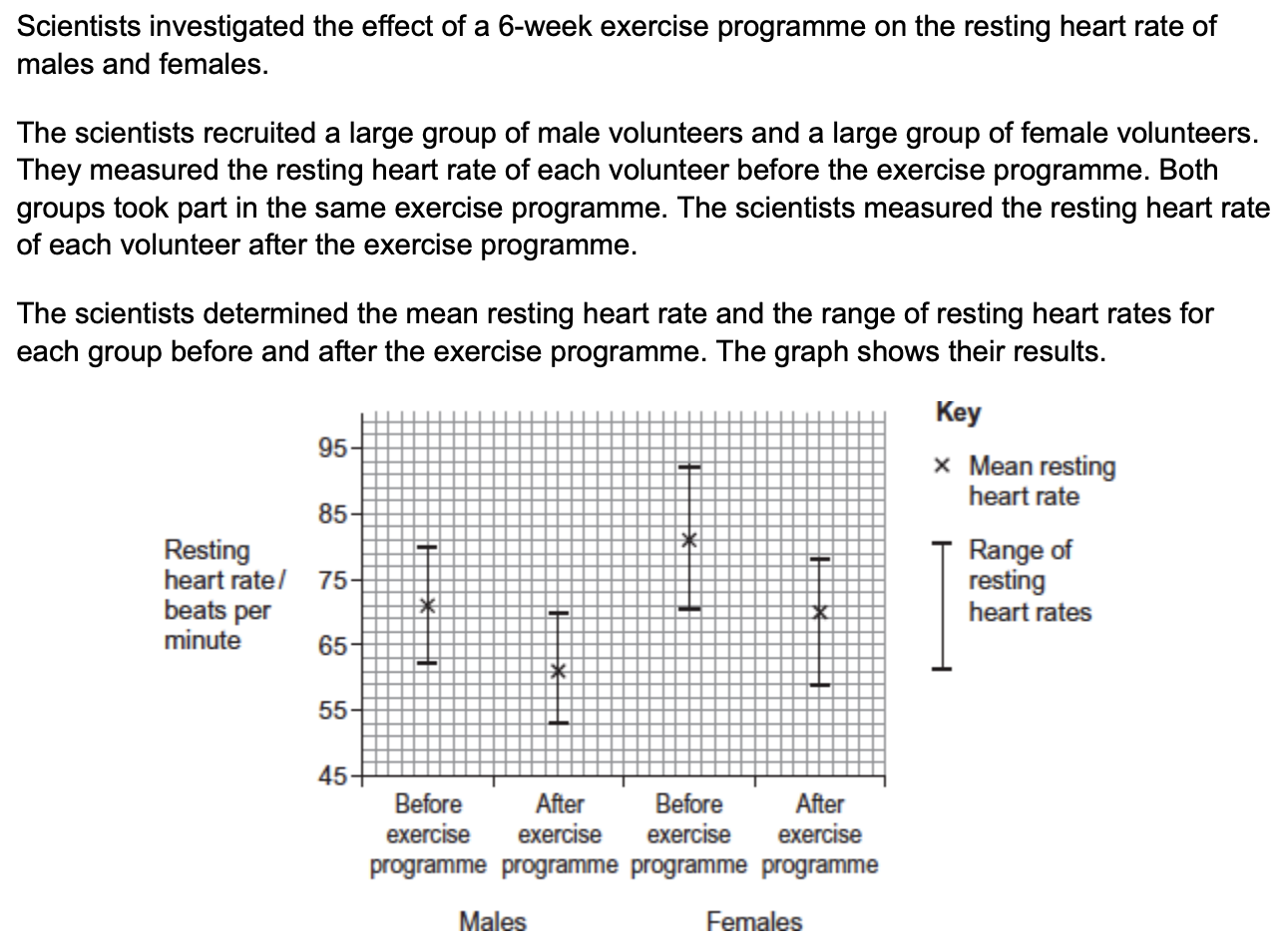
the scientists calculated the cardiac output of the volunteers before and after the exercise programme. in some volunteers, their cardiac output stayed the same, even though their resting heart rate decreased.
explain how their cardiac output could stay the same even when their resting heart rate had decreased (2)
cardiac output = stroke volume x heart rate
so stroke volume increases
what is tissue fluid? what does it contain?
fluid which passes out of the blood and bathes the tissue cells
contains mostly water, glucose, amino acids, fatty acids, ions and oxygen
(virtually same composition as blood plasma, just w/o proteins and cells)
describe the process of tissue fluid formation:
at the arterial end of the capillary, there is a high hydrostatic pressure due to contraction of the ventricles
there is a Ψ gradient into the capillaries (due to the hydrophilic plasma proteins exerting an oncotic pressure), but the hydrostatic pressure is greater and so overcomes this
ultrafiltration - water and dissolved substances, e.g. glucose forced out through the gaps (fenestrations) between the capillary endothelial cells, forming tissue fluid
proteins and RBCs are too large to pass through so remain in the capillaries
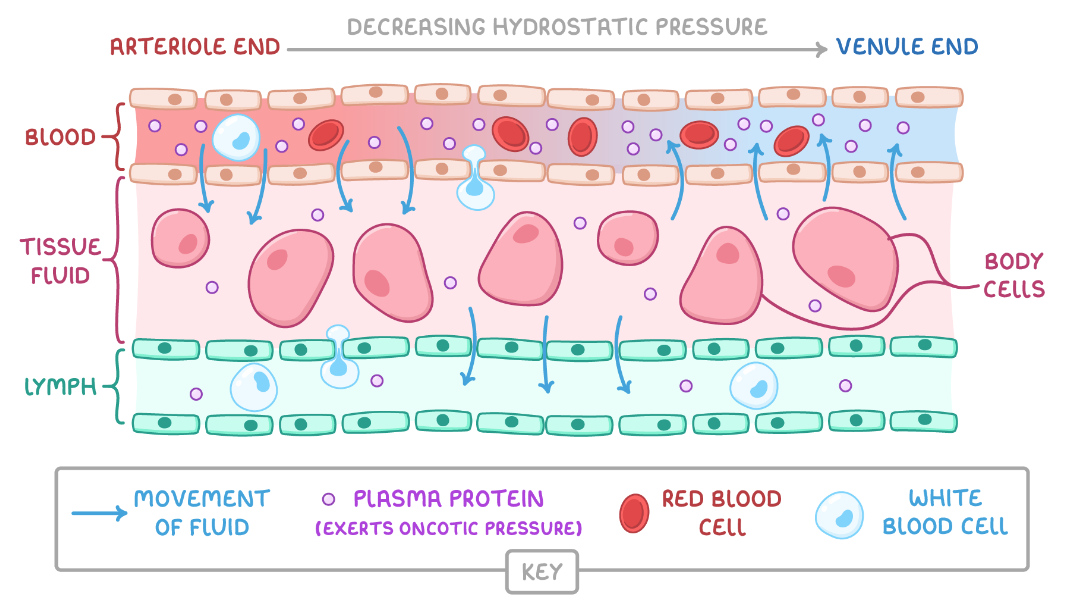
describe the process of tissue fluid reabsorption:
at the venule end of the capillary, the hydrostatic pressure is lower due to loss of water/fluid
Ψ in capillaries is lower than in the tissue fluid due to proteins remaining in the blood
water returns from tissue fluid to the venous end of the capillaries by osmosis down the Ψ gradient
the lymphatic system collects any XS tissue fluid which returns to the circulatory system
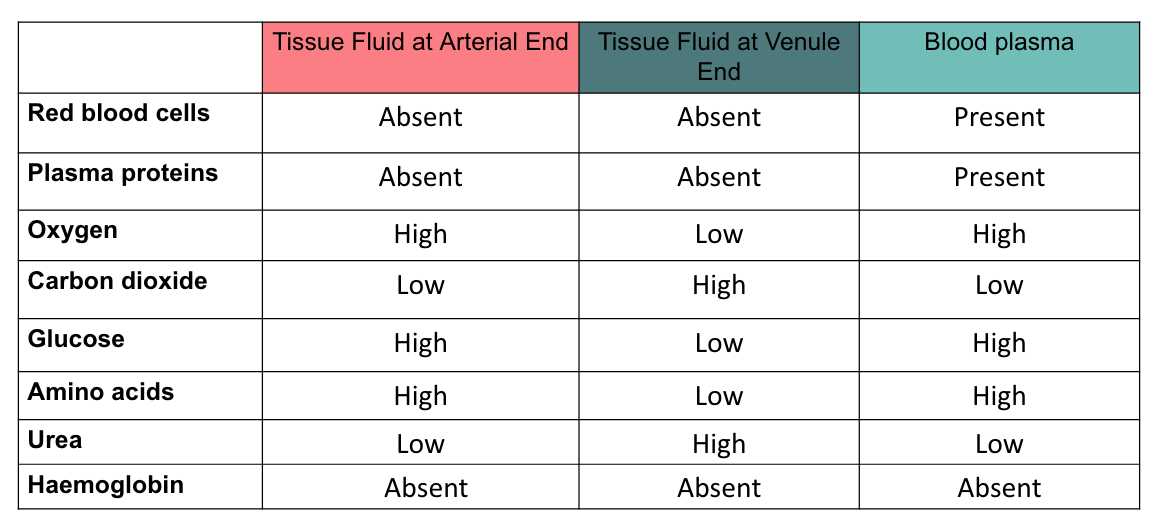
summarise the composition of tissue fluid surrounding the arterial and venule end of the capillaries and that of the blood plasma at the arterial end:
what is mass transport?
movement of fluids down a pressure gradient
(can occur over long distances)
what is the transpiration stream?
movement of water and dissolved ions up a plant
why is transpiration necessary for a plant?
provides water for photosynthesis (compromise between losing water and taking in CO2)
allows mineral ions to be transported from roots to leaves
evaporation has a cooling effect on leaves, preventing enzymes denaturing
what is transpiration?
process by which water is lost from the leaves by evaporation and diffusion