Micro-L14- Host Pathogen Interface
1/13
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
14 Terms
what is the host pathogen interface?
it is the dynamic cross talking between the pathogen and the host cells that determines infection outcome
this is where pathogens adhere and is the main battlefield where host immunity fights infection
what are the main innate defences against pathogens? PPACS
rapid, non specific mechanis
physical barriers- skin, mucosal membranes
pattern recognition receptors- TLRs, NLRs
secretion of AMPs, stomach acid, tears, saliva, mucus
cellular defenses- neutrophils, macrophages, DCs, NK
soluble mediations: cytokines chemokines, complement, IFN
what is the role of epidermal and epithelial barrier
skin: squamous and pathogens fall off
fibroblasts- EM and supports tissue structure
resident immune cells: DCs
cilia in airways: brush off pathogens away from
provides a physical removal and chemical defence to block infection
what is mucus and mucins and their defensive roles? chemical barriers and the 2 types of mucins
contain glycoproteins that line mucosal surfaces
provide a physical barrier: prevents pathogens from reaching epithelial cells
chemical barriers: neg charged and repels neg bacteria
tethered mucins: anchored to the epithelial surface: MUC1 in the gastrointestinal.
secreted mucins: MUC5AC- ciliated airways, MUC2 gastrointestinal. extracellular—>trap pathogens
produce AMPS
how do pathogens interact with mucins?
use mucins to attach to mucosal surface by binding to tethered or secreted mucin
some produce mucins to attach and then digest via mucinase to liberate nitrogen and carbon sources for bacterial growth
allows bacteria to penetrate mucus barrier
what are PRRs and their roles? list the types
TLR1/26- lipoporteins
TLR4- LPS- gram neg
TLR5- flagellin
TLR9- unmethylated CpG DNA
TLR11- flagellin
NOD1/2- detect peptidoglycan
inflammasome- pyroptosis
NFkB and make pro inflammatory cytokines IL-1/6/8/12, IFN-gamma
steps of phagocytosis? steps
chemotaxis: move toward pathogen
attachment: via PAMPs, TLRs interaction or opsonisation
ingestion of pathogen
phagolysosome formation- vesicle with lysosome
destrcution- superoxide, enzymes, H2O2, pH
expulsion or antigen presentation
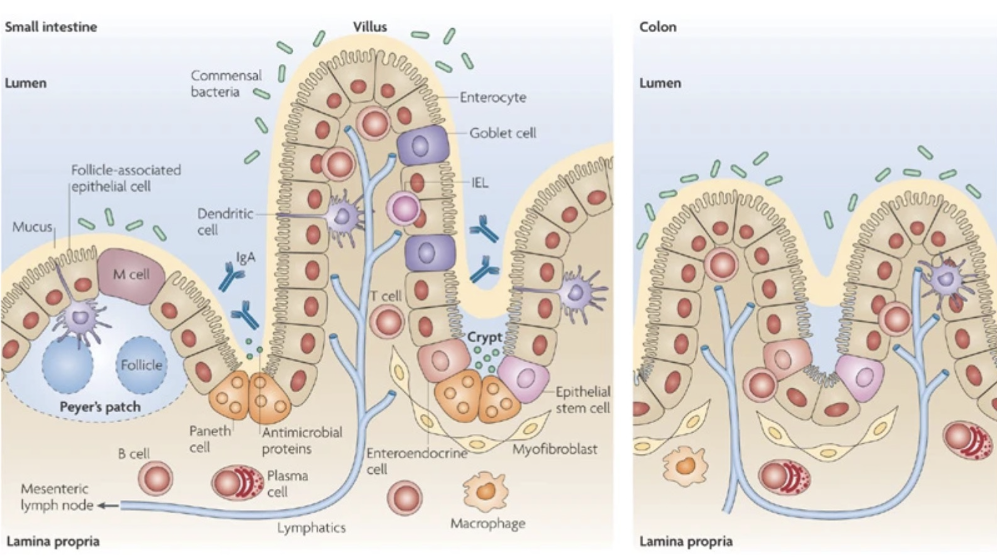
what is GALT and its components? PMLPGSM
gut associated lymphoid tissues
peyers patches: B cells that make IgA
M cells- transports microbes to Peyers patches
lamina propria- extracellular matrix under the epithelial
panted cells- secrete AMPs
Goblet cells- secrete mucus
stem cell progentiros- replenish the epithelium
mesenteric lymph nodes: drain microbes
what is programmed cellular heterogeneity? what is used to study this? why study this?
in a microbe population in a host- the cells can have different phenotypes: diff growth rates, metabolism and stress response
FISH- bacteria embedded in agora's and fixed with probes to identify mRNA in individual cells. can look at many traits and sequences
in cystic fibrosis- some cells exhibit high oxidative stress and others cluster- drug treatment may kill some cells while others survive. need to keep this in mind to combat ALL microbes!! due to programmed cellular hetergenity→some will survive
how do microbes know they are in a cell?
temperature change
pH change
nutrient availability
they can also detect surface metabolites and change gene expression to change behaviour accordingly
key features of streptococcus pneumoniae? morphology, disease, virulence factors, route of infection, clinical signs, treatment
morphology: gram pos, forms chains
diseases: pneumonia, sepsis, meningtiitis
virulence factors: capsule and pneuomolysin
route of infection: inhalation and colonises nose and lungs
clinical signs: lobar pneumonia, alveoli filled with fluid
treatment: amoxicillin
discuss the pneumoniae capsule? what it does to decrease immune response. also how is it synthesised? WGWWW
protects against antibiotics, phagocystsos
decrease IL-8, TNF, IL-6
protects against complement
synthesised:
o WchA initial transferase: links first sugar as a sugar phosphate Glc-P to membrane lipid carrier
o Glycosyl transferase: links further sugarsmake repeat units
o Wzx flippase: transports this across cytoplasmic membrane
o Wzy polymerase: links these units to make a lipid linked unit- to make a capsule polysaccharide
o Wzd translocates the capsular polysaccharide this to the peptidoglycan
specialised defenses to the respiratory tract? CGBCB
Ciliated cells- beat at 15 beats per sec
Goblet cells- mucus MUC5AC- mostly water- 1.5L per day
Basal STEM cells
Club cells- make AMPs- lysozyme, glycosaminoglycans and can act as stem cells
Brush cells- sensory roll and modulate mucociliary—> more ciliated activity and modulate immune response. first line defense of pathogens
dcesribe the Griffith experiment
- Rough vs smooth strains. S has a capsule and is virulent, R has no capsule and non virulent
- When rough R is incoluated with killed Smice died
- Live R transformed into Sgot a capsule
- Natural transformation