NSG 3105: Musculoskeletal Issues
1/87
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
88 Terms
Osteomyelitis
Infection of bone, surrounding soft tissue, and bone marrow
Staphylococcus aureus
What bacteria is the most common cause of osteomyelitis?
Vascular issues related diabetes/renal dysfunction
What condition can make an adult more susceptible to indirectly infected osteomyelitis?
Direct invasion
Bacteria enter the bone via an open wound; knee/hip replacements allow for easier entry
False (a lot of room for contamination when collecting the specimen)
True or false? A bone culture is the gold standard of diagnosing osteomyelitis, therefore no other tests need to be performed once it has been completed.
1 multiple choice option
Broad spectrum antibiotic, then narrow spectrum once cultures are back
What does the treatment plan for osteomyelitis look like?
Insertion of a PICC line (for long-term use of antibiotics)
What might the nurse anticipate in the care plan of a patient who has just been diagnosed with osteomyelitis?
Curative approaches to osteomyelitis
Surgical debridement, negative pressure dressing, bone grafts
Palliative approaches to osteomyelitis
Long term antibiotic use, hyperbaric O2 therapy (stimulates healing), taking out part of bone/amputation
Pain control, gentle immobilization, bed rest, monitoring for other infections, antibiotic teaching
Nursing interventions for osteomyelitis
False (other way around!)
True or false? Osteoporosis is a non-inflammatory degenerative disease, while osteoarthritis is a metabolic disorder
1 multiple choice option
Osteoporosis
Metabolic bone disease in which creation of new bone (osteoblasts) does not keep up with the removal of old bone (osteoclasts)
Primary osteoporosis
Occurs in women after menopause and in men later in life; NOT merely a consequence of aging, but failure to develop optimal peak bone mass during childhood, adolescence, and young adulthood
Secondary osteoporosis
Result of medications or other conditions and diseases that affect bone metabolism
Less calcium intake, smaller frames, and bone reabsorption begins at a younger age
Why are women at a higher risk of developing osteoporosis?
Modifiable risk factors for osteoporosis
Getting active (weight bearing activities, walking), limiting alcohol intake and cigarette exposure; increase Ca+ and vitamin D intake
Loss of height, back pain, kyphosis, bone fractures
What are some symptoms of advnaced osteoporosis?
DEXA scan (Dual-energy x-ray absorptiometry)
Diagnostic test that measures bone density; evaluates changes in bone density over time (people get tested annually)
Alkaline phosphatase
Enzyme produced by osteoblasts that increases local concentrations of inorganic phosphate, facilitating the calcification process while reducing pyrophosphate, an inhibitor of mineral formation
True (Alk-phos might be elevated after a fracture because osteoblasts are highly active in repairing the damaged bone)
True or false? When looking at a CBC of a patient with osteoporosis, calcium and phosphorus will be at normal levels and alk-phos (alkaline phosphatase) levels might be elevated after a fracture
1 multiple choice option
Prevent bone loss and fragility fractures
What is the goal of care for a patient with osteoporosis?
Hormonal replacement therapy
Pharmaceutical therapy option for a patient with osteoporosis; replenishes estrogen, slowing bone loss and maintaining bone density; benefits must be weighed against risks
Calcitonin
Pharmaceutical therapy option for a patient with osteoporosis; IM or intranasal; inhibits osteoclastic bone resorption by directly interacting with active osteoclasts (AKA keeps calcium in bones & out of blood stream)
Calcium supplementation
What is important to implement in a patient's care plan if they are taking calcitonin? (hint: it will prevent secondary hyperparathyroidism)
Bisphosphonates
Pharmaceutical therapy option for a patient with osteoporosis; inhibit osteoclast-mediated bone resorption; ex. Etidronate, alendronate, risedronate
Drink with 8oz water and remain upright for minimum 30 min
What is an important teaching point to give patients taking bisphosphonates?
Osteoarthritis
Slowly progressing disorder of synovial joints; degenerative in origin, NOT inflammatory - cartilage destruction and inadequate repair
Commonly affected joints in OA
Hands, hips, knees, vertebral areas
Heberden's nodes
Swelling of distal interphalangeal finger joints, characteristic of osteoarthritis
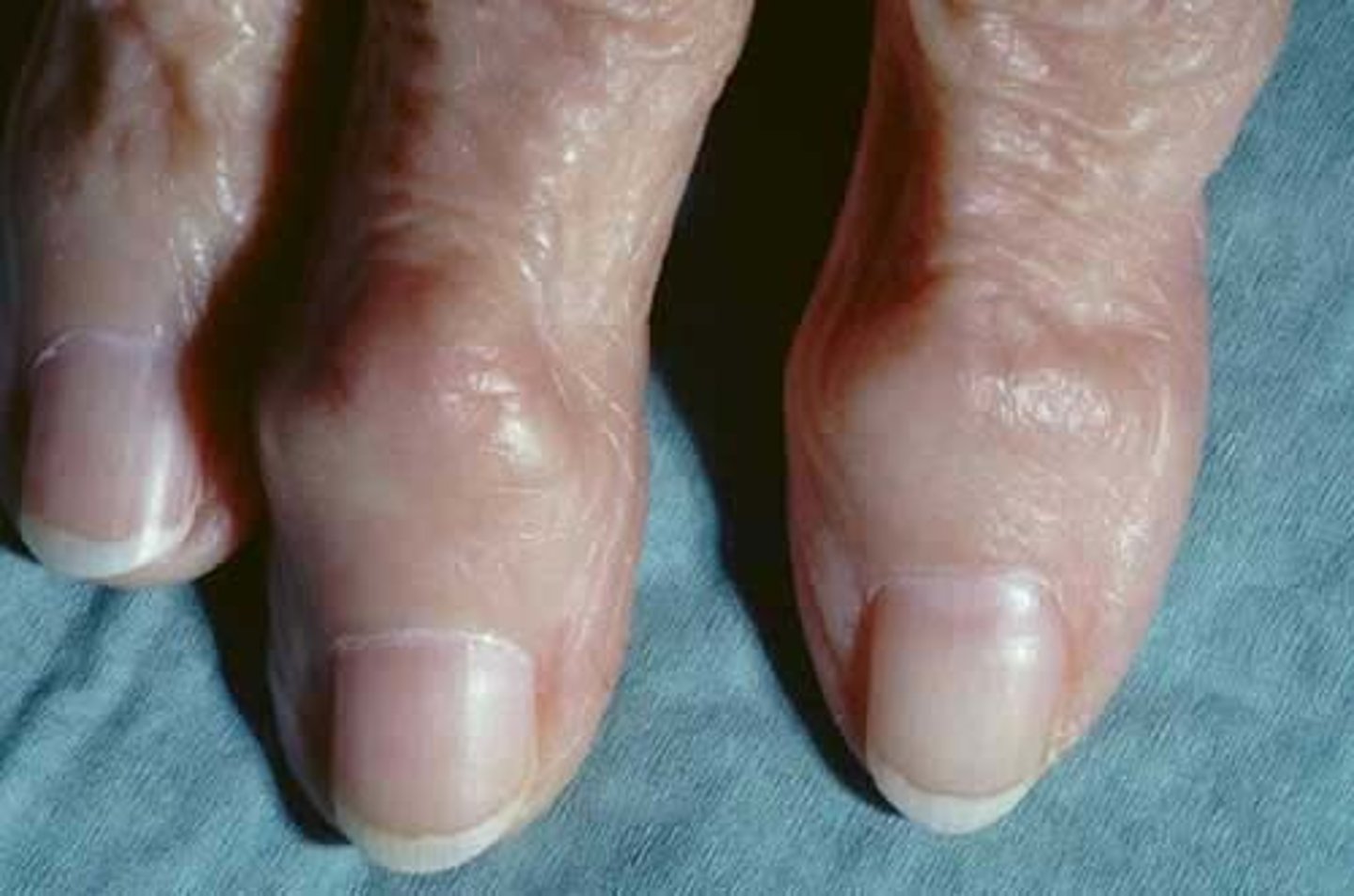
Age (higher risk after 50), sex (women), weight (higher BMI), genetics
What are the 4 risk factors for OA?
Physical exam, x-ray, MRI, CT, joint fluid analysis
Diagnostic tests used for OA
Erythrocyte sedimentation rate
Measures time it takes for erythrocytes to settle to the bottom of a test tube; elevated when synovium is inflamed
Heat, weigh reduction, joint rest, orthotic devices, pharmacological therapy
OA management
Rheumatoid arthritis
Chronic systemic autoimmune disorder characterized by inflammation of connective tissue in synovial joints
Antigen triggers the formation of abnormal IgG → antibodies form against this IgG, aka rheumatoid factor → affects joints causing an inflammatory response → neutrophils go to inflamed area which cause synovial lining to thicken
Etiology of RA
Obesity, immune system issues, smoking, age, genetics
Ulnar drift
Clinical manifestation of rheumatoid arthritis; ulnar deviation of the fingers at the metacarpophalangeal joints
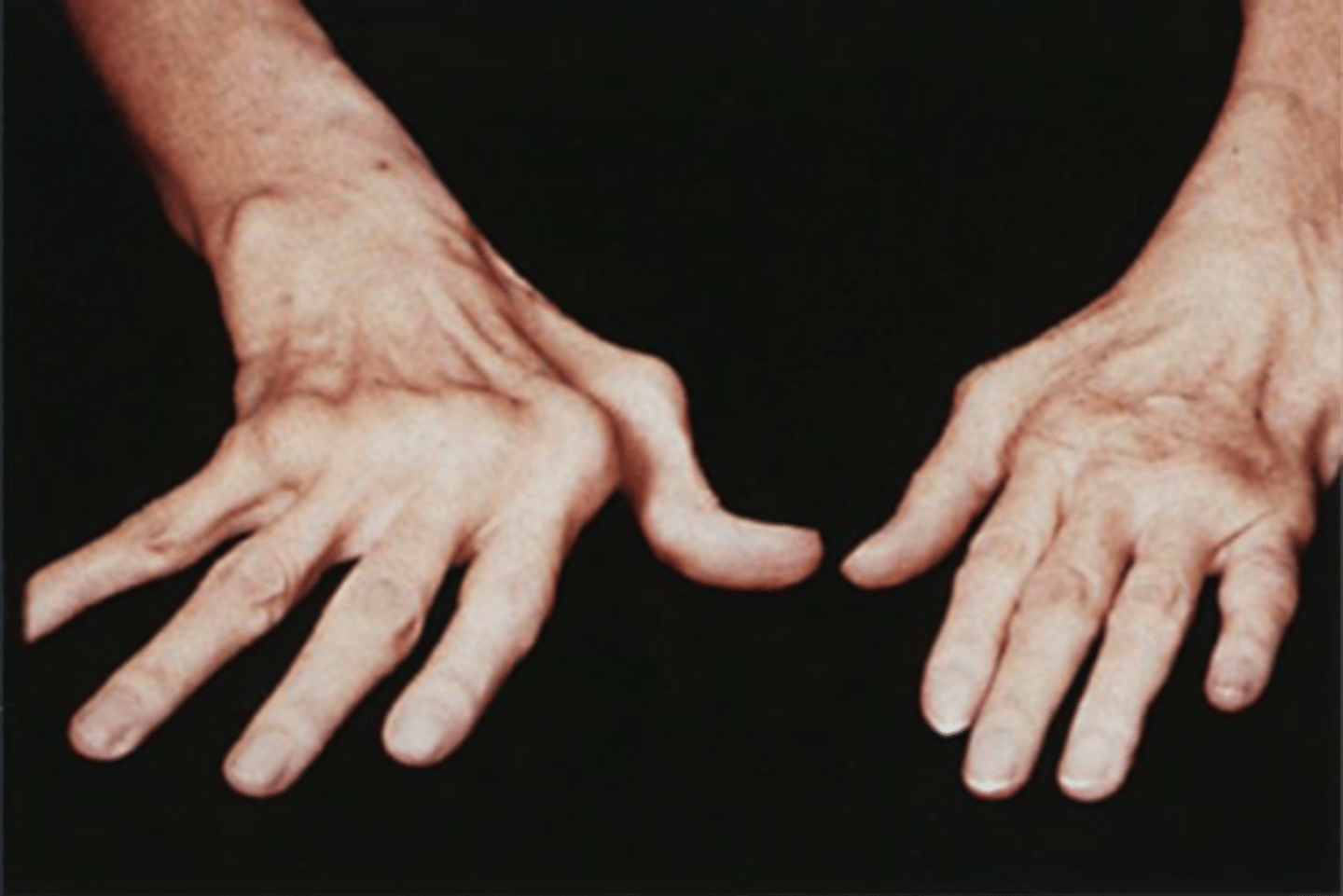
Boutonniere deformity
Flexion of proximal interphalangeal joint and hyperextension of distal interphalangeal joint

Hallux vagus (bunion)
Abnormal enlargement of the joint at the base of the great toe
Swan neck deformity
Hyperextension of proximal interphalangeal joint and flexion of distal interphalangeal joint
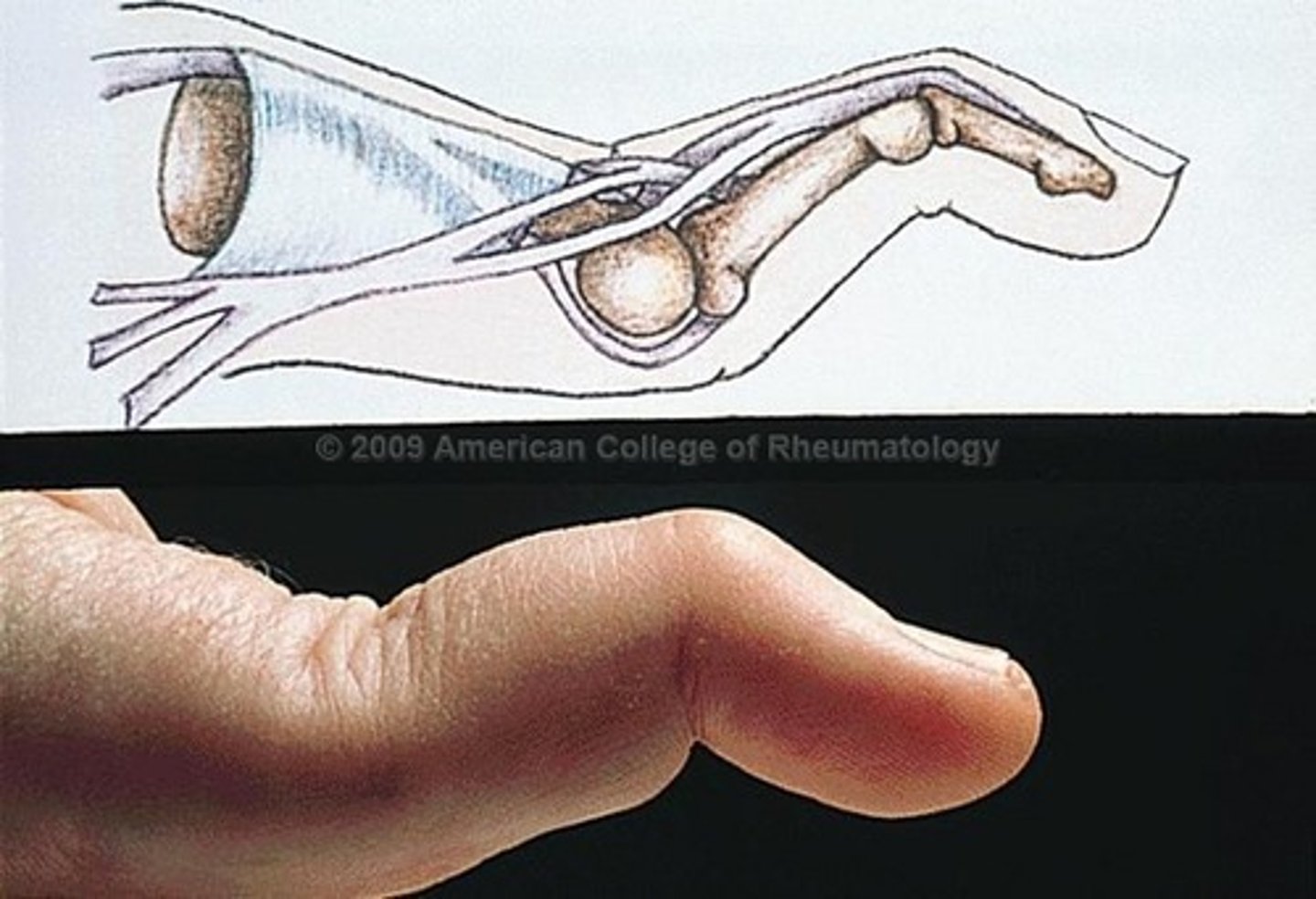
Rheumatoid nodules
Firm, nontender, unattached subcutaneous nodules at pressure points (e.g., elbow, back of forearm) associated with rheumatoid arthritis; develop in 20% of patients with RA
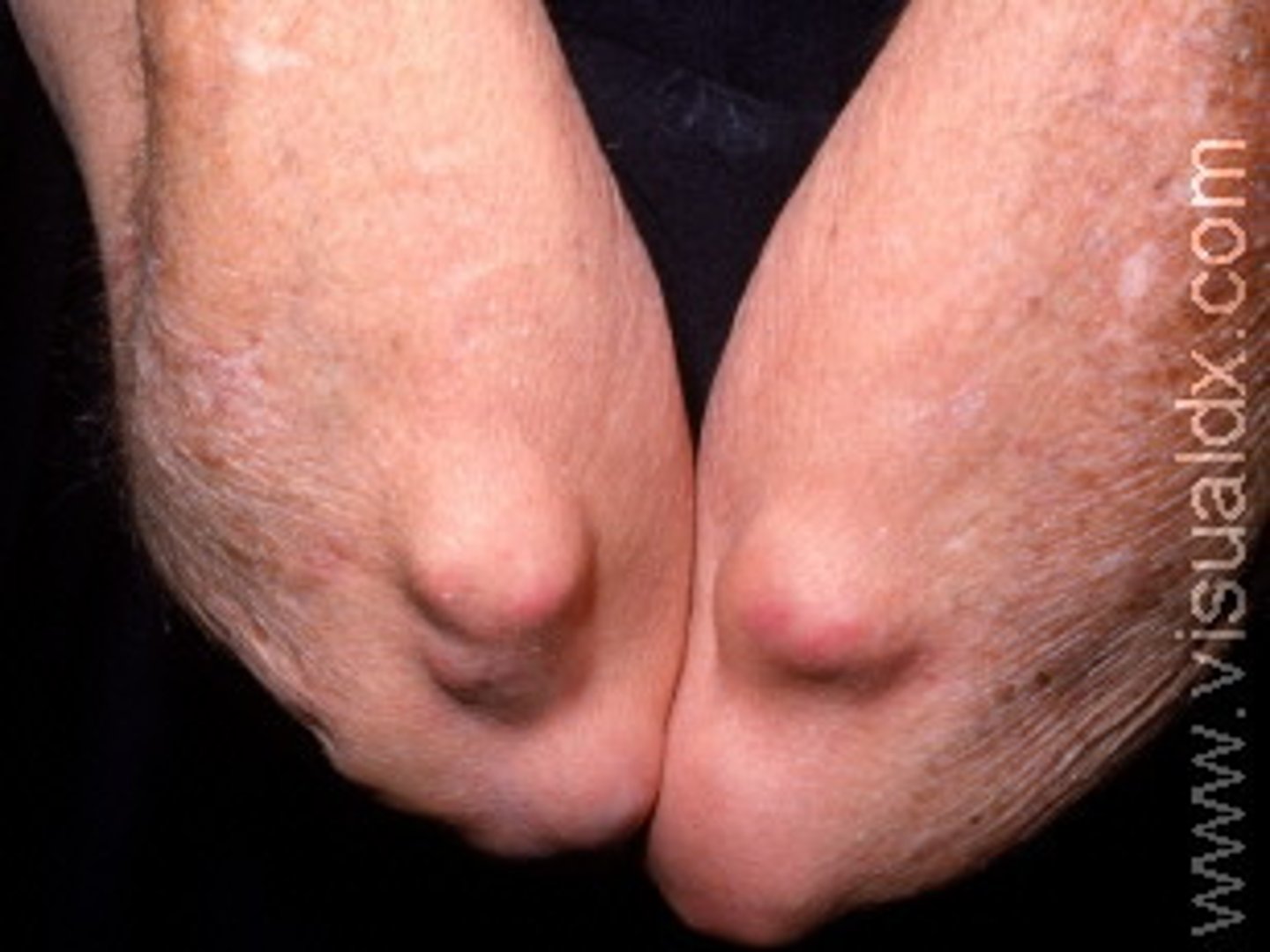
Sjogren syndrome
Extra-articular manifestation of RA characterized by degeneration of the salivary and lacrimal glands causing dryness of the mouth and eyes and other mucous membranes
Felty syndrome
Seen in pts with severe, long standing > 10 years RA characterized by neutropenia and splenomegaly; can have a hard time with flexion and contraction
Nursing goals of RA
Acceptable pain management, minimal loss of function, maintain positive self-image, perform self care
Methotrexate
Disease modifying antirheumatic medication; works in days to weeks, less toxicity but suppresses bone marrow so frequent lab monitoring for liver toxicity
Sulphasalazine
Disease modifying antirheumatic medication; antimalarial drug for mild to moderate disease; rapidly absorbed, synthetic and well tolerated
Leflunomide
Disease modifying antirheumatic medication; contraindicated with pregnancy
Tofacitinib
JAK inhibitor; interferes with JAK enzymes that contribute to joint inflammation
Sprain
Injury related to ligaments around a joint caused by a twisting or wrenching motion; classified by degree of tearing in ligaments
1st degree sprain
Tears in only a few fibers, mild tenderness, minimal swelling
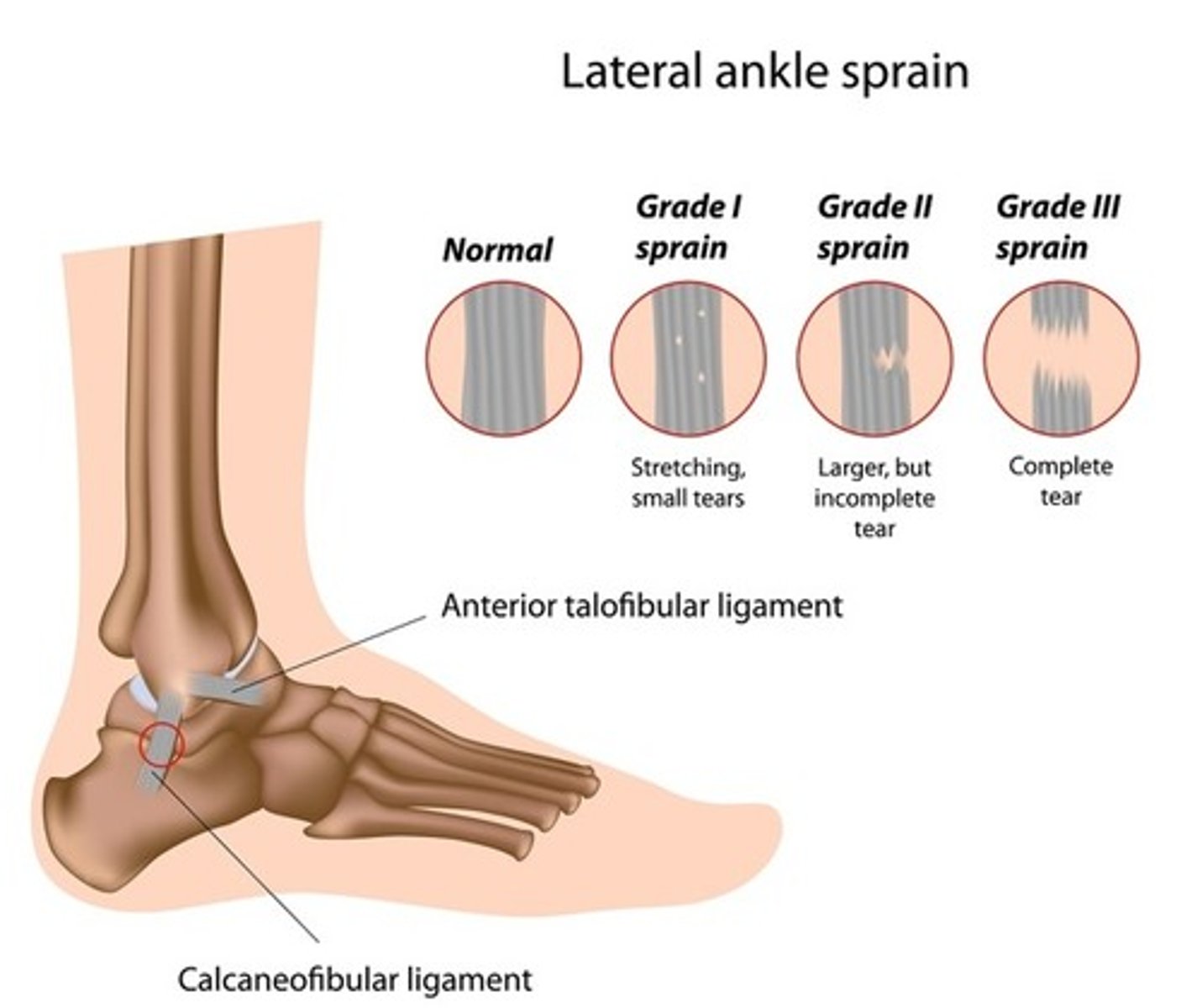
2nd degree sprain
Partial tearing of ligament with swelling and tenderness
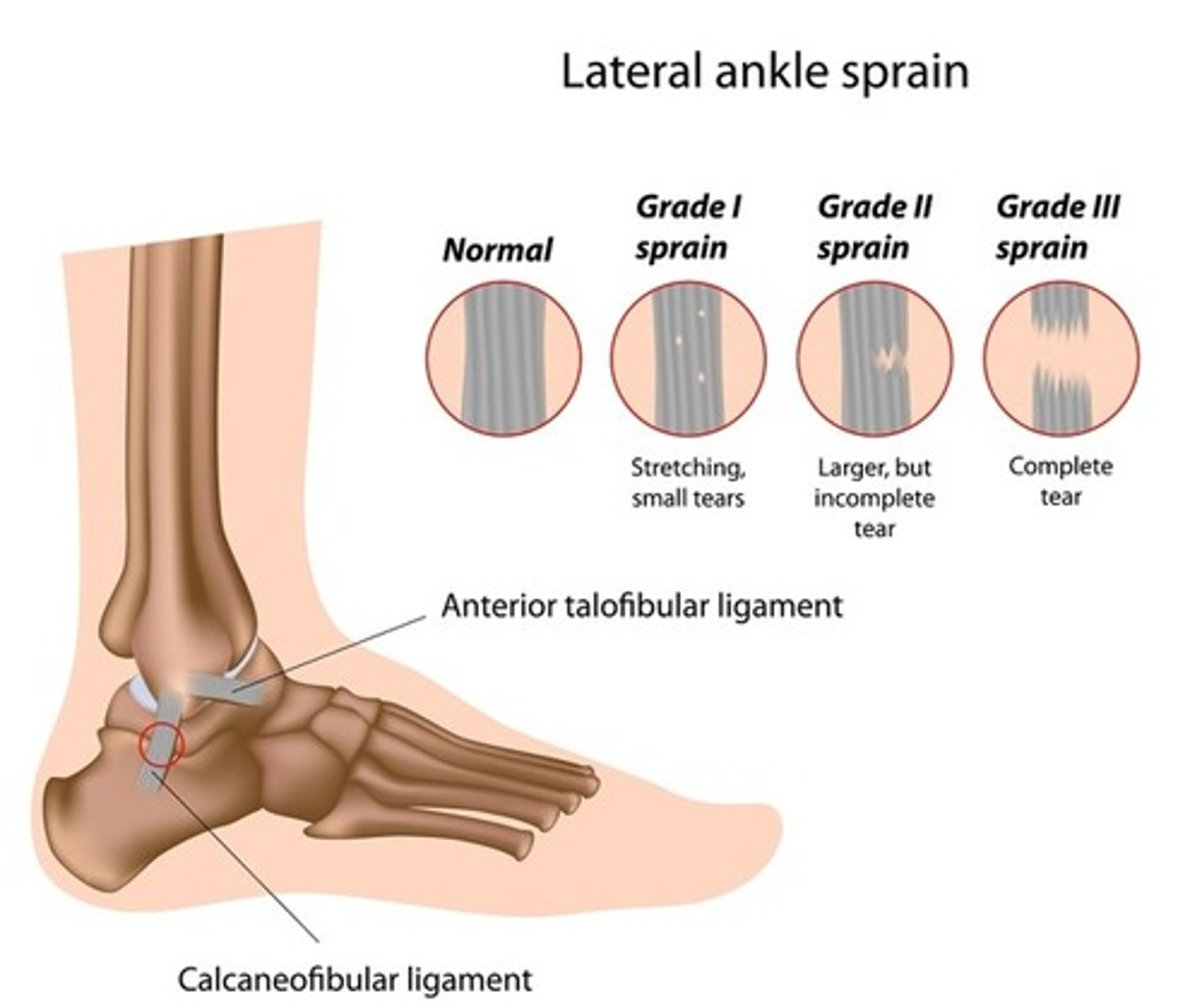
3rd degree sprain
Complete tearing of ligament in association with swelling; gap may be present between tear
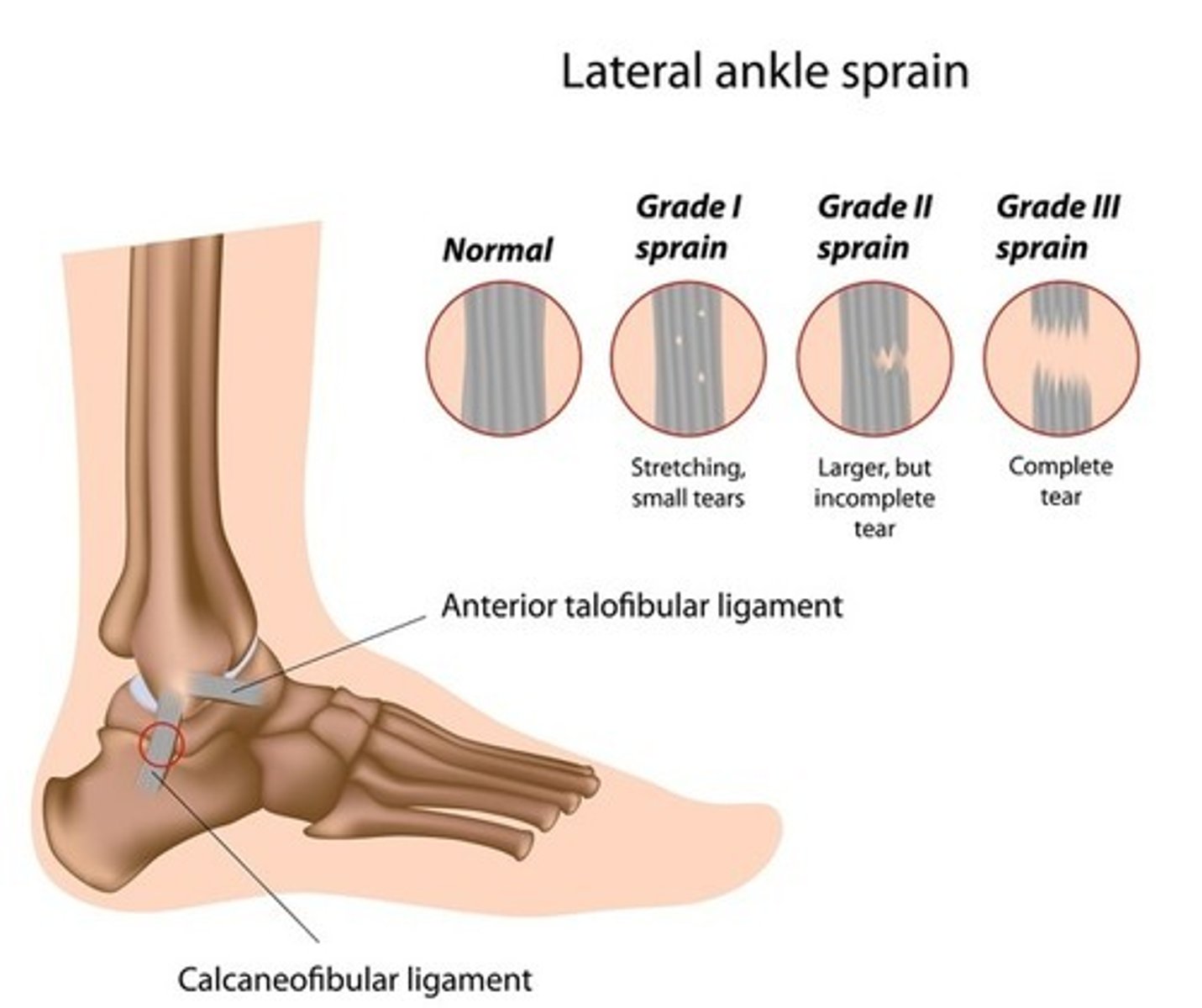
Strain
Excessive stretching of a muscle or tendon; mostly occur in hamstring, foot, or back; pain, swelling, bruising, decreased ROM, pain aggravated by continue use
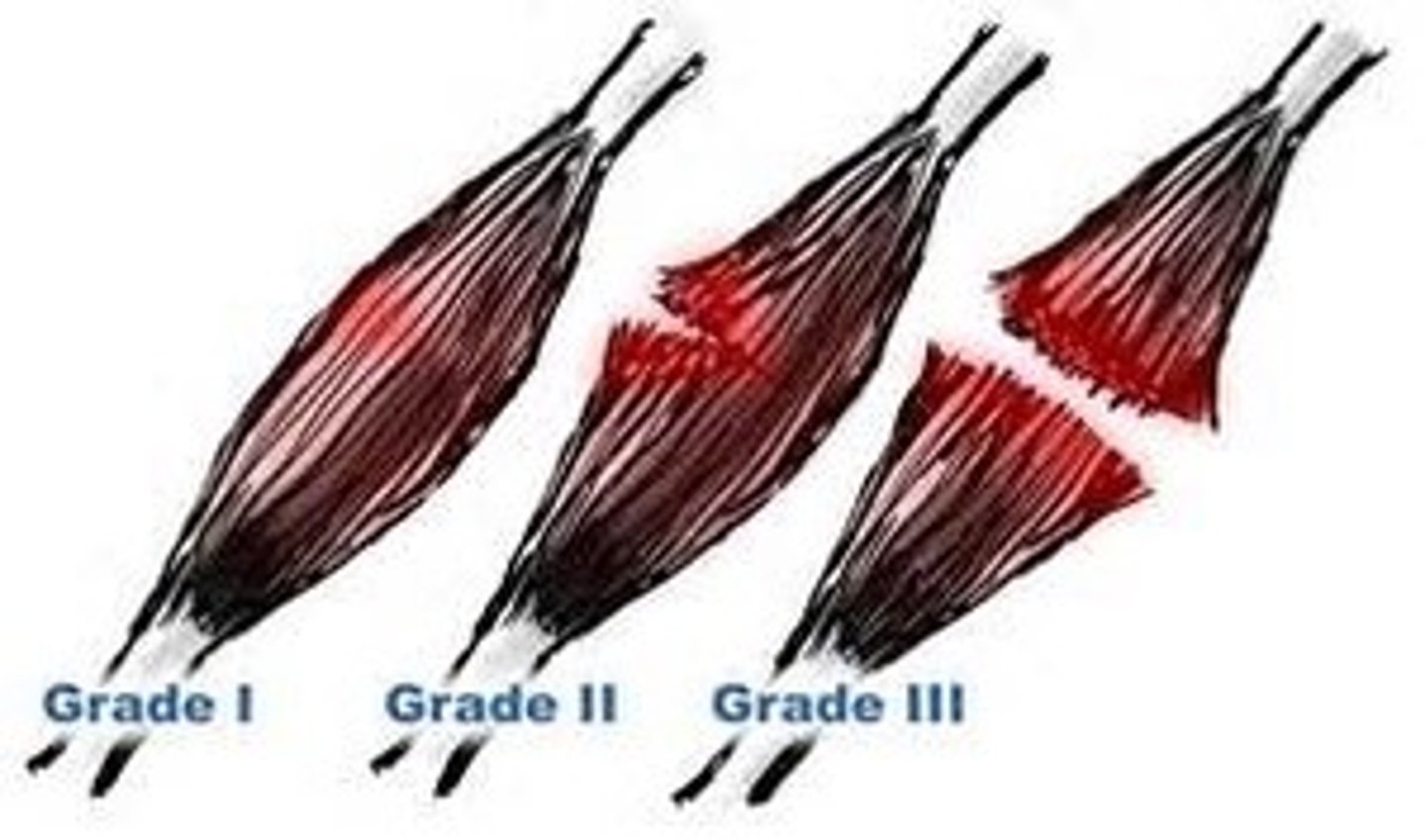
1st degree strain
Partial tear with strong but painful muscle activity
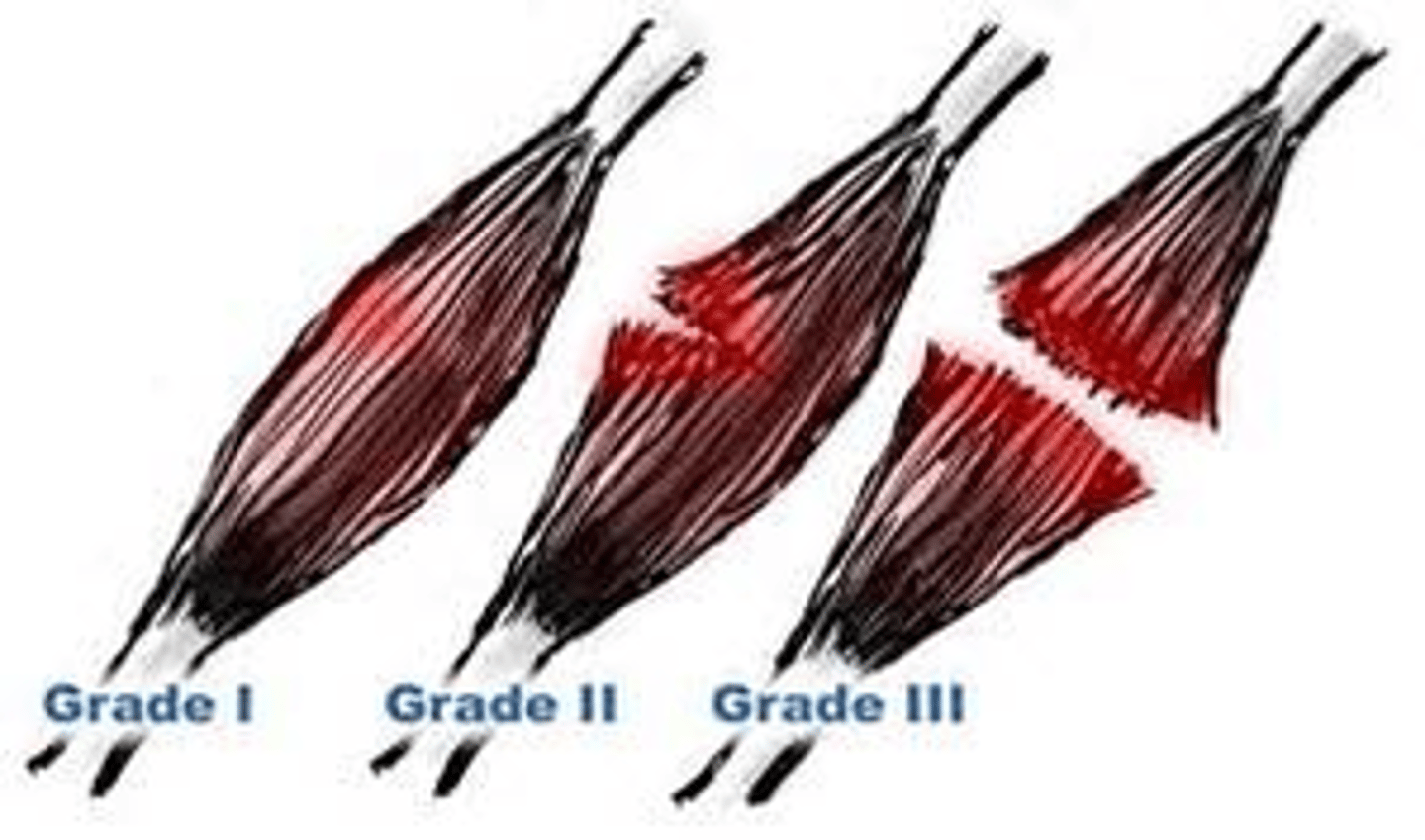
2nd degree strain
Moderately torn muscle
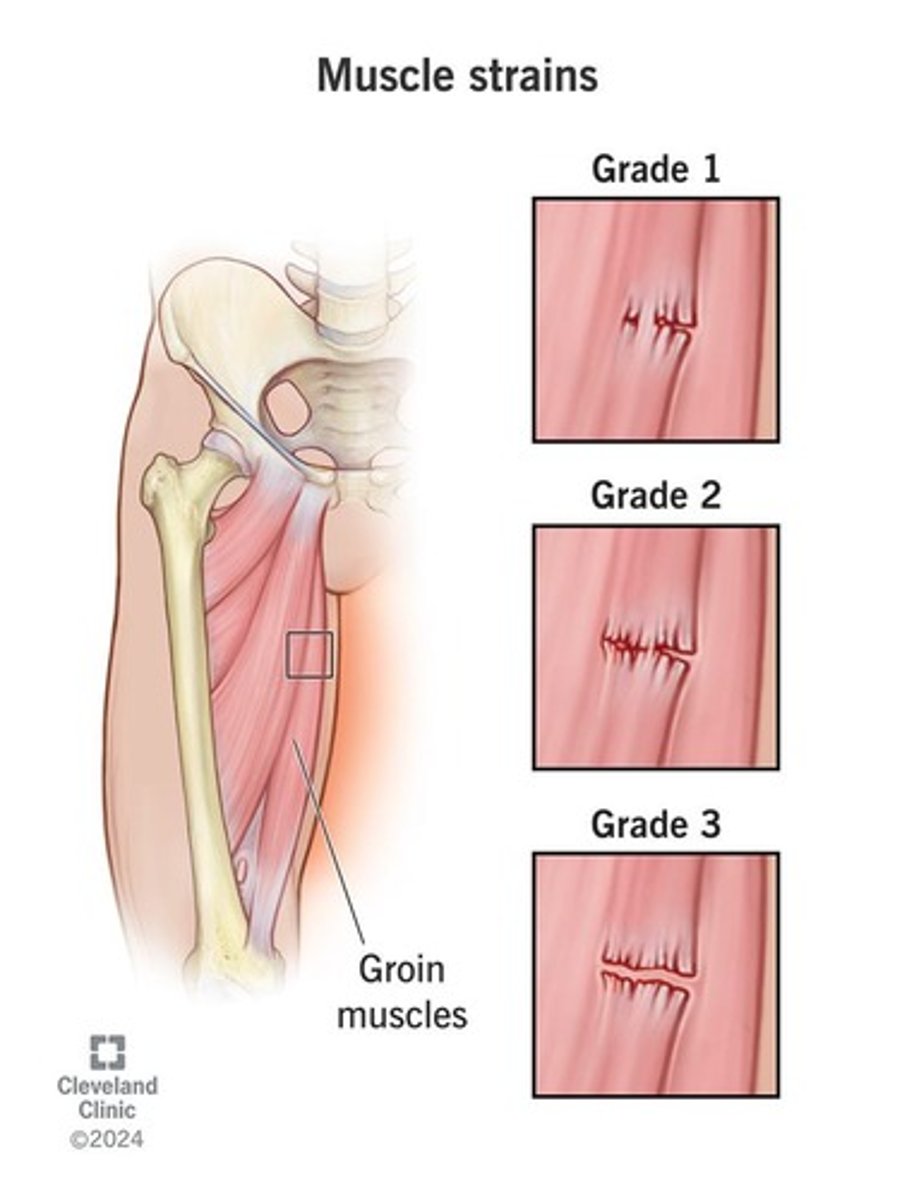
3rd degree strain
Severely torn or even rupture muscle
Avulsion fracture
Tendon forcibly extracts a piece off of the bone; complication of a 2nd or 3rd degree strain
Fracture
Discontinuity of bone, primary or secondary to a disease process (like cancer or osteoporosis); mechanism of injury can dictate how the patient might present
Open fracture
Fracture comes through the skin, very dangerous because it can also introduce infection into that area
Closed fracture
The break happens but no skin is broken
Transverse fracture
Complete fracture that is straight across the bone at right angles to the long axis of the bone
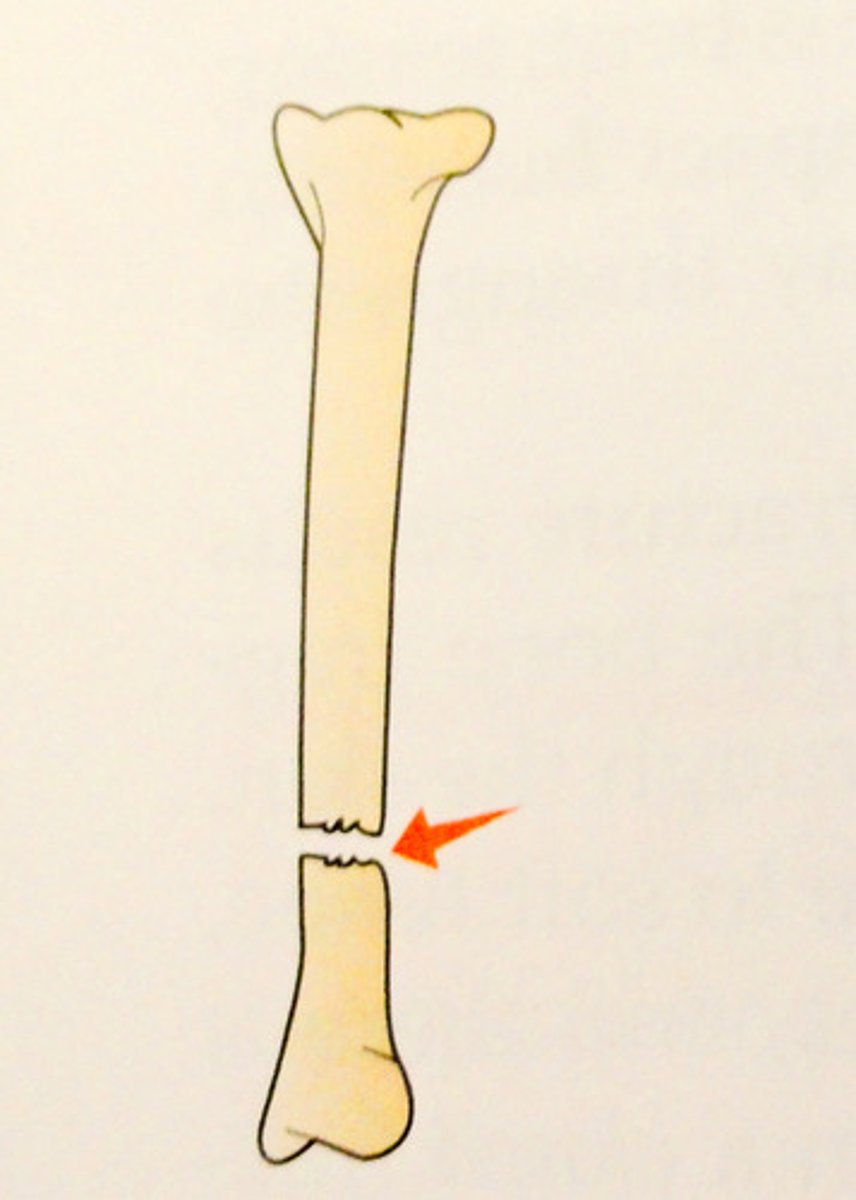
Stress fracture
Small crack in the bone that often develops from chronic, excessive impact such as running
Oblique fracture
Bone break in which fracture line runs along an angle to shaft of the bone
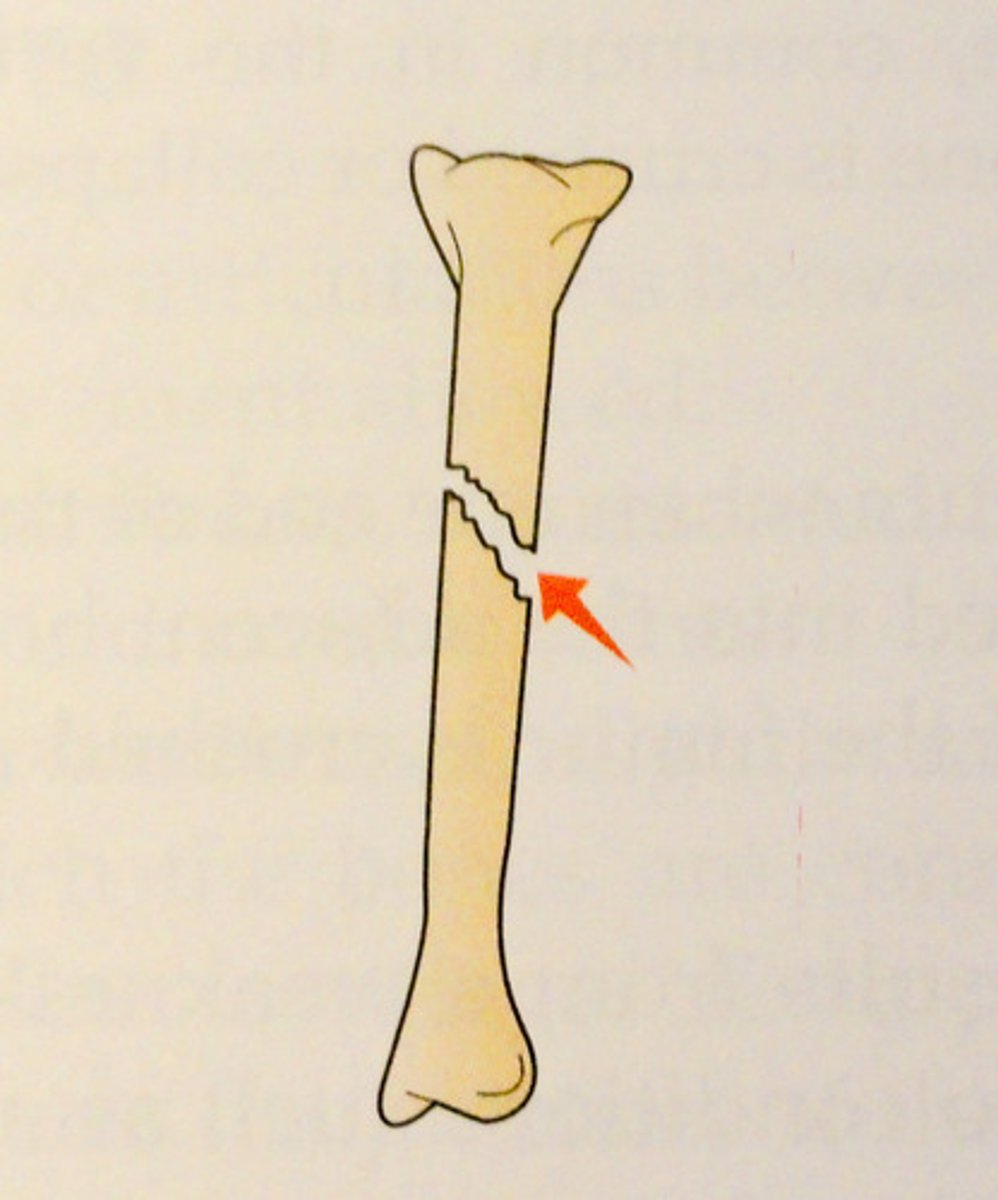
Greenstick fracture
Bending and incomplete break of a bone; most often seen in children
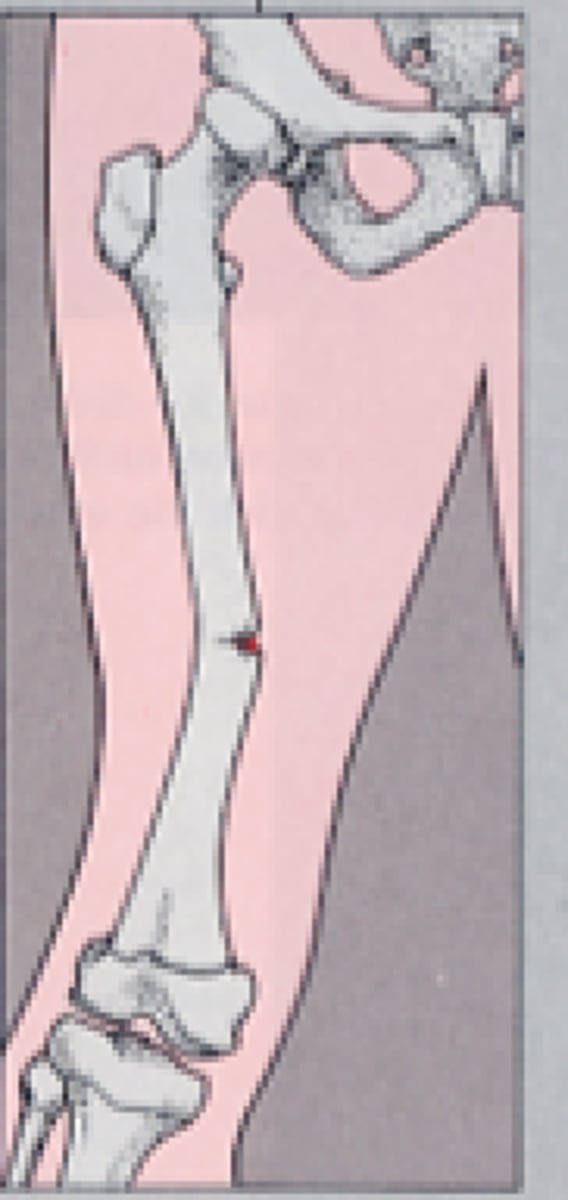
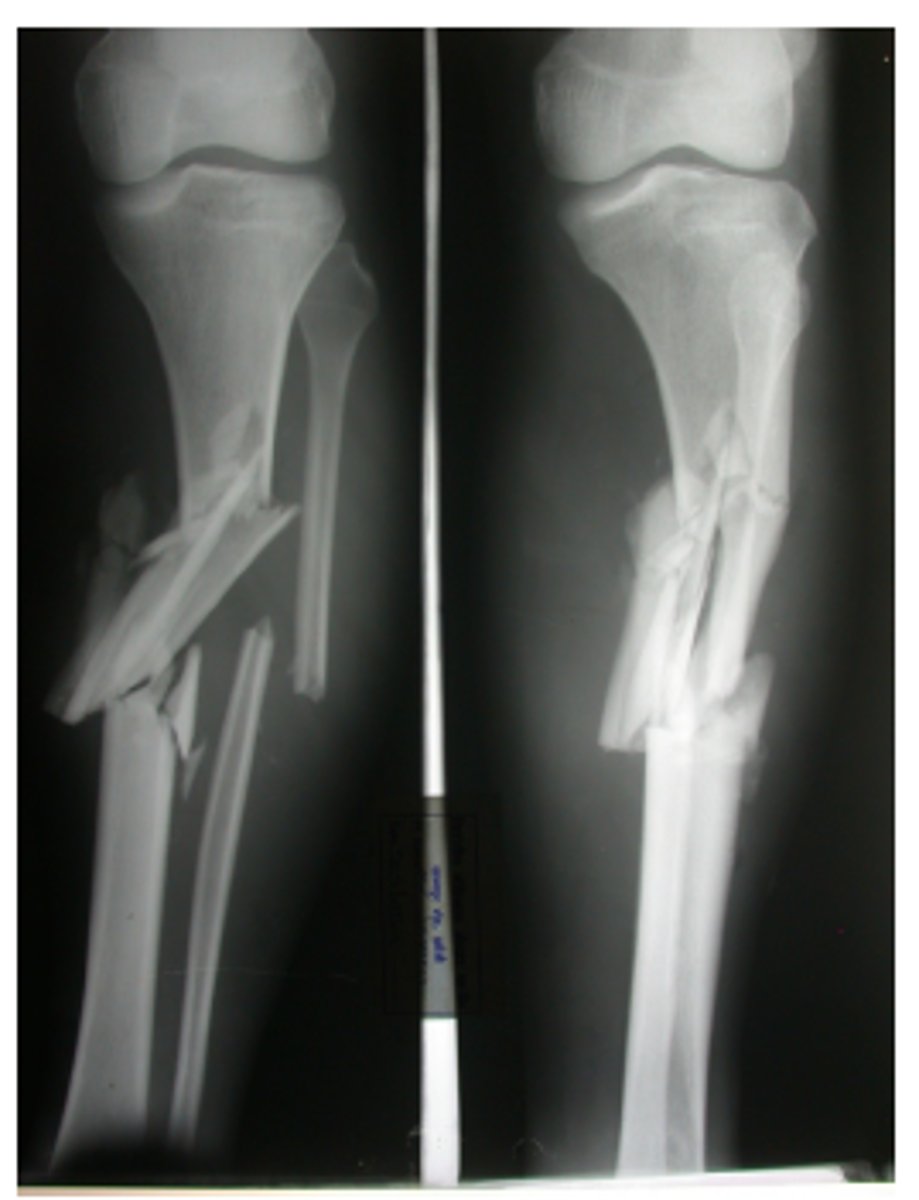
Communicated fracture
Fracture in which the bone breaks into small pieces
Hematoma
1st phase of fracture healing, blood swells around area of inflammation; lasts 72 hours
Granulation tissue formation
2nd phase of fracture healing; new blood vessels, osteoblasts, and fibroblasts form; lasts 3-14 days
Callus formation
3rd phase of fracture healing; calcium, phosphorus, magnesium start to be deposited
Ossification of callus
4th stage of fracture healing: occurs from 3 weeks to 5 months after injury and continues until the fracture has healed
Consolidation
5th stage of fracture healing; callus continues to develop, the area of injury is almost unnoticeable, bony fragments are gone but area is still fragile
Remodeling
6th stage of fracture healing; lasts months to years; hard callus (woven bone) is replaced by stronger lamellar bone
Pain, poikilothermia (cooler temp at injury), paresthesia (numbness), paralysis, pulse, pallor
What are the 6 Ps used to assess fractures?
Temperature, pulse, colour, edema, sensation, strength
What should be assessed in the extremities following a fracture? (thick pulsing cocks emit sticky substances)
Closed fracture reduction
Nonsurgical, manual replacement of bone fragments to previous anatomical position; traction and countertraction manually applied to bone fragments to restore position, length, and alignment
Open fracture reduction
Correction of bone alignment through surgical incision; includes internal fixation with use of wires, screws, pins, plates, intramedullary rods, or nails
Traction
Application of pulling force to an injured or disease part of body while countertraction pulls in opposite direction; helps maintain bones in alignment and expands joint space to give more room to heal; prevents soft tissue damage from fracture moving around
Skin traction
Traction is attached to skin; short term treatment of holding a limb in alignment until bones are aligned or until surgery occurs; i.e. tape/boot/splint put on limb; helps diminish muscle spasms
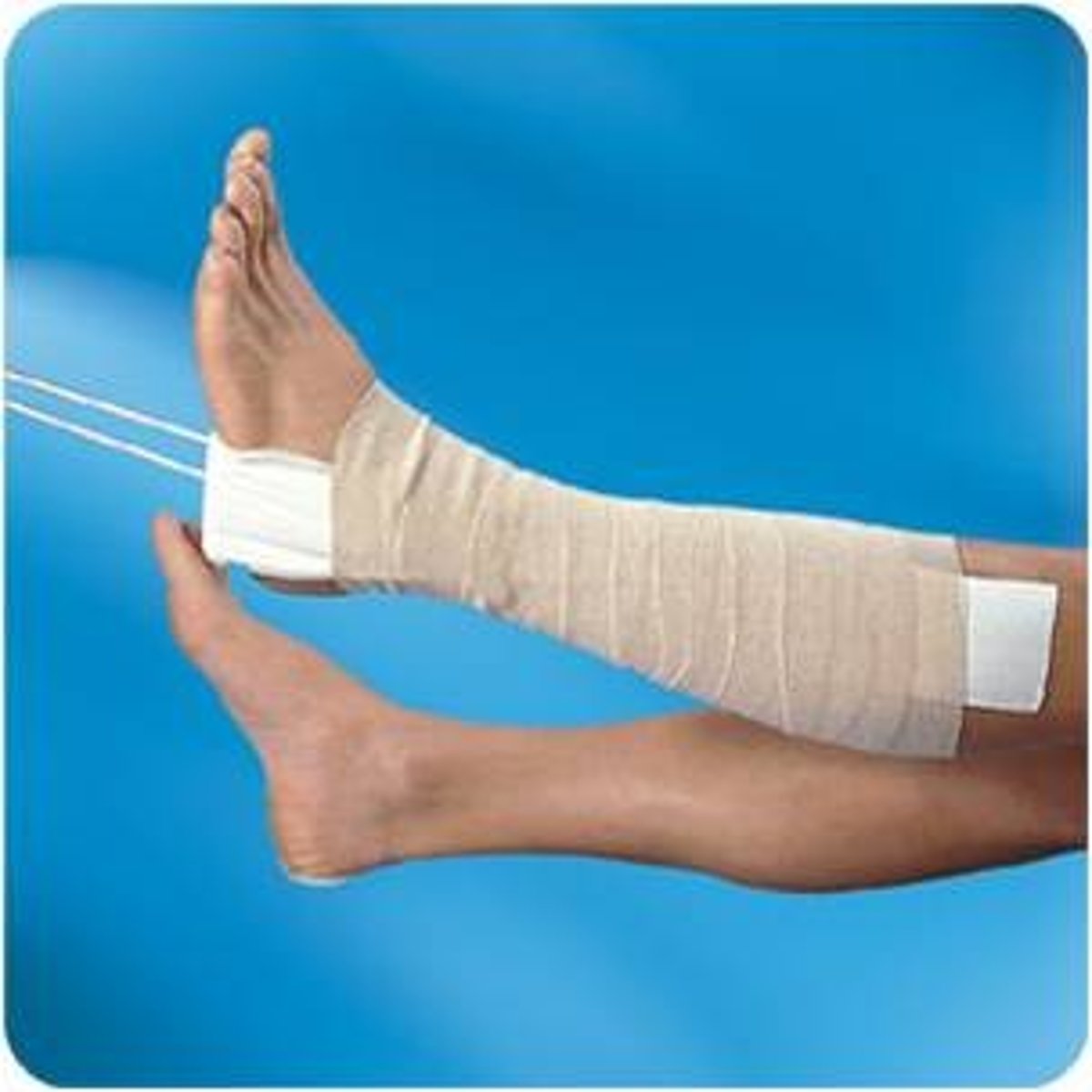
2.3-4.5 kg
How much weight can you apply to skin traction?
Skeletal traction
Long term traction; aligns injured area and treats contractures; screws are placed into bones which pull on the bones to keep things in alignment; weight can be much heavier because the securement can tolerate it
2-20kg
How much weight can you apply to skeletal traction?
Plaster of Paris cast
Inexpensive, easy to apply cast with a low incidence of allergic reactions; takes 24-48 hours to dry and weight bearing must be delayed until dried; prone to cracking or crumbling and softens when wet
Fiberglass cast
Lightweight, porous, quick-to-dry cast that allows for immediate weight bearing; expensive, macerates skin if padding becomes wet, not recommended for severe injuries or those accompanies by excessive swelling
Petaling the cast
Used to prevent edges of a cast from causing skin breakdown
Compartment syndrome
Swelling in a confined space that produces dangerous pressure; may cut off blood flow or damage sensitive tissue
Patients with limited mobility
What patient population is most susceptible to a venous thromboembolism?
Inability to get up from a fall, severe pain in hip/groin, shorter let on side of injured hip, bruising and swelling in/around hip area
S&S of a hip fracture
Total hip replacement
Procedure in which a surgeon removes the damaged sections of the hip joint and replaces them with parts usually constructed of metal, ceramic, or very hard plastic
4-6 weeks
How long should a patient post-op from a hip replacement wait before bathing in a tub or driving?
True
True or false? The nurse should instruct a patient who just received a hip replacement to avoid bending over, crossing legs/feet, and sitting on low seats