Human Physiology Yr1
1/62
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
63 Terms
Total Body Fluid & Cellular fluid
31 Extracellular fluid Eg. Blood plasma
32 Intracellular fluid
Fluid mosaic model
Cell membrane - Phospholipid bilayer consisting of Hydrophilic heads & Hydrophobic tails
Transmembrane Proteins to allow for pores - Allow movement of molecules
Permeability to molecules:
Very permeable to H2O
Increased size = Decreased permeability
Lipid soluble
Charge = most important, increasing charge = decreased permeability
Impermeability to molecules:
Sugars
Proteins
Inorganic ions
Unless helped
Diffusion
Random movement from High conc to Low conc (Down Gradient)
Filtration
Pores allow this process due to size
Osmosis
Movement of H2O in response to a solute conc Grad
Osmotic Pressure
The pressure that would stop H2O from moving
Protein facilitated movement
Carriers/Channels
High to low = Facilitated diffusion
Low to high = Active transport
Exocytosis
Out of cells
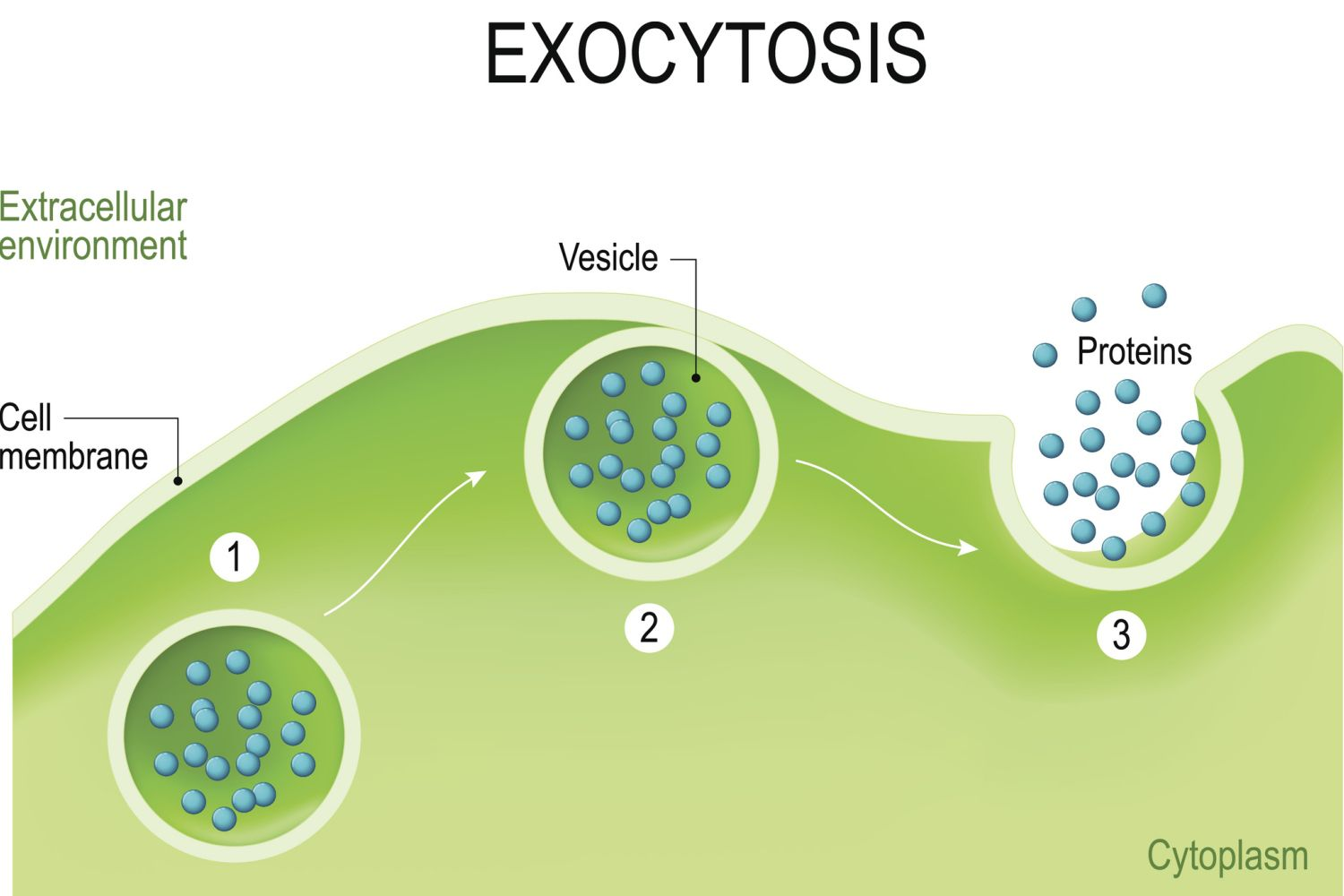
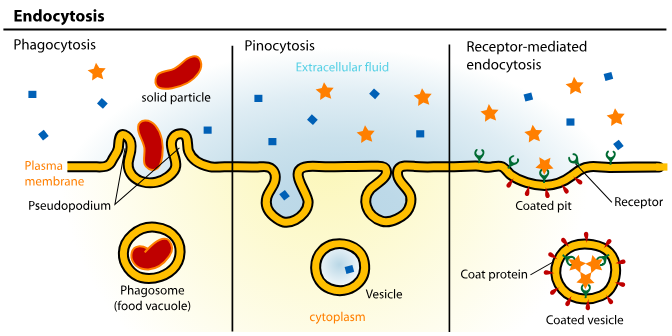
Endocytosis
In to cells - Proteins and very large molecules
Pinocytosis - Membrane pinches off
Phagocytosis - Arms of cytoplasm encapsulate
Functional anatomy of a Synapse
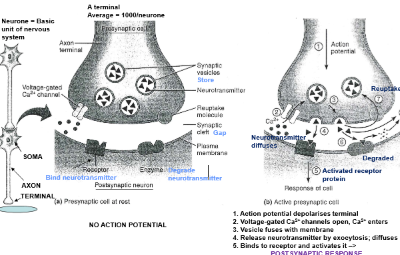
Generation of an Action Potential
Nerve cells have a low threshold for excitation
Electrical/Mechanical/Chemical factors impact ion distribution
Local/non-propergated ( Generator potential (EPSP & IPSP))
Propergated ( Action Potential)
Action potential (Propergated) & Nerve cell structure
All or none law
If stimulus is sufficient = Response
Action Potential leads to Na+ , K+ across the membrane
Absolute refractory - Cell cannot fire = No more AP ( One way movement)
Relative refractory- Only larger than normal Stimuli = New AP
Action potential starts in the Axon Hillsneck
Travels in one direction to synapse
Myelinated Axons - Jumps between nodes of Ravier (Ensures Conduction Velocity)
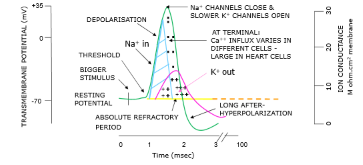
Neurones & The Transmembrane Resting Potential
Neurones release neurotransmitters across the synapse
Transmission through the movement of charged ions across the cell membrane
Transmembrane Resting Potential = -70mV
This is the electrical gradient between Extra 7 Intracellular fluid
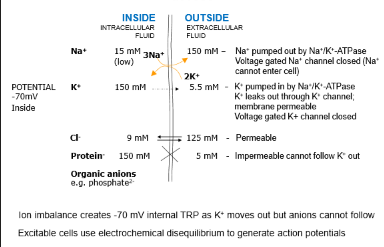
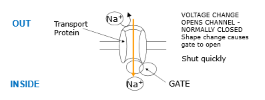
Voltage Gated ion channels
Closed at rest & play an important role in the generation of action potentials
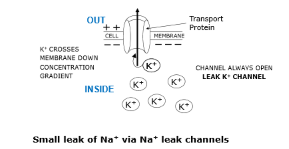
K+ channels
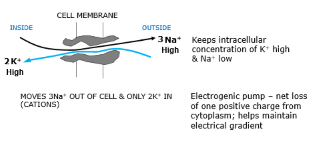
Sodium potassium pump/ NaKATPase
K+ channels
Sodium potassium pump/ NaKATPase
Post synaptic Potentials
Local change in transmembrane potential
Not propagated
No Refractory
Can summate - Add together
IPSP
Inhibitory Postsynaptic potential
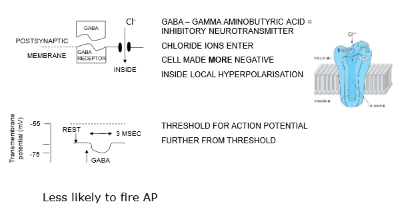
EPSP
Excitatory Postsynaptic potential
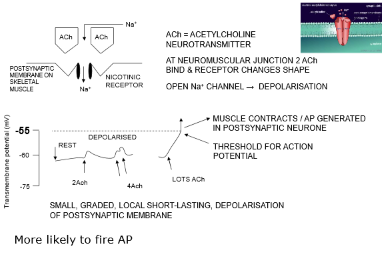
Summation of IPSPs & EPSPs
EPSPs synapse mainly on dendrites
IPSPs synapse mainly on cell body
Spatial summation - 2 EPSPs on adjacent membranes add
Temporal summation 2 EPSPs close in time add together
IPSPs / EPSPs can cancel out
Pre synaptic inhibition
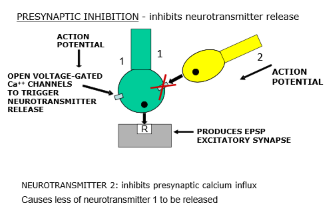
Peripheral Nervous system
Senses
Somatic:
Touch
Temp
Proprioception
Pain
Visceral:
BP
Internal Temp
PH
Blood Glucose
Special senses:
Smell
Taste
Hearing
Vision
Balance
Receptor cells synapse with sensory neurone
Sensory Pathway
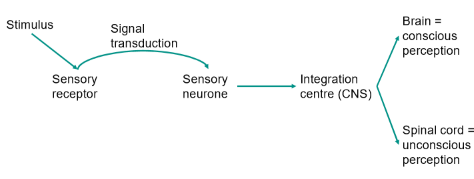
Somatic Nerves System Pathway
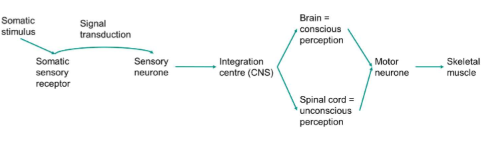
Nerves system schematic
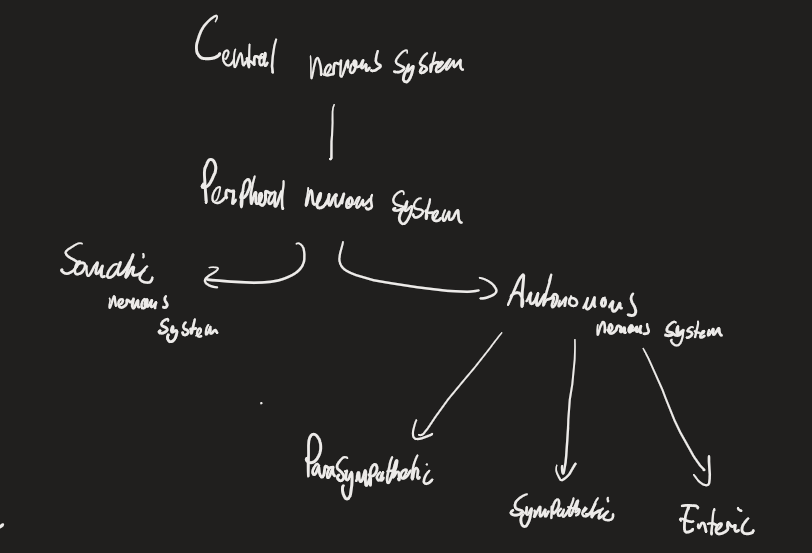
Autonomic Nerves system
Subconscious control over internal organs, conditions and homeostasis
EG. HR or Hormones
Ganglia
Cell bodies of many peripheral autonomic neurons occurring in clusters swell on nerve trunks
Motor/ Efferent pathways of ANS
Axons that form with ganglionic cells = preganglionic fibres
Axons innervating effector cells = Postganglionic fibres
ANS Facts
Conveys all outputs from the CNS to the body, other than control of skeletal muscle
Regulates most of homeostasis
The sympathetic and parasympathetic systems work separately
Sympathetic = increase in stress, Parasympathetic = Rest and digest
Influenced by sensory info/ Brain ( control centres)
Sympathetic Nerves system
Excitement - Adrenaline “ Fight or Flight”
CV response = 89- 155 BPM
Neurotransmitter = Noradrenaline
Formed from tyrosine
Released across the synapse & taken up by Beta receptors on the postsynaptic cell
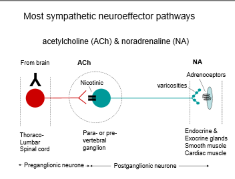
Other sympathetic pathway
Adrenaline into the blood
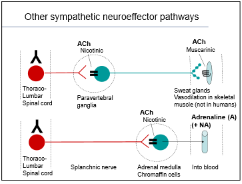
Synaptic Receptors
Alpha:
Postsynaptic -A1/A2
Presynaptic -A1
A1 antagonist promotes relaxation
A1 Agonist promotes vasoconstriction
Beta:
Post synaptic - b1/b2/b3
B1 promote heart and muscle function - used for cardiac arrest
B2 agonists - Used a as a treatment for asthma - enhance bronchioles
B antagonists ( Beta blockers) - Slow heart
Parasympathetic nervous system
Keeps the body at low energy use
Parasympathetic contribution to HR
Ach (SA node) → M2 receptor = Decreased HR
Atrial muscle = Decreased HR
AV node = Decreased rate of conduction
Ach Receptors
Nicotinic - at ganglia/brain/NMJ ( Ionotropic - ion channel receptor controls Na+/K+ transport)
Muscarinic - at autonomic target tissues/brain ( Metabotropic - G protein & 2nd messenger controls k+/Ca+ transport)
M1 - Neuronal/gut - Increase gastric acid
M2 - Cardiac - Decreased HR/Force
M3 - Smooth muscle constriction
Parasympathetic Neuroeffector pathway
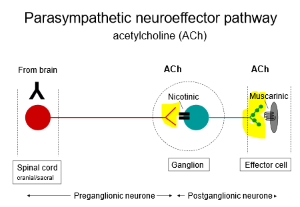
PNS drugs
Agonists (Increase PNS activity)
Pilocarpine
Muscarine
Nicotine
Antagonists ( Decreased PNS activity)
Atropine - Blocks receptors
Transduction
Converting stimulus into electrical signals
Activation of receptors = movement of ion channels
Sensory neuron - Action potential
Mechanoreceptors
Mostly located on the skin / visceral organs
Stimuli = Physical distortion
Free nerve endings
Ruffini corpuscles
Pacunian corpuscles
Merkles disk
Meisser corpuscles
Free nerve endings
Thermoreceptors
Mostly on the skin
Stimuli = Temperature
Free nerve endings
TRPV1 = Hot
TRPV8 = Cold
Nociceptors
Mostly on skin
Potential to cause tissue damage (stimuli)
Free nerve endings
mechanical, thermal, chemical
Proprioreceptors
Location: Muscles, tendons, ligaments & joints
Stimuli = Muscle tension
Subtypes:
Muscle spindles
Golgi tendon organs
Proprioreception in joints
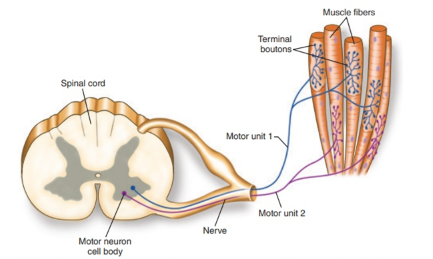
Cardiac pumps
Right ventricle = Pulmonary circulation
Left ventricle = Systemic circulation
Cardiac output
HR x SV
Rest = 5L
Exercise = 12.5 - 30L
CV response to Exercise
Increase venous return due to CO increase/ Compression of veins from skeletal muscle
Increased SNS activity
Decreased PSNS activity (increased HR)
Cardiac hypertrophy from prolonged training (LV enlarges /SV increases)
Aorta/ Large arteries
Thich walls
Highly elastic
Role = distribution - High pressure - propulsion
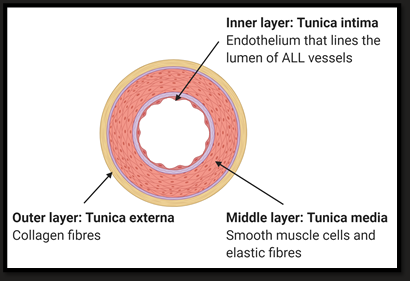
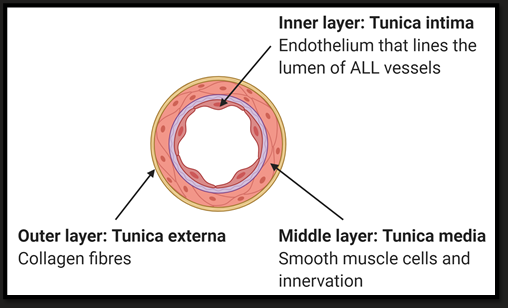
Arterioles
Thick walls
Muscular
Role = Tissue distribution, variable resistance
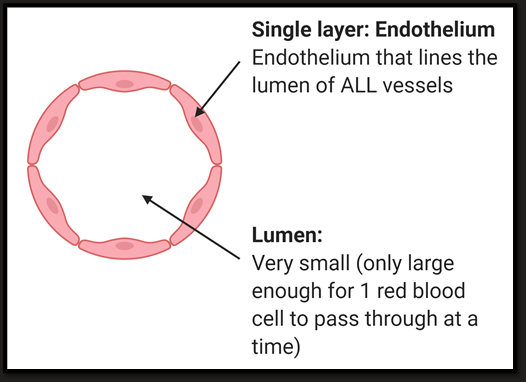
Capillaries
Single cell thick
Lack of elastin/ muscle
Functional for exchange
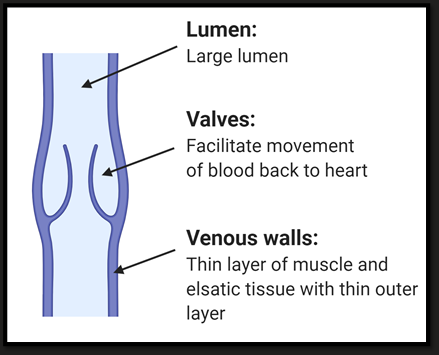
Veins & venules
Thin walls
Some muscle
Valves
Reservoir = 60% of blood
Equations - Flow rate, velocity & TPR
Flow rate = volume/ unit time
Peripheral res = pressure dif/flow
Velocity = Distance/ unit time
Cardiac excitation
Action potential generated at the SA node
Rapid excitation of both atria
Reaches AV - slows conduction ( Allows atria to contract/ Ventricle emptying)
Excitation down BOH & Purkunje fibres to ensure activity of ventricular cells
Poiseulle’s law
Factors that affect flow through a vessel:
Pressure (pi - po)
Length (L)
Radius (r4 )
Viscosity (n)
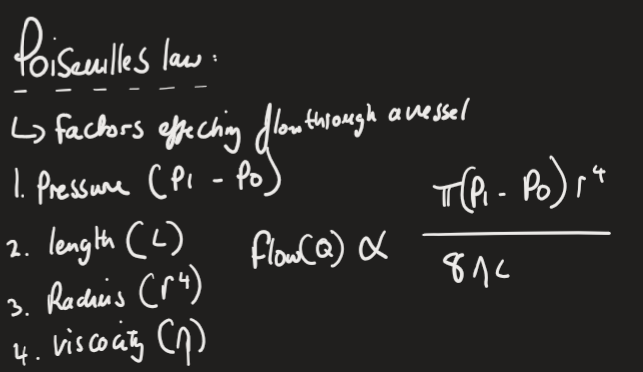
SA node
SA node = Pacemaker - Creates its own action potential for the heart
8mm long/2mm thick - in the right atrial wall
Phases:
0 - Upstroke of action potential is less steep than in myocytes
3 - Plateau is not sustained
4 - Membrane potential deviates from k+ potential
Action potential in SA:
Slow depolarisation - Na influx, ca influx, reduced K+ efflux
Rapid depolarisation - Ca efflux
Repolarisation - K+ Exflux
Cardiac Contraction
Atrial systole
Av valves open + blood into ventricles
Atria excitation should be complete before ventricular contraction
Ventricular systole
Ventricles contract - pressure increase closes av valves
Pressure in ventricles rises above aortic pressure - aortic valve opens + Blood pumped out
Ventricular diastole
Pressure falls in ventricles ( Below aortic) - Aortic valves close
Pressure continues to fall below atrial pressure - AV valves close
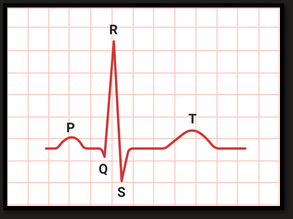
ECG
4 Events - 3 visable
Arterial depolarisation (P wave)
Ventricular depolarisation ( Masks atrial repolarisation) ( QRS)
Ventricular repolarisation ( T wave)
Systolic BP
The force the heart exerts on the walls of arteries every time it beats
120mmHg
Determined by:
SV - Increased SV = Increased SBP
Decreased Aortic elasticity = Increased SBP
Diastolic BP
Pressure in the arteries during the period when the heart is not beating
80mmHg
Determined by:
Increased TPR = Decreased DBP
Decreased Aortic elasticity = Decreased DBP
Decreased HR = Decreased DBP
Key measurements of BP
SV = EDV - ESV
CO = HR x SV
Pulse pressure = SBP - DBP
Mean BP = DBP x 1/3 Pulse pressure
Flow ( CO) = Mean BP/TPR
Why is BP control important
Too low = Inadequate supply of o2 to tissues
Too high = Excessive strain on heart / increased damage to vascular tissue
NEXT TOPICS
INFLUNCE BP HR etc EFFECTOR MECHANISM, Detereminaents of blood flow. High bp. Map = co x TPR