Quiz 8: Medicinal Chemistry
1/52
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
53 Terms
What are monoamines?
neurotransmitters with one NH₂ group (serotonin, NE, dopamine
What are MAOs and where are they located?
mitochondrial membrane enzymes that break down monoamines
What does MAO-A vs MAO-B metabolize?
MAO-A → serotonin, NE, tyramine
MAO-B → dopamine, phenethylamine
What drug led to MAOI discovery and what was the first MAOI?
isoniazid → iproniazid (hepatotoxic)
What causes hypertensive crisis with MAOIs?
tramine buildup → ↑ NE → severe hypertension
What must patients avoid on MAOIs?
tyramine foods (cheese, wine, beer, chocolate, meats)
When are MAOIs used clinically?
last-line when TCAs or SSRIs don't work due to severe drug-food + drug-drug interactions
What are the 3 monoamine transporters?
DAT, NET, SERT
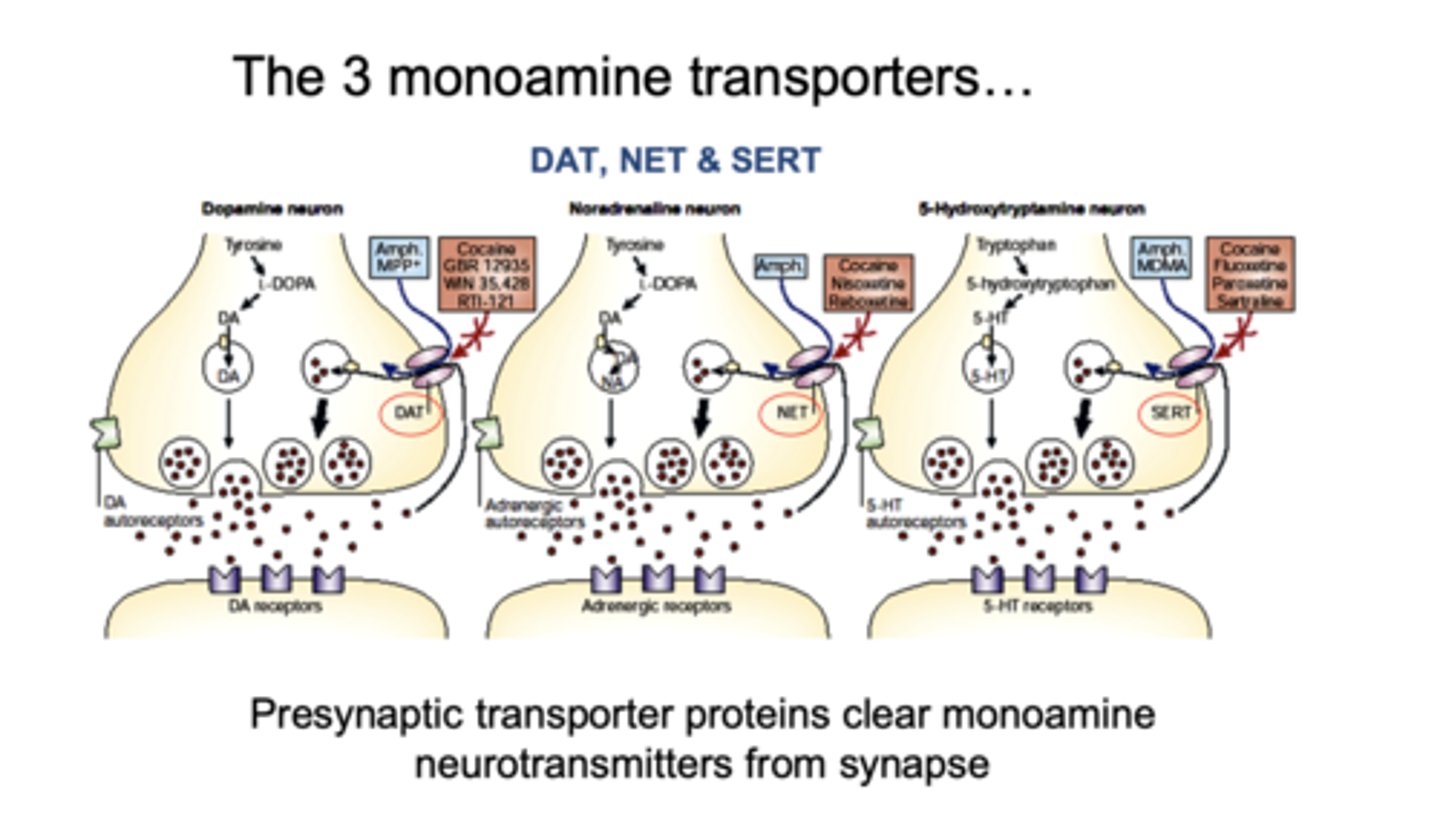
What do these monoamine transporters do?
reuptake neurotransmitters from synapse
What happens when transporters are inhibited?
↑ neurotransmitter levels → ↑ signaling
What defines tricyclic antidepressants (TCAs)?
3-ring structure; inhibit NET & SERT non selectively
What does a smaller Ki value mean?
higher binding affinity
What receptors cause TCA side effects?
M1, H1, and alpha-1
How long does it take for TCAs to be effective?
2-4 weeks
What are TCAs used to treat?
depression, panic attacks, OCD, enuresis, insomnia
What are key adverse effects of TCAs?
anticholinergic, orthostatic hypotension, reflex tachycardia
What was the goal of SERT-selective TCAs?
increase serotonin selectivity, reduce side effects
ex. amitriptyline
Which drug is strongly SERT-selective?
clomipramine (also used for OCD)
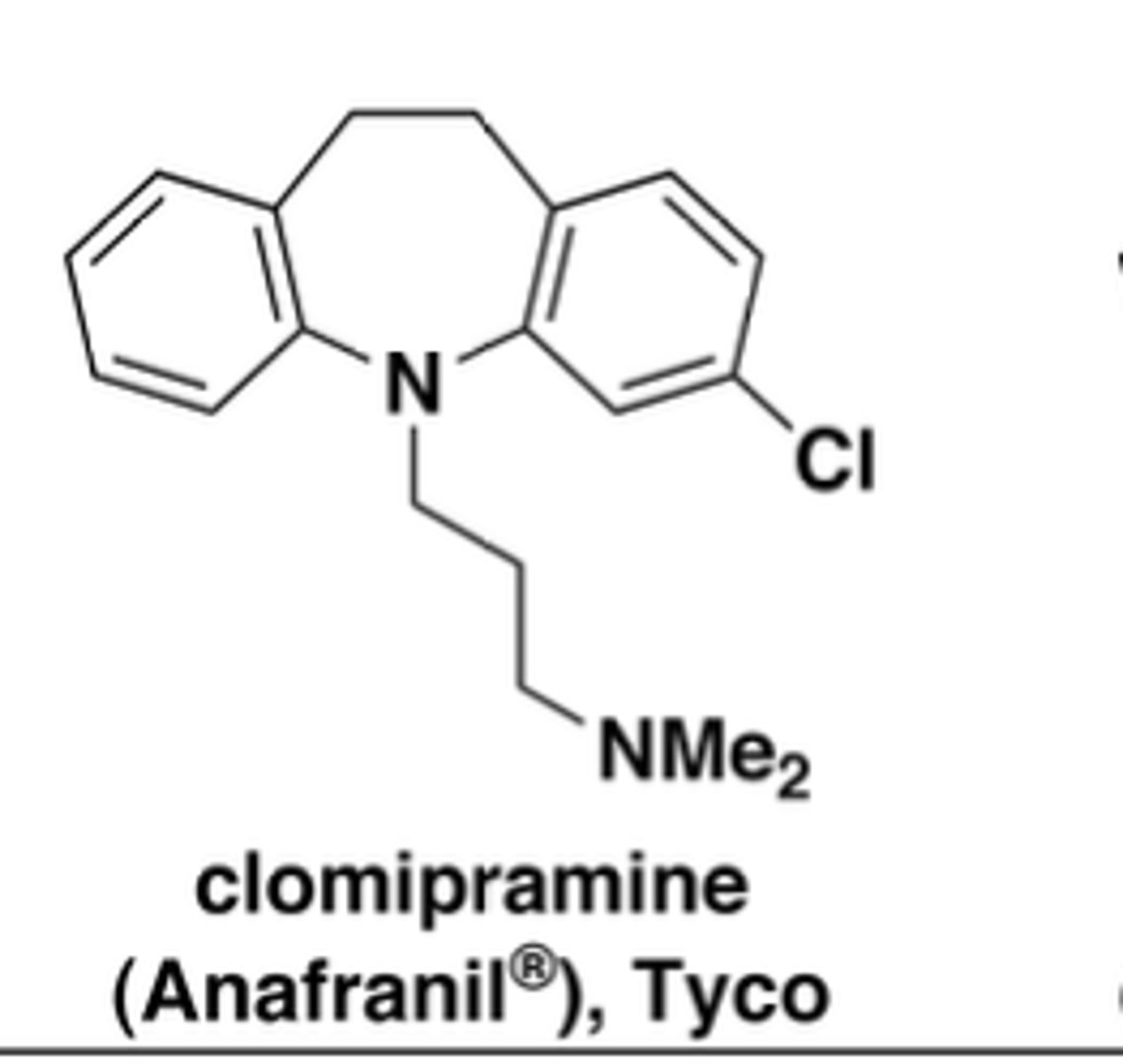
Why didn't SERT-selective TCAs fully solve issues?
still had off-target receptor effects
What defines 2nd gen antidepressants?
structurally diverse; less tricyclic-like (trazodone, buprorion)
How are trazodone dose effects different at low vs. high doses?
Low = sedating
High = antidepressant
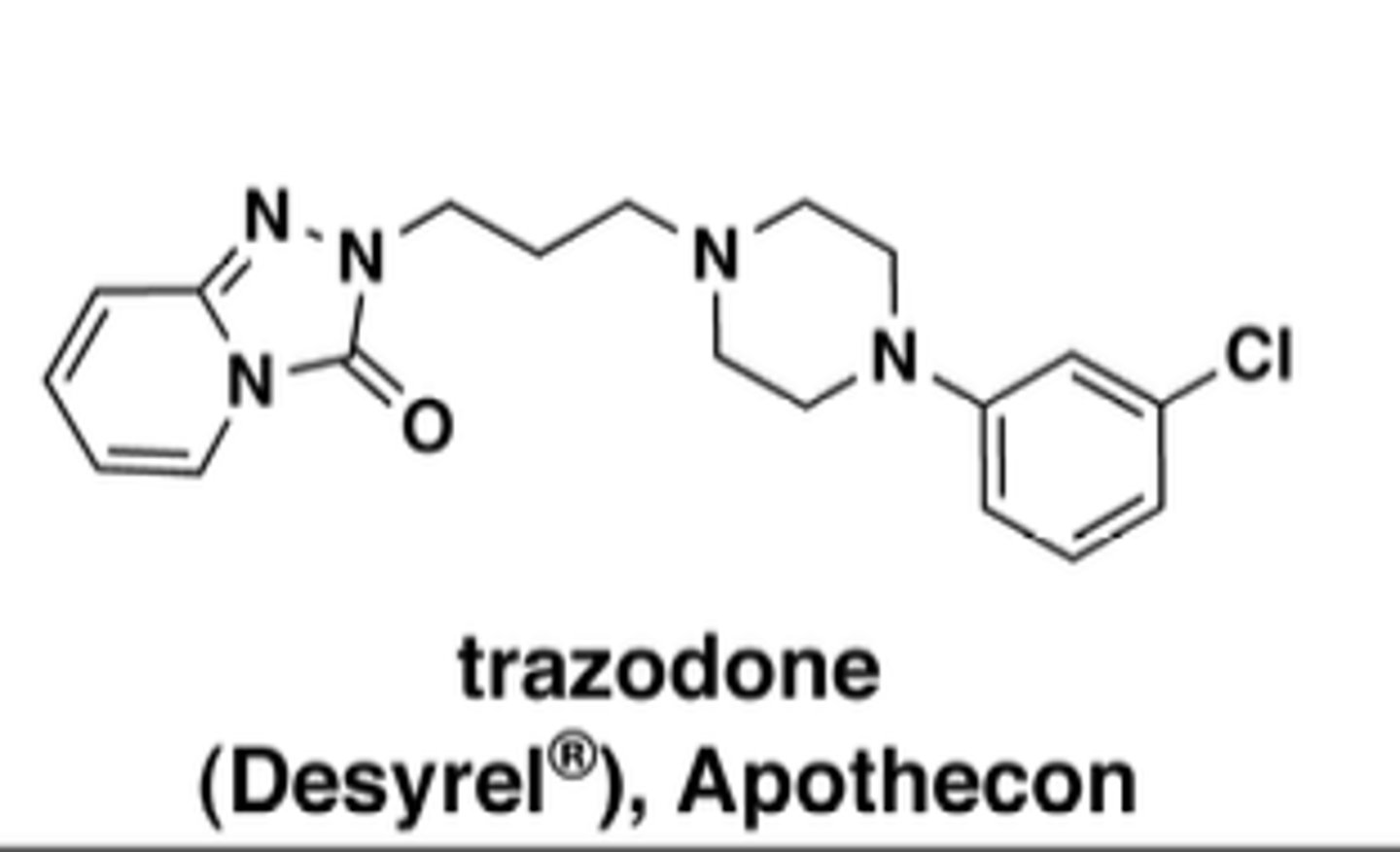
What are key trazodone adverse effects?
priapism
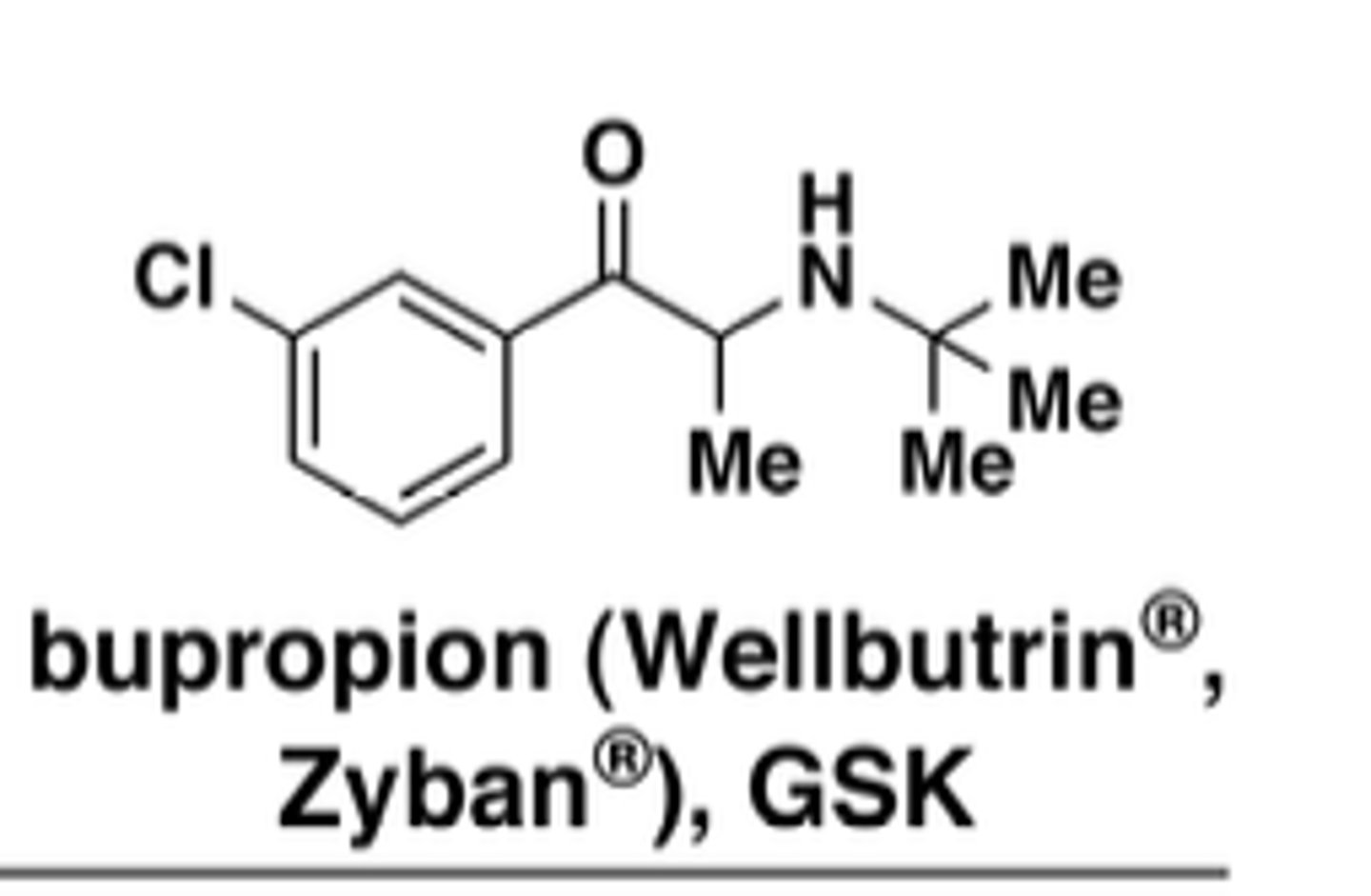
What is bupropion's key mechanism + effect?
DAT inhibitor; CNS stimulant (↑ energy, ↓ appetite) which may cause mania
Why is mirtazapine sedating and weight-gaining?
strong H1 blockade
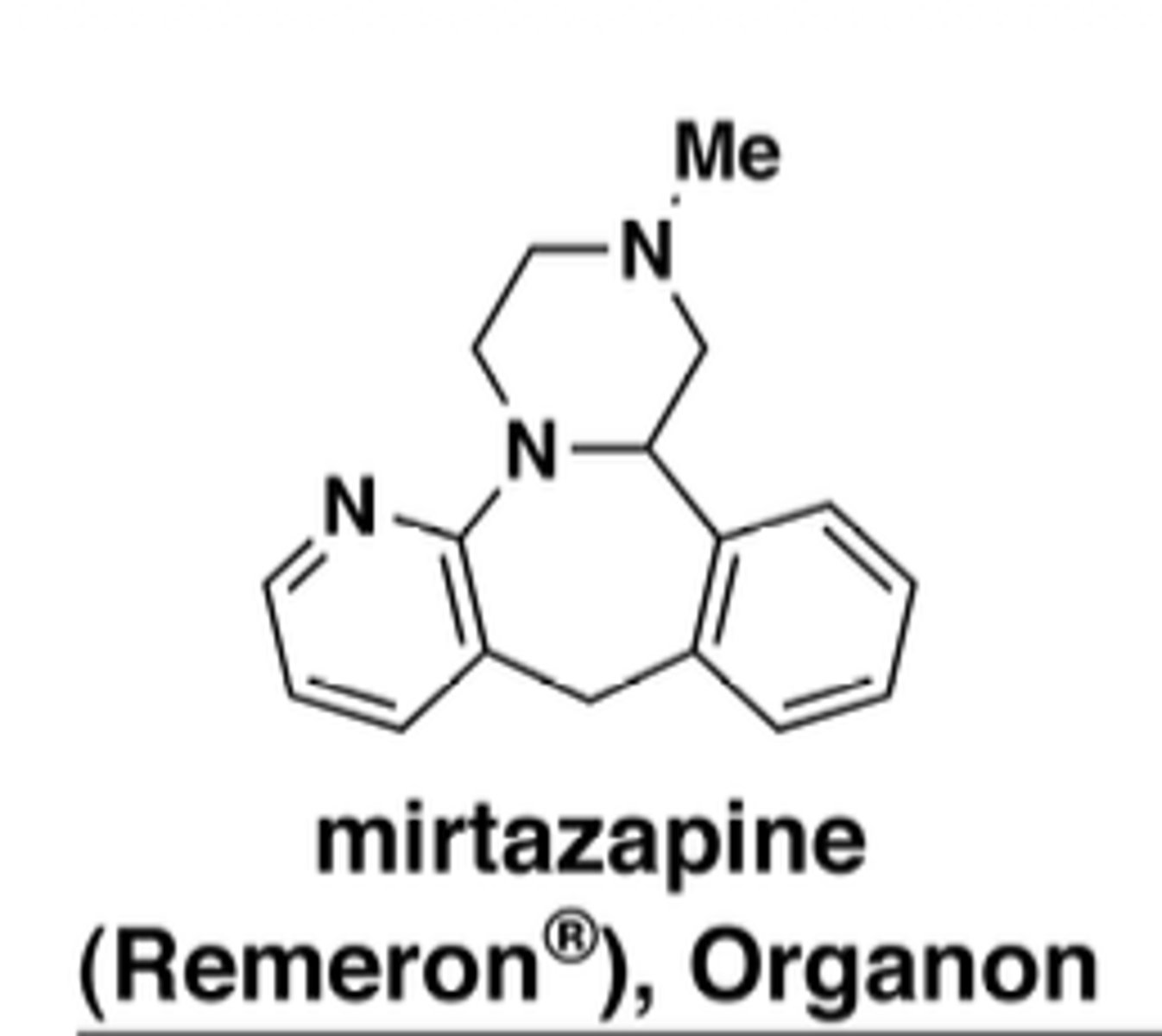
What is unique about mirtazapine onset?
faster (days vs weeks)
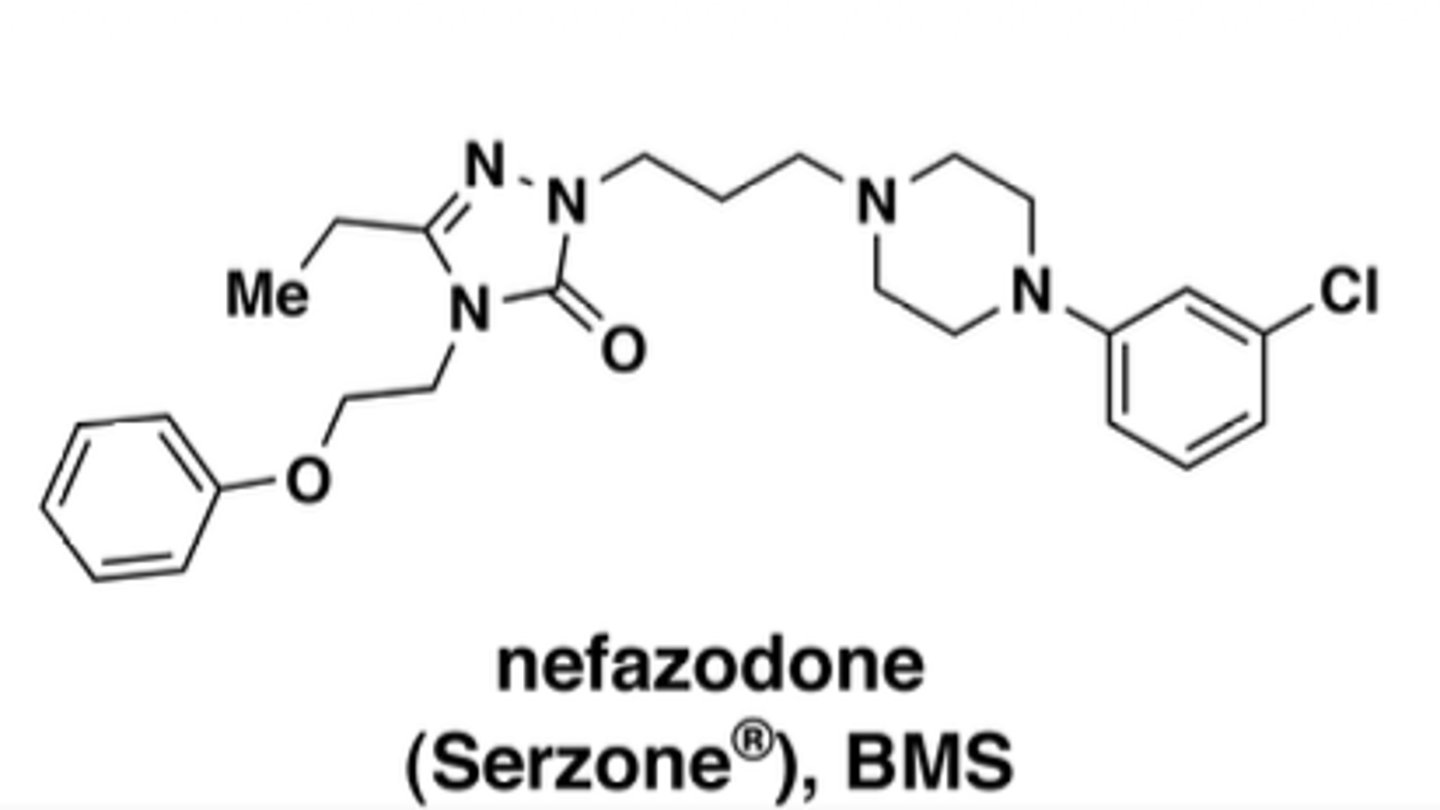
Nefazodone
more potent than trazodone, but less sedating
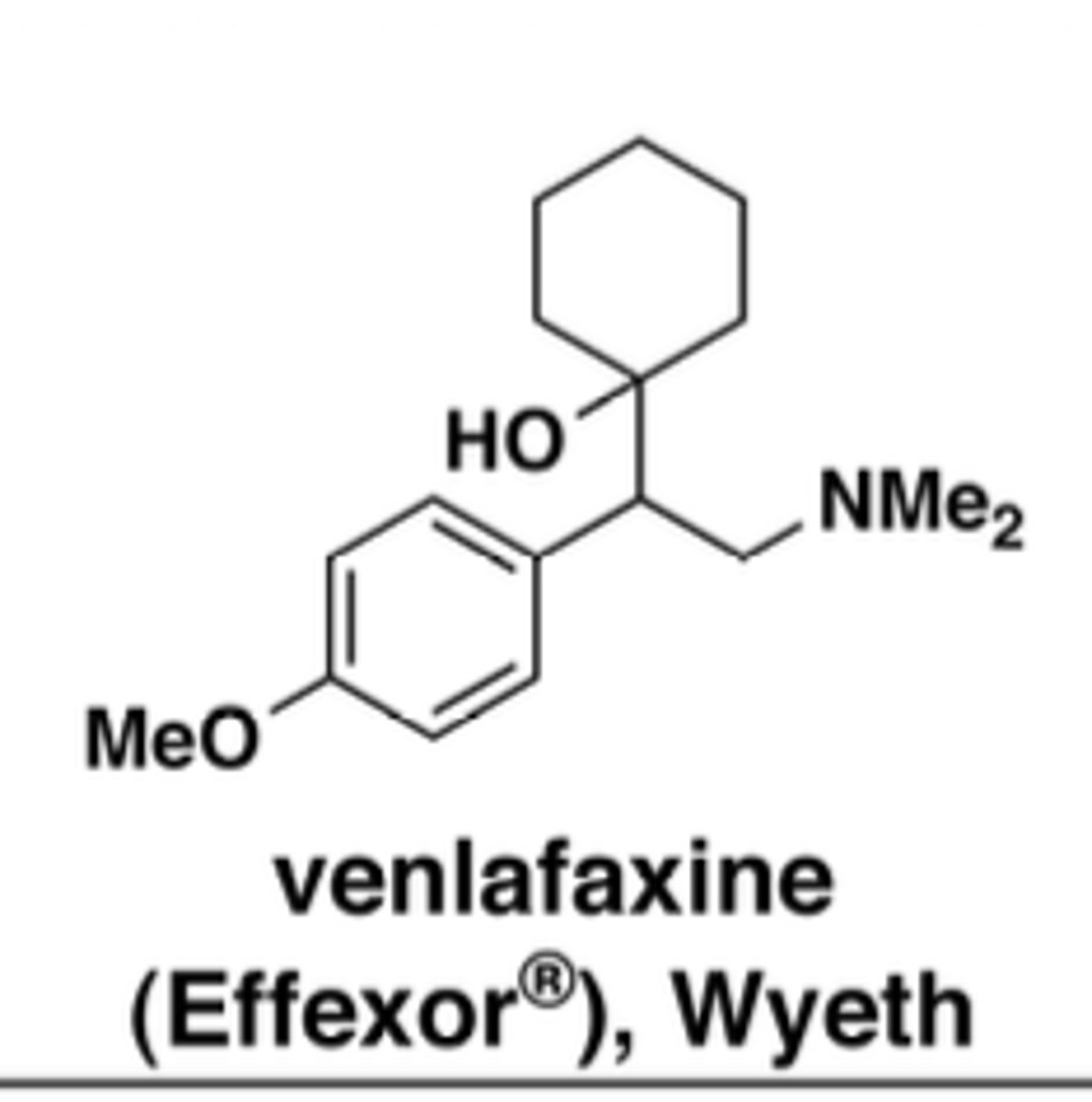
Why is venlafaxine well tolerated?
selective for SERT; minimal M1, H1, alpha-1 effects
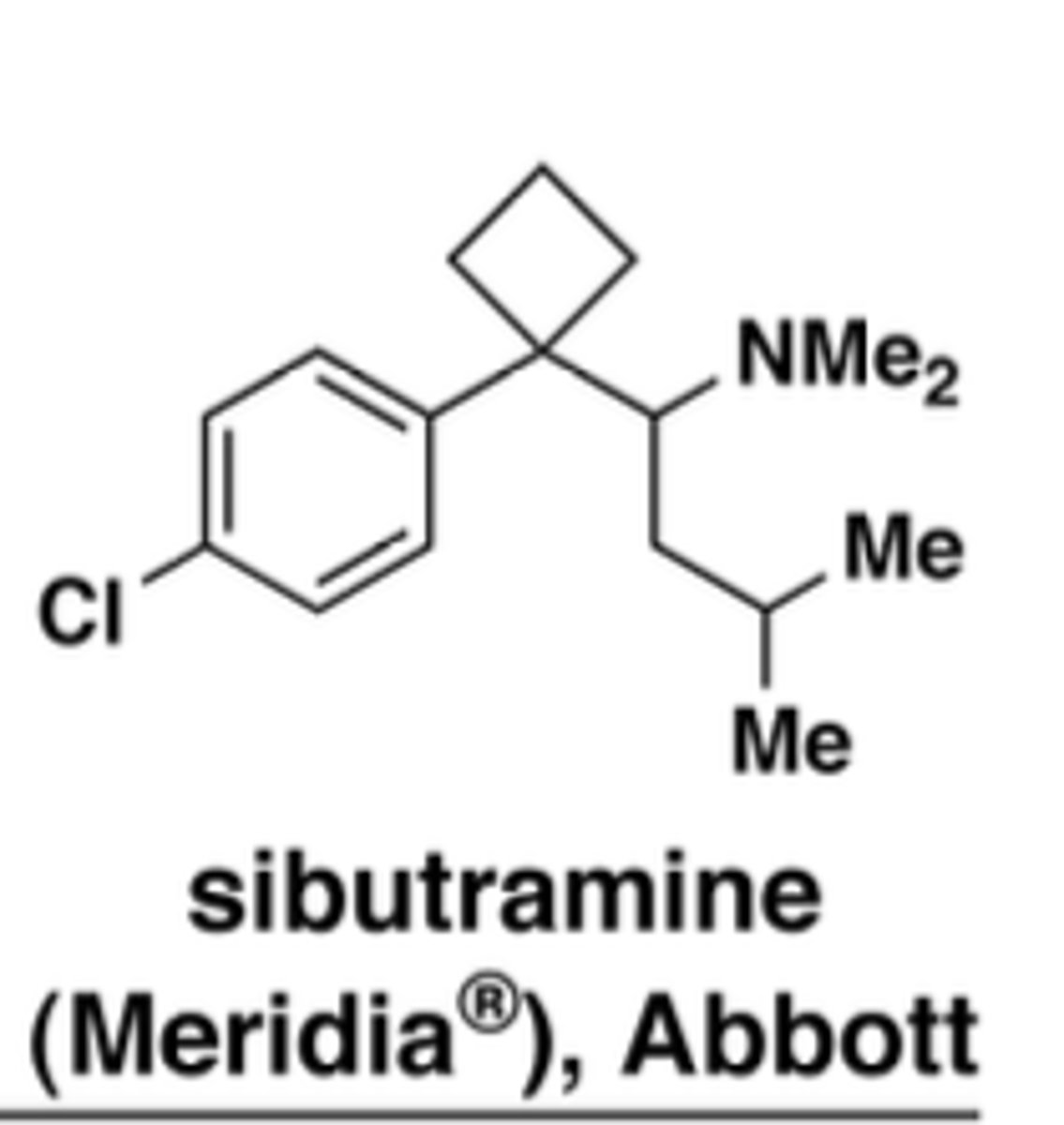
Why was sibutramine discontinued?
↑ BP and heart rate; despite weight loss benefit
What are SSRIs?
selective serotonin reuptake inhibitors
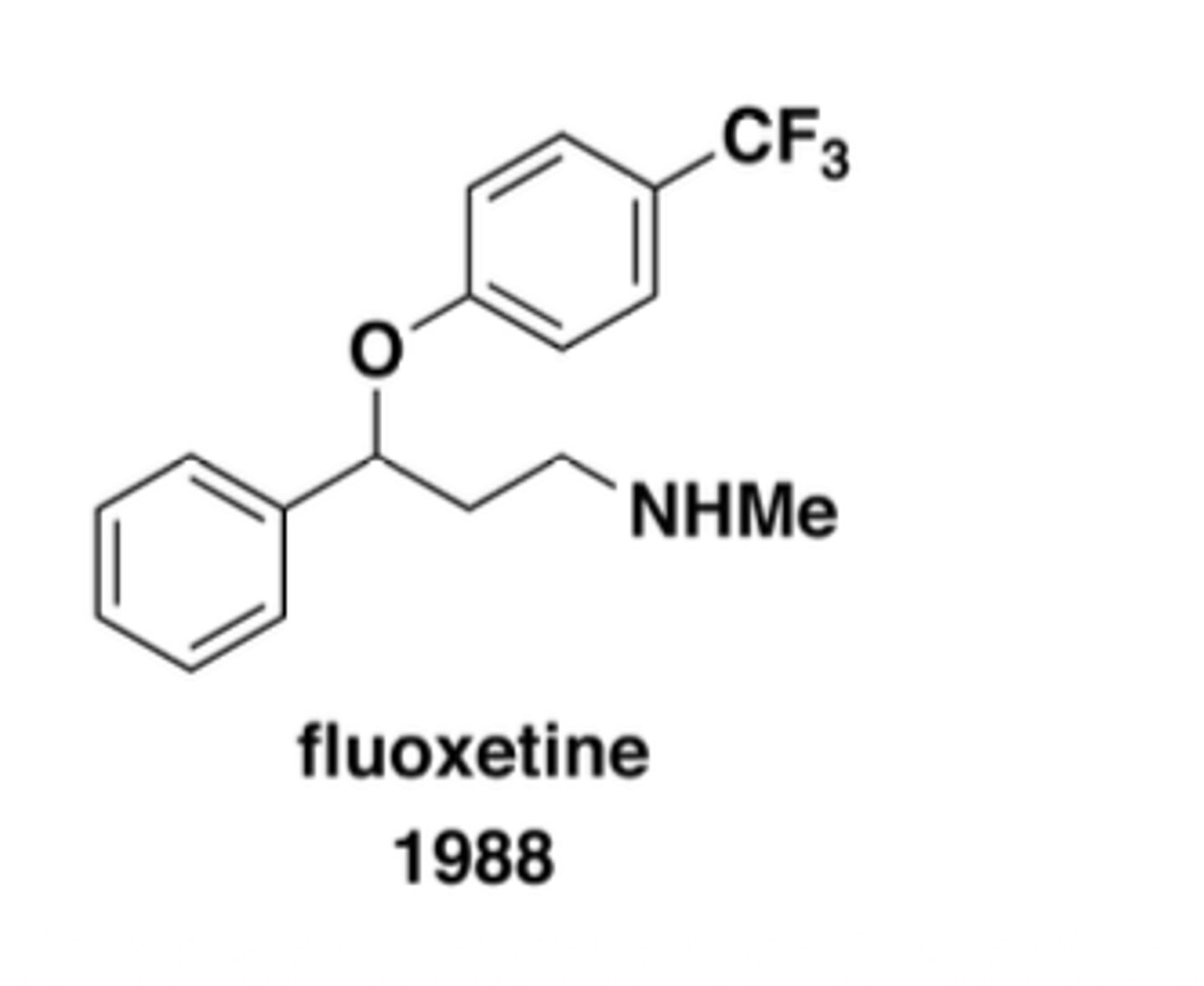
What was the first successful SSRI?
fluoxetine (Prozac)
What drug class led to SSRI development?
antihistamines (e.g., diphenhydramine)
What are key advantages of fluoxetine?
minimal weight gain, safe in overdose; BUT can cause tremor
What issues occurred with early SSRIs?
suicide risk, anorexia (e.g., zimelidine, fluvoxamine)
Citalopram vs Escitalopram?
Citalopram = racemic
Escitalopram = S-enantiomer (more selective)
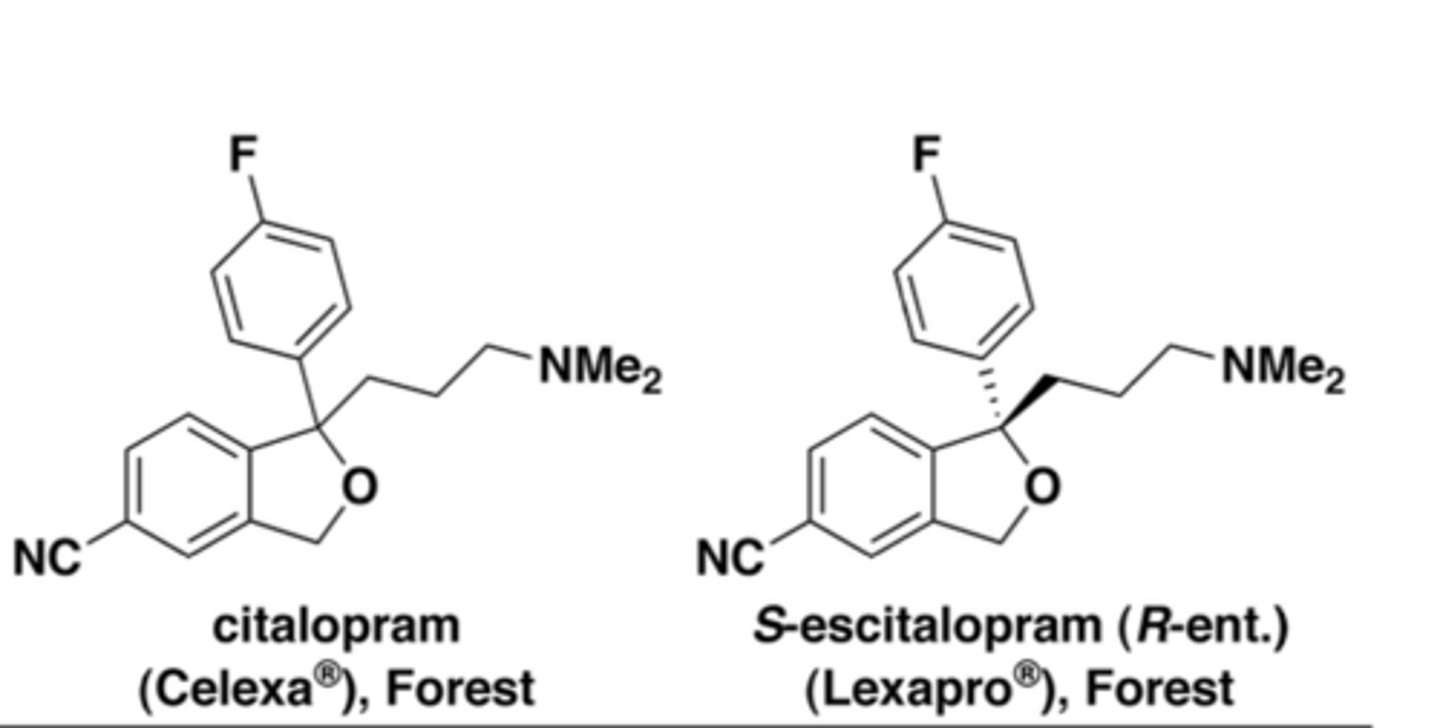
Why is escitalopram better tolerated?
less H1 and alpha-1 activity
What is a key clinical advantage of citalopram compared to other SSRIs?
it has fewer stimulant effects (less activating)
What is paroxetine used for?
panic disorder, anxious depression, GAD, social phobia
What is similar about SSRI onset and efficacy vs TCAs?
similar efficacy; onset ~2-3 weeks
What side effects do SSRIs generally avoid?
anticholinergic, sedative, hypotensive effects
What are common SSRI side effects?
insomnia, agitation, sexual dysfunction, tremor, mania in bipolar patients
What is serotonin syndrome?
life-threatening excess serotonin (esp. with MAOIs)
What is discontinuation syndrome?
insomnia, nausea, flu-like symptoms resulting from abrupt discontinuation of SSRI
What do SNRT inhibitors target?
NET + SERT (favor SERT)
What is duloxetine used for?
depression, physical pain associated with depression, or stress urinary incontinence
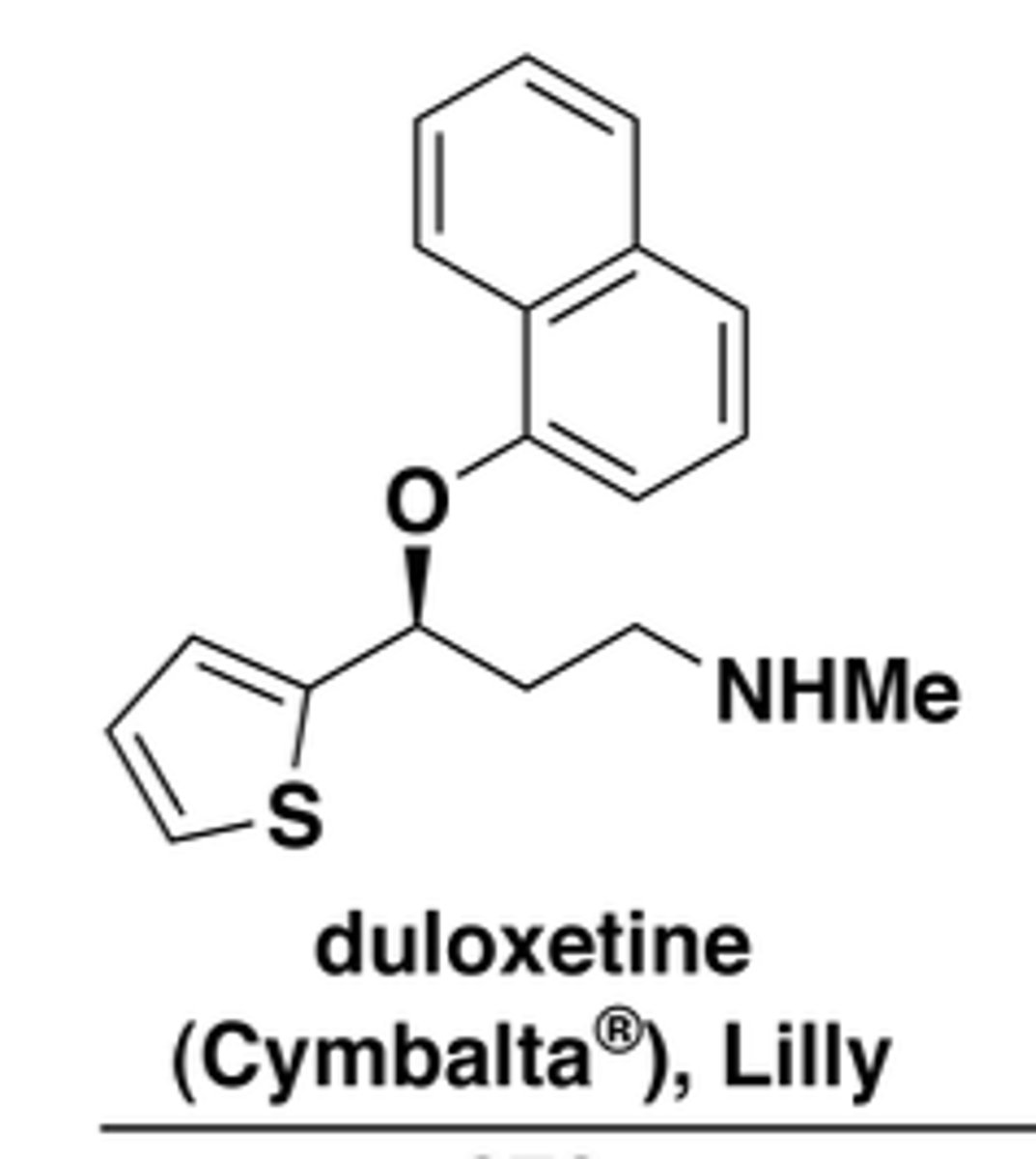
How is duloxetine metabolized?
metabolized by CYP2D6 and CYP1A2 into hydroxylated metabolites; t½ ≈ 10-15 hours
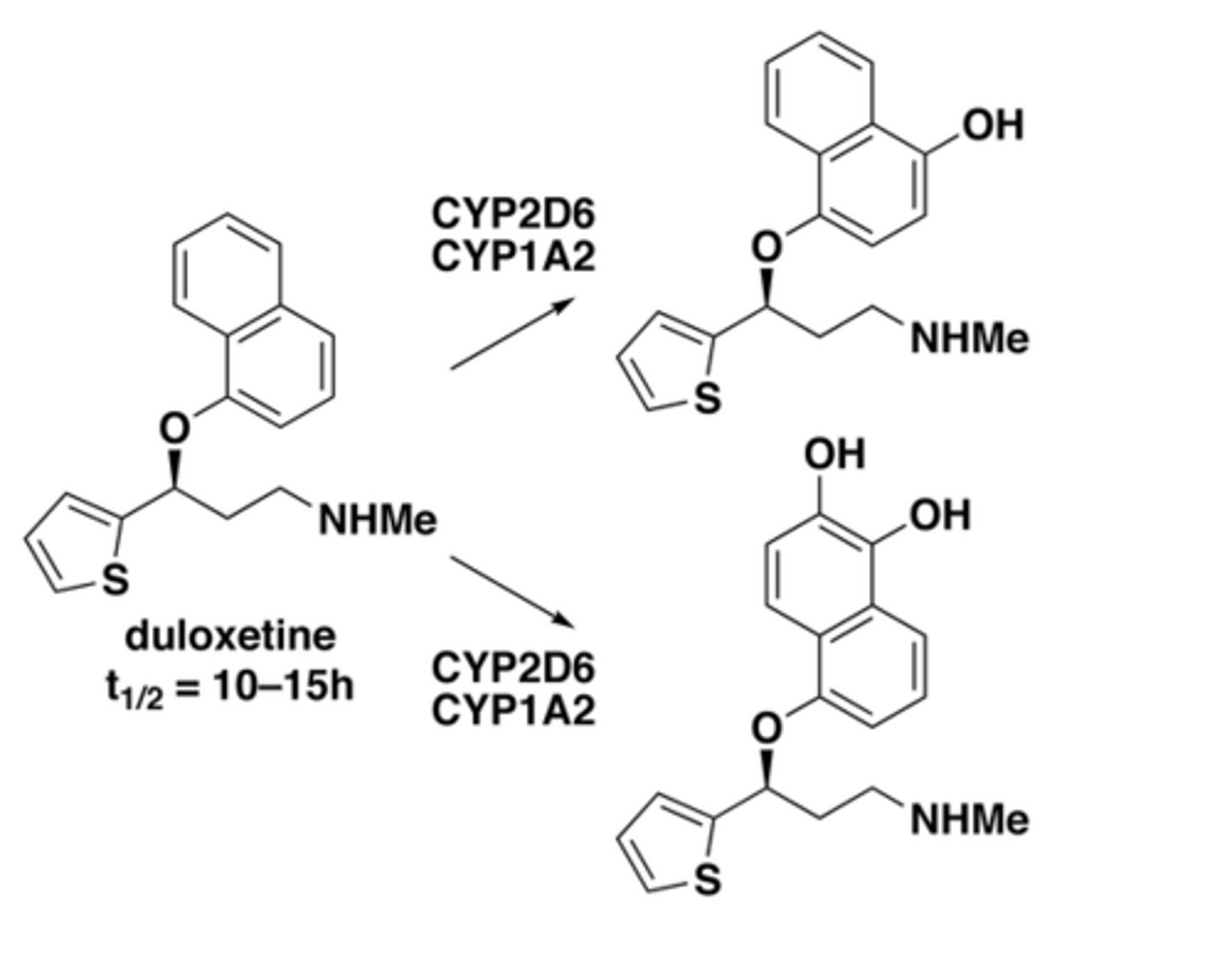
What are common duloxetine side effects?
nausea, dry mouth, constipation, fatigue, headache, insomnia
What is atomoxetine used for?
ADHD
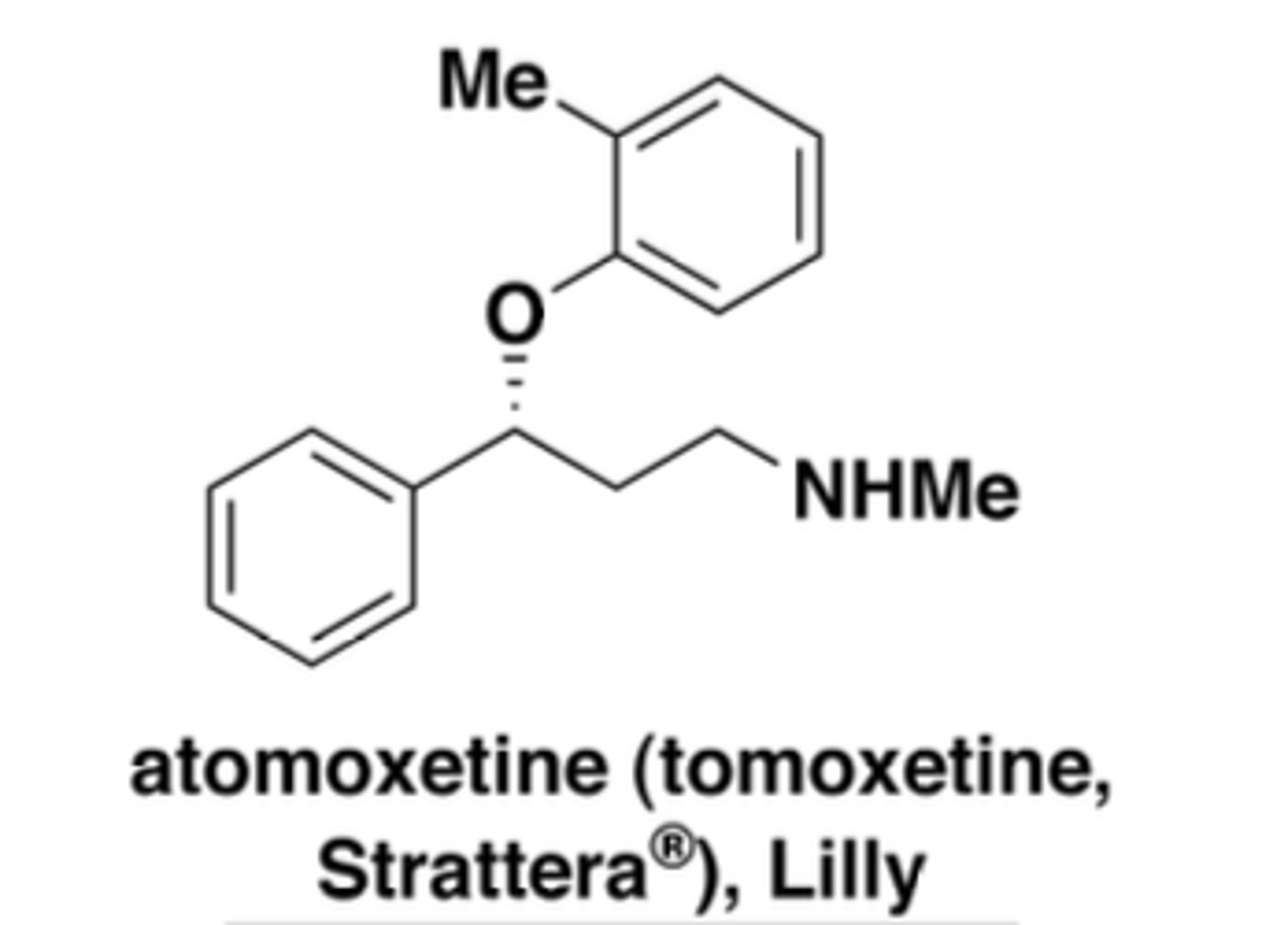
What are key atomoxetine side effects?
dyspepsia, N/V, fatigue, decreased appetite, mood swings, dizziness, sexual dysfunction
What enzyme metabolizes atomoxetine?
CYP2D6
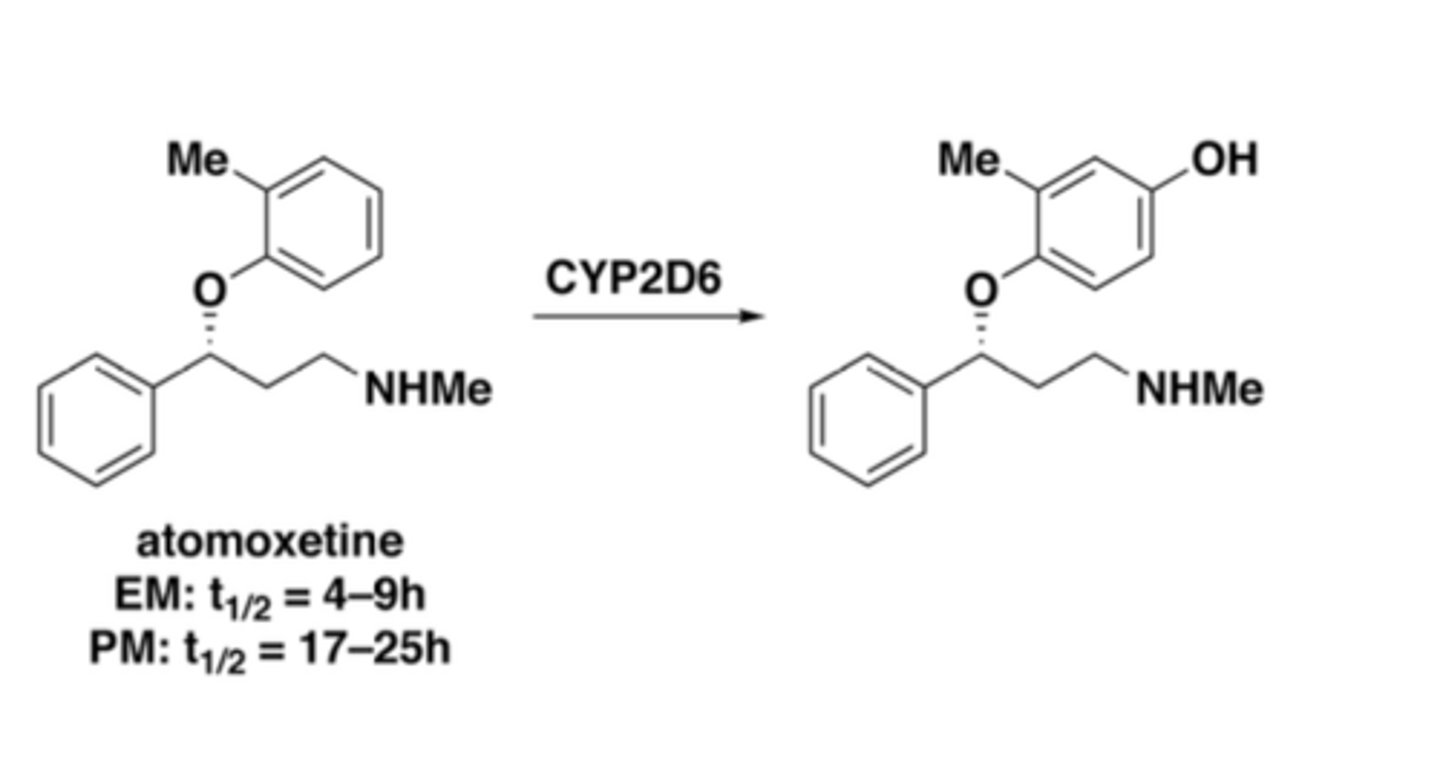
What is a SPARI?
serotonin reuptake inhibitor + 5-HT1A partial agonist
What is unique about vilazodone vs SSRIs?
fewer sexual side effects
How is vilazodone dosed?
titrated from 20 to 40mg to mitigate GI side effects
What is vilazodone used for?
major depressive disorder (or GAD, OCD)