`1.Anatomy and Flow in the Circulatory System
1/38
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
39 Terms
What does the cardiovascular system consist of?
heart, arteries/veins, blood
What is cardiovascular system cycle?
The right ventricle ejects the de-oxygenated blood via the pulmonary artery into the lung where the blood receives oxygen and is returned to the left atrium.
The blood then moves to the left ventricle and ejected into the ascending aorta.
The blood then travels to the lower body organs and upper body organs.
At the end of the arterial system at the organ-tissue level, the exchange of oxygen takes place.
The blood then begins its travel back to the right side of the heart carrying the de-oxygenated blood via the venous system and pooled in the upper and lower vena cava.
The blood then goes to the right atrium and from there to the right ventricle, where the blood cycle starts again.
What is the heart made up of?
The heart is a complex pump with 4 chambers, 2 of which are pumping (ventricles) and 2 are for pooling (atriums)
What is the heart wall composed of?
Myocardial tissue

Why is the heart wall arranged in a certain orientation?
Withstand tension along its length (long axis direction)
Withstand the twisting force
Withstand the pressure in the ventricular cavity
What do heart valves prevent?
backflow
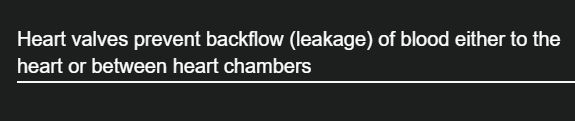
What happens on the left side of the heart?
The aortic valve: prevents blood returning to the left ventricle from the aorta
Bicuspid valve: prevents blood returning to the left atrium from the left ventricle
What happens on the right side of the heart?
Pulmonary valve and Tricuspid valve
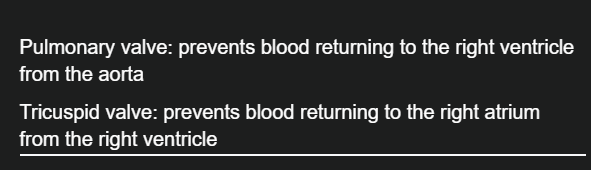
What are the atrioventricular valves?
Valves between the atria and ventricles

Heart Conduction System (the heart electric system)
It is the system by which the heart generates its electrical signals to initiate contraction (and hence ejection/pumping blood)
What are the main elements of the heart conduction system
Sinoatrial node, AV node, AV bundle, Purkinje fibers
Sinoatrial node
natural pacemaker of the heart

AV node
Mass of autorhythmic cells

AV bundle
Autorhythmic cells located in the interventricular septum; the only electrical connection between atria and ventricles (AV=atrioventricular); also known as bundle of His. This branches into right and left to deliver the signal to the right and left ventricles.
Purkinje fibers
specialized electrical conduction fibers in the heart.

What are the 5 main peaks in an ECG
The electrical signal generated by the SA node can be recorded on the skin; commonly known as the ECG
P wave: signals onset of atrial contraction
QRS complex: signals onset of ventricular contraction. Repolarization of atria simultaneously
T wave: repolarization of atria simultaneously
T wave: repolarization of ventricles; precedes ventricular relaxation
PQ interval: atria contract and begin to relax, ventricles begin to contract
QT interval: ventricles contract and begin to relax
ECG
electrocardiogram
What is the coronary circulation
a highly-complex branching system with hundreds/thousands of small scale arteries
What is the main function of the coronary circulation
To provide flow and nutrients to the myocardium and remove carbon dioxide and waste

What is stenosis
Blockage

Stroke Volume
Volume of blood ejected by the left/right ventricle into the aorta/pulmonary artery per beat
Heart Rate
The number of times the heart contracts and ejects blood into the aorta/pulmonary artery per minute
Cardiac Output
The volume of blood ejected from the left/right ventricle into the aorta/pulmonary artery per minute
How to calculate the cardiac output
CO=HR*SV
How to convert from mmHg to Pa
1mmHg=133.33Pa
What are the normal values of mmHg values for LV and RV
LV: 5mmHg-120mmHg
RV: 5mmHg-40mmHg
What is the arterial system
Highly complex branching system made of flexible vessels
What is the artery composed of
intima, media and adventitia
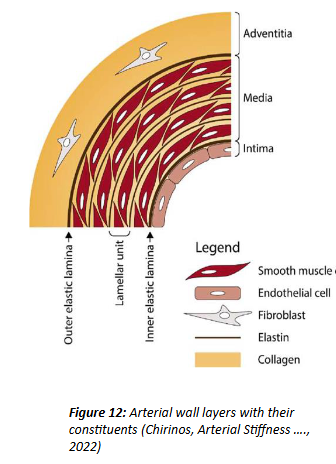
Intima
Innermost layer composed of endothelial cells

Media
Middle layer, composed of muscle cells, elastin, collagen, and proteoglycans.

Adventitia
Outer layer composed of fibroblasts.

What happens to arteries when they move from the heart
tapering

Mean arterial pressure (MAP)
an estimate of the maintained/sustained average load seen by the left ventricle

Diastolic pressure
known as the afterload and it is indeed what the left ventricles ‘sees/experiences’ at the onset of systole, when the aortic valve opens
MAP equation
MAP=Pd + (1/3) (PP)
PP equation
PP=Ps-Pd
What are normal values of Ps and Pd in healthy adults
120 and 80

Hypertensive
If Ps and Pd are >=90 and 130 mmHg
Hypotensive
Ps and Pd <90 and 60 mmHg