3.4.1 Mass transport in animals
1/123
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
124 Terms
Explain the formation of tissue fluid.
1. High hydrostatic pressure of blood at arterial end; (capillaries narrower than arterioles, and have small gaps in the walls. contraction of ventricles.)
2. Ultrafiltration: water / soluble molecules pass out
3. Plasma proteins / large molecules remain;
4. This lowers the Ψ (Ψ becomes more -ve);
5. WATER moves back into venous end of capillary (reject tissue fluid) by OSMOSIS;
6. Lymph system collects any excess tissue fluid which returns to blood
Explain the return of tissue fluid to the circulatory system.
At the venule end of capillaries:
1. Hydrostatic pressure reduces as fluid leaves capillary (also due to friction)
2. Tissue fluid is forced back into the capillaries by the higher hydrostatic pressure outside them, down the pressure gradient.
3. Plasma proteins and large molecules remain while most of liquid forced out capillary, Increasing conc, lowers Ψ in capillary below that of tissue fluid
4. Water enters capillaries from tissue fluid by osmosis, down a water potential gradient
5. The water being reabsorbed into the capillaries also contains dissolved waste metabolic products like carbon dioxide (from respiration) and urea which is taken away by the blood to be removed from the body.
6. Excess water taken up by lymph capillaries and returned to circulatory system through veins
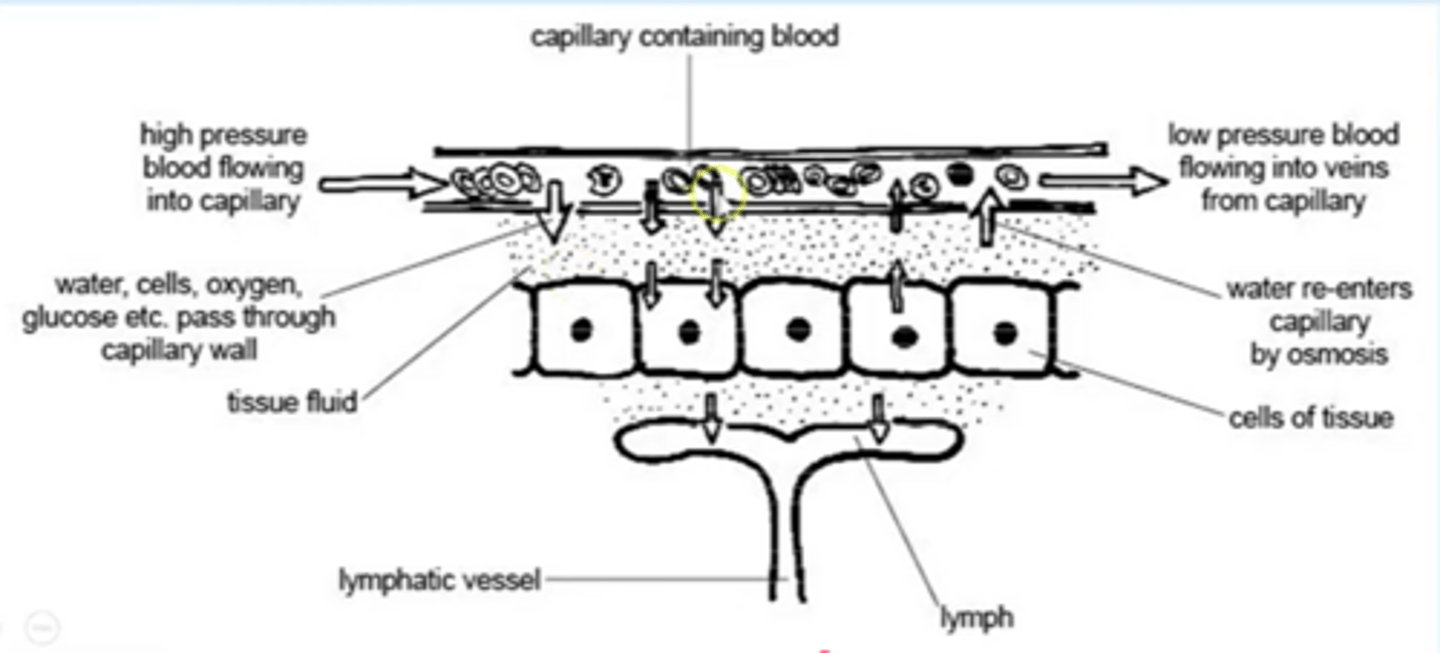
Explain the return of tissue fluid to the circulatory system (diagram)
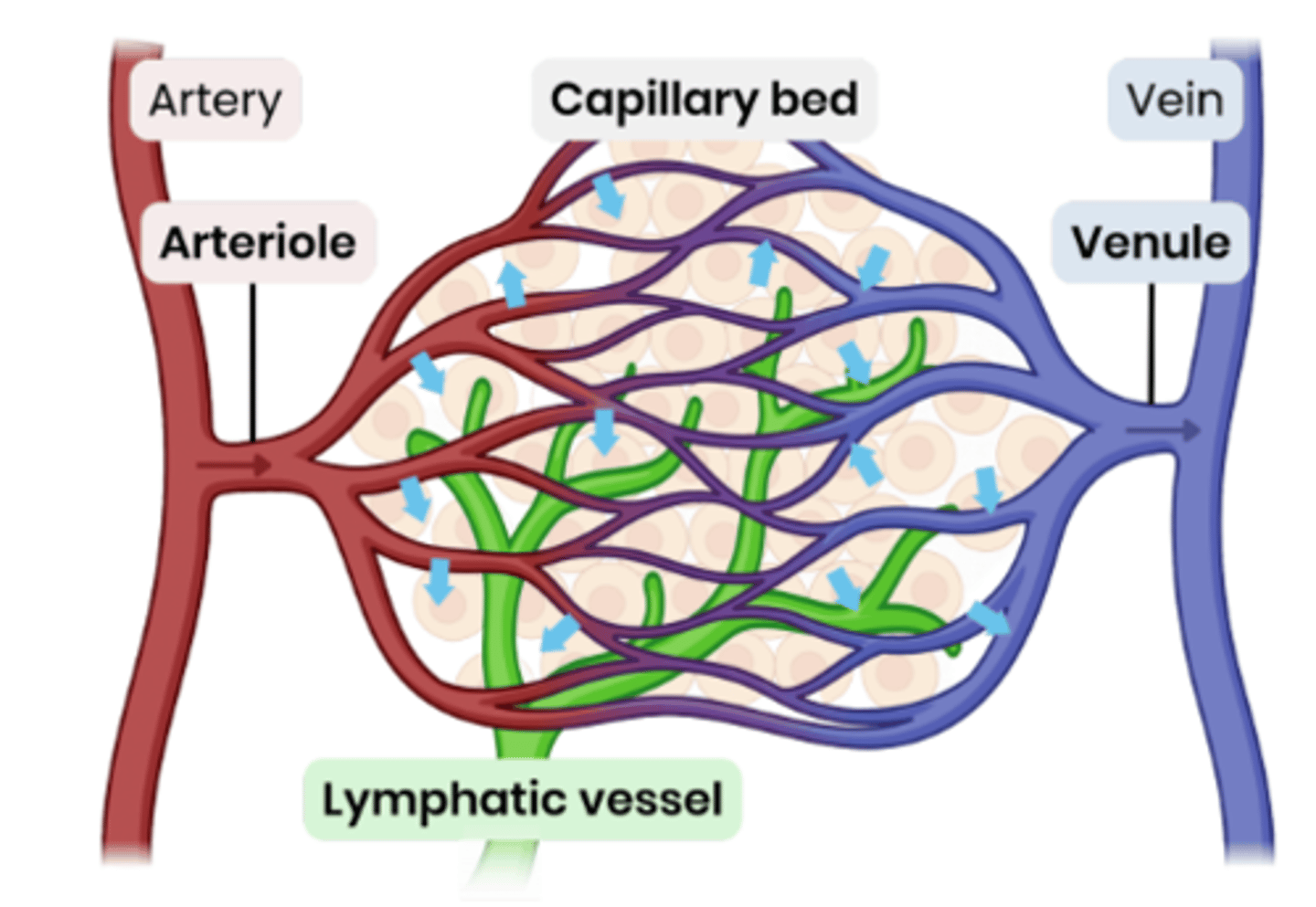
Describe the role of the lymphatic system in reabsorbing tissue fluid.
1. Equilibrium of water will be reached as water moves back into the capillary, so therefore not all of the tissue fluid is reabsorbed.
2. The excess tissue fluid is absorbed by the lymphatic system.
3. These vessels (resemble capillaries) drain their contents back into the bloodstream via 2 ducts that join veins close to the heart.
How are the contents of the lymphatic system moved?
- Hydrostatic pressure of the tissue fluid that has left the capillaries.
- Contraction of body muscles that squeeze the lymph vessels, valves in the lymph vessels ensure that the fluid inside them moves away from the tissues in the direction or the heart.
Suggest and explain causes of excess tissue fluid accumulation.
● Low concentration of protein in blood plasma
○ Ψ in capillary not as low → Ψ gradient is reduced
○ So more tissue fluid formed at arteriole end / less water absorbed at venule end by osmosis
○ Lymph system may not be able to drain excess fast enough
● High blood pressure (e.g. caused by high salt conc) → high hydrostatic pressure
○ Increases outward pressure from arteriole end AND reduces inward pressure at venule end
○ So more tissue fluid formed at arteriole end / less water absorbed at venule end by osmosis
○ Lymph system may not be able to drain excess fast enough
Elephantiasis is a disease in which parasitic worms occupy lymph vessels.
a) Suggest why this disease can cause severe swelling of the legs and feet.
b) Explain how these processes in the circulatory system may cause the swelling to reduce over time.
- Lymph vessels blocked
- So excess fluid cannot be absorbed
- So fluid accumulates / builds up
- Water potential gradient at venous end
- Tissue fluid/water moves back into capillary
- Via osmosis
Explain the role of the heart in the formation of tissue fluid.
1. Contraction of ventricles produces high blood / hydrostatic pressure;
2. (This) forces water (and some dissolved substances) out of blood capillaries;
In a healthy person, blood moves in one direction as it passes through the heart.
Give 2 ways in which this is achieved.
1. Pressure gradient / moves from high to low pressure;
2. Valves stop backflow;
S3 Explain how the structures of the walls of arteries and arterioles are related to their functions (5)
Elastic tissue
1. Elastic tissue stretches under pressure / when heart beats then recoils / springs back;
2. Evens out pressure / flow; Do not allow credit for expands / contracts / relaxes in this context.
3. Muscle contracts to reduce diameter of lumen /
4. Changes flow / pressure;
Epithelium
5. Epithelium smooth;
6. Reduces friction / blood clots / less resistance;
S3 Explain how the structures of the walls of arteries, veins and capillaries are related to their functions. (6)
Artery
1. Thickest wall, enabling it to carry blood at high pressure / withstand pressure surges;
2. Most elastic tissue, which smoothes out flow / maintains pressure;
3. Most muscle which maintains pressure;
4. Muscle in wall to control blood flow;
Vein
5. Thin wall does not have to withstand high pressure;
Capillary
6. Thin wall, allowing diffusion / exchange;
7. Only endothelium present, allowing short diffusion pathway;
All vessels
8. Have endothelium that reduces friction;
Suggest how widening of blood vessels can reduce ventricular blood pressure.
1. Larger lumen/volume of blood vessels;
2. Reduces blood pressure (in blood vessels);
3. Less friction/resistance (in blood vessels);
Explain how the heart muscle and the heart
valves maintain one-way flow of blood from the left atrium to the aorta. (cardiac cycle) (5)
1. Atrium has higher pressure than ventricle (due to filling contraction) causing atrioventricular valves to open; (Muscle / atrial / ventricular) contraction causes increase in pressure;
2. Ventricle has higher pressure than atrium (due to filling contraction) causing atrioventricular valves to close;
3. Ventricle has higher pressure than aorta causing semilunar valve to open;
4. Higher pressure in aorta than ventricle (as heart relaxes) causing semilunar valve to close;
Describe and explain 4 ways in which the structure of a capillary
adapts it for the exchange of substances between blood and the surrounding tissue. (4)
1. permeable capillary wall / membrane;
2. single cell thick, reduces diffusion distance;
3. flattened (endothelial) cells, reduces diffusion distance;
4. small diameter / narrow, gives a large SA:V / short diffusion distance;
5. narrow lumen, reduces flow rate giving more time for diffusion;
6. red blood cells in contact with wall / pass singly, gives short diffusion distance / more time for diffusion;
What is a risk factor? Give examples for cardiovascular disease.
● An aspect of a person's lifestyle or substances in a person's body / environment
● That have been shown to be linked to an increased rate of disease
● Examples - age, diet high in salt or saturated fat, smoking, lack of exercise, genes, high blood pressure, damaged artery walls
How do most cardiovascular diseases begin?
Atheroma formation: fatty material that builds up inside arteries, made of cholesterol and other substances that circulate in your blood.
Atheromas grow over time
Describe myocardial infarction.
A heart attack
1. The heart muscle is supplied with blood by the coronary arteries.
2. This blood contains the oxygen needed by heart muscle cells to carry out respiration.
3. If blocked, (e.g. by a blood clot) an area of the heart muscle will be totally cut off from its blood supply, receiving no oxygen.
- This causes a myocardial infarction - a heart attack.
- If large areas of the heart muscle are affected complete heart failure can occur, which is often fatal.
- Symptoms include pain in the chest and upper body, shortness of breath and sweating.
How does a poor diet which is high in cholesterol cause a myocardial infarction?
1. A diet high in saturated fat is associated with high blood cholesterol levels.
2. If the blood cholesterol level is high then the risk of cardiovascular disease is increased.
3. Cholesterol is one of the main constituents of the fatty deposits that form atheromas.
4. A diet high in salt also increases the risk because it increases the risk of high blood pressure which cause atheromas.
5. Atheromas can lead to increased blood pressure and blood clots, which could cause a myocardial infarction.
How can smoking lead to myocardial infarction?
1. Carbon monoxide combines with haemoglobin and reduces the amount of oxygen transported in the blood
2. Reduces the amount of oxygen available to tissues.
3. If the heart muscle doesn't receive enough oxygen it can lead to myocardial infarction.
How would you interpret data questions about cardiovascular disease?
Describe overall trend:
- Positive / negative correlation
- Linear / non linear
- Describe most obvious trend
- Anomalies
Manipulate data to support your statement
- Calculations
- Work out the difference from two points
- Work out how many times greater
- Work out percentage change
Evaluating study design
- Small sample size
- Take into account other risk factors (variable) that could have affected results
- Used similar groups e.g. age, gender
- Way in which info collected e.g. questionnaires may be unreliable as people lie or give inaccurate information
- Results reproduced by other scientist by carrying out more studies and collecting more results
Varicose veins are caused by valves becoming weak or damaged. Suggest why varicose veins often appear in legs and feet.
1. Far from heart (so pressure is low)
2. Blood must travel against gravity to reach the heart
3. Weak valves mean blood accumulates in veins/ travel backwards
What does an ECG show?
- Electrocardiogram, shows electrical activity of the heart.
- Each peak represents ventricular contraction
- Distance between peaks give time between heartbeats
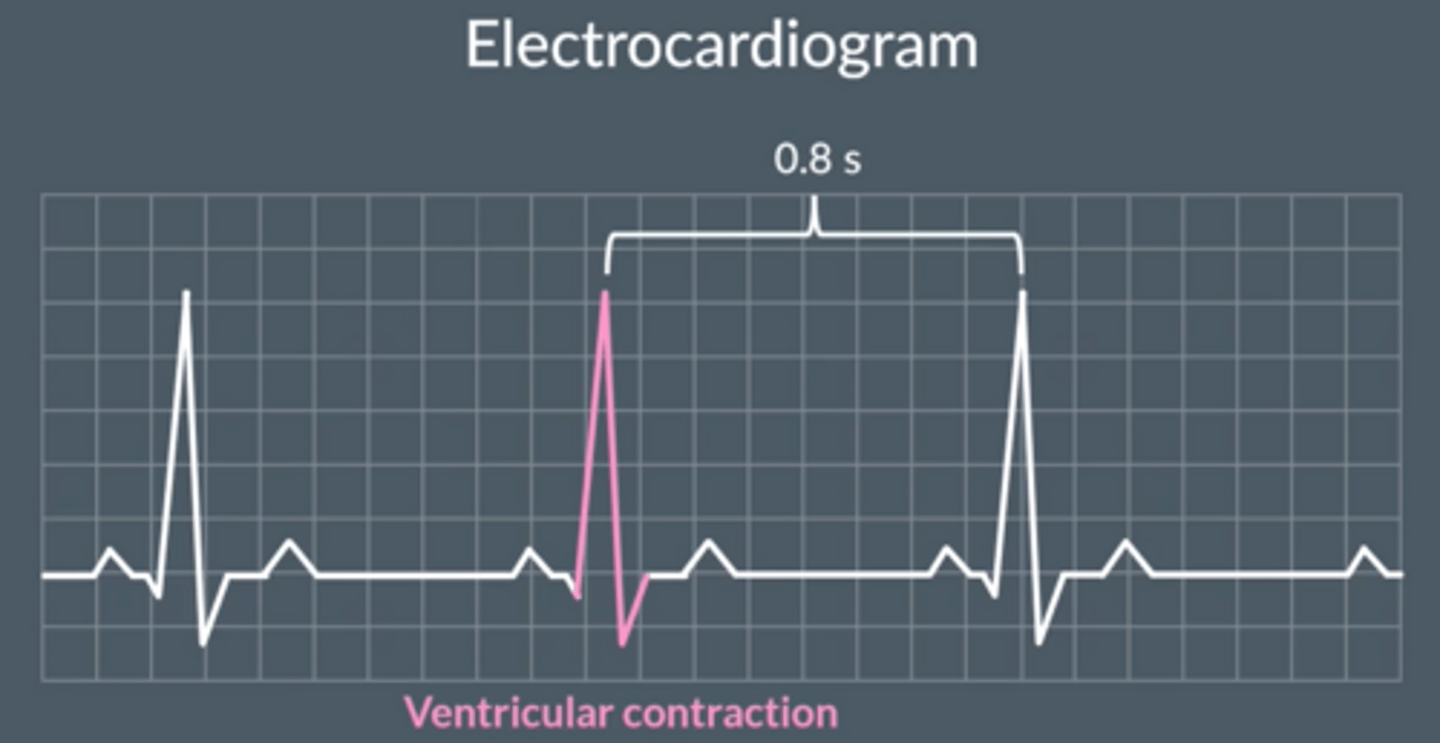
Describe the role of red blood cells & haemoglobin (Hb) in oxygen transport.
● Red blood cells contain lots of Hb.
○ No nucleus & biconcave → more space for Hb, high SA:V & short diffusion distance.
● Hb loads oxygen at gas exchange surfaces (lungs) where partial pressure of oxygen (pO₂) is high.
● This forms oxyhaemoglobin which transports oxygen.
○ Each can carry 4 oxygen molecule, one at each Haem group.
● Hb unloads oxygen near cells / tissues where pO₂ is low.
Give the words you can use for when haemoglobin ______ with oxygen
Hb associates with / loads oxygen
Associates / dissociates is best.
What does blood carry ?
Gases- O₂, CO₂
Nutrients- amino acids, lipids, ions
Hormones, antibodies
Waste products- urea
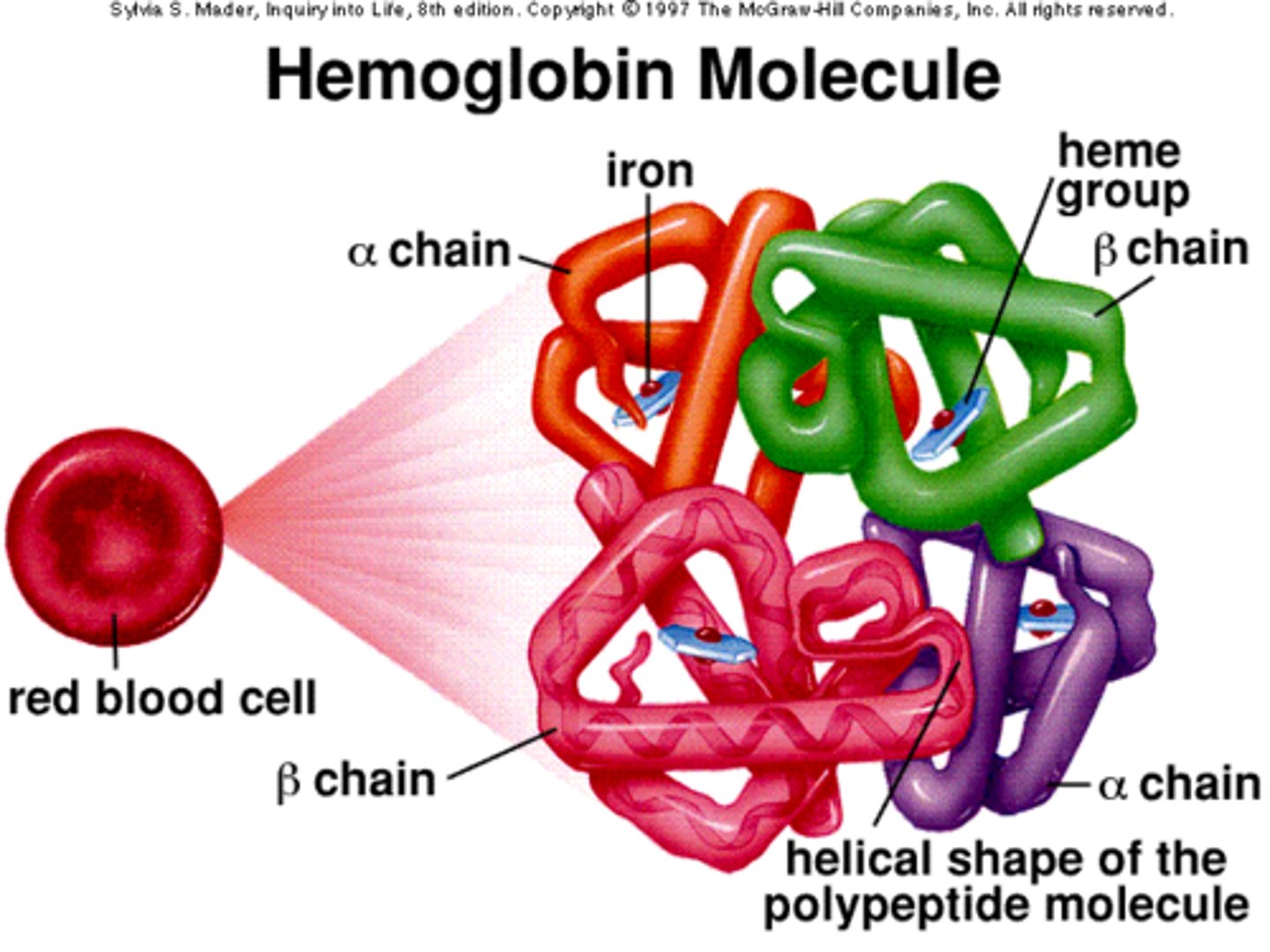
Describe the structure of haemoglobin.
● Protein with a quaternary structure
● Made of 4 polypeptide chains
● Each chain bonded to a Haem group containing an iron ion (Fe²⁺)
● Each Fe²⁺ can bind to 1 molecule of oxygen
The haemoglobins are a group of chemically similar molecules found in many different organisms
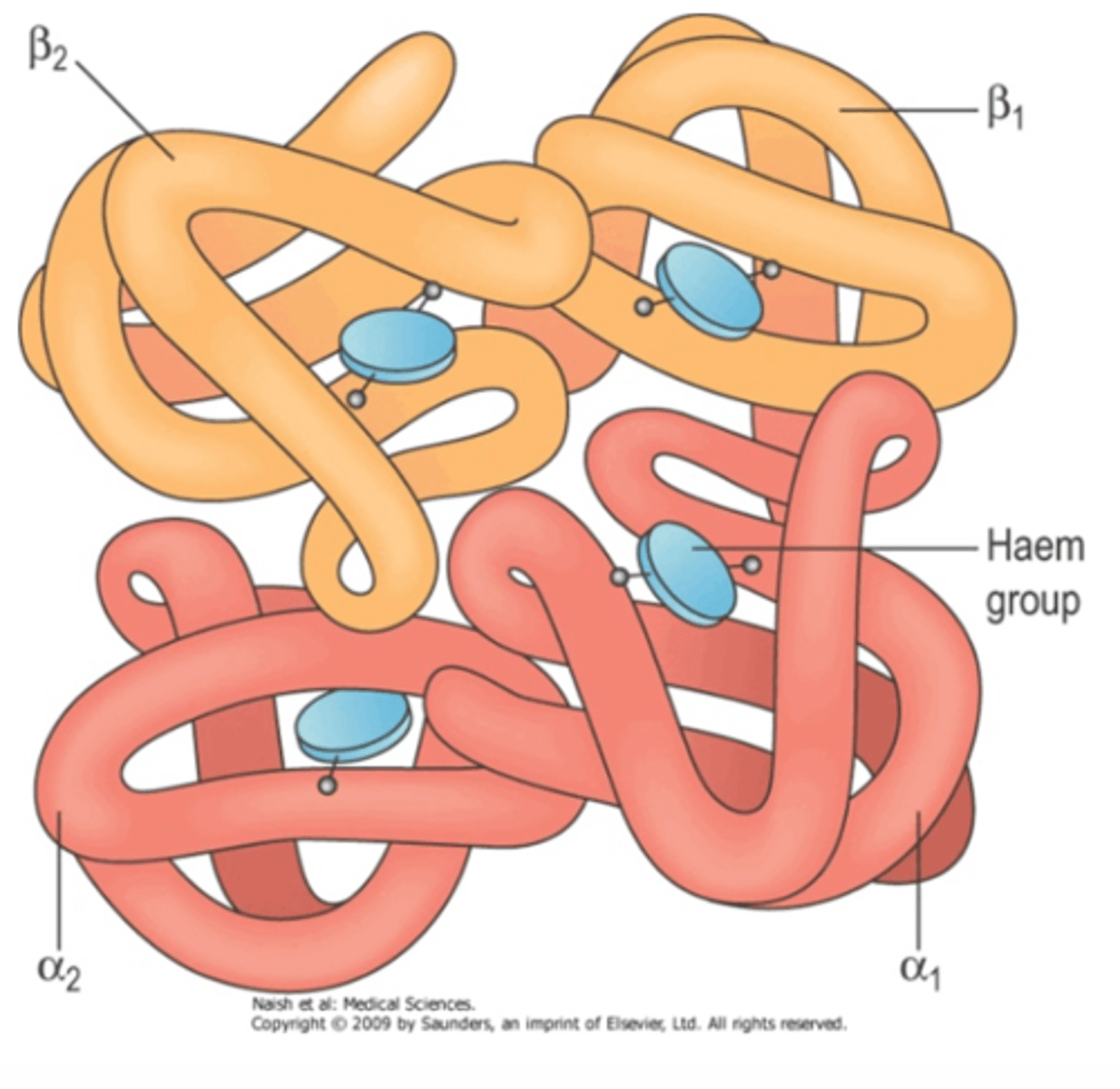
Why do some animals such as snails and octopuses have blue blood?
- Their haemoglobin have copper instead of iron.
- When copper binds to oxygen, it turns blue.
Haemoglobin diagram
What is meant by affinity?
The tendency a molecule has to bind with oxygen.
- Hb affinity for oxygen varies in the conditions it is in.
- As pO₂ increases, Hb's affinity for oxygen also increase.
Describe the loading, transport and unloading of oxygen in relation to the oxyhaemoglobin dissociation curve.
Areas with low pO₂ - respiring tissues
● Low oxygen conc so low pO₂ as respiring cells use up oxygen which lowers the pO₂
● Hb has a low affinity for oxygen
● So oxygen readily dissociates from Hb
● So low % saturation
Areas with high pO₂ - (lungs) gas exchange surfaces
● High oxygen conc so high pO₂ as oxygen enters blood capillaries at the alveoli in the lungs.
● Hb has a high affinity for oxygen
● So oxygen readily associates with Hb
● So high % saturation
Dissolved oxygen
Oxygen dissolved in blood plasma
Describe what is meant by loading
- Haemoglobin has a high affinity for oxygen at low pO₂ (respiring tissue)
- Positive cooperativity, so when 1 oxygen binds this uncovers further binding sites so a higher % saturation.
Oxyhaemoglobin dissociation curve
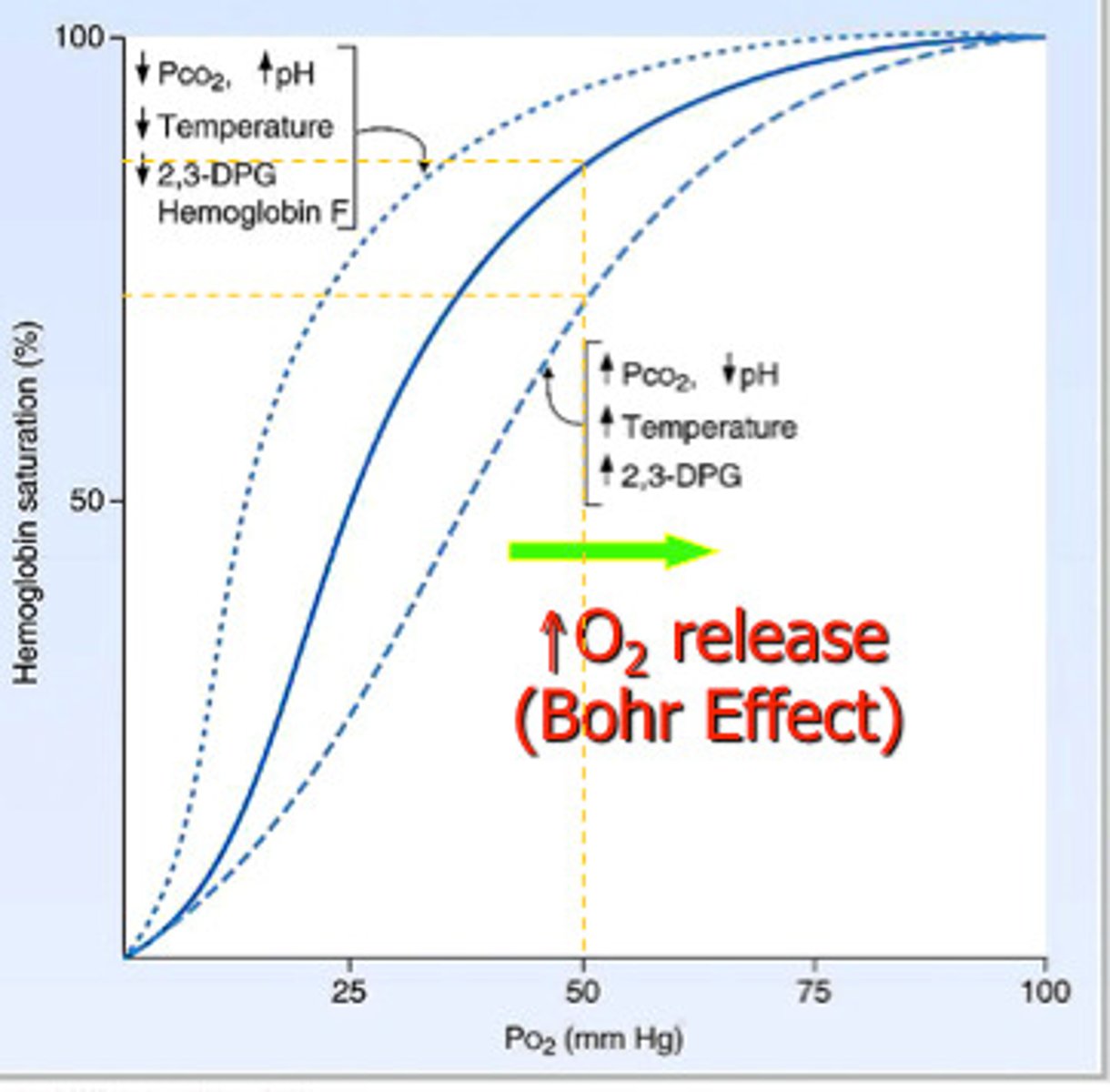
Explain positive cooperativity of oxygen binding.
(resulting in an S-shaped sigmoid oxyhaemoglobin dissociation curve)
1. Binding of first oxygen changes quaternary structure of haemoglobin
2. This uncovers Haem group binding sites, making further binding/unbinding of oxygens easier
Positive cooperativity can be for both oxygen association and dissociation
Positive cooperativity speeds up the transfer of oxygen from...
- Air in the alveoli to red blood cells (rapid oxygen association in the lungs)
- Red blood cells into aerobically respiring tissue (rapid oxygen dissociation in the respiring tissues)
Alveoli → red blood cells → aerobically respiring cells
(each arrow shows movement of oxygen)
How does oxygen enter red blood cells?
- There is a high pressure of oxygen in the lungs, and a low pressure of oxygen in the blood
- Oxygen moves from an area of high to low pressure, down pressure gradient
- Blood reaches tissue cells carrying out aerobic resp which has a low pressure of oxygen
- So oxygen dissociates from Hb, moves down the pressure gradient, to tissue cells
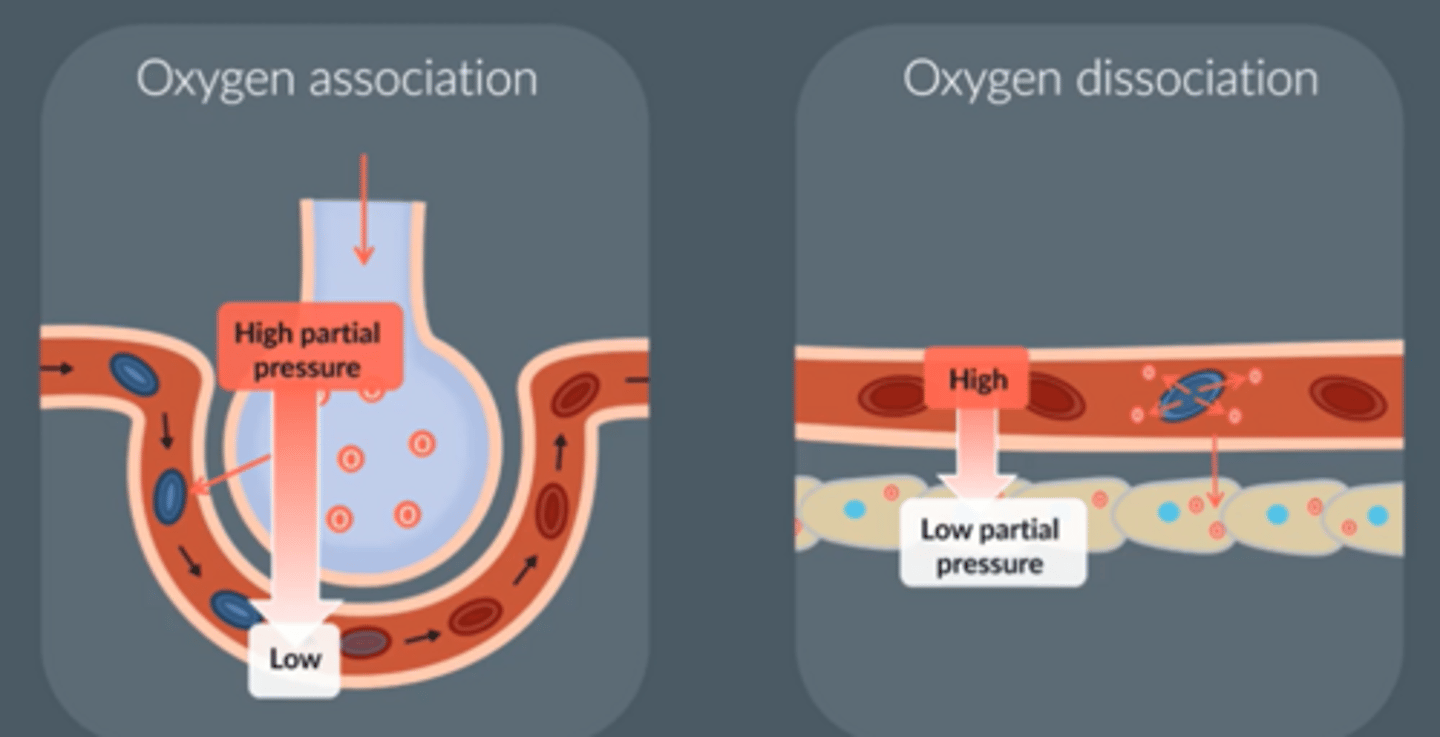
What is partial pressure (pO₂) of oxygen?
- Imagine a container has both CO₂ and O₂
- Total pressure of gas = 100 units
- O₂ contributes 60 units of this pressure
- 'Partial pressure of O₂' distinguishes this individual pressure from the overall pressure of the combined gases
What are the units of partial pressure?
Mainly kPa (kilopascals) as the values are quite high
May be mm Hg (millimetres of mercury)
What is 'percentage saturation of haemoglobin with oxygen?'
A measure of how many iron atoms in the haemoglobin molecules are bound to oxygen.
As the partial pressure of oxygen increases, the percentage saturation of haemoglobin with oxygen...
Increases.
What do we call the graph which shows % saturation of haemoglobin with oxygen against partial pressure?
Describe it's rough shape.
- Oxyhaemoglobin dissociation curve
- Gently curves up at start and end, rapidly goes up in middle
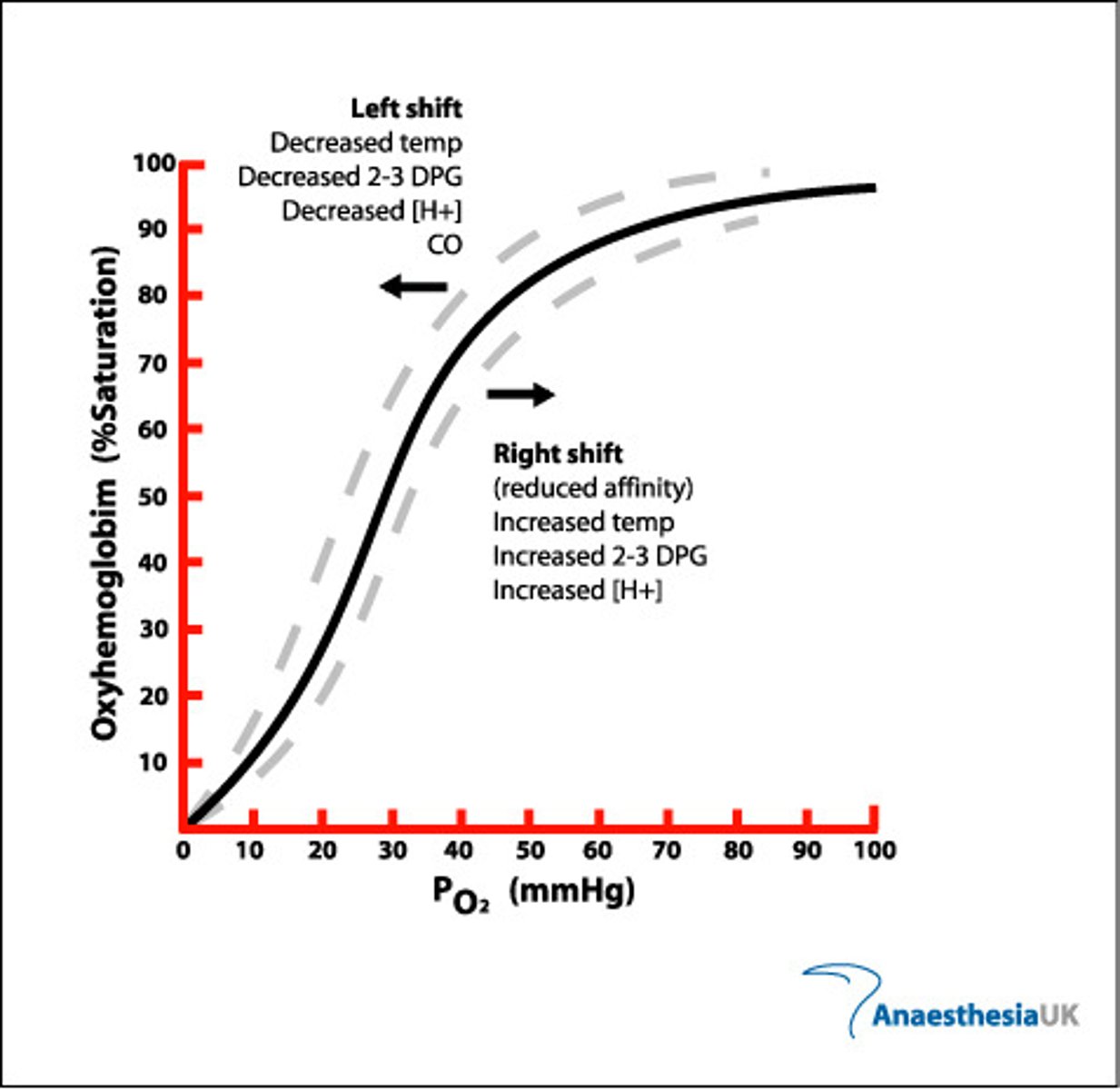
Describe evidence for the cooperative nature (positive cooperativity) of oxygen binding.
● At low pO₂, as oxygen increases there is slow increase in % saturation of Hb with oxygen.
○ When 1st oxygen is binding.
● At higher pO₂, as oxygen increases there is a big increase in % saturation of Hb with oxygen.
○ Showing it has got easier for oxygens to bind.
Suggest why the percentage saturation of haemoglobin with oxygen does not reach 100% in the lungs.
- The probability of a collision between an unbound iron atom and an oxygen molecule is low.
- Most iron atoms are already bound to oxygen molecules.
Give the mneumonic to remember what happens when the curve shifts left and right.
Low oxygen - Lefty Likey Loady
Righty Rapid Respiration
What is the Bohr effect?
Effect of CO₂ concentration on dissociation of oxyhaemoglobin → curve shifts to right.
Summarise the effect CO₂ concentration on the curve.
- As the CO₂ concentration decreases, the curve shifts to the left
- O₂ associates more readily, dissociates less readily
- As the CO₂ concentration increases, the curve shifts to the right
- O₂ associates less readily, dissociates more readily
Explain effect of CO₂ concentration on the dissociation of oxyhaemoglobin.
1. Increasing blood CO₂ e.g. due to increased rate of respiration
2. Lowers blood pH (more acidic)
3. Reducing Hb's affinity for oxygen as shape / quaternary structure changes slightly
4. So faster unloading /dissociation of oxygen to respiring cells at a given pO₂
5. Curve shifts right
Explain effect of CO₂ concentration on the dissociation of oxyhaemoglobin (graph)
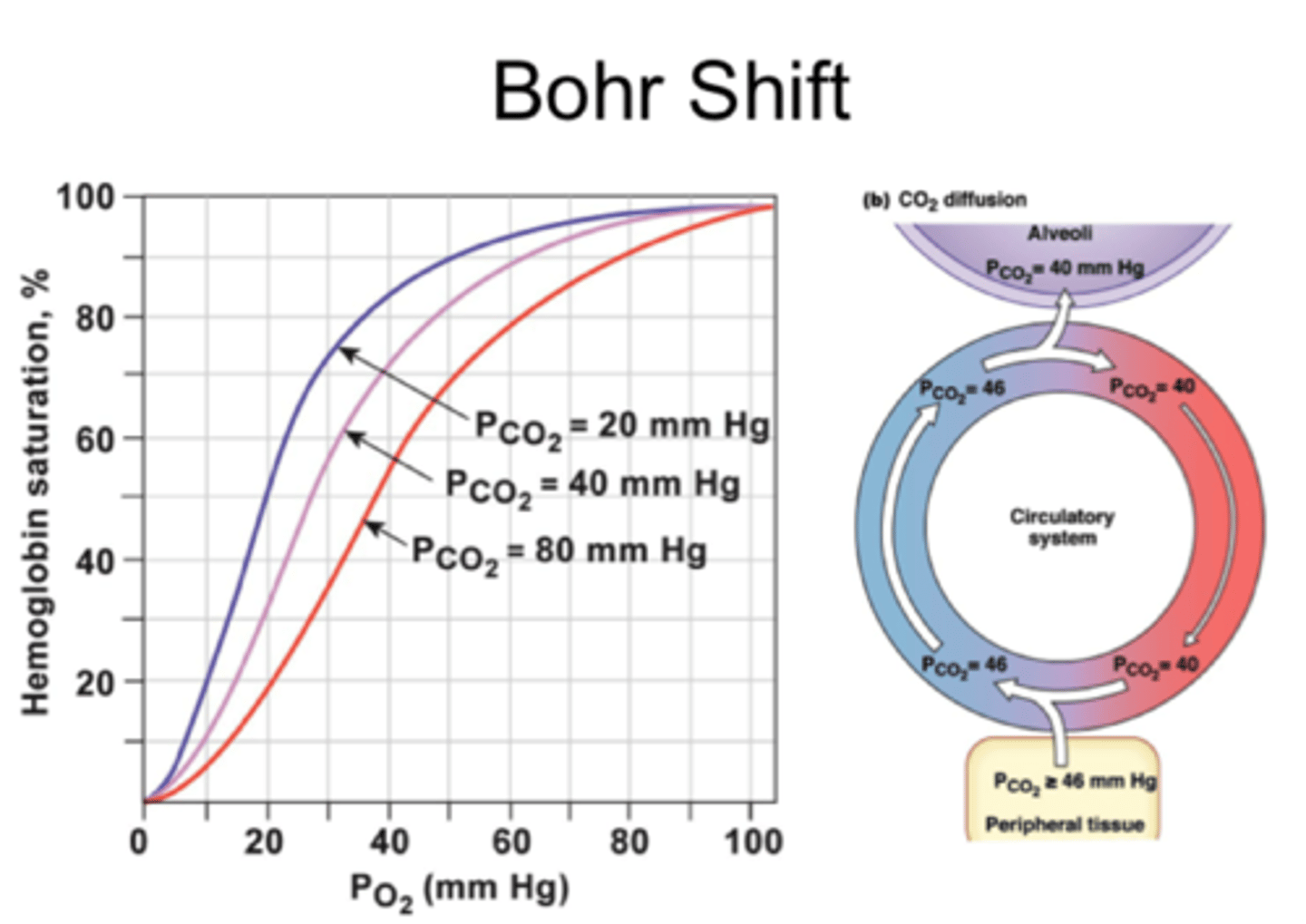
Explain the advantage of the Bohr effect (e.g. during exercise)
More dissociation of oxygen → faster aerobic respiration / less anaerobic respiration → more ATP produced
Hyperventilation occurs when a person breathes too quickly, and exhales more carbon dioxide than usual.
Predict the effect of hyperventilation on the oxyhaemoglobin dissociation curve.
- Shifts to the left, as the blood becomes less acidic as CO₂ is exhaled
- So haemoglobin binds more readily with oxygen and releases it less readily
- Tissues receive less oxygen for respiration → dizziness, fainting
Anaemia is a condition in which the concentration of haemoglobin in the blood is reduced.
The table below shows data for the average percentage saturation of haemoglobin with oxygen in healthy people and people with anaemia.
(Table shows: People with anaemia have a lower % saturation of Hb at every measured PO₂ of oxygen)
Explain the advantage of the changes seen in the haemoglobin of people with anaemia.
- At every measured partial pressure of oxygen, the % saturation is lower in people with anaemia.
- Oxyhaemoglobin dissociation curve shifts to the right.
- So Hb releases oxygen more readily in the tissues for respiration.
- Allows the body to meet its energy demands despite having less haemoglobin in the blood.
Emperor penguins can stay submerged underwater for up to 27 minutes.
Suggest why penguin haemoglobin has a higher affinity for oxygen than human haemoglobin.
- To maximise the absorption of oxygen from the lungs while above water
- This oxygen will sustain its tissues while the penguin is submerged underwater, where it cannot breathe.
What do we mean by haemoglobin's affinity for oxygen?
- For a lower CO₂ concentration, oxygen associates more readily and dissociates less readily
- The haemoglobin has a HIGHER affinity for oxygen
When does haemoglobin have the highest affinity for oxygen?
- At low CO₂ concentrations.
- in blood passing away from the lungs.
- At higher pH's
Explain why different types of haemoglobin can have different oxygen transport properties.
● Different types of Hb are made of polypeptide chains with slightly different amino acid sequences
● Resulting in different tertiary / quaternary structures / shape
● So they have different affinities for oxygen
Explain how organisms can be adapted to their environment by having different types of haemoglobin with different oxygen transport properties.
Curve shift left → Hb has higher affinity for O₂
● More O₂ associates with Hb more readily
● At gas exchange surfaces where pO₂ is lower
● E.g. organisms in low O₂ environments - high
altitudes, underground, or foetuses
Curve shift right → Hb has lower affinity for O₂
● More O₂ dissociates from Hb more readily
● At respiring tissues where more O₂ is needed
● E.g. organisms with high rates of respiration /
metabolic rate (may be small or active)
What 4 factors may affect the shape of oxyhaemoglobin dissociation curves?
- OXYGEN CONC: higher = more oxygen transported by Hb
- ALTITUDE: higher = air pressure & oxygen conc decreases, harder for Hb to transport oxygen.
- TEMPERATURE: higher = increases solubility of oxygen in blood, easier for Hb to transport oxygen.
- ACIDITY: higher = more dissociation
Explain the shape of the oxyhaemoglobin dissociation curve for organisms with high activity levels.
- High oxygen demand, so have haemoglobin with a lower affinity for oxygen than human haemoglobin.
- As they need their haemoglobin to easily dissociate oxygen, so it's available to use.
- Dissociation curve of their haemoglobin is to the right of the human one.
What does it mean if the curve is further to the left? Further to the right?
LEFT: greater affinity of Hb for oxygen (readily associates with oxygen, dissociates less readily).
RIGHT: lower affinity of Hb for oxygen (associates with oxygen less readily but readily dissociates).
Explain the shape of the oxyhaemoglobin dissociation curve for a mouse.
- Small mammals= higher SA:V ratio than larger mammals.
- So lose heat quickly, so have a high metabolic rate to help them keep warm.
- So have a high oxygen demand.
- So have Hb with a lower affinity for oxygen than human Hb.
- Hb must easily unload oxygen to meet their high oxygen demand.
- Dissociation curve to the right of human one.
Explain the shape of the oxyhaemoglobin dissociation curve for organisms living at high altitudes/underground.
- Lower pO₂ at higher altitudes & underground.
- Low concentration of oxygen, so Hb with a higher affinity for oxygen than human Hb.
- Beneficial: can obtain enough oxygen saturation in their blood when pO₂ in the air is low.
- Dissociation curve LEFT of ours, higher affinity, higher saturation at any pO₂
How can animals adapt to living in different environments?
- By possessing different types of Hb with different oxygen transport properties.
- Structure of Hb coded for by DNA.
- Mutation could change the shape of Hb, beneficial for the animal, allele will increase in the population by natural selection.
- Also mutations which can cause harm i.e sickle cell anaemia:
- A genetic disorder that causes abnormal Hb, resulting in some red blood cells assuming an abnormal sickle shape and cannot carry as much oxygen
Describe foetal haemoglobin (fHb), and it's effect on the oxyhaemoglobin dissociation curve.
- Has a higher affinity for oxygen than adult Hb.
- Vital: allows foetus to obtain oxygen from its mother's blood at the placenta. Can't inhale/exhale, mother's Hb the only oxygen source.
- fHb can bind to oxygen at low PO₂.
- At this low PO₂, the mother's Hb is *dissociating* with *oxygen.*
- Dissociation curve graph: curve for fHb shifts to LEFT of that for adult Hb
- So at any given PO₂, fHb has a higher % saturation than adult Hb
- After birth, baby begins to produce adult Hb which gradually replaces fHb → easy release of oxygen in the respiring tissues of a more metabolically active individual
Myoglobin
A protein in muscle cells that stores oxygen for cellular respiration, 1 polypeptide chain which holds oxygen at low PO₂
What is myoglobin?
- A single polypeptide chain in a tertiary structure
- Only 1 oxygen binding site, so fully saturated after one oxygen molecule has bound to it.
- Higher affinity for oxygen than Hb, as Mg has a simpler job: only has to store and release oxygen to the muscles (not carry or release oxygen at right places)
People with sickle cell anaemia exhibit symptoms such as fatigue, dizziness, and a fast heart rate.
Sickle cell anaemia is a red blood cell disorder in which there are not enough red blood cells to transport oxygen around the body.
It is caused by a mutation that changes the structure of haemoglobin.
i) Explain why sickle cell anaemia may lead to these particular symptoms
ii) A doctor advises that patients with sickle cell anaemia should avoid activists at high altitudes like skiing. Why?
i) - Hb's quaternary structure altered so different shape
- Sickle cells cannot transport oxygen as efficiently as normal red blood cells due to their shape
- Sickle cells block narrow blood vessels
- Less oxygen dissociates at respiring tissues
- Less aerobic resp so less ATP produced
ii) - Lack of oxygen at high altitudes
- Sickle cells cannot transport anaemia patients have a low affinity for oxygen
Describe the general pattern of blood circulation in a mammal.
Closed double circulatory system - blood passes through heart twice for every circuit around body:
1. Deoxygenated blood in right side of heart pumped to lungs; oxygenated returns to left side
2. Oxygenated blood in left side of heart pumped to rest of body; deoxygenated returns to right
Acronym LORD
Left oxygenated
Right deoxygenated
Suggest the importance of a double circulatory system.
● Prevents mixing of oxygenated / deoxygenated blood
○ So blood pumped to body is fully saturated with oxygen for aerobic respiration
● Blood can be pumped to body at a higher pressure (after being lower from lungs)
○ Substances taken to / removed from body cells quicker
Describe the role of blood.
- Transports respiratory gases, products of digestion, metabolic wastes and hormones around the body.
- Blood always flows from a higher pressure to a lower pressure in the circulatory system.
Which blood vessel carries the lowest pressure blood ?
- The vena cava
- The final blood vessel that takes the blood back to the heart from the body, so has the lowest pressure.
Why do large organisms need a circulatory system?
SA:V ratio too small to rely on diffusion to get oxygen/glucose to all parts of the organism quickly enough
Draw a diagram to show the general pattern of blood circulation in a mammal, including the names of key blood vessels.
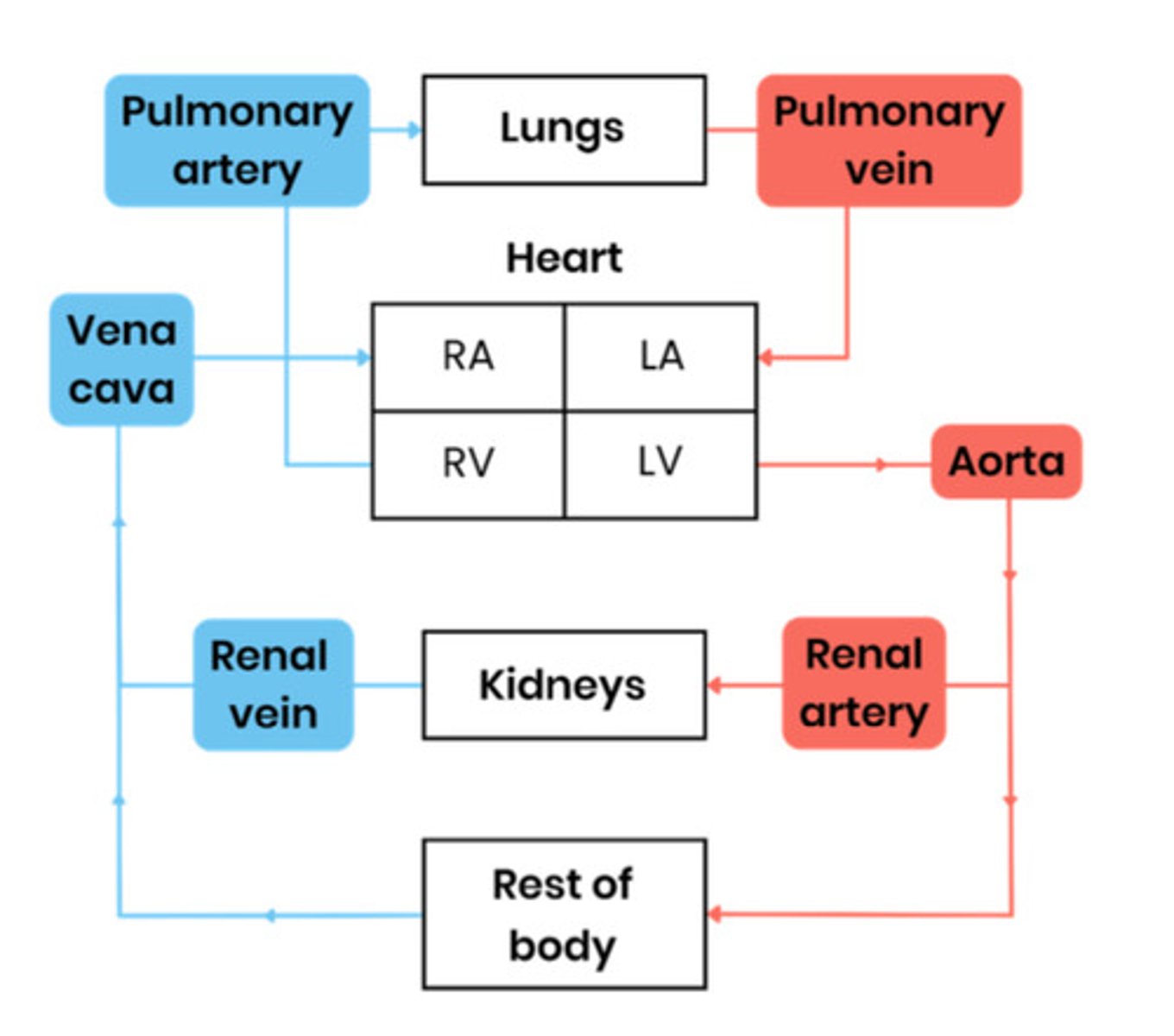
Name the blood vessels entering and leaving the heart and lungs.

Name the blood vessels entering and leaving the kidneys
● Renal arteries - ARRIVES. oxygenated blood, heart → kidneys
● Renal veins - LEAVES. deoxygenated blood, kidneys → vena cava
Name the blood vessels that carry oxygenated blood to the heart muscle.
Coronary arteries - located on surface of the heart, branching from aorta.
What can happen if there is a blockage of the coronary arteries?
- e.g. a blood clot, leads to myocardial infarction (heart attack),
- because an area of the heart muscle is deprived of blood, so also no oxygen.
- The muscle cells in this region are unable to respire (aerobically) and so die.
Label a diagram to show the gross structure of the human heart (inside)
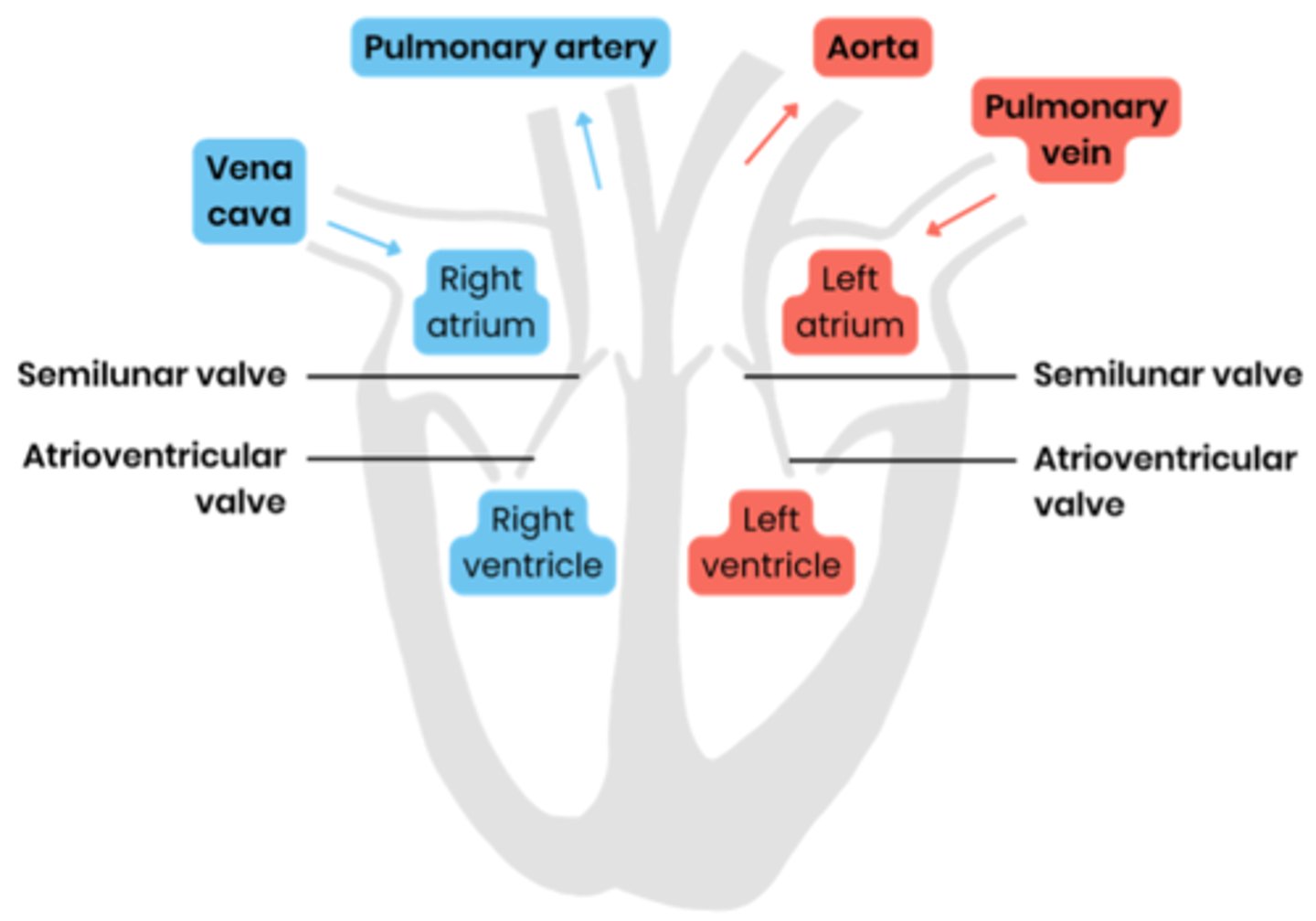
Suggest why the wall of the left ventricle is thicker than that of the right.
● Thicker muscle to contract with greater force
● To generate higher pressure to pump blood around entire body (rather than to lungs)
Describe the route of oxygenated blood through the body from the lungs to the kidneys.
1. Pulmonary vein
2. Left atrium
3. Left ventricle
4. Aorta
5. Renal artery
What is the correct order of structures that blood passes through on the right side of the heart?
Right atrium, atrioventricular valve, right ventricle, semi-lunar valve
What is the cardiac cycle?
The sequence of events that occurs during ONE COMPLETE heartbeat.
Summarise the cardiac cycle in very simple terms.
1. Blood enters the atria
2. The atria contract
3. The ventricles contract
Give the 2 phases of the cardiac cycle.
1. Systole (contraction) - occurs separately in the ventricles and the atria and is therefore described in 2 stages.
2. Diastole (relaxation) - For some of the time, relaxation takes place simultaneously in all chambers of the heart and is therefore treated as a single phase.
Where are the atrioventricular (AV) and semilunar (SL) valves located?
AV- Between atria and ventricles
Semilunar- Between blood vessels and ventricles
Give the order of the cardiac cycle. (may not start this way but order is same)
DAV
Diastole
Atrial systole
Ventricular systole
How to remember describing the cardiac cycle
Contract
Pressure
Valves
Flow
Cats Pee Very Fast
Explain the pressure & volume changes and associated valve movements during the cardiac cycle that maintain a unidirectional flow of blood.
c) Diastole
● Blood returns to heart via vena cava and pulmonary vein.
● Atria & ventricles relax
● So their volume increases, pressure decreases
● SL shut when pressure in arteries exceeds pressure in ventricles
● AV valves open when pressure in atria exceeds pressure in ventricles
● So blood fills atria via veins & flows passively to ventricles
Explain the pressure & volume changes and associated valve movements during the cardiac cycle that maintain a unidirectional flow of blood.
a) Atrial systole
● Atria contract
● So their volume decreases, pressure increases
● AV valves open when pressure in atria
exceeds pressure in ventricles
● Sl valves remain shut as pressure in arteries exceeds pressure in ventricles
● So blood pushed into ventricles, down pressure gradient
Explain the pressure & volume changes and associated valve movements during the cardiac cycle that maintain a unidirectional flow of blood.
b) Ventricular systole
● Ventricles contract
● So their volume decreases, pressure increases
● AV valves shut when pressure in ventricles exceeds pressure in atria (prevent backflow)
● SL valves open when pressure in ventricles exceeds pressure in arteries
● So blood pushed out of heart through arteries, down pressure gradient
What prevents blood being forced back into the atria during ventricular systole?
The atrioventricular (AV) valves close.
When do the AV valves and semilunar valves open/close ?
Open when pressure is higher behind the valve
Close when pressure is higher in front of the valve
Explain how graphs showing pressure or volume changes during the cardiac cycle can be interpreted, eg. to identify when valves are open / closed
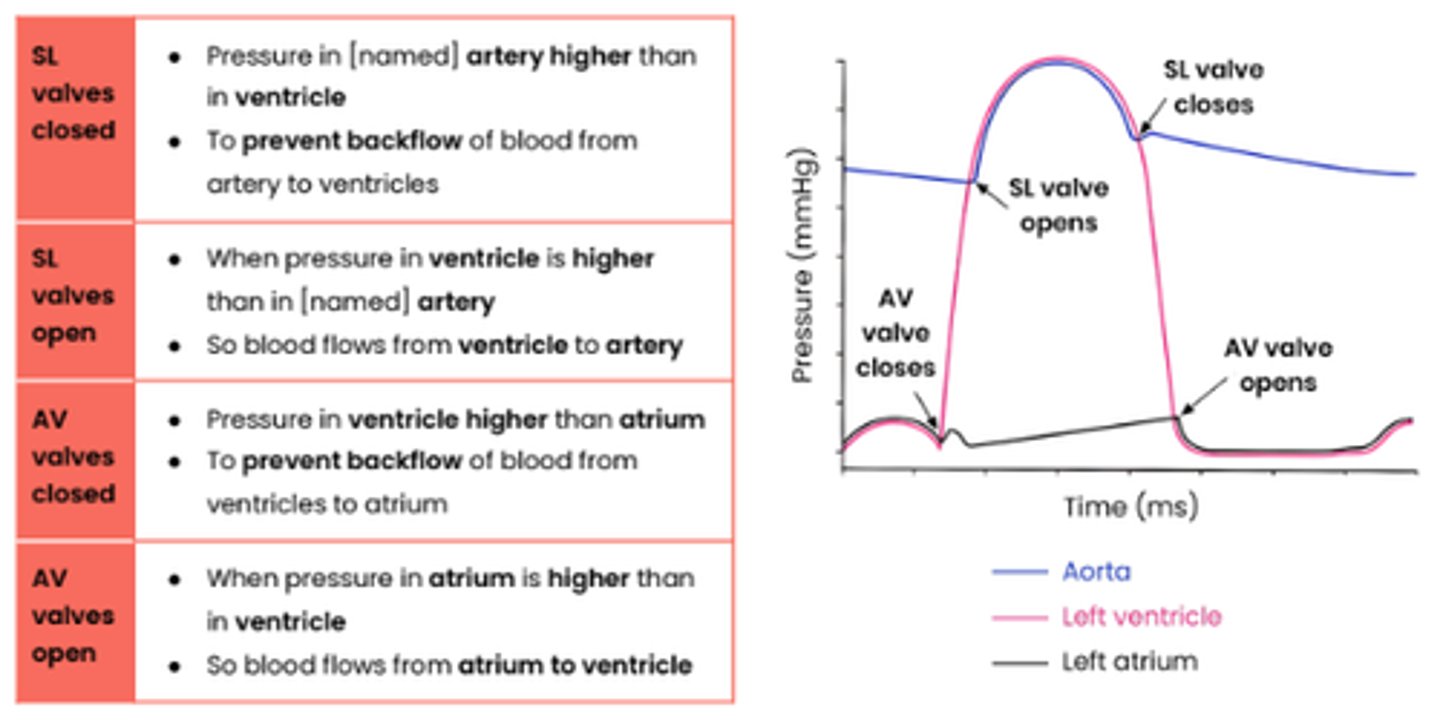
How can heart rate be calculated from cardiac cycle data?
Heart rate (beats per minute) = 60 (seconds) / length of one cardiac cycle (seconds)
What is cardiac output?
Volume of blood pumped by one ventricle of the heart in 1 minute.
What is the equation for cardiac output?
Cardiac output (cm³/min) = stroke volume (cm³) x heart rate (bpm)
What is stroke volume?
Volume of blood pumped by one ventricle of the heart in one contraction.
What is heart rate?
Number of beats per minute
Sprinter A is warming up for his first ever race. During his warm up, his heart rate and breathing rate increase. Sprinter B, who has been competing for several years, is also warming up.
i) Explain what will happen to Sprinter A's cardiac output as he warms up. [2]
ii) Describe and explain why Sprinter B has a greater cardiac output than Sprinter A, even though their heart rates are the same. [2]
i) • Cardiac output increases;
• To match metabolic demands of cells.
ii) • Sprinter B has thicker and stronger ventricular muscles in his heart;
• So stroke volume increases (and thus cardiac output).