HBS 11 + 12
1/47
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
48 Terms
Urinary system role
• Filter and eliminate waste (blood is constantly filtered by kidneys)
• Maintain homeostasis
• Contributes to acid-base balance
kidneys: what is it, where is it
major excretory organ
in retroperitoneal location: under the muscles of back and behind parietal pleura
surrounded by heavy cushion of fat to keep in place
receive highest percent of total body blood flow per min
ureters
transport urine from kidneys to bladder
urinary bladder
temporary storage reservoir for urine
urethra
transports urine out of the body
rugae
folds in transitional epithelium
trigone
smooth muscle region of bladder, when stretched, bladder signals to brain it is time to empty
kidney function
regulated overall fluid volume in the body via urine formation
excrete waste and regulate concentration of many substances in blood
regulate blood pressure
secretes EPO to stimulate erythrocyte formation
also an endocrine organ by secreting aldosterone (blood pressure regulation) and sex hormones
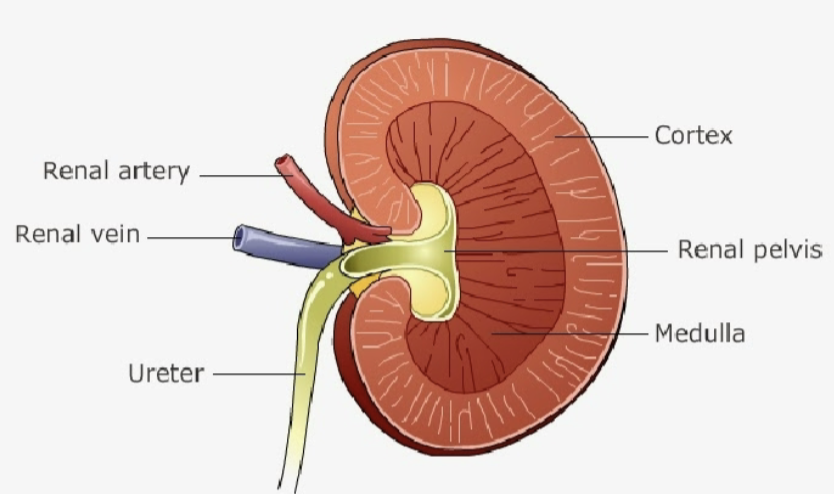
kidney structure (macro level)
cortex
medulla
hilium: renal pelvis)
nephron functions
produces urine
1) filtration: filter water and dissolved substances from blood
2) reabsorption: recover most of the filtrate from tubules and return it to blood
3) secretion: moving substances from blood into tubule
excretion of substance= filtration - reabsorption + secretion
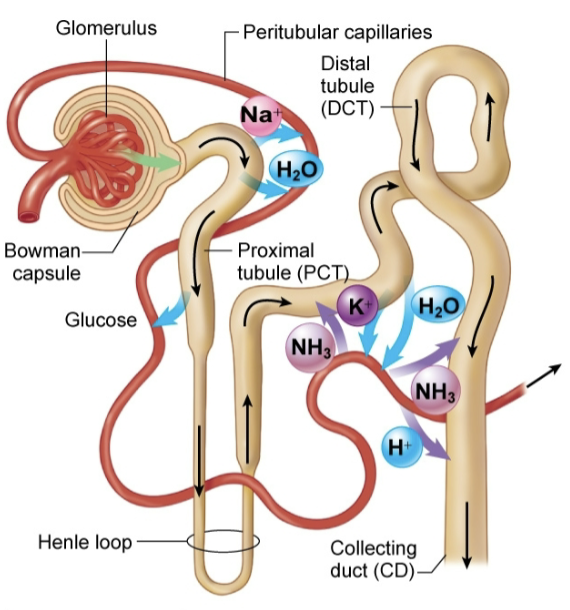
How nephron works
glomerulus: filtration
proximal tubule: reabsorb 65% of filtrate
loop of henle: reabsorb 25% of filtrate
distal tubules: reabsorb 5% of filtrate, secrete
collecting ducts: reabsorb 5% of filtrate, secrete
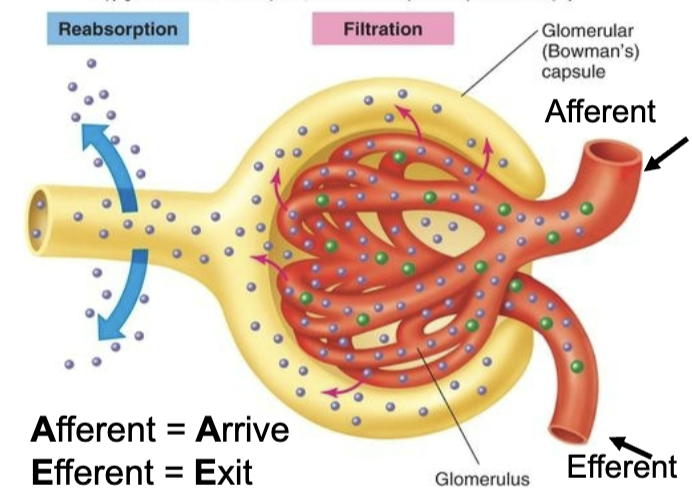
Filtration
Glomerulus: network of capillaries surrounded by Bowman Capsule
blood enters and filtered from afferent arteriole
blood leaves via efferent arteriole
only small stuff gets filtered
Reabsorption
movement of substances out of the renal tubule and back to the blood
Most solutes are reabsorbed in the proximal tubule
additional ions and water reabsorbed later in Loop of Henle, distal tubule and collecting duct
Secretion
Secretion is the process of moving substances from the blood into the tubules
• Sometimes substances that were reabsorbed earlier in the nephron are secreted back into the tubules later
• Secretion also serves as a way to clear the blood of drugs or excess ions
• Nitrogenous waste (urea) and drugs are secreted into the lumen of the kidney (forming urine) in the proximal tubule
• Ammonia, Potassium, Hydrogen, and some drugs are secreted in the distal tubule and collecting duct
What is reabsorbed+ secreted in each part of the nephron
glucose, amino acids, and protein: ~99-100% reabsorbed in proximal tubule
urea: ~50% reabsorbed in proximal tubule, secreted back in loop of henle, reabsorbed again in collecting ducts (secretion due to regulating urine concentration)
sodium and water: most sodium and water reabsorbed in proximal tubule, then reabsorbed at lower rates later on, but if high water intake, some secretion of water
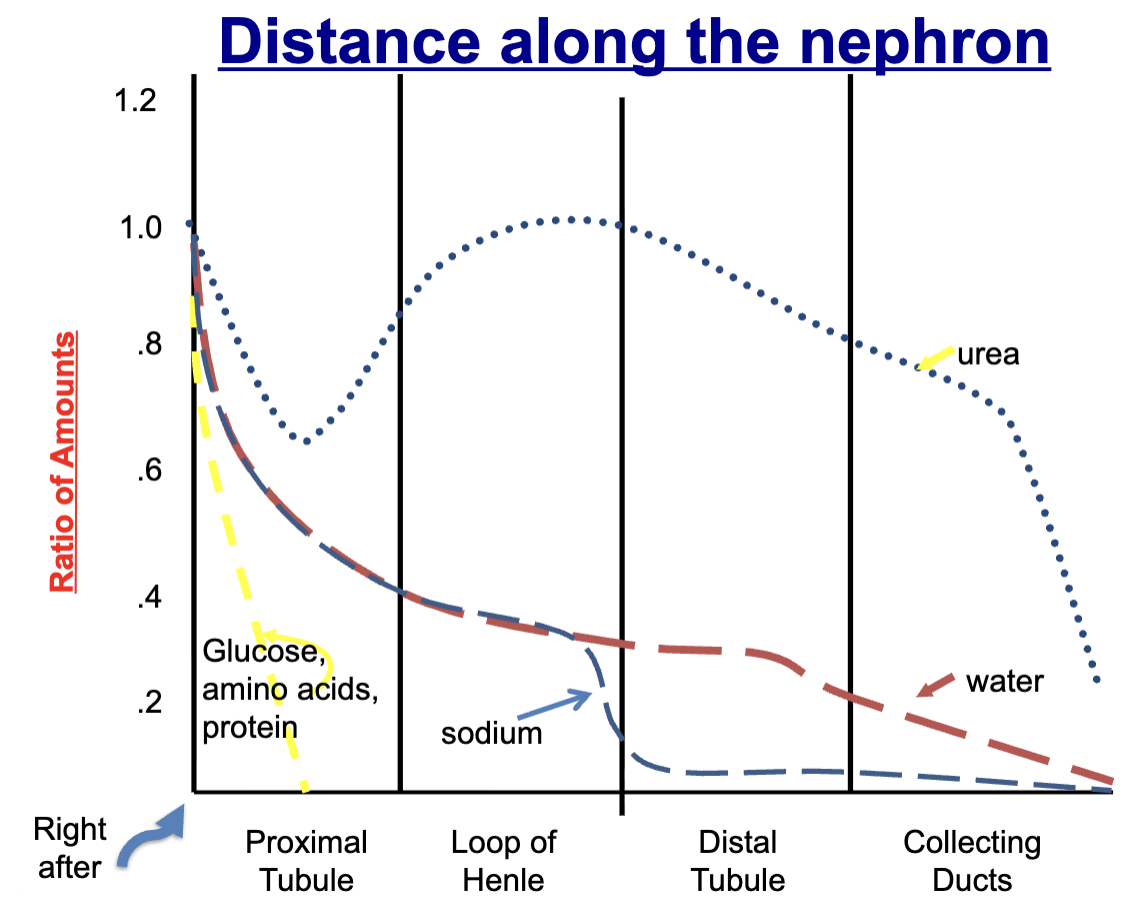
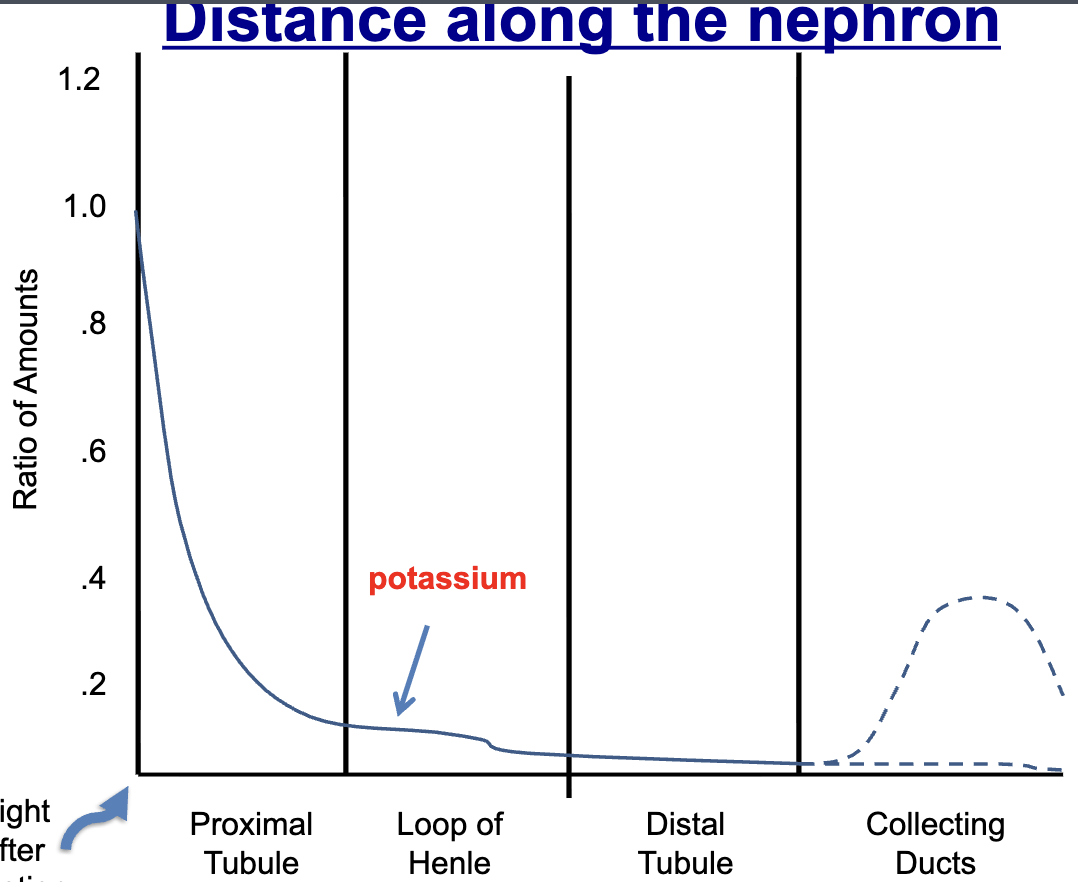
potassium reabsorption rates
Mostly reabsorbed in proximal tubule, until collecting ducts
depends on diet,
If low potassium intake, reabsorb most of it
If high potassium intake, some later secreted
Diuresis
increased production of urine
Osmolality
concentration of the solutes in the tubule (inside the lumen)
There is a linear relationship between osmolality and water reabsorption:
Increase in osmolality – solutes are more concentrated = water is reabsorbed
Decrease in osmolality – solutes are more diluted = water stays in the tubule
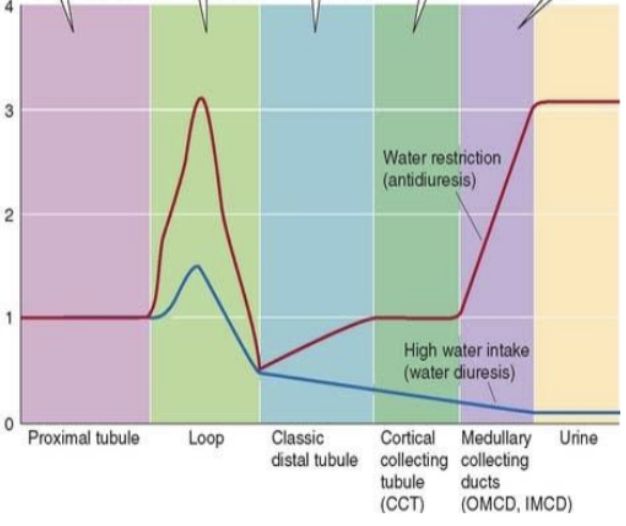
anti-diuretic hormone (ADH)/vasopressin
regulates water permeability (ability to reabsorb water) in collecting duct, usually when dehydrated
diabetes insipidus
don’t produce sufficient ADH, can’t reabsorb water —> pee all the time
Digestive System
• Digestion (break down) of food
• Absorption of nutrients
• Elimination of waste products
Digestive system major functions
1. Ingestion
2. Propulsion (peristalsis)
3. Mechanical digestion (segmentation)
4. Chemical digestion
5. Absorption
6. Defecation
Alimentary Canal
(digestive tract) long, winding, continuous tube, MAIN ORGANS
1) Mouth
2) Esophagus
3) Stomach (pancreas afterwards but not main)
4) Small intestine
5) Large intestine
6) anus
Accessory oragns
surround alimentary canal, not direct segment of tube
liver, gallbladder, pancreas, salivary glands, teeth, tongue
Mouth
ingestion (mechanical and chemical with teeth and saliva)
roof of mouth (hard and soft palate)
Uvula: prevent food from entering nasal cavity
Frenulum: thin membrane attaching tongue to floor of mouth
salivary amylase
enzyme in saliva
Teeth
Incisors: front teeth for cutting
Canine (cuspids): pointed, pierce and tear food
Premolars (bicuspids): two points, saw food
Molars (tricuspids): grind food
deciduous teeth: baby teeth
bolus
food after mouth
Esophagus
Connects the oral cavity with the stomach
Thin, collapsible, muscular, mucus-lined tube
Each end guarded by sphincter; valve-like rings keeping food moving in one direction (upper esophageal sphincter and lower esophageal sphincter)
Food moves via peristalsis due to muscle contractions.
Heartburn/acid indigestion (GERD)
backflow of stomach acid into esophagus called gastroesophageal reflux disease or GERD
Combat GERD
1) avoid stimulating foods
2) antacids
3) H2 receptor antagonists blocks acids from being released
Stomach
Sections: fundus, body and pylorus - mixing and acid secretion
Secretions from cells: gastric juices (HCl and pepsin)
3 layers of smooth muscle
Mucosal barrier protects the stomach: mucus protects stomach wall, damaged epithelial cells are quickly replenished
Pyloric sphincter holds the chyme (semisolid mixture of partially digested food) in the stomach until protein digestion begins
Small Intestine
Where most nutrient digestion takes place
Absorption occurs to move nutrients from SI into blood
Parts: duodenum, jejunum, ileum
Enzymes and digestive juices of its own and from pancreas
Gallbladder delivers bile salts to aid in digestion of fats
4 layers
Layers of small intestine
Mucosa – absorption + secretion; Villi, epithelial cells, microvilli
Submucosa –connective tissue; contains blood vessels and nerves
Muscularis – muscle; peristalsis moves food down tract, helps with mixing of digestive juices, contributes to mechanical digestion
Serosa – connective tissue in outermost layer
Ruggae
folds occur throughout the GI tract for high surface area for absorption
Liver
Glycogen storage (excess glucose)
Makes glucose (gluconeogenesis)
Makes bile —> secrete to gallbladder that helps with fat digestion in SI
Make plasma proteins (prothrombin, fibrinogen, albumin)
Detoxifies
Stores excess nutrients and vitamins
Liver disorders
fatty liver: when there is excess fat, sugar, or toxins in the body
Hepatitis – inflammation of the liver
Cirrhosis – scar tissue forms in the liver
Pancreas
Both an endocrine (glucagon/insulin) and exocrine organ (pancreatic juices)
exocrine gland secretes pancreatic juice (digestion and neutralization of stomach acid that enters the small intestine)
Large Intestine
complete digestion, absorb water, concentrate feces
Intestinal microbiome (bacteria) helps to break down undigested material releasing nutrients
Cells do not have microvilli: not much absorption
Appendix
next to junction of ileum and cecum
the appendix serves as a vital safe house for the intestinal microbiome
Digestion of carbohydrates
Salivary amylase (mouth) and pancreatic amylase (SI)—> disaccharides
Small Intestine enzymes (SI) —> monosaccharides
Digestion of proteins
Pepsin (stomach) —> polypeptides
Pancreatic enzymes and SI enzymes —> amino acids
Digestion of lipids/fats
Bile (SI via liver/gallbladder) —> emulsified lipid droplets
Pancreatic lipases (SI) —> glycerol and fatty acids
Metabolism
sum total of all the chemical activities occurring in the cell
Anabolism: synthesis of large molecules from small ones (takes energy)
Catabolism: break down of complex structures to simpler ones (makes energy)
Digestion is anabolism or catabolism
catabolism which explains why digestion creates ATP
____ are main energy source, then ____, then ____
carbs, lipids, proteins
cells of juxtaglomerular apparatus are very important in
regulating blood pressure
when blood pressure is low
juxtaglomerular cells secrete renin that increases blood pressure via Renin-angiotensin- aldosterone system (RAAS) by constricting blood vessels and increasing sodium reabsorption