hsci 210 lecture midterm 2
1/294
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
295 Terms
circulatory system parts
heart
blood vessels
blood
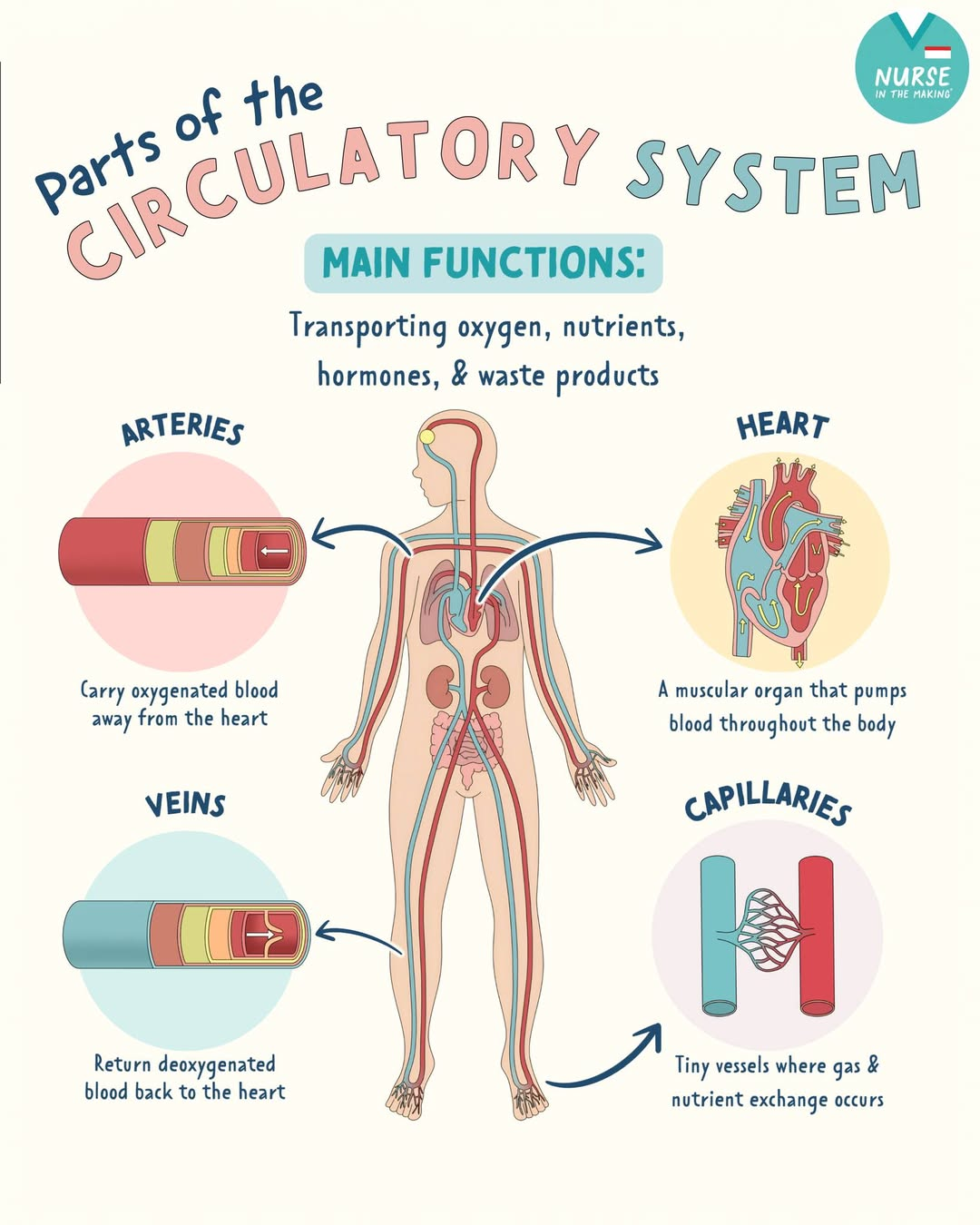
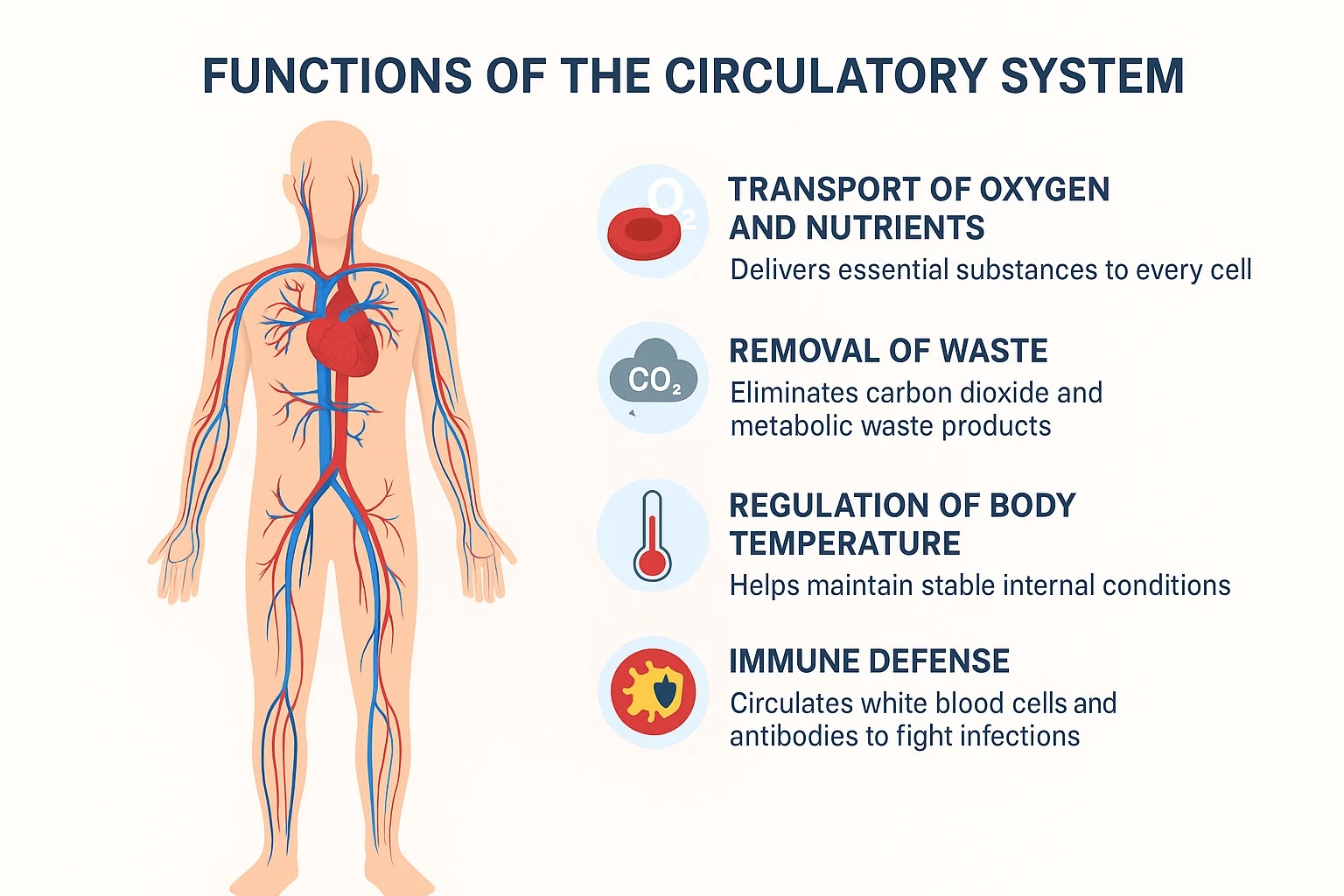
circulatory system function
transport blood, oxygen, nutrients to the body
help get rid of waste products
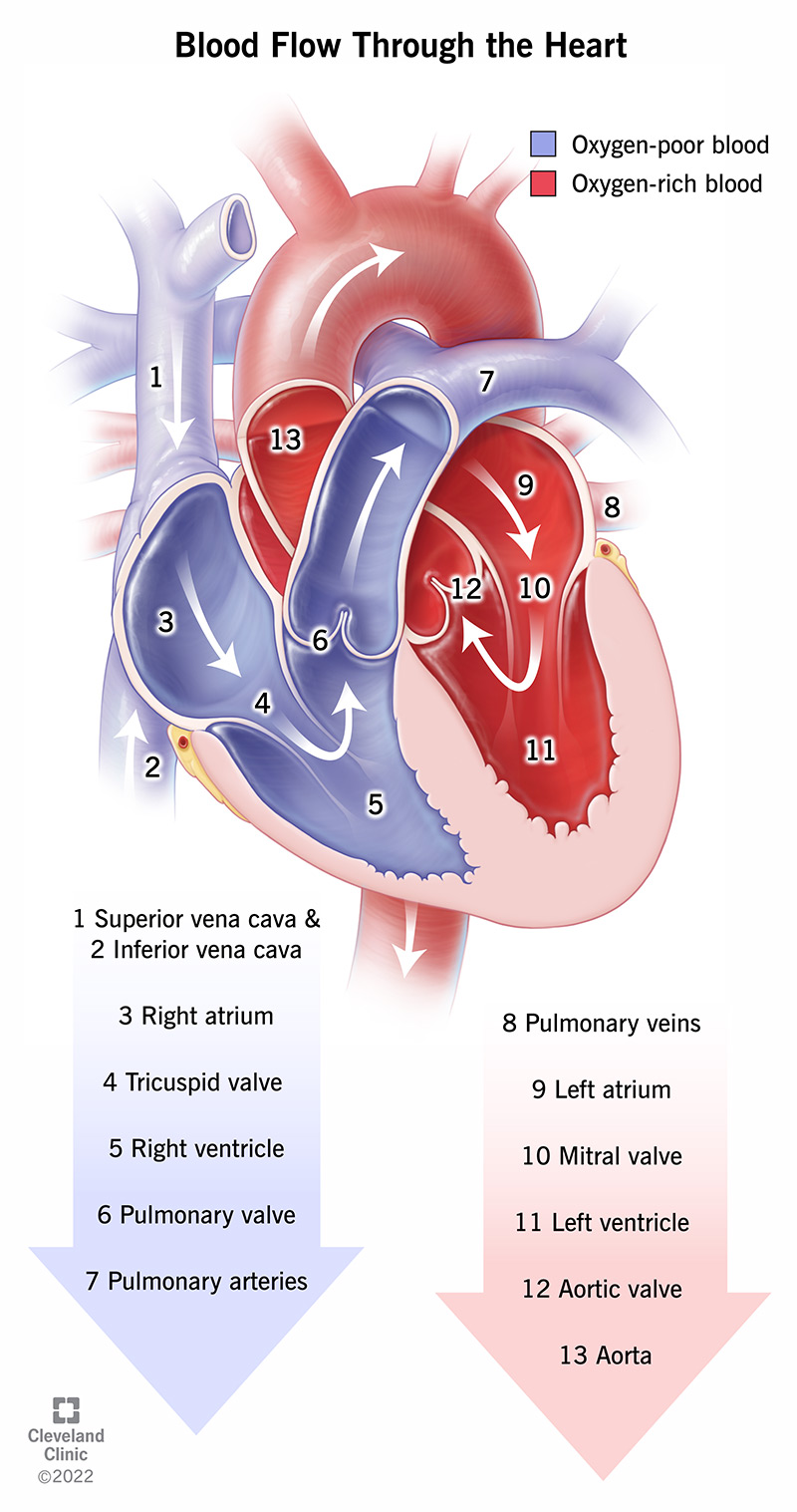
heart
blood carrying carbon dioxide
right atrium → tricuspid valve → right ventricle → pulmonary valve → lungs (oxygen replaces carbon dioxide)
blood carrying oxygen
lungs → left atrium → bicuspid valve → left ventricle → aortic valve → aorta (blood throughout body)
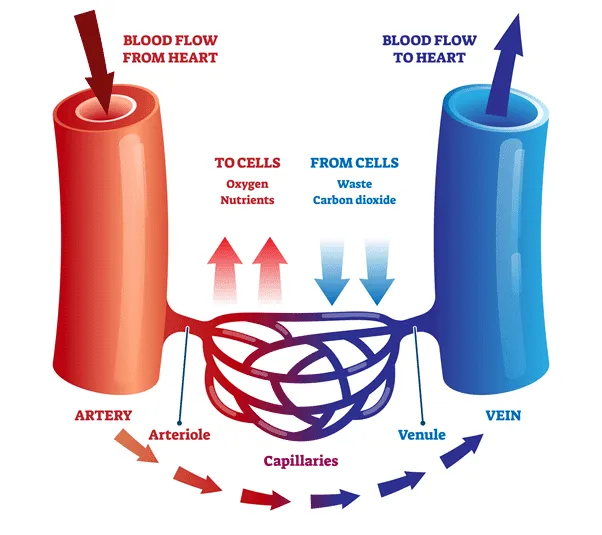
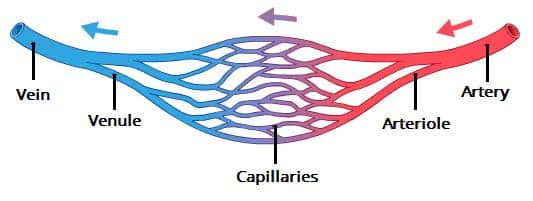
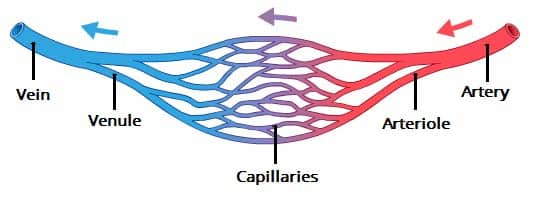
blood vessels
veins: bring deoxygenated blood to heart (blue)
venule: intermediate between vein & capillary
arteries: bring oxygenated blood to the body away from heart
arteriole: intermediate between artery & capillary
capillaries: handoff between veins & arteries: exchange of substances between blood and tissues
arterial side & venous side
vasodilation & vasoconstriction
venule
intermediate between vein & capillary
arteriole
intermediate between artery & capillary
artery
carries blood away from heart
thickest wall
withstand high pressure
more (thick smooth) muscle
constrict & dilate
regulate internal temperature
carries oxygenated blood (except pulmonary artery → lungs)
blood travels through lumen
capillary
assists in exchange of substances between blood and tissues
oxygen & sugars allowed to pass through walls (in and out of blood)
thinnest wall
bigger lumen
vein
carries blood to the heart
thinner wall
thinner smooth muscle layer
less muscular and stretchy
low pressure
carries deoxygenated blood (except pulmonary veins ← lungs)
special valve: keep blood flowing only one way
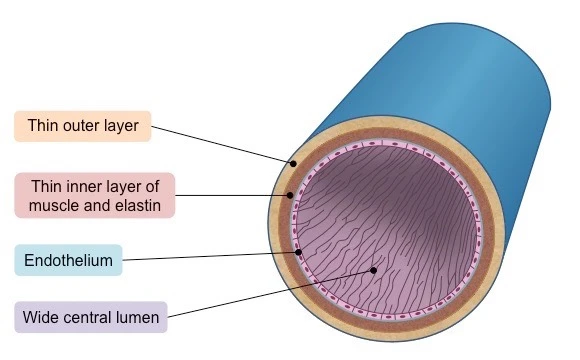
pulmonary artery
carries deoxygenated blood away from heart → lungs
exception of pulmonary circuit
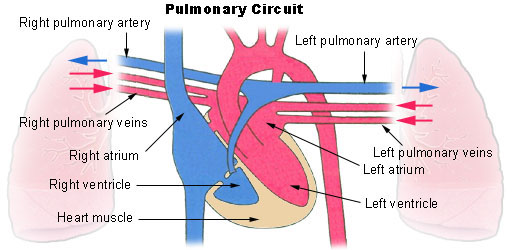
pulmonary vein
carries oxygenated blood toward the heart ← lungs
exception of pulmonary circuit
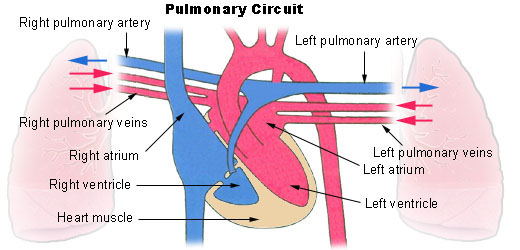
pulmonary circuit
arteries carry oxygenated blood away from body
pulmonary artery: carry deoxygenated blood
veins carry deoxygenated blood to the body
pulmonary veins: carry oxygenated blood
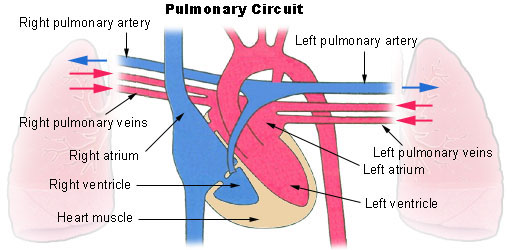
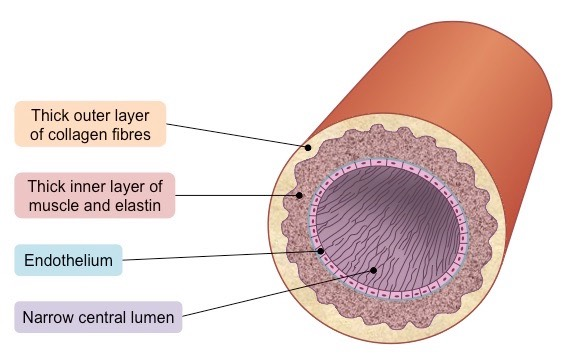
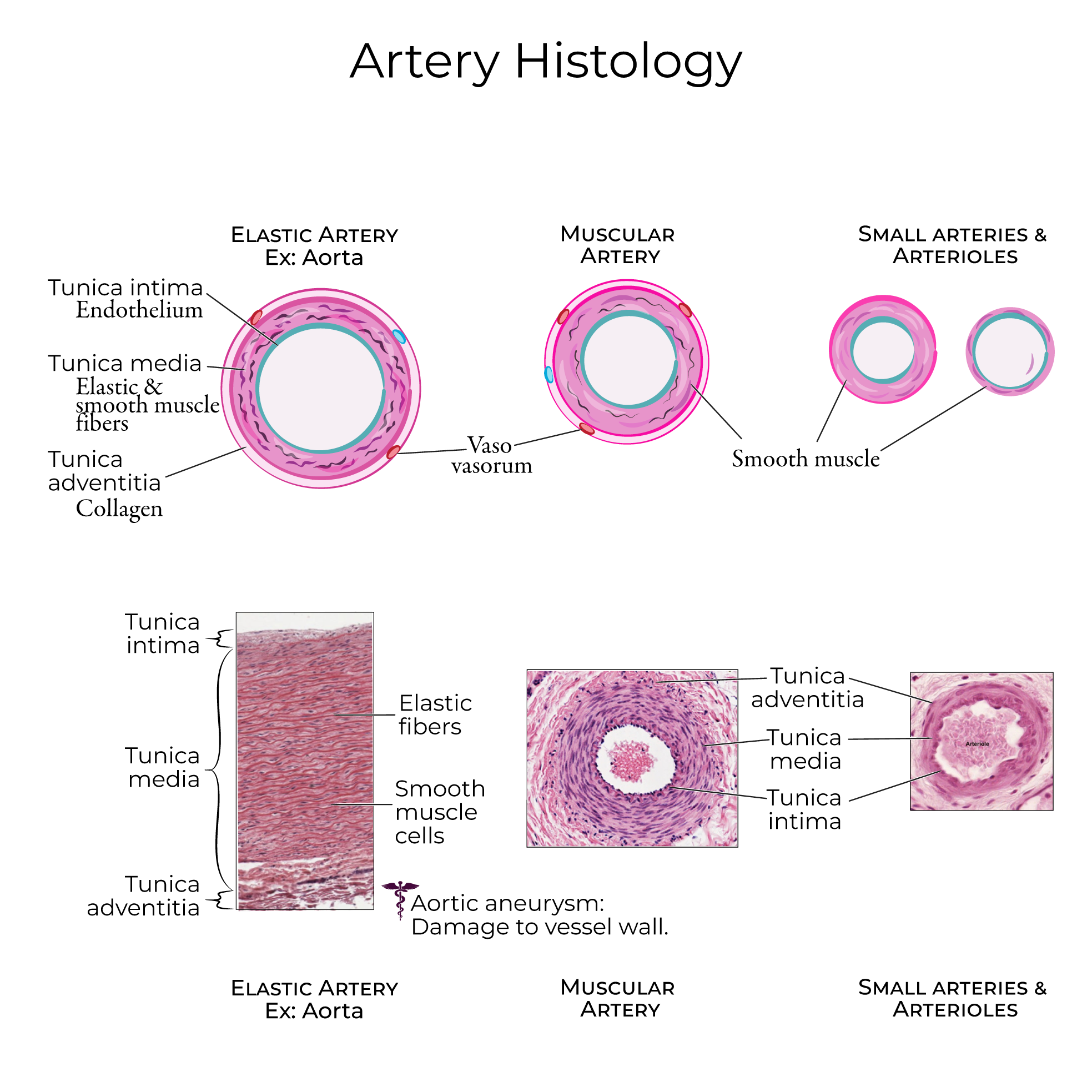
artery layers
tunica adventitia (externa): outer layer (collagen)
collagen: maintain structure to keep artery open
tunica media (smooth muscle tissue: thick elastic muscle layer): middle layer
smooth muscle (autonomic ns control): thick and elastic
tunica intima (endothelium) (endothelial layer) inner layer
endothelial layer produce serous mucous lining for easy blood flow
lumen: opening
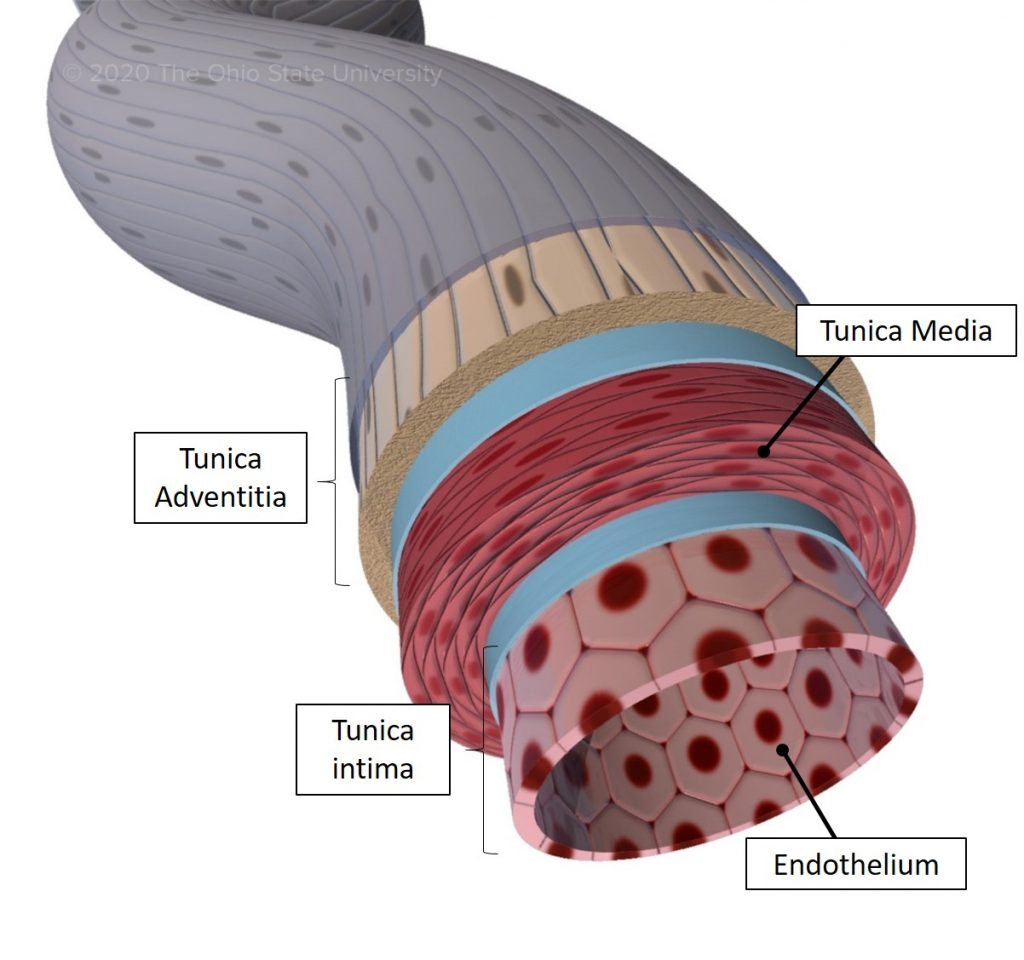
tunica adventitia (externa)
collagen: maintain structure to keep artery open
most outer layer of artery
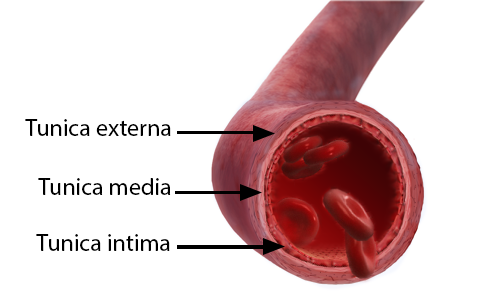
tunica media
smooth muscle: thick and elastic
middle layer of artery
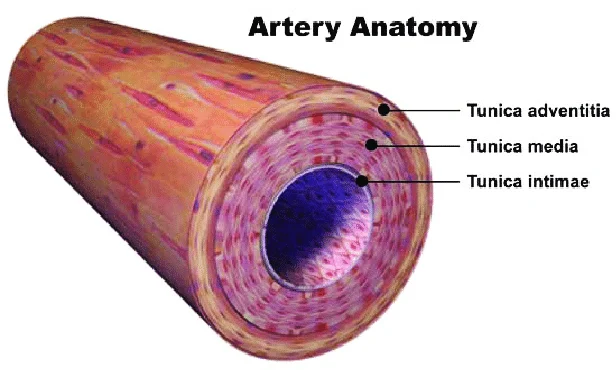
tunica intima
endothelium: endothelial cells produces serous mucous lining to ease blood flow
inner layer of artery
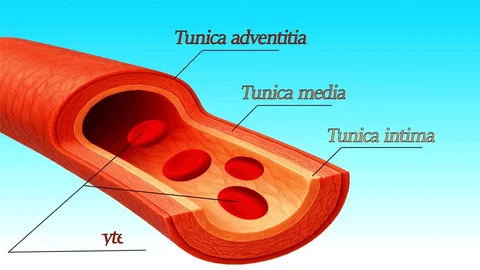
classification of arteries
organized by size & histology
largest to smallest
elastic
muscular
arterioles
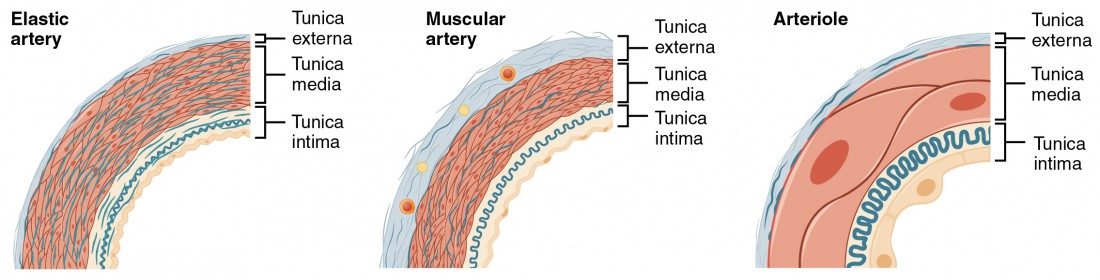
elastic artery
largest artery (1.0-2.5 cm diameter)
closest to heart
flexible in left ventricle, pushes out
smooth muscle
ex. aorta
large tunica media layer
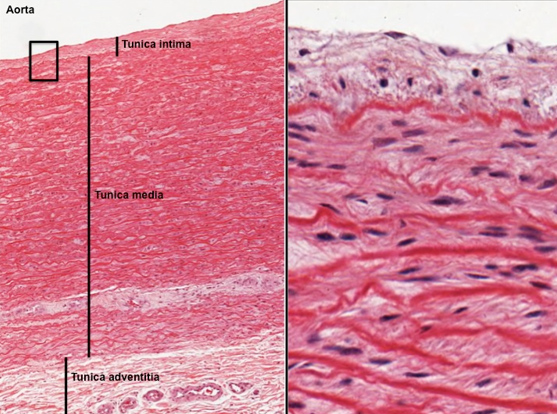
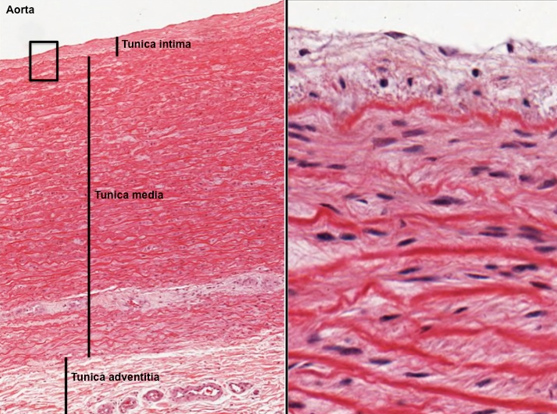
elastic artery histology
largest artery
largest tunica media (smooth muscle) layer
muscular artery
medium sized artery
peristalsis (smooth muscle): allow movement of materials through slow, wave-like contractions
surrounded by adipose tissue
located in digestive system & distal locations
lots of tunica adventicia/externa
patent: large, open lumen (structure so blood flows through)
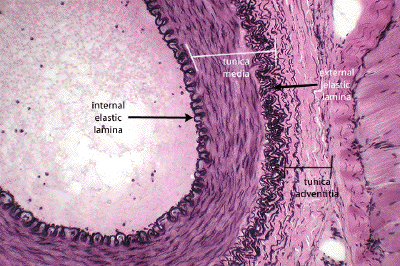
muscular artery histology
medium-sized artery
lots of tunica adventicia/externa
patent: large, open lumen (structure so blood flows through)
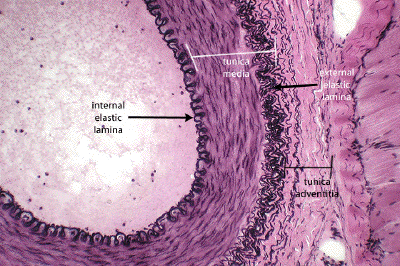
arteriole
smallest arteries
regulate blood pressure by restricting or dilating; changes overall resistance to blood flow (drop blood pressure to prevent capillary burst)
mid-size betwen arteries and capillaries
open / close capillary beds to control blood flow to certain tissues
sphincters: open and close to manage where blood goes
layer of endothelium surrounded by smooth muscle (thin tunica externa & tunica media)
narrow, round lumen
simple squamous epithelial tissue
red blood cells in lumen
no tunica externa
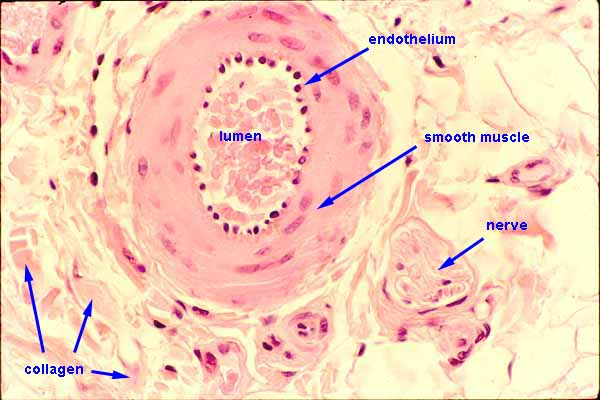
arteriole histology
smallest arteries
layer of endothelium surrounded by smooth muscle (thin tunica externa & tunica media)
narrow, round lumen
simple squamous epithelial tissue
red blood cells in lumen
no tunica externa
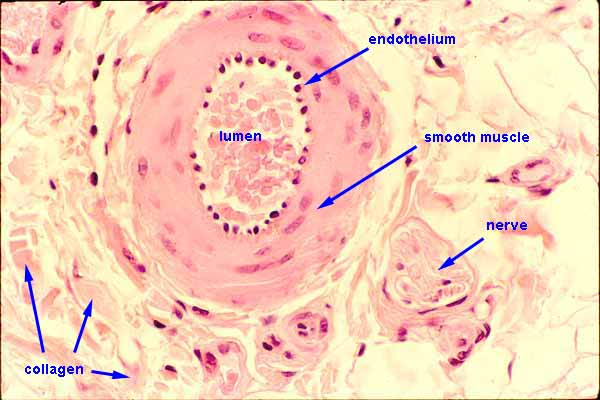
artery type histology
elastic artery
largest tunica media
muscular artery
large tunica adventitia/externa
large open lumen
arterioles
endothelium surrounded by smooth muscle cells
thin tunica externa & thin tunica media
narrow, round lumen
simple squamous epithelial tissue
no tunica externa
capillary
smallest vessels
one red blood cell, single file
one layer of endothelium surrounded by a basement membrane
venuole → vein → inferior vena cava/superior vena cava → heart
endothelium sealed by tight junctions
selectively leaky
fenestrations: holes for passage (diffusion) of substances
in: nutrients, oxygen
out: carbon dioxide, waste
histology:
endotholeial layer: simple squamous epithelium
tunicas intima: lined up red blood cells
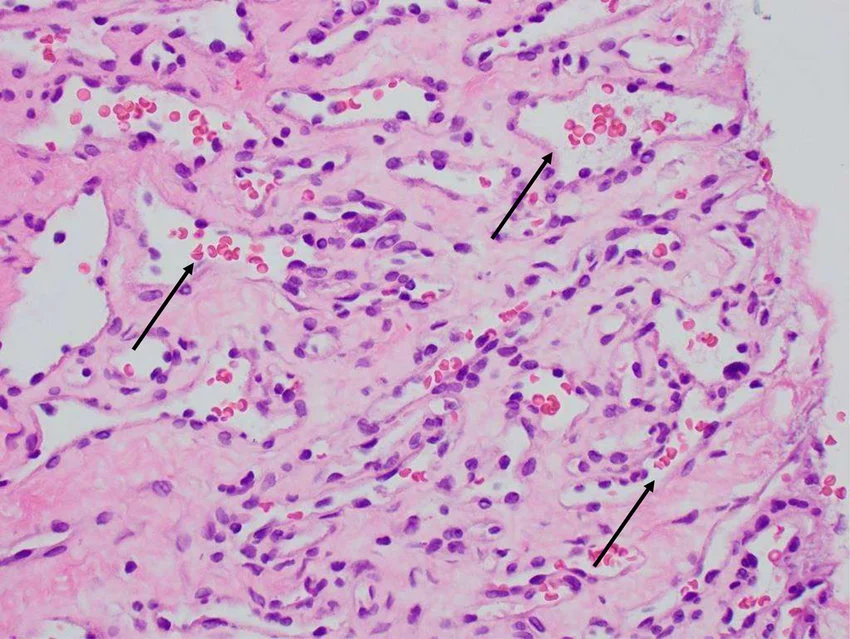
fenestration
hole for passage (diffusion) of substances
in: nutrients, oxygen
out: carbon dioxide, waste
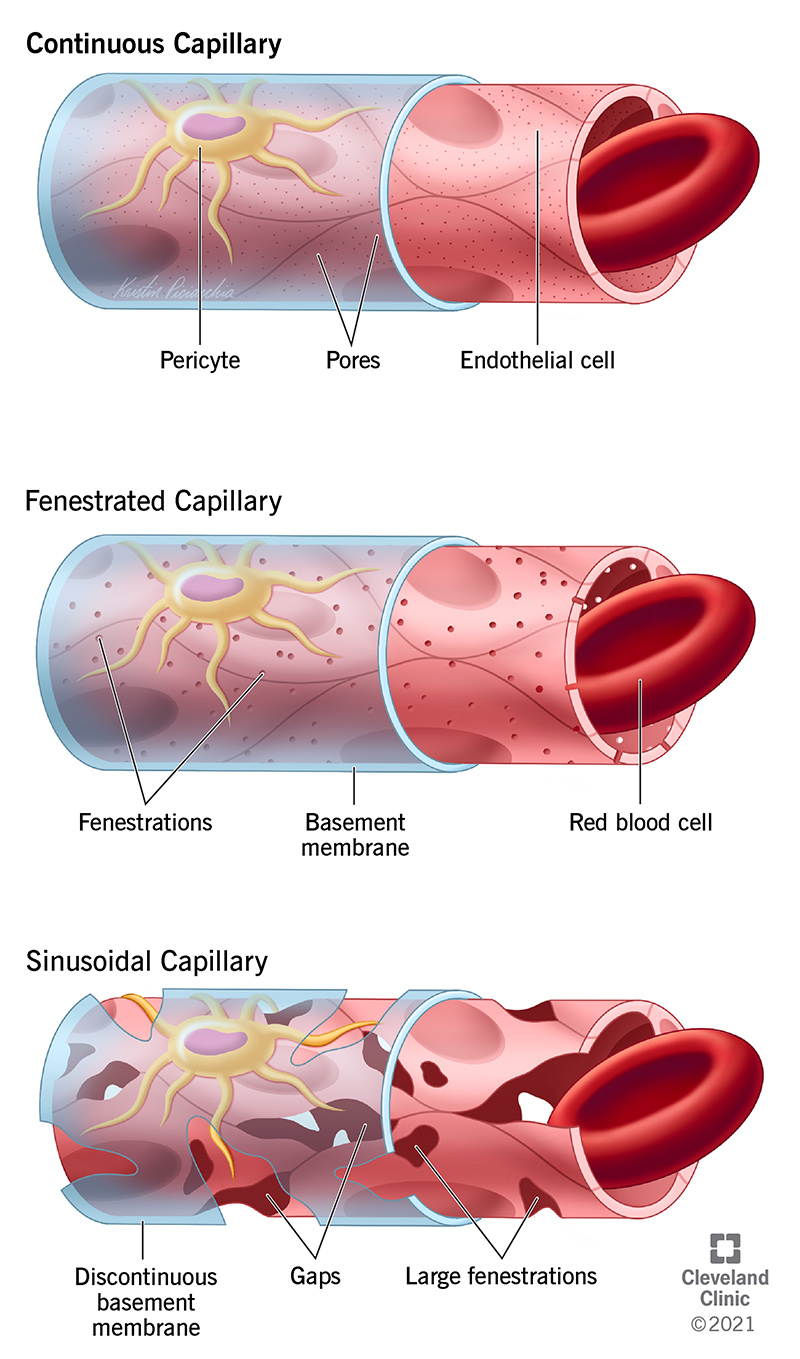
capillary endothelium
simple squamous epithelium
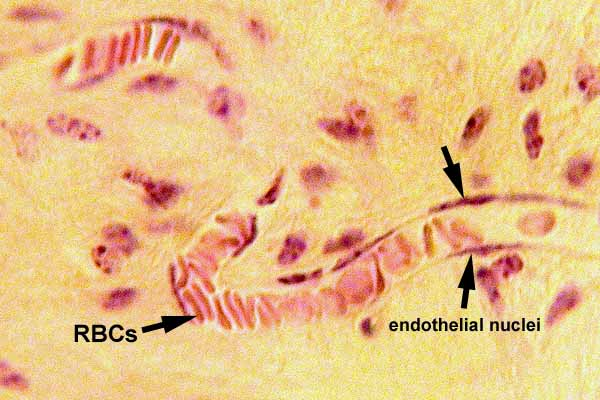
capillary exchange
from artery oxygenated RBC: oxygen & nutrients diffuse → body cells
from body cells: carbon dioxide and waste diffuse → dexoygenated RBC
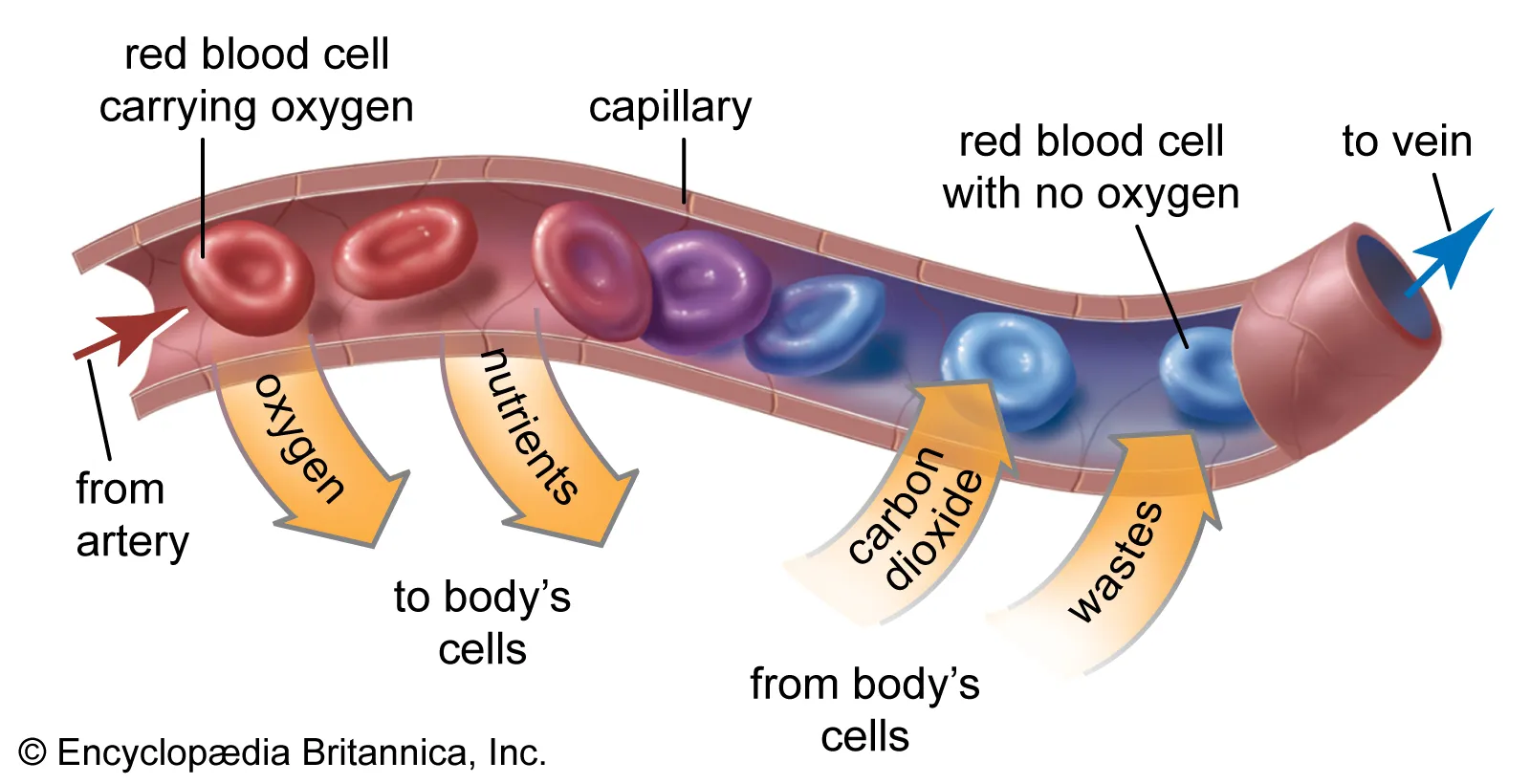
endothelial (tunica intima)
epithelial on inner lining of vessels (tunica intima)
simple squamous epithelium
secrete and absorb
capillary endothelial: exchange blood and lymph with surrounding interstitial tissues
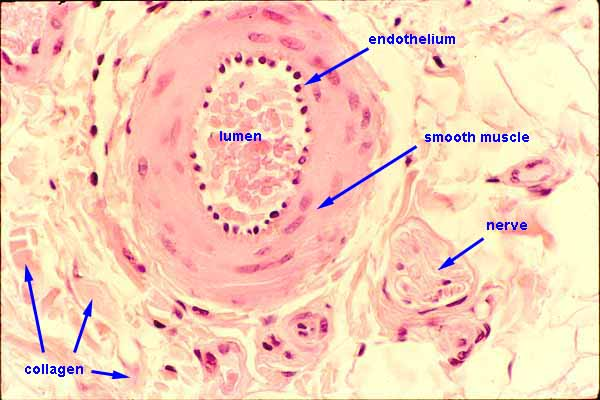
capillary endothelial tissue
exchange blood and lymph with surrounding interstitial tissue
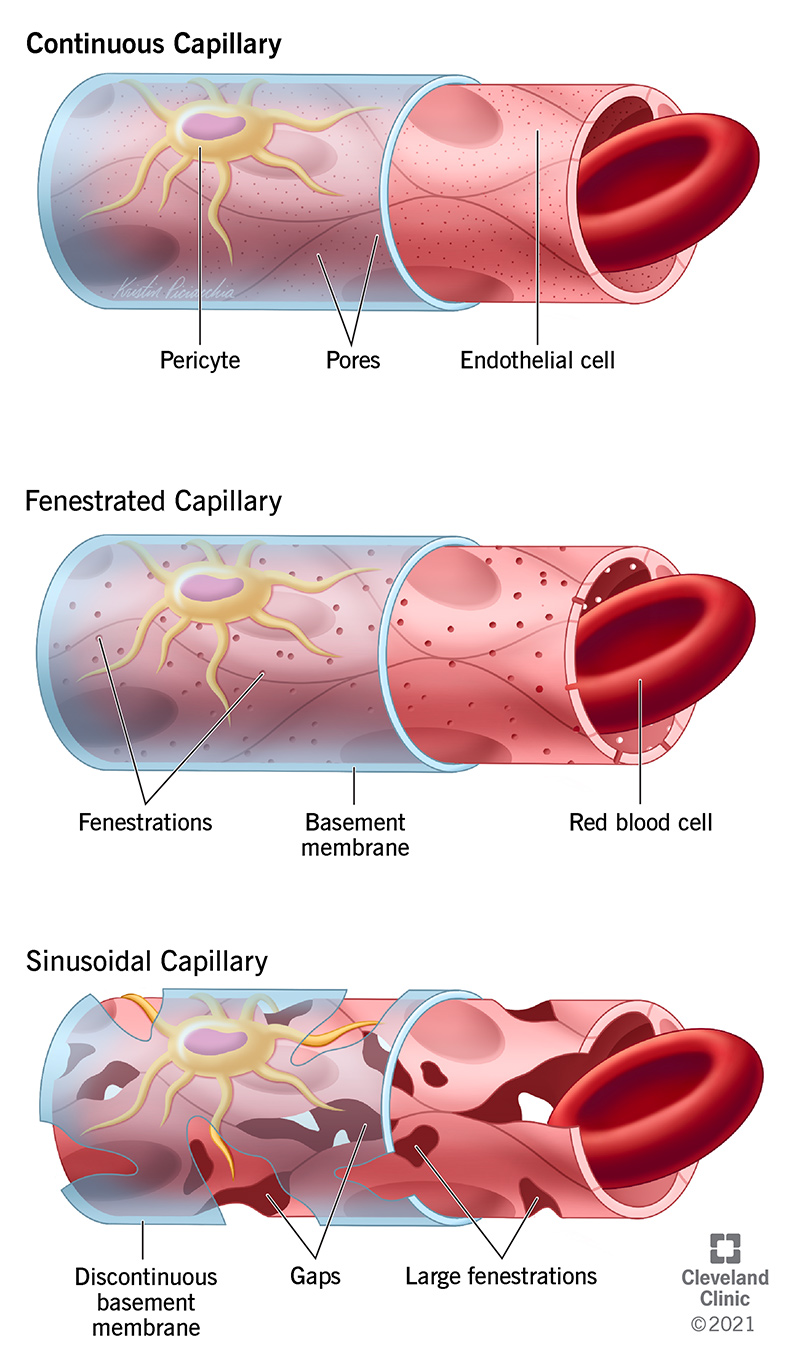
capillary types
least to most vascular permeability
continuous: tight junctions, no seeping
fenestrated: holes for exchange
sinusoid: most permeable
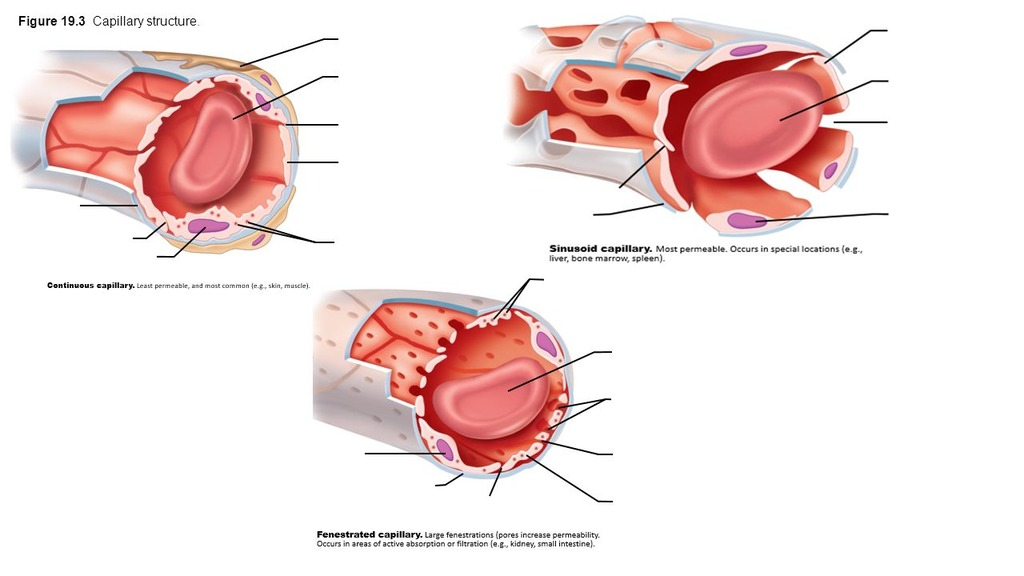
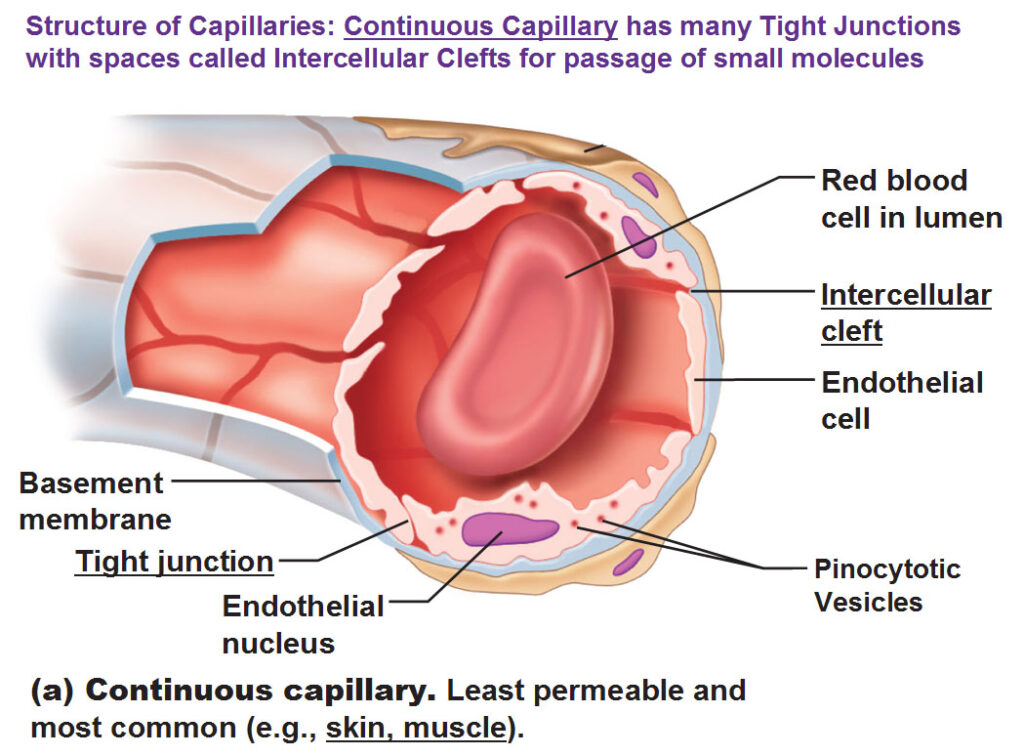
continuous capillary
least permeable, most common
tight junctions → no seeping
fenestrated capillary
middle permeability
fenestrations (pores) for exchange
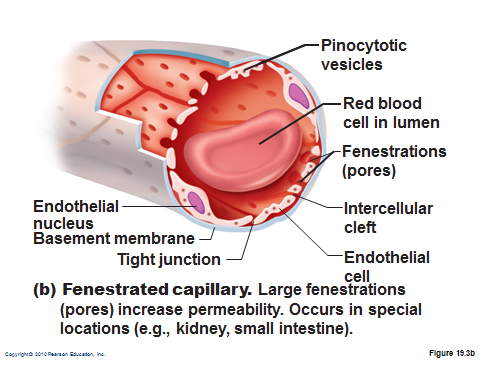
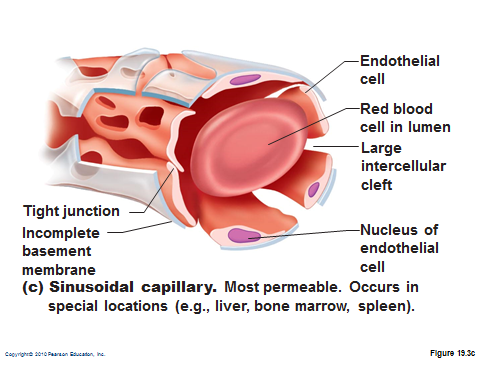
sinusoid capillary
most permeable
wide gaps to allow exchange
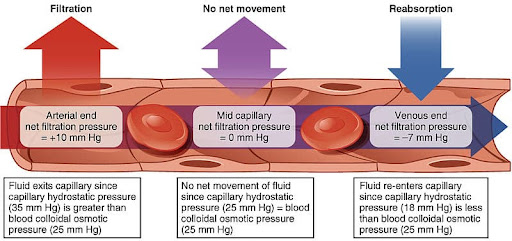
capillary selective permeability
arterial end - bed for exchange - venous end
filtration (arterial end): fluid exit capillary
high pressure inside → low pressure outside
oxygen & nutrients EXIT
no net movement: no filtration
equal pressure inside = equal pressure outside
reabsorption (venous end): fluid re-enters capillary
high pressure outside → low pressure inside
carbon dioxide & waste ENTER
inside: capillary hydrostatic
outside: blood colloidal osmotic
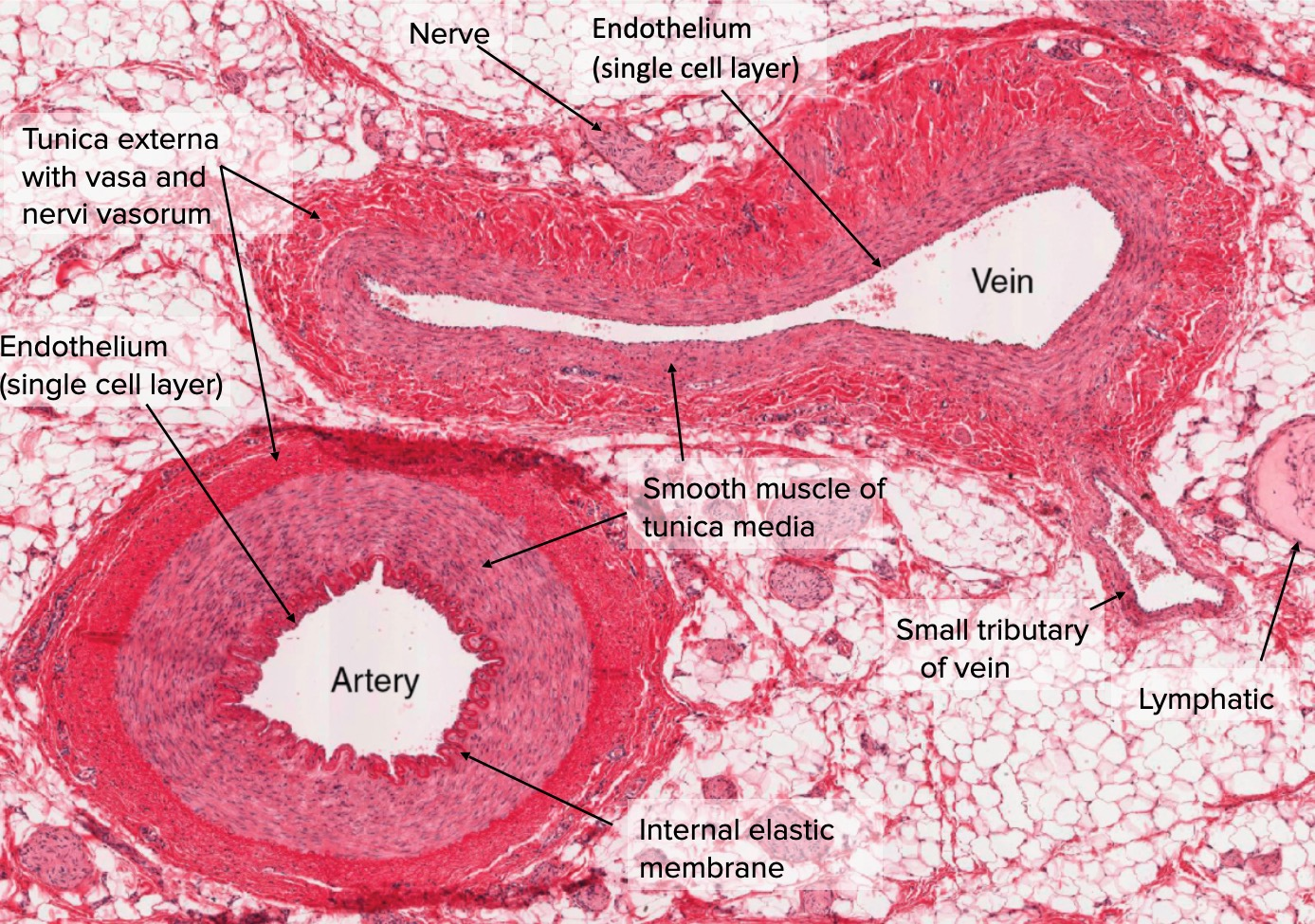
vein
tubes or channels carry blood from body’s capillary beds → heart
larger opening (carries more blood)
blood pressure declines by time blood has passed in/out of arterioles and capillaries
vein walls much thinner than arteries
return blood against gravity with less blood pressure
closes to heart → widest in diameter
simple squamous epithelium
lumen not round
less muscle → collapse when less blood
blood back to heart
pressure
valves: in arms & legs (some head & neck; no torso)
normal body movement: swinging arms & legs
skeletal muscle pump: muscle contraction causes blood flow (open valve, closes after push to prevent backflow)
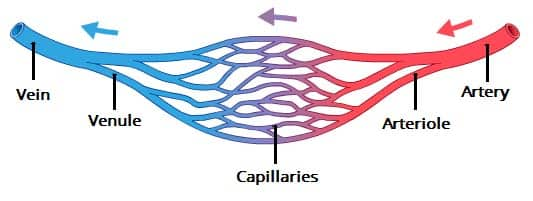
venuole
link capillaries & veins
most permeable region of vascular system
no tunica media (no
smooth muscle)tunica adventitia (externa): loose fibrous connective tissue
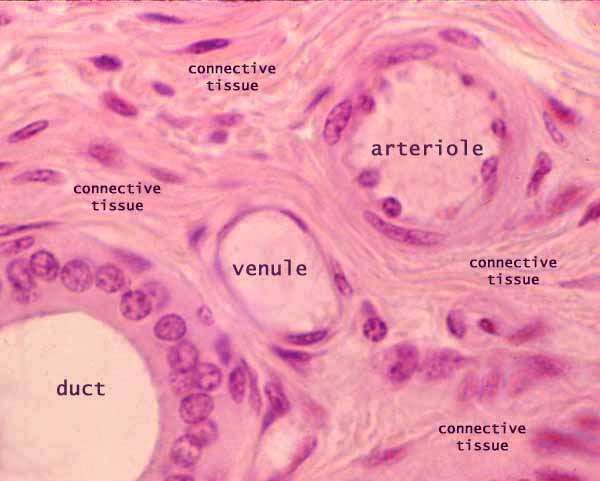
venuole function
maintain blood flow
regulate fluid exchange between vessels & surrounding interstitial tissues
immune response (cancer, auto-immune, inflammatory, neuro-degenerative disease)
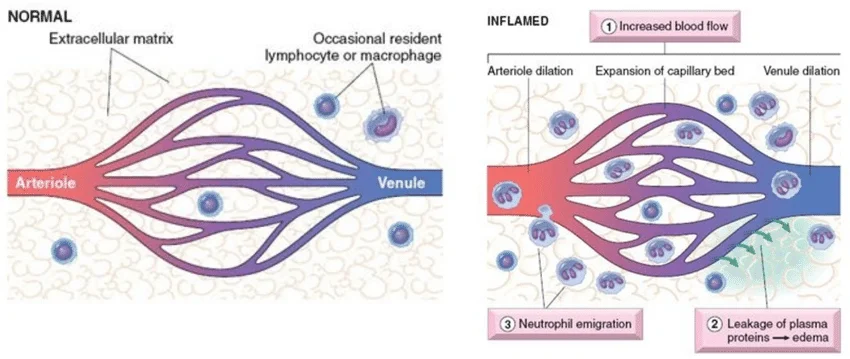
increased permeability of venuoles
inflammation
endothelial cellls contract when triggered by histamines or bradykinan during inflammatory response
cells contract → bigger gaps in between
bigger gaps → allow exudate (plasma, proteins, WBCs) to leak out
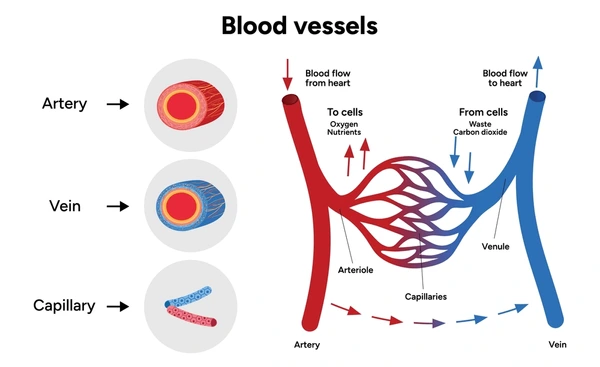
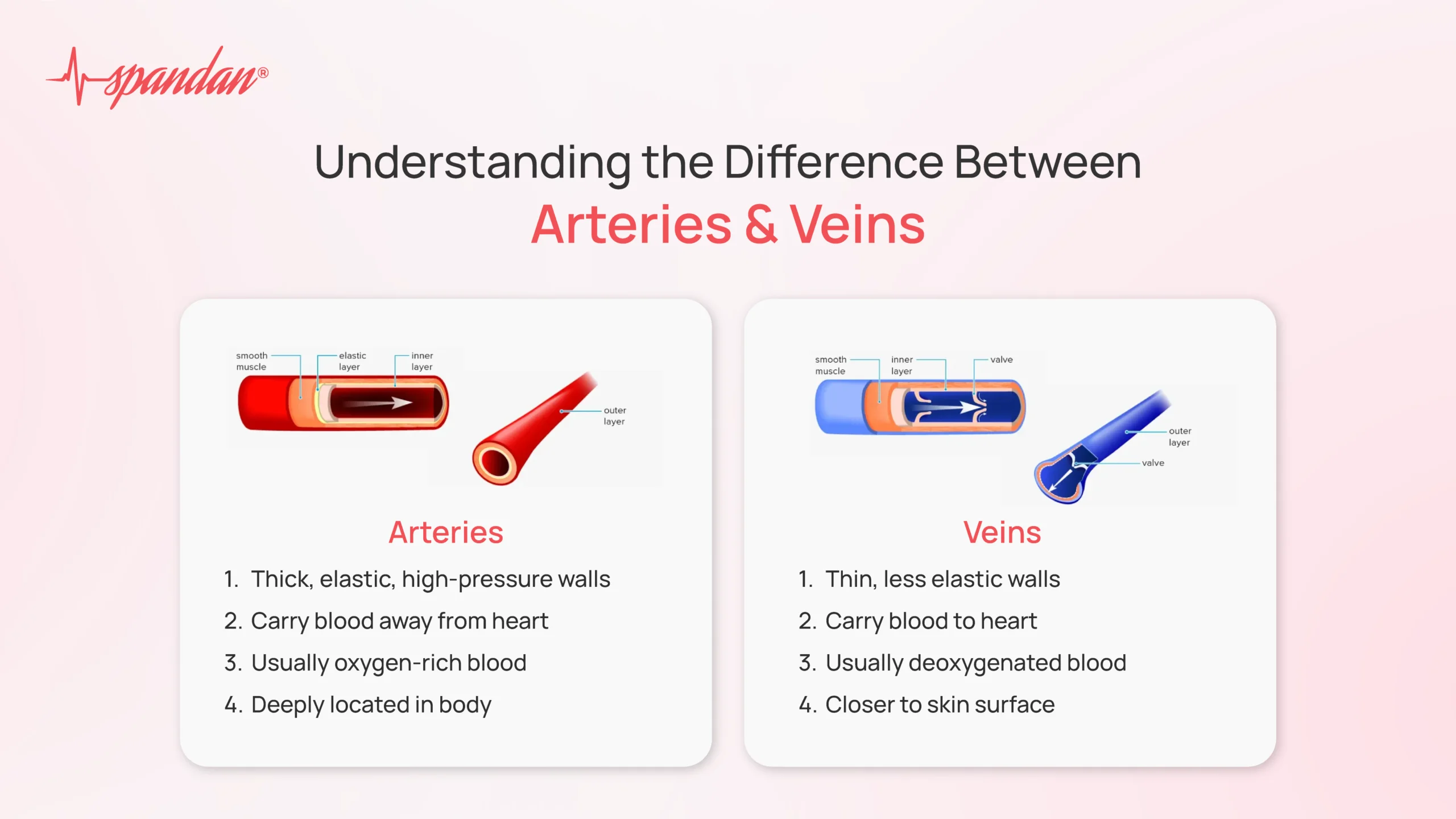
blood vessels
artery
away from heart
more smooth muscle; high pressure
smaller lumen
vein
toward the heart
less smooth muscle, more skeletal muscle; low pressure
larger lumen
valves
vascular pathologies
aortic dissection
capillary rupture
edema (pulmonary)
varicose veins
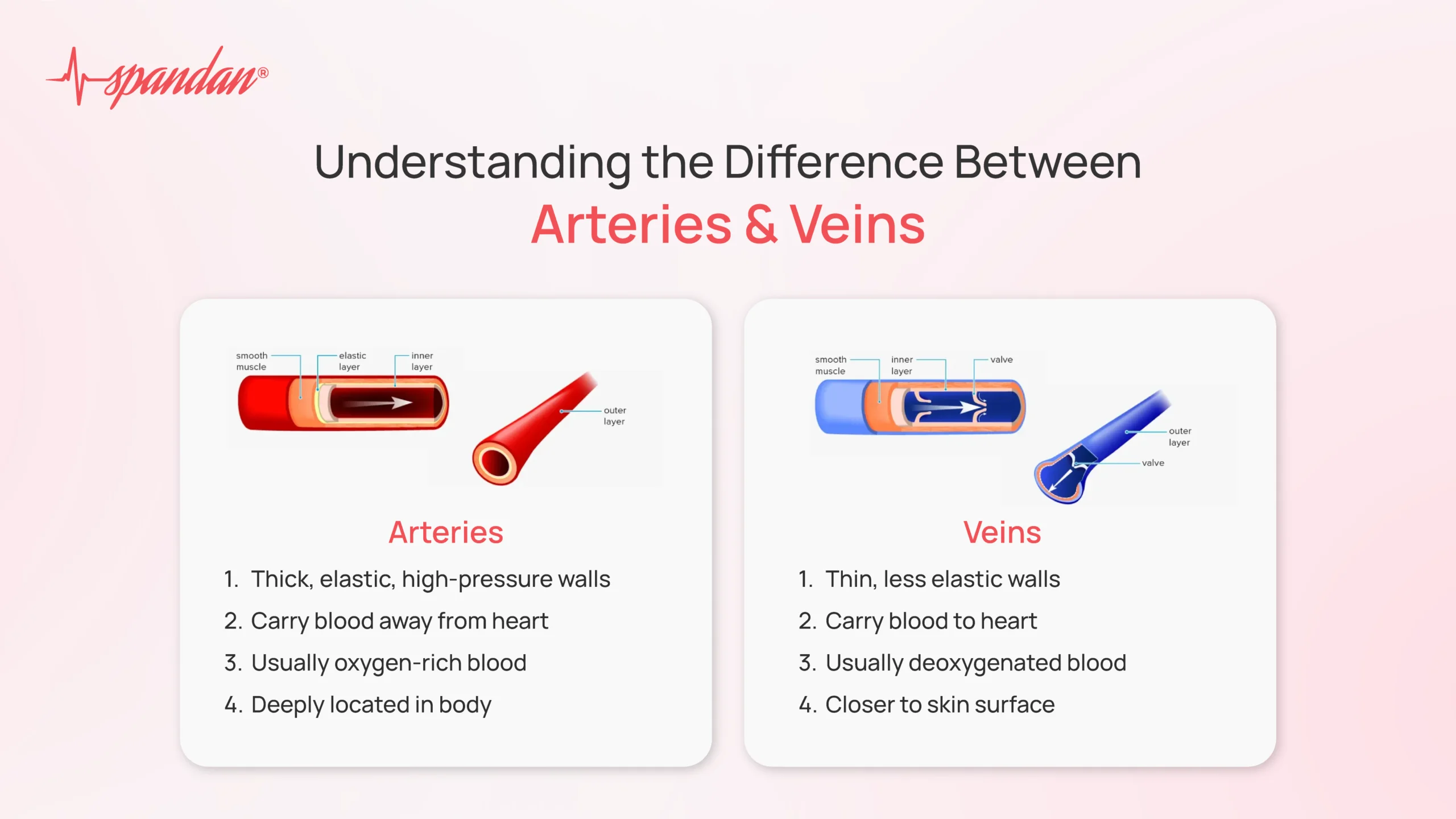
aortic dissection
tear in aorta inner wall → blood leak between layers of wall (separates)
weak spot (wall starts to bubble → pressure on walls → burst → aneurysm)
etiology:
hypertension, atherosclerosis, aortic aneurysm (weakening of tunica intima), connective tissue disorders, trauma, medications (corticosteroids), family history
treatment:
surgery & aggressive control of risk factors; surgical graft before blood burst
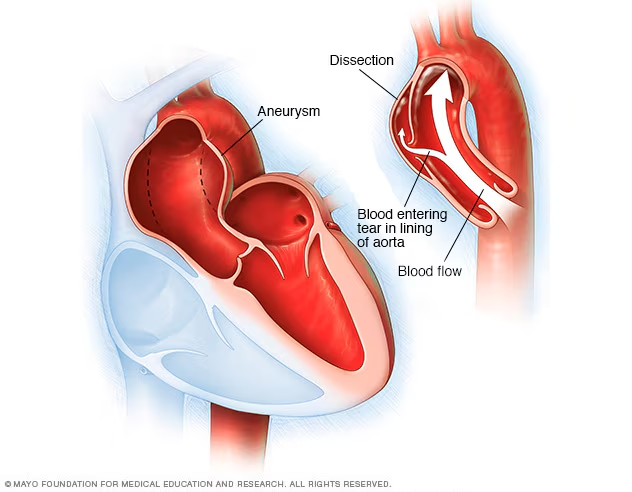
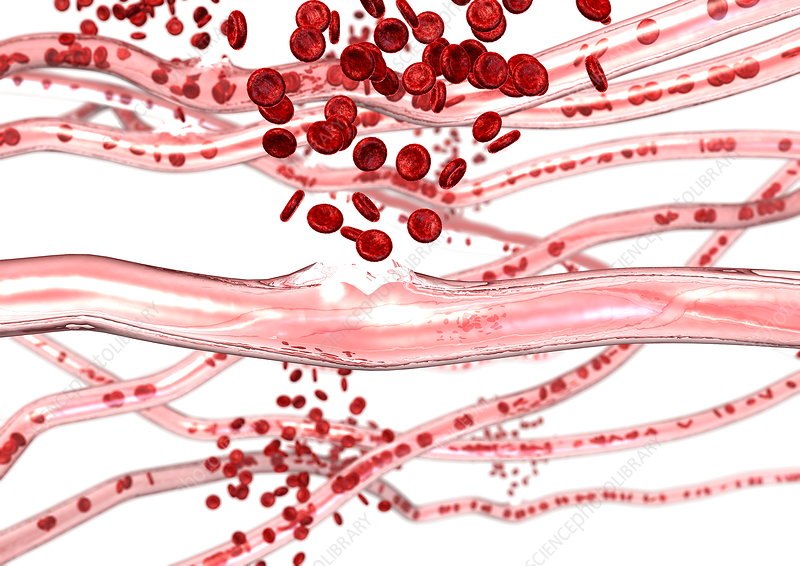
capillary rupture
capillary (tiny) burst → blood cells leak out under
spidery veins
treatment:
resolves independently
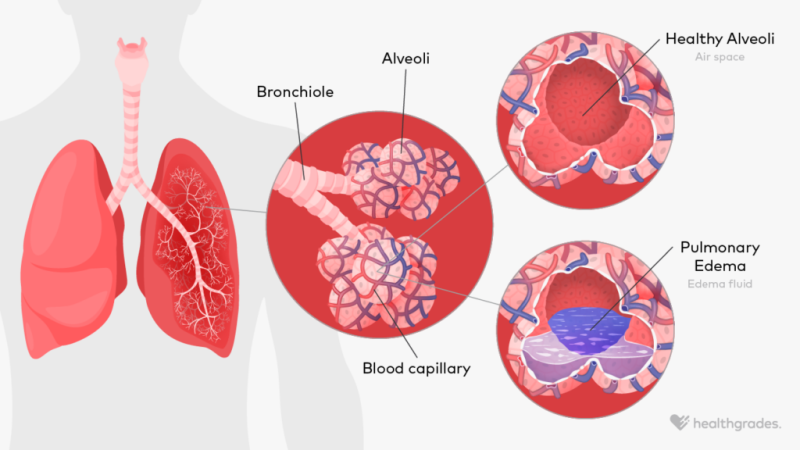
edema (pitting)
interstitial tissues not draining back into capillaries & post capillary venules normally → swelling in lungs (alveoli: air sacs) due to excess fluid accumulation
similar to edema in systemic tissue
etiology:
injury, infection, heart failure, liver/kidney disease, medication, pregnancy
treatment:
elevation, garments, medicine, activity
varicose veins
weak venous valves → blood flow not good from increased pressure → veins swollen from blood pooling → backflow into lower extremities
etiology:
weak valves, increased pressure, family history
treatment:
surgical removal, techniques to close off affected veins
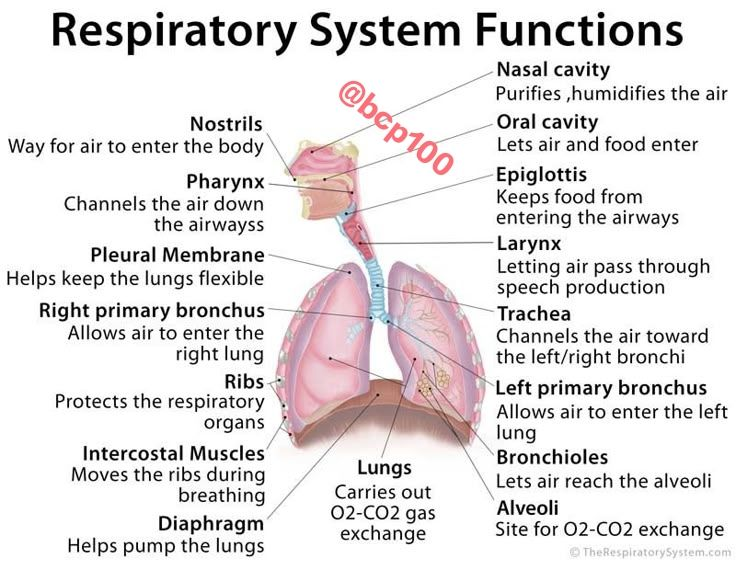
respiratory system function
moves air into the body and removes waste products
body cells require oxygen for respiration
respiratory network and gas exchange in blood: oxygen breathed → body cells
carbon dioxide exhaled → out
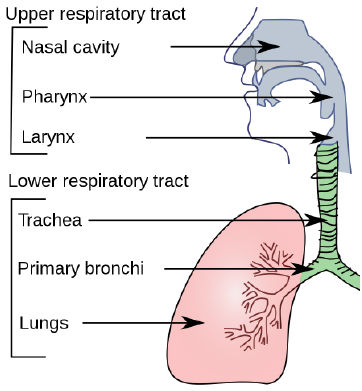
respiratory system structure
upper respiratory tract
nasal cavity
pharynx
larynx
lower respiratory tract
trachea
primary bronchi
lungs
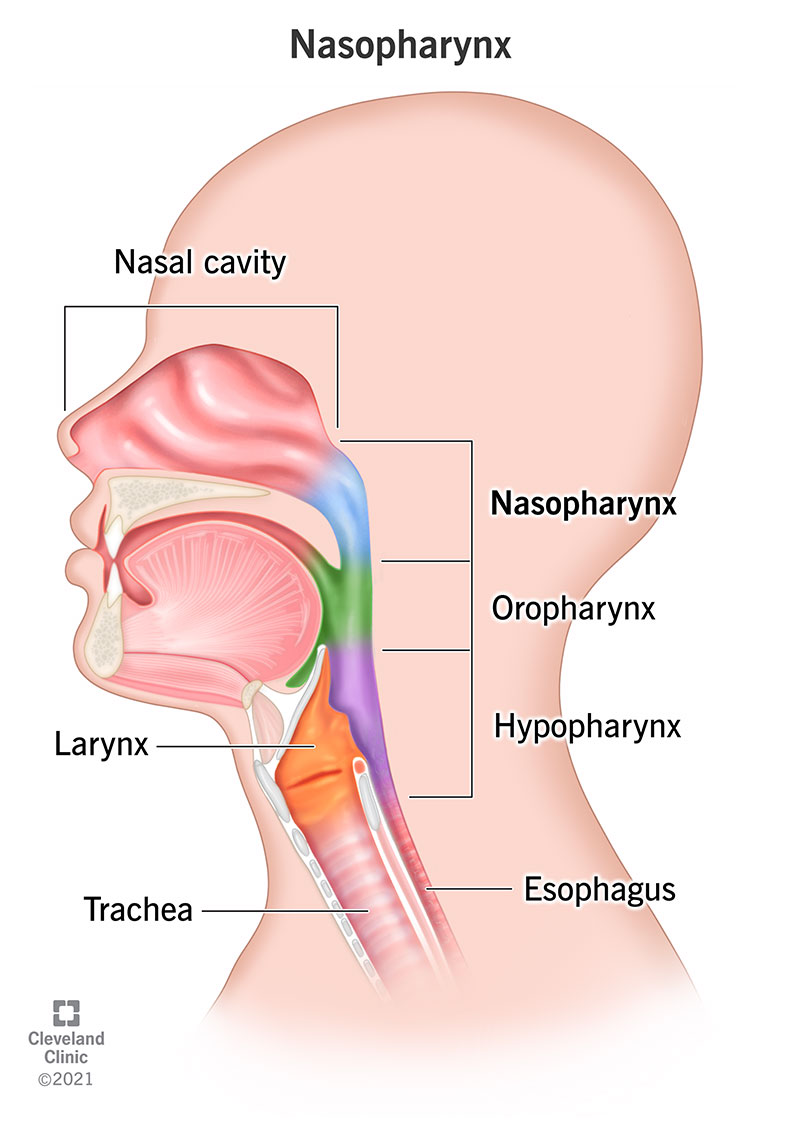
nasal cavity & mouth
allow air to be inhaled & enter the body
nasal conchae (tubinates): warm & moisturize air
conchae filter out dirt, pollen, particles
adjust size to control airflow
help with sense of smell
nasal conchae (turbinates)
warm & moisturize air
filter dirt, pollen, particles
adjust size to control airflow
help with sense of smell
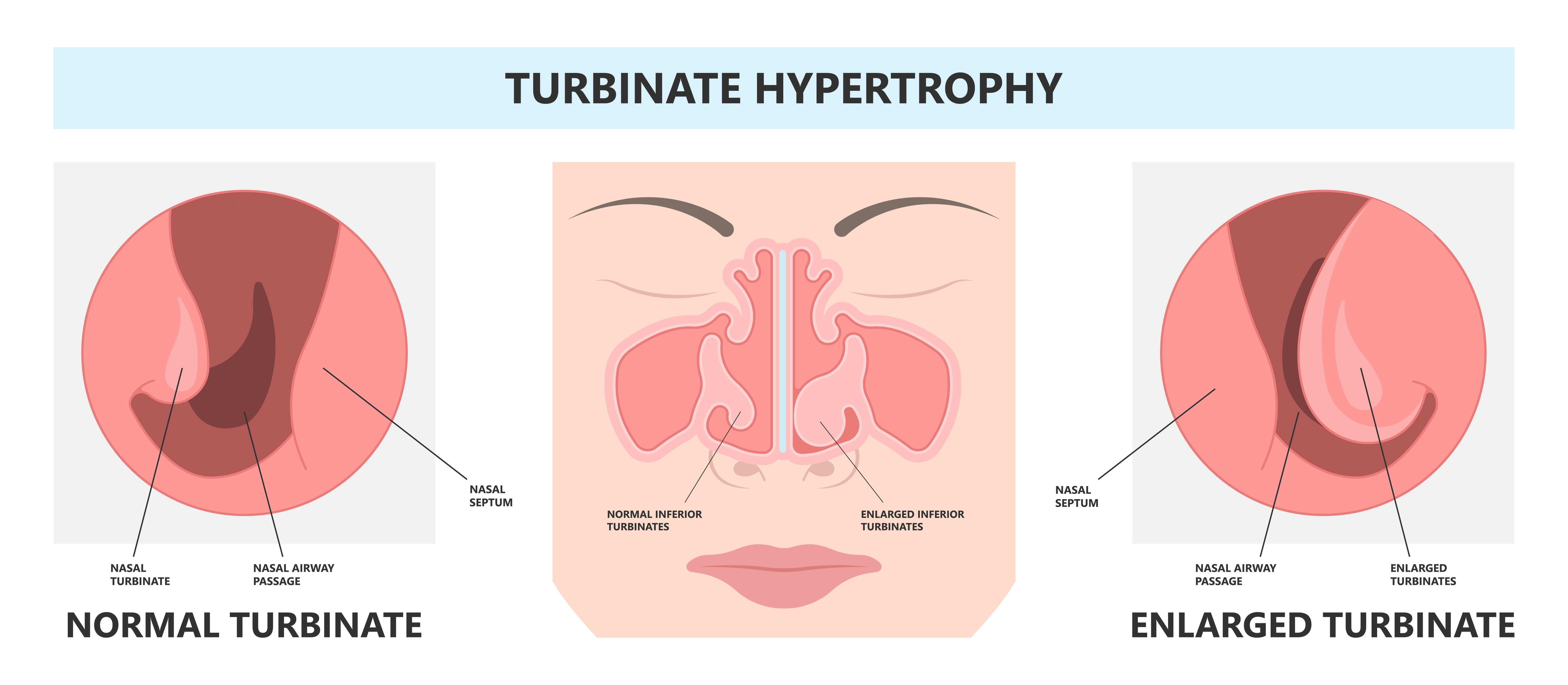
nasal cavity lining
vascular ciliated columnar epithelial cells lining
mucosa: mucous secreting goblet cells
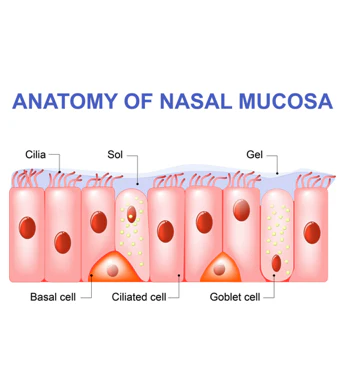
mucosa
additional nerve cells change chemical odors → chemical impulses & send through olfactory bulb (CN I) to brain
ciliated cell: mucous transport
goblet cell: mucous production
connective tissue
pseudostratified columnar epithelium
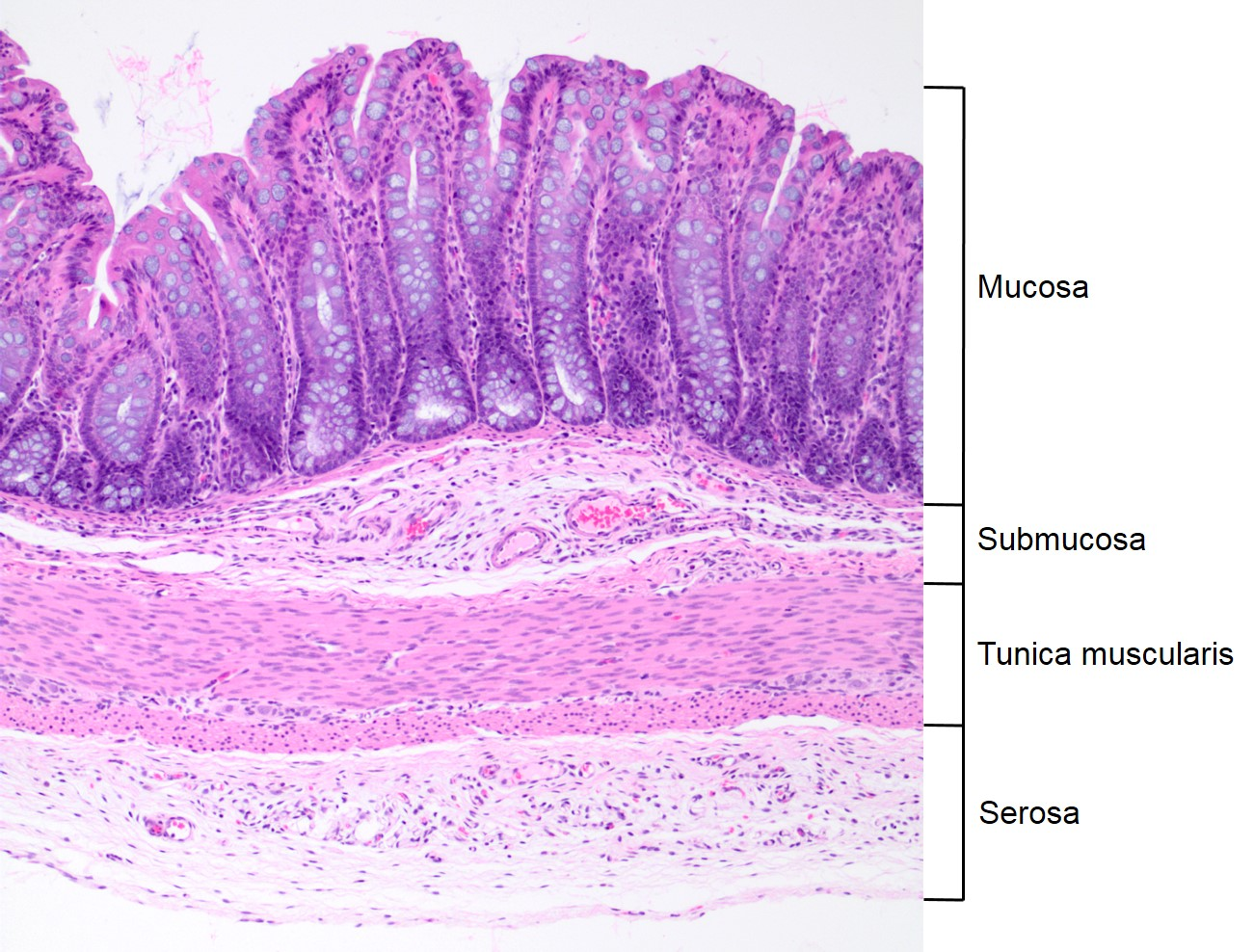
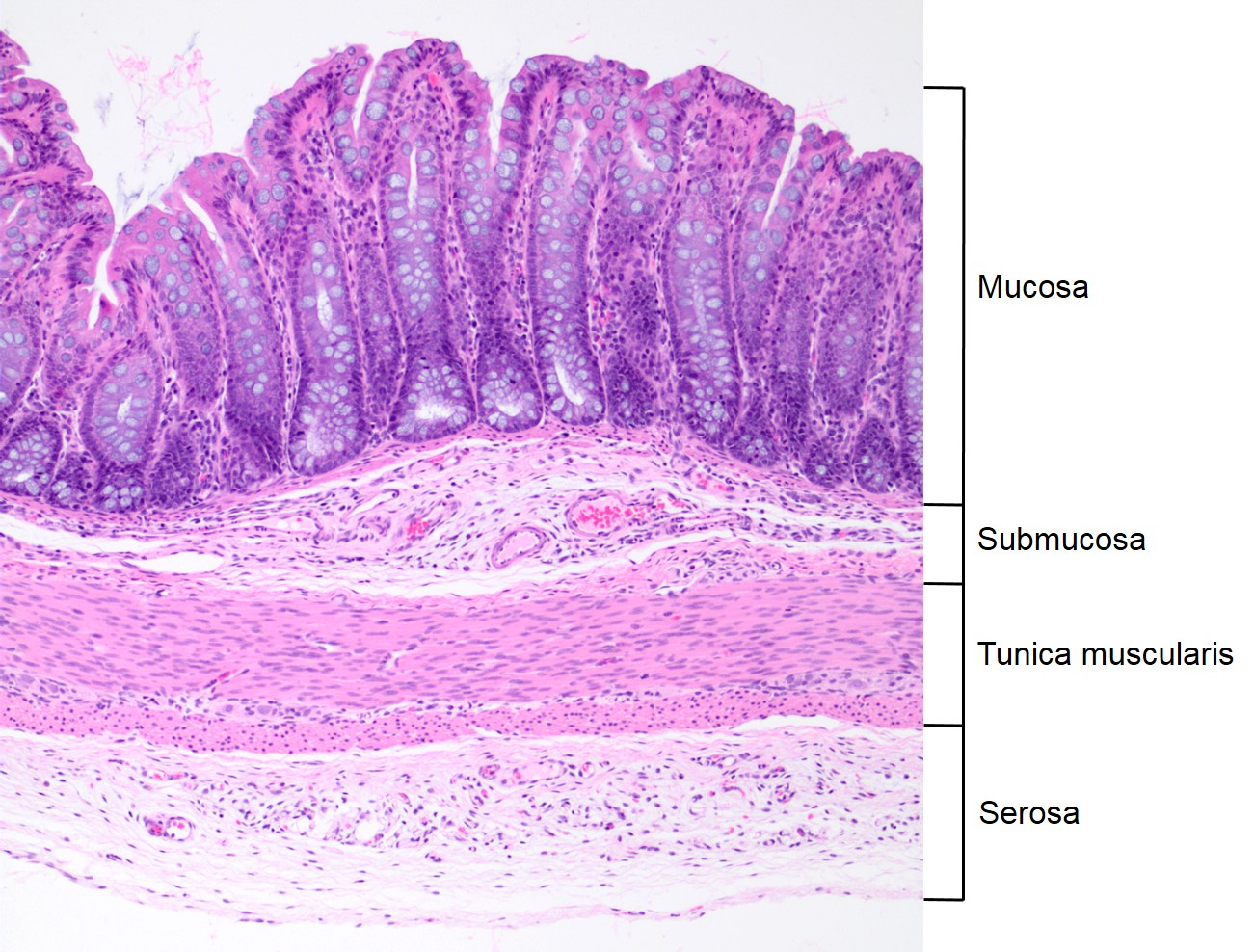
mucosa epithelium
pseudostratified columnar epithelium
sinus
warm & humidify air
hollow space produce mucous to trap stuff we don’t want in our lungs
weight of head (skull) produce mucous to trap
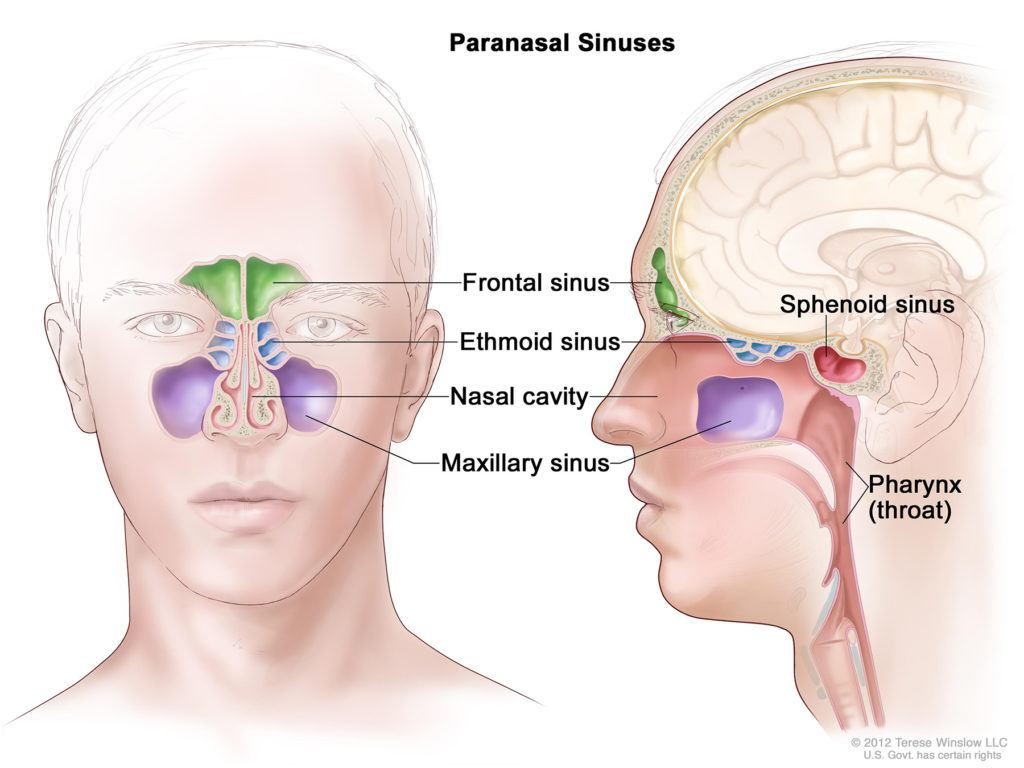
oral mucosa
moist, protective lining of mouth
essential for protection, sensation, oral function
stratified squamous epithelium
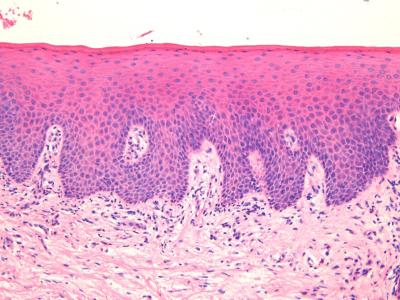
tonsils and adenoids
lymphoid tissue
plays important role in first line of defense efforts of immune systems
tonsils removed when bacteria accumulates
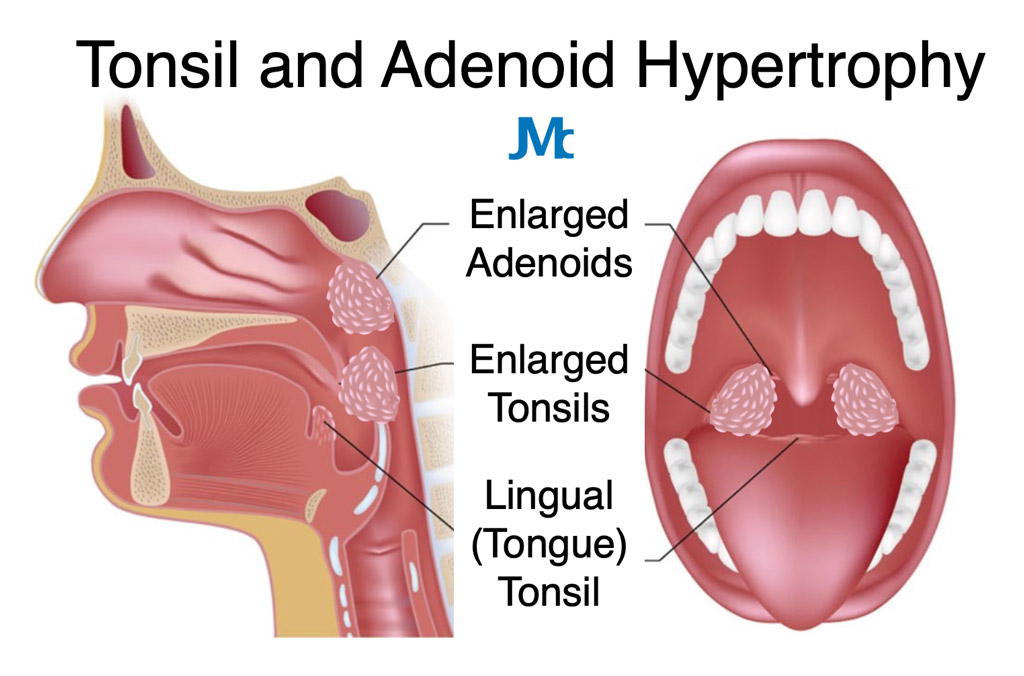
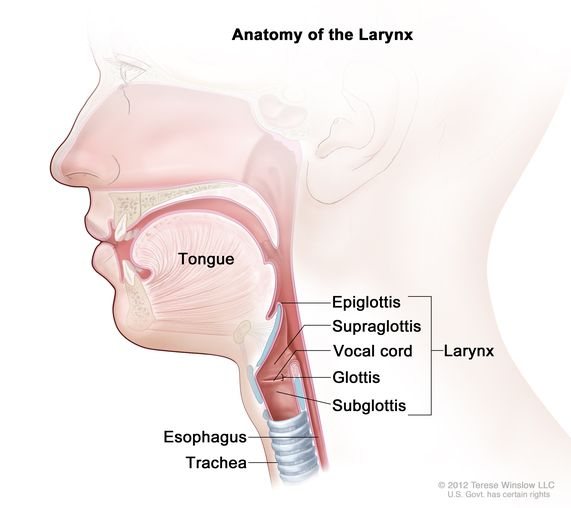
larynx
voicebox controlled by muscles
tracheal cartilage allows trachea to stay open to allow air in
epiglottis: flap closes to cover trachea
supraglottis
vocal cord
glottis
subglottis
thyroid cartilage: adam’s apple
growth of cartilage draws it anteriorly to stretch & lower voices in octave
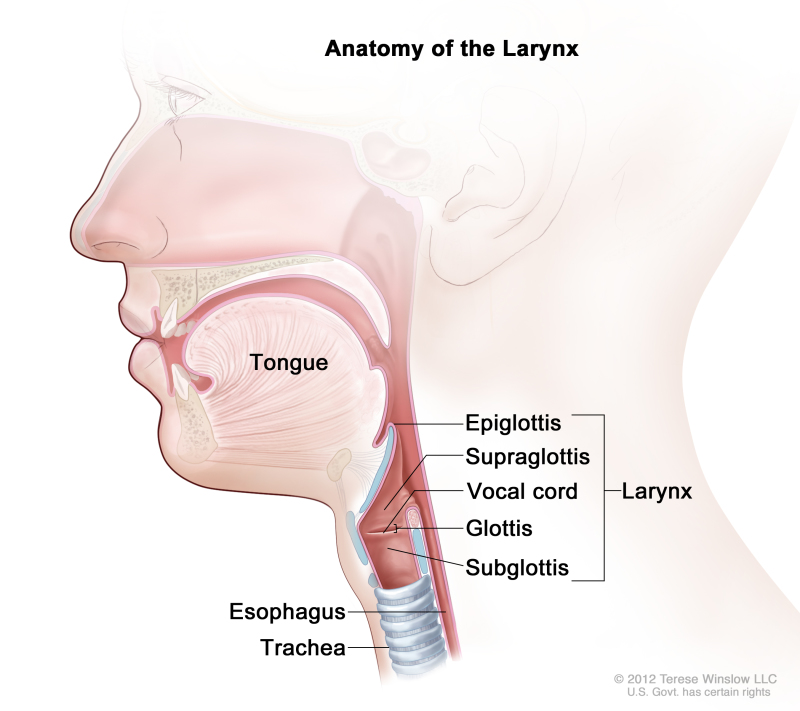
epiglottis
part of larynx
flap closes to cover trachea
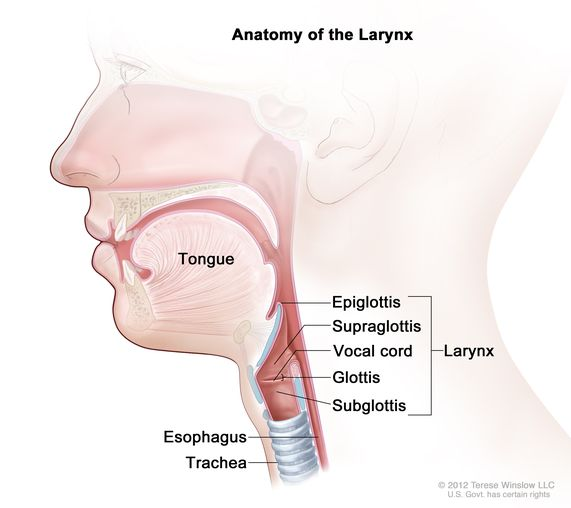
glottis
part of larynx
consist of vocal cords & openings between
voice production; muscles open/close → sound
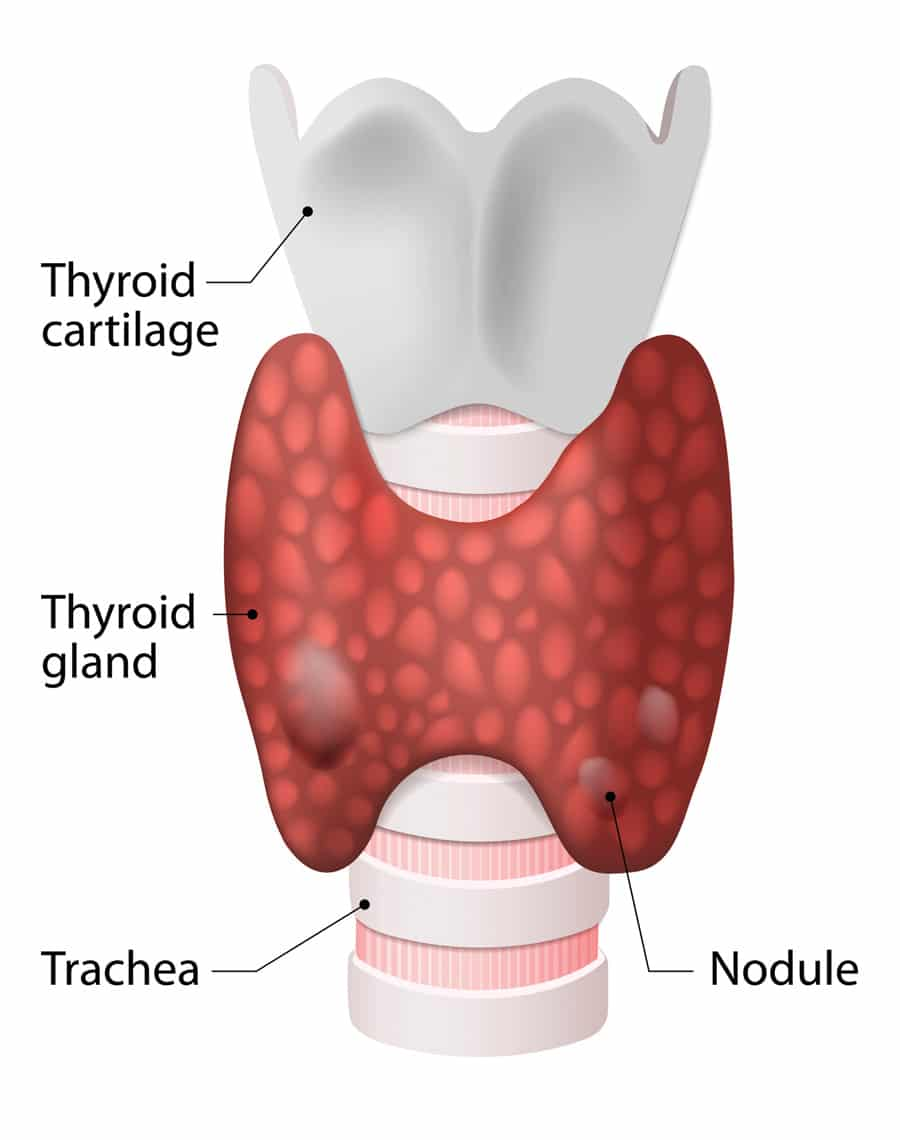
thyroid cartilage
part of larynx
adam’s apple
growth of cartilage draws it anteriorly to stretch & lower voices in octave
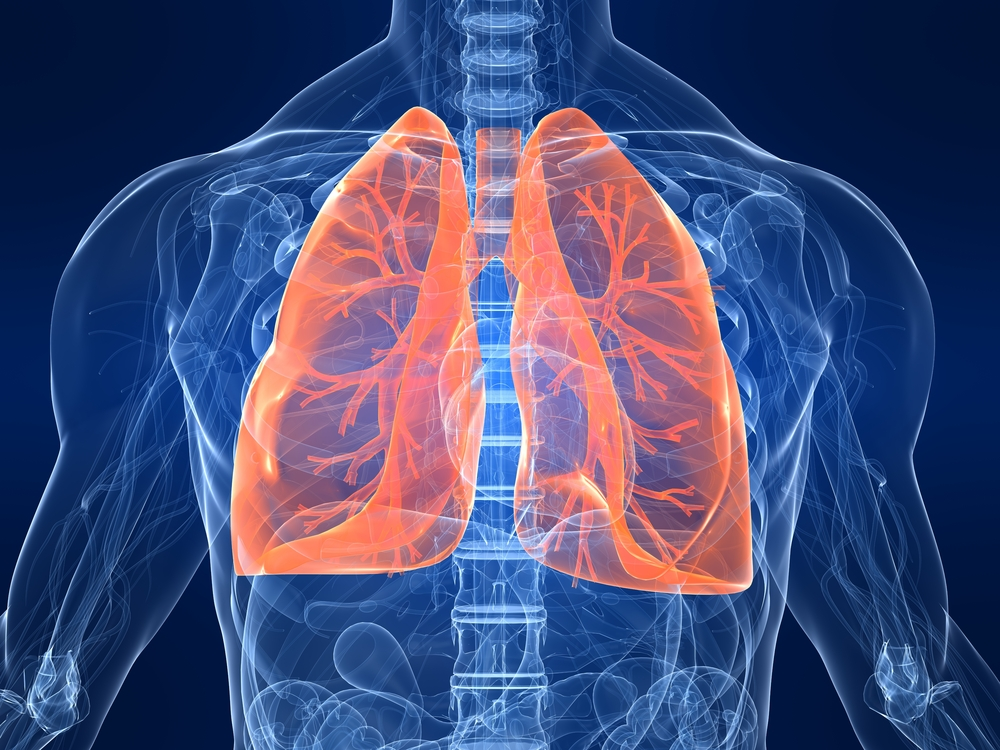
lung location
located in thoracic cavity
sits in pleural cavity
superior to diaphragm
flanks the heart (mediastinum)
lung surface anatomy
right lung:
3 lobes (superior, middle, inferior)
horizontal fissure
right oblique fissure
left lung:
2 lobes (superior, inferior)
left oblique fissure
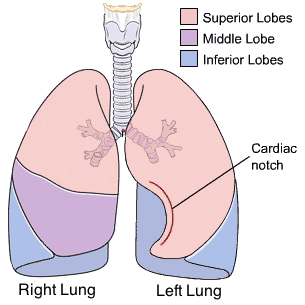
cardiac notch: makes space for apex of the heart
left lung has leess tissue
lingula
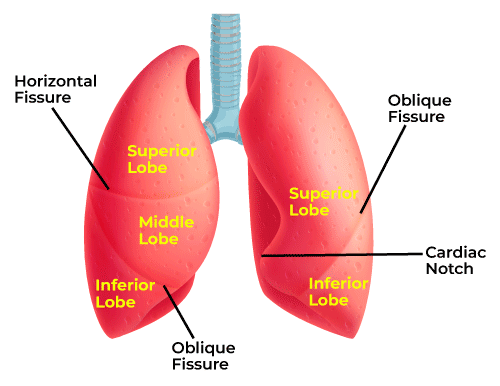
right lung
3 lobes (superior, middle, inferior)
horizontal fissure
right oblique fissure
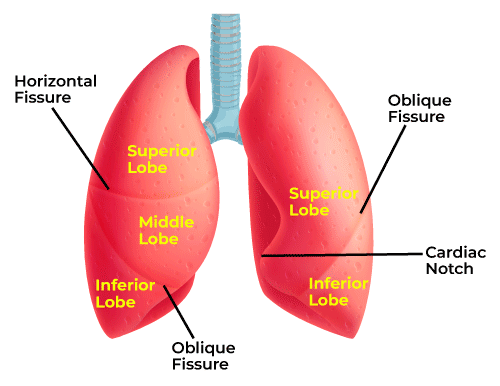
left lung
2 lobes (superior, inferior)
left oblique fissure
cardiac notch: makes space for apex of the heart
left lung has less tissue
lingula
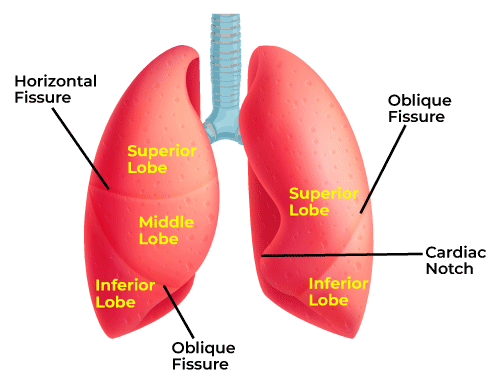
cardiac notch
makes space for apex of heart (left lung)
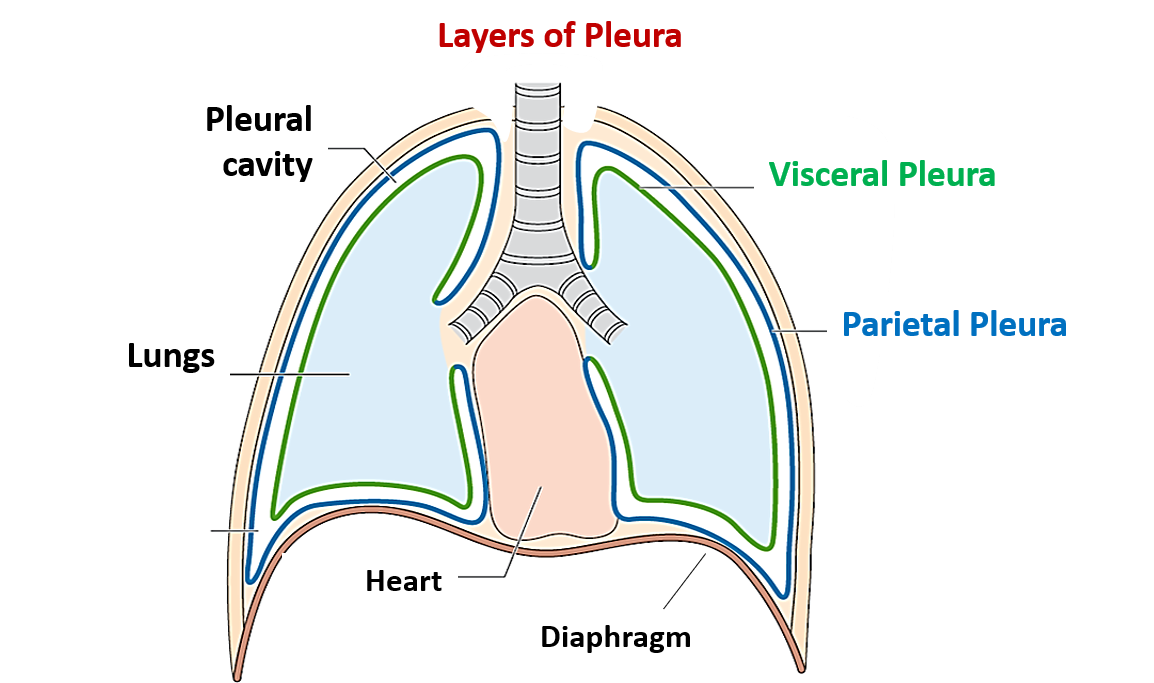
layers of the pleura
parietal pleura: outer
pleural cavity with intrapleural fluid: between
visceral pleura: inner
diaphragm: floor
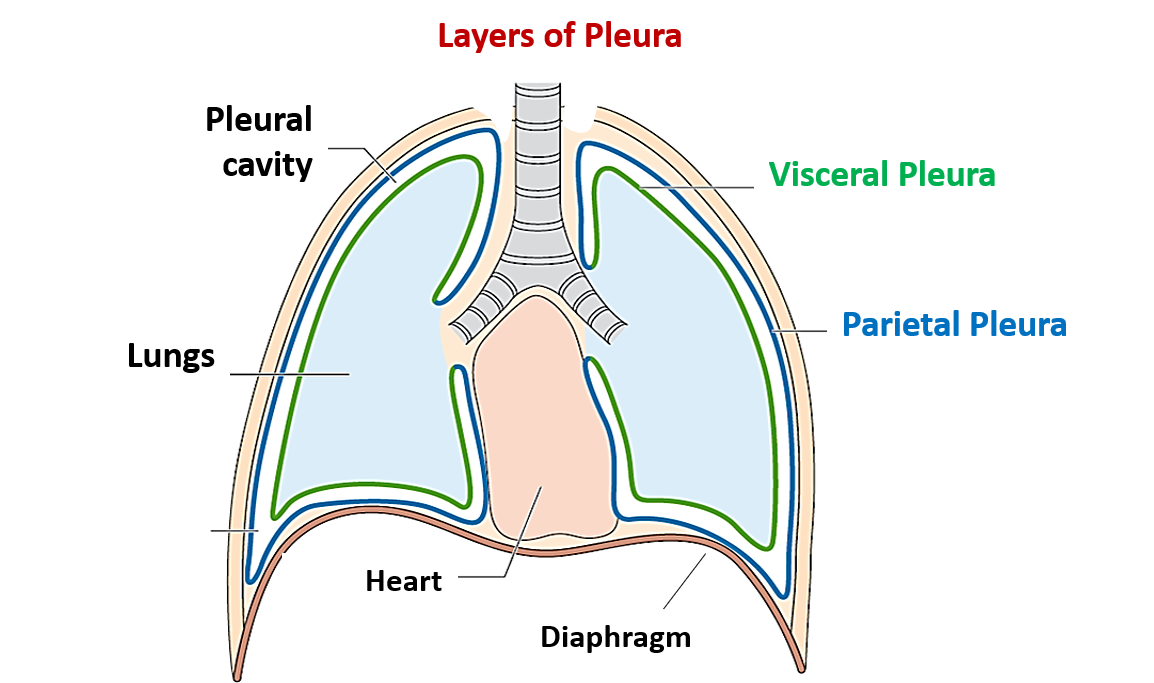
parietal pleura
outer layer of pleura
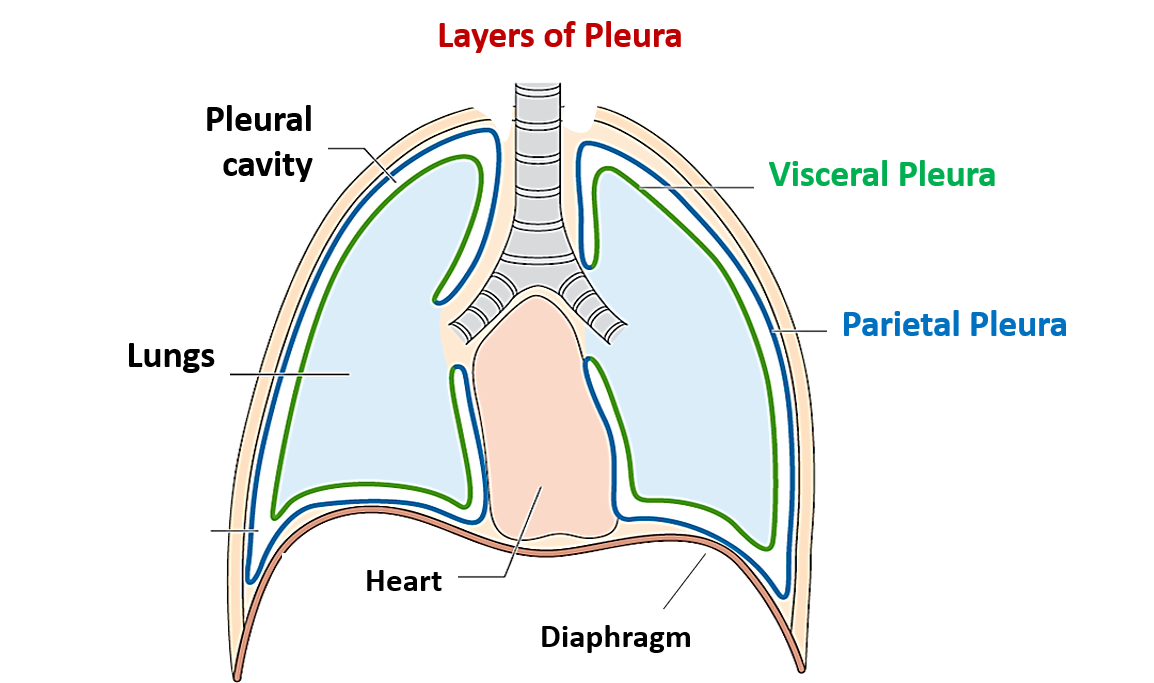
pleural cavity
filled with intrapleural fluid; siutated between parietal & visceral layers
help lungs expand & contract smoothly
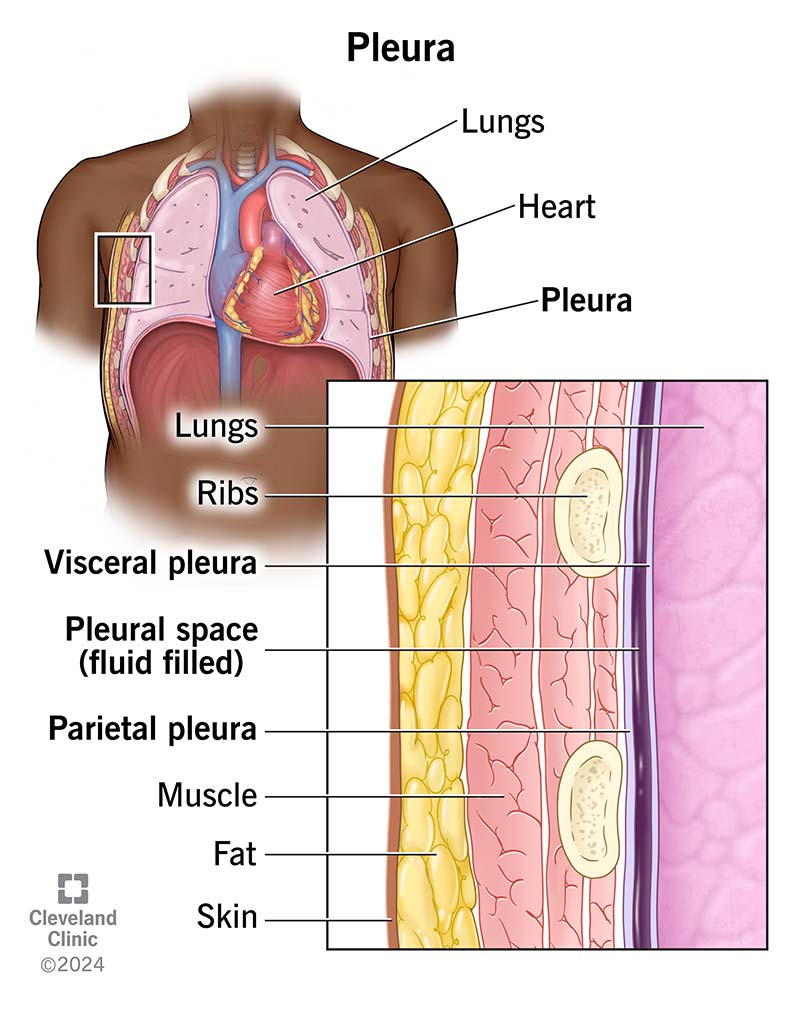
visceral pleura
inner layer of pleura
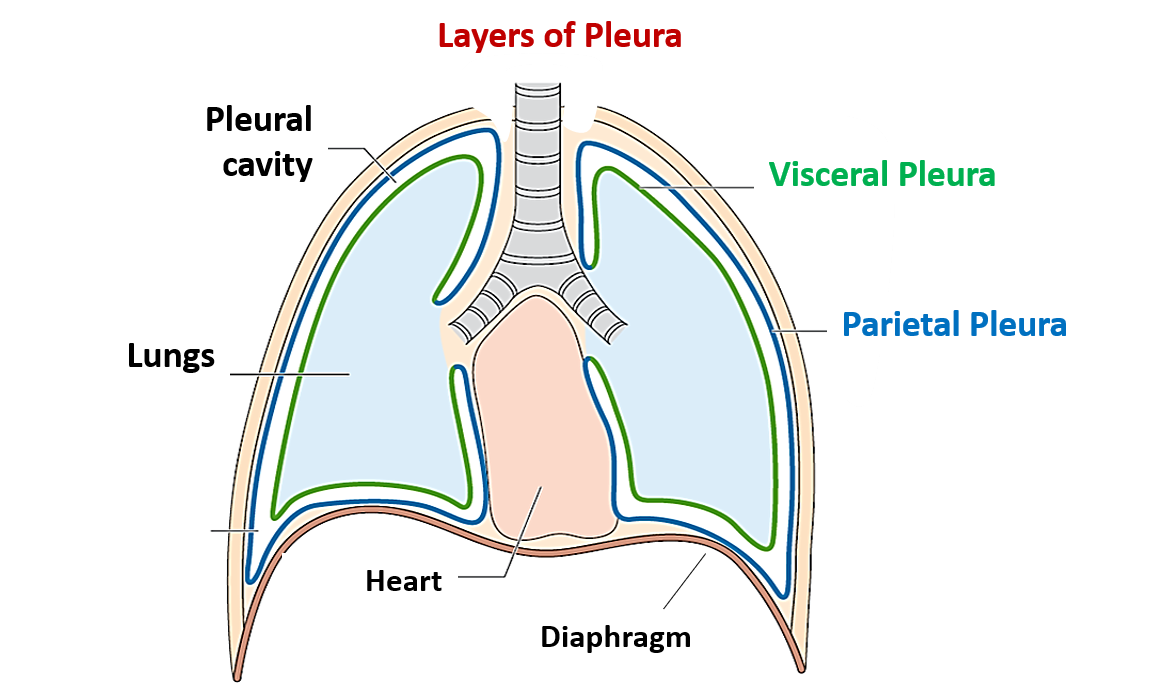
diaphragm (pleura)
floor of pleura
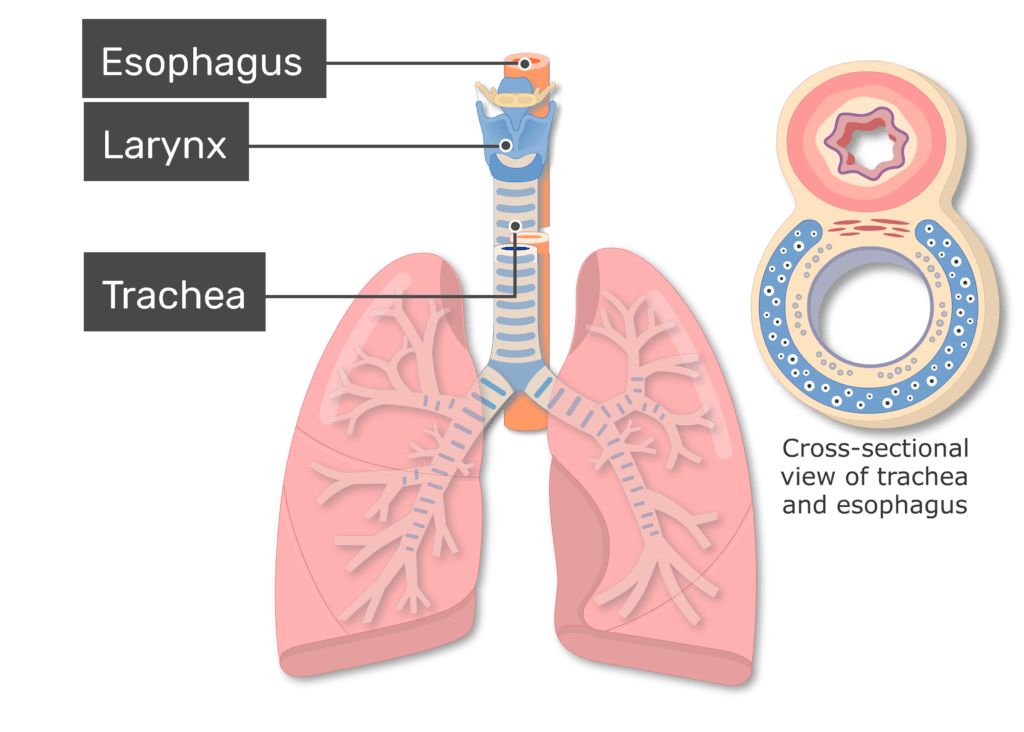
trachea
air passes down long tube connecting mouth + nasal cavity to rest of respiratory system
hyaline cartilage rings: sits on anterior & lateral surfaces
not posterior: esophagus
pseudostratified (ciliated) columnar epithelium
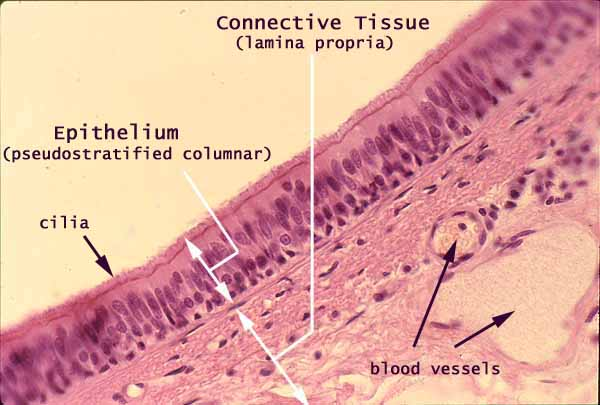
trachea epithelium
pseudostratified (ciliated) columnar epithelium
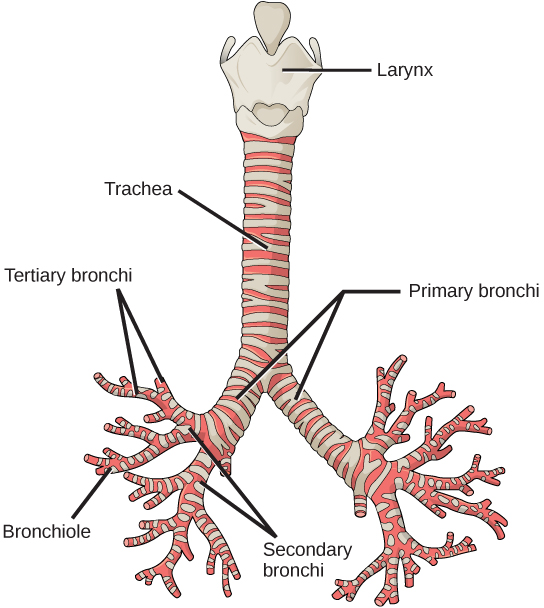
bronchus / bronchi
trachea branches off into two bronchi (bifurcation occurs keep to manubrium)
left main bronchus / right main bronchus
ciliated pseudostratified columnar epithelium lining
just like oral mucosa & trachea
bronchus / bronchi epithelium
ciliated pseudostratified columnar epithelium lining
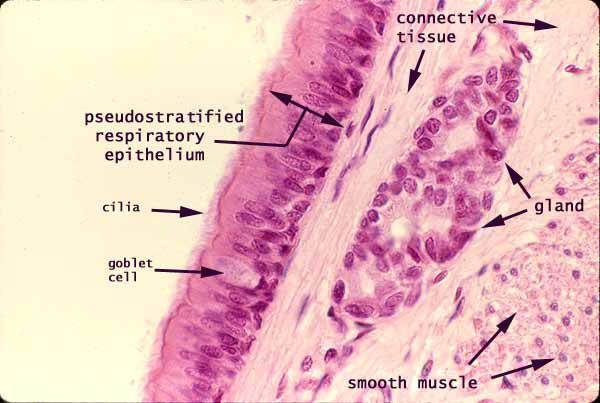
secondary bronchi / lobar bronchi
primary bronchi branch into smaller secondary tubes
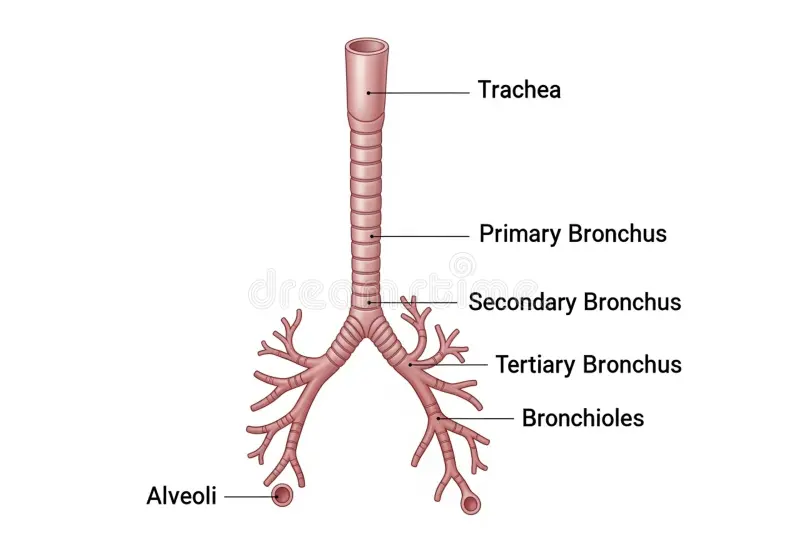
bronchioles
secondary bronchi / lobar bronchi branches off into small tubes
air passes
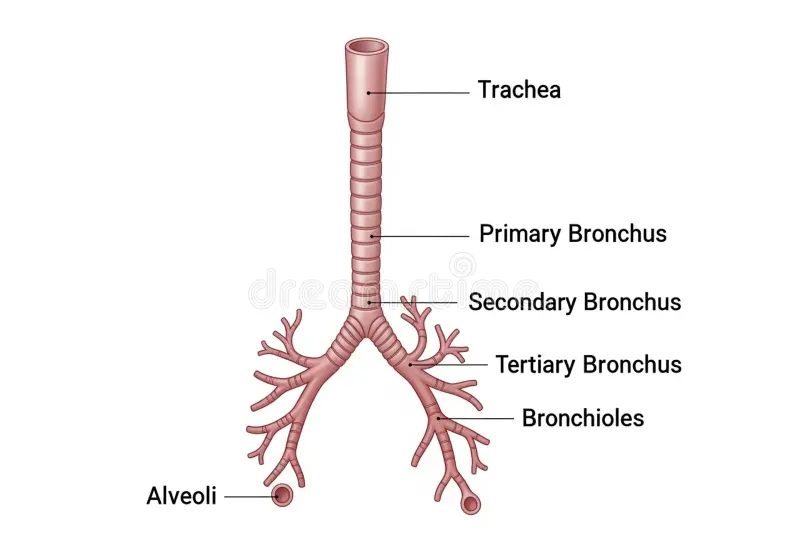
alveolus / alveoli
bronchioles terminal branches end in microscopic balloon-like air sacs
thin epithelium for readily capillary air exchange
site of gas exchange between air & bloodstream (oxygen inhaled, carbon dioxide exhaled)
covered in capillaries to allow gas exchange
deoxygenated blood from heart → alveolus
oxygenated blood from alveolus → heart
central open air sac
95% simple squamous epithelium
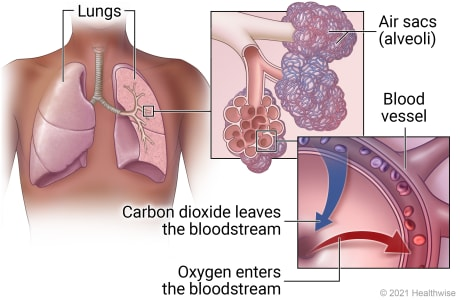
alveolus epithelium
simple squamous epithelium (95%)
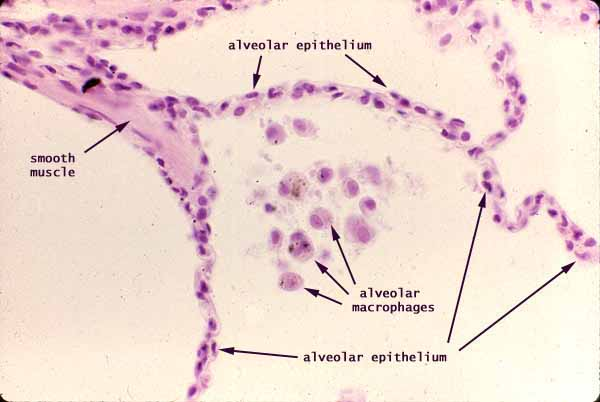
alveolus cells
type I cells: pneumocytes
thin, flat cells allow gas exchange between alveolus & capillaries
from birth; cannot replicate themselves
type II cells: progenitor (stem) cells
able to turn into more than one type of cell
replication & differentiation into type I cells
pneumocytes secrete surfactant to prevent collapse of alveolus & prevent innner walls from sticking together
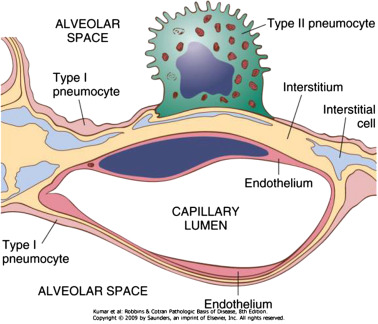
type I pneumocytes
alveoli cells (pneumocytes)
thin, flat cells allow gas exchange between alveolus & capillaries
from birth; cannot replicate themselves
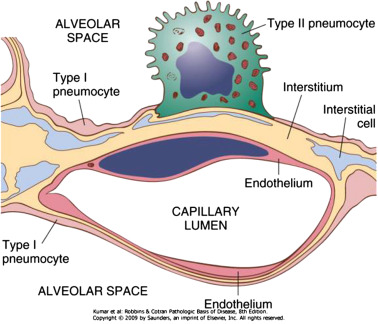
type II pneumocytes
alveoli cells (pneumocytes)
progenitor cells for replication & differentiation into different cells (i.e. type I cells)
secrete surfactant to prevent alveolus collapse & inner wall sticking
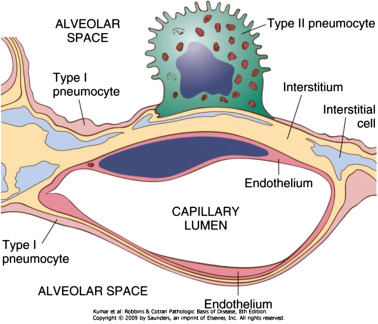
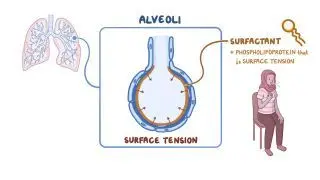
surfactant
hydrophilic lipoprotein secreted by type II alveolar cells
maintains strucutre of alveolus upon exhale
prevent deflating of sacs during exhalation by decreasing surface tension
production begins 24-28 weeks; premies (<32 weeks) may have respiratory distress syndrome
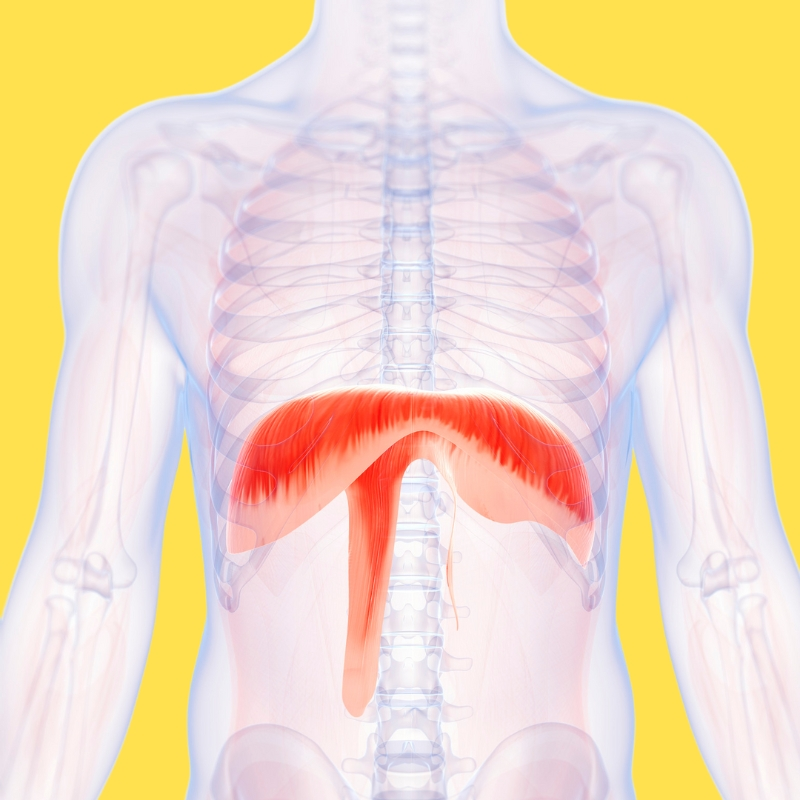
diaphragm
primary breathing muscle sheet (skeletal muscle)
facilitates inhalation & exhalation
maintain adominal pressure → aid digestion
inhalation: contracts and moves downward (bigger thoracic cavity)
exhalation: relaxes and moves upward
ribs flexible
thoracic cavity flexibility → ribs connected to cartilage
respiration muscles
principal:
diaphragm: increases thoracic cavity dimension, elevates lower ribs
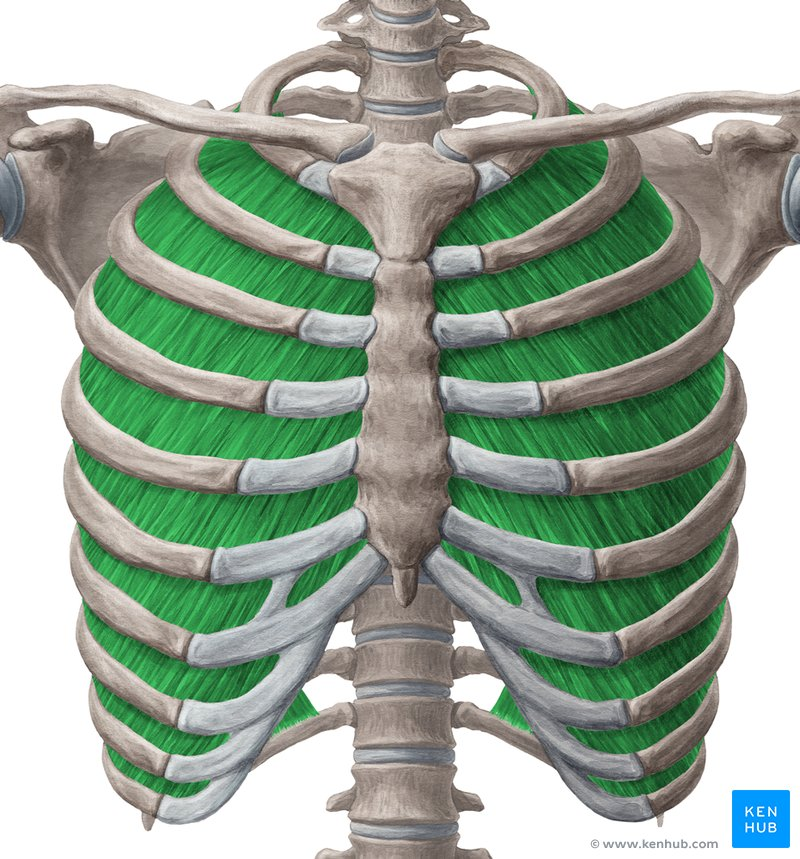
external intercostals: muscles in-between ribs
accessory:
sternocleidomastoid (elevates sternum)
scalenes (elevates upper ribs)
pectoralis minor
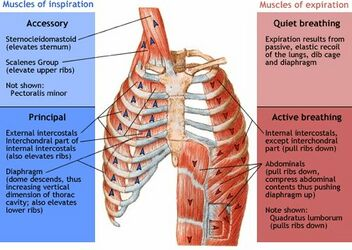
accessory muscles of inspiration
extra aid for respiration; last effort to get ribs to elevate, expand, open
sternocleidomastoid (elevates sternum)
scalenes (elevates upper ribs)
pectoralis minor
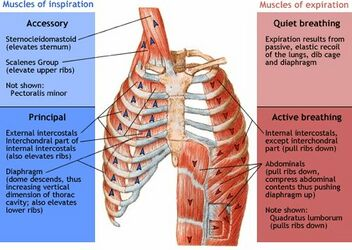
principal muscles of inspiration
main muscles for respitation
external intercostals (elevates ribs)
interchondral part of internal intercostals (elevates ribs)
diaphragm (dome descend to increase vertical dimension of thoracic cavity (elevates ribs))
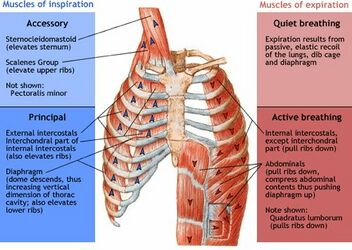
muscles of expiration
quiet breathing
passive, elastic recoil
lungs, rib cage, diaphragm
active breathing
internal intercostals (pull ribs down)
abdominalis (pull ribs down, compress abdominal contents to push diaphgram up)
quadratus lumborum (pulls ribs down)
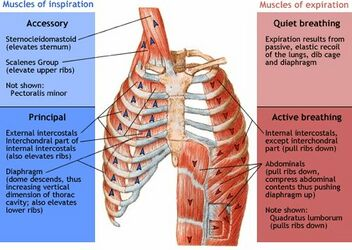
thoracic cage
ribs
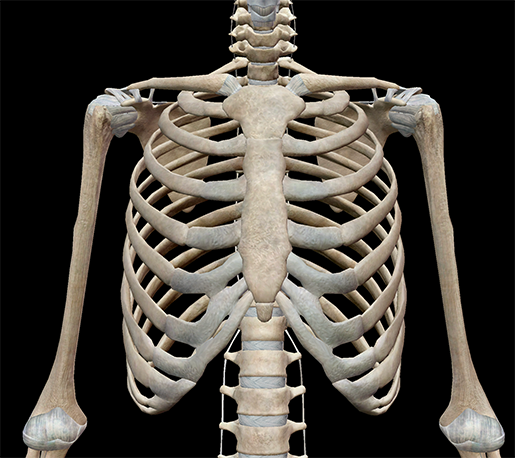
external intercostals
muscles in between ribs (superficial)
on external obliques
same fiber directions: superior → inferior ; lateral → medial
“hands in pockets”
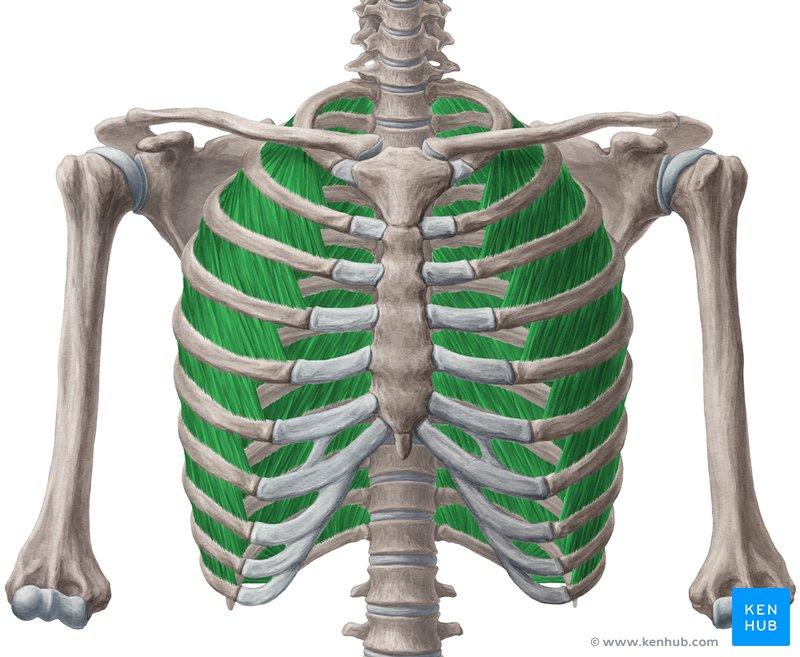
internal intercostals
same fiber directions: inferior → superior ; medial → lateral
breathing mechanics
air takes path of least resistance AWAY from pressure
inspiration: high out → low in
expiration: high in → low out
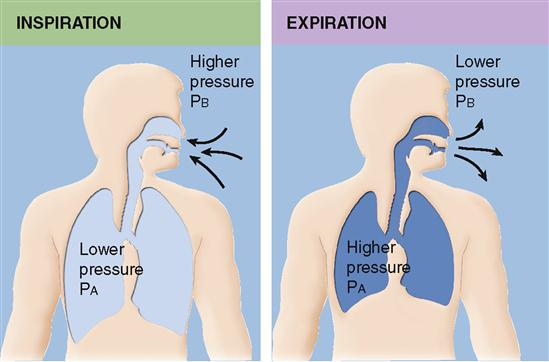
inspiration
high atmospheric pressure → low internal pressure
diaphgram contract downward
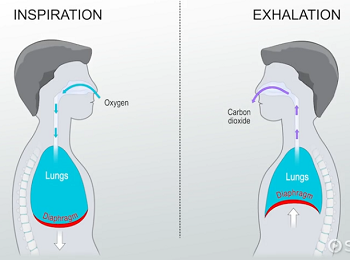
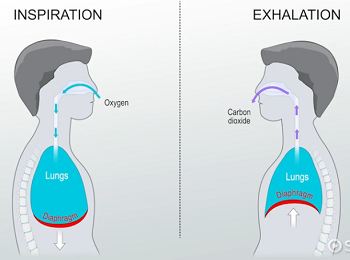
expiration
high internal pressure → low atmospheric pressure
diaphragm relax upward
sternocleidomastoid
accessory muscle elevates sternum
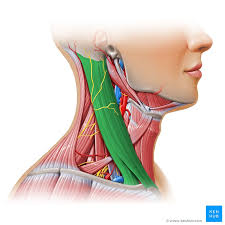
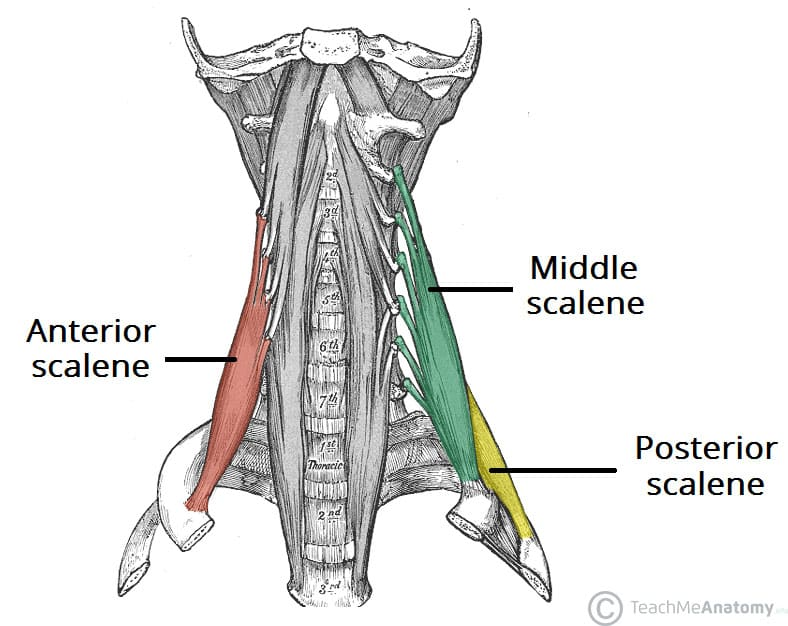
scalenes group
accessory muscle elevate upper ribs
quiet breathing
expiration from passive, elastic recoil
lungs
rib cage
diaphragm
active breathing
internal intercostals
abdominals
quadratic lumborum
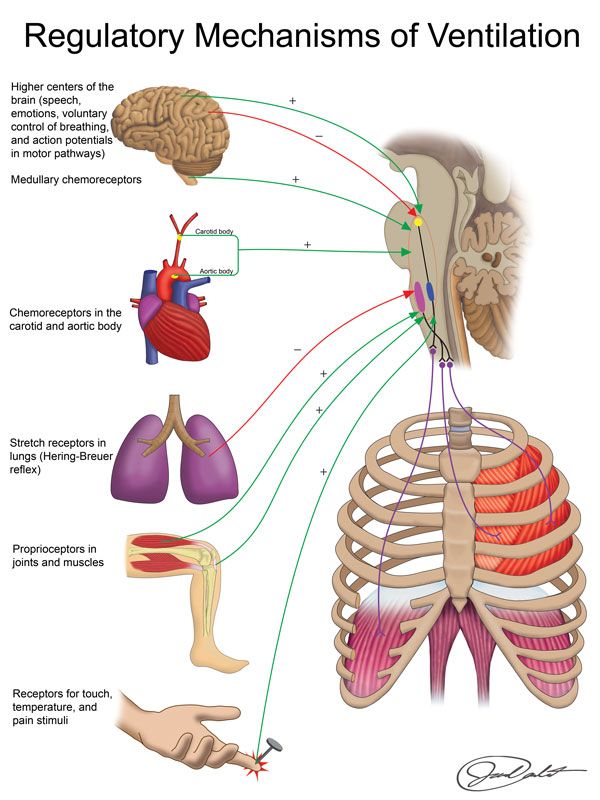
regulatory mechanisms of ventilation
voluntary control
involuntary control
higher centers of brain
chemoreceptors (medullary, carotid body, aortic body)
stretch receptors in lung
proprioceptors in joints & muscles
touch, temperature, pain stimuli receptors
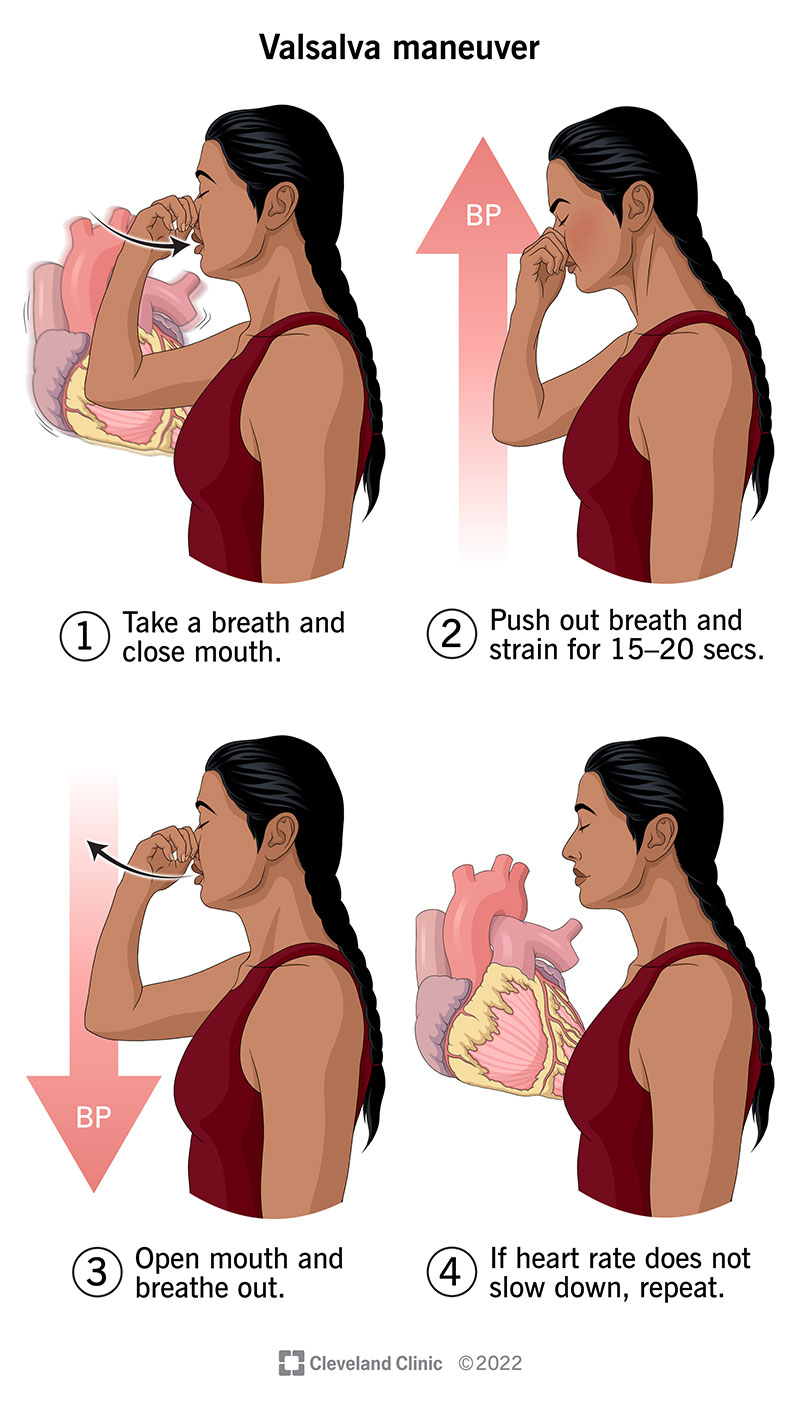
val salva manuever
take deep breath & pinch nostrils closed → increase internal pressure
increase pressure → pressure on heart and lungs → decreases cardiac output, decreases venous return, and decreases blood pressure
heart tells SA node to increase heart rate to compensate
blood pressure initially drops in brain → hold for more than 10-20 seconds → brain blood pressure increase → hemorrhagic stroke (especially in cardiovascularly compromised)
can cause passing out
cardiac output
volume of blood the heart pumps per minute