Lecture 2 -- Proteins and Lipids
1/21
Earn XP
Description and Tags
These flashcards cover key concepts of protein and lipid biochemistry, including measurement techniques, types of proteins, pathophysiological conditions, and the roles of lipoproteins in the body.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
22 Terms
What are the methods of measuring globulins?
Calculated by subtracting albumin from total protein (TP − albumin)
Measured directly using serum protein electrophoresis (SPE)
What is serum protein electrophoresis (SPE)?
Laboratory technique that separates serum proteins into distinct fractions (bands) based on their electrical charge and molecular size
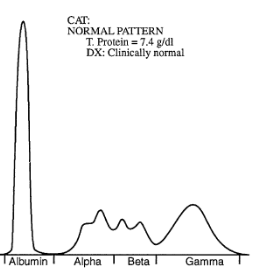
SPE from a dogs. What is the most likely diagnosis?
Normal
Albumin (Narrow base and spiky)
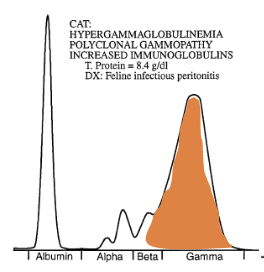
SPE from a dogs. What is the most likely diagnosis?
Chronic inflammation (Polyclonal gammopathy)
Increased production of gamma globulin BUT those gamma globulin are produced by different clones of B lymphocytes
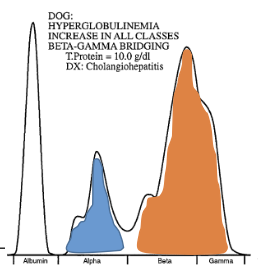
SPE from a dogs. What is the most likely diagnosis?
Actue phase or active inflammation (Polyclonal gammopahty)
Increased both alpha and gamma globulin
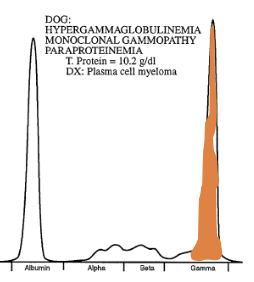
SPE from a dogs. What is the most likely diagnosis?
B cell neoplasia (Monoclonal gammopathy)
Only one clone of B lymphocytes or plasma cell producing the gamma globulin
What acute phase proteins are produced in response to inflammation?
Positive acute phase proteins:
C-reactive protein (CRP) in dogs
Serum amyloid A in ruminants, horses, and cats
Alpha-1 acid glycoprotein in cats
Negative acute phase proteins
Albumin
Transferrin
Delayed acute phase proteins
Complement proteins
Immunoglobulins
What is alpha-1 acid glycoprotein used for diagnosing in cats?
Feline infectious peritonitis (FIP)
What stimulates the liver to produce acute phase proteins?
Pro-inflammatory cytokines such as IL-1, IL-6, and TNF
What are the causes of hyperproteinaemia?
Inflammation (Increased globulin)
B-cell neoplasia (Increased globulin)
Vomiting, diarrhoea, polyuria
Relative increase due to dehydration or hemoconcentration, which leads to an increase in total protein without a true increase in protein production
What are the causes of hypoproteinaemia?
Blood loss
Third-space loss
Protein-losing dermatopathy
Protein-losing enteropathy
Protein-losing nephropathy
Hepatic insufficiency
Inflammation (decreased albumin)
Malabsorption
Malnutrition
Failure of passive transfer (in foals or calves)
Why is protein-losing nephropathy considered selective protein loss?
Globulin has a larger molecular size than albumin → Only albumin can pass through glomerulus
Why can hepatic insufficiency cause non-selective hypoproteinaemia?
The liver produces albumin and clotting factors, but immunoglobulins are produced by B lymphocytes, so protein changes are mixed
Which protein is selectively decreased in hypoproteinaemia caused by inflammation? Why?
Albumin
It a negative acute phase protein = Protein that decreases during inflammation
What are the causes of increased fibrinogen?
Increased fibrinogen + Decreased albumin → Indicates inflammation
Increased fibrinogen + albumin + total protein → Indicates Dehydration
What are the causes of decreased fibrinogen?
Decrease synthesis of fibrinogen
Hepatic insufficiency
Congenital deficiency
Afibrinogenaemia or hypofibrinogenaemia
Increased fibrinogen consumption
Disseminated intravascular coagulation (DIC)
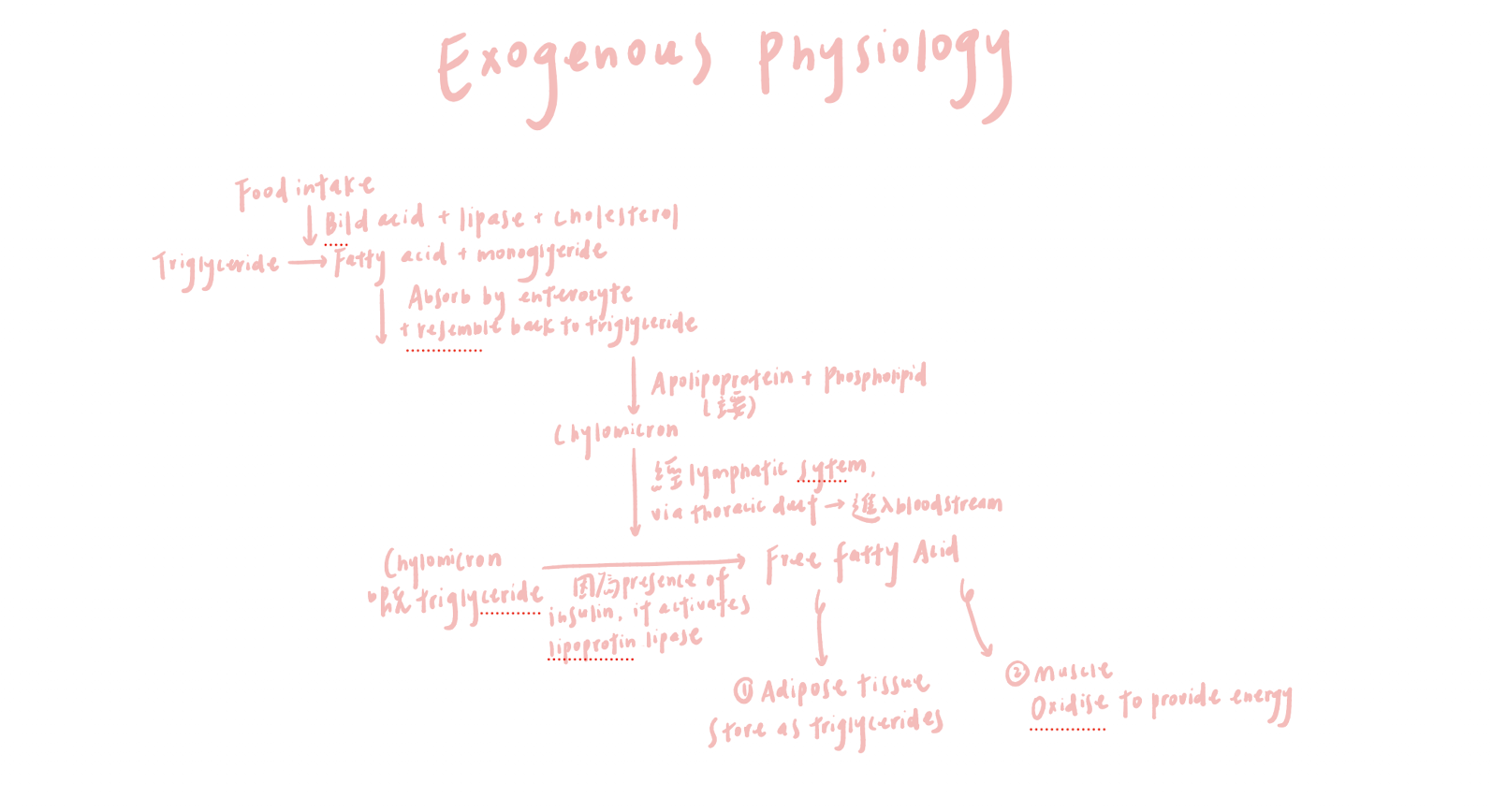
How are dietary lipids digested, transported, and used in the body?
Dietary lipids are digested in the intestine
With the help of bile acids, cholesterol, and lipase, producing free fatty acids and monoglycerides
Inside enterocytes, they are reassembled into triglycerides
With apolipoproteins and phospholipids, triglycerides form chylomicrons
Chylomicrons travel through the lymphatic system via the thoracic duct into the bloodstream
Insulin activates lipoprotein lipase → Breaks down the triglycerides in chylomicrons into free fatty acids
These fatty acids are then used by…
Adipose tissue for storage
Muscle for energy
How is VLDL metabolized and what is the role of LDL?
The liver synthesizes VLDL, which contains a high level of triglycerides
VLDL is broken down by lipoprotein lipase into free fatty acids, which are used by …
Adipose tissue for storage
Muscle for energy
VLDL is hydrolysed into intermediate-density lipoprotein (IDL) → Then hydrolysed into low-density lipoprotein (LDL)
LDL contains a high level of cholesterol, which is important for …
Maintaining cell membranes
Steroid hormone synthesis
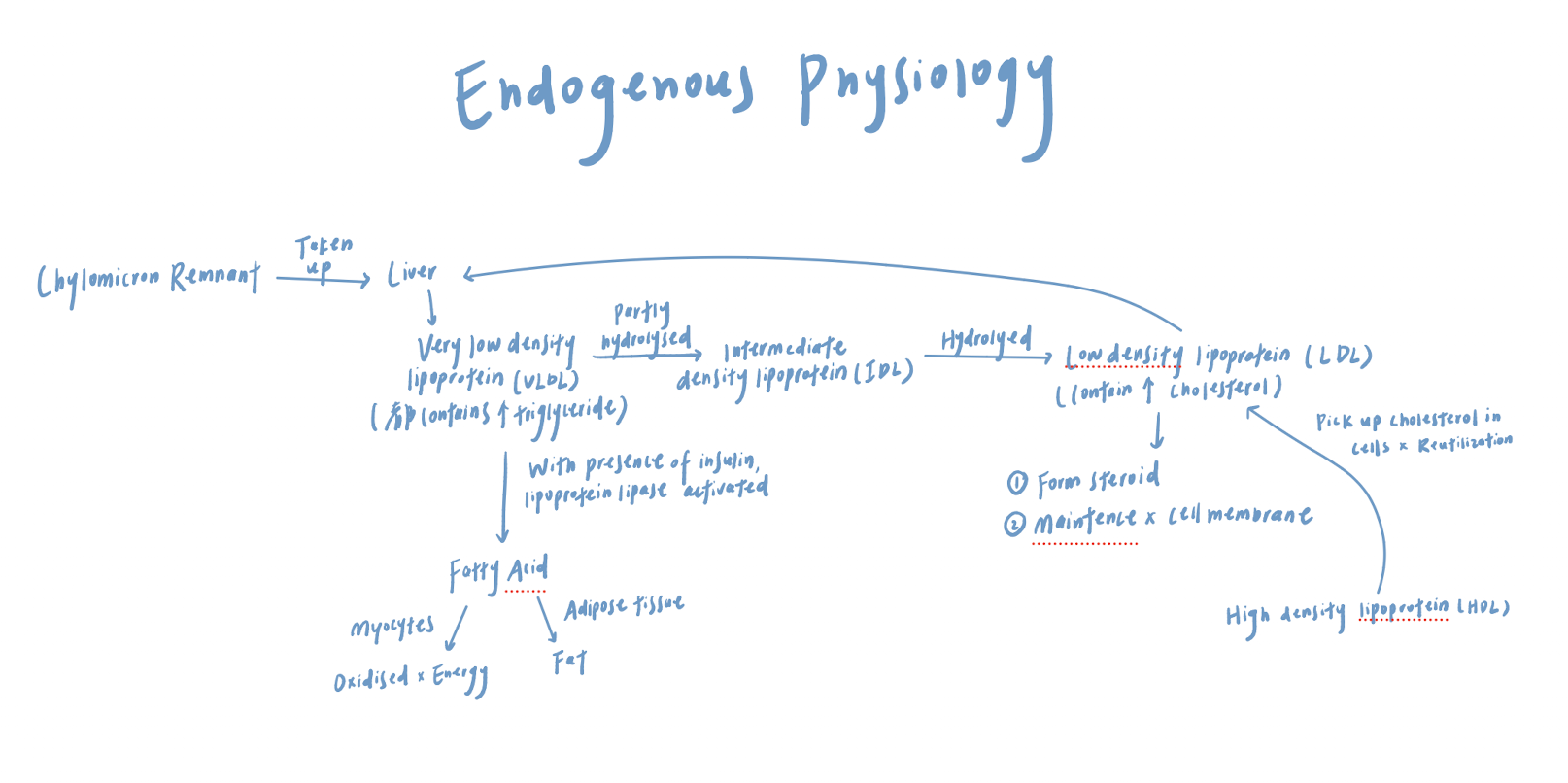
What is the function of high density lipoproteins?
Pick up the cholesterol from tissues for reutilisation or degradation
What are the causes of increased serum cholesterol?
Cholestasis
Acute pancreatitis
Because pancreatitis often associate with cholestasis
Nephrotic syndrome
Postprandial state/
Diet e.g. high fat diet
Obesity
Endocrine diseases (diabetes mellitus, hyperadrenocorticism, hypothyroidism)
Drug administration (e.g. glucocorticoids)
What are the causes of decreased serum cholesterol?
Pancreatic insufficiency
Cannot produce lipase → No breakdown into free fatty acid and monoglyceride)
Hepatic insufficiency
Portosystemic shunt (PSS)
Hypoadrenocorticism
Malabsorption or malnutrition
What are the causes of increased serum triglycerides?
Similar to causes of increased cholesterol
BUT NOT nephrotic syndrome and chloestasis