Laboratory Medicine and Hematopoiesis
1/75
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
76 Terms
Laboratory Quality Management
All the policies and procedures used to ensure that laboratory
results are reliable
Guidelines for Laboratory Quality Management are outlined by what organization?
American Society for Veterinary Clinical Pathology
Three types of laboratory error:
1.) pre-analytical
2.) analytical
3.) post-analytical
pre-analytical laboratory errors
occur prior to actual sample testing
Examples of pre-analytical laboratory errors
-not using correct patient and test
-not doing proper sample collection and handling
-not labeling and storage properly
-sample transport
Pre-analytical laboratory errors account for ___-___% of total errors!
52-77%
analytical laboratory errors
occurs during sample analysis by a pathologist
Examples of analytical laboratory errors
-equipment malfunction
-reagent expiration and degeneration
-pipetting errors
-quality control and assurance
post-analytical laboratory errors
errors that occur after results are generated
Examples of post-analytical laboratory errors
-transcription errors (writing wrong number/putting decimal in wrong place, etc)
-failure to report test results
-improper delivery of test results
-misinterpretation of results
Hematopoiesis
formation of blood cells; process through which all circulating blood cells are constantly regenerated
hematopoietic stem cells (HSC)
The cell type from which all lineages of blood cells arise
Where does hematopoiesis take place in adults?
red bone marrow (flat bones and ends of long bones)
Three things that are required for normal hematopoiesis:
1.) hematopoietic stem cells (HSC)
2.) growth factors
3.) bone marrow microenvironment
Hematopoietic tissue consists of three things:
1.) hematopoietic cells
2.) stromal tissue (fat, fibrous tissue)
3.) vascular sinuses lined by endothelium
hematopoietic stem cells (HSC) have the ability to _________ themselves through division
replenish
hematopoietic stem cells (HSC) differentiate into two main groups:
1.) myeloid progenitors
2.) lymphoid progenitors
Myeloid progenitors give rise to four cell types:
1.) RBCs
2.) granulocytes
3.) monocytes
4.) platelets
Lymphoid progenitors give rise to three cell types:
1.) T cells
2.) B cells
3.) natural killer cells
Erythropoiesis
Production of RBCs from
hematopoietic progenitor cells committed to the erythroid lineage
Two things required for erythropoiesis:
1.) iron
2.) erythropoietin (EPO)
iron for erythropoiesis is provided by...
macrophages
erythropoietin (EPO)
hormone secreted by the kidney to stimulate the production of red blood cells by bone marrow
The most immature stage of red blood cell development is called the...
rubriblast
Progression of Erythropoiesis starting with the rubriblast
rubriblast --> Prorubricyte --> Rubricyte --> Metrubricyte --> Polychromatophil --> mature RBC
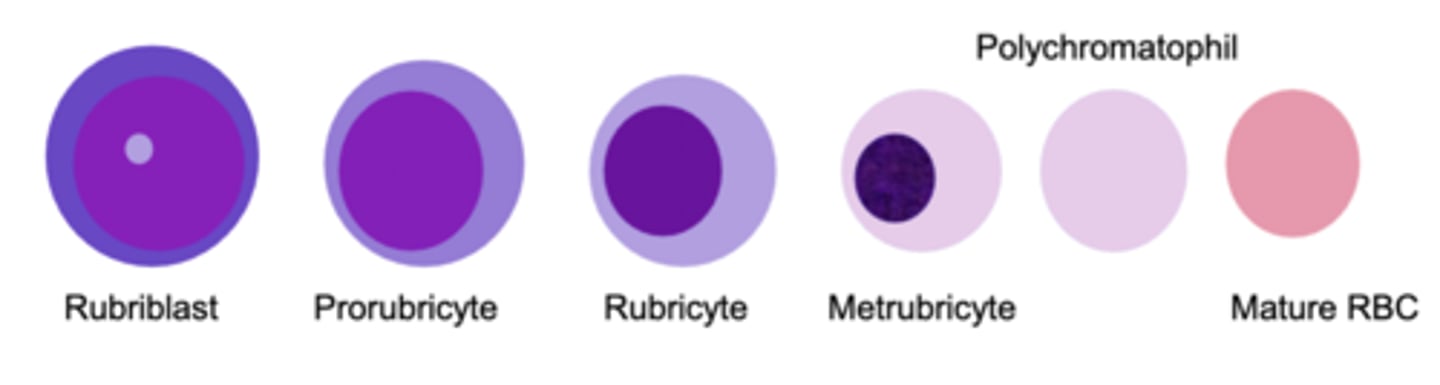
Process of erythropoiesis (4):
-cell size and nuclear size decrease
-chromatin condensation increases
-nuclei are extruded
-cytoplasm becomes less basophilic
Why does the cytoplasm become less basophilic during erythropoiesis?
due to hemoglobin production, which will make the cell appear pink, as opposed to purple color (basophilic)
How long does it take for a rubriblast to differentiate into a mature RBC?
approximately 7 days
What stage of erythropoiesis will have the nucleus completely extruded?
Polychromatophil
Granulopoiesis
Production of neutrophils, eosinophils, and basophils from common myeloid progenitors and myeloid precursors
Myeloblast
immature bone marrow that gives rise to granulocytes
Progression of Granulopoiesis starting with the myeloblast
myeloblast --> promyelocyte --> myelocyte --> metamyelocyte --> band --> mature
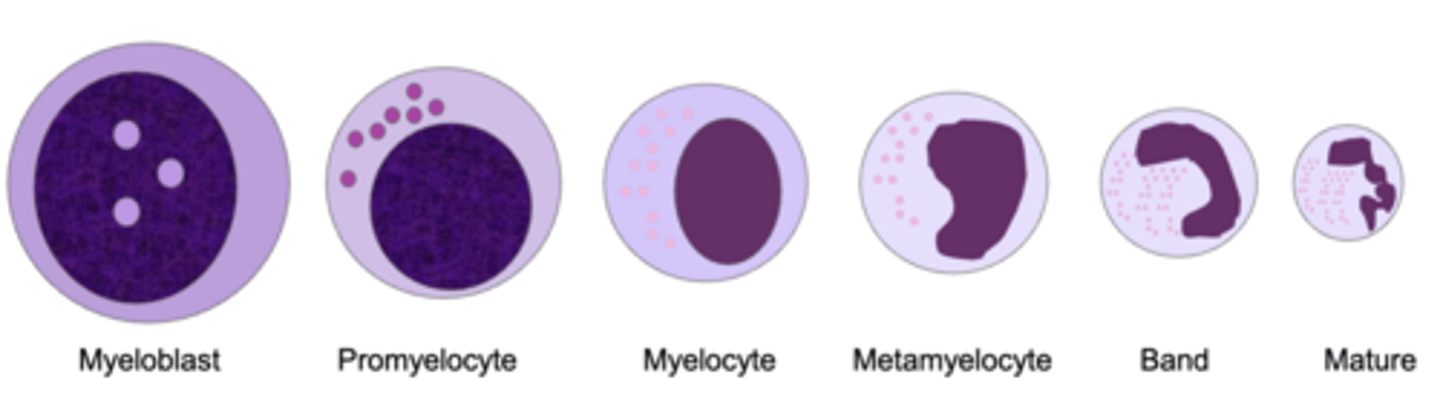
Process of Granulopoiesis (3)
-size decreases,
-chromatin becomes more
condensed
-nucleus becomes segmented
Thrombopoiesis
formation of platelets from megakaryoblast
Progression of thrombopoiesis starting with Megakaryoblast
Megakaryoblast --> promegakaryocyte --> megakaryocyte
During thrombopoiesis, the _________ does not divide
nucleus
Megakaryocytes
large cells that develop into platelets; produce
cytoplasmic extensions that protrude into the lumen of the sinuses and form platelets
What hormone regulates thrombopoiesis?
thrombopoietin (TPO)
Complete Blood Count (CBC)
Determination of numbers of blood cells, hemoglobin concentration, hematocrit, and red cell values-MCH, MCV, MCHC
Five components of a CBC
1.) Erythrogram
2.) Leukogram
3.) Thrombogram
4.) Microscopic blood smear review
5.) Plasma protein
Erythrogram
The red cell portion of a CBC; includes RBC count, hematocrit (HCT), and hemoglobin (Hgb)
hematocrit (HCT)
percentage of red blood cells in the blood; aka PCV
Five indications for a CBC
1.) Healthy animal screening test
2.) Sick animal baseline laboratory data
3.) Determine the need for additional testing
4.) Monitor disease progression
5.) Evaluate response to therapy
Collection of blood samples for CBC
clean venipuncture with minimal excitation; site used for collection depends on species
Lavender top tube
contains EDTA which is an anticoagulant for CBC in mammals
EDTA
calcium chelating (binding) agent that is used as an anticoagulant for laboratory blood specimens
Red top tube
Contains no additive or anticoagulant; used for biochemical profiles
Green top tube
Used for CBCs in non-
mammalian species
Blue top tube
contains sodium citrate; used for coagulation tests
Whole blood
blood in EDTA; blood from which none of the elements have been removed.
Centrifuged samples of blood separate into three layers:
1.) plasma
2.) buffy coat
3.) RBCs
plasma
fluid portion of blood collected in a lavender top tube; water, proteins, lipids, and clotting factors
plasma vs serum
Plasma has clotting factors serum doesn't
buffy coat
platelets and WBCs
What color tube is used during a CBC?
lavender top tube
True or false: you must gently mix the blood prior to performing a CBC
true!
Why must you gently mix the blood prior to performing a CBC?
to allow EDTA to be evenly distributed to prevent clotting
Three functions of RBCs
1.) Carry O2 to cells
2) remove CO2 from tissues
3.) circulate back to the lungs to get more O2
Why are RBCs red?
due to protein hemoglobin (Hgb)
hemoglobin
molecule that carries oxygen; requires iron!
Six factors evaluated on a CBC:
1.) hematocrit
2.) RBC number
3.) hemoglobin
4.) size
5.) color
6.) variation in RBC ssize
hematocrit
calculated value; percentage of all the blood that is due to RBC
*aka PCV
size of RBC is measured in...
MCV
MCV
mean corpuscular volume; average red blood cell size
Three size categories for red blood cells:
1.) normocytic (normal)
2.) macrocytic (large)
3.) microcytic (small)
color of a RBC is based on...
how much hemoglobin is present in a cell
Two was color of RBCs is evaluated:
1.) MCHC
2.) CHCM
MCHC
mean corpuscular hemoglobin concentration; average concentration of hemoglobin in the volume of blood
CHCM
Corpuscular hemoglobin concentration mean; average concentration of hemoglobin in a single red blood cell
Two categories for color of red blood cells:
1.) normochromatic
2.) hypochromatic
Variation in RBC size is measured using...
red cell distribution width (RDW)
red cell distribution width (RDW)
Determines the range of sizes of RBCs
Numbers from a CBC are compared to what value?
reference interval (RI)
Blood smears are prepared using what stains?
Wright's stain or quick stain (Diff-quik)
Wright's stain
used for identifying heinz bodies and reticulocytes
quick stain (Diff-quik)
used for routine evaluation of blood smears