Microbio - Chapter 15 Antimicrobial Drugs
1/84
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
85 Terms
______ are drugs against microbes
Antimicrobials
Antimicrobials are therapeutic compounds that _____ microbes or ______ to prevent pathogenic action
kill; inhibit their growth
Alexander Fleming noticed a plate of
Staphylococcus aureus was contaminated with mold and the bacteria were unable to grow near the mold
Mold ______ that could interfere with bacterial growth
excreted acompound
Named ______ after the species of contaminating mold
penicillin
____ was the 1st antibiotic tested clinically and mass produced
Penicillin
What are the basic criteria for drugs used as chemo-therapeutic agents?
effective against microbes
nontoxic to the host
able to be purified in high amounts
_______ is the range of different microbes against which an antimicrobial agent acts
Spectrum of activity
______ spectrum drugs are effective against a broad range of microbes
Broad
____ spectrum are antimicrobials that target a limited range of microbes
Narrow
______ spectrum drugs are effective against a single organism/disease
Limited
Why are narrow spectrum drugs preferred?
They present less disruption to the normal microbiota
_______ is medical treatment with a broad spectrum drug initiation while waiting for culture results
Empiric therapy
Broad spectrum antimicrobials may lead to the development of
superinfection
Ideal antimicrobials should meet as many of the following criteria as possible
1 Nontoxic to the host and without undesirable side effects
2. Nonallergenic to the host
3. Not eliminate the normal microbiota of the host
4. Able to reach the infected part of the human body
5. Inexpensive and easy to produce
6. Chemically-stable (have a long shelf-life)
7. Microbial resistance is uncommon and unlikely to develop
______ antimicrobials are substances produced by microorganisms that inhibit other living microorganisms
Naturally occurring (soil-dwelling microbes)
_______ antimicrobials are manufactured by chemical processes
Synthetic
______ antimicrobials have chemical modification of naturally occurring antibiotics
Semi-synthetic
_________ drugs result from each successive round of chemical modification
Next generation
Selective toxicity
inhibit/kill pathogen with little to no toxic effects on the patient
Selective toxicity is achieved by _______ for the drug in the microbe that do not exist in the patient
exploiting vulnerable targets
What bacteria processes are unique
cell wall synthesis, protein synthesis, or nucleic acid synthesis
The ratio of the toxic dose (to the patient) to the therapeutic dose (to eliminate the infection)
TI - Therapeutic Index
TI estimated the ________ of a drug
margin of safety
Margin of safety is the dose range where
drug efficacy is optimized while side effects are minimized
Drugs with a ____ TI have a large margin of safety and less danger of producing toxic effects
wide/high
Which organs are most susceptible to damage along with the microbiota?
Kidneys and liver
____ toxic to the liver
Hepatotoxic drugs
Toxic to the kidneys
Nephrotoxic
What is the preferred administration route?
oral administration
Why is oral administration preferred?
Easiest, most convenient, least cost
However, oral drugs must be
stable in the acidic environment of the stomach
Sufficiently absorbed in the intestines but not irritating to GI mucosa
____ administration is any route not involving the intestines
Parenteral
Advantages of parenteral administration include
Rapid absorption and faster onset of drug action
Intradermal/subcutaneously
under the skin
intravenously
into a vein
intramuscularly
into the muscle tissue
Half life is the time it takes for
half of a drug dose to be eliminated or deactivated by the body
____ half life requires frequent administration
short
antibiotics used to prevent infection
prophylaxis (broad)
____ therapy when organism is unknown but syndrome is known
Empirical (broad)
____ therapy when organism is known but susceptibility is unknown
Pathogen directed (narrow)
_____ therapy when organism is known and susceptibility is known
Susceptibility-guided (narrow and the goal)
______ stops the growth of bacteria
Bacteriostatic
______ kills the bacteria
Bactericidal
Bacteriostatic tend to target
bacterial protein/folic acid synthesis and metabolic pathways
With _______ antibacterial drugs, patient’s own immune system kills of the bacteria
bacteriostatic
Bactericidal tend to target
bacterial cell walls, cell membranes, or nucleic acids
What is the largest family of antibacterial drugs?
Beta-lactam superfamily
____ drugs do not destroy their target pathogen
Antiviral
What is the goal of antiviral drugs?
To inhibit viral development to treat active infection
Why is it hard to design safe and effective antiviral drugs?
Because viruses utilize host cell machinery for replication, making it challenging to target them without harming host cells.
Antiviral drugs can target
viral replication cycle
Antiviral drugs can stimulate
the host’s anti-viral immune system
____ the primary and most effective wat to reduce severe viral infection
Vaccinations
Drugs that target eukaryotic pathogens are limited by their
toxicity to host cells
Many eukaryotic drugs have a very narrow
therapeutic index
Mycoses
fungal infections
Antifungals target
fungal specific compounds
Antifungals interfere with _______ and _____ synthesis
Nucleic Acid - leads to failure of fungal cell replication
Cell wall - glucans/chitin
Antifungals also interfere with ______ causing death
cell membrane stability and structure - targets ergosterol
Eukaryotic parasites have a complex life cycle so drugs that target one stage may be
ineffective against other stages
Antiparasitic drugs target
intracellular components
Antiparasitic drugs function to
stun or kill
_____ drugs are limited by their toxicity
Antiparasitic
What does MIC stand for?
Minimum Inhibitory Concentration
_____ disk diffusion test determine susceptibility
Kirby Bauer
_____ test determines susceptibility and MIC
Epsilometer (E-test)
Describe Kirby Bauer Test
1. Drug-infused disks are placed on a freshly inoculated agar surface
2. Plates are incubated to allow for bacterial growth and drug diffusion from the disc
3. Zone of inhibition appears if the bacteria are prevented from growing
What is the zone of inhibition used for?
Compare diameter zone to a standard table
Determines if susceptible, resistant, or intermediate
What does MBC stand for?
Minimum Bactericidal Concentration
MIC determines the
lowest concentration of an antimicrobial agent that prevents visible growth
MBC determines the
lowest concentration of an antimicrobial agent required to kill the organsim
____ occurs when a microbe is not affected by a drug therapy that is intended to inhibit or eliminate the pathogen
Antimicrobial resistance
_____ resistance is natural resistance to antimicrobial drugs based on inherent microbial structure
Intrinsic resistance
Intrinsic resistance makes certain pathogens/infections _______
harder to treat/eliminate
IR - lacks a PG therefore intrinsically resistant to drugs that target CW synthesis
Mycoplasma pneumoniae
IR - forms endospores and resist to most antibiotics
Clostridium difficile
IR - waxy cell wall enriched with mycolic acid
Mycobacterium tuberculosis
Acquired resistance is acquired by
genetic mutation or acquisition of resistance genes
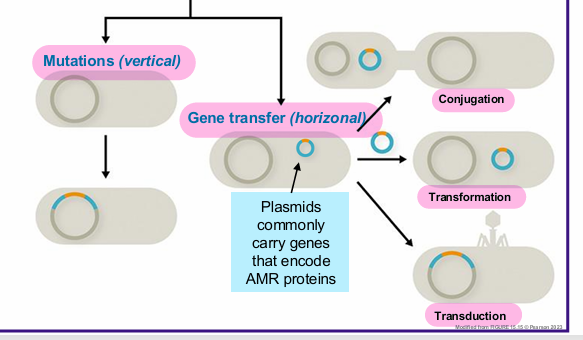
Acquired resistance occurs when drug concentration levels within the cell are
Kept below the MIC
How does acquired resistance work?
alter drug’s target
inactivate drug
reduced drug concentrations inside the cell (block entry or pump drug out)
strains of bacteria, viruses, parasites, and fungi that are resistant to the antimicrobials commonly used to treat the infections they cause
super bugs
results when superbugs emerge from the initial infection resistant to the treatment and become the primary cause of a second infection
superinfections
Antibiotic resistance is fueled by
natural selection