Muscle Bio Exam #4
1/113
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
114 Terms
Limb Girdle Muscular Dystrophy (LGMD)
describes a group of inherited diseases resulting from mutations in gene encoding proteins involved in maintaining skeletal muscle membrane stability
disease onset (2nd or 3rd decade)
Limb Girdle Muscular Dystrophy (LGMD) varies in time of…
Big muscles in hip and shoulder
For Limb Girdle Muscular Dystrophy (LGMD), ________ are affected first
milder; slower
LGMD has generally ____ and _____ progression than DMD
8; 15
LGMD can be divided into ____ autosomal dominant forms and ____ autosomal recessive forms
caveolinopathy
Caveolin Deficiency (LGMD1C) is known as…
autosomal dominant
caveolinopathy is an _______ for of LGMD; is very rare; and has a normal range of life expectancy
very distal form of myopathy (doesn’t affect the “things that matter” as much, such as heart and respiratory muscles)
why is caveolinopathy (LGMD1C) not as problematic of other forms of LGMD?
Myostatin
______ Inhibition Reverses Muscle Atrophy
mutant Cav and mutant MSTN
double Tg is __________ and is very similar to wild type
LGMD2B
Myoshi myopathy (MM)
Distal anterior compartment myopathy
Mutation in gene Dysferlinopathy (LGMD2B) gives rise to these 3 forms of muscular dystrophy
skeletal
Although dysferlin is expressed widely, its mutation affects only _____ muscle phenotype
muscle cell membrane repair
dysferlin plays an essential role in…
Sudden onset: late teens or early 20s
Inability to tiptoe
Calf pain and swelling
Good prior muscular prowess
Very high serum CK
Inflammation prominent (mostly T cells and macrophages)
Greatly reduces membrane repair efficiency of cardiac muscle
phenotype of Dysferlinopathy (LGMD2B)
Dysferlinopathy (LGMD2B)
diamond on quadriceps is a phenotypical sign of…
Sarcoglycanopathies (LGMD2C-F)
Collective name for a genetically and phenotypically heterogeneous group of muscular dystrophies caused by mutation of any of the four genes alpha, beta, gamma, delta; Severe childhood-onset autosomal recessive muscular dystrophy(SCARMD), Normal dystrophin levels but other DGC proteins are compromised
alpha-sarcoglycanopathy
First to be discovered and Most frequent form of Sarcoglycanopathies; Onset 8-10 months; Difficulties running and climbing stairs; Weak pelvic area muscles. Proximal muscles show marked atrophy while calf muscles are hypertrophic; Weakness in the scapular muscles; Trunk muscles affected and neck muscles spared; Advanced stage marked by muscle contracture; Cardiac function normal
CK; variation
alpha-sarcoglycanopathy has elevated levels of serum ___, and muscle biopsies show _____ in muscle fiver size
Myotonic Dystrophy
Inherited disorder of the muscles and other body systems; Most common form of muscular dystrophy that begins in adulthood
progressive muscle wasting and weakness, particularly in the lower legs, hands, neck, and face; Other defects may include cataract, cardiac conduction defect, infertility
Myotonic Dystrophy is characterized by…
second, third
phenotype for myotonic dystrophy usually occurs in the _____ or _____ decade
severity
______ varies widely among people with MMD/MD
Type I
there are two types of MMD/MD, is type I or type II more severe? (two types are caused by mutations in 2 different genes)
40,000
About ______ people in US have MD
dystrophia myotonica-protein kinase (DM-PK) gene (or CNBP for Type II)
MD is caused by a defect in…
triplet (CTG) repeats [severity varies with number of repeats]
MD is caused by _______ in the 3’ un-translated region of the gene (3’UTR)
Muscle weakness
Abnormal EMGs
Balding in the prefrontal area
Cataract
Genetic testing to look for CTG repeat
diagnosis of MD is based on…
Treating the manifestation of the disease:
Wheelchair
Orthotics
ECG to monitor heart performance
Pacemaker when necessary
Pain management
Hormone replacement for hyopgonadism
Cataract surgery if necessary
Genetic counseling
Treatment of MD
Emery-Dreifuss Muscular Dystrophy (EMD)
Due to a defect in either Emerin or Lamin A/C (nuclear membrane); Most common cause is defective emerin protein (1 in 100,000)
Can be inherited in X-linked (X-EDMD) autosomal recessive (Emerin) or Autosomal dominant form (AD-EDMD) as a result of defect in LMNA gene
Slowly progressive muscle weakness and wasting in shoulders/upper chest/back
Muscle contracture present
Onset in teen years
Heart problems may cause sudden death
Major cause of mortality and morbidity in EDMD is cardiac disease, which is consistently present
EMD phenotype
Facioscapulohumeral muscular dystrophy (FSHD)
third most common muscular dystrophy after DMD and MD; First described in 1886 as Landouzy Dejerine; Prevalence is 1:20,000
Usually adult onset - Age 20 for men; Age 30 for women'; Only 5% children
Progresses very slowly
Facial muscle weakness - Eyelids, Whistling, Pronunciation
Shoulder weakness
Weakening of arm muscles - Do not respond to exercise
Phenotype of Facioscapulohumeral muscular dystrophy (FSHD)
autosomal dominant; D4Z4; 4
cause of Facioscapulohumeral muscular dystrophy (FSHD) - _________ inheritance; due to deletion of ____ repeat of chromosome ___
DUX4 (DUX4 usually silent due to tight heterochromatin packing; As a result of deletion, the DNA is less tightly packed and DUX4 is more available for transcription)
Usually have 11-150 repeats of D4Z4; Less than 11 as well as overexpression of _____ leads to FSHD – toxic gain of function
transcriptional activator; zygotic genome activation; embryo genesis
DUX4 acts as a _________, likely stimulating ________ during early __________. Its expression is normally restricted to cleavage stage embryos, testes, and thymus, and it is silenced in most adult somatic tissues
toxic gain of function
Misexpression of DUX4 triggers a _________, causing apoptosis, oxidative stress, and chronic inflammation in muscle cells, which results in muscle weakness and atrophy over time
no
Are there any drugs to treat FSHD?
Accumulation of genetic damage or mutations in genes, chromosomes, and mitochondria
Loss of immune functions and autoimmunity
Accumulation of insoluble aggregates
Abnormal modification of proteins
Damage by reactive oxygen species (ROS)
Hormone imbalance and a decline in homeostasis
causes of aging
Sarcopenia
Involuntary loss of lean muscle mass as a result of ageing; Often associated with increase in fat
10-24; 30
_____% in 65-70 year olds and over ____% muscle loss in those over 80
growth hormone; IGF-1; sex hormone; cytokine production
sarcopenia causes a decrease in _____, _____, and ______, and increased _______
chronic malnutrition, sedentary life style, and smoking
sarcopenia is enhanced by…
25-50
Ageing process is associated with a _____% reduction of the a-motoneurons (a-MN). Small MN, which are more preserved than large a-MN, continue to innervate type I fibers
IGF-1
overexpression of ______ prevents type IIb myosin loss in mice due to aging
64; 28
Testosterone levels decrease by ___% in males between the age of 25 and 85; In females there is ___% decline in the levels of bio-available testosterone between ages 25 and 85
women
Decline in bio-available testosterone is not linked to decreased muscle mass and strength in _______
cross sectional area; cell number and myogenesis; cancer
Testosterone dosing increases __________ of type I and II fibers; Testosterone promotes muscle growth by increasing _________; Giving Tstne as a supplement increases risk of ________
Cachexia
Complex condition that involves weight loss, lipolysis, loss of muscle, and some visceral protein, anorexia, chronic nausea, and weakness
Some autoimmune disorders
Addiction to certain drugs
Chronic obstructive pulmonary disease
Congestive heart failure
Cancer
AIDS
Tuberculosis
common causes of Cachexia
you lose both at the same time (which is not typical, usually when losing weight you should lose fat first and then muscle)
In cachexia, do you lose muscle or fat first?
spindle, striated
smooth muscle is ____ shaped and is not ____
parallel, series
smooth muscle forces add in _____, not in _____
actin
Smooth muscle has higher ratio of _____ filaments
directional
smooth muscle has greater _____ freedom
6:1; 15:1
Actin:Myosin for smooth is ____ while it is ____ for striated
We don’t know!
How is force of smooth muscle maintained even after signal turns off?
neurotransmitters, hormones, drugs, stretch
Ca Entry into Smooth Muscle can be caused by…
Vascular
Respiratory
Urinary
Reproductive
Gastrointestinal
Ocular
common places where there are smooth muscle disorders
75
Premature births account for ___% of all neonatal death
12
___% of US births are premature
50
In ___% of cases, the cause of premature births is never determined
quiescent phase
As myometrium stretches, leads to increased chance of contractility, yet it doesn’t occur; This “uncoupling” is known as ________
CAP
Upregulation of endogenous inhibitors causes “coupling” again; ____ proteins signal “coupling”
Caldesmon; ERK activation; Caldesmon phosphorylation at ERK sites
______ increases during pregnancy; ______ increases during labor; ___________ increases during labor
ERK
____ Inhibitor Delays Onset of Labor
cardiovascular disease (CVD)
leading cause of death in the world
Age, gender, hypertension, cholesterol, smoking, alcohol, family history, metabolic syndrome (obesity, diabetes), physical inactivity, aortic stiffness
risk factors to cardiovascular events
Aortic stiffening
________ transmits increased pulse pressure to more fragile peripheral vessels.
ECM, calcification
what contributes to aortic stiffness?
focal adhesions
smooth muscle stiffness can be regulated via…
formation; maintenance; repair
Myogenesis is fundamental to the ______, ______ and _____ of skeletal muscle and associated tissues
myoblasts; multinucleated myofibers
Skeletal muscle development requires the formation of ______ that can fuse with each other to form ______________
birth
Distinct primary, secondary, slow, fast myofibers are formed by the time of _____; These fibers arise at distinct stages of development: embryonic, fetal and perinatal
build, break down, mature
blast (_____), clast (_____), cyte (____)
myocytes, myofibers
Myoblasts receive a cue to develop into ______ which aggregate into ______
KNOW THIS IMAGE FOR EXAM!!!
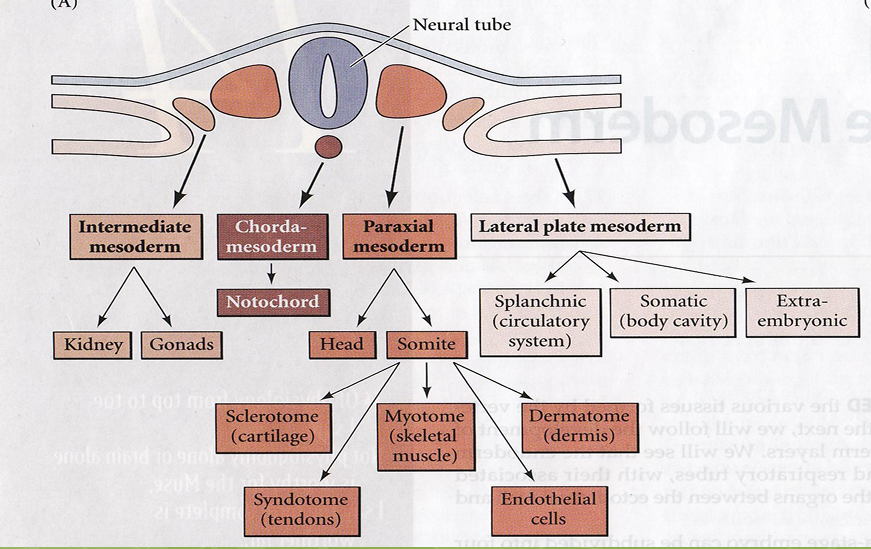
ectoderm; mesoderm; endoderm
zygote blastula gastrula differentiates into ____, ____ and _____
ectoderm
develops/differentiates into epidermis and associated structures and the brain and nervous system
endoderm
develops/differentiates into inner lining of digestive tract, glands, and inner lining of respiratory tract
mesoderm
develops/differentiates into notochord, somites (further develops into muscle), and mensenchyme (further develops into heart and circulatory system)
segmented somites
The paraxial mesoderm will develop into…
muscle, dermis, cartilage, tendons, and the axial skeleton
Somites are transient embryonic structures that later give rise to…
segmented somites
The paraxial mesoderm will develop into…
somites
Limb and trunk muscle arise from the _____
non-somitic paraxial mesoderm
Head muscles arise from the _______________ that is with in the developing head region
back muscles (epaxial)
Dorsal –medial portion of the somite give rise to _________
Abdominal and body wall (hypaxial)
Ventral lateral portion of the somites give rise to _________
limb field; lateral lip of dermomyotome
At the limb level, the cells predetermined to form skeletal muscle migrate to the _______ from ________
head
Somites migrate from head down (rostral to caudal), thus maturing near _____ first
Basic Helix Loop Helix protein
Consist of 2 alpha-helices connected at a fixed angle by a short stretch of polypeptide chain (the “turn”)
E-box; major
Basic Helix Loop Helix protein- Recognition helix recognizes and bind to specific DNA sequences (____) by forming H-bonds with bases located in the _____ groove
hydrophobic; recognition
Basic Helix Loop Helix protein- Second helix stabilizes the overall configuration through _______ interactions with the _______ helix; Generally dimeric
Muscle Regulatory factors (MRFs)
a family of basic helix-loop-helix (b HLH) transcription factors that regulate myogenesis
MyoD
Myf 5
Myogenin
MRF4
examples of Muscle Regulatory factors (MRFs)
differentiated skeletal muscle cells
Muscle Regulatory factors (MRFs), when over expressed in fibroblasts, converts the cells to ______________ that transcriptionally activate expression of muscle-specific genes such as myosin and actin
MyoD; Myf5
_____ and _____ are the earliest markers of myogenic cells. However, they are expressed in specific spatio-temporal fashion at earlier stage but later they overlap
epaxial; hypaxial
Myf5 is expressed in the cells that will give rise to _____ muscles and MyoD is expressed in cells that give rise to _____ muscles, although at a later point than Myf5
there is no muscle development, will lead to embryonic death
if you double knock out MyoD and Myf5…
Myogenin
______ is required for late but not early aspects of myogenesis during mouse development
severe skeletal muscle reduction (Myoblasts form and proliferate, but never differentiate into myocytes)
knocking out myogenin leads to…