APA 4118 wrist and hand
1/204
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
205 Terms
What is the wrist joint complex composed of?
Eight carpal bones, distal radius, structures in ulnocarpal space, and metacarpals.
What bones make up the proximal row of the wrist? features?
Lunate and triquetrum (lacks MSK attachments, motion occurs indirectly 2ndary to movement of distal row)
What is the function of the scaphoid in the wrist?
Functions as a bridge between the proximal and distal rows and coordinates their motion.
How does flexion and extension occur in the wrist (row theory)?
Through motion between the proximal and distal rows of carpal bones.
How does flexion and extension occur in the wrist (column theory)?
occurs through articulations in central column
where do radial and ulnar deviation occur in the wrist (row theory)?
articulation of scaphoid and radius
where do radial and ulnar deviation occur in the wrist (column theory)?
rotation of scaphoid and triquetrum about central colum
What is the radial column of the wrist composed of?
Scaphoid, trapezium, and trapezoid.
Distal row of the wrist
trapezium, trapezoid, capitate, hamate. tightly bound to metacarpals, move as a rigid unit
What is the central column of the wrist composed of?
Capitate, hamate, and lunate.
What is the ulnar column of the wrist composed of?
Triquetrum.
Do row and column theories adequately describe wrist function?
No, but still useful for grouping anatomically.
what is a thumb digital ray
metacarpal, 2 phalanges
what is a finger digital ray
metacarpal, 3 phalanges
What are the three arches of the hand?
Proximal transverse, distal transverse, and longitudinal arch.
What is the keystone of the proximal transverse arch?
Capitate (fixed position)
What is the keystone of the distal transverse arch?
Head of the third metacarpal (more mobile)
what is the longitudinal arch comprised of?
digital rays+ proximal carpus (2nd+3rd mcp’s are central pillar)
what is the organization of the arches?
the 2 transverse arches are connected by a rigid section of longitudinal arch
What are the consequences of a collapsed arch
severe disability/deformity
What role do intrinsic muscles play in the hand?
They maintain the shape of the arches of the hand.
What are the three peripheral nerves that innervate the wrist and hand?
Radial, median, and ulnar nerves.
What is the primary function of the radial nerve?
Innervates wrist flexor/extensor muscles and affects hand grasp.
What is the primary function of the median nerve?
Innervates long wrist and hand extrinsic flexors, affecting fine motor skills.
What is the primary function of the ulnar nerve?
Innervates ulnar hand flexors and hand intrinsics, providing power for grasp.
What can cause a collapse in the arches of the hand?
Injury, rheumatic disease, or paralysis of intrinsic muscles.
How does the dorsal skin of the hand differ from the palmar skin?
Dorsal skin is thin, mobile, and flexible, while palmar skin is thick, glabrous, and less elastic.
What is the impact of median nerve impairment?
Affects the radial flexor muscles and compromises fine motor skills in the first three digits.Ulnar flexors less impacted
What is the consequence of ulnar nerve irritation or compression?
May impair hand function and power for grasp.
What is the primary cause of carpal tunnel syndrome?
Pressure on the median nerve within the carpal tunnel.
What are common symptoms of carpal tunnel syndrome?
Numbness, tingling, and/or pain in the wrist, hand, or fingers. Weakness/trouble grasping objects
risk factors for carpal tunnel?
anatomy: smaller carpal tunnel, fracture
work involving vibrating tools, repetitive wrist + hand motions
diabetes, menopause, hypothyroidism, obesity, rheumatoid arthritis, pregnancy
theorized to be related to hormonal changes, no evidence
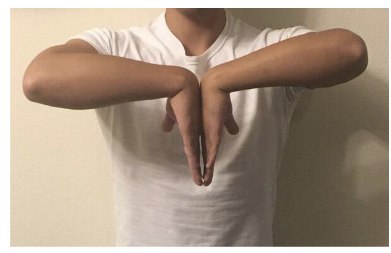
What is the Phalen test used for?
To diagnose carpal tunnel syndrome by reproducing symptoms when the wrist is flexed.
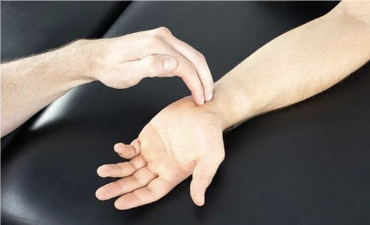
What indicates a positive Tinel test?
A tingling or prickling sensation felt when lightly tapping over the nerve distal to the site of injury.
What is the typical demographic affected by carpal tunnel syndrome?
Approximately 1 in 10 people develop carpal tunnel syndrome at some point. Most common nerve entrapment syndrome
What are the two rows of carpal bones?
Proximal row: scaphoid, lunate, triquetrum, pisiform; Distal row: trapezium, trapezoid, capitate, hamate.
What is the significance of the carpal tunnel syndrome diagnosis?
It confirms compression of the median nerve, often leading to treatment options like surgery.
should static resting splints be used to treat rheumatoid arthritis (study)?
RCT evaluated static resting splints + OT vs OT alone in early rheumatoid arthritis over 12 months. No added benefit of splints for grip strength, pain, dexterity, function, or deformity. Study was well-designed but limited by poor adherence and self-reported compliance. Conclusion: static resting splints should not be routine and should be used selectively based on individual patient needs.
What non-surgical treatments are recommended for carpal tunnel syndrome?
Patient education, ergonomic tools, splints, and physical therapy.
What is the sensitivity and specificity of Tinel's sign?
Sensitivity: 38-100%, Specificity: 55-100%.
What is the sensitivity and specificity of Phalen's sign?
Sensitivity: 42-85%, Specificity: 54-98%.
What role does nerve conduction studies play in diagnosing carpal tunnel syndrome?
They determine the degree of demyelination and axonal loss.
What is the role of corticosteroids in treating carpal tunnel syndrome?
They are used to reduce inflammation and relieve symptoms.
What is the purpose of using splints in carpal tunnel syndrome treatment?
To immobilize the wrist and reduce pressure on the median nerve.
What is the clinical relevance of understanding wrist anatomy?
It aids in diagnosing and treating musculoskeletal disorders affecting wrist function.
What is the anticipated impact of findings from research on musculoskeletal disorders?
To improve treatment methods and patient outcomes for conditions like carpal tunnel syndrome.
What tests are used to diagnose carpal tunnel syndrome?
Tinel's sign and Phalen's sign are used for diagnosis, along with nerve conduction studies.
What is the most effective treatment for carpal tunnel syndrome?
Surgical release of the carpal tunnel by transaction of the transverse carpal ligament is considered the most effective treatment.
biomechanical effects of carpal tunnel surgery
inc carpal arch width and carpal tunnel volume, reduced strength, alteration of alignment + tracking of piso-triquetral joint, possible pillar pain, palmar displacement of flexor tendons/bowstringing (inc tendon travel distance, may cause musc weakness)
What is the expected outcome of surgery for carpal tunnel syndrome?
Surgery is more effective at resolving symptoms long-term compared to corticosteroids.
What is the effectiveness of ultrasound in diagnosing carpal tunnel syndrome?
Ultrasound can reveal morphological changes in the nerve, with sensitivity of 77.6% and specificity of 86.8%.
What arteries supply blood to the wrist and hand?
Ulnar and radial arteries
What can threaten the cycle of vasodilation-vasoconstriction in the hand?
Injury or disease
consequences of vasodilation/constriction cycle issues in the hand?
progressive wrist edema leading to pathology
what makes blood supply to the hand unique?
complex/dense cap system for more variation in cap pressure
required because hand is so distal to heart and exposed to many thermal + postural variants
What condition impairs blood supply to the lunate?
Kienbock disease (resulting in deterioration of bone and loss of carpal stability/mobility=pain)
What is the role of extrinsic and intrinsic muscles in wrist control?
They coordinate the movement of the wrist and hand.
Are there any muscles that are localized to the carpus?
none
which carpal bones are wedge shaped?
scaphoid, lunate
which bones stop the scaphoid from extending under compression, pushing it into flexion instead?
trapezium, trapezoid
which bone balances out the flexion of the scaphoid, tending more towards extension?
lunate
what does the concept of “carpal instability in one direction, can be
balanced by single force” mean?
Carpal instability often occurs when:
One bone moves excessively in one direction (e.g., lunate overextends)
Because the system is normally balanced:
A single opposing force (ligament, bone contact, or muscle force)
Can restore stability
What are the two types of ligaments in the wrist?
Palmar (thick and strong) and dorsal (thinner and fewer) ligaments.
what ligaments bind carpal bones tightly together?
Short intrinsic ligaments
What is the function of the triangular fibrocartilage complex?
It stabilizes the distal radioulnar joint, reinforces the ulnar aspect of the wrist, and forms ulnar aspect of articulating surface.
what comprises the triangular fibrocartilage complex?
meniscus homologue, articular disc of triangular fibrocartilage, palmar ulnocarpal ligament, ulnar collateral ligament, dorsal/palmar radioulnar ligs
what does the retinacular sys of the hand do?
encloses, compartmentalizes, and restrains joint and tendon
Do all digital articulations (MCP, PIP, DIP) function more optimally in flexion or extension?
flexion
What is the digital flexor tendon sheath pulley system?
A series of ring shaped ligaments (5 dense annular pulleys, 3 inner cruciform pulleys)that keep flexor tendons tightly against the finger bones, allowing flexor tendons to pass through the carpal tunnel and maintain smooth motion. Prevents bowstringing ~tendon lifting away from bone.
issue with pulley joint interactions and unstable joints (A3 example)
flexor tendon force creates a tug-of-war between the pulley system and the PIP joint. In a normal finger this is stable, but in an unstable joint (like rheumatoid arthritis), the force can cause joint subluxation instead of smooth motion.
What is trigger finger?
Irritation of the tendon sheath/formation of a nodule on the tendon affecting gliding through sheath causing stiffness and a popping sensation in the finger.
What are the symptoms of trigger finger?
Finger stiffness, popping sensation, catching/locking in a bent position, and a tender lump at the base.
risk factors for trigger finger?
repetitive gripping, diabetes/rheumatoid arthritis, female
What is the role of digital collateral ligaments?
They provide stability to the MCP joint, by restricting movement primarily in flexion (extension 2ndary, passive end range). taught in flexion, slack in extension
palmar portion: minimal restraints of extended MCP
dorsal portion: primary restraints of flexed MCP
what does the transverse intercarpal lig of the hand do?
gives additional side-side stability inbetween MCPs
What is the volar/palmar plate?
A thick fibrocartilage structure/anterior capsule that reinforces the MCP joint capsule limits hyperextension, and prevents impingement of flexor tendons
Where is the volar/palmar plate?
firm attachment to base of prox phalanx, loosely attached to volar surface of neck of MCP. can slide proximally to MCP in flexion
what does the digital extensor assembly system do?
couples PIP and DIP motion
extensor digitorum communis tendon role in the phalanges?
Goes up fingers 2 through 5. At each individual MCP/extensor hood, splits into 3 slips (a central slip~inserts onto middle phalanx and 2 lateral bands~inserts onto distal phalanx)
what are the lateral bands (digital extensor assembly)
Lateral bands: insert into base of distal phalanx,
extends DIP
What is rheumatoid arthritis?
A chronic autoimmune disease causing inflammation and pain in multiple joints.
What demographic is more likely to develop rheumatoid arthritis?
Females, who are 2-3 times more likely than males.
What are common hand deformities associated with rheumatoid arthritis?
Boutonniere deformity, swan neck deformity, and ulnar drift.
What is the boutonniere deformity?
Damage to the extensor mechanism preventing straightening of the PIP joint, DIP hyperextended.
what causes rheumatoid arthritis?
immune system attacks synovium of the joints
What causes ulnar drift in rheumatoid arthritis?
Synovitis causing joint damage and destabilization of MCPs (weakening of collateral ligs -esp radial, volar plate, capsule, everyday use causes deviation of fingers towards the ulna through unbalanced ulnar-directed forces.
What is the central slip in the digital extensor assembly?
A thin band that extends the PIP joint by connecting the base of the middle phalanx to the proximal phalanx.
What is the impact of rheumatoid arthritis on function?
It can lead to significant disability and impaired function due to joint damage. Most commonly affects small joints of hands and feet, symmetric distribution
What factors contribute to the higher incidence of rheumatoid arthritis in women?
Changes in estrogen levels (estrogen may regulate immune response), immune cells produce more inflammatory cytokines (testosterone promotes anti-inflammatory signals), immune balance may lean more towards activation, and X inactivation may trigger antibodies
is their a cure for rheumatoid arthritis?
no, treatments reduce inflammation
What happens to the collateral ligaments during MCP joint flexion?
The dorsal portions are taut while the palmar portions are slack.
what happens to extensor mechanism/assembly when PIP is flexed?
the extensor hood shifts distally (towards fingertip)
central slip is taut, lateral bands relaxed
what eliminates active extension of the PIP?
if PIP is in passive or active flexion
What are the primary functions of the retinacular system in the hand?
To enclose, compartmentalize, and restrain joints and tendons.
What is the effect of joint instability on the digital flexor tendon?
It can lead to PIP subluxation and compromised tendon function.
what is a swan neck deformity?
hyperextension of PIP (laxity of volar plate), flexion of DIP
imbalance of forces at PIP (extension>flexion) due to MCP joint volar subluxation
Does the wrist have a collateral ligament system?
no, it mostly relies on Extensor pollicis brevis, Abductor pollicis longus, Extensor carpi ulnaris muscles as an “active collateral system”.
what is excursion?
how much a tendon must slide through tissues to create joint motion
what has more excursion, flexors or extensors?
flexors
what happens if a wrist tendon cannot glide properly (due to scar tissue, trauma, edema, surgery, etc)?
limited excursion = the wrist will not move fully