BIO 222 Lecture6.Homeostasis Review
1/50
Earn XP
Description and Tags
BIO 222 Anatomy & Physiology 2
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
51 Terms
Any of the body’s water-based liquids.
Water is the main component.
body fluid
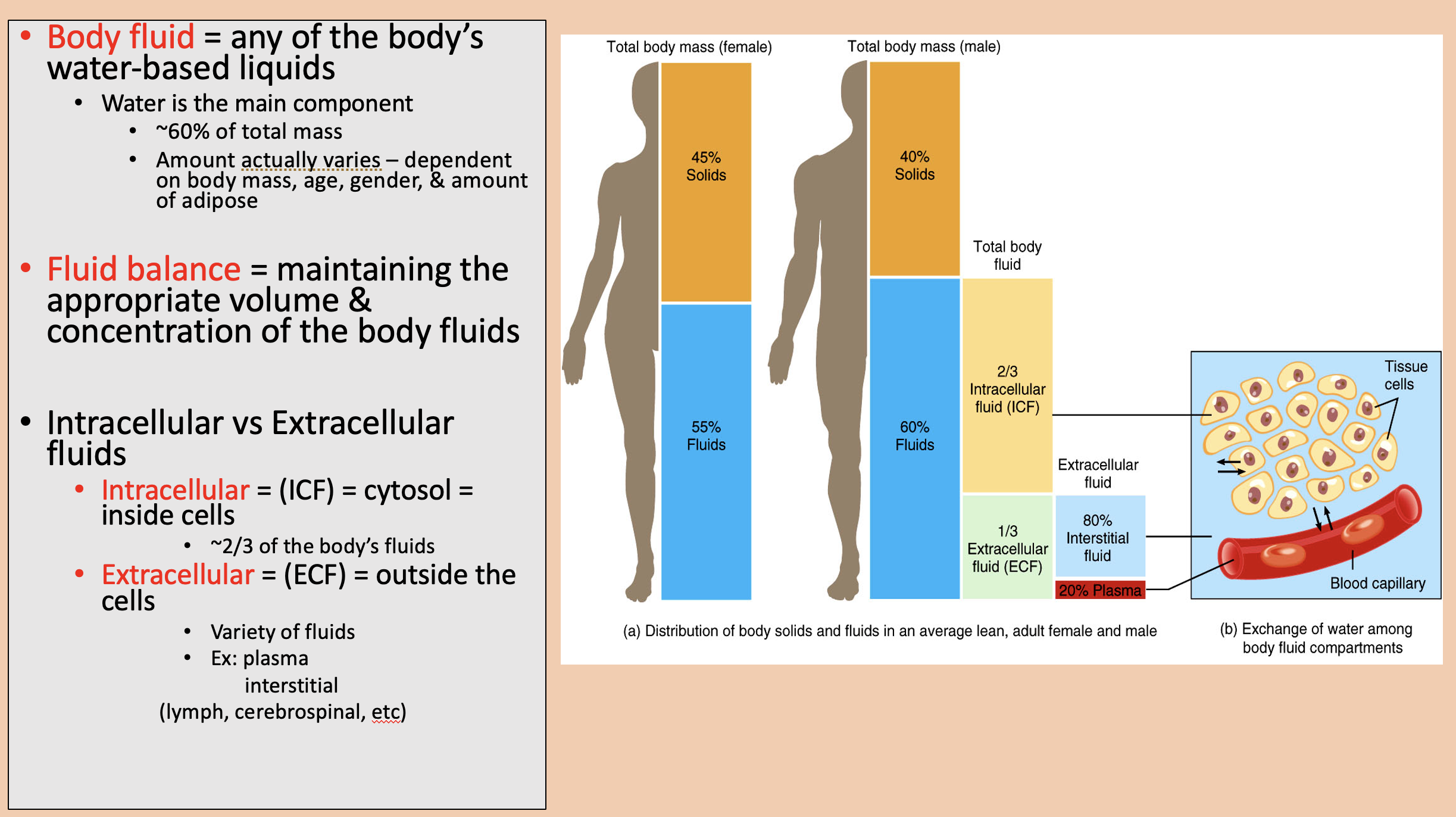
Maintaining the appropriate volume and concentration of the body fluids
fluid balance
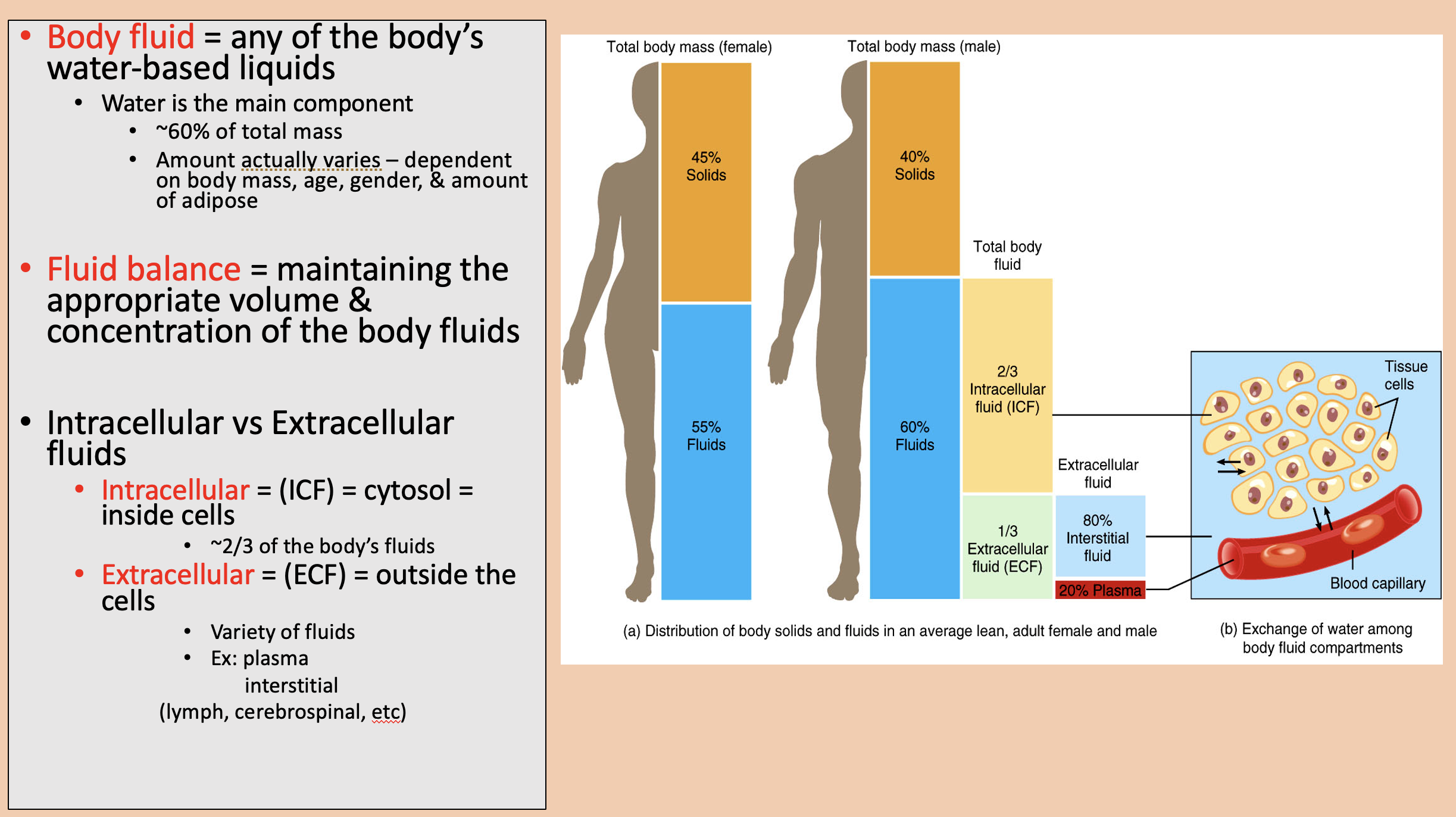
cytosol = inside cells.
~2/3 of the body’s fluids.
intracellular (ICF)
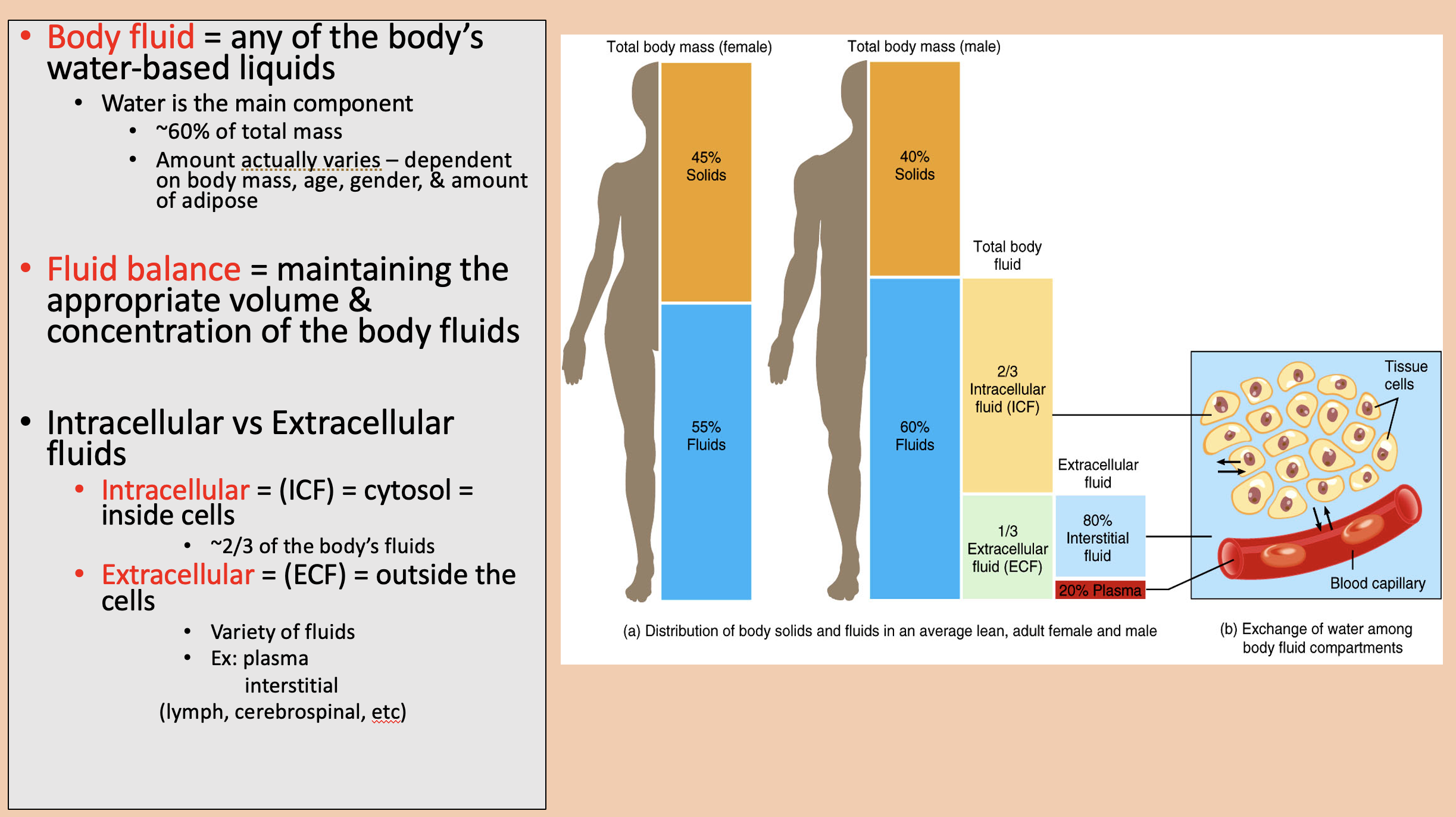
Outside the cells.
Variety of fluids.
extracellular (ECF)
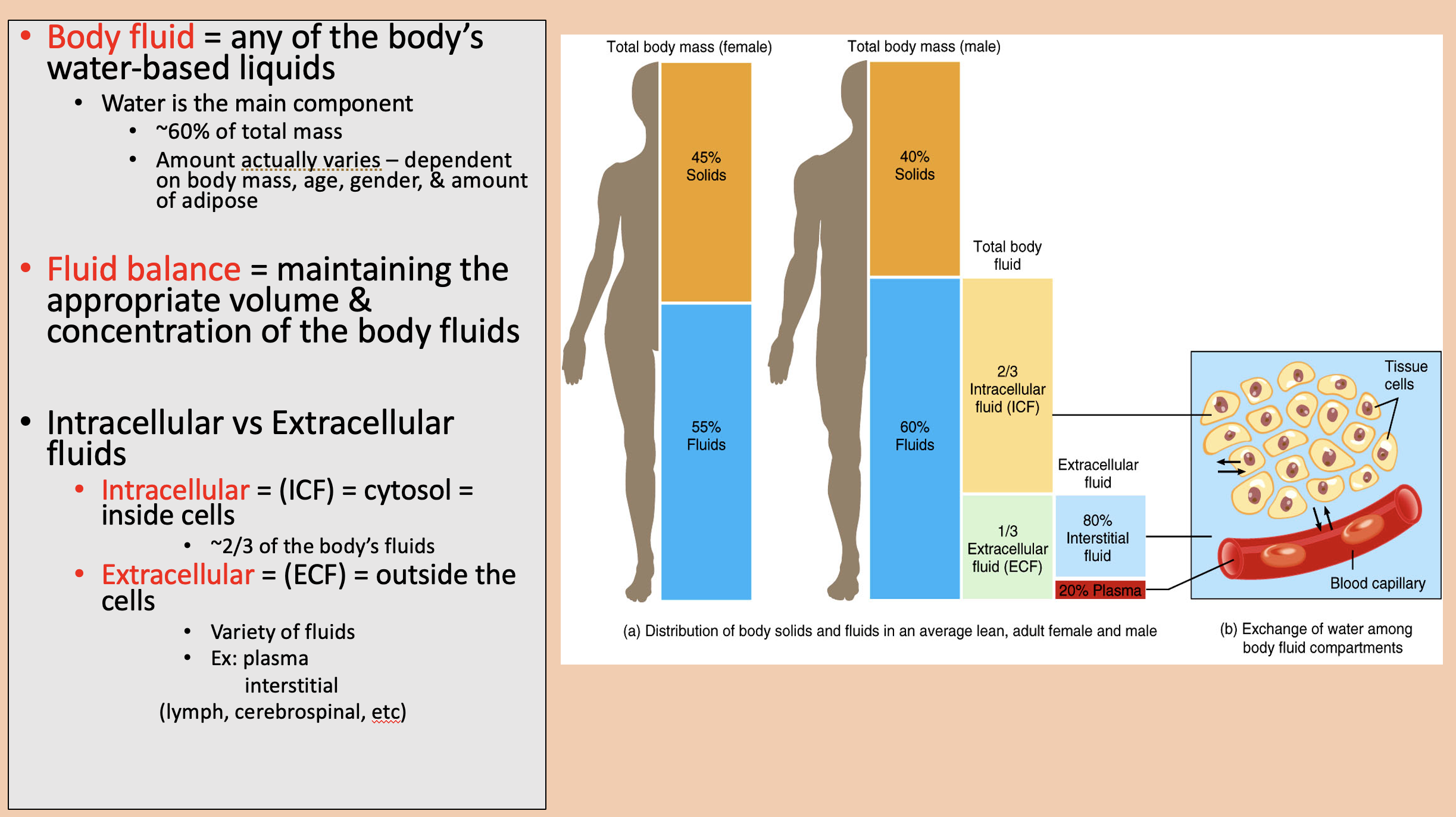
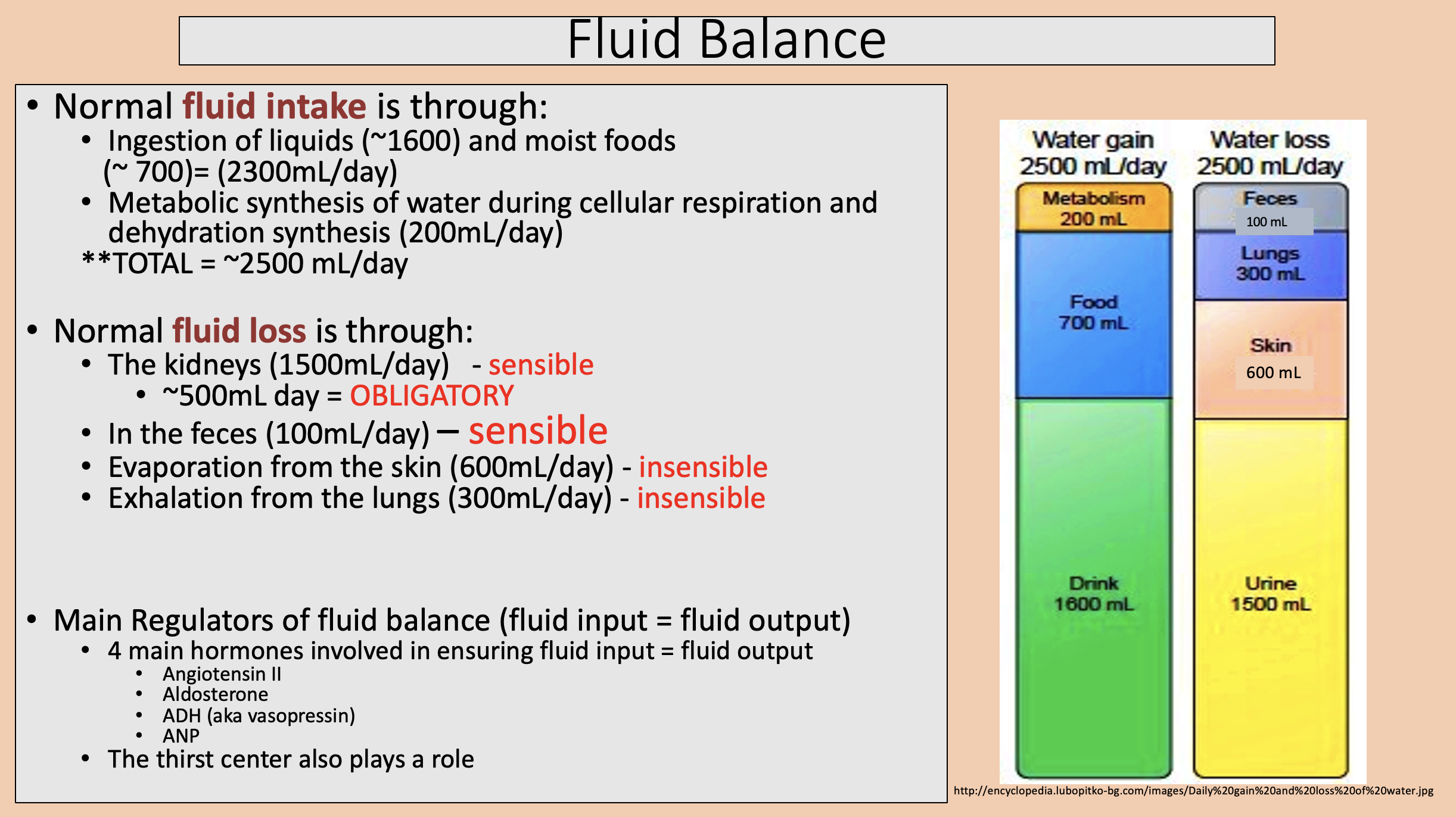
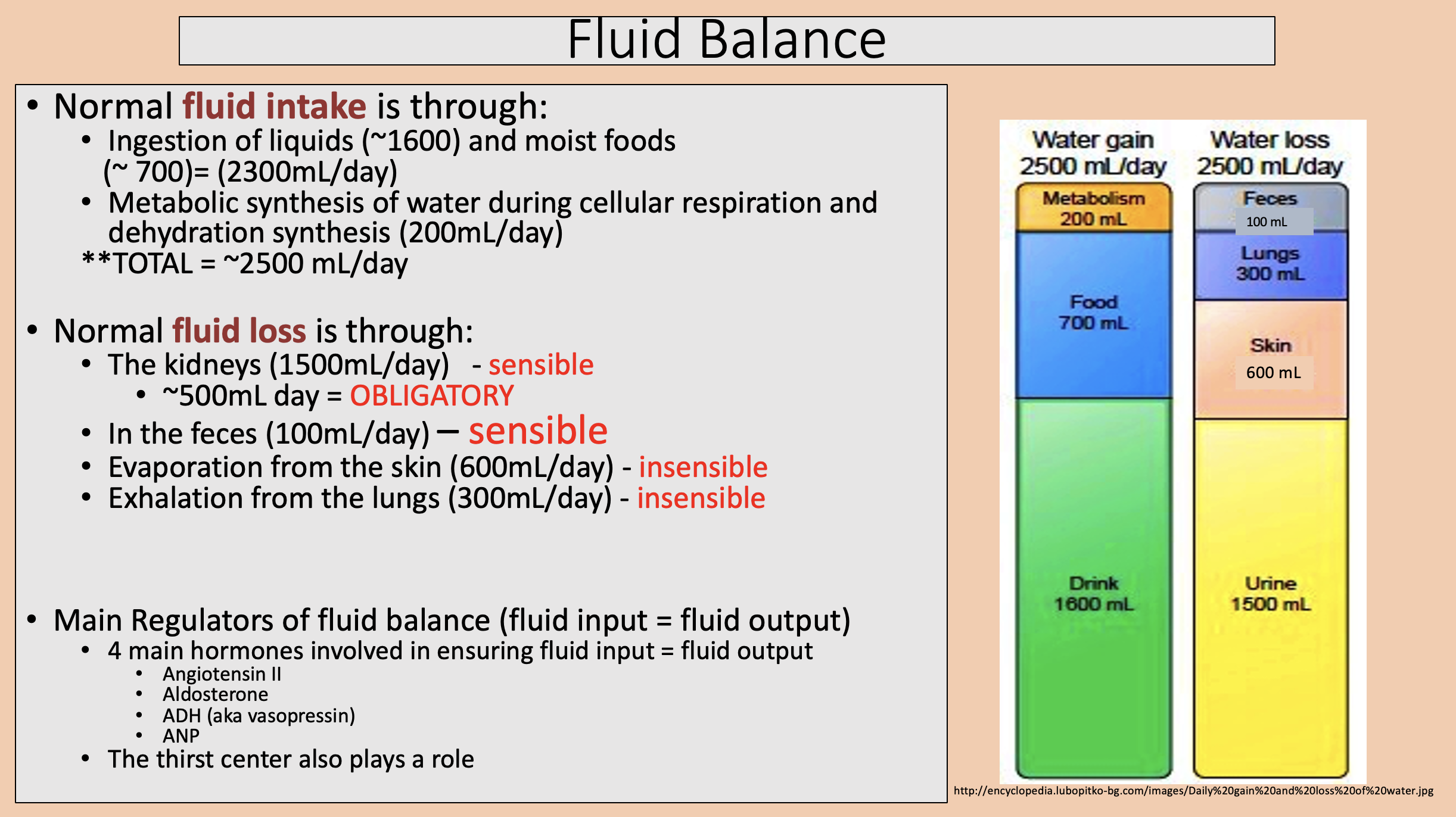
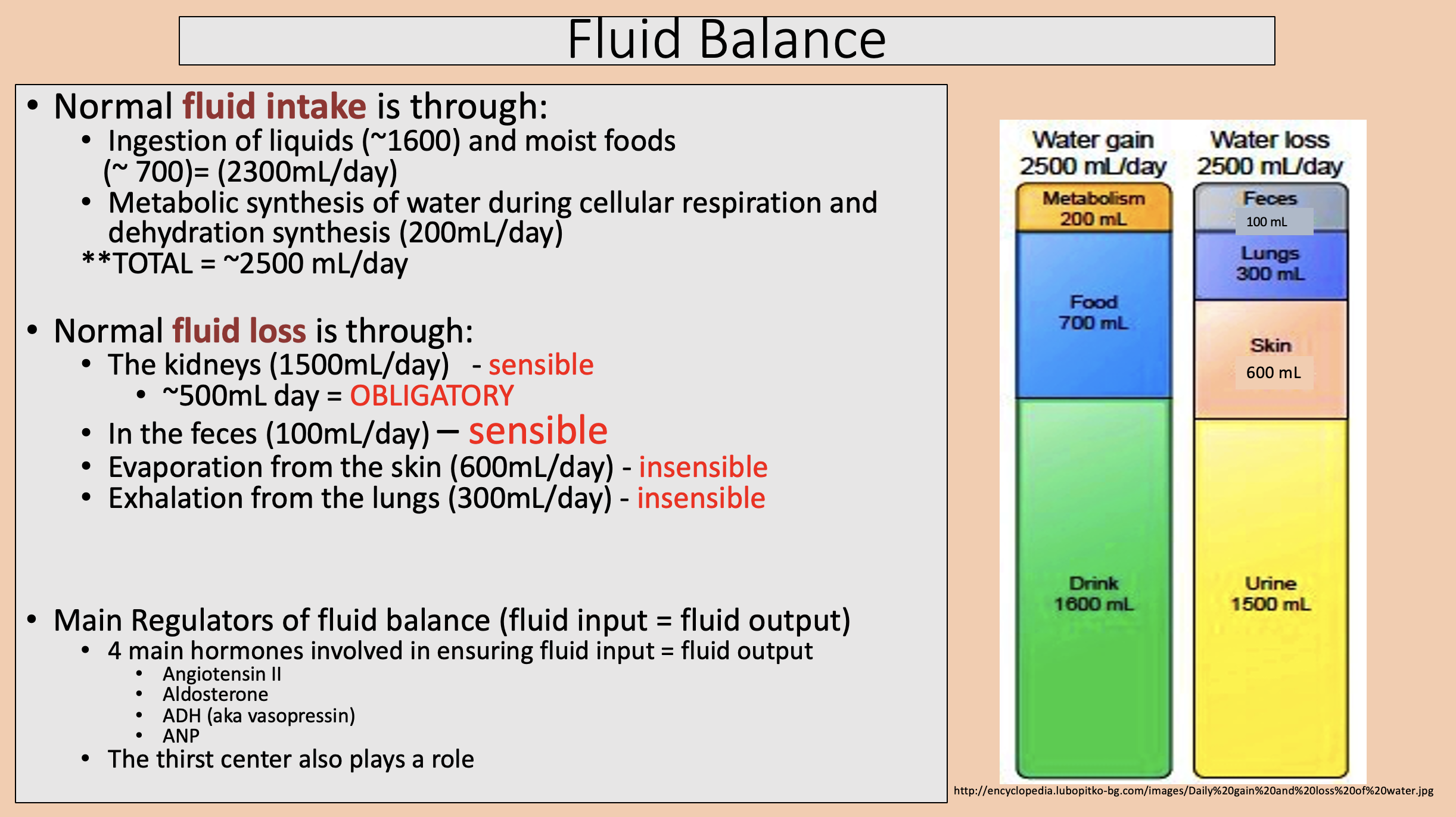
Ingestion of liquids and moist foods.
Metabolic synthesis of water during cellular respiration and dehydration synthesis.
fluid intake
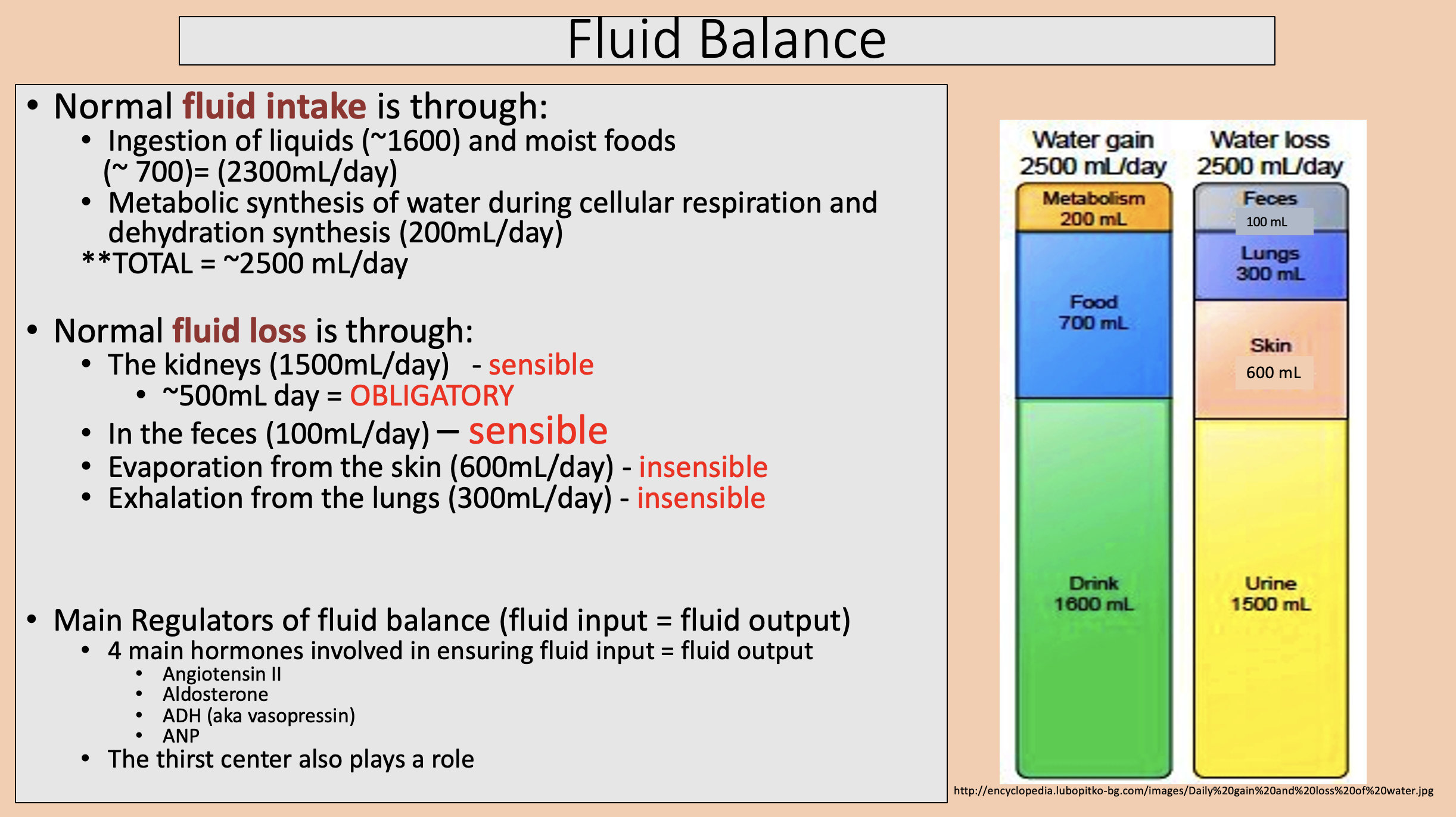
The kidneys.
In the feces.
Evaporation from the skin.
Exhalation from the lungs.
fluid loss
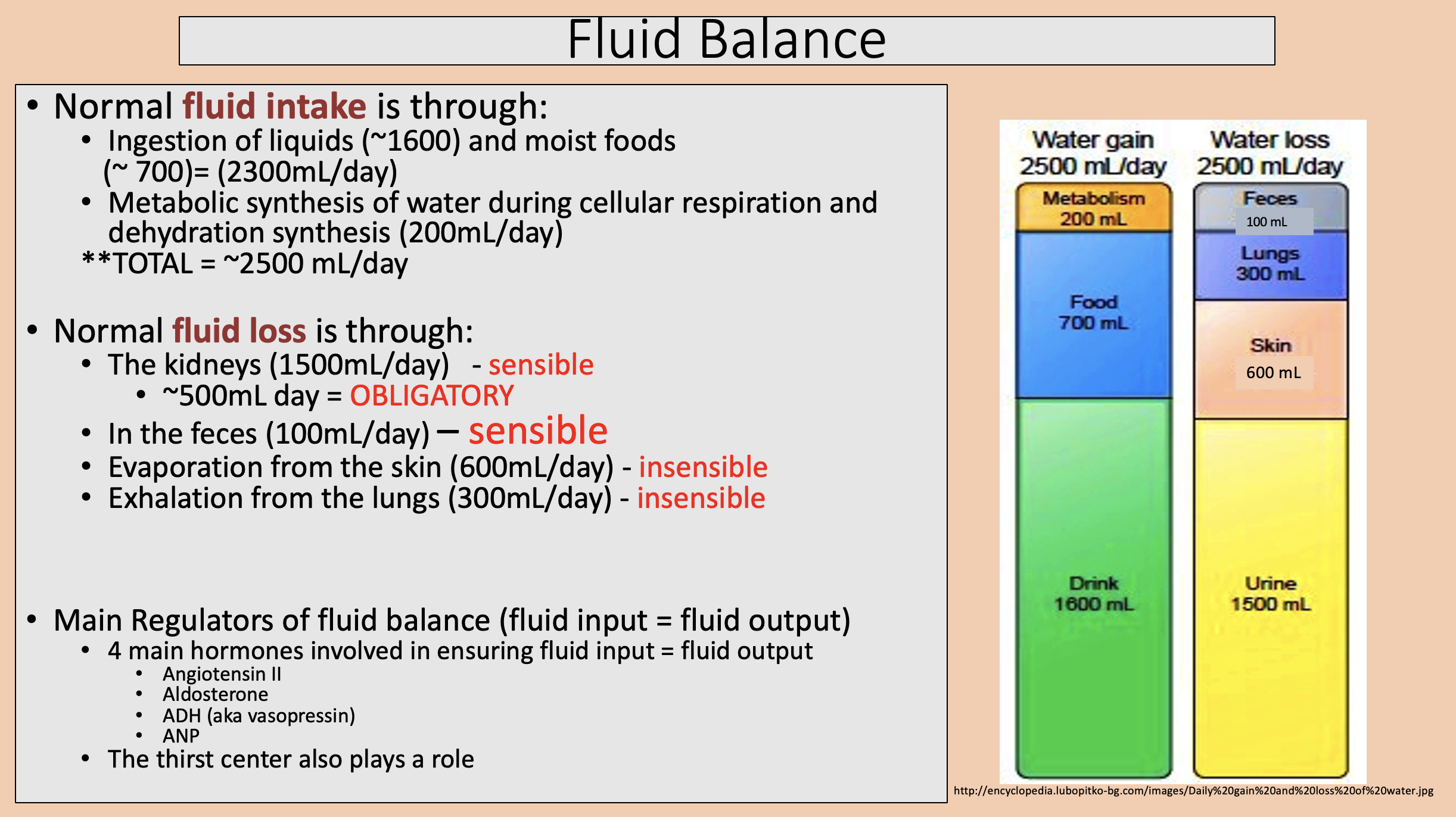
The kidneys.
In the feces.
sensible
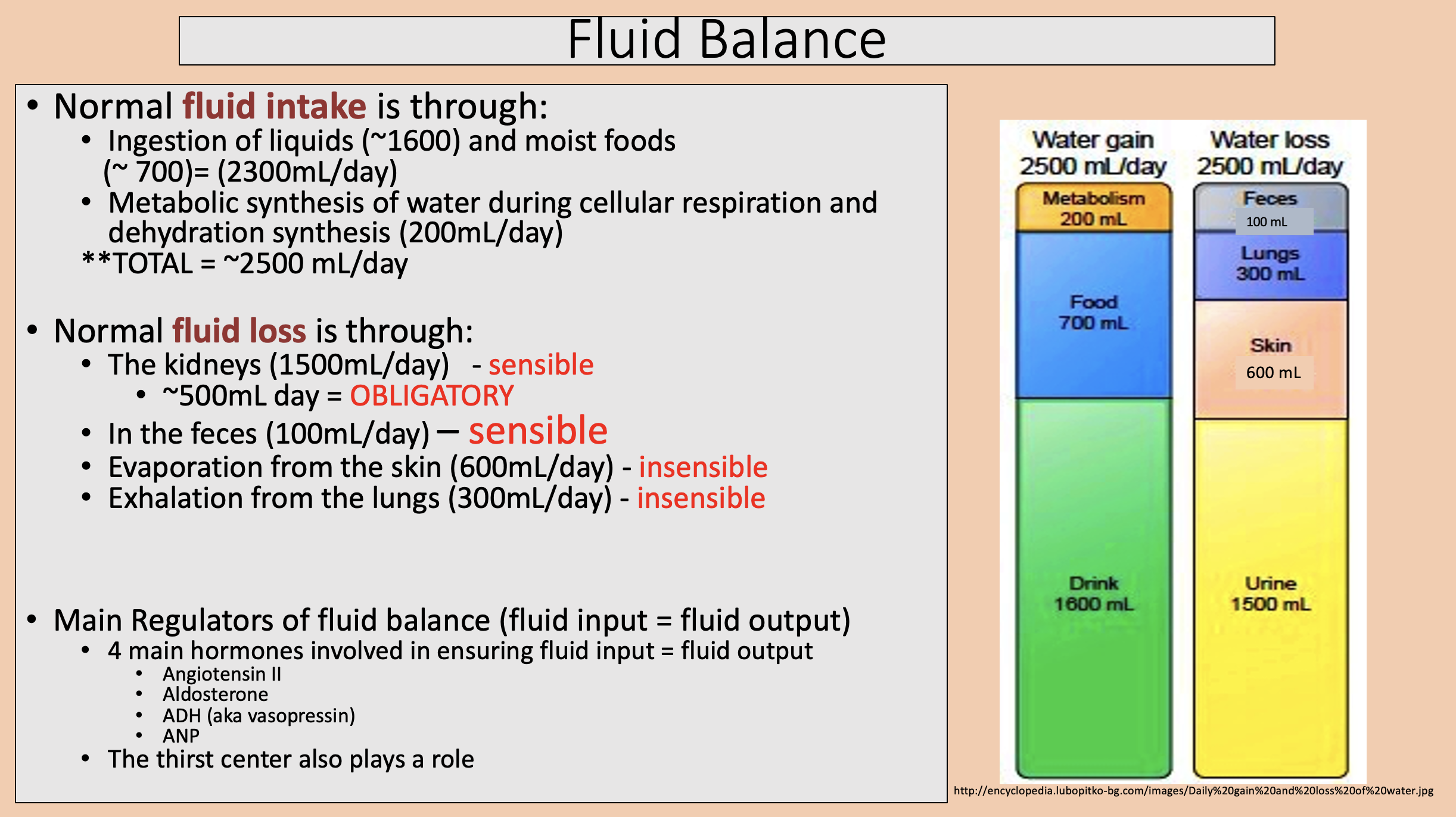
Evaporation from the skin.
Exhalation from the lungs.
insensible
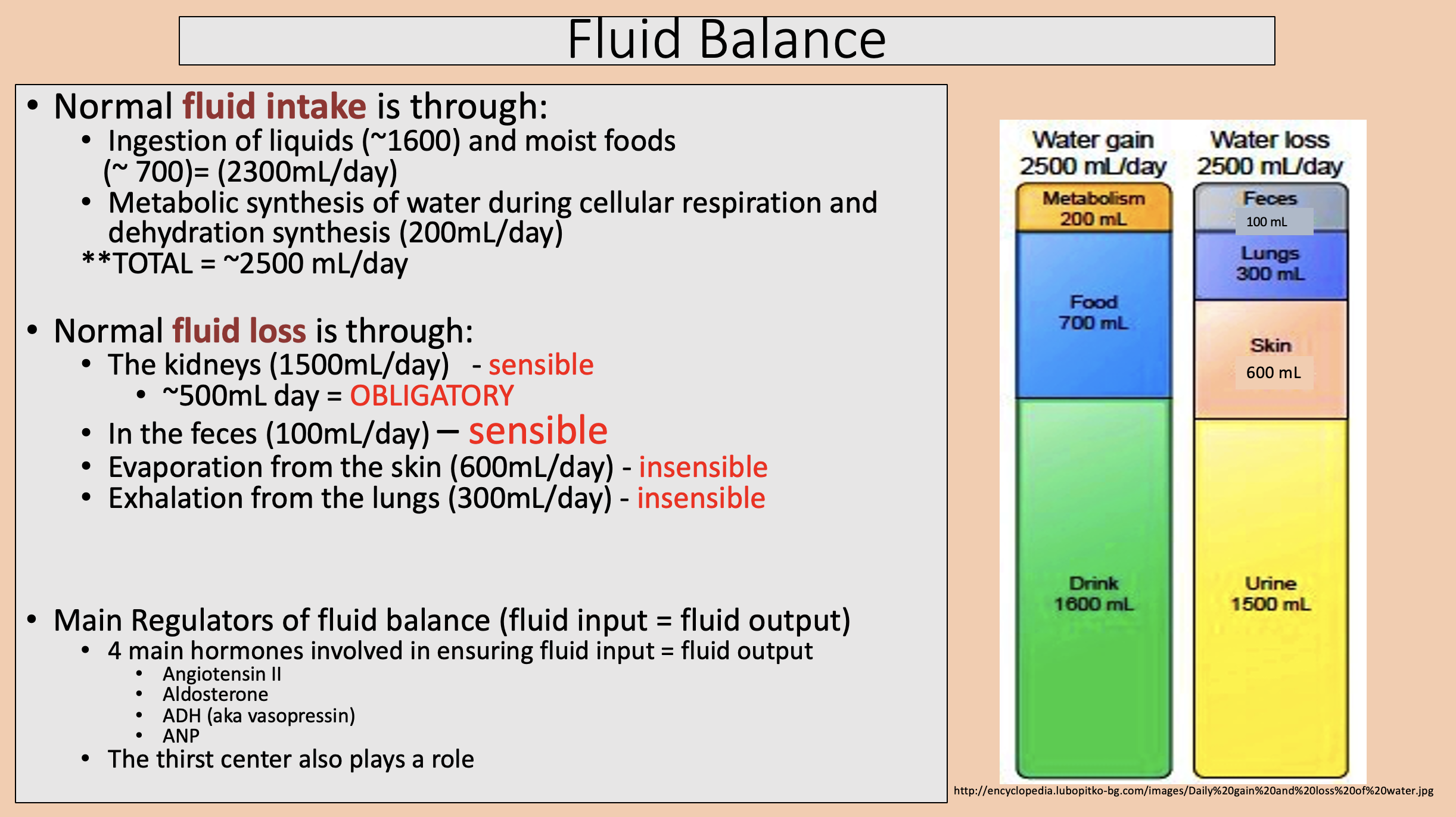
Main Regulators of fluid balance
fluid input = fluid output
4 main hormones
angiotensin II
aldosterone
ADH
ANP
aka vasopressin
ADH
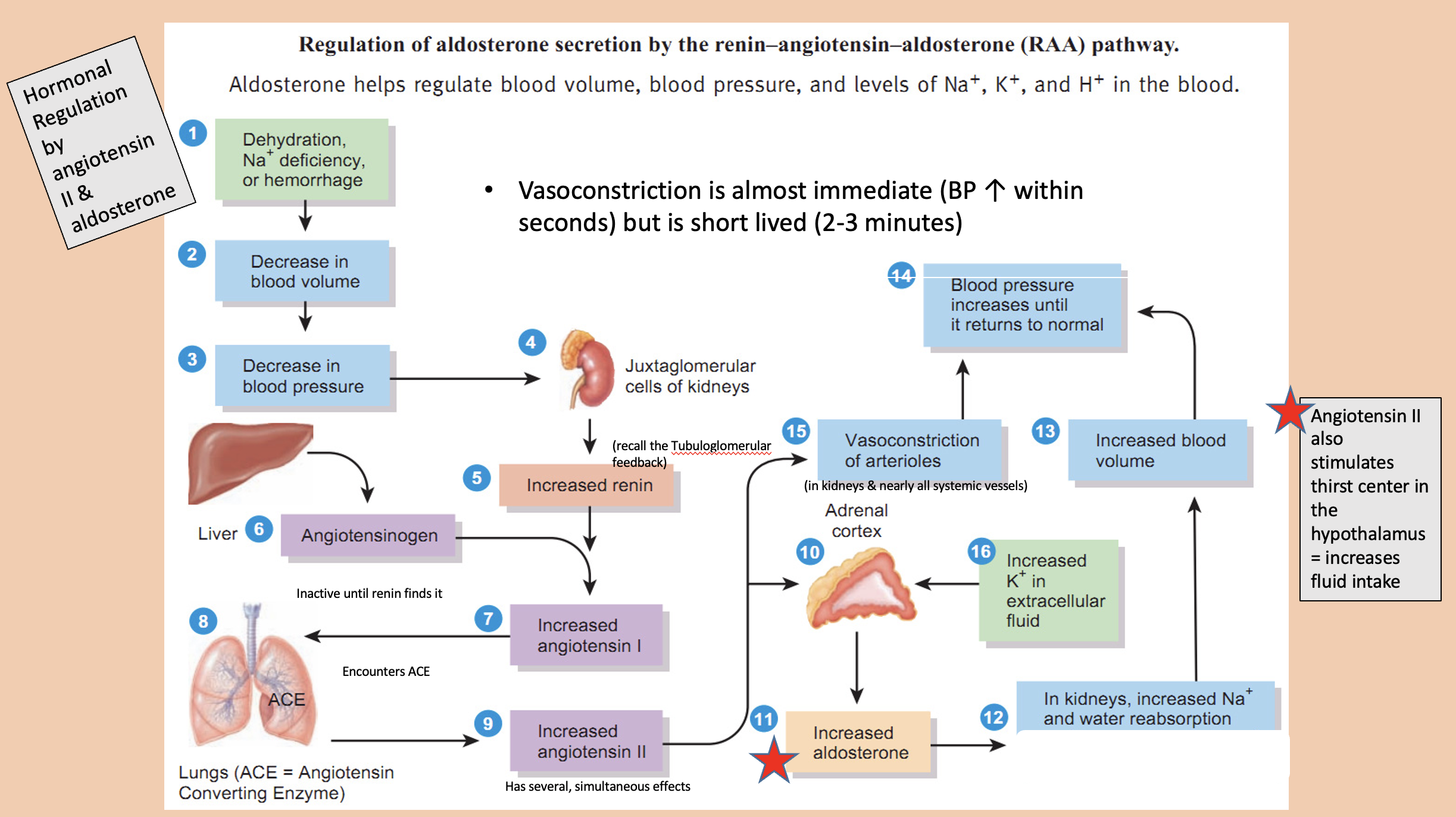
Hormonal Regulation by
angiotensin II
aldosterone
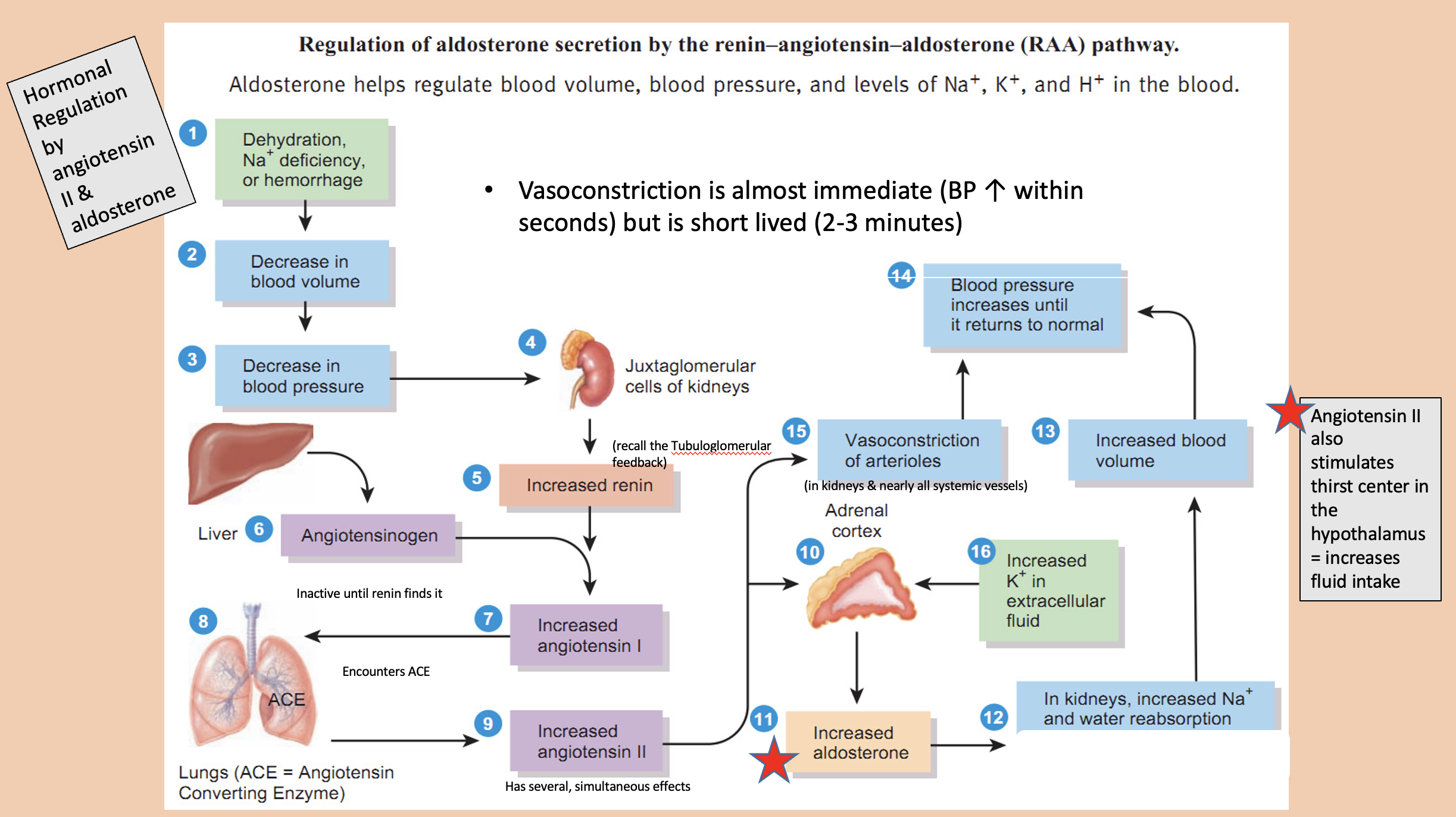
Angiotensin II also stimulates thirst center in the hypothalamus
increases fluid intake
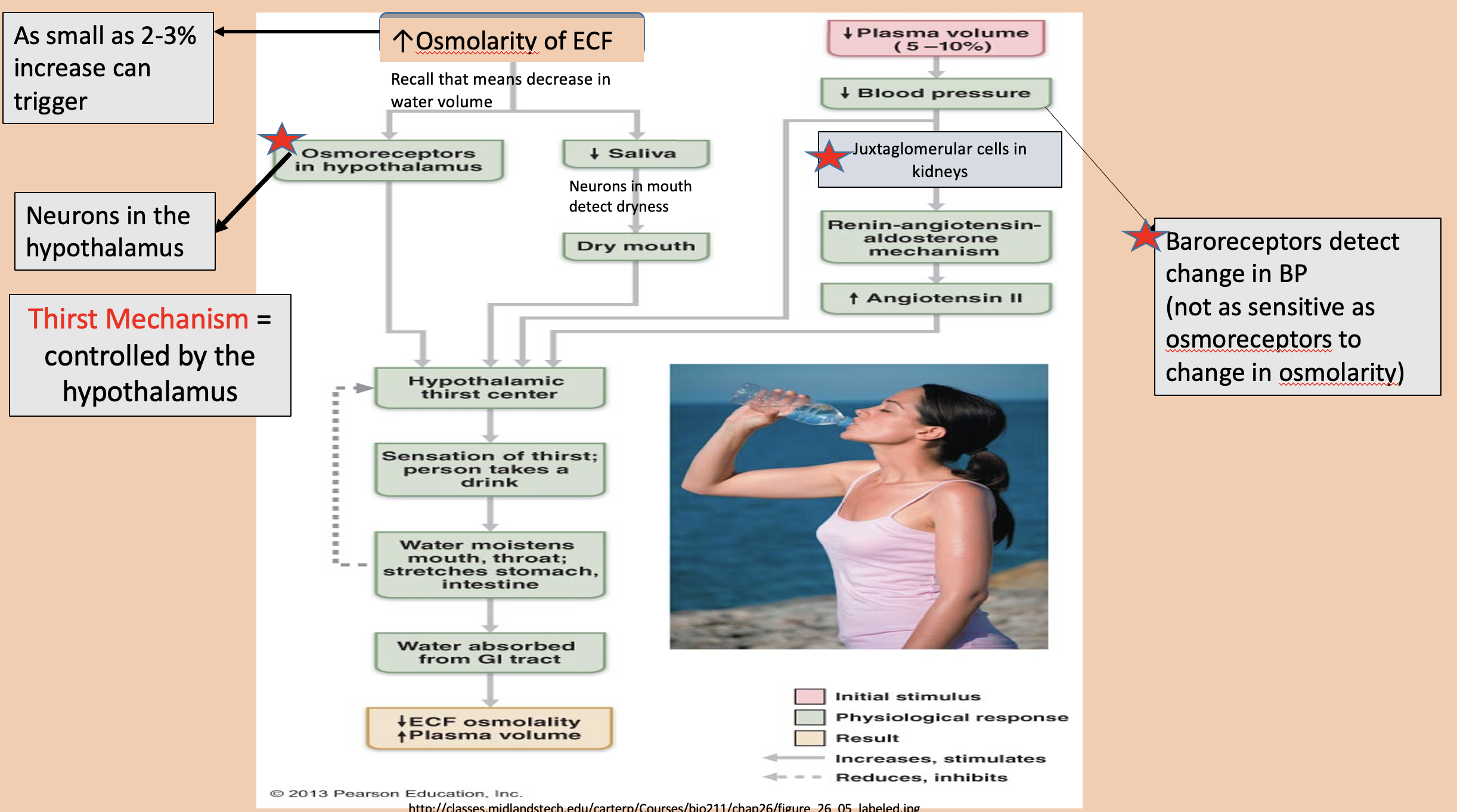
Neurons in the hypothalamus
Osmoreceptors in hypothalamus
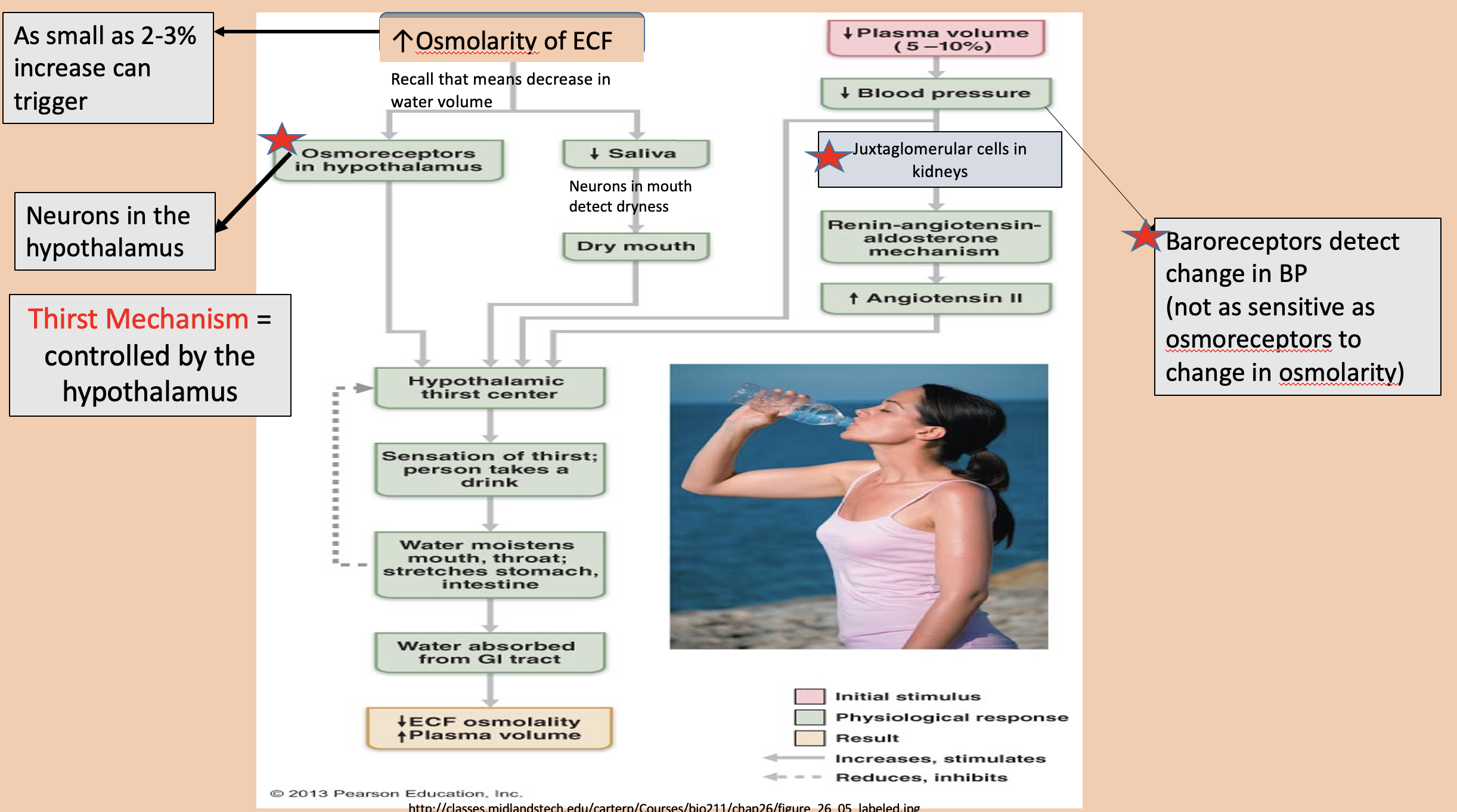
Controlled by the hypothalamus
thirst mechanism
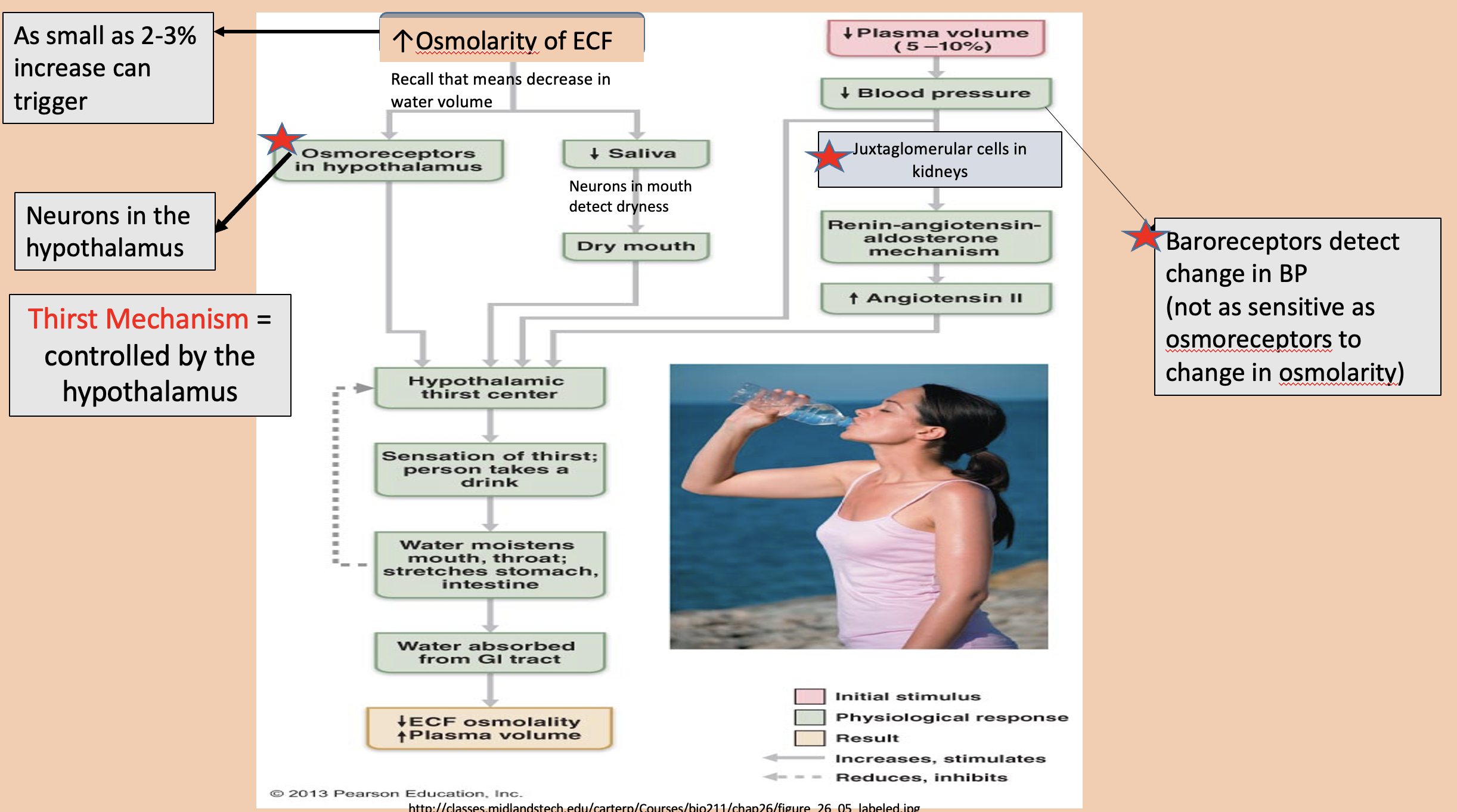
Baroreceptors detect change in BP (not as sensitive as osmoreceptors to change in osmolarity)
decrease blood pressure
Measure of the osmotic pressure gradient between two fluid compartments
tonicity

Cytosol (ICF) & ECF are isotonic
normal condition

Net movement of water into the cell; cells swell ; overhydration/hypotonic hydration
Hypotonic ECF

Net movement of water out of the cell; cell “shrinks” ; dehydration
Hypertonic ECF

Osmotic pressure increases in extracellular fluids.
Water moves out of cells (crenate).
Osmoreceptors in hypothalamus stimulated.
Hypothalamus signals posterior pituitary to release ADH.
Urine output decreases.
Severe thirst, wrinkling of skin, fall in plasma volume and decreased blood pressure, circulator shock, death.
dehydration

water moves out of cells
crenate

Osmotic pressure decreases in extracellular fluids.
Water moves into cells
Osmoreceptors inhibited in hypothalamus.
Hypothalamus signals posterior pituitary to decrease ADH output.
Urine output increases.
Overhydration

Osmotic pressure decreases in extracellular fluids
aka hypotonic hydration

Water moves into cells
cells lyse

‘Drunken’ behavior.
Confusion, hallucinations, convulsions, coma, death
water intoxication

Eliminated via respiratory or urinary
volatile acids

Biggest source of metabolic acids
carbon dioxide

Eliminated via urinary only.
Lactic acid, uric acid, intermediate products of citric acid cycle, ketone bodies.
fixed acids (nonvolatile)

Chemicals to buffer the fluids in the body & resist pH changes
protein
carbonic acid
phosphate

Slowest; only way to eliminate acids other than carbonic acid
urinary

Can change the rate/depth f breathing to adjust CO2 levels
respiratory

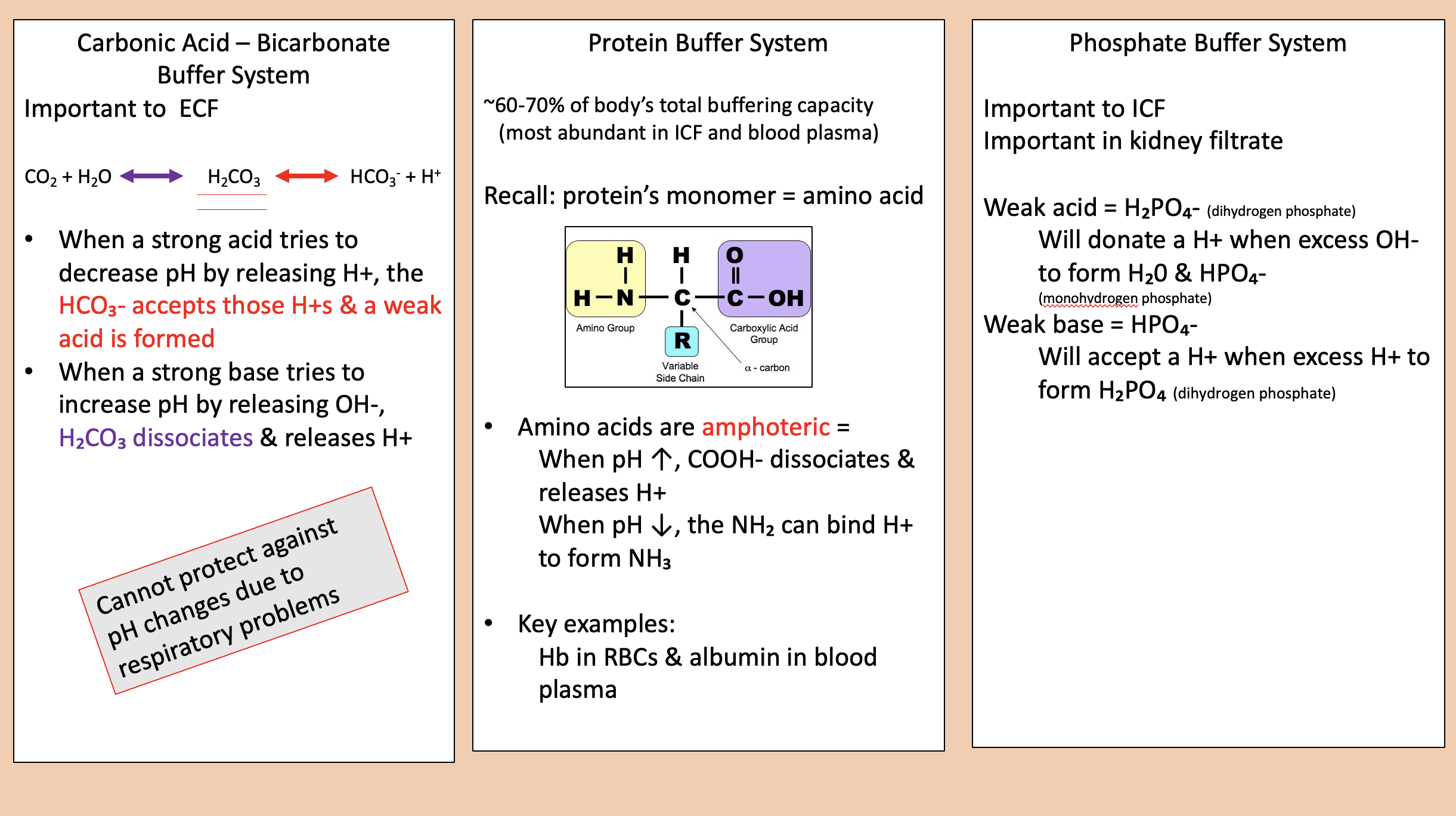
Carbonic Acid.
Important to ECF.
bicarbonate buffer system
Most abundant in ICF and blood plasma
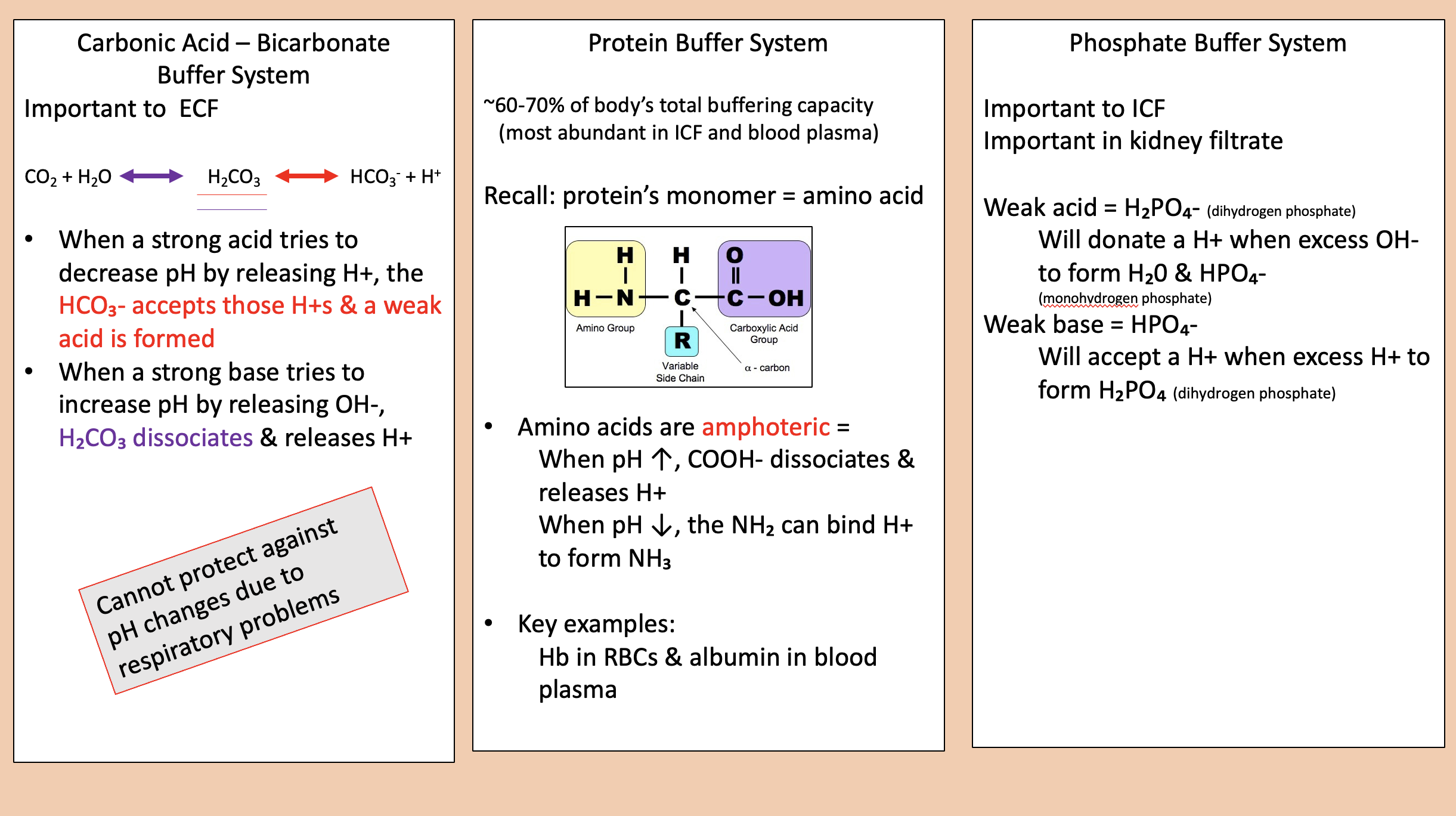
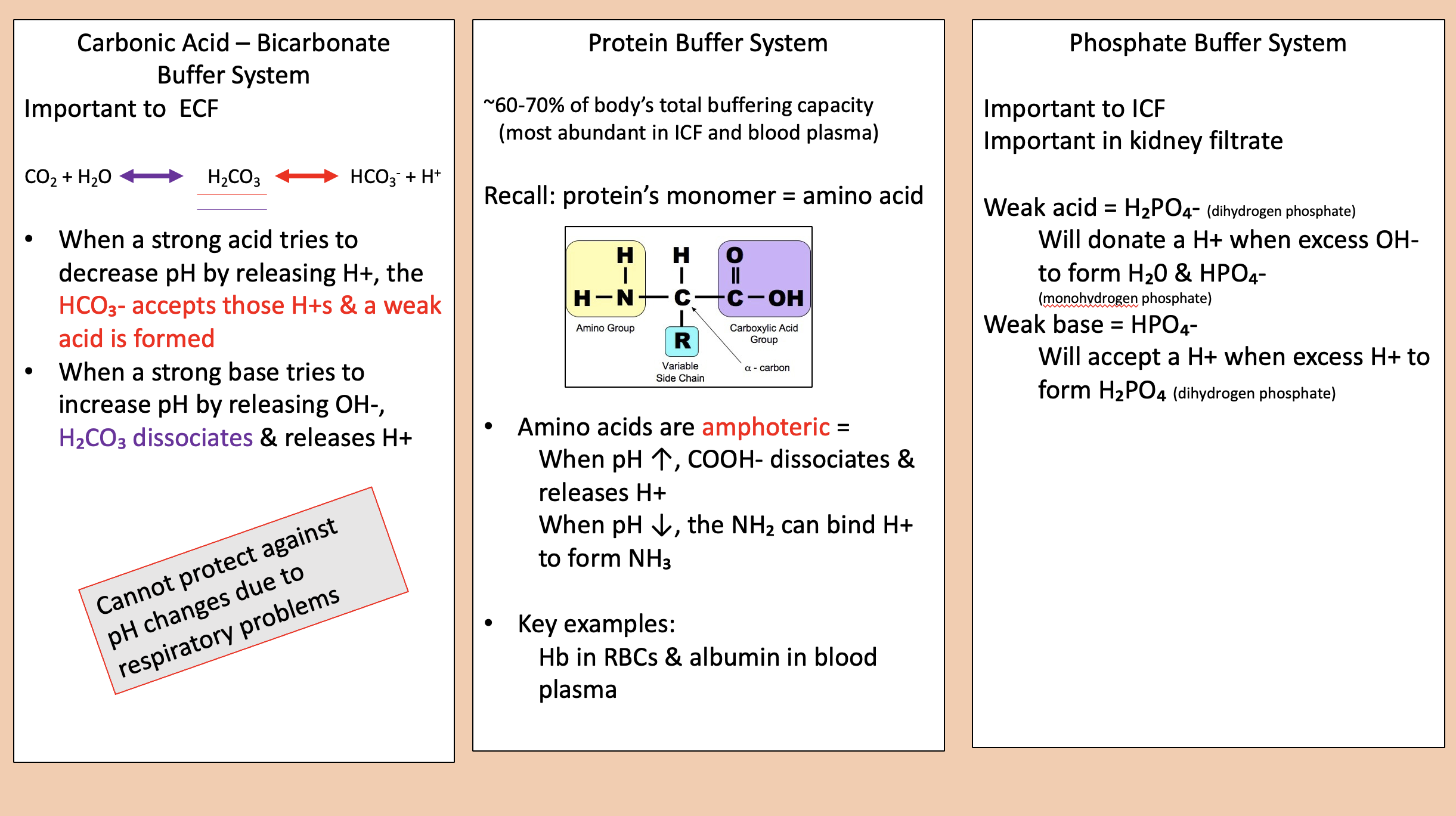
protein buffer system
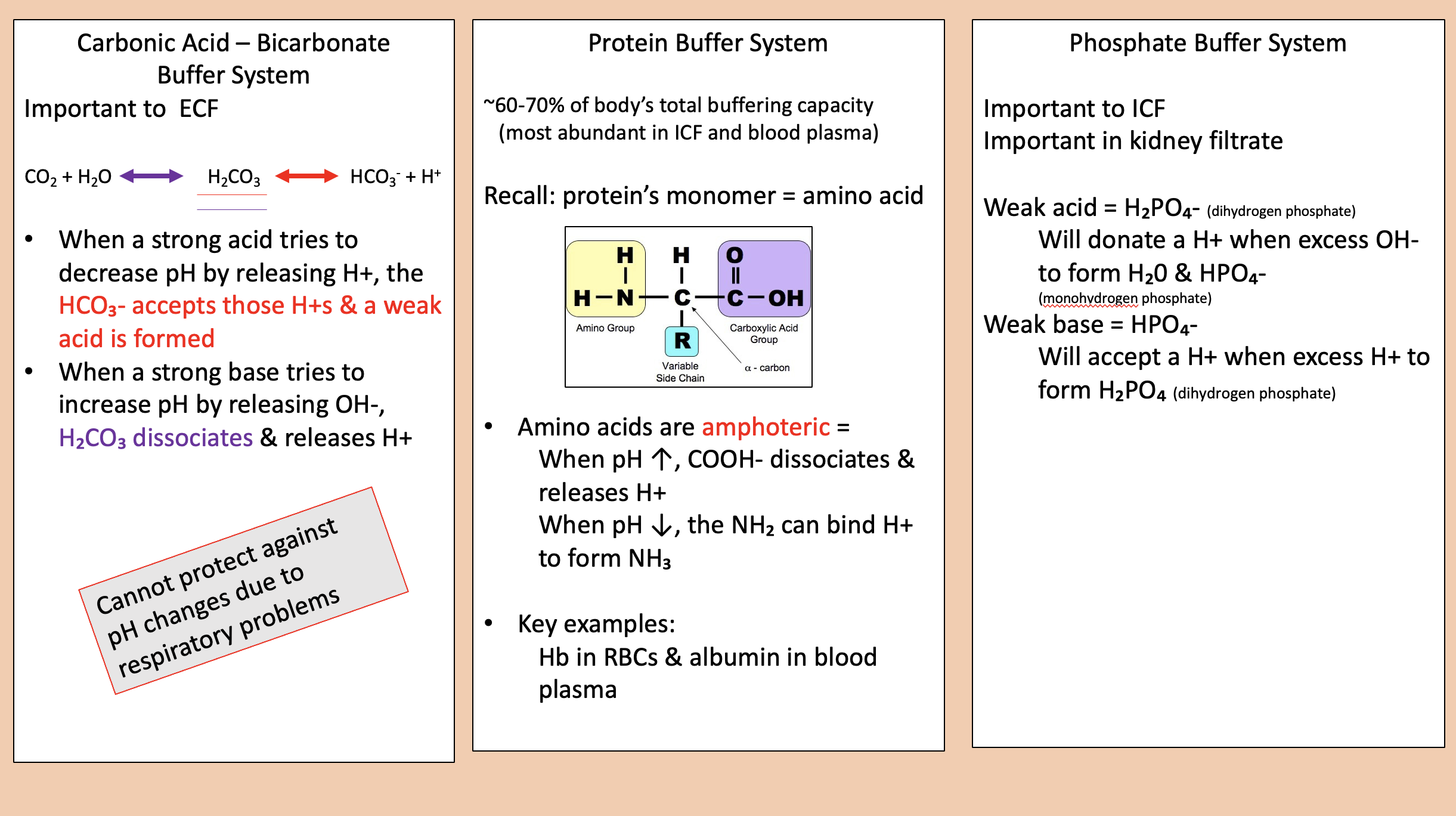
Protein’s monomer
amino acid
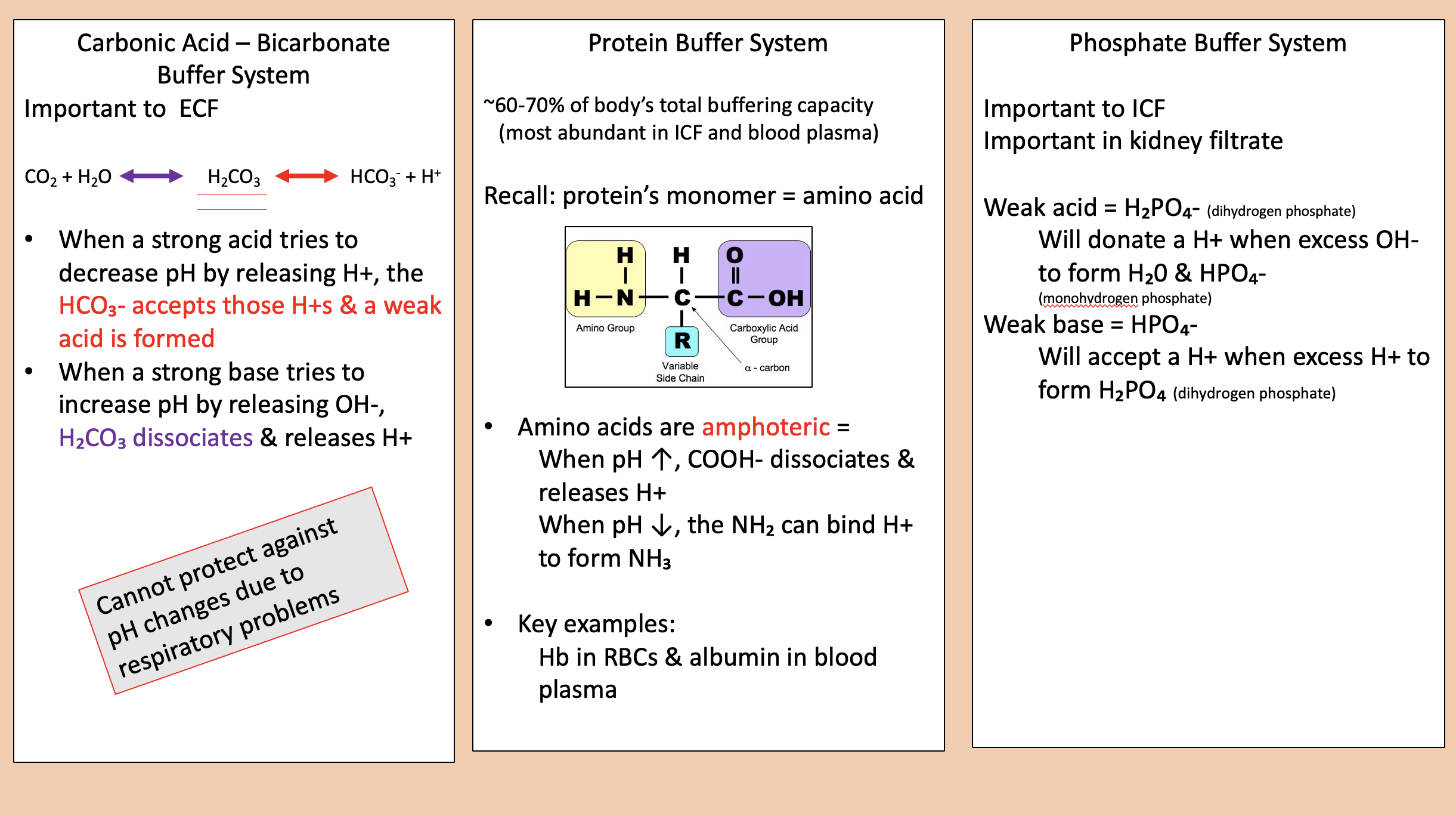
Important to ICF.
Important in kidney filtrate.
phosphate buffer system
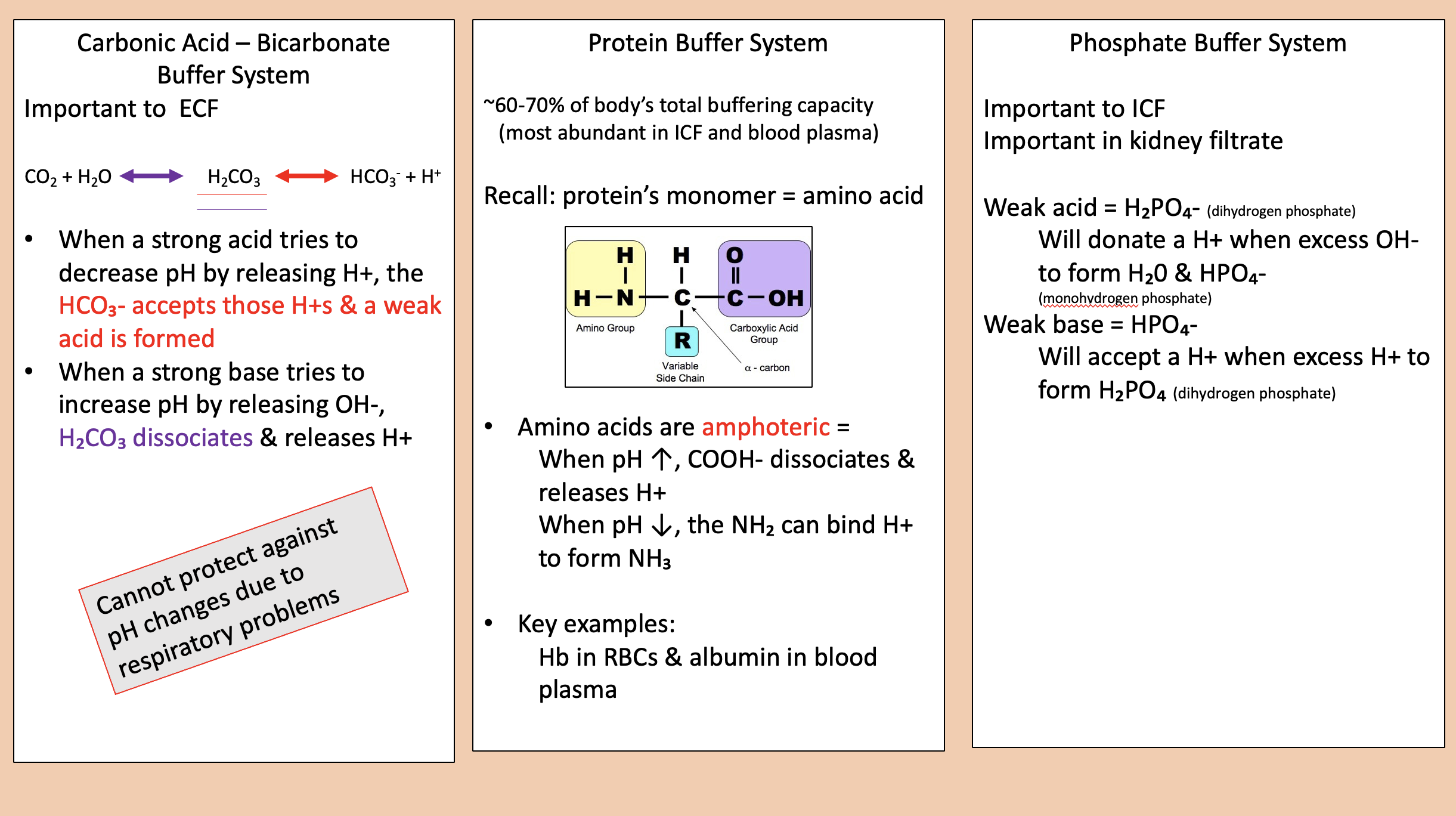
H2PO4- (dihydrogen phosphate).
Will donate a H+ when excess OH- to form H20 & HPO4-
weak acid
HPO4-.
Will accept a H+ when excess H+ to form H2PO4 (dihydrogen phosphate)
weak base
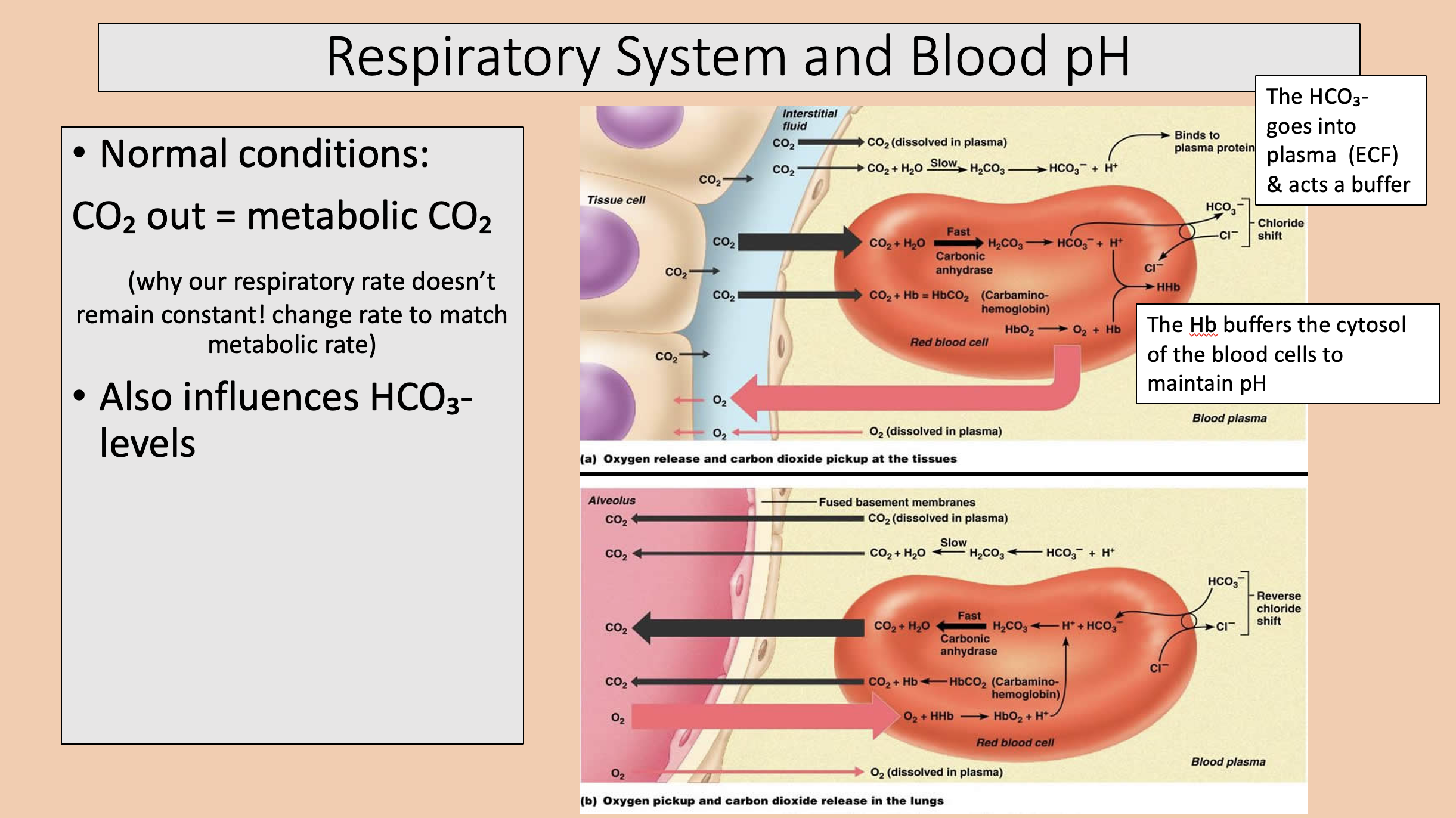
CO2 out
metabolic CO2
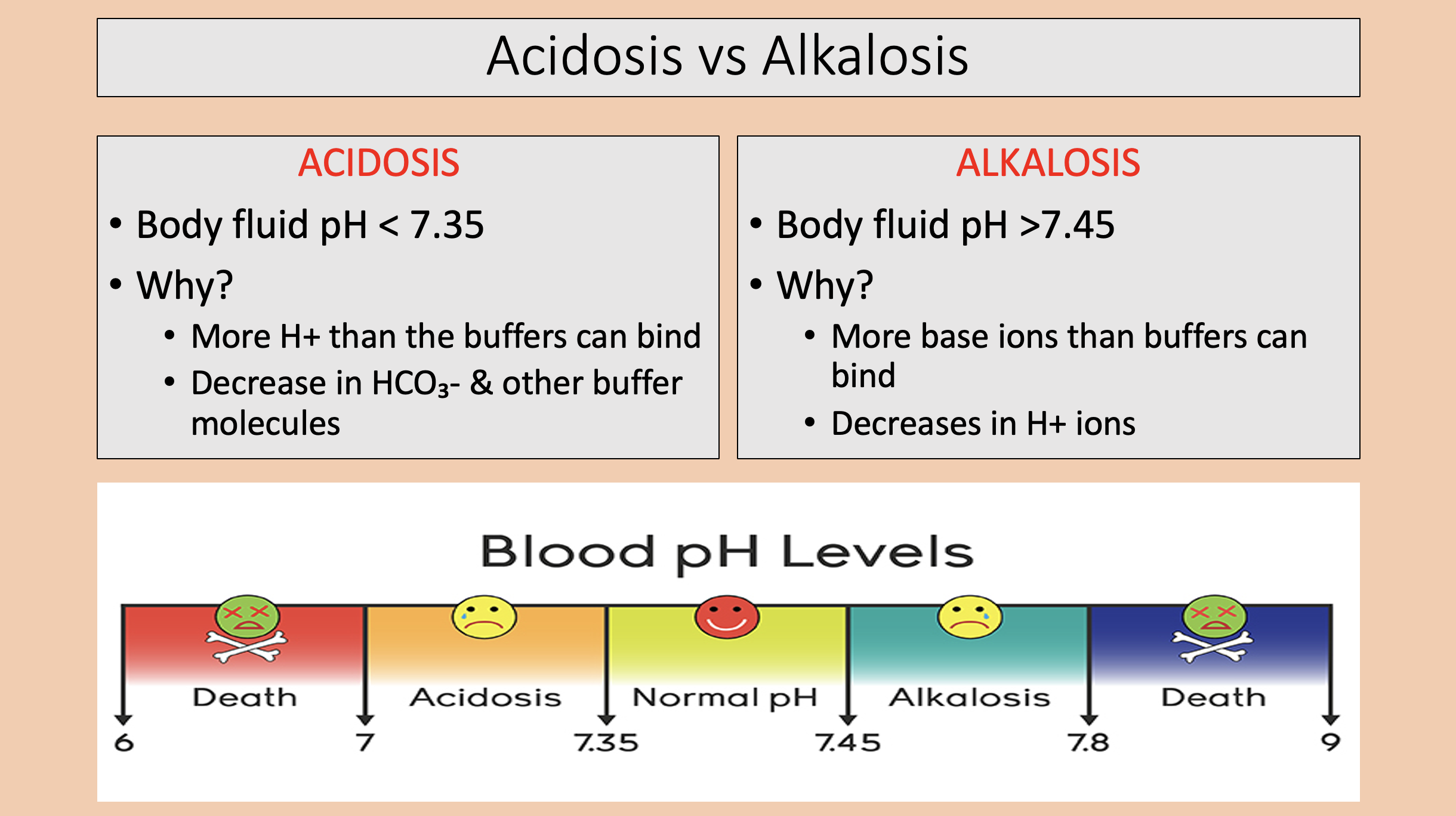
Body fluid pH < 7.35.
More H+ than the buffers can bind.
Decrease in HCO3- & other buffer molecules.
acidosis
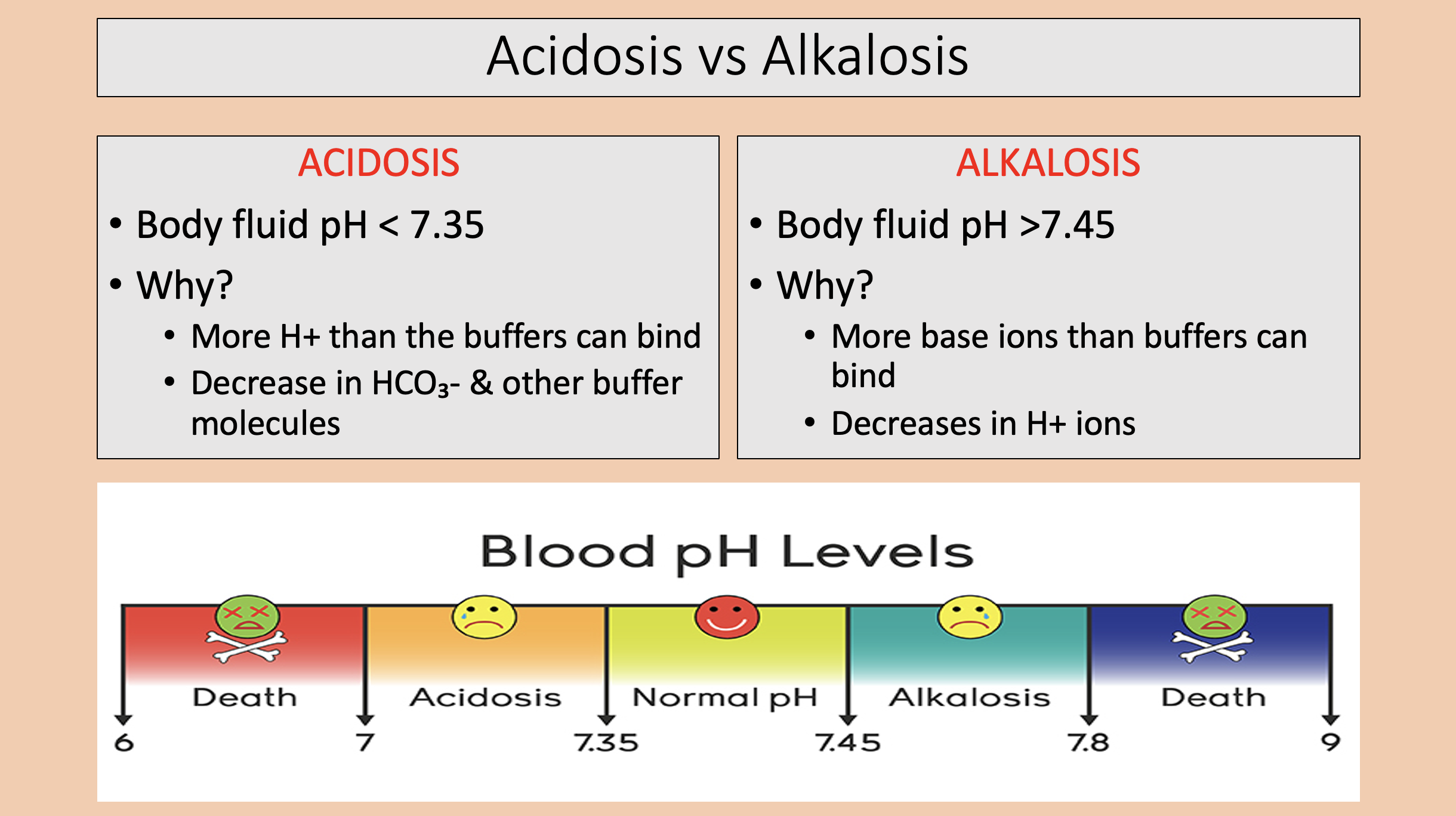
Body fluid pH >7.45.
More base ions than buffers can bind.
Decreases in H+ ions.
alkalosis
Creates resting potential of nerves and muscles.
Drives many secondary active transport mechanisms (symporters; antiporters).
Principal cation of ECF, strongly affecting osmolarity.
sodium (Na+) functions

Sodium (Na+) influencers
ANP (high BP)
aldosterone (low BP)

Most abundant cation in ICF (recall Na+/K+ pump).
Plays key role in creating resting membrane potential for muscle and nerves.
potassium (K+) functions

Potassium (K+) influencers
aldosterone

Calcium (Ca2+) influencers
PTH
calcitriol

The hormone levels affect whether it is withdrawn or deposited in bones, if it’s excreted by kidneys, & if it’s absorbed in the intestines
PTH
calcitriol

Can make nerves & muscles over-excitable
hypocalcemia

Can inhibit depolarization of muscles and nerves
hypercalcemia

Linked to ATP → ADP reaction.
Linked to ATP, GTP, nucleic acid, & phospholipid structure.
phosphate (PO43-) functions

Phosphate (PO43-) influencers
Ca2+ homeostasis
