OCTH614 Conditions in Adults Final
1/139
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
140 Terms
What are the two methods of dressing for burn care?
WET dressing (soaking in a tub and scraping dead tissue) and DRY dressing (wrapping with gauze and applying a solution).
What is the recommended range of motion (ROM) approach for hand injuries?
Active ROM is preferred to help patients feel their limitations, while passive ROM can cause damage.
What is the significance of scar tissue in relation to ROM?
Scar tissue can restrict movement if not managed properly, as it does not know when to stop growing.
What factors contribute to burn severity?
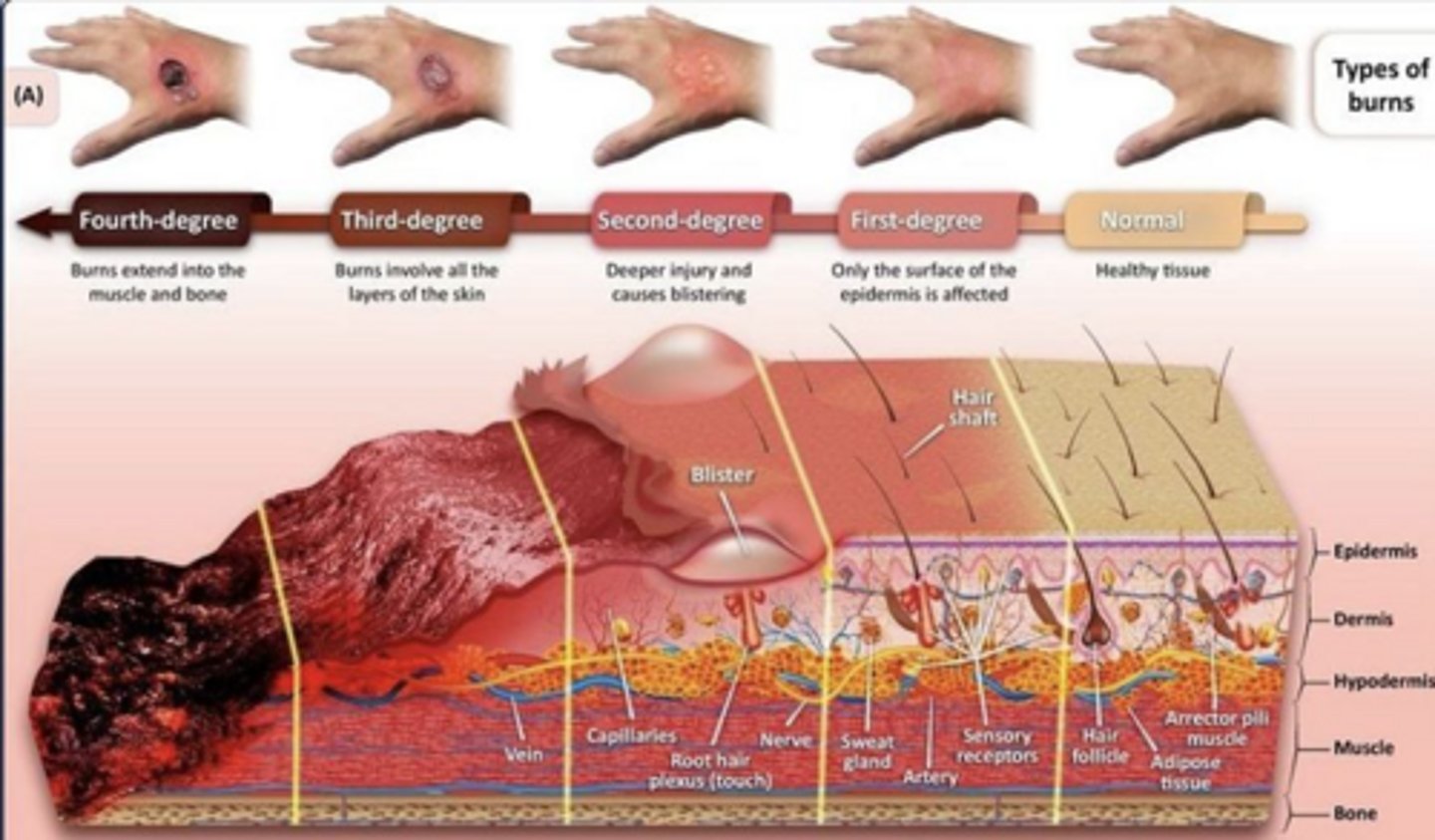
Size of burn, depth of burn (1st, 2nd, 3rd degree), age of victim, type of burn, past medical history, body parts involved, medical status, and additional trauma.
What are the types of thermal burns?
Flame, scald, contact, flash, friction, and sunburn.
What are the zones of injury in burns?
Hyperemia (increased blood flow), Stasis (balance but can worsen), and Coagulation (severe tissue damage).
What is the priority assessment order in burn management?
A = Airway, B = Breathing, C = Circulation, D = Disability, E = Exposure, F = Fluid Resuscitation.
What is the Rule of Nines for burn assessment in adults?
Head and neck 9%, anterior trunk 18%, posterior trunk 18%, arms 9% each, legs 18% each, genitalia 1%.
What characterizes a superficial burn?
Dry and red appearance, no blisters, capillary refill blanches, heals within 7 days with no scarring.
What are the characteristics of a deep partial thickness burn?
Red and fixed stained, may appear white/black, no capillary refill, reduced sensation, healing time >21 days, high chance of hypertrophic scar.

What is the purpose of splinting in burn care?
To maintain proper positioning and prevent contractures in affected areas.
What is the intrinsic plus position in splinting?
A position that maintains the fingers in flexion and thumb abduction to prevent contractures.
What is the rationale for compression therapy in burn management?
It reduces blood flow to scarred areas, minimizing tissue edema, itching, and collagen synthesis.
What types of garments are used for compression therapy?
Ace wraps, conform, Coban, Tubigrip, interim garments, and custom-fitted garments.
What is the impact of palmar arches on hand function?
They provide grip, stability, and conformity to objects; flattening can restrict movement.
What is a Swan Neck Deformity?
Characterized by PIP hyperextension and DIP flexion due to collateral ligament issues.
What is a Boutonniere Deformity?
Occurs with deep partial thickness or full thickness burns, causing PIP flexion and DIP hyperextension.
What is Mallet Finger?
Injury to the terminal slip of the extensor tendon, affecting DIP extension.
What is the role of splints in managing hand injuries?
To maintain joint positions and prevent contractures while allowing for mobility.
What is the recommended duration for wearing compression garments?
22-23 hours a day for effective scar management.
What is the healing time for superficial partial thickness burns?
Healing occurs within 14 days with potential pigmentation changes.
What are the signs of a full thickness burn?
Leathery appearance, no capillary refill, and reduced or absent sensation.
What is the significance of age in burn severity?
Both older and younger individuals are more susceptible to severe burns.
What is the impact of additional trauma on burn assessment?
It can complicate the assessment and management of burn injuries.
What is the importance of early application of compression therapy?
It is most effective in minimizing scarring and promoting healing.
What is the purpose of using adaptive equipment in burn rehabilitation?
To assist patients in regaining full range of motion and function.
What is the role of massage in scar management?
To minimize itching, improve skin texture, and promote flexibility.
What is the most functional web space in the hand?
Between the thumb and index finger.
What condition can result from disruption of the adductor pollicis?
Disruption of the web space between the thumb and index finger.
What is the first priority in treating dorsal scar contractures?
Soft tissue coverage, usually using thick split thickness grafts.
What are the common interventions for circumferential hand burns?
Range of motion (ROM) exercises and gentle passive range of motion (PROM) to each joint.
What is cupping of the palm conformity?
A condition where palmar arches are accentuated, often seen in contact burns of children.
What is a Z-plasty?
A surgical technique to release skin without grafting by cutting and orienting skin flaps.
What are the two main types of prosthetic systems?
Body-Powered (BP) and Externally Powered (Myoelectric).
What does a body-powered prosthetic rely on?
Tension produced from the scapula or contralateral limb movements.
What is the purpose of a harness in prosthetics?
To suspend the prosthesis on the residual limb and transmit force to the control cable.
What is the definition of forequarter amputation?
Removal of any portion of the thorax, shoulder girdle, and all distal parts.
What are the types of wrist units in prosthetics?
Constant friction, quick change, wrist flexion, and ball and socket.
What are voluntary opening terminal devices?
Devices that remain closed by springs or rubber bands and open when force is applied.
What is a myoelectrically controlled prosthesis?
A prosthesis that uses muscle signals to control movements.
What is the goal of myoelectric site testing?
To find a muscle site where a steady contraction can be held for control of the prosthetic.
What are the main factors contributing to cancer etiology?
DNA damage, uncontrollable cell division, genetic inheritance, and environmental carcinogens.
What is Superior Vena Cava Syndrome?
A condition where the superior vena cava becomes blocked, often related to cancer.
What are the three tumor cell types?
Benign, In-Situ, and Malignant.
What characterizes benign tumors?
Cells remain differentiated and do not invade other tissues.
What is the difference between In-Situ and malignant tumors?
In-Situ tumors remain in the original location, while malignant tumors invade surrounding tissues.
What are the classifications of tumors?
Solid tumors and liquid tumors.
What is the TNM classification system used for?
To stage solid tumors based on Tumor size, Node involvement, and Metastasis.
What is the most common type of cancer in terms of occurrence?
Breast, lung, and prostate cancer.
What is the role of surgery in cancer management?
To remove as much of the tumor as possible and prevent spread or recurrence.
What are oncologic emergencies?
Critical conditions like Superior Vena Cava Syndrome and metastatic spinal cord compression.
What lifestyle changes can reduce cancer risk?
Avoiding tobacco, maintaining a healthy diet, and engaging in physical activity.
What is the significance of aging in cancer risk?
Aging is one of the greatest risk factors for cancer.
What does the 'T' in cancer staging represent?
Size of the tumor
What does the 'N' in cancer staging indicate?
Nearby lymph node involvement
What does the 'M' in cancer staging signify?
Presence of metastasis
What stages are included in overall cancer staging?
I through IV; A & B
What is the prognosis for higher cancer stages (III/IV)?
Poorer prognosis
What type of cancer forms in epithelial tissue?
Carcinomas
What is a sarcoma?
A malignant tumor originating in soft tissues or bones
What are hematological tumors?
Blood cancers, including lymphoma and leukemia
What are the two types of lymphoma?
Hodgkin Lymphoma and Non-Hodgkin Lymphoma
What is myeloma?
Cancer of plasma cells
What are the four subtypes of leukemia based on?
The type of white blood cell that is deformed
What is the goal of limb hygiene for prosthetic users?
To ensure cleanliness and prevent skin issues
What is phantom limb sensation?
The perception of the presence of an amputated limb
What psychological factors can influence phantom limb pain?
Stress and emotional state
What is the normal CD4 count in a healthy individual?
500 - 1000 cells/mm3
What happens to CD4 count as HIV infection progresses?
CD4 count decreases
What is the viral load in the context of HIV?
Measurement of the amount of HIV in the blood
What are common symptoms of acute HIV infection?
Flu-like symptoms occurring within the first 2-4 weeks
What characterizes the clinical latency stage of HIV?
Chronic HIV infection that can last for decades
What defines AIDS in terms of CD4 count?
Occurs when CD4 count falls below 200 cells/mm3
What is a common neurological complication for individuals with HIV/AIDS?
Peripheral neuropathies
What is the purpose of combination Antiretroviral Therapy (ART)?
To control HIV replication and manage associated conditions
What is the gradual increase in wearing time for a prosthetic?
Short sessions to start (15-30 minutes a few times per day)
What should be checked during skin inspections after prosthetic use?
Redness and irritation
What is the goal of desensitizing the residual limb?
To prepare the limb for touch and pressure before prosthetic use
What is a safe wrapping technique for residual limbs?
Wrap in a distal to proximal direction to maintain circulation
What is the psychological impact of limb loss?
It can affect self-esteem, body image, and life satisfaction
What is the importance of emotional support for prosthetic users?
To aid in the adjustment and acceptance of the prosthetic
What is the most common form of peripheral neuropathy associated with HIV?
Distal Symmetric Peripheral Neuropathy (DSPN)
What are common symptoms of Distal Symmetric Peripheral Neuropathy?
Abnormal sensations like burning, stiffness, prickling, tingling, pins and needles, or numbness.
What are the two categories of DSPN?
1) Direct damage by the HIV organism to peripheral nerves; 2) Antiretroviral-induced toxic peripheral neuropathy.
What is Necrotizing Vasculitis-associated neuropathy?
An inflammatory response causing necrosis of blood vessels that nourish peripheral nerves.
What are the clinical manifestations of Distal Neuropathy?
Pain, weight loss, and myalgias.
How is Necrotizing Vasculitis-associated neuropathy diagnosed?
By nerve and muscle biopsies revealing inflammatory cell infiltrates and necrosis of blood vessels.
What is the treatment for Necrotizing Vasculitis-associated neuropathy?
Corticosteroids, intravenous y-globulin, and plasmapheresis in combination with ART treatment.
What is HIV-Associated Neuromuscular Wasting Syndrome (HANWS)?
A condition characterized by progressive myopathy and rapidly progressing sensorimotor polyneuropathy.
What are common symptoms of HANWS?
Progressive weakness, weight loss, and metabolic abnormalities such as elevated serum lactate.
What is Vacuolar Myelopathy (VM)?
The most common spinal cord disease in those with HIV, causing painless spastic paraparesis.
What are the symptoms of Infectious Myelitis?
Burning pain, hypersensitive skin, followed by a characteristic rash.
What is the most common pathogen causing myelitis?
M. tuberculosis.
What is Progressive Multifocal Leukoencephalopathy (PML)?
A fatal viral disease characterized by progressive inflammation of the brain's white matter.
What are the risk factors for HIV-associated dementia?
High CSF viral load, illicit drug use, female sex, advanced age, and low educational level.
What is the treatment for HIV-associated dementia?
HAART with aggressive treatment of related psychiatric disorders.
What is the prevalence of fractures in HIV patients compared to the general population?
2.87 per 100 persons for HIV patients vs. 1.77 per 100 for the general population.
What psychological conditions are associated with HIV/AIDS?
Delirium, depression, PTSD, schizophrenia, bipolar disorder, and substance abuse.
What are common treatments for chronic pain syndromes?
Multifactorial approaches including medication, psychotherapy, and lifestyle changes.
What is the significance of HAART therapy in HIV patients?
It provides psychological benefits and increases life expectancy.