Objectives (2-Awasthi) - Immunity to Infection
1/34
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
35 Terms
Obj. 1
Describe the triad of infection including the contributions of the pathogen, host, and drug.
Host
Host: Normal immunity and normal physiology (of all systems) are critical.
a. Nonspecific Host Defenses are of vital importance that cannot be over emphasized.
b. Exposure to microorganisms (i.e., normal flora and transient microbes) is normal and to some extent beneficial but is an ultimate source of the problem.
c. Immunopathology—the host response to infection contributes much to disease
d. Host immune response occurs in different phases: Innate immunity, Inflammation, Adaptive immunity, Protective response, Immunological memory
👉 Key role:
Determines susceptibility, severity, and recovery
Obj. 1
Describe the triad of infection including the contributions of the pathogen, host, and drug.
Self-study:
Describe the changes that may occur in the host and pathogen during a course of infection.
HOST
Changes in the Host
👉 Host response evolves through phases:
Innate → Inflammation → Adaptive → Memory
👉Immunopathology develops
Host response itself causes tissue damage
👉Host condition may change:
Improved immunity → recovery
Immunocompromise → severe/opportunistic infection
👉Outcomes may vary:
Asymptomatic infection
Chronic effects (autoimmune, carcinogenic, etc.)
👉 Summary (host changes):
Immune response activates, escalates, and adapts
May protect OR cause damage
Obj. 1
Describe the triad of infection including the contributions of the pathogen, host, and drug.
Self-study:
Describe the changes that may occur in the host and pathogen during a course of infection.
PATHOGEN
Changes in the Pathogen
Pathogen must adapt to host environment
Different from lab conditions
👉Possible changes:
Slower growth in vivo
Intracellular survival
Persistence in tissues
Evasion of immune system
👉Interaction with therapy:
Reduced growth due to drugs
Increased susceptibility to immune clearance
👉 Summary (pathogen changes):
Adapts to host conditions
May become harder to eliminate (e.g., intracellular, slow-growing)
Obj. 1 Summary
Big Picture (High-Yield Concept)
Infection outcome depends on:
Balance between host defenses, pathogen virulence, and therapy
This balance is:
Dynamic and constantly changing during infection
Quick Exam Summary
Host: immunity, inflammation, immunopathology
Pathogen: virulence, survival, adaptation
Drug: shifts balance toward host
Changes over time:
Host → immune phases + possible damage
Pathogen → adapts, persists, evades
Obj. 1
Describe the triad of infection including the contributions of the pathogen, host, and drug.
Pathogen
Pathogen: The basic requirement for pathogenicity of the pathogen is its ability to survive and thrive in the host
a. Few microorganisms can breach the host defenses sufficiently to cause disease.
Microorganisms, once introduced, do differ in their pathogenicity or virulence; i.e., cell receptors for penetration, mechanisms to resist host defenses, ability to persist in tissues and/or to produce tissue damaging substances.
b. The environment of the pathogen in the host is quite different from that in vitro; i.e., the conditions used for diagnosis and evaluation of anti-infectives.
Slow microbial growth, avascular lesions, and intracellular infection are some of the factors that may complicate both the host defenses and anti-infective therapy.
👉Pathogens differ in:
Pathogenicity / virulence
Ability to:
Penetrate (cell receptors)
Resist host defenses
Persist in tissues
Produce tissue-damaging substances
Important concept:
Environment in vivo ≠ in vitro
Includes:
Slow growth
Intracellular infection
Avascular lesions
👉 Key role:
Determines ability to infect, persist, and cause damage
Obj. 1
Describe the triad of infection including the contributions of the pathogen, host, and drug.
Drug (Therapy)
Therapy: The main function of anti-infectives is to alter the host-pathogen balance of power in the favor of the host.
a. antimicrobial activity is rarely as optimal in vivo as in vitro. Poor drug distribution and rapid metabolism/excretion may complicate therapy along with the factors noted above.
b. Surface damage to a pathogen by anti-infectives may enhance phagocytosis.
c. Early and effective anti-infective therapy may inhibit the immune response (i.e., reduced level and/duration of antigen challenge) which may be good or bad.
👉Important limitations:
Less effective in vivo than in vitro
Poor distribution, metabolism, excretion may affect therapy
Additional effects:
Can enhance phagocytosis (surface damage to pathogen)
May inhibit immune response if too early/effective
👉Overall concept:
Recovery depends primarily on host defenses, assisted by anti-infectives
👉 Key role:
Reduces pathogen burden and supports host defenses
Obj. 1
Describe the triad of infection including the contributions of the pathogen, host, and drug.
Self-study:
Write the definition and give examples for the following terms.
Opportunistic pathogens
Innate and Adaptive immunity
Antigen, Epitope and Antibody
Infections caused by microorganisms with low pathogenicity. Immunocompromised individuals are at increased risk.
👉 In simple terms:
These organisms normally do NOT cause disease in healthy people
They cause infection when host defenses are weakened
👉Examples:
Fungi
Bacteria
Viruses
👉Quick Exam Line
Opportunistic pathogens = low pathogenic organisms that cause disease when host defenses are impaired
Obj. 1
Describe the triad of infection including the contributions of the pathogen, host, and drug.
Self-study:
Write the definition and give examples for the following terms.
Opportunistic pathogens
Innate and Adaptive immunity
Antigen, Epitope and Antibody
Innate Immunity
Definition:
Innate immunity is the nonspecific, immediate defense mechanism of the host.
It is present before exposure to pathogens and does not require prior sensitization.
From notes:
“Nonspecific host defenses are of vital importance”
Key Features
Rapid (minutes–hours)
Nonspecific
No memory
Examples
Physical barriers: skin, mucous membranes
Cells: neutrophils, macrophages (phagocytosis)
Molecules: complement proteins, cytokines
Processes: inflammation, fever
2. Adaptive Immunity
Definition
Adaptive immunity is a specific immune response that develops after exposure to an antigen.
It involves recognition of specific antigens and formation of immunological memory.
From notes:
Occurs as part of host response phases including
“Adaptive immunity… Protective response… Immunological memory”
Key Features
Slower initial response (days)
Highly specific
Has memory → stronger response upon re-exposure
Examples
B cells → antibodies (humoral immunity)
Example: IgG against bacteria toxins
T cells → cell-mediated immunity
Cytotoxic T cells killing infected cells
Vaccination → immunological memory
1-Line Exam Answers
Innate immunity: Immediate, nonspecific host defense present before exposure
Adaptive immunity: Specific, acquired immune response with memory after antigen exposure
Obj. 1
Describe the triad of infection including the contributions of the pathogen, host, and drug.
Self-study:
Write the definition and give examples for the following terms.
Opportunistic pathogens
Innate and Adaptive immunity
Antigen, Epitope and Antibody
Antigen
Definition
An antigen is a substance that is recognized by the immune system and can induce an immune response.
👉 Key idea:
It is the “target” of the immune system
Examples
Bacterial proteins (e.g., surface proteins of Streptococcus)
Viral proteins (e.g., spike protein of viruses)
Toxins (e.g., tetanus toxin)
Epitope (Antigenic Determinant)
Definition
An epitope is the specific part of an antigen that is recognized and bound by an antibody or immune receptor.
👉 Key idea:
It is a small region on the antigen (not the whole antigen)
Examples
A specific amino acid sequence on a viral protein
A small region of a bacterial surface antigen
Antibody (Immunoglobulin)
Definition
An antibody is a protein produced by B cells that specifically binds to an antigen (epitope).
👉 Key idea:
It is the effector molecule that targets antigens
Examples
IgG → neutralizes toxins and pathogens
IgM → early immune response
IgA → mucosal immunity (saliva, tears)
👉High-Yield Relationship (VERY important)
Antigen = whole structure
Epitope = specific part of antigen
Antibody = binds the epitope
👉Quick Exam Line
Antigen = triggers immune response
Epitope = specific binding site on antigen
Antibody = protein that binds the epitope
Obj. 2
Differentiate the four main types of infectious disease - toxigenic, extracellular, facultative intracellular, obligate intracellular-including their basic characteristics, common pathogens, and the most important host defenses.
Toxigenic Infections
(1) Exotoxins
(2) Endotoxins
(1) Exotoxins
Soluble proteins synthesized and secreted by some of the Gram-positive and Gram-negative bacteria.
Intoxication: Botulism
Toxigenic Infection: Diphtheria, Tetanus
Toxin Involvement along with other virulence factors: Scarlet fever, Staphylococcus aureus
-Compared to endotoxin, exotoxins are diverse in their toxicological activity and have potent and specific activity.
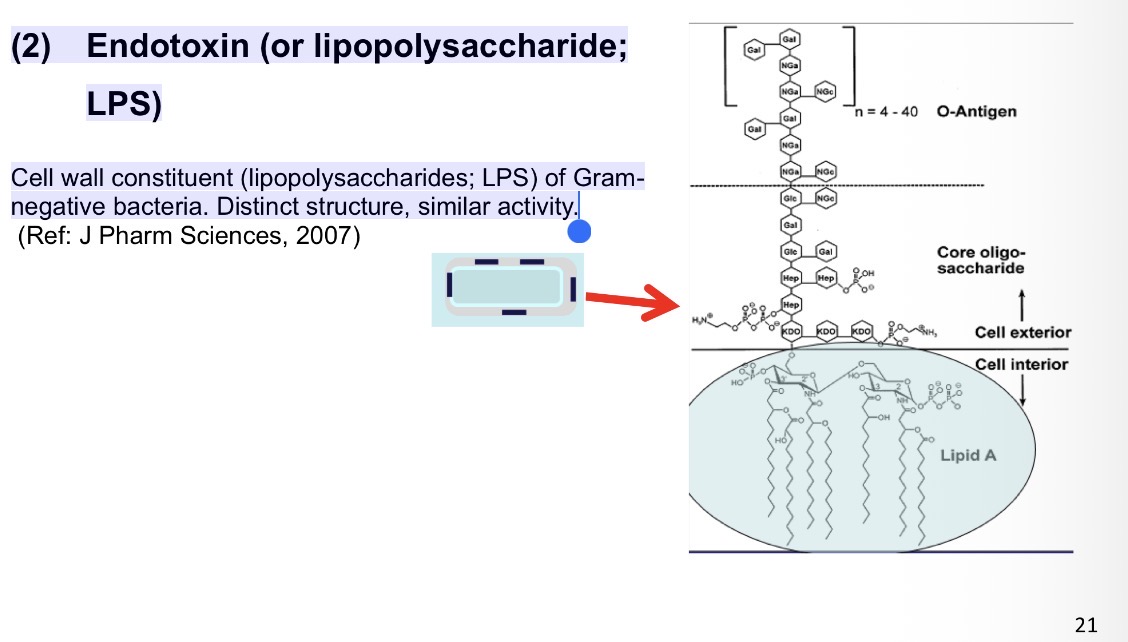
(2) Endotoxin (or lipopolysaccharide; LPS)
Cell wall constituent (lipopolysaccharides; LPS) of Gram-negative bacteria. Distinct structure, similar activity.
Obj. 2
Differentiate the four main types of infectious disease - toxigenic, extracellular, facultative intracellular, obligate intracellular-including their basic characteristics, common pathogens, and the most important host defenses.
Toxigenic Infections
immune response & pathology
Immune response and pathology
Septic Shock: Lipid A induces release of pro-inflammatory (IL-1beta, TNF-alpha) cytokines
Septic Shock: Endotoxin or lipopolysaccharide (specifically, lipid A: portion of endotoxin or LPS) induces IL-1 beta and TNF-alpha release from macrophages.
These cytokines are intensely inflammatory with actions on granulocytes, the complement and coagulation systems.
Bacterial endotoxins are similar in activity regardless of their source but are structurally unique to the organism.
Obj. 2
Differentiate the four main types of infectious disease - toxigenic, extracellular, facultative intracellular, obligate intracellular-including their basic characteristics, common pathogens, and the most important host defenses.
Toxigenic Infections
Protective Mechanisms and Management
Protective Mechanisms and Management
Antibodies
IgM bacteriolysins: causes lysis of Gram negative bacteria
IgG anti-capsular antibody -may actually be more protective but the capsular polysaccharides are often weakly immunogenic.
IgM antibody for lipid A
Anti-sepsis products:
Anti-inflammatory products, Activated protein C
Obj. 2
Differentiate the four main types of infectious disease - toxigenic, extracellular, facultative intracellular, obligate intracellular-including their basic characteristics, common pathogens, and the most important host defenses.
Extracellular Infection
Most common bacterial infections: Gram + & Gram –
Other examples: Spirochetes, Mycoplasma
Most susceptible to current anti-infectives
Important virulence factor for bacteria: anti-phagocytic capsule
Obj. 2
Differentiate the four main types of infectious disease - toxigenic, extracellular, facultative intracellular, obligate intracellular-including their basic characteristics, common pathogens, and the most important host defenses.
Extracellular Infection
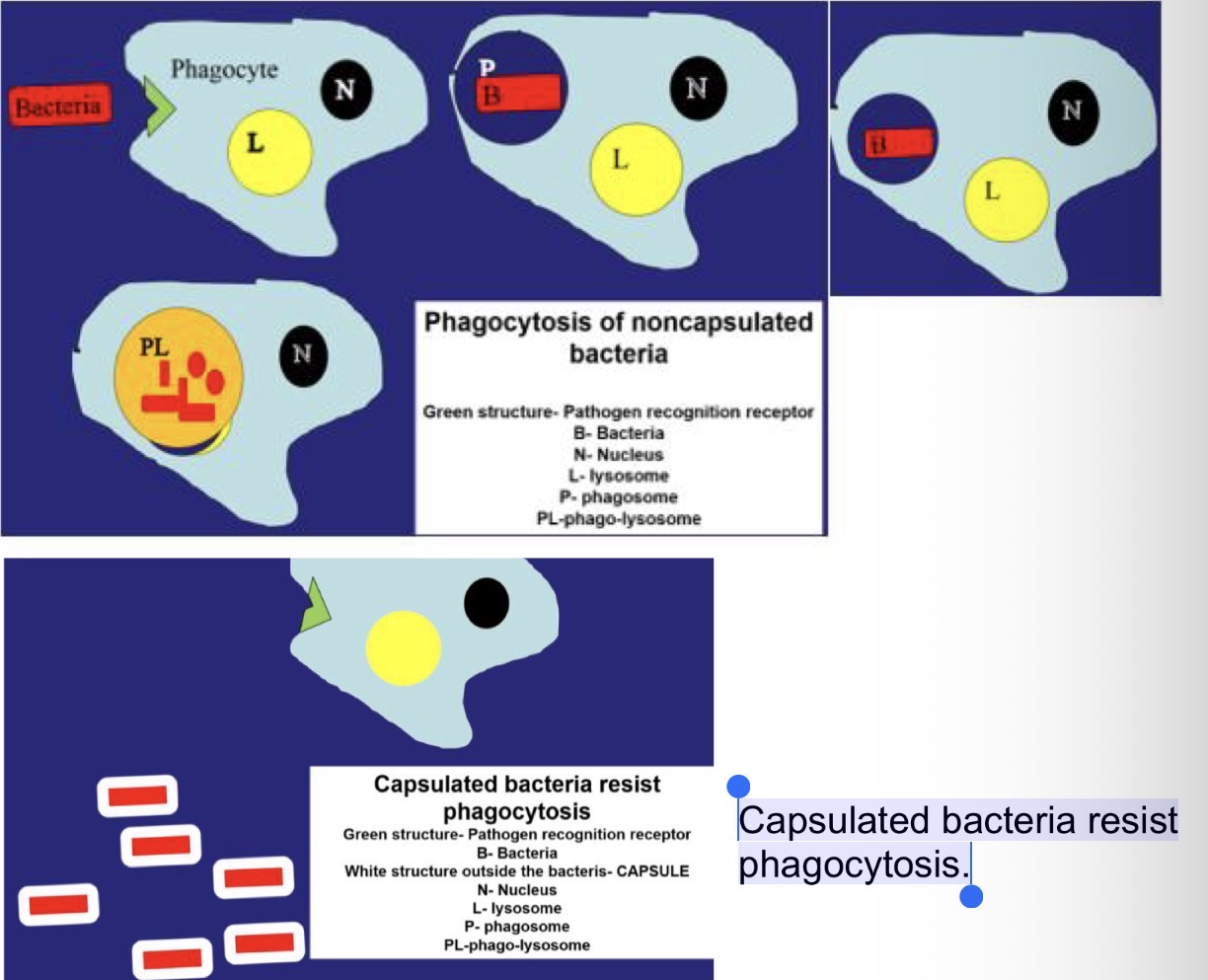
Phagocytosis of non-capsulated bacteria and capsulated bacteria
Capsulated bacteria resist phagocytosis.
(See pic for both noncapsulated and capsulated bacteria)

Obj. 2
Differentiate the four main types of infectious disease - toxigenic, extracellular, facultative intracellular, obligate intracellular-including their basic characteristics, common pathogens, and the most important host defenses.
Extracellular Infection
Establishment of Extracellular Infection
Phase of Infection
Attachment to epithelial receptors:
Bacterial SIgA proteases
Penetration of epithelium (endocytosis):
Intracellular at this stage
Acute inflammatory response:
Neutrophil, complement, anti-phagocytic factors, local Immune response
Lymphatic (&/or hematogenous) spread:
Systemic Immune response
Efferent phase of immune response:
IgG, IgM; sIgA prevents reinfection
Extracellular Infection = Most susceptible to current anti-infectives
Obj. 2
Differentiate the four main types of infectious disease - toxigenic, extracellular, facultative intracellular, obligate intracellular-including their basic characteristics, common pathogens, and the most important host defenses.
Extracellular Infection
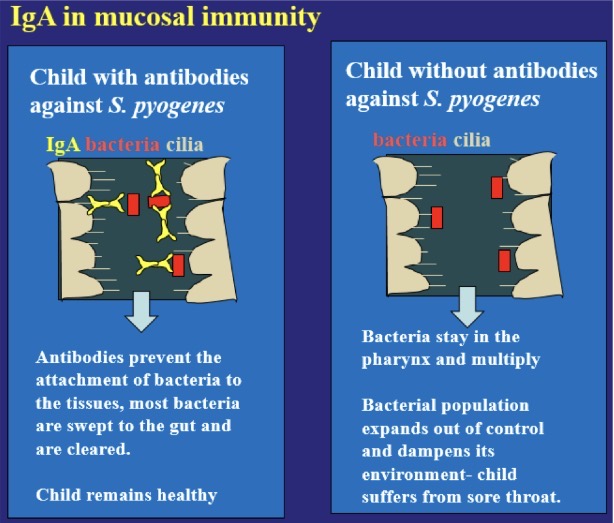
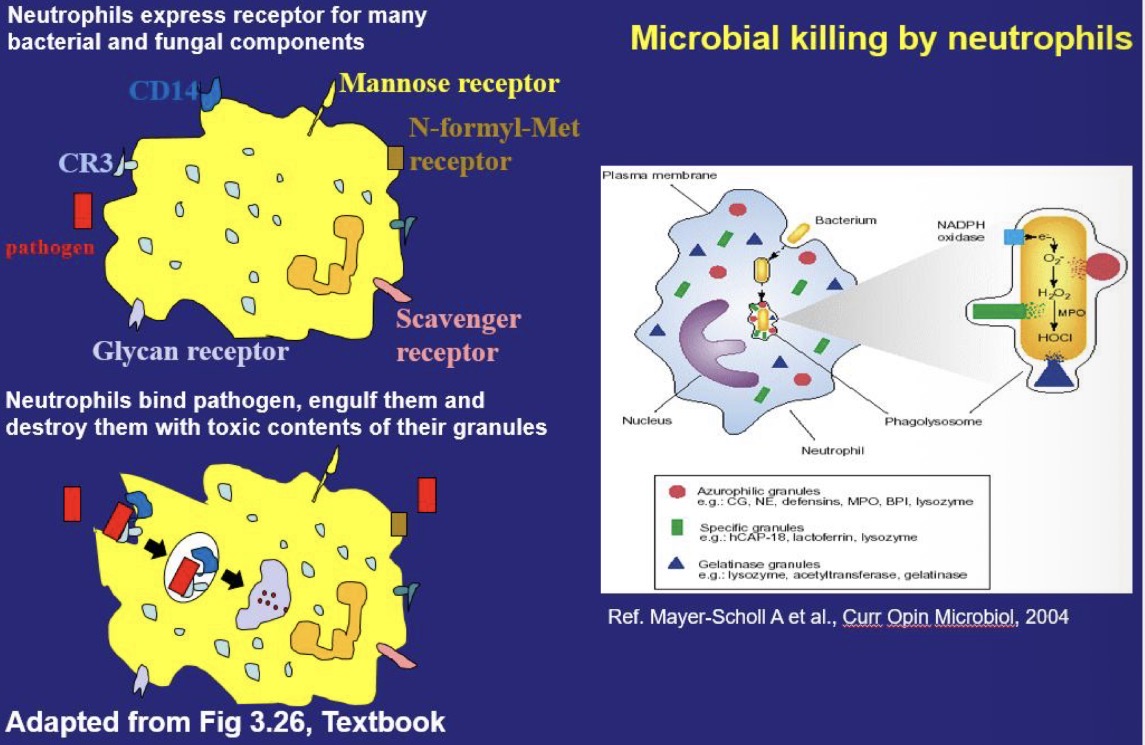
Antibodies and neutrophils are important for mucosal host defense.
Antibodies and neutrophils are important for mucosal host defense.
(See pics)
Obj. 2
Differentiate the four main types of infectious disease - toxigenic, extracellular, facultative intracellular, obligate intracellular-including their basic characteristics, common pathogens, and the most important host defenses.
Self-study:
Study the examples of extracellular infection, pathologies, and protective host immune mechanisms.
Toxigenic: toxin-mediated disease → antibodies neutralize toxins
Extracellular: outside cells → phagocytes + antibodies
Facultative intracellular: inside/outside → T cells + macrophages
Obligate intracellular: inside only → cytotoxic T cells

Obj. 2
Differentiate the four main types of infectious disease - toxigenic, extracellular, facultative intracellular, obligate intracellular-including their basic characteristics, common pathogens, and the most important host defenses.
Facultative Intracellular Infection
Phase of Infection
Attachment to epithelial receptors:
Same as extracellular
Penetration of epithelium (endocytosis):
Same as extracellular
Acute inflammatory response
Resists intracellular killing by neutrophils which die and release organisms
Monocyte/Macrophage Involvement:
May harbor organisms
Efferent phase of immune response
Cell mediated immunity or CMI (e.g., IFN gamma) Macrophage Activation
Facultative Intracellular Infection = Anti-infectives available but therapy generally less effective

Obj. 2
Differentiate the four main types of infectious disease - toxigenic, extracellular, facultative intracellular, obligate intracellular-including their basic characteristics, common pathogens, and the most important host defenses.
Self study:
Study the examples of facultative intracellular infection, pathologies, and protective host immune mechanisms.
Obj. 2
Differentiate the four main types of infectious disease - toxigenic, extracellular, facultative intracellular, obligate intracellular-including their basic characteristics, common pathogens, and the most important host defenses.
Obligate Intracellular Infection
Obligate Intracellular Infection
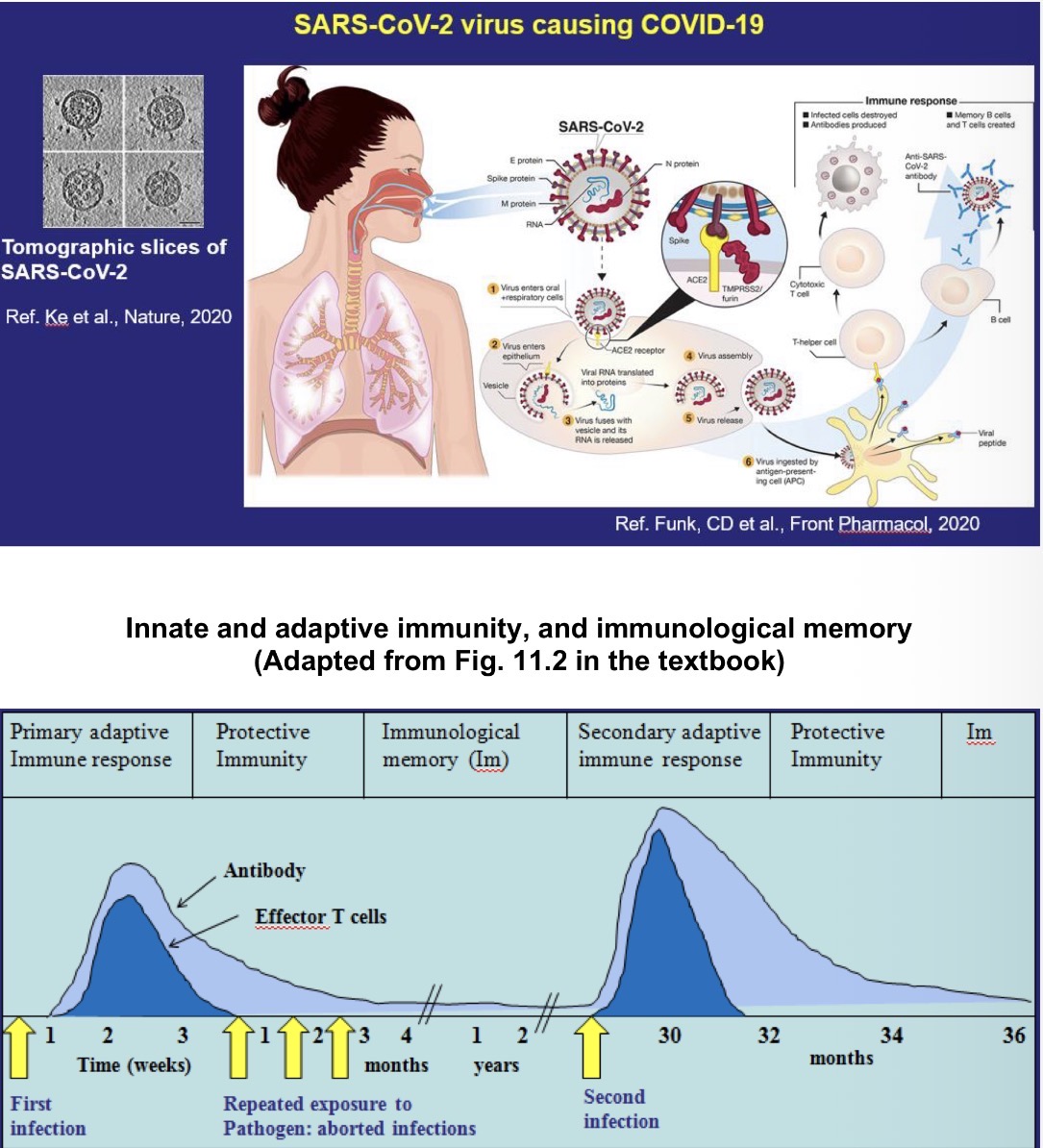
Examples: Viruses (including Coronavirus), Chlamydia, and Rickettsia
Major Virus Interactions: Acute, Chronic, Latent
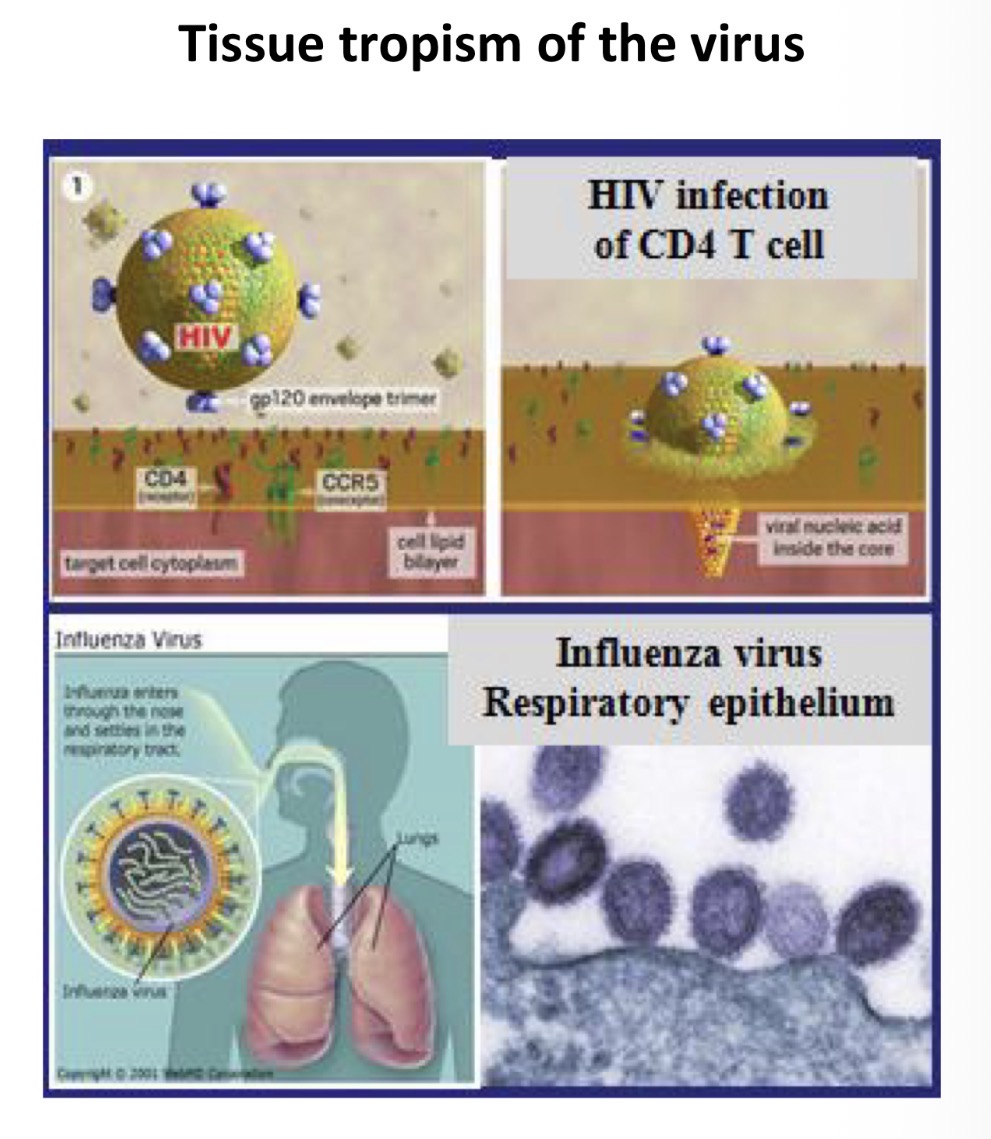
Determinants of pathology in virus disease:
Tissue tropism of the virus
Cytopathology of the virus
Immunologically-mediated tissue damage very common
General Immunologic Principles of Virus Infections
Interferon (Type I) is major nonspecific defense- NK and T cells contribute
CD8+ cytotoxic T cells most important for recovery
sIgA and/or serum IgG prevent reinfection
Obj. 2
Differentiate the four main types of infectious disease - toxigenic, extracellular, facultative intracellular, obligate intracellular-including their basic characteristics, common pathogens, and the most important host defenses.
Self-study
Study the examples of obligate intracellular infection, pathologies, and protective host immune mechanisms.
Obj. 3
Distinguish the host defense mechanisms against four main types of infections
A. Eukaryotic Pathogens
Fungi - Facultative intracellular host-pathogen interaction
B. Bacteria - Extracellular, facultative intracellular host-pathogen interaction
C. Viruses - Obligate intracellular host-pathogen interaction
Self study
1. Define following terms in 2-3 sentences: Innate immunity, inflammation, adaptive immunity, protective
immunity.
Self study
2. Discuss the dynamic nature of the triad of infection: how each of the variables—host, pathogen, therapy—can change significantly during any infection?
Self study
3. Attempt questions provided behind all the chapters in your textbook
(Look into textbook)
Terms
Inflammation
Terms
Innate Immunity
Terms
Adaptive immunity
Terms
Antigen presentation
Terms
Phagocytosis
Terms
Cell mediated immunity
Terms
Endotoxin, LPS
Terms
Intracellular infection
Terms
Effector immune cells
Terms
Effector molecules