Chapter 21
1/57
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
58 Terms
Tunica Interna
Innermost layer, adjacent to lumen
Tunica media
Middle layer of smooth muscle and elastic fibers, allowing arteries to regulate their diameter
Tunica externa
Outermost layer, adjacent to surrounding tissue
Elastic arteries (conducting arteries)
Large-diameter vessels with more elastic fibers, functioning as pressure reservoirs
Muscular arteries (distributing arteries)
Medium-diameter vessels that use smooth muscle to distribute blood to specific body parts
Anastomosis
the union of two or more arteries supplying the same region, providing an alternate route for blood flow
End Arteries
Only 1 artery supplies something, if blocked then fucked
Capillary walls
single layer of squamous cells, thin enough to allow exchange of nutrients and wastes between blood and tissue cells
Continuous capillaries
the most common type, with a sealed wall that only allows small substances through. muscles + lungs
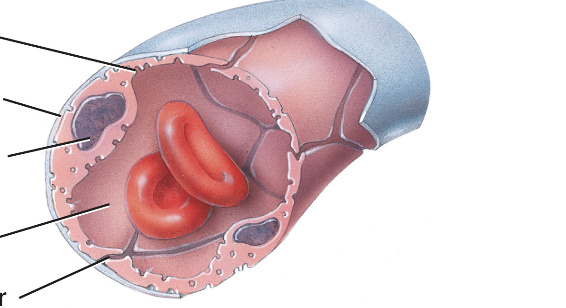
Fenestrated capillaries
have small pores in the wall, allowing more substances to pass through quickly. kidneys + small intestine
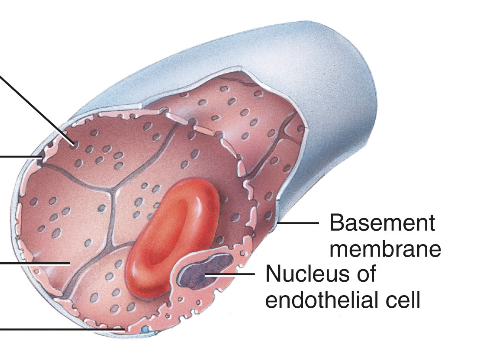
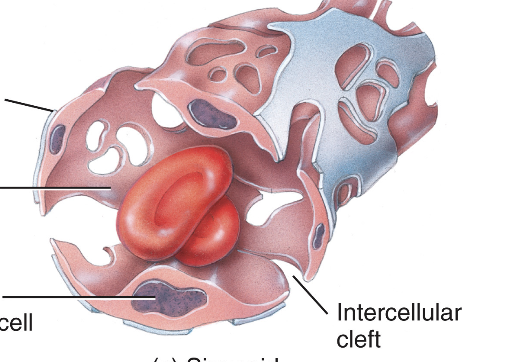
Sinusoid capillaries
have large gaps in the wall, allowing even large substances like proteins and blood cells to pass through. liver + bone marrow
Venules
small vessels that are formed by the union of several capillaries
Veins
formed from several venules, has thinner tunica interna and media but a thicker tunica externa then arteries. (less elastic + smooth muscle)
Varicose veins (varicosities)
formed when venous valves become weak or damaged (looks twisted)
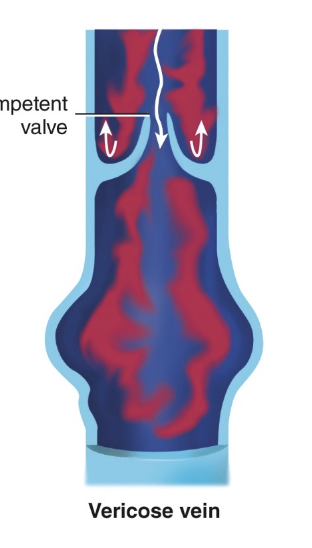
Venous Valves
structures in veins that prevent backflow
Spider veins
same thing as Varicose but in Venules
Blood Distribution
largest portion of blood is in Veins and Venules
Diffusion in Capillaries
Small nonpolar substances like O2 and CO2 pass directly through, while larger polar substances like glucose and a.a require facilitated diffusion
Simple diffusion
substances move freely on their own from high to low concentration, no help needed
Facilitated diffusion
substances are too large to pass through on their own, so they use a protein channel as a "door" to get through
Transcytosis
Endocytosis + Exocytosis, used for large lipid insoluble molecules for capillary exchange
Bulk flow
exchanges fluid by pushing around higher to lower pressure differences using Filtration + Reabsorption
Filtration
when pressure high pushes fluid and dissolved substances out of the capillary into the surrounding tissue (BHP + IFOP)
Reabsorption
when pressure low fluid and dissolved substances go back into the capillary from the surrounding tissue (BCOP + IFHP)
BHP + IFOP
the Blood hydrostatic pressure and Interstitial fluid osmotic pressure pushing shi out of capillary
BCOP + IFHP
the Blood colloid osmotic pressure and Interstitial fluid hydrostatic pressure that put shi into the capillary
Blood flow
mL/min
Cardiac Output (CO)
The volume of blood pumped by the heart per minute
Blood Pressure
Blood pressure is affected by cardiac output, blood volume, and vascular resistance
Mean arterial pressure (MAP)
= CO x resistance (R)
> the BV ↑ the BP
Cardiac Output Equations
CO = heart rate (HR) × stroke volume (SV)
CO = mean arterial pressure (MAP) ÷ resistance (R)
Mean Arterial Pressure (MAP)
The avg BP in the arteries throughout one complete heartbeat
Vascular Resistance
How difficult (resistance) it is for blood to flow through a vessel.
3 Factors of Vascular Resistance
Vessel size — smaller vessel = harder to flow through
Blood thickness — thicker blood = harder to push through
Vessel length — longer vessel = more friction = harder to flow through
Systemic vascular resistance (SVR)/total peripheral resistance (TPR)
total resistance of every single blood vessel in your entire body added together
Venous Return
volume of blood flowing back to the heart through the systemic veins
3 Factors of Venous Return
Relax/Contract Heart — suction from heart relaxing pulls blood in
Skeletal muscle pump — muscles squeeze veins pushing blood toward heart
Respiratory pump — breathing in creates suction that draws blood toward heart
Velocity of Blood Flow
Blood velocity decreases as total cross-sectional area increases, and increases as it decreases
CO = HR × SV
Cardiac output = how fast heart beats × how much blood per beat
If HR or SV goes up, CO goes up
CO = MAP ÷ R
Cardiac output = blood pressure ÷ resistance
More resistance = less blood flow
MAP = CO × R
Blood pressure = cardiac output × resistance
If CO or R goes up, blood pressure goes up
Medulla Oblongata
Contains Cardiovascular Center
Cardiovascular center
A group of neurons in the medulla oblongata that regulate heart rate, contractility, and blood vessel diameter
3 Sensory receptors input to Cardiovascular Center
Proprioceptors (joint),
Baroreceptors (BP),
Chemoreceptors (Blood acidity, H+, CO2, O2)
3 Sensory receptors output to Cardiovascular Center
Vagus nerve (para, slows heart),
cardiac accelerator (sympathetic),
vasomotor nerve (sympathetic constrict vesssels)
Baroreceptors
Sensory neurons that detect stretching in blood vessel walls and atria. Found in carotid sinuses + aorta
Vasoconstriction
(increases BP) → caused by Angiotensin II, ADH, norepinephrine, epinephrine
Vasodilation
decreases BP) → caused by ANP, epinephrine, nitric oxide
Increase blood volume
Aldosterone (sodium) and Antidiuretic (heart)→ they make kidneys hold onto water, keeping more fluid in blood
Decrease blood volume
(decreases BP) → Atrial Natriuretic Peptide — makes you pee more, reducing fluid in blood
Autoregulation
tissues can control their own blood flow without needing the brain to tell them what to do (caused by Physical and chemical stimuli)
Systolic BP
First sound heard
Diastolic blood pressure
Last sound heard
Shock
failure of the cardiovascular system to deliver enough oxygen and nutrients to meet the metabolic demands of body cells
Hypovolemic shock
dangerously low blood volume due to blood or fluid loss
Cardiogenic shock
heart fails to pump enough blood to meet the body's needs
Vascular shock
excessive vasodilation causes blood pressure to drop critically low
Obstructive shock
physical blockage prevents blood from flowing properly through the heart or vessels