Patho (Female Reproductive Tract)
1/337
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
338 Terms
What are parts of the lower GU tract?
- Vagina
- Cervix
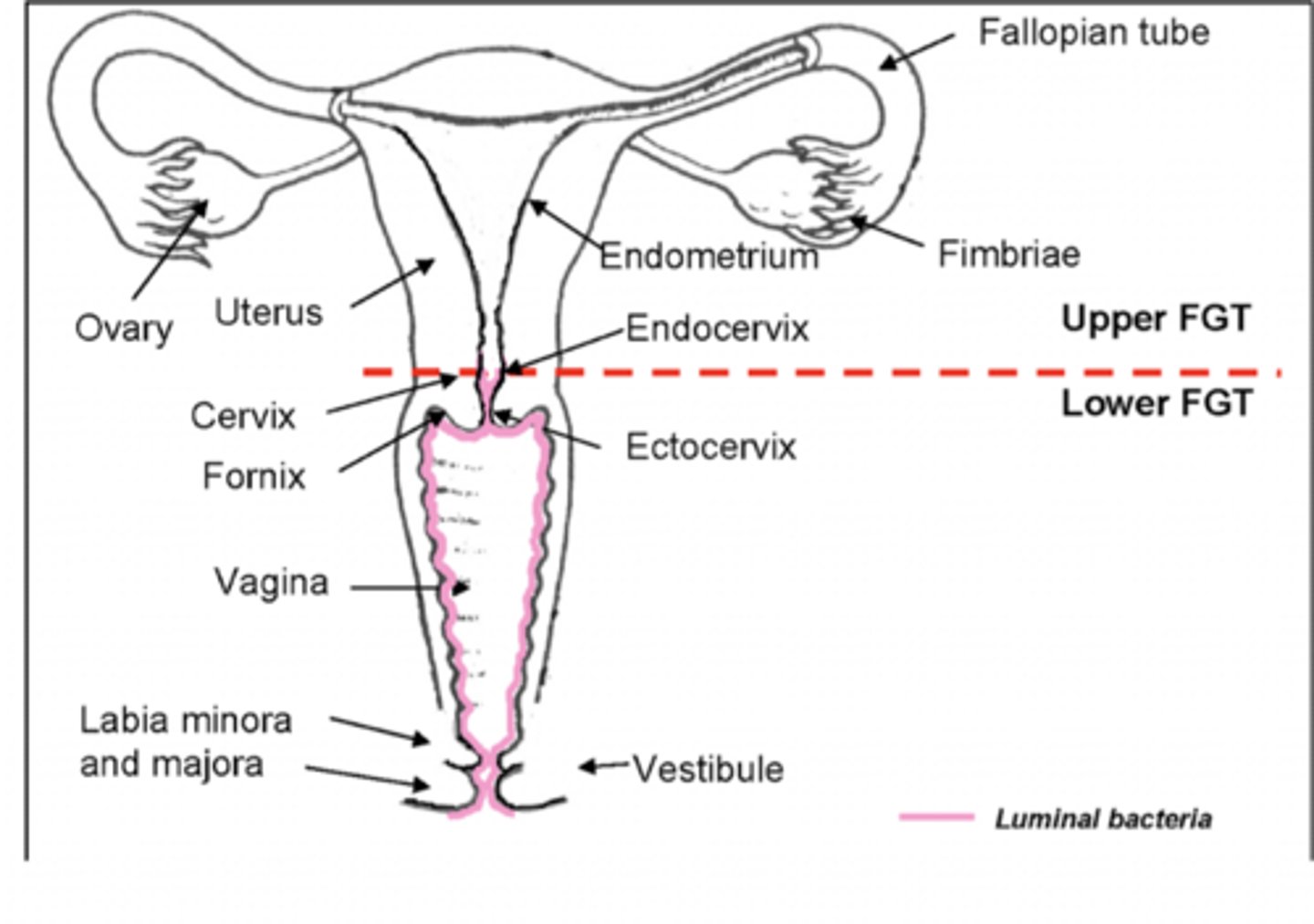
What are parts of the upper GU tract?
- Uterus
- Fallopian tubes
- Ovaries
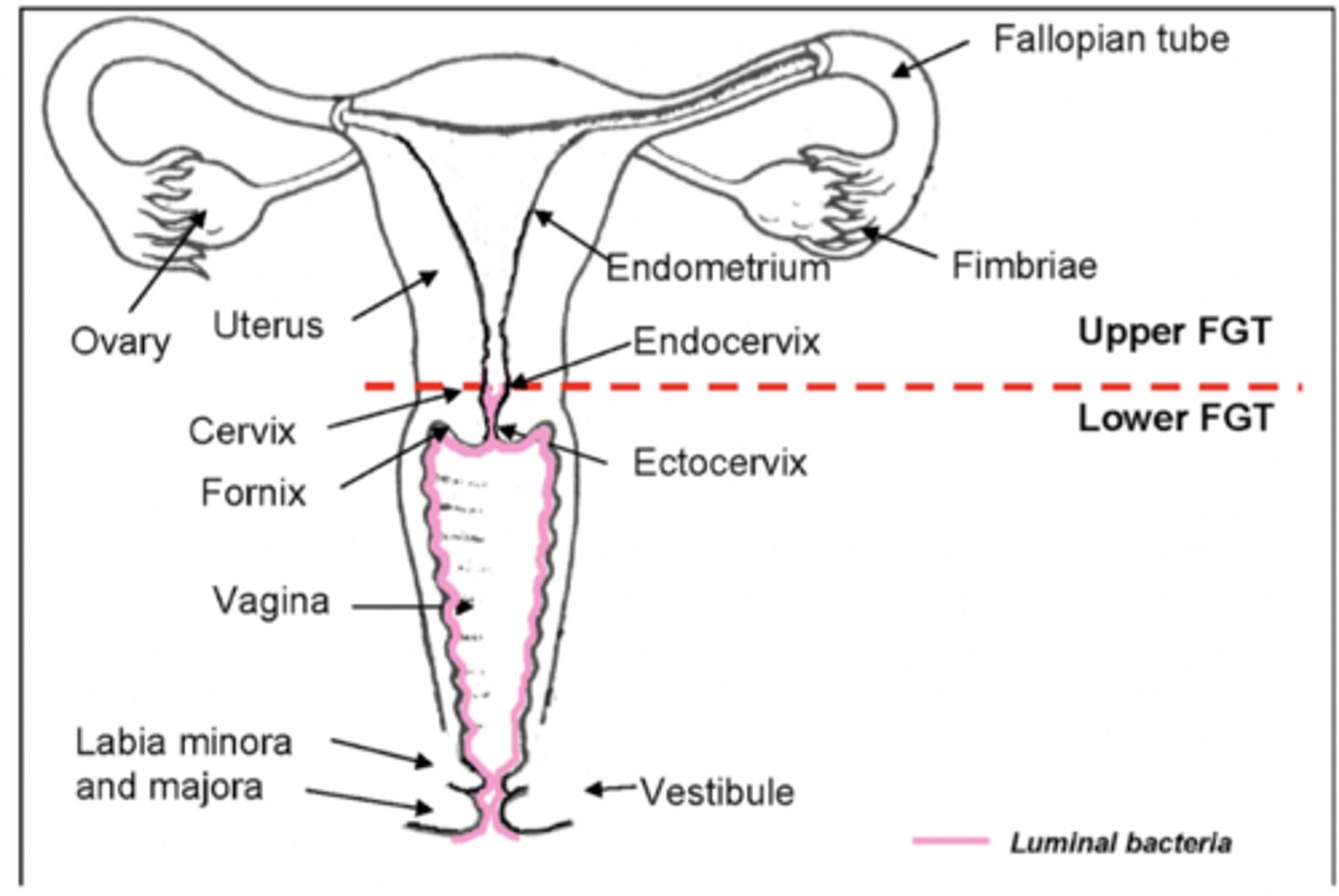
What is the vulva? (what does it include)
Includes mons pubis, labia majora and minora, vestibule (external genitalia)
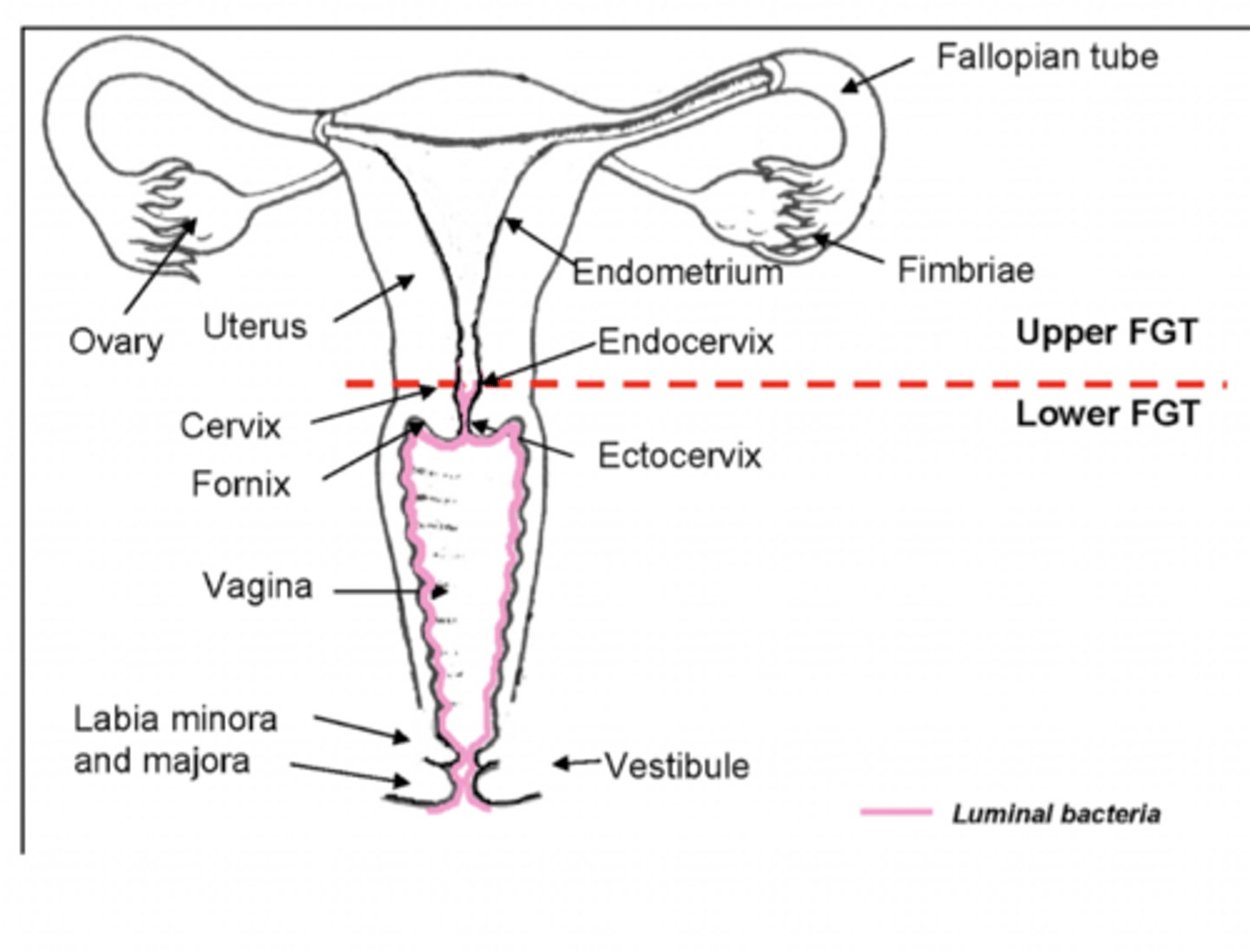
The vagina spans from _________ to __________.
Cervix to vestibule
Why is the cervix considered part of the lower GU tract?
Has different cell types than uterus --> why they are part of lower and upper GU tract, respectively
What causes the hypothalamus to begin releasing gonadotropins in puberty? What does this cause?
Unknown mechanism, will stimulate the anterior pituitary to secrete FSH and LH
How do the ovaries respond to stimulation from the hypothalamic-pituitary axis?
Start making estrogen and progesterone
What is the role of the uterus in the menstrual cycle?
Response to the increased estrogen and progesterone
What is the action of granulosa and theca cells due to LH and FSH stimulation (general overview)?
Start making primarily estrogen
As estrogen increases, this stimulates uterine endometrial build-up
What is the role of the LH surge in the menstrual cycle?
Ovulation!
Expels the ovum into the fallopian tube
What happens to the follicle after expulsion of the ovum?
Does not completely disappear, will become the corpus luteum and produce progesterone (to maintain the endometrial lining)
What stops progesterone production?
Degradation of the corpus luteum
Leads to endometrial shedding and menstruation
An anovulatory cycle is due to lack of:
LH/FSH surge --> ovulation does not occur
Why does an anovulatory cycle lead to abnormal bleeding?
If ovulation does not occur, corpus luteum does not get produced --> production of progesterone does not occur --> will cause overgrowth of the endometrial lining
What happens to the hormones when anovulatory cycles occur?
Estrogen elevated
FSH depressed (negative feedback from estrogen)
What is the action of granulosa cells?
Picks up androgens from the theca cells and converts it to estrogens (estradiol) in the presence of FSH
What is the action of theca cells under LH stimulation?
Under LH stimulation, produce progesterone --> converted to androgens
What happens to the follicles in polycystic ovarian syndrome (PCOS)?
Follicles get arrested in pre-ovulation phase
Due to persistent follicle maturation --> androgens will predominate, LH persistently elevated --> will cause hirsutism, increased weight, male pattern baldness, acne
What is metrorrhagia
bleeding between periods
What is menorrhagia
heavy menstrual bleeding
what is dysmenorrhea
painful menstruation
what is amenorrhea
absence of menstruation
What is dyspareunia
painful intercourse
What is abnormal uterine bleeding?
Formally dysfunctional uterine bleeding (DUB)
What causes abnormal uterine bleeding?
abnormality within the uterus
- hypothalamic immaturity
-inadequate luteal function
What is the most common cause of abnormal uterine bleeding in adolescence?
Disturbance of the hypothalamic-pituitary-ovarian axis (hypothalamic immaturity, inadequate luteal function)
What is the most common cause of abnormal uterine bleeding in reproductive age?
Anovulatory bleeding
What causes anovulatory bleeding?
Excessive estrogen stimulation leads to a continuous proliferative phase of the menstrual cycle
There is no progesterone to start the secretory phase
Thrombosis of tissues will cause bleeding that is out of sync with the other endometrium
Eventual involution of the dominant follicle will drop estrogen production and cause bleeding (severe)
Does PCOS cause severe bleeding?
No, because there are several follicles so the estrogen does not drop after one goes away
What are examples of abnormal uterine bleeding that are not dysfunctional uterine bleeding?
- Growths
- Leiomyoma (fibroids)
- Polyps
- Inflammation
- Pregnancy
- IUD related
What are some examples of bacterial genital infections?
- Gonorrhea
- Chlamydia
- Mycoplasma
- Calymmatobacterium granulomatis
- Haemophilus ducreyi
- Gardnella vaginalis
- Syphilis
Gonorrhea, chlamydia, and mycoplasma typically infect ___________________ causing _______________.
Infect mucous membranes and irritate them --> cause discharge
What is calymmatobacterium granulomatis? What does it cause?
Bacterial genital infection
causes inguinal lymphadenopathy and granulomas (ulcer: granuloma inguinale)
Does not really cause inflammation of the mucous membranes
What is Haemophilus ducreyi? What Does it cause?
Chancroid, painful lesion similar to syphilis
Where is Haemophilus ducreyi and calymmatobacterium granulomatis seen?
Seen in tropical climates
What is the difference between Haemophilus ducreyi and calymmatobacterium granulomatis?
Haemophilus ducreyi --> painful ulcer
Calymmatobacterium granulomatis --> painless ulcer
What is Gardnella vaginalis? What does it cause and How?
Bacterial genital infection that causes non-specific vaginitis (BV)
Is a naturally occurring bacteria in the genital tract, can overgrow and cause BV due to some sort of exogenous reason
is Gardnella vaginalis sexual transmitted?
NOT SEXUALLY TRANSMITTED
What is syphilis?
Bacterial genital infection that penetrates mucous membranes and causes chancroid lesion (ulcer)
No associated mucosal inflammation --> no discharge associated
Which infections do no involve discharge but instead involve ulcers
Haemophilus ducreyi --> painful ulcer
Calymmatobacterium granulomatis --> painless ulcer
Syphlis --> painful ulcer
What is trichomonas vaginalis
A disease caused by protozoa and transmitted through sexual intercourse
- seen in women (and men who have sex with women)
What is gonococcus? What does it do?
Gram negative diplococcus that invades mucous membranes and causes acute inflammation
What are symptoms of gonorrhea?
- Purulent discharge (due to invasion of mucous membranes)
- 1/2 of women remain asx
What does gonorrhea infect?
- Endocervix and vaginal canal (primary site of infection)
- Urethra
What is the primary site of gonorrhea infection in females?
Endocervix and vaginal canal
Where can gonorrhea be seen in men through sexual contact?
Rectum (men who have sex with men)
Gonococcal infection can progress into which areas?
- Ascend to endometrial cavity and cause endometritis
- Salpingitis (fallopian tubes)
- Ovaries --> will cause tubo-ovarian abscesses
- Pelvic and abdominal cavity --> PID
- Systemic --> septicemia, septic arthritis
Gonococcal infection can be transmitted:
To babies (neonatal transmission)
What happens when a gonoccal infection is passed to a baby
As baby is passing through vaginal canal, the infection can be transmitted to the baby --> commonly manifests in the eyes as conjunctivitis
Gonococcal infection can cause __________ in young men.
Septic arthritis!!
A young male presents to the ED with a red, swollen knee joint with no hx of injury/overuse. What do you suspect?
Gonococcal septic arthritis
What is chlamydia trachomatis? What does it cause?
Gram negative intracellular bacteria that can cause genital infection in females
What are symptoms of chlamydia?
- Reactive arthritis
- Invasion of mucous membranes --> discharge, erythema
Is reactive arthritis the chlamydia infection?
No!
A patient can still have reactive arthritis even if infection clears
What can we see on microscopy of chlamydia trachomatis?
Intracytoplasmic coccoid bodies
How will neonatal chlamydia present?
Pneumonia
What is Lymphogranuloma Venereum?
C. trachomatis strains L1-L3
What does Lymphogranuloma Venereum cause?
painless vesicles and ulcers
inguinal lymphadenopathy
What is the difference between regular chlamydia trachomatis and Lymphogranuloma Venereum?
Lymphogranuloma venereum does not invade mucous membranes as regular chlamydia does, presents more like syphilis
What is mycoplasma genitalium? What can it cause?
Small bacteria with no cell wall that is usually a normal, commensal organism that lives in the GU tract
Can overgrow and lead to PID, post gonoccal urethritis
Mycoplasma genitalium infections can cause:
- PID
- Post gonoccocal urethritis
Why do we get Mycoplasma genitalium infections?
Not completely understood
What is trichomonas? Who is it seen in?
Pear-shaped flagellated protozoa
Only grows naturally in females, can be transmitted to males via sex
What are symptoms of trichomonas?
- Heavy, yellow-gray, thick, foamy discharge
- Itchiness
- Dyspareunia (pain on sexual intercourse)
- Dysuria (invades urethra)
What can be seen on wet mount of trichomonas?
Motile trichomonas
What are some locations of genital infections?
- Cervix (cervicitis)
- Urethra (urethritis)
- Endometrium (acute endometritis)
- Fallopian tubes (salpingitis)
- Abdomen/pelvic cavity (PID)
What are some causes of cervicitis?
- STI
- Strep (especially group B), staph, enterococcus (E. coli)
- HSV
- Polymicrobial
How does cervicitis present?
Vaginal discharge
What are some causes of urethritis?
- Most common = E. coli
- Can be due to STI, HIV
How does urethritis present?
Dysuria
What happens if infection spreads past the urethra?
Acute endometritis
What are some causes of salpingitis?
- Typically due to ascending infections
- N. gonorrhea, E. coli, Chlamydia, Mycoplasma
- Most polymicrobial
What are the different types of salpingitis?
- Pyosalpinx
- Hydrosalpinx
- Tubo-ovarian abscess
What is a complication of salpingitis?
Ectopic pregnancy
Causes scarring --> big risk for infertility in females down the road
What is pelvic inflammatory disease (PID)?
Extension of bacteria beyond the uterus
Can result in:
- Salpingitis
- Tubo-ovarian abscess
What are symptoms of PID?
- Lower abdominal pain
What increases risk of PID?
IUDs, STIs
What are some viral infections of the genital tract?
- HPV
- HSV
What is another infection of the genital tract (besides viral and bacterial)?
Candidiasis
What strains of HPV cause visible (condylomata acuminatum) genital infection?
6, 11
Will cause visible warts on the cervix/ectocervix
What strains of HPV cause squamous cell cancer?
16, 18, 31
High grade/high risk HPV strains --> typically do not present with anything visible, will cause cellular dysplasia at the cervix
How does HSV present in the genital tract?
Painful lesions (typically multiple lesions)
What is candidiasis and what causes it?
Overgrowth of yeast, commonly following antibiotic use (especially amoxicillin)
Candida albicans most common organism
Which organism most commonly causes candidiasis?
Candida albicans
How does genital candidiasis present?
- White, thick discharge
- Itchiness
- +/- pain on urination
What are risk factors for genital candidiasis?
- Immunosuppressive tx
- DM
- Oral contraceptives
- Pregnancy
What is toxic shock syndrome?
Staph aureus proliferation and release of toxic shock syndrome toxin-1 --> causes release of cytokines throughout the body
First recognized when long-acting tampons were introduced
Does the actual infection of staph aureus cause toxic shock sndrome?
NO!! The toxin that is released is what causes it
What are symptoms of toxic shock syndrome?
- Fever, shock
- Desquamative erythematous rash (peeling)
- Nausea, vomiting, diarrhea
- Neuro signs (due to neurotoxin) -ex. semiparalysis, AMS
- Thrombocytopenia, DIC
What is a common complication of toxic shock syndrome?
DIC
Significant mortality associated
What are the different disorders of the vulva?
- Bartholin gland cyst
- Hair follicle cyst
- Mucinous cysts
- Dermatitis
- Extramammary Paget disease
- Squamous cell carcinoma
What is a Bartholin gland cyst?
Bartholin gland ducts can get obstructed and inflamed
What are Bartholin glands?
Produce mucus and lubrication for the vagina
What are the different types of dermatitis that can occur in the vulva?
- Atopic, seborrheic
- Lichen planus, psoriasis, lichen sclerosus
What is extramammary Paget disease?
What does it cause?Who does it occur in?
Large, red, moist, sharply demarcated lesions that are rarely associated with carcinoma
Usually occurs in older women
What are symptoms of extramammary Paget disease?
- Pruritus
- Burning sensation
Extramammary Paget disease usually involves the:
Labia majora
What are the two pathways of developing SCC of the vulva?
- Keratinizing squamous cell -- not related to HPV
- Warty and basolateral carcinomas -- related to HPV-16 infection
What is seen with Keratinizing squamous cell
long standing lichen sclerosis --> predispose someone to SCC
Squamous cell carcinoma of the vulva usually occurs in women of what ages?
>60