FNH 351 - Bone nutrients - magnesium
1/23
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
24 Terms
what are the metabolic functions of magnesium?
bone mineralization
enzymatic reactions
other roles:
Blood clotting, reduced platelet aggregation
Second messenger signaling
Ion channel regulation (K and Ca channels)
Antagonism of intracellular calcium
Insulin production, release, and action signalling
how is magnesium involved in bone mineralization/structural component of bone?
50-60% of total body Mg is in the bones in the form of Mg(OH)2 and Mg3(PO4)2). Found on bone surface as available pool to maintain plasma Mg concentration. Together with calcium and phosphorus → forms bone crystal lattice. Mg likely deposited at time of bone formation and important for mineralization
how does magnesium function in enzymatic reactions?
it is a structural cofactor to stabilize enzyme of allosteric activator.
It assists in stabilization of ATP and transfer of phosphate group
enzymatic roles including in glucose, fat, protein, vitamin, and nucleic acid metabolism
needed for hydroxylation of vitamin D in the 25-position (25-hydroxylase)
how is mg digestion
no digestion needed
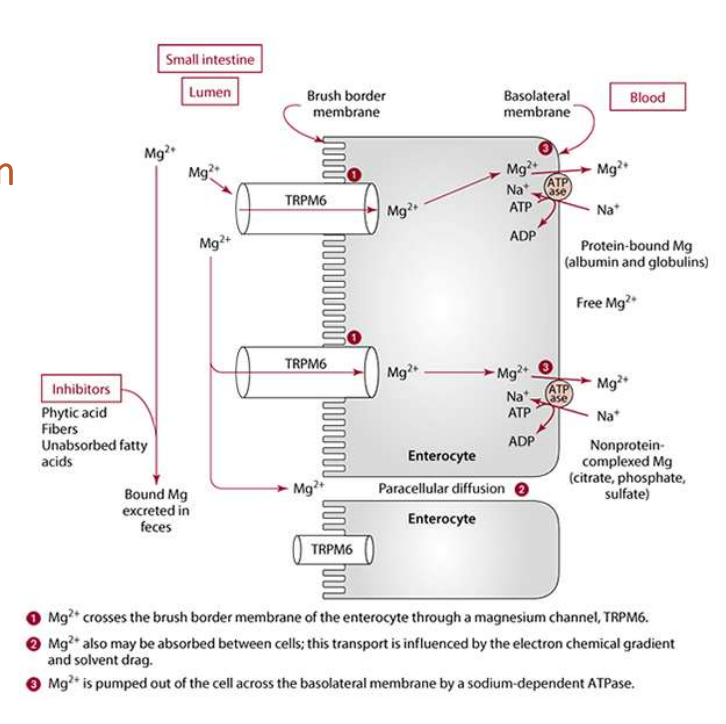
how is mg absorbed?
Where: small intestine
How: in form of Mg2+
Saturable, carrier-mediated, active transport via TRPM6 inhibited by high cytosolic Mg concentration
Paracellular diffusion (main mechanism at high intakes) increases as Mg concentration in lumen increases
Efficiency varies (30 – 60%); depending on Mg intake
what are the enhancers of mg bioavailability
Vitamin D
Protein
Carbohydrates – fructose and oligosaccharides
what are the inhibitors of mg bioavailability?
Phytic acid (whole-grain breads, seeds, legumes)
Non-fermentable fiber (e.g. cellulose) increases the bulk of intestinal content reduces transit time → reduced time available for Mg absorption
Unabsorbed fatty acids (in case of fat malabsorption; form soaps with Mg)
Phosphorus (forming non-bioavailable complex Mg3(PO4)2)
how is mg transported?
→ In enterocyte
Crosses cytosol
→ Across the basolateral membrane
Na+-ATPase pump
→ Transport in blood, including hepatic portal vein
Free Mg2+ (50-55%) = physiologically active form
Bound to protein, mainly albumin (20-30%)
Complexed with sulfate, phosphate, and citrate (5-15%)
(1 and 3 in eq’m)
plasma m is tightly maintained. What is its homeostasis regulated at?
intestinal absorption and urinary excretion
how is mg excreted?
Excretion mainly through kidney
Fecal Mg
minor losses (sweat)
what is Mg excretion thru kidney affected by?
dietary Mg intake
plasma Mg concentration
PTH
what factors promote urinary Mg excretion?
Diuretic medications
Protein
Alcohol
Caffeine
what Mg is excreted through feces?
unabsorbed Mg
endogenous Mg sources
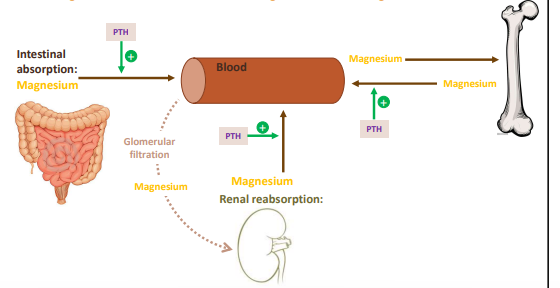
how is Mg homeostasis regulated?
serum Mg concentration underlies tight homeostatic regulation
what are the nutrient-nutrient interactions with Mg?
P and Mg
Ca and Mg
K+ and Mg
what is the nutrient-nutrient interaction between P and Mg?
Mg inhibits P absorption: with increasing Mg intake → decreasing P absorption due to formation and precipitation of Mg3(PO4)2
what is the calcium and Mg nutrient-nutrient interaction?
Low Mg associated with hypocalcemia: Mg2+ cofactor for 25-hydroxylase
Excess Mg interferes with calcium function:
Mg2+ reduces Ca2+ flux across membranes and activates Ca2+-ATPase pumps → reduce intracellular [Ca2+]
Mg2+ competes with Ca2+ for binding sites on troponin C and myosin → alters muscle contraction
Compete for reabsorption in the kidney
what is the nutrient-nutrient interaction btwn K and Mg?
[Mg2+] influences extra-/intra-cellular potassium (K+) balance
Mg2+ depletion → increasing K+ efflux from cells and subsequent renal K+ excretion
what do non-specific symptoms of mg deficiency cause? what are they?
Delayed diagnosis
Fatigue, lethargy, weakness
Anorexia, nausea, vomiting
how is mg deficiency diagnosed?
Plasma/serum magnesium concentration
Routinely measured indicator, but not sensitive and debated cutoff
what are the metabolic consequences of Mg deficiency?
Magnesium deficiency leads to decreased serum concentration of calcium, potassium, and 1,25-(OH)2-D
what are symptoms of Mg deficiency?
neuromuscular impairment (e.g., tremors, latent tetany)
cardiovascular symptoms (e.g., rapid heart rate, higher blood pressure)
central nervous system
what can mg excess be caused by?
Excessive magnesium from food sources does not cause toxicity, due to efficient renal excretion.
Excessive intake possible from high-dose supplements.
what are symptoms of mg excess?
Nausea, vomiting
Depression
Muscle weakness
Paralysis