Staging and grading
1/15
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
16 Terms
Staging
The estimation of the extent of disease (of both primary and metastatic tumours). Aids in treatment planning, prognosis, and evaluation of treatment modalities.
Staging systems
Describe whether or not, and to what extent spread has occured. Considering size of primary, involvement of local structures, spread via lymphatics, presence of absence of distant metastases.
Critea of staging system
Be able to be used for all tumours and sites. Be simple to use and interpret. May not be available in less developed countries. Not be dependent on complex investigations. Criteria for each stage must be set out in a logical progression from the least to the greatest involvement.
TNM System
Most commonly used staging system. Each letter has a number suffix ranging from 0-4. Number indicates degree of involvement.
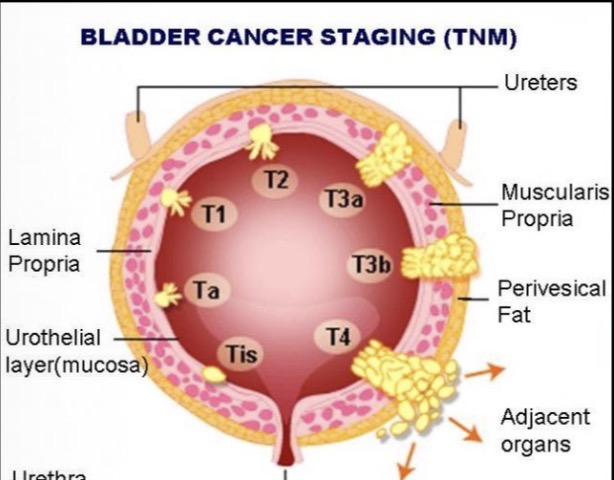
T= Tumour
Reffers to primary tumour size, depth and growth. TX= tumour cannot be measured. T0= no evidence of primary tumour. T(is)= cancer cells growing in most superficial layer of tissue with no growth into deeper layers.
N= Node (lymph)
N1= mobile nodes on ipsilateral side as primary. N2=1 N2= mobile nodes on contralateral side of primary. N3= spread to more distant or numerous involved nodes.
M= metastases
Absence or presence of metasteses. M0= absent. M1= present.
Clinical staging vs pathological staging
cTNM based on evidence aquired before treatment from physical examination, radiological studies and biopses. pTNM based on evidence evidence aquired from surgical procedure, surgical exploration or pathological examination.
y,r,a TNM
yTNM= stage assessed after chemo/ RT. rTNM= stage for reccurent tumour after period of time disease free. aTNM= stage determined at autopsy (after death).
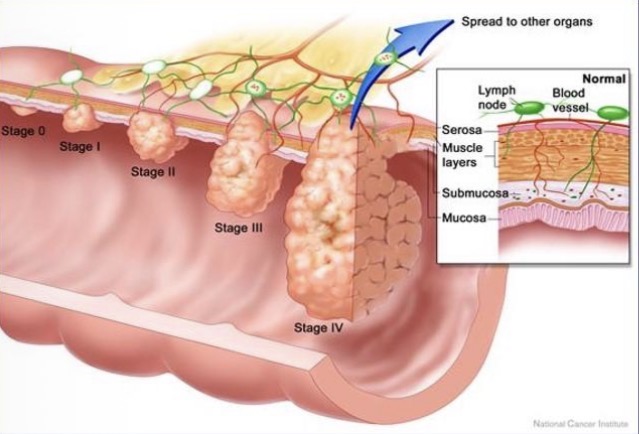
Stage grouping
Tumours can be grouped into stage 0-4. Ensures each group is homogenous in sense of survival.
Other staging systems
CNS cancers staged according to their cell type and grade. Blood or bone marrow is more a systemic disease so no staging system. FIGO used for cervix, uterus, ovary, vagina, and vulva cancers. Some childhood cancers use COG criteria.
Grading
Well differentiated tumours resemble parent tissue and easily recognisable. Undifferentiated tumours are messy and dont resemble parent. Tumours are graded based on degree of malignancy, ranging from 1-4.
Four tier grading system
grade 1= well differentiated. grade 4= undifferentiated. Higher grade= more likely to be malignant.
Grading importance
To determine likely behaviour of tumour (high grades less curable). Help determine treatment choice. Higher grade= worse prognosis

Gleason scoring
Biopsy samples are graded (1-5) to show activity of prostate cancer. Grade 1-2 very rarely found. Malignant tumours graded 3-5. More than 1 grade of cancer, so the grade of 2 most common patterns in biopsy sample are added to give Gleason score with the most common being first.
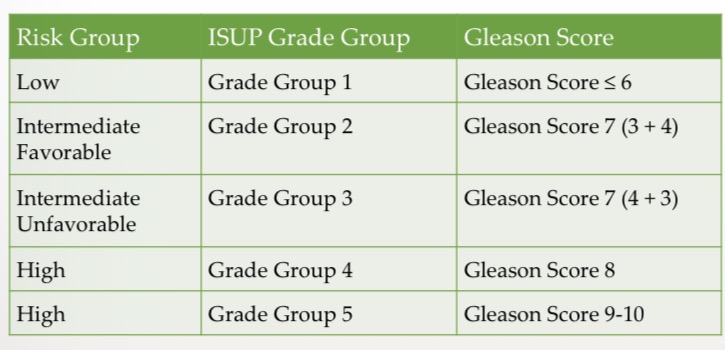
ISUP grouping
Enhanced from gleason score. Simpler with 5 grades