L19. Medical Management of Rheumatologic and Connective Tissue Disorders
1/91
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
92 Terms
What type of disorder is rheumatoid arthritis?
systemic autoimmune disorder
Rheumatoid arthritis is characterized by ---- inflammation of joints, especially of the hands, feet, and knees
What population is rheumatoid arthritis more present in?
Females
Rheumatoid arthritis is --- involving --- of the hands, feet, wrists, and ankles
symmetric polyarhthritis involving small
What is a morning symptoms associated with rheumatoid arthritis?
prolonged morning stiffness > 1hr
True / False: the TMJ is involved in rheumatoid arthritis
true
Rheumatoid arthritis results in --- deviation and --- deformatity
ulnar devaition
swan neck deformity
Rheumatoid Arthritis Diagnosis
morning stiffness
arthritis in 3 or more small joints
symmetric arthritis
rheumatoid nodules
serum rheumatoid factor
radiographic changes
Rheumatoid factor is positive in 85% of patient population with rheumatoid arthritis . Other elevated laboratory findings include --- and ---
ESR and C reactive protein
What are citrullinated proteins?
arginine in proteins is converted to being citrullinated
antibodies develop to citrullinated proteins
What syndrome is consistent with rheumatoid arthritis?
Sjorgen syndorme
What is a classic radiographic finding of rheumatoid arthritis?
erosion of small joints
True / False: there is a cure for rheumatoid arthritis
false - no cure
can control disease by reducing pain/inflammation, preserving function, and improve outcome
True / False: non-steroidal anti-inflammatory drugs and aspirin change the progression / limit rheumatoid arthritis continuation
false = do not change natural course of rheumatoid arthritis
What medications help change the natural course of rheumatoid arthritis?
disease modifying anti rheumatic drugs
---- slow down the damaging components of the rheumatoid arthritis disease process
disease modifying anti rheumatoid drugs
Examples of disease modifying anti-rheumatic drugs
methotrexate
anit-malarials
steroids
TNF-a inhibitors = etanercept / infliximab
What drugs used in the management of rheumatoid arthritis disorders increase infection risk?
Gold compounds (gold sodium thiomolate)
How long do symptoms have to last to be diagnosed with rheumatoid arthritis?
> 6 weeks
Osteoarthritis
degenerative joint disease
True / False: osteoarthritis has systemic manifestations
false
- rheumatoid arthritis has systemic manifestations
- osteoarthritis has local manifestations
What are the morning symptoms of osteoarthritis
brief morning stiffness
There is --- inflammation with osteoarthritis
minimal
In contrast with rheumatoid arthritis, osteoarthritis has a --- prognosis and less serious complications, depending on the joints involved
more favorable
The two most important complications associated with osteoarthritis are --- and ---
pain and disability
What joints does osteoarthritis affect?
Large joints = hips, feet, spines, hands, TMJ
What syndromes are associated with osteoarthritis?
Heberden's nodes = DIP joint
Bouchard nodes = PIP join
Heberdin's nodes refers to --- joint
DIP
Bouchard's nodes refers to --- joint
PIP
Radiographic diagnosis of osteoarthritis
joint space narrowing
ankylosis
remodeling = osteophytes and spurs
True / False: ESR and C reactive protein are elevated with osteoarthritis?
false = not a systemic inflammatory disease but a localized degenerative disease
Treatment of osteoarthritis
NSAIDS
steroid injections into joint
physical therapy
surgery
What is the first line treatment therapy for osteoarthritis?
NSADS and physical therapy
Which arthritis is surgery (joint replacement) a treatment option: rheumatoid arthritis or osteoarthritis?
osteoarthritis
What needs to be completed prior to joint surgery?
Dental examination / procedures
Increased risk of infection if dental infections are not addressed prior to joint surgery
Lupus Erythematosus types
Discoid
Systemic
Lupus Erythematosus Discoid predominantly affects ---
skin
Lupus Erythematosus Systemic predominantly affects ---
multiple organ systems
Lupus Erythematous is a --- disorder
auto-immune
Lupus erythematous systemic disorder has a female to male ratio of --- that rises to ---
3:1
10:1
What patient population is systemic lupus erythematous predominant in?
hispanics and African Americans
What happens in lupus erythermous systemic disorder
antibody and immune complex deposition results in inflammation / vasculopathy
What is a clinical presentation of lupus erythematous?
butterfly rash across nose/cheeks
Systemic lupus erythematous presents as ulcerations on the ---
buccal mucosa
What helps to different lupus erythematous from rheumatoid arthritis and osteoarthritis?
joint pain out of proportion to signs
non-deforming
What is an indicator of a poor prognosis of lupus erythematous?
renal abnormalities
What is associated with anti-phospholipid antibodies in systemic lupus erythematous?
thromboembolism
Libman Sacks endocarditis
nonbacterial verrous endocarditis on mitral valve
Libman Sacks endocarditis is a common finding associated with ---
systemic lupus erythematous
What is the best screening tool for lupus erythematous?
ANA = antinuclear antibody testing
True / False: anti-nuclear antibody testing is sensitive but not specific to systemic lupus erythematous
true
Lyme disease is a ---- disease caused by a tick borne spirochete ---
multi-inflammatory
borellia burgdorferi
What species carries Borrelia burgdorferi
Ixodes dammini
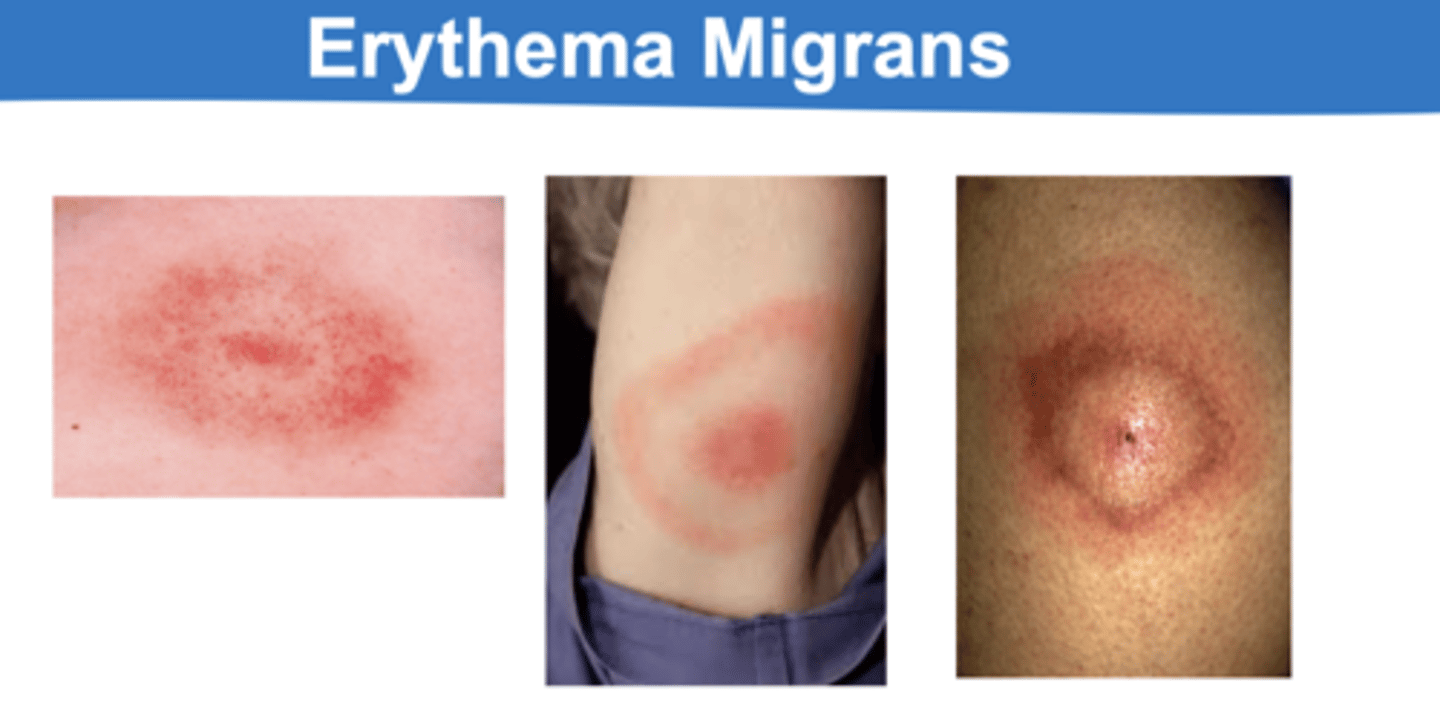
What is a classical patterns of Lyme disease is a characteristic macular skin rash called ---
erythema migrans
Where are deer ticks Ixodes Dammini found?
New York, Conneticut, Pennsylvania, Massachusetts, Rhode Island, New Jersey, Wisconsin, and Minnesota
What are the 3 stages of Lyme Disease:
early localized
early disseminated
late
Erythema migrans is a --- or --- lesion
target or bull
Ankylosing Spondylitis affects which young adult population?
Males
True / False: Lyme disease may or may not have erythema mirgrans (target/bull lesions)
true
What are the classifications of late disease of Lyme disease?
Musculoskeletal problems
Neurological problems
What is a common neurological symptoms of late lyme disease?
Fibromyalgia
True / False: late Lyme disease may not be preceded by earlier manifestations
true
Can Lyme disease be diagnosed with enzyme linked immunosorbent assay or western blot analysis on the early localized stages?
No relies on erythema migrans (target/bull lesion)
How to treat Lyme disease?
Doxycycline adults
Amoxicillin children
Scleroderma types
Limited: CREST SYNDROME
Diffuse
CREST syndrome
calcinosis
raynauds
esophageal dysfunction
scelrodactyl
telangiectasia
Scelerodactylyl
thickening of skin
Telangiectasia
small blood vessels grow near surface of the skin
Sjorgen Syndrome is a ---- disorder often associated with rheumatoid arthritis
auto-inflammatory
Sjorgen syndrome affects --- and --- glands
salivary and lacrimal
What is the triad of clinical conditions of Sjorgens syndrome?
Dry eyes
Dry mouth
Connective tissue disorder = rheumatoid arthritis
Sicca complex
dry eyes and dry mouth in Sjorgens syndrome
What is important in the treatment of sjorgens syndrome?
moisture and lubrication of salivary and lacrimal glands
treatment of secondary mucosal conditions
prevention of oral diseases
Mr. Jones presents with an abnormally highnumber of dental carries. He reports having increasingly dry eyes and mouth. He was recently diagnosed with rheumatoid arthritis.What is the most likely cause of his dental carries?
a) Systemic Lupus Erythematosus
b) Sjögren syndrome
c) Osteoarthritis
d) Fibromyalgia
b) Sjögren syndrome
--- is the most common cause of chronic pain in the US
fibromyalgia
What population does fibromyalgia primarily affect?
primarily woman
What are the clinical symptoms of fibromyalgia?
muscle pain
sleep disturbance
neuropathies
--- of the 18 points must be painful on application of only 4kg pressure
11
Successful management of FM requires a thorough analysis of patient's --- issues, including fatigue, sleep, pain, psychological distress etc.
biopsychosocial
What medications can be given for fibromyalgia?
amitryptyline
trazodone
nortriptyline
SSRI's
anticonvulsants such as gabapentin, topiramate, or pregabalin
True / False: opioids are an optimal treatment therapy for fibromyalgia
false = its a chronic pain and opioids should not be the first choice of therapy
Ehler Danlos Syndrome
---- is a regenerative injection therapy used to manage chronic TMJ dysfunction and pain, particularly when conservative treatments have failed.
Prolotherapy with 10% dextrose
What is the function behind prolotherapy with 10% dextrose
The hyperosmolar solution irritates the tissue, which can lead to strengthening of the joint capsule and ligaments, improved joint stability, and pain reduction over time
With fibromyalgia symptoms are --- and present for > -- months
Widespread
> 3 months
Amyloidosis
Group of diseases in which abnormal protein calledamyloid fibrils, builds up in tissue
What is the treatment for amyloidosis?
high dose chemotherapy
stem cell transplantation Ankylosing Spondylitis
Ankylosing Spondylitis
a form of rheumatoid arthritis that primarily causes inflammation of the joints between the vertebrae
Symptoms of ankylosing spondylitis is chronic pain and stiffness in the --- that usually develops slowly over several weeks or month
lower back, buttocks and hips
Ankylosing Spondylitis
90% of those affected have a specific human leukocyteantigen known as the ---- antigen
HLA-B27
What are treatment for Ankylosing Spondylitis
medication, exercise, and surgery
• Medications used: NSAIDs, steroids, DMARDs such as sulfasalazine, and biologic agents such as infliximab
True / False: There is no cure for ankylosing spondylitis
True